Abstract
Objective
Analysis of infectious complications and risk factors in percutaneous central venous catheters.
Design
One-year observational, prospective, multicenter study (1998–1999).
Setting
Twenty Spanish pediatric intensive care units.
Patients
Eight hundred thirty-two children aged 0–14 years.
Intervention
None.
Measurements and main results
One thousand ninety-two catheters were analyzed. Seventy-four (6.81%) catheter-related bloodstream infections (CRBSI) were found. The CRBSI rate was 6.4 per 1,000 CVC days (95% CI 5.0–8.0). Risk factors for CRBSI were weight under 8 kg (p < 0.001), cardiac failure (RR 2.69; 95% CI 1.95–4.38; p < 0.001), cancer (RR 1.66; 95% CI 0.97–2.78; p = 0.05), silicone catheters (RR 2.82; 95% CI 1.49–5.35; p = 0.006), guidewire exchange catheterization (p = 0.002), obstructed catheters (RR 2.67; 95% CI 1.63–4.39; p < 0.001), and more than 12 days' indwelling time (RR 5.9; 95% CI 3.63–9.41; p < 0.001). Multivariate Cox regression identified lower patient weight (HR 2.4; 95% CI 1.11–5.19; p = 0.002), guidewire exchange catheterization (HR 2.2; 95% CI 1.07–4.54; p = 0.049) and more than 12 days' indwelling time (HR 1.97; 95% CI 0.89–4.36; p = 0.089) as significant independent predictors of CRBSI. Factors which protected against infection were the use of povidone–iodine on hubs (HR 0.42; 95% CI 0.19–0.96; p = 0.025) and porous versus impermeable dressing (HR 0.41; 95% CI 0.23–0.74; p = 0.004). Two children (0.24%) died from endocarditis following catheter-related sepsis due to Stenotrophomonas maltophilia in one case and P. aeruginosa in the other.
Conclusions
Catheter-related sepsis is associated with lower patient weight and more than 12 days' indwelling time, but not with the insertion site. Cleaning hubs with povidone–iodine protects from infection.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Central venous catheters (CVC) are widely used in pediatric intensive care units (PICUs). Although their insertion is relatively simple, they are not risk-free, and associated complications, especially infection, increase morbidity, mortality, hospital stay and healthcare costs [1, 2, 3]. The most frequent cause of nosocomial infection in American PICUs is sepsis, which, in 90% of cases, is related to intravascular devices [4]. A recent bibliographical review [5] and several published studies [6, 7, 8, 9, 10, 11, 12, 13, 14] analyze the complications of CVC in pediatric patients. The objective of our study was to analyze the infectious complications of percutaneous insertion of CVC, and the risk factors associated with infection. Our investigation, the only pediatric, multicenter, observational study covering a large number of patients, may help solve problems associated with CVC.
Methods
Ours was a one-year multicenter, prospective and observational study carried out in Spanish PICUs from April 1998 to March 1999. All PICUs in Spain were invited to participate. The study was approved by the ethics committee of each center and included patients aged 0–14 years.
CVC were inserted with the informed consent of child and/or tutors. Catheterization was performed in the PICU by a ward physician, fellow-in-training or both, using the Seldinger technique [15], under aseptic conditions (except in emergency situations). Heparin-bonded, antibiotic-impregnated, tunneled and umbilical catheters were excluded. The insertion site varied depending on the reason for catheterization, availability of vascular access, and physician preference. It was agreed that catheter care would be carried out according to the individual protocol of each PICU.
When catheter-related infection was suspected, the recommendation was to obtain both CVC and peripheral blood samples for culture; however, there was no standard procedure for location or number. Blood was cultured by qualitative technique using the Bactec pediatric system and germ-specific culture media. There were no standard recommendations on blood sample volume; this depended on culture media (aerobes 1–3 ml, anaerobes and fungi 3 ml, according to the manufacturer's recommendations) and patient weight.
