Abstract
Intraoperative ultrasound has been used for brain tumor surgery since more than 30 years now. In glioma surgery, taking into account the latest advances in ultrasound technology and its integration in a neuronavigation system intraoperative ultrasound is absolutely competitive with more recent imaging or visualization tools like 5-aminolevulinic acid fluorescence and intraoperative MRI. Intraoperative ultrasound allows for precise tumor depiction and intraoperative orientation in various indications. The actual chapter provides information about typical indications for intraoperative ultrasound in brain tumor surgery. It provides a guide for typical transducers and describes the depiction of intracranial lesions in B-mode ultrasound. During the course of resection, intraoperative ultrasound is prone to artifacts. Thus, a description of the most typical artifacts in intracranial surgery and a practical guide how optimize image quality and to avoid artifacts is given in this chapter.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
1 Introduction
Intraoperative ultrasound for brain tumor surgery is an established technique in clinical routine. Application is noninvasive and cheap and can be applied repetitively during any stage of surgery without any harm for the patient [1]. Since the first description of intraoperative ultrasound (iUS) for neurosurgical use in 1982 by Chandler et al. [2], it has mainly been used for brain tumor surgery. Especially when approaching invasive intraaxial lesions, classical landmarks are often missing. iUS allows for a good orientation in these situations. Additionally, brain shift might change the anatomy significantly. Until introduction of intraoperative MRI (iMRI), iUS was the only means of intraoperative imaging depicting residual tumor during surgery [3]. Since its first use in neurosurgery until present, imaging capability has improved significantly. Dedicated probes for dedicated indications are available. Another important innovation is the integration of ultrasound devices into neuronavigation systems [4, 5]. By this method, iUS images can be referenced to a preoperative MRI dataset, which is displayed in the reconstructed plane of the 2D ultrasound image. Thus, interpretation of ultrasound findings becomes much easier and occurring brain shift can be identified early by comparing landmarks between intra and preoperative images. The main challenge when using iUS is interpretation of imaging findings. Especially during the course of surgery, artifacts might increase and identification of residual tumor can get challenging.
In the actual chapter, we will elucidate indications, techniques, and devices to optimize image quality in ultrasound-assisted brain tumor surgery.
2 Indications
As far as our experience goes, there is an indication for the use of ultrasound in every intraaxial brain tumor surgery. Each surgical step has its typical applications. At first, before incision of the dura, ultrasound helps to assess whether the target lesion is centered in the craniotomy (Fig. 5.1). Thus a simple verification of neuronavigation can be performed, and if needed, based on iUS findings, a safe extension of craniotomy can be performed before dural opening. Second, after dural opening by release of CSF or brain swelling, a significant brain shift may occur which unexpectedly changes surgical anatomy. At this step of surgery, a quick ultrasound sweep might help to identify the targeted lesion and important landmarks close by (Fig. 5.2). Further, the ultrasound provides information which gyrus is infiltrated and which might be spared. Since intraoperative ultrasound provides real-time information, when in doubt iUS provides more reliable information compared to neuronavigation.
Intraoperative screenshot of the neuronavigation system with an integrated 15 Mhz linear array transducer. The probes is at a coronary position depicting the border of an anaplastic astrocytoma between superior and medial temporal gyrus, right after dural opening before beginning of tumor resection. In the neuronavigation system, the targeted lesion is depicted with a white line. The white arrows show the direction of the occuring brain shift. Due to brainswelling the tumor is pushed in the direction of the ultrasound probe while it appears deeper in the corresponding MRI image of the neuronavigation
In case of marked brain swelling due to large tumors with cystic components, intraoperative sonography allows for save inline cyst puncture or even ventricular puncture before removal of the solid tumor mass. By this means, a lot of tension is relieved which eases further dissection. If a deep-seated lesion is approached, an ultrasound-based planning of a trajectory is recommended for first, not missing the lesion. Second, the appropriate sulcus leading to a lesion can be verified (Fig. 5.3). During the course of surgery, we recommend using the ultrasound probe from time to time to adapt to surgically induced changes of the tumor or brain surface. Thus, it is easier to distinguish artifacts from residual tumor at a later stage of surgery (Fig. 5.4). Additionally adjacent structures like corpus callosum or the ventricles can be identified and the remaining distance tracked (Fig. 5.5). The short time consumed by the use of the iUS during tumor resection is easily outweighed by the increase of speed after gaining a confident idea of the surrounding structures.
