Abstract
Objectives
Mechanical loading is a potential activator of inflammation and able to stimulate factors for periodontal and alveolar bone destruction. Aim of this study was to investigate the inflammatory response and synthesis of proteinases by human periodontal ligament fibroblast (HPdLF) dependent on different strengths of static tensile strain (STS).
Materials and methods
HPdLFs were loaded with different STS strengths (1, 5, and 10 %) in vitro. Gene expressions of cyclooxygenase (COX)-2 and interleukin (IL)-6 were analyzed by quantitative real-time polymerase chain reaction. Production of IL-6, prostaglandin E2 (PGE2), matrix metalloproteinase (MMP)-8, and tissue inhibitors of matrix metalloproteinase (TIMP)-1 were measured by enzyme-linked immunosorbent assay. Receptor activator of nuclear factor-kappa ligand (RANKL) synthesis was detected by immunocytochemical staining.
Results
Ten percent STS led to an increased gene expression of IL-6 and COX-2 (34.4-fold) in HPdLF, and 1 and 5 % STS slightly reduced the gene expression of IL-6. Synthesis of IL-6 was significantly reduced by 1 % STS and stimulated by 10 % STS. Ten percent STS significantly induced PGE2 production. RANKL was not detectable at any strength of STS. MMP-8 synthesis showed significantly higher values only at 10 % STS, but TIMP-1 was stimulated by 5 and 10 % STS, resulting into highest TIMP-1/MMP-8 ratio at 5 % STS.
Conclusions
High-strength STS is a potent inducer of periodontal inflammation and MMP-8, whereas low-strength STS shows an anti-inflammatory effect. Moderate-strength STS causes the highest TIMP-1/MMP-8 ratio, leading to appropriate conditions for reformation of the extracellular matrix.
Clinical relevance
Furthermore, this study points out that the strength of force plays a pivotal role to achieve orthodontic tooth movement without inducing periodontal inflammation and to activate extracellular matrix regeneration.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Tensile forces applied to the tooth during orthodontic therapy are transmitted to the periodontal ligament (PDL), which is composed of cellular and extracellular components. The predominant cell types such as human periodontal ligament fibroblasts (HPdLFs) and undifferentiated mesenchymal and epithelial cells are then exposed to a tensile strain [1].
Parodontitis represents a multifactorial inflammatory disease that can cause the destruction of periodontal ligament. When stimulated by microorganisms and products of the subgingival biofilm, the production of inflammatory molecules such as interleukin (IL)-6, cyclooxygenase (COX)-2, and prostaglandin E2 (PGE2) by infiltrating immunoinflammatory and resident cells of the periodontium initiates and perpetuates soft tissue degradation and bone resorption [2–4].
The mechanical forces during orthodontic therapy can also cause an increased production of these cytokines by the PDL cells [5, 6]. This is called aseptic inflammation because these cytokines are usually caused by an inflammation associated with a bacterial component. However, the effect of these cytokines is the same as during inflammation. They attract macrophages and promote their differentiation to osteoclasts, leading to bone resorption [7].
The receptor activator of the nuclear factor-kappa ligand (RANKL) is an important activator for bone and root resorption via osteoclast activation. RANKL is known to be upregulated in different cells by inflammation or mechanical loading, especially due to compressive forces [8–10].
Matrix metalloproteinases (MMPs) play a central role in PDL remodeling both physiologically and pathologically due to their ability to cleave native triple-helical interstitial collagens. Active remodeling of PDL must occur in order to cope with orthodontic force and mechanical loading during orthodontic treatment. It is known that orthodontic forces upregulate the production of MMP-1 and MMP-8, particularly on the compression site of tooth movement [11].
In contrast, tissue inhibitors of matrix metalloproteinases (TIMPs) are endogenous inhibitors of matrix degradation by binding to active MMPs, downregulating their activity, and help to regenerate the extracellular matrix on the tension site of tooth movement [12].
