Abstract
This review will discuss some of the implications for using cells from aged donors for retinal pigment epithelium (RPE) transplantation. It will consider age-related changes in the structure and function of RPE cells and the accumulation of potentially damaging photoreactive constituents. The review will focus on the role of the ocular pigments lipofuscin and melanin in respect to age-related changes in composition, photoreactivity and potential role in retinal ageing and age-related macular degeneration. The article concludes by considering the suitability of senescent RPE cells for transplantation and whether such cells can be rejuvenated.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The retinal pigment epithelium (RPE) is essential for maintaining optimal photoreceptor structure and function [7, 10, 47, 48]. Loss or atrophy of the RPE results in not only photoreceptor loss but also abnormalities in the underlying choriocapillaries [38]. Specific gene defects in the RPE have been identified (e.g. RPE65 and mertk) in animals [2, 52, 70] which have also been confirmed in human disease [69, 78, 79]. Most complex eye diseases will have multigene defects which in many instances will render an individual more susceptible to environmental insult rather than the gene defect itself. However, environmental factors per se may well be equally important contributors toward the onset of RPE dysfunction. Evidence for this comes from age-related macular degeneration (AMD), in which abnormalities in the RPE–Bruch’s membrane complex are apparent and may well represent the accumulation of random damage from a variety of direct environmental insults (e.g. age, oxidative stress, smoking, light exposure) [4, 14]. A further major insult to the RPE is the repeated phagocytosis of photoreceptor outer segments by the retinal pigment epithelium. This allows the renewal of outer segments while removing the spent outer segment discs which will have become oxidised and accumulated numerous adducts. This can lead to a reduction in membrane fluid dynamics and increasing phototoxicity. It is highly probable that these oxidative changes to the outer segments render them partially non-degradable when in the phagolysosomal system and that this contributes to the progressive accumulation of lipofuscin in RPE cells throughout life [4, 21]. The age-related changes in RPE often lead to pathological tissue damage that warrants intervention (e.g. transplantation) in order to maintain quality of sight. The compositional changes that occur to and compromise the function of the RPE during life may themselves hinder the benefits of RPE transplantation [9].
RPE ageing
Age-related changes in the RPE and underlying Bruch’s membrane are well documented [7, 10, 29, 49]. The human RPE is normally a non-dividing system which, with increasing age, is seen to undergo a variety of structural and biochemical changes which are generally considered to be detrimental to optical cell function.
Morphology
Structural changes include loss of cell shape, hyperplasia with regions of multilayered cells, atrophy, hyperpigmentation and an increase in cell diameter as cells spread to fill the spaces left by dead cells [34].
RPE cell density decreases by up to 0.3% per year with increasing age [53]. Whether this cell loss is greatest in the macula, where metabolic activity is highest, remains equivocal.
Pigmentation
Both fundus examination and morphology demonstrate significant pigmentary changes in the RPE with increasing donor age. These changes include a linear increase in lipofuscin granules, a decrease in melanosome numbers and an increase in pigment complexes (e.g. melanolipofuscin and melanolysosomes) [7].
Advanced glycation endproducts
There is increasing evidence that advanced glycation endproducts (AGEs) accumulate within Bruch’s membrane and may modulate RPE cell behaviour. AGEs have been identified in RPE cells associated with lipofuscin [67], and AGEs have been shown to decrease lysosomal enzyme function if ingested [46].
Antioxidants
Age-related changes in antioxidant enzyme activity have been reported but their contribution to RPE dysfunction is difficult to interpret. Levels of vitamin E decrease with age [25], catalase activity increases with age (possibly due to an overall increase in H2O2-induced oxidative stress throughout life) and superoxide dismutase levels remain constant throughout life [42].
Molecular damage
Numerous studies in cell types other than the RPE have reported greater amounts of mitochondrial DNA damage, nuclear DNA damage, protein cross-linking and lipid hydroperoxides in aged cells than in their younger counterparts. It is likely such damage will also occur in RPE cells. RPE cells have been shown to demonstrate senescence-related β-galactosidose staining and telomere loss [33, 51].
It is therefore clear that RPE cells undergo significant age-related changes, many of which are non-reversible in such post-mitotic cells. The specialised role of the RPE lends itself to the accumulation of novel inclusions. This review focuses on the photochemical properties of lipofuscin, A2E and melanosomes since their presence impacts on the applicability of RPE cells for transplantation. Furthermore, it is unclear whether aged RPE cells can be rejuvenated in cell culture, and this will be discussed later in the review.
What is lipofuscin?
