Abstract
Inflammation and the related acidity in peri-articular structures may be involved in pain generation and hyperalgesia in knee osteoarthritis. This study investigated pain and associated hyperalgesia provoked by infusion of acidic saline into the infrapatellar fat pad. Twenty-eight subjects participated in two sessions in which acidic saline (AS, pH 5) or neutral saline (NS, pH 7.4) were infused into the infrapatellar fat pad for 15 min. Pain intensity, pain area, mechanical and thermal sensitivity, and maximal voluntary knee extension force were recorded. Repeated infusions were performed in 14 subjects. Infusion of AS caused significantly higher pain intensity, larger pain areas, induced hyperalgesia around the infused knee, and reduced extension force. No significant pain facilitation or spreading of hyperalgesia was found after repeated infusions as compared with single infusions. Acidic saline infused into the infrapatellar fat pad provoked pain and localized mechanical hyperalgesia. Thus, this acid-induced pain model may mimic the early-stage responses to tissue injury of knee osteoarthritis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Osteoarthritis (OA) of the knee is one of the most frequent painful joint disorders (Dieppe 2005; Jinks et al. 2007). Hyperalgesia and spontaneous pain in knee OA are most likely related to increased sensitivity of nociceptors located in deep tissue (peripheral sensitization) and/or by increased responses in dorsal horn or supraspinal neurons (central sensitization) (Felson 2005; Arendt-Nielsen et al. 2010; Schaible 2012). The altered pain processing in knee OA has been investigated in recent studies, but the precise mechanisms underlying pain sensitization in OA remain elusive (Courtney et al. 2012). Like other pain conditions, knee OA can decrease strength and motor control of the muscles surrounding the painful joint (Messier et al. 1992) and affect submaximal muscle force regulation (Hortobagyi et al. 2004).
The infrapatellar fat is an intra-articular structure of knee. It is densely innervated by nociceptors, and considered to be one of the contributing sources of pain in knee OA (Clockaerts et al. 2010). Inflammation of the synovial membrane, which adheres to the infrapatellar fat pad, is associated with pathological changes in the knee of patients with painful OA (Hill et al. 2007), and hence pain manifestations associated with the infrapatellar fat pad are important to understand. Experimental knee pain has been investigated by injection of hypertonic saline into the infrapatellar fat pad of healthy volunteers. Hypertonic saline injections induce acute pain in the infrapatellar fat pad as well as a short-lasting mechanical hyperalgesia in the tissues around the injected area (Henriksen et al. 2011; Hirata et al. 2012; Joergensen et al. 2013). Experimental knee pain also leads to impaired quadriceps muscle strength during contractions, which provides further evidence that joint pain affects motor performance (Hodges et al. 2009). This experimental model of knee pain in healthy subjects may be advantageous to investigate the mechanisms of the nociceptive system related to OA pain.
Tissue acidosis has been observed as a regular phenomenon following inflammation, ischemia, arthritis, cancer, hematomas, and muscle exercise (Hood et al. 1988; Garber 2003; McMahon and Jones 2004) and hence may also contribute to OA-associated pain manifestations. Previous studies have also suggested that a pain-potentiating interaction exists between acidic pH and several inflammatory mediators and neurotransmitters, with low pH being the important factor (Rukwied et al. 2007; Roche-Gonzalez et al. 2009). Acid-sensing ion channels (ASICs) are important for excitation of nociceptors by low pH (Ikeuchi et al. 2008; Sluka et al. 2007). Primary mechanical hyperalgesia was observed following acid injection into human skin and muscle (Steen and Reeh 1993; Jones et al. 2004; Frey et al. 2008). However, acid infusion into the infrapatellar fat pad as an experimental knee pain model to mimic the “early”-stage OA or “acute” stage of response to tissue injury within the joints has not been studied previously.
Previous animal studies have shown that repeated intramuscular acidic injections induced spinal hyperexcitability with contralateral spreading hyperalgesia that indicates a central origin of this phenomenon (Da Silva et al. 2010; Sluka et al. 2001; Hoeger-Bement and Sluka 2003; Skyba et al. 2005). In recent human studies contralateral spreading of pain and hyperalgesia was, however, not observed following repeated infusions of acidic saline (Castrillon et al. 2013; Ernberg et al. 2013). Thus, a preclinical human model that could produce spreading sensitization following acidic saline infusion may help in understanding the mechanistic transition from an acute pain state to chronic pain in humans.
This study aimed to investigate acid-induced knee pain and associated hyperalgesia provoked by acidic infusion into the infrapatellar fat pad.
Materials and methods
Subjects
Thirty healthy subjects (16 females) with a mean age of 23.6 years (range 19–31 years) were included. In total, 28 subjects (15 females) completed 2 sessions of the experiment. Two subjects (1 female) participated in the first session only. Repeated infusions were performed in 14 subjects. None of the subjects had a history of pain, injuries or medical conditions that could interfere with normal somatosensory functioning. Women were excluded if they were menstruating. The study was approved by the local ethics committee (N 2012-0021) and conducted in accordance with the Declaration of Helsinki. All subjects gave written informed consent.
