Abstract
Purpose
The purpose of this study was to compare the maximum load to failure and stiffness of three medial patella-femoral ligament (MPFL) reconstruction techniques: (i) suture anchor fixation (SA), (ii) interference screw fixation (SF), and (iii) suture knot (SK) patellar fixation. The null hypothesis was that the comparison between these three different patella fixation techniques would show no difference in the ultimate failure load and stiffness.
Methods
Reconstruction of the MPFL with gracilis tendon autograft was performed in 12 pairs of fresh-frozen cadaveric knees (24 knees total; mean age, 63.6 \(\pm \) 8.0 years). The specimens were randomly distributed into 3 groups of 8 specimens; SA reconstruction was completed with two 3.0-mm metal suture anchors; (SF) fixation was accomplished by two 6-mm bio-composite interference screws; SK fixation at the lateral side of the patella was accomplished after drilling two semi-patellar tunnels with a diameter of 4.5 mm. The reconstructions were subjected to cyclic loading for 10 cycles to 30 N and tested to failure at a constant displacement rate of 15 mm/min using a materials-testing machine (MTS 810 Universal Testing System). The final load of failure (N), stiffness (N / mm) and failure mode was recorded in each specimen and followed by statistical analysis.
Results
There was no significant difference in mean ultimate failure load among the three groups. The SK group failed at a mean (\(\pm \) SD) ultimate load of 253.5 \(\pm \) 38.2 N, the SA group failed at 243 \(\pm \) 41.9 N and the SF group at 263.2 \(\pm \) 9.06 N. The SF group had a mean stiffness of 37.8 \(\pm \) 5.7 N/mm. This was significantly higher (p < 0.05) than the mean stiffness value achieved for the SK group 21.4 \(\pm \) 9.5 N/mm and the SA group 18.7 \(\pm \) 3.4 N/mm. The most common mode of failure in the SA group was anchor pullout, and in the SK group was failure at the graft–suture interface. All the reconstructions in the SF group failed due to tendon graft slippage from the tunnel.
Conclusion
Load to failure was not significantly different between the 3 techniques. However, screw fixation was found to be significantly stronger than the anchor and the suture knot fixation in terms of rigidity of the reconstruction. From a clinical point of view, all methods of fixation can be used reliably for MPFL reconstruction, since they were found to be stronger than the native MPFL.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Anatomy and biomechanics of the medial patellofemoral ligament (MPFL) have been studied in the last decades [1, 2, 4, 7, 15, 17, 18, 20, 23]. MPFL reconstruction is a surgical option in patients with recurrent dislocations and is currently the first-choice procedure for patients after more than 1 or 2 episodes of patellar dislocation [8, 9, 11, 22]. A variety of surgical techniques for anatomic reconstruction of the MPFL are available in the literature. However, there is no consensus as to which technique yields the best clinical outcome [6, 10, 12, 14, 16, 19, 20, 25, 26, 30,31,32, 34,35,36,37,38,39].
A two-bundle technique, with free tendon grafts replicates the broad attachment site of the native MPFL (fan-shaped insertion) on the patella [36, 40, 41]. Although there are different points of view regarding the graft choice, the majority of them use gracilis or semitendinosus as the graft of choice [6, 11, 12, 25, 26, 30,31,32, 34,35,36,37,38]. The differences of these surgical techniques, concern patella fixation since femoral fixation with a bio-composite screw at the Schöttle point allows isometric adjustments of the graft, resulting in a good clinical outcome [36,37,38]. Some of the popular techniques include utilization of implants, such as suture-anchors [10, 19, 30] and interference screws for graft fixation of the patella [25, 36]. Others describe anatomic hardware-free patellar fixation, whereby the graft is passed through 2 bone tunnels in the patella, or a bone bridge is created on the medial margin of the patella [10, 12, 19, 26, 35].
Several biomechanical studies have been performed to evaluate the biomechanical properties of these techniques, but very few of them have been performed on fresh-frozen human knees [14, 30,31,32]. However, fixation of the graft in a hardware-free patellar fixation using two transverse semi-patellar tunnels has never been studied biomechanically (the modified Siebold technique) [35].
