Abstract
The aim of this study was to evaluate the feasibility of a new method, which should help to avoid cage subsidence after vertebrectomy in short fusions. After implantation of an extendable vertebral body replacement (VBR) the two adjacent endplates to the fractured or destroyed vertebra were augmented with bone cement using the anterior approach in 20 patients with short circumferential fusion. All patients were followed up for 2 years clinically and radiographically. X-rays were reviewed for kyphosis, cage subsidence, presence of a solid fusion mass and instrumentation failure. Changes in every day activities (Oswestry Disability Index-ODI) and visual analogue scale (VAS), pain score, as well as technique-related complications were examined. The mean amount of kyphosis correction was 12.8° (±6.4°) and changed by only 0.3° (±0.4°) until last follow-up. Pain (VAS) and ODI scores were significantly improved and did not change until last follow-up. In all but two cases, the authors observed solid union with incorporation of the cage. No surgery-related complications were recorded. In one case revision was advised because of non-union due to septic loosening. The augmentation of the adjacent vertebras after anterior VBR provides an enhancement of the interface between cage and vertebra in cases with poor bone quality and in revision surgery. The technique is simple and safe, as the needles can be placed under visual control. Cement augmentation of the endplates may reduce interbody device subsidence.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Vertebral fractures of patients with bad bone quality still pose a severe problem in spine surgery. Whereas simple fractures can be treated with percutaneous vertebroplasty or kyphoplasty [10], severely comminuted fractures or metastases may need an anterior vertebral body replacement (VBR). Circumferential instrumentation is known to provide the highest initial stability and is superior to multilevel posterior or only anterior stabilization [20].
Re-kyphosis in 1–3 year follow-up was reported as a problem of formerly widespread techniques such as transpedicular bone grafting [14]. This led to a mean loss of correction of more than 10° and a high degree of pseudarthrosis!
To promote sufficient stability, VBR is often combined with long posterior fusions [15, 27]. Long posterior fusion in combination with VBR provides good initial stability, but consequently screw breakage may occur in segments without anterior support (Fig. 1) and further operations to remove screws from unfused segments may be necessary.
New screw designs which allow cement augmentation are meant to provide higher stability in osteoporotic vertebrae and thus allow for shorter fusions, which spare healthy segments for the patient [11, 24]. Unfortunately this does not necessarily affect the problem of cage subsidence, as the cement, which is injected through the screws distributes more laterally and cranially with respect to the vertebral body; whereas the cage needs support at the central parts of the endplates (Fig. 2). As these regions can easily be reached during anterior VBR we regularly perform an additional anterior augmentation of the endplates after placement of the cage. The technique, feasibility, and first results shall be presented in this study after a 2-year follow-up.
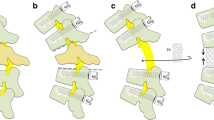
This old fracture with segmental kyphosis of 35° at L3 (a) was restored to 12° with cannulated screws from posterior (b) and anterior reconstruction with an extendable cage (c, d). Note that the cement, that was injected through the screws did not reach the endplates. This was achieved by anterior vertebroplasty (c)
Methods and patients
Patient population
The study included a consecutive series of 20 patients (14 females and 6 males) with single level vertebral collapse due to inadequate trauma with osteoporosis (8 cases), adequate trauma with osteoporosis (8 cases) or tumour (4 cases). Trauma was judged as inadequate if it would not have caused a fracture in an otherwise healthy patient. Osteoporosis was defined according to the criteria of the WHO and DVO-guidelines [1, 16].
In four cases, the operation performed in our hospital was a revision operation due to screw breakage, loosening of the previously used extendable cage or increase of the kyphotic angle after a previous vertebroplasty. These changes developed without neurological deficits.
T10 collapsed in two patients, T12 in four, L1 in seven, L2 in two, L3 in three, L4 and L5 was affected in one patient.
The age of the patients at surgery ranged from 50 to 83 years (mean 66 ± 9 years).
As the recording of the ODI and pain score according to the VAS is part of the clinical routine for all patients at our hospital, a complete prospective comparison of the perioperative and present status could easily be done with no dropouts.
