Abstract
For over two decades, humans have continuously inhabited the International Space Station (ISS). The next steps will consist of human exploration beyond low Earth orbit (LEO), sustained lunar presence (Artemis), and higher risk of harmful effects from ionizing radiation. Therefore, to protect astronauts and to potentially develop on-ground therapies, it is appropriate to understand the behavior of the central nervous system (CNS) neoplasms in the spaceflight environment. So far, only a few on-ground studies have been conducted to analyze the behavior of CNS neoplasms in microgravity and in ionizing radiations.
In this chapter, we aim to confront the molecular mechanisms of tumorigenesis and tumor-suppression on-ground and in space (simulated microgravity and HZE). No experiment in Space—LEO, deep space or Martian surface—has been executed so far, hence, leaving open questions upon the precise behavior of tumor cells in space: how will the tumor-suppression properties of microgravity interact with the carcinogenetic characteristics of ionizing radiations? A literature review has been conducted using PubMed as the database of reference (May 2021). Search words employed were: “Central nervous system neoplasm AND microgravity”; “Central nervous system neoplasm AND spaceflight”; “Solid tumour AND Microgravity”; “Cancer stem cell AND microgravity”; “Glioblastoma AND microgravity”; “Glioblastoma AND spaceflight”; “Cancer Stem Cell AND spaceflight”; “Tumour suppression AND spaceflight”; “Tumour suppression AND microgravity”. The majority of the studies in simulated microgravity suggest an inhibition in the glioma cell malignancy which could contribute to the development of therapeutical possibilities. Conversely, ionizing radiations are deemed to enhance carcinogenesis.
Currently, experimental results in simulated microgravity seem to be auspicious for possible usage of microgravity as a tool for therapies. The role of microgravity in space is hypothesized to be akin to simulated microgravity. The correlation between microgravity effects and space radiations remains obscure, given the speculated propensity of a carcinogenesis enhancement under ionizing radiations. Several questions remain still open. Further research is essential to comprehend the exact behaviour of cancer in space and the combined effects of microgravity and space radiation.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- CNS
- Glioblastoma
- Microgravity
- ISS
- LEO
- Mars
- Ionizing radiations
- HZE
- Simulated microgravity
- Weightlessness
- Cancer stem cells
- Cancer in space
Introduction
Since humans first inhabited the International Space Station (ISS) over two decades ago, the duration of space missions per astronaut have been limited to 1–12 months. Astronauts in low Earth orbit are also partially protected from galactic cosmic radiation (GCR) due to the Earth’s magnetic field. The next steps in human exploration will include long-duration missions beyond low Earth orbit (LEO) and higher concerns for harmful effects of space radiation. Prolonged exposure to microgravity may also alter the central nervous system at the cytoarchitectural level [1], and it has been suggested that microgravity may even inhibit proliferation [2] of malignant glioma. Therefore, with the aim to protect astronaut’s health and exploit space environment conditions to potentially develop on-ground countermeasures, the need to understand the behavior of the central nervous system (CNS) in space has emerged. The dismal knowledge regarding the characteristics of the combined effects of microgravity and space radiations arises interest in researchers, especially regarding the long-term risk to develop neurodegenerative diseases and cancer. Recent progression in aerospace medicine and research opened several questions regarding the behavior of the neoplasms in microgravity and under ionizing radiations and a potential treatment window [3, 4].
Central nervous system (CNS) neoplasms are solid tumors arising from the brain, meninges, or spinal cord with different prognosis dependent on their location and histology.
CNS neoplasms are considered to be rare but lethal tumors as they account around 30% of cancer deaths in children and young adults [5]. The 2016 World Health Organization (WHO) classification categorizes CNS neoplasms based on histogenesis and molecular parameters to help aid in identification and prognostication [6]. The grading of some CNS tumor according to this classification is consultable in Fig. 8.1.
Grading of central nervous system tumors (2016 WHO). Reprinted from [6] with permission
The treatment and prognosis of CNS neoplasms vary according to the location, severity of symptoms, and the type of neoplasm. In adults, the majority of primary CNS tumors are malignant in nature and treated with a combination of surgery, radiation, and chemotherapy depending [7]. Unfortunately, even after initial disease control, the majority of malignant tumors progress and the mortality rate remains high [8].
In this chapter, two main areas of cancer research in the spaceflight environment will be covered: (1) Central Nervous System malignancies tumorigenesis and (2) tumor suppression. We will analyze the molecular bases of tumorigenesis in terrestrial gravity and hypothesize on the tumorigenesis in microgravity with close attention to the contribution of radiation. We with further evaluate the tumor suppressive characteristics of microgravity in the treatment of CNS tumors. The chapter aims to review the currently available literature regarding these arguments and to identify the role of microgravity on CNS neoplasms behavior.
Environment
Microgravity
The space environment is hazardous, outlined by high vacuum, extreme radiation of galactic and solar origin, and extreme temperatures [9]. Perhaps the most obvious unique influence on the pathophysiology of CNS neoplasms during spaceflight is that of microgravity. Microgravity or zero-g is used to describe the condition of weightlessness experienced during spaceflight [10]. The term does not necessarily refer to a reduced level of gravity in an absolute sense, but to the lack of counteracting inertial g-forces or any other forces than gravity. Microgravity is expressed as a fraction of g, where g is the gravitational acceleration at Earth’s surface, on average 9.81 m/s2. This should not be confused with gravitational field. At ISS altitude, the gravitational field is around 90% of that on the Earth’s surface. However, the ISS orbits the Earth in a constant free fall and with almost negligible air resistance. The inertial g-forces on ISS are therefore virtually absent and equivalent to micro-fractions (10−6) of the normal force exerted on an individual on the surface of the Earth due to gravity. The lunar gravity of 0.16 g and Martian gravity of 0.38 g induce less gravitational forces than the Earth’s gravity at ISS altitude, but the astronauts based on the surface of Moon or Mars are still exposed to higher gravitational load as compared to the microgravity environment experienced during orbit.
From now onwards, we will refer to the spaceflight gravitational environment as microgravity [11].
Space Radiations
The next largest hazard to take in consideration is that of ionizing radiations. Ionizing radiations are particles with a sufficient amount of energy which can totally discard an electron from its orbit, consequently generating a more positively charged atom. On the other hand, the non-ionizing radiation (Low energy) does not have adequate energy to separate electrons. There are three naturally occurring types of ionizing space radiations; galactic cosmic rays (GCRs) originating beyond the solar system, localized trapped particle belts of electrons and protons (ERBs)—known also as Van Allen radiation belts—and solar particle events (SPEs) [12]. The Galactic cosmic rays (GCRs) are an isotropic flux of charged particles originating from sources beyond the solar system with unidentified origins which can penetrate through a typical spacecraft or an astronaut [13]. When the particles strike the spacecraft, hadronic cascades are also initiated and result in secondary particles. The average GCR absorbed per day in a mission to Mars has estimated to be around 1.75–3.0 mSv/day [14, 15]. The Van Allen radiation belts or ERBs are two zones confining the Earth in which energetic charged particles are trapped due to the Earth’s magnetic field [16], and the planetary magnetic field various among other planets in our Solar System [17, 18]. The majority of the inner Van Allen Belt is located beyond the ISS orbit and protects the station from incoming particles. However, the South Atlantic Anomaly (SAA) is an area where the inner belt dips closer to Earth and expose ISS to large amounts of radiation. The Solar Particle Events (SPEs) are made mostly of protons with a high-value flux representing a risk for astronaut health, however, in contrary to the GCRs, they are feasible of defense [19]. The SPEs are shielded by the Earth magnetic field, so they are of greater concern for planetary and interplanetary missions. Very large SPEs are rare, but challenges in prediction of their occurrence may impose significant operational constraints or radiation risk to the crew.
