Abstract
The effects of ouabain (OUA) and lipopolysaccharide (LPS) in vivo on hippocampal membranes (RHM) of Wistar male rats aged 3 months were analyzed. After intraperitoneal (i.p.) injection of OUA only, LPS only, OUA plus LPS, or saline, the content of proteins, phospholipids, cholesterol and gangliosides from RHM was analyzed. The total protein and cholesterol contents of RHM were not significantly affected by OUA or LPS for the experimentally paired groups. In contrast, total phospholipids and gangliosides were strongly modulated by either OUA or LPS treatments. LPS reduced the total phospholipids (roughly 23 %) and increased the total gangliosides (approximately 40 %). OUA alone increased the total phospholipids (around 23 %) and also the total gangliosides (nearly 34 %). OUA pretreatment compensated the LPS-induced changes, preserving the total phospholipids and gangliosides around the same levels of the control. Thus, an acute treatment with OUA not only modulated the composition of hippocampal membranes from 3-month-old rats, but also was apparently able to counteract membrane alterations resulting from LPS-induced neuroinflammation. This study demonstrates for the first time that the OUA capacity modulates the lipid composition of hippocampal plasma membranes from rats with LPS-induced neuroinflammation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Neuroinflammation can be summarized as an inflammatory response developed on the central nervous system (CNS) as a consequence of tissue injury, disease, trauma, or toxic action. This leads to activation of glial cells (astrocytes and microglia) and the concomitant expression of helper proinflammatory cytokines and chemokines such as Il-1alpha, Il6, Ccl2, and TNF-α (Morales et al. 2014). These proinflammatory molecules contribute to magnify the lesion (Akiyama et al. 2000). Microglial activation is a relevant pathological event found in several neural disorders such as Parkinson, Alzheimer, and ischemia, among others (Block et al. 2007).
LPS are found as major components on the outer membrane of Gram-negative bacteria and are able, by their own, to elicit strong immune responses in animals and initiate severe inflammation. Therefore, LPS is being used as a model induce of the systemic immunity and the cellular and molecular events which lead to either acute or chronic inflammation (Valero et al. 2014).
LPS molecules consist of three parts: lipid A, a glycolipid responsible for the endotoxic activity, covalently bound to a heteropolysaccharide which by its turn presents two moieties, a variable core polysaccharide and the highly variable O-antigen (or O-polysaccharide). The lipid portion is considered to be the main responsible for the major antigenic action of LPS (Raetz and Whitfield 2002).
LPS shows strong interactions with lipid microenvironments rich in phosphatidylcholine (PC), sphingomyelin (SM), and cholesterol (Ciesielski et al. 2012). Thus, the presence of LPS in such a microenvironment has modulatory effects on the membranes (Ciesielski et al. 2013).
Some neuroprotective molecules with capacity to mitigate LPS-induced neuroinflammation are reported in the literature, such as guanine derivatives, vitamin D, glycyrrhizin, and honey flavonoids, to mention a few (Brewer et al. 2001; Candiracci et al. 2012; Schmidt et al. 2007; Song et al. 2013).
OUA is a cardiotonic steroid (cardiac glycoside) found in the ripe seeds of the African plants Strophanthus gratus and the bark of Acokanthera ouabaio, and has been used in low concentrations as a molecule eliciting a neuroprotective effect (Blaustein 1993; Golden and Martin, 2006; Sibarov et al. 2012).
The plasma membrane is a lipid bilayer that, in response to cell or tissue needs, may present variations in the physical–chemical properties of its components (Jacobson et al. 2007). Membrane lipids found in the CNS cells are represented mainly by gangliosides, phospholipids and cholesterol (Krafft et al. 2005). As in other cell types, lipids in brain cells also possess roles in cell signaling as second messengers, like the phosphoinositides, being relevant for important processes such as neurotransmission, cell proliferation and neuroprotection (Osborne et al. 2001).
The aim of the present study was to characterize the effects of ouabain administration in the lipid composition of hippocampal membrane fractions of rats at the age of 3-months, and relate these actions to a possible neuroprotective effect against LPS-mediated neuroinflammation.
