Abstract
Introduction
Intramedullary nail fixation is a useful treatment option for A3 intertrochanteric fractures. Occasionally, we have encountered displaced lateral femoral wall (LFW) fragment during surgery with intramedullary nail system. We investigated the postoperative spontaneous reduction of displaced LFW fragments without further fixation and the factors that affected the spontaneous reduction of displaced LFW fragments.
Materials and methods
Forty-four patients with A3.3 intertrochanteric fracture were treated by surgery using intramedullary nails (PFNA; Synthes, Paoli) between March 2007 and December 2012. All patients had a minimum follow-up period of 12 months. We calculated the amount of spontaneous reduction of the displaced LFW fragments from immediate postoperative and last follow-up anteroposterior radiographs. We measured the tilting angle of the LFW fragment, tip–apex distance (TAD), and telescoping of the blade, and evaluated the quality of postoperative reduction.
Results
Twenty-five of the 44 patients had displaced LFW fragments, and the average amount of spontaneous reduction of the displaced LFW fragment was 4.8 mm with statistical significance (p = 0.005). The average tilting angle of all patients was −4.97°, telescoping was 6.83 mm, and TAD was 19.77 mm. Twenty-one patients had good quality of reduction, 21 had acceptable quality, and 2 had poor quality. Multivariate logistic regression analysis for these factors indicated that tilting angle was the only significant factor related to spontaneous reduction of a displaced LFW fragment (p = 0.007, odds ratio = 1.336).
Conclusions
In intramedullary nailing of A3.3 intertrochanteric fractures, the displaced LFW fragments tend to reduce spontaneously without any additional fixation during the postoperative period. We conclude that no additional fixation is needed for the displaced LFW fragment after surgery with intramedullary nail.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Most intertrochanteric fractures require surgical treatment and internal fixation with a sliding hip screw after anatomical reduction [1–3]. The lateral femoral wall (LFW), which refers to the lateral femoral cortex distal to the vastus ridge, provides a buttress for sliding of the proximal fragment [4]. Therefore, breakage of the LFW in intertrochanteric fractures is an important contributor to distinguish 31-A3 fractures from 31-A2 fractures according to the AO-OTA classification [5]. The 31 A3.3 intertrochanteric fracture has a unique fracture geometry that makes this specific fracture type more unstable than other subtypes of 31 A3 fractures. In 31 A3.3 fractures, the main fracture line runs along the intertrochanteric line with two additional fractures—a lesser trochanteric fragment with posteromedial defect, and a broken LFW. This combination constitutes a four-part unstable intertrochanteric fracture with a free LFW fragment (Fig. 1). Fixation of this A3.3 fractures with a sliding hip screw often results in excessive sliding of the proximal fragment leading to medial translation of the distal shaft fragment relative to the proximal fragment and causing complications such as cutout of the head, implant failure, and functional impairment [6, 7]. For these reasons, a trochanteric-stabilizing plate (TSP) was introduced and demonstrated to be effective through biomechanical and clinical study [8, 9]. However, applying a TSP causes additional soft tissue dissection, bleeding, and increased surgical time. Cephalomedullary nailing is a useful option for these 31 A3.3 fractures, because the nail itself acts as a lateral buttress and prevents excessive sliding of the proximal fragment or medial translation of the distal shaft fragment [10–13]. In spite of this potential advantage of a nail over a dynamic hip screw, there is concern regarding the stability and healing of the free LFW fragment that cannot be stabilized by nailing. To our knowledge, there is no previous study specifically evaluating the fate of the free LFW fragment after cephalomedullary nailing of 31 A3.3 intertrochanteric fractures. In this study, we investigated postoperative spontaneous reduction of displaced free LFW fragments and the factors that affected the spontaneous reduction of the displaced free LFW fragment.
Materials and methods
We retrieved 66 cases of AO-OTA-classified 31 A3 intertrochanteric fractures from our hospital’s trauma database between March 2007 and December 2012. The inclusion criteria included (1) acute fractures (<2 weeks from injury), (2) cephalomedullary nailing with 130 degree of blade angle without additional fixation (PFNA; Synthes, Paoli), (3) a minimum follow-up period of 12 months or until the time of failure leading to revision surgery, (4) radiological healing at the time of final follow-up, and (5) presence of a 31 A3.3 fracture according to AO-OTA classification. One patient was excluded because comminution extended into the femur neck, five died within 1 year from other causes after discharge from the hospital, eight were lost to follow-up, two underwent additional wiring around the LFW, one was treated with plating, and one was not able to undergo surgery because of serious comorbidities. Four patients had A3.1 or A3.2 fractures and were excluded as well. Therefore, 22 patients were excluded by our inclusion criteria, and 44 patients were included in our study group (Fig. 2). There were 21 men and 23 women with a mean age at operation of 66 years (range 24–97 years). The mean follow-up period was 18.2 months (range 12–50 months). The right side was affected in 22 patients and the left side in 22.