To grasp the impact of ionizing radiations, it is crucial to distinguish the Low Earth Orbit (LEO) and the interplanetary space beyond LEO. In this section, the suborbital flights are not considered, as they operate at a low altitude avoiding the ERBs. On the ISS (LEO), the astronauts are partially protected from SPEs and GCRs due to the magnetosphere [20]. While in deep space, missions do not benefit from the protection against planet atmospheres against SPEs or GCRs. Consequently, SPEs and GCR will stumble the spacecraft with fluxes in a position-dependent manner. The average radiation dose-equivalent rate is around 4.3.84 mSv/day, three times higher than in LEO [14].
Lack of a strong global magnetic field and the thin atmosphere on Mars result in only minimal protection from radiation on the surface of Mars. According to the MSL-Rad workshop data, Mars surface and ISS radiation dose rates are similar, 0.213 mGy/day and 0.240 mGy/day, respectively [21]. The current maximal exposure of an astronaut to radiation, according to NASA indications, is set to 3% of the risk of exposure-induced death (REID) cancer fatality with a 95% confidence interval (C.I.) [22].
CNS Neoplasms Overview
The term central nervous system neoplasms refer to a group of heterogenous benign and malignant tumors [23] which ranges from an extremely invasive and nearly untreatable Glioblastoma multiforme to a non-invasive and treatable pilocytic astrocytoma. The CNS tumors can either be primary or secondary. They are the most common solid tumors in children in the USA, and responsible for approximately 15–20% of all childhood cancers. They are the leading cause of death in children between 0 and 14 years [24,25,26]. CNS tumors are estimated to occur with an incidence rate of 23.8 per 100,000 people in adults, and they account for 2% of all cancers [24].
The classification of this group of tumors has always been challenging, and it has been under constant revision and update since Bailey and Cushing’s publication in 1926 [27].
Currently, the WHO 2016 Classification—in comparison to the WHO 2007 classification based exclusively on histogenesis [28]—categorizes CNS tumors into four grades also basing on molecular markers and genetic factors [6]. Moreover, new changes to the classifications of diffuse glioma have been suggested by the cIMPACT (the Consortium to Inform Molecular and Practical Approaches to CNS Tumor Taxonomy) with an upcoming fifth edition of WHO Classification in the current year 2021 [29, 30].
The criteria of WHO Classification are: (1) anaplasia, (2) mitotic activity, (3) endothelial cell proliferation, and (4) necrosis [31]. Thus, the grading of a CNS tumor is based on these criteria.
Grade I tumors do not meet any criteria, they are benign and slow growing tumors with a good prognosis, i.e., Juvenile Pilocytic Astrocytoma. On the contrary, Grade II tumors fulfill the criterion of anaplasia. They are either malignant or non-malignant slow growing tumors with the potential to recur as higher-grade tumors. For instance, diffuse astrocytoma falls in the Grade II category. Anaplasia and mitotic activity are the two criteria met by III grade tumors like anaplastic astrocytoma. They are malignant tumors that can progress to higher-graded tumors. Grade IV tumors, such as glioblastoma multiforme (GBM), meet all three or four of the above-mentioned criteria. They have a rapid reproducing rate and they are considered to be aggressive malignant tumors [32]. These CNS Grades are predicted to be switched into Arabic numeral nomenclature according to the WHO fifth edition preview [29]. The grading of some selected tumors is consultable in Fig. 8.1.
Glioma, a category of malignant brain tumors that includes high-grade glioma or glioblastoma and low-grade gliomas, is the most common histological form of primary CNS cancer, therefore, this chapter will be focusing mainly on their classification and description [33]. Gliomas originate from progenitor glial cells or stem cells, and they mirror the glial characteristics after undergoing neoplastic transformation. There are several kinds of glial tumors, i.e. diffuse glioma, other astrocytic glioma, ependymal tumor, other glioma, and mixed neuronal-glial tumor (Fig. 8.2) [34].
Decision tree for histologic diagnosis of glial and neuronal-glial central nervous system neoplasms. Reprinted with permission from [34]
Diffuse gliomas account for the vast majority of glial neoplasms in adults. They are defined by diffusive infiltration growth and tumor cell migration into the CNS parenchyma over large distances. The WHO grade II and grade III astrocytic tumors, the grade II and III oligodendrogliomas, the grade IV glioblastomas, and the associated diffuse gliomas of childhood are all classified as diffuse gliomas. The main molecular markers employed in the diagnosis of glioma are isocitrate dehydrogenase (IDH) mutation, chromosomal arm 1p19q deletion, O6-methylguanine-DNA methyltransferase (MGMT) promoter methylation, telomerase reverse transcriptase (TERT) promotor mutation, alpha-thalassemia retardation syndrome linked (ATRX) mutation or loss of nuclear expression, and tumor protein p53 (Tp53) [6]. Other markers introduced by the cIMPACT are H3 K27M mutation and H3.3 G34 mutation, EGFR amplification, CDKN2A homozygous deletion, and +7/−10 genotype [35].
Briefly, IDH marker is at the core of differential diagnosis between glioma and gliosis, and in astrocytoma, oligodendroglioma, and even in 10% glioblastoma, it is positive. Mutation in both IDH 1 and 2, known as IDH Mutant, while the negativity to both forms of IDH is referred to as IDH wild type [36]. The 1p/19q co-deletion, on the other hand, is correlated with the diagnosis of Grade II and Grade III (anaplastic) oligodendroglioma. It plays an important role also in the prognostication of the outcome, and it is linked to procarbazine–lomustine–vincristine (PCV) chemotherapy sensitivity [37]. Basing on these two markers, diffuse gliomas have been classified into diffuse astrocytic tumors IDH-wildtype, diffuse astrocytic tumors IDH-mutant and oligodendroglial tumors IDH-mutant and 1p/19q-codeleted. Where it is not possible to conduct proper molecular testing, the tumor falls into the category of not otherwise specified (NOS).
In gliomas, TERT mutations in the promoter region (C228T and C250T) predict poor survival and radiotherapy resistance, especially in glioblastoma and oligodendroglioma [38]. On the other hand, the methylation of the O6-methylguanine-DNA methyltransferase (MGMT) gene promoter acts as a positive prognostic factor in GBM patients [39].
Grade II, diffuse astrocytomas, known also as low-grade infiltrative astrocytomas, can be IDH mutant or wild-type [40]. It affects mainly young adults with a mean age of 35 years. In almost 40% of the cases this grade II CNS tumor presents with seizure, and depending on the location and size of the lesion, it can induce focal neurological disfunctions [41, 42]. According to the cIMPACT-NOW recommendations, Astrocytoma IDH-mutant WHO grade II, would be graded as Astrocytoma, IDH-mutant, WHO grade 2, characterized as well-differentiated, lacking histologic features of anaplasia and with low or absent mitotic activity. Microvascular proliferation, necrosis, and CDKN2A/B homozygous deletions are absent [43]. A safe total resection and radiographic follow-up are indicated in this type of gliomas [44].
Grade III, anaplastic astrocytoma (AA), is a rapidly growing, diffusely infiltrating tumor with a median age of onset around 41 years [28]. It can also be IDH mutant or wild-type. Depending on the location of the tumor, the clinical manifestation is mutable. The symptoms include focal or generalized neurological deficits, headaches, visual and sensory impairment, strength loss, and gait disturbances; seizures are less common in anaplastic astrocytomas in comparison to low-grade gliomas [45]. The new recommendations characterize AA IDH-mutant WHO grade III glioma as an Astrocytoma, IDH-mutant, WHO grade 3 that manifests focal or dispersed anaplasia in concomitancy of significant mitotic activity. Microvascular proliferation, necrosis, and CDKN2A/B homozygous deletions are absent [43, 46]. Where necessary and regardless of the mutational status of the IDH gene, the first therapeutic strategy in the treatment of AA is a maximal safe surgical resection along with radiographic follow-up and chemotherapy as per Stupp protocol [47].
