Abstract
Purpose
The acute primary (first-time) lateral patellar dislocation is associated with a high rate of functional disability. There is no consensus as to the choice of surgical or non-surgical treatment for these patients. The aim of this study is to compare the clinical results between the surgical (reconstruction of the medial patellofemoral ligament [MPFL]) and non-surgical treatments for acute primary patellar dislocations.
Methods
Sixty-nine skeletally mature patients (69 knees) were included in this prospective non-randomized controlled trial. At least one predisposing factor for patellar dislocation (including patella alta, high lateral patellar tilt, trochlear dysplasia, and increased TT-TG distance) was identified in the included patients. Thirty patients were treated surgically with MPFL reconstruction, and the other 39 patients were treated non-surgically. The main outcome variable was patellar redislocation within a two year follow-up period. The Kujala questionnaire was applied for analyzing the pain and the quality of life. The additional surgeries due to patellofemoral problems were also recorded.
Results
Patellar redislocation occurred in eight patients in the non-surgical group, while no redislocation occurred in the surgical group (P < 0.05). Four patients in non-surgical group underwent further surgery due to patellar redislocation and poor function during the follow-up period. The Kujala score and the percentage of “good/excellent” results on the Kujala score of the surgical group were significantly better than that of the non-surgical group (P < 0.05).
Conclusions
The surgical MPFL reconstruction achieved better clinical outcomes compared with non-surgical treatment for the acute primary patellar dislocation in the skeletally mature patients with the presence of abnormal patellofemoral anatomy. Surgery should be considered as the better choice for these specific patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Acute primary (first-time) lateral patellar dislocation refers to traumatic disruption of the previously uninjured medial peripatellar structures [1]. Amongst the general population, primary patellar dislocation incidences account for about 6 per 100,000 [2]. Further, it is a common cause of traumatic haemarthrosis of the knee, and may lead to knee pain, decreased level sporting activity, and patellofemoral osteoarthrosis [3].
Most primary patellar dislocations have been traditionally treated non-surgically, with exception in patients with chondral or osteochondral fragments [4, 5]. However, high rates of redislocation, anterior knee pain, and functional disability have been reported in prior studies after non-surgical treatment [3, 6]. From a lack of curative effects and advances in understanding the anatomy and biomechanics of the patellofemoral joint, there is a trend of initial surgical treatment for primary patellar dislocation [4, 5]. In addition, inconsistent results based on previous studies comparing surgical with non-surgical strategies have been reported, with some authors regarding that initial surgery could improve outcomes [7,8,9,10]. While, other studies did not advocate repair of the medial patellar stabilizing tissues [11,12,13]. It is worth noting that the previous case-control trials enrolled subjects ranged widely in ages, and whether the predisposing factors for patellar instability play a role in final results were not addressed. Therefore, the best treatment for patients with primary patellar dislocation remains a controversial issue.
Biomechanical studies have confirmed that the medial patellofemoral ligament (MPFL) is the primary medial stabilizer of the patella [14]. Up to 94–100% of patients suffer from medial MPFL injuries after a complete lateral patellar dislocation [15, 16]. Several authors have reported satisfactory results with the use of MPFL reconstruction in the treatment of recurrent or habitual patellar instability [17,18,19,20,21]. However, there clearly lacks evidence whether the MPFL reconstruction strategy could achieve satisfactory clinical results than non-surgical treatment in primary dislocation patients. Thus, the purpose of this study was to compare the clinical results of the two kinds of approaches after first-time patellar dislocation. We hypothesized that the surgical MPFL reconstruction would result in better clinical results and lower redislocation rate than non-surgical treatment.
