Abstract
Background
The laparoscopic approach is widely accepted as the procedure of choice for abdominal surgery. However, laparoscopic liver resection (LLR) has advanced slowly due to the significant learning curve (LC), and only few publications have dealt with advanced training in LLR.
Methods
Two reviewers conducted systematic research through MEDLINE and EMBASE with combinations of the following keywords: (learning curve OR teaching OR training OR simulation OR education) AND (liver OR hepatic) AND (laparoscopic OR laparoscopy). Robotic-assisted, hand-assisted and hybrid LLRs were excluded.
Results
Nineteen studies were retrieved. Overall, the level of evidence was low. Thirteen articles assessed the LC during real-life LLR, and six articles focussed on simulation and training programmes in LLR. The LC in minor LLR comprised 60 cases overall, and 15 cases for standardised left lateral sectionectomy. For major LLR (MLLR), the LC was 50 cases for most studies, but was reported to be 15–20 cases in more recent studies, provided MLLR is performed progressively in selected patients. However, there was heterogeneity in the literature regarding the number of minor LLRs required before MLLR, with 60 minor LLRs reported as the minimum. Six studies showed a potential benefit of simulation and training programmes in this field. The gradual implementation of LLR combined with simulation-based training programmes could reduce the clinical impact of LC.
Conclusions
The LC in LLR is a long process, and MLLR should be gradually implemented under the supervision of experienced surgeons. Training outside the operating room may reduce the LC in real-life situations.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The laparoscopic approach is now widely accepted as the procedure of choice in many abdominal surgical procedures, such as colorectal surgery [1, 2]. In contrast, laparoscopic liver resection (LLR) has developed very slowly due to various obstacles, which include the following [3]: a significant learning curve (LC), especially to become familiar with specific devices and with liver mobilisation and parenchymal transection techniques; the fear of tricky haemorrhage or gas embolism; and a relative lack of standardised procedures.
Despite these drawbacks, LLR provides several potential benefits [4, 5], including reductions in intraoperative blood loss, transfusion rate [6], post-operative morbidity [6], length of stay (LOS) [6] and post-operative pain [7], in addition to parietal preservation [7], earlier resumption of physical activity [7] and facilitation of further surgical procedures [8].
In 2008, these benefits led the Louisville Consensus to conclude that laparoscopic surgery was a safe and effective approach in the hands of expert surgeons for both hepatobiliary surgery and laparoscopy [9]. However, the need for standardisation of procedures was emphasised [9]. Several scoring systems have been created to predict LLR difficulty, but none have gained widespread acceptance [10,11,12,13,14].
The number of procedures required to overcome the LC in LLR is currently under debate. Training in LLR requires a long and progressive LC through performing procedures of increasing complexity, ultimately leading to decreased morbidity and conversion rates [4,5,6,7]. Moreover, as for any new surgical techniques, the training of young surgeons is a major advantage to increase the implementation of LLR.
The aims of this systematic review were to define the LC in LLR and to identify simulation-based training programmes related to LLR.
Materials and methods
The review was planned, conducted and reported in adherence to PRISMA standards of quality for reporting systematic reviews and meta-analyses [15].
Study identification
We sought to include all original studies dealing with training and the LC in LLR. LLR includes pure laparoscopic, hand-assisted and hybrid techniques [9]. In this review, the LC analysis focused on studies that assessed the pure laparoscopic approach, defined as procedures where manual assistance and mini laparotomy for parenchymal transection are not used. All original studies dealing with simulation or training programmes in LLR were also included, where simulation could be used either as a training tool or an assessment tool.
A strategy was designed (Fig. 1) to search the MEDLINE and EMBASE databases using the following search terms (MeSH terms and equivalent free-text terms): (learning curve OR teaching OR training OR simulation) OR education) AND (liver OR hepatic) AND (laparoscopic OR laparoscopy). No beginning cut-off date was used, and the last date of the search was July 2, 2018. The reference lists of all included articles were manually searched to identify additional studies.
