Abstract
A growing body of evidence indicates that creatine (Cr) exerts beneficial effects on a variety of pathologies where energy metabolism and oxidative stress play an etiological role. However, the benefits of Cr treatment for epileptics are still shrouded in controversy. In the present study, we found that acute Cr treatment (300 mg/kg, p.o.) prevented the increase in electroencephalographic wave amplitude typically elicited by PTZ (30, 45 or 60 mg/kg, i.p.). Cr treatment also increased the latency periods of first myoclonic jerks, lengthened the latency periods of the generalized tonic–clonic seizures and reduced the time spent in the generalized tonic–clonic seizures induced by PTZ (60 mg/kg). Administration of PTZ (all doses) decreased Na+, K+-ATPase activity as well as adenosine triphosphate (ATP) and adenosine diphosphate levels in the cerebral cortex, but Cr treatment prevented these effects. Cr administration also prevented increases in xanthine oxidase activity, adenosine monophosphate levels, adenosine levels, inosine levels and uric acid levels that normally occur after PTZ treatment (60 mg/kg, i.p.). We also showed that Cr treatment increased the total Cr (Cr + PCr) content, creatine kinase activity and the mitochondrial membrane potential (ΔΨ) in the cerebral cortex. In addition, Cr prevented PTZ-induced mitochondrial dysfunction characterized by decreasing ΔΨ, increasing thiobarbituric acid-reactive substance levels and increasing protein carbonylation. These experimental findings reinforce the idea that mitochondrial dysfunction plays a critical role in models of epileptic seizures and suggest that buffering brain energy levels through Cr treatment may be a promising therapeutic approach for the treatment of this neurological disease.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Creatine (Cr; N-[aminoiminomethyl]-N-methyl glycine) is a guanidine compound synthesized from glycine, arginine and S-adenosylmethionine in the kidneys, liver, pancreas, testis and brain (Wyss and Kaddurah-Daouk 2000). Its administration increases intracellular stores of both Cr and its phosphorylated form, phosphorylcreatine (PCr), in several tissues including skeletal muscle and the brain (Ipsiroglu et al. 2001; Royes et al. 2006). Due to its role in spatial and temporal energetic buffering, Cr has become one of the most common nutritional supplements taken for improvement of athletic performance (Kraemer and Volek 1999).
Experimental and clinical studies have indicated that chronic Cr supplementation provides neuroprotective effects against several neurological disorders, including Alzheimer’s, Parkinson’s disease, Huntington’s disease, brain ischemia and traumatic brain injury (Adhihetty and Beal 2008, Klein and Ferrante 2007). Furthermore, we have shown that acute administration of Cr protects against seizures induced by methylmalonic (Royes et al. 2003, 2006) and glutaric acids (Magni et al. 2007), suggesting an anticonvulsant role for this guanidine compound in experimental models of inborn metabolism errors that present as epileptic phenotypes.
Although there is increasing evidence supporting the use of Cr in the treatment of several neurological diseases, the potential benefits of this compound for patients with convulsive disorders remain poorly defined. While some authors suggest a proconvulsant role of chronic Cr treatment (Mikati et al. 2004; Vielhaber et al. 2003), others suggest that Cr may be an anticonvulsant agent (Rambo et al. 2009). The basis for this discrepancy is unknown; however, methodological differences may account for the apparent disagreement between findings. Important methodological considerations that may have impacted the results of various studies include the convulsant agents administered, the drug doses studied, the administration routes, the animal model species and the parameters evaluated.
Convulsive disorders increase brain energy consumption, and maintenance of energy homeostasis requires a distinct molecular circuitry that provides tight coupling between energy consumption and production (Fox et al. 1988; Jost et al. 2002). As expected under this model, PTZ-induced seizures lead to an increase in local cerebral glucose, a higher creatine kinase (CK) rate constant, increased cellular energy (ATP) utilization and higher ATP turnover (Bonan et al. 2000; Holtzman et al. 1998). Thus, epilepsy is related to a pathological increase in energy demand, mitochondrial dysfunction, decreased ATP levels, alteration of neuronal Ca2+ homeostasis, generation of reactive oxygen species (ROS) and ROS-induced modifications of ion channels (Folbergrova and Kunz 2011).
Neuronal hyperactivity and increased energy consumption are common findings in excitotoxic conditions (Carmody and Brennan 2010), and the Cr-PCr/CK/ATP system may play an important role in the maintenance of ATP levels at sites of ATP consumption, such as Na+, K+-ATPase. As a result, more detailed studies are required to assess the anticonvulsant potential of acute Cr administration in diseases that present epileptic phenotypes and to elucidate the underlying molecular mechanisms of Cr activity. For this purpose, we evaluated the effects of acute Cr administration on PTZ-induced electrographic, oxidative (TBARS; protein carbonylation; XO activity) and neurochemical alterations [uric acid levels, purine levels, Na+, K+-ATPase activity, CK activity and mitochondrial membrane potential (ΔΨ)] in the rat cerebral cortex.
Methods
Animals and reagents
Adult male Wistar rats (270–300 g) that were maintained under a controlled environment (12:12 h light–dark cycle, 24 ± 1 °C, 55 % relative humidity) with free access to food (Guabi, Santa Maria, Brazil) and water were used in this study. Animal utilization protocols conformed to the Official Government Ethics guidelines and were approved by the University Ethics Committee (#115/2010). All reagents were purchased from Sigma (St. Louis, MO, USA).
Drug administration protocol and behavioral evaluation
Naïve animals were transferred to a round open field (54.7 cm in diameter) and habituated for 20 min before drug administration. After the habituation period, the animals were treated with Cr (300 mg/kg, p.o.) or its vehicle (1 % carboxymethylcellulose, CMC, p.o.) by intragastric gavage, and PTZ (30, 45 or 60 mg/kg, i.p.) or its vehicle (0.9 % NaCl, i.p.) was administered 45 min later. The latency period for the appearance of clonic and generalized tonic–clonic seizures and the time spent in generalized tonic–clonic seizures were recorded over the 20-min period after PTZ injection. All drug doses used in the present study were selected based on previous work by our group (Magni et al. 2007; Souza et al. 2009).
