Abstract
Accurate and detailed knowledge of ACL footprint anatomy is essential for successful anatomical ACL reconstruction. On the femoral side, the discovery of bony landmarks led to the standardization of femoral bone tunnel construction; however, the detailed morphology and location of ACL tibial footprint continue to be a topic of debate, and there are still no standardized methods for tibial tunnel construction. We previously reported the ACL tibial attachment site anatomy and bony landmarks and compared 3D images with visual and histological evaluations. The results from the study found a unique bony landmark surrounding the ACL attachment site, showing the relationship of these bony landmarks and surrounding anatomical landmarks as a useful indicator for determining tunnel positions during arthroscopic surgery. This section will clarify the detailed anatomy and bony landmark of the ACL tibial footprint necessary for reconstructive surgery by reviewing our previous research in conjunction with the available literature.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
With the development of anatomical approach for anterior cruciate ligament (ACL) reconstruction in recent years, a more detailed anatomical research of ACL attachment has become a focus of attention. However, the morphology and location of footprint continue to be a topic of debate, and a general consensus has not yet been reached. We have presented a detailed report on the bony landmarks around the ACL tibial footprint, as well as the relationship between these bony landmarks and anatomical structures around the ACL tibial footprint [1]. This section will clarify the detailed anatomy of the ACL tibial footprint necessary for reconstructive surgery by reviewing our previous research in conjunction with the available literature.
2 Bony Landmark Around ACL Tibial Footprint
In contrast to the femur, reports on bony landmarks of the ACL tibial footprint are rare. Purnell et al. demonstrated in their research using 3D-CT images that there is an absence of anterior/lateral bony landmarks in the tibia, though one can confirm the medial intercondylar ridge in the medial border and a tibial ridge in the posterior border of the ACL attachment [2]. Berg et al. utilized X-ray images to report an anterior bony prominence to the ACL attachment at approximately 30 % of the knee joint called the Parsons’ knob [3]. Ziegler et al. also reported two bony landmarks, the ACL ridge and ACL tubercle, located at the anterior border of the ACL, in addition to the anterolateral fossa located in the lateral border [4]. Hutchinson described the “over-the-back position (ridge)” located posterior to the ACL tibial footprint as the most reliable and accurate bony reference for ACL tibial tunnel creation [5].
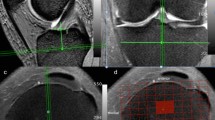
In our research, we found a bony protrusion that approximately corresponds to the ACL footprint, located anterior to the medial and lateral tubercle and the center of the tibial plateau (Fig. 4.1). A bony ridge (anterior ridge) medial laterally extends anterior to the aforementioned protrusion. We believed the anterior ridge might be the same bony structure as the “Parson’s knob”; however, this landmark does not resemble the morphology of a knob but rather a ridgelike structure with some width. Also, this landmark joins with the medial intercondylar ridge at the anterior border to form an L-shaped ridge [1]. Furthermore, between the medial and lateral tubercle, a small depression referred to as the intertubercular fossa can be confirmed, in addition to a lateral groove that extends anteroposteriorly. Although the morphology of bony protrusions can be classified into two categories of oval and triangular types, these morphological characteristics surrounding the protrusion can be confirmed in almost all cases, demonstrating a general morphological tendency.
(a) 3D axial images of left knee tibial plateau. (b) Anterosuperior view of tibial plateau. A (white dash line), bony protrusion of ACL tibial attachment; B (red dash line), lateral groove; C (blue dash line), intertubercular fossa; AR anterior ridge, MIR medial intercondylar ridge, LIT lateral intercondylar tubercle, MIT medial intercondylar tubercle, TAR tibial ACL ridge, OBR over-the-back ridge, LSR L-shaped ridge
3 Anterior and Medial Side of the ACL Tibial Footprint
Soft tissues such as the synovial membrane are absent anteriorly and medially to the ACL tibial attachment, and the border between bone and ligament is distinct. A small protrusion observed by 3D-CT images, corresponding to the anterior ridge, can also be grossly observed and palpated. The anterior ridge is a small protrusion that is 1 mm in width and 10–11 mm in length, and the ACL was attached posterior to this protrusion. Additionally, this protrusion joins together the medial intercondylar ridge and anteromedial border, forming the anteromedial border of the ACL footprint. The anterior ridge can also be clearly confirmed histologically, and it can be observed that the ACL is attached posteriorly to this ridge (Fig. 4.2).
