Abstract
Cerebral amyloid angiopathy (CAA) was observed for the first time nearly 100 years ago and systematically described in 1938. It is a common finding in elderly individuals, defined by β-amyloid peptide (Aβ) depositions in cerebral blood vessels, and associated with Alzheimer’s disease (AD). A variety of genetic mutations cause hereditary forms of CAA; in this review, however, only the sporadic variant of CAA is considered. In CAA, Aβ depositions primarily occur in the abluminal portion of the tunica media, and with increasing severity all layers of the blood vessel wall are infiltrated and an additional spread of Aβ into the surrounding neuropil may be seen (i.e., dyshoric changes). CAA is most pronounced in the occipital lobe and its distribution is usually patchy. The relationship between CAA and AD is poorly understood; however, low positive correlations between the severity of both CAA and AD pathology have been observed. CAA is a frequent cause of (warfarin-associated) intracerebral hemorrhage, and the diagnosis of probable CAA-related hemorrhage can be made during life with high accuracy. Both APOE-ε4 and APOE-ε2 are risk factors for CAA, while only APOE-ε2 increases the risk for hemorrhage in CAA. Although the role of CAA as an independent risk factor for cognitive decline is unclear, severe CAA is likely to lower the threshold for clinically overt dementia in neurodegenerative diseases. As for the origin of Aβ in CAA, it may be both produced by smooth muscle cells (vessel wall) and derived from neurons in the course of perivascular drainage.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Historical annotation and introduction
Cerebral amyloid angiopathy (CAA) was probably observed for the first time by Oppenheim in 1909, when he described metachromasia in the core of plaques, which could also be found in nearby capillaries [97]. In 1909 plaques were generally thought to be necrosis. Their amyloid nature was discovered by Divry in 1927, who also observed CAA [22] (for historical review of amyloid see [62], for review of amyloidosis of the nervous system see [33]). The first systematic study of CAA, however, was made by Scholz in 1938 [116]. In this study, Scholz described a vascular disorder of intracortical arterial vessels with both morphological and staining peculiarities resembling the “drusigen Entartung” of the nervous tissue (i.e., amyloid plaques). This resemblance led to the term “drusige Entartung” of cerebral arteries and capillaries. Other authors called this vascular disorder “dyshoric angiopathy” which referred to CAA with additional congophilic depositions in the surrounding neuropil [81, 82, 83, 121]. The term dyshoric was based on the assumption that amyloid depositions around blood vessels were a consequence of blood-derived amyloid crossing the blood-brain barrier (horos: border, dyshoric refers to dysfunction in the blood-brain barrier; see also section ‘Morphology of CAA’) [81]. As “drusige Entartung” included both congophilic depositions confined to the vessel wall and “dyshoric angiopathy” [114], the latter term referring to a particular pathogenetic mechanism, Pantelakis and other authors disagreed that “dyshoric angiopathy” and “drusige Entartung” are diseases based on the same pathological entity and consequently distinguished between “dyshoric angiopathy” and congophilic angiopathy, the latter referring to congophilic deposition strictly confined to the vessel wall [7, 98].
Today, the term CAA is used to describe the pathological changes occurring in cerebral blood vessels, both leptomeningeal and intracortical, resulting from depositions of amyloid proteins [105, 106]. Mutations in different genes which ultimately result in amyloid depositions in cerebral blood vessels are described in hereditary or familial forms of CAA [19, 45, 100, 105, 106, 107]. In the present review, however, the term CAA refers to the sporadic, non-hereditary variant of CAA. In general, CAA is defined as depositions of a congophilic material (i.e., positive staining with Congo red dye) in leptomeningeal and intracortical (parenchymal) arteries, arterioles, capillaries, and rarely veins, representing depositions of β-amyloid peptide (Aβ) in the vessel walls, sometimes with additional spread into the surrounding neuropil or depositions in the glia limitans in cases of capillary involvement [3, 4, 19, 50, 51, 102, 105, 106, 138, 139, 141, 151, 157]. Aβ is well known for being the major constituent part of cerebral plaques associated with normal aging and a variety of neurodegenerative disorders including Alzheimer’s disease (AD); Aβ was, however, initially isolated from cerebral blood vessels with CAA [34]. Age-related prevalences of CAA range from 2.3% at age 65–74 years [37] to 100% at over 80 years of age [16], while they range from 70% [3] to 97.6% [51] in AD (Table 1), and therefore it is generally assumed that CAA is strongly associated with AD. In the present article, the literature on the morphology and both neuropathological and clinical diagnoses of CAA are reviewed, together with data on the relationships between CAA and AD, APOE genotype, cerebral vascular lesions, and clinical dementia. Finally, some proposed pathomechanisms of CAA are discussed.
Morphology of CAA
In hematoxylin and eosin (HE)-stained sections severe CAA can be recognized by acellular thickening of blood vessel walls. This morphology is, however, nonspecific for CAA, since it occurs in a variety of other disorders, including hypertensive angiopathy [56].
The term amyloid describes highly insoluble fibrils composed of protein polymers consisting of proteins rich in a β-pleated sheet secondary structure. Over 20 amyloidogenic proteins are known. Among other staining methods for amyloid, thioflavin S or T (fluorescent under ultraviolet light) and Congo red (apple green under polarized light) are commonly used [65, 105, 106, 134, 139, 150]. Both staining methods are specific for amyloid, as they rely on the high β-sheet content of amyloid [108]. To identify Aβ as the amyloidogenic protein several antibodies are commercially available (e.g., mouse monoclonal human Aβ protein antibody, clone 4G8, reactive to amino acid residues 17–24 of human Aβ, and other polyclonal antibodies for further distinction between Aβ 1–40 and Aβ 1–42, Signet Laboratories, MA). In CAA, Aβ is deposited extracellularly mainly as amyloid-β fibrils in close contact with smooth muscle cells [28, 146, 147, 149]. Nonfibrillar, monomeric and oligomeric Aβ was also demonstrated inside smooth muscle cells [28, 146]. Of note, antibodies directed against Aβ stain both amyloid composed of Aβ and nonfibrillar Aβ. Weak and focal immunohistochemical staining of smooth muscle cells could thus be indicative of nonfibrillar Aβ (to prove amyloid nature Congo red or thioflavin stains are helpful).
Depending on the severity of CAA, Aβ depositions have been shown primarily in the abluminal portion of the tunica media, often surrounding smooth muscle cells, and in the adventitia. With increasing severity, Aβ infiltrates all layers of the vessel wall, which shows loss of smooth muscle cells. Finally, the vascular architecture is severely disrupted and “double barrelling”, microaneurysm formation, fibrinoid necrosis, and evidence of perivascular leakage may be seen (Figs. 1, 2) [105, 106, 134, 139]. Intracortical (parenchymal) vessels can show additional spread of Aβ into the surrounding neuropil. Historically this has been referred to as dyshoric changes, as it was assumed that amyloid crosses the blood-brain barrier and literally spreads into the surrounding neuropil [81]. Today, however, dyshoric is a purely descriptive term with no implications regarding the underlying pathomechanism (Fig. 2g, i, j). Dyshoric changes have a similarity to vascular plaques. While vascular plaques are dense, well-demarcated amyloid plaques with a central vessel, dyshoric CAA comprises more diffuse periarterial Aβ depositions, lacking a well-defined border, around Aβ-laden blood vessels. In capillaries, CAA presents as linear thin layers of Aβ deposits in the perivascular basement membrane (glia limitans) and as globular deposits of Aβ on the capillary wall, often in continuity with dyshoric Aβ deposits in the adjacent neuropil (Fig. 3) [3, 4, 90, 102, 123, 136, 141, 143, 144]. Because of this latter circumstance, the term dyshoric CAA is sometimes used as a synonym for capillary CAA [15, 90, 123]. Dyshoric CAA, however, also occurs in arteries and arterioles, whereas capillary CAA may be present without dyshoric changes (Fig. 3a, c). Even in very high degrees of CAA-related changes, endothelial cells are well preserved and usually not affected with Aβ depositions (Fig. 2h, i, j).
Progression of CAA: mild, Aβ depositions in abluminal portions of the blood vessel wall; moderate, abundant Aβ depositions in all layers of the blood vessel wall with loss of smooth muscle cells; severe, blood vessel wall replaced by Aβ depositions, additional double barrelling and/or dyshoric changes may be present (for dyshoric changes see section Morphology of CAA) (CAA cerebral amyloid angiopathy, Aβ β-amyloid peptide)
Different degrees of CAA: mild (a, b) to moderate (c, d) leptomeningeal CAA; moderate cortical CAA (e); severe leptomeningeal (f, h) and cortical CAA (g, i, and j), with characteristic double barrelling (arrow) and dyshoric changes (arrowhead); note that even in high grades of CAA endothelial cells are usually preserved; 4G8 immunostaining
There are conflicting data are reported as to whether CAA leads to either thickening or thinning of the tunica media [69, 72, 81, 93, 98, 134, 157], and some authors have shown a reduction [59, 69, 71], others a dilation [25, 46, 72] of the size of the affected blood vessel’s lumen. However, in a morphometric study of 28 CAA cases, Zekry et al. [157] recently found a thickening of the blood vessel walls and the reduction of the lumen diameter in small arteries (40–120 μm) with only moderate Aβ deposits, but conversely a thinning of the walls and dilation of the lumen in vessels with severe Aβ deposits. The authors suggest that initial deposition of Aβ in early stages of CAA causes wall thickening, resulting in narrowing of the lumen. In later, more severe stages of CAA, however, ongoing Aβ deposition causes muscle cell degeneration and fragmentation, which induces thinning and weakening of the vessel walls leading to dilation of the lumen [59, 137, 157].