Materials and Methods
Animal Handling and Procedures
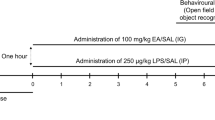
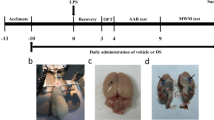
Three-month-old Wistar male rats were kept on a room with controlled temperature (21 ± 2 °C) and 12 h light/dark cycle, with food and water access ad libitum. The experimental animals were euthanized by decapitation. All the experimental protocols followed the rules and ethical principles of the Brazilian Society for Laboratory Animal Sciences (SBCAL) and were approved by the Commission of Ethics in Animal Experimentation (CEEA, protocol nr. 77) from the University of São Paulo (USP), São Paulo, Brazil. Each experimental group was composed of 6 animals that received intraperitoneal (i.p.) administration of either (1) pyrogen-free, sterile saline (CTR), (2) ouabain (OUA) (1.8 μg kg−1) followed 20 min later by the injection of either saline or (3) LPS (200 μg kg−1) (OUA + LPS), and (4) LPS in saline. The animals were decapitated 2 h after the second injection (sufficient to evoke maximal TNF increase in glial cells) and the brains were rapidly removed and kept in ice-cold PBS. Hippocampi were dissected over an ice-cold dish, and then frozen by immersion in liquid nitrogen and stored at −80 °C for later processing. All the reagents used were analytical grade or better. LPS was from Sigma (E. c oli 0111:B4, code L2630).
Rat Hippocampal Membrane (RHM) Preparation
Frozen tissue samples were thawed and homogenized in 5 volumes of ice-cold lysis buffer (10 mM HEPES, pH 7.9, 1.5 mM MgCl2, 10 mM KCl, 0.5 mM PMSF, 2.5 μg mL−1 antipain and leupeptin, 30 mM NaF, 20 mM sodium pyrophosphate (Na4P2O7), 5 mM BG-P, 0.1 mM EDTA in milli-Q water). After homogenization, samples were centrifuged at 12,000×g for 30 s at 4 °C. The resulting supernatant was centrifuged again at 12,000×g for 20 min at 4 °C, and the resulting pellet was suspended in NOS homogenization buffer (320 mM sucrose, 20 mM HEPES, 1 mM EDTA). Each sample resulted in 120 μL of RHM suspension.
Protein Determination
Total RHM protein was determined by the Hartree method using BSA as standard (Hartree 1972).
Extraction of RHM Lipid Fractions
Hundred microlitres samples of the RHM fractions were mixed with 20 volumes of chloroform:methanol (2:1 v/v) in 15 mL Falcon-type tubes and after 1 h at rest were centrifuged at 2100 rpm in a non-refrigerated clinical centrifuge for 20 min. Next, 1/5 volume of distilled water was added and after thorough mixing the samples were settled for 1 h and again centrifuged as above. This mixture was reserved for 24 h for the separation of the aqueous phase on the top (containing mainly gangliosides) and the organic phase on the bottom (containing mainly phospholipids and cholesterol) (Folch et al. 1957). The top and bottom phases were then separately retrieved, dried on a rotary evaporator, dissolved in chloroform:methanol (2:1 v/v) and stored at −20 °C.
Determination of RHM Total Phospholipids
Phospholipids were determined from the amount of phosphate released by acid hydrolysis as described else where amounts of Pi (5–80 nmoles) and samples of commercial dioleoylphosphatidylcholine (DOPC) were used to assess lipid digestion and also as standards (Chen et al. 1956). Hippocampal membrane samples without acid treatment resulted in negligible readings.
Determination of RHM Total Cholesterol
Cholesterol was quantified according to Higgins (1987). Determinations were made in triplicate and the results were extrapolated from a standard curve derived from a 1 mg mL−1 stock cholesterol solution, by diluting samples between 0 and 400 μL to a final volume of 3.5 mL.
Determination of RHM total gangliosides
The total gangliosides in RHM were measured according to Svennerholm (1957). Determinations were made as triplicates, and sialic acid (1 mg mL−1 standard solution) was used to make a standard curve ranging from 0 to 0.5 μM.
Statistical Analysis
All the results are expressed as mean ± S.D. The results were tested by one-way ANOVA followed by Tukey, and considered to be significant for p ≤ 0.05. Graphs and analysis were generated with the GraphPad Prism 5 software.
Results
Determination of Protein Concentration of RHM
Initially the total protein concentration of the RHM from all the experimental groups (CTR, OUA, LPS, and OUA + LPS) was determined. The protein contents of RHM from the treated groups were not found to be significantly different from the control within the duration of the experiment, as shown in Table 1.
Cholesterol Content of RHM
The total cholesterol content of RHM was determined from the organic phase extract of each experimental group. When the effect of either treatment (OUA/LPS/OUA + LPS) on the cholesterol content was compared, no significant difference was observed for any of the treatments (Fig. 1).
