Abstract
Our objective was to retrospectively evaluate the ability of multidetector-row computed tomography (MDCT) to detect previous myocardial infarctions (MIs) and to correlate necrosis with the status of coronary arteries supplying the infarcted territory. After having clinically evaluated 187 patients referred for ECG-gated MDCT of the coronary arteries, 30 previous MIs were identified in 29 patients (9 recent and 21 chronic). MDCT data were evaluated qualitatively and quantitatively by measuring attenuation values and wall thickness within the infarcted region and normal adjacent myocardium. Each MI was also assigned to the distribution territory of a coronary vessel, and morphological data were combined with MDCT angiographic findings. MDCT was able to detect 25/30 MIs showing an overall sensitivity and specificity of 83 and 91%, respectively. Quantitative analysis revealed a statistically significant difference in attenuation values between normal and infarcted regions (38.9±14 HU vs. 104.0±16 HU). Regional wall thinning was observed in chronic MIs (4.1±2 mm vs. 10.5±3.8 mm), and not in patients with recent event (7.9±1.6 mm vs 9.1±4 mm). In 22/25 cases, MDCT angiographic findings showed the presence of suspicious critical lumen narrowing (n=3), previous coronary stenting (n=14) and surgical revascularization (n=5) in the infarct-related coronary. During a single examination, MDCT might provide comprehensive imaging of MI offering a combined morphological and angiographic assessment.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The development of multi-detector row technology combined with retrospective electrocardiographic (ECG) gating has radically changed the role of computed tomography (CT) in cardiac imaging [1–3]. In comparison with conventional or single-slice spiral CT, not only the acquisition time is markedly decreased, but also spatial resolution on the z-axis is substantially improved, enabling non-invasive assessment of the coronary artery anatomy, detection of arterial stenosis and evaluation of left ventricular function (LV) [4–6].
Moreover, by using retrospective ECG gating, CT data and ECG information are recorded simultaneously, and images are successively reconstructed in the diastolic phase, virtually “freezing” the cardiac cycle and minimizing the presence of motion artifacts [7–9].
Thanks to the high spatial and temporal resolution achievable, this method allows not only non-invasive assessment of the coronary arteries, but also provides excellent information concerning myocardial morphology, having the potential to depict regional changes of the density and/or thickness of the LV wall with high diagnostic accuracy [10, 11].
Early studies with electron-beam CT (EBCT ) and single-slice spiral CT have already shown that acute myocardial infarction can be identified as a region of lower attenuation within the normal enhanced myocardium [12, 13]. More recently, multi-detector CT angiography (MDCTA) has been shown to have the potential to identify acute subendocardial and subacute myocardial necrosis [14–16]. Detection of the scar with MDCTA is potentially relevant since information about localization and extension of the necrotic area might be combined with non invasive angiographic findings providing insight into the morphological and hemodynamic significance of a coronary lesion, i.e., into the direct relation between the status of a coronary artery and its dependent myocardial region. The purpose of this study was to evaluate retrospectively the ability of MDCTA in detecting myocardial infarction in a group of patients referred for MDCTA of the coronary arteries and to correlate the presence of necrosis with non-invasive MDCT angiographic findings.
Materials and methods
Study population and clinical assessment
One hundred eighty-seven consecutive patients (140 ♂ and 47 ♀ age range: 32–77 years, mean 58.7 years) referred to our Department for MDCTA of the coronary arteries in the period between September 2003 and October 2004 were retrospectively evaluated for the presence of a previous myocardial infarction (MI). Clinical indications for the MDCTA examination were the following:
-
1)
Typical (n=29) or atypical chest pain (n=47)
-
2)
Cardiovascular risk factors (n=39)
-
3)
Previous coronary percutaneous transluminal angioplasty (PTA) and stent placement (n=48 with a total number of 65 stents)
-
4)
Previous coronary artery by-pass surgery (CABG) (n=24)
In all cases detailed clinical, serological, and ECG data were collected, and the diagnosis of previous MI was established according to the redefined criteria of the Joint European Society of Cardiology and American College of Cardiology Committee [17].
