Abstract
Cognitive impairment is present in patients with depression. We hypothesized that alpha-lipoic acid (ALA) can reduce cognitive impairment, especially when combined to antidepressants. Female mice received vehicle or corticosterone (CORT) 20 mg/kg, s.c. for 14 days. From the 15th to 21st day, the animals were divided in groups: vehicle, CORT, CORT+desvenlafaxine (DVS) 10 or 20 mg/kg, ALA 100 or 200 mg/kg, DVS10+ALA100, DVS20+ALA100, DVS10+ALA200, or DVS20+ALA200. Tail suspension (TST), social interaction (SIT), novel object recognition (NOR), and Y-maze tests were conducted. Acetylcholinesterase activity (AChE) was measured in the prefrontal cortex (PFC), hippocampus (HC), and striatum (ST). CORT caused depressive-like behavior, impairment in SIT, and cognitive deficits. Alpha-lipoic acid and DVS, alone or combined, reversed CORT effect on TST. In the NOR, ALA200 alone, DVS10+ALA100, or DVS10+ALA200 reversed the deficits in short-term memory, while DVS20 alone or DVS20+ALA200 reversed the deficits in long-term memory. In the Y-maze test, ALA200 alone, DVS20+ALA100, or DVS20+ALA200 reversed the deficits caused by CORT in the working memory. CORT increased AChE in the PFC, HC, and ST. ALA200 alone or DVS20+ALA200 reversed this effect in the PFC, while DVS20 or DVS20+ALA100 reversed this effect in the HC. In the ST, DVS10 or 20, alone or combined, and ALA100 reversed the effects of CORT. These results suggest that DVS+ALA, by reversing CORT-induced memory and social deficits, seems to be a promising therapy for the treatment of depression and reversal of cognitive impairment observed in this disorder.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Major depressive disorder (MDD) may become a chronic and lifelong condition, with many patients experiencing recurrent depressive episodes. In this regard, for a significant number of patients, the disorder has an obstinate nature, with fluctuations over time in the severity of depressive symptoms (Kessler 2003, 2012). This disorder has been considered the leading cause of disease-related disability especially among women. The prevalence of this mental disorder among this population has typically been between one and a half to three times that of men (Kessler 2003). Depressed mood, diminished interest/pleasure, and fatigue or loss of energy are among the core symptoms of MDD (Fried and Nesse 2014).
Several studies highlight the importance of cognitive impairment in depressed patients (Panza et al. 2010; Murrough et al. 2011; Lee et al. 2012; Rock et al. 2014). These studies showed that in addition to the core symptoms, memory impairment is widely reported by these patients. Another important observation is that memory deficits can emerge in the first episodes of depression as well as during its progression (Murrough et al. 2011).
Besides the aforementioned, cognitive dysfunction may persist even after depressive episodes or during remission (Herrera-Guzmán et al. 2010; Hasselbalch et al. 2011). Thus, memory deficits, difficulty making decisions, and loss of cognitive flexibility are associated with dependence and limited functional recovery of depressed patients (Vaughn McCall and Dunn 2003; Jaeger et al. 2006; Trivedi and Greer 2014).
To date, MDD treatment has important limitations. According to the “Treatment sequenced alternatives to relieve depression” (STAR*D), only about one quarter of MDD patients achieve remission during the first treatment phase (Trivedi et al. 2007). Furthermore, the antidepressant drugs have limited effectiveness in older depressed adults. Furthermore, in patients with executive dysfunction or dementia, the effectiveness of antidepressants is compromised (Nelson and Devanand 2011; Morimoto et al. 2015). It is important to highlight that the complex relationship between depression and cognitive impairment, especially in the elderly population, makes this disorder difficult to diagnose and treat in this population.
Several studies have pointed to molecular deficits in the cholinergic system as one of the etiological factors of depression (Zhang et al. 2016; Feng et al. 2017). Knowing that the integrity of the cholinergic system is fundamental to the activity of learning and memory (Blokland 1995; Farhat et al. 2017), it is possible that dysfunctions of these neurons contribute to the cognitive damage presented by depressive patients (Stepanichev et al. 2016). Thus, these data reinforce the need of an effective therapy not only for the classic symptoms of depression but also for the associated symptoms such as cognitive deficits.
Several animal models have been developed with the purpose of studying depressive symptomatology (Sterner and Kalynchuk 2010). Among the preclinical models available for the study of depression, a set of evidence has pointed that repeated exogenous administration of corticosterone (CORT) produces reliable behavioral and neurobiological alterations similar to those presented in humans with depression (Zhao et al. 2008; Iijima et al. 2010; Huang et al. 2011; Silva et al. 2013; de Sousa et al. 2015). In line with the memory deficits present in depressed patients, the CORT animal model was recently related to cognitive impairments in both mice (Dobarro et al. 2013) and rats (Trofimiuk and Braszko 2015). Thus, the CORT-induced depression model in rodents seems to be a valuable tool for the evaluation of the antidepressant effect of drugs as well as for the study of possible mechanisms involved in these antidepressant effects (Zhao et al. 2008; Iijima et al. 2010). On the other hand, one pitfall observed in the CORT-induced model is that it does not take directly into account factors such as socio-environmental stressors and the individual response, which are addressed by other animal models, such as chronic unpredictable stress (CMS). Thus, to evaluate environmental stress in depression, CMS seems to be the most reliable model (Gregus et al. 2005).
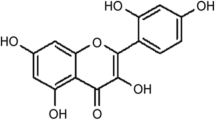
In the last decades, oxidative and nitrosative mechanisms have been associated with MDD (Moylan et al. 2014). In this regard, alpha-lipoic acid (ALA—1,2-dithiolane-3-pentanoic acid), also known as thioctic acid, is a natural antioxidant synthesized in the human body (Ferreira et al. 2009). This molecule is efficient in combating free radicals, promoting the reduction of lipid peroxidation, acting as a cofactor of multiple enzymatic complexes being also capable of regenerating damaged tissues (Chng et al. 2009). It is worth mentioning that ALA is already a well-established treatment for neuropathic symptoms (Hermann et al. 2014), thus reinforcing the idea of its potential as an antioxidant and neuroprotective substance. The first hypothesis of the antidepressant effect of ALA occurred in the last decade (Salazar 2000), and recently, preclinical studies from our research group have added further lines of evidence to this hypothesis (Silva et al. 2013, 2014, 2016; de Sousa et al. 2015).
We have previously showed, in preclinical approaches, that ALA augments the antidepressant-like effects of desvenlafaxine (DVS) (Silva et al. 2013). In line with this augmentation of DVS antidepressant-like effect, we also observed increased levels of brain-derived neurotrophic factor (BDNF) in prefrontal cortex, hippocampus, and striatum of mice administered ALA+DVS when compared to DVS alone.
Thus, given the importance of cognitive impairment in patients with depression, we hypothesized that ALA, based on its potent antioxidant and antidepressant effects, could improve the cognition of female mice submitted to CORT-induced depression model, when given alone or combined with DVS. To test this hypothesis, herein we performed memory tasks for the evaluation of working memory (Y-maze), recognition memory (novel object recognition test—NOR), and social interaction test.
Furthermore, we aimed to determine the activity of acetylcholinesterase (AChE) in the prefrontal cortex (PFC), hippocampus (HC), and striatum (ST) of mice.
Material and methods
Animals
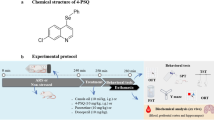
Female Swiss mice (30–32 g) were obtained from the Animal House of the Federal University of Ceará, Brazil. The animals were kept in acrylic cages in a room with a controlled temperature of 23 ± 1 °C, under a standard light-dark cycle with ad libitum access to food and water, except during the experiments. Food was removed 4 h prior to the oral gavage procedure and returned 20 min after. The animals were divided into one of the following ten experimental groups (n = 6–10 animals/group), as described in Fig. 1 and in figure legends. The acrylic cages were located together on the same shelf of the rack in a way that the auditory and visual contacts were maintained. All experiments were performed according to the National Institutes of Health Guide for the Care and Use of Laboratory Animals (NIH 1996), and all efforts were made to minimize the suffering of the animals and to reduce the number of animals used in experiments. The project was approved by the Animal Ethics Committee of the Federal University of Ceará (protocol no. 114/2011).