4 Lateral Side of ACL Tibial Footprint
The ACL comes into adjacency with the anterior horn of the lateral meniscus under gross observation, and parts of the ACL fiber are attached to the anterior horn with an anterior width ranging from 1/3–1/2 of its surface. Moreover, fat and scar tissues cover its border, and the border between the anterior horn of the lateral meniscus and ACL attachment cannot be grossly identified. When these surface layers of soft tissues are carefully detached, both structures are overlapped anteriorly and the lateral meniscus slips under the substratum of the ACL posteriorly (Fig. 4.3). The anterior horn of the lateral meniscus was attached on the base of the lateral groove and lateral aspect of the aforementioned bony protrusion, and the attachment was located almost anterior to the lateral intercondylar tubercle. Although the ACL attaches anteriorly at the base of the groove, in terms of its histology, the lateral meniscus attaches to the base of lateral groove and the lateral aspect of the protrusion mediated by connective tissue as the attachment site moves posteriorly (Fig. 4.4).
(a, b) Macroscopic observation of ACL tibial footprint. (a) ACL and lateral meniscus are overlapped anteriorly, and the lateral meniscus slips under the substratum of the ACL posteriorly. (b) After resection of ACL and lateral meniscus attachment. AH anterior horn of lateral meniscus, MM medial meniscus, LIT lateral intercondylar tubercle, MIT medial intercondylar tubercle, white dot area ACL tibial footprint, blue dot area attachment of anterior horn of lateral meniscus
Coronal histological section of the lateral margin of ACL tibial footprint (original magnification × 1). The lateral meniscus attaches to the base of lateral groove and the lateral aspect of the protrusion with connective tissue. AC: articular cartilage of lateral tibial plateau. White dot area: connective tissue (CT) of anterior horn of lateral meniscus. Black dash line: bony protrusion of ACL tibial footprint. Arrowhead: base of lateral groove
5 Posterior Border of ACL Tibial Footprint
Under gross observation, fibrous tissue was found between the medial intercondylar tubercles, tibial ACL ridge, and ACL. A careful removal of these tissues revealed that ligaments were attached to the medial intercondylar tubercle; however, these ligaments were not attached to the ACL tibial ridge and the intertubercular fossa (Fig. 4.5). The same observation was confirmed histologically, and vascular tissues and synovial membrane were confirmed in the intertubercular fossa (Fig. 4.5). From these findings, we can extrapolate that the main fiber of the ACL is not attached posteriorly to the anterior margin of the medial and lateral intercondylar tubercle, and that its posterior border is positioned relatively anterior to what has been previously believed.
(a) Macroscopic observation of ACL tibial footprint. After removal of fat and synovial tissues, the ACL is attached only to the medial intercondylar tubercle and not attached to the lateral intercondylar tubercle and intertubercular space. Main fiber of the ACL is not attached posteriorly to the anterior margin of the medial and lateral intercondylar tubercle. (b) Axial section of posterior border of ACL tibial footprint (original magnification × 4). Vascular tissues and synovial membrane were confirmed in the intertubercular fossa, and ACL fiber was only attached to medial intercondylar tubercle. AH anterior horn of lateral meniscus, MM medial meniscus, LIT lateral intercondylar tubercle, MIT medial intercondylar tubercle, white solid line anterior margin of the medial and lateral intercondylar tubercle, white dot line anterior margin of tibial ACL ridge
6 Discussion
6.1 Size and Morphology of ACL Tibial Footprint
A detailed anatomical knowledge of the attachment area of the ACL is essential for successful anatomical ACL reconstruction. In contrast to the femoral attachment, previous studies reported various sizes and morphologies of the tibial ACL attachment (Table 4.1). Girgis et al. reported 30 mm of length [6], Tállay et al. reported a length of 19.5 ± 2.6 mm and width of 10.3 ± 1.9 mm [7], Ferretti et al. reported a length of 18.1 ± 2.8 mm and width of 10.7 ± 1.9 mm [8], Purnell et al. reported a length of 10.7 ± 1.3 mm and width of 7.3 ± 1.1 mm [2], and the morphology of the attachment also varies by case, such as oval and triangular attachments [1]. There were various interpretations of ACL components including single bundle [9, 10], double bundle [11, 12], and triple bundle [13], while the arrangement of these components at the tibial footprint was widely varied. In recent years, Siebold reported that the ACL is a flat midsubstance with a ribbonlike anatomy and that the tibial attachment is C-shaped [14]. These results were not only influenced by individual difference, but also by differences in modality, age, sex, race, and body type. Moreover, because many reports grossly observed the attachment site of the ligament in order to determine its borders, the differences in the reviewers’ individual interpretations greatly influenced their results. Additionally, the results may change drastically by how the synovial membrane and fat tissues are managed, resulting in a widely ranging analysis.