Chronological screenshots of the neuronavigation system using linear array intraoperative ultrasound as a resection control. (1) Precise localization of the affected gyrus (upper row). (2) Identification of residual tumor and its adjacent anatomical structures (middle row). (3) Final inspection after tumor removal (lower row) (Copyright Coburger Acta neurochiru. 2015. Springer)
Despite intraoperative orientation, the main indication for iUS while approaching intraaxial lesion is residual tumor assessment. Especially in low-grade glioma surgery, distinguishing between most likely tumor-free tissue and invasive glioma areas is challenging. Extent of resection is a significant predictor of overall survival in low- as well as high-grade gliomas [6, 7]. Intraoperative ultrasound helps to increase extent of resection [8]. Most contemporary iUS probes for intracranial use can discriminate between tumor and normal brain tissue at least at the beginning of surgery. In the chapter “tumor depiction,” we will elucidate visibility of intraaxial tumors in more detail. An issue while performing iUS for residual tumor control is the appearance of surgery-induced artifacts which lead to a lower specificity of iUS during the course of surgery [9]. Surgeons should be aware of possible false-positive findings due to blood or local brain contusions. We will discuss the different types of artifacts and options for image optimization later on in this chapter.
When using iUS referenced to a neuronavigation device, some systems provide the option for intraoperative 3D dataset acquisition. This allows to acquire a new intraoperative image set as a base for neuronavigation comparable to an intraoperative MRI Scan. We will comment on the topic of navigated iUS later on during this chapter.
3 Ultrasound Transducers for Intracranial Use
Ultrasound transducers for intracranial use need to have a small aperture to be positioned in typical craniotomies. Basically, there are 3 types of ultrasound transducers. Naming is based on the positioning of the piezoelectric crystals in the tip of the probes (Fig. 5.6).
The illustration shows the most commonly used types of transducers: (left to right) A linear array transducer produces parallel sound waves. Thus, resolution theoretically stays the same independent from depth. However the higher frequency leads to a decreased penetration depth. Sector array transducers have a small aperture and provide a trapezoid image. Therefore resolution is high close to the transducer and gets lower with increasing depth; however field of view is enlarged in the same matter. Thus, it allows for a wide field of view through small openings. A curved array transducer has a curved arrangement of the piezoelectric elements. It combines the previous transducer types. Penetration depth and field of view are increased while the field of view and the resolution close to the probe are still acceptable. Matrix array transducers are a special type of sector array transducers with piezoelectric elements arranged like on a chessboard. Thus, a real-time 3D image can be created
Linear array transducers are producing parallel ultrasonic waves, thus creating a rectangular image with high-resolution and little artifacts. Based on the parallel sound waves, broadness of image is limited by the aperture of the transducer. Therefore overview is limited in probes with a small footprint which are needed for intracranial use. Usually high frequencies are used for linear transducers leading to a high image resolution. However, there is an inverse correlation of penetration depth and increasing frequency. Typical frequencies used are 7–15 Mhz allowing for a penetration depth roughly from 2 to 7 cm. These parameters are highly variable based on tissue and transducer used.
Sector array transducers provide a triangular image leading to an increasing field of view and due to lower ultrasound frequencies increasing penetration depth. Typical frequencies are 4–8 Mhz. A sector array transducer has a small footprint; therefore it can be used even in small craniotomies or burr holes while still providing a useful overview of the tissue beneath [10]. Apparently, resolution is lower as in linear array transducers. Especially, increasing penetration depth is going along with decreased lateral resolution as the ultrasound waves are diverging. Matrix array transducers are a special type of sector array transducers with piezoelectric elements arranged like a chessboard. Thus, a real-time 3D image or live cross-plane visualization can be created. This increases overview and enhances understanding of the respective intracranial pathology [11].
Curved array transducers are using lower frequencies between 2 and 10 Mhz. The positioning of the piezoelectric elements provides a compromise between the both types mentioned above. Curved array ultrasound was developed for abdominal ultrasound in order to provide a good resolution for superficial liver ultrasound as well as deep lesions. Therefore in the past probes were rather large. With recent technical advances, smaller probes for intracranial use became available, too. While resolution close to the transducer is high, it still provides a good overview due to the trapezoid imaging shape. Additionally, a penetration depth which allows for a good intracranial overview is provided (Fig. 5.7).
