Abstract
In blood, the primary role of RBCs is to transport oxygen via highly regulated mechanisms involving hemoglobin (Hb). Hb is a tetrameric porphyrin protein comprising of two α- and two β-polypeptide chains, each containing an iron-containing heme group capable of binding one oxygen molecule. In military as well as civilian trauma, exsanguinating hemorrhage can lead to suboptimal tissue oxygenation and subsequent morbidity and mortality. In such cases, transfusion of whole blood or RBCs can significantly improve survival. However, blood products including RBCs have limited availability and portability and present additional challenges related to type matching, pathogenic contamination risks, and short shelf-life. These issues lead to substantial logistical barriers to their pre-hospital use in austere battlefield and remote civilian conditions. While robust efforts are underway to resolve these issues, recent research breakthroughs have led to bioinspired engineering of RBC surrogates, using various cross-linked, polymeric, and encapsulated forms of Hb. These “next-generation” Hb-based oxygen carriers (HBOCs) can potentially provide therapeutic oxygenation when whole blood or RBCs are not available. Several of these HBOCs have undergone rigorous pre-clinical and clinical evaluation, but have not yet received clinical approval in the USA for human use. This chapter will comprehensively review both historical and new HBOC designs, including current state-of-the-art and novel molecules in development, along with a critical discussion of successes and challenges in this field.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
In austere battlefield conditions and remote civilian locations, trauma-associated uncontrolled hemorrhage and acute coagulopathy remain one of the leading causes of mortality [1,2,3,4,5,6]. In such scenarios, transfusion of whole blood and blood components (e.g., RBCs, platelets, and plasma), as per Damage Control Resuscitation (DCR) guidelines, can significantly reduce trauma-associated morbidities and mortalities [7,8,9]. However, the limited availability and portability, special storage requirements, and high contamination risks of these blood products present severe logistical challenges that preclude facile, ubiquitous pre-hospital application in military and civilian scenarios, for either immediate (e.g., point-of-injury or en route) or prolonged field (e.g., extended, in place) care at the point-of-injury [10,11,12,13,14,15,16,17]. A robust volume of research is currently being dedicated toward resolving these issues and enhancing the availability and applicability of donor-derived blood products in the field [18,19,20,21]. In parallel, enabled by transformative advances in the areas of synthetic chemistry, biomaterials, and nanofabrication, an exciting area of research has emerged that focuses on the development and evaluation of semisynthetic or synthetic “bioinspired” surrogates of blood products that can be manufactured at large scale (i.e., sufficient availability); can be sterilized without compromising biofunction, and stored as small volume deliverables over long periods of time across broad ambient temperature ranges and environmental conditions (i.e., easy storage and portability); can be easily reconstituted and administered “on demand” in far-forward scenarios (i.e., pre-hospital applicability); can potentially avoid the need for type matching (universal application with minimal immunogenic risk); can circulate safely upon intravascular administration without systemic risks; and can mimic, leverage, and amplify endogenous mechanisms of blood component function to mitigate the effects of traumatic exsanguinating hemorrhage [22,23,24]. This field of research has developed in the areas of functionally mimicking blood’s cellular as well as non-cellular components and continues to focus on resolving translational challenges with regard to biocompatibility, safety, pre-hospital availability, and universal applicability.
The research endeavors on preserving and transporting donor-derived blood started during World War I, and blood transfusions became widely available by World War II. Based on this advance, multiple blood banks were established in the USA from the 1950s onward, and blood donation was promoted as a form of civic responsibility. Subsequent development of processes and methodologies for isolation and storage of various blood components has significantly enhanced utilization of whole blood and its components. Currently, transfusions of whole blood as well as various isolated components are clinically approved for application in civilian and battlefield trauma (e.g., in Damage Control Resuscitation), surgical settings (e.g., transplants), chronic and acute anemias, and disease-associated, drug-induced, or congenital bleeding disorders [25,26,27,28,29,30,31,32]. RBC transfusion is clinically significant in efficient mitigation of hemorrhagic shock, as part of the Massive Transfusion Protocol (MTP) in hypoperfused patients with critically limited oxygen delivery [33,34,35,36,37]. It has also been demonstrated that pre-hospital use of RBC transfusion (if available) can significantly improve survival in critically injured subjects [38, 39]. Such transfusions are dependent on donor-derived RBC products (e.g., packed Red Blood Cell or pRBC). However, according to the Red Cross, only ~40% of US population is eligible to donate blood at any given time, and only 10–15% actually donate. In addition, blood-based products have formally limited shelf-life due to accrual of processing and storage-related damage as well as risks of pathogenic contamination. Currently, RBCs have a maximum shelf-life of 42 days, while platelet suspensions have a shelf-life of 5 days, at room temperature [40]. Also, RBCs (and platelets) develop storage lesions over time, which affect their stability, in vivo circulation lifetime, and post-transfusion physiology [41, 42]. Significant research is underway to enhance the shelf-life of blood products by cold storage, freezing, lyophilization, etc. and to develop pathogen reduction technologies like psoralen-based or riboflavin-based UV irradiation, as well as extensive serological testing of donor blood, leukoreduction, and specialized storage protocols [13, 19, 31, 43,44,45,46,47,48]. Nevertheless, portability of blood products, especially to remote battlefield and civilian locations, especially for pre-hospital point-of-care use, continues to be a major logistical challenge [14, 17, 49].
Such challenges can be potentially addressed by bioinspired engineering of semisynthetic or synthetic surrogates of blood components [22, 50, 51]. In fact, major interest in such synthetic surrogates developed during the HIV crisis of the 1980s due to fear of contaminated blood products, and this research has been ongoing, with several designs and products that have progressed through pre-clinical and clinical evaluations. However, currently no such product is clinically approved by the FDA for human applications in the USA, although certain products have been approved for human use in South Africa and, under special circumstances, dispensed for compassionate use provision in the USA and Europe. Of note, a 2008 meta-analysis of 16 clinical trials of 5 different HBOCs indicated increased risk of both myocardial infarction and death in subjects who received such products [52]. Although this report raised significant concern with regard to the clinical safety and utility of these particular HBOCs, the design of this analysis has been debated and, importantly, this work has directed significant re-emphasis to better understanding the pros and cons of these products at fundamental physiological and mechanistic levels. To this end, the current categorization of such products has shifted from “blood substitutes” to “oxygenation therapeutics” so as to emphasize the important role of such products in scenarios where donor-derived RBCs may not be sufficiently available (e.g., far-forward military setting) as well as for niche scenarios, such as ex vivo perfusion of transplantable organs. In this framework, we will focus on reviewing “hemoglobin-based oxygen carriers” (HBOCs) , comprehensively discussing relevant designs, current state-of-art and novel molecules in development, along with emphasizing criteria for successes and challenges.
Hemoglobin (Hb) Function in RBCs for Oxygen Transport
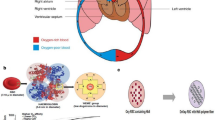
In blood, the primary function of RBCs is the transport of oxygen (O2) and to some extent carbon dioxide (CO2) to and from tissues, by virtue of binding of the gases to hemoglobin (Hb) within RBCs. The average amount of Hb in adult human RBCs (mean corpuscular hemoglobin, or MCH) is 27–31 picograms per cell (~250 million Hb molecules). Hb is a tetrameric protein comprised by two α- and two β-polypeptide chains, each bearing an iron-containing heme prosthetic group that is capable of reversibly binding one oxygen molecule (O2). Figure 11.1a shows a multi-scale representation of an RBC, Hb within an RBC, and the chemical structure of an iron-containing “heme” group within Hb. The O2-binding kinetics to Hb is positively cooperative, such that a small variation in oxygen partial pressure (pO2) as blood transits from lung to tissue (Fig. 11.1b) results in a large change in oxygen that is captured (in lung) and then released (in tissue) by Hb as exhibited by the classic sigmoidal shape of the O2-binding equilibrium curve (OEC, Fig. 11.1c) [53, 54]. O2-carrying iron in Hb is in its reduced “ferrous” (Fe2+) state. Approximately 10% of the O2 molecules release as superoxide, generating methemoglobin (MetHb), in which the iron is oxidized to the “ferric” state (Fe3+) and rendered unable to bind oxygen [55]—this process is accelerated in the setting of increased O2 delivery and/or during other conditions characterized by oxidative stress. Due to this reason, in RBCs, Hb oxygenation/deoxygenation cycling is closely coupled to RBC energetics and anti-oxidant systems (e.g., driven by enzyme NAD-cytochrome b5 reductase), such that the Fe2+-containing Hb is maintained in its O2-binding state. Failure to reverse MetHb formation not only diminishes oxygen-carrying capacity, but the cooperativity is also impaired, leading to increased O2 affinity for remaining ferrous hemes (in “partial met” tetramers), and this also leads to dysregulated vascular tone and inflammatory reactions. Furthermore, Hb in RBCs have the unique capability to undergo conformational changes to allow O2 saturation (loading) in the lungs (higher O2 affinity) and then O2 release in tissue (lower O2 affinity). This reversible conformational regulation of O2-binding affinity of Hb is aided by allosteric effector molecules like 2,3-diphosphoglycerate (2,3-DPG), which forms in RBCs as a glycolytic intermediate. Therefore, maintaining such oxygen-carrying thermodynamic and kinetic characteristics of Hb is one of the important and challenging design considerations in the context of developing a “bioinspired” Hb-based RBC surrogate [56]. In this context, an essential factor is to maintain the intraerythrocytic physicochemical milieu of Hb, since outside of the protective RBC environment (i.e., in plasma, which fundamentally differs from that in RBCs with regard to pH, redox potential, key ion/small molecule abundance, etc.), the Hb tetramer is prone to rapidly oxidize and disassemble into its dimeric and monomeric protein units, which in turn results in rapid clearance from circulation into extravascular space and kidneys. This results in reduced circulation residence time and increased risk of nephrotoxicity. Extraerythrocytic Hb is also devoid of oxygen affinity regulatory effectors, such as 2,3-DPG, as well as protective anti-oxidant enzymes and reducing equivalents. As a result, free Hb in plasma exhibits dysregulated tissue oxygenation capacity compared to RBC-encapsulated Hb and is also prone to rapid MetHb accrual (without reversal systems available in RBCs), thereby degrading its oxygen transport ability. Unencapsulated Hb is also a potent nitric oxide (NO) scavenger, which is produced by endothelial cells as a principle effector molecule to achieve vasodilation in response to multiple physiologic reflexes that optimize tissue perfusion; notably, this pathologic Hb-NO interaction has been implicated in hypertensive and (paradoxical) perfusion-limiting side effects of unencapsulated Hb. Hence, providing efficient tissue oxygenation while maintaining reasonable circulation lifetime, minimizing hypertensive side effects, and avoiding Hb-induced toxicity are the three prominent design requirements for HBOCs. The following sections review and discuss the various design approaches that attempt to address these requirements.