6.2 Anatomical Landmark for Tibial Tunnel Creation
An important factor in surgery is how to create bone tunnels that are accurate and reproducible amid these varied tibial footprints. Thus, when creating tibial bone tunnels, various intraoperative landmarks have been reported (Table 4.2). Tállay et al. recommended deciding the position from the anterior border of the tibia [7], Morgan et al. from the PCL [15], and Hutchinson and Edwards and Heming et al. from the distance from the over-the-back ridge [5, 10, 12]. Furthermore, there were reports that consider the intermeniscal ligament [8, 16] in the anterior and medial tibial eminence [8] in the posterior landmarks. However, these landmarks are difficult to reproduce due to the fact that they are determined by the distance from its target, making them unreliable landmarks to define an accurate position for bone tunnel construction in the varying tibial footprint. Moreover, recent detailed anatomical studies suggest that the posterior border of the ACL footprint is positioned relatively anterior to what has been previously believed with narrower bounds in the AP aspect [1, 14, 17], and a clinical application of these traditional methods to current reconstructive procedures was difficult. We utilized both macro-/microscopic observation and CT images to study the positions of the attachment boundaries and its surrounding tissues in detail, and we presented a method for bone tunnel creation with the aforementioned bony/anatomical landmarks in order to standardize surgical management. In our study, a square structure (Fig. 4.6) consisting of the following landmarks can be observed: ACL footprint, anterior; anterior ridge, medial; medial intercondylar ridge (anteromedial; L-shaped ridge), lateral; and anterior horn of the lateral meniscus, posterior; in addition, the anterior border of the medial and lateral intercondylar tubercles is invariable, regardless of size and morphology. In our anatomical study, we believe that if bone tunnels are positioned within this square structure, we can create bone tunnels with reproducibility.
Ideal tunnel position for (a) single-bundle reconstruction, (b) double-bundle reconstruction from our results. White dot line, L-shaped ridge; red line, attachment of anterior horn of lateral meniscus; blue dot line, anterior margin of the medial and lateral intercondylar tubercle; yellow circle, tibial tunnel for single-bundle ACL reconstruction; red circle, tibial tunnel of anteromedial bundle for double-bundle ACL reconstruction; blue circle, tibial tunnel of posterolateral bundle for double-bundle ACL reconstruction
6.3 Anatomical Pitfalls of Tibial Tunnel Creation
From recent studies, there are two important points that we must consider when creating tibial bone tunnels. Firstly, the tibial tunnel position greatly affects graft obliquity in the sagittal and coronal plane that is extremely important in obtaining postoperative stability for ACL reconstruction. Hatayama et al. reported that positioning the tibial tunnel anteriorly obtains better postoperative anterior knee stability [18]. Inderhaug stated that the posterior placement of the tibial tunnel had inferior rotational stability and clinical scores compared to anterior tibial tunnel placement [19]. Zampeli reported a greater rotational instability of the tibia with less oblique graft in the coronal plane and recommended a more anteromedial placement of the tunnel on the tibial side [20]. Anterior placement of the tibial tunnel was previously thought to induce the risk of graft failure or limitation in range of motion due to roof impingement. However, recent studies have proved that such risks from the anterior placement of the tibial tunnel are rather low [21–23], and we believe that the anteromedial placement of the tibial tunnel within the anatomical tibial footprint is a method we can endorse.
The second point is that the ACL attachment is extremely proximate to the anterior horn of the lateral meniscus attachment. Several articles reported the proximity of the ACL tibial attachment and the anterior horn of the lateral meniscus attachment, and in addition, that creating a bone tunnel in the center of the attachment site reduced the surface area, lowering the pullout strength [24–26]. Our detailed macroscopic/histological observation also established that the anterior horn of the lateral meniscus is positioned centrally as it runs posteriorly. The lateral meniscus is attached on the base of the lateral groove and lateral side of the bony protrusion, and the attachment is positioned more centrally at the posterolateral margin of the ACL tibial footprint and almost anteriorly to the lateral intercondylar tubercle. Thus, surgeons should be aware that there is risk of damaging the anterior horn of the lateral meniscus attachment when creating a large bone tunnel in the center of the tibial footprint for single-bundle reconstruction and positioning the PL bone tunnel posterolaterally to the attachment site for double-bundle reconstruction. From the two aforementioned points, the bone tunnel should be created anteromedially within the square structure for single-bundle reconstruction (Fig. 4.6). Like single-bundle reconstruction, the AM bone tunnel should be positioned anteromedially within the attachment site for double-bundle reconstruction, and the PL bone tunnel should be positioned posterior, not posterolateral, to the AM bone tunnel to avoid damaging the anterior horn of the lateral meniscus attachment. To this end, we believe that the L-shaped ridge we have proposed may be an important landmark for anteromedial placement of the tibial tunnel.
