Abstract
Medial unicompartmental knee arthroplasty is an excellent surgical option for the treatment of isolated medial compartment arthritis. Modern implants demonstrate outstanding function and survivorship. Additionally, the procedure is less demanding for both the surgeon and the patient. The potential for enhanced patient recovery utilizing straightforward surgical techniques and same-day surgery protocols has helped repopularize the procedure. Exceptional clinical results persist even as contemporary indications expand. Moreover, unicompartmental knee arthroplasty is associated with a lower occurrence of complications and mortality. The most common modes of failure for fixed-bearing medial unicompartmental knee arthroplasty are progression of adjacent compartment arthritis and aseptic loosening. Revision results closely approximate that of a revision total knee arthroplasty.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Case Example
Active 70-year-old male with chief complaint of medial right knee pain. Patient has a past medical history of hypertension and coronary artery disease and past surgical history significant for right knee arthroscopy with medial meniscectomy 2 years previously. His symptoms are recalcitrant to conservative treatment with activity modification, physical therapy, anti-inflammatory medications, and multiple intra-articular injections. On physical examination, he stands 5′10″ tall and weighs 265 lbs. with a BMI of 38. He walks with a shortened stance phase on the right side, has focal tenderness isolated to the medial joint line, range of motion 10–115°, and is ligamentously stable in all planes. Radiographs reveal osteoarthritis localized to the medial compartment (Fig. 7.1).
Introduction
Unicompartmental knee arthroplasty (UKA) was introduced in the 1970s by Marmor and was initially met with great enthusiasm, promising an alternative to osteotomy [1]. Early excitement disappeared with poor results reported by several authors. Laskin reported on 37 patients in 1978, finding contralateral compartment degeneration at 4–7 years and results inferior to bicompartmental and tricompartmental arthroplasty of the knee [2]. In 1980, Insall and Aglietti also reported poor results, with early deterioration at an average follow-up of 6 years [3]. These early failures were likely due to the degree of constraint of the initial implants, poor implant design, imprecise instrumentation, and unclear indications. A unicompartmental knee arthroplasty could not be treated as “half” a total knee arthroplasty (TKA) and in that early form, with excellent results being reported with TKA, most surgeons abandoned UKA.
Learning from the initial mistakes, indications were proposed, instrumentation improved, and implant designs were refined. Proposed indications addressed age, weight, level of activity, pain, range of motion, and angular deformity, and limitations in the degeneration of the remaining compartments [4]. Several authors then began to publish promising results. In 1999, Berger et al. found 98% survival at 10 years in 62 knees [5], and more recently 90% survival at 20 years [6]. Pandit also published results from 1000 cases, showing 94% survival at 10 years and 91% survival at 15 years [7]. These promising results suggest that solutions had been found to the early challenges and partial knee replacements were once again a viable treatment option for select patients with knee arthritis.
Current Trends
With the development of surgical pathways, multimodal pain strategies, improvement in surgical technique and the advent of same-day surgery protocols, patient’s expectations about unicompartmental knee replacement surgery have changed. The promise of simpler, quicker surgery, and faster recovery has led to a significant increase in the frequency of UKA [8], particularly for isolated medial compartment arthritis. Additionally, indications have expanded with continued excellent results [9,10,11]. Long-term follow-up has shown encouraging longevity and function from the implants currently available and published data suggests increasing utilization of ambulatory surgery centers (ASC) is safe and effective for same-day procedures [12,13,14]. To that end, Centers for Medicare and Medicaid Services has designated partial knee replacements as an outpatient procedure and indications for hospital stays greater than 23 hours must now be well indicated.
Indications/Contraindications
The primary indications for medial UKA are isolated anteromedial arthritis and spontaneous osteonecrosis of the knee [15,16,17]. Approximately three decades ago, Kozinn & Scott described their ideal candidate as less the 60 years of age, weighing less than 180 pounds, and low demand with minimal pain at rest, less than 5° flexion contracture, a preoperative arc of flexion of 90°, and a passively correctable angular deformity of less than 10° of varus. Additionally, patellofemoral joint arthritis, inflammatory arthropathy, chondrocalcinosis, and cruciate ligament deficiency were suggested as contraindications [4].