Surgical procedures
A subset of the animals were surgically implanted with electrodes under stereotaxic guidance. In brief, animals were anesthetized with Equitesin (1 % phenobarbital, 2 % magnesium sulfate, 4 % chloral hydrate, 42 % propylene glycol, 11 % ethanol; 3 ml/kg, i.p.) and placed in a rodent stereotaxic apparatus. Under stereotaxic guidance, animals had two screw electrodes placed bilaterally over the parietal cortex (coordinates from bregma, in mm: AP, −4.5; L, 2.5) along with a ground lead positioned over the nasal sinus (Paxinos and Watson 1986). The electrodes were connected to a multipin socket and were fixed to the skull with dental acrylic cement. Chloramphenicol (200 mg/kg, i.p.) was administrated immediately before the surgical procedure. After surgery, all rats received a single s.c. injection of 0.01 mg/kg buprenorphine hydrochloride for amelioration of pain. Electroencephalographic recordings were performed 7 days after the surgery.
EEG recording, analyses and seizure evaluation
Seizures were monitored in animals by electroencephalographic recording. The rats were allowed to settle for habituation in a Plexiglas cage (25 × 25 × 60 cm) for at least 20 min. Rats were then connected to the lead socket on a swivel inside a Faraday’s cage. Routinely, a 10-min baseline recording was obtained to establish an adequate control period. The effect of oral administration of Cr on the seizure activity induced by PTZ was investigated by administrating Cr (300 mg/kg, p.o.) or its vehicle (1 % carboxymethylcellulose, p.o.) 45 min before an injection of PTZ (30, 45 or 60 mg/kg, i.p.). The behavior of the animals was monitored, and EEG was concomitantly recorded using a digital encephalographer (Neuromap EQSA260, Neurotec LTDA, Brazil). EEG signals were amplified, filtered (0.1–70.0 Hz, bandpass; 60 Hz, Notch), digitalized (sampling rate 256 Hz) and stored on a PC for off-line analysis. EEG recordings were visually analyzed for the appearance of seizure activity. Seizures were defined by the occurrence of episodes consisting of alterations in the recording leads, according to McColl et al. (2003). Digitalized data from basal, Cr administration and seizure periods were divided in 30-s segments and a 4-s sample from each segment was used to measure the amplitude wave.
Sample processing
Immediately after the seizure evaluation period, the animals were killed by decapitation, and their brains were exposed by removal of the parietal bone. The cerebral cortex was quickly dissected on an inverted ice-cold Petri dish, and the material was stored at −80 °C for subsequent biochemical analyses. Samples were prepared according to the guidelines for each technique, as described below.
Na+, K+-ATPase activity measurements
The cerebral cortex was homogenized in cold 30 mM Tris–HCl buffer (pH 7.4). The resultant homogenate was used to determine Na+, K+-ATPase activity. The enzyme activity was measured according to Oliveira et al. (2009). Briefly, the assay medium consisted of 30 mM Tris–HCl buffer (pH 7.4), 0.1 mM EDTA, 50 mM NaCl, 5 mM KCl, 6 mM MgCl2 and 50 µg of protein in the presence or absence of ouabain (1 mM) in a final volume of 350 µl. The reaction was initiated through addition of adenosine triphosphate (ATP) to a final concentration of 5 mM. After 30 min at 37 °C, the reaction was stopped through the addition of 70 µl of 50 % (w/v) trichloroacetic acid. Saturating substrate concentrations were used, and the reaction was linear with regard to protein and time. Appropriate controls were included in the assays to control for non-enzymatic hydrolysis of ATP. The amount of inorganic phosphate (Pi) released was quantified with the colorimetric method described by Fiske and Subbarow (1925), using KH2PO4 as reference standard. Specific Na+, K+-ATPase activity was calculated by subtracting the ouabain-insensitive activity from the overall activity (in the absence of ouabain) and expressed in nmol Pi/mg protein/min.
Creatine kinase (CK) activity
To determine the levels of CK activity in rat plasma, the rats treated with Cr or CMC were euthanized by decapitation, and the whole blood and the brain were quickly collected. The blood was collected in heparinized tubes, incubated at room temperature for 30 min and centrifuged at 1,500g for 10 min at room temperature for plasma separation. The brain samples of the cerebral cortex were processed in the same fashion as the Na+, K+-ATPase activity samples. The CK activity in the incubation medium was assayed colorimetrically at a wavelength of 340 nm according to the manufacturer’s protocol (Labtest reagents, Brazil).
Xanthine oxidase activity measurements
Xanthine oxidase assay was adapted from Prajda and Weber (1975). Briefly, each cerebral cortex was gently homogenized in cold phosphate buffer saline (PBS 30 mM, pH 7.4) containing (in mM): 1 EDTA, 10 dithiothreitol and 1 phenylmethylsulfonyl fluoride. The samples were centrifuged at 2,500 rpm for 10 min (4 °C). After centrifugation, the pellet was discarded and an aliquot of supernatant (0.5 mg/mL) was added to the assay medium containing xanthine (0.5 mM). The assay medium was incubated at 37 °C for 1 h, and the reaction was stopped by boiling for 10 min. After boiling, acid buffer (sodium acetate/acetic acid, 80 mM, pH 5.5) was added to the medium, and the samples were analyzed spectrophotometrically at a wavelength of 290 nm. Uric acid was used as standard reference, and all experiments were performed in triplicate.
Uric acid determination
For uric acid determination, each cerebral cortex was gently homogenized in cold PBS (30 mM, pH 7.4) and the resulting homogenate was diluted 1:10 with distilled H2O. Uric acid levels were determined with a standard commercial kit (Labtest, Porto Alegre, RS, Brasil), according to the manufacturer’s protocol. Sample absorbance was determined spectrophotometrically at a wavelength of 290 nm.
