Abstract
Animals have evolved sophisticated means to detect and defend themselves against colonization by microorganisms. Mammals differentiate self from nonself by the use of germline encoded pattern recognition receptors (PRRs) of the innate immune system in addition to pathogen-specific recognition by the adaptive immune system. Conserved microbial structures, termed microbe-associated molecular patterns (MAMPs) are recognized by the innate immune system. Pathogens succeed in subverting these immune mechanisms by the production of effector proteins and modification of MAMPs. While many PRRs and their cognate ligands have been extensively examined, most studies addressed the immune response toward the whole microorganism, isolated MAMPs, or effector proteins. Both Gram-negative and Gram-positive bacteria produce membrane vesicles that contain several MAMPs and bacterial effector proteins, and the study of the interplay of these with immune PRRs is a recently emerging field. Here we summarize key components of the innate and adaptive immune systems and discuss current knowledge regarding the immune recognition and immunomodulatory functions of bacterial membrane vesicles in mammalian hosts.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
8.1 Bacterial Membrane Vesicles
Both Gram-negative and Gram-positive bacteria produce vesicles known as outer membrane vesicles (OMVs) or membrane vesicles (MVs), respectively. They contain components derived from the parent bacterium, including proteins, lipids, and nucleic acids (reviewed in Schwechheimer and Kuehn 2015). Originally thought to be an artifact of bacterial growth, recent studies have demonstrated that OMVs and MVs may contribute to disease pathogenesis and progression due to their immunostimulatory cargo. OMVs are naturally released by bacteria as part of their normal growth. There are a number of mechanisms by which OMVs are produced and bacteria can actively increase their production (Kulp and Kuehn 2010). In contrast to OMVs, the mechanisms of MV biogenesis are not well characterized. This is because Gram-negative OMVs were discovered long before Gram-positive MVs, and consequently we have a greater understanding of OMV production, composition, and their effects on the host. Although research has been focused on examining the immunostimulatory effects of OMVs derived from pathogens, recent studies have begun investigating the role of OMVs from commensal bacteria in modulating the hosts immune response. In contrast, due to their more recent discovery, limited studies have examined the immunostimulatory effects of Gram-positive MVs on the host.
A number of studies have suggested that OMV production may be increased during the course of infection; however, the mechanisms behind OMV biogenesis during infection have not been completely elucidated. It has been identified that the disruption of genes encoding for outer membrane proteins and peptidoglycan synthesis can lead to changes in OMV production (McBroom et al. 2006). OMV production is also thought to be a response to stress stimuli such as antibiotic treatment, envelope stress, and increase in temperature (Baumgarten et al. 2012; Kadurugamuwa and Beveridge 1995; Macdonald and Kuehn 2013; McBroom and Kuehn 2007; Yun et al. 2018). Moreover, the immunogenicity of OMV cargo can be altered by certain bacteria, such as Vibrio cholerae, in response to changes in the expression of virulence factors upon quorum sensing (Bielig et al. 2011). Therefore, it is thought that during infection, factors such as environmental stress, bacterial regulators, and host immune molecules contribute to increased production of bacterial OMVs. Collectively, this increased production of OMVs and their composition of immunogenic cargo is thought to contribute to pathogenesis.
8.1.1 Bacterial Membrane Vesicles Contain Immunogenic Cargo
Numerous studies have demonstrated the pro-inflammatory nature of Gram-negative OMVs, their ability to stimulate the immune system, and their use as vaccines for humans (Holst et al. 2009; Kaparakis-Liaskos and Ferrero 2015; Manning and Kuehn 2011; Ellis and Kuehn 2010; Pathirana and Kaparakis-Liaskos 2016). OMVs have been observed in a number of samples from human patients and tissue biopsies. For example, OMVs from Neisseria meningitidis were observed using electron microscopy in the cerebrospinal fluid of an infected infant, and in samples from a patient with fatal meningococcal disease (Stephens et al. 1982; Namork and Brandtzaeg 2002). Additionally, OMVs from Helicobacter pylori have been found in gastric biopsies from infected individuals and in cultures from several clinical patient samples (Fiocca et al. 1999; Keenan et al. 2000). OMVs have also been observed in samples from the sinus of a child infected with Moraxella catarrhalis (Vidakovics et al. 2010), and in the lungs of patients with nontypeable Haemophilus influenza infections (Ren et al. 2012). In addition to their presence during infection, a number of studies have revealed that OMVs contain specific microbe-associated molecular patterns (MAMPs), known to stimulate the immune system, such as lipopolysaccharide (LPS), peptidoglycan (PG), nucleic acids, as well as other bacterial cell wall components (Vanaja et al. 2016; Chatterjee and Das 1967; Renelli et al. 2004; Choi et al. 2011).
In addition to their ability to carry immunostimulatory cargo, OMVs have been shown to be important in the structure and function of biofilms, in the environment as well as during the course of infection (Schooling and Beveridge 2006; Yonezawa et al. 2009). Additionally, they are able to act as bacteriophage and antibiotic decoys and can “trap” complement proteins produced by the host immune system (reviewed in Manning and Kuehn 2011; Tan et al. 2007). Because of this, it is thought that OMVs may be harnessed by bacteria to further establish colonization and pathogenesis within the host.
Conversely, the biogenesis, contents and immunostimulatory ability of Gram-positive MVs is not well characterized. Some studies have reported that Gram-positive MVs contain immunogenic cargo (Lee et al. 2009; Gurung et al. 2011; Peschel et al. 2001; Rivera et al. 2010); however, further studies are required to elucidate their immunogenic profiles and interactions with the host immune system. Chapter 3 contains a more detailed review of the biogenesis and functions of Gram-positive MVs.
The contribution of bacterial OMVs and MVs to pathogenesis and immunity is quickly becoming apparent as more studies uncover their roles as a novel transport system for bacterial derived molecules. Here we discuss the various mechanisms by which OMVs are able to interact with the host’s innate and adaptive immune system, their contributions to pathogenesis, as well as the recent discovery of immunogenic Gram-positive MVs.
8.2 Bacterial Membrane Vesicles Interact with and Modulate the Hosts Innate Immune System
In order to survive within a human host, microorganisms must circumvent host immune defenses. All multicellular organisms have developed innate defense mechanisms which have the capacity to be activated by foreign microorganisms and that function to defend the host by destroying pathogens and neutralizing their virulence factors (Medzhitov and Janeway 1997). One of the major mechanisms by which bacteria are able to interact with host cells is by the secretion of immunostimulatory products (Young et al. 1999; Bruno et al. 2009). Bacterial membrane vesicles are released from both Gram-negative and Gram-positive bacteria and act as secretory transporters for proteins, lipids, and other bacterial products to host cells (reviewed in Ellis and Kuehn 2010). The innate immune system is the first line of defense against invading and resident bacteria, and it is able to rapidly detect and initiate an immune response to bacteria membrane vesicles. In humans, the immune system is comprised of innate and adaptive immunity. The innate immune system is the frontline defense against bacteria, whereas adaptive immunity functions to develop pathogenic-specific immune responses while generating long-lived immunity.
8.2.1 OMVs Protect Bacteria Against Host Innate Immune Molecules
The hosts innate immune system is multifaceted in its ability to respond to pathogens and is composed of a range of defense mechanisms which include innate immune receptors, innate immune cells, and the production of antimicrobials and inflammatory molecules. For example, pathogens can trigger the activation of the complement system, a group of small proteins made by hepatocytes which circulate in the bloodstream. The complement system enhances the ability of antibodies and phagocytic cells to clear microbes, in addition to damaging bacteria by attacking their cell membrane (Rus et al. 2005). Although part of the innate immune system, complement can also regulate aspects of the adaptive immune system by recruiting and activating immune cells using anaphylatoxins, small peptide mediators (Barrington et al. 2001).
Pathogens are often able to inhibit activation of the complement system; however, the mechanisms by which this can occur have not been entirely elucidated (Joiner 1988). It has been shown that Porphyromonas gingivalis OMVs can degrade complement components such as the complement 5a (C5a) cluster of differentiation 88 receptor (CD88) (Jagels et al. 1996) and CD14 from the surface of human macrophage cells. CD88 and CD14 are both involved in the recognition of bacteria (Duncan et al. 2004) and their targeting leads to reduced efficacy of immune responses and allows bacteria to evade the immune system. Similarly, Haemophilus influenzae can survive complement-mediated attacks when supplemented with M. catarrhalis OMVs, further potentiating a mutually beneficial role for invading pathogens and their OMVs (Tan et al. 2007).
Moreover, the innate immune system also employs antimicrobial peptides (AMPs), such as defensins, as another defense mechanism against invading pathogens. AMPs can directly attack invading microbes to limit pathogenesis; however, resistance to AMPs has been observed for a number of pathogens, including Staphylococcus aureus (Peschel et al. 2001), Salmonella enterica serovar Typhimurium (S. Typhimurium) (Gunn et al. 2000), Listeria monocytogenes (Abachin et al. 2002), and Pseudomonas aeruginosa (Moskowitz et al. 2004). OMVs have been demonstrated to contribute to AMP resistance, as V. cholerae OMVs were shown to protect other bacteria from membrane attack by AMPs (Duperthuy et al. 2013). This was proposed to be a more general mechanism of immune evasion, where OMVs can function to sequester host immune molecules (Band and Weiss 2015). Moreover, the host limits the availability of transition metals by siderophores, such as calprotectin, to restrict pathogen growth, referred to as “nutritional immunity” (Hood and Skaar 2012).
8.2.2 Recognition of Bacterial Membrane Vesicles by Host Pattern Recognition Receptors Results in a Pro-Inflammatory Response
An integral feature of the innate immune system involves a number of specific pattern recognition receptors (PRRs), which recognize MAMPs and subsequently results in the generation of a pro-inflammatory innate immune response (Janeway and Medzhitov 2002). MAMPs are conserved microbial structures such as bacterial nucleic acids and bacterial cell wall components including LPS and PG, which are distinguishable from host molecules (Boller and Felix 2009). PRRs are protein receptors expressed by a number of innate immune cells such as neutrophils, macrophages, and dendritic cells (DCs) (Thomas and Schroder 2013; Takeuchi and Akira 2010) as well as non-immune cells, such as epithelial cells (Kawai and Akira 2010). Once PRRs are activated by detection of their respective MAMP ligand, a signaling cascade initiates the release of inflammatory mediators such as cytokines and chemokines which are responsible for the recruitment and the activation of immune cells and for mediating an inflammatory response (Kawai and Akira 2010). PRRs are vital for the recognition of, and downstream effects initiated by invading bacteria.
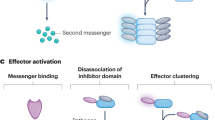
PRRs include Toll-like receptors (TLRs) which are membrane bound (Fig. 8.1), intracellular nucleotide-binding oligomerization domain (NOD)-like receptors (NLRs) (Fig. 8.1), retinoic acid inducible gene-I (RIG-I)-like receptors (RLRs) and C-type lectins, which can be either soluble or function as membrane associated receptors (Kawai and Akira 2008; Kanneganti et al. 2007). TLRs and NLRs are activated upon recognition of MAMPs, such as components of the bacterial cell wall or microbial DNA (Fig. 8.1). RIG-I-like receptors are responsible for the recognition of virally derived dsRNA within the cytoplasm (Wells et al. 2011), and C-type lectins contribute to innate immune responses to many pathogens (reviewed in Robinson et al. 2006). Activation of PRRs leads to a number of outcomes, namely the induction of signaling pathways resulting in the transcription of pro-inflammatory cytokines that drive inflammation, in an effort to combat the invading pathogen (Fig. 8.1). Bacterial membrane vesicles can activate these signaling pathways in a number of ways, which will be discussed below.