Total cholesterol of RHM from animals treated with LPS and/or ouabain. The total cholesterol of RHM from the 3-month submitted to treatment with LPS and/or ouabain was measured. Data are presented as mean ± SD for groups of 6 (3-month) animals. All data were subjected to 1-way ANOVA followed by Tukey post hoc test
Total Phospholipids of RHM
The total phospholipids were also quantified from the organic phase of the lipid extraction of RHM, by determining the amount of phosphate released by acid hydrolysis of the lipids. A significant decrease, of nearly 23 % of the phospholipid content present in RHM, was observed for the 3-month aged, LPS-treated group, when compared with the CTR group. In contrast, for this same 3-month aged group the treatment with ouabain induced a significant increase (also roughly 23 %) on the phospholipid content of RHM relative to control. Notably, the OUA pretreatment resulted in a compensatory effect, and phospholipid levels on this 3-month aged group were found to be similar to the CTR (Fig. 2).
Total phospholipids of RHM from animals treated with LPS and/or ouabain. The total phospholipids of RHM from the 3-month submitted to treatment with LPS and/or ouabain was measured. Data are presented as mean ± SD for groups of animals. All data were subjected to 1-way ANOVA followed by Tukey post hoc test. *Different from control, p < 0.05; ##different from LPS, p < 0.01
Total Gangliosides of the RHM Fractions
From the aqueous phase of the RHM lipid extraction, we were able to determine the total amount of gangliosides on the samples from the different treated groups. The group treated with LPS showed a significant increase on the total gangliosides (101.80 ± 11.62 pmol) when compared with the CTR group (75.59 ± 2.89 pmol). A significant increase was also observed for the group treated with OUA (106.70 ± 0.85 pmol). Conversely, the supply of OUA pretreatment did not result in any significant difference (74.69 ± 0.59 pmol) from the CTR. Therefore, although the independent addition of either OUA or LPS resulted in similarly increased RHM total ganglioside levels, the concomitant addition of these molecules gave ganglioside levels close to the CTR (Fig. 3).
Total gangliosides of RHM from animals treated with LPS and/or ouabain. The total gangliosides of RHM for the 3-month submitted to treatment with LPS and/or ouabain was measured. Data are presented as mean ± SD for groups of 6 (3-month) animals. All data were subjected to 1-way ANOVA followed by Tukey post hoc test. *Different from control, p < 0.05; **different from control, p < 0.01; #different from LPS, p < 0.05
Discussion
Cholesterol is a paramount component of biological membranes and, in the CNS, its concentration is tightly regulated and depends on local synthesis and membrane export mechanisms, since this molecule cannot be taken up from blood circulation. In addition to its known roles in the regulation of membrane fluidity, plasticity, and release of neurotransmitters, cholesterol metabolism in the CNS is directly involved in the onset and development of several structural and/or functional pathologies, like Smith-Lemli-Opitz syndrome, Niemann-Pick type C disease, Huntington disease, and Alzheimer disease (Cho et al. 2007; Orth and Bellosta 2012). Therefore, any compound capable of reversing, or impeding, deleterious membrane lipid changes induced by injury or inflammation would be of interest for the treatment of diverse pathologies, mostly if the use of that specific compound is already approved by regulatory agencies, as is the case for OUA.
A recent work from Oselkin showed that small amounts of OUA could protect hippocampal slice cultures from ischemia within a 2 h period of trauma. In addition, OUA was shown to increase NFκB in cultured cerebellar cells in a short-term response which peaks approximately 2 h after OUA administration (de Sá Lima et al. 2013; Oselkin et al. 2010). Thus, a possible neuroprotective effect of OUA within 2 h of trauma is already reported.
Changes in the total cholesterol content could result either from altered rates of synthesis of the molecule as well as to fluctuations of the activity of the 24-hydroxylase (CYP46) and the membrane carriers responsible for its metabolization and removal from neuronal cells. Previous studies reported that i.p. LPS administration did not alter the amounts of cholesterol in rat brains (Kheir-Eldin et al. 2001). We could not find any report concerning any effect of OUA on the cholesterol content of RHM, although OUA and digoxin were already described to increase the synthesis of cholesterol in human liver-derived HepG2 cells when delivered at concentrations ranging from 1 nM to 1 mM. Those authors showed an upregulation of HMG-CoA-reductase (HMGCR) activity and suggested that cardiac glycosides could be potential modulators of cholesterol synthesis due to the steroidal nature of their core structure (Campia et al. 2009). A previous work by Kurup and Kurup (2003) also showed that an increase of the endogenous digoxin in patients with severe bowel inflammation resulted in an increase of HMGCR activity, which by its turn led to an increased synthesis of cholesterol.