Purine levels determination
Determination of ATP, ADP, AMP, ADE and INO levels in the rat cerebral cortex was performed by HPLC–UV detection modified method of Özogul et al. (2000). Briefly, cerebral cortex samples were homogenized in 0.6 mM perchloric acid (1/5, w/v) and centrifuged at 2,400g at 4 °C for 10 min. The supernatant fraction was neutralized to pH 6–6.5 with 1 M potassium hydroxide. The neutralized fractions were held on ice for 30 min for total precipitation of potassium crystals and filtered through a membrane (0.45 µm pore size Millipore®) before injection onto the HPLC instrument. Samples were analyzed on a Shimadzu® HPLC apparatus. The analytical column had 5 µm particles and a 100 Å pore size Phenomenex® ODS-2 C18 reverse-phase column (4.6 × 250 mm, Allcrom, BR). The mobile phase was 0.04 M potassium dihydrogen orthophosphate and 0.06 M dipotassium hydrogen orthophosphate dissolved in purified distilled water and adjusted to pH 7 with 0.1 M potassium hydroxide. HPLC analysis was performed under isocratic conditions at a flow rate of 1 mL/min with the UV detector set to 257 nm.
Cr and PCr (total Cr) levels determination
The Cr and PCr (total Cr) levels were measured in the cerebral cortex and in blood plasma. Briefly, rats that had been treated with Cr or CMC were euthanized by decapitation and the whole blood and the brain were quickly collected. The blood was collected in heparinized tubes, incubated at room temperature for 30 min and centrifuged at 1,500g for 10 min at room temperature for plasma separation. Both brain and plasma were homogenized in 1 ml of 3 mM perchloric acid. The samples were centrifuged at 12,000g for 5 min at −7 °C. After centrifugation, the supernatant was separated and the pH was adjusted to 7.4 with KOH (5 M) and KH2PO4 (25 mM). Total Cr content (Cr + PCr) was assayed in the neutralized supernatants by HPLC at controlled room temperature (20 °C) under isocratic conditions using a reversed-phase 125 × 4 mm analytical column protected by a 4 × 4 mm guard cartridge (5 µm particle size, RP-18 Li-Chrosphere 100, Hewlett Packard, The Netherlands). The mobile phase was 14.7 mM KH2PO4 in 1.15 mM tetra-n-butylammonium hydrogen malate aqueous solution adjusted to pH 5.3 with 5 mM KOH with a flow rate of 1 mL/min. The total Cr peak was identified by UV detection at 214 nm, as described by Karatzaferi et al. (1999).
Isolation of rat brain mitochondria
Rat brain mitochondria were isolated as described by Tonkonogi and Sahlin (1997) with some modifications. First, the cerebral cortex was quickly removed from the rat skull and homogenized in a buffer containing (in mM): 100 sucrose, 10 EDTA, 100 Tris–HCl, and 46 KCl (pH 7.4). After homogenization, the resulting suspension was centrifuged for 3 min at 2,000g (4 °C) to obtain a low-speed supernatant fraction (S1). S1 was centrifuged for 20 min at 12,000g (4 °C). The pellet was re-suspended in a buffer containing (in mM): 100 sucrose, 10 EDTA, 100 Tris–HCl, 46 KCl and bovine serum albumin (BSA, 0.5 %; pH 7.4) and re-centrifuged for 10 min at 12,000g (4 °C). The supernatant was decanted and the final pellet re-suspended in a buffer containing (in mM): 70 sucrose, 0.02 EDTA, 20 Tris–HCl, 230 mannitol, 1 K2HPO4, to yield a protein concentration of 30–40 mg/mL. The isolated mitochondria were used to perform an analysis of the mitochondrial membrane potential (ΔΨ).
Mitochondrial ΔΨ determination
The mitochondrial ΔΨ determination was assayed according to Akerman and Wikstrom (1976). Briefly, samples of mitochondria from the cerebral cortex (300 µg protein/mL) were incubated in a medium containing mannitol (230 mM), sucrose (70 mM), EDTA (0.02 mM), K2HPO4 (1 mM), Tris (20 mM, pH 7,4), safranine-O (10 µM) and respiratory substrates, glutamate (5 mM) and succinate (5 mM). The reaction was initiated with the addition of mitochondria, and the medium was stirred constantly during the assay period. The fluorescence analysis was performed at 495 nm for excitation and 586 nm for emission with slit widths of 5 nm.
Protein determination
Protein content was colorimetrically determined by the method of Bradford (1976) using BSA (1 mg/mL) as standard.
Statistical analysis
Behavioral data were analyzed by the Mann–Whitney test and presented as median and interquartile ranges. EEG, XO, uric acid, purine levels and Na+, K+-ATPase activity measures were analyzed by one- or two-way ANOVA in accordance with the experimental designs. Parametric tests were followed by the post hoc Student–Newman–Keuls test, and data are expressed as the mean + SEM. A probability of p < 0.05 was considered significant.
Results
Figure 1 shows the effect of acute Cr administration (300 mg/kg) on behavioral seizures induced by PTZ (60 mg/kg). Statistical analysis revealed that acute Cr treatment increased the latency periods for both the first myoclonic jerk (U = 79.50; Fig. 1a) and the first generalized tonic–clonic seizure (U = 68.00; Fig. 1b). Cr treatment also reduced time spent in generalized tonic–clonic seizure (U = 76.00; Fig. 1c). As depicted in the representative EEG recordings (Fig. 2), administration of PTZ (30 and 45 mg/kg, i.p) did not induce convulsive behavior (data not shown), but PTZ induced the appearance of an EEG pattern characterized by multiple sharp waves in brief spindle episodes and increased wave amplitude (Fig. 2a, 30 mg/kg; Fig. 2c, 45 mg/kg; signal amplification in b and d, respectively). Additionally, PTZ injection at a fully convulsant dose (60 mg/kg) induced convulsive behavior characterized by myoclonic jerks and generalized tonic–clonic seizures. The behavior repertoire observed after PTZ injection (60 mg/kg) occurred concomitantly with electrographically recorded seizures: myoclonic jerks were characterized by multiple sharp waves in brief spindle episodes, whereas generalized seizures were characterized by the appearance of 2–3 Hz high-amplitude activity (Fig. 2e with signal amplification in f). Quantification of electroencephalographic wave amplitude revealed similar EEG signals in both CMC and Cr treatment before PTZ administration (Fig. 2m), indicating that Cr administration did not elicit detectable alterations in basal EEG. On the other hand, Cr prevented the increase in wave amplitude after injection of PTZ at the doses of 30 [F(2,28) = 8.04, p < 0.05; Fig. 2m], 45 [F(2,20) = 36.40, p < 0.05; Fig. 2m] and 60 mg/kg [F(2,34) = 136.39, p < 0.05; Fig. 2m].
