Abstract
Purpose
Historically poor results of survivorship and functional outcomes of patellofemoral arthroplasty (PFA) have been reported in the setting of isolated patellofemoral osteoarthritis. More recently, however, fairly good results of PFA were reported, but the current status of PFA outcomes is unknown. Therefore, a systematic review was performed to assess overall PFA survivorship and functional outcomes.
Methods
A search was performed using PubMed, Embase and Cochrane systems, and the registries were searched. Twenty-three cohort studies and one registry reported survivorship using Kaplan–Meier curve, while 51 cohort studies reported functional outcomes of PFA.
Results
Twelve studies were level II studies, while 45 studies were level III or IV studies. Heterogeneity was mainly seen in type of prosthesis and year the cohort started. Nine hundred revisions in 9619 PFAs were reported yielding 5-, 10-, 15- and 20-year PFA survivorships of 91.7, 83.3, 74.9 and 66.6 %, respectively, and an annual revision rate of 2.18. Functional outcomes were reported in 2587 PFAs with an overall score of 82.2 % of the maximum score. KSS and Knee Function Score were 87.5 and 81.6 %, respectively.
Conclusion
This systematic review showed that fairly good results of PFA survivorship and functional outcomes were reported at short- and midterm follow-up in the setting of isolated patellofemoral osteoarthritis. Heterogeneity existed mainly in prosthesis design and year the cohort started.
Clinical relevance
These results provide a clear overview of the current status of PFA in the setting of isolated patellofemoral osteoarthritis.
Level of evidence
IV.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Isolated patellofemoral osteoarthritis (OA) is a common degenerative knee disease and accounts for 10–24 % of all patients presenting with knee pain [23, 26, 61, 91]. Joint replacement treatments for isolated patellofemoral OA include patellofemoral arthroplasty (PFA) and total knee arthroplasty (TKA). In 1979, the first results of PFA were presented and although patellofemoral pain was alleviated, the reoperation rates were high (35 %) [12, 60]. In the following years, satisfaction results of 20–72 % had been reported after PFA [5, 8, 44, 82, 85, 100]. Many surgeons therefore advocate the use of total knee arthroplasty (TKA) over PFA in the setting of isolated patellofemoral OA [21, 63, 69, 80].
Controversy, however, remains if an invasive procedure such as TKA is justified in young patients with isolated patellofemoral OA [27, 41, 43, 59, 97]. This is of particular interest due to the higher risk of TKA revision in younger patients [28, 35, 48, 62], the predicted increase in TKA revisions [81] and inevitable bone loss with each subsequent revision [42]. PFA is correlated with less blood loss [19], shorter hospital stay [19], preservation of bone stock and ligaments [76] and better functional outcomes and stair climbing abilities [54] when compared to TKA. Moreover, it has been shown that second-generation PFA implants had equivalent reoperation and revision rates, pain and mechanical complications when compared to TKA [27].
In order to optimize the outcomes of PFA for isolated patellofemoral OA, it is important to accurately characterize the survivorship and functional outcomes of PFA. To our knowledge, however, studies assessing overall survivorship and functional outcomes of PFA are lacking. Therefore, a systematic review was performed to assess survivorship, revision rates and functional outcomes of PFA. The purpose of this study was to (1) assess survivorship in cohort studies and registries, (2) determine whether revision rates are lower in the more recent studies and (3) evaluate the functional outcomes of PFA. The hypothesis of the study was that fairly good 10-year survivorship could be achieved with good functional outcomes and that more recent studies had lower revision rates than older studies.
Materials and methods
A systematic search in the electronic databases PubMed, Embase and Cochrane Library was performed for studies reporting survivorship and functional outcomes of PFA. The search terms were “arthroplasty AND (patellofemoral OR PF OR PFA OR PFR) AND (outcome OR functional outcome OR scores OR results OR revision OR revision rate OR reoperation OR treatment failure OR prosthesis failure OR failure OR failure rate OR survivorship OR survival)”. Two authors (JPL and HC) independently scanned all identified studies by title and abstract. Eligible studies were subsequently scanned for the full text on the inclusion and exclusion criteria. In addition, the references of the scanned articles were checked for any missed studies, and annual registries were scanned for survivorship and functional outcomes. If a disagreement existed between authors, a third author (HAZ) was consulted. Consensus was reached on the inclusion and exclusion of all articles.
Inclusions criteria consisted of studies that (I) reported survivorship, revision rates or functional outcomes, (II) were published between 1995 and 2015 and (III) were minimum level IV case series using adjusted Oxford Centre for Evidence-Based Medicine 2011 Levels of Evidence [74, 101]. Exclusion criteria consisted of (I) studies that regarded patellar subluxation as primary surgery indication, (II) studies that had acute concurrent knee pathology (e.g. patella tendon ruptures, anterior cruciate ligament injuries), (III) case reports, systematic reviews and expert opinions and (IV) studies using the same database.
