Abstract
Intestinal inflammation results in disturbed intestinal motility in humans as well as in animal models. This altered function of smooth muscle cells and/or the enteric nervous system may be caused by activation of macrophages in muscularis externa and a thereby following release of cytokines and chemokines that causes influx of mononuclear cells and neutrophilic granulocytes. We subjected osteopetrotic (op/op) mice that lack certain macrophage subtypes, e.g. macrophages in the muscularis externa and +/+ mice to LPS to induce inflammatory cell influx. The densities of F4/80+, MHCII+, and myeloperoxidase+ cells were quantified using stereological sampling. In +/+ mice we found that MHCII+ cells outnumber F4/80+ cells and that LPS injection increased the density of MHCII+ cells temporarily but not that of F4/80+ cells. This indicates that an upregulation of MHCII antigen takes place and that two or more macrophage subtypes with comparable morphologies exist. Osteopetrotic mice lacked MHCII+, CD169+, and F4/80+ cells after either treatment, which indicate that these cells are CSF-1-dependent. LPS induced VCAM-1 activation of the vessels, modest influx of granulocytes, as well as an iNOS-activation in a cell type different from macrophages in both +/+ and op/op mice.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Disturbed intestinal motility is seen in both human inflammatory intestinal diseases as well as in animal models for sepsis and inflammatory intestinal diseases (De Winter et al. 2005; Eskandari et al. 1997; Nissan et al. 1997). It has been suggested that this altered function of the enteric nervous system and/or the smooth muscle cells is caused by activation of the macrophages that reside in the tunica muscularis. The macrophage activation is thought to increase the secretion of cytokines and chemokines, thereby resulting in an influx of mononuclear leucocytes (Henderson et al. 2003).
It has been shown that lipopolysaccharide (LPS) administration to mice causes disturbed gastrointestinal motility with altered transit time and intussusceptions of the small and large intestine (Nissan et al. 1997; De Winter et al. 2005). Both NO and various inflammatory mediators have been shown to contribute to these effects. Lipopolysaccharide is an activator of the innate immune system and thereby of NF-κB, which controls transcriptional activity of the promoters of proinflammatory cytokines, enzymes (cycloxygenase-2, inducible nitric oxide synthase), and adhesion molecules (ICAM-1, VCAM-1) (Jersmann et al. 2001; Ruetten et al. 1999).
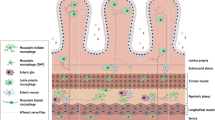
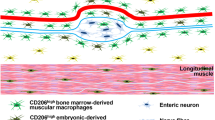
The op/op mouse (Csf1op/Csf1op) lacks a functional macrophage colony stimulating factor-1 (CSF-1) (Yoshida et al. 1990) as well as subgroups of macrophages (Cecchini et al. 1994; Wiktor-Jedrzejczak et al. 1992) in particular the macrophages residing in the tunica muscularis of the small intestine (Mikkelsen and Thuneberg 1999). The aim of our present study was to evaluate if presence/absence of macrophages in the muscularis externa plays a role regarding cell recruitment and/or activation during LPS-induced inflammation in mice. The cells were demonstrated using MHCII antibodies as well as the pan-macrophage antibody F4/80. F4/80 has been identified as a maturation marker on mononuclear phagocytes, eosinophils and subset of dendritic cells (McGarry and Stewart 1991; McGarry and Stewart 1991; Vremec et al. 2000). We have previously shown that F4/80 is expressed on macrophages in the muscularis externa (Mikkelsen et al. 1988a, 2004; Mikkelsen and Thuneberg 1999). MHC class II antigens are expressed by B lymphocytes, some macrophages, monocytes, and dendritic cells. To further characterize the macrophages we used an antibody towards sialoadhesin (CD169), a lectin which is expressed by some macrophages (Crocker and Gordon 1989; Hartnell et al. 2001) and also has been shown to be present on stellate cells in mouse muscularis externa (De Winter et al. 2005). To demonstrate granulocytes we used antibodies towards myeloperoxidase. To demonstrate interstitial cells of Cajal we used antibodies towards the kit-receptor. As activation markers we used antibodies towards iNOS and VCAM1.
Materials and methods
Animals
Six to eight week-old female op/op and +/+ mice were used. The original op/op line was bought from Jackson (Bar Harbor, ME) (Mikkelsen and Thuneberg 1999) and has been backcrossed onto a C57Bl/6 background. The breeding pairs were op/op males and op/+ females. The op/op mice were bred under specific pathogen-free conditions and the +/+ mice were C57Bl/6 mice bred under identical conditions in Panum’s animal stable. In pilot studies op/+ mice were used as controls as well. The op/op mice were fed with TRANSWEAN IRR diet powder (SDS, England) and the +/+ mice were fed with standard laboratory chow. The animals had free access to water and food.
