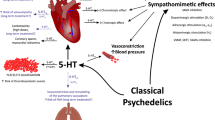
Abstract
Stimulant and psychedelic drugs of abuse exert their effects through interactions with monoaminergic systems. Compared to other monoaminergic receptors and transporters, the 5-hydroxytryptamine 2B (5-HT2B) receptor represents a relatively little studied target of serotonergic drugs of abuse. However, studies suggest the involvement of 5-HT2B receptors in the mechanism of action of serotonergic stimulants and receptor activation may additionally lead to specific adverse effects such as cardiac valvulopathy in users. 5-HT2B receptor activation has been demonstrated for stimulant-type new psychoactive substances of the benzofuran class and for substituted amphetamines with a distinct serotonergic vs. dopaminergic profile. Besides stimulants, many psychedelic drugs activate the 5-HT2B receptor but the consequence thereof remains unclear. Cardiac valvulopathy is likely not an adverse effect to consider when psychedelics are used occasionally but this may be different for “microdosing” which involves low doses of psychedelics taken daily or multiple times per week.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
A variety of drugs of abuse affect monoaminergic neurotransmission including the serotonergic system. On the one hand, serotonergic stimulants target the plasmalemmal serotonin transporter (SERT), either as blockers such as cocaine or as substrates such as 3,4-methylenedioxymethamphetamine (MDMA) [1,2,3,4,5]; on the other hand, serotonergic psychedelics mediate their mind-altering effects mainly through activation of serotonergic 5-hydroxytryptamine (5-HT) 2A receptors [6,7,8,9,10,11]. Moreover, several stimulant-type substances interact with serotonergic receptors [2, 12,13,14,15,16] and some psychedelics inhibit transporter-mediated serotonin reuptake [17] in addition to their main action at the 5-HT2A receptor. Besides stimulants and psychedelics, other drug classes such as synthetic cannabinoids and opioids have been shown to interact with serotonin transporers and receptors [18,19,20] in addition to their main effects at cannabinoid and opioid receptors, respectively. The 5-HT2B receptor is one potential interaction site for serotonergic drugs of abuse. However, the 5-HT2B receptor is not a primary target for serotonergic drugs as its main expression is in peripheral organs such as liver, kidneys, stomach, and gut, and there is only limited expression in the brain [21,22,23,24,25]. Nevertheless, it has been associated with pathways that modulate drug abuse and reinforcing effects of stimulants [26,27,28]. Furthermore, 5-HT2B receptor interactions with drugs of abuse are of interest as receptor activation has been associated with cardiac valvulopathy, resulting in the market removal of several 5-HT2B agonist prescription drugs, including the appetite suppressant fenfluramine [29,30,31,32]. The major metabolite of fenfluramine, norfenfluramine (3-trifluoromethylamphetamine), displays higher affinity and efficacy at the 5-HT2B receptor in comparison to the parent compound [32, 33], indicating that it is mainly responsible for fenfluramine-induced cardiac valvulopathy. Even though fenfluramine has structural similarity to amphetamine, it does not share the potent stimulant effects and abuse is therefore rare [34, 35]. However, the chemical structures of fenfluramine and norfenfluramine suggest that drug-induced cardiac valvulopathy is a potentially severe complication to consider for any amphetamine-type drugs of abuse that stimulate serotonin 5-HT2B receptors [36]. This chapter should give a basic overview over the involvement of 5-HT2B receptors in recreational drug action and associated adverse effects such as cardiac valvulopathy. Different stimulant and psychedelic drugs for which activity at the 5-HT2B receptors has been tested will be discussed.
2 Drugs Stimulating 5-HT2B Receptors
Interference with monoaminergic signaling is the main mechanism of action for stimulants and psychedelics [1, 4, 37]. In addition, interactions with monoaminergic targets have been shown for other drug classes, such as opioids [17] or dissociative anesthetics [38, 39]. Compared to other monoaminergic targets such as 5-HT2A or dopamine receptors, relatively little research has focused on the interactions of drugs of abuse with 5-HT2B receptors. Nevertheless, 5-HT2B receptor interactions have been assessed for various stimulant and psychedelic drugs of abuse, including many new psychoactive substances (NPS) [3, 14, 16, 17, 40,41,42,43,44,45], which are shown in Tables 16.1 and 16.2, respectively.
