Abstract
Purpose
The accuracy of patient-specific instrumentation (PSI) in total knee arthroplasty (TKA) is still controversial, especially in the tibial prosthesis. It was hypothesized that the design modification of PSI improved the tibial prosthetic alignment and reduced the associated complications. The aim of this study was to compare the accuracy of a conventional PSI with that of a newly designed PSI for total knee arthroplasty (TKA) using a new three-dimensional (3D) measurement method.
Methods
Thirty TKAs each using the conventional and newly designed PSIs were studied. The postoperative 3D-computed tomography (3D CT) image was superimposed on the preoperative 3D CT plan. The absolute differences in the tibial prosthetic alignment between the preoperative and postoperative 3D CT images were directly measured in the coronal, sagittal, and axial planes. Knees in which the difference in the prosthetic alignment was > 3° were considered deviations.
Results
The new PSI showed less mean absolute differences and lower rate of deviations than the conventional PSI in the coronal and axial planes (p = 0.045 and p = 0.004, respectively). The deviations (> 3°) of the tibial prosthesis using the conventional PSI were 27, 30, and 63% and of those using the new PSI were 0, 20, and 20% in the coronal, sagittal, and axial planes, respectively.
Conclusions
This is the first report to evaluate the effect of improvement in PSI design on the postoperative alignment using 3D method, and it clearly showed that the modification significantly improved the accuracy of alignment and reduced the deviations.
Level of evidence
Therapeutic study, case–control study, Level III.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Prosthetic alignment is one of the most important factors affecting the long-term clinical results associated with total knee arthroplasty (TKA) [7, 19, 20]. To improve prosthetic alignment and decrease cases of prosthetic deviations, patient-specific instrumentation (PSI) has recently been introduced for TKA [10, 12]. PSI, based on the data from either magnetic resonance imaging (MRI) or computed tomography (CT), is designed to correctly reproduce the preoperative three-dimensional (3D) plan during an operation. The accuracy of the PSI is still controversial [30]. Some previous reports showed that PSIs were accurate [16, 29], but other reports showed that PSIs were not accurate [1, 2, 23] because of two reasons. First, there have been many designs of PSIs. Each PSI design varies; thus, the accuracy of each PSI is not always the same. Second, the evaluation method for the prosthetic alignment was not appropriate. To evaluate the accuracy of PSI, the preoperative 3D CT plan should be superimposed on the postoperative 3D CT image, and the prosthetic alignment between the preoperative 3D CT plan and postoperative 3D CT image should be directly compared.
Excellent intraobserver and interobserver reliabilities were shown in the new evaluation method for the accuracy of PSI, which superimposed the preoperative 3D CT plan on the postoperative 3D CT image and directly compared the prosthetic alignment between the preoperative 3D CT plan and postoperative 3D CT image [33]. In a previous report, even with a CT-based PSI, the alignment of the tibial prosthesis is less accurate in the axial plane than in the coronal and sagittal planes [33]. To improve the accuracy of the prosthetic alignment, several designs of the CT-based PSI have been improved (Fig. 1) as follows: (1) enlargement of the contact area between the bone and PSI (Fig. 2); (2) rotational marker to be lined up to the bony landmark on the tibial plateau (Fig. 3); (3) extension of the hole length for the extramedullary rod to aid attachment of the ankle cramp (Fig. 4); and (4) the hole of the anteroposterior (AP) marker pin was added in the tibial cutting jig (Fig. 5).
Rotational marker has been added on the newly designed PSI (a). This line was lined up to the anteroposterior (AP) axis of the tibia (red dotted line). The AP axis is drawn on the tibial plateau according the preoperative plan (b). The rotational marker of the newly designed PSI and the AP axis of the tibia are lined up to reproduce the preoperative plan of the axial alignment (c, d)
It was hypothesized that the improvement of the design of PSI enhanced the tibial prosthetic alignment, especially in the axial plane. The aim of this study was to compare the accuracy of a conventional PSI and a newly designed PSI using a new 3D measurement method. However, to the best our knowledge, no report has evaluated the effect of improvement in PSI design on the postoperative alignment using a 3D measurement method.
Materials and methods
Sixty consecutive knees that underwent TKA due to varus osteoarthritis of the knee using PSI were studied. Conventional PSI was used in the first 30 knees, and the newly designed PSI was used in the remaining 30 knees (Fig. 1).