The 44 patients in the study were divided into two groups depending on the displacement of the LFW fragment: a minimally displaced group (19 patients) with a <4 mm laterally displaced distal apex of the LFW fragment and a displaced group (25 patients) with a more than 4 mm laterally displaced distal apex of the LFW fragment. We categorized the minimal displaced group as having no fragment spontaneous reduction and measured the amount of postoperative spontaneous reduction of the displaced LFW fragment for the displaced group. We also measured the tilting angle of the LFW fragment, tip–apex distance (TAD), and telescoping of blade, and evaluated the quality of postoperative reduction for all 44 patients.
Radiographic measurements
Two measurements were obtained: the perpendicular distance from the apex of the LFW fragment to the lateral border of the nail on the immediate postoperative anteroposterior radiograph, and the perpendicular distance from the lateral femoral cortex (at the same level as the postoperative measurement) to the lateral border of the nail on the anteroposterior radiograph of the latest follow-up (Fig. 3). We corrected for variation in radiological magnification and rotation using comparison between the real blade length and the measured blade length. We defined the tilting angle of the LFW fragment as the angle between a straight line drawn from the vastus ridge to the apex of the LFW fragment and the lateral border of the nail on an immediate postoperative anteroposterior radiograph (Fig. 4). The TAD and telescoping value were measured according to the method described by Baumgaertner et al. [14] on an immediate postoperative radiograph and Gardner et al. [15] on immediate postoperative and last follow-up radiographs. TAD was defined as the sum of the distance from the tip of the blade to the apex of the femoral head on the anteroposterior and lateral radiographs. Telescoping was defined as the distance from the lateral border of the nail to the blade end along the blade (Fig. 5). We considered sliding of the proximal fragment as the difference in telescoping between the immediate postoperative radiograph and the last follow-up radiograph. The quality of postoperative reduction was graded as good, acceptable, and poor (Table 1) [16, 17].
Measurement of LFW displacement. Immediate postoperative AP view (a) and last follow-up (postoperative 17 months) AP view (b). a Perpendicular distance from the apex of the LFW fragment to the lateral border of the nail. A’ perpendicular distance from the lateral femoral cortex (at the same level as the postoperative measurement) to the lateral border of the nail. b B’ distance from the tip of the nail to the point crossed by the blade along the lateral border of the nail. c Level of measurement, distance from the tip of the nail to the point crossed by a perpendicular line drawn from the distal apex of the LFW fragment along the lateral border of the nail. C’ level of measurement, C’ = C × B’/B. We used B’/B as a constant of correction to designate the same level with the previous measurement on the immediate postoperative AP view
All measurements were performed using the picture archiving and communication system (PACS, Pi View Star, Infinitt, Seoul, Korea) by two orthopedic trauma fellows and one orthopedic senior resident. The mean value of the three observers’ measurements was used for statistical analysis.
Statistical analysis
Clinical information including age, gender, amount of postoperative spontaneous reduction of LFW fragment, tilting angle of LFW fragment, TAD and telescoping of blade, and quality of postoperative reduction were subjected to statistical analysis (IBM® SPSS version 19). We used the paired t test to demonstrate the postoperative spontaneous reduction of displaced LFW fragment with rejection of our null hypothesis “There is no change in displacement between immediate postoperative radiograph and last follow-up radiograph.” Student’s t test, Mann–Whitney test, Chi Square test, and Fisher’s exact test were used to investigate the variables related to spontaneous reduction according to the characters of the variables. Simple and multivariate logistic regression analyses were used to identify factors that affected postoperative spontaneous reduction of the LFW fragment.
Results
The results of our study demonstrate that the amount of postoperative spontaneous reduction of a displaced LFW fragment was 4.80 mm and that it was statistically significant (Table 2). Four patients of the 25 patients in this displaced group had no postoperative spontaneous reduction. The data from all 44 patients in the study group are summarized in Table 3. The mean tilting angle of all patients was −4.97°, mean sliding was 6.83 mm, and the mean TAD was 19.77 mm. Twenty-one patients showed good quality of reduction, 21 had acceptable quality, and 2 had poor quality of reduction. The mean age of the 21 patients with postoperative spontaneous reduction was 60.4 years, whereas the 23 patients without postoperative spontaneous reduction had an age of 71.7 years (p = 0.039, Mann–Whitney test). The mean tilting angle was 4.86 degrees in the 21 patients with postoperative spontaneous reduction and −13.95° in the 23 patients without postoperative spontaneous reduction (p < 0.0001, Student’s t test). These two variables showed statistically significant differences between patients with postoperative spontaneous reduction and those without postoperative spontaneous reduction (p < 0.05). Other variables such as gender, TAD, sliding, and quality of reduction had no statistical difference (Table 3). We found that the tilting angle was the only variable related to postoperative spontaneous reduction through univariate and multivariate logistic regression analysis (p = 0.007, odds ratio = 1.336, 95 % CI; 1.082–1.652).