2.1 5-HT2B Receptor-Mediated Effects of Stimulants
Despite its limited expression in the brain, the 5-HT2B receptor has been shown to contribute to the mechanism of action of stimulants. For instance, it has been demonstrated that selective 5-HT2B receptor antagonism and 5-HT2B receptor knockout reversed MDMA-induced hyperactivity in mice [28]. Furthermore, it has been demonstrated that inhibition and knockout of the 5-HT2B receptors abolished MDMA-induced efflux of serotonin in the nucleus accumbens and ventral tegmental area [28]. The authors of that study hypothesized that presynaptic 5-HT2B receptors modulate MDMA-induced 5-HT release in serotoninergic raphe neurons. In addition, inhibition and knockout of the 5-HT2B receptor led to an absence of dopamine efflux in the nucleus accumbens, which may have been the result of a lack of activation of postsynaptic serotonin receptors [28]. In a follow-up study, MDMA was shown to induce locomotor sensitization and conditioned place preference in wildtype but not in 5-HT2B receptor knockout or 5-HT2B receptor antagonized mice, underscoring the possible role of 5-HT2B receptors in the reinforcing effects of serotonergic stimulants [27]. However, an increased dose of MDMA induced behavioral effects in all mouse models, potentially due to direct and therefore 5-HT2B receptor independent interaction of MDMA with the dopamine transporter [27]. This assumption is supported by in vitro studies showing serotonin transporter inhibition at low and dopamine transporter inhibition by MDMA at high concentrations [5, 12].
2.2 Stimulant-Induced Cardiac Valvulopathy
5-HT2B receptors are, among others, expressed in cardiovascular tissues [47] and their activation potentially leads to cardiac valvulopathy [29, 48,49,50]. Therefore, cardiac valvulopathy is a concern to consider for drugs that increase plasma 5-HT levels, directly activate the 5-HT2B receptor, or both. In fact, several prescription drugs have previously been removed from the market due to their potential to induce cardiac valvulopathy in patients [29,30,31,32]. However, serotonergic drugs of abuse are typically not associated with a high abuse liability [51,52,53,54] and are therefore mostly used sporadically and not on a regular basis. This raises the question of the relevance of 5-HT2B-mediated cardiac valvulopathy in recreational drug use. The regular use of the serotonergic drug MDMA has been associated with mild to moderate valvular heart disease, based on a case control study [55]. In this study, 8 of 29 regular MDMA users displayed abnormal echocardiographic results compared with none of the control group. The average use of the MDMA users was very high and described to have consisted of 3.6 MDMA tablets per week with an average duration of drug use of 6.1 years [55]. This underscores the assumption that in particular heavy recreational use of serotonergic stimulants may induce cardiac valvulopathy. Besides these clinical findings from a case control study, 5-HT2B receptor-mediated proliferation of cardiac valvular interstitial cells induced by MDMA has also been demonstrated in vitro [56].
2.3 Stimulants Acting on 5-HT2B Receptors
Table 16.1 shows an overview of 5-HT2B receptor binding and activation potency values for various stimulants, assessed in different studies. Notably, in a study by Rickli and colleagues, MDMA did not activate the 5-HT2B receptor in the functional assay at investigated concentrations (EC50 > 20 μM); however, 3,4-methylenedioxyamphetamine (MDA), the main psychoactive N-demethylated phase I metabolite of MDMA, potently activated the receptor at submicromolar concentrations [14]. This suggests that the metabolite MDA rather than MDMA itself may lead to valvulopathy and that there could be a significant metabolic contribution to MDMA-induced effects and adverse effect. MDA formation is mainly mediated by cytochrome P450 (CYP) 2B6, with additional contributions from CYP1A2, CYP2C19, and CYP2D6 [57,58,59,60]. Therefore, genetic polymorphisms in the genes coding for these enzymes could potentially influence the 5-HT2B receptor-mediated adverse effects in MDMA users. Notably, however, the sensitivity of the calcium mobilization assays used to determine the functional 5-HT2B receptor activity and the inter-correlation of data obtained with different assays is not clearly understood. For example, only poor correlation between 5-HT2A receptor activation and effects for psychedelics has been observed in several studies [61,62,63], whereas binding affinity at this receptor was a good predictor of the clinical potency of psychedelics [63]. Thus, the available in vitro 5-HT2B receptor functional data may not be a good predictor of cardiac valvulopathy risk in vivo.