Bacterial products are detected by TLRs and NLRs by the host cell. On the surface of the host cell, TLR5 detects flagellin, TLR2 and TLR1/6 detect bacterial cell wall components and TLR4 detects LPS. Within the cytoplasm, caspase-11 detects LPS, and NOD1 and NOD2 detect peptidoglycan subunits iE-DAP and MDP, respectively. Endosome-bound TLR9 detects bacterial DNA. Detection of bacterial MAMPs leads to the recruitment of adaptor proteins, downstream activation of transcription factors and subsequent production of pro-inflammatory chemokines and cytokines or pyroptotic cell death in the case of caspase-11 activation. Type I IFN production can also occur in response to the detection of bacteria or bacterial products, via the JAK/STAT pathway
8.2.2.1 Recognition of Bacteria by Toll-like Receptors
Toll-like receptors (TLRs) are a family of transmembrane proteins expressed by both leukocytes and non-immune cells, such as epithelial and endothelial cells. They contain an extracellular leucine-rich repeat (LRR) domain that is necessary for the detection of MAMPs, a transmembrane domain and a cytoplasmic tail (Toll/interleukin-1 receptor (TIR) domain). TLRs can be found on the cell surface or on intracellular endosomal membranes. To date, 10 members of the TLR family have been identified in humans (Akira and Takeda 2004). TLRs are capable of detecting a range of molecules derived from bacteria, viruses, and fungi. Importantly, TLRs detect molecules such as LPS, PG, and nucleic acids from both Gram-positive and Gram-negative bacteria (Fig. 8.1).
Upon detection of MAMPs, most TLRs form either homodimers or heterodimers (Fig. 8.1). Once activated, adaptor molecules are recruited to TLRs to initiate downstream signaling. TLR2, TLR4, TLR5, and TLR1/6 signal via the adaptor proteins Myeloid Differentiation Primary Response Gene 88 (MyD88) and TIR-Domain-Containing Adaptor Protein (TIRAP). This leads to the activation of IL-1 Receptor-Associated Kinases (IRAKs) and the adaptor molecules TNF Receptor-Associated Factor 6 (TRAF6) and eventually the nuclear translocation of transcription factors Nuclear Factor Kappa B (NF-ĸB) and Activator Protein 1 (AP-1). TLR9 also uses this pathway; however, it is located on the endosomal membrane (Fig. 8.1). Both NF-ĸB and AP-1 have functions in the expression of pro-inflammatory cytokines (Fig. 8.1). As a result of NF-ĸB and AP-1 activation, cytokines and chemokines are produced, for example interleukin-6 (IL-6), IL-8 (CXCL8) and Tumor Necrosis Factor Alpha (TNF/TNFα).
Additionally, TLR4 can signal independently of MyD88, via TIR-Domain-Containing Adaptor Inducing Interferon-β (TRIF) and TRIF-related adaptor molecule (TRAM) (Fig. 8.1). This leads to the activation of adaptor molecules, such as Receptor-Interacting Protein 1 (RIP1), and the translocation of NF-ĸB and AP-1 or Interferon Regulatory Factor-3 (IRF3) to the nucleus. IRF3 is a transcription factor which induces the production of type 1 interferons (Fig. 8.1, Kumar et al. 2009). Type I IFNs can signal in a paracrine or autocrine manner by interacting with Interferon Alpha/Beta Receptor (IFNAR) on the cell surface, and signal using the Janus Kinases and Signal Transducer and Activation of Transcription Proteins (JAK/STAT) pathway (Fig. 8.1, Akira and Takeda 2004). Type 1 interferons have been demonstrated to limit bacterial infections by upregulating the production of host defense molecules (reviewed in Boxx and Cheng 2016). Therefore, membrane-bound TLRs are collectively important receptors of bacteria and bacterial products. In addition, intracellular receptors from other protein families are also vital in the host response to internalized MAMPs, as discussed below.
8.2.2.2 Recognition of Bacteria by Cytoplasmic Innate Immune Receptors
In the cytoplasm of the host cell, a large family of PRRs known as NOD-like receptors (NLRs) are expressed. They are characterized by the presence of a central conserved NTPase (NACHT) domain, required for nucleotide binding and self-oligomerization (Inohara et al. 2000). These proteins generally contain a variable N-terminal effector-binding domain, which is responsible for protein–protein interactions, as well as C-terminal LRRs to detect MAMPs (Inohara and Nunez 2001). NOD1 and NOD2 are cytoplasmic receptors that recognize bacterial peptidoglycan (PG). NOD1 recognizes γ-D-Glu-mDAP (iE-DAP), a dipeptide present in the PG of almost all Gram-negative and some Gram-positive bacteria. NOD2 recognizes muramyl dipeptide (MDP) which is common to PG of all bacteria (Girardin et al. 2003a, b).
Activation of either NOD1 or NOD2 leads to the recruitment of Receptor-Interacting Serine/Threonine-Protein Kinase 2 (RIP2, RIPK2) by their CARD domain, the activation of NF-ĸB (Inohara et al. 2000) and the production of pro-inflammatory cytokines and chemokines (Fig. 8.1). Other NLRs, such as those from the NLR-pyrin domain containing (NLRP) subfamily are namely responsible for the formation of “platforms,” known as inflammasomes, in response to host signals, which contribute to inflammation (Elliott and Sutterwala 2015). NLRP3, for example, can be triggered by caspase-11 activation by cytoplasmic LPS (Shi et al. 2014), cell membrane damage, and extracellular ATP released by damaged cells (Fig. 8.1, Martinon et al. 2002). Activation of these inflammasome forming NLRs leads to the recruitment of the adaptor Apoptosis-Associated Speck-Like Protein Containing a CARD (ASC) that links NLRP3 to caspase-1 (Fig. 8.1). This complex, termed inflammasome, triggers caspase-1 activation, resulting in the production and release of the key inflammatory mediators IL-1β and IL-18, and leads to pyroptotic cell death (Schroder et al. 2010).
The activation of PRRs is a pivotal prerequisite to prime the adaptive immune system and to induce antigen-specific responses to bacterial pathogens (Fritz et al. 2007). As a result, TLRs and NLRs are key regulators of the innate immune response (Milward et al. 2007; Faure et al. 2000). Collectively, there are a range of mechanisms by which bacteria can interact with host PRRs to trigger TLR and NLR signaling to mediate a pro-inflammatory response.
8.2.2.3 Bacterial Membrane Vesicles Are Detected by Host Pattern Recognition Receptors Resulting in the Induction of an Innate Immune Response
The mucosal epithelial cell surface is the first line of defense in the host, and often the location where bacterial vesicles first come into contact with the host. The gut epithelium and the underlying lamina propria contains a diverse subset of innate and adaptive immune cells within the gut-associated lymphoid tissue (GALT). Long seen as a classical barrier, we now know that the intestinal epithelium is actively involved in immune regulation (Rhee et al. 2004). Epithelial cells express PRRs and can detect pathogens and respond to cytokines, such as IL-22, to produce antimicrobial peptides to control the microbiota composition and to secrete cytokines that recruit immune cells (Peterson and Artis 2014). The mucosal epithelial cell surface has evolved to cope with the constant presence of microbial products and foreign antigens without inducing inflammation. Indeed, the presence of microbiota and their derived MAMPs are needed for the development of the GALT and to maintain tissue homeostasis (Stappenbeck et al. 2002). A wealth of current work aims to delineate how the host can mediate tolerance of commensals at the mucosal surface, while still being able to detect and respond toward bacterial pathogens. We still know little about the microbial substances and molecular details that mediate these responses, and the role of OMVs and MVs in these processes remains largely elusive. It has been demonstrated that the interaction of OMVs with host epithelial cells results in the production of cytokines and chemokines. Therefore, OMVs and MVs are thought to be a mechanism whereby bacteria can transport their products to non-phagocytic cells at the mucosal surface in order to modulate innate and adaptive immune responses which will be discussed below.
8.2.2.4 Gram-Negative OMVs Are Detected by PRRs Expressed by Epithelial Cells
A number of in vitro studies using human epithelial cells have reported the production of chemokines and cytokines in response to stimulation by bacterial OMVs. H. pylori is a gastric pathogen, which produces OMVs demonstrated to modulate the proliferation of, and IL-8 production by gastric adenocarcinoma cells (Ismail et al. 2003). This was the first study to indicate that OMVs could induce pro-inflammatory cytokine production by human epithelial cells. Further investigation revealed that the production of IL-8, stimulated by H. pylori OMVs was dependent on detection of their peptidoglycan cargo by the intracellular NOD1 receptor (Fig. 8.2, Kaparakis et al. 2010). Similarly, OMVs from the pathogen V. cholerae were found to induce the production of IL-8 and granulocyte-macrophage colony-stimulating factor (GM-CSF) in a NOD1-dependent manner (Fig. 8.2, Chatterjee and Chaudhuri 2013; Bielig et al. 2011). NOD2 is able to detect PG from both Gram-positive and Gram-negative membrane vesicles, and has been shown to induce a pro-inflammatory immune response upon the detection of OMVs, such is the case for the pathogen Aggregatibacter actinomycetemcomitans (Fig. 8.2, Thay et al. 2014). In addition, OMVs from the Gram-negative pathogen Legionella pneumophila were found to induce the production of a number of chemokines and cytokines by human alveolar epithelial cells (Galka et al. 2008). OMVs from periodontal pathogens have also been implicated in the progression of disease by interaction with epithelial cells, similarly to the studies discussed above (Cecil et al. 2019).
Bacterial membrane vesicles interact with PRRs on the surface and cytoplasm of host cells to initiate an innate immune response. OMVs produced by E. coli, V. cholerae, and H. pylori, for example, can interact with TLR4, TLR2, and TLR1/6 on the surface of the cell. OMVs produced by H. pylori and A. actinomycetemcomitans can interact with NOD1 and NOD2, respectively. The activation of these PRRs results in the induction of an intracellular signaling cascade that ultimately results in the production of pro-inflammatory cytokines and chemokines
Opportunistic pathogens can utilize OMVs as a virulence factor when establishing disease. P. aeruginosa produces OMVs which can stimulate IL-8 production by primary human bronchial epithelial cells (Bauman and Kuehn 2006). OMVs from the opportunistic pathogen, A. baumannii were also found to upregulate the production of a number of cytokines and chemokines by human epi thelial cells (Jun et al. 2013).
Lastly, OMVs derived from the commensal Gram-negative bacterium Bacteroides fragilis have been shown to modify the expression of TLR2 and TLR4 in epithelial cells, in addition to increasing the expression of anti-inflammatory cytokines (Ahmadi Badi et al. 2019). OMVs from commensal and probiotic E. coli can interact with epithelial cells and activate NOD1, leading to the release of the pro-inflammatory cytokines IL-6 and IL-8 (Fig. 8.2, Canas et al. 2016). Collectively, these studies demonstrate the complex role Gram-negative OMVs play at the epithelium in immune tolerance, and conversely, in the initiation of an innate immune response by pathogens.