Discussion
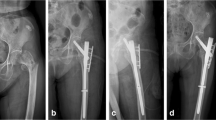
This is the first study to investigate the radiologic healing process of the LFW fragment after surgery using intramedullary nail for A3.3 intertrochanteric fracture. We demonstrate here that the laterally displaced LFW fragments found in intramedullary nailing of A3.3 intertrochanteric fractures tend to reduce spontaneously without any additional fixation during the postoperative period (Fig. 6). Moreover, the tilting angle of the LFW fragment was a prognostic factor for postoperative spontaneous reduction of the laterally displaced LFW fragment. We suggest that there is no requirement to fix the LFW fragment even when there is a temptation to fix it due to displacement with a large tilting angle.
The integrity of the LFW in intertrochanteric fractures plays an important role in choosing the type of implant. In the past, the proximal femoral locked compression plate was recommended for use in fixation of complex proximal femur fractures such as A3 intertrochanteric fracture. However, high rates of mechanical failure after fixation using locked compression plate for those fractures were reported [18, 19]. LFW fracture can also occur intraoperatively or postoperatively. The incidence of LFW fracture treated with intramedullary nailing was 21 % intraoperatively and postoperatively, similar to the incidence of LFW fracture treated with sliding hip screw intraoperatively and postoperatively. However, the reoperation rate (4 %) after surgery with intramedullary nailing because of LFW fracture occurring intraoperatively or postoperatively was significantly lower than that after surgery with sliding hip screw (21 %) [20, 21]. Therefore, LFW reconstruction should be performed when using a sliding hip screw for intertrochanteric fracture with LFW fracture [9], since it seems that the integrity of the LFW has little effect on the healing process after surgery with intramedullary nailing. This could be because the nail functions act as a lateral buttress against excessive sliding of the proximal fragment or medial translation of the distal shaft fragment by itself [13]. Nevertheless, there is no clear guideline for management of a laterally displaced LFW fragment. We expect that this study will help surgeons make a decision in these situations.
We tried to identify the factors affecting postoperative spontaneous reduction of the LFW fragment. The mean sliding value in our study population was 6.61 mm, which is slightly higher than that in previous studies [15, 22]. We had three cases with excessive sliding over 15 mm and two patients with postoperative spontaneous reduction. However, we had no cases with complications such as cutout, cut through or implant failure caused by excessive sliding. We achieved bone union in all 44 cases, but 1 patient without postoperative spontaneous reduction underwent autogenous cancellous bone graft from the ipsilateral iliac crest to the undersurface of the LFW fragment tail. Because a solid union was observed between the main portions of the shaft and the LFW fragment at the operation field, we included that case in our study group. The mean TAD was 19.61 mm, lower than the 25 mm previously shown to be generally predictive of a successful result [23]. Out of 44 cases, 3 showed poor reduction, but bony union was achieved without additional procedures in all three cases. Our statistical analysis indicated that these three factors (sliding, TAD, and quality of reduction) were not related to postoperative spontaneous reduction of the LFW fragment.
We were unable to find clear reasons for postoperative spontaneous reduction of the LFW fragment. We hypothesize that recovery of vastus lateralis strength contributes to movement of the LFW fragment because our results indicate that the average age was significantly lower in the group with spontaneous reduction than in the group with no spontaneous reduction (Table 3). The tilting angle was the only significant factor related to spontaneous reduction of the LFW fragment. From this, we also hypothesize that displaced LFW fragment with large tilting angle means it has a reference point at the proximal apex near the main greater trochanter fragment and this point may play a role as a hinge of postoperative spontaneous reduction through the recovery of vastus lateralis strength like closing a door. If displaced LFW fragment has small tilting angle, it might be an absolute free fragment. Therefore, it might be difficult for displaced LFW fragment with small tilting angle to get spontaneous reduction into its original location, because there is no reference point. However, further studies related to muscle power and serial follow-up are needed to demonstrate this presumption.