(a) Multi-scale representation of RBCs and Hemoglobin (Hb), showing a scanning electron micrograph (SEM) image of RBC depicting the biconcave discoid structure, along with sequential schematic of RBC structure, Hb structure, and “Heme” structure; (b) shows a schematic of RBC movement between lung (oxygen loading site) and tissue (oxygen off-loading site), while (c) shows corresponding oxygen equilibrium curve (OEC) characteristics of Hb. (From 2017 Military Supplement: Hemoglobin-based Oxygen Carriers Current State-of-the-Art and Novel Molecules, Anirban Gupta, Shock Injury, Inflammation and Sepsis, Oct 3, 2018, Publish Ahead of Print, Figs. 1–4, with permission of Wolters Kluwer Health, Inc.)
Hb-Based Oxygen Carrier (HBOC) Systems
HBOCs are semisynthetic systems that utilize biologically generated Hb as the oxygen-carrying component and are formulated either as chemically modified cell-free suspensions or conjugated and cross-linked with polymers along with protective enzymes or encapsulated within microparticulate or nanoparticulate vehicles [51, 57]. The Hb used in these systems is usually derived from outdated human or bovine RBCs or from recombinant sources [57,58,59,60,61,62,63]. In the case of outdated human or bovine RBCs, the Hb is isolated via cell lysis, purified by sterile filtration and chromatographic techniques, and sterilized (e.g., by low heat) [64]. Using cell-free Hb presents the advantage of minimum antigenicity and improved oxygen diffusivity, due to the lack of interference by cell membrane. In fact, reported in the early twentieth century, suspension of cell-free Hb in lactated Ringer’s solution was used to intravenously treat 15 patients; however, a large number of them developed renal toxicity and cardiovascular complications [64]. Similar results were also found in the 1950s when US Navy treated several patients with cell-free Hb [65]. Cell-free Hb was also found to have a very short circulatory residence time because the Hb tetramer rapidly dissociates into dimeric and monomeric forms that can bind non-specifically to plasma proteins or are captured by scavenging proteins devoted to this purpose (haptoglobin, hemopexin) and thus undergo rapid clearance by the reticulo-endothelial system (RES) into spleen and liver, as well as renal clearance into kidneys, leading to Hb-induced toxicities in these organs [66, 67]. Additionally, cell-free Hb and its dissociated derivatives can also extravasate into the subendothelial domain of the circulatory system and rapidly sequester nitric oxide (NO), resulting in its conversion into nitrate (dioxygenation reaction) and of oxy-Hb to MetHb [68]. NO is an essential endogenous vasodilator (e.g., endothelial-derived relaxant factor) and therefore such NO scavenging results in vasoconstriction and cardiovascular complications, paradoxically, thereby diminishing tissue O2 delivery. Furthermore, 2,3-DPG absence in plasma (as well as lack of Bohr and Haldane-based OEC “shifting,” which is enabled in “intact” RBCs) leads to unnaturally high cell-free Hb oxygen affinity, limiting O2 off-loading across physiologic O2 gradients—further diminishing tissue O2 delivery. Cell-free Hb can also change blood osmolarity, leading to alteration of blood volumes and associated side effects. Altogether, for these reasons, cell-free human Hb appears problematic for in vivo oxygen-carrying applications. Instead of human Hb, studies have also been conducted with bovine Hb, but this also presents similar issues of stability, extravasation, NO scavenging, and renal clearance and toxicity. Historically, an innovative approach to address some of these issues was by development of “designer” recombinant Hb (e.g., in E. coli) where targeted mutations decrease the likelihood of tetramer dissociation, optimize heme redox behavior, and modulate propensity for NO consumption, but an optimal combination of mutations that results in free-Hb performance similar to that observed for intraerythrocytic Hb remains elusive [69,70,71]. Recombinant technologies are also prohibitively expensive, in comparison to human or bovine sourcing for Hb. Therefore, a substantial volume of research has been directed to achieve in vivo stabilization and performance optimization via chemical modification of purified Hb utilizing techniques (alone or in combination) such as cross-linking, polymerization, and macromeric surface conjugations. The goals of these modifications are to reduce Hb dissociation, extravasation, and renal clearance, while maintaining reasonable circulation lifetime and O2-transport capacities.
Chemically Modified HBOCs
Hb tetramers can be cross-linked both intra- and intermolecularly. For example, intramolecular cross-linking in human Hb formed between its two α-subunits using acylation with bis-(3,5 dibromosalicyl)-fumarate (also known as Diaspirin) led to a product called HemAssist from Baxter, USA [57, 72, 73]. This product showed an increase in circulation residence time up to 12 h compared to <6 h for unmodified Hb, but in human trials, cross-linked Hb unfortunately led to a 72% increase in mortality compared to saline, and clinical trials were discontinued [74]. An analogous approach to cross-link the α-subunits of recombinant Hb using Glycine led to a product called Optro from Somatogen, USA, but this also resulted in increased risks of cardiac arrest and mortality [75,76,77]. Instead of site-specific intramolecular cross-linking only, polymerized Hb has also been created from using bifunctional cross-linking reagents like glutaraldehyde-based cross-linking of bovine Hb (e.g., Hemopure originally from Biopure, USA, now HbO2 Therapeutics, USA) or human Hb (e.g., PolyHeme from Northfield Labs, USA) and o-raffinose-based cross-linking of human Hb (e.g., the product HemoLink from Hemosol, Canada) [78, 79]. Such polymeric cross-linking creates higher-molecular-weight cell-free Hb that retains “simple” oxygen-binding properties (physiologic OEC shifting is not retained) while minimizing dissociation and rapid clearance observed for unmodified Hb tetramers, when free in plasma. One challenge in these approaches is to precisely control polymer molecular weight and geometry, and rigorous purification steps are necessary to ensure product quality. PolyHeme was reported to progress into Phase III clinical trials in the USA in treating trauma-associated blood loss and showed a decreased need of natural blood transfusions [77]. Clinical trials with HemoPure also showed a reduced need of additional blood transfusions in cardiac surgery [80]. HemoPure has received clinical approval in South Africa and Russia for acutely anemic human patients and is occasionally used on a compassionate basis in the USA. An analogous product from the same company (HbO2 Therapeutics, USA) called Oxyglobin is currently approved in the USA for veterinary use, but has not gained widespread acceptance. HemoLink also advanced to Phase III clinical trials but was discontinued in 2003 when patients receiving treatment experienced adverse cardiac events. In fact, as noted in the meta-analysis which led to FDA stopping clinical trials for this HBOC class, all of these products in their clinical studies have shown various degrees of transient hypertension, organ damage through microvascular constriction and dysfunction, gastro-intestinal distress, nephrotoxicity, neurotoxicity, and increased mortality [52, 80,81,82].
Instead of intramolecular cross-linking and intermolecular polymerization , Hb modification has also been carried out with macromeric bioconjugation to increase stability and vascular residence time while reducing immune recognition [83,84,85]. Important examples of this approach are found in polyethylene glycol (PEG) modification (e.g., the products Hemospan from Sangart Inc., USA, and PEG-Hb from Enzon, USA) and poly(oxyethylene) modification of pyridoxylated cross-linked Hb (e.g., the product PHP from Apex Bioscience, USA). PEG-ylated Hb products have undergone extensive clinical trials, and the studies showed risks of bradycardia and elevation of hepatic pancreatic enzymes even at low doses [86]. Nonetheless, the Phase I and Phase II clinical trials showed that Hemospan was well tolerated in humans for efficient oxygen delivery, and Phase III trials in orthopedic surgery patients were carried out in Europe [87]. The trials suggested that the risk of cardiovascular and renal dysfunction still persisted with such chemically modified Hb products. During the past two decades, it has been identified that cell-free Hb (including chemically modified versions) are potent scavengers of nitric oxide (NO) via rapid irreversible binding (rate constant ~107 M−1 s−1), which in turn can affect systemic and pulmonary vascular tone, resulting in vasoconstriction, hypertension, and lowering of cardiac output [88, 89]. A resolution of this issue has been attempted by (NO pre-loading) Hb modifications, such as S-nitrosylation of cysteine residues in the β-subunits of Hb; however, this approach is critically constrained by natural limits imposed by simple stoichiometry [90]. Of note, RBCs contain anti-oxidant enzymes, such as catalase (CAT) and superoxide dismutase (SOD) that mitigate oxidative stress arising from Hb-generated superoxide. In an interesting approach, these enzymes have been cross-linked to polymerized Hb to form PolyHb-SOD-CAT, which has shown combined advantages of long circulation time and reduced oxidative damage [91, 92]. Another interesting approach is to incorporate regulatory molecules such as 2,3-DPG and methemoglobin reductase along with Hb in appropriate HBOC systems, to prevent hemoglobin oxidation [93]. In recent years, a product named HemoTech has been reported that uses purified bovine Hb cross-linked intramolecularly with ATP and intermolecularly with adenosine, and conjugated with reduced glutathione (GSH) [94]. This unique design employs pharmacologically active molecules (ATP, adenosine, and GSH) as the chemical modifiers, in that ATP is intended to regulate vascular tone through purinergic receptors, adenosine is intended to counteract the Hb-based vasoconstriction via stimulating adenosine receptors, and GSH is intended to protect heme from NO and various reactive oxygen species. Pre-clinical and early-phase clinical studies have shown that HemoTech works as an effective oxygen carrier in treating blood loss, anemia, and ischemic vascular conditions, and further studies are warranted [95]. Another polymeric Hb reported in recent years is OxyVita®, which is produced through modification of a zero-linked polymerization mechanism using carbodiimide chemistry on bovine tetramer hemoglobin to produce “super-polymeric” macromolecules [96]. In yet another recent approach, a polynitroxylated PEG-ylated hemoglobin (PNPH) nanostructure design has been reported, named VitalHeme™ (SynZyme Technologies LLC, Irvine, CA), where PEG-ylated hemoglobin is covalently modified with catalytic-caged NO [97]. These designs reportedly allow for higher Hb stability in vivo and are currently under pre-clinical investigation. Figure 11.2 shows some of the prominent designs based on chemical modification of cell-free Hb that have undergone (or are still undergoing) pre-clinical and clinical evaluation for oxygen transport. In spite of promising pre-clinical results, many of the chemically modified Hb products have been withdrawn from clinical studies and discontinued in production, due to indication of clinical risks stemming from chemical heterogeneity and variable stability of final product, suboptimal vascular residence time, non-ideal oxygen loading and off-loading capabilities, rapid irreversible conversion to methemoglobin, and increased cardiovascular and renal dysfunction issues. While some of the newer products are refining their design and processing to address these issues, a “next-generation” approach has focused on Hb encapsulation within various micro- and nanocarrier vehicles, to more closely mimic the physiological encapsulated state of Hb in RBCs.
