Abstract
Posterior shoulder dislocation with humeral head impression fracture is rare and its early diagnosis and treatment remain a challenge for the orthopaedic surgeon. Although literature describes several surgical options, most are based on the detachment of the subscapularis or on more complex techniques that change the humeral joint anatomy even more. This report describes a new operative technique that is only slightly invasive, where the depressed chondral surface is raised to regain a normal articular contour. The chondral surface is supported by an interference biabsorbable screw and the insertion of the subscapularis tendon is left intact. Two male patients with an acute shoulder posterior dislocation associated with anteromedial impression fracture of about 40 and 50%, respectively, of the articular humeral shape were treated in our department. The average follow-up was 26 months where plain X-ray and CT scan showed an anatomical humeral surface free from signs of arthritis or necrosis. Functional results were excellent in both cases. This new technique is easy, less invasive than others and ensures a stable cartilage and subchondral support without the use of grafts.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Acute shoulder posterior dislocation is a rare and often misdiagnosed trauma [7, 9]. Many surgical solutions have been proposed for cases of acute impression defect that involve 20–50% of the articular surface of the humerus [1–4, 6, 8, 11]. Most of these implicate the subscapularis detachment or other changes in the shoulder joint anatomy.
We defined a new “trouble-free” anatomical surgical technique, without the detachment of subscapularis tendon, which is done through a cortical window on the opposite side of the impression fracture. The indications for this surgical approach are a recent lesion (within 3–4 weeks), impacted osteochondral tissue without major free fragments, an involvement of less than 50% of the articular surface of the humerus. Two cases were herein described.
Case reports
Two male patients, aged 60 (Case 1) and 41 (Case 2), respectively, presented to our Emergency Department with a diagnosis of acute shoulder posterior dislocation associated with head impression fracture (McLaughlin lesion), between 1999 and 2002.
The patients’ right shoulders (dominant) had been affected in both cases. One patient (Case 1) had a high-energy car crash but the trauma mechanism was not defined, whilst the other patient (Case 2) had tripped and fallen on his outstretched arm.
Both patients reported pain symptoms and inability to move their upper extremity. On physical examination there was a slight passive motion but no active motion, with no peripheral neurovascular deficits.
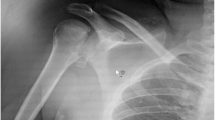
Standard shoulder radiograph (anteroposterior), performed in both cases, showed posterior shoulder dislocation with a McLaughlin lesion without major osteochondral fragments. Although closed reduction was done at once in the acute phase, the shoulder dislocated as soon as the arm reached more than 30°–35° of internal rotation at forward flexion and 40°–45° in the anatomical position. The articular injury and the extension of the lesion were confirmed by computer tomographic (CT) scans where an articular surface defect of 40% was observed in Case 1 and 50% in Case 2 (Fig. 1a).
a Preoperative CT scan of a posterior dislocation of the shoulder with an impression fracture of the humeral head used for the determination and classification of the size of the defect; the impression defect, in this case, involved about 40% of the humeral head and b CT scan, at 26 months postsurgery, showing good anatomical reduction
Clinical, radiographic (anteroposterior and axillary radiographs) and CT scan evaluations were performed postoperatively, at 3 months and the last follow-up examination, respectively (an average of 26 months).
Clinical examination was evaluated using both Constant score [5] and Simple Shoulder Test (SST) [12] while the Samilson classification system [14] was used for the evaluation of osteoarthritis.
Surgical technique
The procedure was performed with the patient under general anaesthesia, in the beach chair position.
An anterior deltopectoral standard approach was used. The cephalic vein and the deltoid were retracted laterally and the pectoralis major medially, splitting the two muscles apart. The subacromialis bursa was removed and the rotator cuff interval opened. The visualisation of the fracture was obtained by opening the rotator interval without detaching the subscapularis tendon from the lesser tuberosity. The haematoma and fracture debris were removed, to allow for a precise assessment of the lesion and to evaluate the size and position of the humeral head fracture.