Patient-specific instrumentation was designed based on the preoperative plan (Prophecy; MicroPort Orthopedics, Inc., Arlington, TN, USA) developed using the data from the 3D CT of the whole leg. The preoperative plan was the same for the two groups, but there were several design improvements in the newly designed PSI. First, the contact area between the bone and PSI was enlarged (Fig. 2). Larger contact area ensured a tight fit between the newly designed PSI and the tibial bone. Second, a rotational marker, which lined up to the bony landmark on the tibial plateau during the operation, was added in the newly designed PSI (Fig. 3). This modification was expected to improve the axial alignment. Third, the length of the hole for the extramedullary rod was extended to aid attachment of the ankle cramp (Fig. 4), which helped the surgeons to check for the coronal and sagittal alignments before cutting the bone. This change was expected to reduce sagittal and coronal alignment errors. Fourth, the hole of the anteroposterior (AP) marker pin was added in the tibial cutting jig. The tibial component was placed parallel to this AP marker pin (Fig. 5). This procedure was expected to reduce the axial alignment error.
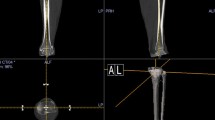
A postoperative 3D CT image taken 2 weeks postoperatively was superimposed on the preoperative 3D plan using a computer software (ZedView, ZedKnee; LEXI Co., Ltd., Tokyo, Japan) (Fig. 6). The preoperative 3D plan was provided by the company (MicroPort Orthopedics, Inc.). Prosthetic computer-aided design data were installed and combined on postoperative CT image using ZedKnee. These preoperative and postoperative images were installed in ZedKnee. This computer software indicated the coronal, sagittal, axial, and 3D views at the same time. The postoperative CT image was carefully moved to completely overlap the tibial bone image of the postoperative CT image and that of the preoperative 3D CT plan. First, in the coronal view, the tibial condyle and malleolus were superimposed. Second, in the sagittal view, the tibial tuberculum was superimposed. Third, in the axial view, the tibial condyle and malleolus were superimposed. Finally, in the 3D view, the superimposition of the tibial bone image was checked. Then, the absolute difference in the tibial prosthetic alignment between the preoperative 3D plan and postoperative 3D CT image in the coronal, sagittal, and axial planes was directly measured in degrees up to one decimal place using the software. Cases demonstrating a difference > 3° in the prosthetic alignment were considered deviations [13]. The intraclass correlation coefficients of the 3D measurement method of the intra-rater reliabilities were 0.90, 0.95, and 0.98 in the coronal, sagittal, and axial planes, respectively. Whereas those of the inter-rater reliabilities were 0.95, 0.97, and 0.95 in the coronal, sagittal, and axial planes, respectively. The mean absolute differences between two measurements by one observer were 0.8 ± 0.5° in the coronal plane, 0.6 ± 0.5° in the sagittal plane, and 0.8 ± 0.6° in the axial plane. The mean absolute differences between two observers were 0.5 ± 0.5° in the coronal plane, 0.8 ± 0.7° in the sagittal plane, and 0.9 ± 1.1° in the axial plane. The same total knee prosthesis (Evolution PS; MicroPort Orthopedics, Inc. Arlington, TN, USA) was used in all cases. All operations were performed by one surgical team. The knees were exposed using a medial parapatellar approach, and the anterior and posterior cruciate ligaments were resected.

(reprinted by permission from [33])
Tibia of the postoperative 3D CT image is superimposed onto the tibia of the preoperative 3D CT plan. Differences in the prosthetic alignment between the preoperative 3D CT plan (red) and postoperative 3D CT image (blue) are measured
Statistical analysis
The Mann–Whitney U test after an F test to determine variance equality was used to compare the absolute difference in the prosthetic alignment between the preoperative 3D CT plan and postoperative 3D CT image in the coronal, sagittal, and axial planes. The Pearson Chi-square and Fisher exact tests were used to determine the deviations. A sample size calculation was performed using G*Power 3.1.9.2 [8], and the results showed that a sample of 21 knees in each group was required to achieve a power of 0.8 to detect a significant difference (α = 0.05, two-sided significance level). All data analyses were performed using SPSS version 24.0 (SPSS Inc., Chicago, IL, USA). The level of significance (p value) was set at 0.05.