Tangential iUS image of a supratentorial metastasis close to the falx using a curved array transducer. Tumor depiction after dural opening before start of tumor preparation (left). Final scan after tumor removal (right). Typical signals of residual blood at the floor of the resection cavity and along the tentorium. Residual tumor can only be excluded when comparing with previous images (no tumor along the tentorium). In comparison to the left image, a typical attenuation artifact is seen: The echo intensity of the cerebellar folia is increased (Images were provided by Mrs Nadji-Ohl, Department of Neurosurgery, Klinikum Stuttgart, Germany)
Depending on the indication several types of transducers may be required. Based on the technical features, the best compromise for typical intraaxial lesions is a small curved array transducer. For intraoperative use, hockey stick shaped linear array high-frequency transducer have been developed by several companies. The hockey stick shape allows for an intracavital use. Thus, penetration depth is not a limiting factor and the advantage of the high local resolution can be seized [12] (Fig. 5.8). In low- and high-grade glioma surgery, accuracy of residual tumor detection has been shown to be significantly higher as compared to conventional sector array probes [13, 14].
Typical application of a hockey stick-shaped linear array high-frequency transducer. Using the device, even small resection cavities can be scanned meticulously without use of a coupling fluid. Due to the small distance to the target and the absence of substances with different attenuation coefficients, attenuation artifacts are not relevant in this setup
All types of ultrasound transducers can be referenced to a conventional neuronavigation system (Brainlab Vector vision, Brainlab AG, Feldkirchen, Germany) [15–17] or are available for the SonoWand system (Trondheim, Norway) as a dedicated device of navigated intraoperative ultrasound [3].
4 Tumor Depiction
Echogenicity of an intracranial tumor is dependent on cell density. With increased cell density especially in high-grade gliomas or in metastasis, a strong hyperechogenic signal can be depicted. Therefore, in low-grade gliomas, differentiation of the border of the lesion again might be more challenging. This effect is more pronounced in sector or curved array transducers as in linear array probes (Fig. 5.9). As a first step, we recommend to optimize contrast between most likely tumor-free tissue and tumor even before dural opening. Thus, based on imaging settings and depth of the lesion contrast, focus and other imaging settings can be optimized before any artifacts will obscure vision. In general contrast between “uninfiltrated” brain tissue and tumor is higher when using a linear array transducer [18]. Using a high-resolution linear array device, normal subcortical tissue reflects very little signal and appears blackish. In Fig. 5.10 we provide a schematic table comparing signal intensity of typical anatomical structures (green), pathological structures (red and yellow), and surgically induced artifacts (gray). Obviously based on ultrasound conditions and transducers applied, a high variability may occur. Therefore, the provided gray scales have to be used as a schematic illustration and not as a calibration scale. Mair et al. established a grading system for ultrasound visibility of typical intracranial lesions and its discrimination at the border [19]. Grade 0 describes lesions that are not visible. Grade 1 describes tumors difficult to visualize without an exact border with normal brain tissue. Grade 2 is a clearly identifiable lesion lacking a clear boarder with normal brain tissue and grade 3 is a lesion clearly identifiable with a clear border with normal tissue. Figure 5.11 shows an illustration by the abovementioned authors describing grade I to grade III lesions. Figure 5.12 shows a characteristic of typical intracranial lesions by the same authors and the respective visibility using intraoperative ultrasound. The specific value of the cited study is that the authors used sector and linear array probes from 5 to 12 MHz. Therefore the data provide an extraordinary overview on ultrasound depiction in 105 intracranial lesions. Depiction of tumor borders is not only dependent on the quality of the ultrasound images but on the type of lesion itself. Especially diffuse low-grade gliomas and lymphomas do not have a histologically defined border. In high-grade gliomas, intraoperative ultrasound is capable to identify different multiforme compartments of the solid lesion (Fig. 5.13) like necrosis, cysts, bleedings, irregular dense tumor, and the invasion zone. Especially the latter is difficult to differentiate from edema. A direct comparison of intraoperative MRI and sector and linear array ultrasound showed that linear array ultrasound is more sensitive for tumor detection than the other two techniques. However, it also detects the infiltration zone of the lesions (Table 5.1 unpublished data by our group). Histologically in glioblastoma, 60–100 % of tumor cell density can be found between 6 and 14 mm distant to the border of contrast enhancement [20]. Thus, an “over detection” might be favored by the surgeon. However, caution must be paid close to eloquent areas: Even though Gd-DTPA contrast enhancement does not enter an eloquent area, it does not mean the tumor does. New motor or language deficits are not only associated with decreased quality of life but with significant decreased overall survival [21]. Thus, when using these very detailed and sensitive imaging techniques in eloquent areas, we recommend using intraoperative monitoring. Additionally, surgeons should always keep in mind that contrast enhancement in iMRI and tumor depiction using intraoperative ultrasound might not be congruent at the border of the lesion. From our experience especially in low-grade gliomas, the signal of the FLAIR sequence of iMRI matches very well with iUS. In these entities, when using the iUS referenced to the navigation system, we recommend performing a T2 space sequence providing a 3D dataset with isovoxel for a precise reconstruction of the corresponding pre- or intraoperative MRI image (Fig. 5.14) In HGG, the same goes for a T1 MPRAGE with contrast.
