Abstract
Stroke, a global disease with a high disability rate, has limited options for functional rehabilitation and results in an adverse impact on patients’ lives. In recent years, mesenchymal stem cells (MSCs) have become a new focus of treatment owing to their potential for neuroregeneration. MSCs have demonstrated therapeutic efficacy capable of cell migration, angiogenesis, immunomodulation, neuroprotection and neural circuit reconstruction. The paracrine action of MSCs can also exert neurotrophic effects and improve the functional recovery. This review shows the transplantation protocol for MSCs, discusses the potential therapeutic mechanisms, and summarizes clinical trials on MSCs for treating ischemic stroke. The current proofs show that MSC therapy for ischemic stroke is safe and feasible. The timing and optimal dose of MSC administration are the main challenges in its clinical use. Although still under research, MSC therapy has the potential to be a new therapeutic approach for neurological recovery from ischemic stroke in the future.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Stroke is one of the three major diseases causing the highest lethality and disability rate globally [1]. Current management for acute ischemic stroke consists of intravenous thrombolysis and endovascular recanalization [2]. However, given the short therapeutic window, many patients failed to receive the necessary treatment and developed lifelong disabilities [3]. Current treatments have rarely been effective in neurogenesis and functional recovery during the chronic phase, resulting in an adverse impact on patients’ lives and socioeconomic conditions [4].
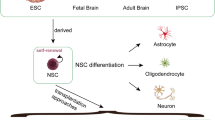
Therefore, neuroregenerative approaches are being developed to facilitate the repair of damaged neural networks and reduce the risk of disability from ischemic stroke [5]. Advances in regenerative medicine indicated the possibility of tissue repair and functional improvement. Stem cell therapy is a promising therapeutic strategy for ischemic stroke, owing to the stem cells’ capacity of self-renewal, homing, and multi-lineage differentiation [6]. The stem cells used for this purpose include mesenchymal stem cells (MSCs), neural stem cells (NSCs), embryonic stem cells (ESCs) and induced pluripotent stem cells (iPSCs) [7].
In this review, we focus on MSCs. MSCs are defined as cells that can self-renew and develop the characteristics of mesenchymal tissues [8]. MSCs can be obtained from the bone marrow, muscle, dental pulp, adipose tissue, or umbilical cord [9,10,11,12,13]. The ability of orientable differentiation makes MSCs an ideal cell source for nerve regeneration [14]. Meanwhile, sufficient evidence has shown that MSCs promote recovery through angiogenesis, secretion of neurotrophic factors, inhibition of apoptosis and modulation of the immune system [15,16,17,18,19,20]. MSCs administration can help reconstruct function area [21], promote synaptogenesis and stimulate nerve regeneration [22]. In clinical research, the potential tumorigenic risks limit the utility of ESCs and iPSCs [23,24,25]. The unique immunomodulatory effect of MSCs can modulate inflammatory response caused by ischemic stroke, thereby reducing brain tissue damage. These factors make MSCs the focus of stem cell studies. Here, we review the research progress on MSC therapy, especially the therapeutic mechanisms in functional recovery. We also discuss the experimental evidence and clinical trials on the use of MSCs in ischemic stroke patients and prospect the future direction of MSC research.
The Mesenchymal and Tissue Stem Cell Committee of the International Society for Cellular Therapy (ISCT) defined the minimum criteria for MSCs as follows:
-
(i)
Isolated cells showing adherence to plastic in culture.
-
(ii)
Cells expressing mesenchymal or endothelial surface markers (CD73, CD90, and CD105) and negative for hematopoietic markers (CD11b, CD14, CD19, CD34, CD45, CD79α and HLA-DR).
-
(iii)
Ability to differentiate into osteoblasts, adipocytes, and chondroblasts in vitro [26,27,28].
Recent studies identify several new markers, such as SSEA1/4, CD44, CD146, and CD271. And CD271 is considered one of the most specific MSC markers [29,30,31,32]. These surface markers are related to the stemness within MSCs and contribute to the identification of MSCs in vivo. The identification by markers can improve the purity of MSCs than isolation based on traditional plastic adherence. MSCs differentiate into neural cells by expressing neuronal markers (NeuN and MAP-2) and migrate to brain lesions [33,34,35,36,37]. Meanwhile, MSCs can also play a regenerative role by secreting a variety of paracrine factors, such as vascular endothelial growth factor (VEGF), hepatocyte growth factor (HGF), brain-derived neurotrophic factor (BDNF), glial-derived neurotrophic factor (GDNF), and fibroblast growth factor (FGF) [38,39,40,41,42]. In preclinical studies, MSC transplantation has been found to be a safe and recommended recovery strategy for treatment.
Principles of mesenchymal stem cell (MSC) therapy
Generally, MSC transplantation is carried out by intracranial and intravascular methods. The main intracranial methods are stereotactic injection and intraventricular injection [43]. Stereotactic injection helps transport the MSCs to the infarction area directly. This method requires high precision to reach the target area [44]. Intraventricular injection distributes MSCs to a wider range of cerebral regions. The therapeutic efficacy in such cases depends on the number of cells [45].
Intravascular methods include intravenous and intra-arterial injection. The level of inflammatory cytokines increases after infarction attracting MSCs to the center of the ischemic area [46]. MSCs by intravenous injection are difficult to pass through pulmonary vessels due to the large volume, and few cells are able to reach the target area [47]. Intra-arterial injection through the internal carotid artery can deliver MSCs in a short time. However, intra-arterial injection may cause occlusion of the end arteries in the brain [48, 49].
Intracranial transplantation may cause mechanical damage, but it is better at transporting the cells to the target sites than other methods. Intravascular transplantation requires more cells and is better for large infarctions than intracranial method. In clinical applications, intravascular delivery is easier to perform than the intracranial method.
Intranasal injection, a new transplantation method, needs further research [50]. Cells can be transported from the nasal mucosa to the injured area by blood circulation [51]. Intranasal injection, as a noninvasive method, could be a prospective method of cell transplantation [52, 53].
Recent studies have shown that extracellular vesicles (EVs) derived from MSCs have therapeutic effects comparable to those of direct cell transplantation. EVs can reduce neuroinflammation, enhance angiogenesis, and increase neurogenesis. Compared to MSCs transplantation, EVs show unique advantages in stroke treatment, such as no first-pass effect, ability to pass the blood–brain barrier (BBB), and ability to reduce the risk of cell-related infarction. EVs therapy is a new therapeutic approach for neuroprotection in acute ischemic stroke [54,55,56].
Although there are clinical trials of MSCs in ischemic stroke treatment, there is still no consensus on the optimal dose in cell therapy. Currently, the recommended dose for clinical trials is 1–2 × 106/kg of weight [57, 58]. Furthermore, it is still questionable whether the MSCs dose should be personalized according to the infarct size.
The different phases of pathological ischemic process offer different targets for MSC therapy. In the early phase, MSC delivery may reduce the inflammatory response, regulate the dynamic environment against toxicity, and decrease the injury in the peri-infarct area. At 2–3 weeks after ischemia, late cell transplantation can modulate the reparative processes in favor of angiogenesis and neurogenesis [59]. Clinically, MSCs administration has been found to be safe in stroke populations in early-phase trials [60, 61]. However, the effectiveness of MSC therapy in subacute and chronic ischemic stroke has yet to be validated. Therefore, the optimal timing of administration needs further evaluation.
Therapeutic mechanisms of MSC therapy
MSCs can differentiate into neurons and glial cells to repair structural damage [62, 63]. However, MSCs lack the voltage-gated ion channels expressed in functional nerve cells for generating action potentials [64]. Thus, direct cellular replacement may not be the primary method for achieving a therapeutic effect. Currently, many studies show that the paracrine actions of MSCs exert neurotrophic effects, improving the functional benefit directly or indirectly. Paracrine signaling may be the main condition for the recovery process [65,66,67].
Reparative mechanisms of MSCs mainly include cell migration, angiogenesis, immunomodulation, neuroprotection and neural circuit reconstruction.
Cell migration
Most of the current MSC trials use intravascular delivery methods. Therefore, MSCs need to cross the BBB to migrate towards the target regions. The BBB is composed of endothelial cells (ECs), basal layer, pericytes, and astrocytes. Tight junctions between ECs and membrane transport proteins make the BBB a selective barrier. Influenced by ischemic stroke, the junctions between ECs disrupt, leading to paracellular permeability elevation. MSCs engage with ECs by multistage homing cascade, including selectin-mediated rolling, integrin-associated adhesion, and chemokine-directed migration. MSCs release CXCL-11 and bind with CXCR-3 on ECs. This can activate ERK1/2 signaling and open the tight junctions [68]. Moreover, activating PI3K/Akt and inhibiting Rho/ROCK signaling lead to the disassembling of tight junctions and opening of paracellular pathways for MSCs transmigration [69]. The interactions between vascular EC adhesion molecule (VCAM)-1 and very late antigen (VLA)-4 also regulate the passage across the barrier [70]. However, some studies have found that the transmigration action of MSCs is independent of VCAM-1 [71]. The mechanism and molecular pathway in the passage of MSCs across the BBB need further clarification.
MSCs migration is usually achieved by responding to different chemotactic signals. In the infarct zone, microglia and astrocytes secrete chemokines such as SDF-1 in the surrounding environment. The expression of CXCR-4, as the physiological receptor for SDF-1, increases on the surface of MSCs [72]. The interaction between SDF-1 and CXCR-4 mediates cell migration [73]. Recent studies show that CXCR-7 may exert a synergistic effect with CXCR-4 in promoting MSC migration [74]. Valproate can promote MSCs migration by inducing CXCR-4 overexpression, and lithium can upregulate MMP-9 to enhance chemotaxis [75]. MSCs are mainly transported to the ischemic penumbra and subventricular zone in response to chemotactic signals, including those of MCP-1 and MIP-1a [76].
In addition, c-Met signaling induces MSC migration to the damaged areas [77]. Recent studies have shown that overexpression of neurogenin-1 can increase the homing ability of MSCs and enhance the engraftment efficiency in the ischemic area [78].