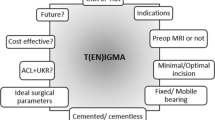
Modern indications do not strictly exclude patients based on age, weight, activity level, having chondrocalcinosis , or the presence of arthritis within the patellofemoral joint [11, 18, 19]. Contraindications are limited to active infection, inflammatory arthropathy, ligamentous instability, contracture of the medial collateral ligament, a functionally absent ACL, and previous high tibial osteotomy [18, 20]. Medial UKA has been shown to be a viable option in patients 75 years and older [21,22,23] as well as in younger, active patients [24,25,26,27]. Good results and survival have also been demonstrated in the obese population [28,29,30,31]. Patellofemoral arthrosis of the medial facet and/or central trochlea have not been shown to adversely affect medial UKA outcomes [32, 33]. Furthermore, the presence of lateral osteophytes does not preclude excellent results at 15-year follow-up [34]. Acceptable results have been achieved in ACL-deficient patients without subjective instability by decreasing the posterior slope of the tibial component [35, 36]. Moreover, respectable results have also been reported with medial UKA performed concurrently with ACL reconstruction [37, 38]. A more detailed discussion of appropriate patient selection and the necessity of the ACL are discussed in Chaps. 2 and 11 of this book (Fig. 7.2).
Technique
The patient is positioned supine on the operating room table. All bony prominences are well padded. A tourniquet is placed high on the operative thigh and Foley catheter may be inserted. The operative extremity is prepped and draped in normal sterile fashion. Antibiotics are given within 1 hour of incision. The leg is exsanguinated and tourniquet inflated. With the knee in moderate flexion, incision is made medial to midline, extending from the proximal pole of the patella to just medial to the tibial tubercle. Full-thickness skin flaps are developed, and underlying extensor mechanism and joint capsule are exposed. The knee joint is accessed via a mini-midvastus arthrotomy , taking great care to avoid damage to the intact cartilage at the superior aspect of the arthrotomy. All compartments of the knee are inspected to confirm moving forward with UKA is appropriate. The patella is subluxed laterally and a portion of the retropatellar fat pad is excised to facilitate visualization. Marginal osteophytes are removed with combination of osteotome and rongeur. The anterior horn of the medial meniscus is released from its coronary ligament attachment laterally and subperiosteal medial release is performed as needed along the medial face of the tibia utilizing Bovie electrocautery . Partial medial meniscectomy is carried out to improve exposure. Extramedullary tibial cutting guide is placed parallel to the long axis of the tibia in the coronal plane and matching the tibia’s native slope in the sagittal plane (up to 7°). A conservative horizontal cut is performed with an oscillating saw, typically 1–2 mm below the arthritic surface, depending on the amount of cartilage and bone loss. Resection is completed with a vertical cut, utilizing a narrow, reciprocating saw blade, just medial to the peak of the medial tibial eminence. Care is taken to avoid disrupting the cruciate ligament attachments laterally, the tibial collateral ligament medially, and breaching the posterior tibial cortex distally. Proximal tibial bone fragment, residual meniscus, and guide are removed. Flexion and extension gaps are checked with a spacer block and ensured to be equal before turning attention to the distal femur. In extension, the resection guide is placed flush with the distal femoral condyle, perpendicular to the tibial shaft, and rotationally parallel to the resected tibial surface. The anatomic angle of the distal femoral cut is typically 4–6° of valgus relative to the anatomic axis of the femur, matching the tibial cut in the coronal plane. The cut is made using an oscillating saw with retractors positioned to protect the medial collateral ligament and adjacent soft tissues. The guide and excess bone are removed. Extension gap is again checked using a spacer block before sizing the femoral component with the knee in flexion. In an effort to avoid patellar impingement, the appropriate sized femoral component will have 1–2 mm of exposed bone between the anterior edge of the guide and the cartilage tidemark with the posterior aspect of the guide resting against the posterior femoral condyle and parallel to the tibial resection. The appropriate resection guide is then secured in position with the posterior surface parallel to the tibial resection and biased laterally toward the intercondylar notch. Lug holes are drilled, and posterior femoral condyle and chamfer cuts completed. The tibia is then sized to maximize coverage without generating overhang of the tibial cortex. Trial components are inserted, and all retractors are removed. The knee is taken through a range of motion and stability tested. Gap spacers are used to assess the flexion and extension gaps. The joint should have 1–2 mm of laxity in both flexion and extension, ideally just a touch looser in flexion. Care should be taken to avoid overstuffing the joint. Unacceptable tightness or asymmetry should be addressed by adjusting the thickness of the polyethylene insert, resecting additional tibia, altering its slope, or changing the size of the femoral component. Once adequate balance is achieved, femoral and tibial preparation is completed. Supplementary anchorage holes are created in particularly sclerotic bone as needed. All components and retractors are then removed. The wound is copiously irrigated using pulsatile lavage. Bone is then carefully dried. Vacuum mixed polymethylmethacrylate (PMMA) is used for fixation of the final components. Cement is placed on the components first and subsequently pressurized into the bone using cement gun. Final components are inserted, and excess PMMA is carefully removed. The cement hardens with trial polyethylene insert and the knee in approximately 30° of flexion. A 1-mm gap spacer can be used to help pressurize the components while the cement cures. Once the cement is mature, knee range of motion, stability, and gap balance are again verified prior to insertion of definitive polyethylene liner. The wound is then copiously irrigated and closed in layered fashion (Fig. 7.3).
