Abstract
Cancer vaccine trials frequently report on immunological responses, without any clinical benefit. This paradox may reflect the challenge of discriminating between effective and pointless immune responses and sparse knowledge on their long-term development. Here, we have analyzed T cell responses in long-term survivors after peptide vaccination. There were three main study aims: (1) to characterize the immune response in patients with a possible clinical benefit. (2) To analyze the long-term development of responses and effects of booster vaccination. (3) To investigate whether the Th1/Th2-delineation applies to cancer vaccine responses. T cell clones were generated from all nine patients studied. We find that surviving patients harbor durable tumor-specific responses against vaccine antigens from telomerase, RAS or TGFβ receptor II. Analyses of consecutive samples suggest that booster vaccination is required to induce robust T cell memory. The responses exhibit several features of possible clinical advantage, including combined T-helper and cytotoxic functionality, recognition of naturally processed antigens and diverse HLA-restriction and fine-specificity. CD4−CD8− T cell clones display unconventional cytotoxicity and specifically kill tumor cells expressing mutated TGFβ receptor II. Cytokine profiling on the long-term survivors demonstrates high IFNγ/IL10-ratios, favoring immunity over tolerance, and secretion of multiple chemokines likely to mobilize the innate and adaptive immune system. Interestingly, these pro-inflammatory cytokine profiles do not follow a Th1/Th2-delineation. Most IFNγhigh/IL4low/IL10low cultures include high concentrations of hallmark Th2-cytokines IL-5 and IL-13. This does not reflect a mixture of Th1- and Th2-clones, but applies to 19/20 T cell clones confirmed to be monoclonal through TCR clonotype mapping. The present study identifies several factors that may promote clinical efficacy and suggests that cytokine profiling should not rely on the Th1/Th2-paradigm, but assess the overall inflammatory milieu and the balance between key cytokines.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Immune responses against tumor antigens have been demonstrated in a number of cancer vaccine trials. Clinical responses, however, are less frequent, and the comparison of immune responses and clinical outcome often produces confusing results. In the majority of trials, tumor regression or prolonged survival is observed only for certain immune responders, while other “responders” have no apparent clinical benefit [44, 48, 54]. This paradox points to a need for refining immunological monitoring in vaccine trials and to improve our understanding of what characterizes the effective immune response.
The cytokine profile of an immune response may provide useful indications on clinical effect. According to the Th1/Th2-paradigm, effector T cells predominantly secrete either Th1- or Th2-cytokines. The Th1-group includes IFNγ, TNFα and IL-2, while IL-4, IL-5, IL-9, IL-10 and IL-13 are regarded as key Th2-cytokines [17, 36]. In an anti-tumor response, a Th1 profile is considered to be desirable. IFNγ may promote anti-tumor responses, e.g. by stimulating CD8+ T cells and macrophages, and by inducing HLA up-regulation on tumor cells [36]. In contrast, Th2-cytokines are believed to suppress anti-tumor activity because Th1- and Th2-responses have been shown to be mutually inhibitory [46]. Moreover, the Th2-like cytokine IL-10 is strongly associated with regulatory T cells and tumor tolerance [12, 28, 60].
In clinical trials, cytokine monitoring is often limited to one or two cytokines, but the data tend to be interpreted as indicators of an overall pattern. For instance, an IFNγhigh/IL-4low response is frequently referred to as “Th1”, suggesting that it is unlikely to include unmeasured Th2-cytokines like IL-5, IL-10 and IL-13. However, though there is substantial knowledge on the effects of individual Th1- or Th2 cytokines, the validity of the Th1/Th2-dichotomy for humans has been questioned [11, 26]. The Th1/Th2 delineation is to a large extent based on studies in mice models [45]. In the human system, most experimental data have been obtained in vitro by use of Th1/Th2 differentiation protocols [26]. The physiological setting is clearly different, and no genetic program has been identified that explain why cytokine patterns would fall into two distinct categories.
Here, we report in depth analyses of T cell responses in patients surviving for an extended time after cancer vaccination. Tumor specific T cell clones were generated from nine patients, from samples obtained 2–9 months (eight patients) or 9 years (one patient) after start of vaccination. There were three main study aims: (1) to characterize the immune response in patients with a possible clinical benefit, as suggested by unexpected survival times. (2) To analyze the long-term development of responses and effects of booster vaccination. (3) To investigate whether the Th1/Th2-delineation applies to responses elicited by cancer vaccination. The immunological characterisation focused on selected factors likely to be important for clinical efficacy: specificity, duration, diversity, cytokine profile and natural processing of vaccine antigens. The results demonstrate that the long term survivors harbor durable tumor-specific responses. Further, a diverse spectrum of T cell clones has been recruited, with different CD4/CD8 phenotypes, HLA-restrictions and functional properties. Regarding the Th1/Th2-question, we have previously reported surprisingly mixed Th1/Th2 cytokine patterns in three vaccinated melanoma patients, responding to unknown antigens encoded by tumor-mRNA [40, 41]. Here, we have analyzed responses with known specificity and have selected patients from seven vaccination protocols to obtain a general picture. As reported, we still find broad cytokine patterns not fitting with the Th1/Th2-dichotmy. Most data forming the basis of the Th1/Th2-theory have been obtained by analyzing T cell clones [45]. We therefore asked whether our broad cytokine patterns were due to a mixture of Th1- and Th2 clones. As reported, the results demonstrate mixed Th1/Th2-profiles even at the clonal level.
Materials and methods
Selection criteria
The present study was performed on nine cancer patients included in peptide vaccine trials in the period 1997–2005. The patients were selected for extended immunological studies after completion of routine monitoring, based on the following selection criteria: (1) measurable immune response. (2) Availability of samples for T cell cloning/long term monitoring. (3) Long term survival, compared to prognosis at start of vaccination. (4) Diversity with regard to vaccination protocol. The latter criterion was applied to obtain a general picture on the Th1/Th2-patterns after cancer vaccination. Not all clones generated from the patients could be subjected to the extensive cytokine profiling. For this purpose, clones were selected on the following criteria: (1) specificity for tumor antigens. (2) Diversity with regard to CD4/CD8 phenotype, cytotoxic/helper functionality, HLA-restriction and fine-specificity. The diversity criterion was again applied to obtain a general picture on the Th1/Th2 cytokine profiles. The present report includes all patients and all clones that were selected for cytokine profiling. The clone data from patient E are therefore reported here, though he was not a long term survivor.
Clinical trials
The clinical trials were conducted at Rikshospitalet University Hospital, Oslo, Norway, Ullevaal University Hospital (Oslo, Norway), Akershus University Hospital (Loerenskog, Norway) and Inselspital, Bern, Switzerland. The studies were approved by the appropriate regulatory authorities and ethical committees and performed in compliance with the World Medical Association Declaration of Helsinki. Written informed consent was obtained from the patients. Only minor side effects were observed, with no treatment related grade III or IV toxicity (NCI-common toxicity criteria).
Vaccination protocols and patient characteristics
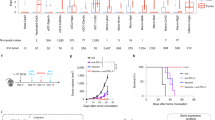
Patient characteristics, vaccination details and survival times are summarized in Table 1. The vaccination schedules started with a “priming period” of frequent vaccinations (weekly/biweekly), intended to provoke a T cell response. The clinical protocols that applied to patients A, C, D, E, F, G and H (not Bern melanoma trial or CTN frameshift) allowed for subsequent “booster vaccinations”, depending on clinical development and immunological response. The booster vaccines were administered at time points specified in each protocol. All vaccines were given as intradermal injections (right paraumbical area) with adjuvant GM-CSF.
Patient A received vaccinations with a 12-Val mutated p21 RAS peptide (p319), after identification of this mutation in her tumor biopsies [24]. K-RAS mutations in codon 12 are found in ~90% of pancreatic adenocarcinomas [1]. Patient B received vaccinations with a mutated TGFβRII peptide (p621) encompassing an HLA-A2 epitope (p573) plus two mutated BAX-peptides ([55] and Gaudernack et al. manuscript in preparation). The TGFβRII-mutation is present in 50–90% of colon cancers with microsatellite instability [43] and was demonstrated in biopsies from patient B. The patient is to date without tumor (5 and 1/2 years follow-up). Patients C and D (lung cancer) received vaccination with two peptides derived from hTERT, GV1001 and I540 [9]. Telomerase activity has been demonstrated in >90% of tumors, including tumor stem cells [29, 35, 50, 66]. Patient E was included in a GV1001 vaccination study on pancreatic cancer patients [6]. Patients F and G were included in a recently completed temozolomide + GV1001-vaccine trial (Kyte et al. manuscript in prep.). Temozolomide therapy started 7 days before the first vaccine injection and was administered 5 days/month until disease progression. Patient H was initially operated for Duke C colon cancer, but relapsed with liver metastases (Duke D) after 1 year. He was operated by hemihepatectomi and thereafter started vaccination with GV1001. Patient I was operated for stage IIB melanoma and received vaccinations with GV1001 and I540 as adjuvant therapy (Kernland Lang et al. manuscript in preparation). After 57 months follow-up, she has no evidence of tumor.
