Abstract
Primary ovarian insufficiency (POI) is defined as a reduction in ovarian function before the expected age of menopause. POI is known to increase the risk of cardiovascular disorders, osteoporosis, cognitive decline, and mood disorders, resulting in a reduced quality of life. Appropriate hormone replacement for premenopausal women decreases these adverse health risks and improves quality of life for women with POI, but does not prolong life expectancy. The potential etiologies of POI include chromosomal abnormalities and genetic mutations, autoimmune factors, and iatrogenic causes, including surgery, chemotherapy, and radiation therapy. A major association is suggested to exist between reproductive longevity and the DNA damage pathway response genes. DNA damage and repair in ovarian granulosa cells is strongly associated with POI. Depletion of oocytes with damaged DNA occurs through different cell death mechanisms, such as apoptosis, autophagy, and necroptosis, mediated by the phosphatase and tensin homolog (PTEN)/phosphoinositide 3-kinase (PI3K)/protein kinase B (AKT)/forkhead transcription factors 3 (FOXO3) pathway. Mesenchymal stem cells (MSCs) are characterized by the ability of self-renewal and differentiation and play an important role in the regeneration of injured tissues. Transplantation of MSCs has been shown to functionally restore ovarian reserve in a POI mouse model. Recent advances in stem cell therapy are likely to be translated to new therapeutic options bringing new hope to patients with POI. The aim of this review is to summarize the pathogenic mechanisms that involve cell death and DNA damage and repair pathways and to discuss the stem cell–based therapies as potential therapeutic options for this gynecologic pathology.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Ovarian insufficiency and menopause
Menopause is a clinically defined condition determined retrospectively after a 12-month permanent cessation of menstruation without other reasons for amenorrhea such as pregnancy, hormonal therapy, or other medical conditions [1]. Most women go through menopause between the ages of 49 and 52 years. Worldwide, a typical woman experiences menopause at an average age of 50.5 years, although differences exist between races and geographic areas [2]. Approximately 5% of women experience menopause between the ages of 40 and 45 years, and approximately 1% women enter menopause before the age of 40 years [3, 4]. This clinical syndrome defined by loss of ovarian function under the age of 40 is called premature ovarian insufficiency (POI), formerly referred to as “premature menopause” or “premature ovarian failure (POF).” About 1 in 1000 women develops POI under the age of 30, sometimes as early as the teenage years.
Menopause reflects a decline in follicular function. As estrogen decreases with great variability, women may experience the various signs and symptoms during the months or years leading up to menopause or after menopause such as irregular menstrual periods, hot flashes, night sweats, sleep disruption, and mood changes. In the postmenopausal state, women sometime experience vaginal dryness, vulvovaginal atrophy, lower urinary tract symptoms, thinning hair, and dry skin [5]. Among these signs and symptoms, loss of menstruation is the first or only symptom of POI, which can be preceded by irregular menstrual cycles.
In addition, POI patients develop different health risks compared to women undergoing natural menopause because they are exposed to a longer hypoestrogenic state. Given that POI occurs during childbearing ages, one of the most severe outcomes associated with POI is severely reduced fertility with low birth rates [6,7,8]. Women with POI also have a decreased life expectancy, largely due to cardiovascular morbidity and mortality [9,10,11,12]. Because POI leads to estrogen deficiency, patients have a higher risk of osteoporosis and bone fractures, which is known to result in worsening quality of life later in life [9, 13,14,15,16,17,18]. Women who undergo “surgical menopause” to remove both ovaries due to benign (adnexal masses and risk reducing surgery) or malignant (endometrial cancer and ovarian cancer) diseases undergo abrupt POI, if not given hormone replacement therapy, with subsequent cognitive decline as a result of Alzheimer’s disease [19,20,21]. Often unexpected diagnosis of POI leads to psychological confusion in young women, resulting in higher rates of depression compared to their healthy controls due to reduced self-esteem and social anxiety [22].
Genetic, autoimmune, and chemo/radiation causes
The etiology of POI is known to be related to chromosome X–associated abnormalities, single genetic mutations, autoimmune factors, and iatrogenic factors, but the cause of many cases goes unidentified [7]. Genetic factors are major determinants of menopausal age in the general population and have been associated with approximately 7% of POI cases [23,24,25]. Chromosomal abnormalities causally related to POI are fragile X chromosome syndrome (FXS) [26,27,28] and Turner syndrome [29]. FXS leads to the most common cause of inherited intellectual disability, caused by a loss-of-function mutation in the fragile X mental retardation 1 (FMR1) gene located on the X-chromosome, locus Xq27.3. Turner syndrome is a condition of partial or complete absence of the X chromosome, such as 45XO or 45X/46XX mosaicism in females. Notable X-linked genetic mutations associated with POI involve growth differentiation factor-9 (GDF-9) and bone morphogenetic protein-15 (BMP-15) [30, 31], whereas autosomal abnormalities were found in forkhead box l2 (FOXL2) [32], follicle-stimulating hormone receptor (FSHR) [33], stromal antigen 3 (STAG3) [34], x-Ray repair cross complementing 2 (XRCC2) [35], and minichromosome maintenance 8 homologous recombination repair factor (MCM8) [36] genes. Although the cause of POI has not been clearly identified, about 10% of women with POI have a family history of the condition [37].
About 20% of women with POI have a previous diagnosis of an autoimmune disease affecting a variety of different organs, including the heart, kidney, thyroid, pancreas, and the gastrointestinal tract. The autoimmune etiologies for POI are divided into two groups: endocrine and non-endocrine disorders [38,39,40]. Endocrine diseases include Addison’s disease, Hashimoto’s thyroiditis, hypophysitis, and diabetes mellitus type 1, while non-endocrine diseases include chronic candidiasis, rheumatoid arthritis, idiopathic thrombocytopenic purpura, autoimmune hemolytic anemia, pernicious anemia, celiac sprue, alopecia vitiligo, systemic lupus erythematosus, Sjörgren’s syndrome, chronic active hepatitis, primary biliary cirrhosis, and autoimmune polyendocrine syndromes I and II [41, 42]. Autoimmune disease-triggered POI is mediated through an antibody production against ovarian tissue that harms developing follicles in the ovaries and causes ovarian dysfunction [43].
Additional factors responsible for the development of POI include chemotherapy and radiation. Chemotherapy and radiotherapy cause POI by impairing follicle maturation or loss of primordial follicles directly or indirectly [44]. In chemotherapy, alkylating agents such as cyclophosphamide and anthracycline are most well known to cause ovarian dysfunction and POI [45]. The use of new targeted therapies, such as bevacizumab and tyrosine kinase inhibitors (imatinib, pazopanib), may also be associated with an increased risk of POI [46, 47]. Vascular endothelial growth factor A (VEGFA) is believed to play an important role in regulating ovarian angiogenesis [48], and the use of anti-angiogenesis drugs such as bevacizumab increases the risk of POI by inhibiting follicle formation and oocyte maturation [49]. Women receiving whole pelvic or spinal radiation are also at increased risk for developing acute ovarian failure [50, 51]. In particular, age, the distance between the irradiated site and the ovaries, the total dose, and the number of fractionation are important factors that determine the risk of POI [9, 52]. Cranial radiation may cause hypothalamic-pituitary disturbance resulting in amenorrhea [53].
Premature ovarian insufficiency management
POI is a challenging diagnosis that is associated with several emotional and physical consequences (e.g., osteoporosis and cardiovascular events). At the time of diagnosis, patients may experience moderate to severe emotional distress due to the unexpected nature and the health implications associated with POI [54]. It is the physician’s role to deliver the news in a caring manner and provide patients with the support and resources available. An early and timely diagnosis of POI is essential for both treatment and prevention of long-term complications of the hypoestrogenic state [6, 16]. Most patients with POI present with irregular menstrual cycles rather than amenorrhea, contributing to the delay in the diagnosis. Given the varied presentation in menstrual irregularities, it is prudent to consider POI in patients with abnormal uterine bleeding. In addition, the levels of estrogen, FSH, and ovarian ultrasound findings may be used to confirm the diagnosis [55]. Recent findings suggest that anti-Müllerian hormone (AMH) is the best biomarker of ovarian reserve currently available [56]. Its level in circulation is significantly correlated with the number of primordial follicles in healthy women [57].
After the diagnosis is confirmed, multidisciplinary approaches are pivotal in dealing with POI patients. Future fertility concerns and postmenopausal symptoms need to be addressed at the time of the diagnosis. Such concerns shape future treatment plans for patients. For example, assisted reproductive techniques like in vitro fertilization (IVF), cryopreservation, follicle retrieval, and oocyte or embryo donation should be discussed with patients who have future reproductive plans. However, while the fertility strategies are important, the focus on this paper is the management of the non-fertility issues associated with POI and the use of hormone replacement therapy (HRT). Such non-fertility issues include vasomotor instability, sexual dysfunction, and higher long-term risk of cardiovascular diseases and osteoporosis [58].