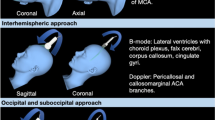
Ultrasonographic visibility of brain lesions. (a) Grade III: the lesion is clearly identifiable and has a clear border with normal tissue; artistic representation, preoperative CT with contrast, and intraoperative ultrasound; coronal image. T tumor, F falx, LV lateral ventricles. (b) The lesion is clearly identifiable but has no clear border with normal tissue; CT with contrast—mesial temporal tumor, power angio mode. Tumor and its relationship to neighboring vessels are visible. T tumor, WC Willis circle, PCA posterior cerebral artery. (c) The lesion is difficult to visualize and has no clear border with normal tissue but remains identifiable on MRI (T2). T tumor, F falx, CP choroid plexus in the lateral ventricles (Copyright Springer Mair et al. Acta neuro 2013)
Characterization of individual lesions using the grading system by Mair et al.: grade 0 describes lesions that are not visible. Grade 1 describes lesions difficult to visualize and no clear boarder with normal tissue. Grade 2 is a clearly identifiable lesion but no clear boarder with normal tissue and grade 3 is a lesion clearly identifiable with a clear boarder with normal tissue
During resection, even though there is still solid tumor depicted under the microscope, we recommend periodic quick iUS sweeps to identify remaining tumor. This approach allows continuous assessment of subtle changes in ultrasound depiction between the solid tumor and the infiltration zone. Otherwise interpretation might be difficult at a later stage of surgery, when the solid tumor mass is almost removed.
Brain metastases are usually well circumscribed and have a defined border in MRI and in the corresponding ultrasound images. A typical depiction of a metastatic lesion is found in Fig. 5.7. Many mainly solid and circumscribed metastatic lesions show infiltrative zones, too. Usually in this type of lesions, infiltration zones are found only in certain parts of the lesion (Fig. 5.15).
Upper row: ultrasound images (US) of a deep-seated small metastasis (*) after dural opening before resection. Left 7 MHz US; right 15Mhz high-resolution US. Lower row: US of the resection cavity after microsurgical complete removal; left 7 Mhz US displays resection cavity with an adjacent sulcus due to a manipulation artifact; the tissue surrounding the resection cavity cannot be assessed. Right:15 Mhz high-resolution US reveals the infiltration zone of the metastasis (big arrows, histologically confirmed). Typical surgery-induced artifacts are shown: blood at the bottom of the resection cavity (small arrows) and a gelfoam (#) that was inserted
5 Artifacts and Image Optimization
When performing intracranial ultrasound, a good knowledge of typical ultrasound artifacts is crucial in order to interpret imaging results properly. Type and extent of artifacts change from type of transducer used and based on the tissue assessed.
Therefore, a change of transducer during surgery might lead to a change of artifacts encountered.
Reverberation artifacts are reflections of ultrasound waves causing a mirrored image or multiple mirrored objects. In brain tumor surgery, this type of artifact might occur when visualizing a resection cavity filled with irrigation. The mirrored images will move when the transducer is changed. Thus, these artifacts are easily identifiable in most cases. Figure 5.16 shows a reverberation artifact as a combination of reflection at the resection cavity and the frontal skull base. Due to the level of artifacts, it is not possible to assess residual tumor in the presented position of the transducer.
