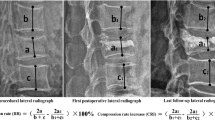
Abstract
The purpose of this study was to analyse the number and types of secondary fractures, and to investigate the impact of intradiscal cement leaks for adjacent vertebral fractures. Patients with osteoporotic vertebral fractures were treated with vertebroplasty. Results were documented and prospectively followed by means of computed tomography (CT) and magnetic resonance imaging. The frequency and the types of cement leakages were analysed from multiplanar CT images and secondary fractures were characterised as follows: (1) adjacent fracture in the immediate vicinity of an augmented vertebra; (2) sandwich fracture, fracture of an untreated vertebra between two vertebrae that had been previously augmented, and (3) distant fractures not in the vicinity of augmented vertebrae. A total of 385 osteoporotic vertebral fractures were treated in 191 patients (61 men, 130 women, age 70.7 ± 9.7 years). The overall rate of cement leaks was 55.6%, including all leaks detectable by CT. Intradiscal leaks through the upper, the lower, and both endplates occurred in 18.2%, 6.8%, and 2.6%, respectively. In 39 patients (20.4%), a total of 72 secondary fractures occurred: 30 adjacent fractures in 23 patients (12.0%) with a time to fracture of 2 months [median; 1.0/4.0 months, first/third quartile (Q1/Q3)]; 11 secondary sandwich fractures in 11 patients (5.8%) after 1.5 months (median; 0.25/7.5 months, Q1/Q3); and 31 distant fractures in 20 patients (10.5%) after 5 months (median; 2.0/8.0 months, Q1/Q3). Ten of 30 adjacent fractures occurred in the presence of pre-existing intradiscal cement leaks and 20 where there was no leakage. Six of 11 sandwich fractures occurred in the presence of intradiscal leaks (five leaks in both adjacent disc spaces, one leak in the lower disc space) and five where there was no leakage. The rate of secondary adjacent and non-adjacent fractures is quite similar and there is no specific impact of intradiscal leakages on the occurrence of adjacent secondary fractures. Adjacent fractures occur sooner than distant secondary fractures. Sandwich fractures are associated with specific biomechanical conditions, with a 37.9% fracture rate in sandwich constellations.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Vertebral fracture is a frequent complication of osteoporosis and might cause minor complaints or substantial local pain and impaired physical function, reduce quality of life, and an increased mortality rate [1, 2]. Vertebroplasty has emerged as a widely accepted modality [3–6]. However, there have been reports suggesting that the restored stiffness and strength of augmented vertebrae may provoke fractures in adjacent non-augmented vertebrae and that the presence of intradiscal cement leaks may trigger those fractures [7–9]. The purpose of the present study was to analyse the extraosseous cement leaks and their potential impact on secondary fractures by means of a computed tomography (CT)-based diagnosis. Furthermore, the study aimed to prospectively investigate whether and to what extent cement leaks in the proximate disc spaces propagate the occurrence of new, secondary fractures in the immediate vicinity of pre-treated vertebrae.
Materials and methods
The study protocol was approved by the institutional ethical committee; all patients gave written informed consent. Osteoporotic vertebral fractures with significant pain represented indications for vertebroplasty. The diagnosis was confirmed by magnetic resonance imaging (MRI), which depicts bone marrow edema even in the absence of or only incipient height loss. MRI was performed with a 1.5-Tesla system (Magnetom Vision, Siemens, Erlangen) or an open 0.2-Tesla system (Magnetom Open, Siemens, Erlangen) using sagittal short-tau inversion recovery (STIR) and T1-weighted spin echo sequences. Vertebral bodies proved positive for bone marrow edema when a signal increase was seen either diffuse or near the endplate in STIR sequences and a respective signal loss in the corresponding T1-weighted images. Vertebral fractures with height loss but no bone marrow edema were judged as old and consolidated fractures and were not indicated for treatment.