All data were collected in a datasheet in Excel 2011 (Microsoft Corp., Redmond, WA, USA). Parameters collected included study authors, year of publication, year the cohort started and ended, total number of PFA, total number of failures, Kaplan–Meier survivorship, reported functional outcomes and mean follow-up.
Outcomes in this study included Kaplan–Meier survivorship, revision rate, annual revision rate and functional outcomes. Survivorship was included for all studies that reported their outcomes using a Kaplan–Meier estimation [46]. All studies were compiled in a scatter plot and a trend line was added to calculate the survivorship at 5, 10, 15 and 20 years of follow-up. Revision rates of all studies were calculated by dividing the number of failures by the total number of PFA at follow-up. Annual revision rate was calculated with the parameter “revision rate per 100 observed component years”, which is used by several orthopaedic studies [53, 77, 78, 86]. This parameter enables comparison of revision rates between different studies or subgroups with varying follow-up intervals. The annual revision rate was used to compare the revision rates of cohort studies and registries and to compare studies published before 2010 with studies published since 2010. Finally, all functional outcomes were collected, and scores were reported as the percentage of the maximum score. This enabled comparison of different functional outcomes and calculation of a mean overall score.
Statistical analysis
Statistical analysis was performed using Excel 2011 and SPSS Statistics 21.0 (SPSS Inc., Armonk, NY, USA). A Chi-square test was used to compare annual revision rate of studies published before 2010 and since 2010. No statistical analysis could be performed when comparing annual revision rates [53, 77, 78, 86]. The statistical analysis was two-sided, and a difference was considered significant when p < 0.05.
Results
Search results
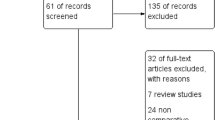
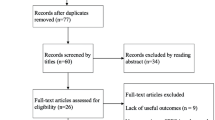
After removing of duplicates and reviewing title, abstract and full text of the articles, a total of 57 cohort studies [1–3, 6, 7, 10, 11, 13, 15–20, 22, 24, 25, 30–34, 37–40, 45, 47, 50, 51, 55, 57, 58, 63–68, 70, 71, 73, 75, 84, 88–90, 92–96, 98, 99, 102–104] and three registries [4, 9, 72] were included in this study (Fig. 1). Twenty-three cohort studies [1–3, 6, 16–18, 20, 32, 33, 39, 40, 50, 57, 64, 70, 71, 75, 84, 88, 92, 96, 102] and one registry [4] reported survivorship using Kaplan–Meier analysis. Forty-two cohort studies [1–3, 6, 11, 13, 15–18, 20, 22, 24, 25, 30–33, 37, 39, 40, 45, 50, 51, 55, 57, 64, 65, 67, 70, 71, 73, 75, 84, 88–90, 92, 96, 98, 99, 102] and three registries [4, 9, 72] reported revision rates of which 22 cohort studies were published between 1995 and 2009 [1, 6, 13, 15, 16, 18, 24, 25, 32, 45, 50, 51, 55, 64, 65, 67, 73, 88–90, 92, 98] and 20 were published since 2010 [2, 3, 11, 17, 20, 22, 30, 31, 33, 37, 39, 40, 57, 70, 71, 75, 84, 96, 99, 102]. Finally, a total of 51 cohort studies reported functional outcomes [1–3, 6, 7, 10, 11, 15–20, 22, 25, 30–34, 37–40, 45, 47, 50, 51, 55, 57, 58, 63–66, 68, 70, 71, 75, 84, 88–90, 92–95, 98, 102–104].
Quality of studies
Twelve studies were level II prospective studies [1, 3, 7, 22, 38, 55, 63, 68, 73, 90, 92, 102], while 45 studies were level III retrospective studies or level IV case series [2, 6, 10, 11, 13, 15–20, 24, 25, 30–34, 37, 39, 40, 45, 47, 50, 51, 57, 58, 64–67, 70, 71, 75, 84, 88, 89, 93–96, 98, 99, 103, 104]. No level I studies were identified, and none of the studies were blinded or randomized. Heterogeneity mainly existed in the type of prosthesis and year the cohort started.
PFA survivorship
Twenty-three cohort studies reported survivorship of 1326 PFAs, and one registry reported survivorship of 2495 PFAs. The trend line of cohort studies showed 5-, 10-, 15- and 20-year PFA survivorships of 91.7, 83.3, 74.9 and 66.6 %, respectively. The trend line of the annual registry showed 5- and 10-year survivorships of 84.7 and 71.4 %, respectively (Fig. 2).