The purpose of this study, was to evaluate the biomechanics (the ultimate failure load and stiffness) of 3 patellar fixation techniques for MPFL reconstruction: (i) suture anchor fixation (SA), (ii) interference screw fixation (SF) and (iii) suture knot (SK), a hardware-free patellar fixation with two semi-patellar tunnels. These surgical techniques employ two points of patellar fixation (upper half of the patella) in an attempt to best recreate the native MPFL anatomy. The null hypothesis was that the comparison between these three different patella fixation techniques would show no difference in the ultimate failure load and stiffness. Furthermore, it was hypothesized that all methods of fixation would provide sufficient strength to use them in clinical practice, for MPFL reconstruction.
Materials and methods
This study was approved by IRB (Institutional Review Board) of the Medical School of University of Thessaly as part of the PhD thesis of one of the authors (ID number 2754). A total of 24 fresh-frozen cadaveric knees (12 matched pairs; 7 male, 5 female; mean age, 63.66 \(\pm \) 9.0 years) were obtained through an Anatomy Donation Program and stored at – 21 °C. The specimens were thawed for 24 h before biomechanical testing at room temperature (18°). There was no medical history of any bone or soft-tissue injury, surgery or osteoporosis in any of the 24 fresh-frozen knee cadavers. The specimens were randomized by a means random number generator into 3 groups (each with 8 specimens), based on the method used to fix the graft to the medial patella: SA group, SF group and SK group. The knees were randomized so that when one cadaveric knee was assigned to a group, the opposite knee from the same cadaveric specimen was assigned to another cohort.
The gracilis tendon autograft was harvested, as this graft has proven clinically to be adequate for MPFL reconstruction [16, 37]. The anatomical length of the native MPFL is an average of 53 mm [35]. A running, locking Krackow suture was placed up to approximately 2 cm from each free end with a No. 2 non-absorbable suture (Ethibond suture 2). For the SA group, the free ends of the graft were sutured together to form a loop.
Patellar fixation techniques
A longitudinal incision (2–3 cm) was performed on the anteromedial side of the patella, the medial aspect of the patella was exposed to the bone surface after subcutaneous preparation, without penetrating the 3rd layer (joint capsule) as Warren and Marshall described [42]. The native MPFL was removed during this procedure.
In the SK group, two blind transverse 2 cm bone tunnels with a diameter of 4 mm were created, for graft fixation at the medial margin of the patella. A guide pin of 2.0-mm with an eyelet diameter was transversely inserted from the midpoint of the medial edge of the patella to the lateral border transversely, with the help of an anterior-cruciate-ligament-reconstruction tibial-aiming device to avoid breaching of either the articular surface or the anterior cortex. The direction of the K-wire was horizontal, perpendicular to the longitudinal axis of the patella and parallel to the coronal patella plane. A second K-wire was placed 15 mm proximally and transversely to the first pin with an intervening interval of 15 mm, as checked using a ruler. The two K-wires were over-drilled with a cannulated 4.5-mm drill bit 2 cm deep, to create two 2 cm transverse blind bone tunnels at the medial side of the patella. Finally, the sutures of each free graft end went through the eyelets of the K-wires and the K-wires were pulled out with a direction from medial to lateral. Both ends of the tendon graft were pulled in the 2 tunnels and the graft sutures were tied together with tension for stable graft fixation at the lateral patella rim (Fig. 1).
In the SF group, 2 transverse guide pins were drilled through the proximal half of the patella. The guide wires were over-drilled with a cannulated 4.5-mm drill to a depth of 20 mm. The two free sutured graft ends were fixed into the patellar holes one after another, using a 6-mm interference screws (Stryker, Mahwah, NJ, USA), achieving aperture fixation of the graft in the patella. The distance between the screws was 15 mm (Fig. 2).
In the SA group, two metal sutures anchors (Stryker, Mahwah, NJ, USA) with diameter of 3 mm, carrying #2 Force Fiber sutures, were seated 15 mm apart at the proximal half of the medial patella. Tension was applied to sutures, confirming purchase within the medial margin of the patella. Finally, the sutures on the anchors were tied around the graft, securing the graft to the medial patella (Fig. 3).
Biomechanical testing- patella stabilization custom device
For the biomechanical testing, the patella was stabilized with a custom device that would injure neither the patella, nor the reconstructed MPFL and could not be incriminated for any possible contribution to a possible patella fracture or failure of the reconstructed MPFL after exertion of forces.