For the procedure, patients were in the prone position and under conscious sedation using Midazolam (2.5–5.0 mg i.v.) and Piritramid (7.0–15 mg i.v.). The intervention commenced with a standard CT scan using a four-row multislice CT scanner (Somatom, Volume Zoom, Siemens, slice 2 mm, collimation 4 × 1 mm, 330 mAs, 120 kV) and multiplanar reformatted images of the spine were acquired. A mobile C-arm fluoroscope was installed between the gantry and the base of the CT table. With this arrangement, cross-sectional imaging and lateral fluoroscopy could be alternated during the procedure. For CT fluoroscopy, the voltage and the current of the CT tube was reduced to 80 kV and 20 mAs.
After local anaesthesia the 10-G cannula of the vertebroplasty set (Cemento set, OptiMed, Ettlingen) was advanced and steered by means of CT fluoroscopy using the transpedicular access as standard in lumbar vertebrae and an intercostotransverse access in thoracic verterbae. Dorsolateral access was only used when the individual anatomy prohibited use of the standard access. The tip of the cannula was placed in the ventral third and in the midsagittal plane of the vertebral body. The PMMA cement was applied under alternating CT fluoroscopy and lateral fluoroscopy to maintain a good control of the cement distribution in both the in-plane cross-sectional and the lateral views. If the cement distribution was unfavourable, for example, into the basal vertebral or epidural veins, the injection was interrupted for 30–60 s until the cement had polymerized at this point and was subsequently continued. Depending on the cement distribution, the bevel cut of the needle was directed towards the contralateral or the ipsilateral half of the vertebral body so that, ultimately, cement was deposited in the middle and to some extent both lateral thirds of the vertebral body. If the cement filled only the ipsilateral half of the vertebral body, an additional contralateral access was used. The mandrin was put in the canula before pulling the canula out of the vertebra. The final result was documented immediately by multislice CT with the parameters mentioned above. All extraosseous cement deposits were analysed according to their source: (1) epidural venous plexus; (2) posterior vertebral wall; (3) neuroforamina; (4) anterior vertebral wall; (5) lateral vertebral wall; (6) upper endplate; (7) lower endplate; (8) both endplates; (9) paravertebral vessels; (10) pulmonary embolism; (11) access site. Every leak location was counted as separate event.
Follow-up consisted of clinical visits at 3, 6, and 12 months and yearly thereafter, and whenever the patient experienced discomfort or pain, and included MRI to look for new bone marrow edema. Secondary vertebral fractures were treated with an additional vertebroplasty and were included in the follow-up. The number and time to secondary fracture were analysed and classified as: (1) secondary adjacent fracture in the immediate vicinity of an upper or lower vertebral body that had been previously treated with vertebroplasty; (2) secondary sandwich fracture, i.e. secondary fracture of a vertebral body located in between two augmented vertebral bodies; (3) secondary distant fracture, more than one segment distant to previously cemented vertebrae (Fig. 1).
Statistical analysis
Statistical analysis was performed using SPSS for Windows, version 12. The quantitative descriptive data are given as mean and standard deviation. Time to secondary fracture is given as median and first and third quartile (Q1/Q2), since this distribution did not fulfill the criteria for a Gaussian distribution. The Kruskall-Wallis test was used to compare the times to fracture. P < 0.05 was considered statistically significant.