Representative approaches and design schematics for HBOCs based on chemical modification (cross-linking, surface modification, polymerization, etc.) of Hb that have undergone significant pre-clinical and clinical evaluation. (From 2017 Military Supplement: Hemoglobin-based Oxygen Carriers Current State-of-the-Art and Novel Molecules, Anirban Gupta, Shock Injury, Inflammation and Sepsis, Oct 3, 2018, Publish Ahead of Print, Figs. 1–4, with permission of Wolters Kluwer Health, Inc.)
Encapsulated HBOC Systems
During the past two decades, particulate drug delivery platform technologies (microparticles and nanoparticles) have revolutionized the packaging and delivery of pharmaceutical compounds, by encapsulating active compounds/biologics to protect them from plasma-induced effects, increase their circulation time, and allow sustained availability to cells, tissues, and organs. This design concept has also been adapted to create HBOCs that encapsulate Hb within suitable particulate vehicles. In fact, the pioneering concept and demonstration of “bio-artificial cells” was presented as early as the 1950s and 1960s by Chang and colleagues, by encapsulating Hb as well as other proteins and enzymes within polymeric membrane-based microvesicles. The membrane material originally used was collodion (cellulose nitrate) and later changed to biodegradable polyethylene glycol-polylactide (PEG-PLA) [98, 99]. These Hb-loaded microvesicles, aptly termed “hemoglobin corpuscles,” showed oxygen equilibrium curves similar to RBCs and also allowed coencapsulation and activity of RBC-relevant enzymes like 2,3-diphosphoglycerate (2,3-DPG), carbonic anhydrase, and CAT [100,101,102]. However, in these systems, a major challenge was posed by the rapid macrophagic uptake and clearance of these micrometer-sized vesicles from circulation, resulting in suboptimal circulation residence time for in vivo use. Reducing the diameter to ~1 micron only marginally improved the circulation lifetime, and a significant research effort has been directed toward further improving the vascular residence time by modifying the surface of the vesicles with lipids and polysaccharides. In another similar design approach, Djordjevich et al. reported on encapsulation of Hb in micron and submicron size lipid vesicles (liposome-encapsulated Hb or LEH), with membrane made of phospholipids and cholesterol [103,104,105]. A number of variations of this design have followed, e.g., “neohemocytes,” “TRM-645 Neo Red Cells,” etc., where the primary focus has been to maintain uniform Hb-encapsulation levels and uniform size distribution of the vesicles, minimize vesicle destabilization or fusion over time, and enhance storage stability of the vesicles while maintaining the RBC-analogous oxygen transport properties of the encapsulated Hb [106,107,108]. During the 1990s, the “Stealth Liposome” technology was clinically established, where lipid nanovesicles (100–200 nm in diameter) were surface-functionalized with polyethylene glycol (PEG) to enhance storage stability, reduce opsonization, and prevent rapid macrophagic uptake, and this significantly enhanced the circulation residence time [109, 110]. Consequently, this technology was adapted to form Hb-encapsulated PEG-ylated liposomal vesicles (HbV) [111,112,113]. 1,2-Dioctadecadienoyl-sn-glycero-3-phosphatidylcholine (DODPC) was used as the major membrane phospholipid for HbV preparation, such that γ-irradiation-induced radiolysis of water molecules in the vesicles generated hydroxy (-OH) radicals that promoted intermolecular polymerization of dienoyl groups to produce highly stable liposomes that could withstand freeze-thawing, freeze-drying, and rehydration processes . The HbV design has shown substantial improvement of circulation lifetime (~60 h in some animal models), and several refinements of this design have been recently reported [114,115,116,117,118]. The oxygen transport ability of these HbV systems was found to be similar to natural RBCs, with comparable oxygen saturation and release kinetics. Also, the liposomal encapsulation of Hb attenuated its NO scavenging effect and thereby appears to reduce the associated negative effects on vasculature. Hb encapsulation in liposomal vesicles also prevented glomerular clearance of Hb (since liposomes are too big for renal clearance) and therefore reduced nephrotoxicity. The current optimized HbV product contains about 30,000 Hb molecules encapsulated within one PEG-ylated liposomal vesicle of ~250 nm in diameter. In comparison, a natural RBC is ~7 μ in diameter and ~2 μ in thickness, containing about 250 million Hb molecules. HbVs have undergone extensive pre-clinical evaluation in suitable animal models for potential use as an RBC surrogate in transfusion and resuscitative mitigation of massive hemorrhagic shock and hemodilution incidents, and oxygenation of ischemic as well as transplanted tissues and organs. Although these studies have shown promise of HbVs as RBC surrogate oxygen carrier, these systems still present issues of broad size distribution of the vesicles, variation in Hb-encapsulation efficiencies, as well as variable pharmacokinetics and complement-mediated immune response in vivo. Further research is currently directed toward resolving these issues for potential clinical translation of HbV designs as well as other analogous designs of liposome-encapsulated hemoglobin (LEH) systems as RBC surrogates (114–118). Interestingly, instead of encapsulating Hb, others have attempted to encapsulate oxygen (O2) directly within phospholipid microvesicles (2–4 μm in diameter) to deliver O2 to deoxygenated RBCs in circulation [119, 120]. Although these oxygen-loaded microbubbles were found to be stable for a few weeks in storage with only small extent of oxygen loss, in vivo they were found to have a very short circulation lifetime (<1 h). Therefore, treatment with these systems would require multiple dosing, which may prompt negative effects of dysregulated oxidative stress and associated toxicity and immune response. Therefore, long-term safety profile of such technologies needs to be rigorously evaluated.
Encapsulation of Hb has also been studied in other microparticle and nanoparticle systems other than lipid vesicles. In pioneering work by Chang et al., Hb was encapsulated within polymeric nanoparticles (80–200 nm in diameter) made from PEG-PLA and analogous block-copolymers [121, 122]. These polymeric nanoparticles allow oxygen transport kinetics of Hb at levels similar to natural RBCs, and the polymeric material could be engineered to be biocompatible and biodegradable. Furthermore, enzymes that maintain the redox environment for Hb stability and function regulation (e.g., carbonic anhydrase, CAT, SOD, MetHb reductase, etc.) could also be encapsulated within the same nanoparticles toward further mimicry of “natural” RBCs [123]. This design approach has also been adopted for other polymer systems including poly(ε-caprolactone)/poly(L-lactic acid) (PCL/PLA) copolymers, poly(L-lysine) (PLL), poly(lactic-co-glycolic acid) (PLGA)/PEG copolymers, etc. [124, 125]. Amphiphilic block-copolymer systems also provide the ideal building blocks for designing polymer vesicles, otherwise known as polymersomes, analogous to liposomes. These polymersome systems have been recently utilized to create polymersome-encapsulated Hb (PEH) systems [126]. Hb loading in these PEH systems is reportedly 1–2 mg/mL, compared to human blood (i.e., within RBC) concentration of ~150 mg/mL. Utilization of hollow fiber-based membrane extrusion system has provided an automated way to manufacture these PEH systems [127]. These PEH systems are reportedly capable of encapsulating both bovine and human Hb, and have shown oxygen equilibrium kinetics and other biophysical parameters similar to RBCs. This suggests considerable promise toward the application of such PEH systems as RBC surrogates, but currently very limited in vivo evaluation data is available for these systems. A potential issue with polymersome systems may be their higher shell thickness compared to liposomes, which may increase oxygen diffusion time beyond the (low millisecond) time window required for physiologic gas exchange during circulatory transit. Modulation of polymer molecular weight of the shell components, and therefore of the shell thickness, can provide a unique way to influence oxygen flux properties of PEH systems. Higher stability of polymersomes compared to liposomes, both in storage and in vivo, is an additional advantage for use as Hb-encapsulated RBC surrogate systems. Ongoing and future studies with these systems should be directed toward establishment of batch-to-batch consistency, sterilization metric and storage stability evaluation, post-sterilization Hb bioactivity determination, in vivo pharmacokinetics and biodistribution determination, and therapeutic evaluation in appropriate animal models (e.g., hemorrhagic shock, ischemia, etc.). Figure 11.3 shows some representative designs and components for encapsulated Hb systems that have undergone and are currently still undergoing in vitro and in vivo evaluation for RBC-mimetic oxygen carrier application.
Representative approaches and design schematics for HBOCs based on encapsulation of Hb in microparticle and nanoparticle systems that have undergone significant pre-clinical evaluation and hold clinical promise. (From 2017 Military Supplement: Hemoglobin-based Oxygen Carriers Current State-of-the-Art and Novel Molecules, Anirban Gupta, Shock Injury, Inflammation and Sepsis, Oct 3, 2018, Publish Ahead of Print, Figs. 1–4, with permission of Wolters Kluwer Health, Inc.)