The previously classified oligodendroglioma, IDH-mutant, and 1p/19q-codeleted, WHO grade II would be remain oligodendroglioma, IDH-mutant, and 1p/19q-codeleted, WHO grade 2 in the new recommendations [43]. Oligodendrogliomas constitutes around 5% of primary brain tumors and in most of the cases the symptoms are non-specific such as headache. Seizure is experienced in around 35–85% of the cases. Surgical therapy, chemotherapy, and radiation therapy are the main treatments of oligodendroglioma [48].
Glioblastoma (GB), a grade IV glioma, is one of the most aggressive brain tumors, with an estimated survival time of just 15 months after diagnosis [6]. This tumor can be either primary—in case of a de-novo development—or secondary, progressing from a low-grade glioma [49]. The former is denominated in the 2016 WHO Classification as IDH wild-type, while the latter as IDH-mutant for its various pathways of progression [50]. Both forms of GB have the same characterization, such as necrosis, pleomorphism, and vascularization. Early relapse is caused by its high resistance to radiotherapy and chemotherapy, as well as incomplete surgery due to diffuse invasion of the guerrilla cells [50, 51]. The main symptoms referred by the patients are headache—due to high intracranial pressure—seizure, cognitive impairment, and nausea. The therapeutical indications consist in a safe total resection followed by radiation and temozolomide. This type of tumors is very hard to treat, therefore, various clinical trials and studies are in progress. The main sword of Damocles in the treating of GB is represented by the heterogeneity dictated by the glioblastoma stem cells (GSCs) which were first described in 2003 [52]. These GSCs, as “the apex of a dynamic network,” are renominated for their two key features being self-renewal and differentiation [53]. The heterogeneity which consists in the unpredictability of cancer cells’ subtypes across individual tumors, de facto, seems to limit the efficacy of selective targeting of oncogenic pathways and of tumor microenvironment [54]. According to the new recommendations, glioblastoma, IDH-mutant, WHO grade IV should be renominated as Astrocytoma, IDH-mutant, WHO grade 4, and the previous wild-type grade II diffuse and anaplastic astrocytomas, as well as glioblastoma, IDH-wildtype, WHO grade IV are suggested to be classified as glioblastoma, IDH-wildtype, WHO grade 4 for their poor outcome predicted by TERT, EGFR and + 7/−10 genotype [43]. The glioblastoma, IDH-wildtype, WHO grade IV, can moreover be classified as Diffuse hemispheric glioma, H3.3 G34-mutant, WHO grade 4 in the presence of a missense mutation in the Histone H3.3 protein, codon 34.
Methodology of Studying CNS Neoplastic Behavior in Space
Real microgravity studies are expensive and rare; thus, on-ground simulated microgravity (SMG) is more prevalent. Several contemporary devices are used to simulate microgravity such as random positioning machine (RPM), rotating wall vessel (RWV), and fast rotating clinostats (Fig. 8.3) [55, 56].
Random positioning machine (a) and 2-D Clinostat (b). Copyright: © 2015 Svejgaard et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited
The main tools utilized in the studies taken in consideration in this chapter are: the 2D clinostat system and the 3D clinostat system. The 2D clinostat system is a 3-dimensional rotational device which rotates around 1 (2D) axis (Fig. 8.3). Essentially, it is a rotating device which prevents the biological system from achieving a sustained gravitational acceleration vector [57, 58]. A random positioning machine (RPM), known also as 3D clinostat, is a simulator based on the principle of vector averaged gravity [59]. This simulator is often compared to the 2D clinostat although it has several differences. The 3D clinostat presents two axes of rotation and a major swimming velocity [55]. The RWV, instead, is a bioreactor of 5–20 cm diameter with liquid-filled container that rotates around a horizontal axis at 10–20 rpm [60].
Most of the studies are made in vitro on 2D or 3D cultures. 2D cultures are well known to be simple, with a low time of culture formation, and low-cost maintenance but they have the disadvantage of not portraying faithfully the natural structures of tumors. Further disadvantages lay in the diverse phenotype loss, lack of representation of the cell-cell and cell-extracellular interactions and a monolayer composition which translates into an unlimited metabolic resource on contrary to the in vivo cells [61]. The other limitation of 2D cultures, as reported by Birgersdotter et al., is the change in gene expression and splicing, topology and the cellular biochemistry [62]. On the other hand, 3D cultures are beloved for the faithful imitation of in vivo tissues and organs, and for the recreation of proper interactions of cell–cell and cell-extracellular environment [61]. Also, the morphology, the phenotype and cellular reproduction phases, as well as the molecular mechanisms, are preserved in 3D cultures in contrast to the 2D cultures [62, 63]. The limitations of 3D cultures reside in a longer time of culture formation, in a worse performance in culture quality and in expensive costs [64, 65].
The analysis part of each studies varies depending on the type of cells and the objective of studies.
The ideal method to observe the behavior of CNS cancer in space would be to have in vivo models analyzed in space. In Cancer and Health research in space, a conference paper, it was intended to examine human GBM derived cancer stem cells (GSCs) in space. The GCSs would be inoculated into mice brain and subsequently, 12 healthy mice, as control, and 12 mice with GBM, sent on the ISS, whereas 24 mice would be maintained in on-ground laboratories under observation for the corresponding on-ground experiments.
Procedures involving animals and their care would be conducted in accordance with the national and international guidelines of the National Institutes of Health Guide (NIH) for the care and use of laboratory animals. On board the ISS, mice will be kept in special cages, previously used by Japan Aerospace Exploration Agency (JAXA) [66], and they would be monitored 24/7 with internal cams. Cages will be equipped with automatized systems to provide food and water, hygiene and adjust sleep/wake cycles. At the end of the mission, mice would be examined with behavioral tests through our specifically projected maze to evaluate their cognitive abilities and scanned with MRI to rate the volumetric variation in dimension and vascularization of the tumor mass. Furthermore, tumor mass would be explanted and study at morphological, cellular, molecular, and genetic levels. The core point of this project consists on the possibility to study cancer models in vivo, rather than in vitro, on the ISS. Unfortunately, for economic restrictions the project is in stand-by. Recently, Larose et al. published a paper on their intention to analyze tumors in space. They intend to observe by 2025 human organoids on the Chinese space station [67].
CNS Neoplasms Behavior in Space
Carcinogenesis in Space
Carcinogenesis in space may differ in comparison to the carcinogenesis on-ground. Thus far, no experiments have been conducted in high linear energy transfer (LET) due to obvious limitations, and our knowledge regarding carcinogenesis derives from studies made in low LET. Consequently, there are no sufficient studies on CNS neoplasms carcinogenesis stages in space. Most of the studies are done on survivors of the atomic bomb from Japan.
Initiation under HZE ions—high energy nuclei originating from GCRs or SPEs [68]—differs from the initiation process described earlier. It produces cluster damage in DNA helix strands, causing multiple lesions, instead of non-clustered lesions [3, 69]. These radiation-induced lesions translate into a genomic instability due to the activation of multiple pathways affecting different carcinogenesis stages.