Sector array ultrasound image (upper left) of a residual tumor of a diffuse astrocytoma confirmed by intraoperative MRI. Reconstructed intraoperative T2 according to the ultrasound position (upper right), sagittal T1 + contrast (lower left), coronary T1 + contrast (lower right); residual tumor is marked with a continuous gray line; reverberation artifacts are marked with #
Distortions and phase range artifacts are less common in neurosurgery since the brain is a rather homogenous organ. Usually this type of artifacts is elicited when a change of speed of sound occurs. Speed of sound in water, for example, is much higher as in brain tissue. Potential issues might be a resection cavity filled with fluid, a cystic lesion, or the ventricle. Errors in deep range might occur in this case since sound travels faster in water as in brain tissue. Thus lesions behind a water-filled cavity could appear closer compared to lesions in brain tissue in the same depth.
A similar problem occurs based on different attenuations between different tissues. Attenuation in brain tissue is relatively high. Brain tissue even when infiltrated by a tumor is relatively homogenous with regard to attenuation. This is the reason for the high image quality in intraoperative ultrasound at the beginning of tumor resection. Water compared to brain tissue shows very little attenuation. Thus, if a resection cavity is filled with irrigation, a significant difference in attenuation between brain tissue at the walls of the resection cavity and the bottom of the resection cavity is found. Therefore, a different signal at the floor of the cavity might be cause by this type of artifact (Fig. 5.7). This area might appear hyperechogenic and might be confound with residual tumor. Additionally, blood and micro-contusions may cause hyperechogenic signals. Therefore the importance of regular ultrasound sweeps during the process of tumor resection cannot be stressed enough. Thus, attenuation artifacts are easily identified since the artifact will move deeper and increase while the resection cavity is enlarged. We encourage also to take screenshots during this process in order to have images to compare to the actual ultrasound images (Fig. 5.17). Another option to decrease attenuation artifacts is to decrease distance of probe and object of interest. Most transducers for intracranial use can be inserted in typical resection cavities. Especially hockey stick shaped linear array high-frequency transducer facilitate intracavital use. Using such a device, irrigation is not needed in most cases (Fig. 5.8). In glioma surgery we found that intracavital use of hockey stick shaped linear array high-frequency transducer is feasible in over 90 % of cases [14]. Serra et al. described the approach to meticulously scan the whole resection cavity. This maneuver is best performed with a hockey stick-shaped probe at least in smaller resection cavities. The angle of the lateral wall is otherwise more difficult to assess. Additionally use of a linear array transducer is favorable for this approach since best tumor depiction is found close to the transducer. A drawback of intracavital ultrasound using a transducer with a small footprint is the relatively small field of view and the uncommon perspective of the acquired images. Thus, orientation and retrieval of detected residual tumor can be challenging. A navigated use of the ultrasound transducer facilitates tumor detection. Additionally, a 3D sweep can be performed to get an “off-line” overview of the walls of the resection cavity (Fig. 5.17).
Navigation display showing the reformatted ultrasound image slices on top of the corresponding reformatted MR image slice. Ultrasound image slice from 3D ultrasound volume acquired prior to start of resection (a), toward the end of resection with some tumor tissue remaining (b), and after completed tumor resection (c). Notice the signal enhancement below the cavity (marked with arrows) seen in c, which is not observed in a or b. Hence, it is very likely that the enhancement is an artifact and not remaining tumor (Selbek et al. [23] Acta Springer Copyright)
Another option to avoid attenuation artifacts easily feasible also with larger transducers is transcortical ultrasound. The lateral wall of the resection cavity is used as a “sound window” to assess the bottom and the walls for residual tumor (Fig. 5.18). Unsgaard et al. even propagated a second burr hole for continuous ultrasound imaging as a resection control in glioma surgery [22].
Selbek et al. described an acoustic coupling fluid with the same attenuation coefficient as brain tissue. Data are still preliminary. First results show a significantly better image quality compared to normal saline as irrigation fluid [23].