Our results show that roughly no alterations of the total cholesterol content of RHM were elicited within the 2-h experimental period after the administration of either LPS, OUA, or OUA + LPS (Fig. 1). Although a redistribution of cholesterol in the cell membrane domains should not be discarded, and in spite of the protective effects of OUA mentioned above, in the short term neither the LPS neuroinflammatory injury and cell response nor the glycoside appear to modulate cholesterol content in rat hippocampal membranes.
Our results showed that within the 2 h of administration OUA alone was able to increase the total phospholipids from RHM in 3-month old rats. Conversely, LPS alone induced a drop on the total phospholipids of RHM from the age-paired experimental group. Noticeably, OUA was able to counteract the effect elicited by the LPS treatment when the OUA pretreatment was done, maintaining the total phospholipids in levels equivalent to those of the control group (Fig. 2). This is highly suggestive of an OUA-stimulated mechanism that, besides resulting in an increase in RHM phospholipids by itself, ended up counteracting the decrease of total phospholipids in RHM from 3-month-old rats caused by i.p. LPS administration. Possibly this alteration is caused by a shift in the balance of synthesis and degradation of specific phospholipids. This could modulate the lipid microenvironment and thus shift it in response to the need of preserving cell plasma membrane integrity and protein function in order to perform tasks such as defense, transport, and cell signaling, among others.
An explanation for the decrease of almost 23 % in the phospholipids from the LPS group (Fig. 2) could be that when LPS is recognized by the TLR4 receptor, this would lead to the production of TNF and IL-1, as well as to the transcription of ROS-generating enzymes (Wang et al. 2004). The production of ROS by its turn would result in peroxidation of different phospholipids, which could thus lead to the decline of the total phospholipid content (Catalá 2009). Reports elsewhere showed that LPS administration (2–10 mg/kg, over a 3–6 h period) induced an acute increase of TNF-α and of lipid peroxidation products, paralleled by glutathione depletion in lung, kidney, and liver, in animal models of maternal infection associated to inflammation. An increment of TNF-α was indeed also observed for our 3-month-old groups (data not shown).
In line with this possibility, it was reported that lipid peroxidation products could increase by 80 % in kidneys from rats treated with LPS (Awad et al. 2011; Mohamadin et al. 2011; Piechota et al. 2011; Zhang et al. 2000). For brain tissue, administration of LPS (2 mg/kg, 2 h earlier) increased the production of free radicals and malondialdehyde, and lead to depletion of GSH and ATP stocks. In parallel, 3 h after LPS inoculation the expression of INOS, COX-2, and TNF-α, mRNAs were significantly increased (Czapski et al. 2010). In other studies, LPS also increased the expression of both iNOS and INF-α, and the production of diacylglycerol and phosphatidic acid. Increased activities of PLC-PC, PLDPC, and PLA2 were also observed (Akundi et al. 2005; Sakata et al. 2007). PLA2 presents selectivity for oxidized phospholipids, removing them from the membranes (Sevanian and Kim 1985; Soliman et al. 2013). In neuroinflammation, the increased activity of PLA2 could induce the loss of phospholipids and thus result in cell death (Sevanian et al. 1988).
LPS reportedly activates the release of cytokines, which in turn will activate cell sphingomyelinase, and this enzyme will thus lead to a decrease of the membrane sphingomyelin content (Rosenberger et al. 2004). In addition, the reported macrophage LPS-induced cell responses and activation through TLR4, CD14, and MAPK are dependent on the recruitment of a specific PLC that would additionally contribute to deplete membrane phospholipids (Chiang et al. 2012; Cuschieri et al. 2006; Monick et al. 1999).
Similarly to what was observed for the total phospholipids, the findings for the total gangliosides show a capability of OUA alone to induce an increase of the total amount of this lipid class for the 3-month-old rats (Fig. 3). On the other side, LPS injection in this case also induced a similar increasing in the total ganglioside amounts of RHM. Nevertheless, it was also observed that, for this age group, OUA injection prior to LPS somehow resulted in the preservation of the gangliosides in values similar to those of the control, avoiding the shift observed with either OUA or LPS administration alone. Although somewhat paradoxical, this result is not unfeasible, since the paths involved on these conflicting effects and the ganglioside profile for each treatment remains to be determined.
For example, a shift in the proportions of the different gangliosides, with a specific increase of the GM3 and GD3 types, was already described in fibroblasts for inflammatory processes induced by LPS (Valaperta et al. 2006).