Acute or recent MI (event occurred<1 month before MDCT examination) was diagnosed if the patient had a typical rise and gradual fall of the biochemical markers of myocardial necrosis (troponin or CK-MB) associated with at least one of the following:
-
1)
Development of pathologic ECG Q waves
-
2)
ECG changes indicative of ischemia
-
3)
Ischemic symptoms
-
4)
Previous coronary artery interventions (coronary stenting or CABG)
For the patients with chronic MI (event occurred ≥1 month before MDCT examination), clinical diagnosis was satisfied according to the following criteria:
-
1)
History of previous myocardiial infarction
-
2)
Presence of pathologic Q waves on serial ECGs with or without previous clinical symptoms
-
3)
Normalized biochemical markers of myocardial necrosis.
MDCT protocol
In all patients, MDCTA examinations were performed using a four-row spiral CT scanner (Siemens Volume Zoom, Forcheim, Germany) with 0.5-s gantry rotation time and retrospective ECG gating. The acquisition protocol used in our Department for MDCTA of the coronary arteries included a preliminary unenhanced scan followed by a post-contrast acquisition performed with the following parameters: 400 mAs, 120 Kv, collimation 4×1 mm, with a slice thickness of 1.25 mm, and recon increment of 0.8 mm covering a volume included from the base of the heart to the tracheal carena, with an acquisition time of about 32–40 s. In 138 patients with a heart rate greater than 65 beats per minute (bpm), 5 mg of Propanolol (Inderal, Astra Zeneca) was intravenously administered 15–20 min prior to the examination. The mean heart rate during the examination was 62 (range 51–78 bpm).
Patients referred for assessment of coronary artery by-pass graft (CABG) were studied with a larger collimation and slice thickness (4×2.5 mm and 3 mm respectively) due to the larger volume to cover, included from the proximal to the distal CABG anastomosis. No delayed enhancement acquisitions were available in any patient. In all patients, a standard volume of 130 ml of high concentration contrast agent (Iomeron 400, Bracco, Milano, Italy) was administered at a flow rate of 4 ml, and delay based on a test bolus protocol. After acquisition, each exam was reconstructed with a temporal window of 40, 50, 60 and 70% of the R-R interval.
Image analysis
After clinical assessment, images were analyzed by two experienced cardiovascular radiologists in consensus, blinded to the clinical data, using a dedicated workstation with VR (volume rendering), MIP (maximum intensity projection) and MPR (multiplanar reformatting) capabilities (Vitrea 3.1; Vital Images, Minneapolis, Minn.). The myocardium was only evaluated in the end-diastolic phase, defined as the available R-R reconstruction interval with the largest ventricular cavity. Data sets were first visualized in the axial view and then reconstructed in the cardiac short axis (SA) and horizontal (HLA) and vertical long axis (VLA) planes using an MPR algorithm; when necessary, other reconstruction planes with different algorhythms were interactively selected by the readers. Images were analyzed qualitatively and quantitatively.
According to previous studies, infarcted area was visually defined as a region of lower attenuation and/or wall thinning within the normally enhanced surrounding myocardium [14–16].
When the necrotic area was identified after visual analysis, differences in the attenuation values between normal and necrotic myocardial tissue were also measured by using standard region of interest (ROI) of about 10 mm2 placed within the perfusion deficit and the contiguous normal areas. Myocardial wall thickness of each infarcted region was also measured in the end-dyastolic phase from the SA images and compared with the thickness of the adjacent normal myocardium. All quantitative measurements (attenuation values and wall thickness) were made in three different points for either normal or infarcted areas, and the average values obtained were used for statistical analysis. Finally, the location of each detected MI within left ventricular myocardium was defined using a 17-segment model in the cardiac short axis as recently suggested by the AHA [18]. According to the segments involved, infarcts were subsequently divided into three different groups depending on the distribution territories of the major coronary arteries [territory A: left anterior descending artery (LAD); territory B: left circumflex (Cx); territory C: right coronary artery (RCA). Territory-dependent coronary arteries were analyzed in all the available reconstruction phases (40–70%) in order to confirm the correlation between the status of the vessel and its related myocardial region [18].