Three HRT agents are commonly used and include ethinyl estradiol, conjugated equine estrogen, and estradiol. Estradiol is recommended for menopausal women because of fewer side effects compared to ethinyl estradiol and conjugated equine estrogen. All women with primary ovarian insufficiency should be offered HRT unless there are contraindications to HRT or they refuse HRT due to informed/shared decisions [59]. However, in young women with an intact uterus, combined hormonal therapy, including progesterone, is recommended to prevent endometrial hyperplasia and carcinoma [6].
Animal models of premature ovarian insufficiency
The current knowledge of POI pathophysiology is based on studies in animal models. A common murine model of POI uses various anticancer drugs, including cyclophosphamide, busulfan, doxorubicin, gemcitabine, and cisplatin [60,61,62,63,64]. Strong evidence demonstrates that exposure to these anticancer agents leads to follicular atresia and apoptosis of granulosa cells [65, 66]. In addition, mice with exposure to high concentrations of galactose were used as a model for POI due to galactose-triggered toxicity causing pituitary dysfunction, resulting in a persistent high levels of follicle stimulation hormone (FSH) and low levels of estradiol (E2) [67]. Another murine model utilizes thymectomy to trigger POI by causing autoimmune oophoritis that progresses to acute oocyte loss with massive infiltration of mononuclear cells [68]. Additional POI models have been established by knockdown of genes involved in primordial germ cell migration and proliferation, including G protein-coupled receptor 3 (GPR3), basonuclin 1 (BNC1), C2HC-type zinc finger 3 (NANOS3) [69,70,71], and knockdown of FMR1 [72] involved in cell death. An additional group of genes comprised of oocyte-specific transcription factors such as folliculogenesis-specific basic helix-loop-helix (FIGLA) [73], oocyte-specific TGF-beta family such as GDF9 [74], and the transcription factors associated with follicular development such as Wilms tumor 1 (WT1) and Forkhead box protein L2 (FOXL2) [75, 76]. Finally, knockdown of genes involved in follicular development and their receptors such as follicle stimulation hormone receptor (FSHR) [77] and AMH [78] have been used to establish the POI in an in vivo model. Different models of POI are summarized in Table 1.
Cell death
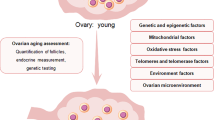
In mammalian females, the formation of primordial follicles, comprised of oocytes surrounded by granulosa cells, is completed prenatally, and the number decreases with aging [79]. Most of primordial follicles remain dormant after birth, but some initiate meiosis through reproductive age, as part of initial recruitment. The primordial follicles that have begun meiosis grow into primary and secondary follicles, undergo cyclic recruitment, and finally ovulate by the appropriate stimulation of gonadotropins [80]. In the absence of gonadotropin stimulation, the follicles undergo atresia and apoptotic cell death [81].
Apoptosis is closely associated with POI, and it is believed to be the major mechanism of cell death associated with oocyte loss in the process of maturation from primordial to antral follicles, or secondary due to chemotherapeutic treatments [82]. Trends of follicles in POI patients cannot be ethically studied. Thus, the effects of chemotherapy on ovarian follicles have only been studied in gene knockout mouse and human ovarian xenograft models [62, 83,84,85]. In human ovarian xenograft models, cyclophosphamide directly damages resting follicles, resulting in a reduced number of primordial follicles [84]. This phenomenon induces significant apoptosis of granulosa cells, which is the cellular basis of ovarian follicular atresia [86, 87], as it leads to reduced levels of sex hormones secreted by non-resting follicular granulosa cells [88].
In addition to apoptosis, inhibition of autophagy has been shown to be involved in follicular loss. Germ cell–specific knockout of the autophagy-inducing gene (Atg7) leads to reduced fertility due to severe ovarian follicular loss in female mice. Germ cell-specific Atg7 knockout causes excessive germ cell loss at the neonatal transition period [89].
Cell-programmed necrosis (necroptosis) is a programmed cell death pathway that exhibits necrotic morphology and is executed by a defined cell signaling cascade that shares some key important members with apoptosis [90,91,92,93]. Necrosis and necroptosis have been shown to be the molecular mechanism of germ cell depletion in aging ovaries, but their role in POI has not been studied. In addition to apoptosis and autophagy, necrosis and necroptosis are involved in germ cell depletion from the mammalian ovarian cohort [94]. Oxidative stress and cytokines induce necrosis and necroptosis in the mammalian oocyte. Also, high levels of cytokines and oxidative stress induce necrosis and necroptosis in granulosa cells, resulting in follicular atresia. In granulosa cells, necrosis, as well as apoptosis, increases with the progression of follicular atresia [95]. Dehydroepiandrosterone (DHEA), reported to improve oocyte quality and pregnancy rates in patients with diminished ovarian reserve [96, 97], can attenuate starvation-induced upregulation of receptor interacting protein kinase 1 (RIPK1) and RIPK3 that transmit necroptosis signaling in human granulosa cells without the induction of mitochondrial reactive oxygen species (ROS) production [98]. The necrostatin1 (NEC-1) inhibits RIPK1 in human granulosa cells affecting RIPK1 kinase activity [99]. Necrosulfonamide (NSA) inhibits mixed lineage kinase domain-like protein (MLKL) and prevents necroptosis in primary cultured human granulosa cells [100]. These necroptosis inhibitors have been suggested to play a role in protecting granulosa cells, resulting in prevention of germ cell depletion, and may be useful in the treatment of POI.
DNA damage and repair
No consistently modified gene variants exist across the POI cohort due to the small sample size of POI patients and their ethnic heterogeneity. Interestingly, genome-wide association studies (GWAS) and array-based comparative genomic hybridization (CGH) have revealed genes that are potentially associated with POI and have proposed relevant candidates [101]. These techniques revealed a large number of genetic mutations in genes involved in DNA damage and repair, homologous recombination (HR), and meiosis. These genes include stromal antigen 3 (STAG3), synaptonemal complex central element 1 (SYCE1), scaffolding protein involved in DNA repair (SPIDR), proteasome 26S subunit ATPase 3-interacting protein (PSMC3IP), ATP-dependent DNA helicase homolog (HFM1), mutS homolog (MSH) 4, MSH5, MCM8, MCM9, cockayne syndrome B-piggyBac 3 (CSB-PGBD3), nucleoporin-107 (NUP107), and breast cancer susceptibility genes (BRCA1 and BRCA2) [102]. In addition, a meta-analysis of 53 GWASs within 70,000 women identified 44 loci associated with POI [103]. Interestingly, two-thirds of harbored genes are involved in the DNA damage and repair pathway, including exonuclease 1 (EXO1), helicase, POLQ Like (HELQ), MCM8, MSH5, Abraxas 1, BRCA1 A Complex Subunit (FAM175A), fanconi anemia complementation group I (FANCI), tousled like kinase 1 (TLK1), DNA polymerase gamma, catalytic subunit (POLG), and BRCA1. A major association between reproductive longevity and the DNA damage pathway response genes has been suggested.
While many types of DNA damage exist, double-strand breaks (DSBs) are considered to be the most severe form [104]. Endogenous and exogenous factors trigger formation of DNA DSBs in primordial follicles. DNA damage accumulates in primitive follicles due to changes in cellular metabolism and elevated oxidative stress as part of ovarian aging. In the process of oxidative respiration in the primordial follicles, a small amount of oxygen is first converted to superoxide in the mitochondria and then to hydroxyl radicals. These hydroxyl radicals cause DNA single-strand breaks, which can cause DSBs and loss of primordial follicles if DSBs occur in multiple adjacent lesions [105]. Exogenous factors that cause DSBs include X-rays, chemotherapy, and environmental toxins [106]. Cisplatin, cyclophosphamide, and doxorubicin induce DNA DSBs in primordial follicles in human ovarian xenograft models and in vitro, causing apoptotic oocyte death associated with the activation of ataxia telangiectasia mutated (ATM) in most cases [66, 85, 107, 108]. Gamma rays and X-ray-generated photons form free radical clusters along their path through the body, which can directly damage DNA duplexes and cause DSBs [109].
Signaling pathways involved in the loss of the ovarian reserve
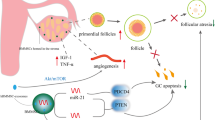
The phosphatase and tensin homolog (PTEN)/phosphoinositide 3-kinase (PI3-K)/protein kinase B (AKT)/forkhead transcription factor 3 (FOXO3) signaling pathway plays an important role in the recruitment from oocytes of primary and further developed follicles. FOXO3a-deficient mice develop initially normal primordial follicles, which later undergo spontaneous global activation, leading to premature loss of all oocytes [110, 111]. FOXO3a suppresses development of the oocyte, granulosa cells, and thecal cells in the follicle at early stages [112]. Downregulation of FOXO3a fails to rescue the apoptotic death of granulosa cells, resulting in oocyte loss [113]. Oocyte-specific deletion of PTEN causes global primordial follicle activation, similar to FOXO3a-knockout mice, resulting in POI [114]. Oocyte-specific deletion of PTEN activates phosphatidylinositol-dependent kinase 1 (PDK1) through PI3K-induced conversion of secondary messengers, resulting in AKT activation [110]. AKT activation causes hyperphosphorylation of FOXO3a, leading to activation of primordial follicles. Therefore, PTEN downregulation may lead to follicular activation and excessive primordial follicle atresia. Furthermore, the PTEN/PI3K/AKT/FOXO3 pathway has been shown to be responsible for chemotherapy-induced POI [63].
