Abstract
In contrast to bronchial and nasal lavages, the analysis of exhaled breath condensate (EBC) is a promising, simple, non-invasive, repeatable, and diagnostic method for studying the composition of airway lining fluid with the potential to assess lung inflammation, exacerbations, and disease severity, and to monitor the effectiveness of treatment regimens. Recent investigations have revealed the potential applications of EBC analysis in systemic diseases. In this review, we highlight the analytical studies conducted on non-volatile compounds/biomarkers in EBC. In contrast to other related articles, this review is classified on the basis of analytical techniques and includes almost all the applied methods and their methodological limitations for quantification of non-volatile compounds in EBC samples, providing a guideline for further researches. The studies were identified by searching the SCOPUS database with the keywords “biomarkers,” “non-volatile compounds,” “determination method,” and “EBC.”
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The conventional methods for the diagnosis of lung diseases (bronchoscopy or biopsy) are invasive or semi-invasive (e.g., nasal swabs, sputum induction), but are currently used in clinical follow-ups [1]. In contrast, non-invasive methods, such as the collection of exhaled breath condensate (EBC) with analysis of diverse biomarkers, which have been used since the 1980s [2], are easy, repeatable for some biomarkers, and not associated with side effects or any appreciable discomfort or risk to the sample donors [3]. This method also reduces the number of interfering substances compared to more complicated matrices, such as blood, plasma, sputum, and urine [4]. Moreover, the collection of EBC can be repeated as often as needed without altering the fluids present on the lung surfaces [5].
EBC is the water vapor contained in breath and very small droplets of lung lining fluid, which are condensed typically by using a cooling or condensing collection device (commonly at 4 °C or sub-zero temperatures) [6]. EBC is a highly diluted and low-protein aqueous matrix [7]. It is a unique matrix for the analysis of inflammatory and oxidative stress biomarkers and enables the study of the early effects of different diseases or exposures on the lung and/or upper airways [8]. The analysis of drugs is also another promising procedure that has attracted increasing attention in recent years [9,10,11,12,13,14,15].
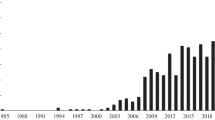
The number of publications on EBC analysis has increased in recent years, and so has the interest at international conferences. Clinicians and clinical chemists are awaiting the sufficient maturation of EBC-based methods to help them with their daily needs in the clinic. Therefore, it is important to summarize the current understanding of the available methods as well as identify the knowledge gaps in the hope of finding suitable applications for this sampling method in both research and clinical practice.
This paper aims to summarize and review the exhaled breath non-volatile compound-related detection and analytical methods, especially the recent developments relating to EBC biomarker detection systems. It is hoped that although similar articles have been published in the past, this article will attract the attention of many research groups as well. The main purpose of this review is to update a previous literature review [16] on the same subject, and to present a broad range of compounds (biomarkers and drugs) used in various diseases; hence, leading researchers from various areas of study are included in this article. In contrast to other related articles, this review is classified on the basis of analytical methods and includes almost all the applied methods and their methodological limitations for quantification of non-volatile compounds in EBC samples, thus providing guidelines for further investigations.
Literature search method
The articles included in this review were identified through literature searches of the SCOPUS database by using the search terms of “biomarkers,” “non-volatile compounds,” “determination method,” and “EBC.” A total of 224,175 studies were identified for the keyword “biomarkers,” out of which 3183 studies pertained to “non-volatile compounds” and 1662 cases related to studies conducted on EBC. Since this study is limited to the determination methods of non-volatile compounds/biomarkers in EBC, the literature search was restricted to the methodological aspects only. It should be noted that published reviews, abstracts, and bibliographies were also examined to identify additional studies.
EBC sampling devices
Various collection and sampling systems have been described by different research groups (Fig. 1). However, the common principle for all of them includes the rapid cooling of exhaled air with consequent condensation of water vapor, as well as the sedimentation of aerosol particles onto a cold surface. Three commercial instruments are available for EBC sampling; the most common according to the literature are EcoScreen (Erich Jaeger, Hoechberg, Germany), which is a stationary system, and RTube™ (Respiratory Research, Charlottesville, VA, USA), which is a portable device and is available in two subtypes. The first subtype is composed of a metal cylindrical tube that is pre-cooled in a freezer at a temperature of less than − 20 °C, then it is placed in the RTube chamber, and the exhaled breath is blown into the tube. Finally, owing to the low temperature of the tube, the exhaled breath is condensed into the chamber [17, 18]. In the second subtype of RTube, instead of cooling by using a freezer or dry ice, liquid nitrogen or a low-temperature fluid is used to reduce the temperature inside the RTube chamber [19, 20]. Turbo-DECCS (transportable unit for research on biomarkers obtained from disposable exhaled condensate collection systems; ItalChill, Parma, Italy) is another commercially available device for EBC collection. In addition, various homemade devices have been described in the literature [21]. One of these homemade EBC collecting devices with the ability to set the temperature from 0 to − 25 °C was also developed by our research group. Variable sampling temperature enables the collection of gaseous substances with boiling points varying from 0 to − 25 °C. The sampling time in this device is between 5 to 15 min, depending on the operating temperature [22]. Ahmadzai et al. [23] compared biomarkers measured in collected EBC by using different devices. The design and inner coating materials used in the collecting device as well as the temperature fluctuations during the process of condensate collection influence the biomarkers’ concentrations [24]. Uneven condensing temperatures may be present not only between different EBC collecting systems but also in cases when the same condenser is used with different airflows or with different cooling temperatures. Moreover, the variability in EBC pH between various collection systems due to the differences in the concentrations of absorbed volatile salivary contaminants during collection (e.g., CO2, ammonia, and acetic acid) can influence the concentrations of biomarkers or non-volatile compounds differently [21]. Finally, to provide consistent data, the EBC collection system needs to be standardized with respect to the collection temperature, material, and flow design, as well as other parameters, such as ventilatory patterns, tidal volumes, breathing frequencies, and exhaled particles.
Non-volatile compounds in EBC
Non-volatile compounds normally present in EBC
The non-volatile compounds in EBC vary from small inorganic ions (anions, cations), larger organic molecules (urea, organic acids, amino acids, and their derivatives) to peptides, proteins, surfactants, and macromolecules. EBC contains many biomarkers of oxidative and nitrative stresses (8-isoprostane, 3-nitrotyrosine (3-NT), S-nitrosothiols, etc.) as well as inflammation mediators (LTB4, cysteinyl leukotrienes (Cys-LTs): LTC4, LTD4, LTE4, prostaglandins, histamine, adenosine, interleukins (IL), etc.). Some of these compounds are listed in Table 1 [25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54,55,56,57,58,59,60,61,62].
Non-volatile compounds generated in EBC with the appearance of disease signs
In addition to the mentioned compounds, EBC contains some other substances that do not exist in a healthy state and they are only detectable along with the appearance of disease signs. Some of these compounds include:
Pepsin
Pepsin is a gastric aspartic proteinase enzyme that degrades food proteins into peptides and initiates digestion. Pepsin is produced only in the stomach; hence, evidence of its presence in other organs indicates that it has reached them as a refluxate. The enzyme has recently been detected within the laryngeal epithelium, in the saliva of patients with suspected reflux laryngitis, and in the EBC of individuals with airways and lung diseases, where reflux has played a part. The advantage of pepsin analysis is that in the normal state, it is not found in the tracheobronchial tree, and thus it may be a specific biomarker for reflux-related lung diseases [63].
Carcinoembryonic antigen
Carcinoembryonic antigen (CEA) is a glycoprotein involved in cell adhesion and is normally produced in gastrointestinal tissue during fetal development, but its production stops before birth. It is usually present only at very low levels in the blood of healthy adults. However, the serum levels of CEA are raised in some types of cancer [64, 65]. Nevertheless, CEA may also exist in EBC and it has been reported in some studies that CEA detection in EBC may diagnose lung cancer earlier than the detection of this biomarker in serum [66]. Therefore, CEA can be used as a possible and promising tumor biomarker in clinical tests.
Nε-(Carboxymethyl)lysine
Nε-(Carboxymethyl)lysine (CML) is one of the best-characterized analytical indicators of advanced glycation end-products (AGEs) and could be formed by a non-enzymatic reaction of reducing carbohydrate with an amino group of protein or other macromolecules followed by a cleavage and/or intramolecular rearrangement [67]. AGE-modified proteins have been found to stimulate monocytes/macrophages to synthesize and release TNF, IL-1, and some growth factors—platelet-derived growth factor (PDGF) and insulin-like growth factor I (IGF-I)—by the AGE receptor system. These cytokines and growth factors secreted by lung macrophages are related to a possible pathogenesis in pulmonary fibrosis [68].
Trimethylamine
Trimethylamine (TMA) is formed in biosynthetic pathways from amino acids via the methylation of monomethylamine, which is metabolically derived from sarcosine or glycine. TMA is also an intermediate product in the metabolism of choline. During the demethylation process, it is decomposed into dimethylamine [68]. Studies have proved that the presence of TMA in breath is typical only for patients with renal disorders. In healthy subjects, the amines are normally removed from the body by renal excretion, whereas the amines accumulate in the case of patients with kidney damage [69].
Exogenous compounds
All the above-mentioned compounds are endogenous and are found in different concentrations according to the health status of the individuals. However, exogenous factors can also have an impact on the exhaled composition and require consideration as confounding factors that impede the reliable identification of breath biomarkers. Compounds with exogenous origin can also be excreted via the lungs and detected in EBC after previous uptake from the environment through inhalation or ingestion, and distribution within the body [70]. However, exogenous compounds are beyond the scope of this article and we just focus on drugs as a sub-set of these compounds.
Drugs
Previous studies on breath have confirmed that many drugs or metabolites are exhaled and can be potentially used as diagnostic markers [71,72,73,74]. Many factors, such as body mass index, health status, polymedication, addiction, and genetics, influence the quantity of therapeutic dose needed. Therefore, therapeutic drug monitoring (TDM) and knowing the exact body drug concentration are essential to maintain the efficacy of many immunosuppressant drugs. TDM allows the physician to immediately adjust the required drug dose before the patient faces any inconvenience. Analyzing EBC as a very convenient and rapid sampling method enables an access to immediate and accurate information about the pharmacokinetics of drugs.
Reported analytical methods for determination of non-volatile biomarkers/compounds in EBC
The application of EBC is dependent on the development of highly sensitive and reproducible assays. Till date, a lot of methods have been reported for the determination of various non-volatile biomarkers/compounds in EBC samples. Depending on the biomarker panel required for diagnosing or monitoring of a specific disease, different methods or their combinations could be applied. The methods for the analysis of breath condensate are usually based on spectrophotometric or fluorometric assays or high-pressure liquid chromatography (HPLC) in combination with different detection methods, such as UV detection, fluorescence detection (FD), electrochemical detection (ECD) or mass spectrometry (MS), gas chromatography (GC) in combination with MS, capillary electrophoresis (CE), antibody-based assays, and some other new methods (Fig. 2). The following sections present the typical instrumentation platforms and their utility for EBC analysis in healthy subjects and patients. In general, the analytical methods reported for EBC analysis may be classified into several categories, including:
Applied analytical methods for determination of non-volatile biomarkers/compounds in EBC. PCR polymerase chain reaction, FD fluorescence detection, ECD electrochemical detection, MS mass spectroscopy, DAD diode array detection, C4D contactless conductivity detection, LIF laser-induced fluorescence, PCR polymerase chain reaction, NMR nuclear magnetic resonance
Optical methods
A number of spectroscopic- and spectrometric-based devices have been developed for use in clinical applications for the detection and monitoring of non-volatile biomarkers/compounds in EBC (Table 2). A range of optical detectors could be used, including absorbance, fluorescence, and luminescence.
Absorbance
The most commonly used detection methods are UV detectors, which rely on the presence of a chromophore in the molecules. The determination of NO2−/NO3− in EBC samples is mostly based on the Griess diazotization reaction, which involves the reaction of NO2− with N-1-napthylethylenediamine in the presence of sulfonic acid and subsequent absorbance measured at 540–550 nm [75,76,77,78, 113]. To measure NO3− content, the NO3− needs to be reduced to NO2− enzymatically by NO3− reductase, followed by the measurement of nitrite. In addition to the Griess diazotization reaction, other colorimetric assays could be used as well. Sepehr et al. [9] determined the NO2− content in EBC samples by using the Berthelot method. For this purpose, NO2− is first reduced to ammonium by adding Zn powder and H2SO4, followed by the derivatization of ammonium with Berthelot’s reagent (i.e. phenol and hypochlorite in alkaline solution) to form a blue product that can be measured at 655 nm. The reagents used in these experiments may be prepared as a kit. For example, the enzyme-linked immunosorbent assay (ELISA) kits which have become very popular recently owing to their relatively low cost and ease of application. Some commercial ELISA kits are available for the determination of 3-NT with absorbance measured at 450 nm [79, 80], S-nitrosothiols with absorbance measured at 540–550 nm (as NO2− after the cleavage of the RS–NO bond with HgCl2 or CuCl/cysteine solution) [81, 114], 8-isoprostane [80, 82, 83, 115, 116], LTB4 [84,85,86,87,88], prostanoids [89, 90], cytokines [26, 91,92,93,94,95,96, 117,118,119,120], GSH [97], TxB2 [98], TGF-β1 [99], and other molecules, such as proteins [121] and keratin [100] in the EBC of patients with various respiratory diseases. In a systematic study, Carpagnano et al. used an enzyme immunoassay (EIA) kit for determining a protein hormone called leptin in patients with obstructive sleep apnea syndrome (OSAS) [122] and non-small-cell lung carcinoma (NSCLC) [123]. Leptin controls body weight by influencing appetite and energy expenditure. They reported higher concentrations of exhaled leptin in obese patients with OSAS and in NSCLC patients with relation to tumor progression. The developed kits are portable, rapid, and highly specific, as well as being simple to use.
Furthermore, Timms et al. [101] reported an in-house quantitative ELISA based on a monospecific antibody test for the determination of pepsin in the EBC of patients with obstructive lung disease with gastroesophageal reflux disease (GERD) in comparison to patients with obstructive lung disease without concurrent GERD. A significantly higher mean pepsin concentration was found in the patients with obstructive lung disease with GERD compared to those without GERD and healthy controls. Soyer et al. [102] also determined pepsin in the EBC of pediatric asthmatic patients with GERD with a homemade indirect ELISA kit. They reported a negative correlation between NOX levels and the severity of gastroesophageal reflux, suggesting decreased levels of NOX in patients with GERD and increased oxidative stress in the airways of these patients. Lee et al. [124] studied the relationship between pepsin concentration and gastroesophageal reflux in bronchiectasis and COPD by spectrophotometry methods (locally developed ELISA).
