Abstract
Introduction
Although neurological complications are well recognized in patients with sickle cell disease, myelopathy has been rarely described, with few reported cases of compressive and ischemic myelopathy. We present the first case report of longitudinally extensive myelitis (LETM) in SCD and review the differential diagnosis of myelopathy in these patients.
Case presentation
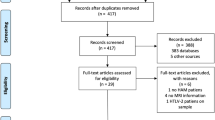
We report the case of a 29-year-old African-Brazilian man with SCD, who experienced a subacute flaccid paraparesis, with T2 sensory level and urinary retention. Cerebrospinal fluid analysis showed a lymphocytic pleocytosis and increased protein levels. MRI disclosed a longitudinally extensive spinal cord lesion, with a high T2/STIR signal extending from C2 to T12. We searched Medline/PubMed, Embase, Scopus, and Google Scholar databases for myelopathy in SCD patients.
Discussion
Spinal cord compression by vertebral fractures, extramedullary hematopoietic tissue, and Salmonella epidural abscess have been reported in SCD. We found only three case reports of spinal cord infarction, which is unexpectedly infrequent compared to the prevalence of cerebral infarction in SCD. We found only one case report of varicella-zoster myelitis and no previous report of LETM in SCD patients. Specific and time-sensitive causes of myelopathy should be considered in SCD patients. In addition to compression and ischemia, LETM is a possible mechanism of spinal cord involvement in SCD patients.
Similar content being viewed by others
Introduction
Sickle cell disease (SCD) is associated with various neurologic complications, including silent and overt cerebral infarction, intracerebral hemorrhage, bacterial meningitis, headache, seizures, neuro-ophthalmological disorders, hearing impairment, neuropathy, and cognitive dysfunction [1,2,3]. Despite common neurological manifestations, spinal cord involvement is rarely described in SCD [1].
Compressive and non-compressive myelopathy have been described in SCD patients. Compressive myelopathy has been associated with vertebral compressive fractures [4], cord compression by extramedullary hematopoietic tissue [5], and Salmonella spp. epidural abscess [6, 7]. Rare case reports of spinal cord infarction, and a single case of infectious myelitis have been described [8,9,10,11].
We conducted a scoping review of the available literature to assess the association between SCD and all major causes of spinal cord injury. In addition, this is the first case report of a longitudinally extensive transverse myelitis (LETM) in a SCD patient.
Methods
We searched electronic databases: Medline/PubMed, Embase, Scopus, and Google Scholar from February 1, 2021, to March 15, 2021. Search strategy with Boolean operators included: “sickle cell” AND “neuro*”; “sickle cell” AND “myelopathy”; “sickle cell” AND “spinal cord”; sickle cell” AND “myelitis”; “sickle cell” AND ischemia”; “sickle cell” AND “neuromyelitis”; “sickle cell” AND “multiple sclerosis”; “sickle cell” AND “sarcoidosis”; “sickle cell” AND “connective tissue”; “sickle cell” AND “lupus”; “hemoglobinopathy” AND “neuro*“. Manuscripts were initially selected by title and abstract, and those considered most relevant were selected for full review. We also performed a manual review of the references of the selected articles to find additional relevant ones. Studies were not restricted by design, and had to be available in English.
Standard Protocol Approvals, Registrations, and Patient Consents
This study used de-identified data and was determined to be exempt from review by the University of São Paulo Review Board. Written informed consent-to-disclose was obtained from the patient for the publication of this case-oriented review.
Case presentation
A 29-year-old African-Brazilian man with SCD presented to a community hospital with an acute episode of right leg pain, not associated with trauma. He was treated with analgesics, and discharged after a few hours of observation. After 5 days, he noted significant worsening of the pain, involving the left leg, and difficulty walking, due to bilateral leg weakness, worse on the left. Over the following 2 weeks, he reported gradual progression of leg weakness, as well as progressive ascending numbness up to the chest. Approximately 6 days after symptom onset the patient required intermittent unilateral assistance to walk. Three days later, he needed bilateral assistance to stand and walk, and after nearly 3 days he was bedridden. He also noted urinary incontinence, constipation, and erectile dysfunction. The patient was hospitalized, and 5 days later was transferred to our hospital. A timeline showing the patient’s clinical course is displayed in Fig. 1.
Relevant medical history included recurrent vaso-occlusive episodes, two previous episodes of acute chest syndrome, avascular femoral head necrosis, osteomyelitis, and splenic sequestration crisis. He was lost to follow-up for about 3 years. He failed to comply with various hydroxyurea treatment trials, and underwent multiple blood transfusions.
On arrival to our hospital, he was alert and oriented. He had had muscle strength grade 0/5 in his lower extremities a flaccid paraparesis with downgoing toes, and preserved arm strength. He had pinprick, temperature, proprioceptive, and vibration sensory loss, with a T2 sensory level, and urinary retention (T2 AIS A paraplegia). Cranial nerve exam was normal. Physical examination was otherwise unremarkable, except for a grade two sacral pressure ulcer.