Besides MDA, several benzofuran NPS potently activated the 5-HT2B receptor at submicromolar concentrations [14, 43]. Therefore, as shown for MDMA in vivo [27, 28], 5-HT2B receptor activation may directly contribute to the effects of these novel drugs of abuse. Furthermore, regular and heavy use of benzofuran NPS may potentially result in heart damage; however, benzofurans have so far not been linked to any case of cardiac valvulopathy. Only a few other non-benzofuran stimulants displayed potent agonism at the 5-HT2B receptor, such as 4-methylamphetamine (4-MA) or 5-(2-aminopropyl)indole (5-IT). The amphetamine derivative 4-MA was originally developed as an appetite suppressant but was never marketed [64]. Its recent reappearance on the illicit drug market has almost exclusively been limited to being a contaminant in street amphetamine samples [65]. The mixture of amphetamine and 4-MA has been linked to extreme hyperthermia and several fatalities, likely explained by the high difference in dopaminergic vs. serotonergic activity of the two substances [15, 16, 65]. The indole derivative 5-IT is a highly potent stimulant NPS that has been associated with various fatal intoxications in recent years [16, 66,67,68,69]. Furthermore, Iversen and colleagues reported submicromolar binding affinities at the 5-HT2B receptor for the NPS 5-iodo-aminoindane, mephedrone, naphyrone, 1-naphyrone, and methylenedioxy-aminotetralin [43]. Mephedrone is not a potent agonist at the receptor [16] and no functional activity has been determined for the other substances. Therefore, it is not certain whether these substances act as agonists at the 5-HT2B receptor.
2.4 5-HT2B Receptor-Mediated Effects of Psychedelics
The subjective effects of psychedelics are primarily mediated by 5-HT2A receptor activation [9,10,11, 70,71,72]. In addition, correlation between receptor activation and psychedelic effect potencies have been reported for the 5-HT2B [46] and 5-HT2C receptors [6, 7, 63], which is not surprising given that 5-HT2 receptors share significant sequence homology [73]. However, there is currently no clear consensus on the importance of the 5-HT2B and 5-HT2C receptors in the mechanism of action of psychedelics.
2.5 Psychedelics Acting on 5-HT2B Receptors
5-HT2B receptor interactions for various psychedelics are listed in Table 16.2. For most of the substances, only receptor activation potency but no receptor affinity values have been reported. Most phenethylamine and tryptamine psychedelics activated the 5-HT2B receptor at submicromolar or low micromolar concentrations. As reported for the 5-HT2A receptor, no correlation between 5-HT2B receptor activation and clinical potency of psychedelic was observed in a study comparing receptor activation potencies of a considerable amount of psychedelics with their reported human doses [63]. Eshleman and colleagues reported 5-HT2 receptor affinities as well as functional activity for six phenethylamine psychedelics and lysergic acid diethylamide (LSD) [42]. All compounds displayed highest binding affinity and activation potency for the 5-HT2A receptors; nevertheless, for several substances, high affinity and activation potency (Ki and EC50 < 100 nM) was observed at the 5-HT2B receptor [42]. A remarkable difference in receptor activation in two different functional assays has been reported for LSD. Whereas an EC50 of 12 μM has been measured with a calcium mobilization assay [40], an EC50 of 3 nM has been reported when a stimulation of inositol monophosphate (IP-1) formation assay was used [42]. To gain a clearer picture of the involvement of 5-HT2B receptors in the action of psychedelics, more in vitro and in vivo research is needed.
3 Conclusion
Several stimulant and psychedelic drugs of abuse activate the 5-HT2B receptor at pharmacologically relevant concentrations. Animal studies with MDMA suggest that the 5-HT2B receptor contributes to the effects of serotonergic stimulants, possibly by 5-HT-dependent regulation of dopamine release. Furthermore, stimulants that activate the 5-HT2B receptor may put regular and heavy users at risk of cardiac valvulopathy. The main classes of stimulant drugs of abuse that interact with 5-HT2B receptors are benzofurans and amphetamines with a distinct serotonergic vs. dopaminergic activity.
In addition to stimulants, various phenethylamine and tryptamine psychedelics activate the 5-HT2B receptor. However, the role of 5-HT2B receptor activation in the mechanism of action of psychedelic remains unclear. As psychedelics do not lead to dependence and are mostly not used on a regular basis, cardiac valvulopathy is likely not a risk to consider for users.
