Abstract
Background
Single-incision distal gastrectomy (SIDG) is technically difficult due to limited range of motion and unstable field of view. Solo surgery using a passive scope holder may be the key in allowing SIDG to be safer and efficient. We report our initial 100 cases of, to what we know, the world’s first solo SIDG, and calculate the learning curve.
Methods
Prospectively collected database of 100 patients clinically diagnosed as gastric cancer who underwent solo SIDG from October 2013 until July 2016 was analyzed. All the operations were held by a single surgeon with no assistants. A passive laparoscopic scope holder was used to fix the field of view.
Results
The mean operation time was 120.6 ± 30.2 min, and the average estimated blood loss was 33.5 ± 55.7 ml. Average body mass index was 23.4 ± 2.9 kg/m2. The median hospital stay was 5 (4–14) days, and the mean number of retrieved lymph nodes was 56.0 ± 22.8. There was no conversion to multiport or open surgery. Early complication of Clavien–Dindo grade III or more was 3%. Learning curve was calculated on operation time, and showed that an experienced surgeon in SIDG required 20 cases or less in stabilizing the operation time for solo SIDG.
Conclusions
Solo SIDG seems to be feasible and safe. The stable field of view created by a scope holder provides a favorable environment for a finer and more consistent operation. In addition, manpower can also be saved without affecting the quality of surgery.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
The innovations in minimally invasive surgery have given rise to concepts such as reduced port surgery, and natural orifice transluminal endoscopic surgery (NOTES). Single-port surgery or single-incision laparoscopic surgery (SILS) bridges conventional laparoscopic surgery and NOTES. SILS is technically fully laparoscopic, but it only uses a single incision to have all the working ports. Until now, SILS has been adapted to various procedures such as cholecystectomy [1], appendectomy [2], colectomy [3], bariatric surgery [4], and various other operations [5]. Some studies suggest that SILS allow less pain and better patient scar satisfaction in than conventional multiport laparoscopic surgery [6].
Since the first report of single-incision distal gastrectomy (SIDG) by Omori et al. [7] in 2011, there have only been few reports of SILS in gastric cancer [8, 9]. The largest case number was our previous retrospective study of 50 patients who underwent SIDG, and were matched with patients who had conventional laparoscopic distal gastrectomy [10]. The reason for the lack of popularity of SIDG among surgeons—despite increasing patient demand—is mainly due to the technical difficulties involved in unstable camera view, collision of instruments, and limited range of motion. Several surgeons in other surgical fields have tried to overcome this problem with the introduction of “solo surgery.” Camera holders have been applied to SILS with results showing less tremor of vision, and more room for motion [11,12,13], with no significant complications or prolongation of operative time. “Solo surgery” can also be applied to single-incision gastric cancer surgery as a means to assist the operator, and make SIDG more feasible, without being have to be influenced by the availability of an experienced scopist.
This study illustrates our initial 100 cases of the world’s first solo SIDG, examines the learning curve, and suggests “solo surgery” as a viable option to overcome the difficulties associated with SIDG.
Methods
Patient criteria and study design
Records of consecutive 100 patients clinically diagnosed as early gastric cancer (EGC) who underwent solo SIDG from October 2013 until July 2016 were retrospectively reviewed. All the operations were done by a single surgeon in a single center. For this type of study, no formal written consent was required, and it was approved by the institutional review board in accordance with the Declaration of Helsinki.
Surgical techniques
Patient set-up
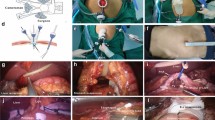
The patient set-up and scope holder placement are illustrated in Fig. 1. The patient was placed in lithotomy position with reverse Trendelenburg. The scope holder used was a passive scope holder (Laparostat; CIVCO Medical Solutions, Kalona, IA, USA) and was fixed on the left side of the patient at the pelvis level. The scope holder was then covered with sterile plastic sleeves (Sani Sleeve™, Dasol Int Co. Ltd, Gwangju, Korea). The operator sat between the patient’s legs facing cephalad. A transumbilical incision of 2.5 cm was made on the skin, with the fascia opened 4 cm more than the skin incision. Then, a four-hole single port (Gloveport; Nelis, Bucheon, Korea) was inserted. A 10-mm HD flexible scope (Olympus, Tokyo, Japan) or a 3D flexible scope (Olympus, Tokyo, Japan) was used and fixed to the scope holder. The whole surgery was done by a single operator and one scrub nurse.