One group of op/op mice (n = 12) and one group of +/+ mice (n = 27) were injected intraperitoneally with 20 μg/g of Escherichia coli LPS (Sigma, Serotype 055:B5, L-2880) dissolved in sterile 0.9% NaCl and were killed after 3, 6, or 24 h (LPS type and dose have been used in comparable studies) (De Winter et al. 2005). Another group of op/op (n = 13) and +/+ mice (n = 23) were sham-injected with 0.9% NaCl and were killed after 3, 6, or 24 h. Furthermore, five C57Bl/6 mice from another stable (Taconic), either treated with saline or LPS were killed after 16 h. The mice were killed by cervical dislocation. Whole mount preparations were prepared from jejunum and ileum. In addition, specimens of the distal part of ileum (about 3 cm, not including the distal 1 cm before caecum) were cut into 4 mm pieces and quick-frozen in isopentane cooled in liquid nitrogen, and stored at −80°C until cryostat sectioning (8 μm). All the animals were housed and experimentally manipulated in accordance with current national regulations issued by The Danish Council on Animal Care.
Antibodies
The fixation protocol, primary and secondary antibodies used in the whole mount preparations are presented in Table 1. Reactions with rat anti-F4/80 were enhanced with Tyramid Signal Amplification, as mice with C57Bl/6 background exhibit a weak staining when using conventional immunohistochemistry. Specimens were double stained by adding two antibodies (rabbit anti-iNOS combined with either rat anti-mouse MHC class II antigen or rat anti-CD169; or rabbit anti-kit receptor combined with rat anti-mouse MHC class II antigen). The specimens were incubated overnight and processed with EnVision followed by Tyramid Signal Amplification, and finally with rhodamine-conjugated goat anti-rat antibodies. Regarding double staining with iNOS/MHCII the whole mounts were also incubated sequentially using a crossover design starting with a complete iNOS staining followed by a complete MHCII staining; alternatively starting with a complete MHCII staining followed by the iNOS staining.
Controls were incubated with rat IgG2b (Serotec), rat IgG2a (Serotec), rabbit IgG (Dako-Cytomation) and irrelevant rat or rabbit antibodies.
Immunohistochemistry
Whole mounts from jejunum were stretched preparations of muscularis externa where mucosa and submucosa had been removed with fine forceps and scissors under a stereomicroscope; they were kept in TBS on ice during the procedure. The isolated muscle coats were placed in TBS with nifedipine 1 μmol/l to ensure relaxation and were pinned and stretched onto a Sylgard plate and fixed according to Table 1. Whole mounts from ileum, (kit receptor for double staining with MHCII) were prepared by inserting flat pieces of dental wax into the gut lumen and subsequently fixated in 2% formaldehyde overnight at +4°C. The mucosa and submucosa were removed and the isolated muscle coats were kept in TBS at +4°C until immunostaining. Before immunostaining the muscle strips and frozen sections were quenched in 1% H2O2. Incubation and washing solutions contained 0.5% Triton-X 100. The tissue was preincubated with 10% goat serum to reduce nonspecific staining.
Stereological analysis
The areal densities (i.e. the number of cells per surface area of the muscle coat) of F4/80+, MHCII+ and myeloperoxidase+ cells were estimated in whole mounts from the proximal jejunum using unbiased stereological counting through the full-thickness of the whole mount specimen (Alberti et al. 2005). F4/80+ cells were counted at a final magnification of 1,024× using an 20× oil immersion objective (NA = 0.8). The sampling fraction was ≈1:49. MHCII+ and myeloperoxidase+ cells were counted at a final magnification of 2,031× using an 40× oil immersion objective (NA = 1.0). The sampling fractions were ≈1:192 and 1:3, respectively.
Statistics
Osteopetrotic mice had virtually no MHCII+ and F4/80+ cells and the cells did not respond to LPS treatment (see Fig. 2), so no statistical tests were regarded necessary to compare the mice types. For each treatment regime (saline and LPS) a single factor analysis of variance (ANOVA) were used to test if various time points following treatment resulted in different response. The ANOVA was used to compare the densities of MHCII+, F4/80+, and myeloperoxidase+ cells in +/+ animals as well as myeloperoxidase+ cells in op/op mice. If there was no difference between the time points all animals were pooled into one group and saline treatment was compared to LPS treatment using the appropriate unpaired two tailed t test (variance homogeneity tested with the F test) using a 5% significance level.
Results
Clinically both op/op and +/+ mice were affected by the LPS treatment. They were lethargic and most had dilated stomachs. These effects were not observed in saline-treated op/op and +/+ mice. In a 6 h LPS-treated +/+ mouse intussusception was observed.
