Abstract
Injection of dendritic cells (DC) pulsed with tumor antigens is a novel treatment strategy against malignancies, and aims to elicit anti-tumoral cell-mediated immune responses. We studied the in vitro proliferative responses and cytokine production in T cell cultures after 2 stimulations with autologous DC loaded with tumor lysates derived from glioblastoma multiforme (GBM) cells in the presence of recombinant interleukin (rIL)−6/rIL-12 in the first, and rIL-2/rIL-7 in the second stimulation. After the second stimulation, T cells were co-cultured with glioblastoma (GBM) cells and tumor growth suppression by T cells was assessed using a MTT assay. Although loaded DC induced a significant shift towards T helper cell type 1 (Th1) cytokine production as compared to unloaded DC, persistent interleukin (IL)-10 production by T cells both at the end of 2 stimulations with loaded DC and during the effector phase was also required for their tumor suppressive activity. A stronger glioma growth suppressive activity by T cells stimulated with tumor lysate-loaded DC than by control T cells, cultured with unloaded DC, was seen only if the relative IL-10 production after two stimulations with loaded DC was at least 40% of the IL-10 production after two stimulations with unloaded DC. If less than 40% IL-10 was produced in the experimental condition compared to the control condition, T cells also lost their tumor growth suppressive activity. Addition of rIL-10 during stimulation increased the suppressive activity on tumor cell viability and interferon (IFN)-γ production by T cells that showed Th1 response upon stimulation with loaded DC. The data point towards the production of both IFN-γ and IL-10 by responding effector T cells, and towards an immune modulatory rather than immune suppressive role of IL-10 to generate anti-tumoral effector T cells against GBM.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Anaplastic astrocytoma and glioblastoma multiforme (GBM) are the malignant end of a spectrum of glial tumors according to malignancy. The yearly incidence of high-grade glioma’s is about 2.4 per 100,000 adults [1] and 2 per million children [2]. Although treatment with surgery, conventional external beam radiotherapy, and chemotherapy [3] can lead to a significant period of tumor control, overall prognosis is still poor. Also in the pediatric group of patients, the prognosis is poor [2]. Even after maximal treatment with surgery, radiotherapy and chemotherapy, relapse is universal and is believed to be due to the extensive spread of tumor cells into surrounding regions of the brain [4]. There is a clear need for well-tolerated long-term treatments that are tumor-specific and able to kill all (residual) tumor cells that infiltrate in the adjacent areas of the brain. The immune system provides us with some promising tools in that regard. Several preclinical investigations for the development of therapeutic vaccines against malignant gliomas were based on the use of dendritic cells (DC) loaded with a mixture of glioma-derived tumor antigens. The concept has been worked-out, in rat [5, 6] as well as mouse [7, 8] models. Several research groups have provided data on safety and efficacy in clinical trials using autologous DC loaded with tumor lysates [9–12].
Although promising experiences with DC vaccination for patients with high grade glioma have been observed, the detailed immunological mechanisms after DC vaccination are not completely understood. We demonstrated earlier that human DC could efficiently take up tumor protein fragments derived from GBM tumor cell lysates [13]. Mature DC presented tumor antigens in the context of both major histocompatibility complex (MHC) class I and MHC class II molecules, and were able to stimulate T cells to generate effective tumor-specific MHC class I-dependent cytotoxic activity. In these experiments, the cytotoxic activity was measured in a 4-h cytotoxicity assay. This assay, however, does not allow to study the overall interaction between stimulated effector T cells and expanding tumor cells. We hypothesised that not only the cytotoxic activity but also the cytokine microenvironment might ultimately determine the final outcome of tumor cell viability. We therefore studied now the proliferative response and cytokine production of human T cells stimulated with loaded DC, and the GBM tumor cell viability and expansion after a prolonged co-culture with stimulated effector T cells.
Material and methods
GBM tumor cell cultures
Early passage cultures from patients with malignant glioma and GBM tumor cell lines (A172, U251, T98G, all kindly provided by JEA Wolff, Regensburg, Germany) were cultured in RPMI1640 (BioWhittaker, Verviers, Belgium) supplemented with 10% fetal calf serum (FCS, Hyclone, Logan, Utah), non essential amino-acids (diluted 1:100), glutamine (2 mM), pyruvate (1 mM/ml), penicilline (200 U/ml) and streptomycine (200 μg/ml) (all four from Cambrex, East Rutherford, New Jersey), ß-mercapto-ethanol (7 × 10−4%) and amphotericine B (1.25 μg/ml) (both from Sigma–Aldrich, St. Louis Missouri, USA) in 160 ml culture flasks (NUNC brand products, Roskilde, Denmark). Early passage cultures were characterised by Glial Fibrillary Acid Protein and vimentine monolayer staining.
Generation of monocyte-derived dendritic cells
Informed consent was obtained from the donors before participating in the study. Peripheral blood mononuclear cells (PBMC) were isolated from blood using LymphoprepTM (Nycomed Pharma, Oslo, Norway). Subsequently, the monocyte fraction was enriched using plastic adherence as described [14]. The monocytes were cultured in 6-well plates (Greiner Bio-One, Sarah SE, Longwood, USA) at a concentration of 107 cells per ml in short-term culture medium (RPMI 1640, supplemented with glutamine, penicilline, streptomycine, and 1% autologous plasma), and differentiated into immature DC in the presence of human rIL-4 (20 ng/ml, PeproTech, Rocky Hill, New York) and rGM-CSF (1,000 U/ml, Novartis Pharma, Brussels, Belgium) for 7 days. Half of the culture medium was refreshed at day 3.