Distal gastrectomy with D1+ or D2 lymphadenectomy
Liver was retracted using the suture method previously explained in our study [14]. Partial omentectomy was performed in all patients. If the patient was diagnosed as advanced gastric cancer (AGC) or the laparoscopic impression was AGC, D2 lymphadenectomy was performed. In patients with EGC, D1+ lymphadenectomy was performed according to the fourth Japanese Gastric Cancer Association (JGCA) treatment guidelines [15]. The Hit and Away technique [16] was performed for lymph node (LN) dissection, using small bites and short activation time of the energy device. During dissection, scope manipulation is done using the right hand while the left hand, usually retracting a tissue using a grasper, stays still in the field. Distal gastrectomy needs only about ten major fields of view, and movement of the scope within the major viewpoints can be done finely by adjusting the knobs of the flexible scope. The image of the field after gastrectomy and lymphadenectomy is shown in Fig. 2.
Surgical field after dissection in solo single-incision distal gastrectomy. A Number 6 lymph node area, B number 4sb lymph node area, C right side suprapancreatic lymph node area (number 7, 8a, 9, 12a), D left side suprapancreatic lymph node area (number 7, 9, 11p). RGEA right gastroepiploic artery, RGEV right gastroepiploic vein, ASPDV anterior superior pancreaticoduodenal vein, GCT gastrocolic trunk, LGEV left gastroepiploic vein, RGA right gastric artery, LGA left gastric artery, PV portal vein, CHA common hepatic artery, SpA splenic artery, SpV splenic vein
Reconstruction was decided depending on the patient characteristics such as age, tumor location, tumor extent, and length of remnant bowels. Patients who are younger (below 70 years) with a relatively low-stage disease have a longer life expectancy, so uncut Roux-en Y reconstruction was favored to reduce bile reflux and heighten patients’ quality of life. Wound closure was done with 1–0 interrupted vicryl sutures, and ropivacaine solution was injected close to the fascia. The skin was then closed with an intradermal suture, and surgical bond was applied over the umbilical wound to allow the patients to take a shower the day after the surgery (Fig. 3). No drain was placed.
Statistical analysis
Data were analyzed and presented as either mean ± standard deviation or median (range). The Cumulative Sum (CUSUM) Control Chart analysis was performed on operative time to determine the learning curve. CUSUM analysis is the running total of differences between each chronological data and the mean. The cases were first ordered chronologically and the CUSUMOT of the first case was the difference between the operation time of the first case and the mean operation time. The CUSUMOT of the second case was the sum of the previous CUSUMOT and the difference between the operation time of the second case and the mean. This process continued until the last case, and a polynomial function was calculated to best represent the learning curve.
Results
Short-term results
The mean age of the patients was 60.0 ± 13.4 years. Average body mass index was 23.4 ± 2.9 kg2/cm, and 59 patients were male. Mean operation time was 120.6 ± 30.2 min, with an estimated blood loss of 33.5 ± 55.7 ml. The most common reconstruction was the uncut Roux-en Y technique, composing of half of the reconstructions. Two patients had a simultaneous excision of another organ, and both were gallbladders due to gallbladder stones. The average number of retrieved nodes was 56.0 ± 22.8. There was no case where insertion of an additional port was needed, nor was there any case that converted to an open procedure. Table 1 summarizes the demographics and operative outcomes.
Mean hospital stay was 5.9 ± 1.8 (range 4–14) days, and the mean time of first flatus was on postoperative day (POD) 3.1 ± 0.8 (range 1–7). Diet was progressed according to patient tolerability, and the mean time of initiation of semi-fluid diet was POD 3.3 ± 1.0 (range 2–8) (Table 2).
The short-term postoperative morbidity is also summarized in Table 2. There were 11 (11.0%) early complications with three intestinal motility disorders, two leakage, two pancreatitis, two pneumonia, one wound infection, and one phlebitis. Three of the complications had a Clavien–Dindo grade [17] of III or more. One patient had fluid collection around the gastrojejunostomy, and was managed with percutaneous drainage. One patient presenting with decreased intestinal motility was found to have internal herniation around the mesenteric space on POD 6. The patient underwent hernia reduction and mesenteric space repair. The last patient complained of severe reflux symptoms, and underwent a bypass operation. There was no mortality within the median follow-up of 27 (4–51) months. Within this median follow-up, there was also no case of incisional hernia.