Novel Molecules and Designs Incorporating Hb as O2 Carrier
The focus of this section is to not distinguish between “chemically modified” and “encapsulated” Hb systems, but rather describe and review emerging novel designs and technologies that incorporate Hb for oxygen transport purposes. In one interesting approach, instead of Hb, PEG-ylation was carried out on bovine carboxyhemoglobin (CO-Hb), and the resultant PEG-CO-Hb system has been evaluated for oxygen transport (and CO transport) properties [128,129,130]. The rationale behind this design is that endogenous CO produced from (hypoxia-enhanced) heme-oxygenase activity is reported to render cytoprotective and homeostatic effects, such as inhibition of apoptosis and inflammation and reduction of oxidative stress and vasodilatory activity [131]. The PEG-CO-Hb product (Sanguinate, Prolong Pharmaceuticals, South Plainfield, New Jersey, USA) has undergone pre-clinical evaluation in small animal models, and is now in Phase I/II clinical trials for sickle cell anemia, thrombotic thrombocytopenic purpura (TTP), and ischemia after subarachnoid hemorrhage, with promising safety profile and oxygenation parameters . In another approach, core-shell cluster structures were formed by conjugating human serum albumin (HSA) on Hb using Hb surface lysines conjugated to HSA cysteine-34 using α-succinimidyl-ε-maleimide cross-linker [132]. These Hb-HSA clusters reported lower risk of rapid clearance and extravasation and thus improve circulation residence time. Further modification of these Hb-HSA core-shell nanoclusters was recently reported in which anti-oxidant enzymes and platinum nanoparticles were embedded in HSA pockets for Hb protection [133]. Thus far, this nanocluster design has been evaluated only in vitro, for oxygen-binding capacity, redox properties, and stability, with promising results. However, rigorous in vivo pharmacokinetics, toxicology, biodistribution, and oxygenation studies, along with demonstrating batch-to-batch compositional and functional consistency, are needed to establish in vivo utility. In another approach, Hb has been loaded in microparticles by coprecipitation with calcium carbonate (CaCO3), followed by glutaraldehyde cross-linking and CaCO3 dissolution, resulting in Hb payload density approaching that of RBCs [134]. However, although these Hb microparticles demonstrate oxygen equilibrium kinetics similar to free Hb (affinity too high for O2 release under physiologic conditions), the circulation lifetime is significantly extended, compared to free Hb. Analogous Hb microparticles carrying about 80% Hb content compared to RBCs have been reported where Hb and MnCO3 were coprecipitated, immediately followed by human serum albumin addition for encapsulation and stabilization of the particles [135]. These particles have shown reduced risks of NO scavenging and associated effect on vasoconstriction. In yet another recent approach, Hb was covalently conjugated directly to the hydrophobic or hydrophilic domain of block-copolymers, and the resultant conjugates were self-assembled to form Hb-loaded micelles [136, 137]. In another interesting design, MnCO3 nanoparticles were used as templates to deposit layer-by-layer (L-B-L) assemblies of Hb and dialdehyde heparin (DHP), followed by cross-linking to stabilize the layers and selective dissolution of the template core [138]. A similar approach was also used to form L-B-L-coated nanotubes where alternate layers of Hb, DHP, and the enzyme CAT were deposited, to create systems for potential application in treating oxidative stress [139]. These complex nanostructures have been characterized in vitro for their morphology, stability, cytotoxicity, and in some cases biofunctionality, but pre-clinical evaluation for oxygen carrying efficacy in vivo is not yet reported. Another recent exciting development in the area of novel HBOC molecules is the utilization of large-molecular-weight extracellular Hb isolated from marine invertebrates like polychaete annelid (e.g., the product HEMOXYCarrier from Hemarina, France) [140]. Pre-clinical studies with this unique Hb molecule have shown reduced microvascular vasoconstriction and no significant impact on mean arterial blood pressure, compared to other HBOCs that utilize bovine or human Hb [139]. Further investigation of this system is currently ongoing to evaluate its potential as a clinical oxygen carrier therapeutic system.
In recent years, some Hb-encapsulation approaches have also focused on adapting the physico-mechanical properties of natural RBCs that significantly influence their biological functions. Healthy RBCs have a biconcave discoid morphology, with a diameter of ~8 μm and a thickness of ~2 μm. These RBCs are also highly flexible (Young’s modulus 0.1–0.2 kPa) that enables them to change their morphology when passing through microvascular circulation [141, 142]. The mechanical integrity and viscoelastic nature of RBCs during their cyclical deformation is rendered by a two-dimensional spectrin network that exhibits context-variable stiffness and tethering to the cytosolic membrane surface. Oxygen loading results in RBCs having significantly more deformability than oxygen unloading, and this enables the flexibility RBCs require to efficiently transit the microvasculature. RBC size, shape, and flexibility also influence their movement and distribution in the blood flow field, where they mostly reside in the center of the parabolic flow field in mid to large vessels, while in small vessels and capillaries, RBCs distribute throughout for efficient oxygen exchange [143, 144]. These considerations have recently led to biomaterials-based mimicry of RBC’s physical (size, shape, and flexibility) attributes into Hb-encapsulating synthetic constructs. For example, polyelectrolyte-driven layer-by-layer assembly has been used to create microparticles that mimic the shape and deformability of natural RBCs [145]. In this approach, Hb and BSA were electrostatically deposited on the surface of discoid PLGA particles of ~7 μm diameter and 400 nm shell thickness, and then the PLGA core was selectively dissolved to yield RBC-shaped Hb-loaded particles that have high elastic deformation. Similar RBC-mimetic flexible particles have been fabricated using PEG hydrogel system in a stop-flow-lithography (SFL) approach where the mechanical properties of resultant particles could be controlled by modulating cross-linking density of the hydrogel systems [146]. In a different approach, RBC shape-mimetic particles were fabricated from acrylate hydrogels using a “particle replication in non-wetting templates” (PRINT®) technology [147]. These particles were made in 2–3 μm molds, such that, upon hydration, the particles swelled to disks with ~6 μm diameter and ~1.5 μm thickness. Also, the meniscus effect from the molds resulted in the particles being thinner in the middle and thicker at the edges, resembling the biconcave morphology of RBCs. RBC morphology and flexibility mimicking particle designs made through these two techniques have demonstrated in vitro elastic deformation capabilities sufficient for transport through narrow channels, and controllable circulation lifetime in vivo, depending on their elastic modulus. Although these particles have been reported to be capable of Hb encapsulation via physical trapping or covalent bonding, detailed oxygen transport capabilities and associated in vivo transfusion applications have not been reported. In another interesting approach, liposome-encapsulated actin-hemoglobin (LEAcHb) constructs were prepared using a polymerized actin core, to mimic morphology of natural RBCs [148]. Although these particles were much smaller (~140 nm) than RBCs, the biconcave shape along with the mechanical support of the membrane improved the half-life to ~72 h. In natural RBCs, the negative surface charge electrostatically prevents RBC aggregation over a distance of 20 nm, and this rationale has led to some research in mimicking RBC-relevant surface charge on Hb-encapsulating PEG-PLA nanoparticles (<200 nm in diameter) using cetyltrimethylammonium bromide (CTAB) or anionic sodium dodecyl sulfate (SDS) surfactants [149]. Of note, cationized particles were found to have a half-life of ~11 h (8-fold higher than untreated particles), while the anionized particles were quickly eliminated, giving a half-life of <1 h. In yet another particularly innovative approach, a biosynthetic artificial RBC (ErythroMer) has been developed following a formal “bioinspired” design principles and is reported to closely emulate RBC physiology, particularly under physiologic stress by preserving cooperative O2 binding/dissociation and by linking O2 affinity to biochemical cues of aerobic sufficiency, while inhibiting methemoglobin (metHb) accumulation and NO sequestration [150]. Importantly, this design is crafted to enable sterile, lyophilized storage suitable for rapid reconstitution even in remote/austere environments. Moreover, due to unique shell properties, this polymeric particle is expected to be immuno-silent, with limited complement activation or other immune-related reactions. ErythroMer is based upon a novel amphiphilic polymeric system that employs polyethylene imine (PEI) grafted to palmitic acid that self-assembles to form payload-bearing toroidal-shaped nanoparticles (termed nanobialys, ~200 nm diameter) that encapsulate Hb, as well as maintain both physiologic, context-responsive O2 affinity and a reductive environment to retard the rate of metHb accrual by coencapsulation of the synthetic allosteric inhibitor RSR-13 and leuko-methylene blue [150]. These novel Hb-containing particles, termed, have shown promising oxygen transport in vivo in rodent models of hemorrhagic shock/resuscitation and near-complete exchange transfusion. Detailed biocompatibility studies (e.g., for PEI which can pose cytotoxicity issues), circulation lifetime and stability, Hb-loading capacity and oxygen transport capabilities, etc. must be further evaluated to establish the clinical potential of such designs as RBC surrogates in transfusion medicine. Figure 11.4 shows design schematics of these novel emerging designs and structures for Hb-based oxygen carriers.
Representative schematics for novel HBOC molecules and designs, including new polymerization strategies, new sources of Hb, and novel encapsulation and biomimetic strategies that are currently under development and pre-clinical evaluation. (From 2017 Military Supplement: Hemoglobin-based Oxygen Carriers Current State-of-the-Art and Novel Molecules, Anirban Gupta, Shock Injury, Inflammation and Sepsis, Oct 3, 2018, Publish Ahead of Print, Figs. 1–4, with permission of Wolters Kluwer Health, Inc.)
Current State-of-Art and Future Perspectives
In traumatic injuries and hemorrhage, tissue oxygenation is severely compromised, resulting in drastic, progressive damage to vital tissues and organs . Therefore, rapid hemorrhage control and restoration of tissue oxygen are critical to optimizing outcomes. To this end, timely transfusion of whole blood or balanced ratio administration of blood components (RBCs, platelets, and plasma) has become the current clinical standard. However, these blood products currently present significant logistical challenges with regard to widespread usage in austere battlefield and pre-hospital settings, where trauma- and hemorrhage-related morbidities and mortalities become significant, particularly in the context of prolonged field care scenarios. One potential solution is the bioengineering of semisynthetic or synthetic surrogates of blood components that are specifically designed for facile use in this challenging environment. In this framework, one important category of technology is that of Hb-based oxygen carriers (HBOCs), which provide the oxygen transport properties of RBCs while enabling higher availability (via in vitro large-scale manufacture), universal applicability (no need for blood type matching), reduced contamination risks (due to sterilization), and longer shelf-life under ambient conditions (for some designs). While a wide variety of approaches have been dedicated to creating HBOCs, with some advancing to clinical trials, major risks associated with cell-free Hb (e.g., short circulation lifetime, renal clearance and associated toxicity, NO scavenging and associated vasoconstrictive/hypertensive side effects, etc.) have led to negative clinical outcomes and deep concerns for viability of this therapeutic class. As a result, no HBOC has attained FDA approval for human use, although one product (HemoPure or HBOC-201) is approved for (restricted) human use in South Africa and has been, under special circumstances, dispensed for compassionate use provision in the USA and Europe [151]. Other HBOC products (PolyHeme, Hemospan, and HemoTech) all advanced to different levels of clinical trials (e.g., Phase I for HemoTech, Phase II for Hemospan, and Phase III for PolyHeme); however, further studies are needed to establish their clinical safety and efficacy profiles. In many clinical studies, functional efficacy comparison has been to natural RBC transfusion, and, though HBOCs have demonstrated a reduction in the number of RBC transfusions, it remains to be answered whether HBOCs are suitable as “RBC substitutes” or rather as “oxygen carriers” in scenarios in which natural RBCs are either unavailable or undesirable. Future considerations of clinical study design should utilize this framework to compare HBOCs to relevant “standard of care” (e.g., saline or plasma expanders in pre-hospital trauma) instead of RBCs, to most appropriately evaluate real-world comparative risk/benefit in this context. Other questions that remain are whether these chemically modified and polymeric HBOC designs based on cell-free Hb have adequately addressed issues of NO scavenging (associated hypertensive effects) and heme toxicity. Newer HBOC designs, both chemically modified cell-free Hb (e.g., HemoTech) and encapsulated Hb (e.g., LEH, PEH, ErythroMer etc.), are still undergoing rigorous pre-clinical evaluation to elucidate and establish batch-to-batch consistency, mechanism of action, pharmacokinetics and biodistribution, tissue oxygenation capability, and in vivo safety profiles. In this framework, it remains to be seen if “encapsulated” Hb designs are superior to chemically modified cell-free systems, in terms of allowing coencapsulation of oxygen affinity regulatory and redox environment preserving molecules. It is important to note here that such multicomponent design will add manufacturing costs and thus the cost–benefit analysis need to be rigorously validated in appropriate pre-clinical models, before clinical studies and translation. Going forward, there is a significant need to systematically study cell-free chemically modified polymeric Hb designs versus encapsulated Hb designs (with or without effector molecule and anti-oxidant enzyme coencapsulation) in a suite of established anatomically and physiologically relevant pre-clinical animal model to compare circulation residence time, tissue oxygenation efficacy, NO scavenging-associated hypertensive risks and heme-associated toxicity, and importantly, suitability for pragmatic field use (both acutely and in prolonged field care scenarios).
