Abstract
Purpose
To examine the association of fear avoidance and self-efficacy psychological factors within 4 weeks after anterior cruciate ligament (ACL) reconstruction with knee impairment resolution and readiness for advanced rehabilitation at 12 weeks post-surgery.
Methods
Seventy-five patients participated. Data collection included demographics; questionnaires on fear avoidance (Pain Catastrophizing Scale, PCS; shortened Tampa Scale for Kinesiophobia, TSK-11) and self-efficacy (modified Self-Efficacy for Rehabilitation Outcome Scale, SER; Knee Activity Self-Efficacy, KASE) at 1, 4, and 12 weeks post-surgery; and knee impairment measures (pain intensity, range of motion, and quadriceps symmetry index) at 12 weeks post-surgery. Readiness for advanced rehabilitation (READY or NOT READY) was determined by knee impairment resolution criteria; demographics and questionnaire scores were compared between groups. Questionnaire scores at 1 and 4 weeks post-surgery and the change between time points were examined for association with knee impairment measures and group assignment.
Results
READY included 32 patients; NOT READY included 43 patients. Questionnaire scores improved in both groups over time. Significant correlations across groups were: PCS scores at 1 and 4 weeks post-surgery with pain intensity at 12 weeks post-surgery (r = 0.24 and 0.29, respectively) and KASE score 4 weeks post-surgery with range of motion deficit at 12 weeks post-surgery (r = − 0.26). Contact injury was more prevalent in READY. After accounting for mechanism of injury, higher TSK-11 and fear of re-injury subscale scores at 4 weeks post-surgery increased the odds of NOT READY assignment at 12 weeks post-surgery (odds ratios 1.10 and 1.31, respectively).
Conclusions
Lower pain catastrophizing and higher knee activity self-efficacy levels 4 weeks after ACL reconstruction were associated with better knee impairment resolution at 12 weeks post-surgery, whereas lower kinesiophobia at 4 weeks post-surgery increased the odds of meeting advanced rehabilitation criteria at 12 weeks post-surgery. The clinical implication of these findings is that measuring pain catastrophizing, knee activity self-efficacy and kinesiophobia at 4 weeks post-surgery may improve prediction of patients at risk for delayed rehabilitation progression 12 weeks post-surgery.
Level of evidence
III.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Psychological factors have an important influence on rehabilitation outcomes following anterior cruciate ligament (ACL) reconstruction [2, 3, 14, 16]. For example, elevated fear of re-injury and kinesiophobia or decreased self-efficacy deter the return to sports participation after ACL reconstruction [7, 14, 23, 24, 28]. The psychological response to sports injury tends to be most negative immediately after injury and improve during rehabilitation [12, 13, 38]. Potentially, psychological factors early in ACL reconstruction rehabilitation could affect early rehabilitation outcomes.
Kinesiophobia, or fear of movement/re-injury, and pain catastrophizing are psychological constructs in the fear-avoidance model [25]. Kinesiophobia and pain catastrophizing become elevated when pain is perceived as a threat, in turn leading to disuse, depression, and disability [25]. Kinesiophobia and pain catastrophizing have variably shown a negative association with self-reported function in the early period after ACL reconstruction; whereas pain catastrophizing has consistently shown a positive association with pain intensity in the same time frame [5, 11, 12, 17, 37]. Self-efficacy is a person’s judgment in their potential ability to carry out a task [4]. Self-efficacy for rehabilitation tasks is positively associated with self-reported function in the early period after ACL reconstruction [12], but less is known about self-efficacy for activities involving the knee.
ACL reconstruction rehabilitation is typically divided into early and advanced phases [1]. The transition from early to advanced rehabilitation occurs when knee impairments are sufficiently resolved, usually around 10–16 weeks post-surgery [6]. It is plausible that a maladaptive psychological response during early rehabilitation could slow knee impairment resolution, delaying the transition to advanced rehabilitation. Limited research has examined the influence of kinesiophobia, pain catastrophizing, and self-efficacy for rehabilitation and knee activity on physical measures following ACL reconstruction [19, 26].
The goal of this study was to examine the association of kinesiophobia, pain catastrophizing, and self-efficacy for rehabilitation and knee activity in the first 4 weeks after ACL reconstruction with knee impairment resolution and readiness for advanced rehabilitation at 12 weeks post-surgery. The study hypothesis was that elevated kinesiophobia and pain catastrophizing and decreased self-efficacy for rehabilitation and knee activity in the first 4 weeks after ACL reconstruction would be associated with poorer knee impairment resolution and a lack of readiness for advanced rehabilitation at 12 weeks post-surgery.