7 Conclusion
The debate in terms of the morphology and structure of the ACL has continued to this day. The choice of graft material and tunnel position of ACL reconstruction is dependent on how various evidences from the current anatomical literature are interpreted. Our proposed method for tibial tunnel creation is greatly simplified, and we believe that our results and method for tibial tunnel creation can be usefully applied to any reconstruction technique; furthermore, we strongly believe that accurate reproducibility of tibial tunnel creation can be achieved by its standardization.
References
Tensho K, Shimodaira H, Aoki T, Narita N, Kato H, Kakegawa A, Fukushima N, Moriizumi T, Fujii M, Fujinaga Y, Saito N (2014) Bony landmarks of the anterior cruciate ligament tibial footprint: a detailed analysis comparing 3-dimensional computed tomography images to visual and histological evaluations. Am J Sports Med 18:1433–1440
Purnell ML, Larson AI, Clancy W (2008) Anterior cruciate ligament insertions on the tibia and femur and their relationships to critical bony landmarks using high-resolution volume-rendering computed tomography. Am J Sports Med 36:2083–2090
Berg EE (1993) Parsons’ knob (tuberculum intercondylare tertium). A guide to tibial anterior cruciate ligament insertion. Clin Orthop Relat Res 292:229–231
Ziegler CG, Pietrini SD, Westerhaus BD, Anderson CJ, Wijdicks CA, Johansen S, Engebretsen L, LaPrade RF (2011) Arthroscopically pertinent landmarks for tunnel positioning in single-bundle and double-bundle anterior cruciate ligament reconstructions. Am J Sports Med 39:743–752
Hutchinson MR, Bae TS (2001) Reproducibility of anatomic tibial landmarks for anterior cruciate ligament reconstructions. Am J Sports Med 29:777–780
Girgis FG, Marshall JL, Monajem A (1975) The cruciate ligaments of the knee joint. Anatomical, functional and experimental analysis. Clin Orthop Relat Res 106:216–231
Tállay A, Lim MH, Bartlett J (2008) Anatomical study of the human anterior cruciate ligament stump’s tibial insertion footprint. Knee Surg Sports Traumatol Arthrosc 16:741–746
Ferretti M, Doca D, Ingham SM, Cohen M, Fu FH (2012) Bony and soft tissue landmarks of the ACL tibial insertion site: an anatomical study. Knee Surg Sports Traumatol Arthrosc 20:62–68
Odensten M, Gillquist J (1985) Functional anatomy of the anterior cruciate ligament and a rationale for reconstruction. J Bone Joint Surg Am 67:257–262
Heming JF, Rand J, Steiner ME (2007) Anatomical limitations of transtibial drilling in anterior cruciate ligament reconstruction. Am J Sports Med 35:1708–1715
Colombet P, Robinson J, Christel P, Franceschi JP, Djian P, Bellier G, Sbihi A (2006) Morphology of anterior cruciate ligament attachments for anatomic reconstruction: a cadaveric dissection and radiographic study. Arthroscopy 22:984–992
Edwards A, Bull AM, Amis AA (2007) The attachments of the anteromedial and posterolateral fibre bundles of the anterior cruciate ligament: part 1: tibial attachment. Knee Surg Sports Traumatol Arthrosc 15:1414–1421
Otsubo H, Shino K, Suzuki D, Kamiya T, Suzuki T, Watanabe K, Fujimiya M, Iwahashi T, Yamashita T (2012) The arrangement and the attachment areas of three ACL bundles. Knee Surg Sports Traumatol Arthrosc 20:127–134
Siebold R, Schuhmacher P, Fernandez F, Śmigielski R, Fink C, Brehmer A, Kirsch J (2015) Flat midsubstance of the anterior cruciate ligament with tibial “C”-shaped insertion site. Knee Surg Sports Traumatol Arthrosc 23:3136–3142
Morgan CD, Kalman VR, Grawl DM (1995) Definitive landmarks for reproducible tibial tunnel placement in anterior cruciate ligament reconstruction. Arthroscopy 11:275–288