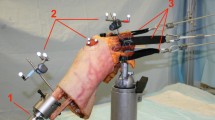
Two steel plates were used and bolted to build a support frame. This support frame and in particular the bottom plate, was fixed in the inferior hydraulic wedge grip. In the upper plate, we created an oval-shaped hole (long axis 2 cm and short axis 1 cm) and the inferior surface of the upper plate was covered by PTFE (Polytetrafluoroethylene). The graft-loop was placed through the oval hole and was attached to a hook which was clamped on the upper-hydraulic wedge grip of the testing machine. With application of an external tensile displacement, the clearance between the frame and the hook was increased and as result the patella was contracted to the lower surface of the upper plate. (Fig. 4).
Patella and reconstructed MPFL mounted on the custom device in the material testing machine. Red arrows demonstrating the forces exertion, which resulted in the removal of the hook from the cage and inevitably, the patella was contrasted to the lower surface of the upper plate. Blue arrow is pointing at the upper plate of the custom device where the patella was stabilized. The yellow arrow points at the hook, which was mounted on the upper-hydraulic wedge grip of the testing machine
Prior to application of tensile load, the MPFL reconstructions were subjected to cyclic loading for 10 cycles to 30 N to reduce the phenomenon of tissue hysteresis and then tested to failure at a constant displacement rate of 15 mm/min with a traction line parallel to the anchors, screws and the tunnel sutures using a materials-testing machine (MTS 810 Universal Testing System MTS). The ultimate tensile load was considered to be the peak force. Stiffness is defined as the slope of the linear region of the load displacement curve. A Savitzky-Golay method [33], was used to smooth existing noise, which was present in the experimental data, based on local least-squares polynomial approximation. The smoothed data corresponding to the linear region of the curve were isolated and a linear regression model was performed as mentioned by Russ et al. [30] using a subroutine in MATLAB software. Stiffness was determined by calculating the slope of the best fit line in the linear part of the force–displacement graph. Failure mode, ultimate failure load as well as stiffness were recorded for each cadaveric specimen.
Statistical analysis
Sample size requirement was calculated to be N = 8 for each group, which corresponds to 0.9 power [24]. SPSS software was used to statistically compare experimental results. The level of significance was set at p < 0.05.
Results
There was no statistically significant difference in mean ultimate failure load among the SA group, the SF group and the SK group (n.s). The SK group failed at a mean (± SD) ultimate load of 253.5 ± 38.2 N, the SA group failed at 243 ± 41.9 N and the SF group at 263.2 ± 9.6 N (Fig. 5).
The SF group had a mean stiffness of 37.850 ± 5.711 N/mm. Based on the performed post hoc tests, this was significantly higher than the mean stiffness value achieved for both the SK group 21.4 ± 9.5 N/mm (p < 0.05) and the SA group 18.7 ± 3.4 N/mm (p < 0.05) (Fig. 6).
Regarding the normality test, for the three groups, the values of significance level were higher than 0.05 for both maximum load and for stiffness. This is indicative of the fact that the obtained results do not approximate a normal distribution in any of the cases examined.
In the SF group, all the reconstructions failed due to tendon graft slippage from the tunnel until final pulling out of the grafts. The most common reason for failure in the SA group was anchor pullout, occurring in 7 out of 8 constructs. In one specimen in this group, failure occurred in the graft–suture connection. In the ‘no-implant’ group (SK), seven of the eight reconstructions failed in the graft–suture interface, while in the eighth, the bone bridge between the sutures collapsed. No patella fracture was recorded in all of the groups during the process.
Discussion
The primary finding of this cadaveric study, was that there were no statistically significant biomechanical differences between the SA, SF and SK reconstructions regarding ultimate load to failure. The secondary finding was that, fixation with interference screws provides significantly increased stiffness than the fixation of the graft with suture anchors and semi-patellar tunnels without hardware.