8.2.2.5 Gram-Positive MVs Interact with Host Epithelial Cells
Conversely, a limited number of studies have demonstrated the immunogenic ability of Gram-positive MVs. A proteomic study examining MVs produced by S. aureus found that they are enriched in penicillin-binding proteins which contribute to antibiotic resistance as well as proteins which have pathological functions during infection (Lee et al. 2009). Later, it was demonstrated that S. aureus MVs can induce inflammation in dermal fibroblasts, but not human epithelial cells, suggesting a potential role for MVs in mediating inflammation during atopic dermatitis (Jun et al. 2017). Another study found that MVs from S. aureus were able to enter and induce host cell death in the human epithelial cell line (HEp-2) (Gurung et al. 2011).
In addition to epithelial cells, MVs are thought to interact with various other cell types throughout the host, both immune and non-immune. Overall, bacterial membrane vesicles are known to interact with epithelial cells and are thought to disseminate throughout the host to interact with cells, such as macrophages, neutrophils, and DCs, distal to the site of infection.
8.3 Bacterial Membrane Vesicles Adhere to, Fuse and Enter Host Cells to Mediate a Pro-Inflammatory Response
OMVs have been identified in a diverse range of host tissues, signifying their ability to travel and exist in a range of environments in the host. In addition to interacting with host surface PRRs, OMVs have been shown to adhere, fuse with, and enter host cells in order to contribute to inflammation, pro-inflammatory immune response, and mediate pathogenesis (Fig. 8.3, Bomberger et al. 2009; Furuta et al. 2009; Kaparakis et al. 2010). Early studies demonstrated the ability of OMVs to fuse with host cells and subsequently release their contents into the cytoplasm (Kadurugamuwa and Beveridge 1998). More recent studies confirmed these findings, and additional examples of OMV uptake into host cells were identified.
Bacterial membrane vesicles interact with epithelial cells via a range of different mechanisms to mediate pathogenesis in the host. OMVs and MVs enter host cells via lipid rafts. OMVs can enter cells in a lipid-raft independent manner, via caveolin- or clathrin-mediated endocytosis, macropinocytosis, or by TLR-mediated endocytosis. Adherence and entry into host cells results in the production of pro-inflammatory cytokines and the recruitment of inflammatory innate immune cells. Within epithelial cells, OMVs can be degraded by autophagy. These processes, as well as the delivery of cytotoxic molecules by OMVs to the host cell can initiate the disruption of the epithelial cell layer, allowing OMVs to enter the submucosa
8.3.1 Lipid Raft-Dependent Entry of OMVs and MVs into Epithelial Cells
The most commonly observed mechanism of entry for bacterial OMVs into non-phagocytic host cells involves cholesterol-rich lipid rafts (Fig. 8.3). This has been demonstrated for entry of OMVs produced by Gram-negative pathogens such as enterotoxigenic E. coli, Campylobacter jejuni, H. pylori, H. influenzae, P. aeruginosa, and P. gingivalis (Bauman and Kuehn 2009; Sharpe et al. 2011; Kaparakis et al. 2010; Kesty et al. 2004; Elmi et al. 2012; Furuta et al. 2009; Bomberger et al. 2009). Although not well-characterized, MVs are also thought to enter host cells via cholesterol-rich lipid rafts (Gurung et al. 2011; Thay et al. 2013).
8.3.2 Lipid Raft-Independent Mechanisms of OMV Entry into Epithelial Cells
OMVs have also been shown to enter host cells by mechanisms which are independent of lipid rafts (Parker et al. 2010). Clathrin-mediated endocytosis of bacterial OMVs into host cells can be triggered by receptor-mediated binding of ligands at the cell surface and subsequent internalization (Fig. 8.3) (reviewed in O’Donoghue and Krachler 2016). The internalization of clathrin-coated pits leads to degradation of the material contained within these endocytic vacuoles (Rewatkar et al. 2015). Several studies have identified OMV entry into host epithelial cells via clathrin-mediated endocytosis, including OMVs produced by H. pylori (Olofsson et al. 2014). However, other studies have demonstrated that inhibition of clathrin-mediated endocytosis did not abolish, but only reduced the entry of H. pylori OMVs into host epithelial cells implying there are several mechanisms of entry into host cells (Parker et al. 2010). Caveolin-mediated endocytosis has also been implicated in the uptake of bacterial OMVs into host cells (Fig. 8.3, reviewed in O’Donoghue and Krachler 2016). Another suggested mechanism of OMV entry into host cells is by macropinocytosis; however, this is not thought to be a deliberate process (Fig. 8.3, Lim and Gleeson 2011). OMVs produced by P. aeruginosa have been shown to enter airway epithelial cells by macropinocytosis (Bomberger et al. 2009). Furthermore, it has recently been shown that OMV size can regulate their mechanism of entry into host cells, as H. pylori OMVs utilized distinct mechanisms of endocytosis or micropinocytosis to enter host cells based on their size (Turner et al. 2018). Collectively, these studies show that OMVs can utilize a range of mechanisms to enter host cells, and their mechanism of entry may be regulated based on receptor-mediated entry, OMV size or their content.
8.3.3 Detection and Degradation of Intracellular OMVs by Epithelial Cells
Until recently, the intracellular fate of OMVs following their entry into host cells remained unknown. It was identified that upon entry into host epithelial cells, H. pylori and P. aeruginosa OMVs were detected by the innate immune receptor NOD1, resulting in the induction of an inflammatory response (Kaparakis et al. 2010). This finding was further supported by subsequent studies showing the ability of V. cholerae OMVs to be detected by NOD1 and NOD2 which resulted in NF-ĸB activation and the production of pro-inflammatory cytokines (Chatterjee and Chaudhuri 2013; Bielig et al. 2011). It was later shown that NOD1 was essential for the degradation of intracellular OMVs in host epithelial cells, as internalized OMVs were degraded via the host cellular degradation pathway of autophagy in a NOD1-dependent manner (Fig. 8.3, Irving et al. 2014). Specifically, the detection of PG contained within H. pylori and P. aeruginosa OMVs by the immune receptor NOD1, resulted in their degradation via autophagy (Fig. 8.3, Irving et al. 2014). Therefore, despite OMVs having a range of mechanisms to enter host cells, they can rapidly be degraded once intracellular via the host degradation pathway of autophagy.
Alternatively, bacterial OMVs are not only restricted to interacting with the mucosal cell surface or being internalized by host epithelial cells, as they are capable of disrupting and passing the epithelial cell layer entirely (Fig. 8.3). This has been demonstrated in studies using OMVs from Treponema denticola which can disrupt intact epithelium as a means to further mediate pathogenesis in the host (Chi et al. 2003), discussed further below.
8.4 Bacterial Membrane Vesicles Are Cytotoxic and Disrupt the Epithelial Cell Barrier
A significant aspect of pathogenesis is the invasion of bacteria or their products into the host tissue. Bacterial membrane vesicles have a range of mechanisms whereby they can function to destroy the epithelial cell barrier integrity and promote cell death to ultimately create damage and promote disease in the host. These mechanisms involve disruption of the epithelial cell barrier and having cytotoxic activities.
8.4.1 OMVs Are Cytotoxic to Host Cells
OMVs have been shown to disrupt the epithelial cell layer, enabling further penetration of bacteria and their products (Fig. 8.3). This has been observed for OMVs including those derived from enterobacteria such as E. coli (Wai et al. 2003; Kouokam et al. 2006), and the dental pathogens T. denticola and P. gingivalis (Chi et al. 2003; Nakao et al. 2014). Once OMVs disrupt the integrity of the epithelial cell layer and gain access to the submucosa, they can interact directly with immune cells and stimulate an inflammatory response (Fig. 8.3, Nakao et al. 2014).
In addition to the disruption of the epithelium, OMVs can interrupt division of epithelial cells and induce death of innate immune cells, such as macrophages, neutrophils, and DCs. For example, Acinetobacter baumannii was shown to deliver cytotoxic OMVs to macrophages (Jin et al. 2011), and OMVs derived from Actinobacillus actinomycetemcomitans contained leukotoxins which could kill neutrophil-like cells in vitro (Kato et al. 2002). Moreover, C. jejuni OMVs contained cytolethal distending toxin, which disrupted the epithelial cell layer by interrupting cell division (Fig. 8.3, Lindmark et al. 2009).
Antibiotic treatment and stress of bacterial cells has widely been demonstrated to affect the production of OMVs; however, only a few studies have addressed the potential downstream immunostimulatory functions of these OMVs. One study demonstrated that A. baumannii produced twofold more OMVs when treated with antibiotics, and these OMVs had an altered proteome compared to control OMVs. When stimulated with OMVs obtained from cells treated with antibiotic, human lung carcinoma cells underwent severe apoptotic cell death, which is suggested to be attributable to the differential expression of OMV proteins in the presence of antibiotic stress (Yun et al. 2018). Collectively, these studies highlight the cytotoxic potential of OMVs on host cells, and the ability of bacteria to modify the cytotoxic abilities of OMVs during conditions of antibiotic stress, to ultimately mediate pathogenesis in the host.
8.4.2 MVs Are Cytotoxic to Host Cells
Gram-positive MVs have been shown to also have cytotoxic effects on host cells. MVs produced by S. aureus have been shown to deliver the α-haemolysin toxin to host cells, inducing cell death (Thay et al. 2013). However, not all MVs of the same genus are cytotoxic or pathogenic, highlighting that these MVs may have different functions in vivo. For example, analysis of MVs from the Gram-positive resident skin bacterium, Staphylococcus haemolyticus, revealed an enrichment of proteins involved in the acquisition of iron by MVs from both commensal and pathogenic S. haemolyticus (Cavanagh et al. 2018). However, MVs from a clinical isolate of a coagulase-negative staphylococci strain were enriched in proteins involved in antimicrobial resistance, such as β-lactamase and other virulence factors when compared to MVs isolated from a commensal S. haemolyticus strain (Cavanagh et al. 2018). This suggests that bacteria from the same genus can produce MVs which differ in functions within the host. Therefore, it should be noted that MVs produced by a number of commensal and probiotic strains are not cytotoxic to host epithelial cells (Canas et al. 2016; Shen et al. 2012). This further demonstrates the dichotomy between MVs produced by commensal and pathogenic microbes and their role in host immunity and pathogenesis, and suggests that bacterial vesicles have a range of functions in the host.
8.5 Bacterial Membrane Vesicles Interact with Host Innate Immune Cells
In addition to their interactions with epithelial cells and cytotoxic abilities, bacterial OMVs have been shown to induce inflammatory responses in innate immune cells such as macrophages, DCs, and neutrophils, which are phagocytic cells responsible for detecting and responding to pathogens. These cells express PRRs, including TLRs and NLRs at high levels (Kawai and Akira 2010). Due to their immunostimulatory abilities, OMVs are thought to interact directly with immune cells within the host and the mechanisms by which they interact with host immune cells are discussed below.
8.5.1 OMVs Interact with Macrophages
A number of studies have examined the effects of OMVs on innate immune cells such as macrophages. Analysis of macrophages from the lung tissue of patients infected with L. pneumophila revealed OMVs within the cytoplasm, suggesting that OMVs directly interact with macrophages in vivo (Jager et al. 2014). Another intracellular pathogen, S. Typhimurium, is able to penetrate and divide within innate immune cells. One study investigated the release of OMVs from S. Typhimurium within macrophages, and showed that OMVs containing virulence proteins were transported to the macrophage cytoplasm from within the Salmonella-containing vacuole (Yoon et al. 2011). Additionally, OMVs from S. Typhimurium could activate DCs and macrophages and stimulate their expression of a number of inflammatory molecules, including TNFα and IL-12 (Alaniz et al. 2007).