Angiogenesis
MSC transplantation can improve revascularization in the ischemic zone, resulting in recovery effects. MSC infusion can enhance microvascular regeneration [79]. Reformation of neurovascular units can be beneficial to neuronal regeneration and functional recovery in ischemic regions [80,81,82,83,84]. The trophic factors secreted by MSCs such as VEGF, induce the formation of immature vessels [81, 85,86,87]. Other growth factors secreted by MSCs, including BDNF, IGF-1, GDNF, bFGF, Ang-1, and Ang-2, probably contribute to enhanced angiogenesis in the ischemic core and border zone [88,89,90,91,92,93,94]. However, VEGF may induce the increased vascular permeability in the BBB causing cerebral edema [95]. In contrast, the anti-edemic effect of Ang-1may counteract vessel leakage [96]. Meanwhile, Ang-1 can specifically combine with Tie-2 on vascular endothelial cells, phosphorylate Tie-2, and promote the maturation and stability of new blood vessels [89]. Ang-1 plays an important role in neovascularization.
In preclinical models, MSCs were found to differentiate into endothelial cells and activate endothelial progenitor cells that can enhance the proangiogenic effect. Notch signaling pathway [97, 98] and mitochondrial nanotube transportation [99] are considered the key mechanisms of MSC-induced angiogenesis. Angiogenesis increases the blood flow in the brain tissue, which is beneficial for endogenous neurogenesis. MicroRNAs (miRNAs) are also important for angiogenesis. Recent trials showed that miRNA-210 was associated with angiogenesis promotion [100].
Immunomodulatory effects
In comparison with other types of stem cells, MSCs have immunomodulatory effects that mediate immune responses. Inflammatory cell proliferation reduced after coculture with MSCs in vitro [101]. Leukocytes gather in the infarct zone after stroke. The strong inflammatory response leads to secondary nerve cells apoptosis [102]. MSC transplantation can modulate the immune response by inhibiting cytotoxic T cells and promoting regulatory T cells [103,104,105]. MSCs suppress maturation and secretion of B-cell antibodies. MSCs reduce the cytotoxicity of immune cells and antibody secretion [106, 107].
In addition to immune cells modulation, MSCs promote immunosuppression by regulating the expression of cytokines. TGF-β secreted by MSCs can block the upregulation of MCP-1 and the infiltration of CD68 + cells [108]. Meanwhile, MSCs attenuate astrocyte reactivity by increasing the expression of IL-10 and decreasing the expression of TNF-α [109, 110]. Inhibition of TNF-α has been shown to limit monocyte maturation, resulting in the lack of antigen-presenting functions in dendritic cells [111]. Although several growth factors and cytokines are involved in MSC-mediated immunomodulatory including IL-6 [112], IL-23/IL-17 [113], MMP2, TGF-β1, HGF, NGF, pGe2, TLR-4, and RAGE [114, 115], the underlying mechanisms have yet to be validated.
Neuroprotection
MSCs can also exert neuroprotective effects, inhibit apoptosis and promote endogenous repair. MSCs increase the expression of neurotrophic factors, achieving neuroprotective effect directly and/or indirectly, such as VEGF, GDNF, BDNF, NGF, IGF-1, HGF, EGF, and bFGF [58, 92, 116, 117]. BDNF interacts with tyrosine kinase receptors promoting neuronal survival [118]. IL-10, as an anti-inflammatory cytokine, induced immune tolerance in preclinical models [119]. MSCs increase the expression of IL-10 [120], which can inhibit microglial activation, reduce inflammatory cytokine expression (IL-1β, IL-6 and TNF-α), and subsequently decrease neuronal degeneration after stroke [112].
In the acute phase of ischemic stroke, the microglia can help reduce brain damage. However, excessive microglia activation or sustained immune response can lead to apoptosis. CXC3CL1 secreted by MSCs has been found to induce the production of the neuroprotective phenotype of the microglia and suppress neurotoxic microglia activity [121]. MSCs can effectively suppress activated microglia and inhibit apoptosis. Apoptotic response to the astrocytes reduced and bFGF expression increased in rat models after MSC transplantation [122, 123]. A recent study showed that MSCs can activate miRNA-29b-3p mediated Akt-dependent anti-apoptotic cascade and inhibit apoptosis [124].
Neural circuit reconstruction
Several mechanisms are involved in MSC-mediated neural circuit reconstruction of the infarct zone and boundary area, including neurogenesis inducement [86], axonal sprout [125, 126], and synaptogenesis enhancement [127].
Endogenous neurogenesis and axonal plasticity may be the basic mechanisms by which MSCs improve the neurological function after ischemic stroke [80, 114]. Axonal sprouting increases the link between different cerebral areas, thus reconstructing neural connections. t-PA activation [125] and PAI-1 downregulation [128] in the boundary area can promote axonal formation and establishment of synaptic connections. In addition, MSCs crosslink peripheral cells, astrocytes, and endothelial cells to repair the BBB [129] and establish a microenvironment promoting neurogenesis and neural circuit recovery.
MSCs can stimulate the production of TGF-β activating the multiplication of endogenous neural stem cells located in the hippocampus and subventricular zone [130, 131]. Neuroblast migration induced by MSCs [114] enhances the survival of cortical cells in the peri-infarct zone and helps repair the neural network [126, 132]. The expression of IL-6 increases in the ischemic penumbra via the nuclear factor kappa-B signaling pathway [133]. This can activate resident stem cells and promote endogenous repair. Meanwhile, angiogenesis induced by MSCs promotes endogenous neurogenesis; miRNA-184 promotes neurogenesis after ischemic stroke [100].
Moreover, the paracrine actions of MSCs can stimulate neurogenesis. MSCs promote the expression of synaptic vesicle protein and BDNF which induce the differentiation of astrocytes and synaptogenesis directly or indirectly [134, 135]. However, the molecular mechanism of MSC-induced neural plasticity requires further research.
Preclinical trials
MSCs have the multidirectional differentiation potential, e.g., osteoblasts, chondrocytes, adipocytes and neurons [62]. The beneficial effects of MSCs include neural lineage trans-differentiation, neurogenesis, angiogenesis induction and synapse formation. Therefore, MSCs are suitable for treating ischemic stroke and preclinical studies.
Researchers found that both allogeneic and heterogenetic MSCs produced a significant recovery in middle cerebral artery occlusion (MCAO) models. In an early preclinical trial, researchers tested the therapeutic efficacy of MSCs in the MACO rat model. Approximately 21% of bone marrow-derived MSCs (BMSCs) were distributed in the MCA territory after intracarotid arterial injection. The treated rats exhibited functional improvement as compared with controls [88]. Then, the same team carried out research on the treatment of rats with ischemic stroke rats using intravenous injection of human MSCs. The researchers observed significant functional recovery in the treated rats. The expression of BDNF and NGF increased in the ischemic tissue, and the level of apoptosis reduced in the penumbral area. The proliferation of endogenous neural stem cells and the formation of new cells occurred in the subventricular area [122].
Although MSCs have the ability to cross the BBB, a limited number of cells can migrate to the ischemic boundary sites. Several studies have shown that despite a small number of MSCs migrating to the injury site, the trophic factors and cytokines secreted by MSCs have a therapeutic effect [136].
Paracrine secretion
After MSCs injection, cells migrate to the infarct zone and differentiate into neuronal, glial, and endothelial cells to enhance neuroplasticity. However, the paracrine action of MSCs can also induce the regenerative process by increasing the level of growth factors or receptors, such as VEGF, NGF, EPOR, TROY, RAGE, and neuropilin. Meanwhile, cytokines or chemokines (IL-13, MMP2, and MIP) are modified after MSC administration [137].
In the ischemic hemisphere, β1-integrin could promote angiogenesis and increase blood supply to the local cortex. In addition, SDF-1, GDNF, and BDNF expression increased significantly after MSC therapy [138]. IGF-1 plays an important role in neurological recovery. The expressions of IGF-1 and IGF-1 receptor (IGF-1R) in MSC-treated rats significantly increased in the ischemic brain tissue. IGF-1 is associated with neurogenesis due to MSC transplantation [139].
Genetic modification with exogeneous cytokines can enhance the roles of MSCs. In a preclinical trial, MSCs transfected with the Ang-1 gene led to significantly more functional recovery than uninfected MSCs in MCAO rat models [89]. To enhance the recovery effect, the research team transfected MSCs with the Ang-1 and VEGF genes. The Ang-VEGF-MSCs showed the greatest structural–functional recovery in all groups [140]. Exogenous gene transinfection has been suggested to enhance the therapeutic effect of MSCs. Combined gene transfection in MSC therapy represents a new strategy.
Angiogenesis and neurogenesis
The multidirectional differentiation potential of MSCs causes their trans-differentiation into endothelial cells and neural cells. Angiogenesis and neurogenesis constitute the mechanisms of structural repair. In rats with ischemic stroke, MSC transplantation may produce functional recovery by inducing angiogenesis [80]. The expression of endogenous growth factors increased after MSCs transplantation and induced the formation of small vessels in the infarct boundary, including VEGF, EGF, and bFGF [90, 141]. The infarct volumes of MCAO rats reduced after MSC therapy. MSCs induced the proliferation of subventricular zone cells, which may promote endogenous neurogenesis [92]. It significantly reduced the mortality of the rats and facilitated behavioral and neurological recovery. MSCs promote the reconstruction of the neurovascular units and recovery of brain function [142].
Immunomodulation and neuroprotective effect
The immunomodulation and neuroprotective effects of MSCs are the basic mechanisms that reduce secondary brain injury after ischemic stroke. MSCs suppress the activation of microglia and delay neuronal death [143]. Besides suppressing microglial activation, MSCs induced an increase in IL-10 expression and reduction in neuronal apoptosis in the peri-infarct area of MACO rats [144]. MSCs can inhibit the production of CD4+ and CD8+ T cells and promote the production of regulatory T cells [145]. Meanwhile, MSCs can significantly inhibit expressions of Bax, caspase-3, IL-18, TLR-4, and PAI-1 [114, 146].
Heterogeneity
MSCs from different sources share morphological, regenerative, and immunomodulatory characteristics [147]. However, these cells show variations in other features such as paracrine functions and neurogenic potential. Adipose-derived MSCs (AD-MSCs) secrete more VEGF, HGF, and TGF-β [148, 149] than BMSCs. Meanwhile, the conditioned media of AD-MSCs have higher levels of MMP3 and MMP-9 and enhance angiogenesis [150].
Clinical trials
Safety is the primary concern in stem cells application in clinic. Currently, almost all studies showed no cases of acute toxicity, thromboembolism, abnormal cell growths, neurological deterioration, or death after MSC transplantation. Transient febrile reaction was the only side effect related to cell administration [151, 152]. MSCs are easy to obtain and proliferate. The immunomodulatory characteristics and potential of nerve regeneration make MSCs the ideal candidate for clinical therapy.