Learning curve
Figure 4 shows the CUSUM control chart based on the operative time. The CUSUM chart is separated into two major phases due to a change in the operation technique after the 48th case. In the first phase, the CUSUMOT peaks at the 19th case then gradually decreases. In the second phase, the CUSUMOT decreases after the 61st case—13th case in this phase—and continues to decrease. A polynomial is drawn to represent the best fitting curve.
Discussion
Solo SIDG, with the use of a passive scope holder, is feasible and safe in short-term morbidity. The calculated learning curve shows that about 20 cases is needed to become accustomed to manipulating the passive scope holder. Once this learning curve is achieved, the difficulties in performing SIDG may be overcome.
Single-port or single-incision laparoscopic surgery is an attractive option for the patients mainly due to possible advantages in cosmesis [6], but recent studies also suggest that it may provide less pain, faster recovery, and better cost-effectiveness [18,19,20,21]. A randomized trial by Tsimoyiannis et al. [19] reported that the SILS group had nonexistent pain 24 h after cholecystectomy. Despite possible benefits, SILS is a technically demanding operation for surgeons. A randomized trial by Abdelrahman et al. [22] analyzed surgeon stress and workload using maximum heart rate, salivary cortisol level, and workload questionnaire. Heart rate, cortisol revel, and surgery task workload index was significantly higher in the single-incision cholecystectomy group. Although there is no study analyzing surgeon stress in SIDG, due to limited range of movement, unstable vision, and instrument collision during fine LND, the technical difficulties can cause severe fatigue on the operator.
Application of scope holders in SILS has been reported in various literatures [2, 11, 23]. Kim et al. described the various scope holders in their review article regarding “Solo Surgery,” and concluded that despite the initial rise in operative time, the disadvantages are outweighed by the stable vision it provides. In our study, the use of a scope holder in SIDG not only provided stable vision, but also gave more room for movement since the head of the scope holder was smaller than a human hand. Once accustomed to using a scope holder, another advantage is that the operation can be very well standardized, without being influenced by the skill of the scopist or the assistant. Once the learning curve is fulfilled, patients can receive a more constant operation, and the operations will be influenced by the patient factor alone.
One hundred SIDG were performed with a mean operation time of 120 min which is comparable or faster than most of the reported operation time for laparoscopic distal gastrectomy (Table 3) [24]. There were three cases of morbidity which had a grade of Clavien–Dindo 3 or more. Although the long-term feasibility and oncologic safety is yet to be known, solo surgery in SIDG seems to be feasible in short-term. Nevertheless, when introducing a new procedure, patient safety cannot be left without upmost attention. Although there was no case of major bleeding or other cases of emergency in our first 100 cases, there was always available personnel to call for when required. In cases of minor bleeding, however, an operator with enough experience with a scope holder will find it easier to solve using the scope holder rather than an inexperienced scopist.
There were two phases for learning curve that had a similar shape. This was due to the fact that starting from the time of the 49th case, the insurance policies have changed in our country, and the closure of the entry holes changed from stapling to hand-sewing. It was at this time that the Peterson’s and mesenteric spaces were also routinely closed using a nonabsorbable suture. There was an addition of procedures that required another learning curve. The interesting fact is that both learning curves reached a peak at 19 and 13 cases respectively, and then entered the mastery phase. Thus, we can deduce that being accustomed to the passive scope holder will require about 15–20 cases. However, it is also important to keep in mind that all 100 cases were performed by a single surgeon who already had an experience of 106 cases of SIDG with a scopist before starting solo SIDG. In a previous study [25], the learning curve of SIDG with a scopist was calculated to be 30 cases, and operation time was 118 ± 34.5 min, and estimated blood loss was 40.7 ± 77.4 ml after reaching the learning curve. Comparing it to the results of solo SIDG from this study, the operative time and blood loss are similar. However, if a surgeon has had no experience with other SILS such as appendectomy or cholecystectomy, the learning curve is expected to be higher.