Materials and methods
This prospective controlled trial was carried out with the approvement of the ethics committee of our institution. Patients diagnosed with primary patellar dislocation were enrolled in the study, and each patient was provided written informed consent. The diagnosis was based on a first episode of laterally patellofemoral dislocation, intra-articular haematoma, tenderness of the medial retinaculum, and a positive apprehension test on physical examination. Initial radiographic evaluation included anteroposterior and lateral views of the knee, and axial patellar radiographs with 30° of flexion. The computed tomography (CT) was performed to detect trochlear dysplasia, and to examine the patellar tilt, tibial tuberosity trochlear groove (TT-TG) distance. Magnetic resonance imaging (MRI) was used to confirm the injury of the MPFL, and to detect potential chondral or osteochondral fragments. The inclusion criteria were as follows: (1) Patients with first-time lateral dislocation of patella up to seven days before treatment, (2) unilateral knee involved, (3) skeletally mature patients older than 16 years, (4) no coexistent knee ligament injuries and previous surgery on the involved knee, (5) absence of chondral or osteochondral fragments, (6) at least one predisposing factor for patellar dislocation was identified. The predisposing factors for patellar dislocation according to the reports of Dejour et al. include patella alta (Caton-Deschamps index greater than or equal to 1.2), lateral patellar tilt (more than 20°), trochlear dysplasia (according to classification of Dejour et al.), and increased TT-TG distance (more than 20 mm) [22, 23]. Patients were excluded if they did not meet the inclusion criteria, were unable to comply with the treatment protocol, and could not finish the follow-up. After diagnosis was made, the protocol was explained to the patient. The decision whether to treat surgically or non-surgically was made by the patient and/or his guardian.
For the non-surgical treatment patients, one or more aspirations were performed to eliminate hemarthrosis and to relieve pain. Quadriceps strengthening exercises were initiated as soon as tolerated by the patient. During the first three weeks, non-weight bearing was permitted and the knee was protected with a long hinged knee brace allowing 0° to 30° passive motion. From three to six weeks, flexion was allowed to progress to 90°, and partial weight bearing was permitted within the patients’ tolerance. At six weeks, the knee brace could be removed, and the patients were allowed to perform active knee motion and full weight bearing exercises. Patients were encouraged to return to sports activities in about six months post-injuries.
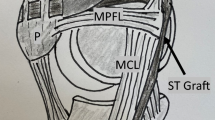
In the MPFL reconstruction group, arthroscopy was routinely performed to assess the MPFL lesion site and tracking of the patella, and to rule out osteochondral fragments. The lateral patellar retinaculum release was performed if the patella could not be everted to neutral. A 2–3-cm longitudinal incision was made at the anteromedial side of the patella, and then the soft tissue and patellar periosteum were peeled back. A 3-mm-depth bony groove was created from the superomedial corner of the patella to the midpoint of the patella using the rongeur (Fig. 1). Tibialis anterior allograft was used with both the free ends sutured in a whipstitch style. One 3.0-mm diameter suture anchor (Suture Anchors, BioComposite SutureTak, Arthrex, Naples, FL, USA) was used to strengthen graft fixation (Fig. 2). The middle part of the graft was put into the bony groove with the sutures on the anchor tied (Fig. 3). Interrupted sutures of patellar fascia were then used to fix the graft (Fig. 4). Thus, a bone-fascia tunnel, two thirds of which formed by the cancellous bone groove and the other one third formed by the covered fascia, was produced at the medial margin of the patella. A 6-mm-wide tunnel was prepared at the anatomical femoral insertion of MPFL under the guidance of intra-operative fluoroscopy. The free ends of the graft were then pulled through the subcutaneous fascial layers, pulled into the femoral tunnel, and fixed with an absorbable interference screw (BioComposite Interference Screw, Arthrex, Naples, FL, USA) (Fig. 5). The post-operative rehabilitation protocol was the same as non-operative treatment group.
The main outcome variable was patellar redislocation within a two year follow-up period. The functional outcome was evaluated by subjective clinical assessments by use of the Kujala score at two years [24]. The Kujala score was qualitatively categorized as excellent/good (85 or more), fair (between 65 and 84), and poor (64 or less) [7]. Complications and additional surgeries due to patellofemoral problems were also recorded. Radiograph examinations were not routinely performed during the follow-up period. All the included cases were followed for two years after primary patellar dislocation.