Safety and efficacy
In a study of autologous BMSCs, 30 patients with ischemic stroke were divided into an MSC group (n = 5) and control group (n = 25). The patients in the MSC group received an intravenous infusion of 1.0 × 108 cells. During the 12-month follow-up period, the Barthel index and modified Rankin Scale (mRS) score of the MSC group improved consistently as compared to the scores of the control group [153]. This shows the safety of MSC transplantation and improvement in patients’ neurological condition. Another clinical trial evaluated the safety and feasibility in stereotactic implantation of autologous BMSCs. This study recruited five patients with cerebral infarction. No adverse events occurred in this study, and improvements were observed in the neurological recovery [154]. However, due to the limited sample size of the two trials, it is difficult to obtain conclusive results.
In a recent randomized controlled trial (RCT), 16 of 31 patients accepted autologous MSCs therapy. During the 2-year follow-up, the MSCs group showed significant improvements in motor National Institute of Health stroke scale (NIHSS), motor Fugl-Meyer score, and task-related fMRI activity in the primary motor cortex. The result shows that MSC treatment for subacute ischemic stroke was safe and feasible. MSCs improved functional recovery via sensorimotor neuroplasticity [155].
Long-term efficacy
Some researchers explores whether MSCs can maintain their therapeutic effect over time. In a 5-year follow-up clinical trial, researchers randomly allocated 85 patients to the MSC group and control group. The MSC group received intravenous autologous MSCs. They were followed for 5 years; finally 52 patients were examined. Compared with the control group, in the MSC group, mRS score decreased and the number of patients with mRS score 0–3 increased significantly. The clinical recovery may be associated with SDF-1 serum levels and subventricular region involvement of the lateral ventricle [156].
Efficacy of different transplantation routes
One study examined the effectiveness of different administration methods used in MSC transplantation. The researchers found that intra-arterial infusion led to higher biological distribution than intravenous delivery. This study also assessed the safety and efficacy of catheter delivery. They recruited four patients with stroke (ischemic stroke three; hemorrhagic stroke (1). The patients received a single dose of 2 × 107 umbilical cord MSCs. The researchers infused the cells to the M1 segment of the MCA via catheterization. Muscle strength and mRS score improved in the two ischemic stroke patients. However, these two patients experienced ischemic stroke again at 3 and 6 months after MSCs infusion [157], probably due to the short-term effects of stem cell therapy.
Different sources of MSCs for cell therapy
Commonly, BMSCs are selected for trials, but the procurement is difficult and the cell number is limited. Compared to BMSCs, AD-MSCs can be obtained by relatively safe methods such as liposuction procedures. This makes AD-MSCs an attractive resource for clinical applications [158].
Intravenous administration of allogeneic AD-MSCs could be a safe therapy for early stages of acute stroke. A clinical trial researching the safety and efficacy of allogeneic MSC transplantation recruited 20 patients with acute ischemic stroke. The enrolled patients were equally divided into two cohorts treated with allogeneic AD-MSCs or placebo. They received a single dose intravenously within the first 2 weeks after symptom onset. During the 2-year follow-up period, the researchers recorded the mRS score, NIHSS score, infarct size, and levels of biochemical markers for efficacy analysis. The result showed that allogeneic AD-MSCs are beneficial for cerebral recovery [159].
Currently, autologous MSCs are the preferred option because of the low risk of rejection. Due to the long culture time, autologous MSCs can hardly be used in the acute phase of ischemic stroke treatment. Allogeneic MSCs could break the limitation. Because MSCs lack HLA-II antigens, allogeneic MSCs could hardly cause an immunologic response, thus eliminating the risk of rejection [160, 161].
In another clinical trial, 15 patients in three groups were treated with allogeneic MSCs. The three doses of 0.5, 1.0, and 1.5 × 106/kg were found to be safe. Then, 21 patients, as an expanded safety cohort, received allogeneic MSCs at a dose of 1.5 × 106/kg. The Barthel score and number of patients achieving excellent functional outcomes in this cohort increased significantly over the 12-months of follow-up. The result supported the fact that transplantation of allogeneic MSCs was safe and effective. Allogeneic MSCs are promising candidates for MSC therapy in acute ischemic stroke [162].
Genetic technology and preconditioning
Gene transfection-induced MSCs may have high therapeutic value. A phase I/IIa study explored the clinical outcomes of modified BMSC transplantation. SB623 cells, as allogenic modified BMSCs, are transinfected with a plasmid coding for the intracellular domain of Notch-1. The study enrolled 18 patients with chronic stroke and divided then into three groups that received stereotactic single doses of 2.5, 5.0, and 10 × 106 SB623 cells. In all, 16 were followed up for 12 months. Comparing to the baseline, significant improvements were observed in the European Stroke Scale (ESS), NIHSS, and Fugl-Meyer score. Thus, SB623 cells were found to be safe and effective for clinical use [163].
Preconditioning with stroke serum before transplantation can activate MSCs into a primed state and reinforce resistance to ischemic microenvironments. The cytoprotective effect of preconditioning enhances the migration and survival of MSCs [164]. In an autologous MSC transplantation study, 12 patients received intravenous auto serum-expanded MSCs 36–133 days after stroke. In the first week of infusion, the median daily rate of NIHSS change increased. The MRI results showed that the mean ischemic area decreased to over 20%. Although the study did not rule out the placebo effects and the effect of natural recovery on treatment outcomes, the result suggested the role of relevant preconditioning in improving the efficacy of MSCs [165].
These studies support that MSC transplantation is safe and effective in cerebral recovery after ischemic stroke. In future, determining the timing of administration and optimum infusion dose could be the predominant challenge in MSC therapy [93, 117, 166].
Conclusion
Mature neurons cannot proliferate and differentiate. Neurological impairment caused by ischemic stroke has been considered difficult to treat. Currently, the capacity of MSCs in neuronal differentiation and functional recovery in ischemic therapy has generated immense interest. The general mechanisms by which MSCs induce improvement include cell replacement, angiogenesis, paracrine actions, neuroprotective effect, immunomodulation and neural circuit reconstruction. However, the molecular pathways of neurogenesis and angiogenesis need further examination.
In recent years, AD-MSCs have become popular in stem cell therapy due to the extensive tissue sources, short culture time and strong ability of differentiation into neural-like cells. Future studies need to focus on the safety and efficacy of MSCs and monitor adverse events before widely using them in clinical practice. Furthermore, large clinical trials are still limited, the optimal timing and doses for MSC transplantation are not yet known. In summary, MSC therapy provides a new therapeutic approach and research direction in the neurological recovery of stroke patients.
References
Zhang H, Lu M, Zhang X, Kuai Y, Mei Y, Tan Q, Zhong K, Sun X, Tan W (2019) Isosteviol sodium protects against ischemic stroke by modulating microglia/macrophage polarization via disruption of GAS5/miR-146a-5p sponge. Sci Rep 9(1):12221. https://doi.org/10.1038/s41598-019-48759-0
Lee WT, Tai SH, Lin YW, Wu TS, Lee EJ (2018) YC-1 reduces inflammatory responses by inhibiting nuclear factor-κB translocation in mice subjected to transient focal cerebral ischemia. Mole Med Rep 18(2):2043–2051. https://doi.org/10.3892/mmr.2018.9178
Chen B, Tao J, Lin Y, Lin R, Liu W, Chen L (2015) Electro-acupuncture exerts beneficial effects against cerebral ischemia and promotes the proliferation of neural progenitor cells in the cortical peri-infarct area through the Wnt/β-catenin signaling pathway. Int J Mol Med 36(5):1215–1222. https://doi.org/10.3892/ijmm.2015.2334
Sung PH, Chen KH, Lin HS, Chu CH, Chiang JY, Yip HK (2019) The correlation between severity of neurological impairment and left ventricular function in patients after acute ischemic stroke. J Clin Med 8:2. https://doi.org/10.3390/jcm8020190