Exclusion criteria
Editorial letters, reviews, guidelines, technical notes and non-English-language publications were excluded. Studies focussed on robotic-assisted, hand-assisted and hybrid LLR were also excluded. In studies that compared LCs in LLR between different approaches, only data regarding the LC in the pure laparoscopic approach were analysed.
Study selection
Two reviewers (T.G. and D.B.) independently screened all article titles and selected studies based on the titles and/or abstracts. Studies that met the defined inclusion criteria were selected for review of the full-text article. If it was not clear from the abstract whether a study fulfilled the inclusion criteria, the full article was reviewed independently by both reviewers. Any discrepancies between the two reviewers were resolved by consensus.
Definitions
Minor LLRs were defined according to the Morioka conference [4], namely resections of one to two hepatic segments according to the Couinaud classification [16], involving the anterior and inferior segments (segments 2, 3, 4b, 5 and 6).
Major LLRs (MLLRs) were defined according to the Louisville conference. They encompassed liver resections with at least three hepatic segments, according to the Couinaud classification [4], but also resections of segments 1, 4a, 7 and 8, and lesions located closed to the hepatic hilum, hepatic veins or inferior vena cava [9].
The LC was defined as a tool to determine the number of cases necessary to obtain a plateau of performance in a predefined task or procedure.
Data extraction
The indicators of LLR quality and assessment of the LC in LLR included conversion to open surgery, which is conventionally used in LLR as an indicator of quality [17,18,19,20,21], quantitative variables such as operative time and intraoperative blood loss [18, 19, 22,23,24], LOS [17], and qualitative variables such as intraoperative pedicle clamping [18] and post-operative morbidity [24, 25]. The extracted data also included the number of procedures, type of LLR (i.e. minor or major) and type of assessment tool (i.e. cumulative sum [CUSUM] method [26]), among other variables.
For studies dealing with simulation-based training programmes in LLR, the following data were extracted: type of training model used for the simulation (i.e. virtual simulators, animals [porcine or other] or cadavers), type of procedure evaluated (i.e. basic skills, transection of the liver parenchyma, minor or major LLR), type of study (i.e. randomised controlled trial, non-randomised controlled trial, single-group pre-/post-test, case series assessing any outcome, or descriptive studies), purpose(s) of the study (i.e. training or assessment), model description (i.e. description of either a procedure on a tool or a whole course), satisfaction of trainees, validation of a model, transfer of skills and learning curve.
Assessment of methodological quality
The instructions provided in the Cochrane Handbook for Systematic Reviews of Intervention [27] and the Cochrane Hepato-Biliary Group module [28] were followed. Given the risk of overestimation of the effect of the intervention in RCTs with inadequate methodological quality, the influence of methodological quality on the results was assessed by evaluating the reported randomisation and follow-up procedures in each trial, including the generation of allocation sequence, allocation concealment, blinding and follow-up.
Results
Description of studies
We identified 493 potentially relevant articles in the database search. Seventy-four articles were retrieved for abstract screening, and 30 articles for more detailed evaluation. From these, we identified 19 appropriate articles for systematic review. Overall, 13 articles assessing LC in LLR and six articles assessing simulation-based training programmes in LLR were included (Fig. 1).
All series assessing LC in LLR were retrospective, and there were no randomised controlled trials [17,18,19,20,21, 23,24,25, 29,30,31,32,33] (Table 1). Of those, 11 studies included over 100 LLRs [17,18,19,20,21, 23,24,25, 29, 30, 33], and seven used the CUSUM method to determine the LC [17,18,19,20, 24, 25, 33]. Most of these studies assessed the LC of a single expert surgeon.
No publications focused on simulation-based training programmes in LLR were randomised controlled trials. They were comparative studies [34, 35], descriptive case series [36,37,38] or a single-group pre-/post-test study [39].