Perivascular hemorrhages are frequent around blood vessels affected with CAA (for further details see section CAA-related vascular lesions).
Several authors reported CAA-associated inflammation/vasculitis [24, 117, 130, 139, 154]. Neuropathologically, these cases were characterized by the presence of severe CAA and chronic inflammation within the leptomeninges and in and around the walls of Aβ-laden blood vessels. The perivascular and intramural inflammatory infiltrate consisted of lymphocytes, macrophages, and multinucleated giant cells [117]. The neuropathological findings in these cases were similar to the ones observed in the first two autopsied patients, who had developed meningoencephalitis after immunization against the human Aβ [27, 89]. Briefly, these cases showed severe CAA with inflammatory cells around Aβ-laden blood vessels, but were largely devoid of Aβ plaques. Some Aβ was still present in the cytoplasm of microglia. The latter observation and the presence of severe CAA, possibly caused by perivascular drainage of Aβ, were interpreted as suggesting immune-mediated clearance of Aβ [89].
Topographical distribution of CAA
In general, the distribution of CAA is characteristically patchy and segmental [134]. In one given histological slide there may be foci showing vessels with varying degrees of Aβ depositions adjacent to foci showing vessels without any Aβ deposition (Fig. 4). The patchy distribution of CAA may thus lead to an under-diagnosis of CAA in postmortem examination, as even in severe cases a given histological slide might not contain Aβ-laden blood vessels.
It has been shown by many authors that CAA is most frequent in the occipital lobe, followed by either frontal, temporal or parietal lobes, respectively [5, 99, 101, 125, 126, 129, 135, 153]. Some authors, however, reported the frontal lobe to be the site most frequently involved in CAA [76, 150]. The occipital lobe is not only the site most frequently affected with CAA but also most severely so [5, 125]. CAA is rarely seen in the basal ganglia, thalamus, and cerebellum, while both white matter and brainstem are usually spared [23, 52, 75, 102, 105].
With respect to the distribution of CAA in the different types of cerebral blood vessels, leptomeningeal arteries seem to be more frequently affected than intracortical ones (i.e., arteries in the gray matter), whereas blood vessels of the white matter rarely show CAA [4, 106]. It is generally assumed that involvement of leptomeningeal arteries represents an early stage in the process of the disease, which is followed by involvement of cortical arteries. In some cases, however, intracortical arteries are affected more severely than leptomeningeal ones (Fig. 5). Conflicting data have been reported on the involvement of intracortical capillaries and leptomeningeal veins. Veins, however, tend to be affected less frequently than arterial vessels [105, 106].
Grading of CAA
For practical purposes two grading systems are commonly used in routine neuropathology. Olichney et al. [94] proposed the scale: 0, no Aβ-positive blood vessels; 1, scattered Aβ positivity in either leptomeningeal or intracortical blood vessels; 2, strong, circumferential Aβ positivity in either some leptomeningeal or intracortical blood vessels; 3, widespread, strong, circumferential Aβ positivity in leptomeningeal and intracortical blood vessels; 4, same as 3 with additional dyshoric changes. This system has a rather quantitative approach, whereas Vonsattel et al. [139] grade CAA with respect to the severity of pathological changes in a given blood vessel: mild, amyloid is restricted to the tunica media without significant destruction of smooth muscle cells; moderate, the tunica media is replaced by amyloid and is thicker than normal; severe, extensive amyloid deposition with focal wall fragmentation or even double barrelling of the vessel wall, microaneurysm formation, fibrinoid necrosis, and leakage of blood through the blood vessel wall.
Despite the practical value of these two grading systems, they have some limitations. The system described by Olichney et al. [94] links leptomeningeal and intracortical involvement, and does not allow scoring cases with strong positivity in intracortical vessels but without (strong) positivity in leptomeningeal vessels. The system by Vonsattel et al. [139], on the other hand, does not distinguish between leptomeningeal and intracortical affection. Many different approaches have been used to evaluate the severity of CAA more precisely, including computer-assisted morphometric methods; these methods, however, are too laborious to be used in every day routine analysis [3, 4, 123, 124, 157]. We use a system that not only distinguishes between leptomeningeal and intracortical affection but also allows noting CAA in different topographical sites. Leptomeningeal and intracortical vessels are scored separately: 0, no Aβ positive vessels; 1, mild (i.e., scattered positivity in few vessels); 2, moderate (i.e., scattered positivity in many vessels or strong positivity in few vessels); 3, severe (i.e., strong positivity in many vessels); 4, severe with dyshoric changes (only in intracortical vessels). For each region, we record both the leptomeningeal and the intracortical score separately. To assess the overall severity of CAA the mean values of all scores are calculated (see [5]).
To date, however, a standardized neuropathological criteria for rating CAA is not available and, as stated by Greenberg et al. [41], “this lack makes it difficult to compare results across different populations and studies... and clearly outlines an obstacle to be addressed by investigators in this field”.
CAA and AD pathology
The prevalence of CAA in AD is over 70% (Table 1) and many authors consider CAA as a feature of AD. Despite this high prevalence, the severity of CAA is highly variable in AD, and therefore does not seem to strongly depend on the severity of AD pathology (e.g., CERAD, Braak stages, NIA-Reagan Institute (RI) criteria) [3, 21, 125, 150].
Several studies addressed the association of CAA with both Aβ and tau pathology in the parenchyma that is in close vicinity to Aβ-laden blood vessels. No significant correlations were seen with respect to the direct association between the density of parenchymal Aβ plaques and the severity of CAA in the same region (i.e., same histological slide) [125, 152]. Of note, on combining data from all investigated regions Tian et al. [125] found a low but significant negative correlation between the ratings of both CAA and senile plaques. Several case reports on various genetically linked familial forms of dementia/CAA observed severe neurofibrillary tau pathology around Aβ-laden blood vessels [31, 104, 132, 133], whereas data on the association between CAA and tau pathology in sporadic late onset AD are rare. Fernando and Ince [26] observed a significant association between intracortical CAA and neurofibrillary tangles, but did not see such an association between the latter and leptomeningeal CAA. In a morphometric study on 51 cases of neuropathologically confirmed AD, Williams et al. [145] recently showed that tau immunolabeling was significantly stronger around Aβ-laden arterial blood vessels compared to non-Aβ-laden ones, where, in turn, it exceeded immunolabeling in the cortex away from blood vessels. The authors proposed that the perivascular accumulation of hyperphosphorylated tau, which is more pronounced around Aβ-laden blood vessels, may be rather a consequence of elevated levels of soluble Aβ around blood vessels (due to perivascular drainage of Aβ), than of a particular aspect of vessel function (e.g., mediators released by the vessel wall).
We correlated the severity of CAA with the severity of neuropathological AD criteria (i.e., CERAD, Braak stages, and NIA-RI criteria) and showed that the severity of CAA significantly increases with increasing AD pathology. Only low correlations, however, were seen (Table 2) [3, 4, 5]. We further distinguished between CAA severities in different brain regions and showed that mainly the severity of CAA in the occipital region significantly increased with increasing AD pathology [5]. Contrasting the low correlation between general CAA and AD pathology, the severity of capillary CAA highly correlated with AD pathology [3].
In addition, we found remarkable differences in the composition of Aβ between capillary CAA and general CAA. Many studies showed that vascular Aβ in general CAA is predominantly composed of Aβ peptides terminating at amino acid position 40 (Aβ40). Conversely both senile and neuritic plaques are mainly composed of Aβ peptides terminating at amino acid position 42 (Aβ42) [1, 4, 11, 35, 47, 48, 49, 70, 73, 74, 111]. Our results indicated that general CAA is characterized by Aβ40 and Aβ42 depositions in leptomeningeal and intracortical arterial vessels, with Aβ40 being more frequent and more severe. By contrast, capillary CAA is characterized by globular Aβ42 deposits in intracortical capillaries and pericapillary spaces, often in conjunction with parenchymal Aβ42 depositions (dyshoric changes). Thal et al. [115] described two different types of CAA. CAA type1 showed Aβ deposits in every type of leptomeningeal and intracortical blood vessels including intracortical capillaries, whereas in CAA type 2 intracortical capillaries were not involved. APOE-ε4 was a risk factor for CAA type 1 and APOE-ε2 for CAA type 2 (APOE: apolipoprotein E, see also section CAA and APOE genotype). Since APOE-ε4 is a known risk factor for Aβ plaque deposition, the same pathomechanism may support intracortical capillary Aβ deposition as a component of neuropil associated Aβ deposition in CAA type 1. In CAA type 1 APOE-ε4 and in CAA type 2 APOE-ε2 possibly promote smooth muscle cell-associated Aβ depositions in leptomeningeal and intracortical blood vessels, respectively. In addition, both types of CAA were seen in mild and severe CAA, and their prevalence did not depend on either the patients’ age or the severity of AD-related Aβ load, suggesting that CAA type 1 and CAA type 2 rather represent different disease entities, than the extent of CAA to a capillary level in cases of CAA type 1 [123]. In a study investigating the association between the low density lipoprotein-receptor related protein (LRP) and CAA, Christoforidis et al. [15] recently showed that LRP was associated with CAA in leptomeningeal and intracortical blood vessels but not with capillary CAA. The authors postulate that particular LRP polymorphisms could impair LRP function (in general and/or in relation to Aβ metabolism, i.e., removal of soluble Aβ [57]) and/or modify LRP expression in noncapillary cerebral vessels, leading to a consecutive promotion of vascular Aβ deposition [15]. The underlying pathomechanisms for each general CAA and CAA involving capillaries are not clear yet. They are, however, likely to differ and it is possible that general CAA and capillary CAA represent different pathologic entities [4, 15, 123].