OMVs produced by the oral pathogen P. gingivalis are thought to contribute to atherosclerosis by inducing lipid droplet accumulation in macrophages (Qi et al. 2003). P. gingivalis OMVs have also been shown to induce the production of nitric oxide and the expression of inducible nitric oxide synthase by mouse macrophages to exacerbate disease (Imayoshi et al. 2011). Additionally, following treatment with P. gingivalis OMVs, macrophages were shown to have reduced CD14 on their surface (Duncan et al. 2004). CD14 is a co-receptor involved in TLR4-mediated recognition of LPS, and therefore loss of CD14 results in a reduced immune response to secondary E. coli LPS stimulation. These OMVs also suppressed TNFα production, further illustrating the effects of OMVs on immune cells (Duncan et al. 2004). Although detected by membrane-bound TLR4, cytoplasmic LPS can also activate the intracellular sensor caspase-11 in mice and caspase-4/5 in human, resulting in the release of IL-1β and pyroptotic cell death. A recent study reported the ability of E. coli OMV-associated LPS to enter the cytosol of host macrophages resulting in caspase-11 activation (Fig. 8.2, Gu et al. 2019). The transport of OMV-associated LPS into the cytosol of macrophages required TLR4 activation and occurred in a TIR domain-containing adaptor-inducing interferon-β (TRIF)-dependent manner (Fig. 8.2, Gu et al. 2019).
Similarly, P. aeruginosa OMVs have been shown to upregulate the production of inflammatory cytokines such as macrophage inflammatory protein-2 (MIP-2), TNFα and IL-6 in mouse macrophages (Ellis et al. 2010). H. pylori OMVs have also been shown to promote IL-6 production by human peripheral blood mononuclear cells (Winter et al. 2014) and Salmonella spp. OMVs induced production of TNF and nitric oxide by mouse macrophages (Alaniz et al. 2007).
N. meningitidis OMVs have also been shown to induce cytokines and chemokines such as CC-chemokine ligand 2 (CCL2), CCL3, CCL5, CXCL8 (IL-8), IL-1β, IL-6, IL-10, IL-12p40, IL-12p70, and TNF production in monocytes and macrophages (Tavano et al. 2009). These OMVs also induced the production of monocyte-derived thrombotic factors such as tissue factor and plasminogen activator inhibitor 2. These molecules facilitate intravascular coagulation, microthrombosis, and organ dysfunction which is observed during septicemia caused by this bacterium (Tavano et al. 2009). Additionally, this study revealed that N. meningitidis OMVs can activate macrophages to induce adaptive immune responses by the upregulation of co-stimulatory molecules HLA-DR, CD80, and CD86, and intracellular adhesion molecule 1 (ICAM1) (Tavano et al. 2009).
8.5.1.1 Anti-Inflammatory Effects of OMVs on Host Macrophages
Despite a number of pro-inflammatory properties, OMVs can also have anti-inflammatory effects on macrophage precursor cells, known as monocytes. Neisseria gonorrhoeae, the causative agent of gonorrhea in humans, has been shown to release OMVs within the mucosa that contain PorB. PorB is a protein which targets the macrophage mitochondrial membrane resulting in host cell death, thus downregulating the innate immune response to the pathogen (Deo et al. 2018). Moreover, H. pylori OMVs induce the production of anti-inflammatory IL-10 by human peripheral blood mononuclear cells to limit inflammation and bacterial clearance, facilitating persistence of the pathogen (Winter et al. 2014). Similarly, Brucella abortus OMVs inhibit TLR2, TLR4, and TLR5 responses, limit IFNγ-induced major histocompatibility complex (MHC) class II expression, and promote the internalization of B. abortus bacteria by monocytes in an effort to enhance pathogenesis (Pollak et al. 2012). Overall, OMVs have been shown to interact with different cell types, such as macrophages and monocytes to result in pro- or anti-inflammatory responses; however, this has not been demonstrated as widely for Gram-positive MVs.
8.5.2 OMVs and MVs Interact with Neutrophils
Similar to macrophages, neutrophil responses can be modulated by bacterial OMVs in different ways. When stimulated with OMVs derived from N. meningitidis, human neutrophils produced TNFα and IL-1β and exhibited upregulation of IL-8, CCL3, and CCL4 expression (Lapinet et al. 2000). Likewise, OMVs from uropathogenic E. coli which contained a toxin, cytotoxic necrotizing factor type 1, impaired the phagocytic and chemotactic abilities of neutrophils (Davis et al. 2006). Additionally, E. coli OMVs were recently demonstrated to effectively recruit neutrophils into the lung by stimulating the release of IL-8 in TLR4-dependent and NF-ĸB manners (Fig. 8.3, Lee et al. 2018).
During cell death, neutrophils produce neutrophil extracellular traps (NETs) which contain antimicrobial peptides, DNA, and histones. NETs are fibrous in structure to assist in trapping and killing pathogens (Brinkmann et al. 2004). OMVs produced by N. meningitidis and Histophilus somni induced neutrophil cell death and NET formation resulting in the killing of these pathogens. Although N. meningitidis OMVs induced NET formation, they also facilitated pathogen colonization and may be a contributing factor to the substantial amount of OMVs in patients with meningococcal disease (Lappann et al. 2013).
More recently, Gram-positive S. aureus MVs were also shown to activate neutrophils and induce an immune response. These MVs induced NET formation and neutrophil cell death. Moreover, mice immunized with MVs had increased production of antibodies such as immunoglobulin M (IgM) and total IgG, and were protected against subsequent S. aureus challenge (Askarian et al. 2018). Collectively, these studies reveal the multiple mechanisms whereby bacterial membrane vesicles interact with neutrophils to ultimately facilitate the onset of pathogenesis in the host.
8.5.3 OMVs Induce DC Maturation
In addition to their interactions with other immune cells, OMVs from pathogens induce the maturation of DCs, which is important for antigen presentation and adaptive immunity. DC maturation is characterized by their upregulation of MHC class II and production of pro-inflammatory cytokines and chemokines (Inaba et al. 1990). N. meningitidis OMVs facilitate their own delivery and internalization into DCs (Schultz et al. 2007), and are known to induce DC maturation, as characterized by the upregulation of MHC class II and co-stimulatory molecules, and their production of pro-inflammatory cytokines and chemokines (Durand et al. 2009). Similarly, Salmonella spp. OMVs induced the expression of CD86 and MHC class II on DCs, and their production of TNF and IL-12, as well as promoting protective T and B cell responses (Alaniz et al. 2007). These studies demonstrate the abilities of OMVs to induce DC maturation, leading to antigen presentation to further facilitate an adaptive immune response.
8.5.4 The Effects of Commensal OMVs on Innate Immune Cells
The effects of commensal OMVs on various innate immune cells is of interest due to their ability to traverse the epithelial cell layer (Chi et al. 2003). Commensal bacteria have been long thought to shape the immune system, and maintain homeostasis between tolerance and immunity (Macpherson and Harris 2004). The contributions of bacterial OMVs and MVs to the host-commensal homeostatic balance is of interest due to the versatility of bacterial vesicles. The Gram-negative commensal B. fragilis was found to produce OMVs containing LPS, a well-characterized MAMP. These OMVs were shown to have a protective effect against experimental colitis in mice, by stimulating DCs through TLR2 to adopt an anti-inflammatory profile (Shen et al. 2012). Additionally, OMVs from the commensal Bacteroides thetaiotaomicron have been demonstrated to package and deliver BtMinpp (the bacterial homolog of eukaryotic multiple inositol polyphosphate phosphatase 1) into host cells. This is thought to have beneficial effects for both the host and the bacterial community by providing the anticarcinogenic properties of BtMinpp and nutrients, respectively (Stentz et al. 2014).
Conversely, B. thetaiotaomicron OMVs were demonstrated to enter and activate mouse macrophages inducing an innate immune response, which may contribute to pathogenesis involved in inflammatory bowel disease (Hickey et al. 2015). Furthermore, OMVs from Bacteroides vulgatus were found to induce semi-maturation of bone marrow-derived cells (BMDCs). OMV-treated BMDCs had increased expression of MHC class II, CD40, CD80, and CD86 on their surface. After stimulation with colitogenic E. coli, BMDCs treated with OMVs from B. vulgatus had unchanged expression of MHC class II and secretion of TNF in the supernatant, indicating the induction of tolerance to bacterial challenge (Maerz et al. 2018). This study highlighted the role of commensal OMVs in immune cell priming. Collectively, these studies highlight the broad and opposing roles of commensal OMVs in host immunity, and their abilities to interact with innate immune cells to ultimately shape the host immune response.
8.6 Interactions of OMVs with Endothelial Cells
In addition to interacting with epithelial cells and innate immune cells, OMVs have been shown to interact with endothelial cells in a number of ways to initiate an immune response. OMVs produced by E. coli induce the production of IL-6 (Soult et al. 2013), tissue factor, thrombomodulin and adhesion molecules P- and E-selectin (Soult et al. 2014) by human endothelial cells. This leads to the recruitment of pro-inflammatory immune cells, platelet aggregation, and coagulation (Soult et al. 2013). E. coli-derived OMVs also upregulate the expression of ICAM1 and vascular cell adhesion molecule 1 on the surface of human microvascular endothelial cells (Kim et al. 2013a). Mice injected intraperitoneally with these OMVs showed neutrophil aggregation in the lung endothelium in an ICAM1- and TLR4-dependent manner (Kim et al. 2013a).
As well as pro-inflammatory responses in the endothelium, OMVs from P. gingivalis were demonstrated to downregulate inflammation in IFNγ-stimulated endothelial cells. OMVs did this by inhibiting the upregulation of MHC class II molecules on the host cell surface, thus limiting antigen presentation (Srisatjaluk et al. 2002). Recently, another study revealed that P. gingivalis OMVs suppress endothelial nitric oxide synthase (eNOS) expression in human umbilical vein endothelial cells in vitro, which may contribute to cardiovascular disease (Jia et al. 2015).
The interaction of bacterial vesicles with host cells, including innate immune cells, can lead to activation of the adaptive immune system. Bacterial vesicles have also been described to interact with the adaptive immune system directly, which is discussed below.
8.7 Adaptive Immune Responses to Bacterial Membrane Vesicles
The adaptive immune system is responsible for generating a pathogen-specific immune response that is capable of clearing the pathogen, in addition to generating immune memory that can be reactivated when the host reencounters the pathogen. Specifically, the adaptive immune system is responsible for the production of antigen-specific T and B cells that can target the pathogen directly, or produce pathogen-specific antibodies (Iwasaki and Medzhitov 2015). The hallmarks of this system are the random generation of receptor specificities (T cell receptor and immunoglobulins) by somatic recombination. This results in the possibility of generating a nearly unlimited spectrum of antigen specificity. Populations of cells with cognate receptors for the pathogen are selected and enriched by clonal selection, which means that specific activation of the cell bearing the receptor with the highest affinity leads to its proliferation.