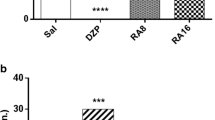
Effect of acute creatine administration (300 mg/kg, p.o.) on the convulsive behavior induced by PTZ (60 mg/kg, i.p.). a Latency for first clonic seizure; b latency for generalized tonic–clonic seizure; c time spent in generalized tonic–clonic seizure. Data are presented as median and interquartile range. *p < 0.05 compared with CMC-treated group (Mann–Whitney test)
Representative electroencephalographic recordings of animals treated with CMC (a–f) or creatine (g–l) after PTZ injection (30 a and g, 45 c and i, and 60 mg/kg e and k, i.p.) and wave amplitude quantification (m). Arrows PTZ injection, arrowheads the first clonic seizure. EEG signals in boxes in a, c, e, g, i and k are shown in higher detail in b, d, f, h, j, l, respectively. *p < 0.05 compared with Basal-CMC period; # p < 0.05 compared with respective CMC-PTZ-treated group
Na+, K+-ATPase activity is essential for the maintenance of membrane electrochemical gradients in the brain, and a decrease in Na+, K+-ATPase activity can increase brain excitability (Li and Stys 2001). As a result, we investigated the effect of PTZ and Cr administration on Na+, K+-ATPase activity. Statistical analysis revealed that PZT (at all doses) administration decreased Na+, K+-ATPase activity and that acute Cr (300 mg/kg) administration prevented the PZT-induced decrease in Na+, K+-ATPase activity [F(7,48) = 26.83, p < 0.05; Fig. 3a].
Effect of acute creatine administration (300 mg/kg, p.o.) on Na+, K+-ATPase activity in the rat cerebral cortex after PTZ injection (30, 45 or 60 mg/kg, i.p.). Data are presented as the mean + SEM (n = 7 per group). *p < 0.05 compared with CMC-NaCl group; ‡ p < 0.05 compared with respective CMC-PTZ-treated group; # p < 0.05 compared with CMC-PTZ30-treated group
Na+, K+-ATPase is responsible for the consumption of approximately 70 % of ATP in the brain (Clausen et al. 1991), and the catabolism of ATP is an important pathway responsible for maintaining an energy supply for this enzyme. As a result, we sought to measure the effect of Cr treatment on brain and plasma CK activity; CK is responsible for the resynthesis of ATP from ADP plus PCr in sites of energy consumption such as Na+, K+-ATPase (Adhihetty and Beal 2008). Statistical analysis indicated that acute Cr administration increased CK activity in brain [t(6) = 3.041; p < 0.05, Fig. 3b] but not in plasma [t(6) = 1.946; p > 0.05, Fig. 3b]. We also measured the effect of Cr treatment on the levels of ATP and ATP metabolites in the cerebral cortex of rats subjected to PTZ injection. Statistical analysis also showed that PTZ (all doses) administration decreased ATP [F(7,32) = 6.72, p < 0.05; Fig. 4a] and ADP [F(7,32) = 8.57, p < 0.05; Fig. 4b] levels, and Cr prevented these changes in ATP and ADP levels. Cr administration also attenuated the increase in AMP [F(7,32) = 5.33, p < 0.05; Fig. 4c], adenosine [F(7,32) = 3.40, p < 0.05; Fig. 4d] and inosine [F(7,32) = 4.50, p < 0.05; Fig. 4e] levels that are typically induced by PTZ administration (60 mg/kg). Furthermore, Cr treatment increased total Cr content both in the brain [t(6) = 3.267; p < 0.05, Fig. 4f] and in the plasma [t(6) = 10.090; p > 0.05, Fig. 4f].
Effect of acute creatine administration (300 mg/kg, p.o.) on ATP (a), ADP (b), AMP (c), ADE (adenosine d) and INO (inosine e) content in the rat cerebral cortex after PTZ injection (30, 45 or 60 mg/kg, i.p.). Data are presented as the mean + SEM (n = 5 per group). *p < 0.05 compared with CMC-NaCl group; # p < 0.05 compared with respective CMC-PTZ group
In the present study, we also found that injection of a fully convulsant dose of PTZ (60 mg/kg) increased both XO activity (Fig. 5a) and uric acid levels (Fig. 5b). Cr treatment prevented both the PTZ-induced increase in XO activity [F(7,48) = 6.63, p < 0.05; Fig. 5a] and the PTZ- induced uric acid accumulation [F(7,32) = 2.42, p < 0.05; Fig. 5b]. In addition, Cr treatment increased ΔΨ (Fig. 6) and blunted the ΔΨ decrease induced by PTZ at doses of 30, 45 and 60 mg/kg [F(7,32) = 14.43, p < 0.05; Fig. 6]. Moreover, Cr treatment also protected against the protein carbonyl [F(7,32) = 9.12, p < 0.05; Fig. 7a] and TBARS [F(7,32) = 5.83, p < 0.05; Fig. 7b] increase induced by all doses of PTZ. The results are summarized in Fig. 8
Effect of acute creatine administration (300 mg/kg, p.o.) on xanthine oxidase activity (a) and uric acid levels (b) in the rat cerebral cortex after PTZ injection (30, 45 or 60 mg/kg, i.p.). Data are presented as the mean + SEM (n = 5–7 per group). *p < 0.05 compared with CMC-NaCl group; # p < 0.05 compared with respective CMC-PTZ group
Effect of acute creatine administration (300 mg/kg, p.o.) on mitochondrial membrane potential (ΔΨ) in the rat cerebral cortex after PTZ injection (30, 45 or 60 mg/kg, i.p.). Data are presented as the mean + SEM (n = 5 per group). *p < 0.05 compared with CMC-NaCl group; # p < 0.05 compared with respective CMC-PTZ group
Effect of acute creatine administration (300 mg/kg, p.o.) on protein carbonyl (a) and TBARS (b) content in the rat cerebral cortex after PTZ injection (30, 45 or 60 mg/kg, i.p.). Data are presented as the mean + SEM (n = 5 per group). *p < 0.05 compared with CMC-NaCl group; # p < 0.05 compared with respective CMC-PTZ group
Illustrative figure highlighting the main findings: PTZ injection antagonizes GABAA receptors. Such decrease of inhibitory components of the neuron elicits behavioral and electrographic seizures by disrupting neuronal membrane potential. It activates Na+, K+-ATPase and increases the ATP catabolism, resulting in ROS generation via increase of xanthine oxidase activity (XO). The excitability induced by PTZ induces an energy demand increase that in turn generates more ROS via mitochondria. The ROS generation increases the reaction with selected cell targets such as phospholipidic membranes and inhibits Na+, K+-ATPase. The creatine treatment maintains and improves mitochondrial function, reducing ROS generation during excitotoxic processes elicited by PTZ
Discussion
In the present study, we confirmed and extended our previous findings that PTZ elicits behavioral seizures, electrographic seizures and oxidative stress (Rambo et al. 2009; Ribeiro et al. 2005; Schneider Oliveira et al. 2004; Souza et al. 2009). For the first time, we showed that acute Cr treatment (300 mg/kg) attenuates EEG alterations and delays the appearance of both clonic and generalized tonic–clonic seizures induced by PTZ. The idea that mitochondrial dysfunction may play a critical role in oxidative stress during seizure onset and spreading was supported by our findings of increased purine degradation, increased lipid peroxidation, protein carbonylation, increased uric acid content and increased XO activity and decreased mitochondrial ΔΨ after single doses of PTZ (Folbergrova and Kunz 2011). Moreover, the observed inhibition of Na+, K+-ATPase activity that resulted from all doses of PTZ suggests that the failure of some selected targets may increase cellular excitability, facilitating the appearance and propagation of convulsions (Patel 2004; Rambo et al. 2009).