When catheter was removed, the recommendation was to culture, if possible; the decision about when to remove an infected catheter was left to the clinician's judgment. Two culture techniques were used, depending on the hospital; if available, Maki's semiquantitative method [16] was used. Once the catheter was removed, the last 5 cm of it was rolled on a blood–agar plate and the number of colony-forming units (CFU) was counted after 48 h incubation. If that was not available, qualitative culture of the catheter segment was made by placing it in enrichment broth (thioglycolate) for 24–48 h before resowing it in blood–agar.
The data collection sheet was prepared and approved by a team of physicians composed of representatives of each PICU. All case-report forms were reviewed by the coordinating center. The following data were collected:
1. Patient data (age, weight, sex, underlying condition); indication for catheterization; reason for withdrawal; catheter (size, lumen, brand, material); person who inserted catheter; number of attempts, defined as number of punctures per line inserted; route of access; circumstances [emergency, scheduled, recatheterization (guidewire exchange), mechanical ventilation, sedoanalgesia]; complications during insertion; obstruction (partial: solution could be infused but no blood aspirated; total: impossible infusion and aspiration); presence of central venous thrombosis (CVT), diagnosed by clinical signs, contrast venography and/or ultrasound, whereby routine ultrasound evaluation was not performed. There were no standard recommendations for obstructed catheters.
2. Infectious complications arising from catheter maintenance:
a) Catheter care [use and type of stopcock and hub protection, number of three-way stopcocks, dressing (porous, impermeable), frequency of dressing change]; location of culture (tip, hub, skin, blood); type of microorganism cultured; culture technique; date of infection; therapy administered; outcome.
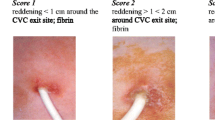
b) Type of infection, classified according to the guidelines of consensus of experts recently published [17], listed in Table 1.
3. Death of patient due to a catheter complication was recorded.
Statistical analysis
Qualitative variables are presented with their frequency distribution. Quantitative variables are summarized as the mean and standard deviation (SD) and/or median and interquartile range (IQR; P25–P75).
Association between qualitative variables was evaluated using the χ2 test, or Fisher's exact test if 25% or more cells had an expected count less than 5. Behavior of quantitative variables was analyzed by each of the response variables using the Student t-test.
Cox regression models were adjusted to identify and evaluate the relationship between the set of explicative variables and occurrence of an event. Models included independent variables whose significance (p) in the univariate analysis was below 0.10. Event-free survival was estimated using a Kaplan–Meier analysis.
Existence of interactions was evaluated by entering the multiplicative independent variables with statistical significance tests, and the model maintained the statistically significant terms of interaction. Adjusted relative risks (adjRR) are presented together with their 95% confidence intervals (CI). In all cases, distribution of variable was checked against the theoretical models and the variance homogeneity hypothesis was contrasted. In all hypothesis contrasts, null hypothesis was rejected with a type 1 error or α error below 0.05.
Data were processed using the SPSS database, version 12.
Results
During the study period, we collected 1092 catheters consecutively inserted in 835 pediatric patients whose ages ranged from 0 to 14 years (mean 3.85 ± 3.95, median 2, IQR 0.74–6 years); 27 children (3.2%) were less than 1 month old. There were 459 boys (55%) and 376 girls (45%). Patient weight ranged from 1 to 80 kg (mean 17.09 ± 13.51, median 12.5, IQR 7.5–22.5 kg).
Twenty PICUs from throughout Spain participated in the study.
Underlying diseases and indications leading to line insertion are shown in Table 2.
A total of 1041 catheters were made of polyurethane (95%) and 51 (5%) of silicone. The most common route of access was the femoral vein (54%) (Fig. 1). Insertion was carried out by a ward physician (49%), fellow-in-training (41%) or both (10%). Catheterization was scheduled in most cases (53%), an emergency procedure in 39.5% and guidewire exchanged in 6.2%. During the procedure, 531 patients (48.6%) were receiving mechanical ventilation. Systemic sedoanalgesia (85.7% of cases), local sedoanalgesia (17.3%) or both (91.5%) were used. There were 10 episodes of central venous thrombosis (1%) and 117 catheters were obstructed (10.7%), 82 partially and 35 totally.