Drugs
CORT (Sigma-Aldrich, St. Louis, MO, USA) was dissolved in a saline solution containing 0.1% dimethyl sulfoxide and 0.3% Tween-80. Corticosterone 20 mg/kg was administered as a single daily subcutaneous injection, from 09:00 to 11:30 a.m. for 21 consecutive days. The dosage and route of administration for CORT was selected based on previous studies (Zhao et al. 2008; Silva et al. 2013; de Sousa et al. 2015). ALA (Sigma-Aldrich, St. Louis, MO, USA) was dissolved in distilled water and 0.2% carboxymethyl cellulose and orally administered (p.o.) for 7 consecutive days at doses of 100 or 200 mg/kg according to previous studies (Silva et al. 2013, 2016; de Sousa et al. 2015). Desvenlafaxine succinate monohydrate (DVS, Pristiq®, Wyeth Lab) was dissolved in distilled water and administered orally (p.o.) for 7 consecutive days at the doses of 10 or 20 mg/kg. DVS was administered alone or 1 h before the administration of ALA. The dosages for DVS were calculated from human doses on a milligram per square meter basis (Reagan-Shaw et al. 2008).
Treatment groups
The animals were randomly divided into ten experimental groups and each group was allocated in a different box, as shown in Fig. 1.
Control group: Mice in this group received daily injections of saline solution containing 0.1% dimethyl sulfoxide and Tween-80 0.3% (s.c.) once a day, between 09:00 and 11:30 a.m., for 21 days.
CORT-induced depression model: Mice in this group received daily subcutaneous injections of CORT (20 mg/kg, s.c.) once a day, between 09:00 and 11:30 a.m., for 21 days (Zhao et al. 2008; Silva et al. 2013; de Sousa et al. 2015).
Corticosterone-induced depression model and treatment with DVS or ALA alone: Mice in these groups received repeated injections of CORT for 14 days to induce depressive-like behavior. From the 15th to 21st days of administration, the animals were randomly divided into the four following groups of treatment: CORT and DVS (10 or 20 mg/kg) or CORT and ALA (100 or 200 mg/kg).
Corticosterone-induced depression model and treatment with the combination of DVS+ALA: Mice in these groups received repeated injections of CORT for 14 days to induce a depressive-like behavior. From the 15th to 21st days of CORT administration, the mice were randomly divided into groups that were further treated with DVS (10 or 20 mg/kg). One hour after DVS administration, the animals were given ALA (100 or 200 mg/kg). The time interval between the administration of DVS and ALA was set at 1 h because a previous study showed that the maximum mean plasma concentration of DVS in mice occurred 1 h after oral administration of the drug (DeMaio et al. 2011).
For behavioral determinations, each treatment group was randomized in four subgroups. Subgroup 1 was submitted to the tail suspension test, subgroup 2 to the Y-maze task, subgroup 3 to the social interaction, and subgroup 4 to the NOR. Acetylcholinesterase was determined in animals not submitted to behavioral tasks. Figure 1 presents a representation of the experimental design.
Behavioral assessment
Tail suspension test (TST)
For the TST, each mouse was suspended by the tail on the edge of a shelf placed 58 cm above a table top. The mouse was secured in place via an adhesive tape placed approximately 1 cm from the tip of the tail. The time during which the mouse remained immobile over a 6-min period was recorded. As previously described, each animal was submitted to this test only once (Steru 1985).
Social interaction test (SIT)
The apparatus consisted of a box divided into three chambers with a small opening between the compartments. In each of the two side chambers, an iron cage was placed with a probe mouse or empty. Mice were allowed 5 min exploration. Afterwards, an unfamiliar, same-sex probe mouse was placed in one of two restraining cages. Social preference was defined as: (% time spent in the social chamber) − (% time spent in the opposite chamber) (Radyushkin et al. 2009).
Novel object recognition test (NOR)
This test is widely used to assess the ability to memorize and recognize new and already known objects. On the first day, before any procedure, considered the day of habituation, the animal was placed in the center of the apparatus and left for 5 min with no object. After 24 h, in the training session, the animal was placed back on the box with two identical objects (A1 and A2), double lego toys, placed in the middle of the box and is left for 5 min for the exploration of the new environment. The time spent exploring each object was recorded for further analysis through the recognition rate. On the same day 1.5 h after the training session, mice were tested for short-term memory. In this procedure, the animal was placed back into the box, with two similar objects (A1 and B1) in color and size, but of different shapes. Again, the animals explored the object for 5 min and the exploration time was registered. To test long-term memory, mice returned to the box 24 h after the training session, with two objects: one familiar (A1) and another completely new (C1) and different in color, shape, and size. The animal had 5 min to explore the new object (Izquierdo et al. 2006). To analyze the results, we used the recognition index which is calculated as follows: TB1 formula − TA1 / TE, where TB1 is the time spent by the animal in exploring the new object, TA1 is the time spent exploring the familiar object, and TE is the total operating time, the sum of animal exploitation time in the old and new object (Izquierdo et al. 2006).
Y-maze test (YMT)
Each mouse was allowed to freely move through the maze during 8 min. The series of arm entries was recorded visually. An alternation was defined as entries in all three arms on consecutive occasions. The percentage of alternation was calculated as total of alternations / (total arm entries − 2) (Dall’Igna et al. 2007).
Dissection of brain areas
Twenty-four hours after the last drug administration, the animals were sacrificed by rapid decapitation, and the brains were quickly removed and placed on aluminum foil in a Petri dish on ice. PFC, HC, and ST were dissected for the measurement of AChE activity.
To remove the PFC, the anterior portion of the frontal lobes (about 1.5 mm from the olfactory bulb) was removed, and a bilateral section taken with the aid of a microdissection scissors (Machado 2000). After the withdrawal of PFC, following the median sagittal fissure, the cerebral cortical layer of the meninges was removed with the aid of a straight clamp microdissection, which, progressing delicate and tangentially to the lateral ventricles, separated the cortex in all its fronto-occipital extension. The cortex separated has been folded to the side, exposing the hippocampal region (HC) and part of the ST. The HC and ST were isolated from the surrounding structures with a microdissection scissors, oriented with its withdrawal by the diameter of the tuberous visible portion of these nuclei after folding the lateral cortex. After the dissection, the CPF, HC, and ST were placed in microtubes properly identified, weighed, and stored at − 70 °C until use for conducting the test.
Determination of acetylcholinesterase activity
AChE activity was determined by measuring thiocholine production rate, i.e., the rate that the acetylthiocholine (ATC), used as a substrate, is hydrolyzed. The specific activity was expressed in nanomoles of ATC hydrolyzed per milligram of protein per minute (nmol/mg protein/min). Tissues were homogenized in 10% phosphate buffer and 5 L of the homogenate was added to a cuvette containing 500 μL of buffer, 895 μL of distilled water, and 50 μL of dithiobisnitrobenzoic acid (DTNB) (Ellman et al. 1961).
After the absorbance is left at zero, the bucket is removed from the spectrophotometer and added with 50 mL of iodide ATC. Absorbance was recorded for 3 min at a wavelength of 412 nm. The enzyme activity was calculated as changes in absorbance of 3 to 0 min on the protein content contained in the homogenate (Lowry et al. 1951).
Statistical analysis
Statistical analysis was performed with GraphPad Prism 6.0 for Windows, GraphPad Software (San Diego, CA, USA). Homoscedasticity was verified through Bartlett’s test. D’Agostino-Pearson omnibus normality test was performed to verify normal distribution. In the case of parametric data (tail suspension and Y-maze tests), one-way ANOVA followed by Tukey’s was used. In the case of nonparametric data (social interaction, novel object recognition, and activity of AChE tests), Kruskal-Wallis followed by Dunn’s was performed. All results are expressed as means ± SEM (standard errors of the mean). For all analyses, the significance level was set at α = 0.05.
Results
Effects of the administration of CORT, ALA, and DVS on depressive-like behavior of mice subjected to the tail suspension test
The TST was performed to assess depressive-like behavior in all experimental groups (Fig. 2). An increase in the immobility time of animals submitted to CORT was observed when compared to the control animals (P < 0.0001). On the other hand, the administration of DVS (10 or 20) (P < 0.0001) or ALA (100 or 200) (P < 0.0001) alone or in combination (P < 0.0001) reversed the depressive-like alteration induced by CORT (ANOVA: [F(9, 74) = 36.79; P < 0.0001]).
Effects of DVS or ALA treatment alone or in combination on tail suspension test in a chronic CORT-induced depression mice model. Animals received CORT (20 mg/kg s.c.) for 14 days. Between the 15th and 21st days of treatment, mice received in addition to CORT, DVS (10 or 20 mg/kg, p.o.) or ALA (100 or 200 mg/kg, p.o.) or both drugs. Behavioral tests were performed at 1 h after the last administration. Each bar represents the mean ± SEM of n = 6–7 animals/group. aP < 0.05 vs. control and bP < 0.05 vs. CORT, respectively, according to one-way ANOVA followed by Tukey’s multiple comparisons test. Abbreviations: CORT, corticosterone; DVS, desvenlafaxine; ALA, alpha-lipoic acid
Effects of the administration of CORT, ALA, and DVS on social behavior of mice subjected to the social interaction test
In the analysis of social interaction, we observed that the groups CORT (P < 0.05), CORT+DVS10, and CORT+DVS20 (P < 0.01) presented significant deficits in the percentage of social preference when compared to the control group (Fig. 3) [H(10) = 37.80; P < 0.0001]. The administration of DVS10+ALA200 significantly reversed the deficit induced by CORT (P < 0.05).