The last follow-up of the patients was 2 years (24–26 months) after the operation. Two patients with malignancy could not complete the follow-up due to death, which was not associated to the surgery.
Indications for surgery included the presence of vertebra-related pain, kyphosis, instability of the posterior wall and possible neurological complications. Unsuccessful conservative therapy or vertebroplasty with progressive kyphosis was an indication for late surgery whereas spinal canal encroachment greater than or equal to 40% by retropulsion of a bone fragment, which was judged to represent “impending paralysis”, led to immediate intervention including decompression. In four cases, metastases of the spine with impending instability or affection of the spinal canal were the reason for anterior vertebrectomy.
No patients with posttraumatic paraplegia or affection of more than one level were enrolled in this study. Preoperative infections and spondylitis were also seen as a contraindication for vertebroplasty.
Surgical technique
In all cases posterior fusion was performed prior to anterior VBR. In cases of spinal canal encroachment additional decompression was performed even if no neurological deficit was present before surgery. The posterior reconstruction in a prone position usually included placement of cannulated pedicle screws in the adjacent vertebrae and cement augmentation of these screws under fluoroscopic control. If possible, short interference screws were placed at least in one pedicle of the affected vertebra to enhance the stability of the posterior construct [2] (Fig. 2).
For the anterior reconstruction the patient was placed in a lateral decubitus position. To access vertebral lesions at or proximal to L1, a transpleural approach combined with a diaphragmatic split was performed. A mini-open extraperitoneal approach was undertaken in cases involving lesions of L2 or below. To prevent cage subsidence and cement extrusion, the subchondral bone of the adjacent endplates was always preserved.
The extendable cages were placed slightly anterior to the centre of the endplates and distracted until their teeth anchored to the endplate. Care was taken not to penetrate them.
After placement of the cage, two 10-G vertebroplasty needles (Optimed Company) were inserted approximately 5 mm off the endplates in the adjacent upper and lower vertebrae under visual control (Fig. 3a). A-p fluoroscopy confirmed that the top of the needles was placed in the centre of the vertebrae and thus right next to the baseplates of the cage (Fig. 3c). No lateral fluoroscopy was necessary during placement as this can be controlled by direct vision (Fig. 3a). Fluoroscopy should be used during application of the bone cement to prevent leakage towards the spinal canal (Fig. 3b). Cement penetration through the endplates or anterior walls could also be detected without fluoroscopy merely by optical control.
Placement of the vertebroplasty needles in the centre of the adjacent endplates under visual control (a, black arrows). The needle tips are positioned right over the centre of the baseplates of the cage in the lateral (b) and a-p (c) view. Cement augmentation is done under fluoroscopic control to avoid cement leakage into the spinal canal
The same extendable titanium cage device (Obelisc®; Ulrich, Germany) was used for all patients [21]. After in situ lengthening small teeth in the edge area of the attachments are meant to be docked, and anchored to the subchondral bone of the endplates and protect the cage from dislocation.
Final lengthening was done after vertebroplasty and a bone substitute mixed with morselized bone obtained either from the vertebra itself, the iliac crest or the resected ribs, was packed around the cage to initiate bony integration.
Imaging and clinical evaluation
Radiographs were reviewed before surgery, upon discharge and for follow-up after 12 weeks, 12 month and for the final follow-up after 24–26 months after surgery. CT scans were done 3 months after operation for evaluation of the fusion (Fig. 4). If changes on the X-rays were seen, made by a possible loosening or cage-movement, additional CT-scans were done.
On lateral X-ray films, the kyphosis of the whole segment according to Cobb was measured from the superior endplate of the vertebral body one level above the injured vertebra to the inferior endplate of the vertebral body one level below, as for this method the highest intra- and interobserver reliability was described [7]. This was repeated by two independent doctors. The deviation was within the measuring tolerance of 2°.
On radiographs and CT scans the presence of homogenous radiodensity of vertebrae and distinct continuity of trabeculae around the cage was considered to indicate bony fusion. The neurological status of the patients was assessed clinically. Pain was measured with a visual analogue scale VAS (0–10). Every day activity was assessed by means of the ODI, which was assessed upon commitment and on follow-up.