The Hippo signaling pathway has been shown to specifically inhibit activation of primordial follicles. Fragmenting ovarian cortex increases actin polymerization and disrupts Hippo signaling, causing [115] increased nuclear localization of Hippo signaling effector and yes-associated protein (YAP), and its decreased phosphorylation leads to increased expression of connective tissue growth factor (CCN), resulting in accelerated follicular development [116].
Recently, an in vitro activation (IVA) model was developed based on the activation of primordial follicles using manipulation of the PTEN/PI3K/AKT/FOXO3 and Hippo pathways by fragmenting ovarian tissue to activate mechanical forces. In this methodology, the surgically obtained ovarian cortex is first fragmented and incubated with AKT stimulators for 2 days. Next, fragments are ectopically transplanted under the serosa of the oviduct [115]. Utilizing this methodology, POI patients were able to deliver healthy babies [117]. IVA appears to be a promising treatment for patients with POI who desire improved fertility. However, IVA for POI patients is still highly experimental and pregnancy rates are low. In addition, special attention should be paid to potential carcinogenic effects, given this method stimulates the PTEN/PI3K/AKT/FOXO3 signaling pathway, which is involved in tumorigenesis [118].
Mesenchymal stem cells to restore ovarian function
Mesenchymal stem cells (MSCs) are multipotent adult stem cells that have capacity to self-renew preserving their stemness as well as capacity to differentiate into various cell types such as osteoblasts, chondrocytes, and adipocytes [119, 120]. One of MSCs properties is growing attached to plastic under standard culture conditions. MSCs express various cell surface markers including cluster of differentiation (CD)73, CD90, CD44, and CD105 and lacking expression of CD34, CD45, CD14 or CD11b, CD79a or CD19, and human leukocyte antigen (HLA) class II. MSCs are derived from various sources: bone marrow, adipose tissue, amniotic fluid, amniotic membrane, placenta, menstrual blood, endometrium, and umbilical cord [60, 121,122,123,124,125,126,127,128,129]. Cellular therapy using MSCs has been in the limelight in recent years as a promising treatment for various degenerative diseases, such as acute renal failure [130], acute lung injury [131, 132], myocardial infarction [133], and cerebral ischemia [134]. It has been reported that MSCs have a role in regulating different populations of immune cells such as T cells, B cells, NK cells, dendritic cells (DCs), and macrophages [135]. MSCs can migrate to damaged tissues by inducing peripheral immune tolerance. They can block the release of inflammatory cytokines, such as tumor necrosis factor-alpha (TNFα) and interleukin-6 (IL-6), and promote the survival of damaged cells [136]. Recently, MSC-based cellular therapy has been studied to restore ovarian function in POI patients. Transplantation of bone marrow-derived MSCs in a mouse POI model restored ovarian function, suggesting that MSCs were the regenerative factor responsible for the bone marrow transplantation phenomenon [137, 138]. Its effectiveness has been evaluated and confirmed in the mouse model of POI. In addition, the therapeutic effect of stem cells on POI has already begun to be demonstrated by clinical trials. Transplantation of human umbilical cord–derived MSC (hUCMSC) into the ovaries of POI patients increased estradiol levels, improved follicle development, and increased follicular follicle numbers. Some of the POI women after transplantation of hUCMSC achieved successful clinical pregnancies [139]. However, there are some ethical and methodological issues regarding treatment with stem cells such as protracted safety concerns that need to be resolved during the process of purification and transplantation of stem cells. These concerns include the potential for the emergence of dangerous clones, the risk of contamination with undifferentiated cells, genomic instability, and the possibility of epigenetic abnormalities [140]. MSCs from adipocytes, placenta, or umbilical cord can be extracted using minimally invasive procedures that do not harm donors, but samples are limited. Also, intra-ovarian injections into patients are invasive and can cause side effects such as an immune response [141]. There are limited clinical studies of MSC transplantation in patients with POI status. Only 10 clinical trials in this field have been conducted (ClinicalTrial.gov) (Table 2). In these clinical trials, autologous bone marrow–derived stem cells and hUCMSCs were used. These therapies restored ovarian function in POI patients, showing increase in AMH levels and follicle development and improved oocyte collection [142, 143]. Several of the POI patients whose ovarian function improved following transplantation of MSCs had successful clinical deliveries [139, 142,143,144].
Differentiation of MSCs into granulosa cells within ovary and reactivation of ovarian function through the paracrine pathway are two mechanisms that MSCs utilize to improve chemotherapy-induced ovarian dysfunction [145]. Adipose-derived MSCs injected into ovaries of cyclophosphamide-treated rats and mice were later located in the thecal layers but not in the follicles [123]. In addition, intraperitoneally transplanted human amniotic epithelial (hAECs)–derived green fluorescent protein (GFP)–positive cells migrate to mouse ovary and differentiate into granulosa cells, but not into follicles [125]. Therefore, restoration of ovarian function is achieved due to MSC differentiation into granulosa cells within the injured ovary, and not due to oocyte differentiation. MSCs secrete various cytokines, such as hepatocyte growth factor (HGF), vascular endothelial cell growth factor (VEGF), insulin-like growth factor-1 (IGF-1), epidermal growth factor (EGF), fibroblast growth factors 2 (FGF2), granulocyte-colony stimulating factor (G-CSF), and interleukin (IL)-6, IL-8, IL-10, IL-11, and IL-15 [123, 146, 147, 138, 148, 149]. MSCs have been shown to inhibit apoptosis of granulosa cell in mammalian model of POI [150] due to increased secretion of steroid hormone and inhibition of apoptosis in granulosa cells through IGF-1 pathway [151]. Transplantation of MSCs overexpressing microRNA-21, involved in apoptotic regulation, repaired the ovarian function and inhibited the apoptosis of granulosa cells by targeting PTEN and programmed cell death 4 (PDCD4) [152]. Transplantation of human placenta–derived mesenchymal stem cell (hPMSC) restored ovarian function in chemotherapy and autoimmune-induced POI mice model by regulating cytokines associated with regulatory T cells (Treg) via the PI3K/AKT signaling pathway [153, 126]. Also, hAEC transplantation promoted ovarian function by reducing inflammation and inhibiting the TNFα-mediated apoptosis [154]. MSCs secrete cytokines that promote angiogenesis, such as VEGF, FGF2, and angiogenin, causing recovery of damaged ovaries following transplantation of cryopreserved ovarian cortex [155]. Injection of hUCMSCs to mice with chemotherapy-induced POI increases total and phospho-AKT as well as VEGF expression, which promotes ovarian angiogenesis [127]. Moreover, EGF secreted by hPMSCs quenches ROS in POI by upregulating the nuclear factor erythroid 2 related factor 2 (NRF2)/heme oxygenase 1 (HO1) pathway that is involved in DNA repair and aging, apoptosis, and embryonic cell death [149]. Transplantation of human amniotic fluid-derived MSC (hAMSCs) attenuated the DNA damage as assessed by phosphorylation of variant histone H2A (p-γH2AX), BRCA1, PARP1, and X-Ray repair cross complementing 6 (XRCC6)) in granulosa cells of aged mice [156]. Based on the above findings, MSCs may play an important role in regenerating granulosa cells and restoring ovarian function through an anti-inflammatory and immunomodulatory effect, as well as through DNA repair. MSC regenerative therapies that have been evaluated in vivo in improving ovarian function are summarized in Table 3.
Conclusion
Overall, POI is a condition of estrogen deficiency that causes both short-term and lifelong implications for health and psychosocial well-being, compared to undergoing menopause at a later age. Healthcare professionals need to effectively manage these complex entities to ensure that physical, psychological, and emotional challenges resulting from POI diagnosis are addressed, and that the short and long-term wellbeing of these young women is preserved. Considering the lifelong health of POI patients, development of treatments to restore ovarian function earlier is essential to improve quality of life. Recent development of regenerative medicine allowed transplantation of various types of human MSCs improving the ovarian function in POI mice. Transplantation of MSCs shows a significant positive effect in an animal model of POI and in some clinical studies, but it has not yet been applied to clinical practice due to methodological and ethical issues. The MSC transplantation regimen should be optimized to identify optimal injection site, frequency of each procedure, and cell number used to make MSC transplantation more effective.
