Abstract
Background
PTHrP, a mediator of humoral hypercalcemia of malignancy, is considered as a potential activator to induce breast cancer cells metastasizing to bone. However, recent clinical evidences and basal research results prove that PTHrP expression in primary tumors indicates good prognosis. BMP-6, as a member of TGF-β superfamily, is closely correlated with tumor differentiation and skeletal metastasis.
Purpose
These experiments were designed to investigate the molecular mechanism of PTHrP regulating BMP-6 in breast cancer cells.
Methods and results
Through detecting mRNA expression levels of PTHrP and BMP-6 in 35 breast cancer specimens, the two genes’ expression were proved to be negatively correlated. Moreover, PTHrP (1–40), instead of PTHrP (107–139), inhibited BMP-6 mRNA expression in MCF-7 cells, indicating that PTHrP exerts its effect on BMP-6 through membranous PTHrP receptor. Inhibitors against signaling pathways downstream of PTHrP were utilized. H89, the PKA pathway inhibitor, eliminated the inhibitory effect of PTHrP on BMP-6. In addition, silencing of BMP-6 strengthened the antimitogenic effect of PTHrP.
Conclusions
These results suggest that PTHrP acts as the upstream molecule of BMP-6, and exerts antimitogenic effect via reducing BMP-6 mRNA expression through PKA signaling pathway in breast cancer cells.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Breast cancer, as one of the most frequent malignant tumors, is the leading cause of cancer death in women worldwide (Pisani et al. 1999). The initiation, progression and metastasis of breast cancer include a series of genetic changes which are regulated by various local growth factors, such as TGF-β superfamily and parathyroid hormone-related peptide (PTHrP).
PTHrP, a mediator of humoral hypercalcemia of malignancy, plays an essential role in normal mammary gland and bone development. The molecular mechanisms by which PTHrP exerts its effects have been widely investigated. Basically, there are two pathways that PTHrP regulates tumorigenesis: (1) pro-proliferative and antiapoptotic effect mediated by the NLS-containing midregion of PTHrP peptide through endocrine pathway; (2) antimitogenic effect mediated by the membrane receptor, PTH1R, through activating the combined actions of the PKA and PKC signaling pathways (Rajendra et al. 2006; Torricelli et al. 2006; Nakamura et al. 2008). By immunohistochemistry, the expression of PTHrP was detected in 60–69% of primary breast cancers. 85% of breast cancers with bone metastasis were PTHrP positive. These findings support the view that PTHrP may be related to the breast cancer bone metastasis (Southby et al. 1990; Powell et al. 1991). However, the exact role that PTHrP plays during the tumorigenesis remains to be investigated further. Henderson et al. performed a prospective study of 526 consecutive patients with operable breast cancer for a median observation of 10 years and found that only in the bone microenvironment and influenced by specific factors, the bone resorption-stimulating effect of PTHrP emerges to favor growth in bone; in contrast, during the early stages of tumor dissemination, increased production of PTHrP by breast cancers confers on them a less invasive phenotype, and patients with PTHrP-positive primary tumors had a significantly improved prognosis for survival (Henderson et al. 2001, 2006). The detailed molecular mechanism underlying the effects of PTHrP on breast cancer behavior remains to be explored.
Bone morphogenetic protein-6 (BMP-6), which belongs to the transforming growth factor-β (TGF-β) superfamily, is expressed in various cancer cells, including breast, prostate, esophagus and osteosarcoma. Recent studies found that BMP-6 is overexpressed in both breast cancer cell lines and tumor samples from breast carcinoma patients (Clement et al. 1999; Akiyoshi et al. 2004). Our previous findings demonstrated that BMP-6 transcription can be activated dose-dependently by estrogen through its demethylated promoter in human estrogen receptor positive (ER+) breast cancer cell line MCF-7 (Zhang et al. 2005, 2007). When considering the fact that estrogen plays a major role in promoting the proliferation of neoplastic breast epithelium (Doisneau-Sixou et al. 2003), we speculate that BMP-6 may be involved in the process of breast carcinogenesis.