Abbreviations
- MDA:
-
3,4-methylenedioxyamphetamine
- MDMA:
-
3,4-methylenedioxymethamphetamine
- CYP:
-
Cytochrome P450
- LSD:
-
Lysergic acid diethylamide
- NPS:
-
New psychoactive substances
- SERT:
-
Serotonin transporter
References
Sitte HH, Freissmuth M (2015) Amphetamines, new psychoactive drugs and the monoamine transporter cycle. Trends Pharmacol Sci 36(1):41–50
Simmler LD, Rickli A, Schramm Y, Hoener MC, Liechti ME (2014) Pharmacological profiles of aminoindanes, piperazines, and pipradrol derivatives. Biochem Pharmacol 88(2):237–244
Luethi D, Kaeser PJ, Brandt SD, Krähenbühl S, Hoener MC, Liechti ME (2018) Pharmacological profile of methylphenidate-based designer drugs. Neuropharmacology 134:133–140
Rothman RB, Baumann MH (2003) Monoamine transporters and psychostimulant drugs. Eur J Pharmacol 479(1–3):23–40
Luethi D, Kolaczynska KE, Walter M, Suzuki M, Rice KC, Blough BE et al (2019) Metabolites of the ring-substituted stimulants MDMA, methylone and MDPV differentially affect human monoaminergic systems. J Psychopharmacol 33:831–841
Nichols DE (2016) Psychedelics. Pharmacol Rev 68(2):264–355
Nichols DE (2004) Hallucinogens. Pharmacol Ther 101(2):131–181
Liechti ME (2017) Modern clinical research on LSD. Neuropsychopharmacology 42(11):2114–2127
Vollenweider FX, Vollenweider-Scherpenhuyzen MF, Bäbler A, Vogel H, Hell D (1998) Psilocybin induces schizophrenia-like psychosis in humans via a serotonin-2 agonist action. Neuroreport 9(17):3897–3902
Preller KH, Herdener M, Pokorny T, Planzer A, Kraehenmann R, Stampfli P et al (2017) The fabric of meaning and subjective effects in LSD-induced states depend on serotonin 2A receptor activation. Curr Biol 27(3):451–457
Kraehenmann R, Pokorny D, Vollenweider L, Preller KH, Pokorny T, Seifritz E et al (2017) Dreamlike effects of LSD on waking imagery in humans depend on serotonin 2A receptor activation. Psychopharmacology 234:2031–2046
Simmler LD, Buser TA, Donzelli M, Schramm Y, Dieu LH, Huwyler J et al (2013) Pharmacological characterization of designer cathinones in vitro. Br J Pharmacol 168(2):458–470
Simmler LD, Rickli A, Hoener MC, Liechti ME (2014) Monoamine transporter and receptor interaction profiles of a new series of designer cathinones. Neuropharmacology 79:152–160
Rickli A, Kopf S, Hoener MC, Liechti ME (2015a) Pharmacological profile of novel psychoactive benzofurans. Br J Pharmacol 172(13):3412–3425
Rickli A, Hoener MC, Liechti ME (2015b) Monoamine transporter and receptor interaction profiles of novel psychoactive substances: para-halogenated amphetamines and pyrovalerone cathinones. Eur Neuropsychopharmacol 25(3):365–376
Luethi D, Kolaczynska KE, Docci L, Krähenbühl S, Hoener MC, Liechti ME (2018) Pharmacological profile of mephedrone analogs and related new psychoactive substances. Neuropharmacology 134:4–12
Rickli A, Moning OD, Hoener MC, Liechti ME (2016) Receptor interaction profiles of novel psychoactive tryptamines compared with classic hallucinogens. Eur Neuropsychopharmacol 26(8):1327–1337
Rickli A, Liakoni E, Hoener MC, Liechti ME (2018) Opioid-induced inhibition of the human 5-HT and noradrenaline transporters in vitro: link to clinical reports of serotonin syndrome. Br J Pharmacol 175(3):532–543
Hill MN, Sun JC, Tse MT, Gorzalka BB (2006) Altered responsiveness of serotonin receptor subtypes following long-term cannabinoid treatment. Int J Neuropsychopharmacol 9(3):277–286
Darmani NA (2001) Cannabinoids of diverse structure inhibit two DOI-induced 5-HT2A receptor-mediated behaviors in mice. Pharmacol Biochem Behav 68(2):311–317