Indwelling time ranged from 0.1 to 145 days (mean 10.81 ± 12.27 SD, median 7, IQR 4–12 days) and varied significantly according to the insertion site: 38% of subclavian lines remained in place for > 12 days compared with 17% of jugular lines and 24% of femoral lines (p < 0.001).
The catheter was withdrawn due to end of therapy in 637 cases (58.3%), complications in 154 (14.1%), death in 106 (9.7%), accidental removal in 91 (8.3%) and other causes in 90 cases (8.2%). This information was not recorded for 14 catheters as the patients were transferred to another center.
Infectious complications
Catheter-tip culture
We cultured 594 catheter tips (54% of the total), of which 167 (28%) were positive. Of these, 116 (20%) were colonized catheters (> 15 CFU) without sepsis and 51 positive tips (8%) were related to systemic infection. Thirty-two catheters were considered contaminated (< 15 CFU).
Blood culture
Blood cultures were obtained in 211 cases on at least one occasion. A blood culture was taken from the catheter in 206 cases (88 were positive), and in 95 the culture was peripheral (47 were positive); both blood cultures were taken in 90 cases.
Microorganisms found in catheter tips and in blood cultures are shown in Table 3.
Catheter-related bloodstream infections
Seventy-four CRBSIs (6.8% of the catheters, 8.8% of the patients) were found. The rate was 6.4 per 1,000 CVC days (95% CI 5–8). Definite CRBSI was present in 26 cases (2.4%), probable CRBSI in 10 (0.9%), and there was a possible CRBSI in 38 (3.5%). The causal agents of sepsis are shown in Table 3. Infection time ranged from 1 to 63 days (mean 16.77 ± 13.91 SD, median 14, IQR 7–20 days).
The results of univariate and multivariate analysis are shown in Tables 4 and 5 respectively. Figure 2 shows the cumulative survival rate of catheters that remained free of CRBSI for each of days 1–60.
Cumulative survival analysis of catheter duration. The probability of a catheter remaining free of catheter-related bloodstream infection decreases with time. At 4, 7 and 12 days after insertion (corresponding to p25, median and p75, respectively), 98.77%, 96.7% and 93.9% of catheters were infection-free, respectively. The median duration of CRBSI-free catheter survival was 60 days
Infection, obstruction and CVT
Infection was more frequent in obstructed catheters (15.4% vs 5.7%, p < 0.001; Table 4), but this was not confirmed in the multivariate analysis. CVT was more common in obstructed catheters (1.8% vs 0.8%), but the difference was not significant (p = 0.29).
Treatment, outcome and catheter-related deaths
Table 6 shows the outcome of infections in terms of catheter removal and etiological agent. The catheter was removed or changed in 58 cases: as soon as infection was suspected in 28, after 1–3 days in 17, and after more than 3 days in 13 cases. Three cases of CRBSI were treated by removing the catheter only, without antibiotic therapy; the remaining 71 (96%) received antibiotics (39 received one, 33 two or more). Four children (0.48%) presented endocarditis after CRBSI, three of them were diagnosed with heart disease.
Two children (0.24%), 4 and 19 months old, died from catheter-related complications. Both had undergone cardiac surgery, both developed endocarditis as a result of catheter-related sepsis, and one had superior cava thrombosis. The causal pathogens were Staphylococcus epidermidis and Stenotrophomonas maltophilia in one case and Pseudomonas aeruginosa in the other.
Discussion
We analyzed the infectious complications of 1092 CVC in 835 patients aged 0–14 years. Ours is one of the widest studies with these characteristics.
Mortality directly related to the catheter was 2.4/1,000 patients, but we did not analyze how complications affected mortality indirectly as this was not our objective.