Results
The differences in age during the operation, sex, BMI, and preoperative hip–knee–ankle angle were not significantly different between the two groups (Table 1). The absolute differences in the tibial prosthetic alignment (coronal, sagittal, and axial planes) between the preoperative 3D plan and postoperative 3D CT data are shown in Table 2. When comparing the conventional PSI and the new PSI, the mean absolute differences were significantly less in the coronal and axial planes when using the new PSI (p = 0.045 and p = 0.004). The deviations (> 3°) of the tibial prosthesis using conventional PSI were 27, 30, and 63% and using the new PSI were 0, 20, and 20% in the coronal, sagittal, and axial planes, respectively (Fig. 7; Table 3). The same prosthetic size as the preoperative plan was implanted in 46 knees (77%). One larger size was used in three knees (5%). One smaller size was used in 11 knees (18%). No knees have used two or more different sizes.
Discussion
The most important finding of this study was that the improvement of the PSI design enhanced its accuracy. Larger contact area, rotational marker on PSI, connection to the extramedullary guide, and AP marker pin proved significantly effective for the improvement of coronal and axial alignments of the tibial component.
Some previous reports showed that PSIs were accurate [16, 29], but other reports showed that PSIs were not accurate [2, 23]. The accuracy of PSIs varies because of the difference in the designs of previous PSIs. Therefore, the usage of PSI is still controversial. A meta-analysis showed that the deviations (> 3°) of the tibial prosthesis using other PSIs were 10.5% in the coronal plane and 29.9% in the sagittal plane [30]. In the axial plane, a previous report showed more than 5° of tibial malrotation in 95% cases using a PSI [28]. Although the deviations of the conventional PSI in the present study were comparable to those of the previous reposts, the deviations of our newly designed PSI were much less than those of the previous reports. This study clearly showed that the minor changes in PSI design (enlargement of the contact area between the bone and PSI, rotational marker, extension of the hole length for the extramedullary rod, and the hole of the AP marker pin) significantly changed the accuracy of PSI. This study suggested that differences in PSI design might result in the inconsistency of the accuracy of PSI in the previous reports. Thus, design improvement is mandatory to improve the accuracy of PSI.
An advantage of this study was that the preoperative 3D CT plan was superimposed on a postoperative 3D CT image, and the prosthetic alignment between the preoperative and postoperative images was directly compared. Most previous reports evaluated the accuracy of PSI using postoperative radiographs [4,5,6] or two-dimensional (2D) CT [18, 21]. However, measuring the prosthetic alignment using radiographs or 2D CT had several limitations [17, 27] and was less accurate than a 3D measurement using CT [11]. To eliminate measurement errors, the postoperative 3D CT image was superimposed on the preoperative 3D CT plan and directly compared. Therefore, our measurement method was suitable for this study, and the method also showed excellent interobserver and intraobserver reliabilities.
In the coronal and sagittal planes, the accuracy of the newly designed PSI was better than that of the conventional technique [9] and was comparable with that of the CT-free navigation system [14] and CT-based navigation system [24]. In the axial plane, a previous report showed more than 3° of tibial malrotation in 67% of cases using conventional technique [15], in 54% of cases using CT-free navigation system [14], and in 49% of cases using CT-based navigation system [15]. The axial alignment of the tibial component was less accurate than that of the coronal and sagittal alignments even with the navigation system. However, this study showed that > 3° of tibial malrotation occurred only in 20% of cases using the newly designed PSI. Rotational malalignment of the tibial component can lead to altered joint kinematics and painful TKA. Excessive malrotation of the tibial component can result in various complications after TKA such as painful knee [25, 26], stiff knee [31], patellofemoral instability [22], or excessive wear of the polyethylene insert [32]. The newly designed PSI is expected to reduce the malrotation of the tibial component and the associated complications.
This study had some limitations. First, the subjects comprised only patients who had primary varus osteoarthritis of the knee. Therefore, the results of this study might not always be applicable to other diseases and deformities. Second, the clinical outcomes were not evaluated in this study. The previous reports showed that the higher accuracy achieved by PSI did not always translate into better clinical outcomes [3]. Further study should be performed to compare the clinical outcomes between two groups.