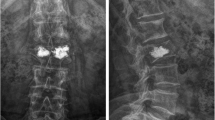
Secondary distant fracture. A 68-year-old female 3 months after vertebroplasty of B9 + 10. There is a secondary fracture with distance to the primary treatment locations at B7 with height loss of the anterior vertebral wall, bone marrow edema in STIR sequence (a) and the respective signal loss in T1-weighted (b). Saggittal reformations of CT demonstrates the augmented vertebrae B9 and 10 and a secondary fracture B7. There is some small cement leak through the upper endplate of B9 into the respective disc space (c). Treatment result after augmentation of B7 (d)
Results
From July 2002 to February 2006 191 patients (61 men, 130 women, age 70.7 ± 9.7 years, range 40–95) were treated with vertebroplasty. Patients entered the study upon occurrence and primary treatment of 317 vertebral fractures, with a mean number of 1.7 ± 0.9 [1–6] fractures per patient. During a follow-up of 19.7 ± 12.7 months (range 3–48), an additional 68 secondary fractures were treated in 39 patients (20.4%), resulting in a total of 385 vertebral bodies treated during 3½ years. The number of vertebrae treated per patient was 1.99 ± 1.25 (range 1–8), the number of interventions per patient and interventions per vertebra was 1.37 ± 0.78 (range 1–6) and 1.01 ± 0.12 (maximum 2 in five vertebrae), respectively. The distribution of all vertebrae treated is given in Table 1 and demonstrates a predominance at the thoracolumbar junction (Fig. 2a). The amount of PMMA cement was 4.8 ± 2.1 ml. However, there were few vertebrae with bilateral accesses in our early experience with a maximum of up to 14 ml cement per vertebra.
Distribution of secondary vertebral fractures. a Incidence and distribution of all vertebral fractures treated with predominance at the thoracolumbar junction. b Incidence and distribution of secondary adjacent fractures with similar distribution. c Location of all sandwich vertebrae after completion of the initial vertebroplasty. Secondary fractures of sandwich vertebrae that have been treated with vertebroplasty indicated in homogeneous dark grey. Secondary fractures of sandwich vertebrae that have not been treated indicated in grey hatching. d Incidence and distribution of secondary non-adjacent fractures
The overall cement leak rate was 55.6%. Every small volume leakage detectable with CT was counted (Table 2); single source leakages as well as complex combinations of leak sources. There were no differences between vertebrae with unilateral and bilateral accesses. The rate of intradiscal leaks through the upper, the lower and both endplates was 70 of 385 vertebrae (18.2%), 26 (6.8%), and 10 (2.6%), respectively. Compared with the pre-interventional VAS score of 7.8 ± 1.9 (6–10), complete pain relief was achieved at discharge from the hospital in 79 of191 patients (41.2%, VAS 1–3) and a significant improvement such that the dose of analgesics could be reduced in 104 of 191 (54.5%, VAS 4–6). However, in seven patients (3.7%) the treatment effect was inconclusive; one patient (0.5%) presented with repeated vertebral fractures under steroid medication because of vasculitis.
After primary treatment, a total of 72 secondary fractures (22.7% of all primary treated) occurred in 39 patients (20.4%) within 3 months (median; 1.5/6.25 months, Q1/Q3, range 1–22): 30 secondary fractures adjacent to pre-treated vertebral bodies, 11 secondary sandwich fractures, and 31 secondary fractures at some distance to pre-treated vertebrae. In some patients, a combination of more than one secondary fracture occurred.
Secondary adjacent fractures
Thirty secondary fractures (9.5% of all primary treated) occurred in 23 patients (12.0%) adjacent to vertebral bodies that had previously been treated with vertebroplasty. The time to fracture was 2 months (median, range 1 week to 16 months), The distribution is analogous to that of the primary fractures (Fig. 1b). Overall, 66.7% of adjacent fractures (n = 20) occurred in the absence of any cement deposits in adjacent discs whereas 33.3% (n = 10) occurred in cases with pre-existing cement leaks in the adjacent disc spaces from previous procedures. Thirteen of 30 adjacent fractures (43.3%) occurred in the upper vertebral bodies, six of them without any cement leak in the disc spaces and seven with intradiscal cement leaks from an upper endplate leak during the previous procedure (disc space below). Another 17 secondary adjacent fractures (56.7%) occured in lower adjacent vertebrae, 14 of them without and three with an intradiscal cement deposit from the previously treated vertebra (Table 3).