Implant Options
Initial failures suggest that constraint is best limited in implant design [2, 3, 39]. Learning from early design limitations has led to reliable survivability in multiple designs. Options for the medial compartment of the knee include fixed- and mobile-bearing designs, monoblock and modular tibial options, and cemented and cementless implants. Functional outcomes and longevity appear similar between fixed- and mobile-bearing designs [40,41,42,43], although progression of lateral compartment arthritis is more common in the mobile-bearing group and polyethylene insert dislocation is a complication unique to mobile-bearing implants [20]. Retrospective analysis has also shown that fixed-bearing implants better tolerate suboptimal rotation of the tibial component [44]. While reasonable midterm results have been reported in an all-polyethylene tibial designs [45, 46] and there is valid concern regarding bone loss in revision of metal-backed modular tibial components [47], the literature more consistently shows superior survivability with metal-backed designs and the risk of early failure with monoblock all-polyethylene tibial implants [48,49,50,51]. Biomechanical data help support and explain these findings, with significantly greater strain on the cancellous bone of the proximal tibia with all-polyethylene tibial components [52, 53]. Cementless implants offer the potential for faster surgery, avoidance of cementation errors, and diminished aseptic loosening. The limited available evidence is promising, with survival, reoperation rate, failure, and clinical outcomes similar to cemented implants [54, 55]. However, the majority of results are restricted to a single, mobile-bearing implant design , and include only midterm follow-up of 5 years. Long-term follow-up is necessary to validate these findings.
Technology
Interest in leveraging technological advances in surgical technique continues to grow among surgeons, researchers, manufacturers, and patients. The goal of robotics and patient-specific instrumentation (PSI) is to minimize limb malalignment and component malposition in an effort to improve implant durability and outcomes. However, these technologies are expensive and have failed to show significant clinical benefit as of yet. Two Level 1 studies have been conducted using PSI guides for medial unicompartmental knee arthroplasty [56, 57], and neither showed an advantage when compared to conventional instrumentation. The majority of studies investigating robotic-assisted UKA have reported on accuracy of component placement and shown a statistical advantage when compared to conventional techniques, but there are few reports documenting clinical outcomes and long-term follow-up results are lacking [58, 59]. It remains unknown if more accurate component position leads to improved clinical outcomes or enhances long-term survival of implants.
Outcomes and Survival
Although there is some debate regarding improvement in patient-reported outcomes when compared to TKA [60,61,62,63], it is generally accepted that appropriately selected patients have high satisfaction rates and improved function following UKA. Nevertheless, UKA is associated with a lower occurrence of complications, readmission, and mortality [64, 65]. If 100 patients receiving TKA received UKA instead, the result would average one fewer death and three more reoperations in the first 4 years following surgery [65]. It is important to point out that the threshold for revision of UKA is much lower, and UKA still compares favorably in economic evaluations of estimated cost and health outcome even when considering slightly higher rates of revision [66].
The results of UKA have significantly improved in the past few decades, with greater than 94% survival at 10 years for metal-backed, fixed-bearing medial UKA in multiple cohort studies [6, 67, 68] and an average of 91% for all medial UKA in a systematic review [69]. Of note, registry data consistently shows worse outcomes, with an average 10-year survival of only 84.1% in the aforementioned systematic review [69]. A plausible explanation for this trend is that registry data includes multiple implants performed by multiple surgeons with varying levels of experience. The revision rate is significantly lower for surgeons performing at least 30 UKAs per year [70]. Cohort studies may allow better understanding of how specific implants perform at single center institutions by high volume surgeons [16].
Complications
A recent systematic review found the most common modes of failure for fixed-bearing medial UKA are progression of adjacent compartment arthritis (36%) and aseptic loosening (28%). Instability (12%), polyethylene wear (12%), tibial subsidence (4%), unexplained pain (2%), and infection (2%) are less common. When looking at all medial UKAs, that is, mobile- and fixed-bearing, early failures (<5 years) were most commonly caused by aseptic loosening (25%), progression of osteoarthritis (20%), and bearing dislocation (17%) [71].