Statistical analysis
The baseline characteristics of the two groups were compared using χ2 test for patient gender and side of affected knee, and using Mann-Whitney test for patient age and the interval from injury to consulting day. The presence of predisposing factors between the two groups was compared using t tests for continuous variables, and χ2 test for nominal variables. Comparison of the Kujala score between the two groups was analyzed by t test. The Mann-Whitney U was used to test differences of the Kujala categories. Comparisons of redislocation and range of motion deficit between the two groups were analyzed by Fisher exact test. The level of significance was set at P < 0.05. SPSS software (version 19.0; SPSS Inc., Chicago, IL) was used for data analysis.
Results
A total of 73 patients with the diagnosis of a primary patellar dislocation met the criteria, and were recruited in this study from 2012 to 2015. Thirty-one patients were initially treated surgically with the reconstruction of the MPFL and 42 non-surgically. Four patients (1 in the surgical group and 3 in the non-surgical group) were lost within a two year follow-up. Finally, 69 patients (30 in the surgical group and 39 in the non-surgical group) with a mean age of 18 (15–26) years completed the final follow-up for analysis. The epidemiologic data showed no difference between the two groups with respect to gender, age, side of affected knee, and the interval from injury to consulting day (Table 1). The presence of predisposing factors was comparable in both groups with no statistical difference (Table 2).
There was no case of neurological, vascular, or wound complication in the surgical group. However, one patient with flexion deficit underwent additional arthrolysis due to joint conglutination in operative group (Table 3). The subjective assessment of symptoms and functions are shown in Table 3. The results from the Kujala score showed that the surgical group presented better score when compared with the non-surgical group at the final follow-up evaluation. The analysis also indicated that the populations of Kujala score are not equal in patients receiving MPFL reconstruction and non-surgical treatment, with higher percentage of good/excellent results observed in surgical group.
In relation to patellar redislocation, there was no report of recurrence in the surgical group. It was noted that 20.5% (8 of the 39) non-surgically treated patients presented with recurrence at a two year follow-up. Four patients underwent further surgery due to patellar redislocation and poor functional results during the follow-up period. It was worth noting that one patient presented with severe patellar osteochondral fracture during recurrence of patellar dislocation.
Discussion
The most important finding of the present study was that surgical treatment with MPFL reconstruction produced the better final results of the Kujala score, and significantly reduced the risk of patellar redislocation compared to non-surgical strategy for treatment of acute primary patellar dislocation in patients with abnormal patellofemoral anatomy.
The presence of abnormal patellofemoral anatomy was reported to be associated with patellar dislocation. The major instability factors include trochlear dysplasia, patella alta, increased TT-TG distance, and the high lateral patella tilt [23, 25]. Steensen et al. reported that at least one anatomic risk factor was identified in 58.3% of patients with recurrent dislocation compared with only 1.7% of patients without histories of patellar dislocation [26]. Balcarek et al. [27] and Seeley et al. [28] also reported that anatomic abnormalities contributed to patellofemoral instability in first-time patellar dislocation patients, and more than 30% of patients suffered subsequent recurring dislocations. In addition, there was a strong trend of association between recurrence and both TT-TG distance and lateral trochlear inclination (LTI) [28]. We believe that the presence of abnormal anatomic factors play an important role in the recurrence after primary acute patellar dislocation. Unfortunately, none of the previous comparative studies took the predisposing factors for patellar dislocation into account. The strength of the evidence could be weakened due to the mixed population analyzed together. In our study, only acute patellar dislocation patients with at least one predisposing factor identified were included. On the basis of current results, we found that patients who underwent surgical treatment reached lower risk of redislocation and a higher quantitative Kujala score. When analyzing Kujala score qualitatively according to the Bitar et al. study [7], the results still showed superiority of the surgical group. It seems reasonable to assume that, if primary patellar dislocation has occurred and predisposing anatomic factor is identified, the ideal management would be operation rather than conservative treatment.
