Abstract
Background
Several studies have examined controlling nutritional status (CONUT), which is one of the useful biomarkers for predicting patients’ prognosis following cancer treatment. The aim of this study was to evaluate the value of CONUT as a postoperative prognostic marker in patients with intrahepatic cholangiocarcinoma (ICC) following curative hepatectomy.
Methods
We retrospectively analyzed 71 patients who underwent curative hepatectomy for ICC between May 2002 and November 2016. Patients were divided into two groups according to their preoperative CONUT score (i.e., CONUT ≧ 2 or CONUT < 2).
Results
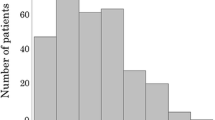
The number of patients assigned to the normal, mild, moderate, or severe malnutrition groups was 40, 28, two, and one, respectively. The high CONUT group (CONUT ≧ 2) consisted of 31 patients (43.7%) and had a poor prognosis with regard to overall survival (OS) (p = 0.0149). A high CONUT score is also identified as one of the independent predictors of poor prognosis in OS (hazard ratio 3.02; 95% confidence interval 1.4–6.8; p = 0.007). However, in the current study, a high CONUT score was not associated with postoperative complications (Clavien–Dindo classification ≧ III or more).
Conclusions
CONUT may be useful for the preoperative assessment of prognosis in patients with ICC who have undergone curative hepatectomy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Intrahepatic cholangiocarcinoma (ICC) is the second most common primary liver cancer, after hepatocellular carcinoma [1]. Although its incidence is increasing worldwide, patients with ICC still have a poor prognosis when compared to patients with other cancers, such that the 5-year survival rate is only 3% to 31% because of frequent lymph node involvement, intrahepatic metastasis, and/or refractoriness to chemotherapies or radiations [2,3,4]. Thus, the management of advanced ICC is shifting toward multidisciplinary approaches in an attempt to improve patients’ prognosis; however, surgical resection is considered as the only curative treatment for ICC at present.
Predicting a patient’s prognosis preoperatively using reliable biomarkers is very important in order to perform the appropriate treatment and incorporate the right follow-up strategies after surgery. Some studies have demonstrated tumor markers like carbohydrate antigen 19-9 (CA19-9) to be one of the major prognostic factors for poor prognosis following surgery [5]. It has also been demonstrated that cancer-related inflammation is associated with tumor cell survival, proliferation, and metastasis [6, 7]. Therefore, the molecular biomarkers for cancer-related inflammation, such as preoperative neutrophil to lymphocyte ratio (NLR), platelet to lymphocyte ratio (PLR), or modified Glasgow prognostic score (mGPS), are currently some of the strong prognostic factors after curative resections for ICC [8,9,10].
The patient’s nutritional status is also reported to be associated not only with short-term results but also with the patients’ long-term prognosis after cancer treatment [11, 12]. In cases of ICC, the prognostic nutritional index (PNI) has been reported to be a useful biomarker to evaluate patients’ nutritional status and predict their prognosis [13]. Controlling nutritional status (CONUT) was also reported, in 2005, to be a screening tool for nutritional status and an effective biomarker for patients’ prognosis [11, 14, 15]. CONUT consists of three parameters: serum albumin concentration (Alb), total peripheral lymphocyte counts (T-LC), and total cholesterol concentration (T-Cho). Our previous studies have suggested that CONUT is useful to estimate postoperative complications and prognosis in cases of esophageal cancer and colorectal cancer [12, 15].
However, the significance of CONUT in ICC still remains unclear. Therefore, in this study, we examine the relationship between CONUT and postoperative complications or prognosis in 71 patients with ICC who underwent curative hepatectomy in an attempt to further clarify the relationship.
Materials and methods
Patients
Between May 2002 and November 2016, 87 consecutive patients underwent hepatectomy for ICC in the Department of Gastroenterological Surgery, Kumamoto University. Of these 87 patients, we excluded 11 patients who underwent re-hepatectomy for ICC recurrence and five patients who underwent non-curative hepatectomy. Overall, the final study population consisted of 71 patients. Patients’ characteristics as well as information on other nutritional index, postoperative complications, recurrence, and survival were analyzed in these 71 patients. In all cases, we performed hepatectomy according to the number, size, and site of the ICC and each patient’s general condition [16]. Adjuvant chemotherapy was administered to the patients with lymph node metastasis or vascular invasion if their performance status was 0 or 1. The Kumamoto University Hospital Ethics Committee approved this study, and informed consent was obtained from each patient according to the institutional review board protocols.