During orthodontic treatment, cyclic forces are applied to the teeth by a multibracket appliance overlaid with occlusal forces. These forces are simulated in vitro by cyclic tensile strain [13]. Modern materials as nickel titanium coil springs are able to provide continuous forces during tooth movement [14, 15]. These continuous forces lead to a static tensile strain in the PDL. The cellular response to tensile strain depends on the magnitude, frequency, and type of the tensile strain imposed. The effect of cyclic tensile strain on the expression of inflammatory molecules and MMPs has been demonstrated using different cell types [16, 17]. However, few reports have examined the correlation between different strengths of cyclic tensile strain and the cellular activity of PDL cells, including inflammation cytokines and extracellular matrix metabolism [18, 19]. The relationship between static tensile strain (STS) and the development of periodontal inflammation and the synthesis of MMPs and TIMPs by HPdLF is not yet known, particularly with respect to varying STS strengths.
The aim of this in vitro study was, therefore, to investigate whether the production of the inflammatory cytokines IL-6, PGE2, RANKL, or the proteinase MMP-8 and its controller TIMP-1 by HPdLF is dependent on the STS strength.
Material and methods
Cell culture
Cell cultures were prepared and maintained according to standard cell culture procedures. Commercially available HPdLFs (Lonza, Basel, Schweiz) were maintained in the Dulbecco's modified Eagle's medium (DMEM; Invitrogen, Carlsbad, USA) containing 10 % FCS, 1 % l-glutamine, and 1 % penicillin/streptomycin/neomycin. The cells were cultured in an incubator with 5 % CO2 and 95 % air at 37 °C. Cells were passaged at regular intervals depending on their growth characteristics using 0.05 % trypsin–EDTA solution (PAA, Pasching, Austria). Cells were used for experiments at passages 4 to 6.
Tensile strain devices
As an experimental model of mechanical stretch, HPdLFs were seeded at a density of 1.0 × 105 cells/well on six-well flexible-bottomed plates coated with pronectin (Bioflex® plates; Flexcell International Corporation, Hillsborough, USA) and cultured in supplemented DMEM. Pronectin provides optimal cell adhesion and simulates interaction of extracellular matrix proteins with integrin receptors of the cells [20]. After 2 days for cell attachment, spread and growth to a subconfluence medium was replaced by a medium as described above, but without fetal calf serum (starvation medium). A Flexercell Strain Unit (Modell FX 3000, Dunn Labortechnik GmbH, Asbach, Germany), which is capable of controlling the magnitude, type, and frequency of cell deformation, was used to generate STS in cells. This unit was placed in a humidified atmosphere of 5 % CO2 and 95 % air at 37 °C, and a vacuum was applied across the plate surface according to instructions provided by the manufacturer. Cells were subjected to STS of 1 % (0.7 cN/mm2), 5 % (3 cN/mm2), and 10 % (5.2 cN/mm2) for 12 h to simulate low, moderate, and high forces.
Messenger RNA extraction and reverse transcriptase polymerase chain reaction
Cells were detached with 0.05 % trypsin–EDTA solution directly after stretching and were individually harvested. Messenger RNA (mRNA) was isolated using the peqGOLD Total RNA Kit (peqLab Biotechnologie Gmbh, Erlangen, Germany). This included a DNAse digestion step. Both the quantity (260 nm) and quality (ratio, 260/280 nm) of the RNA were determined by using the NanoDrop Spectrophotometer ND-100 (peqLab Biotechnologie Gmbh, Erlangen, Germany). Reverse transcription of RNA (100 ng) was performed by standard protocols with GeneAmp PCR System 2400 (Perkin Elmer, Massachusetts, USA) and iScript cDNA Synthesis Kit (Bio-Rad Laboratories, Hercules, USA) in a total volume of 20 μl.
COX-2 and IL-6 primers (Eurofins MWG Operon, Ebersberg, Germany) were designed using the NCBI nucleotide library and primer3 design to detect the mRNA levels (Table 1). The primers had been matched to the mRNA sequences of the target genes (NCBI Blast Software).
As housekeeping genes, actin and glyceraldehyde-3-phosphate dehydrogenase (GAPDH) were evaluated. We were able to show the most stable expression for the actin and GAPDH by comparing the stretched versus non-stretched cells using specialized freeware called GeNorm.