Experimental protocol
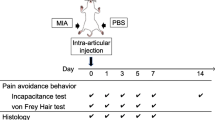
The study was designed as a randomized, controlled, double-blinded, crossover trial (session 1 and 2). A third session was added to the design to test the effects of repeated infusion. In total, the subjects attended three separated sessions and a follow-up visit 1 day after each session (Fig. 1a).
Assessments in each session. a Neutral or acid-buffered saline was infused into the infrapatellar fat pad of either the right or left knee for 15 minutes in each session. Pain intensity (visual analogue scale, VAS) was recorded from the beginning of the infusion and until the pain returned to zero. Pain areas and the quality of pain (McGill Pain Questionnaire) were assessed after infusion. Pressure pain threshold (PPT), cutaneous mechanical pain sensitivity (MPS), thermal pain threshold (HPT/CPT), and maximal voluntary contraction (MVC) upon knee extension (infused side) were assessed at each time point as indicated. b Five assessment sites around the infused (ipsilateral) knee/leg and six sites on the contralateral leg were selected for assessment. Infusions were given at site 1 on either the right or left knee. In this figure, site 1 on the left knee (circle) is presented as the infusion site
In each session, neutral phosphate-buffered saline (pH 7.4, neutral saline = NS) or acidic phosphate-buffered saline (pH 5.0, acidic saline = AS) was infused in a random order into the infrapatellar fat pad of the right or left knee over a period of 15 min. A randomization code for the 30 subjects was generated using a computer program and used to assign treatment for the session (http://www.randomizer.org). A 1-week interval between the first two sessions was used to eliminate a possible carryover effect. To investigate the effects of repeated infusions, the same buffer infused in the second session was also infused in the third session. The third session took place 2 days after the second session.
Pressure pain threshold (PPT), cutaneous mechanical pain sensitivity (MPS), and thermal (heat/cold) pain threshold (HPT/CPT) were assessed before (baseline), during, immediately after, 1 h after, and/or 1 day after the infusion. In addition, maximal voluntary contraction (MVC) during knee extension was assessed.
Acidic infusions and pain assessment
NS or AS was infused (5 ml) into the medial infrapatellar fat pad of the right or left side, respectively, in a randomized, double-blinded manner. Both buffers were iso-osmotic and prepared by the pharmacy of Aalborg University Hospital.
The infusion site was cleaned with alcohol and dried prior to the needle insertion. A needle (27 G, 19 mm, BD Microlance 3, Becton Dickinson, Ireland) was inserted at an angle of 45° in a superolateral direction to a depth of 15 mm. The inserted needle was fixed to the skin using surgical tape and sterile cotton. A tube (200 cm, 1.5 ml, G30303M, Care Fusion, Switzerland) was connected to the needle from the syringe. The sterile solutions were infused at a constant rate of 20 ml/h for 15 min using a syringe pump (Asena CC MK-III, Alaris medical systems, USA). The needle and tube were removed after completion of the infusion.
The pain intensity was continuously scored by the subjects on a 10-cm visual analogue scale (VAS) with the lower extreme labelled “no pain” and the upper extreme labelled “worst pain imaginable”. The VAS signal was sampled by a custom-designed computer program (Aalborg University, Aalborg, Denmark) every 2 s from the beginning of the infusion until the pain intensity returned to zero. The maximal pain (VAS peak) and the area under the curve (VAS AUC) were calculated. After the infusion, the subjects were asked to draw the pain areas on an anatomical map and describe the quality of the pain on a McGill Pain Questionnaire (MPQ) (Drewes et al. 1993). The pain area was measured using a digitizer (Vistametrix v. 1.38, Skillcrest LLC, USA) and presented in arbitrary units.
Assessment sites
The somatosensory sensitivity was assessed at local sites (assessing local sensitization) over the knees and mirrored contralateral locations (central sensitization) (Fig. 1b). The test sites were chosen based on previous literature (Frey et al. 2008; Jorgensen et al. 2013) as follows: site 1, 2 cm proximal to the inferior medial edge of patella (injection site); site 2, 2 cm distal to the inferior lateral edge of patella; site 3, 2 cm proximal to the superior medial edge of the patella. These sites (site 1, 2, 3) were chosen to test the local distribution of mechanical hyperalgesia. Furthermore, two regional sites (site 4, 5) away from the knee were assessed to test for possible spreading of the mechanical hyperalgesia as follows: site 4, the vastus lateralis muscle (VL, 7 cm from the lateral upper rim of patella); and site 5, the tibialis anterior muscle (TA, 10 cm below tibial tuberosity). In addition, one distant site was tested to assess for possible generalized hyperalgesia as follows: site 6, the brachioradialis muscle of the arm contralateral to the infusion site (BR, 5 cm from the lateral epicondyle). To avoid excessive stimulation during the experiment, only PPTs were tested at all testing sites whereas the cutaneous mechanical pain sensitivity was tested at sites 1, 2, and 3, and cutaneous mechanical pain sensitivity was measured only at site 1 in both knees.
