Abstract
Purpose
Amyand’s hernia is a very rare type of hernia and is characterised by the presence of a vermiform appendix in the inguinal hernia sac. It may present as a tender inguinal or inguinoscrotal swelling, and is usually misdiagnosed as an irreducible or strangulated inguinal hernia. This is a presentation of our experiences with these unusual hernias.
Methods
This study conducted a retrospective analysis of 21 patients with Amyand’s hernias operated on at our institution between April 2007 and February 2011. The age and sex distributions of the patients, the types of hernias, and preoperative diagnostic tests were evaluated.
Results
Twenty patients were male (95.3 %) and one was female (4.7 %). The median age was 20.3 months (ranging from 2 months to 10 years). In nine patients, the conditions were diagnosed using ultrasonographic (USG) imaging preoperatively. Nine of the 21 patients underwent emergency operations. The 12 remaining patients were operated on after preparations were completed. The operative findings included 12 normal appendixes, five inflamed appendixes, one perforated appendix, and three hernias whose inner hernia sac surface was adhered to the appendix. Nine patients underwent inguinal hernia repair with appendectomy, and 12 patients had hernia repair without an appendectomy. Recurring hernias and appendicitis were not detected in any patients within the follow-up time.
Conclusions
Although a routine appendectomy is not required for a normal-looking appendix, in a case where the inflammatory status of the appendix adheres to the surface of the hernia sac, an appendectomy is required. We believe that USG examination in the diagnosis of Amyand’s hernias can provide additional contribution.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The first resection for appendicitis was conducted by Claudius Amyand’s in 1735. Since then, the presence of the vermiform appendix, whether inflamed or not, within a hernia sac has been known as an Amyand’s hernia (AH) [1, 2]. The diagnosis of AH is very difficult; it is often misdiagnosed as an irreducible or strangulated hernia [3]. Ultrasonography (USG) can be used if the appendix is suspected to be in the sac and/or the hernia is irreducible. We present our experiences in treating 21 patients with AHs. To our knowledge, this is the largest series of AHs ever reported from a single institution (Table 1).
Materials and methods
A total of 2,159 children with inguinal hernias were operated on at our hospital (Van Education and Research Hospital) between April 2007 and February 2011; 21 children diagnosed with AH were retrospectively examined. The age and sex distributions of the patients, the types of hernias, and the preoperative diagnostic tests used were evaluated. Sonographic groin examinations were performed using Logic7 sonographic equipment with a 7–14 MHz linear probe (General Electric, Milwaukee, WI, USA). Operative findings, surgical treatment techniques, histopathology reports, postoperative outcomes, duration of postoperative hospital stays, and postoperative follow-up periods were analysed.
Results
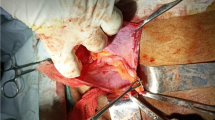
A total of 2,159 children with inguinal hernias were operated on, and in 21 of the patients, the appendix was found within the hernia sac (Fig. 1). The incidence of Amyand’s hernias in this study was 0.97 %. Twenty patients were male (95.3 %) and one was female (4.7 %). The median age was 20.3 months (ranging from 2 months to 10 years). Physical examination revealed swelling in the right groin with pain, tenderness, and an irreducible right inguinal hernia in all patients. Four patients had fevers over 38 °C. Vomiting and gastrointestinal symptoms of intestinal obstruction were noted in only one child. Four patients had leukocytosis, and their radiographic examinations were normal. Preoperative inguinal sonography was performed on 12 patients; the other nine patients did not receive preoperative USG. Nine of the twelve patients on whom preoperative inguinal sonography was performed were diagnosed with Amyand’s hernias. Appendectomies and hernia repairs were conducted in three of the nine patients who were diagnosed ultrasonographically; the remaining six patients were treated with hernia repair only. In all cases, the appendectomies and hernia repairs were conducted at the same time through inguinal transverse incisions. The operative findings included 12 normal AHs, five inflamed AHs (Fig. 2), one perforated AH, and three AHs whose internal hernia sac surface had adhered to the appendix. Twelve patients with normal appendixes that were reduced into the abdomen had hernia repair without an appendectomy. Histopathology confirmed acute appendicitis in five patients, and three appendixes had normal histopathology.