Promotion and progression stages are also different due to the duplex promoter and initiator role of radiation [70]. As reported by Hanahan and Weinberg, the above-mentioned genetic instability promotes the carcinogenesis through several mechanisms, such as evasion of apoptosis, self-sufficiency in growth signals, insensitivity to anti-growth signals, and limitless replicative potential [71]. Other factors deemed to contribute to the carcinogenesis are the extracellular matrix remodeling, persistent inflammation, and oxidative damage [22, 72]. According to Cucinotta et al. fatal cancer risks are less than 10% at upper 95% of confidence interval, deducing that the risk model is accurate. In the hypothesis that the risk model is incorrect, the percentage of fatality could approach 20% with significant life loss [73].
Nevertheless, the risk assessment of carcinogenesis in space, and in particular of central nervous carcinogenesis, is so far, not possible due to a lack of sufficient data and studies. As a matter of fact, mechanisms and inter-species variations are still poorly understood.
Tumor Suppression in Space: A Dual Theory
In the past couple of decades, particular attention has been given to the cancerous cell behavior in microgravity. Sahebi et al. defined microgravity as a dual edge sword as it is still not clear the exact function of microgravity in relation to cancer [74].
It is hypothesized that microgravity impacts the cancerous cells by repressing survival signaling pathways and inducing apoptosis. De facto, the role of microgravity in cellular viability and apoptosis is demonstrated by the inhibition or downregulation of BCL-2 and Bnip3 anti-apoptotic proteins, and by the enhancement of Bax, p53, Caspase -3, 7,8, and PARP pro-apoptotic proteins [74,75,76]. Another characteristic of microgravity consists in the ability of preventing the formation of spherical colonies and cell proliferation due to a downregulation of ATM/ATR and CDK1/2 proteins which prevents the transition from the cellular phase S to G2 [74, 75, 77]. A key factor is also the induction of early alterations of cytoskeleton, of extracellular matrix (ECM) and focal adhesions [78,79,80], as a matter of fact, many studies reported a spheroid formation in some types of cancers [81]. Spheroid cultures are cell clusters organized in 3D which alters some signaling pathways and gives a greater differentiation potential in microgravity to stem cells [82]. Furthermore, it seems that this remodeling of cytoskeleton and ECM is an adaptive response to microgravity [74] and that actin microfilament structures are sensitive to microgravity leading to an alteration of signal transduction [83].
Concerning the CNS neoplasms, several changes in cell viability, proliferation, and apoptosis were studied in the past few decades. Especially, U251MG glioma cell line and U87 cells were analyzed in simulated microgravity in a time-dependent manner. U251 cells and U87 derive both from a malignant glioblastoma tumor but with different phenotypes and variances in nicotinamide nucleotide metabolic process regulation, RNA splicing, glycolysis, and purine metabolism [84, 85].
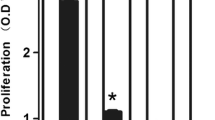
Deng et al. reported a time-dependent inhibition of U251 cell viability by SMG as well as a blockage of cell cycle in G2/M phases. Additionally, an upregulation of cleaved caspase 3 and 9, and a downregulation of BCL-2 and BNIP-3 were evident after a Western blot analysis [86]. Similarly, Zhao et al. identified an upregulation of p21 and a downregulation of Insulin-like growth factor binding protein-2 (IGFBP-2) (Fig. 8.4) [87]. An upregulation of p21 translates into a major tumor suppression, hence to an increased apoptosis. The Insulin-like growth factor binding protein-2, instead, is one of the over-expressed factors and a biomarker in high-grade glioma. A downregulation of IGFBP-2 is linked to an inhibition of glioma cells proliferation [88]. Additionally to the changes in proliferation, apoptosis, and morphology, SMG effects also the migration and the invasion of U87 and U251 cells [86, 89]. In fact, SMG was associated to an inhibition of focal adhesion kinase (FAK), and to a reduced RhoA/Rock signaling and Nek2 expression which transposes into a decreased viability and migration of U251 glioma cells [86] (Fig. 8.5). Focal adhesion kinase (FAK) is an integrin-based focal adhesion tyrosine kinase and it has a crucial role in the regulation of cytoskeletal networking and cellular signaling [90]. Moreover, FAK appears to be over-expressed in highly invasive tumors and it is interconnected with RhoA/Rock pathway which regulates the cytoskeleton and morphology [91]. By the inhibition of FAK by SMG, also GTP-RhoA gets inhibited with a consequent arrest of Rock, LIMK, MLC, and Cofilin phosphorylation which along with the Nek-2 inhibition results into an inhibited glioma cell malignancy [86]. Likewise, the invasion and migration potentials of U87 cells were found to be effected by SMG, through an inhibition of store-operated Ca2+ entry (SOCE) and a subsequent downregulation of Orai1, a cell membrane pore structure, and expression [92, 93].
Expression of on p21 and of Insulin-like growth factor binding protein-2 (IGFBP-2) in simulated microgravity vs. normal gravity. (a) The bar graph shows the ratios of p21 (left panel) and IGFBP-2 (right panel) mRNA relative to the amount of β-actin mRNA. The western blot images of p21 and IGFBP-2 are, respectively, shown in (b, left panel) and (c, left panel). The right panels represent the densitometric analysis of the data. β-Actin was used as a loading control. Reprinted and cited with permission from the authors [87]
Systematic diagram of the signaling pathways affected by SMG in glioma cell via FAK activation. Reprinted with permission of the authors [86]
Overall, majority of the studies in simulated microgravity suggests an inhibition in the glioma cell malignancy which could contribute to the development of therapeutical possibilities. Conversely, ionizing radiations are deemed to enhance the carcinogenesis [94,95,96]. As a matter of fact, according to Hanahan and Weinberg, the space radiations could lead to DNA damage with subsequent mutations and genomic changes, and to epigenetic changes, i.e., methylation, altered replication or inflammatory responses. These could potentially lead to a genetic instability which could trigger mechanisms that could lead to an incremented carcinogenesis (Fig. 8.6) [71].
Another important aspect to take in consideration while analyzing the effects of microgravity on tumor suppression is the enhanced sensitizing of cancer stem cells (CSCs) to chemotherapeutic agents [97]. Kelly et al. performed experiments on CSC in a hydrofocusing bioreactor (HBR) and in the rotary cell culture system (RCCS). The HBR is constituted of a 50 mL fluid-filled sphere that rotates at a set speed to furnish a particular hydrofocusing capability that, in the absence of gas bubbles, permits for a low-shear culture conditions in which cells can grow in simulated microgravity [98]. The RCCS is also 50 mL horizontally rotating culture vessel that decreases the shear and turbulence caused by traditional stirred bioreactors, reducing mechanical cell damage, and simulating microgravity [99]. The result of the study indicates that potentially, basing on the core concept of elimination of cancer stem cells which are reputed to be the responsible of tumor recurrence after invasive therapies, it might be possible to develop an anti-cancer therapy through microgravity. As a matter of fact, in T98G, U87MG cell lines CD133 (+) in HBF appear to be more sensitive to chemotherapeutics in comparison to RCCS and normal gravity. Not many studies have been conducted on CD133—positive stem cells, even if they could be an ideal target for further therapy implementations [100]. Also, Takeda M et al. reported an increased chemosensitivity to cisplatin in microgravity in GBM cells, suggesting microgravity might serve as an expectable role of protection for GBM patients [2]. These results were confirmed also by Yuan et al. in their study as well [101]. Unfortunately, studies on other solid CNS tumors in microgravity is lacking. No other relevant studies were found after researching PubMed, Cochrane or Google Scholar databases. This constitutes a limit in the understanding of CNS neoplasms behavior in space.