Secondary sandwich fractures
After the initial vertebroplasty, a total of 29 sandwich situations resulted in 26 patients. In these cases, one vertebral body was left untreated, whereas the two adjoining vertebrae had been treated with vertebroplasty because of fracture. Secondary fractures occurred in 11 of 29 sandwich vertebrae (3.5% of all primary treated, 37.9% of sandwich vertebrae) after 1.5 months (median, range 1 week to 12 months) and could appear at any level with sandwich vertebrae (Fig. 2c). In five cases (45.5%), the secondary fracture occurred in the presence of cement leaks in both adjoining disc spaces, one fracture (9.1%) occurred in the presence of a cement deposit in the lower disc space (Table 3). Seven sandwich fractures were treated with vertebroplasty because of severe complaints; four vertebral fractures were treated conservatively because of only minimal complaints and no significant height loss.
Secondary distant fractures
Additionally, 31 secondary distant fractures (9.8% of all primary treated) occurred in 20 patients (10.5%) during follow-up with distance to pre-treated vertebral bodies. The median time to fracture was 5 months (range 1 week to 22 months). The distribution of these fractures was seen predominantly in the middle of the thoracic and lumbar spine (Fig. 2d, Table 3).
Discussion
Vertebral fractures often occur in elderly patients with osteoporosis and might present either with minimal symptoms or cause substantial pain, diminish quality of life, and result in a secondary kyphosis. Patients with osteoporotic vertebral compression fracture are at substantial risk of sustaining additional fractures within 1 year, at an incidence of 19.2%, and this risk increases with respect to the number of vertebral fractures at baseline [1]. Moreover, osteoporotic fractures have been associated with an increased mortality rate in prospective cohort studies [2]. Percutaneous vertebroplasty is widely used and provides long-term benefit in terms of pain relief, increased activity, and decreased analgesic drug consumption in patients with osteoporotic vertebral fractures both at single and multiple fracture levels [3–5, 10, 11]. Diamond et al. [11] compared the clinical benefit of vertebroplasty with conservative treatment and demonstrated a significant benefit of vertebroplasty in terms of pain relief, reduction of hospital stay, and physical activity during the first 6 weeks and no differences with respect to new vertebral fractures or death during follow-up during 24 months. Berlemann et al. and others suggested that the stiffness and strength of such vertebral bodies may provoke fractures in adjacent, non-augmented vertebrae [1, 2, 7, 8].
This prospective study gives a detailed insight into the frequency and the sources of extraosseous cement leaks based on CT diagnosis and analyses the rates of secondary fractures and the association with pre-existing intradiscal leakages. The rate of 55.6% extraosseous cement leakage was CT-based without clinical complications and no need for emergency surgery. Intraspinal leaks included those caused by cement spreading to the epidural veins (15.3%) and direct leaks through fracture lines in the posterior vertebral walls (2.3%). Since cement in epidural veins filled the pre-existing anatomical structure of the venous plexus, such leaks did not reduce or compress the dural sac. However, cement polymerization is accompanied with heat effects that might possibly affect the dural structures. CT fluoroscopy could help detect unintended cement distribution at an early stage and thereby contributes to safety so that cement injection can be interrupted betimes. The same applies for direct leaks through the posterior wall, which might not be covered by ligamentous structures or vessel walls and therefore might directly affect the dural structure. In agreement with findings reported in the literature, those clinical complications are fortunately rare and emergency surgery has been reported to be below 1% [12, 13].
In the present study, the overall rate of intradiscal leaks was 27.5% and covered leaks into the upper intradiscal space (18.2%), the lower intradiscal space (6.8%), and both (2.6%). Intradiscal cement leakage is a controversial issue in terms of the particular risk for secondary fractures. Such leaks might occur through fractured endplates or vacuum clefts or may result from iatrogenic endplate perforations with the needle tip. They have not negatively affected patient satisfaction with the procedure with respect to pain, ambulation status, and activity level [14]. Vacuum clefts indicate motion and non-union at the fracture site. They occur in up to 39% predominantly elderly men and may substantially affect the cement distribution with solid cement pattern [15, 16]. Krauss et al. [17] reported an overall cement leakage rate of 18.2% in cases with intravertebral clefts compared with 46% in the non-cleft fractures and a significantly improved reduction of the kyphosis angle in the presence of clefts. In our study, intravertebral clefts often took up greater amounts of cement and resulted in a significant fracture reduction. The amount of cement was therefore relatively high in such individual cases; however, in the whole collective the overall amount was significantly lower. Smaller amounts have been suggested to be sufficient for pain treatment and vertebral stabilization [18].