Phagocytic cells such as macrophages, DCs and B cells act as antigen-presenting cells (APCs) in this process. These cells can present peptide antigens via surface receptors (MHC class I and II), which can be recognized by naïve T lymphocytes, leading to their activation, proliferation, and differentiation to effector cell subsets (reviewed in Unanue 1984; Guermonprez et al. 2002; Rodriguez-Pinto 2005). Helper T lymphocytes (CD4 positive cells) are also essential for the activation of B cells and their differentiation into antigen producing plasma cells. Collectively, the activation of the adaptive immune response results in the generation of memory T and B cells which can confer long lived immunity, and is the basis for the idea of bacterial membrane vesicles functioning as vaccines.
8.7.1 Bacterial Membrane Vesicles Shape Adaptive Immunity
Due to their immune stimulating properties and vast evidence of their interactions with the innate immune system, OMVs and MVs are thought to influence the hosts adaptive immune response. OMVs from H. pylori were able to adsorb antibodies in sera from infected patients, thus providing protection for the bacteria (Hynes et al. 2005). Following this, a number of in vivo studies have further revealed the complexity of OMVs as vehicles for antigens and their initiation of adaptive immune responses, which will be discussed here briefly.
8.7.2 Generation of OMV-Specific Protective Immune Responses
Many in vivo studies have demonstrated the generation of specific antibody responses to bacterial OMVs. For example, OMVs produced by N. meningitidis induce the upregulation of MHC class II receptors as well as costimulatory molecules such as CD80 (B7-1) and CD86 (B7-2) on macrophages (Tavano et al. 2009). Furthermore, S. Typhimurium and V. cholerae OMVs were also described as an abundant source of antigens, which could activate CD4+ T cells in order to generate antibody-specific B cell responses (Alaniz et al. 2007; Chatterjee and Chaudhuri 2013). Specifically, in a mouse model of infection and sepsis, Burkholderia pseudomallei OMVs administered subcutaneously were shown to induce serum IgG and T helper 1 (Th1) cell responses (Nieves et al. 2011). A similar finding was observed in mice immunized intraperitoneally with E. coli OMVs. Exposure to OMVs from E. coli resulted in stimulation of T cell immunity primarily driven by Th1 and Th17 cells (Kim et al. 2013b).
Mice vaccinated intramuscularly with OMVs produced by A. baumannii produced high levels of OMV-specific IgG antibodies, and subsequent challenge with A. baumannii intranasally resulted in mucosal IgA and IgG responses in a pneumonia model (Huang et al. 2014). These mice were also challenged with A. baumannii intraperitoneally as a model for bacterial sepsis, and were found to have increased survival when compared to the control group. In this study, mice passively immunized intravenously with antiserum from vaccinated mice also had protection from A. baumannii intranasal challenge. The antisera from immunized mice was also shown to have opsonophagocytic properties and resulted in killing of numerous clinical isolates of A. baumannii by macrophages in vitro (Huang et al. 2014).
Furthermore, OMVs produced by streptomycin resistant clinical strains of nontypeable H. influenzae used to immunize mice both intranasally and intraperitoneally resulted in robust IgG1 antibody production, and IgA production following intranasal immunization. However, when intraperitoneally immunized mice were challenged with H. influenzae strains, they were found to have a higher rate of bacterial colonization when compared to intranasally immunized mice (Roier et al. 2012). These reports demonstrate the shared capacity of OMVs from different bacteria to induce OMV-specific immune responses in vivo.
8.7.3 OMVs Can Modulate B Cell Responses
OMVs have also been demonstrated to modulate B cell responses directly. OMVs produced by M. catarrhalis were shown to contain an outer membrane protein known as Moraxella immunoglobulin D binding protein (MID). MID is an antigen which potently activates human tonsillar B cells via clustering of B cell receptors which mediates endocytosis. TLR9 was also involved in detection of DNA associated with these OMVs, which induced full B cell activation (Vidakovics et al. 2010). H. influenzae also uses a similar approach to modulate B cell responses, by producing OMVs which sensitize B cells resulting in an increase in IgG and IgM production; however, these antibodies do not recognize H. influenzae (Deknuydt et al. 2014). In a manner independent of T cells, Neisseria lactamica OMVs induce B cell proliferation (Vaughan et al. 2010) and polyclonal antibody production (Vaughan et al. 2009) highlighting the versatile interactions of OMVs with adaptive immune cells.
8.7.4 Gram-Positive MVs Mediate Adaptive Immune Responses
Only a handful of studies have analyzed the effects of Gram-positive MVs on mediating adaptive immunity. MVs produced by the pathogen Clostridium perfringens have been shown to induce the production of high titer IgG1 in mice (Jiang et al. 2014). Additionally, B. anthracis MVs have been demonstrated to induce a robust IgM response in mice (Rivera et al. 2010). Mice immunized intramuscularly with Streptococcus pneumoniae MVs were protected from intranasal S. pneumoniae challenge. These mice had increased IgG levels, and increased survival (Olaya-Abril et al. 2014).
S. aureus MVs administered intramuscularly or intravenously have been demonstrated to induce protective immune responses in mice using various models of infection including oropharyngeal or intravenous challenge, respectively, the latter inducing a Th1-mediated response (Choi et al. 2015; Wang et al. 2018). It is because of the antigenic properties of OMVs and MVs that bacterial membrane vesicles are currently being considered as future vesicle vaccines.
8.7.5 Development of OMVs and MVs for Use as Vaccines
Due to their ability to mediate innate and adaptive immune responses in vivo, OMVs have been examined for their ability to confer protection against bacterial challenge and refine their use as vaccine candidates. There are numerous studies that have demonstrated the effect of OMVs on the adaptive immune system, with studies demonstrating the ability of OMVs and MVs to mediate protection from infection, sepsis, and death (Fantappie et al. 2014; Huang et al. 2014; Camacho et al. 2013; Kim et al. 2013b). OMVs have also been proven to be effective at generating a robust immune response and have been found to be more protective against live challenge than vaccination using bacterial membrane fractions (Tavano et al. 2009). In addition, vaccination with OMVs is more effective at generating a bactericidal serum response in mice when compared to serum responses generated as a result of infection alone (Zhu et al. 2005). There are many examples of the effective use of OMVs and MVs as vaccine candidates, in addition to their future therapeutic applications, and these are discussed in further detail in Chap. 10.
8.8 Conclusions and Perspectives
The innate and adaptive immune systems are complex, as are their interactions with invading and commensal organisms. Bacterial membrane vesicles and their immunostimulatory functions have not been fully characterized; however, studies have examined their effects on host epithelial, innate and adaptive immune cells (reviewed in Kaparakis-Liaskos and Ferrero 2015; Manning and Kuehn 2011). OMVs from various bacterial species have been shown to induce a constant interplay between pro-inflammatory and anti-inflammatory signals, and the overall response can vary depending on the amount of OMVs, as well as their content (reviewed in Kaparakis-Liaskos and Ferrero 2015). Bacterial OMVs are able to stimulate TLRs and NLRs of host cells. Furthermore, OMVs and MVs have a wide variety of inherent properties which can be beneficial to the pathogenic capabilities of their parent bacteria, including their contributions to biofilm formation, and antibiotic and host immune molecule defense (Tan et al. 2007; Jagels et al. 1996; Baumgarten et al. 2012; Schooling and Beveridge 2006; Yonezawa et al. 2009). Overall, the vast mechanisms by which OMVs and MVs can interact with and contribute to immunity and pathogenesis are only emerging at present, and further studies should aim to understand the complex nature of membrane vesicle–immune interactions. This knowledge may contribute to forthcoming nanoparticle technologies, whereby OMVs and MVs can be utilized for therapeutics in addition to novel targets to limit bacterial vesicle-mediated pathology.
References
Abachin E, Poyart C, Pellegrini E, Milohanic E, Fiedler F, Berche P, Trieu-Cuot P (2002) Formation of D-alanyl-lipoteichoic acid is required for adhesion and virulence of Listeria monocytogenes. Mol Microbiol 43(1):1–14
Ahmadi Badi S, Khatami SH, Irani SH, Siadat SD (2019) Induction effects of Bacteroides fragilis derived outer membrane vesicles on toll like receptor 2, toll like receptor 4 genes expression and cytokines concentration in human intestinal epithelial cells. Cell J 21(1):57–61
Akira S, Takeda K (2004) Toll-like receptor signaling. Nat Rev Immunol 4(7):499–511
Alaniz RC, Deatherage BL, Lara JC, Cookson BT (2007) Membrane vesicles are immunogenic facsimiles of Salmonella Typhimurium that potently activate dendritic cells, prime B and T cell responses, and stimulate protective immunity in vivo. J Immunol 179(11):7692–7701
Askarian F, Lapek JD Jr, Dongre M, Tsai CM, Kumaraswamy M, Kousha A, Valderrama JA, Ludviksen JA, Cavanagh JP, Uchiyama S, Mollnes TE, Gonzalez DJ, Wai SN, Nizet V, Johannessen M (2018) Staphylococcus aureus membrane-derived vesicles promote bacterial virulence and confer protective immunity in murine infection models. Front Microbiol 9:262
Band VI, Weiss DS (2015) Mechanisms of antimicrobial peptide resistance in Gram-negative bacteria. Antibiotics (Basel) 4(1):18–41
Barrington R, Zhang M, Fischer M, Carroll MC (2001) The role of complement in inflammation and adaptive immunity. Immunol Rev 180:5–15