Newer designs and better instrumentation have significantly reduced the incidence of aseptic loosening. Varus deformity , younger age, and weight have been advocated as possible risk factors for mechanical failure [72]. Mechanical loosening is also likely influenced by undercorrection of constitutional deformity, component malalignment, excessive tibial slope, and anterior cruciate ligament deficiency. In addition, all these factors may contribute to wear-induced periprosthetic osteolysis , with a further increase in component subsidence and/or loosening [73]. Progression of adjacent compartment arthritis was responsible for 38% and 40% of midterm (5–10 years) and late failures (>10 years), respectively [71]. Overcorrection of the leg mechanical axis may cause degenerative changes in the contralateral compartment [74]. Degeneration of the patellofemoral joint may occur in the presence of an oversized femoral component [6]. Disease progression and component failure are discussed further in Chap. 17.
Revision
Revision of UKA to TKA results in poorer outcomes than primary TKA, but that may be a result of poor preoperative function rather than complexity of the surgery. Revision results were once thought to be equivalent to a primary TKA, but it has been recently suggested that the results may more closely approximate that of a revision total knee, as reported by several authors [75,76,77,78,79,80]. Revision UKA more frequently requires augments, stems, bone graft, and thicker polyethylene components than primary TKA [78]. It may also be associated with longer operative times, higher reoperation rates, and worse postoperative clinical outcome scores [79]. However, the mode of UKA failure affects the complexity of revision. Isolated liner exchange for polyethylene wear has been shown to be a valuable treatment option in a well-fixed, metal-backed fixed-bearing UKA [81] (Fig. 7.4).
Conclusion
In appropriately selected patients, medial UKA is an excellent surgical option for the treatment of isolated medial compartment arthritis of the knee. The procedure is well suited to rapid recovery protocols and outpatient surgery through a well-structured surgical pathway. Long-term results suggest high patient satisfaction and survivability rivaling TKA. Revision occurs most commonly as a result of progression of arthritis within the remaining compartments of the knee and for component loosening. Results of revision to TKA may more closely approximate that of revision TKA than primary arthroplasty.
Case Example
The patient underwent uncomplicated medial UKA for isolated medial compartment arthritis. Note maintained constitutional varus, subtle lateral bias of the femoral component, native slope of tibial component, and penetrating cement mantle. The patient achieved an excellent result and looks forward to having his contralateral side done soon (Fig. 7.5).
References
Marmor L. Results of single compartment arthroplasty with acrylic cement fixation. A minimum follow-up of two years. Clin Orthop Relat Res. 1977;122:181–8.
Laskin RS. Unicompartmental tibiofemoral resurfacing arthroplasty. J Bone Joint Surg Am. 1978;60(2):182–5.
Insall J, Aglietti P. A five to seven-year follow-up of unicondylar arthroplasty. J Bone Joint Surg Am. 1980;62(8):1329–37.
Kozinn SC, Scott R. Unicondylar knee arthroplasty. J Bone Joint Surg Am. 1989;71(1):145–50.
Berger RA, Nedeff DD, Barden RM, Sheinkop MM, Jacobs JJ, Rosenberg AG, et al. Unicompartmental knee arthroplasty. Clinical experience at 6- to 10-year followup. Clin Orthop Relat Res. 1999;367:50–60.
Foran JRH, Brown NM, Della Valle CJ, Berger RA, Galante JO. Long-term survivorship and failure modes of unicompartmental knee arthroplasty. Clin Orthop Relat Res. 2013;471(1):102–8.
Pandit H, Hamilton TW, Jenkins C, Mellon SJ, Dodd CAF, Murray DW. The clinical outcome of minimally invasive phase 3 Oxford unicompartmental knee arthroplasty: a 15-year follow-up of 1000 UKAs. Bone Joint J. 2015;97-B(11):1493–500.
Bolognesi MP, Greiner MA, Attarian DE, Watters TS, Wellman SS, Curtis LH, et al. Unicompartmental knee arthroplasty and total knee arthroplasty among Medicare beneficiaries, 2000 to 2009. J Bone Joint Surg Am. 2013;95(22):e174.
Sébilo A, Casin C, Lebel B, Rouvillain J-L, Chapuis S, Bonnevialle P, et al. Clinical and technical factors influencing outcomes of unicompartmental knee arthroplasty: retrospective multicentre study of 944 knees. Orthop Traumatol Surg Res. 2013;99(4 Suppl):S227–34.