Revision rates
A total of 900 revisions in 9619 PFAs were identified, yielding a revision rate of 9.4 % and an annual revision rate of 2.18 (Table 1; Fig. 3). Registries reported a slightly higher annual revision rate than cohort studies (2.19 vs. 2.14). Cohort studies published since 2010 revealed a lower annual revision rate than more recent cohort studies (1.93 vs. 2.33) (Table 1).
Functional outcomes
Fifty-one cohort studies reported functional outcomes for 2587 PFAs using eleven different scoring systems. Most of the functional outcome scores (70 %) were reported within the first 5 years (Table 2; Fig. 4). The average functional outcome score was 82.2 %. Good to excellent knee function was reported in 87.3 %, and Knee Society Score and Knee Function Score were 87.5 and 81.6 %, respectively. Patella-specific scores (i.e. Melbourne Score and Hungerford and Kenna Score) were 85.6 and 83.3 %, respectively. Pain scores (Knee Pain Score and Bristol Pain Score) were 84.8 and 85.8 %, respectively (Table 2; Fig. 4).
Discussion
The most important finding of this systematic review was that survivorship of PFA at 5-, 10-, 15- and 20-year follow-up was 91.7, 83.3, 74.9 and 66.6 %, respectively. Cohort studies revealed an annual revision rate of 2.14, while registries yielded an annual revision rate of 2.19. Older studies (i.e. published before 2010) reported a higher annual revision rate when compared to more recently published studies (2.33 vs. 1.93). Finally, a mean functional outcome score of 82.2 % of the maximum scores was reported following PFA.
At short-term follow-up of 5–6 years, fairly good results were reported. PFA survivorship at 5-year follow-up was 91.7 %, while the percentage of patients reporting good or excellent knee function varied between 86.8 and 92.5 %. Furthermore, some small studies reported excellent 5-year PFA survivorship (96.2–100 %) [2, 75], which indicates that good results can be achieved at short-term follow-up. At midterm follow-up, the 10-year survivorship was 83.3 %, while the percentage of patients reporting good or excellent knee function varied between 76.2 and 82.4 %. Similarly, individual studies have shown that PFA is durable at 10-year follow-up with survivorship between 88 and 89 % [2, 50]. These results at 5- and 10-year follow-up show fairly good results following PFA, especially when taking into account the fact that different PFA designs were included from 1995 to 2015.
At long-term follow-up of 15 and 20 years, the survivorships of PFA were 74.0 and 66.6 %, respectively, while 79.5–82.3 % of the patients reported good or excellent function at long-term follow-up. To our knowledge, only three studies have reported PFA survivorship at 15 years or later [6, 50, 96]. These studies reported 15- and 16-year survivorships of 58–79 %, while two of these studies reported 20-year survivorship of 59–69 % [50, 96]. Interestingly, the cohorts of these studies started between 1972 and 1977. It has been shown that these first-generation prostheses have higher revision and reoperation rates when compared to second-generation prostheses [14, 27, 79]. These numbers are therefore not representative of the long-term survivorship potential of the current available prostheses, and caution is advised with drawing conclusions about long-term PFA survivorship on the basis of such series.
Similarly, when comparing more recent studies with studies published before 2010, it was noted that the more recent cohort studies reported a lower annual revision rate (1.93 vs. 2.33, Table 1). Several factors may explain these differences including the aforementioned differences in revision and reoperation rate between first- and second-generation prostheses. There are more improved and second-generation prostheses in the group of more recently published studies, which may contribute to the lower failure rate. Similarly to the findings of Dy et al. [27], the results of the present study suggest that better long-term results may be expected with second-generation or improved prostheses, but longer follow-up of these prostheses is not available yet. Secondly, differences in annual revision rate between both study groups can possibly be explained by improved patient selection criteria. Progression of OA in the tibiofemoral components is one of the major failure modes in PFA [1, 73, 96], and OA in the tibiofemoral compartment is therefore considered a contraindication. However, this was not uniformly applied in all studies and may have influenced the results [55]. Thirdly, some prosthesis designs have been consistently associated with unfavourable outcomes. The Lubinus prosthesis (Waldemar Link, Hamburg, Germany) has been used in several studies that were published before 2010 with poor results [13, 89, 92]. This is corroborated by the fact that the highest revision rates in the Australia registry were associated with the Lubinus prosthesis and this prosthesis is consequently no longer seen in studies that are published after 2010.