Peptides and recombinant hTERT protein
Vaccine peptides were manufactured in compliance with GMP. GV1001 (EARPALLTSRLRFIPK) and I540 (ILAKFLHWL) were produced by Avecia Biotechnology (Cheshire, England), manufactured by Isopharma AS (Kjeller, Norway) and released by GemVax AS (Porsgrunn, Norway). Peptides p319 (KLVVVGAVGVGKSALTI), p621 (KSLVRLSSCVPVALMSAMT) and p573 (RLSSCVPVA) were produced, manufactured and released by Norsk Hydro (Porsgrunn, Norway). Truncated peptides, consisting of sequences contained within GV1001, were supplied by Dr. Ø. Rekdal, University of Tromsø, Norway. Recombinant hTERT protein (563–735) was synthesised and tested as previously described [9].
T cell cultures and assays
PBMCs were obtained prior to start of vaccination, after a priming period (usually week 6) and before/after booster vaccinations [6, 9, 24]. The PBMCs were isolated and frozen as previously described [39]. Thawed PBMCs were stimulated once in vitro with the vaccine peptide prior to T cell assays, as described earlier [6, 9, 24].
T cell clones were generated from post vaccination PBMCs obtained at the following time points: Patient A 9 years; B week 6; C week 37; D week 36; E week 10; F week 24; G week 9; H week 23; I week 10. The PBMCs were stimulated once in vitro with the vaccine peptide, followed by limiting dilution seeding (0.3/1/3 T cells/well). The seeded T cells were stimulated with irradiated (30 Gy) allogeneic PBMCs (106 c/ml), PHA (1 μg/ml) and IL-2 (10 U/ml). For patients B and I, a protocol for generating cytotoxic T cell clones was applied. Here, CD4+ T cells were depleted with Dynabeads (Dynal, Oslo, Norway) prior to seeding, and IL-2 was used at 100 U/ml.
T cell proliferation assays (3H Thymidine) were performed essentially as previously described [39]. Pre- and post-vaccination samples were analyzed in parallel for response to peptide stimulation. Irradiated autologous PBMCs or EBV-transformed cells were used as APCs. Stimulation with purified protein derivative of tuberculin or Staphylococcal enterotoxin C was used as positive control and as a measure of immunocompetence. T cell cultures were tested in triplicates. SEM was usually below 10%. T cell bulk responses were considered antigen-specific when the stimulatory index (SI; response with antigen divided by response without antigen) was above 2. All 28 T cell clones reported here exhibited SI >5.
Cytotoxicity assays were performed essentially as described [25], using 51Cr-labeled tumor cells, T2 cells (HLA A2+, antigen processing defective) or EBV-transformed cells as targets. HCT116 was obtained from American Type Culture Collection (Rockville, MD). Specific cytotoxicity was calculated according to the formula: (experimental release − spontaneous release)/(maximum release − spontaneous release) × 100.
Bioplex cytokine analyses were performed on supernatants harvested after 48 h, according to the manufacturer’s protocol (Bio-Rad Laboratories, Hercules, CA, USA). Supernatants were analyzed in duplicates, each parallel kept separate through T cell stimulation and Bioplex assays.
The following mAbs were used in HLA-blocking experiments, each at 10 μg/ml: W6/32: anti-HLA class I (American Type Culture Collection, Rockville, MD, USA); anti-HLA-DR (Becton Dickinson); B8/11: anti-HLA-DR (gift from Dr. N. Malissen, Centre d’Immunologie, Marseille, France); SPVL-3: anti-HLA-DQ (gift from Dr. H. Spitz, The Netherlands Cancer Institute, Amsterdam); FN81: anti-HLA-DQ and 22C1: anti-HLA-DP (gifts from Dr. S. Funderud, The Norwegian Radium Hospital).
Flowcytometry
T cells were stained with the following antibodies: anti-CD3 FITC, anti-CD4 FITC, anti-CD4 PE, anti-CD8 PE (Becton Dickinson, San Jose, CA, USA). FITC- and PE-conjugated IgG1 and IgG2a antibodies (Dako Cytomation, Glostrup, Denmark) of irrelevant specificities were included as negative controls. Flowcytometry was performed using a FACSscan (Becton Dickinson).
TCR clonotype mapping
TCR clonotype mapping was performed at two centres using different techniques. Ten T cell clones were examined by TCR clonotype mapping based on denaturing gradient gel electrophoresis (DGGE), as previously described [37, 62]. Briefly, cDNA was amplified using a panel of 24 Vβ region primers. A total of 10 μl of aliquots were electrophoresed in agarose gel, stained with ethidium bromide and visualized in UV light. To separate fragments belonging to the same Vβ region family, amplified cDNA-fragments (10 μl aliquots) were loaded onto a denaturing gradient gel containing 6% polyacrylamide and a gradient of urea and formamide from 20 to 80%. The products were separated by electrophoresis as previously described [37]. Molecules that differ in one or more nucleotide positions unwind at different concentrations in the DGGE [37, 47, 62].
Eighteen T cell clones were examined by amplification of Vγ and Vβ-rearrangements from DNA (not cDNA). DNA was extracted from cell pellets using EZ1 DNA tissue kit and BioRobot EZ1 (Qiagen, Hilden, Germany) after lysation with proteinase K at 56°C. The TCRβ gene analysis was performed according to the BIOMED-2 protocol [64]. The test comprised three multiplex master mixes targeting conserved regions within the variable (V), diversity (D) and joining (J) regions (InVivoScribe Technologies, San Diego, CA, USA). The protocol for TCRγ gene analysis covered all possible gene rearrangements in four multiplex reactions [27]. The multiplex reactions all included three Jγ region consensus primers (Invitrogen, Paisley, UK) plus one out of four Vγ primers (Vγ1–8, Vγ9, Vγ10, Vγ11) labeled with different fluorochromes (Applied Biosystems, Warrington, UK). DNA (25 ng) was used for Vγ1–8 and Vγ9, 50 ng DNA was used for Vγ10 and Vγ11 (final volume 25 μl). PCR mix (final concentrations): 0.1 mM dNTP (25 μM each), 2.0 mM MgCl2, 1× PCR GOLD Buffer, 0.2 μM Jγ-primers, 0.1–0.15 μM Vγ-primers. 0, 63 U Taq polymerase GOLD is added per reaction (Applied Biosystems). The PCR program was as follows: 7 min polymerase preactivation at 94°C, 35 cycles (94°C for 15 s, 65°C for 15 s, 72°C for 30 s) and finalizing at 60°C for 30 min. PCR products (1–2 μl) were diluted in 25 μl HiDi-formamide to prevent dimerization and analyzed by size separation. The products were detected via automated laser scanning (ABI3100 Genetic Analyzer).
Results
Long term T cell responses in patients with unexpected survival
Nine patients enrolled in cancer vaccine trials were selected for further immunological studies, based on the selection criteria listed above (“Materials and methods”). In the original trials (Table 1), the patients received vaccination over a priming period ranging from 4 to 12 weeks. Immune response was monitored by T cell proliferation assays on pre- and post vaccination PBMCs. A pre-vaccine response was observed in 1/9 patients (patient F), suggesting spontaneous priming against naturally presented hTERT antigens. After vaccination, T cell responses against vaccine antigens were demonstrated in all nine patients ([6, 9, 24] and below). Even in the one patient with a pre-vaccine response, vaccination appeared to enhance the response as the stimulatory index increased from 26 to 122.