Sahota P, Savitz SI (2011) Investigational therapies for ischemic stroke: neuroprotection and neurorecovery. J Am Soc Exper Neuro Thera 8(3):434–451. https://doi.org/10.1007/s13311-011-0040-6
Lin BL, Zhang JZ, Lu LJ, Mao JJ, Cao MH, Mao XH, Zhang F, Duan XH, Zheng CS, Zhang LM, Shen J (2017) Superparamagnetic iron oxide nanoparticles-complexed cationic amylose for in vivo magnetic resonance imaging tracking of transplanted stem cells in stroke. Nanomaterials (Basel, Switzerland) 7:5. https://doi.org/10.3390/nano7050107
Zhang F, Duan X, Lu L, Zhang X, Zhong X, Mao J, Chen M, Shen J (2016) In Vivo targeted MR imaging of endogenous neural stem cells in ischemic stroke. Molecules (Basel, Switzerland) 21:9. https://doi.org/10.3390/molecules21091143
da Silva ML, Malta TM, de Deus Wagatsuma VM, Palma PV, Araújo AG, Ribeiro Malmegrim KC, Morato de Oliveira F, Panepucci RA, Silva WA, Kashima Haddad S, Covas DT (2015) Cultured human adipose tissue pericytes and mesenchymal stromal cells display a very similar gene expression profile. Stem Cells Dev 24(23):2822–2840. https://doi.org/10.1089/scd.2015.0153
Zou Z, Zhang Y, Hao L, Wang F, Liu D, Su Y, Sun H (2010) More insight into mesenchymal stem cells and their effects inside the body. Exp Opinion Biol Ther 10(2):215–230. https://doi.org/10.1517/14712590903456011
Honmou O, Onodera R, Sasaki M, Waxman SG, Kocsis JD (2012) Mesenchymal stem cells: therapeutic outlook for stroke. Trends Mole Med 18(5):292–297. https://doi.org/10.1016/j.molmed.2012.02.003
Sanberg PR, Eve DJ, Metcalf C, Borlongan CV (2012) Advantages and challenges of alternative sources of adult-derived stem cells for brain repair in stroke. Prog Brain Res 201:99–117. https://doi.org/10.1016/b978-0-444-59544-7.00006-8
Wan Safwani WKZ, Choi JR, Yong KW, Ting I, Mat Adenan NA, Pingguan-Murphy B (2017) Hypoxia enhances the viability, growth and chondrogenic potential of cryopreserved human adipose-derived stem cells. Cryobiology 75:91–99. https://doi.org/10.1016/j.cryobiol.2017.01.006
Choi JR, Yong KW, Choi JY (2018) Effects of mechanical loading on human mesenchymal stem cells for cartilage tissue engineering. J Cell Physiol 233(3):1913–1928. https://doi.org/10.1002/jcp.26018
Cai F, Hong X, Tang X, Liu NC, Wang F, Zhu L, Xie XH, Xie ZY, Wu XT (2019) ASIC1a activation induces calcium-dependent apoptosis of BMSCs under conditions that mimic the acidic microenvironment of the degenerated intervertebral disc. Biosci Rep 39:11. https://doi.org/10.1042/bsr20192708
Yong KW, Choi JR, Mohammadi M, Mitha AP, Sanati-Nezhad A, Sen A (2018) Mesenchymal stem cell therapy for ischemic tissues. Stem Cells internat 2:8179075. https://doi.org/10.1155/2018/8179075
Ryu B, Sekine H, Homma J, Kobayashi T, Kobayashi E, Kawamata T, Shimizu T (2019) Allogeneic adipose-derived mesenchymal stem cell sheet that produces neurological improvement with angiogenesis and neurogenesis in a rat stroke model. J Neurosurg 132(2):442–455. https://doi.org/10.3171/2018.11.jns182331
Chen KH, Lin KC, Wallace CG, Li YC, Shao PL, Chiang JY, Sung PH, Yip HK (2019) Human induced pluripotent stem cell-derived mesenchymal stem cell therapy effectively reduced brain infarct volume and preserved neurological function in rat after acute intracranial hemorrhage. Am J Trans Res 11(9):6232–6248
Chrostek MR, Fellows EG, Crane AT, Grande AW, Low WC (2019) Efficacy of stem cell-based therapies for stroke. Brain Res 1722:146362. https://doi.org/10.1016/j.brainres.2019.146362
Dabrowska S, Andrzejewska A, Strzemecki D, Muraca M, Janowski M, Lukomska B (2019) Human bone marrow mesenchymal stem cell-derived extracellular vesicles attenuate neuroinflammation evoked by focal brain injury in rats. J Neuroinflam 16(1):216. https://doi.org/10.1186/s12974-019-1602-5
Cunningham CJ, Wong R, Barrington J, Tamburrano S, Pinteaux E, Allan SM (2020) Systemic conditioned medium treatment from interleukin-1 primed mesenchymal stem cells promotes recovery after stroke. Stem cell Res Ther 11(1):32. https://doi.org/10.1186/s13287-020-1560-y
Pirzad Jahromi G, Shabanzadeh Pirsaraei A, Sadr SS, Kaka G, Jafari M, Seidi S, Charish J (2015) Multipotent bone marrow stromal cell therapy promotes endogenous cell proliferation following ischemic stroke. Clin Exp Pharmacol Physiol 42(11):1158–1167. https://doi.org/10.1111/1440-1681.12466
Lalu MM, Montroy J, Dowlatshahi D, Hutton B, Juneau P, Wesch N, Zhang Y (2020) From the lab to patients: a systematic review and meta-analysis of mesenchymal stem cell therapy for stroke. Trans Stroke Res 11(3):345–364. https://doi.org/10.1007/s12975-019-00736-5
Tao H, Chen X, Wei A, Song X, Wang W, Liang L, Zhao Q, Han Z, Han Z, Wang X, Li Z (2018) Comparison of teratoma formation between embryonic stem cells and parthenogenetic embryonic stem cells by molecular imaging. Stem Cells Internat 18:7906531. https://doi.org/10.1155/2018/7906531
Deng J, Zhang Y, Xie Y, Zhang L, Tang P (2018) Cell Transplantation for spinal cord injury: tumorigenicity of induced pluripotent stem cell-derived neural stem/progenitor cells. Stem Cells Internat 1:5653787. https://doi.org/10.1155/2018/5653787
Yang X, Wang R, Wang X, Cai G, Qian Y, Feng S, Tan F, Chen K, Tang K, Huang X, Jing N, Qiao Y (2018) TGFβ signaling hyperactivation-induced tumorigenicity during the derivation of neural progenitors from mouse ESCs. J Mole Cell Biol 10(3):216–228. https://doi.org/10.1093/jmcb/mjy013
Horwitz EM, Le Blanc K, Dominici M, Mueller I, Slaper-Cortenbach I, Marini FC, Deans RJ, Krause DS, Keating A (2005) Clarification of the nomenclature for MSC: the international society for cellular therapy position statement. Cytotherapy 7(5):393–395. https://doi.org/10.1080/14653240500319234
Dominici M, Le Blanc K, Mueller I, Slaper-Cortenbach I, Marini F, Krause D, Deans R, Keating A, Dj P, Horwitz E (2006) Minimal criteria for defining multipotent mesenchymal stromal cells. The international society for cellular therapy position statement. Cytotherapy 8(4):315–317. https://doi.org/10.1080/14653240600855905
Luo L, Hu DH, Yin JQ, Xu RX (2018) Molecular mechanisms of transdifferentiation of adipose-derived stem cells into neural cells: current status and perspectives. Stem Cells Internat 8:5630802. https://doi.org/10.1155/2018/5630802
Lv FJ, Tuan RS, Cheung KM, Leung VY (2014) Concise review: the surface markers and identity of human mesenchymal stem cells. Stem Cells (Dayton, Ohio) 32(6):1408–1419. https://doi.org/10.1002/stem.1681
Camilleri ET, Gustafson MP, Dudakovic A, Riester SM, Garces CG, Paradise CR, Takai H, Karperien M, Cool S, Sampen HJ, Larson AN, Qu W, Smith J, Dietz AB, van Wijnen AJ (2016) Identification and validation of multiple cell surface markers of clinical-grade adipose-derived mesenchymal stromal cells as novel release criteria for good manufacturing practice-compliant production. Stem Cell Res Ther 7(1):107. https://doi.org/10.1186/s13287-016-0370-8
Pachón-Peña G, Donnelly C, Ruiz-Cañada C, Katz A, Fernández-Veledo S, Vendrell J, Sackstein R (2017) A Glycovariant of Human CD44 is characteristically expressed on human mesenchymal stem cells. Stem Cells (Dayton, Ohio) 35(4):1080–1092. https://doi.org/10.1002/stem.2549
Liu GB, Pan YM, Liu YS, Hu JH, Zhang XD, Zhang DW, Wang Y, Feng YK, Yu JB, Cheng YX (2020) Ghrelin promotes neural differentiation of adipose tissue-derived mesenchymal stem cell via AKT/mTOR and β-catenin signaling pathways. Kaohsi J Med Sci. https://doi.org/10.1002/kjm2.12188
Ji W, Álvarez Z, Edelbrock AN, Sato K, Stupp SI (2018) Bioactive Nanofibers induce neural transdifferentiation of human bone marrow mesenchymal stem cells. ACS Appl Mater int 10(48):41046–41055. https://doi.org/10.1021/acsami.8b13653
Zainal Abidin S, Fam SZ, Chong CE, Abdullah S, Cheah PS, Nordin N, Ling KH (2019) miR-3099 promotes neurogenesis and inhibits astrogliogenesis during murine neural development. Gene 697:201–212. https://doi.org/10.1016/j.gene.2019.02.014
Lam PK, Wang KKW, Chin DWC, Tong CSW, Wang Y, Lo KKY, Lai PBS, Ma H, Zheng VZY, Poon WS, Wong GKC (2020) Topically applied adipose-derived mesenchymal stem cell treatment in experimental focal cerebral ischemia. J Clin Neurosci Soc Aust 71:226–233. https://doi.org/10.1016/j.jocn.2019.08.051
Hazeri Y, Irani S, Zandi M, Pezeshki-Modaress M (2020) Polyvinyl alcohol/sulfated alginate nanofibers induced the neuronal differentiation of human bone marrow stem cells. Int J Biol Macromol 147:946–953. https://doi.org/10.1016/j.ijbiomac.2019.10.061
Jedari B, Rahmani A, Naderi M, Nadri S (2020) MicroRNA-7 promotes neural differentiation of trabecular meshwork mesenchymal stem cell on nanofibrous scaffold. J Cell Biochem 121(4):2818–2827. https://doi.org/10.1002/jcb.29513
Kwon HM, Hur SM, Park KY, Kim CK, Kim YM, Kim HS, Shin HC, Won MH, Ha KS, Kwon YG, Lee DH, Kim YM (2014) Multiple paracrine factors secreted by mesenchymal stem cells contribute to angiogenesis. Vasc Pharmacol 63(1):19–28. https://doi.org/10.1016/j.vph.2014.06.004