Lipofuscin is a lipid/protein aggregate that is generated within the lysosomal system of a variety of postmitotic cell types [71]. Lipofuscin accumulation has a positive correlation with increasing age which has led to this pigment being referred to as “age pigment” or a “senescence marker”. However, the photochemical properties of lipofuscin may themselves influence the ageing process. The common substrate for lipofuscin formation is autophagy of spent intracellular organelles such as mitochondria, Golgi bodies and endoplasmic reticulum [7, 13, 21]. However, the RPE is unique in that in this cell the major substrate for lipofuscin appears to be photoreceptor outer segment tips [7, 21]. An extrafoveal human RPE will phagocytose in the region of 40 outer segment tips per day and 40 complete rod outer segments every 10 days. It is believed that these tips undergo oxidative modification with the formation of cross-links and adducts which renders the outer segments only partially digestible [7]. It is this indigestible material which accumulates within the lysosomes in the form of lipofuscin granules. A unique feature of RPE lipofuscin is that it contains retinoid metabolites derived from the ingestion of outer segments [21]. These granules are about 1 μm in diameter and located within the mid-portion of RPE cells beneath the melanosomes (Fig. 1) [34]. Analyses have shown that lipofuscin progressively accumulates throughout life to eventually occupy up to 19% of cytoplasmic volume by 80 years of age [24]. Topographically, maximal accumulation of lipofuscin granules occurs in the posterior pole, albeit with a decrease at the fovea [81, 82]. This correlates with the density distribution of rod photoreceptor cells and points to outer segments being the primary substrate for lipofuscin [48, 82].
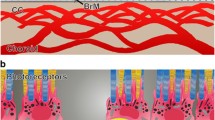
Photographs of the RPE. A Electron micrograph of human RPE from a 52-year-old donor (reproduced courtesy of John Marshall, St Thomas’s Hospital, London). Lipofuscin granules (thick arrows) can be seen in the mid portion of the cell and are often associated with small melanin deposits. Melanosomes (thin arrows) can be seen in the apical portion of the cell and are predominantly vertically oriented. Magnification ×13,100. B Fluorescence light micrograph showing RPE cells filled with fluorescent granules. Magnification ×1,000
A characteristic feature of RPE lipofuscin is its golden-yellow fluorescence (Fig. 1). Studies have revealed that there are substantial differences in emission properties between individual lipofuscin granules, and within a single granule, indicating a great heterogeneity within and among lipofuscin granules [16, 31, 32, 39].
Due to the complex nature of lipofuscin granules it has been difficult to identify constituent components. Eldred and Katz undertook a Folch’s chloroform/methanol extraction of RPE cells and identified at least 10 fluorophores in the chloroform fraction [22]. One of the fluorophores was a yellow–orange emitter. Further analyses of this fluorophore by Eldred and Lasky [23] led to the identification and structural characterisation of A2E [5, 61] now known to be a pyridinium bisretinoid occurring as a Schiff base reaction product derived from two molecules of vitamin A aldehyde and one molecule of ethanolamine. A2E can also exist as a slightly less hydrophobic photoisomer, iso-A2E, and other cis-isomers. In addition, there is recent evidence that A2E can photogenerate A2E epoxides [75]. Eldred and Katz also identified retinylpalmitate in RPE extracts [22], and this was later confirmed as a constituent of lipofuscin [41].
More extensive analysis did not take place until 2002, when Schutt and colleagues published a proteome of RPE lipofuscin [65]. Using a combination of 2D-gel electrophoresis, MALDI and HPLC-coupled electrospray tandem mass spectroscopy they were able to identify 76 proteins representing membrane, cytoskeletal, mitochondrial, metabolic and phototransduction and chaperone proteins. While these data provide an important insight into lipofuscin composition, any cellular contaminants in the granule preparation could have accounted for some or many of these proteins. The same group have also reported the presence of proteins modified by malondialdehyde, 4-hydroxynonenal and advanced glycation end-products (AGEs) in lipofuscin granules, which supports the view that much of lipofuscin is made up of oxidatively modified proteins [67].
The phototoxicity of lipofuscin
Taking into account the absorption spectra of lipofuscin, the repeated exposure of lipofuscin to visible light and its location in a region of high oxygenation, it is reasonable to hypothesise that lipofuscin may have the capacity to generate reactive oxygen species (ROS) [11, 83]. We have previously confirmed this hypothesis by demonstrating (a) that exposure of isolated lipofuscin granules to white light results in the generation of superoxide anions, their rate of production increasing with increasing light intensity and decreasing wavelength [11]; (b) that oxygen uptake (a measure of ROS production and susceptibility to photooxidation) by isolated RPE cells increases with donor age and that this is due to lipofuscin [57]; (c) that exposure to blue light results in the photogeneration of superoxide anions, hydroxyl radicals, singlet oxygen and lipid hydroperoxides [26, 57, 58]; (d) that triplet excited states, singlet oxygen and radical species produced by lipofuscin have sufficient lifetimes to allow interaction with biomolecules such as DNA, proteins and lipids [12]; and (e) that the increase in the susceptibility to photooxidation and photoinduced generation of ROS per lipofuscin granule with increasing donor age is due to an increase in the amount of the chloroform-insoluble fraction rather than a change in the concentration of chloroform-soluble fluorophores [60].