Clinical diagnosis of CAA
As CAA is a common cause of intracerebral hemorrhage, a reliable method for diagnosing CAA during life would facilitate both future clinical drug trials and clinical decision making [37, 60]. The latter is highlighted by data showing CAA to be an important cause of warfarin-associated intracerebral hemorrhage [43, 110]. The clinical diagnosis of CAA-related hemorrhage is based on analysis of biopsy tissue and radiographic techniques which identify the patterns of hemorrhages characteristic for CAA [37]. Athough a sample of cortical tissue can be obtained safely by biopsy or hematoma evacuation [42, 64, 77, 80], tissue samples are generally not available and their interpretation is complicated by the patchy and segmental distribution of CAA, which could lead to negative results even in cases of severe CAA [38, 60]. Greenberg and Vonsattel [38] showed that the presence of mild to moderate vascular Aβ is a sensitive marker for CAA-related hemorrhage and the additional presence of fibrinoid necrosis is specific for CAA-related hemorrhage. As some degree of Aβ in cerebral blood vessels is a common finding in the elderly, its presence should be interpreted with respect to the patient’s age. Therefore, the specificity of vascular Aβ for identifying CAA as cause of hemorrhage decreases with increasing patient age [38]. Gradient echo MRI is the most useful radiographic technique to demonstrate the pattern of hemorrhage characteristic for CAA [37]. The localization of CAA-related hemorrhage follows the localization of CAA in the cerebral cortex and corticosubcortical or lobar regions [37, 58, 134], and is typically absent in regions characteristic of hypertensive hemorrhages (e.g., putamen, thalamus, pons, and cerebellum [37]).
The Boston criteria for diagnosis of CAA-related hemorrhage are based on the tendency for CAA-related hemorrhage to be multiple and to occur primarily in cortical and corticosubcortical (or lobar) brain regions. According to these criteria, the diagnosis of definite CAA-related hemorrhage might only be possible by full postmortem examination. However, based on tissue from evacuated hematoma or cortical biopsy (not necessarily needed), MRI/CT, and clinical data, the diagnosis of probable CAA-related hemorrhage can be made during life with high accuracy, as indicated by correlation of these criteria with postmortem neuropathological findings [60]. In addition, APOE genotyping might be useful in diagnosing CAA-related hemorrhage in some cases; in general, however, it has been shown to be neither sensitive nor specific [37].
CAA and APOE genotype
The apolipoprotein E (APOE) gene encodes a protein, which is involved in the transport of cholesterol and other hydrophobic proteins. It is located on the long arm of human chromosome 19 and has three common alleles designated ε2, ε3, and ε4. These genetic variations result in different amino acid substitutions at positions 112 and 158, respectively (ApoE2: Cys 112, Cys 158; ApoE3: Arg 112, Cys 158; ApoE4: Arg 112, Arg 158). In the majority of Caucasian populations APOE-ε3 is the most common allele; APOE-ε2 and APOE-ε4 are considered variants [113, 140]. It is now well established that possession of at least one APOE-ε4 is a risk factor for both CAA and AD [17, 119, 152]. APOE-ε4 has been shown to be associated with increased Aβ deposition in both AD [103] and CAA [2]. On the other hand, APOE-ε4 was strongly associated with the severity of CAA in AD but not with parenchymal Aβ load, respectively, suggesting that APOE-ε4 favors vascular over parenchymal Aβ deposition [13]. In addition, APOE-ε4-associated AD cases exhibited more severe CAA than AD cases lacking APOE-ε4, and AD cases with severe CAA tend to have less parenchymal Aβ than those with moderate CAA [13, 143]. Capillary CAA was associated with APOE-ε4 [123], and Tian et al. [126, 128] noted that in AD only the extent of CAA within the occipital cortex increased with possession of APOE-ε4.
APOE-ε2 decreases the risk of AD [18] but increases the risk of early onset CAA [40, 88] and of hemorrhages in CAA, as APOE-ε2 promotes the rupture of Aβ-laden blood vessels [14, 78, 91].
CAA-related vascular lesions
CAA has been associated with intracerebral hemorrhages, ischemic infarcts, and white matter loss. With increasing severity of CAA, smooth muscle and elastic elements in blood vessel walls are replaced by Aβ depositions, which may result in microaneurysm formation and ultimately lead to intracerebral (lobar) hemorrhage. Indeed, CAA-related intracerebral hemorrhages are seen in 5–20% of all spontaneous (non-traumatic) cerebral hemorrhages in elderly subjects [23, 51, 139]. Despite the high prevalence of CAA in the occipital cortex, CAA-related hemorrhages have been shown to be more evenly distributed [38, 134]. Patients with both APOE-ε2 and CAA seem to be particular prone to spontaneous hemorrhage [40, 78, 88, 91] and APOE-ε2 was associated with severe pathomorphological changes such as “double barrelling”, fibrinoid necrosis, and evidence of paravascular bleeding in CAA [40, 79]. It was consequently suggested that CAA patients exposed to clinical risk factors such as anti-platelet/anticoagulant medication, hypertension, and minor head trauma may be most at risk of lobar hemorrhage if they are also APOE-ε2 carriers [78]. Given that CAA can imitate transient ischemic attacks, maybe due to focal seizures secondary to petechial hemorrhages [10, 39, 93], caution should be exercised in prescribing anticoagulant medications to elderly patients with transient neurological deficits in the absence of significant carotid stenosis [79]. Vessels affected with CAA frequently demonstrate a “double barrel” lumen, suggestive of weakened vascular extracellular matrix, resulting in the separation of intima from media during tissue preparation [32, 93]. Matrix metalloproteinases, a family of enzymes with over 20 members identified to date, have been shown to be involved in the regulation of vascular integrity and have been implicated in a variety of vasculopathies, including hemorrhagic transformation after cerebral ischemia [55, 63, 120]. Lee et al. [66, 67] showed recently that Aβ peptide induced transcription, cellular release, and proenzyme activation of matrix-metalloproteinase-9 in cultured cerebral endothelial cells, resulting in increased extracellular matrix degradation. Additionally, in aged APPsw transgenic mice [i.e., mouse model overexpressing the Swedish familial AD mutation of Aβ precursor protein (APP): K670N/M671L], the majority of CAA vessels with evidence of microhemorrhage demonstrated matrix-metalloproteinase-9 immunostaining. These findings suggest that spontaneous hemorrhage in CAA might be partly caused by Aβ-induced vascular matrix-metalloproteinase-9 activation [67].
Although less frequently than in hemorrhages, CAA has been observed in patients with ischemic cerebral infarctions of variable extent [9, 72, 93, 94, 95, 96]. In tissue biopsies of 108 cases with recent cerebral or cerebellar infarctions, Cadavid et al. [9] found CAA in 13%, while CAA was present in only 3.7% of controls, suggesting CAA to be a risk factor for ischemic cerebral infarction. The mechanisms by which CAA increases the risk of ischemic infarctions are unknown. However, the deposition of Aβ in the blood vessel walls could induce a disturbance in the vascular reactivity to focal ischemia, with reduction in collateral circulation and more severe injury to ischemic tissues at risk for infarction [9, 159]. In addition, CAA causes both impaired vascular autoregulation and hypoperfusion as a result of thickening of the blood vessel wall and narrowing of the lumen, respectively [94, 128]. In addition to cortical ischemic infarcts, this may also lead to white matter damage.
Albeit CAA is only rarely detected in the white matter, neuropathologically confirmed CAA in the gray matter and leptomeninges correlated with white matter loss [127]. CAA causes degeneration of the tunica media in corticomeningeal arteries, leading to an impairment of cerebrovascular autoregulation in response to blood pressure [46]. This impairment may in turn lead to lesions in the white matter supplied by Aβ-laden meningocortical arteries. White matter lesions in CAA sometimes resemble those seen in Binswanger’s subcortical encephalopathy and a common mechanism of hypoperfusion in these two disorders was suggested [36, 125]. In anecdotal reports CAA was associated with reversible leukoencephalopathy, this, however, is a very unusual presentation of CAA [12, 92, 112].