Regarding Hb sourcing, most designs have utilized either human or bovine Hb, although some newer designs have adapted utilization of recombinant Hb where the physicochemical and biological properties can be precisely engineered, as well as giant Hb sourced from marine invertebrates with salutary properties. One critical aspect regarding Hb sourcing for efficient HBOC design is the regulation of oxygen loading/off-loading capacity of the Hb used. For human Hb, this is regulated by allosteric effector molecules like 2,3-DPG, which maintains the P50 of human Hb at 26–28 mm mercury. However, oxygen affinity for cell-free human Hb (i.e., in absence of DPG) is much higher (OEC curve shifts to left), and this will lead to reduced oxygen release across any given physiologic gradient [152]. In contrast, oxygen affinity of bovine Hb is not critically dependent on DPG but rather on chloride ions, which are present in abundance in all mammals including humans. Bovine Hb has also been reported to have higher thermal stability than human Hb during isolation and processing [153]. Furthermore, while human Hb is sourced from outdated human units, bovine Hb can be obtained from dedicated farms and slaughterhouses and hence has more availability. Therefore, from availability, processing, and oxygen transport regulation standpoint, bovine Hb may provide benefit over human Hb and is used for Hemopure (or HBOC-201). However, both human and bovine sourcing share risk of infectious transmission, although this risk can be mitigated by appropriate processing and novel pathogen reduction technologies. Other alternative sources of Hb (recombinant technologies, annelid supramolecular extracellular Hb, etc.) should incorporate isolation and manufacturing costs, as well as physicochemical comparison of oxygen loading/off-loading aspects (with respect to human Hb ), in order to successfully translate the corresponding HBOC designs to the clinic. Importantly, HBOCs designed with cell-free non-human Hb should also carefully analyze product immunogenicity, compared to encapsulated version of the same Hb. Other than Hb-based systems, oxygen carriers based on perfluorocarbons (PFCs) and iron (Fe2+)-containing porphyrin systems have also undergone significant pre-clinical and limited clinical evaluation, but an ideal oxygen carrier system for safe and effective in vivo use from this approach is yet to be realized. It is also important to note that the various HBOC systems should not be categorized as “artificial blood,” but rather as a critical component of such a system. It is now unambiguously clear that attention to hemostatic blood components (platelets and plasma) is critical to successful resuscitation for hemorrhagic shock , and a significant volume of research has evolved in the area of platelet surrogates and plasma expanders, reviewed elsewhere [23, 24, 154,155,156,157,158]. Exciting advancements have also been made in recent years to develop “donor independent” RBCs (and platelets) from stem cells, AKA “blood pharming” [159,160,161,162,163,164]. In continuing evaluation and clinical translation of these technologies, it should be very important to consider and resolve manufacturing challenges (e.g., scaling up of complex multicomponent designs while maintaining batch-to-batch consistent quality and functional efficacy, etc.) as well as meticulously design pre-clinical studies in physiologically relevant animal models and clinical studies where current “standard of care” in the specific application is compared. Through such studies, it is envisioned that Hb-based oxygen carriers will revolutionize combat casualty care in pre-hospital and en route scenarios, as well as allow emergency management of civilian trauma in remote locations or when blood products are not immediately or sufficiently available.
References
Holcomb JB, McMullin NR, Pearse L, Caruso J, Wade CE, Oetjen-Gerdes L, Champion HR, Lawnick M, Farr W, Rodriguez S, et al. Causes of death in U.S. Special Operations Forces in the Global War on terrorism, 2001–2004. Ann Surg. 2007;245(6):986–91.
Blackbourne LH, Baer DG, Eastridge BJ, Kheirabadi B, Bagley S, Kragh JF Jr, Cap AP, Dubick MA, Morrison JJ, Midwinter MJ, et al. Military medical revolution: prehospital combat casualty care. J Trauma Acute Care Surg. 2012;76(6 Suppl 5):S372–7.
Cohen MJ, Kutcher M, Redick B, Nelson M, Call M, Knudson MM, Schreiber MA, Bulger EM, Muskat P, Alarcon LH, et al. Clinical and mechanistic drivers of acute traumatic coagulopathy. J Trauma Acute Care Surg. 2013;75(1 Suppl 1):S40–7.
Dorlac WC, DeBakey ME, Holcomb JB, Fagan SP, Kwong KL, Dorlac GR, Schreiber MA, Persse DE, Moore FA, Mattox KL. Mortality from isolated civilian penetrating injury. J Trauma. 2005;59(1):217–22.
Smith ER, Shapiro G, Sarani B. The profile of wounding in civilian public mass shooting fatalities. J Trauma Acute Care Surg. 2016;81(1):86–92.
van Oostendorp SE, Tan ECTH, Geeraedts LMG Jr. Prehospital control of life-threatening truncal and junctional haemorrhage is the ultimate challenge in optimizing trauma care; a review of treatment options and their applicability in the civilian trauma setting. Scand J Trauma Resusc Emerg Med. 2016;24(1):110.
Holcomb JB, Tilley BC, Baraniuk S, Fox EE, Wade CE, Podbielski JM, del Junco DJ, Brasel KJ, Bulger EM, Callcut RA, et al. Transfusion of plasma, platelets, and red blood cells in a 1:1:1 vs a 1:1:2 ratio and mortality in patients with severe trauma: the PROPPR randomized clinical trial. JAMA. 2015;313(5):471–82.
Holcomb JB, del Junco DJ, Fox EE, Wade CE, Cohen MJ, Schreiber MA, Alarcon LH, Bai Y, Brasel KJ, Bulger EM, et al. The prospective, observational, multicenter, major trauma transfusion (PROMMTT) study: comparative effectiveness of a time-varying treatment with competing risks. JAMA Surg. 2013;148(2):127–46.
Holcomb JB, Jenkins D, Rhee P, Johannigman J, Mahoney P, Mehta S, Cox ED, Gehrke MJ, Beilman GJ, Schreiber M, et al. Damage control resuscitation: directly addressing the early coagulopathy of trauma. J Trauma. 2007;62(2):307–10.
Carmen R. The selection of plastic materials for blood bags. Transfus Med Rev. 1993;7(1):1–10.
Heddle NM, Klama LN, Griffith L, Roberts R, Shukla G, Kelton JG. A prospective study to identify the risk factors associated with acute reactions to platelet and red cell transfusions. Transfusion. 1993;33(10):794–7.
Blajchman MA. Bacterial contamination and proliferation during the storage of cellular blood products. Vox Sang. 1998;74(Suppl 2):155–9.
Seghatchian J, de Sousa G. Pathogen-reduction systems for blood components: the current position and future trends. Transfus Apher Sci. 2006;35(3):189–96.
Cap AP, Pidcoke HF, DePasquale M, Rappold JF, Glassberg E, Eliassen HS, Bjerkvig CK, Fosse TK, Kane S, Thompson P, et al. Blood far forward: time to get moving! J Trauma Acute Care Surg. 2015;78(6 Suppl 1):S2–6.
Borgman MA, Spinella PC, Perkins JG, Grathwohl KW, Repine T, Beekley AC, Sebesta J, Jenkins D, Wade CE, Holcomb JB. The ratio of blood products transfused affects mortality in patients receiving massive transfusions at a combat support hospital. J Trauma. 2007;63(4):805–13.
Boscarino C, Tien H, Acker J, Callum J, Hansen AL, Engels P, Glassberg E, Nathens A, Beckett A. Feasibility and transport of packed red blood cells into special forces operational conditions. J Trauma Acute Care Surg. 2014;76(4):1013–9.
Spinella PC, Dunne J, Beilman GJ, O'Connell RJ, Borgman MA, Cap AP, Rentas F. Constant challenges and evolution of US military transfusion medicine and blood operations in combat. Transfusion. 2012;52(5):1146–53.
Kauvar D, Holcomb JB, Norris GC, Hess JR. Fresh whole blood transfusion: a controversial military practice. J Trauma. 2006;61(1):181–4.
Pidcoke HF, McFaul SJ, Ramasubramanian AK, Parida BK, Mora AG, Fedyk CG, Valdez-Delgado KK, Montgomery RK, Reddoch KM, Rodriguez AC, et al. Primary hemostatic capacity of whole blood: a comprehensive analysis of pathogen reduction and refrigeration effects over time. Transfusion. 2013;53(Suppl 1):137S–49S.
Noorman F, van Dongen TTCF, Plat M-CJ, Badloe JF, Hess JR, Hoencamp R. Transfusion: −80°C frozen blood products are safe and effective in military casualty care. PLoS One. 2016;11(12):e0168401.
Acker JP, Marks DC, Sheffield WP. Quality assessment of established and emerging blood components for transfusion. J Blood Transfus. 2016;2016:4860284.
Blajchman MA. Substitutes for success. Nat Med. 1999;5:17–8.
Modery-Pawlowski CL, Tian LL, Pan V, McCrae KR, Mitragotri S, Sen Gupta A. Approaches to synthetic platelet analogs. Biomaterials. 2013;34(2):526–41.