No data were deemed suitable for statistical pooling due to the heterogeneity of the results.
Learning curve in laparoscopic liver resection
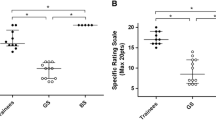
Vigano et al. [17] published the first study of the LC in LLR based on the CUSUM method, in which the main endpoint was the rate of conversion to open surgery. This study included 174 LLRs (including 35 MLLRs), which were subdivided into three consecutive groups with 58 LLRs in each: the pioneering period of experience (group A), intermediate cases (i.e. progressive increase in MLLR, group B) and the latest cases operated using a standardised approach (group C). The authors concluded that 60 procedures were the necessary benchmark in the LC for minor LLR.
Tomassini et al. [33] published the largest series assessing the LC in pure LLR. A difficulty scale of 1 to 10 was assigned to each type of resection, and then the CUSUM method was applied to the difficulty scale to assess the LC in terms of conversion rate, blood loss and operative time. A total of 275 minor LLRs and 44 MLLRs were included. The LC was considered to be completed after 160 procedures, with the first impact observed after 50 procedures on intraoperative blood loss.
Minor laparoscopic liver resection
Left lateral sectionectomy (LLS) is the anatomic liver resection of choice in minor LLRs; however, LLS represents only 7% of hepatectomies [40]. A comparative analysis found that operative time and LOS decreased significantly after 15 LLS [31]. Seven other large studies (Table 2) have sought to define LC for minor LLRs [19, 21, 23,24,25, 29, 32]. The number of procedures necessary to acquire competency in minor LLR ranged from 15 to 64 cases. This large variation can be attributed to two factors: (1) the procedure itself differed from one study to another (the LC of now standardised procedures, such as LLS, seems shorter than that of a wedge resection or segmentectomy) and (2) the main endpoint used to define LC. Ratti et al. [29] collected a total of 245 LLSs performed across four centres by experienced surgeons. In this study, the operative time was chosen as the marker of LC. The skewness of the operative time was calculated, and the cut-off point for LC was determined after 15 LLSs. However, 15 LLS corresponded to the 55th overall laparoscopic procedure in centres 2 and 4, to the 29th in centre 1, and to the 44th in centre 3.
Most authors concluded that acquiring competency with minor LLR is a prerequisite for more complex procedures.
Major laparoscopic liver resection
The LC in MLLR (Table 3) was assessed in six studies [18,19,20,21, 23, 25]. Different endpoints were used to define LC: conversion rate, operative time, blood loss, hepatic pedicle clamping and its duration, morbidity and LOS. Only two of these studies focused solely on MLLR [18, 20].
Nomi et al. [18] presented the largest series, in which the LC was determined using the CUSUM method in terms of the operative time over three phases: phase 1 (P1), initial (n = 45 patients); phase 2 (P2), intermediate (n = 30); and phase 3 (P3), final (n = 98). The operative time was significantly reduced after 45 MLLRs, but was greater in P3 than in P2, which was consistent with the surgeon performing more complex procedures. As for secondary outcomes, hepatic pedicle clamping and its duration, blood loss, conversion rate and LOS were significantly decreased between P1, P2 and P3.
From minor to major laparoscopic liver resection
Most studies assessing LC in MLLR recommend preliminary experience in minor LLRs, but also in performing major hepatectomies by open surgery [19, 20]. There was some heterogeneity in the literature regarding the number of minor hepatectomies required before more complex LLRs should be performed [21, 23, 25, 33].
Hasegawa et al. [25] assessed how MLLR could be safely introduced in a series of 245 resections. Based on previous studies, they divided the study cohort into three phases of gradual experience. The comparative analysis between minor LLR and MLLR showed a significant increase in operative time, blood loss, conversion rate, morbidity and LOS in MLLR. However, the comparative analysis between the three phases did not show any significant differences for these items, except for a decrease in blood loss, which has no significant clinical relevance (60 vs. 30 mL, p = 0.02). Finally, the comparative analysis of MLLR between phases 2 and 3 showed reduced operative time and blood loss in phase 3.