Materials and methods
Patient who had ACL reconstruction and subsequent rehabilitation at UF Health Orthopaedics and Sports Medicine Institute from 2009 to 2013 were eligible for participation. Inclusion criteria were a unilateral, primary ACL reconstruction, time from injury to surgery less than 53 weeks, and a pre-injury Tegner Activity Rating of 5 or greater [35] indicting participation in sports. Potential subjects were excluded for previous lower extremity surgery, bilateral knee injury, concomitant ligamentous injury greater than grade I, and articular cartilage or meniscal repair. Adult subjects gave written informed consent prior to participating in the study, whereas minor subjects gave written assent and the parent or guardian gave written informed consent.
Arthroscopic surgery was performed by a board-certified orthopaedic surgeon using allograft or autograft tissue. Autograft sources were bone–patellar tendon–bone or semitendinosus and gracilis tendons; allograft sources were tibialis anterior, tibialis posterior, or Achilles tendon. The standard post-surgical rehabilitation protocol permitted weight-bearing and unrestricted knee motion immediately following surgery. The first 6 weeks of rehabilitation focused on decreasing knee effusion, improving knee range of motion and quadriceps muscle activation, and obtaining independent gait; whereas the next 6 weeks also included exercises to increase lower extremity muscle strength, muscle endurance and proprioception.
Testing protocol
Testing time points were 1, 4, and 12 weeks post-surgery. Testing was administered by two board-certified sports physical therapists at UF Health Orthopaedics and Sports Medicine Institute. Demographic variables were collected 1 week post-surgery, psychological factor questionnaire responses were collected at all time points, and knee impairment measures were collected at 12 weeks post-surgery.
Demographic variables
Demographic variables were age, sex, body mass index (BMI), time from injury to surgery, pre-injury Tegner Activity Rating, mechanism of injury (contact or non-contact), injury situation (sports or non-sports), graft type (allograft or autograft), and accompanying surgical procedures. Accompanying surgical procedures included meniscectomy or chondroplasty.
Psychological questionnaires
Fear avoidance
Kinesiophobia was measured with the 11-item Tampa Scale for Kinesiophobia (TSK-11) [41]. Scores range from 11 to 44 points and higher scores indicate greater kinesiophobia. Pain catastrophizing was assessed with the 13-item Pain Catastrophizing Scale (PCS) [34]. Scores range from 0 to 52 points and higher scores indicate greater pain catastrophizing. The TSK-11, TSK-11 subscales (fear of pain, fear of injury, and somatic focus), and the PCS have been validated in the ACL reconstruction population [17]; however, reliability and responsiveness have not been examined.
Self-efficacy
A modified ten-item version of the Self-Efficacy for Rehabilitation Outcome Scale (SER) assessed confidence in performing tasks encountered during rehabilitation following knee or hip surgery [12, 39]. Scores range from 0 to 100 points and higher scores indicate greater rehabilitation self-efficacy. The internal consistency coefficient (Cronbach’s alpha) is 0.94 for the unmodified version of this questionnaire [39]. The reliability and responsiveness of the original and modified versions of the SER have not been determined in patients with ACL reconstruction. Confidence performing activities involving the knee was measured with a ten-item questionnaire (Knee Activity Self-Efficacy, KASE) [36] Scores range from 0 to 100 points and higher scores indicate greater self-efficacy in knee-related activity. Although not yet validated, test–retest reliability for the KASE questionnaire has been examined in patients with ACL reconstruction (intraclass correlation coefficient 0.85) [21].