Sen Gupta A. Biomaterials-based strategies for blood substitutes. In: Santambrogio L, editor. Biomaterials in regenerative medicine and the immune system: Springer, Switzerland; 2015. p. 113–37.
Giangrande PLF. The history of blood transfusion. Br J Haematol. 2000;110(4):758–67.
Hillyer CD, editor. Blood banking and transfusion medicine: Churchill Livingstone Elsevier, Philadelphia, USA; 2007.
Carson JL, Hill S, Carless P, Hébert P, Henry D. Transfusion triggers: a systematic review of the literature. Transfus Med Rev. 2002;16(3):187–99.
Sharma S, Sharma P, Tyler LN. Transfusion of blood and blood products: indications and complications. Am Fam Physician. 2011;83(6):719–24.
Whitaker B, Rajbhandary S, Kleinman S, Harris A, Kamani N. Trends in United States blood collection and transfusion: results from the 2013 AABB blood collection, utilization, and patient blood management survey. Transfusion. 2016;56(9):2173–83.
Goodnough LT, Brecher ME, Kanter MH, AuBuchon JP. Transfusion medicine — blood transfusion. N Engl J Med. 1999;340(6):438–47.
Hess JR. An update on solutions for red cell storage. Vox Sang. 2006;91(1):13–9.
Greening DW, Glenister K, Sparrow RL, Simpson RJ. International blood collection and storage: clinical use of blood products. J Proteome. 2009;73(3):386–95.
Tien H, Nascimento B Jr, Callum J, Rizoli S. An approach to transfusion and hemorrhage in trauma: current perspectives on restrictive transfusion strategies. Can J Surg. 2007;50(3):202–9.
Johansson PI, Ostrowski SR, Secher NH. Management of major blood loss: an update. Acta Anaesthesiol Scand. 2010;54(9):1039–49.
Pohlman TH, Walsh M, Aversa J, Hutchison EM, Olsen KP, Lawrence Reed R. Damage control resuscitation. Blood Rev. 2015;29(4):251–62.
Cannon JW, Khan MA, Raja AS, Cohen MJ, Como JJ, Cotton BA, Dubose JJ, Fox EE, Inaba K, Rodriguez CJ, et al. Damage control resuscitation in patients with severe traumatic hemorrhage: a practice management guideline from the Eastern Association for the Surgery of Trauma. J Trauma Acute Care Surg. 2017;82(3):605–17.
Napolitano LM, Kurek S, Luchette FA, Corwin HL, Barie PS, Tisherman SA, Hebert PC, Anderson GL, Bard MR, Bromberg W, et al. American College of Critical Care Medicine of the Society of Critical Care Medicine; Eastern Association for the Surgery of Trauma Practice Management Workgroup: clinical practice guideline: red blood cell transfusion in adult trauma and critical care. Crit Care Med. 2009;37(12):3124–57.
Holcomb JB, Donathan DP, Cotton BA, Del Junco DJ, Brown G, Wenckstern TV, Podbielski JM, Camp EA, Hobbs R, Bai Y, et al. Prehospital transfusion of plasma and red blood cells in trauma patients. Prehosp Emerg Care. 2015;19(1):1–9.
Brown JB, Sperry JL, Fombona A, Billiar TR, Peitzman AB, Guyette FX. Pre-trauma center red blood cell transfusion is associated with improved early outcomes in air medical trauma patients. J Am Coll Surg. 2015;220(5):797–808.
Smith JW, Gilcher RO. Red blood cells, plasma, and other new apheresis-derived blood products: improving product quality and donor utilization. Transfus Med Rev. 1999;13(2):118–23.
D’Alessandro A, Kriebardis AG, Rinalducci S, Antonelou MH, Hansen KC, Papassideri IS, Zolla L. An update on red blood cell storage lesions, as gleaned through biochemistry and omics technologies. Transfusion. 2015;55(1):205–19.
Devine DV, Serrano K. The platelet storage lesion. Clin Lab Med. 2010;30(2):475–87.
Jobes D, Wolfe Y, O’Neill D, Calder J, Jones L, Sesok-Pizzini D, Zheng XL. Toward a definition of “fresh” whole blood: an in vitro characterization of coagulation properties in refrigerated whole blood for transfusion. Transfusion. 2011;51(1):43–51.
D’Amici GM, Mirasole C, D’Alessandro A, Yoshida T, Dumont LJ, Zolla L. Red blood cell storage in SAGM and AS3: a comparison through the membrane two-dimensional electrophoresis proteome. Blood Transfus. 2012;10(Suppl 2):s46–54.
Paglia G, D'Alessandro A, Rolfsson Ó, Sigurjónsson ÓE, Bordbar A, Palsson S, Nemkov T, Hansen KC, Gudmundsson S, Palsson BO. Biomarkers defining the metabolic age of red blood cells during cold storage. Blood. 2016;128:e43–50.
Chaudhari CN. Frozen red blood cells in transfusion. Med J Armed Forces India. 2009;65(1):55–8.
Hess JR. Red cell freezing and its impact on supply chain. Transfus Med. 2004;14(1):1–8.
Solheim BG. Pathogen reduction of blood components. Transfus Apher Sci. 2008;39(1):75–82.
Chang R, Eastridge BJ, Holcomb JB. Remote damage control resuscitation in austere environments. Wilderness Environ Med. 2017;28(2S):S124–34.
Squires JE. Artificial blood. Science. 2002;295(5557):1002–5.
Chang TMS. Blood substitutes based on nanobiotechnology. Trends Biotechnol. 2006;24:372–7.
Natanson C, Kern SJ, Lurie P, Banks SM, Wolfe SM. Cell-free hemoglobin-based blood substitutes and risk of myocardial infarction and death: a meta-analysis. JAMA. 2008;299(19):2304–12.
Klotz IM. Hemoglobin-oxygen equilibria: retrospective and phenomenological perspective. Biophys Chem. 2003;100(1–3):123–9.
Goutelle S, Maurin M, Rougier F, Barbaut X, Bourguignon L, Ducher M, Maire P. The Hill equation: a review of its capabilities in pharmacological modelling. Fundam Clin Pharmacol. 2008;22(6):633–48.
Umbreit J. Methemoglobin—It's not just blue: a concise review. Am J Hematol. 2007;82(2):134–44.
Dorman SC, Kenny CF, Miller L, Hirsch RE, Harrington JP. Role of redox potential of hemoglobin-based oxygen carriers on methemoglobin reduction by plasma components. Artif Cells Blood Substit Immobil Biotechnol. 2002;30(1):39–51.
Stowell CP, Levin J, Spiess BD, Winslow RM. Progress in the development of RBC substitutes. Transfusion. 2001;41(2):287–99.
Winslow RM. Red cell substitutes. Semin Hematol. 2007;44(1):51–9.
Chang TMS. From artificial red blood cells, oxygen carriers, and oxygen therapeutics to artificial cells, nanomedicine, and beyond. Artif Cells Blood Substit Immobil Biotechnol. 2012;40(3):197–9.
Napolitano LM. Hemoglobin-based oxygen carriers: first, second or third generation? Human or bovine? Where are we now? Crit Care Clin. 2009;25(2):279–301.
Piras AM, Dessy A, Chiellini F, Chiellini E, Farina C, Ramelli M, Valle ED. Polymeric nanoparticles for hemoglobin-based oxygen carriers. Biochim Biophys Acta. 2008;1784(10):1454–61.
Buehler PW, Alayash AI. All hemoglobin-based oxygen carriers are not created equally. Biochim Biophys Acta. 2008;1784(10):1378–81.
Winslow RM. Cell-free oxygen carriers: scientific foundations, clinical development, and new directions. Biochim Biophys Acta. 2008;1784(10):1382–6.
Alayash AI. Setbacks in blood substitutes research and development: a biochemical perspective. Clin Lab Med. 2010;30(2):381–9.
Amberson WR, Jennings JJ, Rhode CM. Clinical experience with hemoglobin-saline solutions. J Appl Physiol. 1949;1(7):469–89.
Bunn H, Jandl J. The renal handling of hemoglobin. Trans Assoc Am Phys. 1968;81:147–52.
Buehler PW, D’Agnillo F, Schaer DJ. Hemoglobin-based oxygen carriers: from mechanisms of toxicity and clearance to rational drug design. Trends Mol Med. 2010;16(10):447–57.
Kim-Shapiro DB, Schechter AN, Gladwin MT. Unraveling the reactions of nitric oxide, nitrite, and hemoglobin in physiology and therapeutics. Arterioscler Thromb Vasc Biol. 2006;26(4):697–705.
Looker D, Abbott-Brown D, Cozart P, Durfee S, Hoffman S, Mathews AJ, Miller-Roehrich J, Shoemaker S, Trimble S, Fermi G, et al. A human recombinant haemoglobin designed for use as a blood substitute. Nature. 1992;356(6366):258–60.
Fronticelli C, Koehler RC, Brinigar WS. Recombinant hemoglobins as artificial oxygen carriers. Artif Cells Blood Substit Immobil Biotechnol. 2007;35(1):45–52.
Varnado CL, Mollan TL, Birukou I, Smith BJZ, Henderson DP, Olson JS. Development of recombinant hemoglobin-based oxygen carriers. Antioxid Redox Signal. 2013;18(17):2314–28.
Lamy ML, Daily EK, Brichant JF, Larbuisson RP, Demeyere RJ, Vandermeersch EA, Kehot JJ, Parsloe MR, Berridge JC, Sinclair CJ, et al. Randomized trial of Diaspirin cross-linked hemoglobin solution as an alternative to blood transfusion after cardiac surgery. Anesthesiology. 2000;92:646–56.
Saxena R, Wijnhoud A, Carton H, Hacke W, Kaste M, Przybelski R, Stern KN, Koudstaal PJ. Controlled safety study of a hemoglobin-based oxygen carrier, DCLHb, in acute ischemic stroke. Stroke. 1999;30:993–6.
Sloan EP, Koenigsberg MD, Philbin NB, Gao W. DCLHb Traumatic Hemorrhagic Shock Study Group. European HOST investigators. Diaspirin cross-linked hemoglobin infusion did not influence base deficit and lactic acid levels in two clinical trials of traumatic hemorrhagic shock patient resuscitation. J Trauma. 2010;68(5):1158–71.
Winslow RM. New transfusion strategies: red cell substitutes. Annu Rev Med. 1999;50:337–53.