Finally, in the study by Komatsu et al. [21], implementation of minor LLRs progressed to MLLR over a gradual increase in experience. The conversion rate significantly decreased after 60 LLSs. The LC was shorter for left hepatectomy (16 procedures), and there was no LC threshold for right hepatectomy, i.e. the last procedure performed over time.
Simulation-based training programmes
The six included studies are summarised in Table 4. The main training models used were the animal model and the cadaver, with only one study assessing the relevance of an augmented reality simulator [34]. Two studies assessed the educational value of simulation-based training programmes in LLR [36, 39].
Udomsawaengsup et al. [36] assessed a training programme on cadavers. However, the only assessment was the satisfaction of trainees, and the type of LLR was not specified. White et al. [39] designed an intensive 2-day course comprised of procedures on cadavers including basic skills, LLS and laparoscopic right hepatectomy. Thirty-two participants were involved, and again, only participants’ feedback was analysed, with the overall rating for teaching sessions scored as excellent in 43%, good in 32% and fair in 25% of cases.
Strickland et al. [34] assessed the construct validity of liver tumourectomy using an augmented reality simulator and an ex vivo lamb liver. The aim of the study was to develop a model for the technical skills involved in LLR. Twenty participants were included, all of whom had varying levels of laparoscopic experience. The first task was to identify a tumour and to assess the surrounding liver to ensure that it was a solitary lesion. Division of the liver parenchyma was designated as the second task. The last tasks were the simulated control of bleeding from the liver, either through an easy stitch or a difficult stitch at the inferior surface of the liver. All four tasks demonstrated construct validity according to experience for time and path length.
Several teams have sought to identify a relevant animal model with educational value in LLR [35, 37, 38]. Komorowski et al. [38] showed that the porcine model provided a realistic learning environment in which exposure, dissection and surgical injuries could be taught, specified and anticipated. Teh et al. [37] assessed the feasibility of LLR in a sheep model. The inflow and outflow structures of the sheep liver were analysed via surgical dissection and contrast studies, and then a left MLLR was performed. The authors showed that the surgical anatomy of sheep liver was very similar to the human liver and that MLLR could be performed with accuracy. More recently, implementation of a perfused ex vivo liver training model has increased the fidelity of the animal model and simulated intrahepatic bleeding [35]. This model was constructed using fresh lamb liver, with the portal veins perfused with a red-dyed liquid gelatine solution. Construct validity was assessed in 33 participants (novices, intermediate and experts), who were asked to perform one superficial stitch and one deep stitch for suture haemostasis. The educational value was compared to that of a standard box-trainer and was found to have better results.
Discussion
The development of new techniques, devices and standardised procedures has enabled the gradual evolution of LLR techniques [3]. LLR has been growing in the number of procedures performed and their complexity, with nearly 10000 cases published worldwide [41]. The consensus meeting in Louisville in 2008 [8] reviewed the feasibility of LLR, whereas the following meeting in Morioka in 2014 [4] focused on the comparison of laparoscopic and open resections, demonstrating a clear role of the laparoscopic approach in the modern era of liver surgery. Recently, the Southampton Guidelines have presented clinical practice guidelines designed specifically to ensure the safety of future development of LLR [42]. As previously reported by Brown et al. [43], the present review confirmed that a progression in skill set and competency is required to safely perform LLR. Competency in minor LLR is acquired after 15 to 60 cases, whereas 20 to 60 cases are needed to reach proficiency in MLLR, provided proficiency has been already reached for minor LLR.
