Abstract
RNA-based genetic immunization represents an alternative novel strategy for antigen-specific cancer vaccines. In the present paper we investigate the use of synthetic messenger RNA in an experimental melanoma model. We show that gene gun-based immunization using synthetic RNA mediates gene expression in the epidermis and effectively induces antigen-specific cellular and humoral immunity in mice in vivo. Importantly, bombardment of the skin with RNA coding for the melanocytic self-antigen TRP2 linked to the immunogenic protein EGFP was associated with protection against experimentally induced B16 melanoma lung metastases and vitiligo-like fur depigmentation. Our results provide a scientific basis for clinical trials using synthetic mRNA encoding melanocytic antigens linked to immunogenic helper proteins for vaccination of patients with melanoma.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The molecular identification of tumor antigens recognized by specific cytotoxic T lymphocytes (CTL) has revolutionized the field of cancer immunotherapy, opening up new possibilities for the induction and measurement of antigen-specific immune responses. The concept of antigen-specific vaccination has generated great interest particularly for the immunotherapy of melanoma, a tumor entity, which has been the focus of interest of many tumor immunologists over years and for which a large series of different antigens have been defined. These include lineage specific differentiation antigens such as the tyrosinase family of enzymes involved in melanin synthesis, which are endogenously expressed in melanocytes and melanoma cells, cancer-germline antigens such as the MAGE family, overexpressed antigens such as telomerase and individually mutated proteins [1–4]. Currently, it is still unclear, which antigen and which vaccination strategy should be applied to optimally induce clinically effective immune responses against melanoma.
Our group has previously tested several vaccination strategies in an experimental mouse model targeting the melanocytic self-antigen TRP2, which has been identified as a tumor rejection antigen with melanoma-specific cytotoxic T cells [5]. We and others observed that peripheral immune tolerance limits the induction of potentially autoreactive CD8+ T cells [6–8]. Strong TRP2-specific cellular immunity could only be stimulated when immunogenic helper determinants were linked to the weakly immunogenic self-antigen TRP2 [9]. Here we investigated the use of synthetic messenger RNA as an alternative antigen format for a gene gun-based genetic immunization protocol. We show that gene gun immunization using synthetic mRNA coding for TRP2 linked to the immunogenic EGFP can also effectively induce antigen-specific cellular immunity in mice in vivo and mediate protection against B16 lung metastases and vitiligo-like fur depigmentation.
Materials and methods
Animals, donors and cell lines
C57BL/6 mice (H-2b), 6–12 weeks old, were bred at the Central Animal Facility of the University of Bonn. B16 (H-2b) is a spontaneous murine melanoma and was maintained in DMEM supplemented with 10% heat-inactivated FCS, 2 mM L-glutamine, 50 μM 2-mercaptoethanol, 100 IU/ml penicillin, and 100 μg/ml streptomycin (all reagents were from Life Technologies GmbH, Eggenstein, Germany). All experiments with mice were approved by the local governmental authorities and carried out according to standard guidelines for the care of laboratory animals.
Plasmids and in vitro transcription and polyadenylation of RNA
The plasmids pCI-β-gal and pCI-EGFP.TRP2 expressing Escherichia coli β-gal and the fusion protein of EGFP and murine TRP2 (EGFP.TRP2) have been described previously [9]. Plasmids were grown in E. coli strain DH5α and purified using Qiagen Plasmid Maxi Kits (Qiagen, Hilden, Germany). Plasmids were linearized with Bam H I (Roche, Mannheim, Germany). In vitro transcription was performed as described previously [10]. With the Ribomax large-scale RNA production system T7 (Promega, Mannheim, Germany) according to the manufacturer’s instructions. Briefly, linearized DNA templates were incubated for 4 h at 37°C in a reaction containing T7 10 times reaction buffer, ATP, CTP, UTP (7.5 mM each), 1 mM GTP, 5 mM m7G(5′)ppp(5′)G cap-analogon (Invitrogen GmbH, Karlsruhe, Germany) and T7 RNA Polymerase. The RNA was resuspended in water and stored at −80°C. In vitro-transcribed RNA was polyadenylated using the Poly (A) Polymerase (USB Cleveland, OH, USA) according to the manufacturer’s instructions. Briefly, in vitro-transcribed RNA was incubated for 1 h at 30°C in a reaction containing Poly (A) polymerase reaction buffer, ATP (Promega; 600 pmol per pmol RNA) and Poly (A) polymerase (USB; 12U per pmol RNA). mRNA was resuspended in water and stored at −80°C.