Pressure pain sensitivity
Pressure pain thresholds (PPTs), which can be used to examine the pressure sensation from deep tissues, are an efficient tool to detect deep tissue mechanical pain thresholds and deep tissue mechanical hyperalgesia (Graven-Nielsen et al. 2004; Rolke et al. 2006). A decrease in PPT around the knee has been found in both experimental and clinical knee pain (Frey et al. 2008; Graven-Nielsen and Arendt-Nielsen 2010; Arendt-Nielsen et al. 2010). A hand-held pressure algometer (Somedic Senselab, Sweden) was used to assess PPT at all testing sites. The pressure was applied at a constant rate of 30 kPa/s through a 1 cm2 probe. The subjects were instructed to push a button immediately when the applied pressure became painful. PPTs were measured twice at each site (except for site 1 during the infusion). The interval between the two PPT trials was at least 40 s and the mean of the two measurements was used in the statistical analysis.
Cutaneous mechanical pain sensitivity
Cutaneous sensitivity was assessed using weight-calibrated pins (128 mN) at assessment sites 1, 2 and 3. The interval between the pin prick stimulations was at least 10 s. The subjects rated the cutaneous mechanical pain sensitivity (MPS) on a 0–5–10 numeric rating scale (NRS) in which “0” represented “no sensation”, “5” represented “pain threshold”, and “10” presented “most pain imaginable”. The mean of the three measurements was used in the statistical analysis.
Cutaneous thermal pain sensitivity
Cold pain (CPT) and heat pain thresholds (HPT) were measured [TSA 2001 II (CHEPS-MEDOC, Israel)] at assessment site 1 in both knees at each time point except during the infusion. The contact area of the thermode was 9 cm2. The baseline temperature was 32 °C (centre of neutral range). The method of limits was used by applying ramp stimuli at a velocity of 1 °C/s. Cut-off temperatures were 0 and 55 °C. The volunteers were asked to press a button when the respective thermal sensations were perceived. The mean threshold temperature of three consecutive measurements was calculated.
Maximal voluntary contraction during knee extension
The maximal voluntary contraction (MVC) force during isometric knee extension was assessed twice in the infused leg at each time point except during the infusion. The mean of the two measurements was used for the statistical analysis. A six-axis force sensor (MC3A 250, AMTI, USA) was used to yield three force components (F x , F y , F z ) (Salomoni and Graven-Nielsen 2012a, b; Mista et al. 2014). The sensor was secured and adjusted to fix its lower edge 5 cm above the medial malleolus. The hip was flexed at 90° and the knee extended at 120° (180° = straight leg). The arms were placed on the thighs. The analogue output of the task-related (F z ) force component was amplified (MSA-6 MINIAMP, AMTI, USA), sampled at 60 Hz, and stored after 12 bit A/D conversion. The subjects were instructed to extend their knee with maximal force for 4 s. The timing of each task was controlled by a cue signal.
Statistics
The statistical analysis was conducted using the SAS System (version 9.2, SAS Institute, USA). The normality of the pain, sensory and motor variables was assessed using Shapiro–Wilk tests. Logarithmic transformation was performed for data that were not normally distributed (Rolke et al. 2006). Side-to-side differences were assessed with paired t tests. The homogeneity of the baseline means of sensory and motor variables was assessed using repeated measures of analysis of variance (ANOVA).
The data from the crossover study (session 1 and 2) were first analysed. The VAS and MPQ were analysed using a two-way mixed-model analysis of variance (ANOVA; gender and sessions). The PPT, MPS, HPT/CPT, and MVC were then analysed using a three-way mixed-model ANOVA with gender as between-subject factor, and sessions (NS or AS) and time (baseline, during, immediately after, 1 h after, and 1 day after the infusion) as within-subject factors.
Subsequently, the data from the repeated session (session 3) were compared with session 2 using a two-way repeated measures ANOVA to assess the main effects and interactions between sessions (first infusion vs second infusion) and time (baseline, during, immediately after, 1 h after, and 1 day after the infusion).
A post hoc Tukey test was used to explore the pairwise differences if required. p values < 0.05 (with Bonferroni correction applied where appropriate; p = 0.05/3 = 0.017) were considered statistically significant. The data are presented as mean and standard error of the mean (SEM).
Results
Acid-evoked pain
The VAS time profiles for the first and second infusions were comparable (Fig. 2). The mean VAS peak and AUC after the first and second infusion of AS [peak 5.2 ± 0.4 cm (first), 5.3 ± 0.5 cm (second); AUC 59.6 ± 4.4 cm x s (first), 62.4 ± 6.3 cm x s (second)] were significantly higher compared with the NS [peak 1.7 ± 0.5 cm (first), 1.4 ± 0.6 cm (second), ANOVA–Tukey, p < 0.001; AUC; 17.3 ± 5.0 cm x s (first), 15.4 ± 6.7 cm x s (second), ANOVA–Tukey, p < 0.001] without a gender difference or differences between first and second infusion.