Data Availability
Not applicable
References
Lumsden MA, Davies M, Sarri G, 23) GDGfMDaMNCGN (2016) Diagnosis and management of menopause: the National Institute of Health and Care Excellence (NICE) Guideline. JAMA Intern Med 176(8):1205–1206
Team IS (2019) Variations in reproductive events across life: a pooled analysis of data from 505 147 women across 10 countries. Hum Reprod 34(5):881–893
Coulam CB, Adamson SC, Annegers JF (1986) Incidence of premature ovarian failure. Obstet Gynecol 67(4):604–606
Luborsky JL, Meyer P, Sowers MF, Gold EB, Santoro N (2003) Premature menopause in a multi-ethnic population study of the menopause transition. Hum Reprod 18(1):199–206
Takahashi TA, Johnson KM (2015) Menopause. Med Clin North Am 99(3):521–534
Committee opinion no. 605: primary ovarian insufficiency in adolescents and young women (2014). Obstet Gynecol 124 (1):193-197. doi:
Nelson LM (2009) Clinical practice. Primary ovarian insufficiency. N Engl J Med 360(6):606–614
Jankowska K (2017) Premature ovarian failure. Prz Menopauzalny 16(2):51–56
Webber L, Davies M, Anderson R, Bartlett J, Braat D, Cartwright B, Cifkova R, de Muinck K-SS, Hogervorst E, Janse F, Liao L, Vlaisavljevic V, Zillikens C, Vermeulen N, POI ESfHRaEEGGo (2016) ESHRE Guideline: management of women with premature ovarian insufficiency. Hum Reprod 31(5):926–937
Tao XY, Zuo AZ, Wang JQ, Tao FB (2016) Effect of primary ovarian insufficiency and early natural menopause on mortality: a meta-analysis. Climacteric 19(1):27–36
Archer DF (2009) Premature menopause increases cardiovascular risk. Climacteric 12(Suppl 1):26–31
Shuster LT, Rhodes DJ, Gostout BS, Grossardt BR, Rocca WA (2010) Premature menopause or early menopause: long-term health consequences. Maturitas 65(2):161–166
Gallagher JC (2007) Effect of early menopause on bone mineral density and fractures. Menopause 14(3 Pt 2):567–571
Malabanan AO, Holick MF (2003) Vitamin D and bone health in postmenopausal women. J Womens Health (Larchmt) 12(2):151–156
Sullivan SD, Lehman A, Nathan NK, Thomson CA, Howard BV (2017) Age of menopause and fracture risk in postmenopausal women randomized to calcium + vitamin D, hormone therapy, or the combination: results from the Women's Health Initiative Clinical Trials. Menopause 24(4):371–378
Anasti JN, Kalantaridou SN, Kimzey LM, Defensor RA, Nelson LM (1998) Bone loss in young women with karyotypically normal spontaneous premature ovarian failure. Obstet Gynecol 91(1):12–15
Kurtoglu-Aksoy N, Akhan SE, Bastu E, Gungor-Ugurlucan F, Telci A, Iyibozkurt AC, Topuz S (2014) Implications of premature ovarian failure on bone turnover markers and bone mineral density. Clin Exp Obstet Gynecol 41(2):149–153
Popat VB, Calis KA, Vanderhoof VH, Cizza G, Reynolds JC, Sebring N, Troendle JF, Nelson LM (2009) Bone mineral density in estrogen-deficient young women. J Clin Endocrinol Metab 94(7):2277–2283
Kodaman PH (2010) Early menopause: primary ovarian insufficiency and surgical menopause. Semin Reprod Med 28(5):360–369
Sarrel PM, Sullivan SD, Nelson LM (2016) Hormone replacement therapy in young women with surgical primary ovarian insufficiency. Fertil Steril 106(7):1580–1587
Bove R, Secor E, Chibnik LB, Barnes LL, Schneider JA, Bennett DA, De Jager PL (2014) Age at surgical menopause influences cognitive decline and Alzheimer pathology in older women. Neurology 82(3):222–229
Schmidt PJ, Cardoso GM, Ross JL, Haq N, Rubinow DR, Bondy CA (2006) Shyness, social anxiety, and impaired self-esteem in Turner syndrome and premature ovarian failure. JAMA 295(12):1374–1376
Bachelot A, Rouxel A, Massin N, Dulon J, Courtillot C, Matuchansky C, Badachi Y, Fortin A, Paniel B, Lecuru F, Lefrère-Belda MA, Constancis E, Thibault E, Meduri G, Guiochon-Mantel A, Misrahi M, Kuttenn F, Touraine P, Group P-GS (2009) Phenotyping and genetic studies of 357 consecutive patients presenting with premature ovarian failure. Eur J Endocrinol 161(1):179–187
Murabito JM, Yang Q, Fox C, Wilson PW, Cupples LA (2005) Heritability of age at natural menopause in the Framingham Heart Study. J Clin Endocrinol Metab 90(6):3427–3430
Vegetti W, Grazia Tibiletti M, Testa G, de Lauretis Y, Alagna F, Castoldi E, Taborelli M, Motta T, Bolis PF, Dalprà L, Crosignani PG (1998) Inheritance in idiopathic premature ovarian failure: analysis of 71 cases. Hum Reprod 13(7):1796–1800
Bussani C, Papi L, Sestini R, Baldinotti F, Bucciantini S, Bruni V, Scarselli G (2004) Premature ovarian failure and fragile X premutation: a study on 45 women. Eur J Obstet Gynecol Reprod Biol 112(2):189–191
Conway GS, Payne NN, Webb J, Murray A, Jacobs PA (1998) Fragile X premutation screening in women with premature ovarian failure. Hum Reprod 13(5):1184–1187
Gersak K, Meden-Vrtovec H, Peterlin B (2003) Fragile X premutation in women with sporadic premature ovarian failure in Slovenia. Hum Reprod 18(8):1637–1640
Conway GS (2000) Premature ovarian failure. Br Med Bull 56(3):643–649
Di Pasquale E, Beck-Peccoz P, Persani L (2004) Hypergonadotropic ovarian failure associated with an inherited mutation of human bone morphogenetic protein-15 (BMP15) gene. Am J Hum Genet 75(1):106–111
Laissue P, Christin-Maitre S, Touraine P, Kuttenn F, Ritvos O, Aittomaki K, Bourcigaux N, Jacquesson L, Bouchard P, Frydman R, Dewailly D, Reyss AC, Jeffery L, Bachelot A, Massin N, Fellous M, Veitia RA (2006) Mutations and sequence variants in GDF9 and BMP15 in patients with premature ovarian failure. Eur J Endocrinol 154(5):739–744
Crisponi L, Deiana M, Loi A, Chiappe F, Uda M, Amati P, Bisceglia L, Zelante L, Nagaraja R, Porcu S, Ristaldi MS, Marzella R, Rocchi M, Nicolino M, Lienhardt-Roussie A, Nivelon A, Verloes A, Schlessinger D, Gasparini P, Bonneau D, Cao A, Pilia G (2001) The putative forkhead transcription factor FOXL2 is mutated in blepharophimosis/ptosis/epicanthus inversus syndrome. Nat Genet 27(2):159–166
Aittomäki K, Lucena JL, Pakarinen P, Sistonen P, Tapanainen J, Gromoll J, Kaskikari R, Sankila EM, Lehväslaiho H, Engel AR, Nieschlag E, Huhtaniemi I, de la Chapelle A (1995) Mutation in the follicle-stimulating hormone receptor gene causes hereditary hypergonadotropic ovarian failure. Cell 82(6):959–968
He WB, Banerjee S, Meng LL, Du J, Gong F, Huang H, Zhang XX, Wang YY, Lu GX, Lin G, Tan YQ (2018) Whole-exome sequencing identifies a homozygous donor splice-site mutation in STAG3 that causes primary ovarian insufficiency. Clin Genet 93(2):340–344
Zhang YX, Li HY, He WB, Tu C, Du J, Li W, Lu GX, Lin G, Yang Y, Tan YQ (2019) XRCC2 mutation causes premature ovarian insufficiency as well as non-obstructive azoospermia in humans. Clin Genet 95(3):442–443
Zhang YX, He WB, Xiao WJ, Meng LL, Tan C, Du J, Lu GX, Lin G, Tan YQ (2020) Novel loss-of-function mutation in MCM8 causes premature ovarian insufficiency. Mol Genet Genomic Med:e1165. https://doi.org/10.1002/mgg3.1165
Cordts EB, Christofolini DM, Dos Santos AA, Bianco B, Barbosa CP (2011) Genetic aspects of premature ovarian failure: a literature review. Arch Gynecol Obstet 283(3):635–643
Forges T, Monnier-Barbarino P, Faure GC, Béné MC (2004) Autoimmunity and antigenic targets in ovarian pathology. Hum Reprod Update 10(2):163–175