Strategy of patient follow-up
Treatment data were retrospectively obtained from the records of these 71 patients. All patients involved were monitored either until December 2016 or their death. The mean follow-up period was 36.9 months. We staged the cancer based on the seventh edition of the American Joint Committee on Cancer (AJCC)/International Union Against Cancer (UICC) staging manual [17]. Patients were followed up with in our hospital or in affiliated hospitals, as previously reported [18]. Postoperative complications were defined as grade III or greater according to the Clavien–Dindo classification (CD) [19].
The definition of CONUT
The method of assessment of nutritional status according to CONUT is summarized in Table 1 [14]. Preoperative Alb, T-LC, and T-Cho were classified and scored according to their values. The total score of the three parameters was categorized as follows: zero to one is normal, two to four is mildly abnormal, five to eight is moderately abnormal, and nine or more is severely abnormal [14]. Therefore, we decided to take the cutoff value as two and defined low CONUT as within normal range and high CONUT as two or more in the current study. We calculated CONUT score for each case by the blood test within a month before hepatectomy.
Statistical analysis
Comparisons between the two groups were examined using the Student’s t test in continuous variables and the Fisher’s exact test where appropriate in categorical variables. Continuous variables are presented as the mean ± standard deviation (SD). The relapse-free survival (RFS) rate and the overall survival (OS) rate were calculated using the Kaplan–Meier method and compared using log-rank test. The scores of NLR, PLR, mGPS, and PNI were calculated as previously reported [8, 9, 20, 21]. The cutoff value of PNI was reported previously, and the cutoff values of NLR and PLR were detected as 3.0 and 163.4, respectively, using receiver operating characteristic (ROC) curve. The cutoff values of blood loss and operative time were median in 71 patients. All results with two-tailed values of p < 0.05 were considered to be statistically significant. The variables in which p value was less than 0.1 in univariate analysis of RFS and significant variables in univariate analysis of OS were included in a Cox proportional hazard model in order to identify independent prognostic factors. All statistical analyses were performed using JMP software (version 12; SAS Institute, Cary, NC, USA).
Results
Clinical and pathologic characteristics
The number of patients assigned to the normal, mild, moderate, or severe malnutrition groups was 40, 28, two, and one, respectively. According to the CONUT score, we divided 71 patients into two groups: 40 patients were in the low CONUT group (CONUT < 2) and 31 patients were in the high CONUT group (CONUT ≧ 2). Table 2 shows comparisons of patients’ background characteristics and tumor-related factors between the two groups. The number of patients who were hepatitis C virus antibody-positive (p = 0.017) or who had Child–Pugh B classification (p = 0.005) or lower BMI (p = 0.009) was significantly higher in the high CONUT group than in the low CONUT group. In addition, Alb (p = 0.002) and prothrombin time (p = 0.012) were also found to be lower in the high CONUT group. The numbers of patients with liver cirrhosis were significantly higher in the high CONUT group (p = 0.038). In light of the collected inflammatory and nutritional scores, PLR (p = 0.240) and mGPS (p = 0.184) were determined to be not significantly different, but NLR (p = 0.023) and PNI (p = 0.001) were found to be significantly worse in the high CONUT group than in the low CONUT group. There were no significant differences in any of the tumor-related factors between the two groups.
Operative factors and short-term surgical results
In Table 3, comparisons of operative factors and short-term surgical results are summarized. In terms of significant comparisons, only operative time was significantly different, which was longer in the high CONUT group (p = 0.007). Postoperative complications, which are one of the poor prognosis factors in patients with ICC [22, 23], were not significantly different between the two groups (p = 0.785). The mortality rate was also not significantly different between the two groups (p = 0.187).