After 7 days, the immature DC were collected. Maturation was induced with a cytokine mixture consisting of recombinant Tumor Necrosis Factor (rTNF)-α (120 ng/ml, Strathmann Biotec, Hamburg, Germany), rIL-1β (120 ng/ml, Strathmann Biotec) and Prostaglandin (PG) E2 (20 μg/ml, Pharmacia, Puurs, Belgium) [15].
The phenotypes of immature and mature loaded and unloaded DC were controlled by Fluorescence Activated Cell Sorter (FACS) (FACSort and Cellquest software, BD, Mountain View, CA) using Fluorescein Isothiocyanate (FITC)- (CD1a, CD86) or Phycoerythrin (PE)- (CD80, CD83, HLA-DR) labelled monoclonal antibodies (mAb) (BD Biosciences Pharmingen, San Jose, USA).
DC loading with tumor cell lysate
Tumor cells were harvested and 6 snap freeze-thaw cycles and filtration through the 70 μm Cell-Strainer were performed. Tumor cell death was verified by Trypan-Blue Exclusion. Part of the immature DC were loaded overnight with lysates from GBM tumor cells (about 100 μg tumor proteins per 106 DC). DC maturation was induced by addition of the maturation cytokine mixture at the moment of loading.
In vitro priming of autologous T cells
Highly purified T cells were isolated as described [16]. Briefly, peripheral blood mononuclear cells were isolated by centrifugation of blood on LymphoprepTM, and resuspended in short-term culture medium and inactivated autologous plasma at 10%. T cells were further purified using a complement-mediated depletion of all non-T cells with lympho-KWIK-T (One Lambda Inc, Los Angeles, CA). The percentage of contaminating NK cells at baseline and after two stimulations was less than 3%. T cells were stimulated with autologous mature loaded DC at a ratio of 10:1. As control conditions, T cells were co-cultured with autologous unloaded DC in the presence of cytokines, or were cultured in the presence of cytokines without addition of DC. In some experiments lysate only was added to T cells as control. During the first stimulation of 7 days, rIL-6 (10 ng/ml, Peprotech INC, Rocky Hill, NJ) and rIL-12 (10 ng/ml, Genetics Institute, INC, Cambridge, Massachusetts) were added as described [17–19]. Cells were harvested and cultured again for 7 days with newly differentiated and loaded DC in the presence of rIL-2 (10 U/ml, Roche Diagnostics Gmbh, Mannheim, Germany) and rIL-7 (5 ng/ml, Peprotech INC). In some experiments (Fig. 3), rIL-10 (PeproTech EC Ltd, London, England) was added at a concentration of 5 ng/ml during both stimulations. At the end of the second stimulation, T cells were harvested and their effector functions analysed. Similar to our previous report [13], donor T cells were matched with the GBM tumor cells for at least one Human Leukocyte Antigen (HLA)-A allele (n = 12) or complete autologous paired T cell-tumor cultures were used (n = 11). No difference was observed between these two settings.
Cytokine measurement
IL-4, IL-5, IL-10, IL-13, IFN-γ and TNF-α were measured in the supernatant by sandwich-ELISA using 96-well plates (Nunc-Immuno™, Roskilde, Denmark). Respective antibodies to coat the plates and biotinylated antibodies for detection were all purchased from BD Biosciences Pharmingen. Streptavidine (Jackson ImmunoResearch, West Grove, PA) was used as enzyme and TMB (3,3′,5,5′-Tetramethylbenzidine dihydrochloride hydrate, Acros Organics, New Jersy USA) as substrate. Absorbance at 450 nm was read using an ELISA reader (Labsystems Multiskan Plus, Helsinki, Finland).
Proliferation of T cells
Before the first stimulation and at the end of the second stimulation, T cells primed in the different conditions were tested for proliferation capacity. Briefly, 5 × 104 T cells per well (96-well plate, Sarstedt, Nümbrecht, Germany) were incubated overnight with 0.2 μCi [3H]-TdR/ml (ICN, Costa Mesa, CA) in triplicate for each condition. Afterwards, cells were harvested (MicroCell Harvester, Skatron Instruments, Norway) and [3H]-TdR uptake was measured with a β-counter (Packard Instruments, Meriden, CT).
GBM tumor cell viability assay
GBM tumor cells were harvested, washed, counted and replated in 96-well plates (Nunc-Immuno™) in the appropriate fresh medium at a density of 8,000 cells per well. They were further cultured overnight to become adherent to the plate. Afterwards, 8 × 104 effector T cells were added. After 48, 144 and 216 h of co-culture, proliferation of tumor cells was measured with the MTT assay [20]. For this, the non-adherent effector T cells were gently washed away with DPBS (BioWhittaker, Verviers, Belgium) and 100 μl of MTT solution (0.5 mg/ml medium, Sigma–Aldrich Gmbh, Steinheim, Germany) was added to residual adherent target cells, which were further cultured for 2 h. Afterwards, the MTT solution was taken off and 100 μl DMSO (B/Braun, Boulogne, France) per well was added to resolve the formazan produced in viable cells. After stirring the plate for 30 min, the amount of viable cells was assessed with a spectrophotometer measuring the absorbance at 570 and 620 nm (as reference). Four wells with only medium served as blanco wells. A culture of tumor cells without T cells served as the baseline tumor cell viability. Each experimental condition at each time point was measured in quadruplicate. The mean optical densities (OD) of the different conditions at the different time points were plotted in a graph displaying the proliferation kinetics of the tumor cells in the absence or presence of primed T cells. The resulting area under the curve (AUC), for each condition relative to the AUC of the baseline condition with tumor cells alone, represents the residual tumor load in each condition [21].