Through detecting the expression levels of BMP-6 and PTHrP in breast cancer specimens, we found that the expression of these two genes is negatively correlated. After a series of experiments focused on the molecular mechanism of PTHrP regulating BMP-6 expression in breast cancer cell line MCF-7, we demonstrated that BMP-6 expression can be downregulated by PTHrP through PKA signaling pathway, thus inhibiting the mitosis of breast cancer cells.
Materials and methods
Tumor samples
Tumor and non-tumor samples were collected from excised tissues of 35 breast cancer patients in Tianjin Medical University Cancer Institute and Hospital. The patients had a mean age of 53.6 ± 13.5 years and were recruited from the same department.
Cell culture
Human breast cancer cell line MCF-7 was maintained in RPMI 1640 (GIBCO BRL, Grand Island, NY, USA) supplemented with 10% FBS (Hyclone, Logan, UT, USA), and 100 U/ml penicillin and streptomycin (growth medium) at 37°C in a humidified atmosphere with 5% CO2. The cells were seeded at 105 cells in 6-well plates and allowed to attach for 24 h and transfection were performed.
RNA isolation and real-time PCR
Human breast cancer cell line MCF-7 was transient transfected with PTHrP expression plasmid or treated with PTHrP (1–40) or PTHrP (107–139) (100 nM, Sigma, Madison, WI, USA) for 24 h before the total RNA was extracted. In certain cases, the cells were pretreated with a series of kinase inhibitors (Sigma, Madison, WI, USA), including H-89 (10 µM) for PKA inhibition, GO-6976 (12 µM) for PKC inhibition, SB203850 (10 µM) for p38MAP kinase inhibition, and U0126 (10 µM) for MEK inhibition, and PKA signaling pathway activator dbcAMP (0.5 mM). Total RNA was isolated using TRIzol Reagent (Life Technologies Inc., Grand Island, NY, USA) according to the manufacturer’s protocol. After reverse transcription reaction (20 µl) using 2 µg of total RNA, real-time PCR was carried out in a 25 µl final volume by an ABI PRISM 7000 (ABI, USA) sequence detection system according to the manufacturer’s protocol. The reaction mixture contained 1× SYBR Green I, 0.5 pmol/l of each primer, 2.5 mM MgCl2, and 0.5 µl cDNA from (20 µl) reverse transcription reaction. The conditions of real-time PCR were as follows: 94°C 4 min followed by 40 cycles at 94°C for 30 s, 68°C for 1.5 min. There is no non-specific amplification determined by dissolve curve. There are three repeat tubes per cDNA specimen, three cDNA specimens independently for each data point. The real-time PCR results were reported as the fold of relative light units for experimental groups when compared with those for control group after normalization with GAPDH expression. Error bars represent the standard errors for three independent experiments, with each data point done in triplicate. The primers used for real-time PCR are as follows:
BMP-6
Upstream primer: 5′-CAACAGAGTCGTAATCGCTCTACC-3′ (+1,323 to +1,346)
Downstream primer: 5′-TTAGTGGCATCCACAAGCTCT-3′ (+1,701 to +1,721) PCR product is 308 bp.
GAPDH
Upstream primer: 5′-ACCACAGTCCATGCCATCAC-3′ (+526 to +545)
Downstream primer: 5′-TCCACCACCCTGTTGCTGTA-3′ (+958 to +977) PCR product is 451 bp.
Transient transfection and luciferase assay
PTHrP expression plasmid and the human 1.2 kb (−1,119/+37) BMP-6 promoter-luciferase plasmid were previously constructed in our laboratory. The plasmids were transfected into MCF-7 cells by LipofectAMINE reagents (Invitrogen, Carlsbad, CA, USA) following the manufacturer’s instructions in 6-well plates. 24 h after transfection, luciferase activity was detected using a kit from Promega Corp. (Madison, WI, USA) with a luminometer. The efficiency of transfection was monitored by cotransfection with phRL-null vector (0.5 µg/well). The luciferase results were reported as relative light units of firefly luciferase activity normalized with the Renilla luciferase activity. Error bars represent the standard errors for three independent experiments, with each data point done in triplicate.
