Abstract
Amyotrophic lateral sclerosis (ALS) is the most common neurodegenerative disease affecting motor neurons (MNs). Although a small percentage of ALS has a familial origin, the vast majority of cases are sporadic in which genetic factors and environment interact with each other leading to disease onset in genetically predisposed individuals. In the current model of the disease, each individual has a determined genetic load, some degree of cell degeneration related to age and several risky environmental exposures. In this scenario, MN degeneration would occur when the sum of these factors reach a certain threshold. To date, an extensive list of environmental factors has been associated to ALS, including different categories, such as exposure to heavy metals and other toxicants, cyanotoxins or infectious agents. In addition, in recent years, lifestyle and other demographic parameters are gaining relevance in the genesis of the disease. Among them, physical activity, nutrition, body mass index, cardiovascular risk factors, autoimmune diseases and cancer are some of the conditions which have been related to the disease. In this review, we will discuss the potential mechanisms of environmental conditions in motor neuron degeneration. Understanding the role of each one of these factors as well as their interactions appears as a crucial step in order to develop new preventive, diagnostic and therapeutic approaches for ALS patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Amyotrophic lateral sclerosis (ALS) is the most common neurodegenerative disease affecting motor neurons (MNs) (Zufiria et al. 2016) with an annual incidence that ranges from two to three cases per 100,000 habitants across Caucasian populations (Riancho et al. 2016d). Lower incidences rates have been reported in other populations, such as Asians and Afro-Americans (Zufiria et al. 2016). Regarding gender, the vast majority of epidemiological studies have showed a male predominance with a male/female ratio ranging from 1.2:1 to 1.5:1 (Zufiria et al. 2016).
ALS pathogenesis has not been fully elucidated yet; however, our knowledge about disease mechanisms has significantly improved (Zufiria et al. 2016). The impairment of various cellular functions has been related to MN degeneration (Zufiria et al. 2016). Among them, dysfunction of gene processing, proteostasis, axonal transport, as well as the involvement of glial cells surrounding MNs seem to be some of the most relevant mechanisms (Riancho et al. 2016c). ALS cases can be divided into familial (fALS) and sporadic (sALS). fALS represent a small percentage of cases. These are secondary to mutations in specific genes (Cr9orf72, SOD1, FUS, TDP43, etc.) which directly induce MN degeneration and disease onset (Table 1) (Zufiria et al. 2016). By contrast, most cases are thought to be sporadic (sALS) in which genes and environment interact with each other leading to disease onset and progression in genetically predisposed individuals (Zufiria et al. 2016). On this basis, the role of environmental factors in the pathogenesis of ALS is receiving increasing attention (Zufiria et al. 2016). Thus, without negating the role of genetic and other conditions as ageing, in this review, we will particularly focus on the evidences supporting the role of the environment in ALS.
ALS as the result of the interaction of genes, environment, age and chance
Not only ALS but also other neurodegenerative diseases are considered to be the final result of the interactions between genes, ageing, environmental conditions and a component of chance which can not be easily measured (Fig. 1) (Al Chalabi and Hardiman 2013).
In this line, each subject has a determined genetic load, some degree of cell damage according to ageing, and a variety of environmental risk exposures. The development of ALS would then occur when the sum of these factors reached a certain threshold. Upon this basis, in fALS cases, the genetic load and the MN damage related to ageing would be sufficient for developing the disease without the environmental influences. However, environment may be crucial in the genesis of the disease in an important proportion of sporadic cases (Fig. 2). It would be particularly relevant in aged subjects harbouring ALS genetic risk variants. In those cases, risky environmental factors could be determinants for developing ALS or not; thus behaving as modifiers of genetic ALS. This fact is supported by several studies performed in discordant-ALS monozygotic twins. As an example, Al Chalabi et al. studied 49 ALS twin pairs. Among them, 5 and 44 monozygotic twin pairs were concordant- and discordant-affected, respectively. After applying several statistical tests, the authors estimated the heritability of sporadic ALS around 0.60, with an unshared environmental component of 0.4 (Al Chalabi et al. 2010).
Main involved components in the genesis of ALS. Each individual has a determined prenatal genetic load and during life accumulates a number of risky environmental exposures and progressive age-related cell damage. Regardless of the particular ‘weight’ of each of these components, ALS would develop when the sum of them reach a certain threshold. Once established, several auto-perpetuating mechanisms would occur leading to disease progression. In familiar cases of ALS, the ‘genetic load’ has a high relevance; however, in the vast majority of cases (sporadic ALS cases), the environmental exposures may be crucial to reach the threshold or not
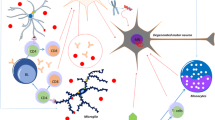
Genes and environment in ALS. Genetics and environmental factors interact promoting ALS onset in predisposed individuals. The final result of such alterations induces MN degeneration through the impairment of several cellular pathways including (i) DNA damage and gene processing disorders, (ii) proteostasis impairment, (iii) oxidative stress and mitochondrial dysfunction, (iv) immune dysregulation, (v) axonal transport abnormalities, and (vi) surrounding glial cells dysfunction. In the field of genetics, a number of causative genes which directly promote MN degeneration and a group of susceptibility genes predispose to ALS. Regarding environmental factors, toxicants and other external factors, as well as several lifestyle conditions and comorbidities, are likely involved. Toxicants and other external factors could promote MN degeneration directly by impairing some crucial cellular functions or in an indirect way, by modulating gene expression throughout epigenetic modifications. By contrast, most comorbidities and lifestyles are supposed to act mainly through the latter. In this complex scenario, ageing would behave as a facilitating factor, inducing age-related degeneration and accelerating the disease in those predisposed subjects
Environmental factors
There is evidence for a role of environmental conditions in ALS. A wide number of epidemiological, ecological and experimental studies have highlighted the role of the environment in ALS pathogenesis. Next, we will discuss the most relevant studies published in the literature until 31 October 2017 regarding the role of environmental factors in ALS.
2.1. Cluster studies
Cluster studies leaded to the identification of specific regions with increased ALS incidence. Interestingly, this increase of ALS cases was not only related to genetic factors, thus highlighting the importance of the environment in ALS. Some of the most representative are summarised in Table 2.
In 1945 in Guam, a disproportionate incidence of an ALS complex syndrome which also included dementia and Parkinsonian features was reported among the Chamorros population (Reed et al. 1966) Two decades later, the neurotoxin b-N-methylamino-L-alanine (BMAA) was discovered in the indigenous cycad (Cycas micronesica), the seeds of which were used by Chamorros to make flour (Torres et al. 1957; Reed and Brody 1975). Not long after, the causal inference was further supported when the BMAA was detected in brains of Guamanian patients with ALS, but not in Guamanian control brains (Murch et al. 2004a, b). Further studies demonstrated that BMAA in cycads came from a symbiotic cyanobacteria resident in specialised coralloid roots of this plant and that it got concentrated during the process of flour production (Murch et al. 2004a). A similar explanation was given for another cluster of ALS patients also presenting with Parkinsonism that was reported in 1962 in the Indonesian part of New Guinea, where Cycas circinalis seeds are also consumed by indigenous (Gajdusek and Salazar 1982). More recently, a third major cluster in the Pacific area was reported in Japan in the Kii Pensinsula of the Honshu Island (Kuzuhara and Kokubo 2005). Differently from previous clusters, no direct relationship with Cycas seed consumption was found, but the type of drinking water was postulated as a possible link among patients (Kuzuhara and Kokubo 2005; Kuzuhara 2011). To elucidate if these clusters were due to due genetic variants among affected subjects or not, several genetic studies were carried out. Interestingly, these studies only demonstrated mutations in several ALS-related genes in a small subset of patients (Ishiura et al. 2012), thus highlighting the role of environment. In addition, the reduction of cases among these populations after modifying dietetic habits clearly supported the role of external factors in the genesis of the disease (Spencer et al. 2005).