Key factors influencing normal and abnormal biochemical signaling in the brain include cellular and mitochondrial bioenergetics (Shin et al. 2011). In this context, mitochondrial dysfunction contributes to several neurological disorders and has been recently implicated in acquired epilepsies (Waldbaum and Patel 2010). Compelling evidence for mitochondrial dysfunctions in this neurological disease comes from the observation that metabolic and bioenergetic changes occur following acute seizures. For example, rats submitted to PTZ administration present increased nucleotide hydrolysis in blood serum (Bruno et al. 2003) and cerebrospinal fluid (Oses et al. 2007). Additionally, a significant increase in nucleotide hydrolysis in hippocampal synaptosomes was observed soon after status epilepticus was induced by pilocarpine and kainic acid (Bonan et al. 2000), suggesting that nucleotide and nucleoside metabolism are involved in epilepsy. The activation of this neurochemical pathway increases the production of ROS (Tada et al. 1991; Zagnoni et al. 1994) and facilitates the appearance and/or propagation of seizures in several models of epilepsy (Frantseva et al. 2000; Gupta et al. 2003; Patsoukis et al. 2005; Souza et al. 2009). Moreover, the increases in uric acid levels and XO activity documented in this report support the idea that uric acid levels reflect the increase in XO activity and subsequent free radical production (Kanemitsu et al. 1989). Thus, in an environment lacking adequate supplies of primary and alternative sources of energy that is simultaneously limited by constraints on energy expenditure, brain dysfunction and seizures are expected (Masino and Geiger 2008). On the other hand, Cr supplementation can supply a potent energy source that helps the cell maintain the ATP/ADP ratio by activating CK in sites of energy production (mitochondria) and consumption (ATPase), reducing ADP formation and the formation of all successive catalytic products downstream. As a result, hydrogen peroxide and superoxide formation through the XO reaction would be attenuated (Mills et al. 1997). Accordingly, our results show that acute Cr supplementation increased neuronal CK activity, stabilized the purine content, stabilized XO activity and reduced the oxidative damage to proteins and lipids triggered by seizures.
Findings in the literature have shown that Cr increases the prevalence of the octameric form of mitochondrial creatine kinase (MtCK); this enzyme interacts with components of the mitochondrial permeability transition pore (MtPTP), suppressing pore opening and potentially reducing apoptotic susceptibility (Adhihetty and Hood 2003). Additionally, we found that acute Cr supplementation increases mitochondrial ΔΨ and CK activity. In this sense, we believe that Cr can maintain and improve both mitochondrial function and energy generation while reducing ROS formation during excitotoxic processes, like seizures, that result in energy depletion. Given the role of Cr in cellular energy homeostasis, the therapeutic efficacy of Cr is most promising in the neurological disorders that have marked impairment in energy metabolism (Adhihetty and Beal 2008). For example, mice with a gene knockout of cytosolic CK show decreased habituation in open field, reduced learning in the Morris Water Maze, and delayed development of PTZ-induced epileptic seizures (Jost et al. 2002). These experimental studies suggest that Cr depletion in the brain may be associated with disruption of neuronal functions and increased excitability.
Epileptic seizures are associated with decreased PCr/ATP ratios in the brain (Pan et al. 2005), indicating that vast amounts of energy are being used. In this context, a considerable body of data provides evidence that ROS generation during status epilepticus affects oxidative phosphorylation by inhibiting mitochondrial respiratory enzymes (Bruce and Baudry 1995; Patel and Li 2003; Poderoso et al. 1996; Sullivan et al. 2003). Furthermore, recent findings suggest that treatment with compounds possessing antioxidant properties targeting mitochondria can influence the extent of oxidative stress and mitochondrial dysfunction in models of epileptic seizures (Folbergrova and Kunz 2011). As decreased ATP levels may increase neuronal excitability by causing a reduction in neuronal plasma membrane potential (Patel 2004), it is plausible to propose that Cr maintains neuronal energy provision and it protects against purine catabolism, Na+, K+-ATPase inhibition, disruption of mitochondrial functions and ROS generation after PTZ administration.