The disadvantage of these commercial or homemade kits is that they are for single use only. Additionally, competitive ELISA suffers from a limited detection range due to the narrow sensitivity of the antibodies.
Fluorescence
Till date, a number of fluorescence-based methods for sensing non-volatile biomarkers/compounds in EBC have been presented. For example, the determination of NO2− concentration in the EBC of asthma patients performed fluorometrically after derivatization with 2,3-diaminonaphthalene (DAN) by Chladkova et al., a reaction that takes place intramolecularly, because the DAN molecule contains two amino groups in the ortho position. This reaction yields 2,3-naphthotriazole (NAT), a stable fluorescent compound with emission at around 430 nm. NO3− was assayed after reduction to NO2− with enzymatic reductase [103]. Commercial fluorescence-based kits are also available. Balint et al. reported the determination of 3-NT in the EBC of CF patients by fluorescence-based EIA; they found no significant differences in the levels of NO2− and NO3− in CF patients and normal subjects [114].
Another fluorescence-based method is flow cytometry. The original name for fluorescence-based flow cytometry technology was “pulse cytophotometry.” Modern flow cytometers are able to analyze several thousand particles per second, in real time, and can actively separate and isolate particles with specified properties. Gessner et al. [104] and Robroeks et al. [125] developed a flow cytometry method for the determination of cytokines in COPD patients and in children with asthma and CF, respectively. They observed a significant increase in the concentration of cytokines in acute exacerbation of COPD, asthma, and CF patients compared to healthy volunteers. However, they concluded that cytokine concentration did not differ significantly in children with asthma vs. CF. Similar studies have been performed by Sack et al. [105] and Rosias et al. [106] for the determination of cytokines in acute lung injury (ALI) cases and in asthma patients, respectively. Sack et al. reported that in patients with ALI, the cytokine levels for all the investigated cytokines were higher in comparison to those in healthy subjects, and Rosias et al. found a significant decrease in TNF-α in the EBC of atopic asthmatic children compared to children with viral wheeze and healthy controls. Schumman et al. [107] also reported the detection of erythropoietin (EPO) in the EBC of patients with COPD, OSAS, and OSA by the cytophotometry method. However, they found no significant difference in the EPO levels of patients with COPD compared to non-COPD (OSAS, OSA, and healthy) subjects. Their team also detected TNF-α simultaneously; TNF-α was at significantly higher concentrations in COPD patients.
Chemiluminescence
Chemiluminescence (CL) is one of the most attractive methods with a number of clear advantages, such as its high sensitivity, wide linear range, the simplicity of the instrumentation used, and the lack of interference from background scattered light [126]. Pasha et al. [108] determined NO2−/NO3− levels in the EBC of mild persistent asthmatic patients treated with a low dose of fluticasone propionate/salmeterol (FSC) by initial conversion of NO2−/NO3− to NO and then NO was measured by a gas-phase chemiluminescence reaction between NO and ozone. They reported a rapid reduction in airway inflammation and airway hyper-responsiveness in asthmatic patients following a week of low-dose combination therapy with FSC. Furthermore, Hussain et al. [109] used the NO analyzer for the determination of NO2−/NO3− levels in subjects with asthma. A similar study for NO2−/NO3− determination was performed by Arcêncio et al. [110] for the EBC of patients admitted for heart valve surgery. They reported that in patients with postoperative respiratory complications, the postoperative levels of NOx were significantly higher in EBC from the fourth postoperative hour as compared to those who experienced uneventful postoperative periods. Matsunaga et al. [111] used a CL-based membrane protein array for a simultaneous analysis of cytokine expression in asthmatic subjects. The results showed that IL-4, IL-8, IL-17, TNF-α, RANTES, IFN-γ-inducible protein 10, TGF-β, macrophage inflammatory protein (MIP) 1α, and MIP-1β exhibited significantly upregulated expression in asthmatic airways compared to those of healthy subjects. Lázár et al. determined ATP in the EBC of COPD [56] and asthma [127] patients by using the luciferin–luciferase assay. Luciferase is an enzyme that oxidizes luciferin in the presence of ATP. During the reaction, light is produced and it can be detected by using a luminometer. They reported that the ATP concentration was similar in COPD, asthma, and non-smoking and smoking healthy individuals. Chen et al. [112] used a CL microparticle immunoassay for the determination of CEA in EBC samples collected from patients with NSCLC and healthy individuals. They demonstrated that the CEA levels in the EBC of the NSCLC group were higher as compared to those of the healthy group.
Electrochemical methods
Electrochemical sensors take a biological input and convert it to an electrical signal. In the case of electrochemical sensors for breath analysis, the electrical current produced on the sensor electrode is directly proportional to the concentration of the chemical in the sample. Some reported studies that used electrochemistry methods in EBC are summarized in Table 3, and the following text provides a brief explanation for each applied method:
Effros [128] and Zacharasiewicz [129] used ion-selective electrodes (ISE) for the determination of sodium, potassium, and chloride ions in the EBC of subjects with OSAS, asthma, and CF. Electrochemical sensors for other small molecules in the breath, such as lactate, have also been developed. Karyakina et al. [130] reported a flow-injection (FI) electrochemical system coupled with an ion-exchange pre-concentration column (filled with Strata SAX sorbent-silica gel with quaternary ammonium substituents) for lactate sensing in the EBC of pulmonary patients. The lactate concentration was at the level of (1.5–3) × 10−4 mol L−1 for both healthy subjects and pulmonary patients.
These types of sensors offer the possibility of miniature or hand-held sensing capabilities; but so far, they have been limited to the detection of one or a few compounds of interest in biological samples. Melker et al. [133] developed electrochemical- or coulometric-based sensing or monitoring devices to analyze EBC for quantifying glucose concentrations in patients with severe respiratory distress. They found that the concentrations of glucose in the EBC were correlated to the glucose concentrations in the individual subject’s body, in particular in blood, and suggested that the developed devices could be applied to improve prognosis and/or reduce the adverse side effects associated with a disease state or condition in a subject. Karyakin et al. [131] also used an electrochemical sensor for monitoring the glucose level in the EBC of diabetic patients. They reported that breath condensate glucose levels correlated positively with blood glucose levels. Carlsen et al. [134] and Bikov et al. [132] investigated the effect of physical exercise on EBC pH during the development of exercise-induced bronchoconstriction (EIB) in asthmatic individuals. They reported that the decrease in EBC pH was related to the development and severity of EIB, thereby supporting the causal role of airway pH in EIB.
Separation methods
The detection and quantification of extraordinarily low concentrations of non-volatile biomarkers/compounds in EBC requires highly sensitive analytical methods. During the last decade, separation methods have become the method of choice for the trace analysis of various compounds contained in complex biological matrices. In order to achieve such a relatively low detection limit, it is often necessary to incorporate pre-concentration steps (solid-phase extraction, lyophilization, etc.). A number of separation methods developed for the analysis of non-volatile biomarkers/compounds in the EBC of pulmonary patients have been extracted from the literature, and they are classified and explained in brief (Table 4).
Chromatography
Ion chromatography
Ion chromatography (IC) is a sensitive and well-tested separation method that allows the determination of multiple anions or cations in a time scale of minutes, and no sample preparation is needed for making condensate samples. A great advantage of IC is that cations or anions can be separated and quantified simultaneously. An IC method with UV detection was reported for the determination of NO2−/NO3− [103] in well-controlled asthma patients by Chladkova et al.; they reported that the mean level of NO2−/NO3− in the EBC of healthy subjects and patients did not differ. An IC method with conductivity detection was reported for the determination of sodium and potassium [135] in the EBC of healthy volunteers by Svensson et al.; they found that the level of sodium decreased during the day, while the levels of potassium fluctuated.
Greenwald et al. developed an IC method for the simultaneous measurement of EBC’s ionic composition, including inorganic anions, cations, and organic acids [172], before and after exercise in adolescent athletes. They reported that exercise resulted in a decrease and an increase in the concentration of propionate and urea, respectively. The source of this variation is gas-phase diffusion from epithelial and oral surface liquids.
In addition, it is possible to determine ammonium by using IC [172], which may be valuable in the determination of other biomarkers in EBC, for example, pH. Normally, the pH of EBC is within the range of 7–8, typical of that for human blood. Any decreases in pH that are observed in some lung disorders largely reflect the effects of these diseases on the production of NH3 in the mouth and the efficiency with which NH3 is collected in the condenser. NH3 is derived principally from the catalytic degradation of urea in the mouth and it is delivered as ammonia gas in the air exhaled to the condenser. NH3 is trapped as NH4+ in the condenser. It is therefore unlikely that the EBC pH will provide a reliable index of the change in the lung pH [135].
Liquid chromatography
Liquid chromatography (LC) with various applicable detectors is an analytical method used to separate, identify, and quantify each component in a mixture. The simplest LC method uses isocratic reversed-phase high-pressure liquid chromatography (RP-HPLC) and UV absorbance detection. Montuschi et al. used RP-HPLC-UV for the determination of LTB4 in the EBC of subjects with different lung diseases to qualitatively validate an EIA to measure LTB4 [136]. Folesani et al. [137] reported a HPLC-UV method for the determination of urea as a normalization factor for non-volatile biomarkers/compounds in EBC. They measured urea EBC concentrations in different clinical conditions and reported that the concentrations were unaffected by the three chronic airway diseases examined—COPD, asthma, and CF. Csoma et al. [138] determined adenosine in the EBC of both asthmatic and control subjects by using a HPLC-UV method. They indicated that physical exercise resulted in bronchoconstriction along with a significant increase of adenosine levels in the EBC of asthmatic patients, but not in that of the healthy subjects. Lázár et al. determined ATP in the EBC of COPD patients [56] to qualitatively validate a luciferin–luciferase fluorometric assay.
However, the main drawback of HPLC-UV methods is the lack of adequate selectivity and sensitivity. For compensation, usually a sample preparation step is applied prior to the injection of the biological sample into the system. Khoubnasabjafari et al. [10] used a liquid–liquid extraction (LLE) procedure to extract/pre-concentrate methadone from the EBC of patients receiving methadone maintenance treatment (MMT) prior to sample injection of HPLC-UV. In a similar study [11], they used two amplified sample preparation procedures, namely dispersive liquid–liquid microextraction (DLLME) and ultrasonic liquid–liquid microextraction (ULLME). They reported a good correlation between the methadone concentration measured in patients and the daily intake of methadone (R = 0.997) by using the developed method.
Compared to a UV detector, FD may be applied as a selective detector for HPLC methods. Rihák et al. [139] measured the levels of biomarkers of nitrosative stress (i.e., NO2− and NO3−) in the EBC of adult patients of asthma, COPD, and idiopathic pulmonary fibrosis (IPF) by using HPLC-FD. They reported that NO2− concentration increased in adult corticosteroid-naive patients with asthma, active IPF, and exacerbation of COPD, whereas in stable COPD, its concentration was comparable to that in healthy subjects.
Electrochemical detection (ECD) with HPLC has the potential to be more selective than the HPLC-UV or HPLC-FD methods. Celio et al. [36] used a HPLC-ECD method for the determination of 3-NT in the EBC of children with asthma, CF, and healthy controls. However, they reported that this method was not suitable for the analysis of free 3-NT in EBC because many of the samples showed concentration levels close to or below the detection limit.
As already described, due to low selectivity of the above-mentioned HPLC detectors, these methods are unable to detect concentrations of non-volatile biomarkers/compounds of interest and require complicated and time-consuming pre-treatment procedures to eliminate interfering substances from the samples. One of the analytical challenges of the HPLC analysis of biological samples is to obtain the necessary selectivity. One straightforward way to achieve this is to couple HPLC with a MS method. This combines the flexibility of LC separation with the robust and unambiguous identification of the MS instrument, especially when used in the MS/MS mode [173]. The sensitivity, selectivity, and superior ability to separate and detect low concentrations, i.e., parts per billion (ppb) and parts per trillion (ppt), of the chemicals offered by MS are likely to be instrumental in the future development of diagnostic biomarker methods for EBC.
Furthermore, LC-MS offers an ideal method for the simultaneous detection of hundreds or even thousands of compounds that differ greatly in size and polarity in the same EBC sample. Other methods of detection of breath compounds, such as some immunoassays and sensors, are very specific for the detection of only one compound. Therefore, LC-MS is considered to be the gold standard, especially for determining low-molecular-weight non-volatile compounds in human breath [174], since they are highly specific and generally sufficiently sensitive. For example, for the analysis of 3-NT in EBC, the highest sensitivity was obtained by using tandem MS. Baraldi et al. [32] measured 3-NT by LC-MS/MS in isotopic dilution in the EBC of asthmatic and healthy children. They reported that 3-NT formation was high in asthmatic children, indicating that nitrosative processes were more active in the lungs of asthma patients.
Sometimes, the limit of detection (LOD) and the limit of quantitation (LOQ) are inadequate, even by the LC-MS methods, to allow a quantitative determination of biomarkers in most biological samples. In order to improve sensitivity, solid-phase extraction (SPE) needs to be used for sample clean-up and pre-concentration prior to analysis. Göen et al. [33] used a clean-up and pre-concentration step before LC-MS/MS for 3-NT measurement. SPE was performed using C18 POLAR RP cartridges with reverse-phase material. Montuschi et al. [140] also used two coupled methods, i.e., ion trap LC-MS and LC-MS/MS, for measuring LTB4 in the EBC of asthmatic patients on anti-inflammatory treatment and asthmatic patients who were not on anti-inflammatory drugs with LTB4-d4 as the internal standard. They reported that exhaled LTB4 was detected only in the asthmatic patients who were not on anti-inflammatory therapy. Other studies performed by LC-MS methods include the determination of LTB4 [141], 8-isoprostane [142, 175, 176], the profile of eicosanoid lipid mediators [143, 144], adenyl purines (ATP, AMP) [145], CML [67], O-Tyr [146], lactate [147], amino acids [148], fatty acid metabolites (9,12,13-trihydroxyoctadecenoic acid (9,12,13-TriHOME), 9,10,13-TriHOME, 12,13-dihydroxyoctadecenoic acid (12,13-DiHOME), 12-hydroxyeicosatetraenoic acid (12-HETE), 12(13)-epoxy octadecanoic acid (12(13)-EpOME)) [149], proteins [150], methadone [151], and proteomic and metabolomic studies [152], which along with some of their analytical details are listed in Table 4.