Statistical analysis
After MDCTA analysis, all results were compared with the clinical data. Results of the quantitative analysis are expressed as the mean ±SD. Analysis of the variance was performed using a paired Student’s t test in order to identify significant differences in attenuation values and end-diastolic wall thickness between the normal and infarcted regions. A P<0.05 was considered to indicate a statistically significant difference.
Results
Prevalence, age and localization of infarctions
After clinical assessment, the presence of a previous MI was found in 29 patients (15.5% of the population). A total of 30 MIs were clinically identified: 20 infarcts were assigned to the distribution territory of the LAD (territory A), 1 to the Cx (territory B), 7 to the RCA (territory C) and 1 patient had a double anterior and inferior apical MI, which was assigned to the RCA and LAD coronary arteries territories (territories A–C). Localization of MI in all patients is reported in detail in Table 1. The mean interval between the acute event and MDCTA examination was 210±63 days; nine infarcts (30%) were classified as recent (mean 20±5 days), and 21 infarctions (70%) were chronic (mean 311±96 days). In 3/30 cases (10%) an anterior non-Q infarction was diagnosed.
Visual analysis results
After visual analysis, MDCTA was able to detect the presence of MI in 25/30 cases (diagnostic accuracy of 91%), showing a regional hypoattenuation of the myocardium and/or wall thinning (Fig. 1). Five false-negative and 12 false-positive cases were recorded, resulting in an overall sensitivity and specificity of 83 and 91%, respectively; the method showed a negative predictive value for the presence of a previous MI of 97% and a positive predictive value of 68%.
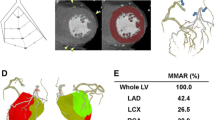
Comprehensive imaging of acute myocardial infarction in a 54-year-old man. The infarcted region appears as a thinned, hypoattenuated rim within the normally enhanced myocardium (a).Multiplanar reformations on cardiac short axis and vertical long axis planes show the precise longitudinal and 50% transmural extension of necrosis involving the antero-septal wall in the mid-apical part of the left ventricle (arrows) (b–c). In the same patient, MDCT angiographic findings reveal the presence of a critical stenosis in the mid part of the infarct-related coronary artery (LAD) (arrow heads) (c)
The five false-negative cases were attributed in three cases (one acute MI; two chronic MI), to the presence of sub-endocardial anterior MIs not visually detectable by MDCT and in two cases (two chronic inferior infarctions) to the presence of motion artifacts due to fast heart rate (78 and 71 bpm), which affected image quality and impeded detection of the myocardial scar.
Assessment of transverse images enabled diagnosis in 18/21 anterior MIs: 0/1 lateral and 1/8 inferior. Detection of 1/1 lateral (territory B) and 5/8 inferior (territory C) MIs was achievable only after reconstruction of the images in the cardiac short axis and vertical long axis planes using MPR algorithms (Fig. 2).
Chronic myocardial infarction in a 68-year-old woman. Multiplanar reformation on cardiac short axis (a) and vertical long axis (b) show the presence of a large necrotic area located in the antero-lateral wall of the left ventricle. The infarcted segments are not clearly depicted on conventional transverse images (c)
Quantitative analysis results
Quantitative analysis showed a statistically significant (P<0.01) difference in attenuation values between the normal (104.0±16 HU) and infarcted regions (38.9±14 HU) in post-contrast acquisition images. No statistically significant differences (P=0.61) were found in attenuation values between acute and chronic infarctions (Fig. 3a). Regional wall thinning was observed in 17/21 (80.9%) subjects with chronic MI (mean thickness 4.1±2 mm vs 10.5±3.8 mm P<0.01); in 9/9 (100%) patients with recent onset of MI no significant differences in wall thickness were found between the normal and infarcted regions (mean thickness 7.9±1.6 mm vs 9.1±4 mm P=0.078) (Figs. 3b, 4, 5). Attenuation values were also measured at the level of territories presumably infarcted on the basis of clinical data in the five false negative cases, showing no significant differences between these regions and the surrounding myocardium.