In general, treatment of isolated patellofemoral OA is difficult in younger patients (i.e. <55 years). Due to the historically poor results of PFA, several surgeons have advocated to TKA over PFA in the setting of isolated patellofemoral OA [21, 43, 63, 69, 80]. However, TKA in this setting entails the replacement of two healthy tibiofemoral compartments, which is considered to be invasive [56, 58, 87] and is particularly problematic in the young population where TKA revision rates are higher when compared to older patients [28, 35, 62]. This bears consideration given that the number of primary and revision TKA is projected to increase between 2005 and 2030 in the USA by 673 and 601 %, respectively [52]. When taking these findings into account along with the fact that younger patients have more years to live, these patients are at higher risk of multiple revision surgeries with subsequent rehabilitations and risk of infections [83]. Therefore, replacing only the patellofemoral compartment could delay the replacement of all compartments or even make this procedure redundant. The findings in this study showed that at 10-year follow-up, 83.3 % of the patients retain their PFA and that on average 82.7 % of these patients report good or excellent knee function. This suggests that 69 % of patients undergoing PFA have good or excellent function and could theoretically postpone the need for TKA by 10 years. Furthermore, PFA survivorship is likely to be higher due to second-generation prostheses and improved patient selection. Inevitable OA progression in the tibiofemoral components may occur in some patients, requiring revision to TKA, but in other patients, the need for TKA can be postponed by several years. PFA may even serve as a permanent solution in the absence of OA progression. Furthermore, several studies have shown that good results can be achieved with PFA to PFA revision [36, 49] and PFA to TKA revision, if necessary [59, 97]. We agree therefore with several authors that state PFA can be a useful technique for treating isolated patellofemoral OA in younger patients or can be utilized as a bridging technique for future TKA if OA progression occurs [29, 55, 57]. However, future comparative clinical studies are necessary to assess the exact role of PFA in the setting of isolated patellofemoral OA, especially in the young patient [76].
Several limitations are present in this study. Firstly, long-term survivorship in this study is probably underestimated as a consequence of including data from both first- and second-generation prostheses [14, 27]. However, long-term survivorship was only available from first-generation prostheses. It was aimed to counter this phenomenon by reporting the annual revision rate in studies published before and since 2010 because this corrects for follow-up length. Secondly, heterogeneity in surgical technique could influence the results. Thirdly, a possible publication bias exists in this study. Non-English articles were included to minimize publication bias, but this possibility cannot be excluded.
This study provides an overview of the functional outcomes and survivorship of PFA in the setting of isolated patellofemoral OA. The data suggest that PFA could be a fairly good treatment option for patients with isolated patellofemoral OA. Therefore, a surgeon might consider PFA as a treatment over TKA in young patients with isolated patellofemoral OA.
Conclusion
This systematic review showed that outcomes of PFA for isolated patellofemoral OA were fairly good with 5-, 10-, 15- and 20-year survivorships of 91.7, 83.3, 74.9 and 66.6 %, respectively, and overall functional outcomes of 82 %. Furthermore, it was shown that the more recently published studies reported lower revision rates when compared to prior studies.
References
Ackroyd CE, Chir B (2005) Development and early results of a new patellofemoral arthroplasty. Clin Orthop Relat Res 436:7–13
Akhbari P, Malak T, Dawson-Bowling S, East D, Miles K, Butler-Manuel PA (2015) The Avon patellofemoral joint replacement: mid-term prospective results from an independent centre. Clin Orthop Surg 7(2):171–176
Al-Hadithy N, Patel R, Navadgi B, Deo S, Hollinghurst D, Satish V (2014) Mid-term results of the FPV patellofemoral joint replacement. Knee 21(1):138–141