Hydrophilic interaction liquid chromatography (HILIC) as a variant of normal-phase liquid chromatography provides an alternative approach to effectively separate small polar compounds at polar stationary phases [177]. Like normal-phase LC, HILIC employs traditional polar stationary phases [178], but the mobile phase used is similar to those employed in the reverse-phase LC mode [179]. HILIC also allows the analysis of charged substances, as in IC. Some of the reported studies on EBC for the determination of non-volatile biomarkers/compounds with this method are the simultaneous determination of 3-NT and its precursor Tyr and also trans-hydroxyproline and its precursor proline in EBC as markers of nitrosative/inflammatory stress as well as fibrotic alterations in the lung in the EBC of smokers and healthy subjects [153], and the simultaneous quantifications of CML and lysine as a precursor of CML in the EBC of patients undergoing dialysis [154].
Most HPLC instrument and column manufacturers have introduced ultra-high-pressure liquid chromatography (UHPLC) in recent years [180]. UHPLC substantially enhances performance over conventional HPLC and it is particularly attractive in method-development situations, which demand quick run time and rapid responses to changes in column/mobile-phase conditions [181]. Some measurements for biomarkers in EBC have been performed using this method, including glucose quantification in the EBC of cystic fibrosis-related diabetes (CFRD) patients [155] with three MS-based methods: UHPLC coupled to either time-of-flight (TOF) MS or triple quadrupole (QqQ) tandem MS (MS/MS) and traveling wave ion mobility spectrometry (TWIMS) with TOF-MS detection, Arg metabolome with a UHPLC-MS/MS method enriched online in a trap column [58] in the EBC of asthmatic adolescents, and metabolic patterns with UHPLC coupled with high-resolution mass spectrometry (HRMS) [156] in the EBC of patients suffering from shock with acute respiratory failure in a pilot study.
Metabolomics is a powerful method that provides metabolic patterns from a combination of small molecules. The analytical methods detect metabolites across a large spectrum of concentrations, polarities, and masses [182,183,184]. The metabolome may reflect the evolution of physiological states in response to environmental variations or aggressions, such as microbial infections. These approaches enable the semi-quantification of metabolites up to 1500 Da, including organic acids, lipids, amino acids, carbohydrates, peptides, vitamins, steroids, xenobiotics, and many others.
Gas chromatography
Gas chromatography (GC) is a common type of chromatography used for separating and analyzing compounds that can be vaporized without decomposition. GC coupled with MS is very useful for analyzing small molecules with molecular masses of up to about 1000 Da. The GC front end allows for pre-separation of chemicals prior to MS identification. The signal-to-noise ratio (S/N) can be increased by several times by using fluorine-containing derivatization agents and ionization conditions such as negative ion electron capture (NIEC) [173].
However, one challenge associated with the GC-MS analysis of breath is the removal of water from the EBC samples, as its presence could damage the capillary column of GC. So, human breath traditionally requires the isolation and separation of biomarker chemicals from the background. By taking advantage of the polarity of the extractant, LLE can be used to separate compounds from the aqueous matrix before GC-MS characterization.
Alternatively, SPE can be used to concentrate the EBC components and remove matrix interfering components [185]. Peralbo-Molina and his co-workers reported a method for an untargeted metabolomics analysis of EBC in healthy subjects based on GC-TOF-MS profiling in a high-resolution mode. Two different sample preparation methods, i.e., LLE and SPE, were compared for analyzing this biofluid. They found that LLE provided more information on EBC composition [157]. Sanak et al. [158] used GC-negative ion chemical ionization (NICI)-MS for a targeted lipidomics analysis of EBC in healthy subjects. They measured 20 different eicosanoid compounds, representing major arachidonic acid lipoxygenation and cyclooxygenation pathways, by this method. Since these mediators are non-volatile, the EBC extracts were prepared by a three-step derivatization to pentafluorobenzyl ester, trimethylsilyl esters, and methoxyoxime, which modified the carboxyl, hydroxyl, and keto groups of eicosanoids.
Other biomarkers measured by GC-MS include 3-NT [34,35,36], 8-isoprostane [159, 186], LTB4, Cys-LTs [49], TMA [187], and fatty acids [160] (see Table 4).
Electrophoresis
Capillary electrophoresis
Capillary electrophoresis (CE) is a family of electrokinetic separation methods performed with submillimeter diameter capillaries and in micro- and nano-fluidic channels. CE surpasses other analytical methods in terms of separation efficiency, short analysis time, high resolution, low sensitivity to sample matrix, and low consumption of sample (about 10–20 nL), solvents, and energy [188].
In the context of CE, different detectors have been reported for determining non-volatile biomarkers/compounds in EBC. Some of the used detectors are reviewed here:
-
CE system with diode array detection (DAD): Due to a high rate of data collection, DAD is superior over single-wavelength detection. It is proven that DAD detection can help in developing separation methods, identifying peaks according to their UV-visible spectra, and checking peak purity [189]. Hamidi et al. [14] used CE-DAD in stacking mode for the determination of methadone in the EBC of patients receiving MMT by direct injection of EBC samples. In another study [15], they also used an electro-driven separation method for the quantification of methadone enantiomers in patients receiving racemic methadone. They found no significant differences in the concentrations of R- and S-methadone in the investigated EBC samples, thereby revealing no stereo-selective penetration of methadone from systemic blood flow to the lung lining fluid. In this study, the inter-correlation of methadone concentrations between EBC and serum or urine was also investigated and a relatively poor correlation was reported between the methadone levels in EBC and those in the serum (R = 0.45) or urine (R = 0.44) samples.
-
CE system with contactless conductivity detection (C4D): C4D is one of the best detection modes for the analysis of compounds with low molecular weight. Greguš et al. [161] used a CE-C4D system for an ionic profile analysis of EBC from a single breath. They reported that the breathing pattern had a significant impact on the concentration of analytes in the collected EBC. As the ventilatory pattern can be easily controlled during a single exhalation, conducting the analysis for a single breath provides a method with applicability in point-of-care diagnostics. In another study, this research group developed a portable CE-C4D system for an ionic profile (of nitrosative stress markers, including NO2− and NO3−) analysis in EBC from a single exhalation [162]. A miniature EBC sampler connected online was used to collect EBC, which was analyzed immediately after collection. The instrument was lightweight (< 5 kg), and all the necessary parts were placed in a plastic brief-case, allowing for the hydrodynamic injection of small sample volumes (10 μL), and could continuously operate for at least 10 h, with peak area repeatability below 5%. This method presents a fast screening tool that can be applicable in clinical practice. Kubáň et al. [163] used a CE-C4D for the separation of oxalate, formate, and glycolate as the toxic metabolites after methanol and ethylene glycol intoxication in the EBC of people with suspected intoxication. They found that the EBC of healthy individuals contained small amounts of the analytes, all within physiological ranges. However, in all the samples of the patients intoxicated with methanol, elevated concentrations of formate (8.6–16.6 mmol L−1) were found.
The significant advantage of CE is its ability to analyze anions and cations simultaneously in a single run by applying dual-opposite injection capillary electrophoresis (DOI-CE) [190]. DOI-CE is a separation method that utilizes both ends of the capillary for sample introduction. For example, Greguš et al. [164] reported an analysis of 14 ions (inorganic anions, cations, and organic acids) with a DOI-CE-C4D method in EBC samples obtained from patients with various respiratory diseases (COPD, asthma, pulmonary fibrosis, sarcoidosis, and CF) in less than 5 min. Kubáň et al. [165] also reported the analysis of ionic contents of EBC in less than 2 min with a DOI-CE-C4D method. It has been shown that changes in ion concentrations could be observed in acute inflammation of the upper airways and in patients diagnosed with mild COPD. Furthermore, they suggested that lactate concentrations could also be monitored and an approximately fourfold increase of lactate concentration in EBC was determined following an exhausting cycling exercise.
It is worth mentioning that small molecules such as chloride, sodium, potassium, and small organic acids are not considered as biomarkers of pulmonary diseases, but contribute, for instance, to the neutrality of the EBC, pH, and dilution standardization [16]. However, their determination of EBC is important.
-
CE system with laser-induced fluorescence (LIF) detection: LIF is another CE detector used for EBC analysis. LIF is much more widespread among CE methods because it can achieve very low LODs. Hodáková et al. [166] have described the use of a 515 nm green laser module and CE-LIF for the quantification of GSH in EBC. Eosin-5-maleimide (EMA) is used as a fluorescent tag for GSH derivatization. They reported that this method could quantify GSH in as little as 20 μL of EBC in less than 3 min.
Gel electrophoresis
Gel electrophoresis is a method for the separation and analysis of macromolecules (DNA, RNA, and proteins) and their fragments based on their size and charge. The gel is typically made of agar or polyacrylamide [191]. Gel electrophoresis is used for analytical purposes, often after the amplification of DNA via polymerase chain reaction (PCR), but may also be employed as a preparative method prior to the use of other methods, such as MS, restriction fragment length polymorphism (RFLP), PCR, cloning, and DNA sequencing. Griese et al. [167] reported a two-dimensional gel electrophoresis (2-DE) method for a protein pattern analysis of the EBC of healthy subjects. 2-DE is a form of gel electrophoresis commonly used to analyze proteins. 2-DE begins with electrophoresis in the first dimension and then separates the molecules perpendicularly to the first dimension to create an electropherogram in the second dimension. Comparing the spot pattern observed in EBC to the proteome observed in bronchoalveolar lavage fluid, it can be said that the proteins in EBC mirror those present in ELF.
Gel electrophoresis may be coupled with other separation methods; this combination of sensitive methods enables the identification of potential biomarkers in biological samples. For example, a combination of 1-DE/2-DE/μ-HPLC/MS methods for protein profile analysis of EBC from patients with pulmonary emphysema associated whit α1-antitrypsin deficiency (AATD) [17], gel electrophoresis coupled with MS/MS for keratin content detection in the EBC of healthy smokers [168], gel electrophoresis coupled with MS for proteomic characterization of healthy subjects [169], gel electrophoresis coupled with MALDI/TOF-MS for cytokeratin analysis in patients with ALI/ARDS [170], and gel electrophoresis (SDS-PAGE) followed by Western blot (WB) and surface-enhanced laser desorption ionization (SELDI)-MS for the detection and validation of several inflammatory cytokines (IL-1α, IL-1β, IL-2; IL-12, α, and β subunits, IL-15, interferon α and γ, TNF α), type I and II cytokeratins, two SP-A isoforms, calgranulin A and B, and α1-antitrypsin in the EBC of non-smokers and healthy smokers, COPD patients without emphysema, and subjects with pulmonary emphysema associated with AATD [171].
Other methods
Ion mobility mass spectrometry
Mass spectrometry (MS) is an analytical method that ionizes chemical species and sorts the ions on the basis of their mass-to-charge ratio. In addition to its application coupled with other analytical methods, it can also be used as an independent method, known as ion mobility mass spectrometry, for the analysis of non-volatile biomarkers/compounds in EBC. Zang et al. [192] reported transmission-mode direct analysis in real time (TM-DART)-TWIMS-TOF-MS as a feasible approach and a high-throughput alternative to the conventional direct infusion (DI), ESI, and atmospheric pressure chemical ionization (APCI) methods for metabolomics studies of EBC samples. They found that multivariate analyses of the resulting TM-DART-TWIMS-TOF-MS datasets could successfully differentiate between EBC samples from CF patients and healthy controls.
Polymerase chain reaction-based assays
Polymerase chain reaction (PCR) is a relatively simple and inexpensive tool used in molecular biology to amplify a single copy or a few copies of a DNA segment across several orders of magnitude, generating thousands to millions of copies of a particular DNA sequence. PCR is used every day to diagnose diseases, identify bacteria and viruses, match criminals to crime scenes, and in many other ways [193]. A PCR-based assay may also be used for diagnostic purposes pertaining to EBC samples. Some of these studies include the detection of human DNA in the EBC of patients with NSCLC and healthy volunteers with PCR followed by Gel Doc System (Bio-Rad) analysis [194], PCR followed by laser fluorescence in patients with NSCLC as per Carpagnano [195], IS6110 repetitive DNA element of Mycobacterium tuberculosis in patients with newly diagnosed active pulmonary tuberculosis [196], fungal DNAc in lung transplant recipients and lung microbiota in patients with ventilator-associated pneumonia (VAP) [197, 198], human papillomavirus (HPV) in patients with lung cancer [199], miR-570-3p as a potential regulator of asthmatic inflammation in asthmatic patients [200], Let-7a in patients with COPD [201], and mitochondrial DNA mutations in patients with lung cancer [202]; the merits of the methods applied for different analytes of interest are tabulated in Table 5.
Nanoparticle-based methods
The application of nanotechnology has enormous potential to greatly influence our world and improve the quality of human life. Plasmonic and paramagnetic nanoparticles, quantum dots, nanoshells, and others are some of the nanoparticles used as contrast agents, fluorescent materials, or molecular research tools for different medical aspects, such as diagnostics and therapeutics, owing to their unique optical, electrical, and mechanical properties [213]. Some studies have reported the detection of biomarkers in EBC with nanotechnology-based methods. For example, Melker et al. [214] used nanoparticle-based assembly systems for the diagnosis of different physical conditions or disease/disorder states. A nanoparticle-based assembly comprises a nanotube, a surrogate marker, and the means for detecting a specific chemical entity (SCE) consisting of an antibody, a protein, and an aptamer. The identification of an SCE by this novel way results in the release of the surrogate marker from the nanoparticle. Since the surrogate marker is released from the nanoparticle only in the presence of an SCE, the detection of the surrogate marker indicates that the SCE is present in the EBC sample and, consequently, enables the diagnosis of the specific condition, disorder, or disease. The SCE can be found in a broad range of analytes including steroids, viruses, α-fetoprotein, isoprene αII-spectrin breakdown products, and isoprostanes in various pulmonary diseases. In another work [215], this research group used the same system for the determination of a nucleic acid, a protein, an illicit drug, an explosive, a toxin, a pharmaceutical, a carcinogen, a poison, an allergen, and an infectious agent in body fluids including blood and EBC samples. As we know, the most popular molecular recognition agent is an aptamer, which is a highly specific nucleic acid-based ligand that is highly selective for a target analyte/biomarker. Thus, the proposed systems include aptamers in combination with nanotubes attached to signaling agents to provide the means for detecting, signaling, and/or quantifying virtually any compound of interest in EBC.