Effects of DVS or ALA treatment alone or in combination on social interaction test in a chronic CORT-induced depression mice model. Animals received CORT (20 mg/kg s.c.) for 14 days. Between the 15th and 21st days of treatment, mice received in addition to CORT, DVS (10 or 20 mg/kg, p.o.) or ALA (100 or 200 mg/kg, p.o.) or both drugs. Behavioral tests were performed at 1 h after the last administration. Each bar represents the mean ± SEM of n = 6–7 animals/group. aP < 0.05 vs. control, bP < 0.05 vs. CORT, cP < 0.05 vs. CORT+DVS 10 mg/kg, and dP < 0.05 vs. CORT+DVS 20 mg/kg, respectively, according to one-way ANOVA followed by Tukey’s multiple comparisons test. Abbreviations: CORT, corticosterone; DVS, desvenlafaxine; ALA, alpha-lipoic acid
Effects of the administration of CORT, ALA, and DVS on memory of mice subjected to the object recognition test
Corticosterone-treated animals submitted to NOR presented a deficit in short-term memory when compared with the control group (P < 0.01) [H(10) = 48.46; P < 0.0001] (Fig. 4a). The administration of DVS10 maintained CORT-induced cognitive deficits. On the other hand, ALA200 (P < 0.001) and DVS10 with both doses of ALA (P < 0.05) reversed CORT-induced memory recognition impairment. Besides that, that same treatment presented a better index of recognition when compared with CORT+DVS10 (P < 0.01) and CORT+ALA100 (P < 0.01). However, the administration of DVS20+ALA200 did not reverse the effects of CORT and showed significant reduction in recognition index when compared to the group CORT+ALA200 (P < 0.0001).
Effects of DVS or ALA treatment alone or in combination in short-term memory (a) and long-term memory (b) on object recognition test in a chronic CORT-induced depression mice model. Animals received CORT (20 mg/kg s.c.) for 14 days. Between the 15th and 21st days of treatment, mice received in addition to CORT, DVS (10 or 20 mg/kg, p.o.) or ALA (100 or 200 mg/kg, p.o.) or both drugs. Behavioral tests were performed at 1 h after the last administration. Each bar represents the mean ± SEM of n = 6–10 animals/group. In a, aP < 0.05 vs. control, bP < 0.05 vs. CORT, cP < 0.05 vs. CORT+DVS 10 mg/kg, dP < 0.05 vs. CORT+ALA 100 mg/kg, and eP < 0.05 vs. CORT+ALA 200 mg/kg, and in b, aP < 0.05 vs. control, bP < 0.05 vs. CORT, cP < 0.05 vs. CORT+DVS 10 mg/kg, and dP < 0.05 vs. CORT+DVS 20 mg/kg, respectively, according to one-way ANOVA followed by Tukey’s multiple comparisons test. Abbreviations: CORT, corticosterone; DVS, desvenlafaxine; ALA, alpha-lipoic acid
Corticosterone also caused a deficit in long-term memory (Fig. 4b) when compared to the control group (P < 0.001) [H(10) = 40.75; P < 0.0001]. Administration of DVS20 (P < 0.0001) and DVS20+ALA200 (P < 0.05) reversed long-term memory deficit induced by CORT.
Effects of the administration of CORT, ALA, and DVS on memory of mice subjected to the Y-maze test
As illustrated in Fig. 5, treatment with CORT significantly reduced the number of spontaneous alternations when compared with the control group (P < 0.05) ([F(9, 77) = 4.758; P < 0.0001]). Animals treated with DVS10 presented a percentage of alternations similar to the CORT-treated group. On the other hand, the groups CORT+ALA200 (P < 0.05), CORT+DVS20+ALA100 (P < 0.05), and CORT+DVS20+ ALA200 (P < 0.01) presented a reversal of memory impairment when compared to the CORT-treated group. Treatments with DVS20, ALA100, or the combinations of DVS10 with both doses of ALA present no significant alteration.
Effects of DVS or ALA treatment alone or in combination on Y-maze test in a chronic CORT-induced depression mice model. Animals received CORT (20 mg/kg s.c.) for 14 days. Between the 15th and 21st days of treatment, mice received in addition to CORT, DVS (10 or 20 mg/kg, p.o.) or ALA (100 or 200 mg/kg, p.o.) or both drugs. Behavioral tests were performed at 1 h after the last administration. Each bar represents the mean ± SEM of n = 6–10 animals/group. aP < 0.05 vs. control and bP < 0.05 vs. CORT, respectively, according to one-way ANOVA followed by Tukey’s multiple comparisons test. Abbreviations: CORT, corticosterone; DVS, desvenlafaxine; ALA, alpha-lipoic acid
Effects of CORT, ALA, and DVS in acetylcholinesterase activity
The results in Fig. 6 show that treatment with CORT increases the enzymatic activity of AChE in the PFC (P < 0.01) [H(10) = 40.24; P < 0.0001]), HC (P < 0.05) [F(10) = 24.42; P < 0.01]), and ST (P < 0.05) [H(10) = 11.45; P < 0.001]) when compared to the control group.
Effects of DVS or ALA treatment alone or in combination on acetylcholinesterase activity in the PFC (a), HC (b), and ST (c) of mice submitted to chronic CORT-induced depression model. Animals received CORT (20 mg/kg s.c.) for 14 days. Between the 15th and 21st days of treatment, mice received in addition to CORT, DVS (10 or 20 mg/kg, p.o.) or ALA (100 or 200 mg/kg, p.o.) or both drugs. Acetylcholinesterase activity measurement was performed 24 h after the last administration. Each bar represents the mean ± SEM of n = 6–10 animals/group. aP < 0.05 vs. control, bP < 0.05 vs. CORT, cP < 0.05 vs. CORT+ALA100, dP < 0.05 vs. CORT+DVS20, and eP < 0.05 vs. CORT+ALA200, respectively, according to one-way ANOVA followed by Tukey’s multiple comparisons test. Abbreviations: CORT, corticosterone; DVS, desvenlafaxine; ALA, alpha-lipoic acid
In the PFC, ALA200, alone (P < 0.01) or combined with DVS20 (P < 0.05), reversed the effects of CORT in AChE activity. Furthermore, the combination DVS10+ALA100 showed higher enzymatic activity when compared to the control group (P < 0.01).
In the HC, DVS20 (P < 0.01) and the combination DVS20+ALA100 (P < 0.01) reversed the effects of CORT.
In the ST, all treatments (DVS10 or 20, ALA100 and combinations DVS10+ALA100 or 200, DVS20+ALA100 or 200) reversed the effect of CORT (P < 0.05).
Discussion
This study, as far as we know, is the first to show the effects of ALA and DVS combination on working memory performance and social interaction of animals subjected to the model of depression induced by CORT. Behavioral and neurochemical aspects investigated here are seeking evidence related to symptoms and clinical findings, providing preclinical lines of evidence to prospects for treating depression.
Antidepressant-like effect of ALA and DVS in CORT-induced depression
In the present study, depressive-like behavior was evaluated by the TST, a widely used test for screening antidepressant drugs. A number of studies have shown that animals submitted to repeated CORT administration present a depressive-like phenotype as observed by the increases in immobility time in the forced swimming test and TST and anhedonic-like represented by reduction in sucrose consumption in the sucrose preference test (Silva et al. 2013; Mao et al. 2014; Sturm et al. 2015; de Sousa et al. 2015). Our results showed that DVS and ALA exhibited antidepressant-like effect in the CORT-induced model of depression. Desvenlafaxine, the major pharmacologically active metabolite of venlafaxine, has had important antidepressant-like effects in preclinical (Silva et al. 2013, 2016; Wang et al. 2014; de Sousa et al. 2015) and clinical approaches (Kornstein et al. 2014), being prescribed in patients with poor therapeutic response.
Alpha-lipoic acid alone also presented antidepressant-like effects as observed in TST. Indeed, recent reports suggested a possible antidepressant-like effect by the acute and repeated administration of ALA (Silva et al. 2013, 2014; de Sousa et al. 2015). Furthermore, another study demonstrated that ALA restores the levels of reduced glutathione (GSH), the major brain antioxidant; decreases lipid peroxidation (Silva et al. 2016); and increases BDNF levels (de Sousa et al. 2015) in CORT-induced depression model. All these parameters have been shown to be altered in depressed patients (Carballedo et al. 2013; Chung et al. 2013; Dalby et al. 2013) and in animals submitted to CORT-induced model of depression (Huang et al. 2011).