Graphs showing the differences in the attenuation values (a) and left ventricular wall thickness (b) between normal and infarcted regions in patients with recent (<1 month) and non-recent (>1 month) event. The infarcted segments show significantly lower attenuation values as compared with normal myocardium (a); however, a cut-off value to discriminate between acute and chronic infarctions cannot be found. Left ventricular wall thinning in the infarcted regions is exclusively observed in patients with chronic infarctions (b)
MDCT angiography in a 46-year-old man with previous double coronary stenting on LAD (arrows) (a). Assessment of transverse images reveals the presence of a small, transmural myocardial infraction in the distribution territory of the coronary vessel (b). Stents (arrows) and infarcted area (circle) are also visualized on volume rendering reconstruction (c)
Quantitative analysis was also performed in the 12 false-positive infarctions, revealing significant differences in the attenuation values between normal (93±21 HU) and presumably infarcted regions (51.6±16 HU) (P<0.01); wall thinning was not observed in these cases (mean thickness 6.8±2.5 mm vs. 11.1±1.9 mm P=0.074)
Infarcted regions and non-invasive angiographic findings
In 22/25 detected infarctions, MDCT angiographic findings were perfectly compatible with the localization of the necrotic area.
Assessment of the infarct-related coronary arteries revealed the presence of vessel lumen narrowing suspicious for critical stenosis in 3 cases, previous coronary stenting in 14 cases and surgical revascularization with coronary artery by-pass graft (CABG) in 5 (Figs. 1 and 4). In three cases, the presence of motion artifacts (n=2) and severe coronary calcifications (n=1) impaired image quality, and images of the coronary arteries were considered not diagnostic. For false-positive MIs (n=12) assessment of the apparent territory-dependent coronary artery showed the following findings: a previous CABG and coronary stenting was identified respectively in four and two cases and suspicious lumen narrowing was found in one case. In three MIs, no significant angiographic findings were identified and image assessment was not possible in one case, due to the poor image quality of the available data.
Discussion
Recently, a few clinical studies have evaluated the usefulness of MDCTA in detecting previous MIs. [16, 19]. After having occasionally observed several myocardial infarctions during MDCTA examinations of the coronary arteries, we became aware that the method might provide information not only on the status of a coronary vessel, but also, at the same time, on the coronary-dependent myocardial territories [16]. It already has been shown that MDCTA has the potential to depict accurately not only the infarct localization, but also to quantify infarct size on a porcine model of complete coronary occlusion [20]. In the present study, we aimed to systematically investigate the feasibility of ECG-gated MDCTA in detecting MI, and to correlate the localization of necrosis with non-invasive angiographic findings considering retrospectively a population of subjects with a previous clinical indication for MDCTA of the coronary arteries. The results of this study demonstrate that MDCTA with retrospective ECG gating enables the detection of previous MIs with high diagnostic accuracy (91%). This finding is clinically relevant since the presence of previous MIs seems to be not uncommon in patients with a clinical indication for MDCTA of the coronary arteries; in our series, the clinical diagnosis of acute or chronic MI was established in 15% of the patients, with a lower incidence as compared to the data recently published by Nikolaou et al. (27 infarctions in 106 patients) [16]. Myocardial infarction in fact represents one of the main clinical expressions of coronary atherosclerosis occurring during the natural course of the disease when an acute arterial occlusion or critical stenosis determines a prolonged ischemia of the myocites leading to disruption of the cell’s membrane and, finally, to myocardial necrosis [21].
Infarct appearance and radiological-pathological interpretation of the findings
As previously described, the infarcted region was visualized in all cases as a segmental area of hypoattenuation in comparison with the normally enhanced myocardium during the arterial first pass of the contrast agent [22, 23] .This visual finding was also confirmed after quantitative assessment of the data, showing statistically significant lower attenuation values in the infarcted segments in comparison with the non-infarcted myocardium. The regional hypodensity of the infarcted area during the first pass of the iodinated contrast agent might be either the expression of edematous imbibition of the necrotic myocardium, which is typically observed in the first 2–4 weeks after the acute event, or the consequence of the replacement of the necrotic tissue with poorly enhancing fibrous tissue, which occurs in the chronic phase of the MI [24]. However, we could not find a cut-off density value to discriminate acute from chronic infarctions.