With the demonstration that lipofuscin is a photoinducible generator of ROS it was not surprising that lipofuscin under laboratory conditions was able to cause extragranular lipid peroxidation, inactivate lysosomal enzymes and reduce antioxidant activity [80]. In order to confirm the potential of lipofuscin to cause RPE dysfunction it is important to determine whether lipofuscin is able to elicit damage in a cellular system with a full complement of antioxidant enzymes and repair systems. Cultured RPE cells loaded with lipofuscin granules and exposed to “blue” light (400–550 nm) at an irradiance of 2.8 mW/cm2 demonstrated vacuolation and blistering of the cell membrane, a time-dependent loss of cells, loss of lysosomal stability, a two-fold increase in the lipid peroxidation endproducts, malondialdehyde and 4-hydroxynonemal [18] and an increase in oxidised membrane proteins (Fig. 2). Early changes in RPE dysfunction (usually within 3 h exposure to blue light) are associated with a decrease in lysosomal enzyme activity, a reduction in antioxidant status [68], changes in gene expression and nuclear DNA damage.
The phototoxic effects of lipofuscin on cell viability and lysosomal integrity [18]. Lipofuscin-fed cells (+) and cells lacking lipofuscin (−) were A exposed to “blue” light (390–550 nm) or B exposed to “amber” light (550–800 nm) or maintained in the dark for up to 48 h. The loss of cell viability is confirmed by the photomicrographs, which show C cell death following exposure of lipofuscin-fed cells to blue light for 48 h and D lipofuscin-fed cells appearing normal after exposure to amber light or being maintained in the dark for 48 h. Fluorescent micrographs of acridine orange-stained lipofuscin-fed cells demonstrated a loss of lysosomal integrity in cells exposed to blue light (E) but a normal lysosome distribution and appearance in cells exposed to amber light (F). Magnification ×240
Thus there is clear evidence that lipofuscin has the potential to damage RPE cells and to increase oxidative stress as the number of lipofuscin granules increase throughout life. It is also likely that lipofuscin will be at its most damaging in regions of hyperfluorescent RPE cells as seen in some forms of AMD. However, while lipofuscin is likely to contribute to the ageing process and pathology in the RPE-Bruch’s membrane complex it is unlikely to be the sole cause with a variety of other environmental insults and genetic susceptibilities making a contribution.
How important is A2E?
A2E is one of the emissive molecules in the chloroform soluble component of lipofuscin responsible for its golden yellow fluorescence. Since the chloroform soluble fraction represents only a small portion of the lipofuscin granule with the majority being in the chloroform insoluble fraction (greater than 65% in lipofuscin from individuals older than 50 years of age [60]), A2E itself is only a minor constituent of lipofuscin. A2E contained in the chloroform soluble fraction of lipofuscin [68] has only a minor contribution to the absorption of blue light [55], and it is so also in the whole lipofuscin granules [32]. The majority of photoexcited A2E (above 96% in alcohol) returns to the ground state via non-radiative relaxation [40]. Even though A2E has a low quantum yield of fluorescence [40], it can significantly contribute to lipofuscin fluorescence by serving as an energy acceptor from other blue-light-absorbing molecules of lipofuscin and therefore increasing the number of excited A2E molecules [32].
Furthermore A2E is only weakly photoreactive due to inefficient intersystem crossing and quantum yield of singlet oxygen photosensitisation, which is substantially lower than that determined for the hydrophobic components of lipofuscin [15, 26, 40, 55, 56]. The weak photoreactivity of A2E in comparison to lipofuscin has also been confirmed in cell culture experiments. Exposure of these cells to blue light resulted in a significant loss of cell viability by 72 h which was not observed in A2E-loaded cells maintained in the dark [64]. A comparison in phototoxicity between lipofuscin granules and their endogenous A2E equivalent demonstrates that A2E was at least 2 orders of magnitude less photoreactive than lipofuscin, further confirming its weak photoreactivity [68].
Despite its relatively weak photoreactivity compared to lipofuscin, studies have clearly demonstrated that A2E can induce cellular damage and RPE dysfunction in cell culture [73, 77]. A2E-loaded cells exposed to blue light undergo apoptosis executed by a proteolytic caspase cascade involving caspase-3 [72, 73]. Not surprisingly for a photoreactive system, A2E mediates its action via the generation of ROS [74] which have the ability to cause DNA damage [76], possibly through the formation of A2E epoxides [75].