Among the symptoms of depression, social isolation stands out as a significant loss in quality of life of patients with depression (Kupferberg et al. 2016). Based on this fact, here we conducted the SIT. This test is one of the most relevant to investigate the social deficits in animal models (Radyushkin et al. 2009). In our study, CORT for 21 days caused a reduction in the percentage of social preference, replicating previous findings (Vasconcelos et al. 2015a). Indeed, rodents subjected to chronic stress or trauma developed behavioral alterations similar to social anxiety and aversion (Barik et al. 2013; Mineur et al. 2013). These behavioral alterations seems to be related to an overactivation of the hypothalamic-pituitary-adrenal (HPA) axis leading, thus, to high levels of CORT, possibly one of the mechanisms involved in the onset of the behavioral changes (Barik et al. 2013). Moreover, the glucocorticoid receptor has been implicated in the resilience to stress and in the modulation of emotional and social behavior (Barik et al. 2013). In our results, DVS alone could not reverse the social impairment caused by CORT administration, reinforcing the importance of investigating antidepressants that can improve the social behavior of patients with depression.
Alpha-lipoic acid and desvenlafaxine improve cognition in CORT-induced depression
Since cognitive impairment in depression plays a crucial role in the reduction of quality of life and psychosocial dysfunction (Lam et al. 2014; Gonda et al. 2015), here we conducted behavioral tasks to evaluate cognitive alterations in mice. NOR is a useful tool for the study of neural and behavioral processes involved in the acquisition, consolidation, and recall from memory without disturbing the natural behavior of the animal (Ennaceur and Delacour 1988). In this context, NOR measures exploratory behavior, perception, and recognition memory in rodent models. In our study, repeated CORT administration caused deficits in short- and long-term memory. These data point to the fact that HC, the brain area intimately involved in processing memories, is closely linked to the regulation of the HPA axis (Sterner and Kalynchuk 2010). Furthermore, recent findings show that chronic administration of CORT causes reductions of BDNF levels in the HC (de Sousa et al. 2015), possibly impairing synaptogenesis in that brain region. Previous studies indicate that depressive episodes are associated with high concentrations of cortisol in 40–50% of patients, with hypercortisolemia being associated with stress, neural damage, reduced hippocampal volume, and declarative memory deficits (Bremner et al. 1995; Bremner 1999).
Here, the animals administered ALA200 or the combinations DVS10+ALA100 or DVS10+ALA200 presented an improvement in recognition rates in short-term memory. In the evaluation of long-term memory, treatment with DVS20 and the combination DVS20+ALA200 reversed the cognitive impairments caused by CORT. These data suggest a beneficial effect of ALA and DVS in memory being in line with the studies that show similar effects with other antioxidant and antidepressant drugs (Nemets et al. 2002; Scapagnini et al. 2012; Greer et al. 2014). In addition, treatment with ALA shows encouraging results in diseases that present cognitive impairment such as Alzheimer’s disease and schizophrenia (Galasko et al. 2012; Mecocci and Polidori 2012; Ooi et al. 2012; Vasconcelos et al. 2015b). Since distinct mechanisms are involved in short- and long-term processes of memory and the drugs used here may distinctly interfere in these mechanisms, this may be one possible explanation for the different effects of ALA and DVS.
Another interesting result observed here was the response observed with DVS10+ALA100 which is not seen with the treatment of drugs alone. These results can suggest a possible reduction of DVS dosage when administered in combination with ALA.
On the other hand, the group treated with DVS20+ALA200 presented a deficit in short-term memory, noticed by a reduction of the recognition index. Likely, a pharmacodynamic interaction between DVS and ALA at these dosages may explain this deleterious effect.
Spontaneous alternation in Y-maze measures hippocampal-dependent memory with this area being particularly vulnerable in depression (Czéh and Lucassen 2007; Frodl et al. 2008). The hippocampus works like a site of modulatory influence of many types of memory such as working, spatial, verbal, and contextual, among others (Izquierdo and Medina 1991; Bechara et al. 1995).
In our results, CORT administration for 21 days caused a reduction in the number of spontaneous alternations. This data together with the one obtained in NOR reflects a cognitive deficit probably related to the high concentrations of CORT. This finding corroborates data demonstrating that supraphysiologic concentrations of this hormone cause neuronal damage and reduce the size of brain areas such as the HC, amygdala, and PFC, resulting in a series of impairments and cognitive deficits (Drevets 2000, 2001; Jaracz 2008). In addition, several studies suggest that the exposure to stress or CORT compromises learning and hippocampal-dependent memories (Conrad et al. 1999; Coburn-Litvak et al. 2003; Cerqueira et al. 2005).
We also observed that mice treated with ALA200 or DVS20 combined with both ALA100 or 200 presented an increase in the number of spontaneous alternations when compared to animals treated with CORT, evidencing that treatment with DVS presents better response when combined with ALA.
One possible explanation for the ALA-positive effects in cognition is related to its potent antioxidant and anti-inflammatory effects (Schillace et al. 2007; Bist and Bhatt 2009; Silva et al. 2016). Studies have shown that ALA has the property of removing free radicals in both lipid and aqueous media (Chng et al. 2009; Bist and Bhatt 2009) acting as a natural antioxidant and a cofactor for the dehydrogenases of the mitochondrial system (Smith et al. 2004). Its oxidized form is capable of inducing the regeneration of other low molecular weight antioxidants, such as glutathione, coenzyme Q10, and vitamins A and C (Bilska et al. 2007); decreasing the cellular reduction power; and preventing the destruction of glutathione in the cytoplasm and mitochondria (Salinthone et al. 2008). ALA is also able to prevent neuronal damage caused by the reactive oxygen species produced during neurodegenerative diseases. In addition, it acts as a metal chelator, reducing the levels of oxidative stress (Ferreira et al. 2009). It is also attributed to this substance an anti-inflammatory activity by being able to block the action of NFkB (Ying et al. 2011). Thus, we suggest that through these effects, ALA can avoid the damage caused by CORT.
Alterations in acetylcholinesterase activity
Acetylcholine (ACh) is an important neurotransmitter involved in learning and memory processes, an effect related to its binding on muscarinic and nicotinic receptors (Leaderbrand et al. 2016). The mechanisms of ACh on memory are related to increments in the strength of afferent input relative to feedback, resulting in an improvement of theta rhythm oscillations, and by increasing the modification of synapses (Hasselmo 2006). An important observation related to ACh metabolizing enzyme, AChE, is that this enzyme was recently implicated in a constitutive microglial activation with elevated levels of proinflammatory cytokines, factors associated with the pathogenesis of various types of dementia (Gnatek et al. 2012; Furukawa et al. 2014; Arikawa et al. 2016). Hence, to further elucidate the mechanisms involved in the improvement of cognitive impairment induced by CORT, we carried out measurements of AChE activity.
Chronic administration of CORT increased AChE activity in the PFC, a brain structure highly involved in the control of emotional responses, cognitive performance, and synaptic plasticity (Koechlin et al. 2003; Fogaça et al. 2012). Since AChE metabolizes acetylcholine, the increase of this enzyme activity may be related to decreased synaptic levels of ACh. Besides presenting anti-inflammatory effects, the brain cholinergic system is impaired in psychiatric disorders such as depression (Janowsky et al. 1972; Mineur et al. 2013).
Our data showed that ALA, alone or combined with DVS, reversed the cognitive impairment induced by CORT, especially the combinations of ALA200 and DVS. This effect may be related to the restoration of cholinergic pathways leading, thus, to an increase in ACh anti-inflammatory effects, which was not evaluated in the present study. Notably, ALA200 when combined with DVS10 is not able to reverse the effects of CORT on AChE activity. We believe that this combination was not effective because DVS10 alone was like CORT.
Acetylcholine also binds to nicotinic receptors. Of note, nicotinic receptors, mainly the α7 receptors, present important effects in diverse components of cognitive function, including learning, memory, and attention (Levin 2012).
Our data showed that ALA200, alone or combined with DVS20, reversed the cognitive impairment caused by CORT in working memory. This effect was accompanied by reductions in the enzymatic activity of AChE in the PFC, a brain area related to working memory performance (Malm et al. 2006), suggesting that the improvement of working memory is possibly related to the effect of ALA and DVS in the cholinergic system. Several studies point to an association of cholinergic system disruption with other types of dementia as well as with neuropsychiatric disorders, such as schizophrenia, depression, delirium, and traumatic brain injury, being a common mechanism for these diseases (Dilsaver and Coffman 1989; Battaglia 2002; Arciniegas 2003; Overshott and Burns 2005; Raedler et al. 2007; Hshieh et al. 2008; Johannsson et al. 2015). This fact suggests that drugs capable of reducing the activity of AChE may be beneficial for depressive symptoms like cognitive improvement.