CAA and dementia
Several studies suggest severe CAA to be an independent risk factor for cognitive decline [26, 39, 41, 86, 150, 157], while others did not find significant differences between the prevalences of CAA in demented and non-demented subjects [3, 99]. In the population-based MRC Cognitive Function and Aging Study, CAA was identified at autopsy in 34 of 93 demented (36.6%) and in 7 of 99 non-demented patients (7.1%), yielding an elevated odds ratio for dementia of 9.3 in multivariable analysis controlling for age, brain weight, neuritic and diffuse plaques, neocortical and hippocampal neurofibrillary tangles, Lewy bodies, and cerebrovascular disease [86]. In the Honolulu-Asia Aging Study (HAAS), however, autopsy performed on 211 individuals did not reveal a significantly higher prevalence of CAA in clinically demented patients (demented: 54.8% versus non-demented: 38.4%) [99]. While the role of CAA as an independent, primary cause of dementia awaits further elucidation, it is, however, widely assumed that CAA has an aggravating effect on the pathology/pathogenesis of other neurodegenerative diseases. Thus, severe CAA may lower the threshold for clinically overt dementia, especially in AD, where subjects with only medium AD pathology (e.g., Braak III or IV) but considerable CAA were clinically demented [51, 53, 99]. As both widespread CAA and arteriosclerosis are associated with cognitive deficits in AD, the combination of these may contribute to neurodegeneration in AD [124]. The exact mechanisms by which CAA affects cognitive function are yet unclear. However, neuronal loss in AD was associated with severity of CAA, and ultrastructural studies have demonstrated the deposition of Aβ in capillaries, which might impede the functional transport of essential nutrients across the blood-brain barrier [85, 128, 156]. The associations between CAA, white matter changes, and cognitive impairment suggest that advanced CAA causes clinically important vascular dysfunction [41].
Pathomechanisms for CAA
The origin of Aβ in blood vessel walls is poorly understood, and several mechanisms have been proposed. As the APP is a membrane protein of nearly every cell type, it was suggested that Aβ derives from the circulation [105, 106]. Recently, however, two other possible pathomechanisms received wider attention: (1) production of Aβ by smooth muscle cells within the vessel walls and/or pericytes, and (2) derivation of Aβ from the neuropil in the course of perivascular drainage.
Production of Aβ by smooth muscle cells within the vessel walls and/or pericytes
Aβ fibrils that have been shown in vascular tunica media in close contact with smooth muscle cells were mainly composed of Aβ40 [4, 28, 122, 146, 147, 149], while Aβ42 was present in only some deposits in AD [4, 35] and in Down’s syndrome [68]. Production of Aβ by vascular smooth muscle cells has been confirmed by cell culture studies which showed intracellular and recently also extracellular Aβ depositions [29, 30, 148]. These Aβ depositions were immunoreactive for Aβ sequences 1–16 and 17–24, but not 37–42, suggesting that vascular smooth muscle cells produce Aβ40 [30]. It was further suggested that proliferating and degenerating smooth muscle cells produce Aβ. Among other factors, including cytokines, injury by hemodynamic stress or ischemia might be responsible for the smooth muscle cell activation, proliferation, formation of Aβ, and eventually degeneration [6, 146]. Similar to smooth muscle cells, degenerating pericytes overproduce Aβ (for review see [8]). It has been suggested that smooth muscle cells mainly secrete non-fibrillary Aβ and that aggregation of monomers in fibrils is an extracellular modification promoted by factors that are present in the ground substance, which in turn is also produced by smooth muscle cells. It is consequently assumed that both Aβ and factors promoting fibrillogenesis are secreted by smooth muscle cells [147].
Derivation of Aβ from the neuropil in the course of perivascular drainage
This hypothesis proposes that Aβ in the blood vessel walls is of neuronal origin. Brain parenchyma is devoid of lymphatic vessels, and interstitial fluid has been shown to drain via perivascular pathways which, by analogy with other species, are the lymphatic drainage pathways of the human brain [20, 142, 158]. The driving force behind that drainage is believed to be, at least partly, the pulsatile flow of blood in the lumina of arteries [90]. There is emerging evidence that soluble Aβ, which is constantly produced by neural cells, is cleared from the brain via several different routes: perivascular pathways with interstitial fluid drainage, directly across the blood-brain barrier into the bloodstream (apparently mediated by LRP-1), and by glia (microglia, astrocytes) [87, 90, 143]. As indicated by animal studies (wild-type and APP transgenic mice), clearance via the perivascular pathway becomes more significant with age [61, 118]. Weller and colleagues [90, 102, 141, 143, 144] propose that CAA occurs due to deposition of Aβ in the vessel walls in the course of perivascular drainage. The reason for this deposition might be both increased production of Aβ by neuronal cells and additional degenerative vascular changes, which commonly affect aged individuals (e.g., atherosclerosis, fibrohyalinosis). The latter leads to reduced elasticity of arterial walls, which in turn might reduce perivascular drainage by diminishing pulsatile-driving movements in the perivascular pathway. It has been shown that thrombosis of a superficial cortical artery was associated with accumulation of Aβ in the walls of capillaries supplied by that artery [155]. It was further suggested that impaired clearance of Aβ leads to an increased concentration of soluble Aβ, which in turn results in precipitation of Aβ in the form of plaques, the development of tau pathology, and neuronal and synaptic loss [90].
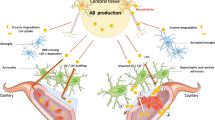
In view of the literature and in combining the 2 pathomechanisms outlined above, the present author hypothesizes the following (Fig. 6): Aβ40 is produced by smooth muscle cells within the vessel walls [30, 84, 146]. For unknown reasons this process is most pronounced in the occipital lobe [99, 101, 125, 126, 129, 135, 153]. With the onset of AD, cortical Aβ load increases. Because of the highly fibrillogenic nature of Aβ42 [54], it does generally not enter the perivascular drainage pathway, but fibrillizes in plaques and deposits on capillary walls/pericapillary spaces. Mainly Aβ40 remains soluble and therefore enters the perivascular drainage pathway [44, 54, 90, 131]. In the course of its perivascular drainage Aβ40 accumulates in blood vessel walls [90, 102, 109, 141, 143, 144]. This accumulation is probably facilitated by both preexisting Aβ derived from smooth muscle cells and other, additional degenerative vascular changes (e.g., atherosclerosis). This process seems to be most pronounced in the occipital lobe as indicated by the significant increase of the severity of CAA in the occipital lobe with increasing AD pathology [5]. This might be because elimination of Aβ in the occipital lobe is, due to high amounts of initially produced Aβ40 by smooth muscle cells (see above), more impaired than in other regions, which in turn results in an “over additive” interaction in-between preexisting, smooth muscle-derived Aβ and draining, neuronally derived Aβ.
Hypothetical pathomechanism for CAA: Neuronally derived Aβ42 fibrillizes into plaques and is the major constituent of Aβ in capillary CAA, while Aβ40 remains soluble and enters the perivascular drainage pathway where it accumulates in blood vessel walls in the presence of Aβ40, which is produced by smooth muscle cells
Conclusions
Sporadic CAA is a common disease in elderly individuals and its incidence and severity increase with age. The most important clinical implication of CAA is its role as a frequent cause for non-traumatic cerebral hemorrhage. From a pathological point of view, however, CAA provides a plethora of topics to be addressed in future research. To better evaluate CAA and to compare data of different study groups it seems necessary to refine the criteria for grading CAA in a way that they are both accurate and practicable. Investigations addressing the origin of Aβ in CAA are likely to further elucidate some of the principal pathomechanisms of AD/dementia and may have implications on future therapeutic strategies. The relationship between CAA and AD is yet to be resolved; it seems, however, that CAA and AD have a mutual aggravating effect with respect to the severity of both pathomorphological changes and clinical dementia.