The role of BMAA in motor neuron disease has been further supported by other clusters reported in France and USA (Field et al. 2013; Caller et al. 2013; Lannuzel et al. 2015; Masseret et al. 2013). The precise mechanisms explaining BMAA toxicity have not been completely elucidated. It has been postulated that BMAA behaves as an endogenous neurotoxic reservoir, stored in a bound form, which would be slowly released within brain and spinal cord tissues inducing its neurotoxic effects over years (Murch et al. 2004a). Regarding histological characterisation, the vast majority of neuropathological studies were performed in Guam while other BMAA clusters have not been extensively characterised. It has been reported that Guamanian patients exhibited a constellation of neuropathological hallmarks which combined (i) abundant neurofibrillary tangle pathology, (ii) neuronal loss, (iii) amyloid plaques resembling those observed in Alzheimer’s disease (AD) patients, (iv) alfa-sinuclein pathology in the substantia nigra and cerebellum and (v) TDP43-positive inclusions in both hippocampus and motor neurons reactive (Schmidt et al. 1998; Buee-Scherrer et al. 1995; Sebeo et al. 2004; Geser et al. 2008). Complementary experimental studies have shown that the neurotoxic effects of BMAA are related to the depletion of glutathione, glutamatergic toxicity, synergism with other neurotoxins, the capacity to induce protein misfolding and the accumulation of intracellular aggregates (Bradley 2015). The interindividual BMAA susceptibility has been assessed by several investigators without having identified any risk gene variant (Sieh et al. 2009).
Apart from the previously discussed clusters, other high-incidence clusters have been reported in the literature. As example, recently, Nicoletti et al. (2016) studied ALS patients in Catania, the Italian region of Mount Etna. During 2005 to 2010, authors identified 126 ALS cases. Remarkably, ALS incidence was almost three times higher in the population living on the eastern flank compared to the western flank of the volcano (2.4 vs 0.9 cases per 100,000, respectively). These differences were interpreted by the authors as being secondary to distinct volcanogenic trace elements spreading depending on the mountain flank (Nicoletti et al. 2016). Importantly, some clusters of low incidence of ALS have also been reported. For example, there have been recently identified two low-incidence areas after analysing the Irish ALS register from 1995 to 2013 (Rooney et al. 2015a). Despite the potential relevance of this finding, ALS was not associated to obvious demographic nor other common environmental factors (Rooney et al. 2015b).
As a conclusion, cluster studies provided some of the earliest evidences supporting the role of the environment in ALS. They may represent a useful tool for generating new hypothesis. However, they require complementary confirmatory approaches because these studies commonly present several weaknesses and they are prone to be biased. A common drawback of cluster studies lies on the difficulty in distinguishing between fALS and sALS. Families also tend to be spatially clustered, which could lead investigators to mix up a potential environmental condition with genetic influences (Rothman et al. 2008). In addition, these approaches might frequently miss other environmental confounders which can falsify the final results. On the other hand, when considering rare diseases with low incidences such as ALS, minimal changes in the number of cases (numerator of the fraction) substantially influence the final result, thus increasing the risk of random error and subsequently resulting in wide confidence intervals of the effect estimates, which should be cautiously interpreted (Rothman et al. 2008).
2.2. Environmental factors
In the last decades, a wide number of external factors have been proposed as etiologic or underlying conditions for ALS. In this section, we will review some of the most important ones.
2.2.1. Heavy metals: lead, mercury and selenium
Heavy metals probably constitute one of the groups of external factors that has been most assessed during the last decades (Johnson and Atchison 2009; Talbott et al. 2016). Among them, lead, selenium and mercury have been the most studied ones (Sutedja et al. 2009; Johnson and Atchison 2009). Although the role of these toxicants has been widely investigated, the precise mechanisms by which these induce MN degeneration have not been fully elucidated yet.
Lead
Lead is the heavy metal most studied in ALS patients. Interestingly, it has some intriguing paradoxical effects. Several studies have reported increased lead levels in both blood and cerebrospinal fluid of ALS patients (Fang et al. 2010; Kamel et al. 2005). We recently performed an ecological study to correlate ALS mortality with air lead levels across Spanish provinces during a 10-year period. In this study, we described that those provinces with higher air lead levels had up to a 25% higher rate of ALS deaths (Santurtun et al. 2016a).
However, paradoxically, basic studies in the SOD1 murine model of ALS have demonstrated that transgenic mice exposed to low doses of lead had significant longer survivals. Histological and biochemical analyses showed that lead-exposed mice had a less prominent astroglial response that seemed to be mediated through an increased expression of the vascular endothelial growth factor (VEGF) (Barbeito et al. 2010). In addition, based on the potential relationship between lead and ALS, it has been studied if there is an association between variants in genes encoding for proteins regulating lead toxico-kinetics and ALS. Kamel et al. (2005) studied whether polymorphisms in aminolevulinic acid dehydratase (ALAD) and vitamin D receptor (VDR) genes (both of them potentially modulating susceptibility to lead exposure) were associated to ALS risk. Interestingly, some variants in the ALAD gene were significantly associated to lower lead levels, concluding that genetic susceptibility conferred by polymorphisms in ALAD may affect ALS risk, possibly through a mechanism related to internal lead exposure. Regarding VDR, no significant associations were reported (Kamel et al. 2005).
Further studies will help to elucidate the precise role of lead in MN degeneration as well. They will eventually clarify the potential of the ‘lead pathway’ as a new therapeutic target.
Selenium
Selenium was initially implicated in ALS after two epidemiological studies that reported an increased risk of ALS in two seleniferous regions (Kilness and Hichberg 1977; Vinceti et al. 1996). One of them included more than 5000 Italian people for an 11-year period and concluded that those subjects who drank high-selenium tap water had almost seven times higher risk of ALS than those who did not drink high-selenium tap water (Vinceti et al. 1996). Additionally, animal models have demonstrated that swine exposure to selenium is associated to anterior horn atrophy and MN degeneration at the spinal cord (Casteignau et al. 2006). The neurotoxic effects of selenium seemed to be related to selenium-induced oxidative stress, decreased cholinergic signalling, increased accumulation of mitochondrial SOD1 protein and the degeneration of cholinergic MNs (Estevez et al. 2012; Maraldi et al. 2011).
Mercury
Mercury was initially thought to be implicated in the genesis of ALS due to the fact that patients with long-term accidental exposure to mercury developed a characteristic clinical syndrome that is very similar to that reported in classic ALS (Schwarz et al. 1996). Regarding epidemiological studies, although there is no full concordance, most of them showed a slight positive correlation between mercury exposure and ALS (Adams et al. 1983; Pamphlett and Waley 1998; Praline et al. 2007).
Several basic experimental studies also support the role of this metal in the genesis of ALS, particularly in those genetically predisposed individuals. Studies with ALS transgenic mice have described mice exposed to mercury exhibit a more abrupt disease course (Johnson and Atchison 2009). Complementary in vitro studies have demonstrated that mercury influenced the secretion of proinflammatory cytokines, thus impairing the interaction between microglia and astrocytes (Bassett et al. 2012). More recently, Rooney et al. postulated that mercury also interfered with normal DNA methylation (Rooney 2011).
2.2.2. Other chemical toxicants
In the evaluation of other toxicants stands out the study published by Weisskopf et al. (2009) a few years ago. In their study, they assessed the relation between self-report of regular exposure to 11 different chemical classes or x-rays and ALS mortality. More than 1 million of participants were included with a 15-year follow-up period. During that time, 1156 (617 men, 539 women) ALS deaths occurred. Among the different chemicals studied, the authors found a small and non-significant association between pesticide/herbicide exposure and ALS (Weisskopf et al. 2009). In contrast, a clear significant association was found between the exposure to formaldehyde and ALS (relative risk (RR) 2.45; 95% CI 1.58 to 3.56) (Weisskopf et al. 2009). Remarkably, they also described a strong dose-response relationship between the years of formaldehyde exposure and the risk of developing the disease (Weisskopf et al. 2009; Roberts et al. 2015). These results are concordant with other subsequent studies (Pinkerton et al. 2013). In vitro assays have shown that formaldehyde induce mitochondrial disorders and reduced SOD1 activity, thus increasing oxidative stress and inducing neurodegeneration (Nie et al. 2007; Gurel et al. 2005). Inter-individual susceptibility to formaldehyde has been suggested to be mediated by allelic variants in genes encoding paraoxonase and cytochrome P450 (Boccia et al. 2007).
Regarding pesticides, two other meta-analysis have revealed a moderate positive association between ALS risk and the use of organochlorine insecticides, pyrethroids, herbicides and fumigants (Malek et al. 2012; Kamel et al. 2012). In addition, some polymorphisms in the metallothionein family of genes have been postulated to modulate the capacity to detoxify pesticides, thus influencing the risk of MD degeneration (Morahan et al. 2007).