He B, Yao Q, Liang Z, Lin J, Xie Y, Li S, Wu G, Yang Z, Xu P (2016) The dose of intravenously transplanted bone marrow stromal cells determines the therapeutic effect on vascular remodeling in a rat model of ischemic stroke. Cell Transplant 25(12):2173–2185. https://doi.org/10.3727/096368916x692627
Hofer HR, Tuan RS (2016) Secreted trophic factors of mesenchymal stem cells support neurovascular and musculoskeletal therapies. Stem Cell Res Ther 7(1):131. https://doi.org/10.1186/s13287-016-0394-0
Khan S, Villalobos MA, Choron RL, Chang S, Brown SA, Carpenter JP, Tulenko TN, Zhang P (2017) Fibroblast growth factor and vascular endothelial growth factor play a critical role in endotheliogenesis from human adipose-derived stem cells. J Vasc Surg 65(5):1483–1492. https://doi.org/10.1016/j.jvs.2016.04.034
Li X, Huang M, Zhao R, Zhao C, Liu Y, Zou H, Chen L, Guan Y, Zhang YA (2018) Intravenously delivered allogeneic mesenchymal stem cells bidirectionally regulate inflammation and induce neurotrophic effects in distal middle cerebral artery occlusion rats within the first 7 days after stroke. Cell Physiol Biochem Internat J Exp Cell Physiol Biochem Pharmacol 46(5):1951–1970. https://doi.org/10.1159/000489384
Toyoshima A, Yasuhara T, Date I (2017) Mesenchymal stem cell therapy for ischemic stroke. Acta Med Okayama 71(4):263–268. https://doi.org/10.18926/amo/55302
Jin K, Sun Y, Xie L, Mao XO, Childs J, Peel A, Logvinova A, Banwait S, Greenberg DA (2005) Comparison of ischemia-directed migration of neural precursor cells after intrastriatal, intraventricular, or intravenous transplantation in the rat. Neurobiol Dis 18(2):366–374. https://doi.org/10.1016/j.nbd.2004.10.010
Wang L, Lin Z, Shao B, Zhuge Q, Jin K (2013) Therapeutic applications of bone marrow-derived stem cells in ischemic stroke. Neurol Res 35(5):470–478. https://doi.org/10.1179/1743132813y.0000000210
Ahmadian Kia N, Bahrami AR, Ebrahimi M, Matin MM, Neshati Z, Almohaddesin MR, Aghdami N, Bidkhori HR (2011) Comparative analysis of chemokine receptor's expression in mesenchymal stem cells derived from human bone marrow and adipose tissue. J Mole Neurosci MN 44(3):178–185. https://doi.org/10.1007/s12031-010-9446-6
Mello TG, Rosado-de-Castro PH, Campos RMP, Vasques JF, Rangel-Junior WS, Mattos RSAR, Puig-Pijuan T, Foerster BU, Gutfilen B, Souza SAL, Boltze J, Paiva FF, Mendez-Otero R, Pimentel-Coelho PM (2020) Intravenous human umbilical cord-derived mesenchymal stromal cell administration in models of moderate and severe intracerebral hemorrhage. Stem Cells Dev 29(9):586–598. https://doi.org/10.1089/scd.2019.0176
Du S, Guan J, Mao G, Liu Y, Ma S, Bao X, Gao J, Feng M, Li G, Ma W, Yang Y, Zhao RC, Wang R (2014) Intra-arterial delivery of human bone marrow mesenchymal stem cells is a safe and effective way to treat cerebral ischemia in rats. Cell Transplant 1:S73–82. https://doi.org/10.3727/096368914x685023
Fukuda Y, Horie N, Satoh K, Yamaguchi S, Morofuji Y, Hiu T, Izumo T, Hayashi K, Nishida N, Nagata I (2015) Intra-arterial transplantation of low-dose stem cells provides functional recovery without adverse effects after stroke. Cell Mol Neurobiol 35(3):399–406. https://doi.org/10.1007/s10571-014-0135-9
Chau MJ, Deveau TC, Gu X, Kim YS, Xu Y, Yu SP, Wei L (2018) Delayed and repeated intranasal delivery of bone marrow stromal cells increases regeneration and functional recovery after ischemic stroke in mice. BMC Neurosci 19(1):20. https://doi.org/10.1186/s12868-018-0418-z
Matsushita T, Kibayashi T, Katayama T, Yamashita Y, Suzuki S, Kawamata J, Honmou O, Minami M, Shimohama S (2011) Mesenchymal stem cells transmigrate across brain microvascular endothelial cell monolayers through transiently formed inter-endothelial gaps. Neurosci Lett 502(1):41–45. https://doi.org/10.1016/j.neulet.2011.07.021
Li YH, Feng L, Zhang GX, Ma CG (2015) Intranasal delivery of stem cells as therapy for central nervous system disease. Exp Mol Pathol 98(2):145–151. https://doi.org/10.1016/j.yexmp.2015.01.016
Rodríguez-Frutos B, Otero-Ortega L, Gutiérrez-Fernández M, Fuentes B, Ramos-Cejudo J, Díez-Tejedor E (2016) Stem cell therapy and administration routes after stroke. Trans Stroke Res 7(5):378–387. https://doi.org/10.1007/s12975-016-0482-6
Shi Y, Shi H, Nomi A, Lei-Lei Z, Zhang B, Qian H (2019) Mesenchymal stem cell-derived extracellular vesicles: a new impetus of promoting angiogenesis in tissue regeneration. Cytotherapy 21(5):497–508. https://doi.org/10.1016/j.jcyt.2018.11.012
Bang OY, Kim EH (2019) Mesenchymal stem cell-derived extracellular vesicle therapy for stroke: challenges and progress. Front Neurol 10:211. https://doi.org/10.3389/fneur.2019.00211
Otero-Ortega L, Laso-García F, Frutos MCG, Diekhorst L, Martínez-Arroyo A, Alonso-López E, García-Bermejo ML, Rodríguez-Serrano M, Arrúe-Gonzalo M, Díez-Tejedor E, Fuentes B, Gutiérrez-Fernández M (2020) Low dose of extracellular vesicles identified that promote recovery after ischemic stroke. Stem Cell Res Ther 11(1):70. https://doi.org/10.1186/s13287-020-01601-1
Bhasin A, Srivastava MV, Mohanty S, Bhatia R, Kumaran SS, Bose S (2013) Stem cell therapy: a clinical trial of stroke. Clin Neurol Neurosurg 115(7):1003–1008. https://doi.org/10.1016/j.clineuro.2012.10.015
Li G, Yu F, Lei T, Gao H, Li P, Sun Y, Huang H, Mu Q (2016) Bone marrow mesenchymal stem cell therapy in ischemic stroke: mechanisms of action and treatment optimization strategies. Neural Regen Res 11(6):1015–1024. https://doi.org/10.4103/1673-5374.184506
Muir KW (2017) Clinical trial design for stem cell therapies in stroke: what have we learned? Neurochem Int 106:108–113. https://doi.org/10.1016/j.neuint.2016.09.011
Kim SJ, Moon GJ, Chang WH, Kim YH, Bang OY (2013) Intravenous transplantation of mesenchymal stem cells preconditioned with early phase stroke serum: current evidence and study protocol for a randomized trial. Trials 14:317. https://doi.org/10.1186/1745-6215-14-317
Oshita J, Okazaki T, Mitsuhara T, Imura T, Nakagawa K, Otsuka T, Kurose T, Tamura T, Abiko M, Takeda M, Kawahara Y, Yuge L, Kurisu K (2020) Early transplantation of human cranial bone-derived mesenchymal stem cells enhances functional recovery in ischemic stroke model rats. Neurol Med Chir 60(2):83–93. https://doi.org/10.2176/nmc.oa.2019-0186
Azad TD, Veeravagu A, Steinberg GK (2016) Neurorestoration after stroke. Neurosurg Focus 40(5):E2. https://doi.org/10.3171/2016.2.focus15637
Park J, Lee N, Lee J, Choe EK, Kim MK, Lee J, Byun MS, Chon MW, Kim SW, Lee CJ, Kim JH, Kwon JS, Chang MS (2017) Small molecule-based lineage switch of human adipose-derived stem cells into neural stem cells and functional GABAergic neurons. Sci Rep 7(1):10166. https://doi.org/10.1038/s41598-017-10394-y
Hofstetter CP, Schwarz EJ, Hess D, Widenfalk J, El Manira A, Prockop DJ, Olson L (2002) Marrow stromal cells form guiding strands in the injured spinal cord and promote recovery. Proc Natl Acad Sci USA 99(4):2199–2204. https://doi.org/10.1073/pnas.042678299
Hsuan YC, Lin CH, Chang CP, Lin MT (2016) Mesenchymal stem cell-based treatments for stroke, neural trauma, and heat stroke. Brain Behav 6(10):e00526. https://doi.org/10.1002/brb3.526
Gunawardena TNA, Rahman MT, Abdullah BJJ, Abu Kasim NH (2019) Conditioned media derived from mesenchymal stem cell cultures: the next generation for regenerative medicine. J Iss Eng Regen Med 13(4):569–586. https://doi.org/10.1002/term.2806
Cunningham CJ, Redondo-Castro E, Allan SM (2018) The therapeutic potential of the mesenchymal stem cell secretome in ischaemic stroke. J blood Flow Metab Internat Soc Cerebral Blood Flow Metab 38(8):1276–1292. https://doi.org/10.1177/0271678x18776802
Feng Y, Yu HM, Shang DS, Fang WG, He ZY, Chen YH (2014) The involvement of CXCL11 in bone marrow-derived mesenchymal stem cell migration through human brain microvascular endothelial cells. Neurochem Res 39(4):700–706. https://doi.org/10.1007/s11064-014-1257-7
Geranmayeh MH, Nourazarian A, Avci ÇB, Rahbarghazi R, Farhoudi M (2017) Stem cells as a promising tool for the restoration of brain neurovascular unit and angiogenic orientation. Mol Neurobiol 54(10):7689–7705. https://doi.org/10.1007/s12035-016-0286-4
Steingen C, Brenig F, Baumgartner L, Schmidt J, Schmidt A, Bloch W (2008) Characterization of key mechanisms in transmigration and invasion of mesenchymal stem cells. J Mol Cell Cardiol 44(6):1072–1084. https://doi.org/10.1016/j.yjmcc.2008.03.010
Heiskanen A, Hirvonen T, Salo H, Impola U, Olonen A, Laitinen A, Tiitinen S, Natunen S, Aitio O, Miller-Podraza H, Wuhrer M, Deelder AM, Natunen J, Laine J, Lehenkari P, Saarinen J, Satomaa T, Valmu L (2009) Glycomics of bone marrow-derived mesenchymal stem cells can be used to evaluate their cellular differentiation stage. Glycoconj J 26(3):367–384. https://doi.org/10.1007/s10719-008-9217-6
