Abstract
Blood pressure target in the initial stabilization of patients with shock is a key point for the clinician. We will focus in this chapter on blood pressure targets in the setting of septic shock.
The aim of this chapter is to understand the physiological rationale and clinical evidence for low pressure threshold, high pressure threshold, and increasing mean arterial pressure. The beneficial and harmful effects of such increase will be discussed. Finally, the prerequisites and the difficulties of an individual approach for blood pressure targes will be discussed.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
FormalPara Learning ObjectivesIn this chapter, students will:
-
Understand the potential benefits and harm of increasing blood pressure.
-
Learn the knowledge regarding low- and high-pressure threshold according to what is known from the literature.
-
Understand the prerequisites and the difficulties of an individual approach for blood pressure targets.
1 Introduction
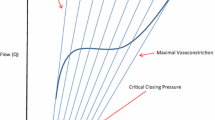
Circulatory shock is defined as the imbalance between oxygen delivery and demand and may be associated with systemic arterial hypotension (systolic arterial pressure less than 90 mm Hg or mean arterial pressure less than 70 mm Hg), clinical signs of hypoperfusion, and increase in arterial lactate [1]. Physiologically, cardiac output and systemic arterial pressures are pulsatile. The physiological role of the arterial bed is to demodulate the pulsatile flow via resistive arteries and to decrease arterial blood pressure in order to perfuse capillaries with the lowest acceptable intraluminal pressure. The adequacy of peripheral perfusion blood pressure and the microcirculatory blood flow is maintained only within the range of physiological mean arterial pressure. When MAP decreases below a critical threshold value, organ blood flow becomes dependent from perfusion pressure. This leads to organ hypoperfusion and then to organ dysfunction and ultimately to organ failure. Some organs (heart, brain, and kidneys) have an adaptive mechanism to blood pressure variations called autoregulation. Autoregulation is the ability of organs to keep the blood flow rate constant entering the organ, no matter what the perfusion pressure is, over a range of values that is the “autoregulation range” [2]. The autoregulation relationship is presented in ◘ Fig. 29.1. Autoregulation threshold values vary among organs as well as between individuals [3,4,5], for example, kidney circulation has the highest autoregulation threshold values [3]. In addition, autoregulation thresholds differ in accordance with patient’s comorbidities, especially in case of chronic hypertension.
MAP, mean arterial pressure; A, lower critical value of MAP; B, higher critical value of MAP. The autoregulation zone is between the vertical lines. When MAP fall under a critical perfusion pressure (point A), organ blood flow becomes dependent on pressure level, and this relationship was reported in the heart, brain, and kidney [2,3,4]. On the right side of the autoregulation zone, organ blood flow is dependent on pressure level and was reported in the brain circulation [5]. In case of chronic hypertension, the relationship between MAP and blood flow is right-shifted, as presented with the black arrow [5]
It must be emphasized that a low systemic pressure is associated with decreased microcirculatory blood flow and that the correction of MAP does not necessarily improve microcirculatory blood flow, as many other mechanisms are involved in the microcirculatory blood flow dysfunction (endothelial dysfunction, impaired inter-cell communication, altered glycocalyx, adhesion and rolling of white blood cells as well as platelets, and altered red blood cell deformability) [6].
The determinants of MAP are cardiac output, systemic arterial resistance, and venous return. During shock, one or more of these determinants fail, and MAP decreases when physiological compensatory mechanisms are overwhelmed. MAP is commonly accepted as a surrogate of organ perfusion pressures and is therefore a main target for hemodynamic resuscitation. To increase MAP and obtain the target MAP, fluids (in shock states with decreased venous return) and vasopressors are required. Norepinephrine is the first recommended vasoactive drug and stimulates alpha- and beta-receptors. Consequently, norepinephrine increases both systemic vascular resistances and cardiac output. A high target of MAP requires a higher load of vasopressor drug and may induce excessive arterial systemic vasoconstriction, which in turn may induce organ ischemia.
Consequently, the main challenge for the clinician driving the early hemodynamic resuscitation phase of patients with shock is to set the vasopressor infusion rate to target MAP within the adequate pressure range to avoid from one hand a low perfusion pressure and, from the other hand, excessive vasoconstriction and other side effects due to vasoactive drug such as arrhythmias.
Currently, for resuscitation of hemorrhagic shock, there is no available data supporting specific blood pressure targets as stated by the recommendations [7, 8]. The only randomized controlled trial focusing on systolic arterial pressure in patients with hemorrhagic shock and without traumatic brain injuries aimed at comparing early aggressive fluid resuscitation to maintain systolic blood pressure above 100 mm Hg versus delayed fluid administration with permissive low systolic blood pressure until bleeding control. The aggressive fluid resuscitation strategy was associated with higher mortality rate [9]. Therefore, the European guidelines suggest to tolerate a lower level of blood pressure in patients with uncontrolled bleeding without severe head injury with a recommendation of weak level with low quality of evidence [8].