2.2.3. Electromagnetic fields and electrocution
During the last decades, the growth of telecommunication systems has raised the question whether electromagnetic fields increase the risk of neurodegenerative diseases. Up to date, more than 20 studies evaluating the role of electromagnetic radiation and ALS have been published. In 2012, a meta-analysis including 19 of these studies was carried out (Zhou et al. 2012). After the combined analysis, the authors concluded that exposure to extremely low frequencies-electromagnetic fields slightly increased ALS risk (relative risk 1.29; 95% CI 1.02–1.69) (Zhou et al. 2012). From a pathogenic perspective, the exposure to these fields seemed to induce increased oxidative stress, DNA damage and apoptotic-pathways activation (Falone et al. 2008), although these findings have not been replicated in murine models (Poulletier et al. 2009). Regarding electrical injury, more than 30 studies have been conducted without having demonstrated any causal relationship between this type of injury and ALS condition (Abhinav et al. 2007).
2.2.4. Infectious agents
A few studies have also highlighted the potential role of viral, bacterial and fungal infections in ALS. Although the evidences supporting the involvement of microbiological agents are not very solid yet, this is an intriguing field that will probably help us to better understand the disease in the future. Among infectious agents, viruses have been the most studied ones. Initial studies identified reverse transcriptase (RT) in serum of patients with ALS at levels comparable to those observed in human immunodeficiency virus (HIV)-infected patients (Steele et al. 2005; MacGowan et al. 2007). Subsequently, Douville et al. (2011) reported an active locus of a human endogenous retrovirus in brain neurons and described a specific pattern of HERV-K expression among ALS patients. In line with this concept, more recently, Li et al. (2015) demonstrated that expression of HERV-K or its envelope protein in human neurons induced retraction and beading of neuritis. In addition, the authors reported that transgenic animals expressing the envelope protein gene developed a progressive MN disease phenotype (Li et al. 2015).
Regarding bacterial infections, Borrelia burgdorferi, the agent of Lyme disease, has been the most studied one. Recently, in a large case-control study including 491 ALS patients and 982 matched controls, no significant association between these diseases was found therefore not supporting the inclusion of Borrelia antibodies in the diagnostic work-up in patients with classical ALS (Visser et al. 2017b).
Interestingly, as a novel line of research in this field, gut microbiota has been postulated as a promising line of research. Each individual can be considered as an ecological community composed by a large number of prokaryotic microorganisms known as microbiota (Potgieter et al. 2015). Interestingly, microbiota behaves as a dynamic agent depending on environmental conditions and other host substrates (Potgieter et al. 2015). Microbiota has been widely involved in several diseases such as diabetes, obesity and other autoimmune diseases as inflammatory bowel disease or multiple sclerosis. In the field of neurodegenerative diseases, there are some evidences supporting its potential role in AD and Parkinson’s disease (Tremlett et al. 2017). Regarding ALS, microbiota changes have been reported in ALS murine models (Fang 2016; Zhang et al. 2017) thus postulating it as both a new pathogenic issue to elucidate and at the same time as a new potential therapeutic approach.
The evidences of fungal involvement are also very limited. Recently, one study described fungal infection traces (fungal DNA and fungal antigens) in CSF and brain tissue from a limited subset of ALS patients (Alonso et al. 2015). Although these findings are doubtlessly interesting, we consider that future studies with larger cohorts of patients are needed to better clarify this potential relationship.
2.3. Lifestyle and demographic factors
Social factors, lifestyle and comorbidity
During the last decade, several groups have been studying how lifestyle and comorbid situations predispose/modulate ALS development. This is a rapidly growing emerging field which will doubtlessly help us to better understand the disease and that will probably provide us both new pathogenic and preventive approaches. In this section, we will discuss the most interesting issues concerning this field.
2.3.1. Socioeconomic factors
Classically, richness has been inversely correlated to neurodegenerative diseases such as dementia (Satizabal et al. 2016). In this way, those countries or regions with lower incomes had a higher age-adjusted incidence of dementia, probably due to insufficient prevention of cardiovascular risk factors, as well as less optimal strategies for early diagnosis.
When evaluating the role of richness in a particular disease, it should be realised that richness and socioeconomic status are complex factors that are commonly associated to other than merely monetary income, such as race, education level, type of job or the access to healthcare system and preventive measures. To date, there are two studies which have addressed the association between richness or other socioeconomic parameters and ALS both with intriguing results (Roberts et al. 2016; Santurtun et al. 2016b). First, our group correlated ALS mortality and richness across Spanish provinces during an 11-year period (2000–2011). Our results demonstrated a significant positive correlation between gross domestic product (GDP) per capita and ALS mortality (r = 0.73; p < 0.00003) (Santurtun et al. 2016b). Subsequently, after performing an economic sector-stratified analysis, we observed a clear positive correlation between the degree of development of the industrial sector and ALS mortality (r = 0.73; p < 0.0001). By contrast, those regions which had a more developed primary (cattle and fishing) sector exhibited significant lower ALS mortality (r = − 0.41; p < 0.0001) (Santurtun et al. 2016b). Although our results show a clear positive correlation between richness and ALS, they might be influenced by other confounding factors such as pollution or the distinct styles of life (in terms of nutrition, physical activity, social habits) which typically vary among the different activity sectors. Shortly after this study, Roberts et al. studied the association between race/ethnicity, socioeconomic status and ALS in USA (Roberts et al. 2016). They included more than 2 million of people with a follow-up period of more than 30 years. In their study, they reported lower ALS incidence in non-Hispanic blacks, Hispanics, and other non-Hispanic races when compared with white people. However, after adjusting by race and ethnicity, they did not find a significant association between income and ALS, thus highlighting race as potential confounder when evaluating socioeconomic status and welfare. Altogether, these studies bring up a new important issue to clarify, providing a starting point for future studies that will have to elucidate the precise factors and mechanisms involved in these economy-related associations.
2.3.2. Tobacco and alcohol
The role of smoking and alcohol consumption has been widely studied in many neurodegenerative diseases (Plassman et al. 2010). Regarding ALS, multiple studies have tried to elucidate if smokers were more likely to develop ALS (Gallo et al. 2009; Schmidt et al. 2010). This hypothesis lies on several facts, such as the high concentration of toxic substances in cigarettes, including lead, formaldehyde, selenium or cadmium. Recently, Alonso et al. (2010) published a meta-analysis of 18 studies previously published. They reported a pooled relative risk of 1.28 (95% CI 0.97–1.68). After gender-stratification, they described a significant increase of risk among smoker women (relative risk 1.66; 1.31–2.10), without significant differences reported in males (Alonso et al. 2010). In conclusion, although there is not an overall strong association between smoking and ALS risk, tobacco seems to be associated with increased risk of ALS in women.
Regarding alcohol consumption, epidemiological studies have not reported a clear relationship between alcoholism and ALS (Nelson et al. 2000). Importantly, in some of these studies, smoking seemed to behave as a confounding factor, suggesting a non-causal association between alcohol intake and risk of ALS development (Nelson et al. 2000).
2.3.3. Physical activity
Since the appearance of several ALS cases in professional sportsmen such as Lou Gehrig or Italian football players, many studied have tried to elucidate if exercise is associated with an increased risk of ALS (Feddermann-Demont et al. 2017; Janssen et al. 2017; Pearce et al. 2015; Kuwahara and Sato 2013). However, there is some controversy because some of them have reported a positive association (Hamidou et al. 2014) while others did not find it. The first prospective cohort study on ALS and physical activity was recently published by Gallo et al. (2016). It was based on the EPIC cohort (European Prospective Investigation into Cancer and Nutrition) and included a total of 472,100 individuals and 219 ALS deaths. In that study, after adjusting by potential confounding factors, authors reported that physical activity was weakly inversely associated with ALS mortality with a borderline statistically significant trend (p = 0.042), with those physically active being 33% less likely to die from ALS compared to those inactive (HR = 0.67; 95% CI 0.42–1.06) (Gallo et al. 2016). A few months later, Eaglehouse et al. evaluated the role of exercise in a cohort of postmenopausal women aged 50 to 79 years (Eaglehouse et al. 2016). In their study, they identified 165 ALS cases among a cohort of more than 161,000 women followed up for 10 years. Interestingly, they found a positive significant association between women practising strenuous exercise and ALS (odds ratio 1.56; 95% CI, 1.02–2.37; p = 0.04) (Eaglehouse et al. 2016). Similar tendencies were reported in a cohort of more than 200,000 cross-country skiers in Sweden. Interestingly, long-distance cross-country skiing was associated with a higher risk of ALS, but only among the best skiers while recreational skiers appeared to have a largely reduced risk (Fang et al. 2016). In addition, other studies have directly related the gruelling exercise practice, at a professional level, with the risk of ALS (Gotkine et al. 2014).