Viele MK, Weisopf RB, Fisher D. Recombinant human hemoglobin does not affect renal function in humans: analysis of safety and pharmacokinetics. Anesthesiology. 1997;86(4):848–58.
Gould SA, Moore EE, Hoyt DB, Burch JM, Haenel JB, Garcia J, DeWoskin R, Moss GS. The first randomized trial of human polymerized hemoglobin as a blood substitute in acute trauma and emergent surgery. J Am Coll Surg. 1998;187(2):113–20.
Jahr JS, Moallempour M, Lim JC. HBOC-201, hemoglobin glutamer-250 (bovine), Hemopure (Biopure Corporation). Expert Opin Biol Ther. 2008;8(9):1425–33.
Cheng DC, Mazer CD, Martineau R, Ralph-Edwards A, Karski J, Robblee J, Finegan B, Hall RI, Latimer R, Vuylsteke A. A phase II dose-response study of hemoglobin raffimer (Hemolink) in elective coronary artery bypass surgery. J Thorac Cardiovasc Surg. 2004;127(1):79–86.
Alayash AI. Blood substitutes: why haven’t we been more successful? Trends Biotechnol. 2014;32(4):177–85.
Chang TMS. Future generations of red blood cell substitutes. J Intern Med. 2003;253(5):527–35.
Chen J-Y, Scerbo M, Kramer G. A review of blood substitutes: examining the history, clinical trial results, and ethics of hemoglobin-based oxygen carriers. Clinics. 2009;64(8):803–13.
Vandegriff KD, Winslow RM. Hemospan: design principles for a new class of oxygen therapeutic. Artif Organs. 2009;33(2):133–8.
Bobofchak KM, Tarasov E, Olsen KW. Effect of cross-linker length on the stability of hemoglobin. Biochim Biophys Acta. 2008;1784(10):1410–4.
Caretti A, Fantacci M, Caccia D, Perrella M, Lowe KC, Samaja M. Modulation of the NO/cGMP pathway reduces the vasoconstriction induced by acellular and PEGylated haemoglobin. Biochim Biophys Acta. 2008;1784(10):1428–34.
Jahr JS, Akha AS, Holtby RJ. Crosslinked, polymerized, and PEG-conjugated hemoglobin-based oxygen carriers: clinical safety and efficacy of recent and current products. Curr Drug Discov Technol. 2012;9(3):158–65.
Olofsson CAT, Johansson T, Larsson S, Nellgård P, Ponzer S, Fagrell B, Przybelski R, Keipert P, Winslow N, Winslow RM. A multicenter clinical study of the safety and activity of maleimide-polyethylene glycol-modified Hemoglobin (Hemospan) in patients undergoing major orthopedic surgery. Anesthesiology. 2006;105(6):1153–63.
Buehler PW, Alayash AI. Toxicities of hemoglobin solutions: in search of in-vitro and in-vivo model systems. Transfusion. 2004;44(10):1516–30.
Alayash AI. Oxygen therapeutics: can we tame haemoglobin? Nat Rev Drug Discov. 2004;3:152–9.
Roche CJ, Cassera MB, Dantsker D, Hirsch RE, Friedman JM. Generating S-Nitrosothiols from hemoglobin. Mechanisms, conformational dependence and physiological relevance. J Biol Chem. 2013;288(31):22408–25.
D’Agnillo F, Chang TMS. Polyhemoglobin–superoxide dismutase-catalase as a blood substitute with antioxidant properties. Nat Biotechnol. 1998;16(7):667–71.
Powanda D, Chang TMS. Cross-linked polyhemoglobin–superoxide dismutase–catalase supplies oxygen without causing blood brain barrier disruption or brain edema in a rat model of transient global brain ischemia–reperfusion. Artif Cells Blood Substit Immob Biotechnol. 2002;30(1):25–42.
Ogata Y, Goto H, Kimura T, Fukui H. Development of neo red cells (NRC) with the enzymatic reduction system of methemoglobin. Artif Cells Blood Substit Immobil Biotechnol. 1997;25(4):417–27.
Simoni J, Simoni G, Moeller JF, Feola M, Wesson DE. Artificial oxygen carrier with pharmacologic actions of adenosine-5′-triphosphate, adenosine, and reduced glutathione formulated to treat an array of medical conditions. Artif Organs. 2014;38(8):684–90.
Simoni J, Simoni G, Wesson DE, Feola M. ATP-adenosine-glutathione cross-linked hemoglobin as clinically useful oxygen carrier. Curr Drug Discov Technol. 2012;9(3):173–87.
Wollocko H, Anvery S, Wollocko J, Harrington JM, Harrington JP. Zero-link polymerized hemoglobin (OxyVita®Hb) stabilizes the heme environment: potential for lowering vascular oxidative stress. Artif Cells Nanomed Biotechnol. 2017;45(4):701–9.
Ma L, Thompson FM, Wang D, Hsia CJC. Polynitroxylated PEGylated Hemoglobin (PNPH): a nanomedicine for critical care and transfusion, chapter 16. In: Kim HW, Greenberg AG, editors. Hemoglobin-based oxygen carriers as red cell substitutes and oxygen therapeutics. Berlin: Springer-Verlag; 2013. p. 299–313.
Chang TMS. Hemoglobin corpuscles’ report of a research project for Honours Physiology, Medical Library, McGill University 1957. Reprinted as part of ‘30 anniversary in Artificial Red Blood Cells Research’. J Biomat Artif Cells Artif Organs. 1988;16:1–9.
Chang TMS, Poznansky MJ. Semipermeable microcapsules containing catalase for enzyme replacement in acatalsaemic mice. Nature. 1968;218(5138):242–5.
Chang TMS. Semipermeable microcapsules. Science. 1964;146(3643):524–5.
Djordjevich L, Miller IF. Synthetic erythrocytes from lipid encapsulated hemoglobin. Exp Hematol. 1980;8(5):584.
Hunt CA, Burnette RR, MacGregor RD, Strubbe A, Lau D, Taylor N. Synthesis and evaluation of a prototypal artificial red cell. Science. 1985;230(4730):1165–8.
Rudolph AS, Klipper RW, Goins B, Phillips WT. In vivo biodistribution of a radiolabeled blood substitute: 99mTc-labeled liposome-encapsulated hemoglobin in an anesthetized rabbit. Proc Natl Acad Sci U S A. 1991;88(23):10976–80.
Sakai H, Sou K, Horinouchi H, Kobayashi K, Tsuchida E. Review of hemoglobin-vesicles as artificial oxygen carriers. Artif Organs. 2009;33(2):139–45.
Pape A, Kertscho H, Meier J, Horn O, Laout M, Steche M, Lossen M, Theissen A, Zwissler B, Habler O. Improved short-term survival with polyethylene glycol modified hemoglobin liposomes in critical normovolemic anemia. Intensive Care Med. 2008;34(8):1534–43.
Kawaguchi AT, Fukumoto D, Haida M, Ogata Y, Yamano M, Tsukada H. Liposome-encapsulated hemoglobin reduces the size of cerebral infarction in the rat: evaluation with photochemically induced thrombosis of the middle cerebral artery. Stroke. 2007;38(5):1626–32.
Agashe H, Awasthi V. Current perspectives in liposome-encapsulated hemoglobin as oxygen carrier. Adv Plan Lipid Bilayers Liposomes. 2009;9:1–28.
Ceh B, Winterhalter M, Frederik PM, Vallner JJ, Lasic DD. Stealth® liposomes: from theory to product. Adv Drug Delivery Rev. 1997;24(2–3):165–77.
Immordino ML, Dosio F, Cattel L. Stealth liposomes: review of the basic science, rationale, and clinical applications, existing and potential. Int J Nanomedicine. 2006;1(3):297–315.
Philips WT, Klpper RW, Awasthi VD, Rudolph AS, Cliff R, Kwasiborski V, Goines VA. Polyethylene glycol modified liposome-encapsulated hemoglobin: a long circulating red cell substitute. J Pharm Exp Ther. 1999;288(2):665–70.
Sakai H, Sou K, Horinouchi H, Kobayashi K, Tsuchida E. Hemoglobin-vesicle, a cellular artificial oxygen carrier that fulfills the physiological roles of the red blood cell structure. Adv Exp Med Biol. 2010;662:433–8.
Tsuchida E, Sou K, Nakagawa A, Sakai H, Komatsu T, Kobayashi K. Artificial oxygen carriers, hemoglobin vesicles and albumin-hemes, based on bioconjugate chemistry. Bioconjug Chem. 2009;20(8):1419–40.
Taguchi K, Urata Y, Anraku M, Watanabe H, Kadowaki D, Sakai H, Horinouchi H, Kobayashi K, Tsuchida E, Maruyama T, et al. Hemoglobin vesicles, Polyethylene Glycol (PEG)ylated liposomes developed as a Red Blood Cell Substitute, do not induce the accelerated blood clearance phenomenon in mice. Drug Metab Dispos. 2009;37(11):2197–203.
Kaneda S, Ishizuka T, Goto H, Kimura T, Inaba K, Kasukawa H. Liposome-encapsulated Hemoglobin, TRM-645: current status of the development and important issues for clinical application. Artif Organs. 2009;33(2):146–52.
Tao Z, Ghoroghchian PP. Microparticle, nanoparticle, and stem cell-based oxygen carriers as advanced blood substitutes. Trends Biotechnol. 2014;32(9):466–73.
Sakai H. Present situation of the development of cellular-type hemoglobin-based oxygen carrier (hemoglobin-vesicles). Curr Drug Discov Technol. 2012;9(3):188–93.
Yadav VR, Nag O, Awasthi V. Biological evaluation of Liposome-encapsulated Hemoglobin surface-modified with a novel PEGylated nonphospholipid amphiphile. Artif Organs. 2014;38(8):625–33.
Yadav VR, Rao G, Houson H, Hedrick A, Awasthi S, Roberts PR, Awasthi V. Nanovesicular liposome-encapsulated hemoglobin (LEH) prevents multi-organ injuries in a rat model of hemorrhagic shock. Eur J Pharm Sci. 2016;93:97–106.
Kheir JN, Scharp LA, Borden MA, Swanson EJ, Loxley A, Reese JH, Black KJ, Velazquez LA, Thomson LM, Walsh BK, et al. Oxygen gas–filled microparticles provide intravenous oxygen delivery. Sci Transl Med. 2012;4(140):140–88.
Kheir JN, Polizzotti BD, Thomson LM, O’Connell DW, Black KJ, Lee RW, Wilking JN, Graham AC, Bell DC, McGowan FX. Bulk manufacture of concentrated oxygen gas-filled microparticles for intravenous oxygen delivery. Adv Healthc Mater. 2013;2(8):1131–41.