Western blot analysis
After 3 days of treatment or 24 h after the transient transfection, cells were then trypsinized for counting or lysed in lysis buffer (50 mM Tris–HCl pH 7.5, 150 mM NaCl, 1% Triton X-100, 0.5% sodium deoxycholate) supplemented with 1 mM sodium orthovanadate, 1 mM ethylene glycol-bis-(beta-amino ethyl ether), 1 mM sodium fluoride, and 1 µM microcysterine. The protein concentrations were determined using the BCA protein assay kit (Pierce, Rockford, IL, USA). The cell extracts (30 µg) were assayed by SDS–PAGE. After transferred to a PVDF membrane (Amersham Biosciences, Piscataway, NJ, USA), the blots were probed with a mouse monoclonal BMP-6 (74219.11) antibody (Santa Cruz Biotechnology, CA, USA, Order number: sc-57042, Specificity: raised against full length BMP-6 of human origin) against BMP-6 or a monoclonal anti-c-myc antibody (Sigma, Madison, WI, USA, Order number: M4439, Specificity: N-terminal or C-terminal c-Myc tagged fusion proteins) against c-Myc which fused to PTHrP’s C-terminus (M-PTHrP) at a dilution of 1:1000. A monoclonal anti-β-actin antibody (Sigma, Madison, WI, USA, Order number: A2228, Specificity: Recognizes an epitope located on the N-terminal end of the β-isoform of actin) at a dilution 1:1000 was used to confirm equal protein loading. The immune complexes were detected using ECL reagents (Amersham Biosciences, Piscataway, NJ, USA) and the results were imaged on films.
Cell proliferation assay and cell cycle assay
The target sequence of the siRNA is 5′-GCGACACCACAAAGAGUUCtt-3′ for human BMP-6 as previously reported (Babitt et al. 2007). BMP-6 siRNA was transfected into MCF-7 cells, 24 h after the transfection, cells were treated with 100 nM PTHrP (1–40) or 0.5 mM dbcAMP for 72 h. The cell proliferation assay was performed by the addition of 10 μl CCK-8 (Cell counting kit-8, Jindojin, Japan) solution to each well, followed by incubation at 37°C for 2 h. Absorbance was measured at 450 nm using a microplate reader. As for the cell cycle assay, 48 h after the serum starvation, cells were trypsinized, then washed twice with PBS. Cells was fixed in 70% ethanol on ice for 30 min and stored at −20°C overnight. Then the cells were centrifuged at 1,500 g for 4 min, washed with PBS, and treated with 50 µl of 1 mg/mL RNase A (Sigma) followed by the addition of 500 μl of 100 μg/ml propidium iodide (Sigma, Madison, WI, USA) in the dark for 30 min at 37°C, samples were then analyzed on a FACSCalibur flow cytometry (BD Biosciences, San Jose, CA, USA) and data were analyzed by MODFIT software (Verity, Topsham, ME).
Statistical analysis
Statistical significance was determined by ANOVA and Scheffe’s test, and the levels of probability are noted. The results are expressed as mean ± standard error (SE) for at least three separate experiments. The comparisons of the expression levels of PTHrP and BMP-6 in 35 tumor specimens were performed by χ2 test and Fisher’s exact test.
Results
mRNA expression of BMP-6 and PTHrP in breast cancer specimens are reversely correlated
We analyzed 35 tumor tissue samples and compared the amount of BMP-6 mRNA and PTHrP mRNA with tumor-free resection margins (non-tumor samples) from the same patient. As shown in Table 1, in 17/35 patients with higher amount of PTHrP mRNA in the tumor versus non-tumor samples, there are 12 specimens with lower amount of BMP-6 mRNA in tumor samples; on the contrary, in the 18/35 patients with lower amount of PTHrP mRNA, there are 17 specimens with higher BMP-6 mRNA expression, indicating that the expression levels of these two genes are reversely correlated.