Statistical analysis
The results are expressed as mean ± standard deviation. Statistic analyses were performed with SPSS 12 (SPSS Inc., Chicago, IL). Because of the small group size, non-parametric tests were used. The significance level was set at p ≤ 0.05. Signed Rank Test (Wilcoxon paired) was used for statistical evaluation before and after the operation and for the follow-up.
The box-and-whisker plots display the first and third quartiles as the ends of the box, the maximum and minimum as the whiskers and the median as a vertical bar in the interior of each box.
Results
General complications
Two patients, who suffered from a metastatic osteolysis with instability (adenocarcinoma) died before completion of the 2-year follow-up. In one patient revision was advised because of postoperative infection of the posterior stabilization device. All of the remaining patients could be included in the study.
Surgery-related complications
No serious complications such as cement extrusions in the spinal canal or neurological deficits occurred during anterior surgery. Furthermore, no implant-related complications like dislocation or breaking through the vertebral endplates happened.
Perioperative complications included pneumonia in one case, transient atelectasis after transthoracal access in three and superficial infection, treated with wound dressing and antibiotic therapy, in two. A low-grade asymptomatic compression fracture occurred in vertebrae one to three levels above or below the reconstruction site in two patients by the time of the final follow-up examination. These two patients reported of no traumatic event during the postoperative period.
Clinical and radiographic results
The mean kyphotic deformity before surgery measured 14° ± 11.4° and could be reduced by a mean of 12.8° ± 6.4° (p < 0.0001). After 12 and 24 months the mean change was 0.3° (±0.4°) (p = 0.4), thus smaller than the measuring tolerance (Fig. 5). Cage subsidence of more than 2° could only be found in the case with postoperative septic loosening.
Stability with new trabecular bone around the cage was found in all cases operated due to osteoporotic fractures. Bony union was observed in three out of four tumour cases. In the fourth case pseudarthrosis occurred after postoperative radiation (Fig. 6). This pseudarthrosis did not affect the implant position or result into screw loosening.
The median VAS pain score was 7.6/10 before surgery, 3.8/10 after surgery and 3.5/10 at follow up. Median ODI was 32 before surgery, 18 after surgery and 12 at the final follow-up 1 year after surgery (Fig. 7). Surgery improved pain and disability significantly (p < 0.001).
Discussion
Although currently, many vertebral fractures are treated successfully by vertebroplasty or kyphoplasty [19], anterior column reconstruction is still an important treatment option for patients with posterior wall involvement, spinal metastases or kyphosis after failed conservative treatment or failed vertebroplasty. Although considerable literature about treatment of fractures of the thoracolumbar region exists [10, 13, 17], very little data were found about the special problem of cage subsidence in osteoporotic or metastatic bone [18, 26]. Nevertheless, every surgeon knows about the problem of cage subsidence or loosening which is linked to bad bone quality and a too stiff construct compared with the bone and its much lower e-module [23].
Posterior rod extension increases the stability at the side of corporectomy, but increases motion of the adjacent levels and bears the risk of screw breakage at levels not fused from anterior (Fig. 1) [24].
As we did not want to fuse more than the affected segments, we searched for ways to improve the overall stability of the construct. Augmentation of screws does help to diminish the risk of screw loosening [3, 5, 8], but it is unclear whether it prevents cage subsidence as well. As thoracic and higher lumbar transpedicular screws are introduced with minor convergence, cement, which is injected through the screws, does not reach the central part of the endplates where endplates provide the least resistance to subsidence [18].
We routinely perfomed the reduction of the kyphosis from posterior followed by anterior VBR but a reverse order is conceivable. One should take care that cement is not placed in regions where screws should be introduced. In most fresh osteoporotic fractures adequate kyphosis correction was possible from posterior without forceful manipulation. Vertebroplasty screws helped to prevent screw loosening during the manipulation procedure. If no adequate correction could be achieved, we proceeded with anterior column reconstruction and then opened the posterior wound again, so that correction was performed simultaneously from anterior and posterior. This was done in one single case with an old osteoporotic fracture, which was healed in kyphosis. Augmenting the endplates helped us during anterior correction as remarkable pressure was administrated to the endplates.