Moreover, nanoparticle-based methods can be used for monitoring drugs in EBC samples. Recently, our research group, with the aim of conducting a systematic study on drug analysis in EBC samples, used amidosulfonic acid-capped silver nanoparticles (ASA-AgNPs) for the determination of lamotrigine (LTG) in the EBC of epileptic patients undergoing LTG treatment [12]. The method is based on the visual color changes of ASA-AgNPs from yellow to red to violet due to LTG-induced aggregation of nanoparticles. We have also developed an AgNPs-enhanced terbium fluorescence method for quantifying deferiprone (DEF) in the EBC of patients undergoing DEF treatment [13]. Since AgNPs significantly improve the fluorescence intensity of the terbium-DEF system, it allows for the quantification of DEF at very low levels (60 μg L−1).
Surface acoustic wave immunosensors
Surface acoustic wave (SAW) sensors are a class of microelectromechanical systems (MEMS) that rely on the modulation of surface acoustic waves to sense a physical phenomenon. SAW as a piezoelectric sensor is a well-performing mass sensing device for label-free immunoassay due to its attractive advantages, including real-time monitoring and simplicity of use [216]. Zhang et al. [64] reported a SAW immunosensor for the detection of CEA in the EBC of cancer patients. A conventional sandwich immunoassay using AuNPs–antibody conjugates and subsequent mass enhancement with gold staining solutions was utilized. In the developed SAW immunosensor, CEA mixed with gold nanoparticles (AuNPs)–antibody conjugates was first recognized by the capture antibody immobilized on the sensor surface; then the sensitivity was enhanced by injecting the gold staining solution. The response of the immunosensor was proportional to the CEA concentration. In another study, this research group [203] reported a miniaturized SAW immunosensor with great ability for automatic and online detection of CEA in EBC as compared to the previous version. The detection approach was the same and was based on a sandwich immunoassay using an antibody labeled with AuNPs and, subsequently, mass enhancement with the use of gold staining solutions was integrated onto the SAW sensor surface. The reported cut-off value for the CEA concentration in EBC to distinguish between lung cancer patients and healthy subjects is 1.85 ng mL−1 [66]. Since the detection limit of the presented method is less than the cut-off value, this immunosensor could be successfully used for CEA detection in EBC.
High electron mobility transistors
High electron mobility transistors (HEMT), which is also known as a heterostructure field-effect transistor (HFET) or modulation-doped FET (MODFET), is a field-effect transistor that incorporates a junction between two materials with different band gaps (i.e., a heterojunction) as the channel instead of a doped region. Aluminum gallium nitride (AlGaN)/GaN HEMT is an extremely stable system chemically and includes a high electron sheet carrier concentration channel induced by the piezoelectric polarization of the strained AlGaN layer and spontaneous polarization. Positive countercharges at the HEMT surface layer are induced by the two-dimensional electron gas cloud located at the AlGaN/GaN interface. Any slight change in ambient conditions can affect the HEMT’s surface charge, thus changing the electron concentration in the channel at the AlGaN/GaN interface [204]. HEMT sensors have response times of seconds and are probably the cheapest sensing technologies available today. Chu et al. [205] used an AlGaN/GaN HEMT sensor for measuring pH and glucose in EBC for an investigation related to airway pathology. They designed the sensor as a portable, wireless package for remote monitoring applications. Data from the sensor is sent wirelessly and can be recorded by any device that has an appropriate receiver. Chu et al. [204] and Ren et al. [217] also reported a ZnO nanorod-gated HEMT sensor with immobilized glucose oxidase for detecting glucose in EBC. Furthermore, Chu et al. [204] demonstrated that depending on the immobilized material, HEMT-based sensors can be used for sensing different materials. They used a HEMT sensor immobilized on a thin film of AgCl for the determination of chloride ion and a Sc2O3-gated AlGaN/GaN HEMT sensor for measuring pH in the EBC of diabetic patients. This technology offers the possibility of biomarker detection in EBC without the need for clinical visits.
Nuclear magnetic resonance-based metabolomic analyses
Nuclear magnetic resonance (NMR) spectroscopy is one of the most powerful methods to provide an overall biochemical profile of low-molecular-weight endogenous metabolites in biological fluids [206], including amino acids, polar/nonpolar metabolites, sugars, and large metabolites. This method enables the characterization of the most represented proton-containing compounds, both known and unknown metabolites as well as novel biomarkers, and their representation in a spectrum, thereby providing a metabolic fingerprint of the analyzed sample that may provide insights into disease mechanisms. Multivariate statistical methods can be applied to extract information from these complex NMR spectra [218]. NMR-based metabolomics has several advantages over other methods such as MS. NMR requires little pre-treatment of samples; it is also rapid (10–15 min), non-invasive, nondestructive, and provides highly reproducible results [219,220,221].
A wide range of NMR-based metabolomics studies have been performed on EBC samples and all of them have shown a clear discrimination between the NMR spectra of patients and healthy individuals. Some of these studies are listed in Table 5, including the metabolomic analysis for discriminating between children with asthma and healthy children by Carraro et al. [206]; discrimination of healthy subjects, laryngectomized, and COPD patients in three separate groups by de Laurentiis et al. [207]; discrimination of obese asthmatic (OA) patients and patients independently affected by asthma or obesity by Maniscalco et al. [222]; discrimination of COPD and OSAS by Ząbek’s research group [223]; discrimination of obese and lean subjects by Paris’ research group [208]; asthmatic patients by Motta et al. [209]; and CF subjects compared to healthy subjects by Montuschi et al. [210]. Some pilot studies were also undertaken by Airoldi et al. [211] with the aim to differentiate AATD patients, who were diagnosed with moderate to severe emphysema, from healthy individuals and by Ahmed [212] for the identification of metabolic biomarkers of lung cancer with NMR-based metabolomic analysis.
Critical points for EBC analysis methods
The main advantages of EBC as an alternative biological sample were reviewed in a short work recently [224]. The simpler matrix of EBC as compared to other biological sample provides more facilities for an analyst to apply various pre-concentration methods that are required for most analytes due to their very low concentrations in EBC.
All the quantification methods used for EBC analysis have their particular strengths and weaknesses. Although the optical and electrochemical methods are simple, low cost, and portable (in most cases), the main limitations of these methods include low sensitivity, low specificity, and sample throughput for screening applications in routine laboratories. Immunochemical methods (fluoroimmunoassay, ELISA, and EIA kits) as semiquantitative methods are also subject to inherent uncertainties in selectivity. Lack of selectivity and poor reproducibility/repeatability of electrochemical methods should be considered during their clinical applications. Moreover, most of the above-mentioned methods require a large sample volume depending on the selected analytical method and can only analyze one analyte at a time. Sequential assay processes could be conducted by highly specific analytical methods such as HPLC, GC, and CE instruments with different mentioned detectors for high-throughput applications. The spectrophotometric, spectrofluorimetric, or electrochemical methods cannot compete with the separation methods. However, HPLC and GC methods are more time-consuming and need an extra step for sample preparation prior to injecting the sample into the system. The possibility of directly injecting EBC and the ability to analyze minute sample volumes (< 10 nL) into a CE system is an important characteristic for this analytical method. Online pre-concentration of analytes in CE provides further advantages that could cover for the low sensitivity of CE systems. However, as a separation method, CE has provided less successful results compared to HPLC methods and is not as robust as HPLC. In contrast to HPLC, CE methods can be made portable and can thus be used for point-of-care analysis. MS is a key tool for the selective and sensitive detection of biomarkers at trace levels in biofluids and MS is preferred as the detection section for most methods because of its unambiguity in identification. This hyphenated analytical method has been proved to be highly selective, reproducible, and free from artifacts. GC/MS provides excellent separation and detection, but its applications are relatively few, because most of the investigated compounds are non-volatile; so, a derivatization step is needed that prolongs analysis time. As an alternative to LC, post-ionization gas-phase separation via ion mobility mass spectrometry has shown great promise for analysis due to its ability to separate isobars. High electron mobility transistors-based sensors, which were introduced in the last decades, have high precision, compact size, fast response time, and sensitive to small amounts of biological material. These have potential for point-of-care applications or on-field measurements in order to reduce medical costs and emergency room visits.
Nanoparticle-based method, NMR-based analysis, and SAW-immunosensors could be promising developments for the future of EBC analysis. Recent research has focused on developing innovative nanomaterials and to control their properties to meet the needs of specific applications. The power and scope of such nanomaterials can be improved by coupling with other analytical methods, such as electrical or optical readout protocols. NMR-based analysis being a very new and expensive method is still applied as a diagnostic approach (e.g., for the discrimination of patients from healthy controls) because of poor understanding of disease processes at the metabolic level.
Conclusion
The analysis of EBC that well reflects the composition of the airway surface liquid may provide information about inflammation, oxidative stress, and other conditions (e.g., metabolic disorders, bacterial and viral infections) in the lungs. The detection and quantification of non-volatile biomarkers related to various diseases could help in classifying the severity and type of disease and could be also used for the diagnosis as well as the monitoring of therapy of these diseases. Since many different types of methods are available for breath analysis, the selection of an instrumentation platform for a given application will be easy if the respective merits and limitations of each of the methods are considered carefully. The goal of this review was to provide an overview of the various methods used for the determination of non-volatile biomarkers/compounds in the EBC of patients.
References
Yates DH, Krishnan A, Chow S, Thomas PS. Non-invasive assessment of exhaled biomarkers in lung transplantation. J. Breath Res. 2011;5:024001.
Hunt J. Exhaled breath condensate: an evolving tool for noninvasive evaluation of lung disease. J Allergy Clin Immunol. 2002;110:28–34.
Chow S, Yates DH, Thomas PS. Reproducibility of exhaled breath condensate markers. Eur Respir J. 2008;32:1124–6. https://doi.org/10.1183/09031936.00085408.
de Paiva MJN, Menezes HC, de Lourdes Cardeal Z. Sampling and analysis of metabolomes in biological fluids. Analyst. 2014;139:3683–94. https://doi.org/10.1039/C4AN00583J.
Effros RM, Biller J, Foss B, Hoagland K, Dunning MB, Castillo D, et al. A simple method for estimating respiratory solute dilution in exhaled breath condensates. Am J Respir Crit Care Med. 2003;168:1500–5. https://doi.org/10.1164/rccm.200307-920OC.
Johnson GR, Morawska L. The mechanism of breath aerosol formation. J Aerosol Med Pulm Drug Deliv. 2009;22:229–37. https://doi.org/10.1089/jamp.2008.0720.
Hunt J. Exhaled breath condensate: an overview. Immunol Allergy Clin. 2007;27:587–96. https://doi.org/10.1016/j.iac.2007.09.001.
Mutlu GM, Garey KW, Robbins RA, Danziger LH, Rubinstein I. Collection and analysis of exhaled breath condensate in humans. Am J Respir Crit Care Med. 2001;164:731–7.
Sepehr B, Bavili-Tabrizi A, Jouyban-Gharamaleki V, Khoubnasabjafari M, Jouyban A. A sensitive determination of ammonia and nitrite in exhaled breath condensate of healthy humans by using berthelot reaction. Curr Pharm Analysis. 2017;13 In press.
Khoubnasabjafari M, Jouyban A, Ansarin K, Jouyban-Gharamaleki V, Panahi-Azar V, Hamidi S, et al. Methadone concentrations in exhaled breath condensate, serum and urine of patients under maintenance treatment. Iran J Pharm Res. 2017;16:1621–30.
Khoubnasabjafari M, Ansarin K, Jouyban-Gharamaleki V, Panahi-Azar V, Shayanfar A, Mohammadzadeh L, et al. Extraction and analysis of methadone in exhaled breath condensate using a validated LC-UV method. J Pharm Pharm Sci. 2015;18:207–19. https://doi.org/10.18433/J3WK65.
Jouyban A, Samadi A, Khoubnasabjafari M, Jouyban-Gharamaleki V, Ranjbar F. Amidosulfonic acid-capped silver nanoparticles for the spectrophotometric determination of lamotrigine in exhaled breath condensate. Microchim Acta. 2017;184:2991–8. https://doi.org/10.1007/s00604-017-2325-x.
Mohamadian E, Shayanfar A, Khoubnasabjafari M, Jouyban-Gharamaleki V, Ghaffary S, Jouyban A. Analysis of deferiprone in exhaled breath condensate using silver nanoparticle-enhanced terbium fluorescence. Anal Methods. 2017;9:5640–5.
Hamidi S, Khoubnasabjafari M, Ansarin K, Jouyban-Gharamaleki V, Jouyban A. Direct analysis of methadone in exhaled breath condensate by capillary zone electrophoresis. Curr Pharm Anal. 2016;12:137–45.
Hamidi S, Khoubnasabjafari M, Ansarin K, Jouyban-Gharamaleki V, Jouyban A. Chiral separation of methadone in exhaled breath condensate using capillary electrophoresis. Anal Methods. 2017;9:2342–50. https://doi.org/10.1039/c7ay00110j.
Kubáň P, Foret F. Exhaled breath condensate: determination of non-volatile compounds and their potential for clinical diagnosis and monitoring: a review. Anal Chim Acta. 2013;805:1–18. https://doi.org/10.1016/j.aca.2013.07.049.
Fumagalli M, Dolcini L, Sala A, Stolk J, Fregonese L, Ferrari F, et al. Proteomic analysis of exhaled breath condensate from single patients with pulmonary emphysema associated to α1-antitrypsin deficiency. J Proteome. 2008;71:211–21. https://doi.org/10.1016/j.jprot.2008.03.002.
Rosso MI, Roark S, Taylor E, Ping X, Ward JM, Roche K, et al. Exhaled breath condensate in intubated neonates-a window into the lung’s glutathione status. Respir Res. 2014;15:1. https://doi.org/10.1186/1465-9921-15-1.
Van Beurden W, Harff G, Dekhuijzen P, Van Den Bosch M, Creemers J, Smeenk F. An efficient and reproducible method for measuring hydrogen peroxide in exhaled breath condensate. Respir Med. 2002;96:197–203. https://doi.org/10.1053/rmed.2001.1240.
Rosias PP, Dompeling E, Hendriks HJ, Heijnens JW, Donckerwolcke R, Jöbsis Q. Exhaled breath condensate in children: pearls and pitfalls. Pediatr Allergy Immunol. 2004;15:4–19. https://doi.org/10.1046/j.0905-6157.2003.00091.x.
Frey U, Merkus P. European respiratory monograph: Paediatric lung function. Plymouth: European Respiratory Society; 2010.