PTHrP (1–40) inhibits BMP-6 expression in breast cancer cell line MCF-7
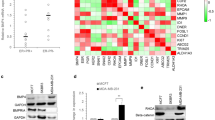
To detect the regulation pattern of PTHrP on BMP-6 in breast cancer, PTHrP expression plasmid at different doses (0, 0.2, 0.6 and 1.8 µg) was transiently transfected into breast cancer cell line MCF-7, BMP-6 mRNA expression was detected through real-time PCR. As shown in Fig. 1a and b, BMP-6 mRNA expression was obviously reduced in PTHrP overexpressed group (about 90% downregulation in the PTHrP 1.8 µg group when compared with the PTHrP 0 µg group). We also performed western blot to detect the inhibitory effect of PTHrP on BMP-6. As shown in Fig. 1c, BMP-6 protein level can be reduced significantly by PTHrP in a dose-dependent manner. To further confirm this result, we examined the effect of PTHrP on the endogenous expression of BMP-6 in MCF-7 cells at different time points. As shown in Fig. 1d, PTHrP remarkably downregulated BMP-6 expression at 12 h and exhibited a maximal inhibition at 24 h after transfection. These results confirm the expression of BMP-6 is suppressed following PTHrP overexpression in MCF-7 breast cancer cells.
Overexpression of PTHrP inhibits BMP-6 expression in breast cancer cell line MCF-7. PTHrP expression plasmid at different doses (0, 0.2, 0.6 and 1.8 µg) was transient transfected into breast cancer cell line MCF-7 cells, BMP-6 mRNA expression was detected through both PCR a and real-time PCR b. c PTHrP expression plasmid at different doses (0, 0.2, 0.6 and 1.8 µg) was transient transfected into MCF-7 cells, BMP-6 protein expression was detected through western blot by a monoclonal human antibody against BMP-6. PTHrP with a c-myc tag fused to its C-terminus was detected by a monoclonal mouse antibody against c-Myc. d PTHrP expression plasmid was transient transfected into MCF-7, total RNA was harvested at different time points (0, 1, 3, 6, 12, 24 and 48 h), BMP-6 mRNA expression level was detected through real-time PCR. *P < 0.05 compared with 0 h group
To determine whether the membranous PTHrP receptor, PTH1R, is necessary for the regulation of PTHrP on BMP-6, MCF-7 cells were treated with PTHrP (1–40) or PTHrP (107–139) for 24 h and BMP-6 mRNA expression was detected through real-time PCR. As shown in Fig. 2a, PTHrP (1–40) significantly downregulated the BMP-6 mRNA expression at the concentration of 10 nM. When compared with the inhibitory effect of PTHrP (1–40), PTHrP (107–139) showed no obvious effect on the regulation of BMP-6 mRNA. To further confirm this result, we also detected the effect of these two constructs on BMP-6 promoter, and found that PTHrP (1–40) downregulated BMP-6 promoter activity significantly (about 40% at the concentration of 10 nM; while PTHrP (107–139) showed no effect on BMP-6 promoter activity (Fig. 2b). We also demonstrated that PTHrP (1–40) repressed the BMP-6 protein expression at the concentration of 10 nM by Western blot (Fig. 2c). These results indicate that PTHrP (1–40), but not PTHrP (107–139), downregulates BMP-6 mRNA expression through PTH1R.