Statistical analysis
All statistics, including calculation of the AUC, were performed using Prism software (Prism3, GraphPad Software, Inc., San Diego, CA). Nonparametric statistics were used. To overcome interexperimental variability, we performed paired analyses of matched observations within each experiment. An index of a variable was calculated as the ratio between the variable derived after stimulation with loaded DC (exp) divided by the variable derived after stimulation with unloaded mature DC (co): index = [variable]exp / [variable]co.
Results
T cell response after stimulation with DC loaded with tumor lysate
A series of 23 similar independent experiments was performed to study T cell activation by autologous DC that were loaded with tumor lysate from GBM tumor cells. T cells were stimulated first in the presence of rIL-6 and rIL-12, and thereafter in the presence of rIL-2 and rIL-7 [17–19]. At the end of the secondary stimulation, T cell proliferation and cytokine production was measured (Table 1). For the latter, we focused on the production of IFN-γ as a Th1 cytokine, IL-5 as a T helper cell type 2 (Th2) cytokine and IL-10 as a T helper cell type 0 (Th0) cytokine. In this experimental set-up, there was a high background response in the control conditions, likely due to a phenomenon called auto-MLR (Mixed Lymphocyte Reaction) [22] and to the presence of the stimulating cytokines used. However, we found that the IL-10 production in the stimulation culture with autologous loaded DC and cytokines was significantly lower than in the culture with unloaded DC and cytokines, or in the culture in the presence of cytokines alone (paired non-parametric test: P = 0.0013). Remarkably, the amount of IL-10 produced was significantly correlated with T cell proliferation (Spearman R = 0.7011, 0.8852 and 0.8354 respectively, P = 0.0052, < 0.0001, 0.0002 respectively) for the experimental and both control conditions. There was no correlation between the IFN-γ production on the one hand and proliferation or IL-10 production on the other hand.
The activity of stimulated T cells during co-culture with tumor cells
In a previous study, T cells stimulated with autologous, tumor cell lysate-loaded DC in the presence of the cytokine cocktails have clearly been shown to generate effective tumor-specific MHC class I-dependent and MHC class I-restricted cytotoxic T cell activity against tumor cells in a 4-h assay [13]. We here studied the activity of stimulated T cells during co-culture with tumor cells as a model for in vivo anti-tumoral activity. First, the production of cytokines after 144 h of co-culture during the effector phase was measured. The IFN-γ production was highest in the co-cultures of tumor cells and T cells that were stimulated with loaded DC, pointing towards a Th1 type response (Table 2, paired non-parametric test: P = 0.0075). We did not find any IL-5 production.
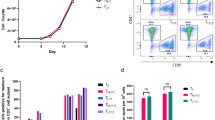
We next studied whether these stimulated T cells exerted tumor growth suppressive effects on a monolayer of proliferating tumor cells during a prolonged co-culture period. In all these experiments, patient-derived tumor cells were autologous to patient-derived T cells, or cell lines were matched with donor-derived T cells for at least one HLA-A allele. At 3 different time points effector T cells were washed away, and the viability of residual tumor cells was assessed with MTT. The area under the curve, calculated using dedicated Prism Software, for the experimental condition was compared to the area under the curve of proliferating tumor cells without addition of effector cells, and the percentage residual viability of tumor cells was calculated, refering to the tumor suppressive activity of the effector T cells. The activity by T cells cultured with unloaded DC for 2 stimulation periods was assessed as control. As shown in Fig. 1, T cells that were stimulated with loaded DC had more suppressive activity on the tumor growth than T cells that were cultured twice with unloaded DC. In all of the 16 experiments, a reduction of tumor cell viability could be demonstrated by T cells stimulated with loaded DC. However, due to high background response, a tumor suppressive activity of T cells co-cultured in the presence of unloaded DC and cytokines was also present in 10 experiments.
T cells stimulated with tumor cell lysate-loaded mature DC (DC-loaded) have suppressive capacity on autologous tumor cell viability, more than T cells stimulated with unloaded DC (DC). T cells were primed with loaded DC or cultured with unloaded DC as described, and effector T cells were co-cultured with GBM tumor cells. After 48, 144 and 216 h during the effector phase, viability of cultured tumor cells was measured with the MTT assay. Culture of tumor cells alone was performed, and the area under this curve was calculated and referred to as 100% tumor cell viability
The specificity of the suppressive activity on tumor cell viability using this experimental approach was evaluated in 2 experiments with patient-derived T cells, DC, tumor cells and fibroblasts. T cells stimulated with autologous DC that were loaded with autologous tumor lysates were able to reduce viability of autologous tumor cell to 8%, respectively 58%, whereas the viability of autologous fibroblasts remained 81 and 91% respectively. T cells cultured twice unloaded DC had no differential effect on the growth of tumor cells versus fibroblasts. These data are consistent with our published data on tumor-specificity of the in vitro generated cytotoxic T cells [13].