Visual analogue scale (VAS) profile. Mean VAS scores after first (filled) or second (open) infusion of either neutral (pH 7.4, triangle) or acid (pH 5, square)-buffered saline into the infrapatellar fat pad in healthy humans (mean ± standard error, N = 14). The VAS signal was sampled by a computer program every 2 s and the figure shows the mean VAS values across that were calculated each minute
The pain area drawings after the first and second infusions are illustrated in Fig. 3. The mean area of the pain drawings after the first and second infusion of AS was significantly larger than for the NS infusion (AS; 2.9 ± 0.6 (first), 5.1 ± 2.4 (second), NS; 0.6 ± 0.2 (first), 0.4 ± 0.2 (second), ANOVA–Tukey, p < 0.001). There was no significant difference in the mean area of pain when men and women were compared or between the first and second infusion. No significant difference in pain intensity between the left knee infusion and the right knee infusion was detected. Pain in the contralateral knee was observed in two subjects only after a single injection of AS.
Mean MPQ scores after the first and second infusion of AS were significantly increased compared with NS in the sensory, affective, and evaluative dimensions, and total scores (ANOVA–Tukey, p < 0.001) without a gender difference or differences between the first and second infusion. The data are listed in Fig. 4.
Mean MPQ scores after the first and second infusion. The McGill Pain Questionnaire (MPQ) scores after acidic saline (AS, bold) infusions were significantly increased compared with neutral saline (NS) (ANOVA–Tukey, p < 0.01). No significant difference in the MPQ score between the first and second infusion was found. There was no difference in the MPQ score when men and women were compared (mean ± standard error, N = 14)
Pressure pain sensitivity with and without acid-evoked pain
The PPTs around the infusion site of the ipsilateral knee (sites 1–3) were significantly reduced after the AS infusion compared with NS during, immediately after, and/or 1 h after the first and second infusion (ANOVA-Tukey, p = 0.013). There was no difference in the PPT measured after the first and second infusions (Fig. 5a). On the contralateral side, the PPT was significantly higher at sites 2 and 4 during the first or second infusion of the AS compared with NS (repeated measures ANOVA–Tukey, p = 0.011). There was no difference in the PPT measured after the first and second infusions (Fig. 5b).
Pressure pain threshold. The graph shows the mean relative change (%) in pressure pain threshold (PPT) from the baseline on the infused (a) and contralateral (b) side after the first (filled) and second (open) infusions of either neutral (pH 7.4, triangle) or acid (pH 5, square)-buffered saline into the infrapatellar fat pad in healthy humans (mean ± standard error, N = 14). ** and * indicate significant (p < 0.01, 0.05, respectively) differences from the first infusion of the neutral buffer at each time point. ## indicates significant (p < 0.01) differences from the second infusion of the neutral buffer at each time point
Cutaneous pain sensitivity
There were no significant differences in MPS (Fig. 6), CPT, and HPT (Fig. 7) between the AS and NS infusions after the first and second infusion at any assessment site (p > 0.05). There were no significant differences in any of these parameters between the first and second infusions.
Mechanical pain threshold. The graph shows mean change (Δ) in cutaneous pain sensitivity (MPS) on infused side over the first and second infusions of either neutral or acid-buffered saline into the infrapatellar fat pad in healthy humans. No significant difference was detected between the first and second infusions (p > 0.05) (mean ± standard error, N = 14)
Thermal pain threshold. The graph shows mean change (Δ) in cold pain threshold (CPT) and heat pain threshold (HPT) from baseline of the infused site by the first and second infusions of either neutral or acid-buffered saline into the infrapatellar fat pad in healthy humans. No significant difference was detected between the first and second infusions (p > 0.05) (mean ± standard error, N = 14)
Maximal voluntary contraction (MVC)
The MVC was significantly reduced immediately after both the first and second AS infusion compared with NS (repeated measures ANOVA–Tukey, p < 0.001; Fig. 8). There was no difference in the MVC measured after the first and second infusions.
Maximal voluntary contraction. The graph shows the mean relative change (%) in maximal voluntary contractions from in the infused side over the first (filled) and second (open) infusions of either neutral (pH 7.4, triangle) or acid (pH 5, square)-buffered saline into the infrapatellar fat pad of healthy humans (mean ± standard error, N = 14). ** and ## indicate significant (p < 0.01) differences between the first and second infusions
Discussion
Infusion of AS evoked pain and localized deep tissue mechanical hyperalgesia but did not alter cutaneous mechanical or thermal sensation. The maximal isometric voluntary knee extension force was decreased in legs infused with the AS. Contrary to previous animal studies, no spreading hyperalgesia could be detected and repeated acid infusions did not enhance these sensory and motor effects.