Head and neck CT were unremarkable. Brain and whole spine MRI showed a longitudinally extensive spinal cord swelling, with T2/STIR hyperintensities extending from C2 to T12. Lesions involved more than half of the cord cross-sectional area, including the posterior funiculus (Fig. 2).
A T2-weighted sagittal images of the cervical and thoracic spine showing longitudinally extensive spinal cord lesion, with increased signal involving C2 to T12 with cord swelling. B Axial T2-weighted MRI images at T4 level disclosing increased signal affecting more than half of the cross-sectional cord area. C Brain MRI FLAIR sequences showing increased signal in the deep white matter, predominantly in perivascular spaces.
Brain MRI demonstrated deep white matter T2 hyperintensities, predominantly in perivascular spaces. Some brain lesions showed restricted diffusion, and some were associated with microbleeds. Brain lesions predominated in the left frontobasal region, temporal lobe, and right subinsular region (Fig. 2). Spine and brain lesions were non-contrast enhancing. Magnetic resonance angiography was normal.
A lumbar puncture showed 155 cells/μL, 90% lymphocytes, 7% monocytes, and 1% neutrophils, elevated protein levels (0.79 g/L), and a mild IgG elevation. Glucose, lactate, oligoclonal bands, mycobacterial, and a viral PCR panel and cultures were negative or within normal range.
Laboratory test data included Hb 8.6 g/dL and HCT 27.2%, HbS 93%, HbA2 6%, and HbF 1% on hemoglobin electrophoresis. White blood cell, platelet counts, electrolytes, liver, and renal function tests were normal. Erythrocyte sedimentation rate, C-reactive protein, antinuclear antibody, anti-Ro (SS-A), anti-La (SS-B), rheumatoid factor, C3, C4, thyroid antibodies, antiphospholipid antibodies, glycemic and lipid profiles, vitamin B12 were normal. Folic acid was low (2.2 ng/mL). Hepatitis B and C, HIV, syphilis, Epstein–Barr, cytomegalovirus, varicella-zoster, herpes simplex, Schistosoma mansoni, and HTLV antibodies were negative. Peripheral blood and urine cultures were negative.
Neuro-ophthalmology found no evidence of optic neuritis. Serum anti-aquaporin-4 antibody (AQP-IgG) was negative (cell-based assay). MOG-IgG antibody was not available in our service.
He was admitted to the Neurology service, and received a 5-day course of 1 g/day intravenous methylprednisolone, without significant improvement. He simultaneously underwent total plasma exchange, complicated by recurrent bacteremia and hypotension. The procedure was discontinued after the fourth session (one total plasma volume exchanged per session). No additional benefit was observed. Exchange transfusion was considered for a possible ischemic myelopathy, but was contraindicated due to the patient’s alloimmunization profile, rendering it impossible to obtain the necessary amount of compatible RBC products to be transfused.
Over the following days, the patient presented complications, including urinary tract infection, acute thoracic syndrome, and worsening of the sacral pressure ulcer, requiring surgery.
Two months after the onset of paralysis, the patient was still in hospital for pressure ulcer surgical treatment. He was clinically stable, undergoing physical and occupational therapy sessions. A repeat MRI showed partial resolution of both LETM and brain lesions (Fig. 3), with unchanged neurologic status, except for leg spasticity. The patient remained wheelchair bound and required intermittent bladder catheterization.
Discussion
Differential diagnosis of spinal cord disease is extensive, and includes compressive, vascular, inflammatory, and infectious diseases [12]. Compressive and non-compressive myelopathy are rare neurological complications of SCD. Compressive myelopathy in SCD has been associated with vertebral fractures [4, 13], Salmonella spp. epidural abscess [6, 7], and extramedullary hematopoietic tissue [5]. In addition, SCD patients have a significantly increased risk of perioperative complications when undergoing instrumented spinal surgery [4]. Spinal cord compression by extramedullary hematopoietic tissue has been described mainly in thalassemia, with few reports in SCD patients [5, 14]. Timely diagnosis of spinal cord involvement is important, as surgical decompression and radiation therapy are effective in treating cord compression [15].