Gangliosides are sialic acid-containing oligoglycosylceramides found in the outer leaflet of plasma membranes. They are known to be essential for cellular recognition, interaction, and adhesion. They play crucial roles in signal transduction, and are particularly abundant in the CNS, where their expression is developmentally regulated. Their composition varies with the differentiation stage and also with the age of a cell. Something like 200 gangliosides that differ on their carbohydrate moieties are known only in vertebrates (Yu et al. 2008). Gangliosides are mostly found associated with cholesterol and sphingolipids in lipid rafts which are well organized membrane domains enriched in proteins and receptors further known to play important roles in signaling, binding, internalization, and neurotransmission. GM1, GD1a, and GD1b contribute with 80–90 % of the total gangliosides in adult mammal brains (Hancock 2006; Simons and Gerl 2010; Wolf et al. 1998).
General and concluding remarks—several reports show that as age increases there is a concurrent increase in the biosynthesis of ceramides, which in turn are key intermediates in the biosynthesis of glycolipids, in different regions of the human brain and also in cultured neuron cells (Cutler et al. 2004; Prinetti et al. 2001). Ceramides are well recognized as regulators of cell proliferation, differentiation, and survival (Billis et al. 1998). Moreover, during aging the existence, structure and function of lipid rafts are modulated by the ceramide portion. The ganglioside proportion in rafts from aging human or rat brain, and of cultured neuronal cells, is increased as well (Sonnino and Chigorno 2000). However, a reduction of the ganglioside-bound sialic acid with aging due to an increase in the activity of sialidase, that could thus shift composition to a more polar pattern due to an increase in the relative concentration of the more polar fractions GQ1b, GT1b, and GD1b and a decrease in GD1a and GM1, was reported. These shifts appear to be region dependent, with human hippocampus presenting only a slight decrease in GD1a (Kracun et al. 1992; Segler-Stahl et al. 1983). Whatever region or lipids are selectively affected, there is ever growing evidence that the lipids of neuronal membranes are affected in response to aging or inflammation as a need for cell adaptation for survival and preservation of function, but these lipid shifts are also involved in the onset of grave pathologies such as Alzheimer and Parkinson (Kristina Mlinac 2010).
Thus, our results show that OUA alone has the potential of altering/modulating the membrane lipid composition of rat hippocampal membranes (RHM) of 3-month-old rats in the short term (2 h), since the ganglioside altered the content of total phospholipids and gangliosides. Furthermore, OUA had the capability of counteracting the lipid changes elicited by LPS-induced neuroinflammation, restoring the levels of phospholipids and gangliosides of RHM from 3-month-old rats. Regarding a counteraction of the LPS-induced inflammation by OUA, some previous reports suggested a promising potential of the cardiac glycoside against diverse inflammation models, since its administration resulted in reduced migration of inflammatory cells, less expression of adhesion molecules, and impaired signaling by chemokines and cytokines (de Vasconcelos et al. 2011; Forshammar et al. 2011; Hillard 2008).
OUA can also act as a neuromodulator on the CNS as it is described to increase the activity of sympathetic neurons in rats (de Wardener 2001). In addition, depending of the concentration tested, this glycoside can either stimulate or inhibit apoptosis in CNS cells. This effect was observed in studies on the regeneration of retinal ganglion cells in vitro, where OUA at micromolar concentrations triggered cell apoptosis, whereas nanomolar concentrations enhanced cell survival (de Rezende Corrêa et al. 2005).
These observations raise the status of OUA to a possible target drug able to counteract the lipid changes and membrane damage induced by aging or inflammation. Additionally, these observations also could raise the need to study whether there is a correlation between the severity of inflammatory responses, neuroinflammation, and even the onset and progress of Alzheimer disease, with the individual levels of endogenous cardiac glycosides.