The clinical relevance of the present study is that the design improvement of PSI enhanced the accuracy of the PSI in the coronal and axial planes. This study suggested that the design improvement is mandatory to improve the accuracy of PSI.
Conclusions
This is the first report to evaluate the effect of a PSI design improvement on postoperative alignment using a 3D measurement method, which superimposed the preoperative 3D CT plan on a postoperative 3D CT image, and then directly compared the prosthetic alignment between the preoperative 3D CT plan and postoperative 3D CT image. This study clearly showed that the design improvement of PSI enhanced the accuracy of PSI in coronal and axial planes.
References
Abdel MP, Parratte S, Blanc G, Ollivier M, Pomero V, Viehweger E et al (2014) No benefit of patient-specific instrumentation in TKA on functional and gait outcomes: a randomized clinical trial. Clin Orthop Relat Res 472:2468–2476
Abdel MP, von Roth P, Hommel H, Perka C, Pfitzner T (2015) Intraoperative navigation of patient-specific instrumentation does not predict final implant position. J Arthroplasty 30:564–566
Anderl W, Pauzenberger L, Kolblinger R, Kiesselbach G, Brandl G, Laky B et al (2016) Patient-specific instrumentation improved mechanical alignment, while early clinical outcome was comparable to conventional instrumentation in TKA. Knee Surg Sports Traumatol Arthrosc 24:102–111
Boonen B, Schotanus MG, Kerens B, van der Weegen W, van Drumpt RA, Kort NP (2013) Intra-operative results and radiological outcome of conventional and patient-specific surgery in total knee arthroplasty: a multicentre, randomised controlled trial. Knee Surg Sports Traumatol Arthrosc 21:2206–2212
Boonen B, Schotanus MG, Kort NP (2012) Preliminary experience with the patient-specific templating total knee arthroplasty. Acta Orthop 83:387–393
Chen JY, Yeo SJ, Yew AK, Tay DK, Chia SL, Lo NN et al (2014) The radiological outcomes of patient-specific instrumentation versus conventional total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 22:630–635
Fang DM, Ritter MA, Davis KE (2009) Coronal alignment in total knee arthroplasty: just how important is it? J Arthroplasty 24:39–43
Faul F, Erdfelder E, Lang AG, Buchner A (2007) G*Power 3: a flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav Res Methods 39:175–191
Fu Y, Wang M, Liu Y, Fu Q (2012) Alignment outcomes in navigated total knee arthroplasty: a meta-analysis. Knee Surg Sports Traumatol Arthrosc 20:1075–1082
Hafez MA, Chelule KL, Seedhom BB, Sherman KP (2006) Computer-assisted total knee arthroplasty using patient-specific templating. Clin Orthop Relat Res 444:184–192
Hirschmann MT, Konala P, Amsler F, Iranpour F, Friederich NF, Cobb JP (2011) The position and orientation of total knee replacement components: a comparison of conventional radiographs, transverse 2D-CT slices and 3D-CT reconstruction. J Bone Jt Surg Br 93:629–633
Howell SM, Kuznik K, Hull ML, Siston RA (2008) Results of an initial experience with custom-fit positioning total knee arthroplasty in a series of 48 patients. Orthopedics 31:857–863
Jiang J, Kang X, Lin Q, Teng Y, An L, Ma J et al (2015) Accuracy of patient-specific instrumentation compared with conventional instrumentation in total knee arthroplasty. Orthopedics 38:e305–e313
Kim YH, Kim JS, Yoon SH (2007) Alignment and orientation of the components in total knee replacement with and without navigation support: a prospective, randomised study. J Bone Jt Surg Br 89:471–476
Kuriyama S, Hyakuna K, Inoue S, Tamaki Y, Ito H, Matsuda S (2014) Tibial rotational alignment was significantly improved by use of a CT-navigated control device in total knee arthroplasty. J Arthroplasty 29:2352–2356
Kwon OR, Kang KT, Son J, Suh DS, Heo DB, Koh YG (2017) Patient-specific instrumentation development in TKA: 1st and 2nd generation designs in comparison with conventional instrumentation. Arch Orthop Trauma Surg 137:111–118
Lee YS, Lee BK, Lee SH, Park HG, Jun DS, do Moon H (2013) Effect of foot rotation on the mechanical axis and correlation between knee and whole leg radiographs. Knee Surg Sports Traumatol Arthrosc 21:2542–2547