Knee impairment measures
Patients rated their best and worst pain levels over 24 h and their current pain level on the 11-point Numeric Pain Rating Scale (NPRS) [29], with 0 representing no pain and 10 representing the worst imaginable pain. The three pain ratings were averaged to obtain a composite knee pain intensity score. The NPRS is widely used for assessing knee pain intensity and has shown acceptable reliability in other populations [29], but to our knowledge, reliability and responsiveness have not been assessed in patients with ACL reconstruction. Knee flexion and extension passive range of motion were measured with a standard clinical goniometer. Range of motion (ROM) deficit was calculated as the surgical side minus the non-surgical side measure. Goniometry has strong inter-tester reliability for measuring knee range of motion [9]. Quadriceps strength was measured with an isokinetic dynamometer (Biodex System 3; Biodex Medical Systems, Shirley, NY, USA). After a 5-min stationary bike warm-up, patients were positioned on the dynamometer with stabilization belts over the pelvis and thigh. The dynamometer moved through a range of 90°–0° of knee motion at 60°/s. Two practice trials were followed by five maximal effort trials. Testing was conducted on the non-surgical side followed by the surgical side. Peak knee extensor torque was recorded. A quadriceps symmetry index was calculated by normalizing peak torque on the surgical side to that of the non-surgical side and multiplying by 100. Isokinetic strength testing is a reliable measure for quadriceps strength [8, 32]. An additional measure was the 2000 International Knee Documentation Committee (IKDC) subjective knee form, which includes 18 items related to knee symptoms and functional activity. Scores range from 0 to 100 and a higher score indicates better knee function. The IKDC has good test–retest reliability [intraclass correlation coefficient (ICC) = 0.94] and has been validated for various knee conditions, including ACL reconstruction [22].
Data management and group assignment
Data were collected on paper forms and transferred to an electronic database (Microsoft Access 2007; Microsoft Corporation, Redmond, WA, USA). Data integrity was insured by verifying appropriate values for questionnaire responses and a full data set for at least three patients randomly selected from consecutive blocks of ten patients. Standardized criteria to determine readiness for advanced ACL reconstruction rehabilitation do not exist, although criteria have been proposed [40]. Logically, the knee must tolerate high-demand activities that will be introduced in advanced rehabilitation. Criteria used to specify readiness for advanced rehabilitation were: (1) composite NPRS score ≤ 2, (2) knee extension range of motion equal to the contralateral side and knee flexion range of motion within 5° of the contralateral side, and (3) quadriceps symmetry index > 60%. Patients who met all criteria were assigned to READY and others were assigned to NOT READY.
The study protocol was approved by the University of Florida Institutional Review Board (IRB Project #548–2006).
Statistical analysis
Statistical analysis was performed with SPSS Statistics version 24 (IBM Corp. Armonk, NY, USA). Descriptive statistics were generated. Data were visually inspected and analysed with the Shapiro–Wilk test for normality. Statistical significance was set at p < 0.05 for all analyses, unless otherwise specified.
Advanced rehabilitation group comparison
Demographic variables were compared between NOT READY and READY groups with independent samples t tests or Chi-square statistic. Longitudinal changes in questionnaire scores were compared between groups with repeated measures general linear models. Knee impairment measures at 12 weeks post-surgery were compared between groups with independent samples t tests.
Knee impairment resolution
Because average knee pain and knee ROM deficit at 12 weeks post-surgery had a non-normal distribution, Spearman’s rank correlation examined the association of questionnaire scores at 1 week, 4 weeks, or the change from 1 to 4 weeks post-surgery with knee impairment measures at 12 weeks post-surgery. The strength of the association was interpreted from the magnitude of the correlation [33].
Readiness for advanced rehabilitation
Separate hierarchical logistic regression models examined the prediction of NOT READY or READY group assignment from questionnaire scores at 1, 4 weeks, or the change between 1 and 4 weeks post-surgery. Any demographic variable significantly different between groups was entered in the first step. Questionnaire scores were entered next with forward conditional selection. The threshold to enter the model was p < 0.05 and for removal was p < 0.10. Group coding was “0” for NOT READY and “1” for READY. The odds ratio was computed for variables in the model. The computed odds ratio is the ratio of odds for assignment to READY to the odds of assignment to NOT READY for a one unit increase in the questionnaire score. An odds ratio above 1 implies that an increase in score increases odds of assignment to READY. An odds ratio below 1 implies that an increase in score decreases odds of assignment to READY; however, to aid interpretation, the inverse was computed and the narrative adjusted to reference the NOT READY group [31].
Sample size justification
Sample size was based on fulfilling the general recommendations for multivariate analysis techniques and the goal of creating a parsimonious prediction model. Recommended sample size for multivariate analysis includes a minimum sample of 50 and a preferred sample exceeding 100, or between 5 and 10 subjects per predictor variable [18]. With 4 questionnaire scores at a given time point or interval (ie. 1, 4 weeks, or the change between 1 and 4 weeks post-surgery) and the potential for at least one demographic variable in each model, the minimum sample size was determined to be 50 patients. Such a sample size would allow for a range of 5–10 variables to be included in predictor models because there was a concern with overfitting.