Kongcharoensombat W, Ochi M, Abouheif M, Adachi N, Ohkawa S, Kamei G, Okuhara A, Shibuya H, Niimoto T, Nakasa T, Nakamae A, Deie M (2011) The transverse ligament as a landmark for tibial sagittal insertions of the anterior cruciate ligament: a cadaveric study. Arthroscopy 27:1395–1399
Hara K, Mochizuki T, Sekiya I, Yamaguchi K, Akita K, Muneta T (2009) Anatomy of normal human anterior cruciate ligament attachments evaluated by divided small bundles. Am J Sports Med 37:2386–2391
Hatayama K, Terauchi M, Saito K, Higuchi H, Yanagisawa S, Takagishi K (2013) The importance of tibial tunnel placement in anatomic double-bundle anterior cruciate ligament reconstruction. Arthroscopy 29:1072–1078
Inderhaug E, Strand T, Fischer-Bredenbeck C, Solheim E (2014) Effect of a too posterior placement of the tibial tunnel on the outcome 10–12 years after anterior cruciate ligament reconstruction using the 70-degree tibial guide. Knee Surg Sports Traumatol Arthrosc 22:1182–1189
Zampeli F, Ntoulia A, Giotis D, Tsiaras VA, Argyropoulou M, Pappas E, Georgoulis AD (2012) Correlation between anterior cruciate ligament graft obliquity and tibial rotation during dynamic pivoting activities in patients with anatomic anterior cruciate ligament reconstruction: an in vivo examination. Arthroscopy 28:234–246
Plaweski S, Rossi J, Merloz P, Julliard R (2011) Analysis of anatomic positioning in computer-assisted and conventional anterior cruciate ligament reconstruction. Orthop Traumatol Surg Res 97:S80–S85
Iriuchishima T, Tajima G, Ingham SJ, Shen W, Smolinski P, Fu FH (2010) Impingement pressure in the anatomical and nonanatomical anterior cruciate ligament reconstruction: a cadaver study. Am J Sports Med 38:1611–1617
Jagodzinski M, Richter GM, Pässler HH (2000) Biomechanical analysis of knee hyperextension and of the impingement of the anterior cruciate ligament: a cinematographic MRI study with impact on tibial tunnel positioning in anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 8:11–19
Watson JN, Wilson KJ, LaPrade CM, Kennedy NI, Campbell KJ, Hutchinson MR, Wijdicks CA, LaPrade RF (2015) Iatrogenic injury of the anterior meniscal root attachments following anterior cruciate ligament reconstruction tunnel reaming. Knee Surg Sports Traumatol Arthrosc 23:2360–2366
LaPrade CM, Smith SD, Rasmussen MT, Hamming MG, Wijdicks CA, Engebretsen L, Feagin JA, LaPrade RF (2015) Consequences of tibial tunnel reaming on the meniscal roots during cruciate ligament reconstruction in a cadaveric model, Part 1: the anterior cruciate ligament. Am J Sports Med 43:200–206
LaPrade CM, Ellman MB, Rasmussen MT, James EW, Wijdicks CA, Engebretsen L, LaPrade RF (2014) Anatomy of the anterior root attachments of the medial and lateral menisci: a quantitative analysis. Am J Sports Med 42:2386–2392
Kopf S, Pombo MW, Szczodry M, Irrgang JJ, Fu FH (2011) Size variability of the human anterior cruciate ligament insertion sites. Am J Sports Med 39:108–113
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer Japan
About this chapter
Cite this chapter
Tensho, K. (2016). Tibial Insertion of the ACL: 3D-CT Images, Macroscopic, and Microscopic Findings. In: Ochi, M., Shino, K., Yasuda, K., Kurosaka, M. (eds) ACL Injury and Its Treatment. Springer, Tokyo. https://doi.org/10.1007/978-4-431-55858-3_4
Download citation
DOI: https://doi.org/10.1007/978-4-431-55858-3_4
Published:
Publisher Name: Springer, Tokyo
Print ISBN: 978-4-431-55856-9
Online ISBN: 978-4-431-55858-3
eBook Packages: MedicineMedicine (R0)