Novosad JA, Kalantaridou SN, Tong ZB, Nelson LM (2003) Ovarian antibodies as detected by indirect immunofluorescence are unreliable in the diagnosis of autoimmune premature ovarian failure: a controlled evaluation. BMC Womens Health 3(1):2
Haller-Kikkatalo K, Salumets A, Uibo R (2012) Review on autoimmune reactions in female infertility: antibodies to follicle stimulating hormone. Clin Dev Immunol 2012:762541
Wheatcroft N, Weetman AP (1997) Is premature ovarian failure an autoimmune disease? Autoimmunity 25(3):157–165
Domniz N, Meirow D (2019) Premature ovarian insufficiency and autoimmune diseases. Best Pract Res Clin Obstet Gynaecol 60:42–55
Petríková J, Lazúrová I (2012) Ovarian failure and polycystic ovary syndrome. Autoimmun Rev 11(6-7):A471–A478
Sukumvanich P, Case LD, Van Zee K, Singletary SE, Paskett ED, Petrek JA, Naftalis E, Naughton MJ (2010) Incidence and time course of bleeding after long-term amenorrhea after breast cancer treatment: a prospective study. Cancer 116(13):3102–3111
Zhao J, Liu J, Chen K, Li S, Wang Y, Yang Y, Deng H, Jia W, Rao N, Liu Q, Su F (2014) What lies behind chemotherapy-induced amenorrhea for breast cancer patients: a meta-analysis. Breast Cancer Res Treat 145(1):113–128
Imai A, Ichigo S, Matsunami K, Takagi H, Kawabata I (2017) Ovarian function following targeted anti-angiogenic therapy with bevacizumab. Mol Clin Oncol 6(6):807–810
Christopoulos C, Dimakopoulou V, Rotas E (2008) Primary ovarian insufficiency associated with imatinib therapy. N Engl J Med 358(10):1079–1080
Stouffer RL, Martínez-Chequer JC, Molskness TA, Xu F, Hazzard TM (2001) Regulation and action of angiogenic factors in the primate ovary. Arch Med Res 32(6):567–575
Hazzard TM, Xu F, Stouffer RL (2002) Injection of soluble vascular endothelial growth factor receptor 1 into the preovulatory follicle disrupts ovulation and subsequent luteal function in rhesus monkeys. Biol Reprod 67(4):1305–1312
Stillman RJ, Schinfeld JS, Schiff I, Gelber RD, Greenberger J, Larson M, Jaffe N, Li FP (1981) Ovarian failure in long-term survivors of childhood malignancy. Am J Obstet Gynecol 139(1):62–66
Bath LE, Critchley HO, Chambers SE, Anderson RA, Kelnar CJ, Wallace WH (1999) Ovarian and uterine characteristics after total body irradiation in childhood and adolescence: response to sex steroid replacement. Br J Obstet Gynaecol 106(12):1265–1272
Vassilakopoulou M, Boostandoost E, Papaxoinis G, de La Motte RT, Khayat D, Psyrri A (2016) Anticancer treatment and fertility: effect of therapeutic modalities on reproductive system and functions. Crit Rev Oncol Hematol 97:328–334
Constine LS, Woolf PD, Cann D, Mick G, McCormick K, Raubertas RF, Rubin P (1993) Hypothalamic-pituitary dysfunction after radiation for brain tumors. N Engl J Med 328(2):87–94
Groff AA, Covington SN, Halverson LR, Fitzgerald OR, Vanderhoof V, Calis K, Nelson LM (2005) Assessing the emotional needs of women with spontaneous premature ovarian failure. Fertil Steril 83(6):1734–1741
Whitcomb BW, Purdue-Smithe A, Hankinson SE, Manson JE, Rosner BA, Bertone-Johnson ER (2018) Menstrual cycle characteristics in adolescence and early adulthood are associated with risk of early natural menopause. J Clin Endocrinol Metab 103(10):3909–3918
Anderson RA, Nelson SM, Wallace WH (2012) Measuring anti-Mullerian hormone for the assessment of ovarian reserve: when and for whom is it indicated? Maturitas 71(1):28–33
Hansen KR, Hodnett GM, Knowlton N, Craig LB (2011) Correlation of ovarian reserve tests with histologically determined primordial follicle number. Fertil Steril 95(1):170–175
Sullivan SD (2011) A mechanism for integrated health care is ideal for women with primary ovarian insufficiency. Fertil Steril 95(6):1901; discussion 1902
Sullivan SD, Sarrel PM, Nelson LM (2016) Hormone replacement therapy in young women with primary ovarian insufficiency and early menopause. Fertil Steril 106(7):1588–1599
Lee HJ, Selesniemi K, Niikura Y, Niikura T, Klein R, Dombkowski DM, Tilly JL (2007) Bone marrow transplantation generates immature oocytes and rescues long-term fertility in a preclinical mouse model of chemotherapy-induced premature ovarian failure. J Clin Oncol 25(22):3198–3204
Lee EH, Han SE, Park MJ, Kim HJ, Kim HG, Kim CW, Joo BS, Lee KS (2018) Establishment of effective mouse model of premature ovarian failure considering treatment duration of anticancer drugs and natural recovery time. J Menopausal Med 24(3):196–203
Morita Y, Perez GI, Paris F, Miranda SR, Ehleiter D, Haimovitz-Friedman A, Fuks Z, Xie Z, Reed JC, Schuchman EH, Kolesnick RN, Tilly JL (2000) Oocyte apoptosis is suppressed by disruption of the acid sphingomyelinase gene or by sphingosine-1-phosphate therapy. Nat Med 6(10):1109–1114
Chang EM, Lim E, Yoon S, Jeong K, Bae S, Lee DR, Yoon TK, Choi Y, Lee WS (2015) Cisplatin induces overactivation of the dormant primordial follicle through PTEN/AKT/FOXO3a pathway which leads to loss of ovarian reserve in mice. PLoS One 10(12):e0144245
Ben-Aharon I, Bar-Joseph H, Tzarfaty G, Kuchinsky L, Rizel S, Stemmer SM, Shalgi R (2010) Doxorubicin-induced ovarian toxicity. Reprod Biol Endocrinol 8:20
Ezoe K, Daikoku T, Yabuuchi A, Murata N, Kawano H, Abe T, Okuno T, Kobayashi T, Kato K (2014) Ovarian stimulation using human chorionic gonadotrophin impairs blastocyst implantation and decidualization by altering ovarian hormone levels and downstream signaling in mice. Mol Hum Reprod 20(11):1101–1116
Yuksel A, Bildik G, Senbabaoglu F, Akin N, Arvas M, Unal F, Kilic Y, Karanfil I, Eryılmaz B, Yilmaz P, Ozkanbaş C, Taskiran C, Aksoy S, Guzel Y, Balaban B, Ince U, Iwase A, Urman B, Oktem O (2015) The magnitude of gonadotoxicity of chemotherapy drugs on ovarian follicles and granulosa cells varies depending upon the category of the drugs and the type of granulosa cells. Hum Reprod 30(12):2926–2935
Bandyopadhyay S, Chakrabarti J, Banerjee S, Pal AK, Goswami SK, Chakravarty BN, Kabir SN (2003) Galactose toxicity in the rat as a model for premature ovarian failure: an experimental approach readdressed. Hum Reprod 18(10):2031–2038
Miyake T, Taguchi O, Ikeda H, Sato Y, Takeuchi S, Nishizuka Y (1988) Acute oocyte loss in experimental autoimmune oophoritis as a possible model of premature ovarian failure. Am J Obstet Gynecol 158(1):186–192
Ledent C, Demeestere I, Blum D, Petermans J, Hämäläinen T, Smits G, Vassart G (2005) Premature ovarian aging in mice deficient for Gpr3. Proc Natl Acad Sci U S A 102(25):8922–8926
Zhang D, Liu Y, Zhang Z, Lv P, Li J, Wu Y, Zhang R, Huang Y, Xu G, Qian Y, Chen S, Xu C, Shen J, Zhu L, Chen K, Zhu B, Ye X, Mao Y, Bo X, Zhou C, Wang T, Chen D, Yang W, Tan Y, Song Y, Zhou D, Sheng J, Gao H, Zhu Y, Li M, Wu L, He L, Huang H (2018) Basonuclin 1 deficiency is a cause of primary ovarian insufficiency. Hum Mol Genet 27(21):3787–3800
Wu X, Wang B, Dong Z, Zhou S, Liu Z, Shi G, Cao Y, Xu Y (2013) A NANOS3 mutation linked to protein degradation causes premature ovarian insufficiency. Cell Death Dis 4:e825
Lu C, Lin L, Tan H, Wu H, Sherman SL, Gao F, Jin P, Chen D (2012) Fragile X premutation RNA is sufficient to cause primary ovarian insufficiency in mice. Hum Mol Genet 21(23):5039–5047