References
Akiyama H, Mori H, Sahara N, Kondo H, Ikeda K, Nishimura T, Oda T, McGeer PL (1997) Variable deposition of amyloid beta-protein (A beta) with the carboxy-terminus that ends at residue valine40 (A beta 40) in the cerebral cortex of patients with Alzheimer’s disease: a double-labeling immunohistochemical study with antibodies specific for A beta 40 and the A beta that ends at residues alanine42/threonine43 (A beta 42). Neurochem Res 22:1499–1506
Alonzo NC, Hyman BT, Rebeck GW, Greenberg SM (1998) Progression of cerebral amyloid angiopathy: accumulation of amyloid-beta40 in affected vessels. J Neuropathol Exp Neurol 57:353–359
Attems J, Jellinger KA (2004) Only cerebral capillary amyloid angiopathy correlates with Alzheimer pathology—a pilot study. Acta Neuropathol 107:83–90
Attems J, Lintner F, Jellinger KA (2004) Amyloid beta peptide 1–42 highly correlates with capillary cerebral amyloid angiopathy and Alzheimer disease pathology. Acta Neuropathol 107:283–291
Attems J, Jellinger K, Lintner F (2005) Alzheimer disease pathology influences severity and topographical distribution of cerebral amyloid angiopathy. Acta Neuropathol 110:222–231
Bauer J, Ganter U, Strauss S, Stadtmuller G, Frommberger U, Bauer H, Volk B, Berger M (1992) The participation of interleukin-6 in the pathogenesis of Alzheimer’s disease. Res Immunol 143:650–657
Braunmühl A (1956) Kongophile Angiopathie und senile Plaques bei greisen Hunden. Arch Psychiat Nervenkr 194:396–414
Burgermeister P, Calhoun ME, Winkler DT, Jucker M (2000) Mechanisms of cerebrovascular amyloid deposition. Lessons from mouse models. Ann N Y Acad Sci 903:307–316
Cadavid D, Mena H, Koeller K, Frommelt RA (2000) Cerebral beta amyloid angiopathy is a risk factor for cerebral ischemic infarction. A case control study in human brain biopsies. J Neuropathol Exp Neurol 59:768–773
Case rotMGH (1996) Weekly clinicopathological exercises. Case 22–1996. Cerebral hemorrhage in a 69-year-old woman receiving warfarin. N Engl J Med 335:189–196
Castano EM, Prelli F, Soto C, Beavis R, Matsubara E, Shoji M, Frangione B (1996) The length of amyloid-beta in hereditary cerebral hemorrhage with amyloidosis, Dutch type. Implications for the role of amyloid-beta 1–42 in Alzheimer’s disease. J Biol Chem 271:32185–32191
Caulo M, Tampieri D, Brassard R, Christine Guiot M, Melanson D (2001) Cerebral amyloid angiopathy presenting as nonhemorrhagic diffuse encephalopathy: neuropathologic and neuroradiologic manifestations in one case. AJNR Am J Neuroradiol 22:1072–1076
Chalmers K, Wilcock GK, Love S (2003) APOE epsilon 4 influences the pathological phenotype of Alzheimer’s disease by favouring cerebrovascular over parenchymal accumulation of A beta protein. Neuropathol Appl Neurobiol 29:231–238
Cho HS, Hyman BT, Greenberg SM, Rebeck GW (2001) Quantitation of apoE domains in Alzheimer disease brain suggests a role for apoE in Abeta aggregation. J Neuropathol Exp Neurol 60:342–349
Christoforidis M, Schober R, Krohn K (2005) Genetic-morphologic association study: association between the low density lipoprotein-receptor related protein (LRP) and cerebral amyloid angiopathy. Neuropathol Appl Neurobiol 31:11–19
Chui HC, Victoroff JI, Margolin D, Jagust W, Shankle R, Katzman R (1992) Criteria for the diagnosis of ischemic vascular dementia proposed by the State of California Alzheimer’s Disease Diagnostic and Treatment Centers. Neurology 42:473–480
Corder EH, Saunders AM, Strittmatter WJ, Schmechel DE, Gaskell PC, Small GW, Roses AD, Haines JL, Pericak-Vance MA (1993) Gene dose of apolipoprotein E type 4 allele and the risk of Alzheimer’s disease in late onset families. Science 261:921–923
Corder EH, Saunders AM, Risch NJ, Strittmatter WJ, Schmechel DE, Gaskell PC Jr, Rimmler JB, Locke PA, Conneally PM, Schmader KE, et al (1994) Protective effect of apolipoprotein E type 2 allele for late onset Alzheimer disease. Nat Genet 7:180–184
Coria F, Rubio I (1996) Cerebral amyloid angiopathies. Neuropathol Appl Neurobiol 22:216–227
Cserr HF, Harling-Berg CJ, Knopf PM (1992) Drainage of brain extracellular fluid into blood and deep cervical lymph and its immunological significance. Brain Pathol 2:269–276
Dermaut B, Kumar-Singh S, De Jonghe C, Cruts M, Lofgren A, Lubke U, Cras P, Dom R, De Deyn PP, Martin JJ, Van Broeckhoven C (2001) Cerebral amyloid angiopathy is a pathogenic lesion in Alzheimer’s disease due to a novel presenilin 1 mutation. Brain 124:2383–2392
Divry P (1927) Etude histochimique des plaques séniles. J Neurol Psychiat 27:643–657
Ellis RJ, Olichney JM, Thal LJ, Mirra SS, Morris JC, Beekly D, Heyman A (1996) Cerebral amyloid angiopathy in the brains of patients with Alzheimer’s disease: the CERAD experience, Part XV. Neurology 46:1592–1596
Eng JA, Frosch MP, Choi K, Rebeck GW, Greenberg SM (2004) Clinical manifestations of cerebral amyloid angiopathy-related inflammation. Ann Neurol 55:250–256
Esiri MM, Wilcock GK (1986) Cerebral amyloid angiopathy in dementia and old age. J Neurol Neurosurg Psychiatry 49:1221–1226
Fernando MS, Ince PG (2004) Vascular pathologies and cognition in a population-based cohort of elderly people. J Neurol Sci 226:13–17
Ferrer I, Boada Rovira M, Sanchez Guerra ML, Rey MJ, Costa-Jussa F (2004) Neuropathology and pathogenesis of encephalitis following amyloid-beta immunization in Alzheimer’s disease. Brain Pathol 14:11–20
Frackowiak J, Zoltowska A, Wisniewski HM (1994) Non-fibrillar beta-amyloid protein is associated with smooth muscle cells of vessel walls in Alzheimer disease. J Neuropathol Exp Neurol 53:637–645
Frackowiak J, Miller DL, Potempska A, Sukontasup T, Mazur-Kolecka B (2003) Secretion and accumulation of Abeta by brain vascular smooth muscle cells from AbetaPP-Swedish transgenic mice. J Neuropathol Exp Neurol 62:685–696
Frackowiak J, Potempska A, LeVine H, Haske T, Dickson D, Mazur-Kolecka B (2005) Extracellular deposits of Abeta produced in cultures of Alzheimer disease brain vascular smooth muscle cells. J Neuropathol Exp Neurol 64:82–90
Ghetti B, Piccardo P, Spillantini MG, Ichimiya Y, Porro M, Perini F, Kitamoto T, Tateishi J, Seiler C, Frangione B, Bugiani O, Giaccone G, Prelli F, Goedert M, Dlouhy SR, Tagliavini F (1996) Vascular variant of prion protein cerebral amyloidosis with tau-positive neurofibrillary tangles: the phenotype of the stop codon 145 mutation in PRNP. Proc Natl Acad Sci USA 93:744–748
Gilbert JJ, Vinters HV (1983) Cerebral amyloid angiopathy: incidence and complications in the aging brain. I. Cerebral hemorrhage. Stroke 14:915–923
Glenner GG, Murphy MA (1989) Amyloidosis of the nervous system. J Neurol Sci 94:1–28
Glenner GG, Wong CW (1984) Alzheimer’s disease: initial report of the purification and characterization of a novel cerebrovascular amyloid protein. Biochem Biophys Res Commun 120:885–890
Gravina SA, Ho L, Eckman CB, Long KE, Otvos L Jr, Younkin LH, Suzuki N, Younkin SG (1995) Amyloid beta protein (A beta) in Alzheimer’s disease brain. Biochemical and immunocytochemical analysis with antibodies specific for forms ending at A beta 40 or A beta 42(43). J Biol Chem 270:7013–7016
Gray F, Dubas F, Roullet E, Escourolle R (1985) Leukoencephalopathy in diffuse hemorrhagic cerebral amyloid angiopathy. Ann Neurol 18:54–59
Greenberg SM (1998) Cerebral amyloid angiopathy: prospects for clinical diagnosis and treatment. Neurology 51:690–694
Greenberg SM, Vonsattel JP (1997) Diagnosis of cerebral amyloid angiopathy. Sensitivity and specificity of cortical biopsy. Stroke 28:1418–1422
Greenberg SM, Vonsattel JP, Stakes JW, Gruber M, Finklestein SP (1993) The clinical spectrum of cerebral amyloid angiopathy: presentations without lobar hemorrhage. Neurology 43:2073–2079