Bonhaus DW, Bach C, DeSouza A, Salazar FH, Matsuoka BD, Zuppan P et al (1995) The pharmacology and distribution of human 5-hydroxytryptamine2B (5-HT2B) receptor gene products: comparison with 5-HT2A and 5-HT2C receptors. Br J Pharmacol 115(4):622–628
Borman RA, Tilford NS, Harmer DW, Day N, Ellis ES, Sheldrick RL et al (2002) 5-HT2B receptors play a key role in mediating the excitatory effects of 5-HT in human colon in vitro. Br J Pharmacol 135(5):1144–1151
Choi DS, Maroteaux L (1996) Immunohistochemical localisation of the serotonin 5-HT2B receptor in mouse gut, cardiovascular system, and brain. FEBS Lett 391(1–2):45–51
Choi DS, Birraux G, Launay JM, Maroteaux L (1994) The human serotonin 5-HT2B receptor: pharmacological link between 5-HT2 and 5-HT1D receptors. FEBS Lett 352(3):393–399
Duxon MS, Flanigan TP, Reavley AC, Baxter GS, Blackburn TP, Fone KC (1997) Evidence for expression of the 5-hydroxytryptamine-2B receptor protein in the rat central nervous system. Neuroscience 76(2):323–329
Lin Z, Walther D, Yu XY, Drgon T, Uhl GR (2004) The human serotonin receptor 2B: coding region polymorphisms and association with vulnerability to illegal drug abuse. Pharmacogenetics 14(12):805–811
Doly S, Bertran-Gonzalez J, Callebert J, Bruneau A, Banas SM, Belmer A et al (2009) Role of serotonin via 5-HT2B receptors in the reinforcing effects of MDMA in mice. PLoS One 4(11):e7952
Doly S, Valjent E, Setola V, Callebert J, Herve D, Launay JM et al (2008) Serotonin 5-HT2B receptors are required for 3,4-methylenedioxymethamphetamine-induced hyperlocomotion and 5-HT release in vivo and in vitro. J Neurosci 28(11):2933–2940
Elangbam CS (2010) Drug-induced valvulopathy: an update. Toxicol Pathol 38(6):837–848
Bhattacharyya S, Schapira AH, Mikhailidis DP, Davar J (2009) Drug-induced fibrotic valvular heart disease. Lancet 374(9689):577–585
Hutcheson JD, Setola V, Roth BL, Merryman WD (2011) Serotonin receptors and heart valve disease—it was meant 2B. Pharmacol Ther 132(2):146–157
Rothman RB, Baumann MH, Savage JE, Rauser L, McBride A, Hufeisen SJ et al (2000) Evidence for possible involvement of 5-HT2B receptors in the cardiac valvulopathy associated with fenfluramine and other serotonergic medications. Circulation 102(23):2836–2841
Fitzgerald LW, Burn TC, Brown BS, Patterson JP, Corjay MH, Valentine PA et al (2000) Possible role of valvular serotonin 5-HT2B receptors in the cardiopathy associated with fenfluramine. Mol Pharmacol 57(1):75–81
Levin A (1975) The non-medical misuse of fenfluramine by drug-dependent young South Africans. Postgrad Med J 51(Suppl 1):186–188
Foltin RW, Haney M, Comer SD, Fischman MW (1996) Effect of fenfluramine on food intake, mood, and performance of humans living in a residential laboratory. Physiol Behav 59(2):295–305
Dawson P, Moffatt JD (2012) Cardiovascular toxicity of novel psychoactive drugs: lessons from the past. Prog Neuro-Psychopharmacol Biol Psychiatry 39(2):244–252
Liechti ME (2014) Novel psychoactive substances (designer drugs): overview and pharmacology of modulators of monoamine signalling. Swiss Med Wkly 144:w14043
Luethi D, Hoener MC, Liechti ME (2018) Effects of the new psychoactive substances diclofensine, diphenidine, and methoxphenidine on monoaminergic systems. Eur J Pharmacol 819:242–247
Wallach J, Kang H, Colestock T, Morris H, Bortolotto ZA, Collingridge GL et al (2016) Pharmacological investigations of the dissociative ‘legal highs’ diphenidine, methoxphenidine and analogues. PLoS One 11(6):e0157021