References
Akiyama H, Barger S, Barnum S, Bradt B, Bauer J, Cole GM, Cooper NR, Eikelenboom P, Emmerling M, Fiebich BL, Finch CE, Frautschy S, Griffin WS, Hampel H, Hull M, Landreth G, Lue L, Mrak R, Mackenzie IR, McGeer PL, O’Banion MK, Pachter J, Pasinetti G, Plata-Salaman C, Rogers J, Rydel R, Shen Y, Streit W, Strohmeyer R, Tooyoma I, Van Muiswinkel FL, Veerhuis R, Walker D, Webster S, Wegrzyniak B, Wenk G, Wyss-Coray T (2000) Inflammation and Alzheimer’s disease. Neurobiol Aging 21:383–421
Akundi RS, Candelario-Jalil E, Hess S, Hüll M, Lieb K, Gebicke-Haerter PJ, Fiebich BL (2005) Signal transduction pathways regulating cyclooxygenase-2 in lipopolysaccharide-activated primary rat microglia. Glia 51:199–208
Awad N, Khatib N, Ginsberg Y, Weiner Z, Maravi N, Thaler I, Ross MG, Itsokovitz-Eldor J, Beloosesky R (2011) N-acetyl-cysteine (NAC) attenuates LPS-induced maternal and amniotic fluid oxidative stress and inflammatory responses in the preterm gestation. Am J Obstet Gynecol 204:450.e15-20
Billis W, Fuks Z, Kolesnick R (1998) Signaling in and regulation of ionizing radiation-induced apoptosis in endothelial cells. Recent Prog Horm Res 53:85–92 discussion 93
Blaustein MP (1993) Physiological effects of endogenous ouabain: control of intracellular Ca2+ stores and cell responsiveness. Am J Physiol 264:C1367–C1387
Block ML, Zecca L, Hong JS (2007) Microglia-mediated neurotoxicity: uncovering the molecular mechanisms. Nat Rev Neurosci 8:57–69
Brewer LD, Thibault V, Chen KC, Langub MC, Landfield PW, Porter NM (2001) Vitamin D hormone confers neuroprotection in parallel with downregulation of L-type calcium channel expression in hippocampal neurons. J Neurosci 21:98–108
Campia I, Gazzano E, Pescarmona G, Ghigo D, Bosia A, Riganti C (2009) Digoxin and ouabain increase the synthesis of cholesterol in human liver cells. Cell Mol Life Sci 66:1580–1594
Candiracci M, Piatti E, Dominguez-Barragán M, García-Antrás D, Morgado B, Ruano D, Gutiérrez JF, Parrado J, Castaño A (2012) Anti-inflammatory activity of a honey flavonoid extract on lipopolysaccharide-activated N13 microglial cells. J Agric Food Chem 60:12304–12311
Catalá A (2009) Lipid peroxidation of membrane phospholipids generates hydroxy-alkenals and oxidized phospholipids active in physiological and/or pathological conditions. Chem Phys Lipids 157:1–11
Chen PSJ, Toribara TY, Warner H (1956) Microdetermination of phosphorus. Anal Chem 28:1756–1758
Chiang CY, Veckman V, Limmer K, David M (2012) Phospholipase Cγ-2 and intracellular calcium are required for lipopolysaccharide-induced Toll-like receptor 4 (TLR4) endocytosis and interferon regulatory factor 3 (IRF3) activation. J Biol Chem 287:3704–3709
Cho WJ, Jeremic A, Jin H, Ren G, Jena BP (2007) Neuronal fusion pore assembly requires membrane cholesterol. Cell Biol Int 31:1301–1308
Ciesielski F, Davis B, Rittig M, Bonev BB, O’Shea P (2012) Receptor-independent interaction of bacterial lipopolysaccharide with lipid and lymphocyte membranes; the role of cholesterol. PLoS One 7:e38677
Ciesielski F, Griffin DC, Rittig M, Moriyón I, Bonev BB (2013) Interactions of lipopolysaccharide with lipid membranes, raft models—a solid state NMR study. Biochim Biophys Acta 1828:1731–1742
Cuschieri J, Billgren J, Maier RV (2006) Phosphatidylcholine-specific phospholipase C (PC-PLC) is required for LPS-mediated macrophage activation through CD14. J Leukoc Biol 80:407–414
Cutler RG, Kelly J, Storie K, Pedersen WA, Tammara A, Hatanpaa K, Troncoso JC, Mattson MP (2004) Involvement of oxidative stress-induced abnormalities in ceramide and cholesterol metabolism in brain aging and Alzheimer’s disease. Proc Natl Acad Sci USA 101:2070–2075
Czapski GA, Gajkowska B, Strosznajder JB (2010) Systemic administration of lipopolysaccharide induces molecular and morphological alterations in the hippocampus. Brain Res 1356:85–94
de Rezende Corrêa G, Araujo dos Santos A, Frederico Leite Fontes C, Giestal de Araujo E (2005) Ouabain induces an increase of retinal ganglion cell survival in vitro: the involvement of protein kinase C. Brain Res 1049:89–94