Genetic immunization of mice
Genetic immunization with synthetic RNA or plasmid DNA using the gene gun has been performed as described previously [9]. Briefly, plasmid DNA was precipitated onto 1.6 μm gold particles at a density of 2 μg per mg of particles. Synthetic RNA was precipitated at a densitiy of 30 μg per mg of particles. Gold particles were resuspended in 100 μl of 0.05 M spermidine (Sigma Chemical Co., St. Louis, MO, USA) and DNA or RNA precipitated by the addition of 100 μl of 1 M CaCl2. Particles were washed with ethanol to remove H2O, resuspended in ethanol containing 0.075 mg/ml of PVP (Sigma), and coated onto the inner surface of Tefzel tubing using a tube loader. The tubing was cut into 0.5 inch segments, each containing approximately 0.5 mg gold coated with 1 μg plasmid DNA or 15 μg of synthetic RNA. For immunizations, shaved skin of the abdomen was transfected in vivo by two shots with the Helios gene gun at a pressure of 400 psi, resulting in the delivery of a total of approximately 2 μg of plasmid DNA or 30 μg of synthetic RNA. Immunizations were repeated after 1 week. Gold particles, tubing, tube loader, and the Helios gene gun were purchased from BioRad (Munich, Germany).
Verification of antigen-expression in vivo
Skin sections were taken 24 h after gene gun bombardement with β-galacotsidase-encoding or EGFP.mTRP2-encoding mRNA or plasmid DNA and cryo-conserved. 4–5 μm section were prepared, fixed with acetone and analyzed. β-gal expression in keratinocytes of superficial epidermis and hair follicles was determined by standard β-gal staining using X-Gal substrate (1 mg/ml X-Gal in PBS/5 mM potassium ferricyanide/5 mM potassium ferrocyanide/2 mM magnesium chloride; Roth, Karlsruhe, Germany). EGFP expression was determined by fluorescence microscopy.
Sandwich ELISA assays
Antibodies against β-gal or EGFP present in serum samples obtained from mice after genetic immunization were measured by ELISA using recombinant EGFP or β-gal produced in E. coli and purified by affinity chromatography as a solid-phase antigen. Briefly, microtiter plates were coated with 5 μg/ml protein in carbonate buffer (pH 9.6) for 16 h at 4°C and blocked with PBS containing 3% BSA and 0.05% Tween. Serum samples were serially diluted in PBS containing 1% BSA and 0.05% Tween (assay buffer) and added for 2 h. Bound antibodies were detected using peroxidase-conjugated donkey anti-mouse IgG (Jackson Immunoresearch, Westgrove, PA, USA) at a 1:5000 dilution in assay buffer followed by color development with ABTS substrate system (Sigma). Plates were read in an ELISA reader at 405 nm.
Peptides and ELISPOT assays
The H-2Kb-binding peptide SVYDFFVWL (TRP2aa180–188) derived from the murine melanosomal protein TRP2 [5] and the H-2Kb-binding peptide ICPMYARV (β-galaa497–504) derived from E. coli β-gal were purchased from Sigma Genosys. Peptides were dissolved at 10 mg/ml in PBS containing 10% DMSO and stored at −20°C. The induction of peptide-specific T-cells was measured using the ELISPOT technique. Briefly, splenocytes were harvested 1 and 2 weeks after immunization and red blood cells depleted. 106 splenocytes/well were restimulated in 200 μl of CM containing 1 μg/ml synthetic peptide and 25 IU/ml rhIL-2 in Millipore HA plates, which were coated overnight with 10 μg/ml (50 μl/well) of anti-mIFNγ mAb (R4-6A2, Pharmingen, Heidelberg, Germany) in PBS. After 22 h cells were washed out of the plates and bound cytokines visualized by incubation with 2.5 μg/ml (50 μl/well) of biotinylated anti-mIFNγ mAb (XMG1.2, Pharmingen) for 1.5 h at 37°C, followed by 100 μl/well streptavidin-peroxidase (Roche, 1:1500 dilution in PBS containing 1% BSA, and 0.05% Tween 20) for 1/2 h at RT, and premixed peroxidase substrate kit DAB (Vector Laboratories, Heidelberg, Germany). The number of spots was counted under a dissecting microscope and expressed as mean number of spots of repeated duplicate or triplicate determinations. All experiments were performed three to five times.
Tumor protection assays and detection of vitiligo
Induction of antitumor immunity was assessed 2 weeks after immunization. Mice were challenged by intravenous injection of 4×105 B16 melanoma cells, which experimentally induces heavily pigmented lung metastases. The number of macroscopically visible metastases on the surface of the lungs was counted with the help of a dissecting microscope 14 days after challenge. All experiments included six mice per group and were performed three times with similar results. Alternatively, mice were followed for the appearance of coat color changes in the bombarded areas of the shaved abdomen.