Results
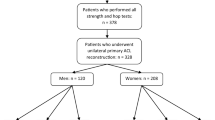
Patient enrollment is found in Fig. 1. Of the 121 patients with ACL reconstruction identified as potential subjects, 75 met all study eligibility criteria for being included in this analysis. The study sample included 43 patients in NOT READY and 32 patients in READY.
Advanced rehabilitation group comparison
Demographic data for NOT READY and READY groups are summarized in Table 1. Only the mechanism of injury significantly differed between groups (p = 0.036), with a higher proportion of contact injuries in READY than NOT READY. Questionnaires scores are found in Table 2. The group × time interaction was not significant for any questionnaire (n.s.). Conversely, the main effect for time was significant for all questionnaires (p < 0.001). Pairwise comparisons showed that scores significantly improved at all time points (p < 0.001) except between 4 and 12 weeks post-surgery for PCS (n.s.) and SER (n.s.). IKDC scores are also found in Table 2. A significant group × time interaction was found for IKDC scores (p = 0.011). Post hoc testing showed that IKDC scores did not differ between groups at 1 week post-surgery (n.s.), but were significantly higher in READY compared to NOT READY at 4 and 12 weeks post-surgery (p = 0.002 and < 0.001, respectively). Knee impairment physical measures are found in Table 3. In concordance with group assignment, NOT READY had significantly higher knee pain intensity, greater knee ROM deficit, and lower quadriceps symmetry index compared to READY (p < 0.05). Advanced rehabilitation criteria missed by patients in NOT READY were pain n = 9, knee ROM n = 29, and quadriceps symmetry index n = 25; 28 of 43 patients (65%) in NOT READY failed to meet more than one criterion.
Knee impairment resolution
Correlations between questionnaire scores and knee impairment measures are found in Table 4. Significant correlations included TSK-11 score at 1 week post-surgery and quadriceps symmetry index at 12 weeks post-surgery, PCS scores at 1 and 4 weeks post-surgery and composite NPRS score at 12 weeks post-surgery; and KASE score at 4 weeks post-surgery and total ROM deficit at 12 weeks post-surgery. Correlation magnitude ranged from 0.22 to 0.29, and correlation sign indicated that a better psychological response was associated with greater knee impairment resolution, except for the association between TSK-11 score at 1 week post-surgery and quadriceps symmetry index.
Readiness for advanced rehabilitation
Mechanism of injury was entered in the first step of the models because of its association with the outcome. After accounting for mechanism of injury, TSK-11 score at 4 weeks post-surgery was identified as a significant predictor of group assignment (odds ratio = 0.908). With conversion, odds of assignment to NOT READY increased 1.10 times for each 1 point increase in TSK-11 score. Further analysis was performed with the TSK-11 subscale scores at 4 weeks post-surgery, and the TSK-11 fear of re-injury subscale score was found to be a significant predictor of group assignment (odds ratio 0.765). With conversion, odds of assignment to NOT READY increased 1.31 times for each 1 point increase in the TSK-11 fear of re-injury subscale score.
Discussion
The most important findings of the present study were that (1) pain catastrophizing and knee activity self-efficacy at 4 weeks post-surgery were weakly correlated with knee impairment resolution at 12 weeks post-surgery, and (2) higher kinesiophobia at 4 weeks post-surgery increased the odds for not meeting advanced rehabilitation criteria at 12 weeks post-surgery. These findings support previous work on the association between psychological factors and ACL reconstruction outcomes [11, 12, 26, 27], that is, pain catastrophizing and knee activity self-efficacy influenced knee impairment resolution, while kinesiophobia influenced readiness for advanced rehabilitation. These findings have clinical relevance by indicating that 4 weeks post-surgery might be an appropriate time to perform psychological assessment in this patient population.
Advanced rehabilitation group comparison
Approximately 57% of patients were assigned to NOT READY, highlighting the potential for insufficient knee impairment resolution at 12 weeks post-surgery. It is important to point out that the advanced rehabilitation criteria used in this study have not been validated and additional or different criteria may better indicate readiness for advanced rehabilitation after ACL reconstruction. Lower IKDC subjective scores in NOT READY compared to READY help corroborate group assignment. All psychological questionnaire scores significantly improved in both groups over time and in the interval from 1 to 4 weeks post-surgery, consistent with previous research [12]. PCS and SER scores did not significantly improve from 4 to 12 weeks post-surgery, and this is potentially from floor (PCS) and ceiling (SER) effects based on the magnitude of the scores. This finding can inform future research about appropriate time frames to assess these psychological factors.