The infection rate (definite, probable and possible CRBSI) in our series (6.4/1,000 catheter-days; 6.8%) is similar to that found by the National Nosocomial Infection Surveillance System from 1990 to 1999 [18] and from 1992 to 2003 [19], which, in 67 and 74 PICUs, respectively, found an infection rate of 7.9 and 7.6/1,000, respectively. Nevertheless, infection rates in adult ICU patients vary widely (from 2.9 to 9.7/1,000) according to the type of ICU [19]. The widely differing definitions of infection and culture methods in different studies mean that it is often difficult to compare infection rates [20]. Recently, an expert committee published the clinical definitions of definite, probable or possible CRBSI in infants and children, for the purpose of identifying infections for epidemiologic and surveillance reasons. They also recommended that only those patients fulfilling definite CRBSI criteria should be enrolled in clinical trials involving sepsis [17]. Our study classified CRBSI according to these new criteria, which facilitates the interpretation of our findings and their comparison with other data on CRBSI.
We cultured slightly over half the catheters because the design of the study involved culturing as many catheters as possible. However, a recent meta-analysis recommended culture only in the case of clinically suspected CRBSI [21]. The yield of different diagnostic techniques varies from one study to another; the above-mentioned meta-analysis (which included 51 selected papers) found that paired quantitative blood cultures of central and peripheral lines had the greatest specificity, followed by qualitative blood culture obtained from the catheter and the acridine orange stain test. The most accurate diagnostic methods involving withdrawal of the catheter were quantitative culture of the tip followed by semi-quantitative culture; qualitative culture of the tip had the highest sensitivity but very low specificity. Nevertheless, these results may vary in pediatric patients [17], as peripheral blood cultures are often difficult to obtain and catheters are not withdrawn for diagnostic purposes, due to the difficulty in inserting another. Therefore, techniques such as calculating the time differential of qualitative blood culture positivity between both lumina, or paired quantitative blood cultures of both lumina, or using a cut-off point of > 100 CFU/ml for the blood culture of a single lumen, could be useful in these patients [17]. Nevertheless, few hospitals routinely use quantitative blood culture techniques.
Some of the risk factors associated with CRBSI found in our study have been described elsewhere. These include an extended indwelling period, which is associated with a greater risk of infection [12, 14]. In our study, more than 12 catheter days meant a greater incidence of infection. Stenzel et al. [10] found no association between infection and indwelling time.
Routine changing of CVC does not reduce the rate of infection [22], and some studies have even shown that the number of infections increases when the change is made by guidewire [20, 22]. Current AAP guidelines on the prevention of CRBSI and a meta-analysis [23] recommend not changing catheters on a routine basis in order to prevent infection. If it is necessary to change the line and catheter-related infection is suspected, a new insertion site should be chosen, except in patients with very limited vascular access sites (e.g. small children), in whom change should be accompanied by antibiotherapy. When no infection is suspected, change may be performed using a guidewire. The results of our study support this recommendation, since CRBSI are more frequent in catheters changed by guidewire. However, the reason for changing our catheters (infection or other) was unknown, as these data were not collected in the protocol. Prophylactic change by guidewire or at a new site is common practice in burn patients [8], an exception which is not considered in the current AAP guidelines for prevention of CRBSI [20].
According to the literature [24], the most frequent path of infection for short-term CVC is the extraluminal route (45%), due to migration of cutaneous flora across the skin surrounding the catheter. Endoluminal colonization is produced by the entry of pathogens via the external hubs during frequent handling or via the infusion of contaminated liquids (26%), this being more serious in long-term catheters [24]. We found fewer infections in catheters whose hubs and three-way stopcocks were protected by povidone–iodine when they are handled. This fact indirectly demonstrates the importance of endoluminal contamination in our catheters, whose mean indwelling period was 10.8 days with a median of 7 days. Several studies in adults show a significant decrease in CRBSI, cost and time required for care when the hub is protected with povidone–iodine by different methods [25, 26, 27, 28].
It is well known that the risk of infection can be reduced by the use of antiseptic at the insertion site [29, 30, 31, 32, 33] before catheterization and during dressing change. Maki et al. [29] and the AAP guidelines [20] prefer 2% chlorhexidine to other antiseptics, although this is still a matter for debate [32, 33]. Other recommendations include minimal handling, heparin-bonded catheters [34], antiseptic-antibiotic-coated catheters when the indwelling time is expected to be more than 7 days [35, 36], tunneled catheters or chlorhexidine dressings. Nevertheless, continuous training of physicians and nursing staff in CVC maintenance is still the most effective way of reducing CRBSI [37, 38, 39].