This study had several limitations. First, we only measured the distance between lateral cortices at the same level on immediate postoperative anteroposterior radiograph and last follow-up anteroposterior radiograph. We were unable to measure the distance between the distal apices of the LFW fragment on the immediate postoperative anteroposterior radiograph and last follow-up anteroposterior radiograph, because the geometry of the fracture site had changed during the union process. Second, the postoperative spontaneous reduction of the LFW fragment was only evaluated on one plane, not on a three-dimensional scale. Third, we divided our 44 cases into two groups based on a 4 mm displacement, because previous studies included 4 mm of displacement as a criterion for quality reduction [24, 25], and it would be difficult to measure the postoperative spontaneous reduction of an LFW fragment with less than 4 mm displacement. However, we may have introduced bias by comparing the spontaneous reduction group with the no spontaneous reduction group. Fourth, we had a broad range of follow-up period from 12 months to 50 months. It means there can be a measurement bias at the fracture site by further bone remodeling beyond the 12th month. Generally, the fracture-healing process is conventionally partitioned into four stages, such as inflammation, soft callus formation, hard callus formation, and bone remodeling. Most osteogenesis including formation of mineralized bone matrix is achieved and soft callus changes to hard callus in the hard callus formation stage. The woven bone hard callus changes into the original lamellar bone within the mineralized bone matrix made in the hard callus stage by a coupled process of bone resorption and formation in the bone remodeling stage through several weeks to even several years [26]. Based on these, we can presume the 12 months is enough time to shape the final geometry of the fracture site and that time is passed over for clinical union, though it is in the middle of the remodeling stage. Therefore, the broad range of follow-up period has just minor influence on our results. Fifth, why four cases with a displaced LFW and large tilting angle did not have postoperative spontaneous reduction is not explained clearly (Fig. 7). Sixth, this study did not include clinical or functional outcomes. A further study is needed to clarify these results. Seventh, the sample size was relatively small and this study was a retrospective study.
Conclusions
In intramedullary nailing of A3.3 intertrochanteric fractures, the displaced LFW fragments tend to reduce spontaneously without any additional fixation during the postoperative period. We conclude that no additional fixation is needed for the displaced LFW fragment after surgery with intramedullary nail.
References
Desjardins AL, Roy A, Paiement G, Newman N, Pedlow F, Desloges D, Turcotte RE (1993) Unstable intertrochanteric fracture of the femur. A prospective randomised study comparing anatomical reduction and medial displacement osteotomy. J Bone Joint Surg Br 75:445–447
Adams CI, Robinson CM, Court-Brown CM, McQueen MM (2001) Prospective randomized controlled trial of an intramedullary nail versus dynamic screw and plate for intertrochanteric fractures of the femur. J Orthop Trauma 15:394–400
Bartonicek I, Dousa P (2002) Prospective randomized controlled trial of an intramedullary nail versus dynamic screw and plate of intertrochanteric fractures of the femur. J Orthop Trauma 16:363–364 (author reply 364)
Gotfried Y (2004) The lateral trochanteric wall: a key element in the reconstruction of unstable pertrochanteric hip fractures. Clin Orthop Relat Res 425:82–86
Marsh JL, Slongo TF, Agel J, Broderick JS, Creevey W, DeCoster TA, Prokuski L, Sirkin M, Ziran B, Henley B, Audigé L (2007) Fracture and dislocation classification compendium—2007: orthopaedic Trauma Association classification, database and outcomes committee. J Orthop Trauma 21:S1–133
Baixauli F, Vicent V, Baixauli E, Serra V, Sánchez-Alepuz E, Gómez V, Martos F (1999) A reinforced rigid fixation device for unstable intertrochanteric fractures. Clin Orthop Relat Res 361:205–215
Müller-Färber J, Wittner B, Reichel R (1988) Late results in the management of pertrochanteric femoral fractures in the elderly with the dynamic hip screw. Unfallchirurg 91:341–350