Taken together, these seminal studies suggested that moderate physical activity was associated to a lower ALS risk, while strenuous exercise, particularly at a professional level and during early stages of life, could promote disease onset.
2.3.4. Body mass index, nutrition and diabetes
The relationship between body mass index (BMI) and ALS appeared as a tantalising question for many years. In this line, clinical case series consistently reported that patients with ALS were generally lean, with a normal or low BMI (Desport et al. 1999; Vaisman et al. 2009). On the other hand, several lines of evidence suggested that patients with ALS have an energetic imbalance (Zufiria et al. 2016; Dupuis et al. 2011).
Recently, Gallo et al. (2013) performed a cohort study to evaluate the association between BMI and ALS risk. It was also based on the EPIC cohort and included more than 518,000 subjects. During a follow-up period of 13 years, 222 ALS deaths occurred. Remarkably, a significant negative association between BMI and ALS was noted. In men, a linear decrease of risk per unit of BMI was observed (hazard ratio = 0.93, 95% confidence interval 0.86–0.99). This tendency was even more marked in the female group, in which ALS risk was more than threefold increased for those underweight compared with normal-weight women (Gallo et al. 2013).
Otherwise, nutrition seems to be important not only at presymptomatic stages but also when the disease is already established. In this line, several studies have tried to assess the role of nutrition in the progression of the disease (Okamoto et al. 2007; Fitzgerald et al. 2013). A case-control study involving 153 ALS patients and 306 matched controls evaluated pre-illness dietary patters in Japan. Interestingly, the investigators found that high intakes of carbohydrate and low intakes of fat and fatty acids (both saturated, mono and polyunsaturated fatty acids), when combined, were linked to an increased the risk of ALS (Okamoto et al. 2007). Not long after, Nieves et al. conducted a study to evaluate the association between nutrients and ALS function in more than 300 ALS patients (178 men and 124 women) at initial stages of the disease (Nieves et al. 2016). After complex software analysis, authors concluded that those patients who regularly consumed antioxidants, carotenes, fruits and vegetables had a better preservation of several disease parameters (Nieves et al. 2016). Regarding carotene-related products, a number of studies have supported their role in ALS pathogenesis (Riancho et al. 2016b). Specifically, we have demonstrated in the SOD1 murine model of ALS that chronic treatment with the retinoid agonist bexarotene had marked neuroprotective effects throughout both proteostasis and astroglial response modulation, thus appearing as a new potential therapeutic approach (Riancho et al. 2015, 2016a).
Among metabolic and cardiovascular diseases, diabetes is probably the one harbouring the strongest association. In this line, one of the most important studied was based on the Danish National Register and performed by Kioumourtzoglou et al. (2015). They included 3650 ALS patients and 365,000 control subjects matched by gender and age between 1982 and 2009. Overall, they found that patients with diabetes had a significantly lower risk of ALS (odds ratio 0.61; 95% CI 0.46–0.80). Remarkably, this protective association was stronger in individuals with a more advanced age. In this way, the odds ratio for patients ageing 40 years or less was 1.66 (95% CI, 0.85–3.21) whereas in those subjects ageing 40 or more, the odds ratio markedly decreased to 0.52 (95% CI, 0.39–0.70) (Kioumourtzoglou et al. 2015). This intriguing finding could be related to the different pathogenic mechanisms underlying both types 1 and 2 diabetes. In this way, type 1 diabetes commonly presents at early ages, has a clear autoimmune aetiology, and is commonly associated to both low uric acid levels and hypoglycaemic states which seem to exert some degree of neurotoxic effects (Alberti and Zimmet 1998; Bjornstad et al. 2014; Leese et al. 2003). By contrast, in people over 40 years, type 2 diabetes is much more prevalent. This is commonly associated with metabolic syndrome, with increased BMI, patients commonly tends to hyperglycemia and are sometimes treated with potential neuroprotective drugs, such as PPAR agonists (Alberti and Zimmet 1998; Hyder et al. 2006; Riancho 2016). An additional explanation for this interaction between age and diabetes on ALS risk could be related to a stronger genetic component in ALS cases appearing in younger individuals (Daneman 2006).
In addition, several reports found a protective association between other vascular risk factors, such as high cholesterol (Seelen et al. 2014) and hyperlipidemia (Dupuis et al. 2008, 2011) and ALS. According to this, a recent study has also pointed out the relationship between a favourable cardiovascular fitness profile and an increased ALS susceptibility (Visser et al. 2017a). However, in all of these situations, correlation rates seemed to be rather weak.
2.3.5. Physical trauma and cerebrovascular injury
Head injury and physical trauma in general have been reported as risk factors for other neurodegenerative disorders such as Alzheimer’s (Van Den et al. 2007) and Parkinson’s diseases (Goldman et al. 2006). Regarding ALS, the identification of a high incidence of ALS among American football players (Feddermann-Demont et al. 2017; Kuwahara and Sato 2013), led to hypothesise that head injury/extensive physical trauma might promote disease (Kuwahara and Sato 2013; Pearce et al. 2015). Several case-control studies in ALS patients have reported an association with physical trauma or head injury, but there exists a scientist agreement that such studies should be taken with caution because they might be influenced by recall bias. Turner et al. (2010) studied the relationship between head and non-head trauma and ALS during a 36-year period. Initially, they reported an increased risk for ALS after head injury (relative risk 1.5; 95% CI 1.1–2.1). However, after adjusting by time, the evidence for increased risk was restricted to the first year after injury, concluding that this was most likely the consequence of an incipient ALS causing a tendency to fall than a cause itself (Turner et al. 2010). In line with this concept which postulated that head injury could not be a cause but a consequence of latent ALS, Watanabe and Watanabe (2017) very recently published a meta-analyses, including 16 studies, to evaluate such a possibility of reverse causation considering time lags between the incidence of head injuries and the occurrence of ALS. As expected, the meta-analyses reported a statistically significant association between head injuries and ALS (OR 1.45, 95% CI 1.21–1.74). However, when considering the time lags between the experience of head injuries and diagnosis of ALS, the association was weaker (OR 1.21, 95% CI 1.01–1.46, time lag ≥ 1 year) or not significant (e.g. OR 1.16, 95% CI 0.84–1.59, time lag ≥ 3 years). Although these data did not exclude an association between head injuries and ALS, they suggested that the relationship between head injury and ALS might have been overestimated. Future prospective studies considering the time lags between the occurrence of head injuries and the ALS onset will be needed to clarify this issue (Tanaka et al. 2012).
The risk of ALS in patients who have suffered a non-traumatic cerebral injury also seemed to be increased. In this line, a study recently evaluated the risk of ALS in patients who had previously presented arterio-venous malformations (AVMs), stroke, transient ischaemic attack (TIA) and subarachnoid haemorrhage (SAH) (Turner et al. 2016). Remarkably, authors found a significant association among patients with previous AVMs, stroke and TIA. This risk was particularly increased in patients with prior AVM (relative risk 2.69; 95% CI 1.23 to 5.12; p = 0.005) (Turner et al. 2016).
2.3.6. Autoimmune diseases
Inflammation and autoimmune disorders are gaining relevance in the pathogenesis of ALS (Riancho et al. 2016c). In this way, glial cell disorders with inflammatory activation appeared as a crucial step in MN degeneration (Zufiria et al. 2016). Interestingly, this is the basis of several ongoing clinical trials with immune modulators (Trias et al. 2016). In this line, the association of ALS with autoimmunity and autoimmune disorders has received increasing attention in recent years. Turner et al. (2013) recently assessed the risk of ALS in patients with autoimmune disease. The study was based on the UK hospital record from 1999 to 2011. The authors reported a significant higher number of ALS cases among subjects with previous autoimmune disease. Remarkably, the ALS risk was specially enlarged (relative risk higher than 4) among patients with type 1 diabetes, multiple sclerosis, myasthenia gravis and polymyositis (Turner et al. 2013). Future epidemiological and pathogenic studies will help to precisely elucidate the role of inflammation in the genesis of ALS.