Delcroix GJ, Schiller PC, Benoit JP, Montero-Menei CN (2010) Adult cell therapy for brain neuronal damages and the role of tissue engineering. Biomaterials 31(8):2105–2120. https://doi.org/10.1016/j.biomaterials.2009.11.084
Cai A, Qiu R, Li L, Zheng D, Dong Y, Yu D, Huang Y, Rao S, Zhou Y, Mai W (2013) Atorvastatin treatment of rats with ischemia-reperfusion injury improves adipose-derived mesenchymal stem cell migration and survival via the SDF-1α/CXCR-4 axis. PLoS ONE 8(12):e79100. https://doi.org/10.1371/journal.pone.0079100
Wang Y, Fu W, Zhang S, He X, Liu Z, Gao D, Xu T (2014) CXCR-7 receptor promotes SDF-1α-induced migration of bone marrow mesenchymal stem cells in the transient cerebral ischemia/reperfusion rat hippocampus. Brain Res 1575:78–86. https://doi.org/10.1016/j.brainres.2014.05.035
Tsai L-K, Wang Z, Munasinghe J, Leng Y, Leeds P, Chuang D-M (2011) Mesenchymal stem cells primed with valproate and lithium robustly migrate to infarcted regions and facilitate recovery in a stroke model. Stroke 42(10):2932–2939. https://doi.org/10.1161/STROKEAHA.110.612788
Wang L, Li Y, Chen X, Chen J, Gautam SC, Xu Y, Chopp M (2002) MCP-1, MIP-1, IL-8 and ischemic cerebral tissue enhance human bone marrow stromal cell migration in interface culture. Hematology (Amsterdam, Netherlands) 7(2):113–117. https://doi.org/10.1080/10245330290028588
Bang OY, Moon GJ, Kim DH, Lee JH, Kim S, Son JP, Cho YH, Chang WH, Kim YH (2017) Stroke induces mesenchymal stem cell migration to infarcted brain areas Via CXCR4 and C-Met signaling. Trans Stroke Res. https://doi.org/10.1007/s12975-017-0538-2
Kim GH, Subash M, Yoon JS, Jo D, Han J, Hong JM, Kim SS, Suh-Kim H (2020) Neurogenin-1 overexpression increases the therapeutic effects of mesenchymal stem cells through enhanced engraftment in an ischemic rat brain. Internat J Stem Cells 13(1):127–141. https://doi.org/10.15283/ijsc19111
Mitkari B, Nitzsche F, Kerkelä E, Kuptsova K, Huttunen J, Nystedt J, Korhonen M, Jolkkonen J (2014) Human bone marrow mesenchymal stem/stromal cells produce efficient localization in the brain and enhanced angiogenesis after intra-arterial delivery in rats with cerebral ischemia, but this is not translated to behavioral recovery. Behav Brain Res 259:50–59. https://doi.org/10.1016/j.bbr.2013.10.030
Bao X, Feng M, Wei J, Han Q, Zhao H, Li G, Zhu Z, Xing H, An Y, Qin C, Zhao RC, Wang R (2011) Transplantation of Flk-1+ human bone marrow-derived mesenchymal stem cells promotes angiogenesis and neurogenesis after cerebral ischemia in rats. Eur J Neurosci 34(1):87–98. https://doi.org/10.1111/j.1460-9568.2011.07733.x
Gutiérrez-Fernández M, Rodríguez-Frutos B, Ramos-Cejudo J, Teresa Vallejo-Cremades M, Fuentes B, Cerdán S, Díez-Tejedor E (2013) Effects of intravenous administration of allogenic bone marrow- and adipose tissue-derived mesenchymal stem cells on functional recovery and brain repair markers in experimental ischemic stroke. Stem Cell Res Thera 4(1):11. https://doi.org/10.1186/scrt159
Hao L, Zou Z, Tian H, Zhang Y, Zhou H, Liu L (2014) Stem cell-based therapies for ischemic stroke. Biomed Res Int 2014:468748. https://doi.org/10.1155/2014/468748
Zong X, Wu S, Li F, Lv L, Han D, Zhao N, Yan X, Hu S, Xu T (2017) Transplantation of VEGF-mediated bone marrow mesenchymal stem cells promotes functional improvement in a rat acute cerebral infarction model. Brain Res 1676:9–18. https://doi.org/10.1016/j.brainres.2017.08.006
Ferguson SW, Wang J, Lee CJ, Liu M, Neelamegham S, Canty JM, Nguyen J (2018) The microRNA regulatory landscape of MSC-derived exosomes: a systems view. Sci Rep 8(1):1419. https://doi.org/10.1038/s41598-018-19581-x
Deng YB, Ye WB, Hu ZZ, Yan Y, Wang Y, Takon BF, Zhou GQ, Zhou YF (2010) Intravenously administered BMSCs reduce neuronal apoptosis and promote neuronal proliferation through the release of VEGF after stroke in rats. Neurol Res 32(2):148–156. https://doi.org/10.1179/174313209x414434
Bao X, Wei J, Feng M, Lu S, Li G, Dou W, Ma W, Ma S, An Y, Qin C, Zhao RC, Wang R (2011) Transplantation of human bone marrow-derived mesenchymal stem cells promotes behavioral recovery and endogenous neurogenesis after cerebral ischemia in rats. Brain Res 1367:103–113. https://doi.org/10.1016/j.brainres.2010.10.063
Zhang Y, Ma L, Su Y, Su L, Lan X, Wu D, Han S, Li J, Kvederis L, Corey S, Borlongan CV, Ji X (2019) Hypoxia conditioning enhances neuroprotective effects of aged human bone marrow mesenchymal stem cell-derived conditioned medium against cerebral ischemia in vitro. Brain Res 1725:146432. https://doi.org/10.1016/j.brainres.2019.146432
Li Y, Chen J, Wang L, Lu M, Chopp M (2001) Treatment of stroke in rat with intracarotid administration of marrow stromal cells. Neurology 56(12):1666–1672. https://doi.org/10.1212/wnl.56.12.1666
Onda T, Honmou O, Harada K, Houkin K, Hamada H, Kocsis JD (2008) Therapeutic benefits by human mesenchymal stem cells (hMSCs) and Ang-1 gene-modified hMSCs after cerebral ischemia. J Blood Flow Metab Internat Soc Cerebral 28(2):329–340. https://doi.org/10.1038/sj.jcbfm.9600527
Wakabayashi K, Nagai A, Sheikh AM, Shiota Y, Narantuya D, Watanabe T, Masuda J, Kobayashi S, Kim SU, Yamaguchi S (2010) Transplantation of human mesenchymal stem cells promotes functional improvement and increased expression of neurotrophic factors in a rat focal cerebral ischemia model. J Neurosci Res 88(5):1017–1025. https://doi.org/10.1002/jnr.22279
Zacharek A, Shehadah A, Chen J, Cui X, Roberts C, Lu M, Chopp M (2010) Comparison of bone marrow stromal cells derived from stroke and normal rats for stroke treatment. Stroke 41(3):524–530. https://doi.org/10.1161/strokeaha.109.568881
Lin YC, Ko TL, Shih YH, Lin MY, Fu TW, Hsiao HS, Hsu JY, Fu YS (2011) Human umbilical mesenchymal stem cells promote recovery after ischemic stroke. Stroke 42(7):2045–2053. https://doi.org/10.1161/strokeaha.110.603621
Toyoshima A, Yasuhara T, Kameda M, Morimoto J, Takeuchi H, Wang F, Sasaki T, Sasada S, Shinko A, Wakamori T, Okazaki M, Kondo A, Agari T, Borlongan CV, Date I (2015) Intra-Arterial transplantation of allogeneic mesenchymal stem cells mounts neuroprotective effects in a transient ischemic stroke model in rats: analyses of therapeutic time window and its mechanisms. PLoS ONE 10(6):e0127302. https://doi.org/10.1371/journal.pone.0127302
Ghazavi H, Hoseini SJ, Ebrahimzadeh-Bideskan A, Mashkani B, Mehri S, Ghorbani A, Sadri K, Mahdipour E, Ghasemi F, Forouzanfar F, Hoseini A, Pasdar AR, Sadeghnia HR, Ghayour-Mobarhan M (2017) Fibroblast Growth Factor Type 1 (FGF1)-overexpressed adipose-derived mesenchaymal stem cells (AD-MSC) induce neuroprotection and functional recovery in a rat stroke model. Stem Cell Rev Rep 13(5):670–685. https://doi.org/10.1007/s12015-017-9755-z
Zhang ZG, Zhang L, Jiang Q, Zhang R, Davies K, Powers C, Nv B, Chopp M (2000) VEGF enhances angiogenesis and promotes blood-brain barrier leakage in the ischemic brain. J Clin Invest 106(7):829–838. https://doi.org/10.1172/jci9369
Thurston G, Suri C, Smith K, McClain J, Sato TN, Yancopoulos GD, McDonald DM (1999) Leakage-resistant blood vessels in mice transgenically overexpressing angiopoietin-1. Science (New York, NY) 286(5449):2511–2514. https://doi.org/10.1126/science.286.5449.2511
Guo F, Lv S, Lou Y, Tu W, Liao W, Wang Y, Deng Z (2012) Bone marrow stromal cells enhance the angiogenesis in ischaemic cortex after stroke: involvement of notch signalling. Cell Biol Int 36(11):997–1004. https://doi.org/10.1042/cbi20110596
Zhu J, Liu Q, Jiang Y, Wu L, Xu G, Liu X (2015) Enhanced angiogenesis promoted by human umbilical mesenchymal stem cell transplantation in stroked mouse is Notch1 signaling associated. Neuroscience 290:288–299. https://doi.org/10.1016/j.neuroscience.2015.01.038
Liu K, Ji K, Guo L, Wei Wu, Huixia Lu, Shan P, Yan C (2014) Mesenchymal stem cells rescue injured endothelial cells in an in vitro ischemia-reperfusion model via tunneling nanotube like structure-mediated mitochondrial transfer. Microvasc Res 92:10–18. https://doi.org/10.1016/j.mvr.2014.01.008
Moon GJ, Sung JH, Kim DH, Kim EH, Cho YH, Son JP, Cha JM, Bang OY (2019) Application of Mesenchymal Stem Cell-Derived Extracellular Vesicles for Stroke: Biodistribution and MicroRNA Study. Trans Stroke Res 10(5):509–521. https://doi.org/10.1007/s12975-018-0668-1
Sato K, Ozaki K, Iekuni Oh, Meguro A, Hatanaka K, Nagai T, Muroi K, Ozawa K (2007) Nitric oxide plays a critical role in suppression of T-cell proliferation by mesenchymal stem cells. Blood 109(1):228–234
Iadecola C, Anrather J (2011) The immunology of stroke: from mechanisms to translation. Nat Med 17(7):796–808. https://doi.org/10.1038/nm.2399