Annual Report 2014 Australian Hip and Knee Arthroplasty Register (2014). https://aoanjrr.dmac.adelaide.edu.au/documents/10180/172286/AnnualReport2014
Arciero RA, Toomey HE (1988) Patellofemoral arthroplasty. A three- to nine-year follow-up study. Clin Orthop Relat Res 236:60–71
Argenson JN, Flecher X, Parratte S, Aubaniac JM (2005) Patellofemoral arthroplasty: an update. Clin Orthop Relat Res 440:50–53
Argenson JN, Guillaume JM, Aubaniac JM (1995) Is there a place for patellofemoral arthroplasty? Clin Orthop Relat Res 321:162–167
Arnbjornsson AH, Ryd L (1998) The use of isolated patellar prostheses in Sweden 1977–1986. Int Orthop 22(3):141–144
Baker PN, Refaie R, Gregg P, Deehan D (2012) Revision following patello-femoral arthoplasty. Knee Surg Sports Traumatol Arthrosc 20(10):2047–2053
Beitzel K, Schottle PB, Cotic M, Dharmesh V, Imhoff AB (2013) Prospective clinical and radiological two-year results after patellofemoral arthroplasty using an implant with an asymmetric trochlea design. Knee Surg Sports Traumatol Arthrosc 21(2):332–339
Benazzo F, Rossi SM, Ghiara M (2014) Partial knee arthroplasty: patellofemoral arthroplasty and combined unicompartmental and patellofemoral arthroplasty implants–general considerations and indications, technique and clinical experience. Knee 21(Suppl 1):S43–S46
Blazina ME, Fox JM, Del Pizzo W, Broukhim B, Ivey FM (1979) Patellofemoral replacement. Clin Orthop Relat Res 144:98–102
Board TN, Mahmood A, Ryan WG, Banks AJ (2004) The Lubinus patellofemoral arthroplasty: a series of 17 cases. Arch Orthop Trauma Surg 124(5):285–287
Borus T, Brilhault J, Confalonieri N, Johnson D, Thienpont E (2014) Patellofemoral joint replacement, an evolving concept. Knee 21(Suppl 1):S47–S50
Butler JE, Shannon R (2009) Patellofemoral arthroplasty with a custom-fit femoral prosthesis. Orthopedics 32(2):81
Cartier P, Sanouiller JL, Khefacha A (2005) Long-term results with the first patellofemoral prosthesis. Clin Orthop Relat Res 436:47–54
Charalambous CP, Abiddin Z, Mills SP, Rogers S, Sutton P, Parkinson R (2011) The low contact stress patellofemoral replacement: high early failure rate. J Bone Joint Surg Br 93(4):484–489
Cossey AJ, Spriggins AJ (2006) Computer-assisted patellofemoral arthroplasty: a mechanism for optimizing rotation. J Arthroplasty 21(3):420–427
Dahm DL, Al-Rayashi W, Dajani K, Shah JP, Levy BA, Stuart MJ (2010) Patellofemoral arthroplasty versus total knee arthroplasty in patients with isolated patellofemoral osteoarthritis. Am J Orthop (Belle Mead NJ) 39(10):487–491
Dahm DL, Kalisvaart MM, Stuart MJ, Slettedahl SW (2014) Patellofemoral arthroplasty: outcomes and factors associated with early progression of tibiofemoral arthritis. Knee Surg Sports Traumatol Arthrosc 22(10):2554–2559
Dalury DF (2005) Total knee replacement for patellofemoral disease. J Knee Surg 18(4):274–277
Davies AP (2013) High early revision rate with the FPV patello-femoral unicompartmental arthroplasty. Knee 20(6):482–484
Davies AP, Vince AS, Shepstone L, Donell ST, Glasgow MM (2002) The radiologic prevalence of patellofemoral osteoarthritis. Clin Orthop Relat Res 402:206–212
De Cloedt P, Legaye J, Lokietek W (1999) Femoro-patellar prosthesis. A retrospective study of 45 consecutive cases with a follow-up of 3–12 years. Acta Orthop Belg 65(2):170–175
de Winter WE, Feith R, van Loon CJ (2001) The Richards type II patellofemoral arthroplasty: 26 cases followed for 1-20 years. Acta Orthop Scand 72(5):487–490
Duncan RC, Hay EM, Saklatvala J, Croft PR (2006) Prevalence of radiographic osteoarthritis—it all depends on your point of view. Rheumatology (Oxford) 45(6):757–760
Dy CJ, Franco N, Ma Y, Mazumdar M, McCarthy MM, Gonzalez Della Valle A (2012) Complications after patello-femoral versus total knee replacement in the treatment of isolated patello-femoral osteoarthritis. A meta-analysis. Knee Surg Sports Traumatol Arthrosc 20(11):2174–2190
Dy CJ, Marx RG, Bozic KJ, Pan TJ, Padgett DE, Lyman S (2014) Risk factors for revision within 10 years of total knee arthroplasty. Clin Orthop Relat Res 472(4):1198–1207
Farr J 2nd, Barrett D (2008) Optimizing patellofemoral arthroplasty. Knee 15(5):339–347