The apparently normal wall thickness of the infarcted segments found in all patients (n=9) with a recent event can be interpreted as another indirect CT sign of myocardial edema and might be a useful criterion to differentiate recent (<1 month) from non-recent (>1 month ) MI, since myocardial wall thickness constantly decreases over time in patients with MI [25, 26]. Myocardial edema gradually resolves, being constantly replaced by progressive wall thinning of the LV due to healing of the infarcted region and to left ventricular remodeling [24, 27]. However, although wall thinning is a typical feature of chronic infarctions, this finding is not observed in non-transmural infarctions [25].
Detection of lateral and inferior MIs
Reconstruction of images on cardiac SA and VLA enabled a better detection of inferior and lateral areas of necrosis otherwise difficult to identify on transverse images as shown in previous experiences with non-spiral CT systems [16, 28]. In comparison with CT transverse images, the assessment of anatomical planes routinely used in US and MR imaging, such as SA and VLA, also provided additional and more accurate information concerning the transmurality of necrosis and left ventricular wall thickness [16, 28].
False-negatives
In five cases, MDCTA provided a false-negative diagnosis. In three out of five cases of missed infarctions, previous clinical and ECG diagnosis of non-Q MI was established. Although already described [14], identification of subendocardial necrosis is challenging by MDCTA since the limited transmural involvement of the left ventricular wall (≤25%) might be obscured by the presence of collateral perfusion in the area of the infarcted myocardium [16]; furthermore, the mechanism of wall thinning and left ventricular remodelling is typically not observed in subendocardial infarctions, even in the chronic phase [25]. Moreover, it has been observed that CT underestimates areas of myocardial necrosis compared to nuclear medicine studies, making their detection troublesome [29]. In two patients, the presence of severe artifacts due to fast heart rate (78 and 71 bpm) affected image quality and did not allow identification of the area of necrosis. This limitation of four-row scans is well known being caused by the relatively long acquisition window that determines motion artifacts in subjects with high heart rates and short diastolic phases [30].
False-positives
Our results showed a high number of false-positive patients, resulting in a relatively low positive predictive value (68%) of the method for detection of infarctions.
This finding might be attributed either to the presence of perfusion defects in patients with transient myocardial ischemia or to local inhomogeneities of myocardial enhancement causing a regional hypodensity during the first pass of contrast agent.
Correlation with non-invasive angiographic findings
Several studies have already shown the feasibility of retrospectively ECG-gated MDCTA not only in detection of coronary stenoses, but also in the characterization of atherosclerotic plaques, assessment of CABG patency and, with more controversial results, the visualization of in-stent restenoses at follow-up [31–33]. Nikolaou et al. reported a 90% diagnostic accuracy of MDCTA for detection of previous MI, suggesting that it might provide information on coronary arteries status and, at the same time, on myocardial morphology [16]. The potential advantage of MDCT compared to previous CT generations and even to others non-invasive diagnostic modalities (US, MR) is therefore the combination of angiographic and morphological findings with high spatial and temporal resolution[35, 36]. As already pointed out in previous studies, even in our series, severely calcified coronary vessels and motion in patients with fast heart rate caused beam artifacts and blurring of the vessel lumen, making assessment of the coronary artery unreliable [36]. However, in most of the cases we found a good correlation between the localization of necrosis and the status of the territory-dependent coronary vessel. The practical consequence and clinical application of the present finding is that assessment of coronary arteries should be combined with visualization of the myocardium and myocardial chambers mostly in patients with severe coronary artery disease or previous procedures of revacularization.
Study limitations
The present study has two major limitations.
First of all, no delayed acquisitions were available for images analysis and therefore the phenomenon of myocardial delayed enhancement previously described by Musuda et al. [22, 26] could not be assessed. However, the clinical utility of CT delayed-enhancement images has not been fully determined, and it still remains controversial whether an additional radiation exposure provides clinical advantages. Patient exposure to ionizing radiation represents in fact a major and still debated issue of cardiac CT, especially when scanning asymptomatic patients or proposing the method as a screening tool for coronary artery disease.