Local and referred pain
Injection of local anaesthetics, which can have pH levels as low as 5, occasionally produces transient pain (Cepeda et al. 2010; Frank and Lalonde 2012) and this property has been used to assess the pain modulatory effects of opioid analgesics (Cohen et al. 2008). In the present study, single infusions of AS into the human infrapatellar fat pad produced significantly higher pain and mechanical hyperalgesia than NS, which is consistent with previous studies on acidic muscle pain models (Issberner et al. 1996; Frey et al. 2008). However, a recent study reported that injections of acidic solution into the masseter muscle did not induce any pain (Castrillon et al. 2013). In that study, the injected acid solution was unbuffered, the volume (0.5 ml) of injection was much lower and the duration of administration was shorter than in the present study. The lack of pain produced by injection of acidic saline into the masseter muscle may have resulted from the ability of the muscle tissue to rapidly buffer pH changes. While the buffering capacity of the infrapatellar fat pad is not known, it is likely that by using buffered acidic saline and a slow infusion, an acidic pH was maintained in fat pad for the duration of the infusion, which may explain the greater pain produced in the present study.
Injections of acidic solution into rat muscles have been reported to increase the spinal excitability and activate the supraspinal pain pathway to produce a spreading hyperalgesia (Sluka et al. 2003; Tillu et al. 2008). Infusion of acidic buffer into the infrapatellar fat pad of the knee caused localized ipsilateral pain with a similar pattern of distribution as was produced by injection of hypertonic saline in a previous study (Joergensen et al. 2013). The findings of the present study are in agreement with a previous study reporting that hyperalgesia was restricted to the ipsilateral side after intramuscular infusion of acidic buffer (Frey et al. 2008). Further, intramuscular infusion of acidic buffer resulted in only short-lasting pain and hyperalgesia; no long-lasting pain was observed. Hence, our model only reflects “early” or “acute” joint pain and does not model chronic arthritis pain.
No gender differences in pain intensity or pain areas were observed in the present study. After intramuscular infusion of buffered acidic saline, women were reported to experience higher referred pain and exhibited a stronger correlation between local and referred pain than men despite the fact that no difference in local pain was detected (Frey et al. 2008). However, the underlying mechanisms for this sex-related difference are not clear. Hormonal levels, genetic factors and neurobiological factors such as differences in descending inhibition may render females more susceptible to acid-induced muscle pain (Bartley and Fillingim 2013; Hunt 2009; Martel et al. 2013).
Mechanical hyperalgesia
The PPT values around the infused knee were significantly decreased during and after the acidic infusion and recovered to baseline after 1 day. A similar mechanical sensitization was observed in an experimental knee pain model which used hypertonic saline injections (Joergensen et al. 2013) and in an experimental muscle pain model which infused acidic buffer solution into tibialis muscle (Frey et al. 2008). In OA patients, decreased PPT values are found at sites distal to the joint (lower leg and arm) (Arendt-Nielsen et al. 2010), but this spread of mechanical sensitization was not produced by infrapatellar fat pad acid infusion in healthy humans. Thus, there was no evidence of “central sensitization” in the current study, which contrasts with findings reported for patients with OA pain.
In addition to deep tissue mechanical hyperalgesia, sensitization to cutaneous thermal and tactile stimulation has been reported for OA patients (Arendt-Nielsen et al. 2010; Courtney et al. 2012). Previous clinical OA studies have reported mechanical allodynia and heat hyperalgesia (Hendiani et al. 2003; Fingleton et al. 2015). These changes in cutaneous thermal and mechanical sensitivity are assumed to be centrally mediated by distinct neurophysiological mechanisms. Altered cutaneous sensitivity was not provoked by acid infusion in the present study. This finding is consistent with a previous study of hypertonic saline injection into the infrapatellar fat pad (Joergensen et al. 2013). The short-lasting mechanical hyperalgesia and lack of cutaneous sensitization found in the current knee pain model are not reflective of the type of persistent pain typical in clinical conditions such as OA.
Motor function
The isometric maximal knee extension force measured from the infused leg decreased after the acid infusion. It has been shown that knee pain is associated with impairment of the motor function in both experimental pain models and OA (Henriksen et al. 2011; Salomoni and Graven-Nielsen 2012a; Hodges et al. 2009). Knee pain provoked by injection of hypertonic saline into the infrapatellar fat pad decreased the muscle force and quadriceps activity by 80% of MVC (Salomoni and Graven-Nielsen 2012b). The present results are consistent with these previous reports and provide evidence for a direct relationship between inhibition of motor function and knee pain evoked by acidic infusion into the infrapatellar fat pad. Interestingly, these novel data show that a physiologically relevant change in tissue pH in a non-contractile structure can impair the motor function.