Immunohistochemistry
In +/+ mice F4/80+ cells were present at three levels (Fig. 1a). In the serosa they appeared as both oblong and ramified cells whereas only ramified cells with a stellate morphology were seen at the level of Auerbach’s plexus (AP). At the level of the deep muscular plexus (DMP), between the inner and outer circular muscle layer, a few bipolar cells were present. LPS treatment did not affect the morphology of F4/80+ cells and we did not observe spherical cells with monocyte morphology (Fig. 1b). In op/op mice very few positive cells were seen, a few clusters of 2–15 ramified F4/80+ cells were occasionally observed after both saline and LPS treatment (Fig. 1c, d). The densities of F4/80-positive cells are shown in Fig. 2a. F4/80+ cells were present in all +/+ mice but were virtually absent in the op/op mice therefore the latter was not subjected to statistical analysis. We did not find a statistical significant effect of LPS treatment when compared to saline treatment in +/+ animals (2P = 0.23, Fig. 2b).
a–d Whole mounts with F4/80+ cells from jejunum. e–h Whole mounts with MHCII+ cells from jejunum. a F4/80+ cells in saline-treated +/+ mouse. Both stellate cells and more oblong cells were present and represent cells in serosa and at the level of Auerbach’s plexus (AP). b F4/80+ cells in serosa and at AP in a +/+ mouse 6 h after LPS treatment. Smaller round cells were not apparent. c op/op mouse 3 h after saline treatment. d op/op mouse 3 h after LPS treatment. Only a few scattered F4/80+ cells were present. e MHCII+ cells in serosa and at AP in saline treated +/+ mouse. Both stellate and more oblong cells were present. f MHCII+ cells in +/+ mouse 6 h after LPS treatment. g op/op mouse 3 h after saline treatment. h op/op mouse 6 h after LPS treatment. Only a few scattered MHCII+ cells were present. The magnification bar is 100 μm in all micrographs
The densities of MHCII+ cells (shown as circles), F4/80+ cells (shown as triangles), myeloperoxidase+ cells (shown as squares), and CD169+ cells (shown as diamonds). Symbols for op/op mice are shown with a circle inside the symbol and symbols for +/+ mice are shown without the circle. a In +/+ mice the densities of MHCII+ cells and F4/80+ cells are given at three different time points following saline treatment (open symbols) or LPS treatment (solid symbols). Data from the same animal are tied by the vertical line. The solid horizontal lines indicate the group means of MHCII+ cells and the dashed lines indicate the group means of F4/80+ cells. b The densities of MHCII+ cells and F4/80+ cell pooled for all time points following both treatments. Symbols as in a. c The densities of myeloperoxidase+ cells following saline treatment and LPS treatment. Symbols as in a. d The densities of MHCII+ cells and CD169+ cells from a pilot study using another C57Bl/6 strain. Symbols as described above
Antibodies towards MHC class II antigen produced a staining pattern comparable to that of F4/80 antibodies. That is, in the serosa MHCII+ cells were present as oblong and ramified cells, at the level of AP as ramified, stellate cells, and at DMP as bipolar cells in all +/+ mice (Fig. 1e, f), but only few cells were observed in op/op mice (both saline- and LPS-treated, Fig. 1g, h). The density of MHCII+ cells differed significantly (2P = 0.045) between LPS and saline treatment in +/+ mice (Fig. 2a, b).
The distribution and morphology of CD169+ cells resembled that of F4/80+ and MHCII+ cells in +/+ mice (Figs. 3a, b and 4h). In op/op mice CD169+ cells were absent in the muscle layers (Fig. 3c). In a small pilot study using C57Bl/6 mice from another breeder we quantitated CD169+ cells in whole mounts 16 h after LPS and saline treatment (see data in Fig. 2d). The data suggest that in saline-treated mice the density of CD169+ cells seems slightly lower than the density of MHCII+ cells.
a–c CD169 reactivity in frozen sections from ileum. a and b CD169+ cells were present in the serosa and between the longitudinal (LM) and circular muscle layer (CM) of +/+ mice 6 h after saline treatment (a) and 6 h after LPS treatment (b). In addition, CD169+ cells were present in the submucosa (SM) and between the crypts. In op/op mice CD169+ cells were absent 6 h after LPS treatment (c). Bar 50 μm. d–f Myeloperoxidase+ cells in whole mounts from jejunum. d Saline-treated +/+ mouse, myeloperoxidase+ cells were not present; however there was a staining of the plexus (P). e Myeloperoxidase+ cells in a +/+ mouse 6 h after LPS treatment, the cells were heavily stained. f op/op mouse 6 h after LPS treatment, myeloperoxidase+ cells were present inside the vessels (arrow), and outside the vessels (arrowhead). Bars 100 μm. g–i VCAM-1 in frozen sections from ileum. Endothelial cells are VCAM-1 positive in vessels (arrows) between the longitudinal (LM) and circular (CM) muscle layers and in vessels in submucosa (SM). g op/op mouse 3 h after LPS treatment. i op/op mouse 6 h after LPS treatment. h +/+ mouse 24 h after LPS treatment. Bar 50 μm