It as been shown that due to the longer exposure time (∼200 ms), a four-row MDCTA acquisition with retrospective ECG gating might provide an effective dose of approximately 10 mSv which is about five times the average exposure of a routine EBCT examination (∼2 mSv) [37]. Overall effective dose can be substantially reduced by means of technical innovations, among which the “ECG tube current modulation” consists of a progressive online reduction of tube output during systolic phases of each cardiac cycle [38–40]. The second limitation is the use of a four-channel CT system now that 16- and 64- slices systems are available [41–43]. Nevertheless, our findings are independent of technological advances and can be considered valid and applicable, presumably with even better results with faster, up-to-date CT scanners.
Conclusions
Our study suggests that MDCTA of the coronary arteries should include analysis of coronary arteries and myocardial density and morphology to correlate the atherosclerotic burden to the coronary arteries with myocardial damage.
References
Ohnesorge B, Flohr T, Becker C, Kopp AF, Schoepf UJ, Baum U, Knez A, Klingenbeck-Regn K, Reiser MF (2000) Cardiac imaging by means of electrocardiographically gated multisection spiral CT: initial experience. Radiology 217:564–571
Achenbach S, Ulzheimer S, Baum U, Kachelriess M, Ropers D, Giesler T, Bautz W, Daniel WG, Kalender WA, Moshage W (2000) Noninvasive coronary angiography by retrospectively ECG-gated multislice spiral CT. Circulation 102:823–828
Dorgelo J, Willems TP, Geluk CA, Van Ooijen PM, Zijlstra F, Oudkerk M (2005) Multidetector computed tomography-guided treatment strategy in patients with non-ST elevation acute coronary syndromes: a pilot study. Eur Radiol 15(4):708–713
Achenbach S, Giesler T, Ropers D, Ulzheimer S, Derlien H, Schulte C, Wenkel E, Moshage W, Bautz W, Daniel WG, Kalender WA, Baum U (2001) Detection of coronary artery stenoses by contrast-enhanced, retrospectively electrocardiographically-gated, multislice spiral computed tomography. Circulation 103:2535–2538
Pannu HK, Flohr TG, Corl FM, Fishman EK (2003) Current concepts in multi-detector row CT evaluation of the coronary arteries: principles, techniques, and anatomy. Radiographics 23:S111–S125
Rodenwaldt J (2003) Multislice computed tomography of the coronary arteries. Eur Radiol 13:748–757
Desjardins B, Kazerooni EA (2004) ECG-gated cardiac CT. Am J Roentgenol 182(4):993–1010
Hamoir XL, Flohr T, Hamoir V, Labaki L, Tricquet JY, Duhamel A, Kirsch J (2005) Coronary arteries: assessment of image quality and optimal reconstruction window in retrospective ECG-gated multislice CT at 375-ms gantry rotation time. Eur Radiol 15(2):296–304
Lu B, Mao SS, Zhuang N, Bakhsheshi H, Yamamoto H, Takasu J, Liu SC, Budoff MJ (2001) Coronary artery motion during thecardiac cycle and optimal ECG triggering for coronary artery imaging. Invest Radiol 36:250–256
Boxt LM, Lipton MJ, Kwong RY, Rybicki F, Clouse ME (2003) Computed tomography for assessment of cardiac chambers, valves, myocardium and pericardium. Cardiol Clin 21(4):561–585
Ohnesorge BM, Becker CR, Flohr TG, Reiser MF (2002) Multi-slice CT in cardiac imaging. Springer, Berlin Heidelberg New York
Doherty PW, Lipton MJ, Berninger WH, Skioldebrand CG, Carlsson E, Redington RW (1981) Detection and quantitation of myocardial infarction in vivo using transmission computed tomography. Circulation 63:597–606
Lipton MJ, Higgins CB (1980) Evaluation of ischemic heart disease by computerized transmission tomography. Radiol Clin North Am 18:557–576