Di Nicola M, Carlo-Stella C, Magni M, Milanesi M, Longoni PD, Matteucci P, Grisanti S, Gianni AM (2002) Human bone marrow stromal cells suppress T-lymphocyte proliferation induced by cellular or nonspecific mitogenic stimuli. Blood 99(10):3838–3843. https://doi.org/10.1182/blood.v99.10.3838
Gerdoni E, Gallo B, Casazza S, Musio S, Bonanni I, Pedemonte E, Mantegazza R, Frassoni F, Mancardi G, Pedotti R, Uccelli A (2007) Mesenchymal stem cells effectively modulate pathogenic immune response in experimental autoimmune encephalomyelitis. Ann Neurol 61(3):219–227. https://doi.org/10.1002/ana.21076
Hess DC, Wechsler LR, Clark WM, Savitz SI, Ford GA, Chiu D, Yavagal DR, Uchino K, Liebeskind DS, Auchus AP, Sen S, Sila CA, Vest JD, Mays RW (2017) Safety and efficacy of multipotent adult progenitor cells in acute ischaemic stroke (MASTERS): a randomised, double-blind, placebo-controlled, phase 2 trial. Lancet Neurol 16(5):360–368. https://doi.org/10.1016/s1474-4422(17)30046-7
Corcione A, Benvenuto F, Ferretti E, Giunti D, Cappiello V, Cazzanti F, Risso M, Gualandi F, Mancardi GL, Pistoia V, Uccelli A (2006) Human mesenchymal stem cells modulate B-cell functions. Blood 107(1):367–372. https://doi.org/10.1182/blood-2005-07-2657
Marigo I, Dazzi F (2011) The immunomodulatory properties of mesenchymal stem cells. Sem Immunopathol 33(6):593–602. https://doi.org/10.1007/s00281-011-0267-7
Yoo SW, Chang DY, Lee HS, Kim GH, Park JS, Ryu BY, Joe EH, Lee YD, Kim SS, Suh-Kim H (2013) Immune following suppression mesenchymal stem cell transplantation in the ischemic brain is mediated by TGF-β. Neurobiol Dis 58:249–257. https://doi.org/10.1016/j.nbd.2013.06.001
Liu N, Chen R, Du H, Wang J, Zhang Y, Wen J (2009) Expression of IL-10 and TNF-alpha in rats with cerebral infarction after transplantation with mesenchymal stem cells. Cell Mol Immunol 6(3):207–213. https://doi.org/10.1038/cmi.2009.28
Li J, Zhu H, Liu Y, Li Q, Lu S, Feng M, Xu Y, Huang L, Ma C, An Y, Zhao RC, Wang R, Qin C (2010) Human mesenchymal stem cell transplantation protects against cerebral ischemic injury and upregulates interleukin-10 expression in Macacafascicularis. Brain Res 1334:65–72. https://doi.org/10.1016/j.brainres.2010.03.080
Aggarwal S, Pittenger MF (2005) Human mesenchymal stem cells modulate allogeneic immune cell responses. Blood 105(4):1815–1822. https://doi.org/10.1182/blood-2004-04-1559
Zhu Y, Guan YM, Huang HL, Wang QS (2014) Human umbilical cord blood mesenchymal stem cell transplantation suppresses inflammatory responses and neuronal apoptosis during early stage of focal cerebral ischemia in rabbits. Acta Pharmacol Sin 35(5):585–591. https://doi.org/10.1038/aps.2014.9
Ma S, Zhong D, Chen H, Zheng Y, Sun Y, Luo J, Li H, Li G, Yin Y (2013) The immunomodulatory effect of bone marrow stromal cells (BMSCs) on interleukin (IL)-23/IL-17-mediated ischemic stroke in mice. J Neuroimmunol 257:28–35. https://doi.org/10.1016/j.jneuroim.2013.01.007
Leu S, Lin YC, Yuen CM, Yen CH, Kao YH, Sun CK, Yip HK (2010) Adipose-derived mesenchymal stem cells markedly attenuate brain infarct size and improve neurological function in rats. J Trans Med 8:63. https://doi.org/10.1186/1479-5876-8-63
Paul G, Anisimov SV (2013) The secretome of mesenchymal stem cells: potential implications for neuroregeneration. Biochimie 95(12):2246–2256. https://doi.org/10.1016/j.biochi.2013.07.013
Song M, Mohamad O, Xiaohuan Gu, Wei L, Shan Ping Yu (2013) Restoration of intracortical and thalamocortical circuits after transplantation of bone marrow mesenchymal stem cells into the ischemic brain of mice. Cell Transplant 22(11):2001–2015. https://doi.org/10.3727/096368912X657909
Ishizaka S, Horie N, Satoh K, Fukuda Y, Nishida N, Nagata I (2013) Intra-arterial cell transplantation provides timing-dependent cell distribution and functional recovery after stroke. Stroke 44(3):720–726. https://doi.org/10.1161/strokeaha.112.677328
Hyman C, Hofer M, Barde YA, Juhasz M, Yancopoulos GD, Squinto SP, Lindsay RM (1991) BDNF is a neurotrophic factor for dopaminergic neurons of the substantia nigra. Nature 350(6315):230–232. https://doi.org/10.1038/350230a0
Liesz A, Bauer A, Hoheisel JD, Veltkamp R (2014) Intracerebral interleukin-10 injection modulates post-ischemic neuroinflammation: an experimental microarray study. Neurosci Lett 579:18–23. https://doi.org/10.1016/j.neulet.2014.07.003
Nakajima M, Nito C, Sowa K, Suda S, Nishiyama Y, Nakamura-Takahashi A, Nitahara-Kasahara Y, Imagawa K, Hirato T, Ueda M, Kimura K, Okada T (2017) Mesenchymal stem cells overexpressing interleukin-10 promote neuroprotection in experimental acute ischemic stroke. Mole Thera Method Clin Dev 6:102–111. https://doi.org/10.1016/j.omtm.2017.06.005
Giunti D, Parodi B, Usai C, Vergani L, Casazza S, Bruzzone S, Mancardi G, Uccelli A (2012) Mesenchymal stem cells shape microglia effector functions through the release of CX3CL1. Stem Cells (Dayton, Ohio) 30(9):2044–2053. https://doi.org/10.1002/stem.1174
Li Y, Chen J, Chen XG, Wang L, Gautam SC, Xu YX, Katakowski M, Zhang LJ, Lu M, Janakiraman N, Chopp M (2002) Human marrow stromal cell therapy for stroke in rat: neurotrophins and functional recovery. Neurology 59(4):514–523. https://doi.org/10.1212/wnl.59.4.514
Jiang W, Liang G, Li X, Li Z, Gao X, Feng S, Wang X, Liu M, Liu Y (2014) Intracarotid transplantation of autologous adipose-derived mesenchymal stem cells significantly improves neurological deficits in rats after MCAo. J Mat Sci Mat Med 25(5):1357–1366. https://doi.org/10.1007/s10856-014-5157-9
Hou K, Li G, Zhao J, Xu B, Zhang Y, Yu J, Xu K (2020) Bone mesenchymal stem cell-derived exosomal microRNA-29b-3p prevents hypoxic-ischemic injury in rat brain by activating the PTEN-mediated Akt signaling pathway. J Neuroinflam 17(1):46. https://doi.org/10.1186/s12974-020-1725-8
Xin H, Li Y, Shen LH, Liu X, Wang X, Zhang J, Pourabdollah-Nejad DS, Zhang C, Zhang L, Jiang H, Zhang ZG, Chopp M (2010) Increasing tPA activity in astrocytes induced by multipotent mesenchymal stromal cells facilitate neurite outgrowth after stroke in the mouse. PLoS ONE 5(2):e9027. https://doi.org/10.1371/journal.pone.0009027
Song M, Mohamad O, Gu X, Wei L, Yu SP (2013) Restoration of intracortical and thalamocortical circuits after transplantation of bone marrow mesenchymal stem cells into the ischemic brain of mice. Cell Transplant 22(11):2001–2015. https://doi.org/10.3727/096368912x657909
Shen LH, Li Y, Chen J, Cui Y, Zhang C, Kapke A, Lu M, Savant-Bhonsale S, Chopp M (2007) One-year follow-up after bone marrow stromal cell treatment in middle-aged female rats with stroke. Stroke 38(7):2150–2156. https://doi.org/10.1161/strokeaha.106.481218
Shen LH, Xin H, Li Y, Zhang RL, Cui Y, Zhang L, Lu M, Zhang ZG, Chopp M (2011) Endogenous tissue plasminogen activator mediates bone marrow stromal cell-induced neurite remodeling after stroke in mice. Stroke 42(2):459–464. https://doi.org/10.1161/strokeaha.110.593863
Fisher M (2009) Pericyte signaling in the neurovascular unit. Stroke 40:S13–15. https://doi.org/10.1161/strokeaha.108.533117
Ming GL, Song H (2011) Adult neurogenesis in the mammalian brain: significant answers and significant questions. Neuron 70(4):687–702. https://doi.org/10.1016/j.neuron.2011.05.001
Cheng Q, Zhang Z, Zhang S, Yang H, Zhang X, Pan J, Weng L, Sha D, Zhu M, Hu X, Xu Y (2015) Human umbilical cord mesenchymal stem cells protect against ischemic brain injury in mouse by regulating peripheral immunoinflammation. Brain Res 1594:293–304. https://doi.org/10.1016/j.brainres.2014.10.065
Liu Z, Li Y, Zhang ZG, Cui X, Cui Y, Lu M, Savant-Bhonsale S, Chopp M (2010) Bone marrow stromal cells enhance inter- and intracortical axonal connections after ischemic stroke in adult rats. J Blood Flow Metab Internat Soc Cerebral Blood Flow Metab 30(7):1288–1295. https://doi.org/10.1038/jcbfm.2010.8
Walker PA, Harting MT, Jimenez F, Shah SK, Pati S, Dash PK, Cox CS (2010) Direct intrathecal implantation of mesenchymal stromal cells leads to enhanced neuroprotection via an NFkappaB-mediated increase in interleukin-6 production. Stem Cells Develop 19(6):867–876. https://doi.org/10.1089/scd.2009.0188
Xin H, Li Y, Chen X, Chopp M (2006) Bone marrow stromal cells induce BMP2/4 production in oxygen-glucose-deprived astrocytes, which promotes an astrocytic phenotype in adult subventricular progenitor cells. J Neurosci Res 83(8):1485–1493. https://doi.org/10.1002/jnr.20834
Schäbitz WR, Steigleder T, Cooper-Kuhn CM, Schwab S, Sommer C, Schneider A, Kuhn HG (2007) Intravenous brain-derived neurotrophic factor enhances poststroke sensorimotor recovery and stimulates neurogenesis. Stroke 38(7):2165–2172. https://doi.org/10.1161/strokeaha.106.477331
Zhao LR, Duan WM, Reyes M, Keene CD, Verfaillie CM, Low WC (2002) Human bone marrow stem cells exhibit neural phenotypes and ameliorate neurological deficits after grafting into the ischemic brain of rats. Exp Neurol 174(1):11–20. https://doi.org/10.1006/exnr.2001.7853