Here, we investigated the long term development of immune responses and effects of booster vaccination. Long term samples were obtained from six patients with a favourable clinical development, including unexpected survival times. Interestingly, we found that all six patients harbored durable T cell responses against vaccine antigens (Table 1). Figure 1 shows long-term monitoring data for three representative patients (A, C and H). Patient A represents the maximum observation period (Table 1). She was operated January 1997 for pancreatic adenocarcinoma, a condition known to relapse rapidly in most patients [10]. She received four vaccinations with p319 (12Val RAS) shortly after surgery and developed a vaccine specific response (stimulatory index 5.5) [24]. The response diminished, but recovered after a sequence of four booster vaccines in 1998 (Fig. 1a, left chart). Unexpectedly, patient A has since stayed in good general health with no evidence of cancer relapse. We therefore asked her to provide new blood samples, 9 years after start of vaccination and nearly 8 years after the last booster vaccine. The immunoassays demonstrate that she still possesses a memory T cell response specific for the RAS-vaccine peptide (Fig. 1a).
Long-term T cell responses after booster vaccination. PBMCs were collected at consecutive time points, stimulated once in vitro and tested for proliferation against irradiated PBMCs ± peptide. Arrows indicate time of booster vaccines. a Patient A. The patient developed a 12Val RAS-specific response after priming vaccination in 1997 (SI 5.5; data not shown). The response diminished, but recovered after a sequence of four booster vaccines in 1998 (a left chart). An additional round of four boosts was given 3 months later. Bar chart to the right shows proliferation of T cell bulk from 2006, collected 73/4 years after the last booster vaccine. Three 12Val RAS-specific T cell clones generated from the 2006 bulk are included. Columns represent mean CPM of triplicates or hexaplicates. Brackets indicate SEM. b T cell bulk response for patient C. Columns represent mean stimulatory index, i.e. response with antigen (GV1001) divided by response without antigen. c T cell bulk response for patient H. Columns represent mean stimulatory index, i.e. response with antigen (GV1001) divided by response without antigen. Samples at week 23 were obtained after boost vaccination (arrow), all later samples (week 32 onwards) were obtained before boost
Patient C was enrolled in an hTERT vaccine trial (Table 1). He had advanced pulmonary cancer at start of vaccination. The tumor was inoperable and did not respond to chemo- or radiotherapy. Interestingly, there was no immune response in his first post-vaccination tests, but a response against GV1001 (16aa) emerged after booster vaccination (Fig. 1b) [9]. The patient also developed a cytotoxic and proliferative response against a short nested CTL epitope (see below). After continued booster injections at 6-month intervals, he has developed a robust hTERT-specific response that is retained even in pre-boost samples (Fig. 1b). Remarkably, post-vaccination CT-scans have demonstrated complete tumor response. The response includes total regression of a 32 × 32 mm pulmonary tumor involving mediastinal lymph nodes [9]. Continued follow-up including regular CT-scans shows that the patient is still free of tumor, 6 years after start of vaccination.
Patient H started vaccination with GV1001 shortly after surgery for relapse of colon cancer (liver metastases; Duke D). He initially received seven vaccinations within a 5-week priming period and developed a GV1001-specific response at week 6 (Fig. 1c). The T cell response appeared to decrease in vaccine-free periods and was hardly detectable before booster vaccination at week 32 (SI 2.3), but recovered after boosting (Fig. 1c). Over time, continued vaccination has resulted in an endurable response that is retained even in pre-boost samples, i.e. 6–8 months after the previous vaccine. The patient is to date without tumor (45 months follow up). In all, the data from our long-term survivors demonstrate durable T cell responses and indicate a beneficial effect of booster vaccination.
Characterisation of tumor antigen-specific T cell clones
T cell clones recognizing tumor antigens (TA) were generated from all nine patients and characterized as shown in Fig. 2 and online supplemental Fig. 1 (Epub only). The results indicated a considerable diversity in antigen sensitivity and response range, even among clones from a single patient (Fig. 2a). Some clones proliferated vividly to peptide concentrations lower than 1 nM, while others required at least 1,000 times more (data not shown). In a number of clones, we observed bell-shaped response-curves (H #17, Fig. 2a). This finding suggests that higher antigen concentrations may render some clones anergic.
Characterisation of GV1001-specific T cell clones (patient H). T cell clone (T) proliferation after stimulation with irradiated EBV-transformed cells (EB) ± antigen. Columns represent mean CPM of triplicate wells. Brackets indicate SEM. a Antigen sensitivity was determined by titration of GV1001. HLA-restriction was determined by blockage with mAbs against DP, DQ or DP-molecules. b Fine specificity analysis by stimulation with truncated peptides covering the GV1001 sequence (aa sequences given in right text box). The core sequence recognized by each clone is highlighted (red) in text boxes bellow chart. c Recognition of naturally processed antigens. T cell clones were stimulated with EBV-transformed cells incubated with recombinant hTERT protein. The assay shown indicates response to protein in clones # 14, 17, 18 and 20 (not #19)
It is desirable to identify vaccine peptides able to bind different HLA-molecules. These promiscuous peptides may be used in a wider population and without prior HLA-typing. Moreover, a broader spectrum of T cells may be recruited if a larger fraction of the patient’s HLA-repertoire is used, limiting the risk of tumor escape [8]. Here, we determined the HLA-restriction of T cell clones by blockage with mAbs against HLA-DR, HLA-DQ or HLA DP (Fig. 2a, Suppl Fig. 1c) and by stimulation with a panel of EBV-transformed cells with known HLA-phenotypes (not shown). The results demonstrated that peptide GV1001 effectively binds to multiple DP, DQ and DR-molecules (Table 2). Further, we noted that several of the long-term survivors mounted broad responses covering different HLA-restrictions. In experiments with truncated peptides, the core antigen-motives recognized by each T cell clone were determined (Fig. 2b). Again, a considerable diversity within each individual was observed, suggesting that their response may circumvent limitations in peptide processing in tumor tissue. For instance, clones #14, 17, 18 and 19 from patient H exhibited four different recognition patterns (Fig. 2b).
Recruitment of T cells may be in vain if the recognized antigens are not naturally presented. We tested GV1001-specific clones for response to APCs incubated with recombinant hTERT protein. The assays demonstrated hTERT-specific proliferation in 31/34 clones tested (Fig. 2c), including clones from all seven patients vaccinated with GV1001 (patients C, D, E, F, G, H and I). This finding strongly suggests that epitopes associated with GV1001 are naturally processed and presented on a wide spectrum of HLA molecules. Cytotoxicity assays with tumor cell lines indicate that also the hTERT I540 and TGFβRII p573 vaccine peptides are naturally processed. Here, we observed specific killing of tumor cells expressing hTERT or mutated TGFβRII by T cell clones specific for I540 or p573, respectively (Fig. 3a and data not shown). Previous experiments have demonstrated recognition of recombinant mutant p21 RAS and TGFβRII (data not shown).
Characterization of CD4− CD8− and CD4+ CD8+ T cell clones. a T cell clones #26 and #30 from patient B were tested for cytotoxicity against HCT116 and EBV-transformed cells (EB) ± p573. HCT116 is a HLA-A2+ colon cancer cell line that expresses the p573 TGFβRII-mutation. Peptide I540 served as negative control. E/T ratios: EB, 25:1 (#26) and 18:1 (#30). HCT116, 100:1 (#26) and 70:1 (#30). Columns represent mean specific Cr-release of triplicate wells. Brackets indicate SEM. b T cell clones B #26 and B #30 were tested in proliferation assays by stimulation with EBV-transformed cells (EB) ± p573. Columns represent mean CPM of triplicate wells. Brackets indicate SEM. c Flowcytometry phenotype analysis of T cell clones B #26 (CD4−CD8−) and E #31 (CD4+CD8+). The figure shows representative dot plots after staining with antibodies against CD4 and CD8. Percentage of cells in each quartile is given. Both clones stained positive for CD3 (not shown). T cell clones were cultured with irradiated PBMCs + PHA prior to staining. The PBMCs visualize as background dots in all quartiles (B #26), unless the PBMCs are completely outnumbered by T cell clone growth (E #31)
Long peptides with nested CTL-epitopes elicit both T-helper and cytotoxic responses
Most peptide vaccine trials have evaluated short peptides designed for eliciting CTL responses, but an effective response is likely to require CD4+ T cell help [5, 8]. To recruit both CD4+ and CD8+ T cells, we have designed long HLA class II-matched peptides including nested CTL epitopes [21, 23]. Colon cancer patient B received vaccination with p621, a 19aa peptide representing a frameshift mutation in TGFβRII. Interestingly, she developed T cell responses both against p621 and p573, a short nested CTL-epitope (Fig. 3a, b). Similarly, after vaccination with GV1001, patient C developed cytotoxic and helper responses against both the vaccine peptide and a nested CTL-epitope (below and [9]).