Results
Expression of antigen in the skin following gene gun bombardment with synthetic RNA
Initially, we wished to optimize expression of antigen in the epidermis following bombardment of the skin with mRNA-coated gold particles. Based on our previous experience with plasmid DNA we used the bacterial protein E. coli β-galactosidase (β-gal) and the melanosomal enzyme TRP2 fused to enhanced green fluorescent protein (EGFP) as model antigens in C57BL/6 mice. β-galactosidase-encoding and EGFP.mTRP2-encoding mRNA were transcribed in vitro from expression plasmids as described in materials and methods and subsequently polyadenylated. Synthetic mRNA was precipitated onto gold beads, loaded into plastic cartridges and used for bombardment of mice into the shaved abdominal skin using the gene gun. Each shot resulted in the delivery of 15 μg mRNA, which had previously been determined to work efficiently. Control mice received 1 μg plasmid DNA encoding β-gal or EGFP.mTRP2 as described [9]. Skin was harvested 24 h after gene gun bombardment and snap frozen. Cryosections were stained with X-gal to visualize expression of β-gal or investigated with a fluorescence microscope to visualize expression of EGFP. Antigen expression by in vivo transfected keratinocytes following bombardment of the skin with synthetic mRNA could clearly be demonstrated (Fig. 1).
Antigen expression in keratinocytes of the superficial epidermis and the hair follicles following gene gun bombardment with plasmid DNA or synthetic mRNA. a , c β-gal galactosidase expression was verified by X-gal staining of mouse skin 24 h after gene gun immunization as indicated. b, d EGFP expression was verified by fluorescence microscopy of mouse skin 24 h after gene gun immunization as indicated
Stimulation of antigen-specific humoral and cellular immunity
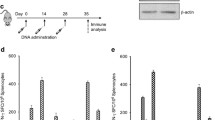
In subsequent experiments, we sought to determine whether gene gun bombardment of the skin with synthetic mRNA was able to induce humoral and cellular immunity to the encoded antigens. Groups of four mice were each bombarded with two shots delivering a total of 30 μg RNA coding for either β-gal or the fusion protein EGFP.mTRP2 and boosted 1 week later. Control groups of mice received 1 μg plasmid DNA encoding β-gal or EGFP.mTRP2. Two weeks later, serum was harvested and tested for the presence of antibodies specifically recognizing recombinant β-gal or EGFP protein using a sandwich ELISA. Alternatively, splenocytes were harvested and tested for the induction of antigen-specific T cells recognizing the H-2Kb -binding peptides ICPMYARV derived from amino acid 497–504 of β-gal or SVYDFFVWL derived from amino acid 180–188 of murine TRP2 using the ELISPOT technique. Importantly, we could verify the in vivo induction of antigen-specific humoral and cellular immunity in mRNA-immunized mice as illustrated in Fig. 2. In direct comparison, we could not detect significant differences between mice vaccinated with synthetic RNA or plasmid DNA.
Stimulation of antigen-specific cellular and humoral immune responses in vivo. Groups of C57BL/6 mice were immunized by particle-mediated gene transfer using the indicated plasmid DNA or synthetic mRNA. a Sera were obtained from groups of mice after immunization, pooled and tested for the presence of antibodies reactive with recombinant EGFP protein as a solid phase antigen using ELISA. Results of triplicate measurements expressed as mean optical density (405 nm) at a serum dilution of 1:100 are shown. These data are representative of three independent experiments. b Similar results were obtained with recombinant β-gal galactosidase as a solid phase antigen. c Alternatively, splenocytes were harvested after immunization. Release of IFNγ in response to the H-2Kb -binding TRP2aa180–188 peptide was tested using IFNγ ELISPOT assays. Results are expressed as mean number of spot forming cells per 106 splenocytes. These data are representative of five independent experiments
Induction of protective immunity to melanoma and autoimmune vitiligo-like depigmentation of the skin
Since gene gun immunization with synthetic RNA was able to induce cellular and humoral immunity, we subsequently investigated the ability to promote protective anti-melanoma immunity against experimentally induced B16 melanoma lung metastases. Groups of four C57BL/6 mice were shaved on the abdomen and bombarded on days 1 and 8 with 30 μg mRNA encoding either β-gal or EGFP.mTRP2. On day 14, mice were challenged intravenously with 4×105 cultured B16 melanoma cells and metastases on the lung surfaces determined 2 weeks later. As illustrated in a representative experiment in Fig. 3a, mice vaccinated with mRNA encoding the fusion protein EGFP.mTRP2 were significantly protected against growth of B16 melanoma lung metastases. Alternatively, mice immunized with mRNA coding for β-gal or EGFP.mTRP2 were monitored for the appearance of coat color changes in the gene gun-transfected skin of the abdomen. Importantly, bombardment with mRNA encoding EGFP.mTRP2 was associated with vitiligo-like fur depigmentation indicating autoimmune destruction of melanocytes in the hair follicles (Fig. 3b). Consistent with our own previous work and that of other research groups using plasmid DNA and recombinant viruses [6, 7, 9, 11, 13, 50] we never observed vitiligo-like coat color changes in mice immunized with synthetic RNA encoding β-galactosidase.