As the radiation has been largely considered as an initiator of cancer through induction of DNA mutation, and on the other hand given the potential tumor suppressive and sensitizing to chemotherapeutic characteristics of microgravity, the questions is whether to protect or to expose. Thus, given the dichotomic outcomes predicted, reported in literature, the main question would be if the astronauts are subject to incremented risk of malignant CNS tumors following prolonged space missions, or if exposure of patients with CNS neoplasms to the space environment will result in tumor suppression? Will tumor suppression effect of microgravity balance the potential carcinogenesis mediated by ionizing radiations? To answer to this dilemma, further studies are needed to analyze the combined effects of microgravity and ionizing radiations in pharmaceutically treated, non-treated, and control subjects.
History of Literature
Several studies have addressed the effects of spaceflight on CNS [1, 102, 103], but, hitherto, no clear view has been obtained regarding the behavior of CNS neoplasms or generally, of cancer, in space.
Already in 2001, Cucinotta et al. have expressed their perplexity regarding the lack of knowledge and the uncertainty deriving from it in matter of cancer behavior and risk assessment [104]. In late 90s, several researches addressed the possibility of a higher cancer induction due to high-LET radiations in space compared to the normal X-rays (Low-LET radiations) with the consequence of a permanent damage to the CNS independently from the site and typology of tumor [105, 106]. Uncertainty remains the key word also today regarding the risk assessment of carcinogenesis in space. As discussed earlier the effect of radiations depends also on the type of radiation taken in consideration, the amount of radiation on LEO (ISS) or Mars surface is different to the one in deeper space [14, 107]. In addition to the studies related to radiation and cancer risk assessment, further studies have been made on the role of microgravity. As discussed in the tumor suppression part, up to day, it is possible that simulated microgravity inhibits the malignancy of high-grade central nervous system cancers [86, 87]. Whereas, it still remains unclear the combined effects of radiations and microgravity in space, placing a shadow on the results and the future of long-term space colonization.
Literature Review Methodology
Concerning the CNS Neoplasm tumor-suppression part, a literature review has been conducted by May 2021. PRISMA guidelines were the point of reference for the literature review. PubMed was the database of reference and several keywords were utilized. Keywords employed were: “Central nervous system neoplasm AND microgravity”; “Central nervous system neoplasm AND spaceflight”; “Solid tumor AND Microgravity”; “Cancer stem cell AND microgravity”; “Glioblastoma AND microgravity”; “Glioblastoma AND spaceflight”; “Cancer Stem Cell AND spaceflight”; “Tumor suppression AND spaceflight”; “Tumor suppression AND microgravity.”
Foreign language literature was excluded. Zotero software was used to manage citations, abstracts, and documents.
The search strategy returned 124 references. Of these 26 were eliminated as duplicates, and a further 82 were excluded at the title and abstract screening stage. The remaining 16 papers were included for full-text screening. Of these 16 papers 7 were included in the study. An additional study was included through citation searching (Fig. 8.7).
Limitations
Several limitations have to be addressed in this chapter. As discussed earlier, a clear view of the CNS neoplasm behavior is not currently available. This may be due to financial or ethical concerns.
Despite extensive space radiation research, significant uncertainties remain in predicting the biological consequences for humans as terrestrial simulations differ from an actual spaceflight environment [108]. As reported by Chancellor et al., it is arduous to properly simulate the spectrum of energies, ion species, concentrations, and dose rates found in the space radiation world.
Additionally, the information available for extrapolating radiation risk concerning the spaceflight is restricted by several factors such as limitations in the emulation of the radiation environment, and choice of surrogate animal model. Also the impossibility to delivery of sufficient complexity, rate, and magnitude of doses can be considered as important limitations [108].
Furthermore, observations in studies conducted in a simulated microgravity environment on Earth may differ from real microgravity. The principle of clinostats and random positioning machines is to vary the gravity between −1 g and +1 g with the purpose of achieving an overage of 0 g over time [109]. Hydrostatic gradients are still present, even if the vector varies. This is different from a real and sustained microgravity.
Conclusion
Heretofore, the precise behavior of central nervous neoplasms in space is dismal. Currently, experiment results in simulated microgravity seem to be auspicious for a possible usage of microgravity as a tool for therapies. The role of microgravity in space is hypothesized to be akin to the simulated microgravity. The correlation between microgravity effects and space radiations remains obscure, given the speculated propension of a carcinogenesis enhancement under ionizing radiations. Several questions remain still open. With the current data, it would be preliminary to declare that extended missions would increase CNS cancer risk, and it is not possible to assert that microgravity could lead to tumor suppression. The dual sword theory reamin pertinant. The CubeSat to study Solar Particles (CuSP) spacecraft, on board of Artemis, might reveal further information in terms of space radiation, widening the understanding, thereby, also of the related cancer risks. Further researches are neded to clarify the aspects and questions raised in this chapter, also in the light of the information which will be obtained from the upcoming missions.
References
Jandial R, Hoshide R, Waters J, Limoli C. Space–brain: The negative effects of space exposure on the central nervous system. Surg Neurol Int. 2018;9(1):9.
Takeda M, Magaki T, Okazaki T, Kawahara Y, Manabe T, Yuge L, et al. Effects of simulated microgravity on proliferation and chemosensitivity in malignant glioma cells. Neurosci Lett. 2009;463(1):54–9.
Barcellos-Hoff MH, Blakely EA, Burma S, Fornace AJ, Gerson S, Hlatky L, et al. Concepts and challenges in cancer risk prediction for the space radiation environment. Life Sci Space Res. 2015;6:92–103.
Furukawa S, Nagamatsu A, Nenoi M, Fujimori A, Kakinuma S, Katsube T, et al. Space Radiation Biology for “Living in Space”. BioMed Res Int [Internet]. 2020 Apr 8 [cited 2021 Apr 30];2020. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7168699/
McNeill KA. Epidemiology of brain tumors. Neurol Clin. 2016;34(4):981–98.
Louis DN, Perry A, Reifenberger G, von Deimling A, Figarella-Branger D, Cavenee WK, et al. The 2016 World Health Organization classification of tumors of the central nervous system: a summary. Acta Neuropathol (Berl). 2016;131(6):803–20.
Ricard D, Idbaih A, Ducray F, Lahutte M, Hoang-Xuan K, Delattre J-Y. Primary brain tumours in adults. Lancet. 2012;379(9830):1984–96.
Buckner JC, Brown PD, O’Neill BP, Meyer FB, Wetmore CJ, Uhm JH. Central nervous system tumors. Mayo Clin Proc. 2007;82(10):1271–86.
Horneck G. Space environment. In: Gargaud M, Irvine WM, Amils R, Cleaves HJ (Jim), Pinti DL, Quintanilla JC, et al, editors. Encyclopedia of astrobiology [Internet]. Berlin: Springer; 2015. p. 2293–9. Available from: https://doi.org/10.1007/978-3-662-44185-5_1469.
Gargaud M, Irvine WM, Amils R, Cleaves HJ, Pinti DL, Quintanilla JC, et al., editors. Encyclopedia of Astrobiology [Internet]. Berlin: Springer; 2015 [cited 2021 Jan 3]. Available from: https://doi.org/10.1007/978-3-662-44185-5
Beysens D, editor. Generation and applications of extra-terrestrial environments on earth. Aalborg: River Publishers; 2015. 282 p. (River publishers series in standardisation).
Benton ER, Benton EV. Space radiation dosimetry in low-Earth orbit and beyond. Nucl Instrum Methods Phys Res Sect B Beam Interact Mater At. 2001;184(1–2):255–94.
Blasi P. The origin of galactic cosmic rays. Astron Astrophys Rev. 2013;21(1):70.