a–c iNOS+ cells in whole mounts from jejunum. a iNOS+ cells in saline-treated +/+ mouse. iNOS+ cells were only present in ganglion cells in AP (arrow); a weak staining was also present in the secondary plexus. b +/+ mouse 6 h after LPS treatment. Ramified iNOS+ cells were situated in the interspaces between ganglia and internodal strands of AP. They had several long cell processes and some of them seemed to be in contact with each other. c op/op mouse 6 h after LPS treatment. Area with iNOS+ cells with long cell ramifications. Bar 50 μm. d–f Confocal micrographs of a whole mount at the level of AP. Double-staining with antibodies towards iNOS and MHCII in a +/+ mouse 6 h after LPS treatment. d iNOS+ cells. e MHCII+ cells and f. iNOS+ and MHCII+ cells. The iNOS+ cells differed from MHCII+ cells. The MHCII+ cells appeared more stellate and had shorter cell processes than the iNOS+ cells; there was no co-staining. Bar 20 μm. g–i Double-staining with antibodies toward iNOS and CD169 in a whole mount from the jejunum of a +/+ mouse at the level of AP 16 h following LPS treatment. g iNOS+ cells. h CD169+ cells. i iNOS+ and CD169+ cells; there was no co-staining. Bar 20 μm. j–l Double-staining with antibodies towards kit receptor and MHCII in a whole mount from the ileum of a +/+ mouse at the level of AP 6 h after LPS treatment. j Kit receptor+ cells. k MHCII+ cells. l Kit receptor+ and MHCII+ cells. The kit receptor+ interstitial cells of Cajal formed a typical network and were in close spatial contact with MHCII+ cells, but they were two separate cell types. Bar 20 μm
Only few myeloperoxidase+ cells were observed following both saline and LPS treatment. They were observed both inside and outside the lumen of vessels and were intensely stained (Fig. 3d–f). Additionally, the antibody stained the Auerbach’s plexus weakly. This was probably an unspecific cross-reaction as it was observed in both H2O2-quenched and unquenched preparations but was absent when using irrelevant rabbit antibodies. The densities are shown in Fig. 2c. LPS treatment resulted in an influx of cells that were significantly different from the saline-treated mice in both +/+ mice (2P = 0.0002) and op/op mice (2P = 0.006).
In both mice types VCAM-1 was present in endothelial cells of the vessels after LPS treatment, both in the vessels between the muscle layers as well as in vessels in the submucosa and the mucosa (Fig. 3g–i). After saline treatment VCAM-1+ cells were not observed in the vessels of either mouse type.
Scattered, ramified iNOS+ cells were present at the level of AP 6, 16 and 24 h after LPS treatment in both +/+ mice and to a lesser extent in op/op mice (Fig. 4b, c). The iNOS+ cells appeared to have thinner and longer processes/ramifications than the F4/80+, CD169+ and MHCII+ cells. Some of the iNOS+ cells bordered the ganglia and were in contact with each other, but they did not create a real network as the interstitial cells of Cajal normally do. Others had a more solitary position and were situated in the interspace between ganglia and internodal strands of AP. Co-staining with MHCII and iNOS and CD169 and iNOS was not apparent (Fig. 4d–i). In saline-treated mice (of both groups) only smaller nerve fibers and solitary ganglion cells in AP were positively stained for iNOS (Fig. 4a). This staining was considered to be a weak cross-reaction with nNOS (neuronal nitric oxide synthase), which is a well-known phenomenon.
In whole mounts from all mice, a typical network of ramified kit receptor+ interstitial cells of Cajal (ICC) was apparent at the level of AP. In addition, more oblong cells with fewer processes were present at the DMP. Double staining with MHCII and kit receptor antibodies showed that ICCs and MHCII+ cells at the level of both AP and of DMP were in close spatial contact, but that they were two separate cell types (Fig. 4j–l). The kit receptor+ cells seemed morphological unaffected by LPS treatment.
Discussion
We did not perform functional studies but observed ventricular distension in both mice types following LPS treatment. This finding is in accordance with another mouse study where the same LPS dose resulted in delayed gastric emptying and intestinal transit (De Winter et al. 2005).
Macrophages and/or dendritic cells
Our studies show that F4/80+ and MHCII+ cells are located at three levels in the muscularis externa of +/+ mice. None of these cells created networks within the population. MHCII+ cells outnumber F4/80+ cells but the cells have similar morphologies. It is therefore possible that the MHCII+ population consists of more than one group, i.e. a F4/80+ and a F4/80− group. The difference in density could theoretically also be caused by differential tissue shrinkage. We attempted, however, to avoid differential shrinkage by relaxing the tissue with nifedipine and stretch the tissue when pinning it onto Sylgard before fixation. To further characterize the cells we added an antibody towards sialadhesin (CD169) and found cells with a distribution and morphology, similar to that of F4/80 and MHCII+ cells. In +/+ mice we found that the density of MHCII+ cells seemed to increase temporarily following LPS treatment compared to saline treatment, whereas there were no significant increase in the density of F4/80+ cells following LPS treatment. Recruited macrophages are described to have a spherical morphology without processes (Kinoshita et al. 2007) and we did not observe cells with that morphology. It seems more likely that an upregulation/downregulation of different antigens takes place in different macrophage subgroups, rather than a regular cell recruitment takes place. In op/op mice the densities of F4/80+ and MHCII+ cells were sparse in the entire whole mount and they had no ability to increase either of the densities following LPS treatment. CD169+ cells were not observed in op/op mice. These observations indicate that the populations of F4/80+, CD169+, and MHCII+ cells in the muscularis are CSF-1 dependent.