In this review, the LC parameters assessed varied quite a bit between studies (i.e. conversion rate, blood loss, operative time or post-operative morbidity), and therefore, it can be difficult to compare one to the other. In addition, other parameters are also involved in acquiring competency in LLR, including training in open liver surgery, as well as in minimally invasive surgery for other procedures, training in ultrasound skills, and familiarisation with the use and pitfalls of surgical energy devices and staplers. These parameters, as well as the standardisation of procedures for LLR over the years [44, 45], may explain the discrepancies in LC observed between studies.
The Southampton Guidelines advocate that the laparoscopic approach should be considered as standard practice for lesions in the left lateral and the anterior segments and that in expert hands, LLR for lesions located in the posterosuperior segments may maintain the advantages seen in the anterolateral segments [42]. However, in posterosuperior segments, the guidelines recommend that LLR be undertaken with caution, depending on the surgeon’s expertise and the available technical equipment. Several scoring systems for predicting LLR difficulty have been created [10,11,12,13,14]. The 10-level difficulty index of Ban et al. [10] was calculated by adding an applicable score for the extent of liver resection, tumour location, liver function, tumour size and the proximity of the tumour to major vessels. Recently, Kawaguchi et al. [14] have aimed to stratify the difficulty of LLR into three groups based on objective intraoperative outcomes, comprising operative time, blood loss and conversion rate: group I represented the first level and included wedge resection and LLS; group II represented the intermediate level with anterolateral segmentectomy and left hepatectomy; and group III represented the highly advanced level including posterosuperior segmentectomy, right hepatectomy, extended hepatectomy and central hepatectomy. This classification was validated by assessing the post-operative outcomes, where global and major morbidity tended to increase along with the classification groups.
In the present review, data regarding the LC for minor LLR and MLLR and the prerequisites for performing MLLR were established by 11 retrospective studies, mostly based on a single experienced surgeon rather than a team. Such methodological choice may induce significant analysis bias. Furthermore, LC is a “moving target”, where, on the one hand, surgeons take on more difficult cases with increasing experience and, on the other hand, the LC may change from the self-taught pioneer to the master/apprentice timeline. Recently, Halls et al. [46] have aimed to compare the LC of the self-taught “pioneers” of LLR, who developed their practice in the earliest stage, with those of the “early adopters”, who received laparoscopic training and developed their practice in the “optimisation” of techniques stage, in order to establish whether the LC could be reduced with specific training, technological innovations and standardisation. Among the “pioneering” surgeons, the LC based on LOS was 50 cases for minor resections and 85 cases for MLLR. After 46 procedures, the outcomes of the “early adopters” were comparable to those achieved by the “pioneers” following 150 procedures in similar cases. Accordingly, the Southampton Guidelines state that supervision by experienced surgeons during LLR is effective in reducing the LC and improving post-operative morbidity rates [42].
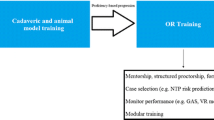
Simulation-based surgical training has become paramount over the past decade, especially in laparoscopic surgery. Many studies have demonstrated the positive impact of simulation on technical skills for basic laparoscopic procedures [47,48,49,50,51], and simulation-based training programmes have shown benefits in shortening the LC of young surgeons and reducing the number of adverse events in the operating room (OR) [52, 53]. Simulation for complex laparoscopic procedures has been assessed to a lesser extent [54]. However, these simulations are associated with a longer LC and are not easily accessible by young surgeons. Indeed, the number of complex resections in hepatobiliary surgery performed by surgeons at the end of their residency is estimated to be fewer than five procedures, which are predominantly open surgery [55]. In colorectal surgery, two studies have shown that simulation promoted the participation of young surgeons in the OR without increasing morbidity [56, 57]. In the present review, we found that only few studies have focused on simulation-based teaching programmes in LLR. Unfortunately, in most of the selected studies, only the participants’ feedback was analysed, and the overall methodological quality was poor. Nevertheless, these studies showed encouraging results in terms of technical skills and educational value. The gradual introduction of LLR, combined with simulation-based training programmes and supervision by experienced surgeons, could reduce the clinical impact of LC and improve patients’ safety [58]. However, additional well-designed studies are required to assess simulation in LLR.