Given the weak photoreactivity of A2E and the fact that A2E has lysosomotropic properties [21], studies have examined the effect of A2E on lysosomal activity. Exogenous A2E has been shown to localise predominantly to the RPE lysosomes, causing an increase in lysosomal pH [64] and exerting an inhibitory effect on protein and glycosaminoglycan catabolic pathways [36]. This effect is likely to be mediated by the ability of A2E to modify the properties of biomembranes and, in the case of the lysosome, may be detrimental to the proton pump [66]. Furthermore, the sensitivity of different cellular membranes is, in decreasing order, mitochondrial > lysosomal > Golgi / endoplasmic reticulum, with the plasma membrane being insensitive [66]. The contribution of A2E to lipofuscin toxicity is unclear and likely to be minimal due to its weak photoreactivity and relatively low concentration in lipofuscin granules. In fact studies in our laboratory (Boulton, unpublished) suggest that A2E cannot be released from lipofuscin granules under physiological or pathological conditions. Release can only be achieved after solvent extraction. Therefore, it seems likely that lipofuscin acts as a sink for A2E, and once A2E is incorporated into lipofuscin any adverse effect of A2E is negated. Thus RPE dysfunction caused by A2E is likely to originate prior to A2E being incorporated into the lipofuscin granule, either indirectly through modification of outer segments or through incorporation of A2E into cellular membranes.
Melanosomes and the RPE
In the eye melanogenesis occurs first in the RPE, with immature melanosomes visible as early as 7 weeks of gestation in man. Between the 8th and the 14th gestational week melanosomes at all stages of maturation can be observed. Production ceases within the next few weeks as the cells attain their full compliment of melanosomes [8]. Maturation of these granules combined with polymerisation of melanin continues until approximately 2 years of age in human RPE cells. Thereafter, the literature is equivocal over whether melanogenesis is significant in the adult RPE. Numerous studies support the concept of melanin production (albeit at a very slow rate) throughout life and melanogenesis can occur in pathological conditions such as proliferative vitreoretinopathy [1]. However, it appears that in the main melanosomes are contained within the RPE throughout life (Fig. 1) and that such granules will be exposed to a variety of environmental and metabolic insults.
Age-related changes in melanosomes include disorientation within the RPE [34], a decline in number after the age of 40 years [24, 81], an increase in melanosome complexes with lysosomes and/or lipofuscin [24], and loss of melanin resulting in the transition of melanin particles with a high extinction coefficient to weakly absorbing aggregates containing less melanin per unit area; these changes manifest as the fading of eye colour with age [62]. In addition to the morphological features, the photophysical characteristics of melanosomes also change with age; absorption increases at the shorter wavelengths, and there is a decrease in the blue and a shift towards the red in fluorescence spectra [7], which may result in diminished antioxidant potential and a reduced ability to bind divalent cations [62]. It appears, therefore, that melanosomes undergo significant age-related changes, possibly as a result of oxidative damage [37, 63]. Recent studies have reported that aged human melanosomes are highly photoreactive and can result in RPE dysfunction, while young melanosomes appear to confer photoprotection [19, 27, 59].
Is there an association between lipofuscin and retinal degeneration?
There is considerable circumstantial evidence to link lipofuscin with a variety of retinal degenerations, in particular AMD. First, pigment granules are observed in early small drusen [30]; drusen always precede AMD. Second, the highest density of lipofuscin is located in the perimacular region where there is the highest density of rod photoreceptor cells [48]. It is interesting to note that there is a loss of rods in this region as a function of age and in age-related maculopathy [17]. Third, high levels of lipofuscin appear to precede RPE cell death associated with geographic atrophy [35, 43]. Fourth, A2E, a component of lipofuscin, has been shown to up-regulate VEGF expression in cells exposed to blue light below the treshold for cell death (Janet Sparrow, Columbia University, personal communication); VEGF is associated with sub-retinal neovascularisation.
Increased lipofuscin accumulation is also associated with Leber’s amaurosis, Best’s disease and Stargardt’s disease. In Stargardt’s, there is an abnormality in the abcr gene that encodes an ATP-binding cassette transporter which leads to a build-up of A2E within the RPE [50].
While there is a clear association between lipofuscin and a variety of retinal degenerations, it remains to be proven whether such accumulation is cause or consequence of retinal dysfunction.
Are RPE cells suitable for transplantation?
Both fresh and cultured RPE cells have been successfully transplanted into the sub-retinal space of animal models and AMD patients. While some success has been observed in animal models with recovery of vision [28, 44], results have been limited in humans with either a halt in progression or 1–2 lines of improvement [3, 6]. The poor outcomes are due to many factors: source of RPE (fresh or cultured), age of donor, type of delivery (suspension or cell sheets), status of host (normally late-stage disease). The influence of melanosomes and lipofuscin on phototoxicity will detract from the normal functioning of the RPE and will not provide the ideal constituents for transplanted RPE cells from aged donors. If young melanosomes confer protection to RPE cells and aged RPE melanosomes appear to be detrimental, it is the former that ideally should be present in transplanted RPE cells. However, for fresh cells the donors tend to be elderly, while in culture cells lose their pigment, which can reduce the phototoxic potential of aged melanosomes but which will fail to confer the protection provided by young melanosomes.
From the findings presented above, the choice of autologous RPE cells from aged donors, while overcoming immune rejection, will provide a senescent, dysfunctional RPE phenotype which will be unlikely to have a major impact on recovering vision in compromised eyes. A young or rejuvenated cell would seem the best option, but many issues will need to be addressed to ensure a beneficial outcome following RPE transplantation.