In the HC, ACh is one of the main mediators of learning and memory processes. As observed in the PFC, here the administration of CORT increased AChE activity in the HC. This increase is probably one of the mechanisms involved in cognitive impairment shown in CORT-treated animals when evaluated in the NOR, since ACh is one of the main neurotransmitters involved in the hippocampal mechanism related to the performance of this task (Stanley et al. 2012).
Currently, many therapies to treat cognitive disorders involve the inhibition of AChE activity as an attempt to increase the brain levels of ACh (Spencer and Noble 1998; Kumar et al. 2000; McKeith et al. 2000; Masanic et al. 2001; Werber and Rabey 2001). Alpha-lipoic acid has been widely investigated as an alternative therapy in the treatment of Alzheimer’s disease including its combination with anticholinesterase drugs (Bertucci et al. 2011; Galasko et al. 2012; Ooi et al. 2012), although as far as we know this antioxidant was never tested for cognitive deficits related to depression.
In our study, we believe that the different results of AChE activity in the HC and PFC are due to the role of ACh in these brain areas. The hippocampus, besides being an extremely sensitive area such as circulating concentrations of corticosterone (Sterner and Kalynchuk 2010), is rich in cholinergic innervation, which is involved in excitation, learning, and memory (Yi et al. 2015). Data also point to the fact that the removal of hippocampal cholinergic innervation leads to a deregulation of the hypothalamic-pituitary-adrenal axis and reduction of glucocorticoid receptors in this area, showing a relationship between these two systems as well as reinforcing the importance of acetylcholine transmission in this brain region (Han et al. 2002).
It is also important to mention that DVS reversed the cognitive impairment in the Y-maze and NOR only when combined with ALA, showing that the augmentation therapy with antioxidants seems to be beneficial for depressive patients with cognitive symptoms.
Corticosterone also increased AChE activity in ST. This brain area is related to reward, cognition, and movement, being primarily responsible for the symptoms of lack of motivation, fatigue, and psychomotor alterations observed in depressed patients (Harrington 2012; Walther et al. 2012). Thus, this region represents the interface between emotion, cognition, and motor control.
Studies have shown that ACh plays an important role in modulating the release of dopamine in the ST, regulating, therefore, the state of motivation and reward (Surmeier and Graybiel 2012). Striatal deficits in ACh are associated with social isolation and anhedonia, whereas treatment strategies that increase the levels of this neurotransmitter improve this behavior (Berman et al. 2012).
One possible limitation of our experimental design is that the animals of each experimental group were allocated in the same cage, and therefore, the results may have been biased by the “cage effect.” Despite this, it was recently shown, for the first time, that animals exposed to the depression model of chronic unpredictable stress present depression contagion (Boyko et al. 2015). Depression contagion refers to a condition in which a person without mood disorders living with a depressed person present an increased chance of developing depression. Therefore, in order to avoid a possible depression contagion in our animals we decided to keep depressed animals in separated cages from control and treated animals.
Taken together, ALA seems to be a therapeutic perspective for the treatment of depressive symptoms as well as cognitive deficits related to depression. Further studies are needed to better clarify the molecular mechanism related to ALA’s effect in memory, which we consider a limitation of this study.
Conclusion
The combination of ALA and DVS, by reversing the working memory impairments and deficits in social interaction induced by CORT as well as by reducing the activity of AChE in the PFC, HC, and ST, seems to be a promising therapy for the treatment of cognitive and social deficits associated or not with depression. Notably, ALA has a greater effect in reversing depressive-like behavior, working memory, and social deficits when combined with DVS. This augmentation effect of ALA may suggest the use of smaller doses of antidepressants for depression treatment as well as the possibility of treating depression-related comorbidities. Thus, the findings of the present study show that the augmentation therapy with ALA and DVS may be promising not only in the reversal of depressive symptoms but also for the treatment of depression comorbidities such as cognitive and social impairment.
References
Arciniegas DB (2003) The cholinergic hypothesis of cognitive impairment caused by traumatic brain injury. Curr Psychiatry Rep 5:391–399. https://doi.org/10.1007/s11920-003-0074-5
Arikawa M, Kakinuma Y, Noguchi T, Todaka H, Sato T (2016) Donepezil, an acetylcholinesterase inhibitor, attenuates LPS-induced inflammatory response in murine macrophage cell line RAW 264.7 through inhibition of nuclear factor kappa B translocation. Eur J Pharmacol 789:17–26. https://doi.org/10.1016/j.ejphar.2016.06.053
Barik J, Marti F, Morel C et al (2013) Chronic Stress triggers social aversion via glucococorticoid receptor in dopaminoceptive neurons. Science 80(339):332–335. https://doi.org/10.1007/s13398-014-0173-7.2
Battaglia M (2002) Beyond the usual suspects: a cholinergic route for panic attacks. Mol Psychiatry 7:239–246. https://doi.org/10.1038/sj/mp/4000997
Bechara A, Tranel D, Damasio H et al (1995) Double dissociation of conditioning and declarative knowledge relative to the amygdala and hippocampus in humans. Science (80(269):1115 LP–1111118
Berman K, Brodaty H, Withall A, Seeher K (2012) Pharmacologic treatment of apathy in dementia. Am J Geriatr Psychiatry 20:104–122. https://doi.org/10.1097/JGP.0b013e31822001a6
Bertucci C, De Simone A, Pistolozzi M, Rosini M (2011) Reversible human serum albumin binding of lipocrine: a circular dichroism study. Chirality 23:827–832. https://doi.org/10.1002/chir.21006
Bilska A, Dubiel M, Sokołowska-Jezewicz M et al (2007) Alpha-lipoic acid differently affects the reserpine-induced oxidative stress in the striatum and prefrontal cortex of rat brain. Neuroscience 146:1758–1771. https://doi.org/10.1016/j.neuroscience.2007.04.002
Bist R, Bhatt DK (2009) The evaluation of effect of alpha-lipoic acid and vitamin E on the lipid peroxidation, gamma-amino butyric acid and serotonin level in the brain of mice (Mus musculus) acutely intoxicated with lindane. J Neurol Sci 276:99–102. https://doi.org/10.1016/j.jns.2008.09.008
Blokland A (1995) Acetylcholine: a neurotransmitter for learning and memory? Brain Res Rev 21:285–300. https://doi.org/10.1016/0165-0173(95)00016-X
Boyko M, Kutz R, Grinshpun Y et al (2015) Establishment of an animal model of depression contagion. Behav Brain Res 0:358–363. https://doi.org/10.1016/j.bbr.2014.12.017
Bremner JD (1999) Does stress damage the brain. Biol Psychiatry 45:797–805. https://doi.org/10.1016/S0006-3223(99)00009-8
Bremner JD, Randall P, Scott TM et al (1995) MRI-based measurement of hippocampal volume in patients with combat-related posttraumatic stress disorder. Am J Psychiatry 152:973–981. https://doi.org/10.1016/j.biotechadv.2011.08.021
Carballedo A, Morris D, Zill P, Fahey C, Reinhold E, Meisenzahl E, Bondy B, Gill M, Möller HJ, Frodl T (2013) Brain-derived neurotrophic factor Val66Met polymorphism and early life adversity affect hippocampal volume. Am J Med Genet B Neuropsychiatr Genet 162B:183–190. https://doi.org/10.1002/ajmg.b.32130
Cerqueira JJ, Pêgo JM, Taipa R, Bessa JM, Almeida OF, Sousa N (2005) Morphological correlates of corticosteroid-induced changes in prefrontal cortex-dependent behaviors. J Neurosci 25:7792–7800. https://doi.org/10.1523/JNEUROSCI.1598-05.2005