Quantitative real-time polymerase chain reaction (PCR) was performed with the IQ5 I-Cycler and IQ5 Optical System software version 2.0 (Bio-Rad Laboratories, Hercules, USA) according to the manufacturer's instructions, which included an initial denaturation at 95 °C, annealing temperature of 56 °C, and an elongation temperature of 71 °C over 40 cycles. q-PCR amplification was conducted with a reaction mixture containing SYBR Green Supermix (Bio-Rad Laboratories, Hercules, USA), an appropriate amount of paired primers, and 2 μl template cDNA; the background was to determine the threshold at the SYBR Green fluorescence curve at the exponential part. This method was applied to calculate the cycle number and cycle threshold (C T) value for quantitation. Furthermore, the C T values of actin and GAPDH as housekeeping genes and the individual primer efficacy were taken into account. Single product formation was confirmed by melting point analysis. Data were obtained from three individual experiments and normalized to the C T of actin and GAPDH. CDNA from individual cell experiments was analyzed in triplicate PCR. The relative expression levels of each mRNA were evaluated by using a modification of the ΔΔC T method [21].
Enzyme-linked immunosorbent assay
The production of IL-6, PGE2, MMP-8, and TIMP-1 was measured in supernatants using the Human DuoSet IL-6 ELISA Development System, the Human DuoSet PGE2 ELISA Development System, the Human DuoSet MMP-8 ELISA Development System, and the Human DuoSet TIMP-1 ELISA Development System (R&D Systems, Inc., Minneapolis, USA) according to the manufacturers' instructions using a microplate reader (Metertech, Inc., Taipei, Taiwan). The assays were performed in triplicate.
Immunocytochemical staining
To illustrate the localization of RANKL after stretching procedure, HPdLFs were fixed with methanol/acetone (1:1) at −20 °C for 10 min. Cells were blocked with 0.25 % casein/0.1 % bovine serum albumin (BSA) for 30 min at room temperature. The antibody against RANKL (FL-317, 1:50 diluted in phosphate-buffered saline (PBS) with 1 % BSA, rabbit antihuman; Santa Cruz Biotech, Heidelberg, Germany) was incubated overnight at 4 °C. Staining was visualized by using a serum (goat anti-rabbit) IgG (H + L) conjugated with Alexa 594 for 45 min (1:50 diluted in PBS with 1 % BSA; Life Technologies, Darmstadt, Germany). Counterstaining (nuclear staining) was performed with 4′,6-diamidine-2-phenylindole (DAPI) for 5 min. HPdLFs were incubated with IL-1β (10 ng/ml) for 24 h as a positive control, which is known to stimulate RANKL expression [8, 22]. Photomicrographs of immunofluorescent staining were made using the Keyence fluorescence microscope (BZ-9000; Keyence, Osaka, Japan).
Statistical analysis
SPSS 19.0 (IBM-SPSS, Ehningen, Germany) was used for statistical analyses. To detect any difference between the groups, one-way ANOVA was used with the post hoc Tukey test. A p value of <0.05 was considered statistically significant.
cDNA from individual cell experiments was analyzed in triplicate PCR. The relative expression levels of each mRNA were evaluated by using a modification of the ΔΔC T method. The mean values and standard deviations were calculated using IQ5 Software (Bio-Rad Laboratories, Hercules, USA). Each time point for relative mRNA is noted as the mean ± standard deviation. Results from immunocytochemical staining were analyzed by descriptive statistics.
Results
Effects of STS on gene expression of IL-6 and COX-2
The key regulator gene of inflammation COX-2 showed a 31.4-fold upregulation compared to the unstretched control cells at 10 % STS (p < 0.001); 1 and 5 % STS did not cause an increased gene expression compared to the unstretched control cells (Fig. 1).
Quantitative RT-PCR results for inflammation regulator genes cyclooxygenase-2 (COX-2) and interleukin-6 (IL-6) in HPdLFs, analyzed after 12 h of STS at strengths of 1, 5, or 10 % relative to control cells (0 %) (means ± SD). An asterisk represents a significant difference between this value and the control (p < 0.05)
Gene expression of the cytokine IL-6 increased at 10 % STS, whereas 1 and 5 % STS caused a halving of IL-6 gene expression (Fig. 1).
Effects of STS on PGE2, IL-6, and RANKL production
The production of PGE2 and IL-6 was detected in supernatants. HPdLF produced undetectable levels of PGE2 when remaining unstretched or at 1 % STS, and low levels were produced at 5 % STS (2.6 pg/ml). Ten percent STS stimulated the production of PGE2 significantly to more than 47.9 pg/ml (p ≤ 0.001; Fig. 2).