We previously classified the ramified, stellate cells in mice and guinea pigs as macrophage-like cells because of their ability to endocytose and to retain FITC-dextran in large vesicles (Mikkelsen et al. 1985, 1988b). We later showed by staining these FITC-dextran containing cells with antibodies towards F4/80, MHCII and CD11b that they were always F4/80+ and CD11b+, whereas MHCII+ cells did not always contain FITC-dextran (Mikkelsen et al. 1988a). The latter observation has been confirmed using rat muscularis externa, Texas red dextran, and MHCII antibodies (Kinoshita et al. 2007). In NMRI mice we have also shown that FITC-dextran containing cells are class A scavenger receptor+ (Mikkelsen et al. 2004). In other studies the stellate cells were shown to be CD169+ (De Winter et al. 2005). The F4/80+ and MHCII+ cells in muscularis externa resemble Langerhans cells, which also have an endocytotic capacity, a stellate morphology, are F4/80+, and MHCII+, but in contrast to ramified cells in muscularis externa Langerhans cells contain Birbeck granules and have not been reported to exhibit class A scavenger receptor. In a recent paper it has been pointed out that 25 and 30% of the MHCII+ cells with a ramified morphology in the muscle layer of the mouse intestine express DEC-205 and CD11c respectively, which are markers for dendritic cells. Upon isolation, using an ovalbumin conjugated DEC-205 antibody, it was possible to target the cells in vivo. The cells were able to stimulate the proliferation of ovalbumin-specific CD4+ and CD8+ T cell antigen receptor-transgenic T cells (Flores-Langarica et al. 2005). In this report it was concluded that this antigen-presenting cell system in the muscle layers consists of dendritic cells, which were compared to cutaneous Langerhans cells. In op/op mice Langerhans cells have been reported to be unaffected by the mutation (Takahashi et al. 1993), whereas subtypes of dendritic cells were reduced in number by 50–70% (MacDonald et al. 2005; Witmer-Pack et al. 1993). So, regarding the muscularis externa it can be concluded that if a population of dendritic cells is present, it is CSF-1 dependent. However, we were unable to demonstrate CD11c+ cells in the muscularis externa. We have tested commercially available antibodies towards CD11c (Pharmingen) on both whole mounts and frozen sections fixed with different fixatives (e.g. acetone, paraformaldehyde, Carnoy, ethanol). Interestingly, recent studies indicate that some macrophages and dendritic cells renew from a common progenitor (Fogg et al. 2006) and that CD11c− macrophages can prime CD8+ T cells (Pozzi et al. 2005).
We quantified myeloperoxidase+ cells to examine for recruitment of these cell types into the muscularis after LPS treatment. A modest number of myeloperoxidase+ cells was recruited into both +/+ and op/op mice.
In a study using intestinal manipulation the number of peroxidase+ cells increased in both op/op and control mice but the increase was four times higher in control mice as compared to op/op mice (Wehner et al. 2006). In another manipulation study, mast cells seemed to be of importance for leukocyte recruitment into the muscularis (de Jonge et al. 2004). This indicates that factors other than presence of macrophages play a role for neutrophil recruitment in that system. This is in accordance with our findings where the discrete granulocyte recruitment seemed to be unaffected by the lack of CSF-1-dependent cells in the muscle layers. Also mast cells are present in the mesenterium of op/op mice (our unpublished observations).
Furthermore, in another experimental animal model (TNBS-induced colitis) where massive influx of granulocytes has been observed, chemoattractant proteins for neutrophilic leukocytes and for macrophages/monocytes have been shown to be upregulated (Kinoshita et al. 2007). Macrophages, mesothelial and endothelial cells have also been reported to be sources of chemoattractant proteins (Sakanashi et al. 1994; Zhang et al. 2005; Mutsaers 2002). In our study the influx of myeloperoxidase+ cells was weak in both +/+ as well as in op/op mice. It is therefore possible that the production of chemoattractants only took place in mesothelial and/or endothelial cells.