Impacts of CONUT on RFS and OS
The 1-, 3-, and 5-year RFS rates were 57.9, 24.6, and 8.2% in the high CONUT group and 71.6, 36.6, and 32.5% in the low CONUT group, respectively. However, there were no statistically significant differences in the RFS rates between the two groups (log-rank p = 0.0734). On the other hand, the 1-, 3-, and 5-year OS rates were 78.3, 55.8, and 39.0% in the high CONUT group and 94.4, 80.2, and 62.5% in the low CONUT group, respectively. In this respect, the patients in the high CONUT group demonstrated significantly poorer prognosis than those in the low CONUT group (log-rank p = 0.0149) (Fig. 1).
CONUT is an independent prognostic factor in ICC
In the current study, CONUT was not statistically associated with RFS (HR 1.58, 95% CI 0.85–2.9, p = 0.146) (Supplementary Table 1). However, CONUT was found to be an independent predictor of poor OS (HR 3.02, 95% CI 1.4–6.8, p = 0.007), with several factors such as lymph node metastasis (HR 3.44, 95% CI 1.2–8.5, p = 0.022) and postoperative complications (HR 3.11, 95% CI 1.3–7.0, p = 0.012) (Table 4). The other preoperative inflammatory and nutritional scores such as NLR, PLR, mGPS, and PNI were not independent predictors of either RFS or OS in the current study (Supplementary Fig. 1).
Discussion
To our knowledge, this current study is the first report of the associations between CONUT and surgical results of patients with ICC following curative hepatectomy. We considered data from 71 patients with ICC, and our findings suggest that CONUT may be a prognostic factor and that it may also be superior to other inflammation-based markers in terms of predictive ability for prognosis.
Several reports show that cancer progression is not only affected by the malignant features of the tumor cells themselves but also is stimulated by local inflammatory and host systemic reactions [24]. Alb and T-LC reflect the host’s nutritional status, systemic inflammation [25,26,27]. Several inflammation markers that include Alb or T-LC, such as PLR, mGPS, and PNI, are associated with a patient’s prognosis [9, 10, 13]. As for cancer immunology, NLR has been reported to be related to poor anti-tumor immunity with low accumulation of tumor-infiltrating CD3+ T cells, CD4+ T cell, CD8+ T cell and could be a poor biomarker for prognosis in ICC [8, 28]. In addition, high NLR has to be also reported itself reflects high accumulation of tumor-associated macrophages, which means poor anti-tumor immunity, in patients with HCC [27]. Our study showed NLR was higher in the high CONUT groups (Table 2), and CONUT score and NLR recognized a significant positive correlation (r = 0.494, p = 0.0017) (Supplementary Fig. 2). Therefore, high CONUT score would also mean poor anti-tumor immunity. In the current study, we performed a multivariate analysis incorporating several factors in the study of inflammatory markers in patients with ICC and determined only CONUT to be a significantly independent prognostic factor.
The difference between CONUT and the other inflammatory markers includes T-Cho, which has also been reported to correlate with tumor progression and patient survival rates with respect to various cancers [29, 30]. Villa et al. [31] reported that the presence of a lower serum cholesterol concentration was indicative of increased metabolism and consumption of cholesterol for the growth of the tumor cells. Calleros et al. [32] also reported that it increases nuclear factor-κ B (NF-κB) and p38 mitogen-activated protein kinase (p38 MAPK) activity, which could induce the proliferation of tumor cells. Moreover, Itatsu et al. [33] demonstrated that the NF-κB activation was associated with upregulation of matrix metalloproteinase-9 (MMP-9). MMP-9 destroys the extracellular matrix and plays a critical role in tumor progression in ICC [34]. This mechanism leads to the aggressive phenotype of ICC. Thus, lower T-Cho may be associated with tumor progression and patients’ prognosis in ICC. However, there was no significant difference in RFS and OS observed based on the value of T-Cho (i.e., normal range; 149 ≦ T-Cho < 200 versus abnormal range; T-Cho ≧ 200 or T-Cho < 149) in the current study (data not shown). However, CONUT consists of not only T-Cho but also includes Alb and T-LC; therefore, CONUT may conceal these factors’ individual shortcomings and instead emphasize the merit of each parameter than do the other inflammatory and nutritional factors.
The current study has several limitations. First, it is retrospectively designed and includes a relatively small number of 71 patients from a single institution. Second, several factors that affect inflammation-based and nutritional scores, such as medications, are included. However, the current study is the first known report of the association between CONUT and prognosis in patients with ICC. Therefore, this study may be a meaningful study. However, to confirm our findings, a large-scale prospective validation study is required.