There are advantages and disadvantages to all patella fixation techniques. The use of screws and anchors in the patella fixation is less time-consuming and easier to use than hardware-free fixation techniques, but it has been accused of causing pain and irritation at the insertion side [34]. However, patellar fixation techniques without implants have the advantage of being less costly. Transverse bone tunnels that pass completely through the patella hold the risk of causing patellar fractures, as they act like stress risers [27,28,29, 34, 39]. A hardware-free technique was chosen for this biomechanical study, which has never been studied before. The advantageous features of this technique, are that it avoids breaching the anterior cortex of the patella, minimizes the bone tunnels and utilizes blind transverse tunnels (not trans-patellar tunnels) minimizing the tunnel size.
Based on the results of this biomechanical study, it is noteworthy that SK patella fixation technique is reliable and equal to the other two fixation techniques (SF, SA) regarding the ultimate load to failure and could offer extra solutions to surgeons. However, this remains to be proven clinically.
The most common mode of failure in the SA group was failure of anchors pullout. In the SF group, all the reconstructions failed due to tendon-graft slippage from the tunnel until the grafts final pulling out of the tunnel. In the SK group, the most common mode of failure was at the graft–suture connection.
In the literature, there have been a few biomechanical studies comparing different patellar fixation strategies in the MPFL reconstruction, but very few have been performed on human fresh-frozen knee specimens [14, 30,31,32]. Αll these studies, were carried out with the help of different approved-material testing systems, which the reconstructions were mounted on [10, 14, 19, 30,31,32]. Various ways of fixing the patella on these systems were used by researchers in the past. In the present study, Steinman-pins and clamps were excluded as a method of fixing the patella on these testing machines, since they would be added as stress risers and probably injure the reconstructions or possibly cause a patella fracture. The cement solution was rejected, since it would cover the fixation point (knot) of the SK patellar fixation technique, and therefore it could alter the biomechanical properties of the construct. Therefore, we relied on the construction of an improvised patella fixation device, which would not have the above limitations.
Gracilis was selected over semitendinosus tendon as a graft for MPFL reconstructions. Biomechanically, a single-strand gracilis construct has a maximum strength of 925 ± 127 N while the tensile strength of the native MPFL is 208 N [3, 13, 21]. In addition, gracilis has a smaller diameter, which implies the creation of smaller tunnels. Different biomechanical studies measured the mechanical properties of the native MPFL and ultimate load to failure ranged from 72 to 208 N [13, 21]. The variability of the load to failure values is partially explained by different experimental conditions under which the ligaments were tested. At this point, it is important to note that all three types of reconstructions evaluated in our study outperformed the maximum recorded value of native MPFL tensile load to failure, as reported by other studies [13, 17]. This may indicate that all three reconstruction techniques are sufficient to recreate the final load to failure of the native MPFL and thus, they could be employed for MPFL reconstruction.
Screw stabilization was found to be significantly more efficient than the other two fixations techniques in terms of rigidity of the reconstruction. In the present study, stiffness was determined using the least squares polynomial approximation to fit the force displacement data. Few studies have examined the stiffness of the native MPFL and even fewer explained how stiffness was calculated [4, 5, 13, 17]. Criscenti et al. [5] measured the stiffness based on the slope of the linear region in the force displacement graph. The stiffness was reported to be 42.5 ± 10.2 N/mm. However, there is no explanation about the exact method of analysis they used to get the most linear part of the curve and calculate the slope. On the other hand, LaPrade et al. [17] measured a mean stiffness of 23 ± 6 N/mm using a linear regression model to fit the forced displacement data of the uniaxial tensile test. Conlan et al. [4] reported that stiffness of the entire medial soft tissue of the knee restraints to lateral patellar displacement decreased from 22.5 N/mm to 10.5 N/mm after cutting of the MPFL. The values of the stiffness of screw fixation technique of this study far exceeded the values of the stiffness of the native MPFL according to LaPrade et al. [17] while the values of the stiffness of the other two fixation techniques fluctuated at the same levels.
Similar to the present study, Russ et al. [30] evaluated two commonly used patellar fixation techniques in MPFL reconstruction, suture anchor fixation on fresh-frozen knee cadavers versus interference screw fixation. In that study, fresh-frozen knee cadavers were utilized and semintendinosus was harvested as an autologous graft. The authors concluded that interference screw fixation was found to be significantly stronger than suture anchor fixation when comparing the ultimate failure load and stiffness. Saper et al. [32] performed a biomechanical study comparing patella fixation with classic solid suture anchors versus all-soft suture anchors fixation. This experimental human cadaver study displayed no statistically significant difference in biomechanical performance between these two fixation techniques. However, in the aforementioned study, the method mounting the reconstruction in the testing machine is presented in a schematic of the test setup without clarifying the method of fixing the patella to the material testing system.