In the setting of cardiogenic shock, it should be underlined that currently, no clinical studies so far have attempted to assess the optimal blood pressure level [8, 10]. This may explain the absence of formal recommendations.
Therefore, in this chapter, we will focus on the blood pressure targets in the initial resuscitation of patients with septic shock.
2 MAP Target in the Initial Stabilization: Is There a Low Threshold?
Many retrospective, observational, and interventional studies investigated whether a specific MAP level was associated with main outcomes such as mortality and/or acute kidney injury.
2.1 Relationship Between Low MAP Threshold and Mortality
In a retrospective study based on continuous MAP recordings during the first 48 hours of resuscitation in patients with septic shock, Varpula et al. reported that the threshold of 65 mm Hg was the best to predict mortality at day 30. The longer the time spent below this threshold, the higher was the mortality rate [11]. Similarly, in another retrospective study based on the same design, the mortality rate at day 28 was higher when MAP was below threshold of 60 mm Hg. Interestingly, there was a linear relationship between the time spent below this threshold Hg and mortality rate [12]. In contrast, targeting a MAP value of 70 mm Hg or higher was not associated with improved survival [13].
To assess whether increasing MAP target improves survival, a multicenter randomized controlled trial (SEPSISPAM trial) compared a MAP target of 65–70 mmHg (low-target group) with that of 80–85 mmHg (high-target group). This pragmatic study failed to show any mortality difference between the two groups at day 28 (primary endpoint) and at day 90 [14].
In the randomized controlled OVATION pilot trial [15], target MAP of 60–65 mmHg was compared to a target MAP of 75–80 mmHg with no difference in mortality at day 28. Interestingly, in the subgroup of patients aged 75 years and older, a lower MAP target was associated with reduced mortality.
2.2 Relationship Between Low MAP Threshold and Kidney Function
In the literature, the impact of MAP target on organ function has been studied only through the evaluation of kidney function. A retrospective study suggests that a higher MAP target could be mandatory to prevent acute kidney injury (AKI) occurrence [12].
The impact of MAP level in the first hours of resuscitation regarding kidney failure occurrence is a key point. Two observational studies reported that in patients with septic shock with early AKI, those who experienced persistent or worsened AKI had lower MAP during their initial hemodynamic management [16, 17].
Three prospective studies, all only recruiting a small number of patients, have tested the effects on renal function of incremental thresholds of MAP, achieved by increasing norepinephrine infusion. MAP was increased from 65 to 75 and then 85 mm Hg. None of these studies demonstrated any beneficial effect on renal function. It should be noticed that in these studies, the timing of the intervention was not mentioned and, hence, delayed intervention after initial stabilization cannot be ruled out (fluids administration and vasopressors infusion) [18,19,20]. The results of these studies are presented in ◘ Table 29.1.
The incidence of renal failure was a secondary outcome in the SEPSISPAM trial. There was no difference in renal outcomes (renal replacement therapy requirement, doubling in serum creatinine level) between the low- and high-target groups [14]. In the predefined subgroup of chronic hypertensive patients, the high-target group required less renal replacement therapy as compared with low-pressure target patients. Conversely to the abovementioned short-term studies, SEPSISPAM trial recruited patients very early within the 6 first hours after initiation of norepinephrine infusion. This may have favorably impacted the renal failure and may suggest a reversibility part of renal dysfunction in the early phase of septic shock.
3 MAP Target in the Initial Stabilization: Is There a High Threshold?
An accurate analysis of the randomized controlled trials, where MAP was reported in patients with septic shock, shows that MAP raised up to 80 mm Hg in studies aimed at comparing vasoactive drugs in patients with septic shock (CATS, comparison of epinephrine versus the association of dobutamine and norepinephrine [21]; VASST, comparison of vasopressin versus norepinephrine [22]; SOAP 2, comparison of dopamine versus norepinephrine [23]). None of these studies reported excessive incidence of ischemic events.
Conversely in 2004, Lopez et al. reported the results of a randomized controlled trial aimed at comparing L-NMMA, a nitric oxide synthase inhibitor, versus norepinephrine, in patients with septic shock. The trial was stopped prematurely for excess in mortality in L-NMMA-treated patients. Interestingly, patients treated with L-NMMA had a higher MAP, and 25% of the patients even had MAP values higher than 90 mm Hg. Whether the higher mortality rate was related to the high MAP level and/or the drug per se remained open.