IL-10 production modulates the generation of suppressive activity on tumor cell viability
In order to focus solely on the stimulatory effect of loaded DC versus unloaded DC, and to overcome aspecific auto-MLR effects [22], we calculated for each experiment the index between the functional read-out data (cytokine production, T cell proliferation, tumor viability) obtained after stimulation with loaded DC versus data obtained after culture with unloaded DC. The index of the IL-10 production ranged from 0.02 to 1.81. In 13/16 experiments, T cells cultured with loaded DC (partially) lost their capacity to produce IL-10 as compared to the T cell co-culture with unloaded DC, which is compatible with the results depicted in Table 1. The index of IL-10 produced at the end of the secondary stimulation, however, was significantly correlated with the proliferation index of the T cells (Spearman R = 0.9121, P < 0.0001). Moreover, as shown in Fig. 2a, the IL-10 index calculated at the end of the second stimulation was strikingly correlated with the tumor viability index during the effector phase (Spearman R = –0.7054, P = 0.0023). Also the proliferation index at the end of the stimulations was significantly correlated with the tumor viability index (Spearman R = –0.6565, P = 0.0438) (Fig. 2b). The correlation of the IL-10 index and proliferation index at the end of the stimulation with the tumor viability index during the effector phase for 16 respectively 10 independent experiments are shown in Fig. 2a and b. A tumor viability index < 1 indicates that effector T cells primed by tumor lysate-loaded DC had a better glioma suppressive activity than control T cells that were primed by unloaded DC.
IL-10 production and proliferation of T cells at the end of 2 stimulations (stimulation phase) with loaded DC, as compared to culture with unloaded DC, correlates with suppressive activity on GBM tumor cell viability. T cells were stimulated as described. IL-10 concentration and T cell proliferation were measured at the end of the second stimulation. For both read-out functions in each experiment, an index of the variable measured after 2 stimulations with loaded DC relative to the same variable measured at the end of 2 cultures with unloaded DC was calculated: e.g. IL-10 index = [IL-10exp] / [IL-10co], with exp = the experimental condition in which T cells were stimulated with GBM tumor lysate-loaded DC and co = the control condition in which T cells were cultured with unloaded DC. After 2 stimulations effector cells or control T cells were co-cultured with GBM tumor cells during the effector phase, and residual viability of tumor cells was measured as described. An index of tumor viability was calculated as described
In 5 out of 16 experiments, T cells cultured twice with loaded DC lost their capacity to produce IL-10 to an extent of less than 40% (IL-10 index < 0.4) of the IL-10 produced in the cultures of these T cells with unloaded DC. Those values showed a remarkable correlation with a much lower proliferation capacity of the T cells at the end of the second stimulation and with a worse tumor growth suppressive activity than T cells co-cultured with the unloaded DC (tumor viability index > 1). The IFN-γ index obtained at the end of the secondary stimulation was not correlated with the T cell proliferation index, nor with the viability index during the subsequent effector phase.
Similar indices were calculated during the effector phase, and, again, a significant correlation of the tumor viability index with the IL-10 index (Spearman R = –0.6565, P = 0.0438) was found, but not with the IFN-γ index. As expected, the IL-10 index calculated at the end of the second stimulation was significantly correlated with the IL-10 index calculated during the effector phase (Spearman R = 0.7903, P = 0.0065).
Thus, after correction for auto-MLR effects giving background response, the suppressive activity on tumor cell viability was clearly correlated with T cell activation as measured by T cell proliferation and persistent IL-10 production at the end of the second stimulation, and persistent IL-10 production during the effector phase. In summary, we observed a stronger glioma growth suppressive activity (tumor viability index < 1) by T cells stimulated with tumor lysate loaded DC than by control T cells cultured with unloaded DC, in general only if the IL-10 index at the end of the second stimulation still was more than 0.4.
We therefore investigated further the role of IL-10 for the in vitro generation of tumor-suppressive T cell activity and finally questioned whether addition of exogeneous IL-10 during stimulation would influence the T cell suppressive activity on tumor cell viability during the effector phase. We performed 4 similar stimulation experiments with unloaded and loaded DC, in which we added rIL-10 to the primary and secondary stimulation. The index of IFN-γ and IL-10 production was calculated at the end of both the primary and secondary stimulation, and at 3 different time points during the effector phase. The experiments are summarised in Fig. 3. In all four experiments, the IL-10 index at the end of the secondary stimulation remained higher than 0.4, which is compatible with the extrapolated critical value to achieve a viability index of < 1 (see Fig. 2a). As a consequence, in all 4 experiments tumor suppressive activity was clearly higher when T cells were stimulated with loaded DC (Fig. 3, condition C) as compared to cultured with unloaded DC (Fig. 3, condition A). Addition of rIL-10 during stimulation resulted in an increase of the IFN-γ index at the end of the first stimulation, and further increased the tumor suppressive activity of effector T cells stimulated with loaded DC in experiment 1 and 4, but not in experiment 2 and 3. Of note, addition of IL-10 during stimulation resulted also in an overall higher increase of IFN-γ index during the effector phase in experiment 1 and 4 (10-fold) as compared to experiment 2 and 3 (2- to 5-fold).