2.3.7. Cancer
A few studies have examined the risk of cancer in neurodegenerative diseases such as Alzheimer’s and Parkinson’s disease, reporting an inverse association between these entities and the overall risk of cancer (Driver et al. 2012; Lo et al. 2010). Regarding ALS, some of the ALS-causative genes, such as FUS or UBQLN play important roles in various oncogenic pathways (Dormann and Haass 2013; Shah et al. 2015). In this scenario, several epidemiologic studies have been performed without having identified an overall increase in the risk of developing ALS among cancer survivors (Freedman et al. 2013, 2014; Fang et al. 2013). Recently, Gibson et al. (2016) conducted an observational longitudinal study based on the Utah Population Dabatase including 1081 ALS patients. Overall, cancer was associated to a lower risk of ALS (hazard ratio 0.80; 95% CI 0.66–0.96; p = 0.014). However, an increased risk of ALS was found in those patients with salivary (hazard ratio 5.27; 95% CI 1.09–15.40; p = 0.041,) and testicular (hazard ratio 3.82; 95% CI 1.06–9.62; p = 0.042) cancers (Gibson et al. 2016). There are also evidences supporting the association between cancer and ALS. In this line, it has recently been reported that the suppressor cancer gene BRCA1, associated with both ovarian and breast cancer, was expressed in human microglia and that it appeared dysregulated in both human and animal models of ALS (Noristani et al. 2015).
Taken together, these results open new perspectives in ALS pathogenesis, but further studies are necessary to elucidate this issue. Moreover, the potential relationship between cancer and ALS points toward novel research strategies such as investigating the role of oncogenic proteins in neurodegenerative diseases.
3. Concluding remarks
In conclusion, ALS appears as the final result of a complex interplay between genes, environment, ageing and perhaps other unidentified factors. During recent years, not only external but also internal environmental conditions have gained more relevance in the genesis of the disease and are currently providing new pathogenic clues.
Although our knowledge of the disease has substantially improved and will continue improving in the future, crucial questions such as how environment and ageing influence familiar forms of the disease or the precise mechanisms (epigenetic modifications, direct toxicity) by which each environmental condition induces motor neuron degeneration remain to be elucidated. In our opinion, investigation strategies in ALS should be reconsidered in order to reach these goals. In this line, for each individual environmental factor, a holistic approach has to be performed. This assessment should include epidemiological, genetic, animal models and other basic tools in order to assess main pathogenic issues involved in ALS. These investigation approaches will doubtlessly improve our dynamic concept of the motor neuron degeneration and also will provide novel opportunities to identify new diagnostic and therapeutic strategies.
References
Abhinav K, Al Chalabi A, Hortobagyi T, Leigh PN (2007) Electrical injury and amyotrophic lateral sclerosis: a systematic review of the literature. J Neurol Neurosurg Psychiatry 78:450–453
Adams CR, Ziegler DK, Lin JT (1983) Mercury intoxication simulating amyotrophic lateral sclerosis. JAMA 250:642–643
Al Chalabi A, Hardiman O (2013) The epidemiology of ALS: a conspiracy of genes, environment and time. Nat Rev Neurol 9:617–628
Al Chalabi A, Fang F, Hanby MF, Leigh PN, Shaw CE, Ye W, Rijsdijk F (2010) An estimate of amyotrophic lateral sclerosis heritability using twin data. J Neurol Neurosurg Psychiatry 81:1324–1326
Alberti KG, Zimmet PZ (1998) Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: diagnosis and classification of diabetes mellitus provisional report of a WHO consultation. Diabet Med 15:539–553
Alonso A, Logroscino G, Hernan MA (2010) Smoking and the risk of amyotrophic lateral sclerosis: a systematic review and meta-analysis. J Neurol Neurosurg Psychiatry 81:1249–1252
Alonso R, Pisa D, Marina AI, Morato E, Rabano A, Rodal I, Carrasco L (2015) Evidence for fungal infection in cerebrospinal fluid and brain tissue from patients with amyotrophic lateral sclerosis. Int J Biol Sci 11:546–558
Barbeito AG, Martinez-Palma L, Vargas MR, Pehar M, Manay N, Beckman JS, Barbeito L, Cassina P (2010) Lead exposure stimulates VEGF expression in the spinal cord and extends survival in a mouse model of ALS. Neurobiol Dis 37:574–580
Bassett T, Bach P, Chan HM (2012) Effects of methylmercury on the secretion of pro-inflammatory cytokines from primary microglial cells and astrocytes. Neurotoxicology 33:229–234
Bjornstad P, Snell-Bergeon JK, McFann K, Wadwa RP, Rewers M, Rivard CJ, Jalal D, Chonchol MB, Johnson RJ, Maahs DM (2014) Serum uric acid and insulin sensitivity in adolescents and adults with and without type 1 diabetes. J Diabetes Complicat 28:298–304
Boccia S, Sayed-Tabatabaei FA, Persiani R, Gianfagna F, Rausei S, Arzani D, La Greca A, D'Ugo D, La Torre G, van Duijn CM, Ricciardi G (2007) Polymorphisms in metabolic genes, their combination and interaction with tobacco smoke and alcohol consumption and risk of gastric cancer: a case-control study in an Italian population. BMC Cancer 7:206
Bradley WG (2015) The John Walton Muscular Dystrophy Research Centre in the University of Newcastle and the BMAA theory of motor neuron disease. J Neuromuscul Dis 2:S77–S81
Buee-Scherrer V, Buee L, Hof PR, Leveugle B, Gilles C, Loerzel AJ, Perl DP, Delacourte A (1995) Neurofibrillary degeneration in amyotrophic lateral sclerosis/parkinsonism-dementia complex of Guam. Immunochemical characterization of tau proteins=. Am J Pathol 146:924–932
Caller TA, Chipman JW, Field NC, Stommel EW (2013) Spatial analysis of amyotrophic lateral sclerosis in northern New England, USA, 1997-2009. Muscle Nerve 48:235–241
Casteignau A, Fontan A, Morillo A, Oliveros JA, Segales J (2006) Clinical, pathological and toxicological findings of a iatrogenic selenium toxicosis case in feeder pigs. J Vet Med A Physiol Pathol Clin Med 53:323–326
Daneman D (2006) Type 1 diabetes. Lancet 367:847–858
Desport JC, Preux PM, Truong TC, Vallat JM, Sautereau D, Couratier P (1999) Nutritional status is a prognostic factor for survival in ALS patients. Neurology 53:1059–1063
Dormann D, Haass C (2013) Fused in sarcoma (FUS): an oncogene goes awry in neurodegeneration. Mol Cell Neurosci 56:475–486
Douville R, Liu J, Rothstein J, Nath A (2011) Identification of active loci of a human endogenous retrovirus in neurons of patients with amyotrophic lateral sclerosis. Ann Neurol 69:141–151
Driver JA, Beiser A, Au R, Kreger BE, Splansky GL, Kurth T, Kiel DP, Lu KP, Seshadri S, Wolf PA (2012) Inverse association between cancer and Alzheimer’s disease: results from the Framingham Heart Study. BMJ 344:e1442
Dupuis L, Corcia P, Fergani A, Gonzalez De Aguilar JL, Bonnefont-Rousselot D, Bittar R, Seilhean D, Hauw JJ, Lacomblez L, Loeffler JP, Meininger V (2008) Dyslipidemia is a protective factor in amyotrophic lateral sclerosis. Neurology 70:1004–1009
Dupuis L, Pradat PF, Ludolph AC, Loeffler JP (2011) Energy metabolism in amyotrophic lateral sclerosis. Lancet Neurol 10:75–82