In our study, lower patient weight (< 8 kg) was an independent factor with a greater risk for catheter-related infection. This may be because of young age and/or malnourishment, both of which are associated with immunodepression. In the published studies we reviewed, we found that lower weight was a risk factor for infection in premature neonates [13, 18, 19], and Damen et al. found greater colonization of CVC in children under 1 year of age [40].
Our study found more infections in subclavian lines than in femoral or jugular lines in the univariate analysis, although this was not significant (p = 0.1). Multivariate analysis showed that insertion site was not a risk factor for infection. There is no increased risk of infection with femoral insertion in infants and children compared with non-femoral insertion [5, 6, 7, 8, 41]. The 1997 meta-analysis by Vekataraman [7] reviews 23 publications about CVC in children and concludes that femoral insertion is safe, with high success rate and no more infections than other access routes. Our results and those reported in the literature recommend femoral insertion over other sites in pediatric patients.
Nevertheless, the experience in adults is different [26, 42, 43, 44, 45]. Thus, Goetz et al. [42] report a greater risk of catheter contamination with femoral insertion, although the rate of CRBSI is not greater. Safdar et al. [24] recommend using subclavian rather than jugular insertion, and jugular rather than femoral insertion to prevent CRBSI in adults.
The type of dressing used to protect the catheter may affect the risk of infection, but published results are contradictory. Some studies claim that impermeable polyurethane reduces the risk of infection, as it avoids exposure to nearby flora (from tracheostomy secretions, saliva, feces or urine), whereas other investigations, including one meta-analysis [46], argue that impermeable dressings macerate the catheter entry and lead to infection by saprophytes. Several studies found no differences. The results of our study support the second hypothesis, thereby maintaining the controversy. Given that both hypotheses are coherent, experts recommend selecting the dressing on an individual basis [5].
No relationship between infection, obstruction and thrombosis has been established in our study, unlike other studies [47]; even though the risk of infection is higher in children with obstruction (univariate analysis p < 0.001), it was not predictive in the multivariate model. The number of thromboses detected in our series was small, probably because they can be asymptomatic and routine ultrasound and X-ray examinations with contrast medium were not performed; furthermore, mere obstruction was not considered a clinical sign of CVT.
As far as catheter management (removal or not) in the presence of infection is concerned, our results on the outcome of infection support the recommendations of other authors [48]: patients not affected by heart disease with coagulase-negative staphylococcus infection can receive antibiotics if catheter removal proves problematic (limited vascular access sites, potential complications related to reinsertion); however, the catheter must be removed in infections caused by Candida spp., Staphylococcus aureus, Gram-negative organisms and in patients suffering from heart disease.
Our study is limited in that it does not analyze the influence of CRBSI on morbidity, duration of admission, or cost, which are extremely important both for the patient and for health service.
Another limitation is that there was no standard procedure for catheter care, only the procedures of the individual protocols of each PICU. Therefore, results on povidone and dressings are based on a non-randomized design.
To conclude, central venous catheterization, a frequent procedure, is not exempt from morbidity and mortality. Catheter-related sepsis is associated with lower patient weight, more than 12 days' indwelling time and recatheterization, but not with the insertion site.
Many studies, especially pediatric studies, are necessary to ascertain the diagnostic capacity and yield of different culture techniques (classic or novel) for diagnosis of CRBSI in pediatric patients.