Zeitlin C, Hassler DM, Cucinotta FA, Ehresmann B, Wimmer-Schweingruber RF, Brinza DE, et al. Measurements of energetic particle radiation in transit to Mars on the Mars science laboratory. Science. 2013;340(6136):1080–4.
Guo J, Zeitlin C, Wimmer-Schweingruber RF, Hassler DM, Posner A, Heber B, et al. Variations of dose rate observed by MSL/RAD in transit to Mars. Astron Astrophys. 2015;577:A58.
Horne RB, Thorne RM, Shprits YY, Meredith NP, Glauert SA, Smith AJ, et al. Wave acceleration of electrons in the Van Allen radiation belts. Nature. 2005;437(7056):227–30.
Fillius W, Ip WH, Mcilwain CE. Trapped radiation belts of Saturn: first look. Science. 1980;207(4429):425.
Acuna MH, Ness NF. The main magnetic field of Jupiter. J Geophys Res 1896–1977. 1976;81(16):2917–22.
Narici L, Rizzo A, Berrilli F, Del Moro D. Solar particle events and human deep space exploration: measurements and considerations. In: Extreme events in Geospace [Internet]. Elsevier; 2018 [cited 2021 Jan 3]. p. 433–51. Available from: https://linkinghub.elsevier.com/retrieve/pii/B9780128127001000170
Allen CS, Giraudo M, Moratto C, Yamaguchi N. Spaceflight environment. In: Space safety and human performance [Internet]. Elsevier; 2018 [cited 2021 Jan 3]. p. 87–138. Available from: https://linkinghub.elsevier.com/retrieve/pii/B9780081018699000042
Ehresmann B, Zeitlin CJ, Hassler DM, Matthiä D, Guo J, Wimmer-Schweingruber RF, et al. The charged particle radiation environment on Mars measured by MSL/RAD from November 15, 2015 to January 15, 2016. Radiat Martian Surf Model Comp Data Radiat Assess Detect Mars Sci Lab MSLRAD Results 1st Mars Space Radiat Model Workshop. 2017;14:3–11.
Cucinotta FA. Risk of radiation carcinogenesis, 52.
Nabors LB, Ammirati M, Bierman PJ, Brem H, Butowski N, Chamberlain MC, et al. Central nervous system cancers. J Natl Compr Cancer Netw JNCCN. 2013;11(9):1114–51.
Ostrom QT, Gittleman H, Truitt G, Boscia A, Kruchko C, Barnholtz-Sloan JS. CBTRUS statistical report: primary brain and other central nervous system tumors diagnosed in the United States in 2011–2015. Neuro-Oncol. 2018;20(Suppl 4):iv1–86.
Ostrom QT, de Blank PM, Kruchko C, Petersen CM, Liao P, Finlay JL, et al. Alex’s Lemonade Stand Foundation infant and childhood primary brain and central nervous system tumors diagnosed in the United States in 2007-2011. Neuro-Oncol. 2015;16(Suppl 10):x1–36.
Subramanian S, Ahmad T. Childhood Brain Tumors. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 [cited 2021 May 18]. Available from: http://www.ncbi.nlm.nih.gov/books/NBK535415/
Bailey P, Cushing HW. A classification of the tumors of the glioma group on a histo-genetic basis, with a correlated study of prognosis... With 108 illustrations. JB Lippincott Company; 1926.
Louis DN, Ohgaki H, Wiestler OD, Cavenee WK, Burger PC, Jouvet A, et al. The 2007 WHO classification of tumours of the central nervous system. Acta Neuropathol (Berl). 2007;114(2):97–109.
Rushing EJ. WHO classification of tumors of the nervous system: preview of the upcoming 5th edition. Memo - Mag Eur Med Oncol [Internet]. 2021 Feb 12 [Cited 2021 May 17]; Available from: https://doi.org/10.1007/s12254-021-00680-x
Wesseling P. Neurooncology: 2021 update. Free Neuropathol. 2021;2(0):5.
Wen PY, Huse JT. 2016 World Health Organization classification of central nervous system tumors. Contin Minneap Minn. 2017;23(6, Neuro-oncology):1531–47.
Gupta A, Dwivedi T. A simplified overview of World Health Organization classification update of central nervous system tumors 2016. J Neurosci Rural Pract. 2017;8(4):629–41.
Patel AP, Fisher JL, Nichols E, Abd-Allah F, Abdela J, Abdelalim A, et al. Global, regional, and national burden of brain and other CNS cancer, 1990–2016: a systematic analysis for the global burden of disease study 2016. Lancet Neurol. 2019;18(4):376–93.
Perry A, Wesseling P. Histologic classification of gliomas. Handb Clin Neurol. 2016;134:71–95.
Weller M, Reifenberger G. Beyond the World Health Organization classification of central nervous system tumors 2016: what are the new developments for gliomas from a clinician’s perspective? Curr Opin Neurol. 2020;33(6):701–6.
Kristensen BW, Priesterbach-Ackley LP, Petersen JK, Wesseling P. Molecular pathology of tumors of the central nervous system. Ann Oncol. 2019;30(8):1265–78.
Cairncross JG, Ueki K, Zlatescu MC, Lisle DK, Finkelstein DM, Hammond RR, et al. Specific genetic predictors of chemotherapeutic response and survival in patients with anaplastic oligodendrogliomas. J Natl Cancer Inst. 1998;90(19):1473–9.
Gao K, Li G, Qu Y, Wang M, Cui B, Ji M, et al. TERT promoter mutations and long telomere length predict poor survival and radiotherapy resistance in gliomas. Oncotarget. 2016;7(8):8712–25.
Håvik AB, Brandal P, Honne H, Dahlback H-SS, Scheie D, Hektoen M, et al. MGMT promoter methylation in gliomas-assessment by pyrosequencing and quantitative methylation-specific PCR. J Transl Med. 2012;10:36.
van den Bent MJ, Chang SM. Grade II and III Oligodendroglioma and astrocytoma. Neurol Clin. 2018;36(3):467–84.
Walker M, Weller RO. Tumors of the central nervous system (AFIP Atlas of tumor pathology, series 4. Fascicle 7). Neuropathol Appl Neurobiol. 2008;34(4):473–4.
Sharma MK, Mansur DB, Reifenberger G, Perry A, Leonard JR, Aldape KD, et al. Distinct genetic signatures among pilocytic astrocytomas relate to their brain region origin. Cancer Res. 2007;67(3):890–900.
Komori T. Updating the grading criteria for adult diffuse gliomas: beyond the WHO2016CNS classification. Brain Tumor Pathol. 2020;37(1):1–4.
Mesfin FB, Al-Dhahir MA. Gliomas. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 [cited 2021 May 19]. Available from: http://www.ncbi.nlm.nih.gov/books/NBK441874/
Caccese M, Padovan M, D’Avella D, Chioffi F, Gardiman MP, Berti F, et al. Anaplastic astrocytoma: state of the art and future directions. Crit Rev Oncol Hematol. 2020;153:103062.
Castle M. cIMPACT recommendations for the classification of diffuse gliomas 2020 | Radiology Reference Article | Radiopaedia.org [Internet]. Radiopaedia. [cited 2021 May 18]. Available from: https://radiopaedia.org/articles/cimpact-recommendations-for-the-classification-of-diffuse-gliomas-2020-1?lang=us
Weller M, van den Bent M, Tonn JC, Stupp R, Preusser M, Cohen-Jonathan-Moyal E, et al. European Association for Neuro-Oncology (EANO) guideline on the diagnosis and treatment of adult astrocytic and oligodendroglial gliomas. Lancet Oncol. 2017;18(6):e315–29.