Biomechanical and clinical studies have confirmed that MPFL is the primary passive restraint to patellar lateral dislocation. Up to 94–100% of patients suffered from MPFL rupture after acute patellar dislocation, and even some authors suggested that lateral patellar dislocation was frankly impossible without damage to the MPFL [16]. Several reports focusing on the injury location of the MPFL based on MRI findings after patellar dislocation have been published. Ruptures of the MPFL could be complete or partial, and the injury site could be categorized into four types including the patellar insertion zone, the femoral insertion zone, the midsubstance, and combined injury [27]. Since some authors have suggested that the injury pattern of MPFL may contribute to recurrence in the treatment to primary dislocation, the severity and identification of the rupture site are crucial to achieve a satisfactory result [16, 29]. However, it is actually difficult to differentiate the midsubstance injury from patellar or femoral injury pattern, especially when the injury occurs in the midsubstance but close to the femoral origin [16]. In addition, multiple site injuries to the MPFL were found in more than 20% of patients after acute lateral patellar dislocation [27, 30]. These negative factors made the medial patellar stability restoration difficult by simple repair, and the overall success would inevitably be undermined. We reviewed the clinical trials comparing surgical with conservative treatment for primary patellar dislocation. Most of the authors reported that surgical treatment did not reduce the risk of redislocation nor did it improve the subjective functional outcomes [11,12,13]. It should be noted that all these studies adopted repair of the medial patellar stabilizing structures with no injury regions were identified. This may be the main reason why they did not find any difference between the surgical and non-surgical treatment strategies. Therefore, MPFL reconstruction may be a more reliable method of stabilizing the patella than MPFL repair [5, 31]. Our initial MPFR reconstruction technique significantly reduced the number of patellar redislocation (none), and presented encouraging results for patient after first-time patellar dislocation within a two year follow-up.
Anatomically, the MPFL is a thin band of soft tissue components that extends from the medial aspect of the patella to its femoral attachment near the adductor tubercle, with a fan-shaped attachment at the patellar side [32, 33]. Numerous surgical techniques for the reconstruction of MPFL have been described, such as single-bundle reconstruction and anatomical double-bundle reconstruction. Bitar et al. treated the acute patellar dislocation with MPFL reconstruction technique, which could be regarded as single-bundle reconstruction with autogeneous patellar tendon [7]. They reported that operative treatment resulted in better subjective outcomes, although potential risks of graft shortness, patellar fracture, and anterior knee pain were not reported. Other work has demonstrated that the single-bundle reconstruction technique actually lost the normal MPFL shape, and may lead to ligament laxity or failure with the passage of time [34]. From a biomechanical view, the double-bundle anatomical reconstruction could restore the biomechanical function to the maximum extent [34]. We constructed the MPFL reconstruction with a bone-fascia tunnel made at the medial margin of the patella. This double-bundle technique restored the anatomical fan-shaped structure of the original MPFL, and provided satisfactory tendon-bone healing. Our study has proved that it was a safe technique, which could avoid the potential risk of patellar fracture and restore patellofemoral kinematics and stability effectively.
There were several limitations to our study, including the non-randomized study design and the small sample size. The short-term follow-up time is another drawback of this study because the advantages of surgical strategies would diminish over time [10, 11].
Conclusions
Outcomes of this study indicated that the surgical MPFL reconstruction technique significantly reduced the risk of recurrent patellar dislocation, and produced better functional results compared with non-surgical treatment for acute primary patellar dislocation in the skeletally mature patients with the presence of abnormal patellofemoral anatomy.