Yu WP, Chang TMS. Submicron polymer membrane hemoglobin nanocapsules as potential blood substitutes: preparation and characterization. Artif Cells Blood Substit Immobil Biotechnol. 1996;24(3):169–84.
Chang TMS, Yu WP. Nanoencapsulation of hemoglobin and RBC enzymes based on nanotechnology and biodegradable polymer. In: TMS C, editor. Blood substitutes: principles, methods, products and clinical trials, vol. 2. Basel: Karger; 1998. p. 216–31.
Chang TMS. Blood replacement with nanobiotechnologically engineered hemoglobin and hemoglobin nanocapsules. Wiley Interdiscip Rev Nanomed Nanobiotechnol. 2010;2(4):418–30.
Rameez S, Alosta H, Palmer AF. Biocompatible and biodegradable polymersome encapsulated hemoglobin: a potential oxygen carrier. Bioconjug Chem. 2008;19(5):1025–32.
Sheng Y, Yuan Y, Liu C, Tao X, Shan X, Xu F. In vitro macrophage uptake and in vivo biodistribution of PLA-PEG nanoparticles loaded with hemoglobin as blood substitutes: effect of PEG content. J Mater Sci Mater Med. 2009;20(9):1881–91.
Arifin DR, Palmer AF. Polymersome encapsulated hemoglobin: a novel type of oxygen carrier. Biomacromolecules. 2005;6(4):2172–81.
Rameez S, Bamba I, Palmer AF. Large scale production of vesicles by hollow fiber extrusion: a novel method for generating polymersome encapsulated hemoglobin dispersions. Langmuir. 2010;26(7):5279–85.
Misra H, Lickliter J, Kazo F, Abuchowski A. PEGylated Carboxyhemoglobin bovine (SANGUINATE): results of a phase I clinical trial. Artif Organs. 2014;38(8):702–7.
Ananthakrishnan R, Li Q, O’Shea KM, Quadri N, Wang L, Abuchowski A, Schmidt AM, Ramasamy R. Carbon monoxide form of PEGylated hemoglobin protects myocardium against ischemia/reperfusion injury in diabetic and normal mice. Artif Cells Nanomed Biotechnol. 2013;41(6):428–36.
Abuchowski A. SANGUINATE (PEGylated Carboxyhemoglobin bovine): mechanism of action and clinical update. Artif Organs. 2017;41(4):346–50.
Wu L. Carbon monoxide: endogenous production, physiological functions, and pharmacological applications. Pharmacol Rev. 2005;57(4):585–630.
Tomita D, Kimura T, Hosaka H, Daijima Y, Haruki R, Ludwig K, Böttcher C, Komatsu T. Covalent core-shell architecture of hemoglobin and human serum albumin as an artificial O2 carrier. Biomacromolecules. 2013;14(6):1816–25.
Hosaka H, Haruki R, Yamada K, Böttcher C, Komatsu T. Hemoglobin-albumin cluster incorporating a Pt nanoparticle: artificial O2 carrier with antioxidant activities. PLoS One. 2014;9(10):e110541.
Duan L, Yan X, Wang A, Jia Y, Li J. Highly loaded hemoglobin spheres as promising artificial oxygen carriers. ACS Nano. 2012;6(8):6897–904.
Xiong Y, Liu ZZ, Georgieva R, Smuda K, Steffen A, Sendeski M, Voigt A, Patzak A, Bäumler H. Nonvasoconstrictive hemoglobin particles as oxygen carriers. ACS Nano. 2013;7(9):7454–61.
Li B, Li T, Chen G, Li X, Yan L, Xie Z, Jing X, Huang Y. Regulation of conjugated hemoglobin on micelles through copolymer chain sequences and the protein’s isoelectric aggregation. Macromol Biosci. 2013;13(7):893–902.
Qi Y, Li T, Wang Y, Wei X, Li B, Chen X, Xie Z, Jing X, Huang Y. Synthesis of hemoglobin-conjugated polymer micelles by thiol Michael-addition reactions. Macromol Biosci. 2016;16(6):906–13.
Jia Y, Cui Y, Fei J, Du M, Dai L, Li J, Yang Y. Construction and evaluation of hemoglobin-based capsules as blood substitutes. Adv Funct Mater. 2012;22(7):1446–53.
Chen B, Jia Y, Zhao J, Li H, Dong W, Li J. Assembled hemoglobin and catalase nanotubes for the treatment of oxidative stress. J Phys Chem C. 2013;117(38):19751–8.
Le Gall T, Polard V, Rousselot M, Lotte A, Raouane M, Lehn P, Opolon P, Leize E, Deutsch E, Zal F, et al. In vivo biodistribution and oxygenation potential of a new generation of oxygen carrier. J Biotechnol. 2014;187:1–9.
Tsai AG, Intaglietta M, Sakai H, Delpy E, La Rochelle CD, Rousselot M, Zal F. Microcirculation and NO-CO studies of a natural extracellular hemoglobin developed for an oxygen therapeutic carrier. Curr Drug Discov Technol. 2012;9(3):166–72.
Wang X, Gao W, Peng W, Xie J, Li Y. Biorheological properties of reconstructed erythrocytes and its function of carrying-releasing oxygen. Artif Cells Blood Substit Immobil Biotechnol. 2009;37(1):41–4.
Goldsmith HL, Marlow J. Flow behaviour of erythrocytes. I. Rotation and deformation in dilute suspensions. Proc R Soc Lond B. 1972;182(1068):351–84.
Charoenphol P, Mocherla S, Bouis D, Namdee K, Pinsky DJ, Eniola-Adefeso O. Targeting therapeutics to the vascular wall in atherosclerosis--carrier size matters. Atherosclerosis. 2011;217(2):364–70.
Doshi N, Zahr AS, Bhaskar S, Lahann J, Mitragotri S. Red blood cell-mimicking synthetic biomaterial particles. Proc Natl Acad Sci U S A. 2009;106(51):21495–9.
Haghgooie R, Toner M, Doyle PS. Squishy non-spherical hydrogel microparticles. Macromol Rapid Commun. 2010;31(2):128–34.
Merkel TJ, Jones SW, Herlihy KP, Kersey FR, Shields AR, Napier M, Luft JC, Wu H, Zamboni WC, Wang AZ, et al. Using mechanobiological mimicry of red blood cells to extend circulation times of hydrogel microparticles. Proc Natl Acad Sci U S A. 2011;108(2):586–91.
Li S, Nickels J, Palmer AF. Liposome-encapsulated actin-hemoglobin (LEAcHb) artificial blood substitutes. Biomaterials. 2005;26(17):3759–69.
Xu F, Yuan Y, Shan X, Liu C, Tao X, Sheng Y, Zhou H. Long-circulation of hemoglobin-loaded polymeric nanoparticles as oxygen carriers with modulated surface charges. Int J Pharm. 2009;377(1–2):199–206.
Pan D, Rogers S, Misra S, Vulugundam G, Gazdzinski L, Tsui A, Mistry N, Said A, Spinella P, Hare G, Lanza G, Doctor A. ErythroMer (EM): nanoscale bio-synthetic artificial red cell proof of concept and in vivo efficacy results. Blood. 2016;128(22):A1027.
Weiskopf RB, Beliaev AM, Shander A, Guinn NR, Cap AP, Ness PM, Silverman TA. Addressing the unmet need of life-threatening anemia with hemoglobin-based oxygen carriers. Transfusion. 2017;57(1):207–14.
Muir WW, Wellman ML. Hemoglobin solutions and tissue oxygenation. J Vet Intern Med. 2003;17(2):127–35.
Sakai H, Masada Y, Takeoka S, Tsuchida E. Characteristics of bovine hemoglobin as a potential source of hemoglobin-vesicles for an artificial oxygen carrier. J Biochem. 2002;131(4):611–7.
Chan LW, White NJ, Pun SH. Synthetic strategies for engineering intravenous hemostat. Bioconjug Chem. 2015;26(7):1224–36.
Lashoff-Sullivan M, Shoffstall A, Lavik E. Intravenous hemostats: challenges in translation to patients. Nanoscale. 2013;5(22):10719–28.
Booth C, Highley D. Crystalloids, colloids, blood, blood products and blood substitutes. Anaesth Intensive Care Med. 2010;11(2):50–5.
McCahon R, Hardman J. Pharmacology of plasma expanders. Anaesth Intensive Care Med. 2007;8(2):79–81.
Hickman DA, Pawlowski CL, Sekhon UDS, Marks J, Sen Gupta A. Biomaterials an advanced technologies for hemostatic management of bleeding. Adv Mater. 2018;30(4) https://doi.org/10.1002/adma.201700859.
Douay L, Andreu G. Ex vivo production of human red blood cells from hematopoietic stem cells: what is the future in transfusion? Transfus Med Rev. 2007;21(2):91–100.
Rousseau GF, Giarratana MC, Douay L. Large-scale production of red blood cells from stem cells: what are the technical challenges ahead? Biotechnol J. 2014;9(1):28–38.
Avanzi MP, Mitchell WB. Ex vivo production of platelets from stem cells. Br J Haematol. 2014;165(2):237–47.
Nakamura S, Takayama N, Hirata S, Seo H, Endo H, Ochi K, Fujita K, Koike T, Harimoto K, Dohda T, et al. Expandable megakaryocyte cell lines enable clinically applicable generation of platelets from human induced pluripotent stem cells. Cell Stem Cell. 2014;14(4):535–48.
Thon JN, Mazutis L, Wu S, Sylman JL, Ehrlicher A, Machlus KR, Feng Q, Lu S, Lanza R, Neeves KB, et al. Platelet bioreactor-on-a-chip. Blood. 2014;124(12):1857–67.
Spitalnik SL, Triulzi D, Devine DV, Dzik WH, Eder AF, Gernsheimer T, Josephson CD, Kor DJ, Luban NL, Roubinian NH, et al. State of the science in Transfusion Medicine Working Groups. Transfusion. 2015;55(9):2282–90.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Sen Gupta, A., Doctor, A. (2020). Oxygen Carriers. In: Spinella, P. (eds) Damage Control Resuscitation. Springer, Cham. https://doi.org/10.1007/978-3-030-20820-2_11
Download citation
DOI: https://doi.org/10.1007/978-3-030-20820-2_11
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-20819-6
Online ISBN: 978-3-030-20820-2
eBook Packages: MedicineMedicine (R0)