Tork CA, Atkinson C. Oligodendroglioma. In: StatPearls [internet]. Treasure Island (FL): StatPearls Publishing; 2021 [cited 2021 May 19]. Available from: http://www.ncbi.nlm.nih.gov/books/NBK559184/
Batash R, Asna N, Schaffer P, Francis N, Schaffer M. Glioblastoma multiforme, diagnosis and treatment; recent literature review. Curr Med Chem [Internet] 2017 Sep 21 [cited 2021 May 19];24(27). Available from: http://www.eurekaselect.com/152454/article
Lah TT, Novak M, Breznik B. Brain malignancies: glioblastoma and brain metastases. Semin Cancer Biol. 2020;60:262–73.
Claes A, Idema AJ, Wesseling P. Diffuse glioma growth: a guerilla war. Acta Neuropathol (Berl). 2007;114(5):443–58.
Singh SK, Clarke ID, Hide T, Dirks PB. Cancer stem cells in nervous system tumors. Oncogene. 2004;23(43):7267–73.
Prager BC, Bhargava S, Mahadev V, Hubert CG, Rich JN. Glioblastoma stem cells: driving resilience through chaos. Trends Cancer. 2020;6(3):223–35.
Muir M, Gopakumar S, Traylor J, Lee S, Rao G. Glioblastoma multiforme: novel therapeutic targets. Expert Opin Ther Targets. 2020;24(7):605–14.
Hemmersbach R, Strauch SM, Seibt D, Schuber M. Comparative studies on gravisensitive protists on ground (2D and 3D clinostats) and in microgravity. Microgravity - Sci Technol. 2006;18(3):257–9.
Svejgaard B, Wehland M, Ma X, Kopp S, Sahana J, Warnke E, et al. Common effects on cancer cells exerted by a random positioning machine and a 2D clinostat. PLoS One. 2015;10(8):e0135157.
Herranz R, Anken R, Boonstra J, Braun M, Christianen PCM, de Geest M, et al. Ground-based facilities for simulation of microgravity: organism-specific recommendations for their use, and recommended terminology. Astrobiology. 2013;13(1):1–17.
van Loon JJWA. Some history and use of the random positioning machine, RPM, in gravity related research. Adv Space Res. 2007;39(7):1161–5.
Borst AG, van Loon JJWA. Technology and developments for the random positioning machine, RPM. Microgravity Sci Technol. 2008;21(4):287.
Klaus DM. Clinostats and bioreactors. Gravitational space. Biol Bull Publ Am Soc Gravitational Space Biol. 2001;14(2):55–64.
Kapałczyńska M, Kolenda T, Przybyła W, Zajączkowska M, Teresiak A, Filas V, et al. 2D and 3D cell cultures – a comparison of different types of cancer cell cultures. Arch Med Sci AMS. 2018;14(4):910–9.
Birgersdotter A, Sandberg R, Ernberg I. Gene expression perturbation in vitro--a growing case for three-dimensional (3D) culture systems. Semin Cancer Biol. 2005;15(5):405–12.
Yamada KM, Cukierman E. Modeling tissue morphogenesis and cancer in 3D. Cell. 2007;130(4):601–10.
Sodunke TR, Turner KK, Caldwell SA, McBride KW, Reginato MJ, Noh HM. Micropatterns of Matrigel for three-dimensional epithelial cultures. Biomaterials. 2007;28(27):4006–16.
Hickman JA, Graeser R, de Hoogt R, Vidic S, Brito C, Gutekunst M, et al. Three-dimensional models of cancer for pharmacology and cancer cell biology: capturing tumor complexity in vitro/ex vivo. Biotechnol J. 2014;9(9):1115–28.
Shimbo M, Kudo T, Hamada M, Jeon H, Imamura Y, Asano K, et al. Ground-based assessment of JAXA mouse habitat cage unit by mouse phenotypic studies. Exp Anim. 2016;65(2):175–87.
Larose T. Tumors in Space: Preparation for Spaceflight. In: Pletser V, editor. Preparation of Space Experiments [Internet]. IntechOpen; 2020 [cited 2021 Jan 14]. Available from: https://www.intechopen.com/books/preparation-of-space-experiments/tumors-in-space-preparation-for-spaceflight
Horneck G. HZE particle effects in space. Acta Astronaut. 1994;32(11):749–55.
Georgakilas AG, O’Neill P, Stewart RD. Induction and repair of clustered DNA lesions: what do we know so far? Radiat Res. 2013;180(1):100–9.
Fry RJM, Ley RD, Grube D, Staffeldt E. Studies on the multistage nature of radiation carcinogenesis [Internet]. United States; 1980. p. 21. Available from: http://inis.iaea.org/search/search.aspx?orig_q=RN:13668558
Hanahan D, Weinberg RA. The hallmarks of cancer. Cell. 2000;100(1):57–70.
Seymour CB, Mothersill C. Radiation-induced bystander effects—implications for cancer. Nat Rev Cancer. 2004;4(2):158–64.
Cucinotta FA, Kim M-HY, Chappell LJ, Huff JL. How safe is safe enough? Radiation risk for a human mission to Mars. PLoS ONE [Internet] 2013 Oct 16 [cited 2021 Apr 30];8(10). Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3797711/
Sahebi R, Aghaei M, Halvaei S, Alizadeh A. The role of microgravity in cancer: a dual-edge sword. Multidiscip Cancer Investig. 2017;1(3):1–2.
Vidyasekar P, Shyamsunder P, Arun R, Santhakumar R, Kapadia NK, Kumar R, et al. Genome wide expression profiling of cancer cell lines cultured in microgravity reveals significant dysregulation of cell cycle and MicroRNA gene networks. PLoS One. 2015;10(8):e0135958.
Simulated Microgravity Promotes Cell Apoptosis Through Suppressing Uev1A/TICAM/TRAF/NF-κB-Regulated Anti-Apoptosis and p53/PCNA- and ATM/ATR-Chk1/2-Controlled DNA-Damage Response Pathways - PubMed [Internet]. [cited 2021 Jan 14]. Available from: https://pubmed.ncbi.nlm.nih.gov/26887372/
Kim YJ, Jeong AJ, Kim M, Lee C, Ye S-K, Kim S. Time-averaged simulated microgravity (taSMG) inhibits proliferation of lymphoma cells, L-540 and HDLM-2, using a 3D clinostat. Biomed Eng Online. 2017;16(1):48.
Uva BM, Masini MA, Sturla M, Prato P, Passalacqua M, Giuliani M, et al. Clinorotation-induced weightlessness influences the cytoskeleton of glial cells in culture. Brain Res. 2002;934(2):132–9.
Modeled microgravity causes changes in the cytoskeleton and focal adhesions, and decreases in migration in malignant human MCF-7 cells - PubMed [Internet]. [cited 2021 Jan 14]. Available from: https://pubmed.ncbi.nlm.nih.gov/19730978/
Grimm D, Bauer J, Kossmehl P, Shakibaei M, Schöberger J, Pickenhahn H, et al. Simulated microgravity alters differentiation and increases apoptosis in human follicular thyroid carcinoma cells. FASEB J Off Publ Fed Am Soc Exp Biol. 2002;16(6):604–6.
Riwaldt S, Bauer J, Wehland M, Slumstrup L, Kopp S, Warnke E, et al. Pathways regulating spheroid formation of human follicular thyroid cancer cells under simulated microgravity conditions: a genetic approach. Int J Mol Sci. 2016;17(4):528.