Babst R, Renner N, Biedermann M, Rosso R, Heberer M, Harder F, Regazzoni P (1998) Clinical results using the trochanter stabilizing plate (TSP): the modular extension of the dynamic hip screw (DHS) for internal fixation of selected unstable intertrochanteric fractures. J Orthop Trauma 12:392–399
Gupta RK, Sangwan K, Kamboj P, Punia SS, Walecha P (2010) Unstable trochanteric fractures: the role of lateral wall reconstruction. Int Orthop 34:125–129. doi:10.1007/s00264-009-0744-y
Haidukewych GJ, Israel TA, Berry DJ (2001) Reverse obliquity fractures of the intertrochanteric region of the femur. J Bone Joint Surg Am 83-A:643–650
Ruecker AH, Rupprecht M, Gruber M, Gebauer M, Barvencik F, Briem D, Rueger JM (2009) The treatment of intertrochanteric fractures: results using an intramedullary nail with integrated cephalocervical screws and linear compression. J Orthop Trauma 23:22–30. doi:10.1097/BOT.0b013e31819211b2
Sadowski C, Lübbeke A, Saudan M, Riand N, Stern R, Hoffmeyer P (2002) Treatment of reverse oblique and transverse intertrochanteric fractures with use of an intramedullary nail or a 95 degrees screw-plate: a prospective, randomized study. J Bone Joint Surg Am 84-A:372–381
Hardy DC, Descamps PY, Krallis P, Fabeck L, Smets P, Bertens CL, Delince PE (1998) Use of an intramedullary hip-screw compared with a compression hip-screw with a plate for intertrochanteric femoral fractures. A prospective, randomized study of one hundred patients. J Bone Joint Surg Am 80:618–630
Baumgaertner MR, Curtin SL, Lindskog DM, Keggi JM (1995) The value of the tip-apex distance in predicting failure of fixation of peritrochanteric fractures of the hip. J Bone Joint Surg Am 77:1058–1064
Gardner MJ, Bhandari M, Lawrence BD, Helfet DL, Lorich DG (2005) Treatment of intertrochanteric hip fractures with the AO trochanteric fixation nail. Orthopedics 28:117–122
Baumgaertner MR, Curtin SL, Lindskog DM (1998) Intramedullary versus extramedullary fixation for the treatment of intertrochanteric hip fractures. Clin Orthop Relat Res 348:87–94
Kim Y, Dheep K, Lee J, Yoon Y-C, Shon W-Y, Oh C-W, Oh J-K (2014) Hook leverage technique for reduction of intertrochanteric fracture. Injury 45:1006–1010. doi:10.1016/j.injury.2014.02.007
Streubel PN, Moustoukas MJ, Obremskey WT (2013) Mechanical failure after locking plate fixation of unstable intertrochanteric femur fractures. J Orthop Trauma 27:22–28. doi:10.1097/BOT.0b013e318251930d
Wirtz C, Abbassi F, Evangelopoulos DS, Kohl S, Siebenrock KA, Krüger A (2013) High failure rate of trochanteric fracture osteosynthesis with proximal femoral locking compression plate. Injury 44:751–756. doi:10.1016/j.injury.2013.02.020
Palm H, Jacobsen S, Sonne-Holm S, Gebuhr P (2007) Integrity of the lateral femoral wall in intertrochanteric hip fractures: an important predictor of a reoperation. J Bone Joint Surg Am 89:470–475. doi:10.2106/JBJS.F.00679
Boopalan PRJVC, Oh J-K, Kim T-Y, Oh C-W, Cho J-W, Shon W-Y (2012) Incidence and radiologic outcome of intraoperative lateral wall fractures in OTA 31A1 and A2 fractures treated with cephalomedullary nailing. J Orthop Trauma 26:638–642. doi:10.1097/BOT.0b013e318244e5ad
Gardner MJ, Briggs SM, Kopjar B, Helfet DL, Lorich DG (2007) Radiographic outcomes of intertrochanteric hip fractures treated with the trochanteric fixation nail. Injury 38:1189–1196. doi:10.1016/j.injury.2007.03.014
Haidukewych GJ (2009) Intertrochanteric fractures: ten tips to improve results. J Bone Joint Surg Am 91:712–719
Baumgaertner MR, Solberg BD (1997) Awareness of tip-apex distance reduces failure of fixation of trochanteric fractures of the hip. J Bone Joint Surg Br 79:969–971
Guerra Pinto F, Dantas P, Moreira R, Mamede R, Amaral LB (2010) Complications relating to accuracy of reduction of intertrochanteric fractures treated with a compressive hip screw. Hip Int 20:221–228
Schindeler A, McDonald MM, Bokko P, Little DG (2008) Bone remodeling during fracture repair: the cellular picture. Semin Cell Dev Biol 19:459–466. doi:10.1016/j.semcdb.2008.07.004
Acknowledgments
This study was presented and nominated for the award of Young Investigator at the Second AO Trauma Asia Pacific Scientific Congress and TK Experts’ Symposium 2014, Seoul, Republic of Korea.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Kim, Y., Bahk, W.J., Yoon, YC. et al. Radiologic healing of lateral femoral wall fragments after intramedullary nail fixation for A3.3 intertrochanteric fractures. Arch Orthop Trauma Surg 135, 1349–1356 (2015). https://doi.org/10.1007/s00402-015-2284-9
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-015-2284-9