Greenberg SM, Vonsattel JP, Segal AZ, Chiu RI, Clatworthy AE, Liao A, Hyman BT, Rebeck GW (1998) Association of apolipoprotein E epsilon2 and vasculopathy in cerebral amyloid angiopathy. Neurology 50:961–965
Greenberg SM, Gurol ME, Rosand J, Smith EE (2004) Amyloid angiopathy-related vascular cognitive impairment. Stroke 35:2616–2619
Greene GM, Godersky JC, Biller J, Hart MN, Adams HP Jr (1990) Surgical experience with cerebral amyloid angiopathy. Stroke 21:1545–1549
Hart RG (2000) What causes intracerebral hemorrhage during warfarin therapy? Neurology 55:907–908
Herzig MC, Winkler DT, Burgermeister P, Pfeifer M, Kohler E, Schmidt SD, Danner S, Abramowski D, Sturchler-Pierrat C, Burki K, Duinen SG van, Maat-Schieman ML, Staufenbiel M, Mathews PM, Jucker M (2004) Abeta is targeted to the vasculature in a mouse model of hereditary cerebral hemorrhage with amyloidosis. Nat Neurosci 7:954–960
Holton JL, Ghiso J, Lashley T, Rostagno A, Guerin CJ, Gibb G, Houlden H, Ayling H, Martinian L, Anderton BH, Wood NW, Vidal R, Plant G, Frangione B, Revesz T (2001) Regional distribution of amyloid-Bri deposition and its association with neurofibrillary degeneration in familial British dementia. Am J Pathol 158:515–526
Imaoka K, Kobayashi S, Fujihara S, Shimode K, Nagasaki M (1999) Leukoencephalopathy with cerebral amyloid angiopathy: a semiquantitative and morphometric study. J Neurol 246:661–666
Iwatsubo T, Odaka A, Suzuki N, Mizusawa H, Nukina N, Ihara Y (1994) Visualization of A beta 42(43) and A beta 40 in senile plaques with end-specific A beta monoclonals: evidence that an initially deposited species is A beta 42(43). Neuron 13:45–53
Iwatsubo T, Mann DM, Odaka A, Suzuki N, Ihara Y (1995) Amyloid beta protein (A beta) deposition: A beta 42(43) precedes A beta 40 in Down syndrome. Ann Neurol 37:294–299
Iwatsubo T, Saido TC, Mann DM, Lee VM, Trojanowski JQ (1996) Full-length amyloid-beta (1–42(43)) and amino-terminally modified and truncated amyloid-beta 42(43) deposit in diffuse plaques. Am J Pathol 149:1823–1830
Jellinger K (1977) Cerebrovascular amyloidosis with cerebral hemorrhage. J Neurol 214:195–206
Jellinger KA (2002) Alzheimer disease and cerebrovascular pathology: an update. J Neural Transm 109:813–836
Jellinger KA, Attems J (2003) Incidence of cerebrovascular lesions in Alzheimer’s disease: a postmortem study. Acta Neuropathol 105:14–17
Jellinger KA, Attems J (2005) Prevalence and pathogenic role of cerebrovascular lesions in Alzheimer disease. J Neurol Sci 229–230:37–41
Jucker M (2005) What have we learned about cerebral amyloid from transgenic animal models of Alzheimer’s disease? Neuropathol Appl Neurobiol 31:216–217
Kaczmarek L, Lapinska-Dzwonek J, Szymczak S (2002) Matrix metalloproteinases in the adult brain physiology: a link between c-Fos, AP-1 and remodeling of neuronal connections? EMBO J 21:6643–6648
Kalimo H, Kaste M, Haltia M (2002) Vascular diseases. In: Graham DI, Lantos PL (eds) Greenfield’s Neuropathology. Arnold, London, pp 293–295
Kang DE, Pietrzik CU, Baum L, Chevallier N, Merriam DE, Kounnas MZ, Wagner SL, Troncoso JC, Kawas CH, Katzman R, Koo EH (2000) Modulation of amyloid beta-protein clearance and Alzheimer’s disease susceptibility by the LDL receptor-related protein pathway. J Clin Invest 106:1159–1166
Kase CS (1994) Cerebral amyloid angiopathy. In: Kase CS, Caplan LR (eds) Intracerebral hemorrhage. Butterworth-Heinemann, Boston, pp 179–200
Kawai M, Kalaria RN, Cras P, Siedlak SL, Velasco ME, Shelton ER, Chan HW, Greenberg BD, Perry G (1993) Degeneration of vascular muscle cells in cerebral amyloid angiopathy of Alzheimer disease. Brain Res 623:142–146
Knudsen KA, Rosand J, Karluk D, Greenberg SM (2001) Clinical diagnosis of cerebral amyloid angiopathy: validation of the Boston criteria. Neurology 56:537–539
Kuo YM, Crawford F, Mullan M, Kokjohn TA, Emmerling MR, Weller RO, Roher AE (2000) Elevated A beta and apolipoprotein E in A betaPP transgenic mice and its relationship to amyloid accumulation in Alzheimer’s disease. Mol Med 6:430–439
Kyle RA (2001) Amyloidosis: a convoluted story. Br J Haematol 114:529–538
Lapchak PA, Chapman DF, Zivin JA (2000) Metalloproteinase inhibition reduces thrombolytic (tissue plasminogen activator)-induced hemorrhage after thromboembolic stroke. Stroke 31:3034–3040
Leblanc R, Preul M, Robitaille Y, Villemure JG, Pokrupa R (1991) Surgical considerations in cerebral amyloid angiopathy. Neurosurgery 29:712–718
Leclercq PD, Murray LS, Smith C, Graham DI, Nicoll JA, Gentleman SM (2005) Cerebral amyloid angiopathy in traumatic brain injury: association with apolipoprotein E genotype. J Neurol Neurosurg Psychiatry 76:229–233
Lee JM, Yin KJ, Hsin I, Chen S, Fryer JD, Holtzman DM, Hsu CY, Xu J (2003) Matrix metalloproteinase-9 and spontaneous hemorrhage in an animal model of cerebral amyloid angiopathy. Ann Neurol 54:379–382
Lee JM, Yin K, Hsin I, Chen S, Fryer JD, Holtzman DM, Hsu CY, Xu J (2005) Matrix metalloproteinase-9 in cerebral-amyloid-angiopathy-related hemorrhage. J Neurol Sci 229–230:249–254
Lemere CA, Blusztajn JK, Yamaguchi H, Wisniewski T, Saido TC, Selkoe DJ (1996) Sequence of deposition of heterogeneous amyloid beta-peptides and APO E in Down syndrome: implications for initial events in amyloid plaque formation. Neurobiol Dis 3:16–32
Maeda A, Yamada M, Itoh Y, Otomo E, Hayakawa M, Miyatake T (1993) Computer-assisted three-dimensional image analysis of cerebral amyloid angiopathy. Stroke 24:1857–1864
Mak K, Yang F, Vinters HV, Frautschy SA, Cole GM (1994) Polyclonals to beta-amyloid(1–42) identify most plaque and vascular deposits in Alzheimer cortex, but not striatum. Brain Res 667:138–142
Mancardi GL, Perdelli F, Rivano C, Leonardi A, Bugiani O (1980) Thickening of the basement membrane of cortical capillaries in Alzheimer’s disease. Acta Neuropathol (Berl) 49:79–83
Mandybur TI (1986) Cerebral amyloid angiopathy: the vascular pathology and complications. J Neuropathol Exp Neurol 45:79–90
Mann DM, Iwatsubo T (1996) Diffuse plaques in the cerebellum and corpus striatum in Down’s syndrome contain amyloid beta protein (A beta) only in the form of A beta 42(43). Neurodegeneration 5:115–120
Mann DM, Iwatsubo T, Ihara Y, Cairns NJ, Lantos PL, Bogdanovic N, Lannfelt L, Winblad B, Maat-Schieman ML, Rossor MN (1996) Predominant deposition of amyloid-beta 42(43) in plaques in cases of Alzheimer’s disease and hereditary cerebral hemorrhage associated with mutations in the amyloid precursor protein gene. Am J Pathol 148:1257–1266
Mann DM, Pickering-Brown SM, Takeuchi A, Iwatsubo T (2001) Amyloid angiopathy and variability in amyloid beta deposition is determined by mutation position in presenilin-1-linked Alzheimer’s disease. Am J Pathol 158:2165–2175
Masuda J, Tanaka K, Ueda K, Omae T (1988) Autopsy study of incidence and distribution of cerebral amyloid angiopathy in Hisayama, Japan. Stroke 19:205–210
Matkovic Z, Davis S, Gonzales M, Kalnins R, Masters CL (1991) Surgical risk of hemorrhage in cerebral amyloid angiopathy. Stroke 22:456–461
McCarron MO, Nicoll JA, Ironside JW, Love S, Alberts MJ, Bone I (1999) Cerebral amyloid angiopathy-related hemorrhage. Interaction of APOE epsilon2 with putative clinical risk factors. Stroke 30:1643–1646
McCarron MO, Nicoll JA, Stewart J, Ironside JW, Mann DM, Love S, Graham DI, Dewar D (1999) The apolipoprotein E epsilon2 allele and the pathological features in cerebral amyloid angiopathy-related hemorrhage. J Neuropathol Exp Neurol 58:711–718
Minakawa T, Takeuchi S, Sasaki O, Koizumi T, Honad Y, Fujii Y, Ozawa T, Ogawa H, Koike T, Tanaka R (1995) Surgical experience with massive lobar haemorrhage caused by cerebral amyloid angiopathy. Acta Neurochir (Wien) 132:48–52