Addition of rIL-10 during stimulation increases the suppressive activity on tumor cell viability and increases IFN-γ production by effector T cells that show increased IFN-γ production during first stimulation with loaded DC. T cells were stimulated as described with loaded DC or cultured with unloaded DC in the presence of cytokines with or without exogenous addition of rIL-10, and effector T cells were then co-cultured with GBM tumor cells. At the end of the primary stimulation, the secondary stimulation and at three different time points during the effector phase, IFN-γ and IL-10 were measured in the supernatant, and the index was calculated as described: in the table, “control” refers to the index of the variable in condition C (graph) in relation to the variable in condition A (graph); “ + IL-10” refers to the index of the variable in condition D (graph) in relation to the variable in condition B (graph)
Discussion
T cells stimulated twice with autologous DC loaded with GBM tumor lysates in the presence of rIL-6/rIL-12 in the first and rIL-2/rIL-7 in the second stimulation, shift towards Th1 cytokine production. T cells stimulated with loaded DC cells (experimental condition) produce IL-10 to a certain, in general lower, extent as compared to T cells that were cultured with autologous unloaded DC (control condition). Surprisingly, the persistent, relative amount of IL-10 production in the experimental condition at the end of the two stimulations and during the effector phase was strongly correlated with the tumor growth suppressive activity. Addition of IL-10 during stimulation improved the subsequent tumor growth suppressive activity and Th1 response when IL-10 resulted in an increase of the IFN-γ index after the first stimulation. The persistent production of IL-10 by T cells stimulated with loaded DC seems to be critical for the subsequent tumor growth suppressive capacity of Th1 shifted effector cells. Why certain T cells loose the ability to produce enough IL-10 if stimulated with tumor-lysate loaded autologous DC and others don’t, remains an open question: the consequence, however, is a clear loss of tumor growth suppressive activity to an extent less than if these T cells would have been stimulated by unloaded DC.
The stimulation procedure that was published earlier [19] appears to be efficient for the generation of Th1 cytokine production by T cells when stimulated with loaded DC. Depending on the type of cytokines produced by activated CD4 + T helper cells, a distinction is made between Th1 cells that produce IL-2, TNF-α and IFN-γ and Th2 cells that produce IL-4, IL-5 and IL-13 [23]. For all vaccination strategies, shifting towards cell-mediated immune response, mainly based on the induction of IFN-γ production, has been considered to be essential for the generation of a long-lasting specific immune response against tumor cells [15, 23]. Nevertheless, recent reports focused on the possibility to induce tumor control based on Th2-type immune responses especially in adoptive immune therapies [24]. The role of CD4 + T cells playing an effective role in tumor immunity against gliomas independent of CD8 + cytotoxic T lymphocyte (CTL) responses has been shown in vaccinated β2-microglobulin-/-mice [25]. A similar distinction in cytotoxic T cells type 1 (Tc1) and type 2 (Tc2) cells, according to cytokine production profiles has been made for CD8 + effector cells [26]. Both Tc1 and Tc2 effector cells could induce long-term tumor immunity, albeit through different mechanisms involving either donor effector cell-derived IFN-γ or IL-4/IL-5 [27]. However, in these experiments, long-term survival and tumor protection were always dependent on recipient T cell-derived IFN-γ and TNF-α.
As read-out system for effective anti-tumoral T cell activity, we did not perform CTL assays, as we did in a previously published work [13], but we performed co-cultures of effector T cells with proliferating tumor cells, and assessed the residual viability of the tumor cells after fixed periods of co-culture. Viability of tumor cells was assessed with MTT [20]. The current read-out system might reflect another aspect of the in vivo situation because it also includes anti-tumoral effects different from CTL-mediated tumor cell killing [20]. We therefore can not make a clear distinction between suppressive activity on tumor cell viability and tumor cell killing by CTL. On the other hand, in other experiments we clearly demonstrated the generation of CTL killing activity using this experimental set-up [13].
A major difficulty in our study was the presence of non-specific reactivity by T cells induced by the combination of rIL-6/rIL-12 and afterwards rIL-2/rIL-7. However, control conditions of cultures of T cells alone in the presence of stimulating cytokines, similar to the control conditions used in this study, were not described in other studies using the same stimulatory cytokine cocktail [19]. Even more problematic is the presence of an auto-MLR phenomenon resulting in activation of T cells by autologous DC. In the referred studies, a culture with autologous unloaded mature DC as control condition is not described, likely due to the existence of these aspecific findings induced by auto-MLR. In our experiments, this phenomenon was not due to the presence of foreign serum, as we used autologous inactivated plasma. On the other hand, beside the exogenous added cytokines in our experiments, factors in autologous serum may influence the strength of the auto-MLR [28]. We calculated indices of the read-out variables obtained from T cells that were stimulated in the presence of loaded DC and stimulating cytokines versus those obtained from T cells that were cultured with unloaded DC in the presence of stimulating cytokines. We thereby were able to correct for the auto-MLR effect within each experiment and could focus on the pure effect of loading the DC with GBM tumor lysate as stimulation factor. Based on the calculations of these indices, we were able to find a striking correlation between the presence of IL-10 during stimulation and effector phase and the tumor growth suppressive activity of the involved T cells. This correlation is remarkable in view of the large ranges depicted in Table 1. A possibly critical relative amount of IL-10 production in the experimental condition, extrapolated at 40% of the IL-10 production in the control condition (IL-10 index > 0.4) is thought to be necessary for a superior glioma growth control in the experimental versus the control condition. Although not demonstrated separately, we strongly believe that IL-10 is produced by CD4 + T cells and not by loaded DC. First, human CD8 + effector T cells do not produce IL-10 [29]. Next, during the effector phase, when tumor cells are co-cultured with effector T cells in the absence of DC, IL-10 was found as well and the IL-10 index at time of the effector phase was correlated with the IL-10 index found at the end of the second stimulation. Finally, the IL-10 index after stimulation and during effector phase were inversely correlated with the tumor viability index reflecting anti-tumoral T cell activity.