Hilfiker PR, Weishaupt D, Marincek B (2001) Multislice spiral computed tomography of subacute myocardial infarction. Circulation 28:104(9):1083
Paul JF, Dambrin G, Caussin C, Lancelin B, Angel C (2003) Sixteen-slice computed tomography after acute myocardial infarction from perfusion defect to the culprit lesion. Circulation 2003:108:373–374
Nikolaou K, Knez A, Sagmeister S, Wintersperger BJ, Boekstegers P, Steinbeck G, Reiser MF, Becker CR (2004) Assessment of myocardial infarctions using multidetector-row computed tomography. J Comput Assist Tomogr 28(2):286–292
Alpert JS, Thygesen K, Antman E, Bassand JP (2000–2001) Myocardial infarction redefined-a consensus document of The Joint European Society of Cardiology/American College of Cardiology Committee for the redefinition of myocardial infarction. J Am Coll Cardiol 36(3):959–969. Erratum in: J Am Coll Cardiol 37(3):973
Cerqueira MD, Weissman NJ, Dilsizian V, Jacobs AK, Kaul S, Laskey WK, Pennell DJ, Rumberger JA, Ryan T, Verani MS (2002) Standardized myocardial segmentation and nomenclature for tomographic imaging of the heart: a statement for healthcare professionals from the Cardiac Imaging Committee of the Council on Clinical Cardiology of the American Heart Association. Circulation;105(4):539–542
Gosalia A, Haramati LB, Sheth MP, Spindola-Franco H (2004) CT detection of acute myocardial infarction. Am J Roentgenol 182(6):1563–1566
Hoffmann U, Millea R, Enzweiler C, Ferencik M, Gulick S, Titus J, Achenbach S, Kwait D, Sosnovik D, Brady TJ (2004) Acute myocardial infarction: contrast-enhanced multi-detector row CT in a porcine model. Radiology 231(3):697–701
Boersma E, Mercado N, Poldermans D, Gardien M, Vos J, Simoons ML (2003) Acute myocardial infarction. Lancet 361(9360):847–858
Koyama Y, Mochizuki T, Higaki J (2004) Computed tomography assessment of myocardial perfusion, viability, and function. J Magn Reson Imaging 19(6):800–815
White RD (2004) MR and CT assessment for ischemic cardiac disease. J Magn Reson Imaging 19:659–675
Abdel-Aty H, Zagrosek A, Schulz-Menger J, Taylor AJ, Messroghli D, Kumar A, Gross M, Dietz R, Friedrich MG (2004) Delayed enhancement and T2-weighted cardiovascular magnetic resonance imaging differentiate acute from chronic myocardial infarction. Circulation 109(20):2411–2416
Baer FM, Smolarz K, Jungehulsing M, Beckwilm J, Theissen P, Sechtem U, Schicha H, Hilger HH (1992) Chronic myocardial infarction: assessment of morphology, function, and perfusion by gradient echo magnetic resonance imaging and 99 mTc-methoxyisobutyl-isonitrile SPECT. Am Heart J 123:636–645
Masuda Y, Yoshida H, Morooka N, Watanabe S, Inagaki Y (1984) The usefulness of X-ray computed tomography for the diagnosis of myocardial infarction. Circulation 70:217–225
Wisenberg G, Prato FS, Carroll SE, Turner KL, Marshall (1988) Serial nuclear magnetic resonance imaging of acute myocardial infarction with and without reperfusion. Am Heart J 115:510–518
Georgiou D, Bleiweis M, Brundage BH (1992) Conventional and ultrafast computed tomography in the detection of viable versus infarcted myocardium. Am J Card Imaging 6:228–236
Schmermund A, Gerber T, Behrenbeck T, Reed JE, Sheedy PF, Christian TF, Rumberger JA (1998) Measurement of myocardial infarct size by electron beam computed tomography: a comparison with 99 mTc sestamibi. Invest Radiol 33:313–321
Giesler T, Baum U, Ropers D, Ulzheimer S, Wenkel E, Mennicke M, Bautz W, Kalender WA, Daniel WG, Achenbach S (2002) Noninvasive visualization of coronary arteries using contrast-enhanced multidetector CT: influence of heart rate on image quality and stenosis detection. Am J Roentgenol 179:911–916