In the present study, we revealed that acute Cr treatment induced mitochondrial ΔΨ increase and was effective against mitochondrial ΔΨ and Na+, K+-ATPase inhibition induced by PTZ (all doses). Furthermore, the Cr administration increased the CK activity in the brain and total Cr content in the brain and plasma. These experimental findings reinforce the importance of sufficient ATP supply for maintenance of normal synaptic transmission (Streijger et al. 2010). In addition, our results are consistent with studies suggesting a direct link between mitochondrial dysfunction, neuronal excitability increase, decreased ATP levels (Canafoglia et al. 2001), alterations of neuronal calcium homeostasis (Brini et al. 1999; Streijger et al. 2010), ROS-induced modifications of ion channels and neurotransmitter release (Bindokas et al. 1998; Kilbride et al. 2008). Considering that failure of some targets, such as Na+, K+-ATPase, increase cellular excitability and facilitate the appearance and/or propagation of convulsions (Rambo et al. 2009, Souza et al. 2009), we suggest that the protection induced by Cr results in decreased neuronal excitability and a lessening of the oxidative damage caused by PTZ. In fact, experimental findings have demonstrated that the Na+, K+-ATPase inhibitor ouabain increases Ca2+ influx in brain slices (Fujisawa et al. 1965), induces electrographic seizures in mice (Jamme et al. 1995), increases glutamate release by reversal of the Na+-dependent transporter (Li and Stys 2001), and increases cell death in rat hippocampi (Lees et al. 1990). Furthermore, Clapcote et al. (2009) showed that a mutation in the catalytic α3 isoform (a mutation that reduces Na+, K+-ATPase activity approximately 42 % in mice brain) was associated with hyperexcitability in the CNS. Additionally, a mutation in the Na+, K+-ATPase α2 isoform has been related to sporadic hemiplegic migraine and epileptic seizures in humans (Gallanti et al. 2008).
In the present study, we demonstrated that neuronal energy levels, mitochondrial membrane potential, Na+, K+-ATPase activity and oxidative stress markers in cortical homogenates were affected after seizures elicited by PTZ. These experimental findings suggest that mitochondrial dysfunction may play a critical role in oxidative stress and brain damage associated with epileptic seizures. Furthermore, CR administration results in an increase in ΔΨ and CK activity and effectively protects against the changes of neuronal energy levels, mitochondrial membrane potential dysfunction, Na+, K+-ATPase activity and oxidative stress in cortical homogenates. This suggests that acute Cr treatment helps maintain an adequate energy supply and buffers brain energy levels, highlighting the potential of acute Cr administration as a strategy for treatment of convulsive disorders. However, it is important to note that Cr metabolism varies among species; consequently, the effects observed in mice do not necessarily translate into similar findings in clinical studies (Andres et al. 2008; Beal 2011; Gualano et al. 2009, 2011; Klopstock et al. 2011).
References
Adhihetty PJ, Beal MF (2008) Creatine and its potential therapeutic value for targeting cellular energy impairment in neurodegenerative diseases. Neuromol Med 10:275–290
Adhihetty PJ, Hood DA (2003) Mechanisms of apoptosis in skeletal muscle. Basic Appl myol 13:171–179
Akerman KE, Wikstrom MK (1976) Safranine as a probe of the mitochondrial membrane potential. FEBS Lett 68:191–197
Andres RH, Ducray AD, Schlattner U, Wallimann T, Widmer HR (2008) Functions and effects of creatine in the central nervous system. Brain Res Bull 76:329–343
Beal MF (2011) Neuroprotective effects of creatine. Amino Acids 40:1305–1313
Bindokas VP, Lee CC, Colmers WF, Miller RJ (1998) Changes in mitochondrial function resulting from synaptic activity in the rat hippocampal slice. J Neurosci 18:4570–4587
Bonan CD, Amaral OB, Rockenbach IC, Walz R, Battastini AM, Izquierdo I, Sarkis JJ (2000) Altered ATP hydrolysis induced by pentylenetetrazol kindling in rat brain synaptosomes. Neurochem Res 25:775–779
Bradford MM (1976) A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem 72:248–254
Brini M, Pinton P, King MP, Davidson M, Schon EA, Rizzuto R (1999) A calcium signaling defect in the pathogenesis of a mitochondrial DNA inherited oxidative phosphorylation deficiency. Nat Med 5:951–954
Bruce AJ, Baudry M (1995) Oxygen free radicals in rat limbic structures after kainate-induced seizures. Free Radic Biol Med 18:993–1002
Bruno AN, Oses JP, Amaral O, Coitinho A, Bonan CD, Battastini AM, Sarkis JJ (2003) Changes in nucleotide hydrolysis in rat blood serum induced by pentylenetetrazol-kindling. Brain Res Mol Brain Res 114:140–145
Canafoglia L, Franceschetti S, Antozzi C, Carrara F, Farina L, Granata T, Lamantea E, Savoiardo M, Uziel G, Villani F, Zeviani M, Avanzini G (2001) Epileptic phenotypes associated with mitochondrial disorders. Neurology 56:1340–1346
Carmody S, Brennan L (2010) Effects of pentylenetetrazole-induced seizures on metabolomic profiles of rat brain. Neurochem Int 56:340–344
Clapcote SJ, Duffy S, Xie G, Kirshenbaum G, Bechard AR, Rodacker Schack V, Petersen J, Sinai L, Saab BJ, Lerch JP, Minassian BA, Ackerley CA, Sled JG, Cortez MA, Henderson JT, Vilsen B, Roder JC (2009) Mutation I810N in the alpha3 isoform of Na+, K+-ATPase causes impairments in the sodium pump and hyperexcitability in the CNS. Proc Natl Acad Sci USA 106:14085–14090
Clausen T, Van Hardeveld C, Everts ME (1991) Significance of cation transport in control of energy metabolism and thermogenesis. Physiol Rev 71:733–774