The role of IL-10 in tumor immunology is enigmatic. In general, IL-10 is considered to be an immune suppressive agent and a large variety of mechanisms have been described: down-regulation of costimulatory and MHC molecule expression [30], decreasing pro-inflammatory cytokine production by Antigen Presenting Cells (APC) [30], a direct inhibitory effect on T cells [31] and inhibition of CD28 tyrosine phosphorylation [32]. Also in tumor immunology IL-10 is known to compromise the ability to reject the tumor as shown in several experimental models [33–35]. More specifically in glioma tumor immunology IL-10 is characterised as one of the immune suppressive agents produced by the tumor to escape immune surveillance [36]. Nevertheless, several other reports documented the ability of IL-10 to augment tumor immunity in several models [37–39] including glioma models [40]. IL-10 producing CD4 + T cells have been shown to manifest anti-glioma functions in vivo [25]. Moreover glioma rejection in primed IL-10-/- mice was significantly impaired as well as in wild-type mice treated with neutralizing antibodies against IL-10. Our in vitro data in the human system confirm the role of IL-10 to mediate generation and functioning of GBM tumor cell suppressive activity by T cells. Of note, addition of rIL-10 to GBM cell cultures did not suppress tumor cell viability directly (data not shown).
The complex interaction between IFN-γ production, IL-10 production, T cell proliferation and tumor growth suppressive activity is not yet clarified. Recent data, however, showed a potential role of autocrine IFN-γ to induce indoleamine 2,3-dioxygenase (IDO) in DC following ligation of CD80/CD86, thereby stimulating immunosuppressive effects through induction of apoptosis of mainly Th1 cells and inhibition of T cell proliferation [41, 42]. IL-10 has been shown to down-regulate the IDO induction by IFN-γ [43]. Taking these interactions into consideration, a certain critical amount of IL-10 in the cytokine environment might prolong the Th1 response, both at the level of T cell proliferation and IFN-γ production, and, as a consequence, also at the level of cell-mediated antitumoral activity. This hypothesis can also explain why in some experiments, addition of IL-10 results in increased IFN-γ production when T cells are stimulated with loaded DC, and why addition of IL-10 during stimulation results in increased IFN-γ production and tumor growth suppressive capacity during the effector phase. The reason why IL-10 production by T cells is diminished in some experiments after stimulation with loaded DC in the presence of rIL-6/rIL-12 and rIL-2/rIL-7 as compared to unloaded DC remains unclear but is likely related to the antigen-presenting functioning of loaded DC as compared to unloaded DC.
In conclusion, we demonstrated that T cells can be primed against GBM tumor cells by autologous DC loaded with GBM tumor cell lysate. Stimulated T cells obtained a Th1 cytokine profile. On the other hand, a residual capacity to produce IL-10 was also required, and correlated with anti-tumor T cell activity, pointing to the importance of IL-10 as an immune modulatory rather than immune suppressive cytokine, both in the priming and effector phase.