Effect of repeated infusions
In rodents, repeated intramuscular (gastrocnemius muscle) or intrarticular (knee joint) injections of acidic saline produce a prolonged bilateral mechanical hyperalgesia lasting up to 30 days (Sluka et al. 2001, 2003). It has been demonstrated that activation of ASIC3 receptor expressed by muscle and joint nociceptors is required to initiate this bilateral hyperalgesia, but is not required for its maintenance (Gautam et al. 2012). The maintenance of the bilateral hyperalgesia appears to result from a mechanism involving central NMDA and non-NMDA receptor activation at the level of the spinal cord as well as at supraspinal pain facilitatory sites (Skyba et al. 2005). Thus, in rodents, prolonged hyperalgesia appears to be a result of the induction of central sensitization after repeated strong nociceptive input from the muscle or joint. In the present human study, contralateral spreading of pain and hyperalgesia was not observed following repeated infusions of acidic saline. This finding is consistent with previous human studies where repeated injection of unbuffered acidic saline or infusion of buffered saline into human masseter or anterior tibialis muscle, respectively, did not produce a prolonged bilateral mechanical hyperalgesia (Castrillon et al. 2013; Ernberg et al. 2013; Frey et al. 2008). In these previous studies, the intensity of muscle pain from administration of acidic solutions was rated as mild by most subjects. Although pain intensity levels were reported to be moderate after acidic saline infusions into the fat pad, this pain was not intense enough to routinely result in reports of pain referral or in alterations of cutaneous pain sensitivity over the injection site, suggesting that it was insufficiently intense to induce signs of central sensitization in these human subjects.
The lack of direct or clear translation of findings in the rodent models to human experimental models could be due to a species difference between rodent and human anatomy and physiology. Species differences are highly apparent at the molecular level as well (e.g., Ahmad et al. 2007; Chen et al. 2013). Another explanation might be the difference in the relative amount of acid stimulation between the animal and human studies as a larger part of the muscle was actually stimulated in the animals, whereas only a small part of the muscle was affected in humans.
Thus, we conclude that the acidic saline injection model of prolonged hyperalgesia in rodents, which might be useful for modelling chronic musculoskeletal pain, could not be translated into a human model of long-term deep tissue hyperalgesia as shown in the present study. Although speculative, widespread mechanical hyperalgesia may be induced using a lower pH level buffered acidic solution, higher flow rate, and/or a larger volume injection to produce higher pain levels. Future studies are needed to address this.
Limitations
It is important to note that the current model appears to reflect the early or acute response to injury. Further, the source of pain in the present study is different from the source in clinical pain conditions such as OA (Hodges et al. 2009). Thus, the sensorimotor changes observed in response to this experimentally produced pain cannot be directly translated to clinical pain conditions. In addition, given the short duration of the hyperalgesia, it is unlikely that the current model can be adequately characterized with pharmacological tools such as NSAIDS or anticonvulsants used in the treatment of OA.
Conclusions
This is the first study to evoke experimental knee pain by acid infusion into the infrapatellar fat pad of healthy humans. Acid infusion induced pain with localized mechanical hyperalgesia around the knee, but did not produce signs of central sensitization like that found in animal models. Despite this difference, the present model may reflect the early stage of responses to tissue injury of clinical knee pain conditions such as knee osteoarthritis.
References
Ahmad S, Dahllund L, Eriksson AB, Hellgren D, Karlsson U, Lund PE, Meijer IA, Meury L, Mills T, Moody A, Morinville A, Morten J, O’donnell D, Raynoschek C, Salter H, Rouleau GA, Krupp JJ (2007) A stop codon mutation in SCN9A causes lack of pain sensation. Hum Mol Genet 16:2114–2121
Arendt-Nielsen L, Nie H, Laursen MB, Laursen BS, Madeleine P, Simonsen OH, Graven-Nielsen T (2010) Sensitization in patients with painful knee osteoarthritis. Pain 149:573–581
Bartley EJ, Fillingim RB (2013) Sex differences in pain: a brief review of clinical and experimental findings. Br J Anaesth 111:52–58