Jouyban A, Khoubnasabjafari M, Ansarin K, Jouyban-Gharamaleki V. Breath sampling setup. Iranian Patent, 2013;81363.
Ahmadzai H, Huang S, Hettiarachchi R, Lin JL, Thomas PS, Zhang Q. Exhaled breath condensate: a comprehensive update. Clin Chem Lab Med. 2013;51:1343–61. https://doi.org/10.1515/cclm-2012-0593.
Tufvesson E, Bjermer L. Methodological improvements for measuring eicosanoids and cytokines in exhaled breath condensate. Respir Med. 2006;100:34–8. https://doi.org/10.1016/j.rmed.2005.04.007.
Anaev EK, Apyari VV, Puganova EA, Borisova AV, Dmitriyenko SG, Karyakina EE, et al. Pulmonary oxidative status in norma and pathologies on the basis of analysis of exhaled breath condensate. Am J Biomed Sci. 2010;2:365–72.
Cunningham S, McColm JR, Ho LP, Greening AP, Marshall TG. Measurement of inflammatory markers in the breath condensate of children with cystic fibrosis. Eur Respir J. 2000;15:955–7. https://doi.org/10.1034/j.1399-3003.2000.15e24.x.
Hunt J, Byrns R, Ignarro L, Gaston B. Condensed expirate nitrite as a home marker for acute asthma. Lancet. 1995;346:1235–6. https://doi.org/10.1016/S0140-6736(95)92947-9.
Formanek W, Inci D, Lauener RP, Wildhaber JH, Frey U, Hall GL. Elevated nitrite in breath condensates of children with respiratory disease. Eur Respir J. 2002;19:487–91. https://doi.org/10.1183/09031936.02.00101202.
Ischiropoulos H, Zhu L, Chen J, Tsai M, Martin JC, Smith CD, et al. Peroxynitrite-mediated tyrosine nitration catalyzed by superoxide dismutase. Arch Biochem Biophys. 1992;298:431–7. https://doi.org/10.1016/0003-9861(92)90431-U.
Van Der Vliet A, Nguyen MN, Shigenaga MK, Eiserich JP, Marelich GP, Cross CE. Myeloperoxidase and protein oxidation in cystic fibrosis. Am J Physiol Lung Cell Mol Physiol. 2000;279:L537–56.
Andreadis AA, Hazen SL, Comhair SAA, Erzurum SC. Oxidative and nitrosative events in asthma. Free Radic Biol Med. 2003;35:213–25. https://doi.org/10.1016/S0891-5849(03)00278-8.
Baraldi E, Giordano G, Pasquale M, Carraro S, Mardegan A, Bonetto G, et al. 3-Nitrotyrosine, a marker of nitrosative stress, is increased in breath condensate of allergic asthmatic children. Allergy. 2006;61:90–6. https://doi.org/10.1111/j.1398-9995.2006.00996.x.
Göen T, Müller-Lux A, Dewes P, Musiol A, Kraus T. Sensitive and accurate analyses of free 3-nitrotyrosine in exhaled breath condensate by LC-MS/MS. J Chromatogr B Anal Technol Biomed Life Sci. 2005;826:261–6. https://doi.org/10.1016/j.jchromb.2005.08.001.
Lärstad M, Söderling AS, Caidahl K, Olin AC. Selective quantification of free 3-nitrotyrosine in exhaled breath condensate in asthma using gas chromatography/tandem mass spectrometry. Nitric Oxide. 2005;13:134–44. https://doi.org/10.1016/j.niox.2005.05.009.
Bodini A, Peroni DG, Zardini F, Corradi M, Alinovi R, Boner AL, et al. Flunisolide decreases exhaled nitric oxide and nitrotyrosine levels in asthmatic children. Mediat Inflamm. 2006:31919. https://doi.org/10.1155/MI/2006/31919.
Celio S, Troxler H, Durka SS, Chládek J, Wildhaber JH, Sennhauser FH, et al. Free 3-nitrotyrosine in exhaled breath condensates of children fails as a marker for oxidative stress in stable cystic fibrosis and asthma. Nitric Oxide. 2006;15:226–32. https://doi.org/10.1016/j.niox.2006.06.008.
Mathews WR, Kerr SW. Biological activity of S-nitrosothiols: the role of nitric oxide. J Pharmacol Exp Ther. 1993;267:1529–37.
Csoma Z, Bush A, Wilson NM, Donnelly L, Balint B, Barnes PJ, et al. Nitric oxide metabolites are not reduced in exhaled breath condensate of patients with primary ciliary dyskinesia. Chest J. 2003;124:633–8.
Samuelsson B, Granstrom E, Green K, Hamberg M, Hammarstrom S. Prostaglandins. Annu Rev Biochem. 1975;44:669–95.
Smyth EM, Grosser T, Wang M, Yu Y, FitzGerald GA. Prostanoids in health and disease. J Lipid Res. 2009;50:S423–8. https://doi.org/10.1194/jlr.R800094-JLR200.
Roberts LJ, Milne GL. Isoprostanes. J Lipid Res. 2009;50:S21923. https://doi.org/10.1194/jlr.R800037-JLR200.
Antczak A, Montuschi P, Kharitonov S, Gorski P, Barnes PJ. Increased exhaled cysteinyl-leukotrienes and 8-isoprostane in aspirin-induced asthma. Am J Respir Crit Care Med. 2002;166:301–6. https://doi.org/10.1164/rccm.2101021.
Janssen LJ. Isoprostanes: an overview and putative roles in pulmonary pathophysiology. Am J Physiol Lung Cell Mol Physiol. 2001;280:L1067–82.
Montuschi P, Collins JV, Ciabattoni G, Lazzeri N, Corradi M, Kharitonov SA, et al. Exhaled 8-isoprostane as an in vivo biomarker of lung oxidative stress in patients with COPD and healthy smokers. Am J Respir Crit Care Med. 2000;162:1175–7. https://doi.org/10.1164/ajrccm.162.3.2001063.
Wardlaw A, Hay H, Cromwell O, Collins J, Kay A. Leukotrienes, LTC 4 and LTB 4, in bronchoalveolar lavage in bronchial asthma and other respiratory diseases. J Allergy Clin Immunol. 1989;84:19–26. https://doi.org/10.1016/0091-6749(89)90173-5.
Ford-Hutchinson A, Bray M, Doig MV, Shipley M, Smith M. Leukotriene B, a potent chemokinetic and aggregating substance released from polymorphonuclear leukocytes. Nature. 1980;286:264–5. https://doi.org/10.1038/286264a0.
Hanazawa T, Kharitonov SA, Barnes PJ. Increased nitrotyrosine in exhaled breath condensate of patients with asthma. Am J Respir Crit Care Med. 2000;162:1273–6. https://doi.org/10.1164/ajrccm.162.4.9912064.
Montuschi P. LC/MS/MS analysis of leukotriene B 4 and other eicosanoids in exhaled breath condensate for assessing lung inflammation. J Chromatogr B. 2009;877:1272–80. https://doi.org/10.1016/j.jchromb.2009.01.036.
Čáp P, Chládek J, Pehal F, Malý M, Petrů V, Barnes PJ, et al. Gas chromatography/mass spectrometry analysis of exhaled leukotrienes in asthmatic patients. Thorax. 2004;59:465–70. https://doi.org/10.1136/thx.2003.011866.
Laberge S, El Bassam S. Cytokines, structural cells of the lungs and airway inflammation. Paediatr Respir Rev. 2004;5:S41–5. https://doi.org/10.1016/S1526-0542(04)90009-7.
Dinarello CA. Proinflammatory cytokines. Chest J. 2000;118:503–8.
Atamas SP, Chapoval SP, Keegan AD. Cytokines in chronic respiratory diseases. F1000 Biol Rep. 2013;5:3564216. https://doi.org/10.3410/B5-3.
Matés JM. Effects of antioxidant enzymes in the molecular control of reactive oxygen species toxicology. Toxicology. 2000;153:83–104. https://doi.org/10.1016/S0300-483X(00)00306-1.
Corradi M, Folesani G, Andreoli R, Manini P, Bodini A, Piacentini G, et al. Aldehydes and glutathione in exhaled breath condensate of children with asthma exacerbation. Am J Respir Crit Care Med. 2003;167:395–9. https://doi.org/10.1164/rccm.200206-507OC.
Idzko M, Panther E, Bremer HC, Sorichter S, Luttmann W, Virchow CJ, et al. Stimulation of P2 purinergic receptors induces the release of eosinophil cationic protein and interleukin-8 from human eosinophils. Br J Pharmacol. 2003;138:1244–50. https://doi.org/10.1038/sj.bjp.0705145.
Lázár Z, Huszár É, Kullmann T, Barta I, Antus B, Bikov A, et al. Adenosine triphosphate in exhaled breath condensate of healthy subjects and patients with chronic obstructive pulmonary disease. Inflamm Res. 2008;57:367–73. https://doi.org/10.1007/s00011-008-8009-6.
King NE, Rothenberg ME, Zimmermann N. Arginine in asthma and lung inflammation. J Nutr. 2004;134:2830S–6.
Di Gangi IM, Pirillo P, Carraro S, Gucciardi A, Naturale M, Baraldi E, et al. Online trapping and enrichment ultra performance liquid chromatography-tandem mass spectrometry method for sensitive measurement of "arginine-asymmetric dimethylarginine cycle" biomarkers in human exhaled breath condensate. Anal Chim Acta. 2012;754:67–74. https://doi.org/10.1016/j.aca.2012.09.032.
Ullah S, Sandqvist S, Beck O. Measurement of lung phosphatidylcholines in exhaled breath particles by a convenient collection procedure. Anal Chem. 2015;87:11553–60. https://doi.org/10.1021/acs.analchem.5b03433.
Calkovska A, Uhliarova B, Joskova M, Franova S, Kolomaznik M, Calkovsky V, et al. Pulmonary surfactant in the airway physiology: a direct relaxing effect on the smooth muscle. Respir Physiol Neurobiol. 2015;209:95–105. https://doi.org/10.1016/j.resp.2015.01.004.
Hohlfeld JM. The role of surfactant in asthma. Respir Res. 2001;3:4. https://doi.org/10.1186/rr176.
Horváth I, Hunt J, Barnes PJ. Exhaled breath condensate: methodological recommendations and unresolved questions. Eur Respir J. 2005;26:523–48. https://doi.org/10.1183/09031936.05.00029705.
Bardhan KD, Strugala V, Dettmar PW. Reflux revisited: advancing the role of pepsin. Int J Otolaryngol. 2011:646901. https://doi.org/10.1155/2012/646901.
Zhang X, Zou Y, An C, Ying K, Chen X, Wang P. Sensitive detection of carcinoembryonic antigen in exhaled breath condensate using surface acoustic wave immunosensor. Sensors Actuators B Chem. 2015;217:100–6. https://doi.org/10.1016/j.snb.2014.10.139.
Grunnet M, Sorensen J. Carcinoembryonic antigen (CEA) as tumor marker in lung cancer. Lung Cancer. 2012;76:138–43. https://doi.org/10.1016/j.lungcan.2011.11.012.
Zou Y, Wang L, Zhao C, Hu Y, Xu S, Ying K, et al. CEA, SCC and NSE levels in exhaled breath condensate—possible markers for early detection of lung cancer. J Breath Res. 2013;7:047101. https://doi.org/10.1088/1752-7155/7/4/047101.
Gonzalez-Reche LM, Kucharczyk A, Musiol AK, Kraus T. Determination of Nε-(carboxymethyl) lysine in exhaled breath condensate using isotope dilution liquid chromatography/electrospray ionization tandem mass spectrometry. Rapid Commun Mass Spectrom. 2006;20:2747–52. https://doi.org/10.1002/rcm.2643.
Matsuse T, Ohga E, Teramoto S, Fukayama M, Nagai R, Horiuchi S, et al. Immunohistochemical localisation of advanced glycation end products in pulmonary fibrosis. J Clin Pathol. 1998;51:515–9. https://doi.org/10.1136/jcp.51.7.515.
Bain MA, Faull R, Fornasini G, Milne RW, Evans AM. Accumulation of trimethylamine and trimethylamine-N-oxide in end-stage renal disease patients undergoing haemodialysis. Nephrol Dial Transplant. 2006;21:1300–4. https://doi.org/10.1093/ndt/gfk056.
Beauchamp J. Inhaled today, not gone tomorrow: pharmacokinetics and environmental exposure of volatiles in exhaled breath. J Breath Res. 2011;5 https://doi.org/10.1088/1752-7155/5/3/037103.
Berchtold C, Bosilkovska M, Daali Y, Walder B, Zenobi R. Real-time monitoring of exhaled drugs by mass spectrometry. Mass Spectrom Rev. 2014;33:394–413. https://doi.org/10.1002/mas.21393.
Di Francesco F, Fuoco R, Trivella MG, Ceccarini A. Breath analysis: trends in techniques and clinical applications. Microchem J. 2005;79:405–10. https://doi.org/10.1016/j.microc.2004.10.008.
Grob NM, Aytekin M, Dweik RA. Biomarkers in exhaled breath condensate: a review of collection, processing and analysis. J Breath Res. 2008;2:037004. https://doi.org/10.1088/1752-7155/2/3/037004.
Chambers ST, Scott-Thomas A, Epton M. Developments in novel breath tests for bacterial and fungal pulmonary infection. Curr Opin Pulm Med. 2012;18:228–32. https://doi.org/10.1097/MCP.0b013e328351f98b.
Malakasioti G, Alexopoulos E, Befani C, Tanou K, Varlami V, Ziogas D, et al. Oxidative stress and inflammatory markers in the exhaled breath condensate of children with OSA. Sleep and Breathing. 2012;16:703–8. https://doi.org/10.1007/s11325-011-0560-7.
Stefanska J, Sarniak A, Wlodarczyk A, Sokolowska M, Pniewska E, Doniec Z, et al. Apocynin reduces reactive oxygen species concentrations in exhaled breath condensate in asthmatics. Exp Lung Res. 2012;38:90–9. https://doi.org/10.3109/01902148.2011.649823.
Stefanska J, Sarniak A, Wlodarczyk A, Sokolowska M, Doniec Z, Bialasiewicz P, et al. Hydrogen peroxide and nitrite reduction in exhaled breath condensate of COPD patients. Pulm Pharmacol Ther. 2012;25:343–8. https://doi.org/10.1016/j.pupt.2012.06.001.