Yang M, Wei X, Li J, Heine LA, Rosenwasser R, Iacovitti L (2010) Changes in host blood factors and brain glia accompanying the functional recovery after systemic administration of bone marrow stem cells in ischemic stroke rats. Cell Transplant 19(9):1073–1084. https://doi.org/10.3727/096368910x503415
Ding D-C, Shyu W-C, Chiang M-F, Lin S-Z, Chang Y-C, Wang H-J, Ching-Yuan Su, Li H (2007) Enhancement of neuroplasticity through upregulation of beta1-integrin in human umbilical cord-derived stromal cell implanted stroke model. Neurobiol Dis 27(3):339–353
Zhang J, Li Y, Chen J, Yang M, Katakowski M, Lu M, Chopp M (2004) Expression of insulin-like growth factor 1 and receptor in ischemic rats treated with human marrow stromal cells. Brain Res 1030(1):19–27. https://doi.org/10.1016/j.brainres.2004.09.061
Toyama K, Honmou O, Harada K, Suzuki J, Houkin K, Hamada H, Kocsis JD (2009) Therapeutic benefits of angiogenetic gene-modified human mesenchymal stem cells after cerebral ischemia. Exp Neurol 216(1):47–55. https://doi.org/10.1016/j.expneurol.2008.11.010
Liew A, O'Brien T (2012) Therapeutic potential for mesenchymal stem cell transplantation in critical limb ischemia. Stem Cell Res Ther 3(4):28. https://doi.org/10.1186/scrt119
Chen J, Venkat P, Zacharek A, Chopp M (2014) Neurorestorative therapy for stroke. Front Human Neurosci 8:382. https://doi.org/10.3389/fnhum.2014.00382
Wei L, Fraser JL, Lu ZY, Hu X, Yu SP (2012) Transplantation of hypoxia preconditioned bone marrow mesenchymal stem cells enhances angiogenesis and neurogenesis after cerebral ischemia in rats. Neurobiol Dis 46(3):635–645. https://doi.org/10.1016/j.nbd.2012.03.002
Darsalia V, Mansouri S, Ortsäter H, Olverling A, Nozadze N, Kappe C, Iverfeldt K, Tracy LM, Grankvist N, Sjöholm Å, Patrone C (2012) Glucagon-like peptide-1 receptor activation reduces ischaemic brain damage following stroke in type 2 diabetic rats. Clin Sci (London, England 1979) 122(10):473–483
Nasef A, Mathieu N, Chapel A, Frick J, François S, Mazurier C, Boutarfa A, Bouchet S, Gorin NC, Thierry D, Fouillard L (2007) Immunosuppressive effects of mesenchymal stem cells: involvement of HLA-G. Transplantation 84(2):231–237. https://doi.org/10.1097/01.tp.0000267918.07906.08
Li D, Fang Y, Wang P, Shan W, Zuo Z, Xie L (2012) Autologous transplantation of adipose-derived mesenchymal stem cells attenuates cerebral ischemia and reperfusion injury through suppressing apoptosis and inducible nitric oxide synthase. Int J Mol Med 29(5):848–854. https://doi.org/10.3892/ijmm.2012.909
Paul G, Özen I, Christophersen NS, Reinbothe T, Bengzon J, Visse E, Jansson K, Dannaeus K, Henriques-Oliveira C, Roybon L, Anisimov SV, Renström E, Svensson M, Haegerstrand A, Brundin P (2012) The adult human brain harbors multipotent perivascular mesenchymal stem cells. PLoS ONE 7(4):e35577. https://doi.org/10.1371/journal.pone.0035577
Rehman J, Traktuev D, Li J, Merfeld-Clauss S, Temm-Grove CJ, Bovenkerk JE, Pell CL, Johnstone BH, Considine RV, March KL (2004) Secretion of angiogenic and antiapoptotic factors by human adipose stromal cells. Circulation 109(10):1292–1298. https://doi.org/10.1161/01.cir.0000121425.42966.f1
Abu Kasim NH, Govindasamy V, Gnanasegaran N, Musa S, Pradeep PJ, Srijaya TC, Aziz ZA (2015) Unique molecular signatures influencing the biological function and fate of post-natal stem cells isolated from different sources. J Tissue Eng Regen Med 9(12):E252–266. https://doi.org/10.1002/term.1663
Kim Y, Kim H, Cho H, Bae Y, Suh K, Jung J (2007) Direct comparison of human mesenchymal stem cells derived from adipose tissues and bone marrow in mediating neovascularization in response to vascular ischemia. Internat J Expe Cell Physiol Biochem Pharmacol 20(6):867–876. https://doi.org/10.1159/000110447
Lalu MM, McIntyre L, Pugliese C, Fergusson D, Winston BW, Marshall JC, Granton J, Stewart DJ (2012) Safety of cell therapy with mesenchymal stromal cells (SafeCell): a systematic review and meta-analysis of clinical trials. PLoS ONE 7(10):e47559. https://doi.org/10.1371/journal.pone.0047559
Hess DC, Sila CA, Furlan AJ, Wechsler LR, Switzer JA, Mays RW (2014) A double-blind placebo-controlled clinical evaluation of MultiStem for the treatment of ischemic stroke. Internat J Expe Cell Physiol Biochem Pharmacol 9(3):381–386. https://doi.org/10.1111/ijs.12065
Bang OY, Lee JS, Lee PH, Lee G (2005) Autologous mesenchymal stem cell transplantation in stroke patients. Ann Neurol 57(6):874–882. https://doi.org/10.1002/ana.20501
Suárez-Monteagudo C, Hernández-Ramírez P, Alvarez-González L, García-Maeso I, de la Cuétara-Bernal K, Castillo-Díaz L, Bringas-Vega ML, Martínez-Aching G, Morales-Chacón LM, Báez-Martín MM, Sánchez-Catasús C, Carballo-Barreda M, Rodríguez-Rojas R, Gómez-Fernández L, Alberti-Amador E, Macías-Abraham C, Balea ED, Rosales LC, Del Valle PL, Ferrer BB, González RM, Bergado JA (2009) Autologous bone marrow stem cell neurotransplantation in stroke patients. An open study. Restorate Neurol Neurosci 27(3):151–161. https://doi.org/10.3233/rnn-2009-0483
Jaillard A, Hommel M, Moisan A, Zeffiro TA, Favre-Wiki IM, Barbieux-Guillot M, Vadot W, Marcel S, Lamalle L, Grand S, Detante O (2020) Autologous mesenchymal stem cells improve motor recovery in subacute ischemic stroke: a randomized clinical trial. Trans Stroke Res. https://doi.org/10.1007/s12975-020-00787-z
Lee JS, Hong JM, Moon GJ, Lee PH, Ahn YH, Bang OY (2010) A long-term follow-up study of intravenous autologous mesenchymal stem cell transplantation in patients with ischemic stroke. Stem Cells (Dayton, Ohio) 28(6):1099–1106. https://doi.org/10.1002/stem.430
Jiang Y, Zhu W, Zhu J, Wu L, Xu G, Liu X (2013) Feasibility of delivering mesenchymal stem cells via catheter to the proximal end of the lesion artery in patients with stroke in the territory of the middle cerebral artery. Cell Transplant 22(12):2291–2298. https://doi.org/10.3727/096368912x658818
Vezzani B, Gomez-Salazar M, Casamitjana J, Tremolada C, Péault B (2019) Human adipose tissue micro-fragmentation for cell phenotyping and secretome characterization. J Visual Exp JoVE 1:52. https://doi.org/10.3791/60117
Díez-Tejedor E, Gutiérrez-Fernández M, Martínez-Sánchez P, Rodríguez-Frutos B, Ruiz-Ares G, Lara ML, Gimeno BF (2014) Reparative therapy for acute ischemic stroke with allogeneic mesenchymal stem cells from adipose tissue: a safety assessment: a phase II randomized, double-blind, placebo-controlled, single-center, pilot clinical trial. J Dis Off J Nat Stroke Ass 23(10):2694–2700. https://doi.org/10.1016/j.jstrokecerebrovasdis.2014.06.011
Ryan JM, Barry FP, Murphy JM, Mahon BP (2005) Mesenchymal stem cells avoid allogeneic rejection. J Inflam (London, England) 2:8. https://doi.org/10.1186/1476-9255-2-8
Griffin MD, Ritter T, Mahon BP (2010) Immunological aspects of allogeneic mesenchymal stem cell therapies. Hum Gene Ther 21(12):1641–1655. https://doi.org/10.1089/hum.2010.156
Levy ML, Crawford JR, Dib N, Verkh L, Tankovich N, Cramer SC (2019) Phase I/II study of safety and preliminary efficacy of intravenous allogeneic mesenchymal stem cells in chronic stroke. Stroke 50(10):2835–2841. https://doi.org/10.1161/strokeaha.119.026318
Steinberg GK, Kondziolka D, Wechsler LR, Lunsford LD, Coburn ML, Billigen JB, Kim AS, Johnson JN, Bates D, King B, Case C, McGrogan M, Yankee EW, Schwartz NE (2016) Clinical outcomes of transplanted modified bone marrow-derived mesenchymal stem cells in stroke: a phase 1/2a study. Stroke 47(7):1817–1824. https://doi.org/10.1161/strokeaha.116.012995
Haider HKh, Ashraf M (2008) Strategies to promote donor cell survival: combining preconditioning approach with stem cell transplantation. J Mol Cell Cardiol 45(4):554–566. https://doi.org/10.1016/j.yjmcc.2008.05.004
Honmou O, Houkin K, Matsunaga T, Niitsu Y, Ishiai S, Onodera R, Waxman SG, Kocsis JD (2011) Intravenous administration of auto serum-expanded autologous mesenchymal stem cells in stroke. Brain J Neurol 134:1790–1807. https://doi.org/10.1093/brain/awr063
Brown J, Park YJ, Lee JY, Chase TN, Koga M, Borlongan CV (2020) Bone Marrow-Derived NCS-01 cells advance a novel cell-based therapy for stroke. Internat J Mole Sci 21:8. https://doi.org/10.3390/ijms21082845
Acknowledgments
Not applicable.
Funding
Not applicable.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest.
Ethical standards
This study was approved by the Institutional Review Board of Beijing Tiantan Hospital.
Informed consent
The manuscript does not contain patient data.
Rights and permissions
About this article
Cite this article
Li, J., Zhang, Q., Wang, W. et al. Mesenchymal stem cell therapy for ischemic stroke: A look into treatment mechanism and therapeutic potential. J Neurol 268, 4095–4107 (2021). https://doi.org/10.1007/s00415-020-10138-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-020-10138-5