References
Domínguez TE, Chalom R, Costarino AT (2001) The impact of adverse patient occurrences on hospital costs in the pediatric intensive care unit. Crit Care Med 29:169–174
Pittet D, Tarara D, Wenzel R (1994) Nosocomial bloodstream infection in critically ill patients: excess length of stay, extra costs, and attributable mortality. JAMA 271:1598–1601
Rello J, Ochagavía A, Sabanes E, Roque M, Mariscal D, Reinaga E, Valles J (2000) Evaluation of outcome of intravenous catheter-related infections in critically ill patients. Am J Respir Crit Care Med 162:1027–1030
Richards MJ, Edwards JR, Culver DH, Gaynes RP and The National Nosocomial Infections Surveillance System (1999) Nosocomial infections in pediatric intensive care units in the United States. Pediatrics 103:103–109
Jonge RC, Polderman KH, Gemke RJ (2005) Central venous catheter use in the pediatric patient: mechanical and infectious complications. Pediatr Crit Care Med 6:329–339
Casado Flores J, Barja J, Martino R, Serrano A, Valdivielso A (2001) Complications of central venous catheterization in critically ill children. Pediatr Crit Care Med 2:57–62
Venkataraman ST, Thompson AE, Orr RA (1997) Femoral vascular catheterization in critically ill infants and children. Clin Pediatr 36:311–319
Goldstein AM, Weber JM, Sheridan RL (1997) Femoral venous access is safe in burned children: an analysis of 224 catheters. J Pediatr 130:442–446
Casado Flores J, Valdivielso Serna A, Pérez Jurado L, Pozo-Román J, Monleón Luque M, García-Pérez J, Ruiz-Beltrán A, García-Teresa MA (1991) Subclavian vein catheterization in critically ill children: analysis of 322 cannulations. Intensive Care Med 17:350–354
Stenzel JP, Green TP, Furhman BP, Carlson PE, Marchesault RP (1989): Percutaneous central venous catheterization in a pediatric intensive care unit: a survival analysis of complications. Crit Care Med 17:984–988
Smith-Wright DL, Green TP, Lock JE, Egar MI, Fuhrman BP (1984) Complications of vascular catheterization in critically ill chidren. Crit Care Med 12:1015–1017
La Quaglia MP, Lucas A, Thaler HT, Friedlander-Klar H, Exelby PR, Groeger JS (1992) A prospective analysis of vascular device-related infections in children. J Pediatr Surg 27:840–842
Fallt ME, Gallinero RN, Stover BH, Wilkerson S, Goldsmith J (1998) Central venous catheter bloodstream infections in the neonatal intensive care unit. J Pediatr Surg 33:1383–1387
Odetola FO, Moler FW, Decher RE, VanDerElzen K, Chenoweth C (2003) Nosocomial catheter-related bloodstream infections in a pediatric intensive care unit: risk and rates associated with various intravascular technologies. Pediatric Critical Care Med 4:432–436
Seldinger SI (1953) Catheter replacement of the needle in percutaneous arteriography. Acta Radiol 39:368–376
Maki DG, Weise CE, Sarafin HW (1977) A semicuantitative culture method for identifying intravenous catheter-related infection. N Engl J Med 296:1305–1309
Randolph AG, Brun-Buisson C, Goldmann D (2005) Identification of central venous catheter-related infections in infants and children. Pediatr Crit Care Meditieren 6(S):S19–S24
National Nosocomial Infections Surveillance (NNIS) (1999) System report, data summary from January 1990 to May 1999, issued June 1999. AJIC 27:520–532
National Nosocomial Infections Surveillance (NNIS) (2003) System report, data summary from January 1992 to June 2003, issued August 2003. AJIC 31:481–498
Grady NP, Alexande M, Dellinger EP, Gerberding JL, Heard SO, Maki DG, Masur H, McCormick RD, Mermel LA, Pearson ML, Raad II, Randolph A, Weinstein RA (2002) Guidelines for the prevention of intravascular catheter-related infections. Pediatrics 110(5):e51