Chng HT, New LS, Neo AH, Goh CW, Browne ER, Chan ECY (2009) Distribution study of orally administered lipoic acid in rat brain tissues. Brain Res 1251:80–86. https://doi.org/10.1016/j.brainres.2008.11.025
Chung CP, Schmidt D, Stein CM, Morrow JD, Salomon RM (2013) Increased oxidative stress in patients with depression and its relationship to treatment. Psychiatry Res 206:213–216. https://doi.org/10.1016/j.psychres.2012.10.018
Coburn-Litvak PS, Pothakos K, Tata DA, McCloskey DP, Anderson BJ (2003) Chronic administration of corticosterone impairs spatial reference memory before spatial working memory in rats. Neurobiol Learn Mem 80:11–23. https://doi.org/10.1016/S1074-7427(03)00019-4
Conrad CD, Lupien SJ, McEwen BS (1999) Support for a bimodal role for type II adrenal steroid receptors in spatial memory. Neurobiol Learn Mem 72:39–46. https://doi.org/10.1006/nlme.1998.3898
Czéh B, Lucassen PJ (2007) What causes the hippocampal volume decrease in depression? Are neurogenesis, glial changes and apoptosis implicated? Eur Arch Psychiatry Clin Neurosci 257:250–260. https://doi.org/10.1007/s00406-007-0728-0
Dalby RB, Elfving B, Poulsen PHP, Foldager L, Frandsen J, Videbech P, Rosenberg R (2013) Plasma brain-derived neurotrophic factor and prefrontal white matter integrity in late-onset depression and normal aging. Acta Psychiatr Scand 128:387–396. https://doi.org/10.1111/acps.12085
Dall’Igna OP, Fett P, Gomes MW et al (2007) Caffeine and adenosine A2a receptor antagonists prevent β-amyloid (25–35)-induced cognitive deficits in mice. Exp Neurol 203:241–245. https://doi.org/10.1016/j.expneurol.2006.08.008
de Sousa CNS, Meneses LN, Vasconcelos GS et al (2015) Reversal of corticosterone-induced BDNF alterations by the natural antioxidant alpha-lipoic acid alone and combined with desvenlafaxine: emphasis on the neurotrophic hypothesis of depression. Psychiatry Res 230:211–219. https://doi.org/10.1016/j.psychres.2015.08.042
DeMaio W, P. Kane C, Nichols AI, et al (2011) Metabolism studies of desvenlafaxine. J Bioequiv Availab 3:151–160. doi: https://doi.org/10.4172/jbb.1000076
Dilsaver SC, Coffman JA (1989) Cholinergic hypothesis of depression: a reappraisal. J Clin Psychopharmacol 9:173–179. https://doi.org/10.1097/00004714-198906000-00003
Dobarro M, Orejana L, Aguirre N, Ramírez MJ (2013) Propranolol reduces cognitive deficits, amyloid β levels, tau phosphorylation and insulin resistance in response to chronic corticosterone administration. Int J Neuropsychopharmacol 16:1351–1360. https://doi.org/10.1017/S1461145712001393
Drevets WC (2000) Neuroimaging studies of mood disorders. Biol Psychiatry 48:813–829
Drevets WC (2001) Neuroimaging and neuropathological studies of depression: implications for the cognitive-emotional features of mood disorders. Curr Opin Neurobiol 11:240–249. https://doi.org/10.1016/S0959-4388(00)00203-8
Ellman GL, Courtney KD, Andres V, Featherstone RM (1961) A new and rapid colorimetric determination of acetylcholinesterase activity. Biochem Pharmacol 7:88–95. https://doi.org/10.1016/0006-2952(61)90145-9
Ennaceur A, Delacour J (1988) A new one-trial test for neurobiological studies of memory in rats. 1: behavioral data. Behav Brain Res 31:47–59. https://doi.org/10.1016/0166-4328(88)90157-X
Farhat SM, Mahboob A, Ahmed T (2017) Cortex- and amygdala-dependent learning and nicotinic acetylcholine receptor gene expression is severely impaired in mice orally treated with AlCl3. Biol Trace Elem Res 179:1–11. https://doi.org/10.1007/s12011-017-0942-1
Feng B, Zhao X-Y, Song Y-Z, Liang WN, Liu JL (2017) Sarsasapogenin reverses depressive-like behaviors and nicotinic acetylcholine receptors induced by olfactory bulbectomy. Neurosci Lett 639:173–178. https://doi.org/10.1016/j.neulet.2016.12.025
Ferreira PMP, Militão GCG, Freitas RM (2009) Lipoic acid effects on lipid peroxidation level, superoxide dismutase activity and monoamines concentration in rat hippocampus. Neurosci Lett 464:131–134. https://doi.org/10.1016/j.neulet.2009.08.051
Fogaça MV, Aguiar DC, Moreira FA, Guimarães FS (2012) The endocannabinoid and endovanilloid systems interact in the rat prelimbic medial prefrontal cortex to control anxiety-like behavior. Neuropharmacology 63:202–210. https://doi.org/10.1016/j.neuropharm.2012.03.007
Fried EI, Nesse RM (2014) Depression is not a consistent syndrome: an investigation of unique symptom patterns in the STAR*D study. J Affect Disord 172C:96–102. https://doi.org/10.1016/j.jad.2014.10.010
Frodl T, Jäger M, Smajistrlova I et al (2008) Effect of hippocampal and amygdala volumes on clinical outcomes in major depression: a 3-year prospective magnetic resonance imaging study. J Psychiatry Neurosci 33:423–430
Furukawa S, Yang L, Sameshima H (2014) Galantamine, an acetylcholinesterase inhibitor, reduces brain damage induced by hypoxia-ischemia in newborn rats. Int J Dev Neurosci 37:52–57. https://doi.org/10.1016/j.ijdevneu.2014.06.011
Galasko DR, Peskind E, Clark CM, Quinn JF, Ringman JM, Jicha GA, Cotman C, Cottrell B, Montine TJ, Thomas RG, Aisen P, Alzheimer’s Disease Cooperative Study (2012) Antioxidants for Alzheimer disease: a randomized clinical trial with cerebrospinal fluid biomarker measures. Arch Neurol 69:836–841. https://doi.org/10.1001/archneurol.2012.85
Gnatek Y, Zimmerman G, Goll Y, Najami N, Soreq H, Friedman A (2012) Acetylcholinesterase loosens the brain’s cholinergic anti-inflammatory response and promotes epileptogenesis. Front Mol Neurosci 5:1–10. https://doi.org/10.3389/fnmol.2012.00066
Gonda X, Pompili M, Serafini G, Carvalho AF, Rihmer Z, Dome P (2015) The role of cognitive dysfunction in the symptoms and remission from depression. Ann General Psychiatry 14:27. https://doi.org/10.1186/s12991-015-0068-9
Greer TL, Sunderajan P, Grannemann BD, Kurian BT, Trivedi MH (2014) Does duloxetine improve cognitive function independently of its antidepressant effect in patients with major depressive disorder and subjective reports of cognitive dysfunction? Depress Res Treat 2014:1–13. https://doi.org/10.1155/2014/627863
Gregus A, Wintink AJ, Davis AC, Kalynchuk LE (2005) Effect of repeated corticosterone injections and restraint stress on anxiety and depression-like behavior in male rats. Behav Brain Res 156:105–114. https://doi.org/10.1016/j.bbr.2004.05.013
Han JS, Bizon JL, Chun HJ, Maus CE, Gallagher M (2002) Decreased glucocorticoid receptor mRNA and dysfunction of HPA axis in rats after removal of the cholinergic innervation to hippocampus. Eur J Neurosci 16:1399–1404. https://doi.org/10.1046/j.1460-9568.2002.02191.x
Harrington ME (2012) Neurobiological studies of fatigue. Prog Neurobiol 99:93–105. https://doi.org/10.1016/j.pneurobio.2012.07.004
Hasselbalch BJ, Knorr U, Kessing LV (2011) Cognitive impairment in the remitted state of unipolar depressive disorder: a systematic review. J Affect Disord 134:20–31. https://doi.org/10.1016/j.jad.2010.11.011
Hasselmo ME (2006) The role of acetylcholine in learning and memory. Curr Opin Neurobiol 16:710–715. https://doi.org/10.1016/j.conb.2006.09.002
Hermann R, Mungo J, Cnota PJ, Ziegler D (2014) Enantiomer-selective pharmacokinetics, oral bioavailability, and sex effects of various alpha-lipoic acid dosage forms. Clin Pharmacol 6:195–204. https://doi.org/10.2147/CPAA.S71574
Herrera-Guzmán I, Gudayol-Ferré E, Herrera-Abarca JE, Herrera-Guzmán D, Montelongo-Pedraza P, Padrós Blázquez F, Peró-Cebollero M, Guàrdia-Olmos J (2010) Major depressive disorder in recovery and neuropsychological functioning: effects of selective serotonin reuptake inhibitor and dual inhibitor depression treatments on residual cognitive deficits in patients with major depressive disorder in recovery. J Affect Disord 123:341–350. https://doi.org/10.1016/j.jad.2009.10.009