Xing Z, Katz J, Jiranek W. Unicompartmental knee arthroplasty: factors influencing the outcome. J Knee Surg. 2012;25(5):369–73.
Carlos Rodríguez-Merchán E, Gómez-Cardero P. Unicompartmental knee arthroplasty: current indications, technical issues and results. EFORT Open Rev. 2018;3(6):363–73.
Cody JP, Pfefferle KJ, Ammeen DJ, Fricka KB. Is outpatient unicompartmental knee arthroplasty safe to perform at an ambulatory surgery center? A comparative study of early post-operative complications. J Arthroplast. 2018;33(3):673–6.
Kort NP, Bemelmans YFL, Schotanus MGM. Outpatient surgery for unicompartmental knee arthroplasty is effective and safe. Knee Surg Sports Traumatol Arthrosc. 2017;25(9):2659–67.
Cross MB, Berger R. Feasibility and safety of performing outpatient unicompartmental knee arthroplasty. Int Orthop. 2014;38(2):443–7.
White SH, Ludkowski PF, Goodfellow JW. Anteromedial osteoarthritis of the knee. J Bone Joint Surg Br. 1991;73(4):582–6.
Jennings JM, Kleeman-Forsthuber LT, Bolognesi MP. Medial unicompartmental arthroplasty of the knee. J Am Acad Orthop Surg [Internet]. 2018; Available from: https://doi.org/10.5435/JAAOS-D-17-00690.
Chalmers BP, Mehrotra KG, Sierra RJ, Pagnano MW, Taunton MJ, Abdel MP. Reliable outcomes and survivorship of unicompartmental knee arthroplasty for isolated compartment osteonecrosis. Bone Joint J. 2018;100-B(4):450–4.
Berend KR, Berend ME, Dalury DF, Argenson J-N, Dodd CA, Scott RD. Consensus statement on indications and contraindications for medial unicompartmental knee arthroplasty. J Surg Orthop Adv. 2015;24(4):252–6.
Hamilton TW, Pandit HG, Jenkins C, Mellon SJ, Dodd CAF, Murray DW. Evidence-based indications for mobile-bearing unicompartmental knee arthroplasty in a consecutive cohort of thousand knees. J Arthroplast. 2017;32(6):1779–85.
Richardson AB, Morris MJ. Medial unicompartmental knee arthroplasty. Instr Course Lect. 2017;66:201–9.
Iacono F, Raspugli GF, Akkawi I, Bruni D, Filardo G, Budeyri A, et al. Unicompartmental knee arthroplasty in patients over 75 years: a definitive solution? Arch Orthop Trauma Surg. 2016;136(1):117–23.
Siman H, Kamath AF, Carrillo N, Harmsen WS, Pagnano MW, Sierra RJ. Unicompartmental knee arthroplasty vs total knee arthroplasty for medial compartment arthritis in patients older than 75 years: comparable reoperation, revision, and complication rates. J Arthroplast. 2017;32(6):1792–7.
Kennedy JA, Matharu GS, Hamilton TW, Mellon SJ, Murray DW. Age and outcomes of medial meniscal-bearing unicompartmental knee arthroplasty. J Arthroplast. 2018;33(10):3153–9.
Heyse TJ, Khefacha A, Peersman G, Cartier P. Survivorship of UKA in the middle-aged. Knee. 2012;19(5):585–91.
Biswas D, Van Thiel GS, Wetters NG, Pack BJ, Berger RA, Della Valle CJ. Medial unicompartmental knee arthroplasty in patients less than 55 years old: minimum of two years of follow-up. J Arthroplast. 2014;29(1):101–5.
Krych AJ, Reardon P, Sousa P, Pareek A, Stuart M, Pagnano M. Unicompartmental knee arthroplasty provides higher activity and durability than Valgus-producing proximal tibial osteotomy at 5 to 7 years. J Bone Joint Surg Am. 2017;99(2):113–22.
Kim KT, Lee S, Lee JS, Kang MS, Koo KH. Long-term clinical results of unicompartmental knee arthroplasty in patients younger than 60 years of age: minimum 10-year follow-up. Knee Surg Relat Res. 2018;30(1):28–33.
Cavaignac E, Lafontan V, Reina N, Pailhé R, Wargny M, Laffosse JM, et al. Obesity has no adverse effect on the outcome of unicompartmental knee replacement at a minimum follow-up of seven years. Bone Joint J. 2013;95-B(8):1064–8.