Cytotoxic T-cell clones with different CD4/CD8 phenotypes
We identified cytotoxic T cell clones with three different CD4/CD8 phenotypes. Clones #6 and #26 from patient I had a classic CD8+ phenotype and killed A2+ target cells in an I540-specific manner (Suppl Fig. 2a). The CD4+ clone C#76 [9] exhibited HLA-DQB*04-restriction and proliferated against GV1001 (16aa), but also specifically killed APCs pulsed with either the nested CTL-epitope p613 or GV1001 itself (Suppl Fig. 2b). Experiments with truncated peptides demonstrated that the aa-sequence recognised by C#76 was identical to p613, while other GV1001 specific clones recognised different motives (Suppl Fig. 2c).
Cytotoxic T cell clones with a rare CD4−CD8− phenotype (Fig. 3c) were generated from patient B. These clones specifically killed A2+ target cells (T2 cells and autologous EBV-transformed cells) loaded with the mutated TGFβRII-peptide p573, as well as HLA A2+ tumor cells harbouring the TGFβRII-mutation (Fig. 3a, Suppl Fig. 3). The killing was blocked by mAbs against HLA class I (Suppl Fig. 3b). The CD4−CD8− clones also mounted strong, p573-specific proliferation responses (Fig. 3b). These clones represent a highly unconventional T cell fraction, as double negative T cells are generally assumed not to be cytotoxic with the exception of NKT-cells. Contrary to the clones from patient B, NKT cells are not HLA class I-restricted and do not express Vβ3 (Table 2) [22].
T cell bulk responses after cancer vaccination exhibit mixed Th1/Th2 profiles
The Th1/Th2-paradigm represents a key element in current understanding of anti-tumor responses, but the delineation has not been extensively studied in humans after cancer vaccination. To explore the cytokine pattern, we have started measuring a wide range of cytokines in patients from vaccine trials. Figure 4 shows data from patients B, F, G, H and I. Their T cell bulk cultures include substantial levels of key Th2-cytokines IL-5 and IL13, in spite of an otherwise “Th1-like” profile (IL4low, IL-10low, IFNγhigh, TNFαhigh). This unconventional Th1/Th2-pattern is representative for most analyzed patients in our peptide- and DC/RNA vaccine trials [6, 40, 41].
Secretion of Th1/Th2-cytokines in post-vaccination T cell bulk cultures. T cells from post vaccination samples (patient B week 10; F week 36; G week 9; I week 12; H month 37) were stimulated with irradiated PBMCs ± peptides. Supernatants were analyzed by Bioplex cytokine assays. Because the measured concentrations vary between the patients, the data are visualized in two separate bar charts (a, b) with different Y-axis scales. Columns represent mean concentration (pg/ml). Brackets indicate SEM. Peptides: p621 (19aa TGFβRII peptide), p573 (nested 9aa CTL epitope within p621), GV1001 (16aa hTERT peptide), I540 (9aa hTERT peptide). Broad cytokine responses were also observed in T cell bulk cultures from patients C (month 63), D (month 16) and E (week 10) (data not shown). Statistical analysis (Wilcoxon signed ranks test), comparing ± peptide for all cytokines taken together, demonstrated peptide specific responses (P < 0.05) in all bulk cultures tested
In patients B and I, who responded to both HLA-class I restricted and HLA-class II restricted peptides, we found that stimulation with short and long peptides yielded similar cytokine profiles (Fig. 4a, b). The presence of Th2-cytokines did not appear to affect the cytotoxicity, as T cell clones from patients B and I effectively killed target cells (Fig. 3a and Suppl Figs. 2a, 3). In fact, a CD8+ cytotoxic clone (I #26) was the only T cell clone in our study displaying a conventional Th2 profile (Table 3).
Mixed Th1/Th2-profiles and high IFNγ/IL10 ratios among T cell clones
We asked whether the mixed Th1/Th2-profiles in our T cell bulk cultures reflected activation of multiple T cell clones, each displaying conventional Th1- or Th2-profiles. To obtain a general picture, a highly diverse set of 28 clones was analyzed (Table 2). The clones represent seven vaccination protocols, four cancer forms and a wide range of antigen specificities, HLA-restrictions and phenotypes (CD4+ cytotoxic, CD4+ helper, CD8+ cytotoxic, CD4−CD8− cytotoxic, CD4+CD8+ helper). Flowcytometry stainings of CD4−CD8− and CD4+CD8+ T cell clones are shown in Fig. 3c.
The vast majority of T cell clones displayed a broad cytokine profile including both Th1- and Th2 cytokines (Table 3). In particular, IFNγ, TNFα, IL-5 and IL-13 were produced by most clones, while secretion of IL4-, IL9- and IL-10 was more restricted. Low levels of Th2-cytokines may be outweighed by large amounts of Th1-cytokines, and vice versa. We therefore looked for Th1/Th2-deviations by calculating ratios between key cytokines. The biological activity differs among particular cytokines at a given concentration, and it is not possible to tell what ratios are exactly “balanced”. In Table 3, we have made an assumption based on current understanding of biological activity and have highlighted ratios suggesting Th1- or Th2 deviation. As shown, most clones (25/28) did not exhibit a constant Th1- or Th2-deviation for the key ratios. We also calculated cytokine activity by WHO standard units, according to the manufacturer’s calibration data (Biorad technical bulletin 3157). Even based on WHO activity units, the same 25/28 exhibited mixed Th1/Th2 cytokine profiles (not shown). In all, the results strongly suggest that the mixed Th1/Th2-profiles in our bulk cultures was not caused by a mixture of Th1- and Th2 clones, but by clones with a truly broad Th1/Th2 pattern. This finding holds true across the diverse set of clones investigated, regardless of CD4/CD8 phenotype, HLA-restriction, antigen specificity, cancer form and vaccination protocol.
Within the dominating group of “Th1/Th2-clones”, there were considerable differences in secretion of individual cytokines that may be of clinical significance. IFNγ may induce anti-tumor effects, while IL-10 may promote tumor tolerance [36]. In Table 3, the T cell clones are ranked based on IFNγ/IL10-ratio. Eighteen clones had IFNγ/IL10-ratios above 5, while only two clones had ratios below 1/5. In T cell bulk cultures, the IFNγ/IL10 ratios were generally above 10 (Fig. 4 and data not shown). There was also a tendency towards high IFNγ/IL4-ratios, particularly in bulk cultures (Fig. 4; Table 3 and data not shown). We noted that 10/11 clones with high IFNγ/IL4-ratios (>20) had high IFNγ/IL10-ratios (>5). By contrast, there was no detectable association between the IFNγ/IL4 and IFNγ/IL5-ratios (Table 3). Most studies suggesting that a Th1-profile is favourable have included only measurements of IFNγ and IL4/IL10. The data from our long-term survivors support the notion that IFNγhighIL4lowIL10low responses may be beneficial, but reveal that T cell clones with this favorable “Th1”-profile may secrete high levels of IL-5 and IL-13.
Secretion of chemokines and pro-inflammatory cytokines by T cell clones
MIP-1α, MIP-1β and RANTES are considered to be key players in attracting monocytes and lymphocytes to tumor [3, 52]. As shown in Fig. 5, all T cell clones available for analysis secreted these three chemokines, generally at high levels. One T cell clone, G #64, stood out from the others by secreting substantially lower amounts of MIP-1α, MIP-1β and RANTES (Fig. 5). This feature did not reflect a generally attenuated response, as clone G #64 secreted considerable levels of other pro-inflammatory cytokines. Moreover, clone G #64 had retained GV1001-specific proliferation in 3H-thymidine assays performed simultaneously with the Bioplex measurements (Suppl Fig. 1c). Monocyte chemoattractant protein-1 (MCP-1) was secreted by about 50% of the clones, generally at low levels. Clone G #73 represented a notable exception, producing more than five times more MCP-1 and IL-9 than any other clone. We also observed a strong general association between MCP-1 and IL-9, as the 10 top-producing clones of these two cytokines were identical. Eotaxin was secreted by all T cell clones tested, suggesting that basophils and eosinophils may be attracted (Fig. 5).