Snchez-Vidaurre S, Cruz MJ, Gmez-Olls S, Morell F, Muoz X. Diagnostic utility of exhaled breath condensate analysis in conjunction with specific inhalation challenge in individuals with suspected work-related asthma. Ann Allergy Asthma Immunol. 2012;108:151–6. https://doi.org/10.1016/j.anai.2011.12.010.
Lee JS, Shin JH, Hwang JH, Baek JE, Choi BS. Malondialdehyde and 3-nitrotyrosine in exhaled breath condensate in retired elderly coal miners with chronic obstructive pulmonary disease. Safety and Health at Work. 2014;5:91–6. https://doi.org/10.1016/j.shaw.2014.03.001.
Yildirim Z, Bozkurt B, Ozol D, Armutcu F, Akgedik R, Karamanli H, et al. Increased exhaled 8-isoprostane and interleukin-6 in patients with helicobacter pylori infection. Helicobacter. 2016;21:389–94. https://doi.org/10.1111/hel.12302.
Corradi M, Montuschi P, Donnelly LE, Pesci A, Kharitonov SA, Barnes PJ. Increased nitrosothiols in exhaled breath condensate in inflammatory airway diseases. Am J Respir Crit Care Med. 2001;163:854–8. https://doi.org/10.1164/ajrccm.163.4.2001108.
Makris D, Paraskakis E, Korakas P, Karagiannakis E, Sourvinos G, Siafakas NM, et al. Exhaled breath condensate 8-isoprostane, clinical parameters, radiological indices and airway inflammation in COPD. Respiration. 2008;75:138–44. https://doi.org/10.1159/000106377.
Ko FWS, Lau CYK, Leung TF, Wong GWK, Lam CWK, Hui DSC. Exhaled breath condensate levels of 8-isoprostane, growth related oncogene α and monocyte chemoattractant protein-1 in patients with chronic obstructive pulmonary disease. Respir Med. 2006;100:630–8. https://doi.org/10.1016/j.rmed.2005.08.009.
Trischler J, Müller CM, Könitzer S, Prell E, Korten I, Unverzagt S, et al. Elevated exhaled leukotriene B4; in the small airway compartment in children with asthma. Ann Allergy Asthma Immunol. 2015;114:111–6. https://doi.org/10.1016/j.anai.2014.11.022.
Kazani S, Planaguma A, Ono E, Bonini M, Zahid M, Marigowda G, et al. Exhaled breath condensate eicosanoid levels associate with asthma and its severity. J Allergy Clin Immunol. 2013;132:547–53. https://doi.org/10.1016/j.jaci.2013.01.058.
Peroni DG, Bodini A, Corradi M, Coghi A, Boner AL, Piacentini GL. Markers of oxidative stress are increased in exhaled breath condensates of children with atopic dermatitis. Br J Dermatol. 2012;166:839–43. https://doi.org/10.1111/j.1365-2133.2011.10771.x.
Csoma Z, Kharitonov SA, Balint B, Bush A, Wilson NM, Barnes PJ. Increased leukotrienes in exhaled breath condensate in childhood asthma. Am J Respir Crit Care Med. 2002;166:1345–9. https://doi.org/10.1164/rccm.200203-233OC.
Dong X, Shen Q, Yao Y, Chen J, Lu G, Zhou J. Determination of biomarkers in exhaled breath condensation of acute exacerbation of chronic obstructive pulmonary disease and its clinical implications. Chin J Tuberculosis Respir Dis. 2017;40:114–7. https://doi.org/10.3760/cma.j.issn.1001-0939.2017.02.007.
Montuschi P, Barnes PJ. Exhaled leukotrienes and prostaglandins in asthma. J Allergy Clin Immunol. 2002;109:615–20. https://doi.org/10.1067/mai.2002.122461.
Ciebiada M, Górski P, Antczak A. Eicosanoids in exhaled breath condensate and bronchoalveolar lavage fluid of patients with primary lung cancer. Dis Markers. 2012;32:329–35. https://doi.org/10.3233/DMA-2011-0890.
Grzela K, Zagorska W, Krejner A, Litwiniuk M, Zawadzka-Krajewska A, Banaszkiewicz A, et al. Prolonged treatment with inhaled corticosteroids does not normalize high activity of matrix metalloproteinase-9 in exhaled breath condensates of children with asthma. Arch Immunol Ther Exp. 2015;63:231–7. https://doi.org/10.1007/s00005-015-0328-z.
Krenke K, Peradzyńska J, Lange J, Banaszkiewicz A, Łazowska-Przeorek I, Grzela K, et al. Inflammatory cytokines in exhaled breath condensate in children with inflammatory bowel diseases. Pediatr Pulmonol. 2014;49:1190–5. https://doi.org/10.1002/ppul.22953.
Ono E, Mita H, Taniguchi M, Higashi N, Tsuburai T, Miyazaki E, et al. Comparison of cysteinyl leukotriene concentrations between exhaled breath condensate and bronchoalveolar lavage fluid. Clin Exp Allergy. 2008;38:1866–74. https://doi.org/10.1111/j.1365-2222.2008.03108.x.
Chan E, Sivagnanam T, Zhang Q, Lewis CR, Thomas PS. Tumour necrosis factor alpha and oxidative stress in the breath condensate of those with non-small cell lung cancer. J Cancer Ther. 2012;3:460–6. https://doi.org/10.4236/jct.2012.324059.
Aliberti S, Morlacchi LC, Faverio P, Fernandez-Botran R, Cosentini R, Mantero M, et al. Serum and exhaled breath condensate inflammatory cytokines in community-acquired pneumonia: a prospective cohort study. Pneumonia. 2016;8:8. https://doi.org/10.1186/s41479-016-0009-7.
Seifi M, Rastkari N, Hassanvand M, Arfaeinia H, Younesian M. Determination of biomarker IL-6 in exhaled breath condensate using exhaled breath condensate collector. Iran J Health Environ. 2017;10:15–24.
Heinicke I, Boehler A, Rechsteiner T, Bogdanova A, Jelkmann W, Hofer M, et al. Moderate altitude but not additional endurance training increases markers of oxidative stress in exhaled breath condensate. Eur J Appl Physiol. 2009;106:599–604. https://doi.org/10.1007/s00421-009-1014-9.
Huszár É, Szabó Z, Jakab Á, Barta I, Herjavecz I, Horváth I. Comparative measurement of thromboxane A2 metabolites in exhaled breath condensate by different immunoassays. Inflamm Res. 2005;54:350–5. https://doi.org/10.1007/s00011-005-1361-x.
Chen J, Chen J, Lv X, Ma H. Clinical significance of TGF-β1 in exhaled breath condensate and serum from patients with non-small cell lung cancer. Int J Clin Exp Pathol. 2017;10:5895–900.
Jackson AS, Sandrini A, Campbell C, Chow S, Thomas PS, D. Yates H. Comparison of biomarkers in exhaled breath condensate and bronchoalveolar lavage. Am J Respir Crit Care Med. 2007;175:222–7. https://doi.org/10.1164/rccm.200601-107OC.
Timms C, Thomas PS, Yates DH. Detection of gastro-oesophageal reflux disease (GORD) in patients with obstructive lung disease using exhaled breath profiling. J Breath Res. 2012;6:016003.
Soyer T, Soyer ÖU, Birben E, Kisa Ü, Kalayci Ö, Çakmak M. Pepsin levels and oxidative stress markers in exhaled breath condensate of patients with gastroesophageal reflux disease. J Pediatr Surg. 2013;48:2247–50. https://doi.org/10.1016/j.jpedsurg.2013.02.100.
Chladkova J, Krcmova I, Chladek J, Cap P, Micuda S, Hanzalkova Y. Validation of nitrite and nitrate measurements in exhaled breath condensate. Respiration. 2006;73:173–9. https://doi.org/10.1159/000088050.
Gessner C, Scheibe R, Wötzel M, Hammerschmidt S, Kuhn H, Engelmann L, et al. Exhaled breath condensate cytokine patterns in chronic obstructive pulmonary disease. Respir Med. 2005;99:1229–40. https://doi.org/10.1016/j.rmed.2005.02.041.
Sack U, Scheibe R, Wötzel M, Hammerschmidt S, Kuhn H, Emmrich F, et al. Multiplex analysis of cytokines in exhaled breath condensate. Cytometry A. 2006;69:169–72. https://doi.org/10.1002/cyto.a.20231.
Rosias PP, Robroeks CM, Van De Kant KD, Rijkers GT, Zimmermann LJ, Van Schayck CP, et al. Feasibility of a new method to collect exhaled breath condensate in pre-school children. Pediatr Allergy Immunol. 2010;21:e235–44. https://doi.org/10.1111/j.1399-3038.2009.00909.x.
Schumann C, Triantafilou K, Krueger S, Hombach V, Triantafilou M, Becher G, et al. Detection of erythropoietin in exhaled breath condensate of nonhypoxic subjects using a multiplex bead array. Mediators Inflamm. 2006:18061. https://doi.org/10.1155/MI/2006/18061.
Pasha MA, Smith TC, Feustel PJ, Jourd’heuil D. Effects of low-dose fluticasone propionate/salmeterol combination therapy on exhaled nitric oxide and nitrite/nitrate in breath condensates from patients with mild persistent asthma. J Asthma. 2013;50:64–70. https://doi.org/10.3109/02770903.2012.733467.
Hussain S, Laumbach R, Coleman J, Youssef H, Kelly-Mcneil K, Ohman-Strickland P, et al. Controlled exposure to diesel exhaust causes increased nitrite in exhaled breath condensate among subjects with asthma. J Occup Environ Med. 2012;54:1186–91. https://doi.org/10.1097/JOM.0b013e31826bb64c.
Arcêncio L, Vento DA, Bassetto S, Évora PR, Rodrigues AJ. Exhaled nitrite/nitrate levels as a marker of respiratory complications after heart valve surgery. J Crit Care. 2013;28:533e1–7. https://doi.org/10.1016/j.jcrc.2012.12.009.
Matsunaga K, Yanagisawa S, Ichikawa T, Ueshima K, Akamatsu K, Hirano T, et al. Airway cytokine expression measured by means of protein array in exhaled breath condensate: correlation with physiologic properties in asthmatic patients. J Allergy Clin Immunol. 2006;118:84–90. https://doi.org/10.1016/j.jaci.2006.04.020.
Chen JL, Lv XD, Ma H, Chen JR, Huang JA. Detection of cancer embryo antigen and endothelin-1 in exhaled breath condensate: a novel approach to investigate non-small cell lung cancer. Mol Clin Oncol. 2016;5:124–8. https://doi.org/10.3892/mco.2016.902.
Ródenas-Torralba E, Peláez-Hernández A, Morales-Rubio C, Morales-Rubio Á, De La Guardia M. Multipumping nitrite determination in exhaled breath condensate. Spectrosc Lett. 2006;39:683–97. https://doi.org/10.1080/00387010600932760.
Balint B, Donnelly LE, Hanazawa T, Kharitonov SA, Barnes PJ. Increased nitric oxide metabolites in exhaled breath condensate after exposure to tobacco smoke. Thorax. 2001;56:456–8. https://doi.org/10.1136/thorax.56.6.456.
Goldoni M, Corradi M, Mozzoni P, Folesani G, Alinovi R, Pinelli S, et al. Concentration of exhaled breath condensate biomarkers after fractionated collection based on exhaled CO2 signal. J Breath Res. 2013;7 https://doi.org/10.1088/1752-7155/7/1/017101.
De Prins S, Dons E, Van Poppel M, Int Panis L, de Mieroop EV, Nelen V, et al. Airway oxidative stress and inflammation markers in exhaled breath from children are linked with exposure to black carbon. Environ Int. 2014;73:440–6. https://doi.org/10.1016/j.envint.2014.06.017.
Stiegel MA, Pleil JD, Sobus JR, Morgan MK, Madden MC. Analysis of inflammatory cytokines in human blood, breath condensate, and urine using a multiplex immunoassay platform. Biomarkers. 2015;20:35–46. https://doi.org/10.3109/1354750X.2014.988646.
Chen Z, Xu Z, Sun S, Yu Y, Lv D, Cao C, et al. TGF-β1, IL-6, and TNF-α in bronchoalveolar lavage fluid: useful markers for lung cancer? Sci Rep. 2014;4:5595. https://doi.org/10.1038/srep05595.
Rozy A, Czerniawska J, Stȩpniewska A, Woźbińska B, Goljan A, Puścińska E, et al. Inflammatory markers in the exhaled breath condensate of patients with pulmonary sacroidosis. J Physiol Pharmacol. 2006;57:335–40.
Dalaveris E, Kerenidi T, Katsabeki-Katsafli A, Kiropoulos T, Tanou K, Gourgoulianis KI, et al. VEGF, TNF-α and 8-isoprostane levels in exhaled breath condensate and serum of patients with lung cancer. Lung Cancer. 2009;64:219–25. https://doi.org/10.1016/j.lungcan.2008.08.015.
Czebe K, Barta I, Antus B, Valyon M, Horváth I, Kullmann T. Influence of condensing equipment and temperature on exhaled breath condensate pH, total protein and leukotriene concentrations. Respir Med. 2008;102:720–5. https://doi.org/10.1016/j.rmed.2007.12.013.
Carpagnano GE, Resta O, De Pergola G, Sabato R, Barbaro MPF. The role of obstructive sleep apnea syndrome and obesity in determining leptin in the exhaled breath condensate. J Breath Res. 2010;4:036003. https://doi.org/10.1088/1752-7155/4/3/036003.
Carpagnano GE, Spanevello A, Curci C, Salerno F, Palladino GP, Resta O, et al. IL-2, TNF-α, and leptin: local versus systemic concentrations in NSCLC patients. Oncol Res. 2007;16:375. https://doi.org/10.3727/000000006783980900.
Lee AL, Button BM, Denehy L, Roberts S, Bamford T, Mu FT, et al. Exhaled breath condensate pepsin: potential noninvasive test for gastroesophageal reflux in COPD and bronchiectasis. Respir Care. 2015;60:244–50. https://doi.org/10.4187/respcare.03570.
Robroeks CM, Jöbsis Q, Damoiseaux JG, Heijmans PH, Rosias PP, Hendriks HJ, et al. Cytokines in exhaled breath condensate of children with asthma and cystic fibrosis. Ann Allergy Asthma Immunol. 2006;96:349–55. https://doi.org/10.1016/S1081-1206(10)61247-1.
Baeyens WRG, Schulman SG, Calokerinos AC, Zhao Y, García Campaña AM, Nakashima K, et al. Chemiluminescence-based detection: principles and analytical applications in flowing streams and in immunoassays. J Pharm Biomed Anal. 1998;17:941–53. https://doi.org/10.1016/S0731-7085(98)00062-4.