Leeuwen JA, Grogaard B, Nordsletten L, Rohrl SM (2015) Comparison of planned and achieved implant position in total knee arthroplasty with patient-specific positioning guides. Acta Orthop 86:201–207
Liu HX, Shang P, Ying XZ, Zhang Y (2016) Shorter survival rate in varus-aligned knees after total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 24:2663–2671
Lombardi AV Jr, Berend KR, Ng VY (2011) Neutral mechanical alignment: a requirement for successful TKA: affirms. Orthopedics 34:e504–e506
Marimuthu K, Chen DB, Harris IA, Wheatley E, Bryant CJ, MacDessi SJ (2014) A multi-planar CT-based comparative analysis of patient-specific cutting guides with conventional instrumentation in total knee arthroplasty. J Arthroplasty 29:1138–1142
Matsuda S, Miura H, Nagamine R, Urabe K, Hirata G, Iwamoto Y (2001) Effect of femoral and tibial component position on patellar tracking following total knee arthroplasty: 10-year follow-up of Miller-Galante I knees. Am J Knee Surg 14:152–156
Maus U, Marques CJ, Scheunemann D, Lampe F, Lazovic D, Hommel H et al (2018) No improvement in reducing outliers in coronal axis alignment with patient-specific instrumentation. Knee Surg Sports Traumatol Arthrosc 26:2788–2796
Mizu-Uchi H, Matsuda S, Miura H, Higaki H, Okazaki K, Iwamoto Y (2009) Three-dimensional analysis of computed tomography-based navigation system for total knee arthroplasty: the accuracy of computed tomography-based navigation system. J Arthroplasty 24:1103–1110
Murakami AM, Hash TW, Hepinstall MS, Lyman S, Nestor BJ, Potter HG (2012) MRI evaluation of rotational alignment and synovitis in patients with pain after total knee replacement. J Bone Jt Surg Br 94:1209–1215
Nicoll D, Rowley DI (2010) Internal rotational error of the tibial component is a major cause of pain after total knee replacement. J Bone Jt Surg Br 92:1238–1244
Okamoto S, Mizu-Uchi H, Okazaki K, Hamai S, Tashiro Y, Nakahara H et al (2016) Two-dimensional planning can result in internal rotation of the femoral component in total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 24:229–235
Parratte S, Blanc G, Boussemart T, Ollivier M, Le Corroller T, Argenson JN (2013) Rotation in total knee arthroplasty: no difference between patient-specific and conventional instrumentation. Knee Surg Sports Traumatol Arthrosc 21:2213–2219
Silva A, Sampaio R, Pinto E (2014) Patient-specific instrumentation improves tibial component rotation in TKA. Knee Surg Sports Traumatol Arthrosc 22:636–642
Thienpont E, Schwab PE, Fennema P (2017) Efficacy of patient-specific instruments in total knee arthroplasty: a systematic review and meta-analysis. J Bone Jt Surg Am 99:521–530
Vince KG (2012) The stiff total knee arthroplasty: causes and cures. J Bone Jt Surg Br 94:103–111
Wasielewski RC, Galante JO, Leighty RM, Natarajan RN, Rosenberg AG (1994) Wear patterns on retrieved polyethylene tibial inserts and their relationship to technical considerations during total knee arthroplasty. Clin Orthop Relat Res 299:31–43
Yamamura K, Minoda Y, Mizokawa S, Ohta Y, Sugama R, Nakamura S et al (2017) Novel alignment measurement technique for total knee arthroplasty using patient specific instrumentation. Arch Orthop Trauma Surg 137:401–407
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Author YM has received research Grants and speaker honorarium from MicroPort.
Ethical approval
This study was approved by the institutional review board of Osaka City University Graduate School of Medicine and Faculty of Medicine (ID number 1992).
Informed consent
All patients provided informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yamamura, K., Minoda, Y., Sugama, R. et al. Design improvement in patient-specific instrumentation for total knee arthroplasty improved the accuracy of the tibial prosthetic alignment in the coronal and axial planes. Knee Surg Sports Traumatol Arthrosc 28, 1560–1567 (2020). https://doi.org/10.1007/s00167-019-05571-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-019-05571-7