Cytokine secretion by TA-specific T cell clones. T cell clones were stimulated with irradiated EBV-transformed cells ± peptides. The following peptides were used for clones from the different patients: A p319; B p573; I I540; C,D,E,F,G,H GV1001. Supernatants were analyzed in Bioplex assays. The figure includes all clones analyzed for each cytokine. Mean concentration is displayed (pg/ml), after subtraction of background in controls without peptide. Bar chart at bottom right shows clones ranked according to levels of IL-1β. The other bar charts show clones listed patient by patient
IL-1β represents a powerful driver of inflammation that is blocked by IL-1ra [38]. All 17 clones analyzed for IL-1β/IL-1ra secreted both factors, and the levels tended to correlate (Fig. 5). Regarding other pro-inflammatory cytokines, most clones produced GM-CSF, IL-8 and IL-6. The CD4+CD8+ T cell clone (E #35), which was HLA-class II restricted, differed from the CD4+ CD8− T cell clones by not producing IL-8 and secreting only low levels of GM-CSF.
IL-17 secreting T cell clones produce IL-15, G-CSF and angiogenic factors
T cells producing IL-17 are suggested to represent a distinct subset, termed Th17 [18, 53]. Among our clones, IL17-secretion was closely correlated to secretion of IL-15, G-CSF and PDGF BB (Fig. 6a). Indeed, the four clones secreting the highest levels of IL-17 were the only ones to secrete IL-15 and PDGF. IL17-secreting clones also generally produced high levels of TNFα and IL-1β, both reported to be produced by “Th17-cells”, and of fellow angiogenic factors FGFb and VEGF (Fig. 6b, c). Regarding Th1/Th2-cytokines, the Th17 cells secreted both IFNγ, IL-4, IL-5 and IL-13 (Fig. 6d–e; Table 3).
Cytokine profile of IL17 secreting (Th17) T cell clones. The figure shows clones listed according to IL-17 levels and include all clones analyzed for IL-17. Only cytokines of particular interest for the Th17-subset are displayed. a Cytokines secreted only by IL-17high clones. b, c Cytokines secreted at higher levels by IL-17 secreting clones. d, e Hallmark Th1- and Th2-cytokines (IFNγ and IL-4, respectively), compared to levels of IL-17. T cell clones were stimulated with APCs ± peptides, as outlined in legend to Fig. 5. Supernatants were analyzed in Bioplex assays. Mean concentration is displayed (pg/ml), after subtraction of background in controls without peptide
TCR clonotype mapping
The T cell clones were generated by conventional limiting dilution seeding, but it is well known that such “clones” are not always derived from a single cell. To determine whether the broad cytokine patterns represented truly monoclonal cultures, we performed TCR clonotype mapping. Twenty-five out of the 28 clones were available for mapping. The TCR analysis was performed by two methods. Ten clones were examined by PCR-based amplification of Vβ-fragments from cDNA. The results demonstrated amplification of only a single Vβ region in 7/10 clones (Table 2). The remaining three clones had two Vβ regions. The latter observation indicates biclonal cultures, but do not imply that both clones contribute to the cytokine response. A biclonal culture most likely included only one TA-specific clonal population, as only a minority of seeded T cells were TA-specific. Two or more clones expressing the same Vβ region would not be distinguished by simple agarose electrophoresis. Amplified cDNA products were therefore separated by DGGE [37, 47, 62]. The seven clones in which only a single Vβ region was amplified, were all confirmed to be monoclonal by DGGE (of cDNA samples) or by the DNA-based analysis described below (Table 2).
Eighteen T cell clones were examined by amplification of Vγ and Vβ-fragments from DNA (not cDNA) and subsequent high resolution capillary electrophoresis (Fig. 7). T cells usually rearrange two Vγ-regions at the DNA-level and may also rearrange two complete Vβ-regions, in addition to incomplete Vβ-rearrangements [64]. In 15/18 T cell clones, we identified only one completely rearranged Vβ-region or one Vγ-region and thus demonstrated monoclonality (Table 2). In total, 20/25 clones available for TCR mapping were found to be monoclonal. This finding demonstrates that the observed broad cytokine patterns were not a result of polyclonal T cell cultures.
TCR clonotype mapping. DNA was extracted from T cell clone cultures. Fragments representing rearranged TCR-genes were amplified by PCR and separated by capillary electrophoresis. DNA-fragments visualize as peaks separated according to base pair (bp) length (resolution 1–2 bp). The figure includes all fragments detected for clones # 31, 49 and 51 from patient E. Vγ: Variable γ-region of TCR. Vβcomp: Completely rearranged (V–D–J genes) variable β-region. Vβinc: Incompletely rearranged variable β-region (D–J genes only; non-functional). Clones # 31, 49 and 51 exhibit a single Vβcomp band, indicating monoclonality. Clones #49 and #51 display bands at identical bp lengths, indicating identical TCRs (sister clones). Rfu relative fluorescence unit
TCR mapping was also utilized to determine if T cell clones were different or originated from the same clone in vivo. We identified three pairs of clones with identical TCRs, B #26&30, E #49&51 and H #17&20 (Fig. 7). These findings fitted well with data from functional assays. Clones H #17&20 and E#49&51 displayed identical HLA-restriction and similar cytokine profiles, while B #26&30 shared a rare cytotoxic CD4−CD8− phenotype. The other 19 clones analyzed by TCR mapping were demonstrated not to be sister clones. Regarding the three clones not growing well enough for TCR-mapping, HLA-restriction data suggested that E #48 and H #14 were unique (Table 2). In all, the results indicated that the 28 T cell clones originated from 24 or 25 different clones in vivo.
Discussion
The vaccines given to the present patients include antigens associated with key oncogenic pathways (K-RAS, TGFβRII, hTERT) [35, 43, 50, 68]. By targeting antigens of biological importance, we aim to reduce the risk of tumor escape. In previous phase I/II trials with K-RAS and hTERT vaccines, we have observed increased survival for immunological responders as compared to non-responders [6, 9, 24]. Similar survival observations have also been reported by others after vaccination with hTERT- or RAS-derived peptides [16, 63]. The correlation between immune response and survival is of interest, though the phase I/II study design does not allow for conclusions on clinical benefit. Eight out of the nine patients included in the present study represent long term survivors based on their prognosis at start of vaccination. The study is merely descriptive in terms of clinical observations, but the patients investigated provide a valuable source of insight. They represent human “models” for in vivo processing and presentation of vaccine peptides, recruitment of T cell clones, induction of cytokine profiles, long term development of T cell memory, etc. In particular, the immunological footprint left in patients with a favourable clinical development is of interest.
Here, we report that the long-term survivors harbour TA-specific T cell responses exhibiting several features of possible importance. First, the responses are highly durable. Sustained T cell responses are detected throughout the observation period (maximum 9 years) in all six patients available for continued immunological follow-up. Second, several of the study patients have mounted diverse responses including T cell clones with a wide range of epitope-specificities and HLA-restrictions. This diversity may be important to combat tumor escape. Third, experiments with recombinant protein and tumor cell lines indicate that the T cell clones recognize naturally processed epitopes. The diversity observed in vitro may therefore translate to tumor-tissues. Fourth, the long-term survivors exhibit cytokine profiles that may be beneficial, as discussed below. Fifth, the responses in several patients comprise both cytotoxic and T-helper cells. In one patient, we identify unconventional CD4−CD8− cytotoxic T cell clones. Regarding peptide vaccine design, our results support the strategies of developing HLA-promiscuous peptides and long T-helper peptides with short nested CTL epitopes. Both hTERT GV1001 ([9] and present paper), TGFβRII p621 (present paper) and mutant RAS peptides [23, 25] elicit cytotoxic responses against short nested CTL epitopes, in addition to CD4+ T-helper responses against the full-length peptides. These observations suggest that the peptides are efficiently processed by APCs in vivo. GV1001, p621 and mutated RAS peptides also exhibit highly promiscuous HLA-binding properties, paving the way for studies in large patient populations without HLA typing ([9, 25], present paper and unpublished data). Based on findings in the present study and our previous GV1001 trials [6, 9], two multi-centre phase III trials evaluating GV1001-therapy in pancreatic cancer have started.
There is no agreement as to how long vaccination should continue [32, 51]. Most trials are performed on patients with short life-time expectancy, and there is a lack of long term data. Circulating tumor antigens might be assumed to provide continuous boosts, but these antigens are presented in a non-inflammatory environment favoring tolerance rather than immunity. The results reported here suggest that repeated immunization may be required. The responses observed 1–2 weeks after boost were generally stronger than in pre-boost samples (Fig. 1 and data not shown). Moreover, the responses decreased after priming and became undetectable in 3/6 patients (Fig. 1), while all six patients developed robust TA-specific responses after continued vaccination. Importantly, these “galvanized” responses prevailed through extended vaccination-free periods lasting up to 8 years. Regarding T cell memory, it may also be of importance that the present vaccines include T-helper epitopes. Considerable evidence suggests that CD4+ T cell help is mandatory for establishing CD8+ T cell memory [33, 58].