Can aged RPE cells be rejuvenated?
The disposable soma theory of ageing proposes that the soma is programmed to ensure multicellular organism survival through development, maturity and production of new progeny. Thereafter, the organism is no longer required, survival is not a prerequisite and tissues begin to degenerate. The retinal/RPE complex is no exception to this theory, with age-related changes and retinal dysfunction appearing around the age of 50 years. With this in mind, many RPE cells from aged individuals may have suffered both genetically programmed and environmentally induced ageing. Rejuvenation of aged RPE cells to improve transplantation outcome will present a number of challenges [e.g. ex vivo gene therapy to promote the “younger” RPE phenotype, up-regulation of depressed enzyme systems, removal of senescent changes in RPE cells (lipofuscin, AGEs) and the potential for increased survival in a potentially hostile host retina].
Conclusions
In conclusion, transplantation of fresh RPE cells from elderly donors imposes a risk of introducing senescent cells which, in addition to accumulated damage, will contain photoreactive constituents—lipofuscin and modified melanosomes. While some rejuvenation of cells can take place in culture, and both types of pigment granules can be “diluted” by cell division in culture before transplantation, it remains to be determined whether the presence of pigment granules and other insults in the initial cells does not irreversibly affect the DNA. Given the limitations of fresh and cultured cells there is a desperate need for a genetically engineered RPE cell that meets all the requirements of a young healthy RPE cell if RPE transplantation is to be truly successful and restore vision.
References
Abe T, Durlu Y, Tamai M (1996) The properties of retinal pigment epithelial cells in proliferative vitreoretinopathy compared with cultured retinal pigment epithelial cells. Exp Eye Res 63:201–210
Acland GM, Aguirre GD, Ray J, Zhang Q, Aleman TS, Cideciyan AV, Pearce-Kelling SE, Anand V, Zeng Y, Maguire AM, Jacobson SG, Hauswirth WW, Bennett J (2001) Gene therapy restores vision in a canine model of childhood blindness. Nat Genet 28:92–95
Algvere P, Gouras P, Dafgard Kopp E (1999) Long-term outcome of RPE allografts in non-immunosuppressed patients with AMD. Eur J Ophthalmol 9:217–230
Beatty S, Koh H-H, Henson D, Boulton M (2000) The role of oxidative stress in the pathogenesis of age-related macular degeneration. Surv Ophthalmol 45:115–134
Ben-Shabat S, Parish CA, Hashimoto M, Liu J, Nakanishi K, Sparrow JR (2001) Fluorescent pigments of the retinal pigment epithelium and age-related macular degeneration. Bioorg Med Chem Lett 11:1533–1540
Binder S, Stolba U, Krebs I, Kellner L, Jahn C, Feichtinger H, Povelka M, Frohner U, Kruger A, Hilgers RD, Krugluger W (2002) Transplantation of autologous retinal pigment epithelium in eyes with foveal neovascularization resulting from age-related macular degeneration: a pilot study. Am J Ophthalmol 133:215–225
Boulton M (1991) Ageing of the retinal pigment epithelium. In: Osborne N, Chader G, (eds) Progress in retinal research. Pergamon, Oxford, pp 125–151
Boulton M (1998) The role of melanin in the RPE. In: Marmor M, Wolfensberger T, (eds) The retinal pigment epithelium. Oxford University Press, Oxford, pp 68–85
Boulton M (2004) The importance of maintaining the RPE phenotype in retinal transplantation. In: Binder S (ed) The macula. Springer, Vienna New York (in press)
Boulton M, Dayhaw-Barker P (2001) The role of the retinal pigment epithelium: topographical variation and ageing changes. Eye 15:384–389
Boulton M, Dontsov A, Jarvis-Evans J, Ostrovsky M, Svistunenko D (1993) Lipofuscin is a photoinducible free radical generator. Photochem Photobiol B: Biol 19:201–204
Boulton M, Różanowska M, Różanowski B (2001) Retinal photodamage. J Photochem Photobiol B 64:144–161
Brizee KR, Ordy JM (1981) Cellular features, regional accommodation, and prospects of modification of age pigments in mammals. In: Sohal RS (ed) Age pigments. Elsevier/North Holland, Amsterdam, pp 101–154
Cai J, Nelson K, Wu M, Sternberg P, Jones D (2000) Oxidative damage and protection of the RPE. Prog Ret Res 19:205–221