References
Fleury A, Menegoz F, Grosclaude P, Daures JP, Henry Amar M, Raverdy N, Schaffer P, Poisson M, Delattre JY (1997) Descriptive epidemiology of cerebral gliomas in France. Cancer 79:1195–1202
Tamber MS, Rutka JT (2003) Pediatric supratentorial high-grade gliomas. Neurosurg Focus 14: http://www.medscape.com/viewarticle/449870
Stupp R, Mason WP, van den Bent MJ, Weller M, Fisher B, Taphoom MJ, Belanger K, Brandes AA, Marosi C, Bogdahn U, Curschmann J, Janzer RC, Ludwin SK, Gorlia T, Allgeier A, Lacombe D, Cairncross JG, Eisenhauer EA, Mirimanoff RO (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Eng J Med 352:987–996
Kleihues P, Soylemezoglu F, Schauble B, Scheithauer BW, Burger PC (1995) Histopathology, classification, and grading of gliomas. Glia 15:211–221
Siesjo P, Visse E, Sjogren HO (1996) Cure of established, intracerebral rat gliomas induced by therapeutic immunizations with tumor cells and purified APC or adjuvant IFN-gamma treatment. J Immunother Emphasis Tumor Immunol 19:334–345
Liau LM, Black KL, Prins RM, Sykes SN, DiPatre PL, Cloughesy TF, Becker DP, Bronstein JM (1999) Treatment of intracranial gliomas with bone marrow-derived dendritic cells pulsed with tumor antigens. J Neurosurg 90:1115–1124
Heimberger AB, Crotty LE, Archer GE, McLendon RE, Friedman A, Dranoff G, Bigner DD, Sampson JH (2000) Bone marrow-derived dendritic cells pulsed with tumor homogenate induce immunity against syngeneic intracerebral glioma. J Neuroimmunol 103:16–25
Insug O, Ku G, Ertl HC, Blaszczyk-Thurin M (2002) A dendritic cell vaccine induces protective immunity to intracranial growth of glioma. Anticancer Res 22:613–621
Yu JS, Liu G, Ying H, Yong WH, Black KL, Wheeler CJ (2004) Vaccination with tumor lysate-pulsed dendritic cells elicits antigen-specific, cytotoxic T-cells in patients with malignant glioma. Cancer Res 64:4973–4979
De Vleeschouwer S, Van Calenbergh F, Demaerel P, Flamen P, Rutkowski S, Kaempgen E, Wolff JEA, Plets C, Sciot R, Van Gool SW (2004) Transient local response and persistent tumor control of recurrent malignant glioma treated with combination therapy including dendritic cell therapy. J Neurosurg Spine 100:492–497
Rutkowski S, De Vleeschouwer S, Kaempgen E, Wolff JEA, Kuhl J, Demaerel P, Warmuth-Metz M, Flamen P, Van Calenbergh F, Plets C, Sorensen N, Opitz A, Van Gool SW (2004) Surgery and adjuvant dendritic cell-based tumour vaccination for patients with relapsed malignant glioma, a feasibility study. Br J Cancer 91:1656–1662
Yamanaka R, Abe T, Yajima N, Tsuchiya N, Homma J, Kobayashi T, Narita M, Takahashi M, Tanaka R (2003) Vaccination of recurrent glioma patients with tumour lysate-pulsed dendritic cells elicits immune responses: results of a clinical phase I/II trial. Br J Cancer 89:1172–1179
De Vleeschouwer S, Arredouani M, Ade M, Cadot P, Vermassen E, Ceuppens JL, Van Gool SW (2005) Uptake and presentation of malignant glioma tumor cell lysates by monocyte-derived dendritic cells. Cancer Immunol Immunother 54:372–382
Romani N, Reider D, Heuer M, Ebner S, Kämpgen E, Eibl B, Niederwieser D, Schuler G (1996) Generation of mature dendritic cells from human blood. An improved method with special regard to clinical applicability. J Immunol Methods 196:137–151
Schuler-Thurner B, Schultz ES, Berger TG, Weinlich G, Ebner S, Woerl P, Bender A, Feuerstein B, Fritsch PO, Romani N, Schuler G (2002) Rapid induction of tumor-specific type 1 T helper cells in metastatic melanoma patients by vaccination with mature, cryopreserved, peptide-loaded monocyte-derived dendritic cells. J Exp Med 195:1279–1288
Bullens DMA, Rafiq K, Charitidou L, Peng X, Kasran A, Warmerdam PAM, Van Gool SW, Ceuppens JL (2001) Effects of costimulation by CD58 on human T cell cytokine production: a selective cyokine pattern with induction of high IL-10 production. Int Immunol 13:181–191
Chaux P, Vantomme V, Coulie P, Boon T, vanderBruggen P (1998) Estimation of the frequencies of anti-MAGE-3 cytolytic T-lymphocyte precursors in blood from individuals without cancer. Int J Cancer 77:538–542
Herr W, Ranieri E, Olson W, Zarour H, Gesualdo L, Storkus WJ (2000) Mature dendritic cells pulsed with freeze-thaw cell lysates define an effective in vitro vaccine designed to elicit EBV-specific CD4(+) and CD(8) T lymphocyte response. Blood 96:1857–1864
van der Bruggen P, Bastin J, Gajewski TF, Coulie PG, Boel P, De Smet C, Traversari C, Townsend A, Boon T (1994) A peptide encoded by human gene MAGE-3 and presented by HLA-A2 induces cytolytic T lymphocytes that recognize tumor cells expressing MAGE-3. Eur J Immunol 24:3038–3043
Knüpfer MM, Knüpfer H, Jendrossek V, Van Gool SW, Wolff JEA, Keller E (2001) Interferon-gamma inhibits growth and migration of A172 human glioblastoma cells. Anticancer Res 21:3989–3994
Matthews JN, Altman DG, Campbell MJ, Royston P (1990) Analysis of serial measurements in medical research. Bmj 300:230–235