Hshieh TT, Fong TG, Marcantonio ER, Inouye SK (2008) Cholinergic deficiency hypothesis in delirium: a synthesis of current evidence. J Gerontol A Biol Sci Med Sci 63:764–772. https://doi.org/10.1093/gerona/63.7.764
Huang Z, Zhong X-M, Li Z-Y, Feng CR, Pan AJ, Mao QQ (2011) Curcumin reverses corticosterone-induced depressive-like behavior and decrease in brain BDNF levels in rats. Neurosci Lett 493:145–148. https://doi.org/10.1016/j.neulet.2011.02.030
Iijima M, Ito A, Kurosu S, Chaki S (2010) Pharmacological characterization of repeated corticosterone injection-induced depression model in rats. Brain Res 1359:75–80. https://doi.org/10.1016/j.brainres.2010.08.078
Izquierdo I, Medina JH (1991) GABAA receptor modulation of memory: the role of endogenous benzodiazepines. Trends Pharmacol Sci 12:260–265. https://doi.org/10.1016/0165-6147(91)90567-C
Izquierdo I, Bevilaqua LRM, Rossato JI, Bonini JS, Medina JH, Cammarota M (2006) Different molecular cascades in different sites of the brain control memory consolidation. Trends Neurosci 29:496–505. https://doi.org/10.1016/j.tins.2006.07.005
Jaeger J, Berns S, Uzelac S, Davis-Conway S (2006) Neurocognitive deficits and disability in major depressive disorder. Psychiatry Res 145:39–48. https://doi.org/10.1016/j.psychres.2005.11.011
Janowsky D, Davis J, El-Yousef MK, Sekerke HJ (1972) A cholinergic-adrenergic hypothesis of mania and depression. Lancet 300:632–635. https://doi.org/10.1016/S0140-6736(72)93021-8
Jaracz J (2008) The anatomy of depression in light of evidence from neuroimaging studies. Psychiatr Pol 42:875–888
Johannsson M, Snaedal J, Johannesson GH, Gudmundsson TE, Johnsen K (2015) The acetylcholine index: an electroencephalographic marker of cholinergic activity in the living human brain applied to Alzheimer’s disease and other dementias. Dement Geriatr Cogn Disord 39:132–142. https://doi.org/10.1159/000367889
Kessler R (2003) Epidemiology of women and depression. J Affect Disord 74:5–13. https://doi.org/10.1016/S0165-0327(02)00426-3
Kessler RC (2012) The costs of depression. Psychiatr Clin N Am 35:1–14. https://doi.org/10.1016/j.psc.2011.11.005
Koechlin E, Ody C, Kouneiher F (2003) The architecture of cognitive control in the human prefrontal cortex. Science 302:1181–1185. https://doi.org/10.1126/science.1088545
Kornstein SG, McIntyre RS, Thase ME, Boucher M (2014) Desvenlafaxine for the treatment of major depressive disorder. Expert Opin Pharmacother 15:1449–1463. https://doi.org/10.1517/14656566.2014.923403
Kumar V, Anand R, Messina J, Hartman R, Veach J (2000) An efficacy and safety analysis of Exelon in Alzheimer’s disease patients with concurrent vascular risk factors. Eur J Neurol 7:159–169
Kupferberg A, Bicks L, Hasler G (2016) Social functioning in major depressive disorder. Neurosci Biobehav Rev 69:313–332. https://doi.org/10.1016/j.neubiorev.2016.07.002
Lam RW, Kennedy SH, Mclntyre RS, Khullar A (2014) Cognitive dysfunction in major depressive disorder: effects on psychosocial functioning and implications for treatment. Can J Psychiatr 59:649–654. https://doi.org/10.1177/070674371405901206
Leaderbrand K, Chen HJ, Corcoran KA, Guedea AL, Jovasevic V, Wess J, Radulovic J (2016) Muscarinic acetylcholine receptors act in synergy to facilitate learning and memory. Learn Mem 23:631–638. https://doi.org/10.1101/lm.043133.116
Lee RSC, Hermens DF, Porter MA, Redoblado-Hodge MA (2012) A meta-analysis of cognitive deficits in first-episode major depressive disorder. J Affect Disord 140:113–124. https://doi.org/10.1016/j.jad.2011.10.023
Levin ED (2012) alpha7-Nicotinic receptors and cognition. Curr Drug Targets 13:602–606
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ (1951) Protein measurement with the Folin phenol reagent. J Biol Chem 193:265–275. https://doi.org/10.1016/0304-3894(92)87011-4
Machado, ABM (2000) Functional Neuroanatomy. Atheneu, São Paulo
Malm J, Bergenheim AT, Enblad P, Hardemark HG, Koskinen LOD, Naredi S, Nordstrom CH, Norrving B, Uhlin J, Lindgren A (2006) The Swedish Malignant Middle cerebral artery Infarction Study: long-term results from a prospective study of hemicraniectomy combined with standardized neurointensive care. Acta Neurol Scand 113:25–30. https://doi.org/10.1111/j.1600-0404.2005.00537.x
Mao QQ, Huang Z, Zhong XM, Xian YF, Ip SP (2014) Piperine reverses the effects of corticosterone on behavior and hippocampal BDNF expression in mice. Neurochem Int 74:36–41. https://doi.org/10.1016/j.neuint.2014.04.017
Masanic C a, Bayley MT, VanReekum R, Simard M (2001) Open-label study of donepezil in traumatic brain injury. Arch Phys Med Rehabil 82:896–901. doi: https://doi.org/10.1053/apmr.2001.23833
McKeith I, Del Ser T, Spano P et al (2000) Efficacy of rivastigmine in dementia with Lewy bodies: a randomised, double-blind, placebo-controlled international study. Lancet 356:2031–2036. https://doi.org/10.1016/S0140-6736(00)03399-7
Mecocci P, Polidori MC (2012) Antioxidant clinical trials in mild cognitive impairment and Alzheimer’s disease. Biochim Biophys Acta - Mol Basis Dis 1822:631–638. https://doi.org/10.1016/j.bbadis.2011.10.006
Mineur YS, Obayemi A, Wigestrand MB, Fote GM, Calarco CA, Li AM, Picciotto MR (2013) Cholinergic signaling in the hippocampus regulates social stress resilience and anxiety- and depression-like behavior. Proc Natl Acad Sci U S A 110:3573–3578. https://doi.org/10.1073/pnas.1219731110
Morimoto SS, Kanellopoulos D, Manning KJ, Alexopoulos GS (2015) Diagnosis and treatment of depression and cognitive impairment in late life. Ann N Y Acad Sci 1345:36–46. https://doi.org/10.1111/nyas.12669
Moylan S, Berk M, Dean OM, Samuni Y, Williams LJ, O’Neil A, Hayley AC, Pasco JA, Anderson G, Jacka FN, Maes M (2014) Oxidative & nitrosative stress in depression: why so much stress? Neurosci Biobehav Rev 45:46–62. https://doi.org/10.1016/j.neubiorev.2014.05.007
Murrough JW, Iacoviello B, Neumeister A, Charney DS, Iosifescu DV (2011) Cognitive dysfunction in depression: neurocircuitry and new therapeutic strategies. Neurobiol Learn Mem 96:553–563. https://doi.org/10.1016/j.nlm.2011.06.006
Nelson JC, Devanand DP (2011) A systematic review and meta-analysis of placebo-controlled antidepressant studies in people with depression and dementia. J Am Geriatr Soc 59:577–585. https://doi.org/10.1111/j.1532-5415.2011.03355.x
Nemets B, Stahl Z, Belmaker RH (2002) Addition of omega-3 fatty acid to maintenance medication treatment for recurrent unipolar depressive disorder. Am J Psychiatry 159:477–479. https://doi.org/10.1176/appi.ajp.159.3.477
NIH (1996) Guide for the care and use of laboratory animals—Institute of Laboratory Animal Research–National Research Council. Washington, National Academies Press
Ooi L, Patel M, Münch G (2012) The thiol antioxidant lipoic acid and Alzheimer’s disease. Syst Biol Free Radicals Antioxid:2275–2288
Overshott R, Burns A (2005) Cholinesterase inhibitors: in search of cholinergic deficits. Adv Psychiatr Treat 11:321–324. https://doi.org/10.1192/apt.11.5.321
Panza F, Frisardi V, Capurso C, D’Introno A, Colacicco AM, Imbimbo BP, Santamato A, Vendemiale G, Seripa D, Pilotto A, Capurso A, Solfrizzi V (2010) Late-life depression, mild cognitive impairment, and dementia: possible continuum? Am J Geriatr Psychiatry 18:98–116. https://doi.org/10.1097/JGP.0b013e3181b0fa13
Radyushkin K, Hammerschmidt K, Boretius S, Varoqueaux F, el-Kordi A, Ronnenberg A, Winter D, Frahm J, Fischer J, Brose N, Ehrenreich H (2009) Neuroligin-3-deficient mice: model of a monogenic heritable form of autism with an olfactory deficit. Genes Brain Behav 8:416–425. https://doi.org/10.1111/j.1601-183X.2009.00487.x
Raedler TJ, Bymaster FP, Tandon R, Copolov D, Dean B (2007) Towards a muscarinic hypothesis of schizophrenia. Mol Psychiatry 12:232–246. https://doi.org/10.1038/sj.mp.4001924