Further, we investigated whether the Th1/Th2-dichotomy applies to cancer vaccine responses. IFNγ-assays are frequently employed as the only indicator of the cytokine profile in clinical trials [4, 15, 30, 31, 56, 61]. It is important to recognize that a positive IFNγ-assay does not indicate an overall “Th1-pattern”. To determine the Th1/Th2-profile, some research groups include assays for IL-4 and/or IL-10 [49, 57, 59]. Such assays should probably routinely be included, but the interpretation is still delicate. First, some cytokines may be biologically active at low concentrations, and the sensitivity of the assays depends on the detection antibodies. Second, our data suggest that even IFNγ-responses devoid of IL-4/IL10 should not be labelled “Th1”. We find that most IFNγhigh IL-4low IL-10low T cell cultures include substantial levels of the hallmark Th2-cytokines IL-5 and IL-13. These unconventional cytokine profiles do not reflect a mixture of Th1- and Th2 clones in bulk cultures, but apply even to clones confirmed to be monoclonal through TCR clonotype mapping (Tables 2, 3). Further, the patterns do not appear to represent a Th0 phenotype during an early stage of differentiation, but are demonstrated in T cell clones obtained up to 8 years after last vaccination (patient A). Interestingly, the mixed Th1/Th2 profiles are observed throughout a highly diverse set of T cell clones, with different CD4/CD8 phenotypes, antigen specificities, HLA-restrictions and helper/cytotoxic functionalities. Data from in vitro generated clones should always be interpreted with caution. T cell clones surviving in vitro represent a highly selected fraction and their cytokine profile may be influenced by repeated stimulations. However, we also observe mixed Th1/Th2 profiles in bulk cultures tested after only a single in vitro stimulation. This applies not only to the study patients reported here, but even to bulk cultures from virtually all other patients tested in our trials. It may also be recalled, that much data forming the basis of the Th1/Th2-paradigm themselves derive from in vitro generated T cell clones [45]. We have not investigated, whether the broad Th1/Th2-profiles are present at the single cell level. In vivo, the most important issue is the overall cytokine milieu. We have therefore concentrated on the cytokine profiles of bulk cultures and clonal populations. The mixed Th1/Th2 profiles appear to represent a general phenomenon in our trials, as they are observed both after DC/mRNA-vaccination [40, 41] and in seven different peptide vaccine protocols (Table 1). In all, our findings suggest that Th1/Th2-labels should probably be avoided in cancer vaccination studies. The message may be more accurately conveyed by referring to key cytokines, e.g. “IFNγhigh/IL-10low responses”.
We describe multiple T cell clones secreting substantial levels of IL-10, but not fitting into the conventional Tr1-cell category due to high secretion of IFNγ [42]. The implications of this IL10+IFNγ++ cytokine profile are not clear. IL-10 is strongly associated with tumor tolerance, but most data have arisen from studies where IL-10 has not been “balanced” by IFNγ [12, 36, 60, 65]. A recent study on glioblastoma has suggested that a moderate threshold level of IL-10 may be required to uphold an IFNγ-driven response [14].
The major goal of our cytokine studies is to identify patterns of clinical benefit. A high IFNγ/IL10-ratio (>10) was observed in 8/9 patients. Further, the T cell clones from our long term survivors secreted a rich array of chemokines and other pro-inflammatory cytokines, pointing to an intriguing ability to transform the inflammatory tumor milieu. This ability extends well beyond conventional “T-helper” effects and is not limited to the CD4+ T cell subset, but also found in CD8+, CD4−CD8− and CD4+CD8+ T cell clones. A broad cytokine repertoire may be important for clinical efficacy. Studies of immunity against infection have suggested that T cells secreting multiple cytokines, termed multifunctional T cells, are functionally superior [34] and associated with protection against HIV and Leishmania [7, 13, 19]. In upcoming trials, we will characterize the cytokine profile in all immunological responders and contrast the profile in patients with favourable contra poor clinical outcome.
The recently described Th17 cells are potent inducers of granulocytic inflammation and probably key players in autoimmunity [18, 53]. The suggested ability of these cells to shape the inflammatory milieu may also be important in cancer vaccine responses, but their overall cytokine profile has not been clarified. Annunziato and co-workers have suggested a developmental relationship between Th17 and Th1 cells, as opposed to Th2 cells, after observing multiple IL17+ IFNγ+ clones and no IL17+ IL4+ clones [2, 53]. By contrast, all our Th17 clones produced both IL-4 and IFNγ, as well as IL-5 and IL-13. Further, we observed that IL-17 production was associated with secretion of IL-15, G-CSF and several angiogenic cytokines (PDGF BB, FGFb, VEGF, IL-1β, TNFα). This profile suggests that Th17 cells may promote tumor immunity, in particular through IL-15 [67], but also enhance tumor angiogenesis. In all, further studies are needed to determine the cytokine profile and beneficial or contra-productive role of Th17 cells in cancer vaccine responses.
In the present study, we have characterized immune responses in patients with a possible benefit from cancer vaccination, as suggested by extended survival times. We demonstrate that these patients have mounted tumor specific T-cell responses against antigens associated with key mechanisms in oncogenesis, and that the responses exhibit several features of possible clinical advantage. In particular, the responses are durable, diverse and directed against naturally processed antigens. The follow-up data suggest that booster vaccination may be important both to enhance activity and to induce tumor-specific T cell memory. With regard to cytokine profiles, we find that the long-term survivors exhibit high IFNγ/IL10-ratios, favoring immunity over tolerance. Further, their polyfunctional T cells secrete multiple chemokines likely to mobilize the innate and adaptive immune system. The cytokine data do not fit with the Th1/Th2-dichotomy, but point to a continuum of different cytokine profiles. Importantly, the broad Th1/Th2-patterns do not reflect a mixture of Th1- and Th2 clones in bulk cultures, but are observed in T cell clones confirmed to be monoclonal through TCR clonotype mapping. The reported results suggest that cytokine profiling of anti-tumor responses should not rely on the Th1/Th2-paradigm, but adapt a wider focus on the overall inflammatory milieu and assess the balance between individual cytokines of particular importance.