Prostaglandin E2 (PGE 2 ) and interleukin-6 secretion in supernatant liquor of HPdLFs, analyzed after 12 h of STS at strengths of 1, 5, or 10 % relative to control cells (0 %) as measured by ELISA. Data are given in picogram per milliliter. The black bar in the middle of each box represents the median. The box includes all values between the 25th and 75th percentiles. Whiskers indicate values still within the 1.5 interquartile range. An asterisk represents a significant difference between the values under the lines
HPdLF showed a significant decrease in IL-6 production at 1 % STS compared to unstretched control cells (5.6 vs. 9.5 pg/ml, p ≤ 0.005). Five percent STS led to an unchanged IL-6 production, but 10 % STS increased the IL-6 production of HPdLF significantly to 13.8 pg/ml (p ≤ 0.005; Fig. 2).
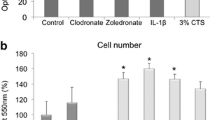
RANKL was not detectable at immunocytochemical staining after application of any strength of STS. RANKL was only detectable in the positive control composed of HPdLF after stimulation with the proinflammatory cytokine IL-1β for 24 h, which is known to increase RANKL protein synthesis (Fig. 3).
The expression of receptor activator of the nuclear factor-kappa ligand (RANKL) was demonstrated on the protein level using immunofluorescence (red). Nuclei were counterstained using DAPI (blue). Positive control shows detectable RANKL in the cytoplasm of HPdLF after stimulation with IL-1β (10 ng/ml) for 24 h. HPdLF as control (no stretch) and after application of static mechanical strain (STS) of 1, 5, and 10 % did not show any detectable RANKL
Effects of STS on MMP-8 and TIMP-1 production
Constitutive production of MMP-8 was very low (3.2 pg/ml) and did not increase at 1 or 5 % STS. Ten percent STS, however, significantly increased MMP-8 production of HPdLF from 3.2 to 38.8 pg/ml (p ≤ 0.001; Fig. 4).
a Matrix metalloproteinase 8 (MMP-8) and tissue inhibitor of matrix-metalloproteinase-1 (TIMP-1) secretion in supernatant liquor of HPdLFs, analyzed after 12 h of STS at strengths of 1, 5, or 10 % relative to control cells (0 %) measured by ELISA. Data are given in picogram or nanogram per milliliter. b TIMP-1/MMP-8 ratio. The black bar in the middle of each box represents the median. The box includes all values between the 25th and 75th percentiles. Whiskers indicate values still within the 1.5 interquartile range. An asterisk represents a significant difference between the values under the lines
According to the MMP-8 levels, HPdLF showed low concentrations of TIMP-1 when remaining unstretched (18.9 ng/ml) and at 1 % STS (17.9 ng/ml). However, 5 % STS caused a significant increase in TIMP-1 production to 54.5 ng/ml, which was enhanced at 10 % STS to 71.2 ng/ml (p ≤ 0.002). TIMP-1/MMP-8 ratio was highest at 5 % STS (Fig. 4).
Discussion
This study investigated for the first time the effect of different strengths of STS on the expression and production of inflammation cytokines and proteinases by HPdLF. STS in vitro corresponds with the continuous force applied to the tooth in vivo, e.g., by modern materials like nickel titanium coil springs during orthodontic tooth movement [14, 23].
We were able to show an increased gene expression of COX-2 and IL-6 at 10 % STS, accompanied by changes in the PGE2 and IL-6 protein production as a pro-inflammatory response. One percent STS, however, led to a decreased gene expression of IL-6 and its protein production, indicating an anti-inflammatory effect of low-strength STS. Long et al. investigated the effect of cyclic tensile strain on human periodontal ligament cells in vitro, which mimics occlusal forces or forces applied by a multibracket appliance in vivo. They found an anti-inflammatory effect of cyclic strain with low magnitude, corresponding with our results for STS [18].
Another study analyzed the COX-2, MMP-1 expression, and PGE2 production in human patellar tendon fibroblasts when applied to repetitive mechanical stretching. The authors also described an anti-inflammatory effect of 4 % stretching, whereas 8 % of stretching led to an increased expression and production of COX-2, MMP-1, and PGE2 [24]. These and our results show that a tensile strain, regardless of whether it is cyclic or static, has a potential pro- or anti-inflammatory effect on different types of fibroblasts, depending on the strength of the strain.