Cantrell A, McGarvey DJ, Roberts J, Sarna T, Truscott TG (2001) Photochemical studies of A2-E. Photochem Photobiol B: Biol 64:162–165
Clancy CMR, Krogmeier JR, et al (2000) Atomic force microscopy and near-field scanning optical microscopy measurements of single human retinal lipofuscin granules. J Phys Chem B 104:12098–12101
Curcio CA, Medeiros NE, Millican CL (1996) Photoreceptor loss in age-related macular degeneration. Invest Ophthalmol Vis Sci 37:1236–1249
Davies S, Elliott MH, Floor E, Truscott TG, Zareba M, Sarna T, Shamsi FA. Boulton M (2001) Photocytotoxicity of lipofuscin in human retinal pigment epithelial cells. Free Radic Biol Med 31:256–265
Dayhaw-Barker P, Davies S, Shamsi F, Różanowska M, Rozanowski B, Boulton M (2001) The phototoxicity of aged RPE melanosomes. Invest Ophthalmol Vis Sci 42:S755
Delori FC, Goger DG, Dorey CK (2001) Age-related accumulation and spatial distribution of lipofuscin in RPE of normal subjects. Invest Ophthalmol Vis Sci 42:1855–1866
Eldred GE (1998) Lipofuscin and other lysosomal storage deposits in the retinal pigment epithelium. In: Marmor M, Wolfensberger T (eds) The retinal pigment epithelium. Oxford University Press, Oxford, pp 651–668
Eldred GE, Katz ML (1988) Fluorophores of the human retinal pigment epithelium: separation and spectral characterization. Exp Eye Res 47:71–86
Eldred GE, Lasky M (1993) Retinal age pigments generated by self-assembling lysosomotropic detergents. Nature 361:724–726
Feeney-Burns L, Hilderbrand E, Eldridge S (1984) Aging human RPE: morphometric analysis of macular, equatorial and peripheral cells. Invest Ophthalmol Vis Sci 25:195–200
Friedrichson T, Kalbach H, Buck P, van Kuijk F (1995) Vitamin E in macular and peripheral tissues of the human eye. Curr Eye Res 14:693–701
Gaillard ER, Atherton SJ, Eldred GE, Dillon J (1995) Photophysical studies on human retinal lipofuscin. Photochem Photobiol 61:448–453
Gaillard ER, Hill C, Griffiths TD (2003) UVC and visible light damage to re-pigmented RPE cells. Invest Ophthalmol Vis Sci Abstract 377
Gouras P, Kong J, Tsang SH (2002) Retinal degeneration and RPE transplantation in Rpe65(-/-) mice. Invest Ophthalmol Vis Sci 43:3307–3311
Guymer R, Bird AC (1998) Bruch’s membrane, drusen, and age-related macular degeneration. In: Marmor M, Wolfensberger T (eds) The retinal pigment epithelium. Oxford University Press, Oxford, pp 693–705
Hageman GS, Luthert PJ, Victor Chong NH, Johnson L, Anderson DH, Mullins RF (2001) An integrated hypothesis that considers drusen as biomarkers of immune-mediated processes at the RPE–Bruch’s membrane interface in aging and age-related macular degeneration. Prog Ret Eye Res 20:705–732
Haralampus-Grynaviski NM, Lamb LE, Simon JD, Krogmeier JR, Dunn RC, Pawlak A, Różanowska M, Sarna T, Burke JM (2001) Probing the spatial dependence of the emission spectrum of single human retinal lipofuscin granules using near-field scanning optical microscopy. Photochem Photobiol 74:364–368
Haralampus-Grynaviski NM, Lamb LE, Clancy CM, Skumatz C, Burke JM, Sarna T, Simon JD (2003) Spectroscopic and morphological studies of human retinal lipofuscin granules. Proc Natl Acad Sci U S A 100:3179–3184
Hjelmeland L (1999) Senescence of the retinal pigmented epithelium. Invest Ophthalmol Vis Sci 40:1–2
Hogan M, Alvarado J, Weddell J (1971) Histology of the human eye. Saunders, Philadelphia
Holz FG, Bellman C, Staudt S, Schutt F, Volcker HE (2001) Fundus autofluorescence and development of geographic atrophy in age-related macular degeneration. Invest Ophthalmol Vis Sci 42:1051–1056
Holz FG, Schutt F, Kopitz J, Eldred GE, Kruse FE, Volcker HE, Cantz M (1999) Inhibition of lysosomal degradative functions in RPE cells by a retinoid component of lipofuscin. Invest Ophthalmol Vis Sci 41:2303–2308
Kayatz P, Thumann G, Luther TT, Jordan JF, Bartz-Schmidt KU, Esser PJ, Schraermeyer U (2001) Oxidation causes melanin fluorescence. Invest Ophthalmol Vis Sci 42:241–246
Korte GE, Reppucci V, Henkind P (1984) RPE destruction causes choriocapillary atrophy. Invest Ophthalmol Vis Sci 25:1135–1145
Krogmeier JR, Clancy CM, Pawlak A, Różanowska M, Sarna T, Simon JD, Dunn RC (2001) Mapping the distribution of emissive molecules in human ocular lipofuscin granules with near-field scanning optical microscopy. J Microsc 202:386–390