Feucht MJ, Cotic M, Beitzel K, Baldini JF, Meidinger G, Schottle PB, Imhoff AB (2015) A matched-pair comparison of inlay and onlay trochlear designs for patellofemoral arthroplasty: no differences in clinical outcome but less progression of osteoarthritis with inlay designs. Knee Surg Sports Traumatol Arthrosc. doi:10.1007/s00167-015-3733-2
Fink B, Schwenninger C (2014) Arthroplasty of the femoropatellar joint—what data are available? Z Orthop Unfall 152(2):182–187
Gadeyne S, Besse JL, Galand-Desme S, Lerat JL, Moyen B (2008) Results of self-centering patellofemoral prosthesis: a retrospective study of 57 implants. Rev Chir Orthop Reparatrice Appar Mot 94(3):228–240
Gao X, Xu ZJ, He RX, Yan SG, Wu LD (2010) A preliminary report of patellofemoral arthroplasty in isolated patellofemoral arthritis. Chin Med J (Engl) 123(21):3020–3023
Goh GS, Liow MH, Tay DK, Lo NN, Yeo SJ (2015) Four-year follow up outcome study of patellofemoral arthroplasty at a single institution. J Arthroplasty 30(6):959–963
Harrysson OL, Robertsson O, Nayfeh JF (2004) Higher cumulative revision rate of knee arthroplasties in younger patients with osteoarthritis. Clin Orthop Relat Res 421:162–168
Hendrix MR, Ackroyd CE, Lonner JH (2008) Revision patellofemoral arthroplasty: three- to seven-year follow-up. J Arthroplasty 23(7):977–983
Hernigou P, Caton J (2014) Design, operative technique and ten-year results of the Hermes patellofemoral arthroplasty. Int Orthop 38(2):437–442
Hernigou P, Flouzat-Lachaniette CH, Delblond W, Duffiet P, Julian D (2013) Computer-assisted navigation in patellofemoral arthroplasty: a new technique to improve rotational position of the trochlea. HSS J 9(2):118–122
Hofmann AA, McCandless JB, Shaeffer JF, Magee TH (2013) Patellofemoral replacement: the third compartment. Bone Joint J 95-B(11 Suppl A):124–128
Hoogervorst P, de Jong RJ, Hannink G, van Kampen A (2015) A 21% conversion rate to total knee arthroplasty of a first-generation patellofemoral prosthesis at a mean follow-up of 9.7 years. Int Orthop 39(9):1857–1864
Hopley CD, Dalury DF (2014) A systematic review of clinical outcomes and survivorship after total knee arthroplasty with a contemporary modular knee system. J Arthroplasty 29(7):1398–1411
Huten D (2013) Femorotibial bone loss during revision total knee arthroplasty. Orthop Traumatol Surg Res 99(1 Suppl):S22–S33
Hutt J, Dodd M, Bourke H, Bell J (2013) Outcomes of total knee replacement after patellofemoral arthroplasty. J Knee Surg 26(4):219–223
Insall J, Tria AJ, Aglietti P (1980) Resurfacing of the patella. J Bone Joint Surg Am 62(6):933–936
Jørgensen PS, Konradsen LAG, Mati WB, Tørholm C (2007) Treatment of patellofemoral arthritis with patello-femoral arthroplasties. Ugeskr Laeger 169(23):2201–2204
Kaplan EL, Meier P (1958) Nonparametric estimation from incomplete observations. J Am Stat Assoc 53(282):457–481
King AH, Engasser WM, Sousa PL, Arendt EA, Dahm DL (2015) Patellar Fracture Following Patellofemoral Arthroplasty. J Arthroplasty 30(7):1203–1206
Koh IJ, Cho WS, Choi NY, Kim TK, Kleos Korea Research G (2014) Causes, risk factors, and trends in failures after TKA in Korea over the past 5 years: a multicenter study. Clin Orthop Relat Res 472(1):316–326
Koh JSB, Yeo SJ, Lo NN, Tan SK, Tay BK, Seow KH (2004) Isolated patellar revisions for failed metal-backed components: 2- to 9-year follow-up. J Arthroplasty 19(7):880–886
Kooijman HJ, Driessen AP, van Horn JR (2003) Long-term results of patellofemoral arthroplasty. A report of 56 arthroplasties with 17 years of follow-up. J Bone Joint Surg Br 85(6):836–840
Krajca-Radcliffe JB, Coker TP (1996) Patellofemoral arthroplasty. A 2- to 18-year followup study. Clin Orthop Relat Res 330:143–151
Kurtz S, Ong K, Lau E, Mowat F, Halpern M (2007) Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am 89(4):780–785
Labek G, Sekyra K, Pawelka W, Janda W, Stockl B (2011) Outcome and reproducibility of data concerning the Oxford unicompartmental knee arthroplasty: a structured literature review including arthroplasty registry data. Acta Orthop 82(2):131–135
Laskin RS, van Steijn M (1999) Total knee replacement for patients with patellofemoral arthritis. Clin Orthop Relat Res 367:89–95
Leadbetter WB, Kolisek FR, Levitt RL, Brooker AF, Zietz P, Marker DR, Bonutti PM, Mont MA (2009) Patellofemoral arthroplasty: a multi-centre study with minimum 2-year follow-up. Int Orthop 33(6):1597–1601