References
Tsai CH, Hsu CJ, Hung CH, Hsu HC (2012) Primary traumatic patellar dislocation. J Orthop Surg Res 7:21
Smith TO, Song F, Donell ST, Hing CB (2011) Operative versus non-operative management of patellar dislocation. A meta-anal-ysis. Knee Surg Sports Traumatol Arthrosc 19:988–998
Atkin DM, Fithian DC, Marangi KS, Stone ML, Dobson BE, Mendelsohn C (2000) Characteristics of patients with primary acute lateral patellar dislocation and their recovery within the first 6 months of injury. Am J Sports Med 28:472–479
Stefancin JJ, Parker RD (2007) First-time traumatic patellar dislocation: a systematic review. Clin Orthop Relat Res 455:93–101
Panni AS, Vasso M, Cerciello S (2013) Acute patellar dislocation. What to do? Knee Surg Sports Traumatol Arthrosc 21:275–278
Mehta VM, Inoue M, Nomura E, Fithian DC (2007) An algorithm guiding the evaluation and treatment of acute primary patellar dislocations. Sports Med Arthrosc Rev 15:78–81
Bitar AC, Demange MK, D'Elia CO, Camanho GL (2012) Traumatic patellar dislocation: nonoperative treatment compared with MPFL reconstruction using patellar tendon. Am J Sports Med 40:114–122
Zheng X, Kang K, Li T, Lu B, Dong J, Gao S (2014) Surgical versus non-surgical management for primary patellar dislocations: an up-to-date meta-analysis. Eur J Orthop Surg Traumatol 24:1513–1523
Saccomanno MF, Sircana G, Fodale M, Donati F, Milano G (2016) Surgical versus conservative treatment of primary patellar dislocation. A systematic review and meta-analysis. Int Orthop 40:2277–2287
Regalado G, Lintula H, Kokki H, Kröger H, Väätäinen U, Eskelinen M (2016) Six-year outcome after non-surgical versus surgical treatment of acute primary patellar dislocation in adolescents: a prospective randomized trial. Knee Surg Sports Traumatol Arthrosc 24:6–11
Palmu S, Kallio PE, Donell ST, Helenius I, Nietosvaara Y (2008) Acute patellar dislocation in children and adolescents: a randomized clinical trial. J Bone Joint Surg Am 90:463–470
Apostolovic M, Vukomanovic B, Slavkovic N, Vuckovic V, Vukcevic M, Djuricic G, Kocev N (2011) Acute patellar dislocation in adolescents: operative versus nonoperative treatment. Int Orthop 35:1483–1487
Petri M, Liodakis E, Hofmeister M, Despang FJ, Maier M, Balcarek P, Voigt C, Haasper C, Zeichen J, Stengel D, Krettek C, Frosch KH, Lill H, Jagodzinski M (2013) Operative vs conservative treatment of traumatic patellar dislocation: results of a prospective randomized controlled clinical trial. Arch Orthop Trauma Surg 133:209–213
Bedi H, Marzo J (2010) The biomechanics of medial patellofemoral ligament repair followed by lateral retinacular release. Am J Sports Med 38:1462–1467
Nomura E (1999) Classification of lesions of the medial patello-femoral ligament in patellar dislocation. Int Orthop 23:260–263
Kang HJ, Wang F, Chen BC, Zhang YZ, Ma L (2013) Non-surgical treatment for acute patellar dislocation with special emphasis on the MPFL injury patterns. Knee Surg Sports Traumatol Arthrosc 21:325–331
Pesenti S, Ollivier M, Escudier JC, Cermolacce M, Baud A, Launay F, Jouve JL, Choufani E (2018) Medial patellofemoral ligament reconstruction in children: do osseous abnormalities matter? Int Orthop 42:1357–1362
Li J, Li Y, Wei J, Wang J, Gao S, Shen Y (2014) A simple technique for reconstruction of medial patellofemoral ligament with bone-fascia tunnel fixation at the medial margin of the patella: a 6-year-minimum follow-up study. J Orthop Surg Res 9(66)
Matsushita T, Oka S, Araki D, Nishida K, Tanaka T, Kanzaki N, Nishida K, Kuroda R (2017) Patient-based outcomes after medial patellofemoral ligament reconstruction. Int Orthop 41:1147–1153