Reagan-Shaw S, Nihal M, Ahmad N (2008) Dose translation from animal to human studies revisited. FASEB J 22:659–661. https://doi.org/10.1096/fj.07-9574LSF
Rock PL, Roiser JP, Riedel WJ, Blackwell AD (2014) Cognitive impairment in depression: a systematic review and meta-analysis. Psychol Med 44:2029–2040. https://doi.org/10.1017/S0033291713002535
Salazar MR (2000) Alpha lipoic acid: a novel treatment for depression. Med Hypotheses 55:510–512. https://doi.org/10.1054/mehy.2000.1103
Salinthone S, Yadav V, Bourdette DN, Carr DW (2008) Lipoic acid: a novel therapeutic approach for multiple sclerosis and other chronic inflammatory diseases of the CNS. Endocr Metab Immune Disord Drug Targets 8:132–142. https://doi.org/10.2174/187153008784534303
Scapagnini G, Davinelli S, Drago F, de Lorenzo A, Oriani G (2012) Antioxidants as antidepressants: fact or fiction? CNS Drugs 26:477–490. https://doi.org/10.2165/11633190-000000000-00000
Schillace RV, Pisenti N, Pattamanuch N, Galligan S, Marracci GH, Bourdette DN, Carr DW (2007) Lipoic acid stimulates cAMP production in T lymphocytes and NK cells. Biochem Biophys Res Commun 354:259–264. https://doi.org/10.1016/j.bbrc.2006.12.195
Silva MCC, De Sousa CNS, Sampaio LRL et al (2013) Augmentation therapy with alpha-lipoic acid and desvenlafaxine: a future target for treatment of depression? Naunyn Schmiedeberg's Arch Pharmacol 386:685–695. https://doi.org/10.1007/s00210-013-0867-y
Silva MCC, Sampaio LRL, de Araújo DP et al (2014) Central effects of lipoic acid associated with paroxetine in mice. Am J Ther 21:85–90. https://doi.org/10.1097/MJT.0b013e318235f1a4
Silva MCC, de Sousa CNS, Gomes PXL, de Oliveira GV, Araújo FYR, Ximenes NC, da Silva JC, Silva Vasconcelos G, Leal LKAM, Macêdo D, Vasconcelos SMM (2016) Evidence for protective effect of lipoic acid and desvenlafaxine on oxidative stress in a model depression in mice. Prog Neuro-Psychopharmacol Biol Psychiatry 64:142–148. https://doi.org/10.1016/j.pnpbp.2015.08.002
Smith AR, Shenvi SV, Widlansky M, Suh JH, Hagen TM (2004) Lipoic acid as a potential therapy for chronic diseases associated with oxidative stress. Curr Med Chem 11:1135–1146. https://doi.org/10.2174/0929867043365387
Spencer CM, Noble S (1998) Rivastigmine. A review of its use in Alzheimer’s disease. Drugs Aging 13:391–411
Stanley EM, Wilson MA, Fadel JR (2012) Hippocampal neurotransmitter efflux during one-trial novel object recognition in rats. Neurosci Lett 511:38–42. https://doi.org/10.1016/j.neulet.2012.01.033
Stepanichev M, Markov D, Pasikova N, Gulyaeva N (2016) Behavior and the cholinergic parameters in olfactory bulbectomized female rodents: difference between rats and mice. Behav Brain Res 297:5–14. https://doi.org/10.1016/j.bbr.2015.09.033
Sterner EY, Kalynchuk LE (2010) Behavioral and neurobiological consequences of prolonged glucocorticoid exposure in rats: relevance to depression. Prog Neuro-Psychopharmacol Biol Psychiatry 34:777–790. https://doi.org/10.1016/j.pnpbp.2010.03.005
Steru L (1985) The tail suspension test: a new method for screening antidepressants in mice. Psychopharmacology 85:367–370
Sturm M, Becker A, Schroeder A, Bilkei-Gorzo A, Zimmer A (2015) Effect of chronic corticosterone application on depression-like behavior in C57BL/6N and C57BL/6J mice. Genes, Brain Behav 14:292–300. https://doi.org/10.1111/gbb.12208
Surmeier DJ, Graybiel AM (2012) A feud that wasn’t: acetylcholine evokes dopamine release in the striatum. Neuron 75:1–3. https://doi.org/10.1016/j.neuron.2012.06.028
Trivedi MH, Greer TL (2014) Cognitive dysfunction in unipolar depression: implications for treatment. J Affect Disord 152–154:19–27. https://doi.org/10.1016/j.jad.2013.09.012
Trivedi MH, Rush AJ, Gaynes BN, Stewart JW, Wisniewski SR, Warden D, Ritz L, Luther JF, Stegman D, Deveaugh-Geiss J, Howland R (2007) Maximizing the adequacy of medication treatment in controlled trials and clinical practice: STAR(*)D measurement-based care. Neuropsychopharmacology 32:2479–2489. https://doi.org/10.1038/sj.npp.1301390
Trofimiuk E, Braszko JJ (2015) Ciproxifan differentially modifies cognitive impairment evoked by chronic stress and chronic corticosterone administration in rats. Behav Brain Res 283:145–153. https://doi.org/10.1016/j.bbr.2015.01.038
Vasconcelos AS, Oliveira ICM, Vidal LTM, Rodrigues GC, Gutierrez SJC, Barbosa-Filho JM, Vasconcelos SMM, de França Fonteles MM, Gaspar DM, de Sousa FCF (2015a) Subchronic administration of riparin III induces antidepressive-like effects and increases BDNF levels in the mouse hippocampus. Fundam Clin Pharmacol 29:394–403. https://doi.org/10.1111/fcp.12120
Vasconcelos GS, Ximenes NC, de Sousa CNS, Oliveira TQ, Lima LLL, de Lucena DF, Gama CS, Macêdo D, Vasconcelos SMM (2015b) Alpha-lipoic acid alone and combined with clozapine reverses schizophrenia-like symptoms induced by ketamine in mice: participation of antioxidant, nitrergic and neurotrophic mechanisms. Schizophr Res 165:163–170. https://doi.org/10.1016/j.schres.2015.04.017
Vaughn McCall W, Dunn AG (2003) Cognitive deficits are associated with functional impairment in severely depressed patients. Psychiatry Res 121:179–184. https://doi.org/10.1016/j.psychres.2003.09.003
Walther S, Hügli S, Höfle O, Federspiel A, Horn H, Bracht T, Wiest R, Strik W, Müller TJ (2012) Frontal white matter integrity is related to psychomotor retardation in major depression. Neurobiol Dis 47:13–19. https://doi.org/10.1016/j.nbd.2012.03.019
Wang J, Qiao J, Zhang Y, Wang H, Zhu S, Zhang H, Hartle K, Guo H, Guo W, He J, Kong J, Huang Q, Li XM (2014) Desvenlafaxine prevents white matter injury and improves the decreased phosphorylation of the rate-limiting enzyme of cholesterol synthesis in a chronic mouse model of depression. J Neurochem 131:229–238. https://doi.org/10.1111/jnc.12792
Werber EA, Rabey JM (2001) The beneficial effect of cholinesterase inhibitors on patients suffering from Parkinson’s disease and dementia. J Neural Transm 108:1319–1325. https://doi.org/10.1007/s007020100008
Yi F, Catudio-Garrett E, Gábriel R et al (2015) Hippocampal “cholinergic interneurons” visualized with the choline acetyltransferase promoter: anatomical distribution, intrinsic membrane properties, neurochemical characteristics, and capacity for cholinergic modulation. Front Synaptic Neurosci 7. https://doi.org/10.3389/fnsyn.2015.00004
Ying Z, Kampfrath T, Sun Q, Parthasarathy S, Rajagopalan S (2011) Evidence that α-lipoic acid inhibits NF-κB activation independent of its antioxidant function. Inflamm Res 60:219–225. https://doi.org/10.1007/s00011-010-0256-7
Zhang J-C, Yao W, Ren Q, Yang C, Dong C, Ma M, Wu J, Hashimoto K (2016) Depression-like phenotype by deletion of α7 nicotinic acetylcholine receptor: role of BDNF-TrkB in nucleus accumbens. Sci Rep 6:36705. https://doi.org/10.1038/srep36705
Zhao Y, Ma R, Shen J, Su H, Xing D, du L (2008) A mouse model of depression induced by repeated corticosterone injections. Eur J Pharmacol 581:113–120. https://doi.org/10.1016/j.ejphar.2007.12.005
Funding
This study was supported by Brazilian Government Institutions National Council for Scientific and Technological Development (CNPq) which provides research grants, Higher Education Personnel Improvement Coordination (CAPES), and Cearense Foundation for the Support of Scientific and Technological Development (FUNCAP) which provided financial support to PhD program in Pharmacology.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
ESM 1
(DOCX 36 kb)
Rights and permissions
About this article
Cite this article
de Sousa, C.N.S., Meneses, L.N., Vasconcelos, G.S. et al. Neuroprotective evidence of alpha-lipoic acid and desvenlafaxine on memory deficit in a neuroendocrine model of depression. Naunyn-Schmiedeberg's Arch Pharmacol 391, 803–817 (2018). https://doi.org/10.1007/s00210-018-1509-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-018-1509-1