The next step was the creation of a little cortical window (of about 10 mm×10 mm) 2 cm distal from the greater tuberosity apex and 2 cm lateral to the long head of the biceps sulcum (Fig. 2). We adopted the instrument used for the treatment of tibial plateau fractures to reduce the depression, i.e. a hollow trephine cutter to create a bone carrot and a bone tapper that allows optimal running into the hollow trephine (10 mm diameter).
We performed the reduction procedure through the cortical window we had created, using the bone tapper; moving from the cortical window to the impression fracture we obtained a bone carrot using the hollow trephine cutter, in a oblique direction. This “carrot” was pushed into the back of the impression fracture by the bone tapper to reduce the defect (Fig. 3a, b). The anatomical reduction was evaluated, throughout the procedure, step by step, through the open rotator cuff. Finally, once the head surface had been adequately reduced, it was definitively secured with an interference biabsorbable screw (biabsorbable interference screw, 10×30 mm2, Centerpulse-Zimmer) (Fig. 4), screwed through the window perpendicularly in the opposite direction to the depression. The last step, when turning the screw, was to screw the thread not only in the tunnel but also into the compacted cancellous bone itself. The window was then covered using a press fit procedure, with the cortical bone that had been previously removed. The posterior capsule was not surgically addressed.
A shoulder brace was applied to hold the shoulder in 20° of external rotation, 10° abduction and 10° extension.
At 2 weeks postsurgery the patients began pendulum exercises and passive-assisted motion. At 5 weeks the brace was removed and full active and passive motion was allowed.
Results
At an average of 26 months (range 24–28 months) postoperative follow-up, the radiographic evaluation and CT scan showed no signs of osteoarthritis or necrosis (Fig. 1b). Constant score was 90 in Case 1 and 95 in Case 2; SST was 10 in Case 1 and 11 in Case 2. No decrease in internal rotation was observed. Patients reached T9 level during internal rotation bilaterally.
Discussion
The treatment of posterior shoulder dislocation with humeral head impression fracture is difficult. Many surgical options have been described in literature with different functional and radiographical results [1–4, 6, 8, 10, 11].
The transfer of the subscapularis tendon with lesser tuberosity is still the goal standard, even if this procedure may limit internal rotation and complicate future prosthetic reconstruction [1, 6, 7]. The restoration of the humeral surface by means of local allograft or autograft [7, 13] is more anatomical but has some critical points: the cost of allograft tissue and patient hesitance in acceptance of it; the instability of the elevated subchondral bone filled with autograft that is prone to collapse; the morbidity associated with the harvesting of the autograft. Therefore, we tried to solve these problems using this new surgical technique.
The advantages of it are that the subscapularis tendon is not detached and has a more complete and faster functional recovery, with no deficit of internal rotation. On the other hand, the use of an interference biabsorbable screw that is screwed and fixed into the cancellous bone represents a strong structural support, thus avoiding the use of grafts and the collapse of the surface. The screwing of the screw progressively into the compacted cancellous bone, moreover, allows a safety expansion of the just compacted cancellous bone tissue. This step determines a well-controlled reduction that can be considered an indirect reduction, avoiding an over-correction of the fracture, besides fixing strongly the screw.
In the two cases treated, the opening of the rotator interval cuff was enough to evaluate the depression fracture of the articular surface and to control the reduction obtained. Should the visualization not be sufficient, the surgeon could extend the interval split more medially; however, detaching the proximal subscapularis tendon from the lesser tuberosity should be the surgeon’s last choice as it will have a negative impact on the patient’s recovery time. The integrity of the subscapularis is very important for the postoperative management and rehabilitation.
The shoulder is positioned in neutral flexion, 10° abduction and 20° external rotation, with the elbow flexed to 90°, the so-called safe position: this avoids a direct contact between the fracture zone and the glenoid.