It is important to know whether inflammation and orthodontic strain impair the bone regeneration on the tension site of tooth movement. Nokhbehsaim et al. analyzed the contribution of tensile strain and IL-1β to inflammation-mediated periodontal destruction. They concluded that the tensile strain and the presence of inflammation do not lead to an augmentation of the periodontal inflammation, but to a downregulation of matrix and osteogenic proteins [19].
PGE2 at high dose is known to stimulate receptor activator of nuclear factor kappa-B ligand gene expression, which activates osteoclast differentiation, leading to bone and root resorption [25]. RANKL was not increased by any strength of STS, indicating that a tensile strain does not directly induce RANKL synthesis in a strength-dependent manner as it is known for compressive forces [8, 26]. The limit of our study was the use of an in vitro model with a commercially available cell line, which is an established experimental setting but cannot imitate the in vivo situation of the periodontal ligament completely [27]. Grant et al., however, analyzed RANKL levels in the gingival crevicular fluid of patients during orthodontic treatment. As consistent with our in vitro results, they could also not detect an increased RANKL level in vivo at tension sites [28], but the increased synthesis of PGE2 at 10 % STS might lead to an increase of RANKL at a later point of time. So, high levels of PGE2 at the tension site of tooth movement are not desirable because they might interfere the apposition of new alveolar bone.
It has been demonstrated that MMPs and TIMPs regulate matrix degradation. The balance between the activities of MMPs in degradation of the extracellular matrix and TIMPs, who control their activity, is believed to determine the rate of this process [26, 29, 30]. Our data showed that 10 % STS stimulated the synthesis of MMP-8 by HPdLF, which might induce the degradation of the extracellular matrix. Analyzing TIMP-1 synthesis showed that TIMP-1 was stimulated by STS of 5 and 10 %. The related increased synthesis of TIMP-1 at 10 % STS indicates that high forces do not degrade the extracellular matrix, because TIMP-1 binds to activated MMP-8 and inhibits its activity. Thus, 10 % STS rather induces a high alteration of the extracellular matrix.
Another study investigated the expression of MMP-13 and TIMP-1 in mouse osteoblast cells when applied to cyclic tensile strain and found a magnitude-dependent increase of MMP-13 and TIMP-1 mRNA and protein levels starting at 6 % of elongation [16]. This study and our study can conclude that both cyclic and static tensile strains lead to a strength-dependent increase of MMPs related with an increase of TIMPs, resulting in an alteration, but not degradation of the extracellular matrix.
More important for the tension site of orthodontic tooth movement is the reformation of the extracellular matrix, which is promoted by TIMP-1 and its ratio to MMP-8. TIMP-1/MMP-8 ratio was highest at 5 % STS, providing favorable conditions for apposition of the extracellular matrix at the tension site of tooth movement. Grant et al. [28] and Bildt et al. [31] analyzed the expression of MMPs and TIMP-1 in humans at different time points during tooth movement in vivo. They both found a strong increase of TIMP-1 on the tension site of tooth movement, indicating an important role of TIMP-1 in promoting apposition of the extracellular matrix at the tension site in vivo.
Bildt et al. also described elevated levels of MMP-1, MMP-2, and MMP-9, but not of MMP-8 [31]. Ingman et al., however, detected MMP-8 in the gingival crevicular fluid of orthodontic patients [32]. They concluded that different types of analysis methods might be responsible for the varying results. Our in vitro results give evidence that different strengths of force applied to the patients might be responsible for the varying results of the in vivo studies.
Conclusion
These findings point out potential stimulation of pro-inflammatory cytokine production and MMP-8 synthesis in periodontal fibroblasts at high-strength STS. However, low-strength STS shows an anti-inflammatory effect. The highest TIMP-1/MMP-8 ratio was found at 5 % STS, indicating the best conditions for an increase of the extracellular matrix on the tension site of tooth movement. The right strength of mechanical strain plays a pivotal role to avoid aseptic inflammation during orthodontic treatment and to activate extracellular matrix regeneration.