Soyal SM, Amleh A, Dean J (2000) FIGalpha, a germ cell-specific transcription factor required for ovarian follicle formation. Development 127(21):4645–4654
Dong J, Albertini DF, Nishimori K, Kumar TR, Lu N, Matzuk MM (1996) Growth differentiation factor-9 is required during early ovarian folliculogenesis. Nature 383(6600):531–535
Uda M, Ottolenghi C, Crisponi L, Garcia JE, Deiana M, Kimber W, Forabosco A, Cao A, Schlessinger D, Pilia G (2004) Foxl2 disruption causes mouse ovarian failure by pervasive blockage of follicle development. Hum Mol Genet 13(11):1171–1181
Gao F, Zhang J, Wang X, Yang J, Chen D, Huff V, Liu YX (2014) Wt1 functions in ovarian follicle development by regulating granulosa cell differentiation. Hum Mol Genet 23(2):333–341
Ghadami M, El-Demerdash E, Salama SA, Binhazim AA, Archibong AE, Chen X, Ballard BR, Sairam MR, Al-Hendy A (2010) Toward gene therapy of premature ovarian failure: intraovarian injection of adenovirus expressing human FSH receptor restores folliculogenesis in FSHR(-/-) FORKO mice. Mol Hum Reprod 16(4):241–250
Durlinger AL, Kramer P, Karels B, de Jong FH, Uilenbroek JT, Grootegoed JA, Themmen AP (1999) Control of primordial follicle recruitment by anti-Müllerian hormone in the mouse ovary. Endocrinology 140(12):5789–5796
Faddy MJ, Gosden RG (1995) A mathematical model of follicle dynamics in the human ovary. Hum Reprod 10(4):770–775
McGee EA, Hsueh AJ (2000) Initial and cyclic recruitment of ovarian follicles. Endocr Rev 21(2):200–214
Adhikari D, Liu K (2009) Molecular mechanisms underlying the activation of mammalian primordial follicles. Endocr Rev 30(5):438–464
Morita Y, Tilly JL (1999) Oocyte apoptosis: like sand through an hourglass. Dev Biol 213(1):1–17
Paris F, Perez GI, Fuks Z, Haimovitz-Friedman A, Nguyen H, Bose M, Ilagan A, Hunt PA, Morgan WF, Tilly JL, Kolesnick R (2002) Sphingosine 1-phosphate preserves fertility in irradiated female mice without propagating genomic damage in offspring. Nat Med 8(9):901–902
Oktem O, Oktay K (2007) A novel ovarian xenografting model to characterize the impact of chemotherapy agents on human primordial follicle reserve. Cancer Res 67(21):10159–10162
Soleimani R, Heytens E, Darzynkiewicz Z, Oktay K (2011) Mechanisms of chemotherapy-induced human ovarian aging: double strand DNA breaks and microvascular compromise. Aging (Albany NY) 3(8):782–793
Amsterdam A, Keren-Tal I, Aharoni D, Dantes A, Land-Bracha A, Rimon E, Sasson R, Hirsh L (2003) Steroidogenesis and apoptosis in the mammalian ovary. Steroids 68(10-13):861–867
Hurwitz A, Adashi EY (1992) Ovarian follicular atresia as an apoptotic process: a paradigm for programmed cell death in endocrine tissues. Mol Cell Endocrinol 84(1-2):C19–C23
Zhao XJ, Huang YH, Yu YC, Xin XY (2010) GnRH antagonist cetrorelix inhibits mitochondria-dependent apoptosis triggered by chemotherapy in granulosa cells of rats. Gynecol Oncol 118(1):69–75
Song ZH, Yu HY, Wang P, Mao GK, Liu WX, Li MN, Wang HN, Shang YL, Liu C, Xu ZL, Sun QY, Li W (2015) Germ cell-specific Atg7 knockout results in primary ovarian insufficiency in female mice. Cell Death Dis 6:e1589
Chefetz I, Grimley E, Yang K, Hong L, Vinogradova EV, Suciu R, Kovalenko I, Karnak D, Morgan CA, Chtcherbinine M, Buchman C, Huddle B, Barraza S, Morgan M, Bernstein KA, Yoon E, Lombard DB, Bild A, Mehta G, Romero I, Chiang CY, Landen C, Cravatt B, Hurley TD, Larsen SD, Buckanovich RJ (2019) A pan-ALDH1A inhibitor induces necroptosis in ovarian cancer stem-like cells. Cell Rep 26(11):3061–3075.e3066
Khan I, Yousif A, Chesnokov M, Hong L, Chefetz I (2020) A decade of cell death studies: breathing new life into necroptosis. Pharmacol Ther:107717. https://doi.org/10.1016/j.pharmthera.2020.107717
Chesnokov M, Khan I, Chefetz I (2021) Induction and detection of necroptotic cell death in mammalian cell culture. In: Alvero AB, Mor GG (eds) Detection of Cell Death Mechanisms: Methods and Protocols. Springer US, New York, pp 119–134. https://doi.org/10.1007/978-1-0716-1162-3_11
Golla N, Hong LJ, Chefetz I (2021) Visualization of necroptotic cell death through transmission electron microscopy. In: Alvero AB, Mor GG (eds) Detection of Cell Death Mechanisms: Methods and Protocols. Springer US, New York, pp 135–147. https://doi.org/10.1007/978-1-0716-1162-3_12
Chaudhary GR, Yadav PK, Yadav AK, Tiwari M, Gupta A, Sharma A, Sahu K, Pandey AN, Pandey AK, Chaube SK (2019) Necrosis and necroptosis in germ cell depletion from mammalian ovary. J Cell Physiol 234(6):8019–8027
Rosales-Torres AM, Avalos-Rodríguez A, Vergara-Onofre M, Hernández-Pérez O, Ballesteros LM, García-Macedo R, Ortíz-Navarrete V, Rosado A (2000) Multiparametric study of atresia in ewe antral follicles: histology, flow cytometry, internucleosomal DNA fragmentation, and lysosomal enzyme activities in granulosa cells and follicular fluid. Mol Reprod Dev 55(3):270–281
Narkwichean A, Jayaprakasan K, Maalouf WE, Hernandez-Medrano JH, Pincott-Allen C, Campbell BK (2014) Effects of dehydroepiandrosterone on in vivo ovine follicular development. Hum Reprod 29(1):146–154
Gleicher N, Barad DH (2011) Dehydroepiandrosterone (DHEA) supplementation in diminished ovarian reserve (DOR). Reprod Biol Endocrinol 9:67
Tsui KH, Wang PH, Lin LT, Li CJ (2017) DHEA protects mitochondria against dual modes of apoptosis and necroptosis in human granulosa HO23 cells. Reproduction 154(2):101–110
Hojo T, Siemieniuch MJ, Lukasik K, Piotrowska-Tomala KK, Jonczyk AW, Okuda K, Skarzynski DJ (2016) Programmed necrosis - a new mechanism of steroidogenic luteal cell death and elimination during luteolysis in cows. Sci Rep 6:38211
Blohberger J, Kunz L, Einwang D, Berg U, Berg D, Ojeda SR, Dissen GA, Fröhlich T, Arnold GJ, Soreq H, Lara H, Mayerhofer A (2015) Readthrough acetylcholinesterase (AChE-R) and regulated necrosis: pharmacological targets for the regulation of ovarian functions? Cell Death Dis 6:e1685
Qin Y, Jiao X, Simpson JL, Chen ZJ (2015) Genetics of primary ovarian insufficiency: new developments and opportunities. Hum Reprod Update 21(6):787–808
Jiao X, Ke H, Qin Y, Chen ZJ (2018) Molecular genetics of premature ovarian insufficiency. Trends Endocrinol Metab 29(11):795–807