Rickli A, Luethi D, Reinisch J, Buchy D, Hoener MC, Liechti ME (2015c) Receptor interaction profiles of novel N-2-methoxybenzyl (NBOMe) derivatives of 2,5-dimethoxy-substituted phenethylamines (2C drugs). Neuropharmacology 99:546–553
Luethi D, Trachsel D, Hoener MC, Liechti ME (2018) Monoamine receptor interaction profiles of 4-thio-substituted phenethylamines (2C-T drugs). Neuropharmacology 134:141–148
Eshleman AJ, Wolfrum KM, Reed JF, Kim SO, Johnson RA, Janowsky A (2018) Neurochemical pharmacology of psychoactive substituted N-benzylphenethylamines: high potency agonists at 5-HT2A receptors. Biochem Pharmacol 158:27–34
Iversen L, Gibbons S, Treble R, Setola V, Huang XP, Roth BL (2013) Neurochemical profiles of some novel psychoactive substances. Eur J Pharmacol 700(1–3):147–151
Maier J, Mayer FP, Luethi D, Holy M, Jantsch K, Reither H et al (2018) The psychostimulant (+/−)-cis-4,4′-dimethylaminorex (4,4′-DMAR) interacts with human plasmalemmal and vesicular monoamine transporters. Neuropharmacology 138:282–291
Luethi D, Widmer R, Trachsel D, Hoener MC, Liechti ME (2019) Monoamine receptor interaction profiles of 4-aryl-substituted 2,5-dimethoxyphenethylamines (2C-BI derivatives). Eur J Pharmacol 855:103–111
Nelson DL, Lucaites VL, Wainscott DB, Glennon RA (1999) Comparisons of hallucinogenic phenylisopropylamine binding affinities at cloned human 5-HT2A, 5-HT2B and 5-HT2C receptors. Naunyn Schmiedeberg’s Arch Pharmacol 359(1):1–6
Nichols DE, Nichols CD (2008) Serotonin receptors. Chem Rev 108(5):1614–1641
Huang XP, Setola V, Yadav PN, Allen JA, Rogan SC, Hanson BJ et al (2009) Parallel functional activity profiling reveals valvulopathogens are potent 5-hydroxytryptamine2B receptor agonists: implications for drug safety assessment. Mol Pharmacol 76(4):710–722
Elangbam CS, Job LE, Zadrozny LM, Barton JC, Yoon LW, Gates LD et al (2008) 5-hydroxytryptamine (5-HT)-induced valvulopathy: compositional valvular alterations are associated with 5-HT2B receptor and 5-HT transporter transcript changes in Sprague-Dawley rats. Exp Toxicol Pathol 60(4–5):253–262
Roth BL (2007) Drugs and valvular heart disease. N Engl J Med 356(1):6–9
Wee S, Woolverton WL (2006) Self-administration of mixtures of fenfluramine and amphetamine by rhesus monkeys. Pharmacol Biochem Behav 84(2):337–343
Wee S, Anderson KG, Baumann MH, Rothman RB, Blough BE, Woolverton WL (2005) Relationship between the serotonergic activity and reinforcing effects of a series of amphetamine analogs. J Pharmacol Exp Ther 313(2):848–854
Ritz MC, Lamb RJ, Goldberg SR, Kuhar MJ (1987) Cocaine receptors on dopamine transporters are related to self-administration of cocaine. Science 237(4819):1219–1223
Kuhar MJ, Ritz MC, Boja JW (1991) The dopamine hypothesis of the reinforcing properties of cocaine. Trends Neurosci 14(7):299–302
Droogmans S, Cosyns B, D’Haenen H, Creeten E, Weytjens C, Franken PR et al (2007) Possible association between 3,4-methylenedioxymethamphetamine abuse and valvular heart disease. Am J Cardiol 100(9):1442–1445
Setola V, Hufeisen SJ, Grande-Allen KJ, Vesely I, Glennon RA, Blough B et al (2003) 3,4-Methylenedioxymethamphetamine (MDMA, “Ecstasy”) induces fenfluramine-like proliferative actions on human cardiac valvular interstitial cells in vitro. Mol Pharmacol 63(6):1223–1229
Kreth K, Kovar K, Schwab M, Zanger UM (2000) Identification of the human cytochromes P450 involved in the oxidative metabolism of “ecstasy”-related designer drugs. Biochem Pharmacol 59(12):1563–1571