In conclusion, the LC for minor LLR is about 60 cases and the LC for MLLR is about 50 cases, after firstly acquiring a level of expertise in minor LLR. These data were established by 11 retrospective studies, which were mostly based on a single experienced surgeon rather than a team. Future studies should assess whether the LC differs for junior surgeons working in a team that already has expertise in this area. In addition, initial training outside the OR could theoretically reduce the LC. However, there are no simulation-based training programmes in which the educational value has been demonstrated with a high level of scientific evidence.
References
Fleshman J, Sargent DJ, Green E et al (2007) Clinical Outcomes of Surgical Therapy Study Group. Laparoscopic colectomy for cancer is not inferior to open surgery based on 5-year data from the COST Study Group trial. Ann Surg 246:655–662
Bonjer HJ, Deijen CL, Abis GA; Color II Study Group (2015) A randomized trial of laparoscopic versus open surgery for rectal cancer. N Engl J Med 372:1324–1332
Tranchart H, Dagher I (2014) Laparoscopic liver resection: a review. J Visc Surg 151:114–122
Wakabayashi G, Cherqui D, Geller DA et al (2015) Recommendations for laparoscopic liver resection a report from the second international consensus conference held in Morioka. Ann Surg 261:619–629
Kasai M, Cipriani F, Gayet B et al (2018) Laparoscopic versus open major hepatectomy: a systematic review and meta-analysis of individual patient data. Surgery 163:985–995
Tranchart H, Di Giuro G, Lainas P et al (2010) Laparoscopic resection for hepatocellular carcinoma: a matched-pair comparative study. Surg Endosc 24:1170–1176
Dagher I, Di Giuro G, Dubrez J et al (2009) Laparoscopic versus open right hepatectomy: a comparative study. Am J Surg 198:173–177
Belli G, Cioffi L, Fantini C et al (2009) Laparoscopic redo surgery for recurrent hepatocellular carcinoma in cirrhotic patients: feasibility, safety, and results. Surg Endosc 23:1807–1811
Buell JF, Cherqui D, Geller DA, World Consensus Conference on Laparoscopic Surgery et al (2009) The international position on laparoscopic liver surgery: the Louisville statement 2008. Ann Surg 250:825–830
Ban D, Tanabe M, Ito H et al (2014) A novel difficulty scoring system for laparoscopic liver resection. J Hepatobiliary Pancreat Sci 21:745–753
Halls MC, Cherqui D, Taylor MA, Collaborators of The Difficulty of Laparoscopic Liver Surgery Survey et al (2018) Are the current difficulty scores for laparoscopic liver surgery telling the whole story? An international survey and recommendations for the future. HPB 20:231–236
Hasegawa Y, Wakabayashi G, Nitta H et al (2017) A novel model for prediction of pure laparoscopic liver resection surgical difficulty. Surg Endosc 31:5356–5363
Tanaka S, Kubo S, Kanazawa A et al (2017) Validation of a difficulty scoring system for laparoscopic liver resection: a multicenter analysis by the endoscopic liver surgery study group in Japan. J Am Coll Surg 225:249–258
Kawaguchi Y, Fuks D, Kokudo N et al (2018) Difficulty of laparoscopic liver resection: proposal for a new classification. Ann Surg 267:13–17
Moher D, Liberati A, Tetzlaff J et al (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med 151:264–269
Couinaud C (1957) Le foie: etudes anatomiques et chirurgicales. Masson et Cie, Paris
Vigano L, Laurent A, Tayar C et al (2009) The learning curve in laparoscopic liver resection. Improved feasibility and reproducibility. Ann Surg 250:772–782
Nomi T, Fuks D, Kawaguchi Y et al (2015) Learning curve for laparoscopic major hepatectomy. Br J Surg 102:796–804