Cement leakages occur in both vertebroplasty and kyphoplasty. Pflugmacher et al. [19] reported overall cement leak rates of 14.2% and 18.7%, respectively, and a better height restoration for kyphoplasty over 1 year. The rates of intradiscal leakages were three of 35 in the kyphoplasty group (8.6%) and two of 32 in the vertebroplasty group (6.3%). In this study, the radiological work-up was performed with conventional X-ray only. However, comparative studies have demonstrated much higher leak rates in CT scans [20, 21]. In a CT-controlled study with 101 vertebral fractures, the overall leakage rate was 48.8% in vertebroplasty and 57.9% in kyphoplasty, with an intradiscal leak rate of 20.7% and 42.1%, respectively [22]. This is consistent with our data and is due to the fact that CT counted every small leak that would not have been detected by conventional X-ray. Therefore, leak rates should not be compared between studies without mentioning the method of leak detection. There have been various reports on techniques for leak rate reduction in vertebroplasty [23, 24]. Using a Fogarty balloon inflation for hole creation, Schulte et al. [24] reported epidural cement leaks in 9.1% and intradiscal leaks in 10.6%. The authors reported balloon ruptures in seven of 66 procedures but no clinical complications. Bhatia et al. [25] attempted to prevent cement leaks by routine gelfoam embolization of venous channels before cementation and reported an overall leak rate of 22.5%. Those data have to be confirmed in a larger number of patients before recommending widespread use.
Secondary fractures of adjacent vertebrae
Clinical and experimental reports have suggested that augmented vertebrae might trigger secondary adjacent fractures, particularly because the cement rigidity reduces the local spinal flexibility and increases the intradiscal pressure [26]. Komemushi et al. [7] reported an increased risk of adjacent vertebral fractures in the presence of intradiscal cement leakages; however, other factors—e.g., the amount of cement injected, the number of vertebrae treated—were not associated with an increased risk. In contrast, Kayanja et al. [27] investigated the biomechanics of multilevel segments of cadaveric human spines. The spine segments were augmented at different levels and numbers of vertebrae and were tested in a dedicated materials testing machine. In this multilevel segment model, the fracture occurrence was independent of the distribution of the augmented vertebrae within the spine segment [27]. Our data demonstrated an overall rate of 22.7% secondary vertebral fractures in 20.4% of patients. Of secondary fractures, 41.7% occurred in the immediate vicinity of pre-treated vertebrae, two-thirds of which occurred in the absence of intradiscal leaks compared with one third with intradiscal leakages. The median time to fracture was 2 months and was significantly earlier compared with distant fractures. This is consistent with Syed et al. [28], who reported a total of 41 adjacent fractures among all 78 secondary fractures (52.5%), with 13 of 41 (31.7%) adjacent fractures occurring in the presence of pre-existing intradiscal cement leaks. Moreover, 37 secondary fractures (47.4%) occurred in non-adjacent locations, which is analogous to our results. Similar results have been reported by Trout et al. [29], who analysed 186 secondary vertebral fractures in 86 (19.9%) of 423 patients. These authors also demonstrated a 41.4% rate of adjacent fractures with a shorter time to fracture compared with non-adjacent fractures. Tanigawa et al. [8] reported 56 secondary vertebral fractures in 28 of 76 patients (36.8%) with a slightly increased number of 38 adjacent fractures (67.9%), 17 non-adjacent fractures (30.4%), and one new fracture in a pre-treated vertebra (1.8%). In concordance with Syed et al. and Trout et al., our data do not suggest an increased risk for adjacent fractures compared to non-adjacent but confirmed a significantly shorter time to fracture in adjacent locations.