Induction of protective immunity to melanoma and vitiligo-like fur depigmentation. Groups of C57BL/6 mice were immunized by particle-mediated gene transfer using the indicated synthetic mRNA. a The induction of protective tumor immunity against experimentally induced B16 melanoma lung metastases was assessed 2 weeks later. Shown are the number of lung metastases in individual mice (dots) and the mean number of metastases in each group (horizontal bar). This experiment was repeated three times with similar results. b Alternatively, mice were followed for the appearance of vitiligo-like fur depigmentation. Shown is a representative picture of a mouse immunized with mRNA coding for EGFP.mTRP2
Discussion
In the present study we provide experimental evidence that synthetic messenger RNA can be used as an alternative antigen format for gene gun-based genetic melanoma vaccination. We show that bombardment of the skin with mRNA encoding a fusion protein between the melanocytic differentiation antigen TRP2 and the immunogenic helper determinant EGFP leads to cutaneous antigen-expression in vivo that induces potent cellular and humoral immune responses. Various melanoma vaccine strategies have recently been experimentally evaluated using TRP2 as a clinically relevant melanocytic self-antigen. Xenogeneic human TRP2 could be used effectively for genetic immunization, which presumably contains strong CD4+ T helper cell epitopes [7, 8]. Alternatively, cultured dendritic cells were used as a biological adjuvant to circumvent peripheral immune tolerance [6, 10, 14–17]. It has been shown that particle-bombardment of the skin with the gene gun is not only able to directly transfect keratinocytes but also dendritic cells in the epidermis [18, 19]. Direct transfection and activation of dendritic cells is thought to be critical for the induction of immune responses in the skin. Therefore, gene gun immunization targeting the skin may potentially be able to circumvent the laborious work to culture dendritic cells in vitro and use them as a biological vaccine adjuvant.
Immunization with synthetic mRNA has one very important advantage over naked DNA and recombinant viruses: it avoids the risk of random integration in the genome leading to mutational inactivation of cellular genes or, more importantly, to oncogenic transformation. When choosing mRNA as alternative antigen-format one biological property has always to be taken into account. mRNA may be rapidly hydrolysed by ubiquitous ribonucleases and therefore may not be an optimal alternative antigen-format for vaccine preparations. Despite these great concerns the injection of mRNA into muscle has been shown to efficiently mediate gene expression in vivo and effectively induce antigen-specific immune responses [20]. The use of synthetic messenger RNA for gene gun-based genetic immunization targeting the skin has first been reported by Qiu et al. [21] using β-gal as a model antigen. Methods that stabilize mRNA in vivo like the introduction of Xenopus laevis beta-globulin 5′ and 3′ flanking sequences or that confer protection from RNAse degradation are now being introduced and may further help to increase the half-life of transferred mRNA and the efficacy of mRNA-based cancer vaccines [22].
RNA as an antigen format has been extensively tested preclinically in mouse models to support clinical RNA-vaccination trials in cancer patients. Gilboa and colleagues showed that dendritic cells pulsed with tumor RNA efficiently induce antitumor immunity in mice against OVA-expressing tumor cells [23] or murine B16 melanoma [24, 25]. Immunization of mice with dendritic cells pulsed with RNA encoding telomerase resulted in the induction of cytotoxic T lymphocytes, which lysed melanoma cells and inhibited the growth of unrelated tumors in mice of distinct genetic backgrounds [26]. Granstein et al. [27] showed that immunization of mice with freshly isolated epidermal cells enriched for Langerhans cells and pulsed with crude tumor cell-derived RNA are able to induce tumor-specific immunity.