Day FR, Ruth KS, Thompson DJ, Lunetta KL, Pervjakova N, Chasman DI, Stolk L, Finucane HK, Sulem P, Bulik-Sullivan B, Esko T, Johnson AD, Elks CE, Franceschini N, He C, Altmaier E, Brody JA, Franke LL, Huffman JE, Keller MF, McArdle PF, Nutile T, Porcu E, Robino A, Rose LM, Schick UM, Smith JA, Teumer A, Traglia M, Vuckovic D, Yao J, Zhao W, Albrecht E, Amin N, Corre T, Hottenga JJ, Mangino M, Smith AV, Tanaka T, Abecasis G, Andrulis IL, Anton-Culver H, Antoniou AC, Arndt V, Arnold AM, Barbieri C, Beckmann MW, Beeghly-Fadiel A, Benitez J, Bernstein L, Bielinski SJ, Blomqvist C, Boerwinkle E, Bogdanova NV, Bojesen SE, Bolla MK, Borresen-Dale AL, Boutin TS, Brauch H, Brenner H, Brüning T, Burwinkel B, Campbell A, Campbell H, Chanock SJ, Chapman JR, Chen YI, Chenevix-Trench G, Couch FJ, Coviello AD, Cox A, Czene K, Darabi H, De Vivo I, Demerath EW, Dennis J, Devilee P, Dörk T, Dos-Santos-Silva I, Dunning AM, Eicher JD, Fasching PA, Faul JD, Figueroa J, Flesch-Janys D, Gandin I, Garcia ME, García-Closas M, Giles GG, Girotto GG, Goldberg MS, González-Neira A, Goodarzi MO, Grove ML, Gudbjartsson DF, Guénel P, Guo X, Haiman CA, Hall P, Hamann U, Henderson BE, Hocking LJ, Hofman A, Homuth G, Hooning MJ, Hopper JL, Hu FB, Huang J, Humphreys K, Hunter DJ, Jakubowska A, Jones SE, Kabisch M, Karasik D, Knight JA, Kolcic I, Kooperberg C, Kosma VM, Kriebel J, Kristensen V, Lambrechts D, Langenberg C, Li J, Li X, Lindström S, Liu Y, Luan J, Lubinski J, Mägi R, Mannermaa A, Manz J, Margolin S, Marten J, Martin NG, Masciullo C, Meindl A, Michailidou K, Mihailov E, Milani L, Milne RL, Müller-Nurasyid M, Nalls M, Neale BM, Nevanlinna H, Neven P, Newman AB, Nordestgaard BG, Olson JE, Padmanabhan S, Peterlongo P, Peters U, Petersmann A, Peto J, Pharoah PDP, Pirastu NN, Pirie A, Pistis G, Polasek O, Porteous D, Psaty BM, Pylkäs K, Radice P, Raffel LJ, Rivadeneira F, Rudan I, Rudolph A, Ruggiero D, Sala CF, Sanna S, Sawyer EJ, Schlessinger D, Schmidt MK, Schmidt F, Schmutzler RK, Schoemaker MJ, Scott RA, Seynaeve CM, Simard J, Sorice R, Southey MC, Stöckl D, Strauch K, Swerdlow A, Taylor KD, Thorsteinsdottir U, Toland AE, Tomlinson I, Truong T, Tryggvadottir L, Turner ST, Vozzi D, Wang Q, Wellons M, Willemsen G, Wilson JF, Winqvist R, Wolffenbuttel BBHR, Wright AF, Yannoukakos D, Zemunik T, Zheng W, Zygmunt M, Bergmann S, Boomsma DI, Buring JE, Ferrucci L, Montgomery GW, Gudnason V, Spector TD, van Duijn CM, Alizadeh BZ, Ciullo M, Crisponi L, Easton DF, Gasparini PP, Gieger C, Harris TB, Hayward C, Kardia SLR, Kraft P, McKnight B, Metspalu A, Morrison AC, Reiner AP, Ridker PM, Rotter JI, Toniolo D, Uitterlinden AG, Ulivi S, Völzke H, Wareham NJ, Weir DR, Yerges-Armstrong LM, Price AL, Stefansson K, Visser JA, Ong KK, Chang-Claude J, Murabito JM, Perry JRB, Murray A, consortium P, Investigators k, Investigators A, Scotland G, Consortium E-I, Study LC (2015) Large-scale genomic analyses link reproductive aging to hypothalamic signaling, breast cancer susceptibility and BRCA1-mediated DNA repair. Nat Genet 47(11):1294–1303
Sancar A, Lindsey-Boltz LA, Unsal-Kaçmaz K, Linn S (2004) Molecular mechanisms of mammalian DNA repair and the DNA damage checkpoints. Annu Rev Biochem 73:39–85
Titus S, Li F, Stobezki R, Akula K, Unsal E, Jeong K, Dickler M, Robson M, Moy F, Goswami S, Oktay K (2013) Impairment of BRCA1-related DNA double-strand break repair leads to ovarian aging in mice and humans. Sci Transl Med 5(172):172ra121
Winship AL, Stringer JM, Liew SH, Hutt KJ (2018) The importance of DNA repair for maintaining oocyte quality in response to anti-cancer treatments, environmental toxins and maternal ageing. Hum Reprod Update 24(2):119–134
Oktay K, Turan V, Titus S, Stobezki R, Liu L (2015) BRCA mutations, DNA repair deficiency, and ovarian aging. Biol Reprod 93(3):67
Kerr JB, Hutt KJ, Cook M, Speed TP, Strasser A, Findlay JK, Scott CL (2012) Cisplatin-induced primordial follicle oocyte killing and loss of fertility are not prevented by imatinib. Nat Med 18(8):1170–1172; author reply 1172-1174
Lieber MR (2010) The mechanism of double-strand DNA break repair by the nonhomologous DNA end-joining pathway. Annu Rev Biochem 79:181–211
John GB, Gallardo TD, Shirley LJ, Castrillon DH (2008) Foxo3 is a PI3K-dependent molecular switch controlling the initiation of oocyte growth. Dev Biol 321(1):197–204
John GB, Shirley LJ, Gallardo TD, Castrillon DH (2007) Specificity of the requirement for Foxo3 in primordial follicle activation. Reproduction 133(5):855–863
Hosaka T, Biggs WH, Tieu D, Boyer AD, Varki NM, Cavenee WK, Arden KC (2004) Disruption of forkhead transcription factor (FOXO) family members in mice reveals their functional diversification. Proc Natl Acad Sci U S A 101(9):2975–2980
Zhang BF, Hu Y, Liu X, Cheng Z, Lei Y, Liu Y, Zhao X, Mu M, Yu L, Cheng ML (2018) The role of AKT and FOXO3 in preventing ovarian toxicity induced by cyclophosphamide. PLoS One 13(8):e0201136
Reddy P, Liu L, Adhikari D, Jagarlamudi K, Rajareddy S, Shen Y, Du C, Tang W, Hämäläinen T, Peng SL, Lan ZJ, Cooney AJ, Huhtaniemi I, Liu K (2008) Oocyte-specific deletion of Pten causes premature activation of the primordial follicle pool. Science 319(5863):611–613
Kawamura K, Cheng Y, Suzuki N, Deguchi M, Sato Y, Takae S, Ho CH, Kawamura N, Tamura M, Hashimoto S, Sugishita Y, Morimoto Y, Hosoi Y, Yoshioka N, Ishizuka B, Hsueh AJ (2013) Hippo signaling disruption and Akt stimulation of ovarian follicles for infertility treatment. Proc Natl Acad Sci U S A 110(43):17474–17479
Cheng Y, Feng Y, Jansson L, Sato Y, Deguchi M, Kawamura K, Hsueh AJ (2015) Actin polymerization-enhancing drugs promote ovarian follicle growth mediated by the Hippo signaling effector YAP. FASEB J 29(6):2423–2430
Suzuki N, Yoshioka N, Takae S, Sugishita Y, Tamura M, Hashimoto S, Morimoto Y, Kawamura K (2015) Successful fertility preservation following ovarian tissue vitrification in patients with primary ovarian insufficiency. Hum Reprod 30(3):608–615
Lee HN, Chang EM (2019) Primordial follicle activation as new treatment for primary ovarian insufficiency. Clin Exp Reprod Med 46(2):43–49
Nombela-Arrieta C, Ritz J, Silberstein LE (2011) The elusive nature and function of mesenchymal stem cells. Nat Rev Mol Cell Biol 12(2):126–131
Dominici M, Le Blanc K, Mueller I, Slaper-Cortenbach I, Marini F, Krause D, Deans R, Keating A, Prockop D, Horwitz E (2006) Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy 8(4):315–317
Johnson J, Bagley J, Skaznik-Wikiel M, Lee HJ, Adams GB, Niikura Y, Tschudy KS, Tilly JC, Cortes ML, Forkert R, Spitzer T, Iacomini J, Scadden DT, Tilly JL (2005) Oocyte generation in adult mammalian ovaries by putative germ cells in bone marrow and peripheral blood. Cell 122(2):303–315
Sun M, Wang S, Li Y, Yu L, Gu F, Wang C, Yao Y (2013) Adipose-derived stem cells improved mouse ovary function after chemotherapy-induced ovary failure. Stem Cell Res Ther 4(4):80
Takehara Y, Yabuuchi A, Ezoe K, Kuroda T, Yamadera R, Sano C, Murata N, Aida T, Nakama K, Aono F, Aoyama N, Kato K, Kato O (2013) The restorative effects of adipose-derived mesenchymal stem cells on damaged ovarian function. Lab Invest 93(2):181–193
Lai D, Wang F, Chen Y, Wang L, Wang Y, Cheng W (2013) Human amniotic fluid stem cells have a potential to recover ovarian function in mice with chemotherapy-induced sterility. BMC Dev Biol 13:34
Wang F, Wang L, Yao X, Lai D, Guo L (2013) Human amniotic epithelial cells can differentiate into granulosa cells and restore folliculogenesis in a mouse model of chemotherapy-induced premature ovarian failure. Stem Cell Res Ther 4(5):124
Yin N, Zhao W, Luo Q, Yuan W, Luan X, Zhang H (2018) Restoring ovarian function with human placenta-derived mesenchymal stem cells in autoimmune-induced premature ovarian failure mice mediated by treg cells and associated cytokines. Reprod Sci 25(7):1073–1082
Yang Z, Du X, Wang C, Zhang J, Liu C, Li Y, Jiang H (2019) Therapeutic effects of human umbilical cord mesenchymal stem cell-derived microvesicles on premature ovarian insufficiency in mice. Stem Cell Res Ther 10(1):250
Liu T, Huang Y, Zhang J, Qin W, Chi H, Chen J, Yu Z, Chen C (2014) Transplantation of human menstrual blood stem cells to treat premature ovarian failure in mouse model. Stem Cells Dev 23(13):1548–1557