Knee impairment resolution
Statistically significant, albeit weak, associations were identified between specific psychological questionnaire scores and knee impairment measures. The association between higher pain catastrophizing at 1 and 4 weeks post-surgery and higher pain intensity at 12 weeks post-surgery follows the fear-avoidance model and has been reported immediately after ACL reconstruction [5]. Higher knee activity self-efficacy at 4 weeks post-surgery was associated with a smaller knee ROM deficit at 12 weeks post-surgery. Research in knee injury populations has inconsistently found an association between psychological factors and recovery of joint motion [10, 15, 20, 30], suggesting the result may depend on the psychological factor studied. It was unexpected to find that higher kinesiophobia at 1 week post-surgery was associated with a higher quadriceps symmetry index at 12 weeks post-surgery, and the interpretation of this result is unclear as kinesiophobia should be associated with avoidant behaviour. Because quadriceps strength recovery is important after ACL reconstruction, further research to understand the influence of psychological factors on this knee impairment is warranted.
Readiness for advanced rehabilitation
A contact mechanism of injury increased the odds of assignment to READY by about 3. After accounting for this demographic variable, higher score on the TSK-11 or fear of re-injury subscale at 4 weeks post-surgery increased odds of assignment to NOT READY. The mechanism of injury is non-modifiable and may be considered baseline risk, whereas kinesiophobia is modifiable and could be addressed during rehabilitation. Odds ratio for TSK-11 score was 1.10 and for fear of re-injury subscale score was 1.31, indicating that the fear of re-injury subscale score may be more discriminative. The TSK-11 fear of re-injury subscale score is calculated from items 1, 2 and 10 of the TSK-11 questionnaire [17], which reduces administrative and patient burden without decreasing predictive ability.
Future directions
This study found that some of the same psychological factors that deter a return to sport after ACL reconstruction (e.g. lower knee activity self-efficacy and higher kinesiophobia) [3, 14] also have a negative association with early rehabilitation outcomes. The finding suggests that it may be beneficial to monitor psychological response early in ACL reconstruction rehabilitation, as opposed to waiting until the time of return to sport. Further research is needed to understand how various psychological factors vary alongside physical recovery during ACL reconstruction rehabilitation and what constitutes a psychological response indicative of poor rehabilitation outcomes. An advantage of this study is that it included multiple psychological factors, whereas many studies focus on a single psychological factor. The study also included physical (knee impairment) outcomes, which extends previous research using only self-reported function as an outcome measure. A notable study limitation is that the criteria for advanced ACL reconstruction rehabilitation were operationally defined, so results may not generalize to clinics that use other criteria. Another limitation is that the sample size was not large enough to include all psychological questionnaires scores in a single regression model.
Conclusions
Lower pain catastrophizing and higher knee activity self-efficacy levels 4 weeks after ACL reconstruction were associated with better knee impairment resolution at 12 weeks post-surgery, whereas lower kinesiophobia at 4 weeks post-surgery increased the odds of meeting advanced rehabilitation criteria at 12 weeks post-surgery. The primary clinical implication of this study is that monitoring these psychological factors for 4 weeks after ACL reconstruction might provide an opportunity to better identify those at risk for not progressing in their rehabilitation program.