Moudgil A, Toyoda M, Galfayan K, Jordan SC (1997) Selective expression of the interleukin-2 gene discriminates between the auto- and allo-mixed lymphocyte reaction. Transpl Immunol 5:35–38
Dong C, Flavell RA (2001) Th1 and Th2 cells. Curr Opin Hematol 8:47–51
Schuler T, Kammertoens T, Preiss S, Debs P, Noben-Trauth N, Blankenstein T (2001) Generation of tumor-associated cytotoxic T lymphocytes requires interleukin 4 from CD8(+) T cells. J Exp Med 194:1767–1775
Segal BM, Glass DD, Shevach EM (2002) Cutting Edge: IL-10-producing CD4 + T cells mediate tumor rejection. J Immunol 168:1–4
Carter LL, Dutton RW (1996) Type 1 and type 2: a fundamental dichotomy for all T-cell subsets. Curr Opin Immunol 8:336–342
Dobrzanski MJ, Reome JB, Hollenbaugh JA, Dutton RW (2004) Tc1 and tc2 effector cell therapy elicit long-term tumor immunity by contrasting mechanisms that result in complementary endogenous type 1 antitumor responses. J Immunol 172:1380–1390
Zinberg M, Francus T, Weksler ME, Siskind GW, Karpatkin S (1982) Abnormal autologous mixed lymphocyte reaction in autoimmune thrombocytopenic purpura. Blood 59:148–151
Rafiq K, Charitidou L, Bullens DMA, Kasran A, Lorré K, Ceuppens JL, Van Gool SW (2000) Regulation of IL-10 production by human T cells. Scand J Immunol
Koch F, Stanzl U, Jennewein P, Janke K, Heufler C, Kämpgen E, Romani N, Schuler G (1996) High level IL-12 production by murine dendritic cells: Upregulation via MHC class II and CD40 molecules and downregulation by IL-4 and IL-10. J Exp Med 184:741–746
Moore KW, de Waal Malefyt R, Coffman RL, O’Garra A (2001) Interleukin-10 and the interleukin-10 receptor. Annu Rev Immunol 19:683–765
Akdis CA, Blaser K (2001) Mechanisms of interleukin-10-mediated immune suppression. Immunology 103:131–136
Hagenbaugh A, Sharma S, Dubinett SM, Wei SH, Aranda R, Cheroutre H, Fowell DJ, Binder S, Tsao B, Locksley RM, Moore KW, Kronenberg M (1997) Altered immune responses in interleukin 10 transgenic mice. J Exp Med 185:2101–2110
Halak BK, Maguire HC Jr, Lattime EC (1999) Tumor-induced interleukin-10 inhibits type 1 immune responses directed at a tumor antigen as well as a non-tumor antigen present at the tumor site. Cancer Res 59:911–917
Kim BG, Joo HG, Chung IS, Chung HY, Woo HJ, Yun YS (2000) Inhibition of interleukin-10 (IL-10) production from MOPC 315 tumor cells by IL-10 antisense oligodeoxynucleotides enhances cell-mediated immune responses. Cancer Immunol Immunother 49:433–440
Nitta T, Hishii M, Sato K, Okumura K (1994) Selective expression of interleukin-10 gene within glioblastoma multiforme. Brain Res 649:122–128
Berman RM, Suzuki T, Tahara H, Robbins PD, Narula SK, Lotze MT (1996) Systemic administration of cellular IL-10 induces an effective, specific, and long-lived immune response against established tumors in mice. J Immunol 157:231–238
Zheng LM, Ojcius DM, Garaud F, Roth C, Maxwell E, Li Z, Rong H, Chen J, Wang XY, Catino JJ, King I (1996) Interleukin-10 inhibits tumor metastasis through an NK cell-dependent mechanism. J Exp Med 184:579–584
Groux H, Cottrez F, Rouleau M, Mauze S, Antonenko S, Hurst S, McNeil T, Bigler M, Roncarolo MG, Coffman RL (1999) A transgenic model to analyze the immunoregulatory role of IL-10 secreted by antigen-presenting cells. J Immunol 162:1723–1729
Book AA, Fielding KE, Kundu N, Wilson MA, Fulton AM, Laterra J (1998) IL-10 gene transfer to intracranial 9L glioma: tumor inhibition and cooperation with IL-2. J Neuroimmunol 92:50–59
Terness P, Bauer TM, Rose L, Dufter C, Watzlik A, Simon H, Opelz G (2002) Inhibition of allogeneic T cell proliferation by indoleamine 2,3-dioxygenase-expressing dendritic cells: mediation of suppression by tryptophan metabolites. J Exp Med 196:447–457
Grohmann U, Orabona C, Fallarino F, Vacca C, Calcinaro F, Falorni A, Candeloro P, Belladonna ML, Bianchi R, Fioretti MC, Puccetti P (2002) CTLA-4-Ig regulates tryptophan catabolism in vivo. Nat Immunol 3:1097–1101
MacKenzie CR, Gonzalez RG, Kniep E, Roch S, Daubener W (1999) Cytokine mediated regulation of interferon-gamma-induced IDO activation. Adv Exp Med Biol 467:533–539
Acknowledgements
This project is supported by the Olivia Hendrickx Research Fund, The Belgian Federation against Cancer, Electrabel Netmanagement Vlaanderen, and charities from private families.
Author information
Authors and Affiliations
Corresponding author
Additional information
SDV and ISL were recipients of a grant from the Emmanuel van der Schueren Fund.
SWVG is Senior Clinical Investigator of the Fund for Scientific Research—Flanders (Belgium) (F.W.O.-Vlaanderen)
Rights and permissions
About this article
Cite this article
De Vleeschouwer, S., Spencer Lopes, I., Ceuppens, J.L. et al. Persistent IL-10 production is required for glioma growth suppressive activity by Th1-directed effector cells after stimulation with tumor lysate-loaded dendritic cells. J Neurooncol 84, 131–140 (2007). https://doi.org/10.1007/s11060-007-9362-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-007-9362-y