The last patient’s diagnosis was consistent with perforated appendicitis. The nine appendectomy patients were discharged in a median of 3 days; one patient with a perforated appendix was discharged on the 7 day after surgery, and the other patients (without appendectomies) were discharged the same day of surgery. Wound infection was seen in the case of the perforated appendix. Recurrent hernias and appendicitis were not detected in any patients within the follow-up time.
Discussion
Inguinal hernias are a common surgical problem that may surprise surgeons with their unusual sac contents. AHs constitute 1 % of all inguinal hernias, whereas only 0.1 % of all cases of appendicitis are present in cases with inguinal hernias [4, 5]. Our incidence of AH was 0.97 %, and the percentage of those with an inflamed appendix in the hernia sac was 0.27 %. A majority of the reported cases are presented with clinical features of an obstructed or strangulated inguinal hernia. Even with perforation, the systemic signs and symptoms of appendicitis are rarely evident [6–8]. Sharma et al. [9] reported 18 adult patients over a 15-year period, and the common symptom that patients experienced upon presentation was a painful inguinal or inguinoscrotal swelling (83 %). The presence of a low or high white blood cell count is not reliable for identifying AH [10]. In our series, only four (19.4 %) patients had fever and leukocytosis. Pain was seen in all cases. Tenderness with irreducible right inguinal hernia or swelling in the right inguinal area was observed in 28.5 and 71.4 % of patients, respectively.
Preoperative diagnosis prevents us from manipulation, provides information to patients’ parents about AHs and preoperatively prepares the surgeon for surgical management. Although a preoperative CT of the abdomen may be helpful in securing the correct diagnosis, this is not a routine practice after the clinical diagnosis of a complicated hernia [11]. Preoperative CT scan was not performed in our study because children are subjected to unnecessary radiation, also it has extra cost. Although USG is widely available, less expensive than other imaging methods and does not involve radiation, it is not necessary in all cases.
In a few studies, preoperative diagnoses of AH with ultrasonography is reported [12, 13] however, in majority of publications, it has not been reported [7, 8, 14]. We think that USG may be useful in cases in which there is a blind-ending tubular structure in the inguinal canal on physical examination. USG was performed on 12 (57.1 %) patients in our study, and AHs were diagnosed in nine patients using preoperative inguinal USG that revealed a blind-ending intestinal loop (Fig. 1). Surgeons must know about AHs and should inform radiologists of these issues.
We informed the radiologist to be aware of the presence of an AH before USG application in all patients who had the symptoms of right hernias and/or swelling. We think that this application can increase the frequency of radiologic diagnosis of AH.
The pathophysiology of appendicitis in the sac is still uncertain. The correlation between inflammation and the incarceration of the appendix has been demonstrated. Abu-Dalu and Urca suggested that as soon as the appendix enters the sac, it becomes vulnerable to trauma and retains three adhesions that result in its blood supply possibly being cut off or significantly reduced, resulting in inflammation and bacterial overgrowth [15]. Weber et al. [16] proposed that inflammatory swelling may lead to incarceration followed by impaired blood supply and bacterial overgrowth. The literature further suggests that the manipulation of a normal appendix may provoke secondary appendicitis [10, 17].
Although the laparoscopic approach could have been used [18], groin incision was preferred as the standard in our cases. Due to the potential for the later utility of an appendix (the appendix could be used for biliary tract reconstruction, urinary diversion, anterograde bowel enemas, etc.), many authors suggest that appendectomy should be avoided in the case of a normal vermiform appendix [3, 8, 19].
Conclusions
AH should be considered in the differential diagnosis in cases with clinical signs of complicated inguinal hernias. USG may be used to diagnose AH preoperatively. A radiologist who is informed preoperatively about AH can increase the frequency of radiologic diagnosis. The inflammatory status of the appendix adhered to the surface of the hernia sac dictates the surgical options.