The experience gathered in animal models have been complemented by comprehensive in vitro data from the human system. It has been shown by multiple investigators that both in vivo primed as well as naïve CD8+ and CD4+ T cell responses can be efficiently stimulated in vitro from peripheral blood mononuclear cells of patients and healthy human donors after stimualtion with RNA-transfected DC. This holds true for the stimulation of T lymphocytes using DC loaded with mRNA coding for defined viral antigens, such as the influenza matrix protein [28], EBV E6/E7 [29], EBV LMP2 [30] or HIV gag [31]. Efficient induction of antigen-specific CD8+ and CD4+ T lymphocytes was also achieved for mRNA of various autoantigens known to be expressed on human tumors, such as CEA [32], PSA [33], telomerase [26, 34], survivin [35], oncofetal antigen-immature laminin receptor [36] or Melan A Mart [37].
Immunization protocols can be based on vaccination with a single defined antigen or a mixture of more than one defined antigen. As mRNA can be extracted and further amplified from tumor tissue it is possible to obtain a vaccine covering the whole range of individual tumor-expressed antigens from a small tissue sample [27, 38]. In preparation of vaccination trials including this broader approach, preclinical experiments were conducted that applied autologous DCs loaded with RNA preparations amplified from tumor cells for the stimulation of human T cells. Resulting T cell populations showed antitumor reactivity and were able to specifically lyse various tumor cells used for stimulation, such as prostate cancer [39], multiple myeloma [40], colorectal Cancer [41] or CLL [42].
Based on the results of preclinical models, first immunotherapy trials with RNA as a vaccine for cancer patients have recently been initiated. Phase I clinical trials using RNA-transfected autologous DC showed safety and feasibility, as well as immunological and some clinical responses for the new antigen format. Heiser and colleagues conducted two initial trials in patients with metastatic prostate cancer and could achieve in vivo induction of T cell responses against prostate-specific antigen by vaccination DCs pulsed with mRNA encoding prostate-specific antigen [43] or transfected with RNA amplified from microdissected tumor cells [39]. These trials were followed by immunization trials initiated for patients with metastatic renal cell cancer. Administration of autologous DC transfected with total renal tumor RNA to patients had the potency to induce T cell reactivities directed against a broad set of renal tumor-associated antigens but not against self-antigens expressed by normal renal tissues [44]. Tumor-specific immune responses that are capable of recognizing and lysing autologous tumor cells have also been successfully induced in a patient with adenocarcinoma of the lung after immunization with autologous DC transfected with total tumor RNA [45]. Kobayashi and colleagues recently demonstrated that cytotoxic T cells, which were able to kill autologous glioma cells, could be elicted in a small group of patients by administration of tumor mRNA-loaded DC [46]. Although the trials published until now provide evidence on vaccine safety and in vivo bioactivity of RNA-loaded DC in a small number of patients with various tumor types, the proof for a broad clinical benefit remains to be delivered in future immunization trials. Further RNA-based immunization protocols are now being developed, that will introduce modifications to the RNA sequence to guarantee for higher in vivo stability, improved antigen-presentation through endosomal targeting or a more efficient T cell induction by the fusion of helper-sequences. It will also have to be shown if new administration routes, such as the direct injection of RNA into skin or draining lymph nodes, will avoid the need for the laborious and expensive generation of cellular carriers.
Independently of the approach used, it has to be kept in mind that a majority of tumor-antigens represent autoantigens and that immunity against these antigens is effectively blocked by peripheral tolerance mechanisms. Recent insights in the immunostimulatory effects of therapeutic nucleic acids suggest that the use of mRNA may activate innate antiviral pathways, which may be different from those stimulated by plasmid DNA. Specifically, bacterial DNA containing CpG motifs is recognized by TLR9, while single stranded RNA is recognized by TLR7 and 8 [47–49]. Future experiments will have to address the question whether the use of synthetic mRNA might be able to directly enhance the immunogenicity of TRP2 and substitute for linkage of immunogenic helper proteins.
Taken together, we demonstrate here that genetic immunization with synthetic mRNA encoding melanocytic antigens linked to immunogenic helper proteins can be successfully employed for the induction of anti-melanoma immunity in mice in vivo. Our results provide proof of principle for melanoma vaccines employing synthetic RNA in an experimental mouse model and provide a scientific basis for the translation of this strategy into future clinical trials.