References
Adams D, Logerstedt DS, Hunter-Giordano A, Axe MJ, Snyder-Mackler L (2012) Current concepts for anterior cruciate ligament reconstruction: a criterion-based rehabilitation progression. J Orthop Sports Phys Ther 42:601–614
Ardern CL (2015) Anterior cruciate ligament reconstruction-not exactly a one-way ticket back to the preinjury level: a review of contextual factors affecting return to sport after surgery. Sports Health 7:224–230
Ardern CL, Taylor NF, Feller JA, Webster KE (2013) A systematic review of the psychological factors associated with returning to sport following injury. Br J Sports Med 47:1120–1126
Bandura A (1977) Self-efficacy: towards a unifying theory of behavioral change. Psychol Rev 84:191–215
Baranoff J, Hanrahan SJ, Connor JP (2015) The roles of acceptance and catastrophizing in rehabilitation following anterior cruciate ligament reconstruction. J Sci Med Sport 18:250–254
Beynnon BD, Johnson RJ, Abate JA, Fleming BC, Nichols CE (2005) Treatment of anterior cruciate ligament injuries, part I. Am J Sports Med 33:1579–1602
Brand E, Nyland J (2009) Patient outcomes following anterior cruciate ligament reconstruction: the influence of psychological factors. Orthopedics 32:335
Brosky JA Jr, Nitz AJ, Malone TR, Caborn DN, Rayens MK (1999) Intrarater reliability of selected clinical outcome measures following anterior cruciate ligament reconstruction. J Orthop Sports Phys Ther 29:39–48
Brosseau L, Balmer S, Tousignant M, O’Sullivan JP, Goudreault C, Goudreault M et al (2001) Intra- and intertester reliability and criterion validity of the parallelogram and universal goniometers for measuring maximum active knee flexion and extension of patients with knee restrictions. Arch Phys Med Rehabil 82:396–402
Brown ML, Plate JF, Von Thaer S, Fino NF, Smith BP, Seyler TM et al (2016) Decreased range of motion after total knee arthroplasty is predicted by the Tampa Scale of Kinesiophobia. J Arthroplasty 31:793–797
Chmielewski TL, Jones D, Day T, Tillman SM, Lentz TA, George SZ (2008) The association of pain and fear of movement/reinjury with function during anterior cruciate ligament reconstruction rehabilitation. J Orthop Sports Phys Ther 38:746–753
Chmielewski TL, Zeppieri G Jr, Lentz TA, Tillman SM, Moser MW, Indelicato PA et al (2011) Longitudinal changes in psychosocial factors and their association with knee pain and function after anterior cruciate ligament reconstruction. Phys Ther 91:1355–1366
Clement D, Arvinen-Barrow M, Fetty T (2015) Psychosocial responses during different phases of sport-injury rehabilitation: a qualitative study. J Athl Train 50:95–104
Czuppon S, Racette BA, Klein SE, Harris-Hayes M (2014) Variables associated with return to sport following anterior cruciate ligament reconstruction: a systematic review. Br J Sports Med 48:356–364
Doury-Panchout F, Metivier JC, Fouquet B (2015) Kinesiophobia negatively influences recovery of joint function following total knee arthroplasty. Eur J Phys Rehabil Med 51:155–161
Everhart JS, Best TM, Flanigan DC (2015) Psychological predictors of anterior cruciate ligament reconstruction outcomes: a systematic review. Knee Surg Sports Traumatol Arthrosc 23:752–762
George SZ, Lentz TA, Zeppieri G, Lee D, Chmielewski TL (2012) Analysis of shortened versions of the Tampa Scale for Kinesiophobia and pain catastrophizing scale for patients after anterior cruciate ligament reconstruction. Clin J Pain 28:73–80
Hair JE, Anderson RE, Tatham RL, Black WC (1998) Multivariate data analysis, 5th edn. Prentice Hall, Upper Saddle River
Hartigan EH, Lynch AD, Logerstedt DS, Chmielewski TL, Snyder-Mackler L (2013) Kinesiophobia after anterior cruciate ligament rupture and reconstruction: noncopers versus potential copers. J Orthop Sports Phys Ther 43:821–832
Hemsley K, Sitler M, Moyer R, Oatis C (2010) Neuromuscular and psychological influences on range of motion recovery in anterior cruciate ligament reconstruction patients. J Electromyogr Kinesiol 20:684–692
Hsu CJ, George SZ, Chmielewski TL (2016) Association of quadriceps strength and psychosocial factors with single-leg hop performance in patients with meniscectomy. Orthop J Sports Med 4:1–8
Irrgang JJ, Anderson AF, Boland AL, Harner CD, Kurosaka M, Neyret P et al (2001) Development and validation of the international knee documentation committee subjective knee form. Am J Sports Med 29:600–613
Kvist J, Ek A, Sporrstedt K, Good L (2005) Fear of re-injury: a hindrance for returning to sports after anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 13:393–397