Lenschow et al. [19] investigated the structural properties of 5 different fixation strategies for a free tendon graft at the patella MPFL reconstruction. Their hardware-free technique is similar to our hardware-free fixation technique, while the main difference is that the loop of the graft is fixed in the patella and not in the free ends of the graft. Τhe models of this experimental study, were porcine patella and flexor tendons, which do not probably reflect MPFL reconstruction conditions in humans. The investigators in this study, mounted the specimens to the base of the testing frame of the material testing machine using a 5-mm Steinmann pin that was drilled through the patella increasing stress-riser at the bone bridge without being able to be sure that it crossed the bone tunnels or the sutures. Nevertheless, the implant free technique had equivocal failure load when compared with interference screws and suture anchors but had significantly lower stiffness. They did not find any difference between suture anchors and interference screws in terms of ultimate failure load or stiffness.
Hapa et al. [10] tested four commonly used techniques for patellar fixation in MPFL reconstruction in a Sawbone model using bovine tendons. Results of the docking technique in Hapa et al.’s study cannot be compared with the hardware-free technique in the present study because it was a non-anatomic patella fixation technique drilling only one blind tunnel and using a different suture.
Limitations of this study, like any other cadaveric biomechanical study, may be attributed to the fact that specimens were tested at time zero, without taking into account any time of healing at the bone–graft interface. Consequently, our conclusions represent biomechanical properties for constructs in the immediate postoperative period and cannot be used to determine optimal reconstruction in the long term. Moreover, the age of the specimen donors is another limitation, so data may contain an age-related bias. In the anchors group, the free ends of the graft were sutured together; however, it should be noted that no reconstruction of the MPFL in the anchor group has failed at this point. Furthermore, the present study lacked a control group. This study is also limited by the potential baseline values mismatch of ultimate load to failure of the native MPFL with the specific testing device used, compared to previous studies. A final limitation is the linear testing in which the constructs were applied. In this way, a worst-case scenario was tested with the tensile load in line with the suture anchors, screws, tunnels and sutures, which might not correspond to in vivo conditions. However, the conditions created to carry out this experiment, were very close to realistic conditions, since human cadaveric specimens were used and cement, claws, pins or Steinmann were not utilized for the patella stabilization.
Conclusion
Load to failure was not significantly different between the three patella fixation techniques. However, interference screw stabilization was found to be significantly stronger than the suture-anchor and suture-knot fixation, in terms of rigidity of the reconstruction.
References
Baldwin JL (2009) The anatomy of the medial patellofemoral ligament. Am J Sports Med 37(12):2355–2361
Bicos J, Fulkerson JP, Amis A (2007) Current concepts review: the medial patellofemoral ligament. Am J Sports Med 35(3):484–492
Cavaignac E, Pailhé R, Reina N, Murgier J, Laffosse JM, Chiron P et al (2016) Can the gracilis replace the anterior cruciate ligament in the knee? A biomechanical study. Int Orthop 40:1647–1653
Conlan T, Garth WP Jr, Lemons JE (1993) Evaluation of the medial soft tissue restraints of the extensor mechanism of the knee. J Bone Joint Surg Am 75(5):682–693
Criscenti G, De Maria C, Sebastiani E, Tei M, Placella G, Speziali A et al (2016) Material and structural tensile properties of the human medial patello-femoral ligament. J Mech Behav Biomed Mater 54:141–148
Deie M, Ochi M, Sumen Y, Adachi N, Kobayashi K, Yasumoto M (2005) A long-term follow-up study after medial patellofemoral ligament reconstruction using the transferred semitendinosus tendon for patellar dislocation. Knee Surg Sports Traumatol Arthrosc 13(7):522–528
Desio SM, Burks RT, Bachus KN (1998) Soft tissue restraints to lateral patellar translation in the human knee. Am J Sports Med 26(1):59–65
Duerr RA, Chauhan A, Frank DA, DeMeo PJ, Akhavan S (2016) An algorithm for diagnosing and treating primary and recurrent patellar instability. JBJS Rev 4(9):01874474–201609000–00003.