The direct comparison of two levels of MAP in patients with septic shock in the SEPSISPAM and OVATION trials did not report a significant benefit in favor of the higher MAP targets. In contrast, increasing MAP in patients with septic shock was associated with significantly more frequent arrhythmias, e.g., new onset atrial fibrillation. In turn, de novo atrial fibrillation was reported to be associated with higher mortality in patients with severe sepsis [24]. In that study, Walkey et al. assessed the impact of new onset atrial fibrillation in the setting of severe sepsis: on the 49,082 septic patients included in this study, new onset atrial fibrillation occurred in 5.9% of patients and was associated with significantly higher mortality (56% versus 36%).
4 MAP Target in the Initial Stabilization: An Individual Approach for MAP Target?
The recent version of the surviving Sepsis campaign guidelines recommends adaptating MAP target to the patient’s condition, using an individualized approach [8, 25]. However, in the daily life, this approach may be challenging for clinicians.
First, outside the intensive care unit setting, the SPRINT randomized controlled trial compared a maximal target of 120 mmHg (intensive treatment) for systolic arterial pressure (SAP) with that of a target of 140 mmHg (standard treatment) in nondiabetic patients with cardiovascular comorbidities. The primary outcome was a composite of significant cardiovascular events (myocardial infarction, stroke, heart failure, and/or death from cardiovascular causes). Albeit the primary composite outcome and mortality were lower in the intensive treatment group, serious adverse events were significantly more frequent in these patients, and especially AKI occurred more frequently [26]. Outside the intensive care unit, lowering blood pressure is apparently beneficial when regarding cardiovascular outcome and mortality, but this therapeutic strategy remains at risk for renal function. Altogether, the results of the SPRINT and SEPSISPAM trials suggest that kidney function may benefit from higher range of blood pressure in patients with chronic hypertension. Nevertheless, a “kidney-centered” resuscitation should be balanced with side effects such as arrhythmias as well as survival outcome related to the timing of norepinephrine infusion. Indeed, the most recent individual patient data meta-analysis showed that increasing MAP after 6 h of norepinephrine infusion start was associated with significant higher mortality rates and thus confirmed the significantly higher rate of cardiac side effects in the high MAP target group [27].
Hence, the individualization of blood pressure targets is complex. Age [15], chronic hypertension [14], and delay of vasopressor start [27] have been reported to impact mortality and renal outcomes. These clinical features should be balanced with the risk of new onset arrhythmias (please refer to ◘ Table 29.2).
-
At the initial phase of hemodynamic management in patients with septic shock, according to available data as well as the most recent guidelines, a MAP target of 65 mm Hg is recommended [8, 25].
-
In particular situation, e.g., chronic hypertension, a higher MAP target could be considered but requires a higher vasopressor load which may be associated with cardiovascular side effects. Therefore, increasing MAP target above 65 mm Hg must be cautiously weighted.
Take-Home Messages
-
In the initial resuscitation, relevant blood pressure target is MAP.
-
The objective of resuscitation is to restore MAP into autoregulation range.
-
In clinical practice, MAP target is 65 mmHg.
-
MAP target should be individualized taking in account the benefit risk ratio of high vasopressor load.
Conclusion
To date, blood pressure target remains a controversial subject during the initial resuscitation of patients with septic shock. A MAP target of 65 mm Hg is recommended. Some patients may benefit from higher targets, but such increases in MAP may be associated with a higher vasopressor load and more frequent cardiac side effects.
References
Finfer SR, Vincent J-L, Vincent J-L, De Backer D. Circulatory shock. N Engl J Med. 2013;369:1726–34.
Johnson PC. Autoregulation of blood flow. Circ Res. 1986;59:483–95.
Bellomo R, Wan L, May C. Vasoactive drugs and acute kidney injury. Crit Care Med. 2008;36:S179–86.
Cupples WA, Braam B. Assessment of renal autoregulation. Am J Physiol Renal Physiol. 2007;292:F1105–23.
Strandgaard S, Olesen J, Skinhoj E, Lassen NA. Autoregulation of brain circulation in severe arterial hypertension. Br Med J. 1973;1:507–10.
De Backer D, Donadello K, Taccone F, Ospina-Tascon G, Salgado D, Vincent J-L. Microcirculatory alterations: potential mechanisms and implications for therapy. Ann Intensive Care. 2011;1:27.
Rochwerg B, Hylands M, Møller MH, et al. CCCS-SSAI WikiRecs clinical practice guideline: vasopressor blood pressure targets in critically ill adults with hypotension and vasopressor use in early traumatic shock. Intensive Care Med. 2017;43:1062–4.
Cecconi M, De Backer D, Antonelli M, et al. Consensus on circulatory shock and hemodynamic monitoring. Task force of the European Society of Intensive Care Medicine. Intensive Care Med. 2014;40:1795–815.