Castrillon EE, Cairns B, List T, Svensson P, Ernberg M (2013) Acidic saline-induced pain as a model for experimental masseter myalgia in healthy subjects. Eur J Pain 17:1438–1746
Cepeda MS, Tzortzopoulou A, Thackrey M, Hudcova J, Arora Gandhi P, Schumann R (2010) Adjusting the pH of lidocaine for reducing pain on injection. Cochrane Database Syst Rev 12:1–65
Chen J, Kang D, Xu J, Lake M, Hogan JO, Sun C, Walter K, Yao B, Kim D (2013) Species differences and molecular determinant of TRPA1 cold sensitivity. Nat Commun 4:2501. https://doi.org/10.1038/ncomms3501
Clockaerts S, Bastiaansen-Jenniskens YM, Runhaar J, Van Osch GJ, Van Offel JF, Verhaar JA, De Clerck LS, Somville J (2010) The infrapatellar fat pad should be considered as an active osteoarthritic joint tissue: a narrative review. Osteoarthr Cartil 18:876–882
Cohen SP, Christo PJ, Wang S, Chen L, Stojanovic MP, Shields CH, Brummett C, Mao J (2008) The effect of opioid dose and treatment duration on the perception of a painful standardized clinical stimulus. Reg Anesth Pain Med 33:199–206
Courtney CA, O’Hearn MA, Hornby TG (2012) Neuromuscular function in painful knee osteoarthritis. Curr Pain Headache Rep 16:518–524
Da Silva LF, De Santana JM, Sluka KA (2010) Activation of NMDA receptors in the brainstem, rostral ventromedial medulla, and nucleus reticularis gigantocellularis mediates mechanical hyperalgesia produced by repeated intramuscular injections of acidic saline in rats. J Pain 11:378–387
Dieppe PA (2005) Relationship between symptoms and structural change in osteoarthritis: what are the important targets for therapy? J Rheumatol 32:1147–1149
Drewes AM, Helweg-Larsen S, Petersen P, Brennum J, Andreasen A, Poulsen H, Jensen TS (1993) McGill Pain Questionnaire translated into Danish: experimental and clinical findings. Clin J Pain 9:80–87
Ernberg M, Castrillon EE, Ghafouri B, Larsson B, Gerdle B, List T, Svensson P (2013) Experimental myalgia induced by repeated infusion of acidic saline into the human masseter muscle does not cause the release of algesic substances. Eur J Pain 17:539–550
Felson DT (2005) The sources of pain in knee osteoarthritis. Curr Opin Rheumatol 17:624–628
Fingleton C, Smart K, Moloney N, Fullen BM, Doody C (2015) Pain sensitization in people with knee osteoarthritis: a systematic review and meta-analysis. Osteoarthr Cartil 23:1043–1056
Frank SG, Lalonde DH (2012) How acidic is the lidocaine we are injecting, and how much bicarbonate should we add? Can J Plast Surg 20:71–74
Frey LA, Sluka KA, McMullen T, Lee J, Arendt-Nielsen L, Graven-Nielsen T (2008) Acidic buffer induced muscle pain evokes referred pain and mechanical hyperalgesia in humans. Pain 140:254–264
Garber K (2003) Why it hurts: researchers seek mechanisms of cancer pain. J Natl Cancer Inst 95:770–772
Gautam M, Benson CJ, Ranier JD, Light AR, Sluka KA (2012) ASICs do not play a role in maintaining hyperalgesia induced by repeated intramuscular acid injections. Pain Res Treat 817347. https://doi.org/10.1155/2012/817347
Graven-Nielsen T, Arendt-Nielsen L (2010) Assessment of mechanisms in localized and widespread musculoskeletal pain. Nat Rev Rheumatol 6:599–606
Graven-Nielsen T. Siegfried Mense S, Arendt-Nielsen L (2004) Painful and non-painful pressure sensations from human skeletal Muscle. Exp Brain Res 159:273–283
Hendiani JA, Westlund KN, Lawand N, Goel N, Lisse J, McNearney T (2003) Mechanical sensation and pain thresholds in patients with chronic arthropathies. J Pain 4:203–211
Henriksen M, Rosager S, Aaboe J, Graven-Nielsen T, Bliddal H (2011) Experimental knee pain reduces muscle strength. J Pain 12:460–467
Hill CL, Hunter DJ, Niu J, Clancy M, Guermazi A, Genant H, Gale D, Grainger A, Conaghan P, Felson DT (2007) Synovitis detected on magnetic resonance imaging and its relation to pain and cartilage loss in knee osteoarthritis. Ann Rheum Dis 66:1599–1603
Hirata RP, Arendt-Nielsen L, Shiozawa S, Graven-Nielsen T (2012) Experimental knee pain impairs postural stability during quiet stance but not after perturbations. Eur J Appl Physiol 112:2511–2521
Hodges PW, Mellor R, Crossley K, Bennell (2009) Pain induced by injection of hypertonic saline into the infrapatellar fat pad and effect on coordination of the quadriceps muscles. Arthritis Rheum 61:70–77
Hoeger-Bement MK, Sluka KA (2003) Phosphorylation of CREB and mechanical hyperalgesia is reversed by blockade of the cAMP pathway in a time-dependent manner after repeated intramuscular acid injections. J Neurosci 23:5437–5445
Hood VL, Chubert C, Keller U, Muller S (1988) Effect of systemic pH on pHi and lactic acid generation in exhaustive forearm exercise. Am J Physiol 255:F479-F485