Lázár Z, Cervenak L, Orosz M, Gálffy G, Komlósi ZI, Bikov A, et al. Adenosine triphosphate concentration of exhaled breath condensate in asthma. Chest. 2010;138:536–42. https://doi.org/10.1378/chest.10-0085.
Effros RM, Hoagland KW, Bosbous M, Castillo D, Foss B, Dunning M, et al. Dilution of respiratory solutes in exhaled condensates. Am J Respir Crit Care Med. 2002;165:663–9. https://doi.org/10.1164/ajrccm.165.5.2101018.
Zacharasiewicz A, Wilson N, Lex C, Li A, Kemp M, Donovan J, et al. Repeatability of sodium and chloride in exhaled breath condensates. Pediatr Pulmonol. 2004;37:273–5. https://doi.org/10.1002/ppul.10431.
Karyakina E, Lukhnovich A, Yashina E, Statkus M, Tsisin G, Karyakin A. Electrochemical biosensor powered by pre-concentration: improved sensitivity and selectivity towards lactate. Electroanalysis. 2016;28:2389–93. https://doi.org/10.1002/elan.201600232.
Karyakin AA, Nikulina SV, Vokhmyanina DV, Karyakina EE, Anaev EK, Chuchalin AG. Non-invasive monitoring of diabetes through analysis of the exhaled breath condensate (aerosol). Electrochem Commun. 2017;83:81–4. https://doi.org/10.1016/j.elecom.2017.09.005.
Bikov A, Galffy G, Tamasi L, Bartusek D, Antus B, Losonczy G, et al. Exhaled breath condensate pH decreases during exercise-induced bronchoconstriction. Respirology. 2014;19:563–9. https://doi.org/10.1111/resp.12248.
Melker RJ, Bjoraker DG, Dennis DM, Stewart JD, Batich CD, Booth MM, Horn Jr JF, Youngblood RE. Condensate glucose analyzer, U.S. Patent No. 7,914,460. Washington, DC: U.S. Patent and Trademark Office, 2011.
Carlsen K, Anderson S, Bjermer L, Bonini S, Brusasco V, Canonica W, et al. Exercise-induced asthma, respiratory and allergic disorders in elite athletes: epidemiology, mechanisms and diagnosis: part I of the report from the joint task force of the European Respiratory Society (ERS) and the European academy of allergy and clinical immunology (EAACI) in cooperation with GA2LEN. Allergy. 2008;63:387–403. https://doi.org/10.1111/j.1398-9995.2008.01662.x.
Svensson S, Isacsson AC, Ljungkvist G, Torén K, Olin AC. Optimization and validation of an ion chromatographic method for the simultaneous determination of sodium, ammonium and potassium in exhaled breath condensate. J Chromatogr B Anal Technol Biomed Life Sci. 2005;814:173–7. https://doi.org/10.1016/j.jchromb.2004.10.018.
Montuschi P, Ragazzoni E, Valente S, Corbo G, Mondino C, Ciappi G, et al. Validation of leukotriene B4 measurements in exhaled breath condensate. Inflammation Res. 2003;52:69–73. https://doi.org/10.1007/s000110300003.
Folesani G, Corradi M, Goldoni M, Manini P, Acampa O, Andreoli R, et al. Urea in exhaled breath condensate of uraemics and patients with chronic airway diseases. Acta Biomed. 2008;79:79–86.
Csoma Z, Huszár É, Vizi É, Vass G, Szabó Z, Herjavecz I, et al. Adenosine level in exhaled breath increases during exercise-induced bronchoconstriction. Eur Respir J. 2005;25:873–8. https://doi.org/10.1183/09031936.05.00110204.
Rihák V, Zatloukal P, Chládková J, Zimulová A, Havlínová Z, Chládek J. Nitrite in exhaled breath condensate as a marker of nitrossative stress in the airways of patients with asthma, COPD, and idiopathic pulmonary fibrosis. J Clin Lab Anal. 2010;24:317–22. https://doi.org/10.1002/jcla.20408.
Montuschi P, Martello S, Felli M, Mondino C, Chiarotti M. Ion trap liquid chromatography/tandem mass spectrometry analysis of leukotriene B4 in exhaled breath condensate. Rapid Commun Mass Spectrom. 2004;18:2723–9. https://doi.org/10.1002/rcm.1682.
Montuschi P, Martello S, Felli M, Mondino C, Barnes PJ, Chiarotti M. Liquid chromatography/mass spectrometry analysis of exhaled leukotriene B 4 in asthmatic children. Respir Res. 2005;6:119. https://doi.org/10.1186/1465-9921-6-119.
Pelclová D, Fenclová Z, Kačer P, Navrátil T, Kuzma M, Lebedová J, et al. 8-Isoprostane and leukotrienes in exhaled breath condensate in Czech subjects with silicosis. Ind Health. 2007;45:766–74. https://doi.org/10.2486/indhealth.45.766.
Fritscher LG, Post M, Rodrigues MT, Silverman F, Balter M, Chapman KR, et al. Profile of eicosanoids in breath condensate in asthma and COPD. J Breath Res. 2012;6:026001. https://doi.org/10.1088/1752-7155/6/2/026001.
Gonzalez-Reche LM, Musiol AK, Müller-Lux A, Kraus T, Göen T. Method optimization and validation for the simultaneous determination of arachidonic acid metabolites in exhaled breath condensate by liquid chromatography-electrospray ionization tandem mass spectrometry. J Occup Med Toxicol. 2006;1:5. https://doi.org/10.1186/1745-6673-1-5.
Esther CR Jr, Jasin HM, Collins LB, Swenberg JA, Boysen G. A mass spectrometric method to simultaneously measure a biomarker and dilution marker in exhaled breath condensate. Rapid Commun Mass Spectrom. 2008;22:701–5. https://doi.org/10.1002/rcm.3408.
Syslová K, Kačer P, Kuzma M, Pankrácová A, Fenclová Z, Vlčková Š, et al. LC-ESI-MS/MS method for oxidative stress multimarker screening in the exhaled breath condensate of asbestosis/silicosis patients. J Breath Res. 2010;4:017104. https://doi.org/10.1088/1752-7155/4/1/017104.
Jackson TC, Zhang YV, Sime PJ, Phipps RP, Kottmann RM. Development of an accurate and sensitive method for lactate analysis in exhaled breath condensate by LC MS/MS. J Chromatogr B. 2017;1061:468–73. https://doi.org/10.1016/j.jchromb.2017.07.041.
Konieczna L, Pyszka M, Okońska M, Niedźwiecki M, Bączek T. Bioanalysis of underivatized amino acids in non-invasive exhaled breath condensate samples using liquid chromatography coupled with tandem mass spectrometry. J Chromatogr A. 2018;1542:72–81. https://doi.org/10.1016/j.chroma.2018.02.019.
Nording ML, Yang J, Hegedus CM, Hegedus CM, Bhushan A, Davis CE, et al. Endogenous levels of five fatty acid metabolites in exhaled breath condensate to monitor asthma by high-performance liquid chromatography: electrospray tandem mass spectrometry. IEEE Sensors J. 2010;10:123–30. https://doi.org/10.1109/JSEN.2009.2035736.
Bloemen K, Van Den Heuvel R, Govarts E, Hooyberghs J, Nelen V, Witters E, et al. A new approach to study exhaled proteins as potential biomarkers for asthma. Clin Exp Allergy. 2011;41:346–56. https://doi.org/10.1111/j.1365-2222.2010.03638.x.
Beck O, Sandqvist S, Eriksen P, Franck J, Palmskog G. Determination of methadone in exhaled breath condensate by liquid chromatography-tandem mass spectrometry. J Anal Toxicol. 2011;35:129–33. https://doi.org/10.1093/anatox/35.3.129.
Kononikhin A, Starodubtseva N, Chagovets V, Ryndin A, Burov A, Popov I, et al. Exhaled breath condensate analysis from intubated newborns by nano-HPLC coupled to high resolution MS. J Chromatogr B. 2017;1047:97–105. https://doi.org/10.1016/j.jchromb.2016.12.036.
Conventz A, Musiol A, Brodowsky C, Müller-Lux A, Dewes P, Kraus T, et al. Simultaneous determination of 3-nitrotyrosine, tyrosine, hydroxyproline and proline in exhaled breath condensate by hydrophilic interaction liquid chromatography/electrospray ionization tandem mass spectrometry. J Chromatogr B Anal Technol Biomed Life Sci. 2007;860:78–85. https://doi.org/10.1016/j.jchromb.2007.10.031.
Schettgen T, Tings A, Brodowsky C, Müller-Lux A, Musiol A, Kraus T. Simultaneous determination of the advanced glycation end product Nɛ-carboxymethyllysine and its precursor, lysine, in exhaled breath condensate using isotope-dilution–hydrophilic-interaction liquid chromatography coupled to tandem mass spectrometry. Anal Bioanal Chem. 2007;387:2783–91. https://doi.org/10.1007/s00216-007-1163-9.
Monge ME, Pérez JJ, Dwivedi P, Zhou M, McCarty NA, Stecenko AA, et al. Ion mobility and liquid chromatography/mass spectrometry strategies for exhaled breath condensate glucose quantitation in cystic fibrosis studies. Rapid Commun Mass Spectrom. 2013;27:2263–71. https://doi.org/10.1002/rcm.6683.
Fermier B, Blasco H, Godat E, Bocca C, Moënne-Loccoz J, Emond P, et al. Specific metabolome profile of exhaled breath condensate in patients with shock and respiratory failure: a pilot study. Metabolites. 2016;6:26. https://doi.org/10.3390/metabo6030026.
Peralbo-Molina A, Calderón-Santiago M, Priego-Capote F, Jurado-Gámez B, Luque de Castro MD. Development of a method for metabolomic analysis of human exhaled breath condensate by gas chromatography-mass spectrometry in high resolution mode. Anal Chim Acta. 2015;887:118–26. https://doi.org/10.1016/j.aca.2015.07.008.
Sanak M, Gielicz A, Nagraba K, Kaszuba M, Kumik J, Szczeklik A. Targeted eicosanoids lipidomics of exhaled breath condensate in healthy subjects. J Chromatogr B Analyt Technol Biomed Life Sci. 2010;878:1796–800. https://doi.org/10.1016/j.jchromb.2010.05.012.
Carraro S, Cogo PE, Isak I, Simonato M, Corradi M, Carnielli VP, et al. Baraldi EIA and GC/MS analysis of 8-isoprostane in EBC of children with problematic asthma. Eur Respir J. 2010;35:1364–9. https://doi.org/10.1183/09031936.00074909.
Mosquera-Restrepo SF, Caro AC, García LF, Peláez-Jaramillo CA, Rojas M. Fatty acid derivative, chemokine, and cytokine profiles in exhaled breath condensates can differentiate adult and children paucibacillary tuberculosis patients. J Breath Res. 2017;11:016003.
Greguš M, Foret F, Kubáň P. Single-breath analysis using a novel simple sampler and capillary electrophoresis with contactless conductometric detection. Electrophoresis. 2015;36:526–33. https://doi.org/10.1002/elps.201400456.
Greguš M, Foret F, Kubáň P. Portable capillary electrophoresis instrument with contactless conductivity detection for on-site analysis of small volumes of biological fluids. J Chromatogr A. 2016;1427:177–85. https://doi.org/10.1016/j.chroma.2015.11.088.
Kubáň P, Ďurč P, Bittová M, Foret F. Separation of oxalate, formate and glycolate in human body fluid samples by capillary electrophoresis with contactless conductometric detection. J Chromatogr A. 2014;1325:241. https://doi.org/10.1016/j.chroma.2013.12.039.
Greguš M, Foret F, Kindlová D, Pokojová E, Plutinský M, Doubková M, et al. Monitoring the ionic content of exhaled breath condensate in various respiratory diseases by capillary electrophoresis with contactless conductivity detection. J Breath Res. 2015;9:027107. https://doi.org/10.1088/1752-7155/9/2/027107.
Kubáň P, Kobrin EG, Kaljurand M. Capillary electrophoresis - a new tool for ionic analysis of exhaled breath condensate. J Chromatogr A. 2012;1267:239–45. https://doi.org/10.1016/j.chroma.2012.06.085.
Hodáková J, Preisler J, Foret F, Kubáň P. Sensitive determination of glutathione in biological samples by capillary electrophoresis with green (515nm) laser-induced fluorescence detection. J Chromatogr A. 2015;1391:102–8. https://doi.org/10.1016/j.chroma.2015.02.062.
Griese M, Noss J, Von Bredow C. Protein pattern of exhaled breath condensate and saliva. Proteomics. 2002;2:690–6. https://doi.org/10.1002/1615-9861(200206)2:6<690:AID-PROT690>3.0.CO;2-6.
Gianazza E, Allegra L, Bucchioni E, Eberini I, Puglisi L, Blasi F, et al. Increased keratin content detected by proteomic analysis of exhaled breath condensate from healthy persons who smoke. Am J Med. 2004;117:51–4. https://doi.org/10.1016/j.amjmed.2004.01.022.
Lacombe M, Marie-Desvergne C, Combes F, Kraut A, Bruley C, Vandenbrouck Y, et al. Proteomic characterization of human exhaled breath condensate. J Breath Res. 2018;12:021001.
Gessner C, Dihazi H, Brettschneider S, Hammerschmidt S, Kuhn H, Eschrich K, et al. Presence of cytokeratins in exhaled breath condensate of mechanical ventilated patients. Respir Med. 2008;102:299–306. https://doi.org/10.1016/j.rmed.2007.08.012.
Fumagalli M, Ferrari F, Luisetti M, Stolk J, Hiemstra PS, Capuano D, et al. Profiling the proteome of exhaled breath condensate in healthy smokers and COPD patients by LC-MS/MS. Int J Mol Sci. 2012;13:13894–910. https://doi.org/10.3390/ijms131113894.
Greenwald R, Ferdinands JM, Teague WG. Ionic determinants of exhaled breath condensate pH before and after exercise in adolescent athletes. Pediatr Pulmonol. 2009;44:768–77. https://doi.org/10.1002/ppul.21055.
Ryberg H, Caidahl K. Chromatographic and mass spectrometric methods for quantitative determination of 3-nitrotyrosine in biological samples and their application to human samples. J Chromatogr B Anal Technol Biomed Life Sci. 2007;851:160–71. https://doi.org/10.1016/j.jchromb.2007.02.001.