Bauman SJ, Kuehn MJ (2006) Purification of outer membrane vesicles from Pseudomonas aeruginosa and their activation of an IL-8 response. Microbes Infect 8(9-10):2400–2408
Bauman SJ, Kuehn MJ (2009) Pseudomonas aeruginosa vesicles associate with and are internalized by human lung epithelial cells. BMC Microbiol 9:26
Baumgarten T, Sperling S, Seifert J, von Bergen M, Steiniger F, Wick LY, Heipieper HJ (2012) Membrane vesicle formation as a multiple-stress response mechanism enhances Pseudomonas putida DOT-T1E cell surface hydrophobicity and biofilm formation. Appl Environ Microbiol 78(17):6217–6224
Bielig H, Rompikuntal PK, Dongre M, Zurek B, Lindmark B, Ramstedt M, Wai SN, Kufer TA (2011) NOD-like receptor activation by outer membrane vesicles from Vibrio cholerae non-O1 non-O139 strains is modulated by the quorum-sensing regulator HapR. Infect Immun 79(4):1418–1427
Boller T, Felix G (2009) A renaissance of elicitors: perception of microbe-associated molecular patterns and danger signals by pattern-recognition receptors. Annu Rev Plant Biol 60:379–406
Bomberger JM, Maceachran DP, Coutermarsh BA, Ye S, O’Toole GA, Stanton BA (2009) Long-distance delivery of bacterial virulence factors by Pseudomonas aeruginosa outer membrane vesicles. PLoS Pathog 5(4):e1000382
Boxx GM, Cheng G (2016) The roles of type I interferon in bacterial infection. Cell Host Microbe 19(6):760–769
Brinkmann V, Reichard U, Goosmann C, Fauler B, Uhlemann Y, Weiss DS, Weinrauch Y, Zychlinsky A (2004) Neutrophil extracellular traps kill bacteria. Science 303(5663):1532–1535
Bruno VM, Hannemann S, Lara-Tejero M, Flavell RA, Kleinstein SH, Galan JE (2009) Salmonella Typhimurium type III secretion effectors stimulate innate immune responses in cultured epithelial cells. PLoS Pathog 5(8):e1000538
Camacho AI, Irache JM, de Souza J, Sanchez-Gomez S, Gamazo C (2013) Nanoparticle-based vaccine for mucosal protection against Shigella flexneri in mice. Vaccine 31(32):3288–3294
Canas MA, Gimenez R, Fabrega MJ, Toloza L, Baldoma L, Badia J (2016) Outer membrane vesicles from the probiotic Escherichia coli Nissle 1917 and the commensal ECOR12 enter intestinal epithelial cells via clathrin-dependent endocytosis and elicit differential effects on DNA damage. PLoS One 11(8):e0160374
Cavanagh JP, Pain M, Askarian F, Bruun JA, Urbarova I, Wai SN, Schmidt F, Johannessen M (2018) Comparative exoproteome profiling of an invasive and a commensal Staphylococcus haemolyticus isolate. J Proteomics 197:106–114
Cecil JD, Sirisaengtaksin N, O’Brien-Simpson NM, Krachler AM (2019) Outer membrane vesicle-host cell interactions. Microbiol Spectr 7(1)
Chatterjee D, Chaudhuri K (2013) Vibrio cholerae O395 outer membrane vesicles modulate intestinal epithelial cells in a NOD1 protein-dependent manner and induce dendritic cell-mediated Th2/Th17 cell responses. J Biol Chem 288(6):4299–4309
Chatterjee SN, Das J (1967) Electron microscopic observations on the excretion of cell-wall material by Vibrio cholerae. J Gen Microbiol 49(1):1–11
Chi B, Qi M, Kuramitsu HK (2003) Role of dentilisin in Treponema denticola epithelial cell layer penetration. Res Microbiol 154(9):637–643
Choi DS, Kim DK, Choi SJ, Lee J, Choi JP, Rho S, Park SH, Kim YK, Hwang D, Gho YS (2011) Proteomic analysis of outer membrane vesicles derived from Pseudomonas aeruginosa. Proteomics 11(16):3424–3429
Choi SJ, Kim MH, Jeon J, Kim OY, Choi Y, Seo J, Hong SW, Lee WH, Jeon SG, Gho YS, Jee YK, Kim YK (2015) Active immunization with extracellular vesicles derived from Staphylococcus aureus effectively protects against staphylococcal lung infections, mainly via Th1 cell-mediated immunity. PLoS One 10(9):e0136021
Davis JM, Carvalho HM, Rasmussen SB, O’Brien AD (2006) Cytotoxic necrotizing factor type 1 delivered by outer membrane vesicles of uropathogenic Escherichia coli attenuates polymorphonuclear leukocyte antimicrobial activity and chemotaxis. Infect Immun 74(8):4401–4408
Deknuydt F, Nordstrom T, Riesbeck K (2014) Diversion of the host humoral response: a novel virulence mechanism of Haemophilus influenzae mediated via outer membrane vesicles. J Leukoc Biol 95(6):983–991
Deo P, Chow SH, Hay ID, Kleifeld O, Costin A, Elgass KD, Jiang JH, Ramm G, Gabriel K, Dougan G, Lithgow T, Heinz E, Naderer T (2018) Outer membrane vesicles from Neisseria gonorrhoeae target PorB to mitochondria and induce apoptosis. PLoS Pathog 14(3):e1006945
Duncan L, Yoshioka M, Chandad F, Grenier D (2004) Loss of lipopolysaccharide receptor CD14 from the surface of human macrophage-like cells mediated by Porphyromonas gingivalis outer membrane vesicles. Microb Pathog 36(6):319–325
Duperthuy M, Sjostrom AE, Sabharwal D, Damghani F, Uhlin BE, Wai SN (2013) Role of the Vibrio cholerae matrix protein Bap1 in cross-resistance to antimicrobial peptides. PLoS Pathog 9(10):e1003620
Durand V, Mackenzie J, de Leon J, Mesa C, Quesniaux V, Montoya M, Le Bon A, Wong SY (2009) Role of lipopolysaccharide in the induction of type I interferon-dependent cross-priming and IL-10 production in mice by meningococcal outer membrane vesicles. Vaccine 27(13):1912–1922
Elliott EI, Sutterwala FS (2015) Initiation and perpetuation of NLRP3 inflammasome activation and assembly. Immunol Rev 265(1):35–52
Ellis TN, Kuehn MJ (2010) Virulence and immunomodulatory roles of bacterial outer membrane vesicles. Microbiol Mol Biol Rev 74(1):81–94
Ellis TN, Leiman SA, Kuehn MJ (2010) Naturally produced outer membrane vesicles from Pseudomonas aeruginosa elicit a potent innate immune response via combined sensing of both lipopolysaccharide and protein components. Infect Immun 78(9):3822–3831
Elmi A, Watson E, Sandu P, Gundogdu O, Mills DC, Inglis NF, Manson E, Imrie L, Bajaj-Elliott M, Wren BW, Smith DG, Dorrell N (2012) Campylobacter jejuni outer membrane vesicles play an important role in bacterial interactions with human intestinal epithelial cells. Infect Immun 80(12):4089–4098
Fantappie L, de Santis M, Chiarot E, Carboni F, Bensi G, Jousson O, Margarit I, Grandi G (2014) Antibody-mediated immunity induced by engineered Escherichia coli OMVs carrying heterologous antigens in their lumen. J Extracell Vesicles 3
Faure E, Equils O, Sieling PA, Thomas L, Zhang FX, Kirschning CJ, Polentarutti N, Muzio M, Arditi M (2000) Bacterial lipopolysaccharide activates NF-kappaB through toll-like receptor 4 (TLR-4) in cultured human dermal endothelial cells. Differential expression of TLR-4 and TLR-2 in endothelial cells. J Biol Chem 275(15):11058–11063
Fiocca R, Necchi V, Sommi P, Ricci V, Telford J, Cover TL, Solcia E (1999) Release of Helicobacter pylori vacuolating cytotoxin by both a specific secretion pathway and budding of outer membrane vesicles. Uptake of released toxin and vesicles by gastric epithelium. J Pathol 188(2):220–226
Fritz JH, Le Bourhis L, Sellge G, Magalhaes JG, Fsihi H, Kufer TA, Collins C, Viala J, Ferrero RL, Girardin SE, Philpott DJ (2007) Nod1-mediated innate immune recognition of peptidoglycan contributes to the onset of adaptive immunity. Immunity 26(4):445–459
Furuta N, Takeuchi H, Amano A (2009) Entry of Porphyromonas gingivalis outer membrane vesicles into epithelial cells causes cellular functional impairment. Infect Immun 77(11):4761–4770
Galka F, Wai SN, Kusch H, Engelmann S, Hecker M, Schmeck B, Hippenstiel S, Uhlin BE, Steinert M (2008) Proteomic characterization of the whole secretome of Legionella pneumophila and functional analysis of outer membrane vesicles. Infect Immun 76(5):1825–1836
Girardin SE, Boneca IG, Carneiro LA, Antignac A, Jehanno M, Viala J, Tedin K, Taha MK, Labigne A, Zahringer U, Coyle AJ, DiStefano PS, Bertin J, Sansonetti PJ, Philpott DJ (2003a) Nod1 detects a unique muropeptide from gram-negative bacterial peptidoglycan. Science 300(5625):1584–1587
Girardin SE, Boneca IG, Viala J, Chamaillard M, Labigne A, Thomas G, Philpott DJ, Sansonetti PJ (2003b) Nod2 is a general sensor of peptidoglycan through muramyl dipeptide (MDP) detection. J Biol Chem 278(11):8869–8872
Gu L, Meng R, Tang Y, Zhao K, Liang F, Zhang R, Xue Q, Chen F, Xiao X, Wang H, Wang H, Billiar TR, Lu B (2019) Toll-like receptor 4 signaling licenses the cytosolic transport of lipopolysaccharide from bacterial outer membrane vesicles. Shock 51(2):256–265
Guermonprez P, Valladeau J, Zitvogel L, Thery C, Amigorena S (2002) Antigen presentation and T cell stimulation by dendritic cells. Annu Rev Immunol 20:621–667
Gunn JS, Ryan SS, Van Velkinburgh JC, Ernst RK, Miller SI (2000) Genetic and functional analysis of a PmrA-PmrB-regulated locus necessary for lipopolysaccharide modification, antimicrobial peptide resistance, and oral virulence of Salmonella enterica serovar Typhimurium. Infect Immun 68(11):6139–6146
Gurung M, Moon DC, Choi CW, Lee JH, Bae YC, Kim J, Lee YC, Seol SY, Cho DT, Kim SI, Lee JC (2011) Staphylococcus aureus produces membrane-derived vesicles that induce host cell death. PLoS One 6(11):e27958
Hickey CA, Kuhn KA, Donermeyer DL, Porter NT, Jin C, Cameron EA, Jung H, Kaiko GE, Wegorzewska M, Malvin NP, Glowacki RW, Hansson GC, Allen PM, Martens EC, Stappenbeck TS (2015) Colitogenic Bacteroides thetaiotaomicron antigens access host immune cells in a sulfatase-dependent manner via outer membrane vesicles. Cell Host Microbe 17(5):672–680
Holst J, Martin D, Arnold R, Huergo CC, Oster P, O’Hallahan J, Rosenqvist E (2009) Properties and clinical performance of vaccines containing outer membrane vesicles from Neisseria meningitidis. Vaccine 27(Suppl 2):B3–B12
Hood MI, Skaar EP (2012) Nutritional immunity: transition metals at the pathogen-host interface. Nat Rev Microbiol 10(8):525–537
Huang W, Yao Y, Long Q, Yang X, Sun W, Liu C, Jin X, Li Y, Chu X, Chen B, Ma Y (2014) Immunization against multidrug-resistant Acinetobacter baumannii effectively protects mice in both pneumonia and sepsis models. PLoS One 9(6):e100727
Hynes SO, Keenan JI, Ferris JA, Annuk H, Moran AP (2005) Lewis epitopes on outer membrane vesicles of relevance to Helicobacter pylori pathogenesis. Helicobacter 10(2):146–156