Lee DY, Karim SA, Chang HC (2008) Return to sports after anterior cruciate ligament reconstruction—a review of patients with minimum 5-year follow-up. Ann Acad Med Singapore 37:273–278
Leeuw M, Goossens ME, Linton SJ, Crombez G, Boersma K, Vlaeyen JW (2007) The fear-avoidance model of musculoskeletal pain: current state of scientific evidence. J Behav Med 30:77–94
Lentz TA, Tillman SM, Indelicato PA, Moser MW, George SZ, Chmielewski TL (2009) Factors associated with function after anterior cruciate ligament reconstruction. Sports Health 1:47–53
Lentz TA, Zeppieri G Jr, George SZ, Tillman SM, Moser MW, Farmer KW et al (2015) Comparison of physical impairment, functional, and psychosocial measures based on fear of reinjury/lack of confidence and return-to-sport status after ACL reconstruction. Am J Sports Med 43:345–353
Lentz TA, Zeppieri G Jr, Tillman SM, Indelicato PA, Moser MW, George SZ et al (2012) Return to preinjury sports participation following anterior cruciate ligament reconstruction: contributions of demographic, knee impairment, and self-report measures. J Orthop Sports Phys Ther 42:893–901
Mintken PE, Glynn P, Cleland JA (2009) Psychometric properties of the shortened disabilities of the Arm, Shoulder, and Hand Questionnaire (QuickDASH) and Numeric Pain Rating Scale in patients with shoulder pain. J Shoulder Elbow Surg 18:920–926
Morrey MA, Stuart MJ, Smith AM, Wiese-Bjornstal DM (1999) A longitudinal examination of athletes’ emotional and cognitive responses to anterior cruciate ligament injury. Clin J Sport Med 9:63–69
Osborne JW (2006) Bringing balance and technical accuracy to reporting odds ratios and the results of logistic regression analyses. Pract Assess Res Eval 11:1–6
Risberg MA, Holm I, Tjomsland O, Ljunggren E, Ekeland A (1999) Prospective study of changes in impairments and disabilities after anterior cruciate ligament reconstruction. J Orthop Sports Phys Ther 29:400–412
Schober P, Boer C, Schwarte LA (2018) Correlation coefficients: appropriate use and interpretation. Anesth Analg. https://doi.org/10.1213/ane.0000000000002864
Sullivan MJ, Bishop SR, Pivik J (1995) The Pain Catastrophizing Scale: development and validation. Psychol Assess 7:524–532
Tegner Y, Lysholm J (1985) Rating systems in the evaluation of knee ligament injuries. Clin Orthop Relat Res 198:43–49
Thomee P, Wahrborg P, Borjesson M, Thomee R, Eriksson BI, Karlsson J (2006) A new instrument for measuring self-efficacy in patients with an anterior cruciate ligament injury. Scand J Med Sci Sports 16:181–187
Tichonova A, Rimdeikiene I, Petruseviciene D, Lendraitiene E (2016) The relationship between pain catastrophizing, kinesiophobia and subjective knee function during rehabilitation following anterior cruciate ligament reconstruction and meniscectomy: a pilot study. Medicina (Kaunas) 52:229–237
Tracey J (2003) The emotional response to the injury and rehabilitation process. J Appl Sport Psychol 15:279–293
Waldrop D, Lightsey OR, Ethington CA, Woemmel CA, Coke AL (2001) Self-efficacy, optimism, health competence, and recovery from orthopedic surgery. J Couns Psychol 48:233–238
Wilk KE, Arrigo CA (2017) Rehabilitation principles of the anterior cruciate ligament reconstructed knee: twelve steps for successful progression and return to play. Clin Sports Med 36:189–232
Woby SR, Roach NK, Urmston M, Watson PJ (2005) Psychometric properties of the TSK-11: a shortened version of the Tampa Scale for Kinesiophobia. Pain 117:137–144
Acknowledgements
The authors acknowledge Trevor Lentz and Giorgio Zeppieri Jr for their assistance with data collection and Ariel Botwin for his assistance with data preparation.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors certify that they have no commercial association that might pose a conflict of interest in connection with this article.
Ethical approval
The study protocol was approved by the University of Florida Institutional Review Board (IRB Project #548-2006).
Additional information
This work was conducted when Terese L. Chmielewski and Steven Z. George were at the University of Florida.
Rights and permissions
About this article
Cite this article
Chmielewski, T.L., George, S.Z. Fear avoidance and self-efficacy at 4 weeks after ACL reconstruction are associated with early impairment resolution and readiness for advanced rehabilitation. Knee Surg Sports Traumatol Arthrosc 27, 397–404 (2019). https://doi.org/10.1007/s00167-018-5048-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-018-5048-6