Conclusion
In conclusion, the current study showed that CONUT could predict long-term survival in patients with ICC after curative hepatectomy and that it may be useful to help identify patients who require adjuvant chemotherapy and more careful follow-up.
References
Khan SA, Taylor-Robinson SD, Toledano MB et al (2002) Changing international trends in mortality rates for liver, biliary and pancreatic tumours. J Hepatol 37:806–813
Shaib YH, Davila JA, McGlynn K, El-Serag HB (2004) Rising incidence of intrahepatic cholangiocarcinoma in the United States: a true increase? J Hepatol 40:472–477
Yoon H, Min JK, Lee JW et al (2011) Acquisition of chemoresistance in intrahepatic cholangiocarcinoma cells by activation of AKT and extracellular signal-regulated kinase (ERK)1/2. Biochem Biophys Res Commun 405:333–337
de Jong MC, Nathan H, Sotiropoulos GC et al (2011) Intrahepatic cholangiocarcinoma: an international multi-institutional analysis of prognostic factors and lymph node assessment. J Clin Oncol 29:3140–3145
Ohtsuka M, Ito H, Kimura F et al (2002) Results of surgical treatment for intrahepatic cholangiocarcinoma and clinicopathological factors influencing survival. Br J Surg 89:1525–1531
Hanahan D, Weinberg RA (2011) Hallmarks of cancer: the next generation. Cell 144:646–674
Mantovani A, Allavena P, Sica A, Balkwill F (2008) Cancer-related inflammation. Nature 454:436–444
Lin G, Liu Y, Li S et al (2016) Elevated neutrophil-to-lymphocyte ratio is an independent poor prognostic factor in patients with intrahepatic cholangiocarcinoma. Oncotarget 7:50963–50971
Chen Q, Dai Z, Yin D et al (2015) Negative impact of preoperative platelet-lymphocyte ratio on outcome after hepatic resection for intrahepatic cholangiocarcinoma. Medicine (Baltimore) 94:e574
Okuno M, Ebata T, Yokoyama Y et al (2016) Evaluation of inflammation-based prognostic scores in patients undergoing hepatobiliary resection for perihilar cholangiocarcinoma. J Gastroenterol 51:153–161
Yoshida N, Harada K, Baba Y et al (2017) Preoperative controlling nutritional status (CONUT) is useful to estimate the prognosis after esophagectomy for esophageal cancer. Langenbecks Arch Surg 402:333–341
Yoshida N, Baba Y, Shigaki H et al (2016) Preoperative nutritional assessment by controlling nutritional status (CONUT) is useful to estimate postoperative morbidity after esophagectomy for esophageal cancer. World J Surg 40:1910–1917. doi:10.1007/s00268-016-3549-3
Zhang C, Wang H, Ning Z et al (2016) Prognostic nutritional index serves as a predictive marker of survival and associates with systemic inflammatory response in metastatic intrahepatic cholangiocarcinoma. Onco Targets Ther 9:6417–6423
Ignacio de Ulibarri J, Gonzalez-Madrono A, de Villar NG et al (2005) CONUT: a tool for controlling nutritional status. First validation in a hospital population. Nutr Hosp 20:38–45
Tokunaga R, Sakamoto Y, Nakagawa S et al (2017) CONUT: a novel independent predictive score for colorectal cancer patients undergoing potentially curative resection. Int J Colorectal Dis 32:99–106
Yamashita Y, Taketomi A, Morita K et al (2008) The impact of surgical treatment and poor prognostic factors for patients with intrahepatic cholangiocarcinoma: retrospective analysis of 60 patients. Anticancer Res 28:2353–2359
Edge S, Byrd DR, Compton CC et al (2010) AJCC cancer staging manual, 7th edn. Springer, New York
Yamashita YI, Wang H, Kurihara T et al (2016) Clinical significances of preoperative classification of intrahepatic cholangiocarcinoma: different characteristics of perihilar vs. peripheral ICC. Anticancer Res 36:6563–6569
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Pinato DJ, North BV, Sharma R (2012) A novel, externally validated inflammation-based prognostic algorithm in hepatocellular carcinoma: the prognostic nutritional index (PNI). Br J Cancer 106:1439–1445