Cell activation
The LPS treatment in our study resulted in VCAM-1+ endothelial cells in vessels of both mice types whereas saline treatment did not activate VCAM-1.
iNOS+ cells were only present at the level of AP six and 24 h after LPS treatment. In both mice types the cells appeared only scattered but judged by eye there were fewer iNOS+ cells in op/op mice than in +/+ mice. iNOS+ cells were demonstrated using both DAB and fluorescence techniques and the cells did not resemble MHCII+ and F4/80+ cell using either of the techniques. Co-staining with iNOS and MHCII was not apparent in double stained whole mounts and the iNOS+ cells did not resemble interstitial cells of Cajal. These findings indicate that the iNOS+ cells constitute a population different from macrophage-like cells in C57Bl/6 mice. This is in contrast to findings in another study where 8% of CD169+ stellate cells in ileum were co-stained with anti-iNOS 18 h following LPS treatment of Swiss OF1 mice (De Winter et al. 2005). In that study LPS dose and type as well as antibodies and fixative used, were similar to our study, whereas mouse strain, gender, weight, possibly age, housing condition and duration of LPS exposure differed. iNOS+ cells with stellate morphologies have also been demonstrated in rats after LPS treatment (Eskandari et al. 1999). In that study the most prominent staining was shown 12 h following LPS. We added a group of +/+ mice, which were treated with LPS or saline for 16 h to examine animals between the two above mentioned time groups (i.e. 12 and 18 h). In these mice we replicated our previous finding regarding iNOS+ cells. In addition, we double-stained with anti-iNOS and anti-CD169 and did not find co-staining in the whole mounts. Furthermore, in this experiment the density of MHCII+ cells seemed unaltered in LPS-treated animals compared to saline-treated mice. This is in accord with our findings 24 h after LPS treatment and indicates that MHCII antigens are upregulated after 3 and 6 h, but subside again after 16 and 24 h.
Kalff et al. 2000 could not demonstrate stellate iNOS+ cells in the muscularis externa 24 h after intestinal manipulation in neither rats nor mice. However, iNOS+ monocytes as well as iNOS+ stellate cells has been described in the muscle layers following intestinal manipulation using iNOS−/− knock-out mice which had previously undergone bone marrow transplantation with iNOS+/+ leucocytes (Turler et al. 2006). This indicates that iNOS induction might differ when using this inflammatory model.
LPS treatment has also been shown to induce iNOS in muscularis macrophages in rats (Eskandari et al. 1999; Hori et al. 2001; Torihashi et al. 2000). The lacking iNOS-staining of macrophages in our present study could be due to a species difference or that an eventual iNOS induction in macrophages was too low to demonstrate. Since macrophages in C57Bl/6J mice have been shown to be high responders regarding inflammatory gene induction after LPS-stimulation (Wells et al. 2003) it is rather surprising. In addition to species difference there may also be strain differences in iNOS-reactivity. It is well known that F4/80-antibodies stain weakly in connective tissue of C57BL/6 mice using immunohistochemistry as compared to other mice strains. Also class A scavenger receptor antibodies (2F8) do not work on C57Bl/6 mice (Daugherty et al. 2000). These differences should be considered in experimental studies using mice with a C57Bl/6 background, which is the case for many knock-out and transgenic mice.
The characteristic network of interstitial cells of Cajal (ICC) appeared to be unaltered after LPS treatment in both +/+ and op/op mice. It was apparent that macrophage-like cells and ICC had close spatial contacts at AP when we double stained whole mounts with MHCII and kit receptor antibodies. This is in accordance with our previous findings using FITC-dextran and Toluidine blue staining (Mikkelsen et al. 1988b). Various experimental inflammatory conditions have been shown to affect the ICC network more or less. Intestinal obstruction in rats gave rise to significant increases in the numbers of CD14+ cells and ED2+ macrophages combined with a disruption of the ICC network and a reduction in the number of ICCs (Won et al. 2006). Another study reported that the ICC network disappeared and that the number of macrophages increased following TNBS-induced colitis in rats (Kinoshita et al. 2007). However, Wang et al. (2002) found only subtle changes in ICCs ultrastructure in mice infested with Trichinella spiralis, indicating that the damage of the ICC-network depends upon the severity of the inflammation.
Conclusion
LPS treatment resulted in VCAM-1 activation of the vessels, a limited recruitment of myeloperoxidase+ cells into the muscle layers, and iNOS activation in a cell type different from macrophages in both mice types. These activations demonstrate that LPS activates other cell groups in addition to macrophages. We can conclude that in mouse muscularis externa F4/80+, MHCII+, CD169+ cells are CSF-1 dependent and that the two latter seem to have comparable densities whereas the densities of F4/80+ cells were lower. This indicates that in the muscularis externa at least two CSF-1 dependent macrophage subtypes exist. Our study had only statistical power to demonstrate an increase in the density of MHCII+ cells when the three time points were pooled together but it appeared that the increase was only present 3 and 6 h after LPS injection indicating that an upregulation of this antigen temporarily takes place.