Erickson BJ, Nguyen J, Gasik K, Gruber S, Brady J, Shubin Stein BE (2019) Isolated medial patellofemoral ligament reconstruction for patellar instability regardless of tibial tubercle-trochlear groove distance and patellar height: outcomes at 1 and 2 years. Am J Sports Med 47(6):1331–1337
Hapa O, Akşahin E, Özden R, Pepe M, Yanat AN, Doğramacı Y et al (2012) Aperture fixation instead of transverse tunnels at the patella for medial patellofemoral ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 20(2):322–326
Hiemstra LA, Kerslake SA, Lafave MR (2019) Influence of risky pathoanatomy and demographic factors on clinical outcomes after isolated medial patellofemoral ligament reconstruction: a regression analysis. Am J Sports Med 47(12):2904–2909
Hinterwimmer S, Imhoff AB, Minzlaff P, Saier T, Rosenstiel N, Hawe W et al (2013) Anatomical two-bundle medial patellofemoral ligament reconstruction with hardware-free patellar graft fixation: technical note and preliminary results. Knee Surg Sports Traumatol Arthrosc 21(9):2147–2154
Huber C, Zhang Q, Taylor WR, Amis AA, Smith C, Hosseini Nasab SH (2020) Properties and function of the medial patellofemoral ligament: a systematic review. Am J Sports Med 48(3):754–766
Joyner PW, Bruce J, Roth TS, Mills FB 4th, Winnier S, Hess R et al (2017) Biomechanical tensile strength analysis for medial patellofemoral ligament reconstruction. Knee 24(5):965–976
Kruckeberg BM, Chahla J, Moatshe G, Cinque ME, Muckenhirn KJ, Godin JA et al (2018) Quantitative and qualitative analysis of the medial patellar ligaments: an anatomic and radiographic study. Am J Sports Med 46(1):153–162
Kyung H-S, Kim H-J (2015) Medial patellofemoral ligament reconstruction: a comprehensive review. Knee Surg Relat Res 27(3):133–140
LaPrade MD, Kallenbach SL, Aman ZS, Moatshe G, Storaci HW, Turnbull TL et al (2018) Biomechanical evaluation of the medial stabilizers of the patella. Am J Sports Med 46(7):1575–1582
LaPrade RF, Engebretsen AH, Ly TV, Johansen S, Wentorf FA, Engebretsen L (2007) The anatomy of the medial part of the knee. J Bone Joint Surg Am 89(9):2000–2010
Lenschow S, Schliemann B, Gestring J, Herbort M, Schulze M, Kosters C (2013) Medial patellofemoral ligament reconstruction: fixation strength of 5 different techniques for graft fixation at the patella. Arthroscopy 29(4):766–773
Mehta V, Mandala C, Akhter A (2017) Cyclic testing of 3 medial patellofemoral ligament reconstruction techniques. Orthop J Sports Med https://doi.org/10.1177/2325967117712685
Mountney J, Senavongse W, Amis AA, Thomas NP (2005) Tensile strength of the medial patellofemoral ligament before and after repair or reconstruction. J Bone Joint Surg Br 87(1):36–40
Mulliez A, Lambrecht D, Verbruggen D, Van Der Straeten C, Verdonk P, Victor J (2017) Clinical outcome in MPFL reconstruction with and without tuberositas transposition. Knee Surg Sports Traumatol Arthrosc 25:2708–2714
Nomura E, Horiuchi Y, Kihara M (2000) Medial patellofemoral ligament restraint in lateral patellar translation and reconstruction. Knee 7(2):121–127
Olson SA, Marsh JL, Anderson DD, Latta Pe LL (2012) Designing a biomechanics investigation: choosing the right model. J Orthop Trauma 26(12):672–677
Panagopoulos A, van Niekerk L, Triantafillopoulos IK (2008) MPFL reconstruction for recurrent patellar dislocation: a new surgical technique and review of the literature. Int J Sports Med 29(5):359–365
Panni AS, Alam M, Cerciello S, Vasso M, Maffulli N (2011) Medial patellofemoral ligament reconstruction with a divergent patellar transverse 2- tunnel technique. Am J Sports Med 39(12):2647–2655
Parikh SN, Nathan ST, Wall EJ, Eismann EA (2013) Complications of medial patellofemoral ligament reconstruction in young patients. Am J Sports Med 41(5):1030–1038
Parikh SN, Wall EJ (2011) Patellar fracture after medial patellofemoral ligament surgery: a report of five cases. J Bone Joint Surg Am 93(17): e 97(1–8).