Imayoshi R, Cho T, Kaminishi H (2011) NO production in RAW264 cells stimulated with Porphyromonas gingivalis extracellular vesicles. Oral Dis 17(1):83–89
Inaba K, Metlay JP, Crowley MT, Steinman RM (1990) Dendritic cells pulsed with protein antigens in vitro can prime antigen-specific, MHC-restricted T cells in situ. J Exp Med 172(2):631–640
Inohara N, Nunez G (2001) The NOD: a signaling module that regulates apoptosis and host defense against pathogens. Oncogene 20(44):6473–6481
Inohara N, Koseki T, Lin J, del Peso L, Lucas PC, Chen FF, Ogura Y, Nunez G (2000) An induced proximity model for NF-kappa B activation in the Nod1/RICK and RIP signaling pathways. J Biol Chem 275(36):27823–27831
Irving AT, Mimuro H, Kufer TA, Lo C, Wheeler R, Turner LJ, Thomas BJ, Malosse C, Gantier MP, Casillas LN, Votta BJ, Bertin J, Boneca IG, Sasakawa C, Philpott DJ, Ferrero RL, Kaparakis-Liaskos M (2014) The immune receptor NOD1 and kinase RIP2 interact with bacterial peptidoglycan on early endosomes to promote autophagy and inflammatory signaling. Cell Host Microbe 15(5):623–635
Ismail S, Hampton MB, Keenan JI (2003) Helicobacter pylori outer membrane vesicles modulate proliferation and interleukin-8 production by gastric epithelial cells. Infect Immun 71(10):5670–5675
Iwasaki A, Medzhitov R (2015) Control of adaptive immunity by the innate immune system. Nat Immunol 16(4):343–353
Jagels MA, Travis J, Potempa J, Pike R, Hugli TE (1996) Proteolytic inactivation of the leukocyte C5a receptor by proteinases derived from Porphyromonas gingivalis. Infect Immun 64(6):1984–1991
Jager J, Marwitz S, Tiefenau J, Rasch J, Shevchuk O, Kugler C, Goldmann T, Steinert M (2014) Human lung tissue explants reveal novel interactions during Legionella pneumophila infections. Infect Immun 82(1):275–285
Janeway CA Jr, Medzhitov R (2002) Innate immune recognition. Annu Rev Immunol 20:197–216
Jia Y, Guo B, Yang W, Zhao Q, Jia W, Wu Y (2015) Rho kinase mediates Porphyromonas gingivalis outer membrane vesicle-induced suppression of endothelial nitric oxide synthase through ERK1/2 and p38 MAPK. Arch Oral Biol 60(3):488–495
Jiang Y, Kong Q, Roland KL, Curtiss R 3rd (2014) Membrane vesicles of Clostridium perfringens type A strains induce innate and adaptive immunity. Int J Med Microbiol 304(3-4):431–443
Jin JS, Kwon SO, Moon DC, Gurung M, Lee JH, Kim SI, Lee JC (2011) Acinetobacter baumannii secretes cytotoxic outer membrane protein A via outer membrane vesicles. PLoS One 6(2):e17027
Joiner KA (1988) Complement evasion by bacteria and parasites. Annu Rev Microbiol 42:201–230
Jun SH, Lee JH, Kim BR, Kim SI, Park TI, Lee JC, Lee YC (2013) Acinetobacter baumannii outer membrane vesicles elicit a potent innate immune response via membrane proteins. PLoS One 8(8):e71751
Jun SH, Lee JH, Kim SI, Choi CW, Park TI, Jung HR, Cho JW, Kim SH, Lee JC (2017) Staphylococcus aureus-derived membrane vesicles exacerbate skin inflammation in atopic dermatitis. Clin Exp Allergy 47(1):85–96
Kadurugamuwa JL, Beveridge TJ (1995) Virulence factors are released from Pseudomonas aeruginosa in association with membrane vesicles during normal growth and exposure to gentamicin: a novel mechanism of enzyme secretion. J Bacteriol 177(14):3998–4008
Kadurugamuwa JL, Beveridge TJ (1998) Delivery of the non-membrane-permeative antibiotic gentamicin into mammalian cells by using Shigella flexneri membrane vesicles. Antimicrob Agents Chemother 42(6):1476–1483
Kanneganti TD, Lamkanfi M, Nunez G (2007) Intracellular NOD-like receptors in host defense and disease. Immunity 27(4):549–559
Kaparakis M, Turnbull L, Carneiro L, Firth S, Coleman HA, Parkington HC, Le Bourhis L, Karrar A, Viala J, Mak J, Hutton ML, Davies JK, Crack PJ, Hertzog PJ, Philpott DJ, Girardin SE, Whitchurch CB, Ferrero RL (2010) Bacterial membrane vesicles deliver peptidoglycan to NOD1 in epithelial cells. Cell Microbiol 12(3):372–385
Kaparakis-Liaskos M, Ferrero RL (2015) Immune modulation by bacterial outer membrane vesicles. Nat Rev Immunol 15(6):375–387
Kato S, Kowashi Y, Demuth DR (2002) Outer membrane-like vesicles secreted by Actinobacillus actinomycetemcomitans are enriched in leukotoxin. Microb Pathog 32(1):1–13
Kawai T, Akira S (2008) Toll-like receptor and RIG-I-like receptor signaling. Ann N Y Acad Sci 1143:1–20
Kawai T, Akira S (2010) The role of pattern-recognition receptors in innate immunity: update on Toll-like receptors. Nat Immunol 11(5):373–384
Keenan J, Day T, Neal S, Cook B, Perez-Perez G, Allardyce R, Bagshaw P (2000) A role for the bacterial outer membrane in the pathogenesis of Helicobacter pylori infection. FEMS Microbiol Lett 182(2):259–264
Kesty NC, Mason KM, Reedy M, Miller SE, Kuehn MJ (2004) Enterotoxigenic Escherichia coli vesicles target toxin delivery into mammalian cells. EMBO J 23(23):4538–4549
Kim JH, Yoon YJ, Lee J, Choi EJ, Yi N, Park KS, Park J, Lotvall J, Kim YK, Gho YS (2013a) Outer membrane vesicles derived from Escherichia coli up-regulate expression of endothelial cell adhesion molecules in vitro and in vivo. PLoS One 8(3):e59276
Kim OY, Hong BS, Park KS, Yoon YJ, Choi SJ, Lee WH, Roh TY, Lotvall J, Kim YK, Gho YS (2013b) Immunization with Escherichia coli outer membrane vesicles protects bacteria-induced lethality via Th1 and Th17 cell responses. J Immunol 190(8):4092–4102
Kouokam JC, Wai SN, Fallman M, Dobrindt U, Hacker J, Uhlin BE (2006) Active cytotoxic necrotizing factor 1 associated with outer membrane vesicles from uropathogenic Escherichia coli. Infect Immun 74(4):2022–2030
Kulp A, Kuehn MJ (2010) Biological functions and biogenesis of secreted bacterial outer membrane vesicles. Annu Rev Microbiol 64:163–184
Kumar H, Kawai T, Akira S (2009) Toll-like receptors and innate immunity. Biochem Biophys Res Commun 388(4):621–625
Lapinet JA, Scapini P, Calzetti F, Perez O, Cassatella MA (2000) Gene expression and production of tumor necrosis factor alpha, interleukin-1beta (IL-1beta), IL-8, macrophage inflammatory protein 1alpha (MIP-1alpha), MIP-1beta, and gamma interferon-inducible protein 10 by human neutrophils stimulated with group B meningococcal outer membrane vesicles. Infect Immun 68(12):6917–6923
Lappann M, Danhof S, Guenther F, Olivares-Florez S, Mordhorst IL, Vogel U (2013) In vitro resistance mechanisms of Neisseria meningitidis against neutrophil extracellular traps. Mol Microbiol 89(3):433–449
Lee EY, Choi DY, Kim DK, Kim JW, Park JO, Kim S, Kim SH, Desiderio DM, Kim YK, Kim KP, Gho YS (2009) Gram-positive bacteria produce membrane vesicles: proteomics-based characterization of Staphylococcus aureus-derived membrane vesicles. Proteomics 9(24):5425–5436
Lee J, Yoon YJ, Kim JH, Dinh NTH, Go G, Tae S, Park KS, Park HT, Lee C, Roh TY, Di Vizio D, Gho YS (2018) Outer membrane vesicles derived from Escherichia coli regulate neutrophil migration by induction of endothelial IL-8. Front Microbiol 9:2268
Lim JP, Gleeson PA (2011) Macropinocytosis: an endocytic pathway for internalising large gulps. Immunol Cell Biol 89(8):836–843
Lindmark B, Rompikuntal PK, Vaitkevicius K, Song T, Mizunoe Y, Uhlin BE, Guerry P, Wai SN (2009) Outer membrane vesicle-mediated release of cytolethal distending toxin (CDT) from Campylobacter jejuni. BMC Microbiol 9:220
Macdonald IA, Kuehn MJ (2013) Stress-induced outer membrane vesicle production by Pseudomonas aeruginosa. J Bacteriol 195(13):2971–2981
Macpherson AJ, Harris NL (2004) Interactions between commensal intestinal bacteria and the immune system. Nat Rev Immunol 4(6):478–485
Maerz JK, Steimle A, Lange A, Bender A, Fehrenbacher B, Frick JS (2018) Outer membrane vesicles blebbing contributes to B. vulgatus mpk-mediated immune response silencing. Gut Microbes 9(1):1–12
Manning AJ, Kuehn MJ (2011) Contribution of bacterial outer membrane vesicles to innate bacterial defense. BMC Microbiol 11:258
Martinon F, Burns K, Tschopp J (2002) The inflammasome: a molecular platform triggering activation of inflammatory caspases and processing of proIL-beta. Mol Cell 10(2):417–426
McBroom AJ, Kuehn MJ (2007) Release of outer membrane vesicles by Gram-negative bacteria is a novel envelope stress response. Mol Microbiol 63(2):545–558
McBroom AJ, Johnson AP, Vemulapalli S, Kuehn MJ (2006) Outer membrane vesicle production by Escherichia coli is independent of membrane instability. J Bacteriol 188(15):5385–5392
Medzhitov R, Janeway CA Jr (1997) Innate immunity: the virtues of a nonclonal system of recognition. Cell 91(3):295–298
Milward MR, Chapple IL, Wright HJ, Millard JL, Matthews JB, Cooper PR (2007) Differential activation of NF-kappaB and gene expression in oral epithelial cells by periodontal pathogens. Clin Exp Immunol 148(2):307–324
Moskowitz SM, Ernst RK, Miller SI (2004) PmrAB, a two-component regulatory system of Pseudomonas aeruginosa that modulates resistance to cationic antimicrobial peptides and addition of aminoarabinose to lipid A. J Bacteriol 186(2):575–579
Nakao R, Takashiba S, Kosono S, Yoshida M, Watanabe H, Ohnishi M, Senpuku H (2014) Effect of Porphyromonas gingivalis outer membrane vesicles on gingipain-mediated detachment of cultured oral epithelial cells and immune responses. Microbes Infect 16(1):6–16
Namork E, Brandtzaeg P (2002) Fatal meningococcal septicaemia with “blebbing” meningococcus. Lancet 360(9347):1741
Nieves W, Asakrah S, Qazi O, Brown KA, Kurtz J, Aucoin DP, McLachlan JB, Roy CJ, Morici LA (2011) A naturally derived outer-membrane vesicle vaccine protects against lethal pulmonary Burkholderia pseudomallei infection. Vaccine 29(46):8381–8389
O’Donoghue EJ, Krachler AM (2016) Mechanisms of outer membrane vesicle entry into host cells. Cell Microbiol 18(11):1508–1517
Olaya-Abril A, Prados-Rosales R, McConnell MJ, Martin-Pena R, Gonzalez-Reyes JA, Jimenez-Munguia I, Gomez-Gascon L, Fernandez J, Luque-Garcia JL, Garcia-Lidon C, Estevez H, Pachon J, Obando I, Casadevall A, Pirofski LA, Rodriguez-Ortega MJ (2014) Characterization of protective extracellular membrane-derived vesicles produced by Streptococcus pneumoniae. J Proteome 106:46–60
Olofsson A, Nygard Skalman L, Obi I, Lundmark R, Arnqvist A (2014) Uptake of Helicobacter pylori vesicles is facilitated by clathrin-dependent and clathrin-independent endocytic pathways. MBio 5(3):e00979–e00914