Bickell WH, Wall MJ, Pepe PE, Martin RR, Ginger VF, Allen MK, Mattox KL. Immediate versus delayed fluid resuscitation for hypotensive patients with penetrating torso injuries. N Engl J Med. 1994;331:1105–9.
O’Gara PT, Kushner FG, Ascheim DD, et al. 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Circulation. 2013;127:e362–425.
Varpula M, Tallgren M, Saukkonen K, Voipio-Pulkki L-M, Pettilä V. Hemodynamic variables related to outcome in septic shock. Intensive Care Med. 2005;31:1066–71.
Dünser MW, Takala J, Ulmer H, Mayr VD, Luckner G, Jochberger S, Daudel F, Lepper P, Hasibeder WR, Jakob SM. Arterial blood pressure during early sepsis and outcome. Intensive Care Med. 2009;35:1225–33.
Dünser MW, Ruokonen E, Pettilä V, Ulmer H, Torgersen C, Schmittinger CA, Jakob S, Takala J. Association of arterial blood pressure and vasopressor load with septic shock mortality: a post hoc analysis of a multicenter trial. Crit Care. 2009;13:R181.
Asfar P, Meziani F, Hamel J-F, et al. High versus low blood-pressure target in patients with septic shock. N Engl J Med. 2014;370:1583–93.
Canadian Critical Care Trials Group, Lamontagne F, Meade MO, et al. Higher versus lower blood pressure targets for vasopressor therapy in shock: a multicentre pilot randomized controlled trial. Intensive Care Med. 2016;42:542–50.
Badin J, Boulain T, Ehrmann S, et al. Relation between mean arterial pressure and renal function in the early phase of shock: a prospective, explorative cohort study. Crit Care. 2011;15:R135.
Poukkanen M, Wilkman E, Vaara ST, et al. Hemodynamic variables and progression of acute kidney injury in critically ill patients with severe sepsis: data from the prospective observational FINNAKI study. Crit Care Lond Engl. 2013;17:R295.
Deruddre S, Cheisson G, Mazoit J-X, Vicaut E, Benhamou D, Duranteau J. Renal arterial resistance in septic shock: effects of increasing mean arterial pressure with norepinephrine on the renal resistive index assessed with Doppler ultrasonography. Intensive Care Med. 2007;33:1557–62.
LeDoux D, Astiz ME, Carpati CM, Rackow EC. Effects of perfusion pressure on tissue perfusion in septic shock. Crit Care Med. 2000;28:2729–32.
Bourgoin A, Leone M, Delmas A, Garnier F, Albanèse J, Martin C. Increasing mean arterial pressure in patients with septic shock: effects on oxygen variables and renal function*. Crit Care Med. 2005;33:780–6.
Annane D, Vignon P, Renault A, et al. Norepinephrine plus dobutamine versus epinephrine alone for management of septic shock: a randomised trial. Lancet Lond Engl. 2007;370:676–84.
Russell JA, Walley KR, Singer J, et al. Vasopressin versus norepinephrine infusion in patients with septic shock. N Engl J Med. 2008;358:877–87.
De Backer D, Biston P, Devriendt J, et al. Comparison of dopamine and norepinephrine in the treatment of shock. N Engl J Med. 2010;362:779–89.
Walkey AJ, Wiener RS, Ghobrial JM, Curtis LH, Benjamin EJ. Incident stroke and mortality associated with new-onset atrial fibrillation in patients hospitalized with severe Sepsis. JAMA. 2011; https://doi.org/10.1001/jama.2011.1615.
Rhodes A, Evans LE, Alhazzani W, et al. Surviving sepsis campaign: international guidelines for management of sepsis and septic shock: 2016. Intensive Care Med. 2017;43:304–77.
The SPRINT Research Group. A randomized trial of intensive versus standard blood-pressure control. N Engl J Med. 2015;373:2103–16.
Lamontagne F, Day AG, Meade MO, et al. Pooled analysis of higher versus lower blood pressure targets for vasopressor therapy septic and vasodilatory shock. Intensive Care Med. 2018;44:12–21.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 European Society of Intensive Care Medicine
About this chapter
Cite this chapter
Demiselle, J., Radermacher, P., Asfar, P. (2019). Blood Pressure Targets in the Initial Stabilization. In: Pinsky, M.R., Teboul, JL., Vincent, JL. (eds) Hemodynamic Monitoring. Lessons from the ICU. Springer, Cham. https://doi.org/10.1007/978-3-319-69269-2_29
Download citation
DOI: https://doi.org/10.1007/978-3-319-69269-2_29
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-69268-5
Online ISBN: 978-3-319-69269-2
eBook Packages: MedicineMedicine (R0)