Beck O, Olin AC, Mirgorodskaya E. Potential of mass spectrometry in developing clinical laboratory biomarkers of nonvolatiles in exhaled breath. Clin Chem. 2016;62:84–91. https://doi.org/10.1373/clinchem.2015.239285.
Syslová K, Kačer P, Kuzma M, Klusáčková P, Fenclová Z, Lebedová J, et al. Determination of 8-iso-prostaglandin F 2α in exhaled breath condensate using combination of immunoseparation and LC–ESI-MS/MS. J Chromatogr B. 2008;867:8–14. https://doi.org/10.1016/j.jchromb.2008.02.019.
Wang CJ, Yang NH, Liou SH, Lee HL. Fast quantification of the exhaled breath condensate of oxidative stress 8-iso-prostaglandin F2α using on-line solid-phase extraction coupled with liquid chromatography/electrospray ionization mass spectrometry. Talanta. 2010;82:1434–8. https://doi.org/10.1016/j.talanta.2010.07.015.
Buszewski B, Noga S. Hydrophilic interaction liquid chromatography (HILIC)—a powerful separation technique. Anal Bioanal Chem. 2012;402:231–47. https://doi.org/10.1007/s00216-011-5308-5.
Oyler AR, Armstrong BL, Cha JY, Zhou MX, Yang Q, Robinson RI, et al. Hydrophilic interaction chromatography on amino-silica phases complements reversed-phase high-performance liquid chromatography and capillary electrophoresis for peptide analysis. J Chromatogr A. 1996;724:378–83. https://doi.org/10.1016/0021-9673(95)00987-6.
Hemström P, Irgum K. Hydrophilic interaction chromatography. J Sep Sci. 2006;29:1784–821. https://doi.org/10.1002/jssc.200600199.
Dong MW, Zhang K. Ultra-high-pressure liquid chromatography (UHPLC) in method development. Trends Anal Chem. 2014;63:21–30. https://doi.org/10.1016/j.trac.2014.06.019.
Wu N, Welch CJ, Natishan TK, Gao H, Chandrasekaran T, Zhang L. Practical aspects of ultrahigh performance liquid chromatography. In: Alan Xu Q, editor. Ultra-high performance liquid chromatography and its applications. Hoboken: Wiley; 2013. p. 55–94. https://doi.org/10.1002/9781118533956.ch3.
Wang JH, Byun J, Pennathur S. Analytical approaches to metabolomics and applications to systems biology. Semin Nephrol. 2010;30:500–11. https://doi.org/10.1016/j.semnephrol.2010.07.007.
Koek MM, Jellema RH, van der Greef J, Tas AC, Hankemeier T. Quantitative metabolomics based on gas chromatography mass spectrometry: status and perspectives. Metabolomics. 2011;7:307–28. https://doi.org/10.1007/s11306-010-0254-3.
Quinones MP, Kaddurah-Daouk R. Metabolomics tools for identifying biomarkers for neuropsychiatric diseases. Neurobiol Dis. 2009;35:165–76. https://doi.org/10.1016/j.nbd.2009.02.019.
Augusto F, Hantao LW, Mogollon NG, Braga SC. New materials and trends in sorbents for solid-phase extraction. Trends Anal Chem. 2013;43:14–23. https://doi.org/10.1016/j.trac.2012.08.012.
Carpenter CT, Price PV, Christman BW. Exhaled breath condensate isoprostanes are elevated in patients with acute lung injury or ARDS. Chest. 1998;114:1653–9. https://doi.org/10.1378/chest.114.6.1653.
Grabowska-Polanowska B, Faber J, Skowron M, Miarka P, Pietrzycka A, Śliwka I, et al. Detection of potential chronic kidney disease markers in breath using gas chromatography with mass-spectral detection coupled with thermal desorption method. J Chromatogr A. 2013;1301:179–89. https://doi.org/10.1016/j.chroma.2013.05.012.
Kemp G. Capillary electrophoresis. Biotechnol Appl Biochem. 1998;27:9–17. https://doi.org/10.1111/j.1470-8744.1998.tb01369.x.
Beck W, van Hoek R, Engelhardt H. Application of a diode-array detector in capillary electrophoresis. Electrophoresis. 1993;14:540–6. https://doi.org/10.1002/elps.1150140182.
Kuban P, Karlberg B. Simultaneous determination of small cations and anions by capillary electrophoresis. Anal Chem. 1998;70:360–5. https://doi.org/10.1021/ac9706133.
Kryndushkin DS, Alexandrov IM, Ter-Avanesyan MD, Kushnirov VV. Yeast [PSI+] prion aggregates are formed by small Sup35 polymers fragmented by Hsp104. J Biol Chem. 2003;278:49636–43. https://doi.org/10.1074/jbc.M307996200.
Zang X, Pérez JJ, Jones CM, Monge ME, McCarty NA, Stecenko AA, et al. Comparison of ambient and atmospheric pressure ion sources for cystic fibrosis exhaled beath condensate ion mobility-mass spectrometry metabolomics. J Am Soc Mass Spectrom. 2017;28:1489–96. https://doi.org/10.1007/s13361-017-1660-9.
Rumsby P. In: Innis MA, Gelfand DH, Sninsky JJ, White TJ, editors. PCR protocols-A guide to methods and applications. San Diego: Academic Press Inc.; 1990.
Gessner C, Kuhn H, Toepfer K, Hammerschmidt S, Schauer J, Wirtz H. Detection of p53 gene mutations in exhaled breath condensate of non-small cell lung cancer patients. Lung Cancer. 2004;43:215–22. https://doi.org/10.1016/j.lungcan.2003.08.034.
Carpagnano GE, Foschino-Barbaro MP, Mulé G, Resta O, Tommasi S, Mangia A, et al. 3p microsatellite alterations in exhaled breath condensate from patients with non-small cell lung cancer. Am J Respir Crit Care Med. 2005;172:738–44. https://doi.org/10.1164/rccm.200503-439OC.
Jain R, Schriever CA, Danziger LH, Cho SH, Rubinstein I. The IS6110 repetitive DNA element of Mycobacterium tuberculosis is not detected in exhaled breath condensate of patients with active pulmonary tuberculosis. Respiration. 2007;74:329–33. https://doi.org/10.1159/000101786.
Bhimji A, Singer L, Kumar D, Humar A, Pavan R, Zhang H, et al. Feasibility of detecting fungal DNA in exhaled breath condensate by the Luminex multiplex xTAG fungal PCR assay in lung transplant recipients: a pilot study. J Heart Lung Transpl. 2016;35:S37.
May AK, Brady JS, Romano-Keeler J, Drake WP, Norris PR, Jenkins JM, et al. A pilot study of the noninvasive assessment of the lung microbiota as a potential tool for the early diagnosis of ventilator-associated pneumonia. Chest. 2015;147:1494–502. https://doi.org/10.1378/chest.14-1687.
Carpagnano GE, Koutelou A, Natalicchio MI, Martinelli D, Ruggieri C, Di Taranto A, et al. HPV in exhaled breath condensate of lung cancer patients. Br J Cancer. 2011;105:1183–90. https://doi.org/10.1038/bjc.2011.354.
Roff AN, Craig TJ, August A, Stellato C, Ishmael FT. MicroRNA-570-3p regulates HuR and cytokine expression in airway epithelial cells. Am J Clin Exp Immunol. 2014;3:68–83.
Pinkerton M, Chinchilli V, Banta E, Craig T, August A, Bascom R, et al. Differential expression of microRNAs in exhaled breath condensates of patients with asthma, patients with chronic obstructive pulmonary disease, and healthy adults. J Allergy Clin Immunol. 2013;132:217–9. https://doi.org/10.1016/j.jaci.2013.03.006.
Yang Ai SS, Hsu K, Herbert C, Cheng Z, Hunt J, Lewis CR, et al. Mitochondrial DNA mutations in exhaled breath condensate of patients with lung cancer. Respir Med. 2013;107:911–8. https://doi.org/10.1016/j.rmed.2013.02.007.
Zhang X, Zou Y, An C, Ying K, Chen X, Wang P. A miniaturized immunosensor platform for automatic detection of carcinoembryonic antigen in EBC. Sensors Actuators B Chem. 2014;205:94–101. https://doi.org/10.1016/j.snb.2014.08.011.
Chu BH, Kang BS, Hung SC, Chen KH, Ren F, Sciullo A, et al. Aluminum gallium nitride (GaN)/GaN high electron mobility transistor-based sensors for glucose detection in exhaled breath condensate. J Diabetes Sci Technol. 2010;4:171–9. https://doi.org/10.1177/193229681000400122.
Chu BH, Kang B, Chang C, Ren F, Goh A, Sciullo A, et al. Wireless detection system for glucose and pH sensing in exhaled breath condensate using AlGaN/GaN high electron mobility transistors. IEEE Sensors J. 2010;10:64–70. https://doi.org/10.1109/JSEN.2009.2035213.
Carraro S, Rezzi S, Reniero F, Héberger K, Giordano G, Zanconato S, et al. Metabolomics applied to exhaled breath condensate in childhood asthma. Am J Respir Crit Care Med. 2007;175:986–90. https://doi.org/10.1164/rccm.200606-769OC.
De Laurentiis G, Paris D, Melck D, Maniscalco M, Marsico S, Corso G, et al. Metabonomic analysis of exhaled breath condensate in adults by nuclear magnetic resonance spectroscopy. Eur Respir J. 2008;32:1175–83. https://doi.org/10.1183/09031936.00072408.
Paris D, Maniscalco M, Melck D, D’Amato M, Sorrentino N, Zedda A, et al. Inflammatory metabolites in exhaled breath condensate characterize the obese respiratory phenotype. Metabolomics. 2015;11:1934–9. https://doi.org/10.1007/s11306-015-0805-8.
Motta A, Paris D, D'Amato M, Melck D, Calabrese C, Vitale C, et al. NMR metabolomic analysis of exhaled breath condensate of asthmatic patients at two different temperatures. J Proteome Res. 2014;13:6107–20. https://doi.org/10.1021/pr5010407.
Montuschi P, Paris D, Melck D, Lucidi V, Ciabattoni G, Raia V, et al. NMR spectroscopy metabolomic profiling of exhaled breath condensate in patients with stable and unstable cystic fibrosis. Thorax. 2012;67:222–8. https://doi.org/10.1136/thoraxjnl-2011-200072.
Airoldi C, Ciaramelli C, Fumagalli M, Bussei R, Mazzoni V, Viglio S, et al. 1H NMR to explore the metabolome of exhaled breath condensate in α1-antitrypsin deficient patients: a pilot study. J Proteome Res. 2016;15:4569–78. https://doi.org/10.1021/acs.jproteome.6b00648.
Ahmed N, Bezabeh T, Ijare OB, Myers R, Alomran R, Aliani M, et al. Metabolic signatures of lung cancer in sputum and exhaled breath condensate detected by 1H magnetic resonance spectroscopy: a feasibility study. Magn Reson Insights. 2016;9:29–35. https://doi.org/10.4137/MRI.S40864.
Surendiran A, Sandhiya S, Pradhan SC, Adithan C. Novel applications of nanotechnology in medicine. Indian J Med Res. 2009;130:689–701.
Melker R, Dennis D. Combined nanotechnology and sensor technologies for simultaneous diagnosis and treatment, U.S. Patent Application No. 10/744,789, 2003.
Melker R, Dennis D, Martin C. Stewart J Novel application of biosensors for diagnosis and treatment of disease, US Patent Application No. 2005;11(/296):757.
Gruhl F, Rapp B, Rapp M, Länge K. Surface acoustic wave (SAW) biosensor chip system-a promising alternative for biomedical applications, In World Congress on Medical Physics and Biomedical Engineering, September 7–12, 2009, Munich, Germany, Springer, 2009, pp. 73–76.
Ren F, Pearton SJ, Lele T, Wang HT, Kang BS. Sensors using high electron mobility transistors, U.S. patent no. 8,835,984. Washington, DC: U.S. patent and trademark Office, 2014.
Lindon JC, Holmes E, Nicholson JK. Pattern recognition methods and applications in biomedical magnetic resonance. Prog Nucl Magn Reson Spectrosc. 2001;39:1–40. https://doi.org/10.1016/S0079-6565(00)00036-4.
Fathi F, Ektefa F, Arefi Oskouie A, Rostami K, Rezaei-Tavirani M, Mohammad Alizadeh AH, et al. NMR based metabonomics study on celiac disease in the blood serum. Gastroenterol Hepatol Bed Bench. 2013;6:190–4.
Fathi F, Kasmaee LM, Sohrabzadeh K, Nejad MR, Tafazzoli M, Oskouie AA. The differential diagnosis of Crohn's disease and celiac disease using nuclear magnetic resonance spectroscopy. Appl Magn Reson. 2014;45:451–9. https://doi.org/10.1007/s00723-014-0530-x.
Godet C, Hira M, Adoun M, Eugène M, Robert R. Rapid diagnosis of alcoholic ketoacidosis by proton NMR. Intensive Care Med. 2001;27:785–6. https://doi.org/10.1007/s001340100892.
Maniscalco M, Paris D, Melck DJ, D'Amato M, Zedda A, Sofia M, et al. Coexistence of obesity and asthma determines a distinct respiratory metabolic phenotype. J Allergy Clin Immunol. 2017;139:1536–47. https://doi.org/10.1016/j.jaci.2016.08.038.
Ząbek A, Stanimirova I, Deja S, Barg W, Kowal A, Korzeniewska A, et al. Fusion of the 1H NMR data of serum, urine and exhaled breath condensate in order to discriminate chronic obstructive pulmonary disease and obstructive sleep apnea syndrome. Metabolomics. 2015;11:1563–74. https://doi.org/10.1007/s11306-015-0808-5.
Khoubnasabjafari M, Rahimpour E, Jouyban A. Exhaled breath condensate as an alternative sample for drug monitoring. Bioanalysis. 2018;10:61–4.
Acknowledgments
The authors would like to thank Dr. Ali Shayanfar for his assistance in this study.
Patent
Jouyban A, Khoubnasabjafari M, Ansarin K, Jouyban-Gharamaleki V. Breath sampling setup. Iranian Patent, 81363, 2013.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Rahimpour, E., Khoubnasabjafari, M., Jouyban-Gharamaleki, V. et al. Non-volatile compounds in exhaled breath condensate: review of methodological aspects. Anal Bioanal Chem 410, 6411–6440 (2018). https://doi.org/10.1007/s00216-018-1259-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00216-018-1259-4