Parker H, Chitcholtan K, Hampton MB, Keenan JI (2010) Uptake of Helicobacter pylori outer membrane vesicles by gastric epithelial cells. Infect Immun 78(12):5054–5061
Pathirana RD, Kaparakis-Liaskos M (2016) Bacterial membrane vesicles: biogenesis, immune regulation and pathogenesis. Cell Microbiol 18(11):1518–1524
Peschel A, Jack RW, Otto M, Collins LV, Staubitz P, Nicholson G, Kalbacher H, Nieuwenhuizen WF, Jung G, Tarkowski A, van Kessel KP, van Strijp JA (2001) Staphylococcus aureus resistance to human defensins and evasion of neutrophil killing via the novel virulence factor MprF is based on modification of membrane lipids with l-lysine. J Exp Med 193(9):1067–1076
Peterson LW, Artis D (2014) Intestinal epithelial cells: regulators of barrier function and immune homeostasis. Nat Rev Immunol 14(3):141–153
Pollak CN, Delpino MV, Fossati CA, Baldi PC (2012) Outer membrane vesicles from Brucella abortus promote bacterial internalization by human monocytes and modulate their innate immune response. PLoS One 7(11):e50214
Qi M, Miyakawa H, Kuramitsu HK (2003) Porphyromonas gingivalis induces murine macrophage foam cell formation. Microb Pathog 35(6):259–267
Ren D, Walker AN, Daines DA (2012) Toxin-antitoxin loci vapBC-1 and vapXD contribute to survival and virulence in nontypeable Haemophilus influenzae. BMC Microbiol 12:263
Renelli M, Matias V, Lo RY, Beveridge TJ (2004) DNA-containing membrane vesicles of Pseudomonas aeruginosa PAO1 and their genetic transformation potential. Microbiology 150(Pt 7):2161–2169
Rewatkar PV, Parton RG, Parekh HS, Parat MO (2015) Are caveolae a cellular entry route for non-viral therapeutic delivery systems? Adv Drug Deliv Rev 91:92–108
Rhee KJ, Sethupathi P, Driks A, Lanning DK, Knight KL (2004) Role of commensal bacteria in development of gut-associated lymphoid tissues and preimmune antibody repertoire. J Immunol 172(2):1118–1124
Rivera J, Cordero RJ, Nakouzi AS, Frases S, Nicola A, Casadevall A (2010) Bacillus anthracis produces membrane-derived vesicles containing biologically active toxins. Proc Natl Acad Sci U S A 107(44):19002–19007
Robinson MJ, Sancho D, Slack EC, LeibundGut-Landmann S, Reis e Sousa C (2006) Myeloid C-type lectins in innate immunity. Nat Immunol 7(12):1258–1265
Rodriguez-Pinto D (2005) B cells as antigen presenting cells. Cell Immunol 238(2):67–75
Roier S, Leitner DR, Iwashkiw J, Schild-Prufert K, Feldman MF, Krohne G, Reidl J, Schild S (2012) Intranasal immunization with nontypeable Haemophilus influenzae outer membrane vesicles induces cross-protective immunity in mice. PLoS One 7(8):e42664
Rus H, Cudrici C, Niculescu F (2005) The role of the complement system in innate immunity. Immunol Res 33(2):103–112
Schooling SR, Beveridge TJ (2006) Membrane vesicles: an overlooked component of the matrices of biofilms. J Bacteriol 188(16):5945–5957
Schroder K, Zhou R, Tschopp J (2010) The NLRP3 inflammasome: a sensor for metabolic danger? Science 327(5963):296–300
Schultz H, Hume J, Zhang DS, Gioannini TL, Weiss JP (2007) A novel role for the bactericidal/permeability increasing protein in interactions of gram-negative bacterial outer membrane blebs with dendritic cells. J Immunol 179(4):2477–2484
Schwechheimer C, Kuehn MJ (2015) Outer-membrane vesicles from Gram-negative bacteria: biogenesis and functions. Nat Rev Microbiol 13(10):605–619
Sharpe SW, Kuehn MJ, Mason KM (2011) Elicitation of epithelial cell-derived immune effectors by outer membrane vesicles of nontypeable Haemophilus influenzae. Infect Immun 79(11):4361–4369
Shen Y, Giardino Torchia ML, Lawson GW, Karp CL, Ashwell JD, Mazmanian SK (2012) Outer membrane vesicles of a human commensal mediate immune regulation and disease protection. Cell Host Microbe 12(4):509–520
Shi J, Zhao Y, Wang Y, Gao W, Ding J, Li P, Hu L, Shao F (2014) Inflammatory caspases are innate immune receptors for intracellular LPS. Nature 514(7521):187–192
Soult MC, Lonergan NE, Shah B, Kim WK, Britt LD, Sullivan CJ (2013) Outer membrane vesicles from pathogenic bacteria initiate an inflammatory response in human endothelial cells. J Surg Res 184(1):458–466
Soult MC, Dobrydneva Y, Wahab KH, Britt LD, Sullivan CJ (2014) Outer membrane vesicles alter inflammation and coagulation mediators. J Surg Res 192(1):134–142
Srisatjaluk R, Kotwal GJ, Hunt LA, Justus DE (2002) Modulation of gamma interferon-induced major histocompatibility complex class II gene expression by Porphyromonas gingivalis membrane vesicles. Infect Immun 70(3):1185–1192
Stappenbeck TS, Hooper LV, Gordon JI (2002) Developmental regulation of intestinal angiogenesis by indigenous microbes via Paneth cells. Proc Natl Acad Sci U S A 99(24):15451–15455
Stentz R, Osborne S, Horn N, Li AW, Hautefort I, Bongaerts R, Rouyer M, Bailey P, Shears SB, Hemmings AM, Brearley CA, Carding SR (2014) A bacterial homolog of a eukaryotic inositol phosphate signaling enzyme mediates cross-kingdom dialog in the mammalian gut. Cell Rep 6(4):646–656
Stephens DS, Edwards KM, Morris F, McGee ZA (1982) Pili and outer membrane appendages on Neisseria meningitidis in the cerebrospinal fluid of an infant. J Infect Dis 146(4):568
Takeuchi O, Akira S (2010) Pattern recognition receptors and inflammation. Cell 140(6):805–820
Tan TT, Morgelin M, Forsgren A, Riesbeck K (2007) Haemophilus influenzae survival during complement-mediated attacks is promoted by Moraxella catarrhalis outer membrane vesicles. J Infect Dis 195(11):1661–1670
Tavano R, Franzoso S, Cecchini P, Cartocci E, Oriente F, Arico B, Papini E (2009) The membrane expression of Neisseria meningitidis adhesin A (NadA) increases the proimmune effects of MenB OMVs on human macrophages, compared with NadA-OMVs, without further stimulating their proinflammatory activity on circulating monocytes. J Leukoc Biol 86(1):143–153
Thay B, Wai SN, Oscarsson J (2013) Staphylococcus aureus alpha-toxin-dependent induction of host cell death by membrane-derived vesicles. PLoS One 8(1):e54661
Thay B, Damm A, Kufer TA, Wai SN, Oscarsson J (2014) Aggregatibacter actinomycetemcomitans outer membrane vesicles are internalized in human host cells and trigger NOD1- and NOD2-dependent NF-kappaB activation. Infect Immun 82(10):4034–4046
Thomas CJ, Schroder K (2013) Pattern recognition receptor function in neutrophils. Trends Immunol 34(7):317–328
Turner L, Bitto NJ, Steer DL, Lo C, D’Costa K, Ramm G, Shambrook M, Hill AF, Ferrero RL, Kaparakis-Liaskos M (2018) Helicobacter pylori outer membrane vesicle size determines their mechanisms of host cell entry and protein content. Front Immunol 9:1466
Unanue ER (1984) Antigen-presenting function of the macrophage. Annu Rev Immunol 2:395–428
Vanaja SK, Russo AJ, Behl B, Banerjee I, Yankova M, Deshmukh SD, Rathinam VAK (2016) Bacterial outer membrane vesicles mediate cytosolic localization of LPS and caspase-11 activation. Cell 165(5):1106–1119
Vaughan AT, Gorringe A, Davenport V, Williams NA, Heyderman RS (2009) Absence of mucosal immunity in the human upper respiratory tract to the commensal bacteria Neisseria lactamica but not pathogenic Neisseria meningitidis during the peak age of nasopharyngeal carriage. J Immunol 182(4):2231–2240
Vaughan AT, Brackenbury LS, Massari P, Davenport V, Gorringe A, Heyderman RS, Williams NA (2010) Neisseria lactamica selectively induces mitogenic proliferation of the naive B cell pool via cell surface Ig. J Immunol 185(6):3652–3660
Vidakovics ML, Jendholm J, Morgelin M, Mansson A, Larsson C, Cardell LO, Riesbeck K (2010) B cell activation by outer membrane vesicles—a novel virulence mechanism. PLoS Pathog 6(1):e1000724
Wai SN, Lindmark B, Soderblom T, Takade A, Westermark M, Oscarsson J, Jass J, Richter-Dahlfors A, Mizunoe Y, Uhlin BE (2003) Vesicle-mediated export and assembly of pore-forming oligomers of the enterobacterial ClyA cytotoxin. Cell 115(1):25–35
Wang X, Thompson CD, Weidenmaier C, Lee JC (2018) Release of Staphylococcus aureus extracellular vesicles and their application as a vaccine platform. Nat Commun 9(1):1379
Wells JM, Rossi O, Meijerink M, van Baarlen P (2011) Epithelial crosstalk at the microbiota-mucosal interface. Proc Natl Acad Sci U S A 108(Suppl 1):4607–4614
Winter J, Letley D, Rhead J, Atherton J, Robinson K (2014) Helicobacter pylori membrane vesicles stimulate innate pro- and anti-inflammatory responses and induce apoptosis in Jurkat T cells. Infect Immun 82(4):1372–1381
Yonezawa H, Osaki T, Kurata S, Fukuda M, Kawakami H, Ochiai K, Hanawa T, Kamiya S (2009) Outer membrane vesicles of Helicobacter pylori TK1402 are involved in biofilm formation. BMC Microbiol 9:197
Yoon H, Ansong C, Adkins JN, Heffron F (2011) Discovery of Salmonella virulence factors trans located via outer membrane vesicles to murine macrophages. Infect Immun 79(6):2182–2192
Young GM, Schmiel DH, Miller VL (1999) A new pathway for the secretion of virulence factors by bacteria: the flagellar export apparatus functions as a protein-secretion system. Proc Natl Acad Sci U S A 96(11):6456–6461
Yun SH, Park EC, Lee SY, Lee H, Choi CW, Yi YS, Ro HJ, Lee JC, Jun S, Kim HY, Kim GH, Kim SI (2018) Antibiotic treatment modulates protein components of cytotoxic outer membrane vesicles of multidrug-resistant clinical strain, Acinetobacter baumannii DU202. Clin Proteomics 15:28
Zhu W, Thomas CE, Chen CJ, Van Dam CN, Johnston RE, Davis NL, Sparling PF (2005) Comparison of immune responses to gonococcal PorB delivered as outer membrane vesicles, recombinant protein, or Venezuelan equine encephalitis virus replicon particles. Infect Immun 73(11):7558–7568
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Johnston, E.L., Kufer, T.A., Kaparakis-Liaskos, M. (2020). Immunodetection and Pathogenesis Mediated by Bacterial Membrane Vesicles. In: Kaparakis-Liaskos, M., Kufer, T. (eds) Bacterial Membrane Vesicles. Springer, Cham. https://doi.org/10.1007/978-3-030-36331-4_8
Download citation
DOI: https://doi.org/10.1007/978-3-030-36331-4_8
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-36330-7
Online ISBN: 978-3-030-36331-4
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)