de Sá Lima L, Kawamoto EM, Munhoz CD, Kinoshita PF, Orellana AM, Curi R, Rossoni LV, Avellar MC, Scavone C (2013) Ouabain activates NFκB through an NMDA signaling pathway in cultured cerebellar cells. Neuropharmacology 73:327–336
de Vasconcelos DI, Leite JA, Carneiro LT, Piuvezam MR, de Lima MR, de Morais LC, Rumjanek VM, Rodrigues-Mascarenhas S (2011) Anti-inflammatory and antinociceptive activity of ouabain in mice. Mediators Inflamm 2011:912925
de Wardener HE (2001) The hypothalamus and hypertension. Physiol Rev 81:1599–1658
Folch J, Lees M, Sloane Stanley GH (1957) A simple method for the isolation and purification of total lipides from animal tissues. J Biol Chem 226:497–509
Forshammar J, Block L, Lundborg C, Biber B, Hansson E (2011) Naloxone and ouabain in ultralow concentrations restore Na+/K+-ATPase and cytoskeleton in lipopolysaccharide-treated astrocytes. J Biol Chem 286:31586–31597
Higgins H (1987) Biological membranes. Pratical approach series. IRL Press, Oxford
Golden WC, Martin LJ (2006) Low-dose ouabain protects against excitotoxic apoptosis and up-regulates nuclear Bcl-2 in vivo. Neuroscience 137:133–144
Hancock JF (2006) Lipid rafts: contentious only from simplistic standpoints. Nat Rev Mol Cell Biol 7:456–462
Hartree EF (1972) Determination of protein: a modification of the Lowry method that gives a linear photometric response. Anal Biochem 48:422–427
Hillard CJ (2008) Role of cannabinoids and endocannabinoids in cerebral ischemia. Curr Pharm Des 14:2347–2361
Jacobson K, Mouritsen OG, Anderson RG (2007) Lipid rafts: at a crossroad between cell biology and physics. Nat Cell Biol 9:7–14
Kheir-Eldin AA, Motawi TK, Gad MZ, Abd-ElGawad HM (2001) Protective effect of vitamin E, beta-carotene and N-acetylcysteine from the brain oxidative stress induced in rats by lipopolysaccharide. Int J Biochem Cell Biol 33:475–482
Kracun I, Rosner H, Drnovsek V, Vukelic Z, Cosovic C, Trbojevic-Cepe M, Kubat M (1992) Gangliosides in the human brain development and aging. Neurochem Int 20:421–431
Krafft C, Neudert L, Simat T, Salzer R (2005) Near infrared Raman spectra of human brain lipids. Spectrochim Acta A 61:1529–1535
Kristina Mlinac SKB (2010) Role of gangliosides in brain aging and neurodegeneration. Transl Neurosci 1:300–307
Kurup RK, Kurup PA (2003) Hypothalamic digoxin, hemispheric chemical dominance, and inflammatory bowel disease. Int J Neurosci 113:1221–1240
Mohamadin AM, Elberry AA, Elkablawy MA, Gawad HS, Al-Abbasi FA (2011) Montelukast, a leukotriene receptor antagonist abrogates lipopolysaccharide-induced toxicity and oxidative stress in rat liver. Pathophysiology 18:235–242
Monick MM, Carter AB, Gudmundsson G, Mallampalli R, Powers LS, Hunninghake GW (1999) A phosphatidylcholine-specific phospholipase C regulates activation of p42/44 mitogen-activated protein kinases in lipopolysaccharide-stimulated human alveolar macrophages. J Immunol 162:3005–3012
Morales I, Guzmán-Martínez L, Cerda-Troncoso C, Farías GA, Maccioni RB (2014) Neuroinflammation in the pathogenesis of Alzheimer’s disease A rational framework for the search of novel therapeutic approaches. Front Cell Neurosci 8:112
Orth M, Bellosta S (2012) Cholesterol: its regulation and role in central nervous system disorders. Cholesterol 2012:292598
Osborne SL, Meunier FA, Schiavo G (2001) Phosphoinositides as key regulators of synaptic function. Neuron 32:9–12
Oselkin M, Tian D, Bergold PJ (2010) Low-dose cardiotonic steroids increase sodium-potassium ATPase activity that protects hippocampal slice cultures from experimental ischemia. Neurosci Lett 473:67–71
Piechota A, Polańczyk A, Goraca A (2011) Protective effects of endothelin-A receptor antagonist BQ123 against LPS-induced oxidative stress in lungs. Pharmacol Rep 63:494–500
Prinetti A, Chigorno V, Prioni S, Loberto N, Marano N, Tettamanti G, Sonnino S (2001) Changes in the lipid turnover, composition, and organization, as sphingolipid-enriched membrane domains, in rat cerebellar granule cells developing in vitro. J Biol Chem 276:21136–21145