PTHrP (1–40) not PTHrP (107–139) inhibits BMP-6 expression in MCF-7 cells. a MCF-7 cells were treated with PTHrP (1–40) or PTHrP (107–139) at different doses (0, 0.1, 1, 10, 100 nM), 24 h later, total RNA was extracted to detect BMP-6 mRNA expression level through real-time PCR. b Human 1.2 kb (−1,119/+37) BMP-6 promoter-luciferase plasmid was transient transfected into MCF-7 cells, 24 h later, the cells were treated with PTHrP (1–40) or PTHrP (107–139) at different doses. Total protein was harvested to detect BMP-6 promoter activity through luciferase assay. *P < 0.05 compared with the 0 nM group. c MCF-7 cells were treated with PTHrP (1–40) at different doses (0, 0.1, 1, 10, 100 nM), 24 h later, total protein was extracted to detect BMP-6 protein level by western blot
PTHrP inhibits BMP-6 transcription through the PKA signaling pathway
To study the mechanism underlying the PTHrP regulating BMP-6 gene expression, we treated MCF-7 cells with a series of inhibitors against the signaling pathways downstream of PTHrP that may be involved in regulating BMP-6 expression. As shown in Fig. 3a, the inhibitory effect of PTHrP on BMP-6 was rescued effectively by the addition of PKA inhibitor H89. As for other signaling pathway inhibitors, PKC inhibitor GO6976 slightly rescued the PTHrP-induced inhibition of BMP-6 gene expression by about 15%, but without statistical significance, while p38MAPK and MEK inhibitors had no effect. These results indicate that PTHrP inhibits BMP-6 gene expression through PKA signaling pathway. To further confirm this result, we performed luciferase assay to detect the BMP-6 promoter activity at the presence of dbcAMP or H89. As shown in Fig. 3b, direct stimulation of PKA activity by 0.5 mM of dbcAMP, a cell membrane-permeable analog of cAMP, resulted in strong inhibition of BMP-6 promoter activity in MCF-7 cells, and PTHrP (1–40), but not PTHrP (107–139) exerted a similar effect as dbcAMP. The addition of H89 rescued the inhibitory effect of PTHrP (1–40) on BMP-6 promoter.
Inhibition of BMP-6 expression by PTHrP is dependent on PKA signaling pathway. a MCF-7 cells were treated with a series of kinase inhibitors against the signaling pathways downstream of PTHrP [H-89 (10 µM) for PKA inhibition, GO-6976 (12 µM) for PKC inhibition, SB203850 (10 µM) for MAP kinase inhibition, and U0126 (10 µM) for MEK inhibition]. 24 h after the treatment, total RNA was extracted and BMP-6 mRNA expression level was detected through real-time PCR. b 1.2 kb BMP-6 promoter-luciferase plasmid was transient transfected into MCF-7 cells, 24 h later, the cells were treated with 0.5 mM dibutyryl cAMP (dbcAMP), 100 nM PTHrP (1–40), 100 nM PTHrP (107–139) and 10 µM H89 (a PKA inhibitor), either alone or in combination, luciferase activities were detected 24 h after the treatment. *P < 0.05 compared with control
PTHrP exerts its antimitogenic effect through downregulating BMP-6
To investigate the biological significance of PTHrP downregulating BMP-6 mRNA expression in breast cancer cells, BMP-6 was silenced in MCF-7 cells (Fig. 4a) and cell proliferation assay was performed. As Fig. 4b shown, the treatment of PTHrP (1–40) inhibits cell proliferation in MCF-7 cells, which is coincident with the previous findings (Maioli and Fortino 2004). The similar effect was observed in the group treated with dbcAMP. The silencing of BMP-6 gene strengthened the antimitogenic effect of PTHrP, and overexpression of BMP-6 gene overcame the antimitogenic effect of PTHrP. To confirm this result, cell cycle assay was performed by flow cytometry. As shown in Fig. 4c and Table 2, a significant decreased number of cells at S–G2–M phase were found in PTHrP treated group, the PTHrP/siBMP-6 group showed more effective inhibition on cell progression, and the PTHrP/BMP-6 group eliminated the inhibition of PTHrP on cell progression. These results indicate that PTHrP functions as the upstream regulator of BMP-6 and exerts its antimitogenic effect through downregulating BMP-6 mRNA expression.