Safdar N, Fine JP, Maki DG (2005). Meta-analysis: methods for diagnosing intravascular device-related bloodstream infection. Ann Intern Med 142:451–466
Coob DK, High KP, Sawyer RG, Sable CA, Adams RB, Lindley DA, Pruett TL, Schwenzer KJ, Farr BM (1992) A controlled trial of scheduled replacement of central venous and pulmonary-artery catheters. NEJM 327:1062–1068
Cook D, Randolph A, Kernerman P, Cupido C, King DB, Soukup C, Brun-Buisson C (1997) Central venous catheter replacement strategies: a systematic review of the literature. Crit Care Med 25:1417–1424
Safdar N, Maki DG (2004) The pathogenesis of catheter-related bloodstream infection with noncuffed short-term central venous catheters. Intensive Care Med 30:62–67
Stotter AT, Ward H, Waterfield AH, Hilton J, Sim A (1987) Junctional care: the key to prevention of catheter sepsis in intravenous feeding. J Parenter Enteral Nutr 11:159–162
Halpin DP, O'Byrne P, Maentee G , Hennessy TP, Stephens RB (1991). Effect of a Betadine connection shield on central venous catheter sepsis. Nutrition 7:33–34
Randolph AG, Cook DJ (1999) Antiseptic hub connectors reduce venous central catheter-related sepsis. Crit Care Med 27 [Suppl]:A141
Leon C, Alvarez-Lerma F, Ruiz Santana S, González V, De la Torre MV, Sierra R, Leon M, Rodrigo JJ (2003) Antiseptic chamber-containeing hub reduces central venous catheter-related infection: a prospective, randomized study. Crit Care Med 31:1318–1324
Maki DG, Ringer M Alvarado CJ (1991) Prospective randomised trial of povidone-iodine, alcohol and chlorhexidine for prevention of infection associated with central venous and arterial catheters. Lancet 338:339–343
Parienti JJ, Cheyron D, Ramakers M, Malbruny B, Leclercq R, Le Coutour X, Charbonneau P (2004) Alcoholic povidone-iodine to prevent central venous catheter colonization: a randomized unit-crossover study. Crit Care Med 32:708
Chaiyakunapruk N, Veenstra DL, Lipsky BA, Saint S (2002) Chlorhexidine compares with povidone-iodine solution for vascular catheter-site care: a meta-analysis. Ann Intern Med 136:792–801
Langgartner J, Linde HJ, Lehn N, Reng M, Scholmerich J, Gluck T (2004) Combined skin disinfection with chlorhexidine/propanol and aqueous povidone-iodine reduces bacterial colonisation of central venous catheters. Intensive Care Med 30:1081–1088
Assadian O (2004) Skin antiseptic in reducing the risk of central venous catheter-related infections. Crit Care Med 32:887–888
Pierce CM, Wade A, Mok Q (2000) Heparin-bonded central venous lines reduce thrombotic and infective complications in critically ill children. Intensive Care Med 2000 26:967–972
Marciante KD, Veenstra DL, Lipsky BA (2003) Wich antimicrobial impregnated central venous catheter should we use? Modeling the costs and outcomes of antimicrobial catheter use. Am J Infect Control 31:1–8
Hanna HA, Raad II, Hackett B, Wallace SK, Price KJ, Coyle DE, Parmley CL (2003) Antibiotic-impregnated catheters associated with significant decrease in nosocomial and multidrug-resistant bacteremias in critically ill patients. Chest 24:1030–1038
Warren DK, Zack JE, Cox MJ, Cohen MM, Fraser VJ (2003) An educational intervention to prevent catheter-associated bloodstream infections in a nonteaching, community medical center. Crit Care Med 31:1959–1963
Daghistani D, Horn M, Rodríguez Z, Schoenike S, Toledano S (1996) Prevention of indewelling central venous catheter sepsis. Med Pediatr Oncol 26:405–408
Puntis JW, Holden CE, Smallman S, Finkel Y, George RH, Booth IW (1991) Staff training. A key factor in reducing intravascular catheter sepsis. Arch Dis Child 66:335–337
Damen J, Van det Tweel I (1988) Positive tip cultures and related risk factors associated with intravascular catheterization in pediatric cardiac patients. Crit Care Med 16:221–228