Parikh SN, Lykissas MG, Gkiatas I (2018) Predicting risk of recurrent patellar dislocation. Curr Rev Musculoskelet Med 11(2):253–260
Russ SD, Tompkins M, Nuckley D, Macalena J (2015) Biomechanical comparison of patellar fixation techniques in medial patellofemoral ligament reconstruction. Am J Sports Med 43(1):195–199
Russo F, Doan J, Chase DC, Farnsworth CL, Pennock AT (2016) Medial patellofemoral ligament reconstruction: fixation technique biomechanics. J Knee Surg 29(4):303–309
Saper MG, Meijer K, Winnier S, Popovich JJR, Andrews JR, Roth C (2017) Biomechanical evaluation of classic solid and all-soft suture anchors for medial patellofemoral ligament reconstruction. Am J Sports Med 45:1622–1626
Savitzky A, Golay MJE (1964) Smoothing and differentiation of data by simplified least squares procedures. Anal Chem 36(8):1627–1639
Shah JN, Howard JS, Flanigan DC, Brophy RH, Carey JL, Lattermann C (2012) A systematic review of complications and failures associated with medial patellofemoral ligament reconstruction for recurrent patellar dislocation. Am J Sports Med 40(8):1916–1923
Siebold R, Borbon CAV (2012) Arthroscopic extraarticular reconstruction of the medial patellofemoral ligament with gracilis tendon autograft - surgical technique. Knee Surg Sports Traumatol Arthrosc 20:1245–1251
Schöttle PB, Hensler D, Imhoff AB (2010) Anatomical double-bundle MPFL reconstruction with an aperture fixation. Knee Surg Sports Traumatol Arthrosc 18(2):147–151
Schöttle PB, Schmeling A, Romero J, Weiler A (2009) Anatomical reconstruction of the medial patellofemoral ligament using a free gracilis autograft. Arch Orthop Trauma Surg 129(3):305–309
Schöttle PB, Fucentese SF, Romero J (2005) Clinical and radiological outcome of medial patellofemoral ligament reconstruction with a semitendinosus autograft for patella instability. Knee Surg Sports Traumatol Arthrosc 13(7):516–521
Tompkins M, Arendt EA (2012) Complications in patellofemoral surgery. Sports Med Arthrosc 20:187–193
Wang C-H, Ma L-F, Zhou J-W, Ji G, Wang HY, Wang F et al (2013) Double-bundle anatomical versus single-bundle isometric medial patellofemoral ligament reconstruction for patellar dislocation. Int Orthop 37(4):617–624
Wang Q, Huang W, Cai D, Huang H (2017) Biomechanical comparison of single- and double-bundle medial patellofemoral ligament reconstruction. J Orthop Surg Res 12(1):29
Warren LF, Marshall JL (1979) The supporting structures and layers on the medial side of the knee. J Bone Joint Surg Am 61:56–62
Acknowledgements
The authors would like to acknowledge H. Kapsouris, Mathematician, for his help regarding graphic design, and Stryker Company for donating anchors and bio-composite screws.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This study and all authors have received no funding.
Conflict of interest
Author Vasilios A. Raoulis, Author Aristidis Zibis, Author Maria Dimitra Chiotelli, Author Alexis T. Kermanidis, Author Konstantinos Banios, Author Philipp Schuster and Author Michael Hantes, declare that they have no conflict of interest.
Ethical approval
This study was approved by IRB (Institutional Review Board) of the Medical School of University of Thessaly as part of the PhD thesis of one of the authors (ID number 2754).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Raoulis, V.A., Zibis, A., Chiotelli, M.D. et al. Biomechanical evaluation of three patellar fixation techniques for MPFL reconstruction: Load to failure did not differ but interference screw stabilization was stiffer than suture anchor and suture-knot fixation. Knee Surg Sports Traumatol Arthrosc 29, 3697–3705 (2021). https://doi.org/10.1007/s00167-020-06389-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-020-06389-4