PTHrP exerts antimitogenic effect through downregulating BMP-6 expression. Cells were transfected with siRNA for silencing BMP-6 (siBMP6) or pcDNA6B-BMP6 for overexpressing BMP6. 24 h after the transfection, the medium was transferred to 2.5% serum and the cells were treated with PTHrP (1–40) (100 nM) or dbcAMP (0.5 mM) for 72 h. The silencing efficiency was validated by real-time PCR (a). Cell proliferation assay was performed using Cell Counting Kit (b) and cell cycle assay was performed through flow cytometry (c). *P < 0.05 compared with control
Discussion
In this study, we observed that the expression of the two genes, BMP-6 and PTHrP, were negatively correlated in breast cancer specimens. PTHrP (1–40), not PTHrP (107–139), exhibited inhibitory effect on the mRNA expression of BMP-6, indicating that PTHrP regulates BMP-6 gene expression through PTH1R. Using inhibitors against different PTHrP signaling pathways, we found that PTHrP inhibits BMP-6 expression through PKA signaling pathway. Our data indicates that BMP-6, acts as a downstream target of PTHrP signaling pathway, is downregulated by PTHrP in breast cancer cells, and the biological significance of this process turns to be the antimitogenic effect.
PTHrP and BMP-6 are two important growth factors for normal development. PTHrP plays a central role during the chondrogenesis. Besides, abnormal breast development was detected in patients with Blomstrand chondrodysplasia because of the impairment of the PTHrPR1 signaling pathway, indicating that the PTHrP is necessary for the formation of human mammary glands (Wysolmerski et al. 2001). BMP-6 regulates proliferation and apoptosis of mesenchymal and epithelial cells during the development (Hogan 1996–1997). If the tumorigenesis of breast carcinoma is the opposite of normal mammary gland growth, the interaction between these two genes during normal development may give us some hints of their exact functions during the disease process. The interaction between PTHrP and BMP-6 was found to contribute to the regulation between cell proliferation and differentiation. Addition of PTHrP abolished the expression of BMP-6 mRNAs in chondrocytes and inhibits chondrocyte maturation (Grimsrud et al. 2001). When exogenous BMP-6 was added to PTHrP containing cultures, maturation occurred with the expression of high levels of type-X collagen, despite the presence of PTHrP in the cultures (Grimsrud et al. 1999).
PTHrP and BMP-6 participate in the process of carcinogenesis. Dai et al. found that BMP-6 contributes to the osteoblastic activity of prostate cancer in vivo indicating that BMP-6 may participates in promoting the ability of tumor cells to invade the bone microenvironment (Dai et al. 2005). Previously, we reported BMP-6 gene expression can be activated dose-dependently by estrogen because of the demethylation status of BMP-6 promoter in ER+ breast cancer cell lines indicating that BMP-6 may play an important role during the process of ER-positive breast tumor growth. In addition to BMP-6, PTHrP has now been shown to function as an paracrine or autocrine growth factor to suppress the growth of transformed cells, such as human astrocytes and hepatoma cells (hep G2) (Li et al.1996; Shankar et al. 2000). Although based on the hypercalcemic effect of PTHrP, PTHrP is defined as a potential activation factor which endows tumor cells with a special property they require to establish and grow in bone, more and more clinical evidences have indicated that PTHrP expression in primary tumors connote prolonged survival in some types of human cancer such as breast cancer (Henderson et al. 2006; Bakre et al. 2002), hepatoma (Li et al. 1996) and lung cancer (Montgrain et al. 2007). Midregion PTHrP (38–94) restrains MDA–MB-231 growth and accelerates cell death through inducing the expression of Bcl-xs, Bad, Rip1 and caspases (Luparello et al. 2008). Studies by Bakre et al. (2002) show that local administration of PTHrP is a potential effective strategy to inhibit angiogenesis and tumor growth. The molecular mechanism of how PTHrP exerts its inhibitory effect on breast cancer cells proliferation needs to be investigated further.
PTHrP activates G-protein-coupled receptor, thereby activating the adenylate cyclase-protein kinase A (AC-PKA) and phospholipase C-protein kinase C (PLC-PKC) pathways (Abou-Samra et al. 1992; Hoare et al. 2001). Previous studies have shown that the activation of PKA by cAMP in MDA-MB-231 cells leads to Raf-1 kinase inactivation and results in significant suppression of cell invasion (Carie and Sebti 2007). PTHrP inhibits endothelial cell migration in vitro and angiogenesis in vivo by activating protein kinase A (Bakre et al. 2002). Maioli and Fortino (2004) found that PTHrP inhibits breast cancer cell proliferation through the combined action of the adenylylcyclase (AC)/PKA and phospholipase C (PLC)/PKC pathways. In our experiment, we have observed the same function of PTHrP/PKA. In addition, we have characterized that BMP-6 is one of the downstream targets of PTHrP/PKA signaling in the process of breast cancer cells proliferation inhibition. This finding may provide us some clues to investigate the detailed role that PTHrP plays during breast carcinogenesis.