Irregularly shaped surfaces can be covered with an ultrasound gel pad to increase coupling of transducer and tissue. We frequently use these devices in peripheral nerve surgery at our center. In brain tumor surgery, it is rarely needed for this indication. However, gel pads can be useful to increase the distance between the tissue of interest and the probe. When using sector or some curved array transducer, a very superficial lesion might not be visualized appropriately due to the triangular or trapezoid field of view. Slightly increasing the distance with a gel pad might be enough to gain an adequate depiction.
Retrieval of areas of interest with the ultrasound which were found in the microscope and vice versa can be challenging. Orientation inside a resection cavity especially in deep lesions when visualization without retractor is not possible and neuronavigation for the ultrasound is not available adds to the problem. As a first step, anatomical landmarks which can be identified by both modalities like adjacent vessels, falx cerebri, ventricle, etc. should be identified. If this is not possible, artificial landmarks are a helpful option to “mark” certain areas of interest. Wong et al. described the use of a blood-soaked gelfoam as an internal fiducial [24]. Gelfoam is easily available and its intraoperative use is saved even if it remains in situ.
References
Wells PNT (1977) Ultrasonics in medicine and biology. Phys Med Biol 22(4):629
Chandler WF, Knake JE, McGillicuddy JE, Lillehei KO, Silver TM (1982) Intraoperative use of real-time ultrasonography in neurosurgery. J Neurosurg 57(2):157–163, Epub 1982/08/01. doi:10.3171/jns.1982.57.2.0157. PubMed
Unsgaard G, Gronningsaeter A, Ommedal S, Nagelhus Hernes TA (2002) Brain operations guided by real-time two-dimensional ultrasound: new possibilities as a result of improved image quality. Neurosurgery 51(2):402–411; discussion 11–12. Epub 2002/08/17. PubMed
Gronningsaeter A, Kleven A, Ommedal S, Aarseth TE, Lie T, Lindseth F et al (2000) SonoWand, an ultrasound-based neuronavigation system. Neurosurgery 47(6):1373–1379; discussion 9–80. PubMed
Schlaier JR, Warnat J, Dorenbeck U, Proescholdt M, Schebesch KM, Brawanski A (2004) Image fusion of MR images and real-time ultrasonography: evaluation of fusion accuracy combining two commercial instruments, a neuronavigation system and a ultrasound system. Acta Neurochir 146(3):271–277. doi:10.1007/s00701-003-0155-6
Sanai N, Berger MS (2008) Glioma extent of resection and its impact on patient outcome. Neurosurgery 62(4):753–764; discussion 264–266. Epub 2008/05/23. doi: 10.1227/01.neu.0000318159.21731.cf. PubMed
Smith JS, Chang EF, Lamborn KR, Chang SM, Prados MD, Cha S et al (2008) Role of extent of resection in the long-term outcome of low-grade hemispheric gliomas. J Clin Oncol 26(8):1338–1345, Epub 2008/03/08. doi:10.1200/jco.2007.13.9337. PubMed
Solheim O, Selbekk T, Jakola A, Unsgård G (2010) Ultrasound-guided operations in unselected high-grade gliomas—overall results, impact of image quality and patient selection. Acta Neurochir 152(11):1873–1886. doi:10.1007/s00701-010-0731-5
Gerganov VM, Samii A, Akbarian A, Stieglitz L, Samii M, Fahlbusch R (2009) Reliability of intraoperative high-resolution 2D ultrasound as an alternative to high-field strength MR imaging for tumor resection control: a prospective comparative study. J Neurosurg 111(3):512–519, Epub 2009/03/31. doi:10.3171/2009.2.JNS08535. PubMed
Masuzawa H, Kanazawa I, Kamitani H, Sato J (1985) Intraoperative ultrasonography through a burr-hole. Acta Neurochir 77(1–2):41–45. doi:10.1007/BF01402304
Bozinov O, Burkhardt JK (2012) Intra-operative computed-tomography-like real-time three-dimensional ultrasound in neurosurgery. World Neurosurg 78(1–2):5–7, Epub 2012/05/29. doi:10.1016/j.wneu.2012.05.025. PubMed