Lai D, Wang F, Yao X, Zhang Q, Wu X, Xiang C (2015) Human endometrial mesenchymal stem cells restore ovarian function through improving the renewal of germline stem cells in a mouse model of premature ovarian failure. J Transl Med 13:155
Togel F, Hu Z, Weiss K, Isaac J, Lange C, Westenfelder C (2005) Administered mesenchymal stem cells protect against ischemic acute renal failure through differentiation-independent mechanisms. Am J Physiol Renal Physiol 289(1):F31–F42
Ortiz LA, Dutreil M, Fattman C, Pandey AC, Torres G, Go K, Phinney DG (2007) Interleukin 1 receptor antagonist mediates the antiinflammatory and antifibrotic effect of mesenchymal stem cells during lung injury. Proc Natl Acad Sci U S A 104(26):11002–11007
Gupta N, Su X, Popov B, Lee JW, Serikov V, Matthay MA (2007) Intrapulmonary delivery of bone marrow-derived mesenchymal stem cells improves survival and attenuates endotoxin-induced acute lung injury in mice. J Immunol 179(3):1855–1863
Lee RH, Pulin AA, Seo MJ, Kota DJ, Ylostalo J, Larson BL, Semprun-Prieto L, Delafontaine P, Prockop DJ (2009) Intravenous hMSCs improve myocardial infarction in mice because cells embolized in lung are activated to secrete the anti-inflammatory protein TSG-6. Cell Stem Cell 5(1):54–63
Sheikh AM, Nagai A, Wakabayashi K, Narantuya D, Kobayashi S, Yamaguchi S, Kim SU (2011) Mesenchymal stem cell transplantation modulates neuroinflammation in focal cerebral ischemia: contribution of fractalkine and IL-5. Neurobiol Dis 41(3):717–724
Lee DK, Song SU (2018) Immunomodulatory mechanisms of mesenchymal stem cells and their therapeutic applications. Cell Immunol 326:68–76
Uccelli A, Moretta L, Pistoia V (2008) Mesenchymal stem cells in health and disease. Nat Rev Immunol 8(9):726–736
Wang S, Yu L, Sun M, Mu S, Wang C, Wang D, Yao Y (2013) The therapeutic potential of umbilical cord mesenchymal stem cells in mice premature ovarian failure. Biomed Res Int 2013:690491
Wang Z, Wang Y, Yang T, Li J, Yang X (2017) Study of the reparative effects of menstrual-derived stem cells on premature ovarian failure in mice. Stem Cell Res Ther 8(1):11
Ding L, Yan G, Wang B, Xu L, Gu Y, Ru T, Cui X, Lei L, Liu J, Sheng X, Zhang C, Yang Y, Jiang R, Zhou J, Kong N, Lu F, Zhou H, Zhao Y, Chen B, Hu Y, Dai J, Sun H (2018) Transplantation of UC-MSCs on collagen scaffold activates follicles in dormant ovaries of POF patients with long history of infertility. Sci China Life Sci 61(12):1554–1565
Ciccocioppo R, Cantore A, Chaimov D, Orlando G (2019) Regenerative medicine: the red planet for clinicians. Intern Emerg Med 14(6):911–921
Na J, Kim GJ (2020) Recent trends in stem cell therapy for premature ovarian insufficiency and its therapeutic potential: a review. J Ovarian Res 13(1):74
Herraiz S, Romeu M, Buigues A, Martinez S, Diaz-Garcia C, Gomez-Segui I, Martinez J, Pellicer N, Pellicer A (2018) Autologous stem cell ovarian transplantation to increase reproductive potential in patients who are poor responders. Fertil Steril 110(3):496–505 e491
Yan L, Wu Y, Li L, Wu J, Zhao F, Gao Z, Liu W, Li T, Fan Y, Hao J, Liu J, Wang H (2020) Clinical analysis of human umbilical cord mesenchymal stem cell allotransplantation in patients with premature ovarian insufficiency. Cell Prolif 53(12):e12938
Gupta S, Lodha P, Karthick MS, Tandulwadkar SR (2018) Role of autologous bone marrow-derived stem cell therapy for follicular recruitment in premature ovarian insufficiency: review of literature and a case report of world's first baby with ovarian autologous stem cell therapy in a perimenopausal woman of age 45 year. J Hum Reprod Sci 11(2):125–130
He Y, Chen D, Yang L, Hou Q, Ma H, Xu X (2018) The therapeutic potential of bone marrow mesenchymal stem cells in premature ovarian failure. Stem Cell Res Ther 9(1):263
Song D, Zhong Y, Qian C, Zou Q, Ou J, Shi Y, Gao L, Wang G, Liu Z, Li H, Ding H, Wu H, Wang F, Wang J (2016) Human umbilical cord mesenchymal stem cells therapy in cyclophosphamide-induced premature ovarian failure rat model. Biomed Res Int 2016:2517514
Zhang Q, Bu S, Sun J, Xu M, Yao X, He K, Lai D (2017) Paracrine effects of human amniotic epithelial cells protect against chemotherapy-induced ovarian damage. Stem Cell Res Ther 8(1):270
Ling L, Feng X, Wei T, Wang Y, Wang Z, Tang D, Luo Y, Xiong Z (2019) Human amnion-derived mesenchymal stem cell (hAD-MSC) transplantation improves ovarian function in rats with premature ovarian insufficiency (POI) at least partly through a paracrine mechanism. Stem Cell Res Ther 10(1):46
Ding C, Zou Q, Wu Y, Lu J, Qian C, Li H, Huang B (2020) EGF released from human placental mesenchymal stem cells improves premature ovarian insufficiency via NRF2/HO-1 activation. Aging (Albany NY) 12(3):2992–3009
Guo JQ, Gao X, Lin ZJ, Wu WZ, Huang LH, Dong HY, Chen J, Lu J, Fu YF, Wang J, Ma YJ, Chen XW, Wu ZX, He FQ, Yang SL, Liao LM, Zheng F, Tan JM (2013) BMSCs reduce rat granulosa cell apoptosis induced by cisplatin and perimenopause. BMC Cell Biol 14:18
Fu X, He Y, Xie C, Liu W (2008) Bone marrow mesenchymal stem cell transplantation improves ovarian function and structure in rats with chemotherapy-induced ovarian damage. Cytotherapy 10(4):353–363
Fu X, He Y, Wang X, Peng D, Chen X, Li X, Wang Q (2017) Overexpression of miR-21 in stem cells improves ovarian structure and function in rats with chemotherapy-induced ovarian damage by targeting PDCD4 and PTEN to inhibit granulosa cell apoptosis. Stem Cell Res Ther 8(1):187
Yin N, Wang Y, Lu X, Liu R, Zhang L, Zhao W, Yuan W, Luo Q, Wu H, Luan X, Zhang H (2018) hPMSC transplantation restoring ovarian function in premature ovarian failure mice is associated with change of Th17/Tc17 and Th17/Treg cell ratios through the PI3K/Akt signal pathway. Stem Cell Res Ther 9(1):37
Zhang Q, Xu M, Yao X, Li T, Wang Q, Lai D (2015) Human amniotic epithelial cells inhibit granulosa cell apoptosis induced by chemotherapy and restore the fertility. Stem Cell Res Ther 6:152
Xia X, Yin T, Yan J, Yan L, Jin C, Lu C, Wang T, Zhu X, Zhi X, Wang J, Tian L, Liu J, Li R, Qiao J (2015) Mesenchymal stem cells enhance angiogenesis and follicle survival in human cryopreserved ovarian cortex transplantation. Cell Transplant 24(10):1999–2010
Huang B, Ding C, Zou Q, Lu J, Wang W, Li H (2020) Human amniotic fluid mesenchymal stem cells improve ovarian function during physiological aging by resisting dna damage. Front Pharmacol 11:272
Code availability
Not applicable
Funding
Regenerative Medicine Minnesota to IC
Author information
Authors and Affiliations
Contributions
AT performed the literature search and wrote the first draft. All authors contributed to manuscript editing. AY and LH wrote a chapter about clinical management and reviewed the final draft. IC conceived the article, edited all drafts, received funding, and reviewed the final draft.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Takahashi, A., Yousif, A., Hong, L. et al. Premature ovarian insufficiency: pathogenesis and therapeutic potential of mesenchymal stem cell. J Mol Med 99, 637–650 (2021). https://doi.org/10.1007/s00109-021-02055-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00109-021-02055-5