References
Alberti E, Mikkelsen HB, Larsen JO, Jimenez M (2005) Motility patterns and distribution of interstitial cells of Cajal and nitrergic neurons in the proximal, mid- and distal-colon of the rat. Neurogastroenterol Motil 17:133–147
Cecchini MG, Dominiguez MG, Mocci S, Wetterwald A, Felix R, Fleisch H, Chisholm O, Hofstetter W, Pollard JW, Stanley ER (1994) Role of colony of stimulating factor-1 in the establishment and regulation of tissue macrophages during postnatal development of the mouse. Development 120:1357–1372
Crocker PR, Gordon S (1989) Mouse macrophage hemagglutinin (sheep erythrocyte receptor) with specificity for sialylated glycoconjugates characterized by a monoclonal antibody. J Exp Med 169:1333–1346
Daugherty A, Whitman SC, Block AE, Rateri DL (2000) Polymorphism of class A scavenger receptors in C57BL/6 mice. J Lipid Res 41:1568–1577
de Jonge WJ, The FO, van der Coelen D, Bennink RJ, Reitsma PH, van Deventer SJ, van den Wijngaard RM, Boeckxstaens GE (2004) Mast cell degranulation during abdominal surgery initiates postoperative ileus in mice. Gastroenterology 127:535–545
De Winter BY, Van Nassauw L, De Man JG, de Jonge F, Bredenoord AJ, Seerden TC, Herman AG, Timmermans JP, Pelckmans PA (2005) Role of oxidative stress in the pathogenesis of septic ileus in mice. Neurogastroenterol Motil 17:251–261
Eskandari MK, Kalff JC, Billiar TR, Lee KKW, Bauer AJ (1997) Lipopolysaccharide activates the muscularis macrophage network and suppresses circular smooth muscle activity. Am J Physiol 273:G727–G734
Eskandari MK, Kalff JC, Billiar TR, Lee KKW, Bauer AJ (1999) LPS-induced muscularis macrophage nitric oxide suppresses jejunal circular muscle activity. Am J Physiol 277:G478–G486
Flores-Langarica A, Meza-Perez S, Calderon-Amador J, Estrada-Garcia T, Macpherson G, Lebecque S, Saeland S, Steinman RM, Flores-Romo L (2005) Network of dendritic cells within the muscular layer of the mouse intestine. Proc Natl Acad Sci USA 102:19039–19044
Fogg DK, Sibon C, Miled C, Jung S, Aucouturier P, Littman DR, Cumano A, Geissmann F (2006) A clonogenic bone marrow progenitor specific for macrophages and dendritic cells. Science 311:83–87
Hartnell A, Steel J, Turley H, Jones M, Jackson DG, Crocker PR (2001) Characterization of human sialoadhesin, a sialic acid binding receptor expressed by resident and inflammatory macrophage populations. Blood 97:288–296
Henderson RB, Hobbs JA, Mathies M, Hogg N (2003) Rapid recruitment of inflammatory monocytes is independent of neutrophil migration. Blood 102:328–335
Hori M, Kita M, Torihashi S, Miyamoto S, Won KJ, Sato K, Ozaki H, Karaki H (2001) Upregulation of iNOS by COX-2 in muscularis resident macrophage of rat intestine stimulated with LPS. Am J Physiol Gastrointest Liver Physiol 280:G930–G938
Jersmann HP, Hii CS, Ferrante JV, Ferrante A (2001) Bacterial lipopolysaccharide and tumor necrosis factor alpha synergistically increase expression of human endothelial adhesion molecules through activation of NF-kappaB and p38 mitogen-activated protein kinase signaling pathways. Infect Immun 69:1273–1279
Kalff JC, Schraut WH, Billiar TR, Simmons RL, Bauer AJ (2000) Role of inducible nitric oxide synthase in postoperative intestinal smooth muscle dysfunction in rodents. Gastroenterology 118:316–327
Kinoshita K, Horiguchi K, Fujisawa M, Kobirumaki F, Yamato S, Hori M, Ozaki H (2007) Possible involvement of muscularis resident macrophages in impairment of interstitial cells of Cajal and myenteric nerve systems in rat models of TNBS-induced colitis. Histochem Cell Biol 127:41–53
MacDonald KP, Rowe V, Bofinger HM, Thomas R, Sasmono T, Hume DA, Hill GR (2005) The colony-stimulating factor 1 receptor is expressed on dendritic cells during differentiation and regulates their expansion. J Immunol 175:1399–1405
McGarry MP, Stewart CC (1991) Murine eosinophil granulocytes bind the murine macrophage-monocyte specific monoclonal antibody F4/80. J Leukoc Biol 50:471–478
Mikkelsen HB, Thuneberg L (1999) Op/op mice defective in production of functional colony-stimulating factor-1 lack macrophages in muscularis externa of the small intestine. Cell Tissue Res 295:485–493
Mikkelsen HB, Thuneberg L, Rumessen JJ, Thorball N (1985) Macrophage-like cells in the muscularis externa of mouse small intestine. Anat Rec 213:77–86
Mikkelsen HB, Mirsky R, Jessen KR, Thuneberg L (1988a) Macrophage-like cells in muscularis externa of mouse small intestine: immunohistochemical localization of F4/80, M1/70, and Ia-antigen. Cell Tissue Res 252:301–306