Sandwich situations and secondary fractures of sandwich vertebrae
This specific situation obviously results in a particular load of the untreated vertebra in between because of the stiffening and the loss of vertical elasticity of the two proximate vertebrae. Our data demonstrated secondary fractures in 37.9% of sandwich vertebrae with a very short time to fracture. However, secondary fractures did not develop in two thirds of those situations, meaning that the anatomical situation must not be the only precondition for triggering secondary sandwich fractures. There are only a few reports focusing on this specific constellation. Komemushi et al. [7] investigated the predictors of secondary fractures and stated explicitly that the presence of a single untreated vertebra between augmented vertebrae was not associated with an increased secondary fracture rate and equivocal data have been reported from experimental studies [27]. In our study, the secondary fracture rate was increased, which might be explained by the presence of intradiscal leakages that could have influenced the specific load of the failed sandwich vertebra.
In summary, we conclude that the rate of secondary adjacent and non-adjacent fractures is quite similar after vertebroplasty and that intradiscal leakage does not have a specific impact on the occurrence of adjacent secondary fractures. However, adjacent fractures occur significantly sooner during follow-up. Sandwich fractures are associated with specific biomechanical conditions and an increased secondary fracture rate. However, two-thirds of sandwich vertebrae do not fail during follow-up.
References
Lindsay R, Silverman SL, Cooper C, Hanley DA, Barton I, Broy SB, Licata A, Benhamou L, Geusens P, Flowers K, Stracke H, Seeman E (2001) Risk of new vertebral fracture in the year following a vertebral fracture. JAMA 285:320–323
Kado DM, Browner WS, Palermo L, Nevitt MC, Genant HK, Cummings SR (1999) Vertebral fractures and mortality in older women. Arch Intern Med 159:1215–1220
Debussche-Depriester C, Deramond H, Fardellone P (1991) Percutaneous vertebroplasty with acrylic cement in the treatment of osteoporotic vertebral crush fracture syndrome. Neuroradiology 33(Suppl):149–152
Deramond H, Depriester C, Galibert P, Le Gars D (1998) Percutaneous vertebroplasty with polymethylmethacrylate: technique, indications, and results. Radiol Clin North Am 36:533–546
Gangi A, Dietmann JL, Guth S, Steib JP, Roy C (1999) Computed tomography (CT) and fluoroscopy-guided vertebroplasty: results and complications in 187 patients. Semin Intervent Radiol 16:137–142
Alvarez L, Alcaraz M, Perez-Higueras A, Granzio JJ, deMiguel I, Rossi RE, Quinones D (2006) Percutaneous vertebroplasty: functional improvement in patients with osteoporotic compression fractures. Spine 31:1113–1118
Komemushi A, Tanigawa N, Kariya S, Kojima H, Shomura Y, Komemushi S, Sawada S (2006) Percutaneous vertebroplasty for osteoporotic compression fracture: multivariate study of predictors of new vertebral body fracture. Cardiovasc Interv Radiol 29:580–585
Tanigawa N, Komemushi A, Kariya S, Kojima H, Shomura Y, Sawada S (2006) Radiological follow-up of new compression fractures following percutaneous vertebroplasty. Cardiovasc Interv Radiol 29:92–96
Berlemann U, Ferguson SJ, Nolte L-P, Heini PF (2002) Adjacent vertebral failure after vertebroplasty. J Bone Joint Surg (Br) 84-B:748–752
Singh AK, Pilgram TK, Gilula L (2006) Osteoporotic compression fractures: outcomes after single-versus multiple-level percutaneous vertebroplasty. Radiology 238:211–220
Diamond TH, Bryant C, Browne L, Clark WA (2006) Clinical outcomes after actue osteoporotic vertebral fractures: a 2-year non-randomised trial comparing percutaneous vertebroplasty with conservative therapy. Med J Aust 184:113–117