Eaglehouse YL, Talbott EO, Chang Y, Kuller LH (2016) Participation in physical activity and risk for amyotrophic lateral sclerosis mortality among postmenopausal women. JAMA Neurol 73:329–336
Estevez AO, Mueller CL, Morgan KL, Szewczyk NJ, Teece L, Miranda-Vizuete A, Estevez M (2012) Selenium induces cholinergic motor neuron degeneration in Caenorhabditis elegans. Neurotoxicology 33:1021–1032
Falone S, Mirabilio A, Carbone MC, Zimmitti V, Di Loreto S, Mariggio MA, Mancinelli R, Di Ilio C, Amicarelli F (2008) Chronic exposure to 50Hz magnetic fields causes a significant weakening of antioxidant defence systems in aged rat brain. Int J Biochem Cell Biol 40:2762–2770
Fang X (2016) Potential role of gut microbiota and tissue barriers in Parkinson's disease and amyotrophic lateral sclerosis. Int J Neurosci 126:771–776
Fang F, Kwee LC, Allen KD, Umbach DM, Ye W, Watson M, Keller J, Oddone EZ, Sandler DP, Schmidt S, Kamel F (2010) Association between blood lead and the risk of amyotrophic lateral sclerosis. Am J Epidemiol 171:1126–1133
Fang F, Al Chalabi A, Ronnevi LO, Turner MR, Wirdefeldt K, Kamel F, Ye W (2013) Amyotrophic lateral sclerosis and cancer: a register-based study in Sweden. Amyotroph Lateral Scler Frontotemporal Degener 14:362–368
Fang F, Hallmarker U, James S, Ingre C, Michaelsson K, Ahlbom A, Feychting M (2016) Amyotrophic lateral sclerosis among cross-country skiers in Sweden. Eur J Epidemiol 31:247–253
Feddermann-Demont N, Junge A, Weber KP, Weller M, Dvorak J, Tarnutzer AA (2017) Prevalence of potential sports-associated risk factors in Swiss amyotrophic lateral sclerosis patients. Brain Behav 7:e00630
Field NC, Metcalf JS, Caller TA, Banack SA, Cox PA, Stommel EW (2013) Linking beta-methylamino-L-alanine exposure to sporadic amyotrophic lateral sclerosis in Annapolis, MD. Toxicon 70:179–183
Fitzgerald KC, O'Reilly EJ, Fondell E, Falcone GJ, McCullough ML, Park Y, Kolonel LN, Ascherio A (2013) Intakes of vitamin C and carotenoids and risk of amyotrophic lateral sclerosis: pooled results from 5 cohort studies. Ann Neurol 73:236–245
Freedman DM, Curtis RE, Daugherty SE, Goedert JJ, Kuncl RW, Tucker MA (2013) The association between cancer and amyotrophic lateral sclerosis. Cancer Causes Control 24:55–60
Freedman DM, Wu J, Daugherty SE, Kuncl RW, Enewold LR, Pfeiffer RM (2014) The risk of amyotrophic lateral sclerosis after cancer in U.S. elderly adults: a population-based prospective study. Int. J Cancer 135:1745–1750
Gajdusek DC, Salazar AM (1982) Amyotrophic lateral sclerosis and Parkinsonian syndromes in high incidence among the Auyu and Jakai people of west New Guinea. Neurology 32:107–126
Gallo V, Bueno-De-Mesquita HB, Vermeulen R, Andersen PM, Kyrozis A, Linseisen J, Kaaks R, Allen NE, Roddam AW, Boshuizen HC, Peeters PH, Palli D, Mattiello A, Sieri S, Tumino R, Jimenez-Martin JM, Diaz MJ, Suarez LR, Trichopoulou A, Agudo A, Arriola L, Barricante-Gurrea A, Bingham S, Khaw KT, Manjer J, Lindkvist B, Overvad K, Bach FW, Tjonneland A, Olsen A, Bergmann MM, Boeing H, Clavel-Chapelon F, Lund E, Hallmans G, Middleton L, Vineis P, Riboli E (2009) Smoking and risk for amyotrophic lateral sclerosis: analysis of the EPIC cohort. Ann Neurol 65:378–385
Gallo V, Wark PA, Jenab M, Pearce N, Brayne C, Vermeulen R, Andersen PM, Hallmans G, Kyrozis A, Vanacore N, Vahdaninia M, Grote V, Kaaks R, Mattiello A, Bueno-De-Mesquita HB, Peeters PH, Travis RC, Petersson J, Hansson O, Arriola L, Jimenez-Martin JM, Tjonneland A, Halkjaer J, Agnoli C, Sacerdote C, Bonet C, Trichopoulou A, Gavrila D, Overvad K, Weiderpass E, Palli D, Quiros JR, Tumino R, Khaw KT, Wareham N, Barricante-Gurrea A, Fedirko V, Ferrari P, Clavel-Chapelon F, Boutron-Ruault MC, Boeing H, Vigl M, Middleton L, Riboli E, Vineis P (2013) Prediagnostic body fat and risk of death from amyotrophic lateral sclerosis: the EPIC cohort. Neurology 80:829–838
Gallo V, Vanacore N, Bueno-De-Mesquita HB, Vermeulen R, Brayne C, Pearce N, Wark PA, Ward HA, Ferrari P, Jenab M, Andersen PM, Wennberg P, Wareham N, Katzke V, Kaaks R, Weiderpass E, Peeters PH, Mattiello A, Pala V, Barricante A, Chirlaque MD, Travier N, Travis RC, Sanchez MJ, Pessah-Rasmussen H, Petersson J, Tjonneland A, Tumino R, Quiros JR, Trichopoulou A, Kyrozis A, Oikonomidou D, Masala G, Sacerdote C, Arriola L, Boeing H, Vigl M, Claver-Chapelon F, Middleton L, Riboli E, Vineis P (2016) Physical activity and risk of amyotrophic lateral sclerosis in a prospective cohort study. Eur J Epidemiol 31:255–266
Geser F, Winton MJ, Kwong LK, Xu Y, Xie SX, Igaz LM, Garruto RM, Perl DP, Galasko D, Lee VM, Trojanowski JQ (2008) Pathological TDP-43 in Parkinsonism-dementia complex and amyotrophic lateral sclerosis of Guam. Acta Neuropathol 115:133–145
Gibson SB, Abbott D, Farnham JM, Thai KK, McLean H, Figueroa KP, Bromberg MB, Pulst SM, Cannon-Albright L (2016) Population-based risks for cancer in patients with ALS. Neurology 87:289–294
Goldman SM, Tanner CM, Oakes D, Bhudhikanok GS, Gupta A, Langston JW (2006) Head injury and Parkinson’s disease risk in twins. Ann Neurol 60:65–72
Gotkine M, Friedlander Y, Hochner H (2014) Triathletes are over-represented in a population of patients with ALS. Amyotroph Lateral Scler Frontotemporal Degener 15:534–536
Gurel A, Coskun O, Armutcu F, Kanter M, Ozen OA (2005) Vitamin E against oxidative damage caused by formaldehyde in frontal cortex and hippocampus: biochemical and histological studies. J Chem Neuroanat 29:173–178
Hamidou B, Couratier P, Besancon C, Nicol M, Preux PM, Marin B (2014) Epidemiological evidence that physical activity is not a risk factor for ALS. Eur J Epidemiol 29:459–475
Hyder F, Patel AB, Gjedde A, Rothman DL, Behar KL, Shulman RG (2006) Neuronal-glial glucose oxidation and glutamatergic-GABAergic function. J Cereb Blood Flow Metab 26:865–877
Ishiura H, Takahashi Y, Mitsui J, Yoshida S, Kihira T, Kokubo Y, Kuzuhara S, Ranum LP, Tamaoki T, Ichikawa Y, Date H, Goto J, Tsuji S (2012) C9ORF72 repeat expansion in amyotrophic lateral sclerosis in the Kii peninsula of Japan. Arch Neurol 69:1154–1158
Janssen PH, Mandrekar J, Mielke MM, Ahlskog JE, Boeve BF, Josephs K, Savica R (2017) High School Football and Late-Life Risk of Neurodegenerative Syndromes, 1956-1970. Mayo Clin Proc 92:66–71
Johnson FO, Atchison WD (2009) The role of environmental mercury, lead and pesticide exposure in development of amyotrophic lateral sclerosis. Neurotoxicology 30:761–765
Kamel F, Umbach DM, Hu H, Munsat TL, Shefner JM, Taylor JA, Sandler DP (2005) Lead exposure as a risk factor for amyotrophic lateral sclerosis. Neurodegener Dis 2:195–201
Kamel F, Umbach DM, Bedlack RS, Richards M, Watson M, Alavanja MC, Blair A, Hoppin JA, Schmidt S, Sandler DP (2012) Pesticide exposure and amyotrophic lateral sclerosis. Neurotoxicology 33:457–462
Kilness AW, Hichberg FH (1977) Amyotrophic lateral sclerosis in a high selenium environment. JAMA 237:2843–2844
Kioumourtzoglou MA, Rotem RS, Seals RM, Gredal O, Hansen J, Weisskopf MG (2015) Diabetes mellitus, obesity, and diagnosis of amyotrophic lateral sclerosis: a population-based study. JAMA Neurol 72:905–911
Kuwahara S, Sato Y (2013) Retired American football players have a four times higher chance of getting Alzheimer disease or amyotrophic lateral sclerosis. Brain Nerve 65:996–997