In a cadaveric study, the interface strength between interbody device and vertebral body was enhanced when cement was used to augment pedicle or anterior vertebral body screws compared to normal screws [23]. These results suggest that interbody device subsidence may be prevented only by augmenting pedicle screws. The limitation of this study was that the cage vertebra interface strength was determined only for the superior vertebral endplates of the caudal vertebrae. Here the screws can be placed very close to the endplate and, thus, support the cage, but similar results could not be implied for the inferior endplates as pedicle screws are placed further away from endplates here. As can be seen in Fig. 2, cement, which is introduced through the screws is not able to support the inferior endplate of the upper adjacent vertebra. This goal can easily be achieved by the technique presented here. The cement can be placed easily and safely right next to the endplates of the VBR. As the needle-placement in the lateral plane is done under visual control (Fig. 3), the correct placement of the needle has to be checked by fluoroscopy only in the a-p plane. It is also recommended to use fluoroscopy during injection of the cement to make sure that it does not reach the spinal canal, although this is quite unlikely after anterior needle placement. The surgeon has to be aware, that cement can easily extrude through the prepared endplates, even though this usually does not cause problems. Of the anterior vertebroplasties performed during this study, no complications or cement leakage occurred.
Introducing bone cement close to the endplates might theoretically compromise osteogenesis as PMMA cement could be toxic to bone [9]. Therefore, we followed all our cases thoroughly. We could not find a necrosis of the vertebrae after cement augmentation (except for the one case shown in Fig. 6 which had post-radiation osteonecrosis before our treatment).
Moreover, bony union was not compromised by cement augmentation, as was proven in the follow-ups. We had no screw loosening and saw trabecular bone around the cages in the CT scans (Fig. 4) indicating bony fusion. A possible reason is that vascularization and osteogenesis does not only come from the endplates but also from the remaining rests of the fractured vertebrae and the surrounding soft tissue (especially the anterior longitudinal ligament). Furthermore not the whole endplate was covered with cement.
No significant loss of correction was observed in our patients using the presented technique. Although our series consists of patients older than found in most other publications and includes patients with metastases and osteoporosis, we found a remarkable subsidence only in one patient who had a septic loosening.
Defino and Rodriguez-Fuentes [6] reported of 43 patients with a dorso-ventral stabilization. For ventral reconstruction autologous bone from the iliac crest was used in 41 patients while a fibular transplant was used in the remaining two cases. The clinical outcome was promising but there was a distinct loss of correction in 11/39 patients; 5–7° in nine and ≥10° in two patients. The use of bovine bone for anterior reconstruction was disappointing and led to bony integration in just 2/11 patients compared to 8/11 patients sustaining autologous bone grafts [22].
Better results were reported if cages similar to ours were used instead of bone grafts.
The only report on the distractable cage, which was used in our study, was published by Ulmar et al. [25]. They report about 40 patients with mixed pathologies (trauma, tumour, discitis). After a kyphosis correction of 13.8°, they found only minor loss of correction of 1.1°. Their patients had mean age of 56.9 years and 65% were male. Only 25% of their patients suffered from osteoporotic fractures.
Other authors [13, 17] who used similar extendable cages also had patient populations which were significantly younger (43 and 48 years), mostly male and often suffered from adequate trauma without osteoporosis. They reported of a kyphosis reduction of 18.4°–18.7° in monosegmental vertebal body replacements and a loss of correction of 1.5°–2.8°. In the lumbar spine and for bisegmental corporectomies, the mean loss of correction was significantly higher. No data were given whether subsidence was a problem in older female patients who might suffer from osteoporosis.
Vieweg et al. [26] who used the same cage, had an overall loss of correction of only 1.6°, but found a mean loss of 10° in those patients with osteoporosis.
This supports our thesis that cage subsidence is a problem in patients with bad bone quality and thus additional support of the cage–bone interface should be attempted. We do not use cement augmentation in all our VBRs, but believe that it is sensible in selected cases. This is why our patient population was significantly older, predominantly female and suffered either of osteoporosis, malignancy or failed vertebroplasty with severe kyphosis.