Lee W, Woo JW, Lee JK et al (2016) Comparison of learning curves for major and minor laparoscopic liver resection. J Laparoendosc Adv Surg Tech A 26:457–464
van der Poel MJ, Besselink MG, Cipriani F et al (2016) Outcome and learning curve in 159 consecutive patients undergoing total laparoscopic hemihepatectomy. JAMA Surg 151:923–928
Komatsu S, Scatton O, Goumard C et al (2016) Development process and technical aspects of laparoscopic hepatectomy: learning curve based on 15 years of experience. J Am Coll Surg 224:841–850
Liu W, Wang Q, Huang J et al (2014) Laparoscopic left lateral sectionectomy—the learning curve and the role of left hepatic inflow occlusion. Hepatogastroenterology 61:417–421
Cai X, Li Z, Zhang Y et al (2014) Laparoscopic liver resection and the learning curve: a 14-year, single-center experience. Surg Endosc 28:1334–1341
Lin CW, Tsai TJ, Cheng TY et al (2016) The learning curve of laparoscopic liver resection after the Louisville statement 2008: will it be more effective and smooth? Surg Endosc 30:2895–2903
Hasegawa Y, Nitta H, Takahara T et al (2017) Safely extending the indications of laparoscopic liver resection: when should we start laparoscopic major hepatectomy? Surg Endosc 31:309–316
van Rij AM, McDonald JR, Pettigrew RA et al (1995) Cusum as an aid to early assessment of the surgical trainee. Br J Surg 82:1500–1503
Higgins JPT, Green, S (2016) Cochrane handbook for systematic reviews of intervention 5.1.0 (updated March 2011). The Cochrane Library. Issue 4. Chichester, Wiley
Gluud C, Als-Nielsen B, D'Amico G, et al (2007) Cochrane hepato-biliary group. about the cochrane collaboration (Cochrane Reviews Groups (CRGs)). Issue 2. Art. no.: LIVER. Wiley, Chichester
Ratti F, Barkhatov LI, Tomassini F et al (2016) Learning curve of self-taught laparoscopic liver surgeons in left lateral sectionectomy: results from an international multi-institutional analysis on 245 cases. Surg Endosc 30:3618–3629
Villani V, Bohnen JD, Torabi R et al (2016) “Idealized” vs. “true” learning curves: the case of laparoscopic liver resection. HPB 18:504–509
Abu Hilal M, Pearce NW (2008) Laparoscopic left lateral liver sectionectomy: a safe, efficient, reproducible technique. Dig Surg 25:305–308
O'Connor VV, Vuong B, Yang ST et al (2017) Robotic minor hepatectomy offers a favorable learning curve and may result in superior perioperative outcomes compared with laparoscopic approach. Am Surg 83:1085–1088
Tomassini F, Scuderi V, Colman R et al (2016) The single surgeon learning curve of laparoscopic liver resection. Medicine (Baltimore) 95:e5138
Strickland A, Fairhurst K, Lauder C et al (2011) Development of an ex vivo simulated training model for laparoscopic liver resection. Surg Endosc 25:1677–1682
Xiao J, Cui Z, Fu M et al (2016) An ex vivo liver training model continuously perfused to simulate bleeding for suture skills involved in laparoscopic liver resection: development and validity. Surg Endosc 30:4553–4561
Udomsawaengsup S, Pattana-arun J, Tansatit T et al (2005) Minimally invasive surgery training in soft cadaver (MIST-SC). J Med Assoc Thai 88:S189–194
Teh SH, Hunter JG, Sheppard BC (2007) A suitable animal model for laparoscopic hepatic resection training. Surg Endosc 21:1738–1744
Komorowski AL, Mituś JW, Sanchez Hurtado MA et al (2015) Porcine model in the laparoscopic liver surgery training. Pol Przegl Chir 87:425–428
White SA, Satchidanand RY, French JJ et al (2014) A cadaver lab training facility to facilitate laparoscopic liver resection. Surg Laparosc Endosc Percutan Tech 24:357–360