Zengerink I, Duivenvoorden T, Niesten D, Verburg H, Bloem R, Mathijssen N. Obesity does not influence the outcome after unicompartmental knee arthroplasty. Acta Orthop Belg. 2015;81(4):776–83.
Woo YL, Chen YQJ, Lai MC, Tay KJD, Chia S-L, Lo NN, et al. Does obesity influence early outcome of fixed-bearing unicompartmental knee arthroplasty? J Orthop Surg. 2017;25(1):2309499016684297.
Plate JF, Augart MA, Seyler TM, Bracey DN, Hoggard A, Akbar M, et al. Obesity has no effect on outcomes following unicompartmental knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. 2017;25(3):645–51.
Song E-K, Park J-K, Park C-H, Kim M-C, Agrawal PR, Seon JK. No difference in anterior knee pain after medial unicompartmental knee arthroplasty in patients with or without patellofemoral osteoarthritis. Knee Surg Sports Traumatol Arthrosc. 2016;24(1):208–13.
Adams AJ, Kazarian GS, Lonner JH. Preoperative patellofemoral chondromalacia is not a contraindication for fixed-bearing medial unicompartmental knee arthroplasty. J Arthroplast. 2017;32(6):1786–91.
Hamilton TW, Choudhary R, Jenkins C, Mellon SJ, Dodd CAF, Murray DW, et al. Lateral osteophytes do not represent a contraindication to medial unicompartmental knee arthroplasty: a 15-year follow-up. Knee Surg Sports Traumatol Arthrosc. 2017;25(3):652–9.
Hernigou P, Deschamps G. Posterior slope of the tibial implant and the outcome of unicompartmental knee arthroplasty. J Bone Joint Surg Am. 2004;86-A(3):506–11.
Engh GA, Ammeen DJ. Unicondylar arthroplasty in knees with deficient anterior cruciate ligaments. Clin Orthop Relat Res. 2014;472(1):73–7.
Pandit H, Beard DJ, Jenkins C, Kimstra Y, Thomas NP, Dodd CAF, et al. Combined anterior cruciate reconstruction and Oxford unicompartmental knee arthroplasty. J Bone Joint Surg Br. 2006;88(7):887–92.
Ventura A, Legnani C, Terzaghi C, Iori S, Borgo E. Medial unicondylar knee arthroplasty combined to anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc. 2017;25(3):675–80.
Mallory TH, Danyi J. Unicompartmental total knee arthroplasty. A five- to nine-year follow-up study of 42 procedures. Clin Orthop Relat Res. 1983;175:135–8.
Whittaker J-P, Naudie DDR, McAuley JP, McCalden RW, MacDonald SJ, Bourne RB. Does bearing design influence midterm survivorship of unicompartmental arthroplasty? Clin Orthop Relat Res. 2010;468(1):73–81.
Parratte S, Pauly V, Aubaniac J-M, Argenson J-NA. No long-term difference between fixed and mobile medial unicompartmental arthroplasty. Clin Orthop Relat Res. 2012;470(1):61–8.
Peersman G, Stuyts B, Vandenlangenbergh T, Cartier P, Fennema P. Fixed- versus mobile-bearing UKA: a systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc. 2015;23(11):3296–305.
Neufeld ME, Albers A, Greidanus NV, Garbuz DS, Masri BA. A comparison of mobile and fixed-bearing unicompartmental knee arthroplasty at a minimum 10-year follow-up. J Arthroplast. 2018;33(6):1713–8.
Ozcan C, Simsek ME, Tahta M, Akkaya M, Gursoy S, Bozkurt M. Fixed-bearing unicompartmental knee arthroplasty tolerates higher variance in tibial implant rotation than mobile-bearing designs. Arch Orthop Trauma Surg. 2018;138(10):1463–9.
Forster-Horváth C, Artz N, Hassaballa MA, Robinson JR, Porteous AJ, Murray JR, et al. Survivorship and clinical outcome of the minimally invasive Uniglide medial fixed bearing, all-polyethylene tibia, unicompartmental knee arthroplasty at a mean follow-up of 7.3years. Knee. 2016;23(6):981–6.
Hawi N, Plutat J, Kendoff D, Suero EM, Cross MB, Gehrke T, et al. Midterm results after unicompartmental knee replacement with all-polyethylene tibial component: a single surgeon experience. Arch Orthop Trauma Surg. 2016;136(9):1303–7.
Rouanet T, Combes A, Migaud H, Pasquier G. Do bone loss and reconstruction procedures differ at revision of cemented unicompartmental knee prostheses according to the use of metal-back or all-polyethylene tibial component? Orthop Traumatol Surg Res. 2013;99(6):687–92.