At the final examination our patients achieved a mean VAS score of 3.5 (out of 10). This represents a significant reduction of 4/10 in comparison to the pre-operative score. The VAS reduction of 2.4 reported by Knop et al. [12] for patients treated with transpedicular intervertebral bone graft was considerably lower, which may be caused by the higher pseudarthrosis rate and inferior primar stability.
Briem et al. [4] reported about a relevant long-term impairment in patients’ quality of life after dorsoventral stabilization of thoracolumbar fractures and concluded that pain is the most important factor which is related to the severity of the injury and to the operation itself. In our study, apart from the significant reduction of the VAS, we also observed a significant reduction of the ODI; suggesting that the quality of life (disability in normal activities) improved for the operated patients. This finding is supported by other authors who used similar instruments for anterior–posterior vertebral column reconstruction [13].
A limiting factor of the current study is that we did not use a control group and, therefore, cannot be certain that without the cement augmentation, the patients could have done just as well. We can only compare our cases to those published in the literature and found a similar or lower loss of correction although we used a short posterior construct and treated an old and difficult patient population.
Conclusions
In cases where anterior vertebral body reconstruction is needed despite poor bone quality, the use of cement to support the pedicle screws as well as the endplates of the adjacent vertebral bodies may be a beneficial alternative. The technique of anterior verebroblasty is easy, safe and quick, as the needles are placed under visual control. It may help to reduce cage subsidence and the need for long posterior constructs even in cases of bad bone quality.
References
(1994) Assessment of fracture risk and its application to screening for postmenopausal osteoporosis. Report of a WHO Study Group. World Health Organ Tech Rep Ser 843:1–129
Anekstein Y, Brosh T, Mirovsky Y (2007) Intermediate screws in short segment pedicular fixation for thoracic and lumbar fractures: a biomechanical study. J Spinal Disord Tech 20:72–77
Becker S, Chavanne A, Spitaler R, Kropik K, Aigner N, Ogon M, Redl H (2008) Assessment of different screw augmentation techniques and screw designs in osteoporotic spines. Eur Spine J 17:1462–1469
Briem D, Linhart W, Lehmann W, Bullinger M, Schoder V, Meenen NM, Windolf J, Rueger JM (2003) Investigation of the health-related quality of life after a dorso ventral stabilization of the thoracolumbar junction. Unfallchirurg 106:625–632
Chang MC, Liu CL, Chen TH (2008) Polymethylmethacrylate augmentation of pedicle screw for osteoporotic spinal surgery: a novel technique. Spine (Phila Pa 1976) 33:E317–E324
Defino HL, Rodriguez-Fuentes AE (1998) Treatment of fractures of the thoracolumbar spine by combined anteroposterior fixation using the Harms method. Eur Spine J 7:187–194
Enad JG, Slakey JB, McNulty PS (2008) Measurement of thoracolumbar kyphosis after burst fracture: evaluation of intraobserver, interobserver, and variability of 4 measurement methods. Am J Orthop (Belle Mead NJ) 37:E60–E63
Frankel BM, Jones T, Wang C (2007) Segmental polymethylmethacrylate-augmented pedicle screw fixation in patients with bone softening caused by osteoporosis and metastatic tumor involvement: a clinical evaluation. Neurosurgery 61:531–537
Kalteis T, Luring C, Gugler G, Zysk S, Caro W, Handel M, Grifka J (2004) Acute tissue toxicity of PMMA bone cements. Z Orthop Ihre Grenzgeb 142:666–672
Kim DH, Vaccaro AR (2006) Osteoporotic compression fractures of the spine; current options and considerations for treatment. Spine J 6:479–487