Fiske CH, Subbarow Y (1925) The colorimetric determination of phosphorus. J Biol Chem 66:375–400
Folbergrova J, Kunz WS (2011) Mitochondrial dysfunction in epilepsy. Mitochondrion 12:35–40
Fox PT, Raichle ME, Mintun MA, Dence C (1988) Nonoxidative glucose consumption during focal physiologic neural activity. Science 241:462–464
Frantseva MV, Velazquez JL, Hwang PA, Carlen PL (2000) Free radical production correlates with cell death in an in vitro model of epilepsy. Eur J Neurosci 12:1431–1439
Fujisawa H, Kajikawa K, Ohi Y, Hashimot Y, Yoshida H (1965) Movement of radioactive calcium in brain slices and influences on it of protoveratrine ouabain potassium chloride and cocaine. Jpn J Pharmacol 15:327–334
Gallanti A, Tonelli A, Cardin V, Bussone G, Bresolin N, Bassi MT (2008) A novel de novo nonsense mutation in ATP1A2 associated with sporadic hemiplegic migraine and epileptic seizures. J Neurol Sci 273:123–126
Gualano B, Artioli GG, Poortmans JR, Lancha Junior AH (2009) Exploring the therapeutic role of creatine supplementation. Amino Acids 38:31–44
Gualano B, Roschel H, Lancha-Jr AH, Brightbill CE, Rawson ES (2011) In sickness and in health: the widespread application of creatine supplementation. Amino Acids 43:519–529
Gupta YK, Veerendra Kumar MH, Srivastava AK (2003) Effect of Centella asiatica on pentylenetetrazole-induced kindling, cognition and oxidative stress in rats. Pharmacol Biochem Behav 74:579–585
Holtzman D, Togliatti A, Khait I, Jensen F (1998) Creatine increases survival and suppresses seizures in the hypoxic immature rat. Pediatr Res 44:410–414
Ipsiroglu OS, Stromberger C, Ilas J, Hoger H, Muhl A, Stockler-Ipsiroglu S (2001) Changes of tissue creatine concentrations upon oral supplementation of creatine-monohydrate in various animal species. Life Sci 69:1805–1815
Jamme I, Petit E, Divoux D, Gerbi A, Maixent JM, Nouvelot A (1995) Modulation of mouse cerebral Na+, K(+)-ATPase activity by oxygen free radicals. Neuroreport 7:333–337
Jost CR, Van Der Zee CE, In ‘t Zandt HJ, Oerlemans F, Verheij M, Streijger F, Fransen J, Heerschap A, Cools AR, Wieringa B (2002) Creatine kinase B-driven energy transfer in the brain is important for habituation and spatial learning behaviour, mossy fibre field size and determination of seizure susceptibility. Eur J Neurosci 15:1692–1706
Kanemitsu H, Tamura A, Kirino T, Oka H, Sano K, Iwamoto T, Yoshiura M, Iriyama K (1989) Allopurinol inhibits uric acid accumulation in the rat brain following focal cerebral ischemia. Brain Res 499:367–370
Kilbride SM, Telford JE, Tipton KF, Davey GP (2008) Partial inhibition of complex I activity increases Ca-independent glutamate release rates from depolarized synaptosomes. J Neurochem 106:826–834
Klein AM, Ferrante RJ (2007) The neuroprotective role of creatine. Subcell Biochem 46:205–243
Karatzaferi C, De Haan A, Offringa C, Sargeant AJ (1999) Improved high-performance liquid chromatographic assay for the determination of "high-energy" phosphates in mammalian skeletal muscle. Application to a single-fibre study in man. J Chromatogr B Biomed Sci Appl 730:183–191
Klopstock T, Elstner M, Bender A (2011) Creatine in mouse models of neurodegeneration and aging. Amino Acids 40(5):1297–1303
Kraemer WJ, Volek JS (1999) Creatine supplementation. Its role in human performance. Clin Sports Med 18:651–666 ix
Lees GJ, Lehmann A, Sandberg M, Hamberger A (1990) The neurotoxicity of ouabain, a sodium-potassium ATPase inhibitor, in the rat hippocampus. Neurosci Lett 120:159–162
Li S, Stys PK (2001) Na+-K+-ATPase inhibition and depolarization induce glutamate release via reverse Na+-dependent transport in spinal cord white matter. Neuroscience 107:675–683
Magni DV, Oliveira MS, Furian AF, Fiorenza NG, Fighera MR, Ferreira J, Mello CF, Royes LF (2007) Creatine decreases convulsions and neurochemical alterations induced by glutaric acid in rats. Brain Res 1185:336–345
Masino SA, Geiger JD (2008) Are purines mediators of the anticonvulsant/neuroprotective effects of ketogenic diets? Trends Neurosci 31:273–278
McColl CD, Horne MK, Finkelstein DI, Wong JY, Berkovic SF, Drago J (2003) Electroencephalographic characterisation of pentylenetetrazole-induced seizures in mice lacking the alpha 4 subunit of the neuronal nicotinic receptor. Neuropharmacology 44:234–243
Mikati MA, Kurdit RM, Rahmeh AA, Farhat F, Abu Rialy S, Lteif L, Francis E, Geha G, Maraashli W (2004) Effects of creatine and cyclocreatine supplementation on kainate induced injury in pre-pubescent rats. Brain Inj 18:1229–1241
Mills PC, Smith NC, Harris RC, Harris P (1997) Effect of allopurinol on the formation of reactive oxygen species during intense exercise in the horse. Res Vet Sci 62:11–16
Oliveira MS, Furian AF, Rambo LM, Ribeiro LR, Royes LF, Ferreira J, Calixto JB, Otalora LF, Garrido-Sanabria ER, Mello CF (2009) Prostaglandin E2 modulates Na+, K+-ATPase activity in rat hippocampus: implications for neurological diseases. J Neurochem 109:416–426
Oses JP, Viola GG, de Paula Cognato G, Junior VH, Hansel G, Bohmer AE, Leke R, Bruno AN, Bonan CD, Bogo MR, Portela LV, Souza DO, Sarkis JJ (2007) Pentylenetetrazol kindling alters adenine and guanine nucleotide catabolism in rat hippocampal slices and cerebrospinal fluid. Epilepsy Res 75:104–111
Özogul F, Taylor AKD, Quantick P, Özogul Y (2000) A rapid HPLC-determination of ATP-related compounds and its applications to herring stored under modified atmosphere. Int J Food Sci Technol 35:549–554
Pan JW, Kim JH, Cohen-Gadol A, Pan C, Spencer DD, Hetherington HP (2005) Regional energetic dysfunction in hippocampal epilepsy. Acta Neurol Scand 111:218–224