References
Abou-Samra AB, Jüppner H, Force T, Freeman MW, Kong XF, Schipani E, Urena P, Richards J, Bonventre JV, JTJr Potts (1992) Expression cloning of a common receptor for parathyroid hormone and parathyroid hormone-related peptide from rat osteoblast-like cells: a single receptor stimulates intracellular accumulation of both cAMP and inositol trisphosphates and increases intracellular free calcium. Proc Natl Acad Sci USA 89:2732–2736
Akiyoshi T, Uchida K, Tateyama S (2004) Expression of bone morphogenetic protein-6 and bone morphogenetic protein receptors in myoepithelial cells of canine mammary gland tumors. Vet Pathol 41:154–163
Babitt JL, Huang FW, Xia Y, Sidis Y, Andrews NC, Lin HY (2007) Modulation of bone morphogenetic protein signaling in vivo regulates systemic iron balance. J Clin Invest 117:1933–1939
Bakre MM, Zhu Y, Yin H, Burton DW, Terkeltaub R, Deftos LJ, Varner JA (2002) Parathyroid hormone-related peptide is a naturally occurring, protein kinase A-dependent angiogenesis inhibitor. Nat Med 8:995–1003
Carie AE, Sebti SM (2007) A chemical biology approach identifies a beta-2 adrenergic receptor agonist that causes human tumor regression by blocking the Raf-1/Mek-1/Erk1/2 pathway. Oncogene 26:3777–3788
Clement JH, Sänger J, Höffken K (1999) Expression of bone morphogenetic protein 6 in normal mammary tissue and breast cancer cell lines and its regulation by epidermal growth factor. Int J Cancer 80:250–256
Dai J, Keller J, Zhang J, Lu Y, Yao Z, Keller ET (2005) Bone morphogenetic protein-6 promotes osteoblastic prostate cancer bone metastases through a dual mechanism. Cancer Res 65:8274–8285
Doisneau-Sixou SF, Sergio CM, Carroll JS, Hui R, Musgrove EA, Sutherland RL (2003) Estrogen and anti-estrogen regulation of cell cycle progression in breast cancer cells. Endocr Relat Cancer 10:179–186
Grimsrud CD, Romano PR, D’Souza M, Puzas JE, Reynolds PR, Rosier RN, O’Keefe RJ (1999) BMP-6 is an autocrine stimulator of chondrocyte differentiation. J Bone Miner Res 14:475–482
Grimsrud CD, Romano PR, D’Souza M, Puzas JE, Schwarz EM, Reynolds PR, Roiser RN, O’Keefe RJ (2001) BMP signaling stimulates chondrocyte maturation and the expression of Indian hedgehog. J Orthop Res 19:18–25
Henderson M, Danks J, Moseley J, Slavin J, Harris T, McKinlay M, Hopper J, Martin T (2001) Parathyroid hormone-related protein production by breast cancers, improved survival, and reduced bone metastases. J Natl Cancer Inst 93:234–237
Henderson MA, Danks JA, Slavin JL, Byrnes GB, Choong PF, Spillane JB, Hopper JL, Martin TJ (2006) Parathyroid hormone-related protein localization in breast cancers predict improved prognosis. Cancer Res 66:2250–2256
Hoare SR, Gardella TJ, Usdin TB (2001) Evaluating the signal transduction mechanism of the parathyroid hormone 1 receptor. Effect of receptor-G-protein interaction on the ligand binding mechanism and receptor conformation. J Biol Chem 276:7741–7753
Hogan BL (1996–1997) Bone morphogenetic proteins: multifunctional regulators of vertebrate development. Harvey Lect 92:83–98
Li H, Seitz PK, Selvanayagam P, Rajaraman S, Cooper CW (1996) Effect of endogenously produced parathyroid hormone-related peptide on growth of a human hepatoma cell line (Hep G2). Endocrinology 137:2367–2374