Leadbetter WB, Ragland PS, Mont MA (2005) The appropriate use of patellofemoral arthroplasty: an analysis of reported indications, contraindications, and failures. Clin Orthop Relat Res 436:91–99
Liow MH, Goh GS, Tay DK, Chia SL, Lo NN, Yeo SJ (2015) Obesity and the absence of trochlear dysplasia increase the risk of revision in patellofemoral arthroplasty. Knee. doi:10.1016/j.knee.2015.05.009
Lonner JH (2004) Patellofemoral arthroplasty: pros, cons, and design considerations. Clin Orthop Relat Res 428:158–165
Lonner JH, Jasko JG, Booth RE Jr (2006) Revision of a failed patellofemoral arthroplasty to a total knee arthroplasty. J Bone Joint Surg Am 88(11):2337–2342
Lubinus HH (1979) Patella glide bearing total replacement. Orthopedics 2(2):119–127
McAlindon TE, Snow S, Cooper C, Dieppe PA (1992) Radiographic patterns of osteoarthritis of the knee joint in the community: the importance of the patellofemoral joint. Ann Rheum Dis 51(7):844–849
McCalden RW, Robert CE, Howard JL, Naudie DD, McAuley JP, MacDonald SJ (2013) Comparison of outcomes and survivorship between patients of different age groups following TKA. J Arthroplasty 28(8 Suppl):83–86
Merchant AC (2004) Early results with a total patellofemoral joint replacement arthroplasty prosthesis. J Arthroplasty 19(7):829–836
Merchant AC (2005) A modular prosthesis for patellofemoral arthroplasty: design and initial results. Clin Orthop Relat Res 436:40–46
Mertl P, Van FT, Bonhomme P, Vives P (1997) Femoropatellar osteoarthritis treated by prosthesis. Retrospective study of 50 implants. Rev Chir Orthop Reparatrice Appar Mot 83(8):712–718
Mofidi A, Bajada S, Holt MD, Davies AP (2012) Functional relevance of patellofemoral thickness before and after unicompartmental patellofemoral replacement. Knee 19(3):180–184
Mohammed R, Jimulia T, Durve K, Bansal M, Green M, Learmonth D (2008) Medium-term results of patellofemoral joint arthroplasty. Acta Orthop Belg 74(4):472–477
Monk AP, van Duren BH, Pandit H, Shakespeare D, Murray DW, Gill HS (2012) In vivo sagittal plane kinematics of the FPV patellofemoral replacement. Knee Surg Sports Traumatol Arthrosc 20(6):1104–1109
Mont MA, Haas S, Mullick T, Hungerford DS (2002) Total knee arthroplasty for patellofemoral arthritis. J Bone Joint Surg Am 84-A(11):1977–1981
Mont MA, Johnson AJ, Naziri Q, Kolisek FR, Leadbetter WB (2012) Patellofemoral arthroplasty: 7-year mean follow-up. J Arthroplasty 27(3):358–361
Morris MJ, Lombardi AV Jr, Berend KR, Hurst JM, Adams JB (2013) Clinical results of patellofemoral arthroplasty. J Arthroplasty 28(9 Suppl):199–201
The New Zealand Joint Registry (2014) Fifteen year report. January 1999 to December 2013. http://www.nzoa.org.nz/system/files/NZJR2014Report.pdf
Nicol SG, Loveridge JM, Weale AE, Ackroyd CE, Newman JH (2006) Arthritis progression after patellofemoral joint replacement. Knee 13(4):290–295
Obremskey WT, Pappas N, Attallah-Wasif E, Tornetta P III, Bhandari M (2005) Level of evidence in orthopaedic journals. J Bone Joint Surg Am 87(12):2632–2638
Odumenya M, Costa ML, Parsons N, Achten J, Dhillon M, Krikler SJ (2010) The Avon patellofemoral joint replacement: five-year results from an independent centre. J Bone Joint Surg Br 92(1):56–60
Odumenya M, McGuinness K, Achten J, Parsons N, Spalding T, Costa M (2011) The Warwick patellofemoral arthroplasty trial: a randomised clinical trial of total knee arthroplasty versus patellofemoral arthroplasty in patients with severe arthritis of the patellofemoral joint. BMC Musculoskelet Disord 12:265
Pabinger C, Berghold A, Boehler N, Labek G (2013) Revision rates after knee replacement. Cumulative results from worldwide clinical studies versus joint registers. Osteoarthritis Cartilage 21(2):263–268
Pabinger C, Lumenta DB, Cupak D, Berghold A, Boehler N, Labek G (2015) Quality of outcome data in knee arthroplasty: comparison of registry data and worldwide non-registry studies from 4 decades. Acta Orthop 86(1):58–62
Parratte S, Ollivier M, Lunebourg A, Abdel MP, Argenson JN (2015) Long-term results of compartmental arthroplasties of the knee: long term results of partial knee arthroplasty. Bone Joint J 97-B(10 Suppl A):9–15
Parvizi J, Stuart MJ, Pagnano MW, Hanssen AD (2001) Total knee arthroplasty in patients with isolated patellofemoral arthritis. Clin Orthop Relat Res 392:147–152