Hochmuth K, Proschek D, Schwarz W et al (2006) Percutaneous vertebroplasty in the therapy of osteoporotic vertebral compression fractures: a critical review. Eur Radiol 16:998–1004
Guglielmi G, Andreula C, Muto M et al (2005) Percutaneous vertebroplasty: indications, contraindications, technique, and complications. Acta Radiol 46:256–268
Mirovsky Y, Anekstein Y, Shalmon E, Blankstein A, Peer A (2006) Intradiscal cement leak following percutaneous vertebroplasty. Spine 31:1120–1124
Mirovsky Y, Anekstein Y, Ahalmon E, Peer A (2005) Vacuum clefts of the vertebral bodies. AJNR Am J Neuroradiol 26:1634–1640
Oka M, Matsusako M, Kobayashi N, Uemura A, Numaguchi Y (2005) Intravertebral cleft sign on fat-suppressed contrast-enhanced MR. Correlation with cement distribution pattern on percutaneous vertebroplasty. Acad Radiol 12:992–999
Krauss M, Hirschfelder H, Tomandl B, Lichti G, Bar I (2006) Kyphosis reduction and the rate of cement leaks after vertebroplasty of intravertebral clefts. Eur Radiol 16:1015–1021
Kaufmann TJ, Trout AT, Kallmes DF (2006) The effects of cement volume on clinical outcomes of percutaneous vertebroplasty. AJNR Am J Neuroradiol 27:1933–1937
Pflugmacher R, Kandziora F, Schröder R, Schleicher P, Scholz M, Schnake K, Haas N, Khodadadyan-Klostermann C (2005) Vertebroplasty and kyphoplasty in osteoporotic fractures of vertebral bodies—a prospective 1 year follow-up analysis. Rofo 177:1670–1676
Mousavi P, Roth S, Finkelstein J, Cheung G, Whyne C (2003) Volumetric quantification of cement leakage following percutaneous vertebroplasty in metastatic and osteoporotic vertebrae. J Neurosurg 99:56–59
Schmidt R, Cakir B, Mattes T, Wegener M, Puhl W, Richter M (2005) Cement leakage during vertebroplasty: an underestimated problem? Eur Spine 14:466–473
Weber CH, Krötz M, Hoffmann R-T, Euler E, Heining S, Pfeiffer K-J, Reiser M, Linsenmaier U (2006) CT-guided vertebroplasty and kyphoplasty: comparing technical success rate and complication in 101 cases. Fortschr Röntgenstr 178:610–617
Vallejo R, Benyamin R, Floyd B, Casto JM, Joseph NJ, Mekhail N (2006) Percutaneous cement injection into a created cavity for the treatment of vertebral body fracture: preliminary results of a new vertebroplasty technique. Clin J Pain 22:182–189
Schulte BU, Brucher D, Trompeter M, Remy C, Reimer P (2006) Balloon-assisted percutaneous vertebroplasty in patients with osteoporotic vertebral body compression fractures—first results. Rofo 178:207–213
Bhatia C, Barzilay Y, Krishna M, Friesem T, Pollock R (2006) Cement leakage in percutaneous vertebroplasty: effect of preinjection gelfoam embolization. Spine 31:915–919
Baroud G, Bohner M (2006) Biomechanical impact of vertebroplasty. Postoperative beiomechanics of vertebroplasty. Jt Bone Spine 73:144–150
Kayanja MM, Schlenk R, Togawa D, Ferrara L, Lieberman I (2006) The biomechanics of 1, 2, and 3 levels of vertebral augmentation with polymethylmethacrylate in multilevel spinal segments. Spine 7:769–774
Syed MI, Patel NA, Jan S, Harron MS, Morar K, Skaikh A (2005) Intrasdiskal extravasation with low-volume cement filling in percutaneous vertebroplasty. AJNR Am J Neuroradiol 26:2397–2401
Trout AT, Kallmes DF, Kaufmann TJ (2006) New fractures after vertberoplasty: adjacent fractures occur significantly sooner. AJNR Am J Neuroradiol 27:217–223
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pitton, M.B., Herber, S., Bletz, C. et al. CT-guided vertebroplasty in osteoprotic vertebral fractures: incidence of secondary fractures and impact of intradiscal cement leakages during follow-up. Eur Radiol 18, 43–50 (2008). https://doi.org/10.1007/s00330-007-0694-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-007-0694-y