Hutt JRB, Farhadnia P, Massé V, LaVigne M, Vendittoli P-A. A randomised trial of all-polyethylene and metal-backed tibial components in unicompartmental arthroplasty of the knee. Bone Joint J. 2015;97-B(6):786–92.
Koh IJ, Suhl KH, Kim MW, Kim MS, Choi KY, In Y. Use of all-polyethylene tibial components in unicompartmental knee arthroplasty increases the risk of early failure. J Knee Surg. 2017;30(8):807–15.
van der List JP, Kleeblad LJ, Zuiderbaan HA, Pearle AD. Mid-term outcomes of metal-backed unicompartmental knee arthroplasty show superiority to all-polyethylene unicompartmental and total knee arthroplasty. HSS J. 2017;13(3):232–40.
Scott CEH, Wade FA, MacDonald D, Nutton RW. Ten-year survival and patient-reported outcomes of a medial unicompartmental knee arthroplasty incorporating an all-polyethylene tibial component. Arch Orthop Trauma Surg. 2018;138(5):719–29.
Small SR, Berend ME, Ritter MA, Buckley CA, Rogge RD. Metal backing significantly decreases tibial strains in a medial unicompartmental knee arthroplasty model. J Arthroplast. 2011;26(5):777–82.
Scott CEH, Eaton MJ, Nutton RW, Wade FA, Evans SL, Pankaj P. Metal-backed versus all-polyethylene unicompartmental knee arthroplasty: proximal tibial strain in an experimentally validated finite element model. Bone Joint Res. 2017;6(1):22–30.
van der List JP, Sheng DL, Kleeblad LJ, Chawla H, Pearle AD. Outcomes of cementless unicompartmental and total knee arthroplasty: a systematic review. Knee. 2017;24(3):497–507.
Campi S, Pandit HG, Dodd CAF, Murray DW. Cementless fixation in medial unicompartmental knee arthroplasty: a systematic review. Knee Surg Sports Traumatol Arthrosc. 2017;25(3):736–45.
Ollivier M, Parratte S, Lunebourg A, Viehweger E, Argenson J-N. The John Insall award: no functional benefit after unicompartmental knee arthroplasty performed with patient-specific instrumentation: a randomized trial. Clin Orthop Relat Res. 2016;474(1):60–8.
Alvand A, Khan T, Jenkins C, Rees JL, Jackson WF, Dodd CAF, et al. The impact of patient-specific instrumentation on unicompartmental knee arthroplasty: a prospective randomised controlled study. Knee Surg Sports Traumatol Arthrosc. 2018;26(6):1662–70.
Lonner JH, Klement MR. Robotic-assisted medial unicompartmental knee arthroplasty: options and outcomes. J Am Acad Orthop Surg [Internet]. 2018; Available from: https://doi.org/10.5435/JAAOS-D-17-00710.
Fu J, Wang Y, Li X, Yu B, Ni M, Chai W, et al. Robot-assisted vs. conventional unicompartmental knee arthroplasty: systematic review and meta-analysis. Orthopade [Internet]. 2018; Available from: https://doi.org/10.1007/s00132-018-3604-x.
Lyons MC, MacDonald SJ, Somerville LE, Naudie DD, McCalden RW. Unicompartmental versus total knee arthroplasty database analysis: is there a winner? Clin Orthop Relat Res. 2012;470(1):84–90.
Horikawa A, Miyakoshi N, Shimada Y, Kodama H. Comparison of clinical outcomes between total knee arthroplasty and unicompartmental knee arthroplasty for osteoarthritis of the knee: a retrospective analysis of preoperative and postoperative results. J Orthop Surg Res. 2015;10:168.
Kim MS, Koh IJ, Choi YJ, Lee JY, In Y. Differences in patient-reported outcomes between unicompartmental and total knee arthroplasties: a propensity score-matched analysis. J Arthroplast. 2017;32(5):1453–9.
Burn E, Sanchez-Santos MT, Pandit HG, Hamilton TW, Liddle AD, Murray DW, et al. Ten-year patient-reported outcomes following total and minimally invasive unicompartmental knee arthroplasty: a propensity score-matched cohort analysis. Knee Surg Sports Traumatol Arthrosc. 2018;26(5):1455–64.
Brown NM, Sheth NP, Davis K, Berend ME, Lombardi AV, Berend KR, et al. Total knee arthroplasty has higher postoperative morbidity than unicompartmental knee arthroplasty: a multicenter analysis. J Arthroplast. 2012;27(8 Suppl):86–90.