Goutte N, Bendersky N, Barbier L et al (2017) Laparoscopic left lateral sectionectomy: a population-based study. HPB 19:118–125
Ciria R, Cherqui D, Geller DA et al (2016) Comparative short-term benefits of laparoscopic liver resection: 9,000 cases and climbing. Ann Surg 263:761–777
Abu Hilal M, Aldrighetti L, Dagher I et al (2018) The southampton consensus guidelines for laparoscopic liver surgery. Ann Surg 268:11–18
Brown KM, Geller DA (2016) What is the learning curve for laparoscopic major hepatectomy? J Gastrointest Surg 20:1065–1071
Hasegawa Y, Nitta H, Sasaki A et al (2013) Laparoscopic left lateral sectionectomy as a training procedure for surgeons learning laparoscopic hepatectomy. J Hepatobiliary Pancreat Sci 20:525–530
Soubrane O, Schwarz L, Cauchy F et al (2015) A conceptual technique for laparoscopic right hepatectomy based on facts and oncologic principles: the caudal approach. Ann Surg 261:1226–1231
Halls MC, Alseidi A, Berardi G et al (2018) A comparison of the learning curves of laparoscopic liver surgeons in differing stages of the IDEAL paradigm of surgical innovation: standing on the shoulders of pioneers. Ann Surg 269:221–228
Sutherland LM, Middleton PF, Anthony A et al (2006) Surgical simulation: a systematic review. Ann Surg 243:291–300
Grantcharov TP, Kristiansen VB, Bendix J et al (2004) Randomized clinical trial of virtual reality simulation for laparoscopic skills training. Br J Surg 91:146–150
Seymour NE, Gallagher AG, Roman SA et al (2002) Virtual reality training improves operating room performance: results of a randomized, double-blinded study. Ann Surg 236:458–463
Scott DJ, Bergen PC, Rege RV et al (2000) Laparoscopic training on bench models: better and more cost effective than operating room experience? J Am Coll Surg 191:272–283
Beyer L, De Troyer J, Mancini J et al (2011) Impact of laparoscopy simulator training on the technical skills of future surgeons in the operating room: a prospective study. Am J Surg 202:265–272
De Win G, Van Bruwaene S, Kulkarni J et al (2016) An evidence-based laparoscopic simulation curriculum shortens the clinical learning curve and reduces surgical adverse events. Adv Med Educ Pract 30:357–370
Bansal VK, Raveendran R, Misra MC et al (2014) A prospective randomized controlled blinded study to evaluate the effect of short-term focused training program in laparoscopy on operating room performance of surgery residents (CTRI /2012/11/003113). J Surg Educ 71:52–60
Beyer-Berjot L, Palter V, Grantcharov T et al (2014) Advanced training in laparoscopic abdominal surgery: a systematic review. Surgery 156:676–688
Helling TS, Khandelwal A (2008) The challenges of resident training in complex hepatic, pancreatic, and biliary procedures. J Gastrointest Surg 12:153–158
Beyer-Berjot L, Pucher P, Patel V et al (2017) Colorectal surgery and enhanced recovery: impact of a simulation-based care pathway training curriculum. J Visc Surg 154:313–320
Lin E, Szomstein S, Addasi T et al (2003) Model for teaching laparoscopic colectomy to surgical residents. Am J Surg 186:45–48
van der Poel MJ, Huisman F, Busch OR et al (2017) Stepwise introduction of laparoscopic liver surgery: validation of guideline recommendations. HPB 19:894–900
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Guilbaud, T., Birnbaum, D.J., Berdah, S. et al. Learning Curve in Laparoscopic Liver Resection, Educational Value of Simulation and Training Programmes: A Systematic Review. World J Surg 43, 2710–2719 (2019). https://doi.org/10.1007/s00268-019-05111-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-019-05111-x