Lamb LE, Ye T, et al (2001) Primary photophysical properties of A2E in solution. J Phys Chem B 105:11507–11512
Lamb LE, Zareba M, Plakoudas SN, Sarna T, Simon JD (2001) Retinyl palmitate and the blue-light-induced phototoxicity of human ocular lipofuscin. Arch Biochem Biophys 393:316–320
Liles M, Newsome D, Oliver P (1991) Antioxidant enzymes in the aging human retinal pigment epithelium. Arch Ophthalmol 109:1285–1288
Lois N, Owens SL, Coco R, Hopkins J, Fitzke FW, Bird A (2002) Fundus autofluorescence in patients with age-related macular degeneration and high risk of visual loss. Am J Ophthalmol 133:341–349
Lund R, Adamson P, Sauve Y, Keegan D, Girman S, Wang S, Winton H, Kanuga N, Kwan A, Beauchene L, Zerbib A, Hetherington L, Couraud P, Coffey P, Greenwood J (2001) Subretinal transplantation of genetically modified human cell lines attenuates loss of visual function in dystrophic rats. Proc Natl Acad Sci USA 98:9942–9947
Lund RD, Kwan AS, Keegan DJ, Sauve Y, Coffey PJ, Lawrence JM (2001) Cell transplantation as a treatment for retinal disease. Prog Ret Eye Res 20:415–449
Mahaffy H, McFarlane S, Simpson D, Curry W, Stitt A (2003) Advanced glycation endproducts accumulate in RPE lysosomal compartments and induce widespread alteration in gene expression: possible role in age-related dysfunction. Invest Ophthalmol Vis Sci Abstract 2274
Marmor M, Wolfensberger T (1998) The retinal pigment epithelium. Oxford University Press, Oxford
Marshall J (1987) The ageing retina: physiology or pathology? Eye 1:282–295
Marshall J, Hussain AA, Starita A, Moore DJ, Patmore AL (1998) Aging and Bruch’s membrane. In: Marmor M, Wolfensberger T (eds) The retinal pigment epithelium. Oxford University Press, Oxford, pp 669–692
Mata NL, Weng J, Travis GH (2000) Biosynthesis of a major lipofuscin fluorophore in mice and humans with ABCR-mediated retinal and macular degeneration. Proc Natl Acad Sci U S A 20:7154–7159
Matsunaga H, Handa JT, Aotaki-Keen A, Sherwood SW, West MD, Hjelmeland LM (1999) Beta-galactosidase histochemistry and telomere loss in senescent retinal pigment epithelial cells. Invest Ophthalmol Vis Sci 40:197–202
Narfstrom K, Katz ML, Ford M, Redmond TM, Rakoczy E, Bragadottir R (2003) In vivo gene therapy in young and adult RPE65-/- dogs produces long-term visual improvement. J Hered 94:31–37
Panda-Jonas S, Jonas J, Jakobczyk-Kmija M (1996) Retinal pigment epithelial cell count distribution, and correlations in normal eyes. Am J Ophthalmol 121:181–189
Parish CA, Hashimoto M, Nakanishi K, Dillon J, Sparrow JR (1998) Isolation and one-step preparation of A2E and iso-A2E, fluorophores from human retinal pigment epithelium. Proc Natl Acad Sci U S A 95:14609–14613
Pawlak A, Różanowska M, Zareba M, Lamb LE, Simon JD, Sarna T. (2002) Action spectra for the photoconsumption of oxygen by human ocular lipofuscin and lipofuscin extracts. Arch Biochem Biophys 403:59–62
Pawlak A, Wrona M, Różanowska M, Zareba M, Lamb LE, Roberts JE, Simon JD, Sarna T (2003) Comparison of the aerobic photoreactivity of A2E with its precursor retinal. Photochem Photobiol 77:253–258
Różanowska M, Boulton M, Burke J, Korytowski W, Jarvis-Evans J, Sarna T (1995) Blue light-induced reactivity of retinal age pigment. J Biol Chem 270:18825–18830
Różanowska M, Wessels J, Boulton M, Burke J, Rodgers M, Truscott T, Sarna T (1998) Blue light-induced singlet oxygen generation by retinal lipofuscin in non-polar media. Free Radic Biol Med 24:1107–1112
Różanowska M, Korytowski W, Różanowski B, Skumatz C, Boulton M, Burke J, Sarna T (2002) Photoreactivity of aged human RPE melanosomes: a comparison with lipofuscin. Invest Ophthalmol Vis Sci 43:2088–2096
Różanowska M, Pawlak A, Różanowski B, Skumatz C, Zareba M, Boulton M, Burke JM, Sarna T, Simon J (2004) Age-related changes in the photoreactivity of retinal lipofuscin granules: role of chloroform insoluble components. Invest Ophthalmol Vis Sci Abstract 678
Sakai N, Decatur J, Nakanishi K, Eldred GE (1996) Ocular age pigment A2E: an unprecedented pyridinum bisretinoid. J Am Chem Soc 118:1559–1560
Sarna T (1992) Properties and function of the ocular melanin—a photophysical view. J Photochem Photobiol B: Biol 12:215–258