Velliou E, Gupta P, Ricci C, Danti S. Chapter 11 - Biomaterial-based in vitro models for pancreatic cancer. In: Kundu SC, Reis RL, editors. Biomaterials for 3D Tumor Modeling [Internet]. Elsevier; 2020 [cited 2021 Jan 14]. p. 235–49. (Materials Today). Available from: http://www.sciencedirect.com/science/article/pii/B9780128181287000113
Boonstra J. Growth factor-induced signal transduction in adherent mammalian cells is sensitive to gravity. FASEB J Off Publ Fed Am Soc Exp Biol. 1999;13(Suppl):S35–42.
Qi S, Liu Y. Differences in protein expression between the u251 and u87 cell lines. Turk Neurosurg [Internet]. 2016 [cited 2021 Mar 26]; Available from: https://doi.org/10.5137/1019-5149.JTN.17746-16.1
Oh S-J, Yang J-I, Kim O, Ahn E-J, Kang WD, Lee J-H, et al. Human U87 glioblastoma cells with stemness features display enhanced sensitivity to natural killer cell cytotoxicity through altered expression of NKG2D ligand. Cancer Cell Int [Internet]. 2017 Feb 10 [cited 2021 Jan 14];17. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5303255/
Deng B, Liu R, Tian X, Han Z, Chen J. Simulated microgravity inhibits the viability and migration of glioma via FAK/RhoA/Rock and FAK/Nek2 signaling. In Vitro Cell Dev Biol Anim. 2019;55(4):260–71.
Zhao J, Ma H, Wu L, Cao L, Yang Q, Dong H, et al. The influence of simulated microgravity on proliferation and apoptosis in U251 glioma cells. In Vitro Cell Dev Biol Anim. 2017;53(8):744–51.
McDonald KL, O’Sullivan MG, Parkinson JF, Shaw JM, Payne CA, Brewer JM, et al. IQGAP1 and IGFBP2: valuable biomarkers for determining prognosis in glioma patients. J Neuropathol Exp Neurol. 2007;66(5):405–17.
Shi Z, Rao W, Wang H, Wang N, Si J-W, Zhao J, et al. Modeled microgravity suppressed invasion and migration of human glioblastoma U87 cells through downregulating store-operated calcium entry. Biochem Biophys Res Commun. 2015;457(3):378–84.
Hyväri L, Ojansivu M, Juntunen M, Kartasalo K, Miettinen S, Vanhatupa S. Focal adhesion kinase and rock signaling are switch-like regulators of human adipose stem cell differentiation towards osteogenic and adipogenic lineages [Internet]. Vol. 2018, Stem Cells International. Hindawi; 2018 [cited 2021 Jan 14]. p. e2190657. Available from: https://www.hindawi.com/journals/sci/2018/2190657/
Rozengurt E. Chapter 4 - Signaling Pathways Induced by G-protein-coupled Receptors. In: Johnson LR, Ghishan FK, Kaunitz JD, Merchant JL, Said HM, Wood JD, editors. Physiology of the gastrointestinal tract (5th Edition) [Internet]. Boston: Academic Press; 2012 [cited 2021 Jan 14]. p. 75–96. Available from: http://www.sciencedirect.com/science/article/pii/B978012382026600004X
Modeled microgravity suppressed invasion and migration of human glioblastoma U87 cells through downregulating store-operated calcium entry - PubMed [Internet]. [cited 2021 Jan 14]. Available from: https://pubmed.ncbi.nlm.nih.gov/25580009/
Chen Y-W, Chen Y-F, Chen Y-T, Chiu W-T, Shen M-R. The STIM1-Orai1 pathway of store-operated Ca 2+ entry controls the checkpoint in cell cycle G1/S transition. Sci Rep. 2016;6(1):22142.
Cucinotta FA. Space radiation risks for astronauts on multiple international Space Station missions. PLoS One. 2014;9(4):e96099.
Cucinotta FA, To K, Cacao E. Predictions of space radiation fatality risk for exploration missions. Life Sci Space Res. 2017;13:1–11.
Fry RJ. Radiation effects in space. Adv Space Res Off J Comm Space Res COSPAR. 1986;6(11):261–8.
Kelly SE, Benedetto AD, Greco A, Howard CM, Sollars VE, Primerano DA, et al. Rapid selection and proliferation of CD133(+) cells from cancer cell lines: chemotherapeutic implications. PLoS One. 2010;5(4):e10035.
Mihailova M, Trenev V, Genova P, Konstantinov S. Process simulation in a mechatronic bioreactor device with speed-regulated motors for growing of three-dimensional cell cultures. Ann N Y Acad Sci. 2006;1091(1):470–89.
Mitteregger R, Vogt G, Rossmanith E, Falkenhagen D. Rotary cell culture system (RCCS): a new method for cultivating hepatocytes on microcarriers. Int J Artif Organs. 1999;22(12):816–22.
Grimm D, Wehland M, Corydon TJ, Richter P, Prasad B, Bauer J, et al. The effects of microgravity on differentiation and cell growth in stem cells and cancer stem cells. Stem Cells Transl Med. 2020;9(8):882–94.
Yuan M, Liu H, Zhou S, Zhou X, Huang Y, Hou F, et al. Integrative analysis of regulatory module reveals associations of microgravity with dysfunctions of multi-body systems and tumorigenesis. Int J Mol Sci [Internet]. 2020 Oct 14 [cited 2021 May 1];21(20). Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7589633/
Panesar SS, Fernandez-Miranda JC, Kliot M, Ashkan K. Neurosurgery and manned spaceflight. Neurosurgery [Internet] 2018 Nov 8 [cited 2021 Jan 5]; Available from: https://doi.org/10.1093/neuros/nyy531/5165256
Michael AP. Spaceflight induced changes in the central nervous system. In: Russomano T, Rehnberg L, editors. Into space - A journey of how humans adapt and live in microgravity [Internet]. InTech; 2018 [cited 2021 Jan 5]. Available from: http://www.intechopen.com/books/into-space-a-journey-of-how-humans-adapt-and-live-in-microgravity/spaceflight-induced-changes-in-the-central-nervous-system
Cucinotta FA, Schimmerling W, Wilson JW, Peterson LE, Badhwar GD, Saganti PB, et al. Space radiation cancer risks and uncertainties for Mars missions. Radiat Res. 2001;156(5):682–8.
Radiation Hazards to Crews of Interplanetary Missions: Biological Issues and Research Strategies [Internet]. Washington, DC: National Academies Press; 1996 [cited 2021 Jan 5]. Available from: http://www.nap.edu/catalog/5540
Fry RJM, Powers-Risius P, Alpen EL, Ainsworth EJ. High-LET radiation carcinogenesis. Radiat Res Suppl. 1985;8:S188.
Cucinotta FA, Durante M. Cancer risk from exposure to galactic cosmic rays: implications for space exploration by human beings. Lancet Oncol. 2006;7(5):431–5.
Chancellor JC, Blue RS, Cengel KA, Auñón-Chancellor SM, Rubins KH, Katzgraber HG, et al. Limitations in predicting the space radiation health risk for exploration astronauts. Npj Microgravity. 2018;4(1):8.
Brungs S, Hauslage J, Hemmersbach R. Validation of random positioning versus clinorotation using a macrophage model system. Microgravity Sci Technol. 2019;31(2):223–30.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Johnson, K.V.L., Michael, A.P., Saehle, T. (2022). Central Nervous System Neoplasms in Microgravity. In: Michael, A.P., Otto, C., Reschke, M.F., Hargens, A.R. (eds) Spaceflight and the Central Nervous System. Springer, Cham. https://doi.org/10.1007/978-3-031-18440-6_8
Download citation
DOI: https://doi.org/10.1007/978-3-031-18440-6_8
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-18439-0
Online ISBN: 978-3-031-18440-6
eBook Packages: MedicineMedicine (R0)