Several studies on SILS give their attention to incisional hernia. A meta-analysis by Antoniou et al. [26] analyzed 19 randomized trials on single-incision surgery. They concluded that transumbilical SILS is associated with higher trocar-site hernia with an odds ratio of 2.26 (95% confidence interval 1.00–5.08, p = 0.05). On the other hand, a study by Lakdawala et al. [6] compared 600 sleeve gastrectomy patients with 300 patients on the SILS arm and 300 on the multiport arm. Among the 300 SILS patients, incisional hernia was only found in 3 (1.0%). In our study of 100 patients, there was no case of incisional hernia at all. Thus, the preconception that single-incision surgery causes more incisional hernia can be overcome with careful and thorough closure of the wound.
There are also concerns regarding resident or fellow training when performing solo SIDG. However, in laparoscopic surgery, most of the main procedures are done by the operator, and usually an assistant holds the scope or simply retracts and makes triangulation for a better dissection plane. Solo surgery is also similar to the DaVinci robot surgery in that aspect, where the operator takes control of the field including the camera. With the evolution of surgical techniques, surgical training must also undergo change. The trainee can first begin with observational learning using various multimedia and even some virtual reality training to have better exposure to the nature of disease and the reality of the surgical field. Then they should proceed to improve their skills with dry lab practice. Once they have enough basic skill training—perhaps with the aid of simulators—they can do hands on solo surgery with the supervision of an expert advisor. After enough supervision, the advisor can decide if the trainee is qualified enough to perform a solo surgery alone.
Conclusion
Solo SIDG is safe in feasible for short-term outcomes. For a surgeon with enough experience in SIDG, the learning curve of using a scope holder is about 20 cases. The scope holder, once the learning curve has been overcome, can provide better vision, easier manipulation of instruments in SIDG, allowing the difficult procedure to become more feasible.
References
Tacchino R, Greco F, Matera D (2009) Single-incision laparoscopic cholecystectomy: surgery without a visible scar. Surg Endosc 23:896–899
Kim S-J, Choi B-J, Lee SC (2015) Novel approach of single-port laparoscopic appendectomy as a solo surgery: a prospective cohort study. Int J Surg 21:1–7
Law WL, Fan JKM, Poon JTC (2009) Single incision laparoscopic left colectomy for carcinoma of distal transverse colon. Colorectal Dis 12:698–701
Park YS, Park DJ, Kim KH, Park DJ, Ahn S-H, Kim H-H (2015) Single incisional laparoscopic sleeve gastrectomy and adolescent bariatric surgery: case report and brief review. J Metab Bariatr Surg 4:40–45
Romanelli JR, Earle DB (2009) Single-port laparoscopic surgery: an overview. Surg Endosc 23:1419–1427
Lakdawala M, Agarwal A, Dhar S, Dhulla N, Remedios C, Bhasker AG (2015) Single-incision sleeve gastrectomy versus laparoscopic sleeve gastrectomy. A 2-year comparative analysis of 600 patients. Obes Surg 25:607–614
Omori T, Oyama T, Akamatsu H, Tori M, Ueshima S, Nishida T (2011) Transumbilical single-incision laparoscopic distal gastrectomy for early gastric cancer. Surg Endosc 25:2400–2404
Ahn S-H, Park DJ, Son S-Y, Lee C-M, Kim H-H (2013) Single-incision laparoscopic total gastrectomy with D1 + beta lymph node dissection for proximal early gastric cancer. Gastric Cancer 17:392–396
Park DJ, Lee J-H, Ahn S-H, Eng AKH, Kim H-H (2012) Single-port laparoscopic distal gastrectomy with D1 + β lymph node dissection for gastric cancers. Surg Laparosc Endosc Percutan Tech 22:e214–e216
Ahn S-H, Son S-Y, Jung DH, Park DJ, Kim H-H (2014) Pure single-port laparoscopic distal gastrectomy for early gastric cancer: comparative study with multi-port laparoscopic distal gastrectomy. J Am Coll Surg 219:933–943
Choi B-J, Jeong WJ, Kim S-J, Lee SC (2017) Solo-surgeon single-port laparoscopic anterior resection for sigmoid colon cancer: comparative study. J Laparoendosc Adv Surg Tech 28:330–336