Luparello C, Sirchia R, Sasso BL (2008) Midregion PTHrP regulates Rip1 and caspase expression in MDA-MB231 breast cancer cells. Breast Cancer Res Treat 111:461–474
Maioli E, Fortino V (2004) PTHrP on MCF-7 breast cancer cells: a growth factor or an antimitogenic peptide? Br J Cancer 90:1293–1294
Montgrain PR, Quintana R, Rascon Y, Burton DW, Deftos LJ, Casillas A, Hastings RH (2007) Parathyroid hormone-related protein varies with sex and androgen status in nonsmall cell lung cancer. Cancer 110:1313–1320
Nakamura H, Hiraga T, Ninomiya T, Hosoya A, Fujisaki N, Yoneda T, Ozawa H (2008) Involvement of cell-cell and cell-matrix interactions in bone destruction induced by metastatic MDA-MB-231 human breast cancer cells in nude mice. J Bone Miner Metab 26:642–647
Pisani P, Parkin DM, Bray F, Ferlay J (1999) Estimates of the worldwide mortality from 25 cancers in 1990. Int J Cancer 83:870–873
Powell GJ, Southby J, Danks JA, Stillwell RG, Hayman JA, Henderson MA, Bennett RC, Martin TJ (1991) Localization of parathyroid hormone-related protein in breast cancer metastases: increased incidence in bone compared with other sites. Cancer Res 51:3059–3061
Rajendra K, John FR, Sue AW (2006) Nuclear targeting of a midregion PTHrP fragment is necessary for stimulating growth in breast cancer cells. Int J Cancer 119:49–59
Shankar PP, Wei H, Davee SM, Funk JL (2000) Parathyroid hormone-related protein is expressed by transformed and fetal human astrocytes and inhibits cell proliferation. Brain Res 868:230–240
Southby J, Kissin MW, Danks JA, Hayman JA, Moseley JM, Henderson MA, Bennett RC, Martin TJ (1990) Immunohistochemical localization of parathyroid hormone-related protein in human breast cancer. Cancer Res 50:7710–7716
Torricelli C, Fortino V, Capurro E, Sacchi G, Ponzo P, Pacini A, Muscettola M, Maioli E (2006) Role of PTHrp and PTHrp-engaged pathways in MCF-7 cells migration/invasion. Matrix Biol 25:104–111
Wysolmerski JJ, Cormier S, Philbrick WM, Dann P, Zhang JP, Roume J, Delezoide AL, Silve C (2001) Absence of functional type 1 parathyroid hormone (PTH)/PTH-related protein receptors in humans is associated with abnormal breast development and tooth impaction. J Clin Endocrinol Metab 86:1788–1794
Zhang M, Yan JD, Zhang L, Wang Q, LV SJ, Zhang J, Zhu TH (2005) Activation of bone morphogenetic protein-6 gene transcription in MCF-7 cells by estrogen. Chin Med J 118:1629–1636
Zhang M, Wang Q, Yuan W, Yang S, Wang X, Yan JD, Du J, Yin J, Gao SY, Sun B (2007) Epigenetic regulation of bone morphogenetic protein-6 gene expression in breast cancer cells. J Steroid Biochem Mol Biol 105:91–97
Acknowledgments
This work was supported by a grant from the National Nature Science Foundation of China to S. Yang (No. 30700471).
Conflict of interest statement
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
D. Mi and M. Zhang contributed equally to this work.
Rights and permissions
About this article
Cite this article
Mi, D., Zhang, M., Yan, Jd. et al. PTHrP inhibits BMP-6 expression through the PKA signaling pathway in breast cancer cells. J Cancer Res Clin Oncol 137, 295–303 (2011). https://doi.org/10.1007/s00432-010-0883-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-010-0883-y