In SCD patients, spinal cord infarction appears to be an even rarer complication. There are only three reported cases [8,9,10]. The first case was reported in 1970, describing a 59-year-old Jamaican woman with sickle cell trait who presented with a stepwise decline over several years to near-complete paraplegia. Postmortem studies revealed a slightly swollen cervical cord, and atrophic thoracic and lumbar spinal segments. Autopsy study of spinal vessels revealed arteries and veins distention, with abnormally shaped sickle red cells [8]. A 1980 case report described a 19-year-old African-American man with SCD, who presented with sudden-onset quadriplegia. Multiple focal and confluent infarcts involving the cervical, thoracic, and lumbar spine, as well as cortical and subcortical white matter infarcts were found on autopsy [9]. An additional report presented the case of a 19-year-old African-American man with SCD, who experienced sudden-onset quadriplegia. Diffusion-weighted spinal MRI showed restricted diffusion, consistent with an anterior spinal infarct. CSF analysis was unremarkable [10]. Spinal cord ischemia in SCD appears to be unexpectedly infrequent, compared to the higher prevalence of cerebral infarcts. Spinal cord infarction might be missed in SCD individuals presenting with neurologic symptoms [10]. Interestingly, posterior circulation vessels are rarely affected in SCD [3].
Infectious myelitis has been reported in SCD patients. A 17-year-old woman was diagnosed with herpes zoster after a 10-day history of fever, gastrointestinal symptoms, and a typical vesicular rash over the left chest. She was started on acyclovir, but after 3 days she developed progressive paraparesis, worse in the right leg, with a T4 sensory level, and urinary incontinence. The patient’s spinal T2 MRI revealed a high signal cord intensity from T4 to T6 levels. CSF analysis revealed a positive polymerase chain reaction for varicella-zoster, and she was successfully treated with intravenous dexamethasone [11]. Although there are case reports of acute transverse myelitis associated with Salmonella and Streptococcus pneumoniae bacteremia in non-SCD patients, we were unable to find reports of Salmonella or pneumococcal myelitis in SCD, despite increased susceptibility of bacteremia due to encapsulated agents in these patients [16, 17].
The differential diagnosis of LETM is broad, and includes neuromyelitis optica spectrum disorders (NMOSD), MOG-IgG-associated disease, and systemic diseases such as sarcoidosis, systemic lupus erythematosus, and Behçet’s syndrome. Vascular, neoplastic, infectious, and nutritional causes can also present as LETM, and should be considered in the differential diagnosis [18].
In our case, clinical, MRI and CSF features were consistent with the diagnosis of an inflammatory myelopathy. The temporal symptom profile is an important factor in the etiologic diagnosis of myelopathy. While a subacute progression (48 h–21 days) is more frequently observed in inflammatory myelopathy, ischemia presents more often with hyperacute onset (<6 h). MRI features in our patient, including posterior cord involvement with simultaneous demyelinating lesions in the brain favored the diagnosis of myelitis. Significant lesion reduction on control MRI after immunosuppressive therapy also favors the diagnosis of an inflammatory etiology, since residual signal abnormalities are usually observed in spinal cord ischemia [19, 20]. Lastly, marked pleocytosis in CSF further supports the diagnosis of inflammatory myelitis [21]. Other possible etiologies (e.g., neoplastic, nutritional, and infectious) were ruled out based on neuroaxis and systemic imaging, along with laboratory tests.
Despite extensive investigation in our case, we were unable to identify a clear causative factor. The patient did not meet diagnostic criteria for NMOSD, since he had a negative serum AQP4-IgG, one core clinical characteristic (acute myelitis) only, and brain lesions were asymptomatic [22]. The absence of bright spotty lesions, gadolinium-enhancement, and AQP4-IgG antibody make the diagnosis of NMOSD less likely.
We found no consistent evidence of association between inflammatory neurological disorders, including multiple sclerosis, NMOSD, and MOG-IgG-associated disease, and SCD, based on electronic database search. The unique inflammatory pathophysiology of SCD may have contributed to our patient’s uncommon presentation, although the paucity of cases does not allow us to postulate any particular risk factor for myelitis in SCD [23].
One of the limitations of our report is that diffusion-weighted images were not performed due to technical issues. Diffusion-weighted MRI could have contributed to the differential diagnosis of ischemic myelopathy, as restricted diffusion is consistent with spinal cord infarction [10]. Another limitation is that MOG-IgG antibody testing was not available at our service. Anti-MOG testing is generally recommended in AQP4-IgG negative LETM patients [22]. It is worth noting, however, that SCD is relatively common in low-income countries with a population with African ancestry.
In our case, the delay in diagnosis and treatment may have contributed to the poor treatment response and clinical outcome. This report should alert health professionals caring for SCD patients to be vigilant to the possibility of inflammatory and other time-sensitive etiologies of myelopathy in individuals with SCD presenting with neurologic symptoms.
Conclusions
Although rare, myelopathy is a possible complication of SCD. In addition to compression and ischemia, LETM should be included in the differential diagnosis of spinal cord lesions in SCD patients. Association of LETM and SCD should be further investigated in future studies, since early recognition and treatment of LETM have a significant impact on outcome.
Data availability
Data were obtained from the patient’s medical record, with the patient’s agreement. Patient personal information—including name or picture —is not mentioned in the text.