Hortobagyi T, Garry J, Holbert D, Devita P (2004) Aberrations in the control of quadriceps muscle force in patients with knee osteoarthritis. Arthritis Rheum 51:562–569
Hunt SP (2009) Genes and the dynamics of pain control. Funct Neurol 24:9–15
Ikeuchi M, Kolker SJ, Burnes LA, Walder RY, Sluka KA (2008) Role of ASIC3 in the primary and secondary hyperalgesia produced by joint inflammation in mice. Pain 137:662–669
Issberner U, Reeh PW, Steen KH (1996) Pain due to acidosis: a mechanism for inflammatory and ischemic myalgia? Neurosci Lett 208:191–194
Jinks C, Jordan K, Croft P (2007) Osteoarthritis as a public health problem: the impact of developing knee pain on physical function in adults living in the community: (KNEST 3). Rheumatology 46:877–881
Joergensen TS, Henriksen M, Danneskiold-Samsoe B, Bliddal H, Graven-Nielsen T (2013) Experimental knee pain evoke spreading hyperalgesia and facilitated temporal summation of pain. Pain Med 14:874–883
Jones NG, Slater R, Cadiou H, McNaughton P, McMahon SB (2004) Acid-induced pain and its modulation in humans. J Neurosci 24:10974–10979
Martel MO, Wasan AD, Edwards RR (2013) Sex differences in the stability of conditioned pain modulation (CPM) among patients with chronic pain. Pain Med 14:1757–1768
McMahon SB, Jones NG (2004) Plasticity of pain signaling: role of neurotrophic factors exemplified by acid-induced pain. J Neurobiol 61:72–87
Messier SP, Loeser RF, Hoover JL, Semble EL, Wise CM (1992) Osteoarthritis of the knee: effects on gait, strength, and flexibility. Arch Phys Med Rehabil 73:29–36
Mista CA, Salomoni SE, Graven-Nielsen T (2014) Spatial reorganisation of muscle activity correlates with change in tangential force variability during isometric contractions. J Electromyogr Kinesiol 24: 37–45
Roche-Gonzalez HI, Herrejon-Abreu E, Lopez-Santillan FJ, Garcia-Lopez BE, Murbartian J, Granados-Soto V (2009) Acid increase inflammatory pain in rats: effect of local peripheral ASICs inhibitors. Eur J Pharmacol 603:56–61
Rolke R, Baron R, Maier C, Tolle TR, Treede RD, Beyer A et al (2006) Quantitative sensory testing in the German Research Network on Neuropathic Pain (DFNS): standardized protocol and reference values. Pain 123:231–243
Rukwied R, Chizh BA, Lorenz U, Obreja O, Margarit S, Schley M, Schmelz M (2007) Potentiation of nociceptive responses to low pH injections in humans by prostaglandin E2. J Pain 8:443–451
Salomoni SE, Graven-Nielsen T (2012a) Experimental muscle pain increases normalized variability of multidirectional forces during isometric contractions. Eur J Appl Physiol 112:3607–3617
Salomoni SE, Graven-Nielsen T (2012b) Muscle fatigue increases the amplitude of fluctuations of tangential forces during isometric contractions. Hum Mov Sci 31:758–771
Schaible HG (2012) Mechanisms of chronic pain in osteoarthritis. Curr Rheumatol Rep 14:549e56
Schaible HG, Ebersberger A, Von Banchet GS (2002) Mechanisms of pain in arthritis. Ann N Y Acad Sci 966:343–354
Skyba DA, Lisi TL, Sluka KA (2005) Excitatory amino acid concentrations increase in the spinal cord dorsal horn after repeated intramuscular injection of acidic saline. Pain 119:142–149
Sluka KA, Kalra A, Moore SA (2001) Unilateral intramuscular injections of acidic saline produce a bilateral, long-lasting hyperalgesia. Muscle Nerve 24:37–46
Sluka KA, Price MP, Breese NM, Stucky CL, Wemmie JA, Welsh MJ (2003) Chronic hyperalgesia induced by repeated acid injections in muscle is abolished by the loss of ASIC3, but not ASIC1. Pain 106:229–239
Sluka KA, Radhakrishnan R, Benson CJ, Eshcol JO, Price MP, Babinski K et al (2007) ASIC3 in muscle mediates mechanical, but not heat, hyperalgesia associated with muscle inflammation. Pain 129:102–112
Steen KH, Reeh PW (1993) Sustained graded pain and hyperalgesia from harmless experimental tissue acidosis in human skin. Neurosci Lett 154:113–116
Tillu DV, Gebhart GF, Sluka KA (2008) Descending facilitatory pathways from the RVM initiate and maintain bilateral hyperalgesia after muscle insult. Pain 136:331–339
Acknowledgements
This study was funded by The Danish Rheumatism Association, The Danish National Advanced Technology Foundation, Aase and Ejnar Danielsen’s Foundation, Lions Club Denmark, and The Danish Council for Technology and Innovation (09-052174). The authors thank professor Brian Edwin Cairns for proofreading the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Asaki, T., Wang, K., Luo, Y. et al. Acid-induced experimental knee pain and hyperalgesia in healthy humans. Exp Brain Res 236, 587–598 (2018). https://doi.org/10.1007/s00221-017-5155-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00221-017-5155-5