References
Khatib H, Berkovitz D, Ratz T, Plotzki Y, Fainsod A, Gruenbaum Y (1995) Mapping the CdxA gene to a new linkage group in chicken. Anim Genet 26(3):211
Belibasakis GN, Guggenheim B (2011) Induction of prostaglandin E(2) and interleukin-6 in gingival fibroblasts by oral biofilms. FEMS Immunol Med Microbiol 63(3):381–386. doi:10.1111/j.1574-695X.2011.00863.x
Liu YC, Lerner UH, Teng YT (2000) (2010) Cytokine responses against periodontal infection: protective and destructive roles. Periodontol 52(1):163–206. doi:10.1111/j.1600-0757.2009.00321.x
Lerner UH (2006) Inflammation-induced bone remodeling in periodontal disease and the influence of post-menopausal osteoporosis. J Dent Res 85(7):596–607
Ren Y, Vissink A (2008) Cytokines in crevicular fluid and orthodontic tooth movement. Eur J Oral Sci 116(2):89–97. doi:10.1111/j.1600-0722.2007.00511.x
Saito M, Saito S, Ngan PW, Shanfeld J, Davidovitch Z (1991) Interleukin 1 beta and prostaglandin E are involved in the response of periodontal cells to mechanical stress in vivo and in vitro. Am J Orthod Dentofac Orthop 99(3):226–240
Nakamura K, Sahara N, Deguchi T (2001) Temporal changes in the distribution and number of macrophage-lineage cells in the periodontal membrane of the rat molar in response to experimental tooth movement. Arch Oral Biol 46(7):593–607
Diercke K, Kohl A, Lux CJ, Erber R (2012) IL-1beta and compressive forces lead to a significant induction of RANKL-expression in primary human cementoblasts. J Orofac Orthop 73(5):397–412. doi:10.1007/s00056-012-0095-y
Kanzaki H, Chiba M, Shimizu Y, Mitani H (2002) Periodontal ligament cells under mechanical stress induce osteoclastogenesis by receptor activator of nuclear factor kappaB ligand up-regulation via prostaglandin E2 synthesis. J Bone Miner Res 17(2):210–220. doi:10.1359/jbmr.2002.17.2.210
Li Y, Zheng W, Liu JS, Wang J, Yang P, Li ML, Zhao ZH (2011) Expression of osteoclastogenesis inducers in a tissue model of periodontal ligament under compression. J Dent Res 90(1):115–120. doi:10.1177/0022034510385237
Apajalahti S, Sorsa T, Railavo S, Ingman T (2003) The in vivo levels of matrix metalloproteinase-1 and -8 in gingival crevicular fluid during initial orthodontic tooth movement. J Dent Res 82(12):1018–1022
Lambert E, Dasse E, Haye B, Petitfrere E (2004) TIMPs as multifacial proteins. Crit Rev Oncol Hematol 49(3):187–198. doi:10.1016/j.critrevonc.2003.09.008
Nokhbehsaim M, Deschner B, Winter J, Bourauel C, Jager A, Jepsen S, Deschner J (2012) Anti-inflammatory effects of EMD in the presence of biomechanical loading and interleukin-1beta in vitro. Clin Oral Investig 16(1):275–283. doi:10.1007/s00784-010-0505-8
Brauchli LM, Senn C, Ball J, Wichelhaus (2011) A Force levels of 23 nickel-titanium open-coil springs in compression testing. Am J Orthod Dentofac Orthop 139(5):601–605. doi:10.1016/j.ajodo.2009.06.033
Rozman J, Mrvar P, Drevensek M, Peclin P (2010) Evaluation of NiTi Superelastic Retraction Coil Springs for orthodontic tooth movement in rats. Biomed Mater Eng 20(6):339–348. doi:10.3233/BME-2010-0647
Li Y, Tang L, Duan Y, Ding Y (2010) Upregulation of MMP-13 and TIMP-1 expression in response to mechanical strain in MC3T3-E1 osteoblastic cells. BMC Res Notes 3:309. doi:10.1186/1756-0500-3-309
Saito S, Ngan P, Rosol T, Saito M, Shimizu H, Shinjo N, Shanfeld J, Davidovitch Z (1991) Involvement of PGE synthesis in the effect of intermittent pressure and interleukin-1 beta on bone resorption. J Dent Res 70(1):27–33
Long P, Hu J, Piesco N, Buckley M, Agarwal S (2001) Low magnitude of tensile strain inhibits IL-1beta-dependent induction of pro-inflammatory cytokines and induces synthesis of IL-10 in human periodontal ligament cells in vitro. J Dent Res 80(5):1416–1420