References
D’Alia C, Lo Schiavo MG, Bonanno L et al (2003) Amyand’s hernia: case report and review of the literature. Hernia 7:89–91
Solecki R, Matyja A, Milanowski W (2003) Amyand’s hernia: a report of two cases. Hernia 7:50–51
Vermillon JM, Abernathy SW, Snyder SK (1999) Laparoscopic reduction of Amyand’s hernia. Hernia 3:159–160
Torres Hernández D, Roselló Fina JR, del Campo Abad R et al (2003) Hernia de Amyand: presentación de un caso y revisión de la literatura. Arch Cir Gen Dig 22
Logan MT, Nottingham JM (2001) Amyand’s hernia: a case report of an incarcerated and perforated appendix within an inguinal hernia and review of the literature. Am Surg 67(7):628–629
Hutchinson R (1993) Amyand’s hernia. JR Soc Med 86:104–105
Laermans S, Aerts R, De Man R (2007) Amyand’s hernia: inguinal hernia with acute appendicitis. JBR-BTR 90(6):524–525
Celik A, Ergün O, Ozbek SS (2003) Sliding appendiceal inguinal hernia: preoperative sonographic diagnosis. J Clin Ultrasound 31:156–158
Coulier B, Pacary J, Broze B (2006) Sonographic diagnosis of appendicitis within a right inguinal hernia (Amyand’s hernia). J Clin Ultrasound 34(9):454–457
Sharma H, Gupta A, Shekhawat N et al (2007) Amyand’s hernia: a report of 18 consecutive patients over a 15 year period. Hernia 11:31–35
Abu-Dalu J, Urca I (1972) Incarcerated inguinal hernia with a perforated appendix and periappendicular abscess. Dis Colon Rectum 15:464–465
Weber RV, Hunt ZC, Kral JG (1999) Amyand’s hernia: etiologic and therapeutic implications of two complications. Surg Rounds 22:552–556
Mullinax EJ, Alexander A, Avital I (2011) Laparoscopic appendectomy for Amyand’s hernia: a modern approach to a historic diagnosis. J Gastrointest Surg 15:533–535
Carey LC (1967) Acute appendicitis occurring in hernias: a report of 10 cases. Surgery 61:236–238
Bakhshi GD, Bhandarwar AH, Govilla AA (2004) Acute appendicitis in left scrotum. Indian J Gastroenterol 23(5):195
Lyass S, Kim A, Bauer J (1997) Perforated appendicitis in left scrotum: case report and review of literature. Am J Gastroenterol 92:700–702
Kueper MA, Kirschsniak A, Ladurner R et al (2007) Incarcerated recurrent inguinal hernia with covered and perforated appendicitis and periappendicular abscess: case report and review of the literature. Hernia 11(2):189–191
Milanchi S, Allins AD (2008) Amyand’s hernia: history, imaging, and management. Hernia 12(3):321–322
Livaditi E, Mavridis G, Christopoulos G et al (2007) Amyand’s hernia in premature neonates: report of two cases. Hernia 11:547–549
Kaymakci A, Akillioglu I, Akkoyun I et al (2009) Amyand’s hernia: a series of 30 cases in children. Hernia 13:609–612
Cankorkmaz L, Ozer H, Guney C et al (2010) Amyand’s hernia in the children: a single center experience. Surgery 147:140–143
Sulu B, İşler S (2010) Using the properties of Amyand’s hernia in children in the preoperative diagnosis: our experience and review of the literature. Turkish J Trauma Emer Sur 16(3):253–259
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Okur, M.H., Karaçay, Ş., Uygun, İ. et al. Amyand’s hernias in childhood (a report on 21 patients): a single-centre experience. Pediatr Surg Int 29, 571–574 (2013). https://doi.org/10.1007/s00383-013-3274-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-013-3274-z