Patel A, Pavlou G, Mujica-Mota RE, Toms AD (2015) The epidemiology of revision total knee and hip arthroplasty in England and Wales: a comparative analysis with projections for the United States. A study using the National Joint Registry dataset. Bone Joint J 97-B(8):1076–1081
Pedersen D (1986) Femoropatellar endoprosthesis. Blazina type II method in 11 patients. Ugeskr Laeger 148(29):1825–1827
Pugely AJ, Martin CT, Gao Y, Schweizer ML, Callaghan JJ (2015) The incidence of and risk factors for 30-day surgical site infections following primary and revision total joint arthroplasty. J Arthroplasty 30(9 Suppl):47–50
Sarda PK, Shetty A, Maheswaran SS (2011) Medium term results of Avon patellofemoral joint replacement. Indian J Orthop 45(5):439–444
Scott RD (1979) Prosthetic replacement of the patellofemoral joint. Orthop Clin North Am 10(1):129–137
Sierra RJ, Kassel CA, Wetters NG, Berend KR, Della Valle CJ, Lombardi AV (2013) Revision of unicompartmental arthroplasty to total knee arthroplasty: not always a slam dunk! J Arthroplasty 28(8 Suppl):128–132
Sisto DJ (1994) Patellofemoral degenerative joint disease. In: Fu FH, Harner CD, Vince K (eds) Knee Surgery. Williams and Wilkins, Baltimore, pp 1203–1221
Sisto DJ, Sarin VK (2006) Custom patellofemoral arthroplasty of the knee. J Bone Joint Surg Am 88(7):1475–1480
Smith AM, Peckett WR, Butler-Manuel PA, Venu KM, d’Arcy JC (2002) Treatment of patello-femoral arthritis using the Lubinus patello-femoral arthroplasty: a retrospective review. Knee 9(1):27–30
Starks I, Roberts S, White SH (2009) The Avon patellofemoral joint replacement: independent assessment of early functional outcomes. J Bone Joint Surg Br 91(12):1579–1582
Stefanik JJ, Niu J, Gross KD, Roemer FW, Guermazi A, Felson DT (2013) Using magnetic resonance imaging to determine the compartmental prevalence of knee joint structural damage. Osteoarthritis Cartilage 21(5):695–699
Tauro B, Ackroyd CE, Newman JH, Shah NA (2001) The Lubinus patellofemoral arthroplasty. A five- to ten-year prospective study. J Bone Joint Surg Br 83(5):696–701
Thienpont E, Opsomer G, Koninckx A, Houssiau F (2014) Joint awareness in different types of knee arthroplasty evaluated with the forgotten joint score. J Arthroplasty 29(1):48–51
Turktas U, Piskin A, Poehling GG (2015) Short-term outcomes of robotically assisted patello-femoral arthroplasty. Int Orthop. doi:10.1007/s00264-015-2786-7
Utukuri MM, Khanduja V, Somayaji HS, Dowd GS (2008) Patient-based outcomes in patellofemoral arthroplasty. J Knee Surg 21(4):269–274
van Jonbergen HP, Werkman DM, Barnaart LF, van Kampen A (2010) Long-term outcomes of patellofemoral arthroplasty. J Arthroplasty 25(7):1066–1071
van Jonbergen HP, Werkman DM, van Kampen A (2009) Conversion of patellofemoral arthroplasty to total knee arthroplasty: a matched case–control study of 13 patients. Acta Orthop 80(1):62–66
van Wagenberg JM, Speigner B, Gosens T, de Waal Malefijt J (2009) Midterm clinical results of the Autocentric II patellofemoral prosthesis. Int Orthop 33(6):1603–1608
Williams DP, Pandit HG, Athanasou NA, Murray DW, Gibbons CL (2013) Early revisions of the Femoro-Patella Vialla joint replacement. Bone Joint J 95-B(6):793–797
Worrell RV (1986) Resurfacing of the patella in young patients. Orthop Clin North Am 17(2):303–309
Wright JG, Swiontkowski MF, Heckman JD (2003) Introducing levels of evidence to the journal. J Bone Joint Surg Am 85-A(1):1–3
Yadav B, Shaw D, Radcliffe G, Dachepalli S, Kluge W (2012) Mobile-bearing, congruent patellofemoral prosthesis: short-term results. J Orthop Surg (Hong Kong) 20(3):348–352
Zhang J, Ye QB, Qiu GX, Wang YP (2002) Patellofemoral replacement for severe patellofemoral osteoarthritis: a 2–10 years follow-up study. Zhongguo Yi Xue Ke Xue Yuan Xue Bao 24(2):174–177
Zhang Q, Guo W, Liu Z, Cheng L, Yue D, Wang W, Zhang N, Shi Z (2014) Treatment of patellofemoral osteoarthritis with patello-femoral joint arthroplasty. Zhonghua Wai Ke Za Zhi 52(5):361–365
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
van der List, J.P., Chawla, H., Zuiderbaan, H.A. et al. Survivorship and functional outcomes of patellofemoral arthroplasty: a systematic review. Knee Surg Sports Traumatol Arthrosc 25, 2622–2631 (2017). https://doi.org/10.1007/s00167-015-3878-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-015-3878-z