Nokhbehsaim M, Deschner B, Winter J, Reimann S, Bourauel C, Jepsen S, Jager A, Deschner J (2010) Contribution of orthodontic load to inflammation-mediated periodontal destruction. J Orofac Orthop 71(6):390–402. doi:10.1007/s00056-010-1031-7
Somamoto S, Tabata Y (2013) Effect of ProNectin F derivates on cell attachment and proliferation. Acta Biomater 9(2):5194–5200. doi:10.1016/j.actbio.2012.07.039
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(-delta delta C(T)) method. Methods 25(4):402–408. doi:10.1006/meth.2001.1262
Stein SH, Dean IN, Rawal SY, Tipton DA (2010) Statins regulate interleukin-1beta-induced RANKL and osteoprotegerin production by human gingival fibroblasts. J Periodontal Res 46(4):483–490. doi:10.1111/j.1600-0765.2011.01364.x
Diercke K, Kohl A, Lux CJ, Erber R (2011) Strain-dependent up-regulation of ephrin-B2 protein in periodontal ligament fibroblasts contributes to osteogenesis during tooth movement. J Biol Chem 286(43):37651–37664. doi:10.1074/jbc.M110.166900
Yang G, Im HJ, Wang JH (2005) Repetitive mechanical stretching modulates IL-1beta induced COX-2, MMP-1 expression, and PGE2 production in human patellar tendon fibroblasts. Gene 363:166–172. doi:10.1016/j.gene.2005.08.0069
Ramirez-Yanez GO, Symons AL (2012) Prostaglandin E2 affects osteoblast biology in a dose-dependent manner: an in vitro study. Arch Oral Biol 57(9):1274–1281. doi:10.1016/j.archoralbio.2012.03.003
Nakashima A, Tamura M (2006) Regulation of matrix metalloproteinase-13 and tissue inhibitor of matrix metalloproteinase-1 gene expression by WNT3A and bone morphogenetic protein-2 in osteoblastic differentiation. Front Biosci 11:1667–1678
Marchesan JT, Scanlon CS, Soehren S, Matsuo M, Kapila YL (2013) Implications of cultured periodontal ligament cells for the clinical and experimental setting: a review. Arch Oral Biol 56(10):933–943. doi:10.1016/j.archoralbio.2011.03.003
Grant M, Wilson J, Rock P, Chapple I (2012) Induction of cytokines, MMP9, TIMPs, RANKL, and OPG during orthodontic tooth movement. Eur J Orthop. doi:10.1093/ejo/cjs057
Uchida M, Shima M, Shimoaka T, Fujieda A, Obara K, Suzuki H, Nagai Y, Ikeda T, Yamato H, Kawaguchi H (2000) Regulation of matrix metalloproteinases (MMPs) and tissue inhibitors of metalloproteinases (TIMPs) by bone resorptive factors in osteoblastic cells. J Cell Physiol 185(2):207–214. doi:10.1002/1097-4652(200011)
Onodera S, Nishihira J, Iwabuchi K, Koyama Y, Yoshida K, Tanaka S, Minami A (2002) Macrophage migration inhibitory factor up-regulates matrix metalloproteinase-9 and -13 in rat osteoblasts. Relevance to intracellular signaling pathways. J Biol Chem 277(10):7865–7874. doi:10.1074/jbc.M106020200
Bildt MM, Bloemen M, Kuijpers-Jagtman AM, Von den Hoff JW (2009) Matrix metalloproteinases and tissue inhibitors of metalloproteinases in gingival crevicular fluid during orthodontic tooth movement. Eur J Orthod 31(5):529–535. doi:10.1093/ejo/cjn127
Ingman T, Apajalahti S, Mantyla P, Savolainen P, Sorsa T (2005) Matrix metalloproteinase-1 and -8 in gingival crevicular fluid during orthodontic tooth movement: a pilot study during 1 month of follow-up after fixed appliance activation. Eur J Orthod 27(2):202–207. doi:10.1093/ejo/cjh097
Acknowledgments
We thank Dr. Jutta Goldschmidt, Ute Zerfass, and Lotte Groothusen for their assistance in the laboratory and Katherine Taylor for orthographic correction of the article.
Conflict of interest
The authors declare that no competing financial interest exists.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jacobs, C., Walter, C., Ziebart, T. et al. Induction of IL-6 and MMP-8 in human periodontal fibroblasts by static tensile strain. Clin Oral Invest 18, 901–908 (2014). https://doi.org/10.1007/s00784-013-1032-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-013-1032-1