Chan AW, Chan SL, Wong GL et al (2015) Prognostic nutritional index (PNI) predicts tumor recurrence of very early/early stage hepatocellular carcinoma after surgical resection. Ann Surg Oncol 22:4138–4148
Doussot A, Lim C, Gomez Gavara C et al (2016) Multicentre study of the impact of morbidity on long-term survival following hepatectomy for intrahepatic cholangiocarcinoma. Br J Surg 103:1887–1894
Miyata T, Yamashita YI, Yamao T et al (2017) Prognostic impacts of postoperative complications in patients with intrahepatic cholangiocarcinoma after curative operations. Int J Clin Oncol 22:526–532
Liu Y, Cao X (2016) Characteristics and significance of the pre-metastatic niche. Cancer Cell 30:668–681
McMillan DC, Watson WS, O’Gorman P et al (2001) Albumin concentrations are primarily determined by the body cell mass and the systemic inflammatory response in cancer patients with weight loss. Nutr Cancer 39:210–213
Halazun KJ, Hardy MA, Rana AA et al (2009) Negative impact of neutrophil-lymphocyte ratio on outcome after liver transplantation for hepatocellular carcinoma. Ann Surg 250:141–151
Mano Y, Shirabe K, Yamashita Y et al (2013) Preoperative neutrophil-to-lymphocyte ratio is a predictor of survival after hepatectomy for hepatocellular carcinoma: a retrospective analysis. Ann Surg 258:301–305
Gomez D, Morris-Stiff G, Toogood GJ et al (2008) Impact of systemic inflammation on outcome following resection for intrahepatic cholangiocarcinoma. J Surg Oncol 97:513–518
Okuyama H, Ichikawa Y, Sun Y et al (2007) Cancer and all-cause mortalities are lower in the higher total cholesterol groups among general populations. World Rev Nutr Diet 96:37–54
Jiang SS, Weng DS, Jiang L et al (2016) The clinical significance of preoperative serum cholesterol and high-density lipoprotein-cholesterol levels in hepatocellular carcinoma. J Cancer 7:626–632
Villa GR, Hulce JJ, Zanca C et al (2016) An LXR-cholesterol axis creates a metabolic co-dependency for brain cancers. Cancer Cell 30:683–693
Calleros L, Lasa M, Toro MJ, Chiloeches A (2006) Low cell cholesterol levels increase NFkappaB activity through a p38 MAPK-dependent mechanism. Cell Signal 18:2292–2301
Itatsu K, Sasaki M, Harada K et al (2009) Phosphorylation of extracellular signal-regulated kinase 1/2, p38 mitogen-activated protein kinase and nuclear translocation of nuclear factor-kappaB are involved in upregulation of matrix metalloproteinase-9 by tumour necrosis factor-alpha. Liver Int 29:291–298
Mon NN, Hasegawa H, Thant AA et al (2006) A role for focal adhesion kinase signaling in tumor necrosis factor-alpha-dependent matrix metalloproteinase-9 production in a cholangiocarcinoma cell line, CCKS1. Cancer Res 66:6778–6784
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
Use of the clinical data in this study was approved by the human ethics review committee of the graduate school of medicine, Kumamoto University.
Electronic supplementary material
Below is the link to the electronic supplementary material.
268_2017_4214_MOESM2_ESM.tiff
Figure shows relapse-free survival and overall survival in patients with ICC after curative hepatectomy according to NLR (a, b), PLR (c, d), mGPS (e, f), and PNI (g, h). There is no significant difference between the two groups with respect to any of the biomarkers in this figure. (TIFF 3565 kb)
268_2017_4214_MOESM3_ESM.tiff
Figure shows the relation between CONUT score and NLR. CONUT score and NLR recognized a significant positive correlation (r = 0.494, p = 0.0017). (TIFF 16352 kb)
Rights and permissions
About this article
Cite this article
Miyata, T., Yamashita, Yi., Higashi, T. et al. The Prognostic Impact of Controlling Nutritional Status (CONUT) in Intrahepatic Cholangiocarcinoma Following Curative Hepatectomy: A Retrospective Single Institution Study. World J Surg 42, 1085–1091 (2018). https://doi.org/10.1007/s00268-017-4214-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-017-4214-1