Stenzel JP, Green TP, Fuhrman BP, Carlson PE, Marhesault RP (1989) Percutaneous femoral venous catheterizations: a prospective study of complications. J Pediatr 114:411–415
Gotezs AM, Wagener MM, Millar JM, Muder RR (1998) Risk of infection due to central venous catheters: effect of site of placement and catheter type. Infect Control Hosp. Epidemiol 19:842–845
Richet H, Hubert B, Nitemberg G, Andremont A, Buu-Hoi A, Ourbak P, Galicier C, Veron M, Boisivon A, Bouvier AM, Ricome JC, Wolff MA, Pean Y, Berardi-Grassias L, Bourdain JL, Hautefort B, Laaban JP, Tillant D (1990) Prospective multicenter study of vascular-catheter-related complications and risk factors for positive central-catheter cultures in intensive care unit patients. J Clin Microbiol 28:2520–2525
Ruesch S, Walter B, Tramer MR (2002) Complications of central venous catheters: Internal jugular versus subclavian access – a systematic review. Crit Care Med 30:454–460
Lorente L, Villegas J, Martin MM, Jiménez A, Mora ML (2004) Catheter related infection in critically ill patients. Intensive Care Med 30:1681–1684
Hoffman KK, Western SA, Samsa GP, Rutala WA (1992) Transparent polyurethane film as an intravenous catheter dressing. A meta-analysis of the infection risks. JAMA 267:2072–2076
Raad I, Luna M, Khalil SA, Costerton JW, Lam C, Bodey GP (1994) The relation between the thrombotic and infectious complications of central venous catheters. JAMA 271:1014–1016
Shah SS, Smith MJ, Zaoutis TE (2005) Device-related infections in children. Pediatr Clin N Am 52:1189–1208
Author information
Authors and Affiliations
Corresponding author
Additional information
The named authors wrote this article on behalf of the Spanish Central Venous Catheter Pediatric Study Group, the members of which are listed in the Appendix.
Appendix
Appendix
The Spanish Central Venous Catheter Pediatric Study Group is composed of M. Angeles García-Teresa, MD and Juan Casado-Flores, MD, PhD, Hospital Infantil Niño Jesús, Madrid; M. Angel Delgado, MD Hospital Infantil La Paz, Madrid; Jorge Roqueta-Mas, MD, PICU, Hospital Vall de Hebrón, Barcelona; Francisco Cambra-Lasaosa, MD, PICU, Hospital Clinic S Joan de Deu, Barcelona; Andrés Concha-Torre, MD PICU, Hospital Central de Asturias, Oviedo; J. Ignacio Sánchez, MD, PICU, Hospital Infantil 12 de Octubre, Madrid; J. Carlos de Carlos-Vicente, MD PICU, Hospital Son Dureta, Palma de Mallorca; Isabel Martos-Sánchez, MD, PICU, Hospital Ramón y Cajal, Madrid; Antonio Rodríguez-Núñez, MD, Hospital Xeral de Galicia, Santiago de Compostela; Julio Melendo-Jimeno, MD, PICU, Hospital Miguel Server, Zaragoza; Alvaro Castellanos Ortega, MD, PICU, Hospital Universitario Marqués de Valdecilla, Santander; Javier Pilar, MD, PICU, Hospital de Cruces, Baracaldo (Vizcaya); Enrique Quiroga-Ordóñez, MD, PICU, Hospital Materno Infantil Teresa Herrera, La Coruña; J. Antonio Soult-Rubio, MD, PICU, Hospital Universitario Virgen del Rocío, Sevilla; Luis Sancho-Pérez, MD, PICU, Hospital Infantil Gregorio Marañón, Madrid; Eduardo Pérez Yarza, MD, PICU, Hospital Ntra Sra de Aranzazu, San Sebastián; J. Espinosa Ruiz-Cabal, MD, Hospital Universitario Infanta Cristina, Badajoz; Elisa Lozano- Arrans, MD Hospital Clínico San Cecilio, Granada; J. Ramón Fernández-Prieto, MD, PICU, Hospital Arquitecto Marcide, Ferrol (La Coruña); Ignacio Ibarra de la Rosa, MD, PICU, Hospital Reina Sofía, Córdoba.
Rights and permissions
About this article
Cite this article
García-Teresa, M.Á., Casado-Flores, J., Delgado Domínguez, M.Á. et al. Infectious complications of percutaneous central venous catheterization in pediatric patients. Intensive Care Med 33, 466–476 (2007). https://doi.org/10.1007/s00134-006-0508-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-006-0508-8