References
Sarnaik SA, Lusher JM. Neurological complications of sickle cell anemia. Am J Pediatr Hematol Oncol. 1982;4:386–94.
Holmstedt C, Adams RJ. Neurologic Complications of Hemoglobinopathies. Continuum 2011;17:56–72.
Farooq S, Testai FD. Neurologic complications of sickle cell disease. Curr Neurol Neurosci Rep. 2019;19:1–8.
Rudy HL, Yang D, Nam AD, Cho W. Review of sickle cell disease and spinal pathology. Glob Spine J. 2019;9:761–6.
Lewkow LM, Shah I. Sickle cell anemia and epidural extramedullary hematopoiesis. Am J Med. 1984;76:748–51.
Gardner RV. Salmonella vertebral osteomyelitis and epidural abscess in a child with sickle cell anemia. Pediatr Emerg Care. 1985;1:87–9.
Khoo HW, Chua YY, Chen JL. Salmonella typhi vertebral osteomyelitis and epidural abscess. Case Rep Orthop. 2016;2016:1–3.
Wolman L, Hardy AG. Spinal cord infarction associated with the sickle cell trait. Spinal Cord. 1970;7:282–91.
Rothman SM, Nelson JS. Spinal cord infarction in a patient with sickle cell anemia. Neurology. 1980;30:1072.
Márquez JC, Granados AM, Castillo M. MRI of cervical spinal cord infarction in a patient with sickle cell disease. Clin Imaging. 2012;36:595–8.
Mousali YM, Sobhi EM, Makkawi SO. Zoster myelitis in sickle cell anemia. Neurosci (Riyadh). 2011;16:273–5.
Kaplin AI, Krishnan C, Deshpande DM, Pardo CA, Kerr DA. Diagnosis and management of acute myelopathies. Neurologist. 2005;11:2–18.
Olaniyi JA, Alagbe K. Spinal Cord Discitis and Pathological Lumbar Fracture in a Sickle Cell Anaemia Patient: a case report. Int J Med Sci Public Health. 2015;48:1709.
Papavasiliou C, Gouliamos A, Vlahos L, Trakadas S, Kalovidouris A, Pouliades GR. CT and MRI of symptomatic spinal involvement by extramedullary haemopoiesis. Clin Radio. 1990;42:91–2.
Salehi SA, Koski T, Ondra SL. Spinal cord compression in beta-thalassemia: case report and review of the literature. Spinal Cord. 2004;42:117–23.
Sato DK, Callegaro D, Lana-Peixoto MA, Nakashima I, Fujihara K. Seronegative Neuromyelitis Optica Spectrum-The challenges on disease definition and pathogenesis. Arq Neuropsiquiatr. 2014;72:445–50.
Richert ME, Hosier H, Weltz AS, Wise ES, Joshi M, Diaz JJ. Acute transverse myelitis associated with Salmonella Bacteremia: a case report. Am J Case Rep. 2016;17:929.
Trebst C, Raab P, Voss EV, Rommer P, Abu-Mugheisib M, Zettl UK. Longitudinal extensive transverse myelitis- it ‘s not all neuromyelitis optica. Nat Rev Neurol. 2011 Dec;7:688.
Alblas CL, Bouvy WH, à Nijeholt GJ, Boiten J. Acute spinal-cord ischemia: evolution of MRI findings. J Clin Neurol. 2012;8:218.
Grassner L, Klausner F, Wagner M, McCoy M, Golaszewski S, Leis S, et al. Acute and chronic evolution of MRI findings in a case of posterior spinal cord ischemia. Spinal Cord. 2014;52:S23–4.
Barreras P, Fitzgerald KC, Mealy MA, Jimenez JA, Becker D, Newsome SD, et al. Clinical biomarkers differentiate myelitis from vascular and other causes of myelopathy. Neurology. 2018;90:e12–21.
Wingerchuk DM, Banwell B, Bennett JL, Cabre P, Carroll W, Chitnis T, et al. International consensus diagnostic criteria for neuromyelitis optica spectrum disorders. Neurology. 2015;85:177–89.
Conran N, Belcher JD. Inflammation in sickle cell disease. Clin Hemorheol Microcirc. 2018;68:263–99.
Author contributions
Brum IV, Silva GD, Sodre DS, Nogueira FM, Pereira SLA, and Castro LHM made substantial contributions to the conception and design of the work, as well as acquisition, analysis, and interpretation of data; drafted the work or revised it critically for important intellectual content; approved the final version to be published; and agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Consent
Written consent was obtained from the patient.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Brum, I.V., Silva, G.D., Sodre, D.S. et al. Myelopathy in sickle cell disease: a case-oriented review. Spinal Cord Ser Cases 7, 85 (2021). https://doi.org/10.1038/s41394-021-00449-8
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41394-021-00449-8
- Springer Nature Limited