Serra C, Stauffer A, Actor B, Burkhardt JK, Ulrich NH, Bernays RL et al (2012) Intraoperative high frequency ultrasound in intracerebral high-grade tumors. Ultraschall Med 33(7):E306–E312, Epub 2012/11/07. doi:10.1055/s-0032-1325369. PubMed
Coburger J, Scheuerle A, Kapapa T, Engelke J, Thal DR, Wirtz CR et al (2015) Sensitivity and specificity of linear array intraoperative ultrasound in glioblastoma surgery: a comparative study with high field intraoperative MRI and conventional sector array ultrasound. Neurosurg Rev 38:499–509, Epub 2015/04/10. doi:10.1007/s10143-015-0627-1. PubMed
Coburger J, Scheuerle A, Thal DR, Engelke J, Hlavac M, Wirtz CR et al (2015) Linear array ultrasound in low-grade glioma surgery: histology-based assessment of accuracy in comparison to conventional intraoperative ultrasound and intraoperative MRI. Acta Neurochir (Wien) 157:195–206, Epub 2015/01/07. doi:10.1007/s00701-014-2314-3. PubMed
Coburger J, König RW, Scheuerle A, Engelke J, Hlavac M, Thal DR et al (2014) Navigated high frequency ultrasound: Description of technique and first clinical comparison with conventional intracranial ultrasound. World Neurosurg
Sure U, Benes L, Bozinov O, Woydt M, Tirakotai W, Bertalanffy H (2005) Intraoperative landmarking of vascular anatomy by integration of duplex and Doppler ultrasonography in image-guided surgery. Technical note. Surg Neurol 63(2):133–141; discussion 41–42. Epub 2005/02/01. doi:10.1016/j.surneu.2004.08.040. PubMed
Tirakotai W, Miller D, Heinze S, Benes L, Bertalanffy H, Sure U (2006) A novel platform for image-guided ultrasound. Neurosurgery 58(4):710–718; discussion −8. Epub 2006/04/01. doi: 10.1227/01.neu.0000204454.52414.7a. PubMed
Coburger J (2015) Linear array ultrasound: a dedicated tool for a dedicated application. Acta Neurochir (Wien) 157:959–960. doi:10.1007/s00701-015-2406-8, Epub 2015/04/08. PubMed
Mair R, Heald J, Poeata I, Ivanov M (2013) A practical grading system of ultrasonographic visibility for intracerebral lesions. Acta Neurochir 155(12):2293–2298. doi:10.1007/s00701-013-1868-9
Yamahara T, Numa Y, Oishi T, Kawaguchi T, Seno T, Asai A et al (2010) Morphological and flow cytometric analysis of cell infiltration in glioblastoma: a comparison of autopsy brain and neuroimaging. Brain Tumor Pathol 27(2):81–87, PubMed
McGirt MJ, Mukherjee D, Chaichana KL, Than KD, Weingart JD, Quinones-Hinojosa A (2009) Association of surgically acquired motor and language deficits on overall survival after resection of glioblastoma multiforme. Neurosurgery 65(3):463–469; discussion 9–70. Epub 2009/08/19. doi:10.1227/01.neu.0000349763.42238.e9. PubMed
Unsgaard GK (1999) Atle; ommedal, steinar; gronningsaeter, aage. An ultrasound-based neuronavigation system, a good solution to the brain-shift problem. Neurosurgery 45(3):696
Selbekk T, Jakola AS, Solheim O, Johansen TF, Lindseth F, Reinertsen I et al (2013) Ultrasound imaging in neurosurgery: approaches to minimize surgically induced image artefacts for improved resection control. Acta Neurochir (Wien) 155(6):973–980, Epub 2013/03/06. doi:10.1007/s00701-013-1647-7. PubMed PMID: 23459867; PubMed Central PMCID: PMC3656245
Wong JM, Governale LS, Friedlander RM (2011) Use of a simple internal fiducial as an adjunct to enhance intraoperative ultrasound-assisted guidance: technical note. Neurosurgery 69(1 Suppl Operative):ons34–ons39; discussion ons9. Epub 2011/02/25. doi:10.1227/NEU.0b013e3182124851. PubMed
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Coburger, J., König, R.W. (2016). Intraoperative Findings in Brain Tumor Surgery. In: Prada, F., Solbiati, L., Martegani, A., DiMeco, F. (eds) Intraoperative Ultrasound (IOUS) in Neurosurgery. Springer, Cham. https://doi.org/10.1007/978-3-319-25268-1_5
Download citation
DOI: https://doi.org/10.1007/978-3-319-25268-1_5
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-25266-7
Online ISBN: 978-3-319-25268-1
eBook Packages: MedicineMedicine (R0)