Patel M (2004) Mitochondrial dysfunction and oxidative stress: cause and consequence of epileptic seizures. Free Radic Biol Med 37:1951–1962
Patel M, Li QY (2003) Age dependence of seizure-induced oxidative stress. Neuroscience 118:431–437
Patsoukis N, Zervoudakis G, Georgiou CD, Angelatou F, Matsokis NA, Panagopoulos NT (2005) Thiol redox state and lipid and protein oxidation in the mouse striatum after pentylenetetrazol-induced epileptic seizure. Epilepsia 46:1205–1211
Paxinos G, Watson C (1986) The rat brain in stereotaxic coordinates. Academic Press, San Diego
Poderoso JJ, Carreras MC, Lisdero C, Riobo N, Schopfer F, Boveris A (1996) Nitric oxide inhibits electron transfer and increases superoxide radical production in rat heart mitochondria and submitochondrial particles. Arch Biochem Biophys 328:85–92
Prajda N, Weber G (1975) Malignant transformation-linked imbalance: decreased xanthine oxidase activity in hepatomas. FEBS Lett 59:245–249
Rambo LM, Ribeiro LR, Oliveira MS, Furian AF, Lima FD, Souza MA, Silva LF, Retamoso LT, Corte CL, Puntel GO, de Avila DS, Soares FA, Fighera MR, Mello CF, Royes LF (2009) Additive anticonvulsant effects of creatine supplementation and physical exercise against pentylenetetrazol-induced seizures. Neurochem Int 55:333–340
Ribeiro MC, de Avila DS, Schneider CY, Hermes FS, Furian AF, Oliveira MS, Rubin MA, Lehmann M, Krieglstein J, Mello CF (2005) alpha-Tocopherol protects against pentylenetetrazol- and methylmalonate-induced convulsions. Epilepsy Res 66:185–194
Royes LF, Fighera MR, Furian AF, Oliveira MS, da Silva LG, Malfatti CR, Schneider PH, Braga AL, Wajner M, Mello CF (2003) Creatine protects against the convulsive behavior and lactate production elicited by the intrastriatal injection of methylmalonate. Neuroscience 118:1079–1090
Royes LF, Fighera MR, Furian AF, Oliveira MS, Myskiw Jde C, Fiorenza NG, Petry JC, Coelho RC, Mello CF (2006) Effectiveness of creatine monohydrate on seizures and oxidative damage induced by methylmalonate. Pharmacol Biochem Behav 83:136–144
Schneider Oliveira M, Flavia Furian A, Freire Royes LF, Rechia Fighera M, de Carvalho Myskiw J, Gindri Fiorenza N, Mello CF (2004) Ascorbate modulates pentylenetetrazol-induced convulsions biphasically. Neuroscience 128:721–728
Shin EJ, Jeong JH, Chung YH, Kim WK, Ko KH, Bach JH, Hong JS, Yoneda Y, Kim HC (2011) Role of oxidative stress in epileptic seizures. Neurochem Int 59:122–137
Souza MA, Oliveira MS, Furian AF, Rambo LM, Ribeiro LR, Lima FD, Dalla Corte LC, Silva LF, Retamoso LT, Dalla Corte CL, Puntel GO, de Avila DS, Soares FA, Fighera MR, de Mello CF, Royes LF (2009) Swimming training prevents pentylenetetrazol-induced inhibition of Na+, K+-ATPase activity, seizures, and oxidative stress. Epilepsia 50:811–823
Streijger F, Scheenen WJ, van Luijtelaar G, Oerlemans F, Wieringa B, Van der Zee CE (2010) Complete brain-type creatine kinase deficiency in mice blocks seizure activity and affects intracellular calcium kinetics. Epilepsia 51:79–88
Sullivan PG, Dube C, Dorenbos K, Steward O, Baram TZ (2003) Mitochondrial uncoupling protein-2 protects the immature brain from excitotoxic neuronal death. Ann Neurol 53:711–717
Tada H, Morooka K, Arimoto K, Matsuo T (1991) Clinical effects of allopurinol on intractable epilepsy. Epilepsia 32:279–283
Tonkonogi M, Sahlin K (1997) Rate of oxidative phosphorylation in isolated mitochondria from human skeletal muscle: effect of training status. Acta Physiol Scand 161:345–353
Vielhaber S, Von Oertzen JH, Kudin AF, Schoenfeld A, Menzel C, Biersack HJ, Kral T, Elger CE, Kunz WS (2003) Correlation of hippocampal glucose oxidation capacity and interictal FDG-PET in temporal lobe epilepsy. Epilepsia 44:193–199
Waldbaum S, Patel M (2010) Mitochondrial dysfunction and oxidative stress: a contributing link to acquired epilepsy? J Bioenergy Biomembr 42:449–455
Wyss M, Kaddurah-Daouk R (2000) Creatine and creatinine metabolism. Physiol Rev 80:1107–1213
Zagnoni PG, Bianchi A, Zolo P, Canger R, Cornaggia C, D’Alessandro P, DeMarco P, Pisani F, Gianelli M, Verze L et al (1994) Allopurinol as add-on therapy in refractory epilepsy: a double-blind placebo-controlled randomized study. Epilepsia 35:107–112
Acknowledgments
The authors thank Dr. Guilherme Bresciani for critical reading of the manuscript. This work was supported by FAPERGS/CNPq (Grant: #11/2082-4). L.F.F. Royes, M.R. Fighera and L.M. Rambo are the recipients of CNPq fellowships (Grant: #141164/2010-7). I. Della-Pace is the recipient of CAPES fellowships. We confirm that we have read the journal’s position on issues involved in ethical publication and affirm that this report is consistent with those guidelines. In addition, we would like to state that all authors have observed and approved the study and that no part of the submitted work has been published or is under consideration for publication elsewhere. Moreover, the present work was supported by government funding and has no financial or other relationships that might lead to a conflict of interest. We also would like to declare that all experiments were carried out according to the National Institute of Health Guide for the Care and Use of Laboratory Animals (NIH Publications No. 80-23) revised 1996 and that the University Ethics Committee approved the respective protocols.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rambo, L.M., Ribeiro, L.R., Della-Pace, I.D. et al. Acute creatine administration improves mitochondrial membrane potential and protects against pentylenetetrazol-induced seizures. Amino Acids 44, 857–868 (2013). https://doi.org/10.1007/s00726-012-1408-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00726-012-1408-6