Kuzuhara S (2011) Muro disease: amyotrophic lateral sclerosis/Parkinsonism-dementia complex in Kii peninsula of Japan. Brain Nerve 63:119–129
Kuzuhara S, Kokubo Y (2005) Atypical Parkinsonism of Japan: amyotrophic lateral sclerosis-Parkinsonism-dementia complex of the Kii peninsula of Japan (Muro disease): an update. Mov Disord 20(Suppl 12):S108–S113
Lannuzel A, Mecharles S, Tressieres B, Demoly A, Alhendi R, Hedreville-Tablon MA, Alecu C (2015) Clinical varieties and epidemiological aspects of amyotrophic lateral sclerosis in the Caribbean island of Guadeloupe: a new focus of ALS associated with Parkinsonism. Amyotroph Lateral Scler Frontotemporal Degener 16:216–223
Leese GP, Wang J, Broomhall J, Kelly P, Marsden A, Morrison W, Frier BM, Morris AD (2003) Frequency of severe hypoglycemia requiring emergency treatment in type 1 and type 2 diabetes: a population-based study of health service resource use. Diabetes Care 26:1176–1180
Li W, Lee MH, Henderson L, Tyagi R, Bachani M, Steiner J, Campanac E, Hoffman DA, von Geldern G, Johnson K, Maric D, Morris HD, Lentz M, Pak K, Mammen A, Ostrow L, Rothstein J, Nath A (2015) Human endogenous retrovirus-K contributes to motor neuron disease. Sci Transl Med 7:307ra153
Lo RY, Tanner CM, Van Den Eeden SK, Albers KB, Leimpeter AD, Nelson LM (2010) Comorbid cancer in Parkinson’s disease. Mov Disord 25:1809–1817
MacGowan DJ, Scelsa SN, Imperato TE, Liu KN, Baron P, Polsky B (2007) A controlled study of reverse transcriptase in serum and CSF of HIV-negative patients with ALS. Neurology 68:1944–1946
Malek AM, Barchowsky A, Bowser R, Youk A, Talbott EO (2012) Pesticide exposure as a risk factor for amyotrophic lateral sclerosis: a meta-analysis of epidemiological studies: pesticide exposure as a risk factor for ALS. Environ Res 117:112–119
Maraldi T, Riccio M, Zambonin L, Vinceti M, De Pol A, Hakim G (2011) Low levels of selenium compounds are selectively toxic for a human neuron cell line through ROS/RNS increase and apoptotic process activation. Neurotoxicology 32:180–187
Masseret E, Banack S, Boumediene F, Abadie E, Brient L, Pernet F, Juntas-Morales R, Pageot N, Metcalf J, Cox P, Camu W (2013) Dietary BMAA exposure in an amyotrophic lateral sclerosis cluster from southern France. PLoS One 8:e83406
Morahan JM, Yu B, Trent RJ, Pamphlett R (2007) Genetic susceptibility to environmental toxicants in ALS. Am J Med Genet B Neuropsychiatr Genet 144B:885–890
Murch SJ, Cox PA, Banack SA (2004a) A mechanism for slow release of biomagnified cyanobacterial neurotoxins and neurodegenerative disease in Guam. Proc Natl Acad Sci U S A 101:12228–12231
Murch SJ, Cox PA, Banack SA, Steele JC, Sacks OW (2004b) Occurrence of beta-methylamino-l-alanine (BMAA) in ALS/PDC patients from Guam. Acta Neurol Scand 110:267–269
Nelson LM, McGuire V, Longstreth WT Jr, Matkin C (2000) Population-based case-control study of amyotrophic lateral sclerosis in western Washington state. I Cigarette smoking and alcohol consumption. Am J Epidemiol 151:156–163
Nicoletti A, Vasta R, Venti V, Mostile G, Lo FS, Patti F, Scillieri R, De Cicco D, Volanti P, Marziolo R, Maimone D, Fiore M, Ferrante M, Zappia M (2016) The epidemiology of amyotrophic lateral sclerosis in the Mount Etna region: a possible pathogenic role of volcanogenic metals. Eur J Neurol 23:964–972
Nie CL, Wang XS, Liu Y, Perrett S, He RQ (2007) Amyloid-like aggregates of neuronal tau induced by formaldehyde promote apoptosis of neuronal cells. BMC Neurosci 8:9
Nieves JW, Gennings C, Factor-Litvak P, Hupf J, Singleton J, Sharf V, Oskarsson B, Fernandes Filho JA, Sorenson EJ, D'Amico E, Goetz R, Mitsumoto H (2016) Association between dietary intake and function in amyotrophic lateral sclerosis. JAMA Neurol 73:1425–1432
Noristani HN, Sabourin JC, Gerber YN, Teigell M, Sommacal A, Vivanco M, Weber M, Perrin FE (2015) Brca1 is expressed in human microglia and is dysregulated in human and animal model of ALS. Mol Neurodegener 10:34
Okamoto K, Kihira T, Kondo T, Kobashi G, Washio M, Sasaki S, Yokoyama T, Miyake Y, Sakamoto N, Inaba Y, Nagai M (2007) Nutritional status and risk of amyotrophic lateral sclerosis in Japan. Amyotroph Lateral Scler 8:300–304
Pamphlett R, Waley P (1998) Mercury in human spinal motor neurons. Acta Neuropathol 96:515–519
Pearce N, Gallo V, McElvenny D (2015) Head trauma in sport and neurodegenerative disease: an issue whose time has come? Neurobiol Aging 36:1383–1389
Pinkerton LE, Hein MJ, Meyers A, Kamel F (2013) Assessment of ALS mortality in a cohort of formaldehyde-exposed garment workers. Amyotroph Lateral Scler Frontotemporal Degener 14:353–355
Plassman BL, Williams JW Jr, Burke JR, Holsinger T, Benjamin S (2010) Systematic review: factors associated with risk for and possible prevention of cognitive decline in later life. Ann Intern Med 153:182–193
Potgieter M, Bester J, Kell DB, Pretorius E (2015) The dormant blood microbiome in chronic, inflammatory diseases. FEMS Microbiol Rev 39:567–591
Poulletier DG, Ruffie G, Taxile M, Ladeveze E, Hurtier A, Haro E, Duleu S, Charlet DS, Billaudel B, Geffard M, Veyret B, Lagroye I (2009) Amyotrophic lateral sclerosis (ALS) and extremely-low frequency (ELF) magnetic fields: a study in the SOD-1 transgenic mouse model. Amyotroph Lateral Scler 10:370–373
Praline J, Guennoc AM, Limousin N, Hallak H, de Toffol B, Corcia P (2007) ALS and mercury intoxication: a relationship? Clin Neurol Neurosurg 109:880–883
Reed DM, Brody JA (1975) Amyotrophic lateral sclerosis and Parkinsonism-dementia on Guam, 1945-1972. I Descriptive epidemiology. Am J Epidemiol 101:287–301
Reed D, Plato C, Elizan T, Kurland LT (1966) The amyotrophic lateral sclerosis/Parkinsonism-dementia complex: a ten-year follow-up on Guam. I Epidemiologic studies. Am J Epidemiol 83:54–73
Riancho J (2016) Retinoids and PPAR agonists: promising partners in neurodegenerative diseases? Free Radic Biol Med 97:616–617
Riancho J, Ruiz-Soto M, Berciano MT, Berciano J, Lafarga M (2015) Neuroprotective effect of bexarotene in the SOD1(G93A) mouse model of amyotrophic lateral sclerosis. Front Cell Neurosci 9:250
Riancho J, Berciano MT, Berciano J, Lafarga M (2016a) Relaunching an old drug: the potential role of bexarotene in neurodegenerative diseases. J Neurol 263:177–178
Riancho J, Berciano MT, Ruiz-Soto M, Berciano J, Landreth G, Lafarga M (2016b) Retinoids and motor neuron disease: potential role in amyotrophic lateral sclerosis. J Neurol Sci 360:115–120
Riancho J, Gonzalo I, Ruiz-Soto M, Berciano J (2016c) Why do motor neurons degenerate? Actualization in the pathogenesis of amyotrophic lateral sclerosis. Neurologia
Riancho J, Lozano-Cuesta P, Santurtun A, Sanchez-Juan P, Lopez-Vega JM, Berciano J, Polo JM (2016d) Amyotrophic lateral sclerosis in northern Spain 40 years later: what has changed? Neurodegener Dis 16:337–341
Roberts AL, Johnson NJ, Cudkowicz ME, Eum KD, Weisskopf MG (2015) Job-related formaldehyde exposure and ALS mortality in the USA. J Neurol Neurosurg Psychiatry
Roberts AL, Johnson NJ, Chen JT, Cudkowicz ME, Weisskopf MG (2016) Race/ethnicity, socioeconomic status, and ALS mortality in the United States. Neurology 87:2300–2308