Liddle AD, Judge A, Pandit H, Murray DW. Adverse outcomes after total and unicompartmental knee replacement in 101,330 matched patients: a study of data from the National Joint Registry for England and Wales. Lancet. 2014;384(9952):1437–45.
Burn E, Liddle AD, Hamilton TW, Pai S, Pandit HG, Murray DW, et al. Choosing between unicompartmental and total knee replacement: what can economic evaluations tell us? A systematic review. Pharmacoecon Open. 2017;1(4):241–53.
Vasso M, Del Regno C, Perisano C, D’Amelio A, Corona K, Schiavone PA. Unicompartmental knee arthroplasty is effective: ten year results. Int Orthop. 2015;39(12):2341–6.
Winnock de Grave P, Barbier J, Luyckx T, Ryckaert A, Gunst P, Van den Daelen L. Outcomes of a fixed-bearing, medial, cemented unicondylar knee arthroplasty design: survival analysis and functional score of 460 cases. J Arthroplast. 2018;33(9):2792–9.
van der List JP, McDonald LS, Pearle AD. Systematic review of medial versus lateral survivorship in unicompartmental knee arthroplasty. Knee. 2015;22(6):454–60.
Liddle AD, Pandit H, Judge A, Murray DW. Effect of surgical caseload on revision rate following total and unicompartmental knee replacement. J Bone Joint Surg Am. 2016;98(1):1–8.
van der List JP, Zuiderbaan HA, Pearle AD. Why do medial unicompartmental knee arthroplasties fail today? J Arthroplast. 2016;31(5):1016–21.
Vasso M, Corona K, D’Apolito R, Mazzitelli G, Panni AS. Unicompartmental knee arthroplasty: modes of failure and conversion to total knee arthroplasty. Joints. 2017;5(1):44–50.
Collier MB, Eickmann TH, Sukezaki F, McAuley JP, Engh GA. Patient, implant, and alignment factors associated with revision of medial compartment unicondylar arthroplasty. J Arthroplast. 2006;21(6 Suppl 2):108–15.
Vasso M, Del Regno C, D’Amelio A, Viggiano D, Corona K, Schiavone PA. Minor varus alignment provides better results than neutral alignment in medial UKA. Knee. 2015;22(2):117–21.
Järvenpää J, Kettunen J, Miettinen H, Kröger H. The clinical outcome of revision knee replacement after unicompartmental knee arthroplasty versus primary total knee arthroplasty: 8-17 years follow-up study of 49 patients. Int Orthop. 2010;34(5):649–53.
Craik JD, El Shafie SA, Singh VK, Twyman RS. Revision of unicompartmental knee arthroplasty versus primary total knee arthroplasty. J Arthroplast. 2015;30(4):592–4.
Leta TH, Lygre SHL, Skredderstuen A, Hallan G, Gjertsen J-E, Rokne B, et al. Outcomes of unicompartmental knee arthroplasty after aseptic revision to total knee arthroplasty: a comparative study of 768 TKAs and 578 UKAs revised to TKAs from the Norwegian Arthroplasty register (1994 to 2011). JBJS. 2016;98(6):431–40.
Sun X, Su Z. A meta-analysis of unicompartmental knee arthroplasty revised to total knee arthroplasty versus primary total knee arthroplasty. J Orthop Surg Res. 2018;13(1):158.
Lee JK, Kim HJ, Park JO, Yang J-H. Inferior outcome of revision of unicompartmental knee arthroplasty to total knee arthroplasty compared with primary total knee arthroplasty: systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc. 2018;26(11):3403–18.
Crawford DA, Berend KR, Lombardi AV. Management of the failed medial unicompartmental knee arthroplasty. J Am Acad Orthop Surg. 2018;26(20):e426–33.
Lunebourg A, Parratte S, Galland A, Lecuire F, Ollivier M, Argenson J-N. Is isolated insert exchange a valuable choice for polyethylene wear in metal-backed unicompartmental knee arthroplasty? Knee Surg Sports Traumatol Arthrosc. 2016;24(10):3280–6.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Fuller, B.C., Gerlinger, T.L. (2020). Medial Unicompartmental Knee Arthroplasty: Indications and Technique. In: Gerlinger, T. (eds) Unicompartmental Knee Arthroplasty. Springer, Cham. https://doi.org/10.1007/978-3-030-27411-5_7
Download citation
DOI: https://doi.org/10.1007/978-3-030-27411-5_7
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-27410-8
Online ISBN: 978-3-030-27411-5
eBook Packages: MedicineMedicine (R0)