Kim HS, Park SK, Joy H, Ryu JK, Kim SW, Ju CI (2008) Bone cement augmentation of short segment fixation for unstable burst fracture in severe osteoporosis. J Korean Neurosurg Soc 44:8–14
Knop C, Fabian HF, Bastian L, Rosenthal H, Lange U, Zdichavsky M, Blauth M (2002) Fate of the transpedicular intervertebral bone graft after posterior stabilisation of thoracolumbar fractures. Eur Spine J 11:251–257
Knop C, Kranabetter T, Reinhold M, Blauth M (2009) Combined posterior-anterior stabilisation of thoracolumbar injuries utilising a vertebral body replacing implant. Eur Spine J 18:949–963
Knop C, Lange U, Bastian L, Oeser M, Blauth M (2001) Biomechanical compression tests with a new implant for thoracolumbar vertebral body replacement. Eur Spine J 10:30–37
Kostuik JP, Shapiro MB (2003) Open surgical treatment of osteoporotic fractures and deformity of the spine. Instr Course Lect 52:569–578
Kurth AA, Pfeilschifter J (2007) Diagnosis and treatment of postmenopausal osteoporosis and osteoporosis in men. German Guidelines Update 2006. Orthopade 36:683–690
Lange U, Edeling S, Knop C, Bastian L, Oeser M, Krettek C, Blauth M (2007) Anterior vertebral body replacement with a titanium implant of adjustable height: a prospective clinical study. Eur Spine J 16:161–172
Lowe TG, Hashim S, Wilson LA, O’Brien MF, Smith DA, Diekmann MJ, Trommeter J (2004) A biomechanical study of regional endplate strength and cage morphology as it relates to structural interbody support. Spine (Phila Pa 1976) 29:2389–2394
McArthur N, Kasperk C, Baier M, Tanner M, Gritzbach B, Schoierer O, Rothfischer W, Krohmer G, Hillmeier J, Kock HJ, Meeder PJ, Huber FX (2009) 1150 kyphoplasties over 7 years: indications, techniques, and intraoperative complications. Orthopedics 32:90
Oda I, Cunningham BW, Abumi K, Kaneda K, McAfee PC (1999) The stability of reconstruction methods after thoracolumbar total spondylectomy. An in vitro investigation. Spine (Phila Pa 1976) 24:1634–1638
Pflugmacher R, Schleicher P, Schaefer J, Scholz M, Ludwig K, Khodadadyan-Klostermann C, Haas NP, Kandziora F (2004) Biomechanical comparison of expandable cages for vertebral body replacement in the thoracolumbar spine 41. Spine(Phila Pa 1976) 29:1413–1419
Schultheiss M, Sarkar M, Arand M, Kramer M, Wilke HJ, Kinzl L, Hartwig E (2005) Solvent-preserved, bovine cancellous bone blocks used for reconstruction of thoracolumbar fractures in minimally invasive spinal surgery-first clinical results. Eur Spine J 14:192–196
Tan JS, Bailey CS, Dvorak MF, Fisher CG, Cripton PA, Oxland TR (2007) Cement augmentation of vertebral screws enhances the interface strength between interbody device and vertebral body. Spine (Phila Pa 1976) 32:334–341
Tan JS, Singh S, Zhu QA, Dvorak MF, Fisher CG, Oxland TR (2008) The effect of cement augmentation and extension of posterior instrumentation on stabilization and adjacent level effects in the elderly spine. Spine (Phila Pa 1976) 33:2728–2740
Ulmar B, Richter M, Kelsch G, Cakir B, Puhl W, Huch K (2005) Distractible vertebral body replacement for the thoracic and lumbar spine. Acta Orthop Belg 71:467–471
Vieweg U, Solch O, Kalff R (2003) Vertebral body replacement system Synex in unstable burst fractures of the thoracic and lumbar spine—a retrospective study with 30 patients. Zentralbl Neurochir 64:58–64
Wuisman PI, van DM, Staal H, Van Royen BJ (2000) Augmentation of (pedicle) screws with calcium apatite cement in patients with severe progressive osteoporotic spinal deformities: an innovative technique. Eur Spine J 9:528–533
Conflict of interest
No conflicts of interest exist. No author has any financial ties to the manufacturer of any product discussed in the study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Geiger, F., Kafchitsas, K. & Rauschmann, M. Anterior vertebroplasty of adjacent levels after vertebral body replacement. Eur Spine J 20, 1385–1392 (2011). https://doi.org/10.1007/s00586-011-1766-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-011-1766-x