Abbreviations
- EGFP:
-
Enhanced green fluorescent protein
- mTRP2:
-
Murine tyrosinase-related protein 2
References
Boon T, Coulie PG, Van den EB (1997) Tumor antigens recognized by T cells. Immunol Today 18:267
Rosenberg SA (2000) Identification of cancer antigens: impact on development of cancer immunotherapies. Cancer J 6(Suppl 3):200
Wölfel T, Van Pel A, Brichard V, Schneider J, Seliger B, Meyer zum Büschenfelde KH, Boon T (1994) Two tyrosinase nonapeptides recognized on HLA-A2 melanomas by autologous cytolytic T lymphocytes. Eur J Immunol 24:759
Wölfel T, Hauer M, Schneider J, Serrano M, Wolfel C, Klehmann-Hieb E, De Plaen E, Hankeln T, Meyer zum Buschenfelde KH, Beach D (1995) A p16INK4a-insensitive CDK4 mutant targeted by cytolytic T lymphocytes in a human melanoma. Science 269:1281
Bloom MB, Perry-Lalley D, Robbins PF, Li Y, el-Gamil M, Rosenberg SA, Yang JC (1997) Identification of tyrosinase-related protein 2 as a tumor rejection antigen for the B16 melanoma. J Exp Med 185:453
Tuting T, Steitz J, Bruck J, Gambotto A, Steinbrink K, Deleo AB, Robbins P, Knop J, Enk AH (1999) Dendritic cell-based genetic immunization in mice with a recombinant adenovirus encoding murine TRP2 induces effective anti-melanoma immunity. J Gene Med 1:400
Bowne WB, Srinivasan R, Wolchok JD, Hawkins WG, Blachere NE, Dyall R, Lewis JJ, Houghton AN (1999) Coupling and uncoupling of tumor immunity and autoimmunity. J Exp Med 190:1717
Steitz J, Bruck J, Steinbrink K, Enk A, Knop J, Tuting T (2000) Genetic immunization of mice with human tyrosinase-related protein 2: implications for the immunotherapy of melanoma. Int J Cancer 86:89
Steitz J, Bruck J, Gambotto A, Knop J, Tuting T (2002) Genetic immunization with a melanocytic self-antigen linked to foreign helper sequences breaks tolerance and induces autoimmunity and tumor immunity. Gene Ther 9:208
Britten CM, Meyer RG, Frankenberg N, Huber C, Wölfel T (2004) The use of clonal mRNA as an antigenic format for the detection of antigen-specific T lymphocytes in IFN-γ ELISPOT assays. J Immunol Methods 287:125
Steitz J, Bruck J, Knop J, Tuting T (2001) Adenovirus-transduced dendritic cells stimulate cellular immunity to melanoma via a CD4(+) T cell-dependent mechanism. Gene Ther 8:1255
Bronte V, Apolloni E, Ronca R, Zamboni P, Overwijk WW, Surman DR, Restifo NP, Zanovello P (2000) Genetic vaccination with and quot;self and quot; tyrosinase-related protein 2 causes melanoma eradication but not vitiligo. Cancer Res 60:253
Lane C, Leitch J, Tan X, Hadjati J, Bramson JL, Wan Y (2004) Vaccination-induced autoimmune vitiligo is a consequence of secondary trauma to the skin. Cancer Res 64:1509
Schreurs MW, Eggert AA, de Boer AJ, Vissers JL, van HT, Offringa R, Figdor CG, Adema GJ (2000) Dendritic cells break tolerance and induce protective immunity against a melanocyte differentiation antigen in an autologous melanoma model. Cancer Res 60:6995
Shibagaki N, Udey MC (2002) Dendritic cells transduced with protein antigens induce cytotoxic lymphocytes and elicit antitumor immunity. J Immunol 168:2393
Wang HY, Fu T, Wang G, Zeng G, Perry-Lalley DM, Yang JC, Restifo NP, Hwu P, Wang RF (2002) Induction of CD4(+) T cell-dependent antitumor immunity by TAT-mediated tumor antigen delivery into dendritic cells. J Clin Invest 109:1463
Shimizu K, Thomas EK, Giedlin M, Mule JJ (2001) Enhancement of tumor lysate-pulsed and peptide-pulsed dendritic cell-based vaccines by the addition of foreign helper protein. Cancer Res 61:2618
Condon C, Watkins SC, Celluzzi CM, Thompson K, Falo LD Jr (1996) DNA-based immunization by in vivo transfection of dendritic cells. Nat Med 2:1122
Porgador A, Irvine KR, Iwasaki A, Barber BH, Restifo NP, Germain RN (1998) Predominant role for directly transfected dendritic cells in antigen presentation to CD8+ T cells after gene gun immunization. J Exp Med 188:1075