Rooney J (2011) Further thoughts on mercury, epigenetics, genetics and amyotrophic lateral sclerosis. Neurodegener Dis 8:523–524
Rooney J, Vajda A, Heverin M, Elamin M, Crampsie A, McLaughlin R, Staines A, Hardiman O (2015a) Spatial cluster analysis of population amyotrophic lateral sclerosis risk in Ireland. Neurology 84:1537–1544
Rooney JP, Tobin K, Crampsie A, Vajda A, Heverin M, McLaughlin R, Staines A, Hardiman O (2015b) Social deprivation and population density are not associated with small area risk of amyotrophic lateral sclerosis. Environ Res 142:141–147
Rothman KJ, Lash TL, Greenland S (2008) Modern epidemiology. Lippincott Williams & Wilkins
Santurtun A, Villar A, Delgado-Alvarado M, Riancho J (2016a) Trends in motor neuron disease: association with latitude and air lead levels in Spain. Neurol Sci
Santurtun A, Villar A, Lopez-Delgado L, Riancho J (2016b) Amyotrophic lateral sclerosis and richness: a correlation study across Spain. J Neurol Sci 367:380–381
Satizabal CL, Beiser AS, Chouraki V, Chene G, Dufouil C, Seshadri S (2016) Incidence of dementia over three decades in the Framingham heart study. N Engl J Med 374:523–532
Schmidt ML, Lee VM, Saido T, Perl D, Schuck T, Iwatsubo T, Trojanowski JQ (1998) Amyloid plaques in Guam amyotrophic lateral sclerosis/Parkinsonism-dementia complex contain species of a beta similar to those found in the amyloid plaques of Alzheimer’s disease and pathological aging. Acta Neuropathol 95:117–122
Schmidt S, Kwee LC, Allen KD, Oddone EZ (2010) Association of ALS with head injury, cigarette smoking and APOE genotypes. J Neurol Sci 291:22–29
Schwarz S, Husstedt I, Bertram HP, Kuchelmeister K (1996) Amyotrophic lateral sclerosis after accidental injection of mercury. J Neurol Neurosurg Psychiatry 60:698
Sebeo J, Hof PR, Perl DP (2004) Occurrence of alpha-synuclein pathology in the cerebellum of Guamanian patients with Parkinsonism-dementia complex. Acta Neuropathol 107:497–503
Seelen M, van Doormaal PT, Visser AE, Huisman MH, Roozekrans MH, de Jong SW, van der Kooi AJ, de Visser M, Voermans NC, Veldink JH, van den Berg LH (2014) Prior medical conditions and the risk of amyotrophic lateral sclerosis. J Neurol 261:1949–1956
Shah PP, Lockwood WW, Saurabh K, Kurlawala Z, Shannon SP, Waigel S, Zacharias W, Beverly LJ (2015) Ubiquilin1 represses migration and epithelial-to-mesenchymal transition of human non-small cell lung cancer cells. Oncogene 34:1709–1717
Sieh W, Choi Y, Chapman NH, Craig UK, Steinbart EJ, Rothstein JH, Oyanagi K, Garruto RM, Bird TD, Galasko DR, Schellenberg GD, Wijsman EM (2009) Identification of novel susceptibility loci for Guam neurodegenerative disease: challenges of genome scans in genetic isolates. Hum Mol Genet 18:3725–3738
Spencer PS, Palmer VS, Ludolph AC (2005) On the decline and etiology of high-incidence motor system disease in West Papua (southwest New Guinea). Mov Disord 20(Suppl 12):S119–S126
Steele AJ, Al Chalabi A, Ferrante K, Cudkowicz ME, Brown RH Jr, Garson JA (2005) Detection of serum reverse transcriptase activity in patients with ALS and unaffected blood relatives. Neurology 64:454–458
Sutedja NA, Fischer K, Veldink JH, van der Heijden GJ, Kromhout H, Heederik D, Huisman MH, Wokke JJ, van den Berg LH (2009) What we truly know about occupation as a risk factor for ALS: a critical and systematic review. Amyotroph Lateral Scler 10:295–301
Talbott EO, Malek AM, Lacomis D (2016) The epidemiology of amyotrophic lateral sclerosis. Handb Clin Neurol 138:225–238
Tanaka H, Hoshino Y, Watanabe Y, Sakurai K, Takekawa H, Hirata K (2012) A case of strategic-infarct mild cognitive impairment. Neurologist 18:211–213
TORRES J, IRIARTE LL, Kurland LT (1957) Amyotrophic lateral sclerosis among Guamanians in California. Calif Med 86:385–388
Tremlett H, Bauer KC, Appel-Cresswell S, Finlay BB, Waubant E (2017) The gut microbiome in human neurological disease: a review. Ann Neurol 81:369–382
Trias E, Ibarburu S, Barreto-Nunez R, Babdor J, Maciel TT, Guillo M, Gros L, Dubreuil P, Diaz-Amarilla P, Cassina P, Martinez-Palma L, Moura IC, Beckman JS, Hermine O, Barbeito L (2016) Post-paralysis tyrosine kinase inhibition with masitinib abrogates neuroinflammation and slows disease progression in inherited amyotrophic lateral sclerosis. J Neuroinflammation 13:177
Turner MR, Abisgold J, Yeates DG, Talbot K, Goldacre MJ (2010) Head and other physical trauma requiring hospitalisation is not a significant risk factor in the development of ALS. J Neurol Sci 288:45–48
Turner MR, Goldacre R, Ramagopalan S, Talbot K, Goldacre MJ (2013) Autoimmune disease preceding amyotrophic lateral sclerosis: an epidemiologic study. Neurology 81:1222–1225
Turner MR, Goldacre R, Talbot K, Goldacre MJ (2016) Cerebrovascular injury as a risk factor for amyotrophic lateral sclerosis. J Neurol Neurosurg Psychiatry 87:244–246
Vaisman N, Lusaus M, Nefussy B, Niv E, Comaneshter D, Hallack R, Drory VE (2009) Do patients with amyotrophic lateral sclerosis (ALS) have increased energy needs? J Neurol Sci 279:26–29
Van Den HC, Thornton E, Vink R (2007) Traumatic brain injury and Alzheimer’s disease: a review. Prog Brain Res 161:303–316
Vinceti M, Guidetti D, Pinotti M, Rovesti S, Merlin M, Vescovi L, Bergomi M, Vivoli G (1996) Amyotrophic lateral sclerosis after long-term exposure to drinking water with high selenium content. Epidemiology 7:529–532
Visser AE, Seelen M, Hulsbergen A, de Graaf J, van der Kooi AJ, Raaphorst J, Veldink JH, van den Berg LH (2017a) Exploring the fitness hypothesis in ALS: a population-based case-control study of parental cause of death and lifespan. J Neurol Neurosurg Psychiatry
Visser AE, Verduyn Lunel FM, Veldink JH, van den Berg LH (2017b) No association between Borrelia burgdorferi antibodies and amyotrophic lateral sclerosis in a case-control study. Eur J Neurol 24:227–230
Watanabe Y, Watanabe T (2017) Meta-analytic evaluation of the association between head injury and risk of amyotrophic lateral sclerosis. Eur J Epidemiol 32:867–879
Weisskopf MG, Morozova N, O'Reilly EJ, McCullough ML, Calle EE, Thun MJ, Ascherio A (2009) Prospective study of chemical exposures and amyotrophic lateral sclerosis. J Neurol Neurosurg Psychiatry 80:558–561
Zhang YG, Wu S, Yi J, Xia Y, Jin D, Zhou J, Sun J (2017) Target intestinal microbiota to alleviate disease progression in amyotrophic lateral sclerosis. Clin Ther 39:322–336
Zhou H, Chen G, Chen C, Yu Y, Xu Z (2012) Association between extremely low-frequency electromagnetic fields occupations and amyotrophic lateral sclerosis: a meta-analysis. PLoS One 7:e48354
Zufiria M, Gil-Bea FJ, Fernandez-Torron R, Poza JJ, Munoz-Blanco JL, Rojas-Garcia R, Riancho J, de Munain AL (2016) ALS: a bucket of genes, environment, metabolism and unknown ingredients. Prog Neurobiol 142:104–129
Conflict of interest
The authors declare that they have no competing interests.
Funding
This research received no specific grant from any funding agency, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Riancho, J., Bosque-Varela, P., Perez-Pereda, S. et al. The increasing importance of environmental conditions in amyotrophic lateral sclerosis. Int J Biometeorol 62, 1361–1374 (2018). https://doi.org/10.1007/s00484-018-1550-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00484-018-1550-2