Morel F (1950) Petite contribution à l‘étude d’une angiopathie apparemment dyshorique et topistique. Rev Mens Psychiatr Neurol 120:352–357
Morel F, Wildi E (1952) General and cellular pathochemistry of senile and presenile alterations of the brain. In: Proceedings of the first international congress of neuropathology. Rosenber and Sellier Rome, pp 347–374
Morel F, Wildi E (1955) Contribution à la connaissance des différentes altérations cérébrales du grand âge. Arch Suisses Neurol Psychiatr 76:190–197
Natte R, Boer WI de, Maat-Schieman ML, Baelde HJ, Vinters HV, Roos RA, Duinen SG van (1999) Amyloid beta precursor protein-mRNA is expressed throughout cerebral vessel walls. Brain Res 828:179–183
Natte R, Yamaguchi H, Maat-Schieman ML, Prins FA, Neeskens P, Roos RA, Duinen SG van (1999) Ultrastructural evidence of early non-fibrillar Abeta42 in the capillary basement membrane of patients with hereditary cerebral hemorrhage with amyloidosis, Dutch type. Acta Neuropathol 98:577–582
Neuropathology GMRCCFaAS (2001) Pathological correlates of late-onset dementia in a multicentre, community-based population in England and Wales. Neuropathology Group of the Medical Research Council Cognitive Function and Ageing Study (MRC CFAS). Lancet 357:169–175
Nicoll JA, Weller RO (2003) A new role for astrocytes: beta-amyloid homeostasis and degradation. Trends Mol Med 9:281–282
Nicoll JA, Burnett C, Love S, Graham DI, Dewar D, Ironside JW, Stewart J, Vinters HV (1997) High frequency of apolipoprotein E epsilon 2 allele in hemorrhage due to cerebral amyloid angiopathy. Ann Neurol 41:716–721
Nicoll JA, Wilkinson D, Holmes C, Steart P, Markham H, Weller RO (2003) Neuropathology of human Alzheimer disease after immunization with amyloid-beta peptide: a case report. Nat Med 9:448–452
Nicoll JA, Yamada M, Frackowiak J, Mazur-Kolecka B, Weller RO (2004) Cerebral amyloid angiopathy plays a direct role in the pathogenesis of Alzheimer’s disease; Pro-CAA position statement. Neurobiol Aging 25:589–597
O’Donnell HC, Rosand J, Knudsen KA, Furie KL, Segal AZ, Chiu RI, Ikeda D, Greenberg SM (2000) Apolipoprotein E genotype and the risk of recurrent lobar intracerebral hemorrhage. N Engl J Med 342:240–245
Oh U, Gupta R, Krakauer JW, Khandji AG, Chin SS, Elkind MS (2004) Reversible leukoencephalopathy associated with cerebral amyloid angiopathy. Neurology 62:494–497
Okazaki H, Reagan TJ, Campbell RJ (1979) Clinicopathologic studies of primary cerebral amyloid angiopathy. Mayo Clin Proc 54:22–31
Olichney JM, Hansen LA, Hofstetter CR, Grundman M, Katzman R, Thal LJ (1995) Cerebral infarction in Alzheimer’s disease is associated with severe amyloid angiopathy and hypertension. Arch Neurol 52:702–708
Olichney JM, Ellis RJ, Katzman R, Sabbagh MN, Hansen L (1997) Types of cerebrovascular lesions associated with severe cerebral amyloid angiopathy in Alzheimer’s disease. Ann N Y Acad Sci 826:493–497
Olichney JM, Hansen LA, Hofstetter CR, Lee JH, Katzman R, Thal LJ (2000) Association between severe cerebral amyloid angiopathy and cerebrovascular lesions in Alzheimer disease is not a spurious one attributable to apolipoprotein E4. Arch Neurol 57:869–874
Oppenheim G (1909) Über “drusige Nekrosen” in der Großhirnrinde. Neurol Zbl 8:410–413
Pantelakis S (1954) Un type particulier d’angiopathie sénile du système nerveux central: l’angiopathie congophile. Topographie et fréquence. Monatsschr Psychiatr Neurol 128:219–256
Pfeifer LA, White LR, Ross GW, Petrovitch H, Launer LJ (2002) Cerebral amyloid angiopathy and cognitive function: the HAAS autopsy study. Neurology 58:1629–1634
Plant G, Revesz T, Barnard R, Harding A, Gautier-Smith P (1990) Familial cerebral amyloid angiopathy with nonneuritic amyloid plaque formation. Brain 113:721–747
Premkumar DR, Cohen DL, Hedera P, Friedland RP, Kalaria RN (1996) Apolipoprotein E-epsilon4 alleles in cerebral amyloid angiopathy and cerebrovascular pathology associated with Alzheimer’s disease. Am J Pathol 148:2083–2095
Preston SD, Steart PV, Wilkinson A, Nicoll JA, Weller RO (2003) Capillary and arterial cerebral amyloid angiopathy in Alzheimer’s disease: defining the perivascular route for the elimination of amyloid beta from the human brain. Neuropathol Appl Neurobiol 29:106–117
Rebeck GW, Reiter JS, Strickland DK, Hyman BT (1993) Apolipoprotein E in sporadic Alzheimer’s disease: allelic variation and receptor interactions. Neuron 11:575–580
Revesz T, Holton JL, Doshi B, Anderton BH, Scaravilli F, Plant GT (1999) Cytoskeletal pathology in familial cerebral amyloid angiopathy (British type) with non-neuritic amyloid plaque formation. Acta Neuropathol 97:170–176
Revesz T, Holton JL, Lashley T, Plant G, Rostagno A, Ghiso J, Frangione B (2002) Sporadic and familial cerebral amyloid angiopathies. Brain Pathol 12:343–357
Revesz T, Ghiso J, Lashley T, Plant G, Rostagno A, Frangione B, Holton JL (2003) Cerebral amyloid angiopathies: a pathologic, biochemical, and genetic view. J Neuropathol Exp Neurol 62:885–898
Revesz T, Ghiso J, Plant G, Holton JL, Frangione B (2003) Inherited amyloidosis and neurodegenerations in Familial British and Danish Dementia. In: Dickson DW (ed) Neurodegeneration: the molecular pathology of dementia and movement disorders. ISN Neuropath Press, Basel, pp 380–385
Revesz T, Ghiso J, Plant G, Lashley T, Rostagno A, Frangione B, Holton JL (2005) Cerebral amyloid angiopathy. In: Kalimo H (ed) Pathology and genetics. Cerebrovascular diseases. ISN Neuropath Press, Basel, pp 94–102
Roher AE, Kuo YM, Esh C, Knebel C, Weiss N, Kalback W, Luehrs DC, Childress JL, Beach TG, Weller RO, Kokjohn TA (2003) Cortical and leptomeningeal cerebrovascular amyloid and white matter pathology in Alzheimer’s disease. Mol Med 9:112–122
Rosand J, Hylek EM, O’Donnell HC, Greenberg SM (2000) Warfarin-associated hemorrhage and cerebral amyloid angiopathy: a genetic and pathologic study. Neurology 55:947–951
Saido TC, Iwatsubo T, Mann DM, Shimada H, Ihara Y, Kawashima S (1995) Dominant and differential deposition of distinct beta-amyloid peptide species, A beta N3(pE), in senile plaques. Neuron 14:457–466
Sarazin M, Amarenco P, Mikol J, Dimitri D, Lot G, Bousser MG (2002) Reversible leukoencephalopathy in cerebral amyloid angiopathy presenting as subacute dementia. Eur J Neurol 9:353–358
Saunders AM (2000) Apolipoprotein E and Alzheimer disease: an update on genetic and functional analyses. J Neuropathol Exp Neurol 59:751–758
Schlote W (1965) Die Amyloidnatur der kongophilen, drusigen Entartung der Hirnarterien (Scholz) im Senium. Acta Neuropathol 4:449–468
Schmechel DE, Saunders AM, Strittmatter WJ, Crain BJ, Hulette CM, Joo SH, Pericak-Vance MA, Goldgaber D, Roses AD (1993) Increased amyloid beta-peptide deposition in cerebral cortex as a consequence of apolipoprotein E genotype in late-onset Alzheimer disease. Proc Natl Acad Sci USA 90:9649–9653
Scholz W (1938) Studien zur Pathologie der Hirngefäße. II. Die drusige Entartung der Hirnarterien und -capillaren (eine Form seniler Gefäßerkrankung). Z Ges Neurol Psychiatr 162:694–715
Scolding NJ, Joseph F, Kirby PA, Mazanti I, Gray F, Mikol J, Ellison D, Hilton DA, Williams TL, MacKenzie JM, Xuereb JH, Love S (2005) Abeta-related angiitis: primary angiitis of the central nervous system associated with cerebral amyloid angiopathy. Brain 128:500–515
Shibata M, Yamada S, Kumar SR, Calero M, Bading J, Frangione B, Holtzman DM, Miller CA, Strickland DK, Ghiso J, Zlokovic BV (2000) Clearance of Alzheimer’s amyloid-ss(1–40) peptide from brain by LDL receptor-related protein-1 at the blood-brain barrier. J Clin Invest 106:1489–1499
Strittmatter WJ, Saunders AM, Schmechel D, Pericak-Vance M, Enghild J, Salvesen GS, Roses AD (1993) Apolipoprotein E: high-avidity binding to beta-amyloid and increased frequency of type 4 allele in late-onset familial Alzheimer disease. Proc Natl Acad Sci USA 90:1977–1981