Wolff JA, Malone RW, Williams P, Chong W, Acsadi G, Jani A, Felgner PL (1990) Direct gene transfer into mouse muscle in vivo. Science 247:1465
Qiu P, Ziegelhoffer P, Sun J, Yang NS (1996) Gene gun delivery of mRNA in situ results in efficient transgene expression and genetic immunization. Gene Ther 3:262
Hoerr I, Obst R, Rammensee HG, Jung G (2000) In vivo application of RNA leads to induction of specific cytotoxic T lymphocytes and antibodies. Eur J Immunol 30:1
Boczkowski D, Nair SK, Snyder D, Gilboa E (1996) Dendritic cells pulsed with RNA are potent antigen-presenting cells in vitro and in vivo. J Exp Med 184:465
Ashley DM, Faiola B, Nair S, Hale LP, Bigner DD, Gilboa E (1997) Bone marrow-generated dendritic cells pulsed with tumor extracts or tumor RNA induce antitumor immunity against central nervous system tumors. J Exp Med 186:1177
Zhang W, He L, Yuan Z, Xie Z, Wang J, Hamada H, Cao X (1999) Enhanced therapeutic efficacy of tumor RNA-pulsed dendritic cells after genetic modification with lymphotactin. Hum Gene Ther 10:1151
Nair SK, Heiser A, Boczkowski D, Majumdar A, Naoe M, Lebkowski JS, Vieweg J, Gilboa E (2000) Induction of cytotoxic T cell responses and tumor immunity against unrelated tumors using telomerase reverse transcriptase RNA transfected dendritic cells. Nat Med 6:1011
Granstein RD, Ding W, Ozawa H (2000) Induction of anti-tumor immunity with epidermal cells pulsed with tumor-derived RNA or intradermal administration of RNA. J Invest Dermatol 114:632
Strobel I, Berchtold S, Gotze A, Schulze U, Schuler G, Steinkasserer A (2000) Human dendritic cells transfected with either RNA or DNA encoding influenza matrix protein M1 differ in their ability to stimulate cytotoxic T lymphocytes. Gene Ther 7:2028
Thornburg C, Boczkowski D, Gilboa E, Nair SK (2000) Induction of cytotoxic T lymphocytes with dendritic cells transfected with human papillomavirus E6 and E7 RNA: implications for cervical cancer immunotherapy. J Immunother 23:412
Su Z, Peluso MV, Raffegerst SH, Schendel DJ, Roskrow MA (2002) Antigen presenting cells transfected with LMP2a RNA induce CD4+ LMP2a-specific cytotoxic T lymphocytes, which kill via a Fas-independent mechanism. Leuk Lymphoma 43:1651
Weissman D, Ni H, Scales D, Dude A, Capodici J, McGibney K, Abdool A, Isaacs SN, Cannon G, Kariko K (2000) HIV gag mRNA transfection of dendritic cells (DC) delivers encoded antigen to MHC class I and II molecules, causes DC maturation, and induces a potent human in vitro primary immune response. J Immunol 165:4710
Nair SK, Boczkowski D, Morse M, Cumming RI, Lyerly HK, Gilboa E (1998) Induction of primary carcinoembryonic antigen (CEA)-specific cytotoxic T lymphocytes in vitro using human dendritic cells transfected with RNA. Nat Biotechnol 16:364
Heiser A, Dahm P, Yancey DR, Maurice MA, Boczkowski D, Nair SK, Gilboa E, Vieweg J (2000) Human dendritic cells transfected with RNA encoding prostate-specific antigen stimulate prostate-specific CTL responses in vitro. J Immunol 164:5508
Su Z, Vieweg J, Weizer AZ, Dahm P, Yancey D, Turaga V, Higgins J, Boczkowski D, Gilboa E, Dannull J (2002) Enhanced induction of telomerase-specific CD4(+) T cells using dendritic cells transfected with RNA encoding a chimeric gene product. Cancer Res 62:5041
Zeis M, Siegel S, Wagner A, Schmitz M, Marget M, Kuhl-Burmeister R, Adamzik I, Kabelitz D, Dreger P, Schmitz N, Heiser A (2003) Generation of cytotoxic responses in mice and human individuals against hematological malignancies using survivin-RNA-transfected dendritic cells. J Immunol 170:5391
Siegel S, Wagner A, Kabelitz D, Marget M, Coggin J Jr, Barsoum A, Rohrer J, Schmitz N, Zeis M (2003) Induction of cytotoxic T-cell responses against the oncofetal antigen-immature laminin receptor for the treatment of hematologic malignancies. Blood 102:4416