Abbreviations
- TGFβRII:
-
Transforming growth factor β receptor II
- hTERT:
-
Human telomerase reverse transcriptase
- DGGE:
-
Denaturating gradient gel electrophoresis
- IL-1ra:
-
Interleukin 1 receptor antagonist
- PDGF:
-
Platelet derived growth factor
- FGFb:
-
Fibroblast growth factor basic
- VEGF:
-
Vascular endothelial growth factor
- TA:
-
Tumor antigen
- IP-10:
-
Interferon-inducible protein-10
References
Almoguera C, Shibata D, Forrester K, Martin J, Arnheim N, Perucho M (1988) Most human carcinomas of the exocrine pancreas contain mutant c-K-ras genes. Cell 53:549–554
Annunziato F, Cosmi L, Santarlasci V, Maggi L, Liotta F, Mazzinghi B, Parente E, Fili L, Ferri S, Frosali F, Giudici F, Romagnani P, Parronchi P, Tonelli F, Maggi E, Romagnani S (2007) Phenotypic and functional features of human Th17 cells. J Exp Med 204:1849–1861
Balkwill F (2004) Cancer and the chemokine network. Nat Rev Cancer 4:540–550
Banchereau J, Palucka AK, Dhodapkar M, Burkeholder S, Taquet N, Rolland A, Taquet S, Coquery S, Wittkowski KM, Bhardwaj N, Pineiro L, Steinman R, Fay J (2001) Immune and clinical responses in patients with metastatic melanoma to CD34(+) progenitor-derived dendritic cell vaccine. Cancer Res 61:6451–6458
Banchereau J, Palucka AK (2005) Dendritic cells as therapeutic vaccines against cancer. Nat Rev Cancer 5:296–306
Bernhardt SL, Gjertsen MK, Trachsel S, Moller M, Eriksen JA, Meo M, Buanes T, Gaudernack G (2006) Telomerase peptide vaccination of patients with non-resectable pancreatic cancer: a dose escalating phase I/II study. Br J Cancer 95:1474–1482
Betts MR, Nason MC, West SM, De Rosa SC, Migueles SA, Abraham J, Lederman MM, Benito JM, Goepfert PA, Connors M, Roederer M, Koup RA (2006) HIV nonprogressors preferentially maintain highly functional HIV-specific CD8+ T cells. Blood 107:4781–4789
Bijker MS, Melief CJ, Offringa R, van der Burg SH (2007) Design and development of synthetic peptide vaccines: past, present and future. Expert Rev Vaccines 6:591–603
Brunsvig P, Aamdal S, Gjertsen MK, Kvalheim G, Markowski-Grimsrud CJ, Sve I, Dyrhaug M, Trachsel S, Moeller M, Eriksen JA, Gaudernack G (2006) Telomerase peptide vaccination: a phase I/II study in patients with non-small cell lung cancer. Cancer Immunol Immunother 55:1553–1564
Butturini G, Stocken DD, Wente MN, Jeekel H, Klinkenbijl JH, Bakkevold KE, Takada T, Amano H, Dervenis C, Bassi C, Buchler MW, Neoptolemos JP (2008) Influence of resection margins and treatment on survival in patients with pancreatic cancer: meta-analysis of randomized controlled trials. Arch Surg 143:75–83
Chaouat G, Ledée-Bataille N, Dubanchet S, Zourbas S, Sandra O, Martal J (2004) TH1/TH2 paradigm in pregnancy: paradigm lost? Int Arch Allergy Immunol 134:93–119
Chen YX, Man K, Ling GS, Chen Y, Sun BS, Cheng Q, Wong OH, Lo CK, Ng IO, Chan LC, Lau GK, Lin CL, Huang F, Huang FP (2007) A crucial role for dendritic cell (DC) IL-10 in inhibiting successful DC-based immunotherapy: superior antitumor immunity against hepatocellular carcinoma evoked by DC devoid of IL-10. J Immunol 179:6009–6015
Darrah PA, Patel DT, De Luca PM, Lindsay RW, Davey DF, Flynn BJ, Hoff ST, Andersen P, Reed SG, Morris SL, Roederer M, Seder RA (2007) Multifunctional TH1 cells define a correlate of vaccine-mediated protection against Leishmania major. Nat Med 13:843–850
De Vleeschouwer S, Spencer Lopes I, Ceuppens JL, Van Gool SW (2007) Persistent IL-10 production is required for glioma growth suppressive activity by Th1-directed effector cells after stimulation with tumor lysate-loaded dendritic cells. J Neuro-oncol 84:131–140
Di Nicola M, Carlo-Stella C, Mortarini R, Baldassari P, Guidetti A, Gallino GF, Del Vecchio M, Ravagnani F, Magni M, Chaplin P, Cascinelli N, Parmiani G, Gianni AM, Anichini A (2004) Boosting T cell-mediated immunity to tyrosinase by vaccinia virus-transduced, CD34(+)-derived dendritic cell vaccination: a phase I trial in metastatic melanoma. Clin Cancer Res 10:5381–5390
Domchek SM, Recio A, Mick R, Clark CE, Carpenter EL, Fox KR, DeMichele A, Schuchter LM, Leibowitz MS, Wexler MH, Vance BA, Beatty GL, Veloso E, Feldman MD, Vonderheide RH (2007) Telomerase-specific T-cell immunity in breast cancer: effect of vaccination on tumor immunosurveillance. Cancer Res 67:10546–10555
Dong C, Flavell RA (2001) Th1 and Th2 cells. Curr Opin Hematol 8:47–51
Dong C (2006) Diversification of T-helper-cell lineages: finding the family root of IL-17-producing cells. Nat Rev Immunol 6:329–333
Duvall MG, Precopio ML, Ambrozak DA, Jaye A, McMichael AJ, Whittle HC, Roederer M, Rowland-Jones SL, Koup RA (2008) Polyfunctional T cell responses are a hallmark of HIV-2 infection. Eur J Immunol 38:350–363
Fossum B, Gedde-Dahl TIII, Hansen T, Eriksen JA, Thorsby E, Gaudernack G (1993) Overlapping epitopes encompassing a point mutation (12 Gly>Arg) in p21 ras can be recognized by HLA-DR, -DP and -DQ restricted T cells. Eur J Immunol 23:2687–2691
Fossum B, Gedde-Dahl TIII, Breivik J, Eriksen JA, Spurkland A, Thorsby E, Gaudernack G (1994) p21-ras-peptide-specific T-cell responses in a patient with colorectal cancer. CD4+ and CD8+ T cells recognize a peptide corresponding to a common mutation (13Gly>Asp). Int J Cancer 56:40–45
Fujii S, Shimizu K, Hemmi H, Steinman RM (2007) Innate Valpha14(+) natural killer T cells mature dendritic cells, leading to strong adaptive immunity. Immunol Rev 220:183–198
Gjertsen MK, Bjorheim J, Saeterdal I, Myklebust J, Gaudernack G (1997) Cytotoxic CD4+ and CD8+ T lymphocytes, generated by mutant p21-ras (12Val) peptide vaccination of a patient, recognize 12Val-dependent nested epitopes present within the vaccine peptide and kill autologous tumour cells carrying this mutation. Int J Cancer 72:784–790
Gjertsen MK, Buanes T, Rosseland AR, Bakka A, Gladhaug I, Soreide O, Eriksen JA, Moller M, Baksaas I, Lothe RA, Saeterdal I, Gaudernack G (2001) Intradermal ras peptide vaccination with granulocyte–macrophage colony-stimulating factor as adjuvant: clinical and immunological responses in patients with pancreatic adenocarcinoma. Int J Cancer 92:441–450
Gjertsen MK, Saeterdal I, Saeboe-Larssen S, Gaudernack G (2003) HLA-A3 restricted mutant ras specific cytotoxic T-lymphocytes induced by vaccination with T-helper epitopes. J Mol Med 81:43–50
Gor DO, Rose NR, Greenspan NS (2003) TH1-TH2: a procrustean paradigm. Nat Immunol 4:503–505
Greiner TC, Raffeld M, Lutz C, Dick F, Jaffe ES (1995) Analysis of T cell receptor-gamma gene rearrangements by denaturing gradient gel electrophoresis of GC-clamped polymerase chain reaction products. Correlation with tumor-specific sequences. Am J Pathol 146:46–55
Groux H (2003) Type 1 T-regulatory cells: their role in the control of immune responses. Transplantation 75:8S–12S
Harley CB (2008) Telomerase and cancer therapeutics. Nat Rev Cancer 8(3):167–179
Heiser A, Coleman D, Dannull J, Yancey D, Maurice MA, Lallas CD, Dahm P, Niedzwiecki D, Gilboa E, Vieweg J (2002) Autologous dendritic cells transfected with prostate-specific antigen RNA stimulate CTL responses against metastatic prostate tumors. J Clin Invest 109:409–417
Hirschowitz EA, Foody T, Kryscio R, Dickson L, Sturgill J, Yannelli J (2004) Autologous dendritic cell vaccines for non-small-cell lung cancer. J Clin Oncol 22:2808–2815
Hoos A, Parmiani G, Hege K, Sznol M, Loibner H, Eggermont A, Urba W, Blumenstein B, Sacks N, Keilholz U, Nichol G (2007) A clinical development paradigm for cancer vaccines and related biologics. J Immunother 30:1–15
Janssen EM, Lemmens EE, Wolfe T, Christen U, von Herrath MG, Schoenberger SP (2003) CD4+ T cells are required for secondary expansion and memory in CD8+ T lymphocytes. Nature 421:852–856
Kannanganat S, Ibegbu C, Chennareddi L, Robinson HL, Amara RR (2007) Multiple-cytokine-producing antiviral CD4 T cells are functionally superior to single-cytokine-producing cells. J Virol 81:8468–8476