Sumii T, Lo EH (2002) Involvement of matrix metalloproteinase in thrombolysis-associated hemorrhagic transformation after embolic focal ischemia in rats. Stroke 33:831–836
Surbek B (1961) L’ángiopathie dyshorique (Morel) de l’écorce cérébrale. Etude anatomo-clinique et statistique, aspect génétique. Acta Neuropathol (Berl) 1:168–197
Suzuki N, Iwatsubo T, Odaka A, Ishibashi Y, Kitada C, Ihara Y (1994) High tissue content of soluble beta 1–40 is linked to cerebral amyloid angiopathy. Am J Pathol 145:452–460
Thal DR, Ghebremedhin E, Rub U, Yamaguchi H, Tredici KD, Braak H (2002) Two types of sporadic cerebral amyloid angiopathy. J Neuropathol Exp Neurol 61:282–293
Thal DR, Ghebremedhin E, Orantes M, Wiestler OD (2003) Vascular pathology in Alzheimer disease: Correlation of cerebral amyloid angiopathy and arteriosclerosis/lipohyalinosis with cognitive decline. J Neuropathol Exp Neurol 62:1287–1301
Tian J, Shi J, Bailey K, Mann DM (2003) Negative association between amyloid plaques and cerebral amyloid angiopathy in Alzheimer’s disease. Neurosci Lett 352:137–140
Tian J, Shi J, Bailey K, Lendon CL, Pickering-Brown SM, Mann DM (2004) Association between apolipoprotein E e4 allele and arteriosclerosis, cerebral amyloid angiopathy, and cerebral white matter damage in Alzheimer’s disease. J Neurol Neurosurg Psychiatry 75:696–699
Tian J, Shi J, Bailey K, Mann DM (2004) Relationships between arteriosclerosis, cerebral amyloid angiopathy and myelin loss from cerebral cortical white matter in Alzheimer’s disease. Neuropathol Appl Neurobiol 30:46–56
Tian J, Shi J, Mann DM (2004) Cerebral amyloid angiopathy and dementia. Panminerva Med 46:253–264
Tomonaga M (1981) Cerebral amyloid angiopathy in the elderly. J Am Geriatr Soc 29:151–157
Uchihara T, Akiyama H, Kondo H, Ikeda K (1997) Activated microglial cells are colocalized with perivascular deposits of amyloid-beta protein in Alzheimer’s disease brain. Stroke 28:1948–1950
Van Dorpe J, Smeijers L, Dewachter I, Nuyens D, Spittaels K, Van Den Haute C, Mercken M, Moechars D, Laenen I, Kuiperi C, Bruynseels K, Tesseur I, Loos R, Vanderstichele H, Checler F, Sciot R, Van Leuven F (2000) Prominent cerebral amyloid angiopathy in transgenic mice overexpressing the london mutant of human APP in neurons. Am J Pathol 157:1283–1298
Vidal R, Frangione B, Rostagno A, Mead S, Revesz T, Plant G, Ghiso J (1999) A stop-codon mutation in the BRI gene associated with familial British dementia. Nature 399:776–781
Vidal R, Calero M, Piccardo P, Farlow MR, Unverzagt FW, Mendez E, Jimenez-Huete A, Beavis R, Gallo G, Gomez-Tortosa E, Ghiso J, Hyman BT, Frangione B, Ghetti B (2000) Senile dementia associated with amyloid beta protein angiopathy and tau perivascular pathology but not neuritic plaques in patients homozygous for the APOE-epsilon4 allele. Acta Neuropathol 100:1–12
Vinters HV (1987) Cerebral amyloid angiopathy. A critical review. Stroke 18:311–324
Vinters HV, Gilbert JJ (1983) Cerebral amyloid angiopathy: incidence and complications in the aging brain. II. The distribution of amyloid vascular changes. Stroke 14:924–928
Vinters HV, Secor DL, Pardridge WM, Gray F (1990) Immunohistochemical study of cerebral amyloid angiopathy. III. Widespread Alzheimer A4 peptide in cerebral microvessel walls colocalizes with gamma trace in patients with leukoencephalopathy. Ann Neurol 28:34–42
Vinters HV, Secor DL, Read SL, Frazee JG, Tomiyasu U, Stanley TM, Ferreiro JA, Akers MA (1994) Microvasculature in brain biopsy specimens from patients with Alzheimer’s disease: an immunohistochemical and ultrastructural study. Ultrastruct Pathol 18:333–348
Vinters HV, Wang ZZ, Secor DL (1996) Brain parenchymal and microvascular amyloid in Alzheimer’s disease. Brain Pathol 6:179–195
Vonsattel JP, Myers RH, Hedley-Whyte ET, Ropper AH, Bird ED, Richardson EP Jr (1991) Cerebral amyloid angiopathy without and with cerebral hemorrhages: a comparative histological study. Ann Neurol 30:637–649
Weisgraber KH (1994) Apolipoprotein E: structure-function relationships. Adv Protein Chem 45:249–302
Weller RO, Nicoll JA (2003) Cerebral amyloid angiopathy: pathogenesis and effects on the ageing and Alzheimer brain. Neurol Res 25:611–616
Weller RO, Kida S, Zhang ET (1992) Pathways of fluid drainage from the brain — morphological aspects and immunological significance in rat and man. Brain Pathol 2:277–284
Weller RO, Massey A, Newman TA, Hutchings M, Kuo YM, Roher AE (1998) Cerebral amyloid angiopathy: amyloid beta accumulates in putative interstitial fluid drainage pathways in Alzheimer’s disease. Am J Pathol 153:725–733
Weller RO, Massey A, Kuo YM, Roher AE (2000) Cerebral amyloid angiopathy: accumulation of A beta in interstitial fluid drainage pathways in Alzheimer’s disease. Ann N Y Acad Sci 903:110–117
Williams S, Chalmers K, Wilcock GK, Love S (2005) Relationship of neurofibrillary pathology to cerebral amyloid angiopathy in Alzheimer’s disease. Neuropathol Appl Neurobiol 31:414–421
Wisniewski HM, Wegiel J (1994) Beta-amyloid formation by myocytes of leptomeningeal vessels. Acta Neuropathol 87:233–241
Wisniewski HM, Frackowiak J, Zoltowska A, Kim KS (1994) Vascular β-amyloid in Alzheimer’s disease angiopathy is produced by proliferating and degenerating smooth muscle cells. Int J Exp Clin Invest:8–16
Wisniewski HM, Frackowiak J, Mazur-Kolecka B (1995) In vitro production of beta-amyloid in smooth muscle cells isolated from amyloid angiopathy-affected vessels. Neurosci Lett 183:120–123
Wisniewski HM, Wegiel J, Vorbrodt AW, Mazur-Kolecka B, Frackowiak J (2000) Role of perivascular cells and myocytes in vascular amyloidosis. Ann N Y Acad Sci 903:6–18
Xu D, Yang C, Wang L (2003) Cerebral amyloid angiopathy in aged Chinese: a clinico-neuropathological study. Acta Neuropathol 106:89–91
Yamada M (2000) Cerebral amyloid angiopathy: an overview. Neuropathology 20:8–22
Yamada M (2002) Risk factors for cerebral amyloid angiopathy in the elderly. Ann N Y Acad Sci 977:37–44
Yamada M, Tsukagoshi H, Otomo E, Hayakawa M (1987) Cerebral amyloid angiopathy in the aged. J Neurol 234:371–376
Yamada M, Itoh Y, Shintaku M, Kawamura J, Jensson O, Thorsteinsson L, Suematsu N, Matsushita M, Otomo E (1996) Immune reactions associated with cerebral amyloid angiopathy. Stroke 27:1155–1162
Yow H, Weller RO (2002) A role for cerebrovascular disease in determining the pattern of beta amyloid deposition in Alzheimer’s disease. Neuropathol Appl Neurobiol 28:149
Zarow C, Zaias B, Lyness SA, Chui H (1999) Cerebral amyloid angiopathy in Alzheimer disease is associated with apolipoprotein E4 and cortical neuron loss. Alzheimer Dis Assoc Disord 13:1–8
Zekry D, Duyckaerts C, Belmin J, Geoffre C, Moulias R, Hauw JJ (2003) Cerebral amyloid angiopathy in the elderly: vessel walls changes and relationship with dementia. Acta Neuropathol 106:367–373
Zhang ET, Inman CB, Weller RO (1990) Interrelationships of the pia mater and the perivascular (Virchow-Robin) spaces in the human cerebrum. J Anat 170:111–123
Zhang F, Eckman C, Younkin S, Hsiao KK, Iadecola C (1997) Increased susceptibility to ischemic brain damage in transgenic mice overexpressing the amyloid precursor protein. J Neurosci 17:7655–7661
Acknowledgements
I thank Prof. Charles Duyckaerts, Prof. Kurt Jellinger, Prof. Seth Love, and Prof. Roy Weller for critical comments during the past 2 years.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Attems, J. Sporadic cerebral amyloid angiopathy: pathology, clinical implications, and possible pathomechanisms. Acta Neuropathol 110, 345–359 (2005). https://doi.org/10.1007/s00401-005-1074-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00401-005-1074-9