Fujii S, Watanabe K, Ota M, Yamagishi S, Kunisaki C, Osada S, Ike H, Ichikawa Y, Endo I, Shimada H (2011) Solo surgery in laparoscopic colectomy: a case-matched study comparing robotic and human scopist. Hepatogastroenterology 58:406–410
Kang SH, Lee Y, Park YS, Ahn S-H, Park DJ, Kim H-H (2017) Solo single-incision laparoscopic resectional Roux-en-Y gastric bypass for morbid obesity with metabolic syndrome. Obes Surg 27:3314–3319
Shabbir A, Lee J-H, Lee M-S, Park DJ, Kim H-H (2010) Combined suture retraction of the falciform ligament and the left lobe of the liver during laparoscopic total gastrectomy. Surg Endosc 24:3237–3240
Kodera Y, Sano T (2016) Japanese gastric cancer treatment guidelines 2014 (ver. 4). Gastric Cancer 20:1–19
Irino T (2015) The Hit and Away technique: optimal usage of the ultrasonic scalpel in laparoscopic gastrectomy. Surg Endosc 30:1–6
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, de Santibañes E, Pekolj J, Slankamenac K, Bassi C, Graf R, Vonlanthen R, Padbury R, Cameron JL, Makuuchi M (2009) The Clavien-Dindo Classification of surgical complications. Ann Surg 250:187–196
Poon JTC, Cheung C-W, Fan JKM, Lo OSH, Law W-L (2012) Single-incision versus conventional laparoscopic colectomy for colonic neoplasm: a randomized, controlled trial. Surg Endosc 26:2729–2734
Tsimoyiannis EC, Tsimogiannis KE, Pappas-Gogos G, Farantos C, Benetatos N, Mavridou P, Manataki A (2010) Different pain scores in single transumbilical incision laparoscopic cholecystectomy versus classic laparoscopic cholecystectomy: a randomized controlled trial. Surg Endosc 24:1842–1848
Chambers WM, Bicsak M, Lamparelli M, Dixon AR (2011) Single-incision laparoscopic surgery (SILS) in complex colorectal surgery: a technique offering potential and not just cosmesis. Colorectal Dis 13:393–398
Markar SR, Karthikesalingam A, Thrumurthy S, Muirhead L, Kinross J, Paraskeva P (2012) Single-incision laparoscopic surgery (SILS) vs. conventional multiport cholecystectomy: systematic review and meta-analysis. Surg Endosc 26:1205–1213
Abdelrahman AM, Bingener J, Yu D, Lowndes BR, Mohamed A, McConico AL, Hallbeck MS (2016) Impact of single-incision laparoscopic cholecystectomy (SILC) versus conventional laparoscopic cholecystectomy (CLC) procedures on surgeon stress and workload: a randomized controlled trial. Surg Endosc 30:1205–1211
Yang YS, Kim SH, Jin CH, Oh KY, Hur MH, Kim SY, Yim HS (2014) Solo surgeon single-port laparoscopic surgery with a homemade laparoscope-anchored instrument system in benign gynecologic diseases. J Minim Invasive Gynecol 21:695–701
Kim W, Kim H-H, Han SU, Kim MC, Hyung WJ, Ryu SW, Cho GS, Kim CY, Yang H-K, Park DJ, Song KY, Lee SI, Ryu SY, Lee JH, Lee H-J, Korean Laparo-endoscopic Gastrointestinal Surgery Study (KLASS) Group (2016) decreased morbidity of laparoscopic distal gastrectomy compared with open distal gastrectomy for stage I gastric cancer: short-term outcomes from a Multicenter Randomized Controlled Trial (KLASS-01). Ann Surg 263:28–35
Lee B, Lee YT, Park YS, Ahn S-H, Park DJ, Kim H-H (2018) Learning curve of pure single-port laparoscopic distal gastrectomy for gastric cancer. J Gastric Cancer 18:182–188
Antoniou SA, Morales-Conde S, Antoniou GA, Granderath FA, Berrevoet F, Muysoms FE, Bonham Group (2016) Single-incision laparoscopic surgery through the umbilicus is associated with a higher incidence of trocar-site hernia than conventional laparoscopy: a meta-analysis of randomized controlled trials. Hernia 20:1–10
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
So Hyun Kang, Yo-Seok Cho, Sa-Hong Min, Young Suk Park, Sang-Hoon Ahn, Do Joong Park, and Hyung-Ho Kim have no conflicts of interest or financial ties to disclose.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kang, S.H., Cho, YS., Min, SH. et al. Early experience and learning curve of solo single-incision distal gastrectomy for gastric cancer: a review of consecutive 100 cases. Surg Endosc 33, 3412–3418 (2019). https://doi.org/10.1007/s00464-018-06638-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-018-06638-1