Kim NW, Piatyszek MA, Prowse KR, Harley CB, West MD, Ho PL, Coviello GM, Wright WE, Weinrich SL, Shay JW (1994) Specific association of human telomerase activity with immortal cells and cancer. Science 266:2011–2015
Knutson KL, Disis ML (2005) Tumor antigen-specific T helper cells in cancer immunity and immunotherapy. Cancer Immunol Immunother 54:721–728
Kollgaard T, Petersen SL, Hadrup SR, Masmas TN, Seremet T, Andersen MH, Madsen HO, Vindelov L, thor Straten P (2005) Evidence for involvement of clonally expanded CD8+ T cells in anticancer immune responses in CLL patients following nonmyeloablative conditioning and hematopoietic cell transplantation. Leukemia 19:2273–2280
Kotter I, Wacker A, Koch S, Henes J, Richter C, Engel A, Gunaydin I, Kanz L (2007) Anakinra in patients with treatment-resistant adult-onset Still’s disease: four case reports with serial cytokine measurements and a review of the literature. Semin Arthr Rheumat 37:189–197
Kyte JA, Kvalheim G, Aamdal S, Saebøe-Larssen S, Gaudernack G (2005) Preclinical full-scale evaluation of dendritic cells transfected with autologous tumor-mRNA for melanoma vaccination. Cancer Gene Ther 12:579–591
Kyte JA, Mu LJ, Aamdal S, Kvalheim G, Dueland S, Hauser M, Gullestad HP, Ryder T, Lislerud K, Hammerstad H, Gaudernack G (2006) Phase I/II trial of melanoma therapy with dendritic cells transfected with autologous tumor-mRNA. Cancer Gene Ther 13:905–918
Kyte JA, Kvalheim G, Lislerud K, Thor Straten P, Dueland S, Aamdal S, Gaudernack G (2007) T cell responses in melanoma patients after vaccination with tumor-mRNA transfected dendritic cells. Cancer Immunol Immunother 56:659–675
Levings MK, Roncarolo MG (2005) Phenotypic and functional differences between human CD4+ CD25+ and type 1 regulatory T cells. Curr Top Microbiol Immunol 293:303–326
Markowitz S, Wang J, Myeroff L, Parsons R, Sun L, Lutterbaugh J, Fan RS, Zborowska E, Kinzler KW, Vogelstein B et al (1995) Inactivation of the type II TGF-beta receptor in colon cancer cells with microsatellite instability. Science 268:1336–1338
Morse MA, Chui S, Hobeika A, Lyerly HK, Clay T (2005) Recent developments in therapeutic cancer vaccines. Nat Clin Prac 2:108–113
Mosmann TR, Cherwinski H, Bond MW, Giedlin MA, Coffman RL (1986) Two types of murine helper T cell clone. I. Definition according to profiles of lymphokine activities and secreted proteins. J Immunol 136:2348–2357
Mosmann TR, Sad S (1996) The expanding universe of T-cell subsets: Th1, Th2 and more. Immunol Today 17:138–146
Myers RM, Maniatis T, Lerman LS (1987) Detection and localization of single base changes by denaturing gradient gel electrophoresis. Methods Enzymol 155:501–527
Nagorsen D, Thiel E (2006) Clinical and immunologic responses to active specific cancer vaccines in human colorectal cancer. Clin Cancer Res 12:3064–3069
Perambakam S, Hallmeyer S, Reddy S, Mahmud N, Bressler L, DeChristopher P, Mahmud D, Nunez R, Sosman JA, Peace DJ (2006) Induction of specific T cell immunity in patients with prostate cancer by vaccination with PSA146–154 peptide. Cancer Immunol Immunother 55:1033–1042
Ponti D, Costa A, Zaffaroni N, Pratesi G, Petrangolini G, Coradini D, Pilotti S, Pierotti MA, Daidone MG (2005) Isolation and in vitro propagation of tumorigenic breast cancer cells with stem/progenitor cell properties. Cancer Res 65:5506–5511
Ridgway D (2003) The first 1000 dendritic cell vaccinees. Cancer Invest 21:873–886
Rollins BJ (1997) Chemokines. Blood 90:909–928
Romagnani S (2008) Human Th17 cells. Arthr Res Ther 10:206–213
Rosenberg SA, Yang JC, Restifo NP (2004) Cancer immunotherapy: moving beyond current vaccines. Nat Med 10:909–915
Saeterdal I, Gjertsen MK, Straten P, Eriksen JA, Gaudernack G (2001) A TGF betaRII frameshift-mutation-derived CTL epitope recognised by HLA-A2-restricted CD8+ T cells. Cancer Immunol Immunother 50:469–476
Salcedo M, Bercovici N, Taylor R, Vereecken P, Massicard S, Duriau D, Vernel-Pauillac F, Boyer A, Baron-Bodo V, Mallard E, Bartholeyns J, Goxe B, Latour N, Leroy S, Prigent D, Martiat P, Sales F, Laporte M, Bruyns C, Romet-Lemonne JL, Abastado JP, Lehmann F, Velu T (2006) Vaccination of melanoma patients using dendritic cells loaded with an allogeneic tumor cell lysate. Cancer Immunol Immunother 55:819–829
Schuler-Thurner B, Schultz ES, Berger TG, Weinlich G, Ebner S, Woerl P, Bender A, Feuerstein B, Fritsch PO, Romani N, Schuler G (2002) Rapid induction of tumor-specific type 1 T helper cells in metastatic melanoma patients by vaccination with mature, cryopreserved, peptide-loaded monocyte-derived dendritic cells. J Exp Med 195:1279–1288
Shedlock DJ, Shen H (2003) Requirement for CD4 T cell help in generating functional CD8 T cell memory. Science 300:337–339
Slingluff CL Jr, Yamshchikov G, Neese P, Galavotti H, Eastham S, Engelhard VH, Kittlesen D, Deacon D, Hibbitts S, Grosh WW, Petroni G, Cohen R, Wiernasz C, Patterson JW, Conway BP, Ross WG (2001) Phase I trial of a melanoma vaccine with gp100(280–288) peptide and tetanus helper peptide in adjuvant: immunologic and clinical outcomes. Clin Cancer Res 7:3012–3024
Strauss L, Bergmann C, Szczepanski M, Gooding W, Johnson JT, Whiteside TL (2007) A unique subset of CD4+ CD25highFoxp3+ T cells secreting interleukin-10 and transforming growth factor-beta1 mediates suppression in the tumor microenvironment. Clin Cancer Res 13:4345–4354
Su Z, Dannull J, Heiser A, Yancey D, Pruitt S, Madden J, Coleman D, Niedzwiecki D, Gilboa E, Vieweg J (2003) Immunological and clinical responses in metastatic renal cancer patients vaccinated with tumor RNA-transfected dendritic cells. Cancer Res 63:2127–2133
thor Straten P, Barfoed A, Seremet T, Saeterdal I, Zeuthen J, Guldberg P (1998) Detection and characterization of alpha-beta-T-cell clonality by denaturing gradient gel electrophoresis (DGGE). Biotechniques 25:244–250
Toubaji A, Achtar M, Provenzano M, Herrin VE, Behrens R, Hamilton M, Bernstein S, Venzon D, Gause B, Marincola F, Khleif SN (2008) Pilot study of mutant ras peptide-based vaccine as an adjuvant treatment in pancreatic and colorectal cancers. Cancer Immunol Immunother 57:1413–1420
van Dongen JJ, Langerak AW, Bruggemann M, Evans PA, Hummel M, Lavender FL, Delabesse E, Davi F, Schuuring E, Garcia-Sanz R, van Krieken JH, Droese J, Gonzalez D, Bastard C, White HE, Spaargaren M, Gonzalez M, Parreira A, Smith JL, Morgan GJ, Kneba M, Macintyre EA (2003) Design and standardization of PCR primers and protocols for detection of clonal immunoglobulin and T-cell receptor gene recombinations in suspect lymphoproliferations: report of the BIOMED-2 Concerted Action BMH4-CT98-3936. Leukemia 17:2257–2317
Vence L, Palucka AK, Fay JW, Ito T, Liu YJ, Banchereau J, Ueno H (2007) Circulating tumor antigen-specific regulatory T cells in patients with metastatic melanoma. Proc Natl Acad Sci USA 104:20884–20889
Vonderheide RH (2002) Telomerase as a universal tumor-associated antigen for cancer immunotherapy. Oncogene 21:674–679
Waldmann TA (2006) The biology of interleukin-2 and interleukin-15: implications for cancer therapy and vaccine design. Nat Rev Immunol 6:595–601
Welsch T, Kleeff J, Friess H (2007) Molecular pathogenesis of pancreatic cancer: advances and challenges. Curr Mol Med 7:504–521
Acknowledgments
This work was supported by the Norwegian Cancer Society and ENACT. The authors thank doctors and nurses at the study hospitals for excellent clinical follow-up and patient care. Special thanks to S. Aamdal, P. Brunsvig, T. Buanes, B. Solheim, I.K. Bukholm, L.R. Braathen, M. Gjertsen and A. Bakka. We also thank H.G. Russnes, H. Vaalerhaugen and T. Seremet for valuable help on TCR clonotype mapping.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kyte, J.A., Trachsel, S., Risberg, B. et al. Unconventional cytokine profiles and development of T cell memory in long-term survivors after cancer vaccination. Cancer Immunol Immunother 58, 1609–1626 (2009). https://doi.org/10.1007/s00262-009-0670-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-009-0670-2