Liao X, Li Y, Bonini C, Nair S, Gilboa E, Greenberg PD, Yee C (2004) Transfection of RNA encoding tumor antigens following maturation of dendritic cells leads to prolonged presentation of antigen and the generation of high-affinity tumor-reactive cytotoxic T lymphocytes. Mol Ther 9:757
Boczkowski D, Nair SK, Nam JH, Lyerly HK, Gilboa E (2000) Induction of tumor immunity and cytotoxic T lymphocyte responses using dendritic cells transfected with messenger RNA amplified from tumor cells. Cancer Res 60:1028
Heiser A, Maurice MA, Yancey DR, Wu NZ, Dahm P, Pruitt SK, Boczkowski D, Nair SK, Ballo MS, Gilboa E, Vieweg J (2001) Induction of polyclonal prostate cancer-specific CTL using dendritic cells transfected with amplified tumor RNA. J Immunol 166:2953
Milazzo C, Reichardt VL, Muller MR, Grunebach F, Brossart P (2003) Induction of myeloma-specific cytotoxic T cells using dendritic cells transfected with tumor-derived RNA. Blood 101:977
Nencioni A, Muller MR, Grunebach F, Garuti A, Mingari MC, Patrone F, Ballestrero A, Brossart P (2003) Dendritic cells transfected with tumor RNA for the induction of antitumor CTL in colorectal cancer. Cancer Gene Ther 10:209
Muller MR, Tsakou G, Grunebach F, Schmidt SM, Brossart P (2004) Induction of chronic lymphocytic leukemia (CLL)-specific CD4-mediated and CD8-mediated T-cell responses using RNA-transfected dendritic cells. Blood 103:1763
Heiser A, Coleman D, Dannull J, Yancey D, Maurice MA, Lallas CD, Dahm P, Niedzwiecki D, Gilboa E, Vieweg J (2002) Autologous dendritic cells transfected with prostate-specific antigen RNA stimulate CTL responses against metastatic prostate tumors. J Clin Invest 109:409
Su Z, Dannull J, Heiser A, Yancey D, Pruitt S, Madden J, Coleman D, Niedzwiecki D, Gilboa E, Vieweg J (2003) Immunological and linical responses in metastatic renal cancer patients vaccinated with tumor RNA-transfected dendritic cells. Cancer Res 63:2127
Nair SK, Morse M, Boczkowski D, Cumming RI, Vasovic L, Gilboa E, Lyerly HK (2002) Induction of tumor-specific cytotoxic T lymphocytes in cancer patients by autologous tumor RNA-transfected dendritic cells. Ann Surg 235:540
Kobayashi T, Yamanaka R, Homma J, Tsuchiya N, Yajima N, Yoshida S, Tanaka R (2003) Tumor mRNA-loaded dendritic cells elicit tumor-specific CD8(+) cytotoxic T cells in patients with malignant glioma. Cancer Immunol Immunother 52:632
Hemmi H, Takeuchi O, Kawai T, Kaisho T, Sato S, Sanjo H, Matsumoto M, Hoshino K, Wagner H, Takeda K, Akira S (2000) A Toll-like receptor recognizes bacterial DNA. Nature 408:740
Heil F, Hemmi H, Hochrein H, Ampenberger F, Kirschning C, Akira S, Lipford G, Wagner H, Bauer S (2004) Species-specific recognition of single-stranded RNA via toll-like receptor 7 and 8. Science 303:1526
Diebold SS, Kaisho T, Hemmi H, Akira S, Reis e Sousa (2004) Innate antiviral responses by means of TLR7-mediated recognition of single-stranded RNA. Science 303:1529
Steitz J, Bruck J, Lenz J, Buchs S, Tuting T (2005) Peripheral CD8+ T cell tolerance against melanocytic in the skin is regulated in two steps by CD4+ T cells and local inflammation: implications for the pathophysiology of vitiligo. J Invest Dermatol 124:144–155
Acknowledgements
We thank Stefanie Büchs and Petra Speuser for excellent technical assistance. This work was supported by the ’‘Deutsche Forschungsgemeinschaft” (For 367/2 to TT and SFB432/A1 to TW) and by the “Deutsche Krebshilfe” (70–2427-Hul to TW and 10–1870-Tü2 to TT).
Author information
Authors and Affiliations
Corresponding author
Additional information
Julia Steitz and Cedrik M. Britten contributed equally to this work.
Rights and permissions
About this article
Cite this article
Steitz, J., Britten, C.M., Wölfel, T. et al. Effective induction of anti-melanoma immunity following genetic vaccination with synthetic mRNA coding for the fusion protein EGFP.TRP2. Cancer Immunol Immunother 55, 246–253 (2006). https://doi.org/10.1007/s00262-005-0042-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-005-0042-5