Meyer MR, Peters FT, Maurer HH (2008) The role of human hepatic cytochrome P450 isozymes in the metabolism of racemic 3,4-methylenedioxy-methamphetamine and its enantiomers. Drug Metab Dispos 36(11):2345–2354
Vizeli P, Schmid Y, Prestin K, Meyer Zu Schwabedissen HE, Liechti ME (2017) Pharmacogenetics of ecstasy: CYP1A2, CYP2C19, and CYP2B6 polymorphisms moderate pharmacokinetics of MDMA in healthy subjects. Eur Neuropsychopharmacol 27(3):232–238
Schmid Y, Vizeli P, Hysek CM, Prestin K, Meyer Zu Schwabedissen HE, Liechti ME (2016) CYP2D6 function moderates the pharmacokinetics and pharmacodynamics of 3,4-methylene-dioxymethamphetamine in a controlled study in healthy individuals. Pharmacogenet Genomics 26(8):397–401
Roth BL, Choudhary MS, Khan N, Uluer AZ (1997) High-affinity agonist binding is not sufficient for agonist efficacy at 5-hydroxytryptamine2A receptors: evidence in favor of a modified ternary complex model. J Pharmacol Exp Ther 280(2):576–583
Rabin RA, Regina M, Doat M, Winter JC (2002) 5-HT2A receptor-stimulated phosphoinositide hydrolysis in the stimulus effects of hallucinogens. Pharmacol Biochem Behav 72(1–2):29–37
Luethi D, Liechti ME (2018) Monoamine transporter and receptor interaction profiles in vitro predict reported human doses of novel psychoactive stimulants and psychedelics. Int J Neuropsychopharmacol 21(10):926–931
Gelvin EP, McGavack TH (1952) 2-Amino-1-(p-methylphenyl)-propane (aptrol) as an anorexigenic agent in weight reduction. N Y State J Med 52(2):223–226
Blanckaert P, van Amsterdam J, Brunt T, van den Berg J, Van Durme F, Maudens K et al (2013) 4-Methyl-amphetamine: a health threat for recreational amphetamine users. J Psychopharmacol 27(9):817–822
Bäckberg M, Beck O, Hulten P, Rosengren-Holmberg J, Helander A (2014) Intoxications of the new psychoactive substance 5-(2-aminopropyl)indole (5-IT): a case series from the Swedish STRIDA project. Clin Toxicol 52(6):618–624
Katselou M, Papoutsis I, Nikolaou P, Spiliopoulou C, Athanaselis S (2015) 5-(2-Aminopropyl)indole: a new player in the drama of ‘legal highs’ alerts the community. Drug Alcohol Rev 34(1):51–57
Kronstrand R, Roman M, Dahlgren M, Thelander G, Wikstrom M, Druid H (2013) A cluster of deaths involving 5-(2-aminopropyl)indole (5-IT). J Anal Toxicol 37(8):542–546
Seetohul LN, Pounder DJ (2013) Four fatalities involving 5-IT. J Anal Toxicol 37(7):447–451
Titeler M, Lyon RA, Glennon RA (1988) Radioligand binding evidence implicates the brain 5-HT2 receptor as a site of action for LSD and phenylisopropylamine hallucinogens. Psychopharmacology 94(2):213–216
Glennon RA, Titeler M, McKenney JD (1984) Evidence for 5-HT2 involvement in the mechanism of action of hallucinogenic agents. Life Sci 35(25):2505–2511
Preller KH, Burt JB, Ji JL, Schleifer CH, Adkinson BD, Stampfli P et al (2018) Changes in global and thalamic brain connectivity in LSD-induced altered states of consciousness are attributable to the 5-HT2A receptor. Elife 7:e35082
Song J, Hanniford D, Doucette C, Graham E, Poole MF, Ting A et al (2005) Development of homogeneous high-affinity agonist binding assays for 5-HT2 receptor subtypes. Assay Drug Dev Technol 3(6):649–659
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Luethi, D., Liechti, M.E. (2021). Drugs of Abuse Affecting 5-HT2B Receptors. In: Maroteaux, L., Monassier, L. (eds) 5-HT2B Receptors. The Receptors, vol 35. Springer, Cham. https://doi.org/10.1007/978-3-030-55920-5_16
Download citation
DOI: https://doi.org/10.1007/978-3-030-55920-5_16
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-55919-9
Online ISBN: 978-3-030-55920-5
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)