Mikkelsen HB, Thuneberg L, Wittrup IH (1988b) Selective double staining of interstitial cells of Cajal and macrophage-like cells in small intestine by an improved supravital methylene blue technique combined with FITC-dextran uptake. Anat Embryol 178:191–195
Mikkelsen HB, Garbarsch C, Tranum-Jensen J, Thuneberg L (2004) Macrophages in the small intestinal muscularis externa of embryos, newborn and adult germ-free mice. J Mol Histol 35:377–387
Mutsaers SE (2002) Mesothelial cells: their structure, function and role in serosal repair. Respirology 7:171–191
Nissan A, Zhang JM, Lin Z, Haskel Y, Freund HR, Hanani M (1997) The contribution of inflammatory mediators and nitric oxide to lipopolysaccharide-induced intussusception in mice. J Surg Res 69:205–207
Pozzi LA, Maciaszek JW, Rock KL (2005) Both dendritic cells and macrophages can stimulate naive CD8 T cells in vivo to proliferate, develop effector function, and differentiate into memory cells. J Immunol 175:2071–2081
Ruetten H, Thiemermann C, Perretti M (1999) Upregulation of ICAM-1 expression on J774.2 macrophages by endotoxin involves activation of NF-kappaB but not protein tyrosine kinase: comparison to induction of iNOS. Mediators Inflamm 8:77–84
Sakanashi Y, Takeya M, Yoshimura T, Feng L, Morioka T, Takahashi K (1994) Kinetics of macrophage subpopulations and expression of monocyte chemoattractant protein-1 (MCP-1) in bleomycin-induced lung injury of rats studied by a novel monoclonal antibody against rat MCP-1. J Leukoc Biol 56:741–750
Takahashi K, Naito M, Schultz LD, Hayashi S, Nishikawa S (1993) Differentiation of dendritic cell populations in macrophage colony-stimulating factor-deficient mice homozygous for the osteopetrosis (op) mutation. J Leukoc Biol 53:19–28
Torihashi S, Ozaki H, Hori M, Kita M, Ohota S, Karaki H (2000) Resident macrophages activated by lipopolysaccharide suppress muscle tension and initiate inflammatory response in the gastrointestinal muscle layer. Histochem Cell Biol 113:73–80
Turler A, Kalff JC, Moore BA, Hoffman RA, Billiar TR, Simmons RL, Bauer AJ (2006) Leukocyte-derived inducible nitric oxide synthase mediates murine postoperative ileus. Ann Surg 244:220–229
Vremec D, Pooley J, Hochrein H, Wu L, Shortman K (2000) CD4 and CD8 expression by dendritic cell subtypes in mouse thymus and spleen. J Immunol 164:2978–2986
Wang XY, Berezin I, Mikkelsen HB, Der T, Bercik P, Collins SM, Huizinga JD (2002) Pathology of interstitial cells of Cajal in relation to inflammation revealed by ultrastructure but not immunohistochemistry. Am J Pathol 160:1529–1540
Wehner S, Behrendt FF, Lyutenski BN, Lysson M, Bauer AJ, Hirner A, Kalff JC (2007) Inhibition of macrophage function prevents intestinal inflammation and postoperative ileus in rodents. Gut 56 (2):176–185
Wells CA, Ravasi T, Faulkner GJ, Carninci P, Okazaki Y, Hayashizaki Y, Sweet M, Wainwright BJ, Hume DA (2003) Genetic control of the innate immune response. BMC Immunol 4:5
Wiktor-Jedrzejczak W, Ansari AA, Szperl M, Urbanowska E (1992) Distinct in vivo functions of two macrophage subpopulations as evidenced by studies using macrophage-deficient op/op mouse. Eur J Immunol 22:1951–1954
Witmer-Pack MD, Hughes DA, Schuler G, Lawson L, McWilliam A, Inaba K, Steinman RM, Gordon S (1993) Identification of macrophages and dendritic cells in the osteopetrotic (op/op) mouse. J Cell Sci 104(Pt 4):1021–1029
Won KJ, Suzuki T, Hori M, Ozaki H (2006) Motility disorder in experimentally obstructed intestine: relationship between muscularis inflammation and disruption of the ICC network. Neurogastroenterol Motil 18:53–61
Yoshida H, Hayashi S, Kunisada T, Ogawa M, Nishikawa S, Okamura H, Sudo T, Schultz LD (1990) The murine mutation osteopetrosis is in the coding region of the macrophage colony stimulating factor gene. Nature 345:442–444
Zhang X, Chen X, Song H, Chen HZ, Rovin BH (2005) Activation of the Nrf2/antioxidant response pathway increases IL-8 expression. Eur J Immunol 35:3258–3267
Acknowledgments
The present study was supported by a grant from S.C.E. Friis and wife D. Friis’s Foundation. The authors wish to thank Ha Nguyen, Pernille Froh and Keld Ottesen for skilled technical assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mikkelsen, H.B., Larsen, J.O. & Hadberg, H. The macrophage system in the intestinal muscularis externa during inflammation: an immunohistochemical and quantitative study of osteopetrotic mice. Histochem Cell Biol 130, 363–373 (2008). https://doi.org/10.1007/s00418-008-0423-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00418-008-0423-x