Raetz CR, Whitfield C (2002) Lipopolysaccharide endotoxins. Annu Rev Biochem 71:635–700
Rosenberger TA, Villacreses NE, Hovda JT, Bosetti F, Weerasinghe G, Wine RN, Harry GJ, Rapoport SI (2004) Rat brain arachidonic acid metabolism is increased by a 6-day intracerebral ventricular infusion of bacterial lipopolysaccharide. J Neurochem 88:1168–1178
Sakata A, Ochiai T, Shimeno H, Hikishima S, Yokomatsu T, Shibuya S, Toda A, Eyanagi R, Soeda S (2007) Acid sphingomyelinase inhibition suppresses lipopolysaccharide-mediated release of inflammatory cytokines from macrophages and protects against disease pathology in dextran sulphate sodium-induced colitis in mice. Immunology 122:54–64
Schmidt AP, Lara DR, Souza DO (2007) Proposal of a guanine-based purinergic system in the mammalian central nervous system. Pharmacol Ther 116:401–416
Segler-Stahl K, Webster JC, Brunngraber EG (1983) Changes in the concentration and composition of human brain gangliosides with aging. Gerontology 29:161–168
Sevanian A, Kim E (1985) Phospholipase A2 dependent release of fatty acids from peroxidized membranes. J Free Radic Biol Med 1:263–271
Sevanian A, Wratten ML, McLeod LL, Kim E (1988) Lipid peroxidation and phospholipase A2 activity in liposomes composed of unsaturated phospholipids: a structural basis for enzyme activation. Biochim Biophys Acta 961:316–327
Sibarov DA, Bolshakov AE, Abushik PA, Krivoi II, Antonov SM (2012) Na+, K+-ATPase functionally interacts with the plasma membrane Na+, Ca2+ exchanger to prevent Ca2+ overload and neuronal apoptosis in excitotoxic stress. J Pharmacol Exp Ther 343:596–607
Simons K, Gerl MJ (2010) Revitalizing membrane rafts: new tools and insights. Nat Rev Mol Cell Biol 11:688–699
Soliman ML, Ohm JE, Rosenberger TA (2013) Acetate reduces PGE2 release and modulates phospholipase and cyclooxygenase levels in neuroglia stimulated with lipopolysaccharide. Lipids 48:651–662
Song JH, Lee JW, Shim B, Lee CY, Choi S, Kang C, Sohn NW, Shin JW (2013) Glycyrrhizin alleviates neuroinflammation and memory deficit induced by systemic lipopolysaccharide treatment in mice. Molecules 18:15788–15803
Sonnino S, Chigorno V (2000) Ganglioside molecular species containing C18- and C20-sphingosine in mammalian nervous tissues and neuronal cell cultures. Biochim Biophys Acta 1469:63–77
Svennerholm L (1957) Quantitative estimation of sialic acids. II. A colorimetric resorcinol-hydrochloric acid method. Biochim Biophys Acta 24:604–611
Valaperta R, Chigorno V, Basso L, Prinetti A, Bresciani R, Preti A, Miyagi T, Sonnino S (2006) Plasma membrane production of ceramide from ganglioside GM3 in human fibroblasts. FASEB J 20:1227–1229
Valero J, Mastrella G, Neiva I, Sánchez S, Malva JO (2014) Long-term effects of an acute and systemic administration of LPS on adult neurogenesis and spatial memory. Front Neurosci 8:83
Wang T, Qin L, Liu B, Liu Y, Wilson B, Eling TE, Langenbach R, Taniura S, Hong JS (2004) Role of reactive oxygen species in LPS-induced production of prostaglandin E2 in microglia. J Neurochem 88:939–947
Wolf AA, Jobling MG, Wimer-Mackin S, Ferguson-Maltzman M, Madara JL, Holmes RK, Lencer WI (1998) Ganglioside structure dictates signal transduction by cholera toxin and association with caveolae-like membrane domains in polarized epithelia. J Cell Biol 141:917–927
Yu RK, Ariga T, Yanagisawa M, Zeng G (2008) Gangliosides in the nervous system: biosynthesis and degradation. Glycoscience. Springer, Berlin, pp 1671–1695
Zhang C, Walker LM, Mayeux PR (2000) Role of nitric oxide in lipopolysaccharide-induced oxidant stress in the rat kidney. Biochem Pharmacol 59:203–209
Acknowledgments
This research was financially supported by the FAPEMIG and FAPESP.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Garcia, I.J.P., Kinoshita, P.F., Scavone, C. et al. Ouabain Modulates the Lipid Composition of Hippocampal Plasma Membranes from Rats with LPS-induced Neuroinflammation. J Membrane Biol 248, 1191–1198 (2015). https://doi.org/10.1007/s00232-015-9840-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00232-015-9840-7