Malecki K, Fabis J, Flont P, Lipczyk Z, Niedzielski K (2016) Preliminary results of two surgical techniques in the treatment of recurrent patellar dislocation: medial patellofemoral ligament reconstruction versus combined technique of vastus medialis advancement, capsular plasty and Roux-Goldthwait procedure in treatment of recurrent patellar dislocation. Int Orthop 40:1869–1874
Wang HD, Dong JT, Gao SJ (2016) Medial patellofemoral ligament reconstruction using a bone groove and a suture anchor at patellar: a safe and firm fixation technique and 3-year follow-up study. J Orthop Surg Res 11:138
Dejour H, Walch G, Nove-Josserand L, Guier C (1994) Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc 2:19–26
Dejour D, Le Coultre B (2007) Osteotomies in patello-femoral instabilities. Sports Med Arthrosc Rev 15:39–46
Kujala UM, Jaakkola LH, Koskinen SK, Taimela S, Hurme M, Nelimarkka O (1993) Scoring of patellofemoral disorders. Arthroscopy 9:159–163
Hernigou J, Chahidi E, Bouaboula M, Moest E, Callewier A, Kyriakydis T, Koulalis D, Bath O (2018) Knee size chart nomogram for evaluation of tibial tuberosity-trochlear groove distance in knees with or without history of patellofemoral instability. Int Orthop. https://doi.org/10.1007/s00264-018-3856-4
Steensen RN, Bentley JC, Trinh TQ, Backes JR, Wiltfong RE (2015) The prevalence and combined prevalences of anatomic factors associated with recurrent patellar dislocation: a magnetic resonance imaging study. Am J Sports Med 43:921–927
Balcarek P, Ammon J, Frosch S, Walde TA, Schüttrumpf JP, Ferlemann KG, Lill H, Stürmer KM, Frosch KH (2010) Magnetic resonance imaging characteristics of the medial patellofemoral ligament lesion in acute lateral patellar dislocations considering trochlear dysplasia, patella alta, and tibial tuberosity-trochlear groove distance. Arthroscopy 26:926–935
Seeley M, Bowman KF, Walsh C, Sabb BJ, Vanderhave KL (2012) Magnetic resonance imaging of acute patellar dislocation in children: patterns of injury and risk factors for recurrence. J Pediatr Orthop 32:145–155
Petri M, Ettinger M, Stuebig T, Brand S, Krettek C, Jagodzinski M, Omar M (2015) Current concepts for patellar dislocation. Arch Trauma Res 4:e29301
Zheng L, Shi H, Feng Y, Sun BS, Ding HY, Zhang GY (2015) Injury patterns of medial patellofemoral ligament and correlation analysis with articular cartilage lesions of the lateral femoral condyle after acute lateral patellar dislocation in children and adolescents: an MRI evaluation. Injury 46:1137–1144
Du H, Tian XX, Guo FQ, Li XM, Ji TT, Li B, Li TS (2017) Evaluation of different surgical methods in treating recurrent patella dislocation after three-dimensional reconstruction. Int Orthop 41(12):2517–2524
Steensen RN, Dopirak RM, McDonald WG 3rd (2004) The anatomy and isometry of the medial patellofemoral ligament: implications for reconstruction. Am J Sports Med 32:1509–1513
Aragão JA, Reis FP, de Vasconcelos DP, Feitosa VL, Nunes MA (2008) Metric measurements and attachment levels of the medial patellofemoral ligament: an anatomical study in cadavers. Clinics (Sao Paulo) 63:541–544
Wang CH, Ma LF, Zhou JW, Ji G, Wang HY, Wang F, Wang J (2013) Double-bundle anatomical versus single-bundle isometric medial patellofemoral ligament reconstruction for patellar dislocation. Int Orthop 37:617–624
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict interest.
Rights and permissions
About this article
Cite this article
Zheng, X., Hu, Y., Xie, P. et al. Surgical medial patellofemoral ligament reconstruction versus non-surgical treatment of acute primary patellar dislocation: a prospective controlled trial. International Orthopaedics (SICOT) 43, 1495–1501 (2019). https://doi.org/10.1007/s00264-018-4243-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-018-4243-x