The indication for this surgical approach is a recent lesion (assessed within 3–4 weeks) with impacted cartilage, not destroyed, involving up to 50% of the articular surface of the humerus.
Moreover, an adequate humeral bone stock and a young, active patient increase the chances of a successful procedure.
Absolute contraindications are: patient aged over 70 years with osteoporotic bone and multifragment fractures of the humeral head or chronic posterior dislocation. A relative contraindication is a very large articular surface defect (more than 50–60%).
In conclusion, this technique allows an accurate and anatomical reduction, without using fluoroscopy, grafts or altering the subscapularis tendon in any way.
References
Checchia SL, Santos PD, Miyazaki AN (1998) Surgical treatment of acute and chronic posterior fracture dislocation of the shoulder. J Shoulder Elbow Surg 7:53–65
Cheng SL, Mackay MB, Richards RR (1997) The treatment of locked posterior fracture-dislocation of the shoulder by total shoulder by total shoulder arthroplasty. J Shoulder Elbow Surg 6:11–17
Cicak N (2004) Posterior dislocation of the shoulder. J Bone Joint Surg [Br] 86-B:324–32
Connor PM, Boatright RJ, D’Alessandro DF (1997) Posterior fracture-dislocation of the shoulder: treatment with acute osteochondral grafting. J Shoulder Elbow Surg 6:480–485
Constant CR, Murley AHG (1987) A clinical method of functional assessment of the shoulder. Clin Orthop 214:160–164
Finkelstein JA, Waddell JP, O’Driscoll SW, Vincent G (1995) Acute posterior fracture dislocation of the shoulder treated with the Neer modification of the McLaughlin procedure. J Orthop Trauma 3:190–193
Gerber C (1997) Chronic, locked anterior and posterior dislocation. In: Warner JJP, Ianotti JP, Gerber C (eds) Complex and revision problems in shoulder surgery. Lippincott-Raven, Philadelphia, pp 99–113
Gerber C, Lambert SM (1996) Allograft reconstruction of segmental defects of the humeral head for the treatment of chronic locked posterior dislocation of the shoulder. J Bone Joint Surg [Am] 78-A:376–382
Hawkins RJ, Neer CS 2nd, Pianta RM, Mendoza FX (1987) Locked posterior dislocation of the shoulder. J Bone Joint Surg [Am] 69-A:9–18
Heller KD, Forst J, Forst R (1995) Different therapy of traumatically-induced persistent posterior shoulder dislocation: review of the literature. Unfallchirurg 98:6–12
Keppler P, Holz U, Thielemann FW, Meinig R (1994) Locked posterior dislocation of the shoulder: treatment using rotational osteotomy of the humerus. J Orthop Trauma 8:286–292
Lippitt SB, Harryman DT, Matsen FA (1992) A practical tool for evaluating function: the simple shoulder test. In: Matsen FA, Fu FH, Hawkins RJ (eds) The shoulder: a balance of mobility and stability. American Academy of Orthopaedic Surgeons, Rosemont, pp 501–518
Randelli M, Gambrioli PL (2001) Chronic posterior dislocation of the shoulder. In: Duparc J (ed) Surgical technique in orthopaedics and traumatology. Elsevier, Paris, pp 55-190-B-10
Samilson RL, Prieto V (1983) Dislocation arthropathy of the shoulder. J Bone Joint Surg [Am] 65-A:456–460
Acknowledgments
The authors would like to thank the following people for the critical and specialist support: for editing and reviewing Mr. Fabrizio Napolitano, MBA, and for the line drawings Anna Casalone.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Assom, M., Castoldi, F., Rossi, R. et al. Humeral head impression fracture in acute posterior shoulder dislocation: new surgical technique. Knee Surg Sports Traumatol Arthr 14, 668–672 (2006). https://doi.org/10.1007/s00167-005-0001-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-005-0001-x