Sarna T, Burke JM, Korytowski W, Różanowska M, Skumatz CM, Zareba A, Zareba M (2003) Loss of melanin from human RPE with aging: possible role of melanin photooxidation. Exp Eye Res 76:89–98
Schutt F, Davies S, Kopitz J, Holz FG, Boulton M (2000) Photodamage to human RPE cells by A2-E, a retinoid component of lipofuscin. Invest Ophthalmol Vis Sci 41:2303–2308
Schutt F, Ueberle B, Schnölzer M, Holz FG, Kopitz J (2002) Proteome analysis of lipofuscin in human retinal pigment epithelial cells. FEBS Lett 528:217–221
Schutt F, Bergmann M, Holz FG, Kopitz J (2002) Isolation of intact lysosomes from human RPE cells and effects of A2-E on the integrity of the lysosomal and other cellular membranes. Graefes Arch Clin Exp Ophthalmol 240:983–988
Schutt F, Bergmann M, Holz FG, Kopitz J (2003) Proteins modified by malondialdehyde, 4-hydroxynonenal, or advanced glycation end products in lipofuscin of human retinal pigment epithelium. Invest Ophthalmol Vis Sci 44:3663–3668
Shamsi FA, Boulton M (2001) Inhibition of RPE lysosomal and antioxidant activity by the age pigment lipofuscin. Invest Ophthalmol Vis Sci 42:3041–3046
Simovich MJ, Miller B, Ezzeldin H, Kirkland BT, McLeod G, Fulmer C, Nathans J, Jacobson SG, Pittler SJ (2001) Four novel mutations in the RPE65 gene in patients with Leber congenital anaurosis. Hum Mutat 18:164
Smith AJ, Schlichtenbrede FC, Tschernutter M, Bainbridge JW, Thrasher AJ, Ali RR (2003) AAV-mediated gene transfer slows photoreceptor loss in the RCS rat model of retinitis pigmentosa. Mol Ther 8:188–195
Sohal RS (1981) Age pigments. Elsevier/North Holland, Amsterdam
Sparrow JR, Cai B (2001) Blue light-induced apoptosis of A2E-containing RPE: involvement of caspase-3 and protection by Bcl-2. Invest Ophthalmol Vis Sci 42:1356–1362
Sparrow JR, Nakanishi K, Parish CA (2000) The lipofuscin fluorophore A2E mediates blue light-induced damage to retinal pigmented epithelial cells. Invest Ophthalmol Vis Sci 41:1981–1989
Sparrow JR, Zhou J, Ben-Shabat S, Vollmer H, Itagal Nakanishi K (2002) Involvement of oxidative mechanisms in blue-light-induced damage to A2E-laden RPE. Invest Ophthalmol Vis Sci 43:1222–1227
Sparrow JR, Vollmer-Snarr HR, Zhou J, Jang YP, Jockusch S, Itagaki Y, Nakanishi K (2003) A2E-epoxides damage DNA in retinal pigment epithelial cells. J Biol Chem 278:18207–18213
Sparrow JR, Zhou J, Cai B (2003) DNA is a target of the photodynamic effects elicited in A2E-laden RPE by blue-light illumination. Invest Ophthalmol Vis Sci 44:2245–2251
Suter M, Reme C, Grimm C, Wenzel A, Jaattela M, Esser P, Kociok N, Leist M, Richter C (2000) Age-related macular degeneration. The lipofusion component N-retinyl-N-retinylidene ethanolamine detaches proapoptotic proteins from mitochondria and induces apoptosis in mammalian retinal pigment epithelial cells. J Biol Chem 275:39625–39630
Thompson DA, McHenry CL, Li Y, Richards JE, Othman MI, Schwinger E, Vollrath D, Jacobson SG, Gal A (2002) Retinal dystrophy due to paternal isodisomy for chromosome 1 or chromosome 2, with homoallelism for mutations in RPE65 or MERTK, respectively. Am J Hum Genet 70:224–229
Wang Q, Chen Q, Zhao K, Wang L, Wang L, Traboulsi E (2001) Update on the molecular genetics of retinitis pigmentosa. Ophthalmic Genet 22:133–154
Wassell J, Davies S, Bardsley W, Boulton M (1999) Photoreactivity of the retinal age pigment lipofuscin. J Biol Chem 274:23828–23832
Weiter J, Delori F, Wing G, Fitch K (1986) Retinal pigment epithelial lipofuscin and melanin and choroidal melanin in human eyes. Invest Ophthalmol Vis Sci 27:145–152
Wing G, Blanchard G, Weiter J (1978) The topography and age relationship of lipofuscin concentration in the retinal pigment epithelium. Invest Ophthalmol Vis Sci 17:601–607
Winkler BS, Boulton M, Gottsch JD, Sternberg P (1999) Oxidative damage and age-related macular degeneration. Mol Vis 5:32
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Boulton, M., Różanowska, M. & Wess, T. Ageing of the retinal pigment epithelium: implications for transplantation. Graefe's Arch Clin Exp Ophthalmol 242, 76–84 (2004). https://doi.org/10.1007/s00417-003-0812-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-003-0812-8