Schoepf UJ, Becker CR, Ohnesorge BM, Yucel EK (2004) CT of coronary artery disease. Radiology 232(1):18–37
Hong C, Chrysant GS, Woodard PK, Bae KT (2004) Coronary artery stent patency assessed with in-stent contrast enhancement measured at multi-detector row CT angiography: initial experience. Radiology 233(1):286–291
Marano R, Storto ML, Maddestra N, Bonomo L (2004) Non-invasive assessment of coronary artery bypass graft with retrospectively ECG-gated four-row multi-detector spiral computed tomography. Eur Radiol 14(8):1353–1362
Kuijpers D, Janssen CH, van Dijkman PR, Oudkerk M (2004) Dobutamine stress MRI. Part I. Safety and feasibility of dobutamine cardiovascular magnetic resonance in patients suspected of myocardial ischemia. Eur Radiol 14(11):1823–1828
Kuijpers D, van Dijkman PR, Janssen CH, Vliegenthart R, Zijlstra F, Oudkerk M (2004) Dobutamine stress MRI. Part II. Safety and feasibility of dobutamine cardiovascular magnetic resonance in patients suspected of myocardial ischemia. Eur Radiol 14(11):2046–2052
Kuettner A, Kopp AF, Schroeder S, Rieger T, Brunn J, Meisner C, Heuschmid M, Trabold T, Burgstahler C, Martensen J, Schoebel W, Selbmann HK, Claussen CD (2004) Diagnostic accuracy of multidetector computed tomography coronary angiography in patients with angiographically proven coronary artery disease. J Am Coll Cardiol 43(5):831–839
Achenbach S, Giesler T, Ropers D, Ulzheimer S, Anders K, Wenkel E, Pohle K, Kachelriess M, Derlien H, Kalender WA, Daniel WG, Bautz W, Baum U (2003) Comparison of image quality in contrast-enhanced coronary-artery visualization by electron beam tomography and retrospectively electrocardiogram-gated multislice spiral computed tomography. Invest Radiol 38(2):119–128
Jung B, Mahnken AH, Stargardt A, Simon J, Flohr TG, Schaller S, Koos R, Gunther RW, Wildberger JE (2003) Individually weight-adapted examination protocol in retrospectively ECG-gated MSCT of the heart. Eur Radiol 13(12):2560–2566
Jakobs TF, Becker CR, Ohnesorge B, Flohr T, Suess C, Schoepf UJ, Reiser MF (2002) Multislice helical CT of the heart with retrospective ECG gating: reduction of radiation exposure by ECG-controlled tube current modulation. Eur Radiol 12(5):1081–1086
Wintersperger BJ, Nikolaou K, Jakobs TF, Reiser MF, Becker CR (2003) Cardiac multidetector-row computed tomography: initial experience using 16 detector-row systems. Crit Rev Comput Tomogr 44(1):27–45
Nikolaou K, Sanz J, Poon M, Wintersperger BJ, Ohnesorge B, Rius T, Fayad ZA, Reiser MF, Becker CR (2005) Assessment of myocardial perfusion and viability from routine contrast-enhanced 16-detector-row computed tomography of the heart: preliminary results. Eur Radiol 15(5):864–871
Cademartiri F, Mollet N, van der Lugt A, Nieman K, Pattynama PM, de Feyter PJ, Krestin GP (2004) Non-invasive 16-row multislice CT coronary angiography : usefulness of saline chaser. Eur Radiol 14(2):178–183
Flohr T, Stierstorfer K, Raupach R, Ulzheimer S, Bruder H (2004) Performance evaluation of a 64-slice CT system with z-flying focal spot. Rofo 176(12):1803–1810
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Francone, M., Carbone, I., Danti, M. et al. ECG-gated multi-detector row spiral CT in the assessment of myocardial infarction: correlation with non-invasive angiographic findings. Eur Radiol 16, 15–24 (2006). https://doi.org/10.1007/s00330-005-2800-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-005-2800-3