Abstract
Background
The optimal caffeine dosing in extremely premature neonates remains elusive. This study aimed to evaluate the impact of birth weight on caffeine pharmacokinetics and various dosing regimens.
Methods
In this pharmacokinetic simulation study, we generated the body weights (0–49 days of postnatal age [PNA]) of neonates <28 weeks gestational age with different birth weights (550, 750, and 1050 g). Their pharmacokinetic parameters were determined based on published pharmacokinetic models. Then, we simulated and compared the caffeine base concentration-time profiles of standard versus off-label caffeine citrate dose regimens.
Results
The half-life decreased and the weight-adjusted clearance increased more significantly in neonates with lower birth weights, resulting in lower caffeine plasma concentrations. The neonate with the lowest birth weight did not achieve a threshold trough concentration of 15 mg/L after receiving the standard dose (5 mg/kg/day), while the higher-birth-weights (≥750 g) had trough concentrations below the threshold around the second week of life. Higher caffeine doses (10 mg/kg/day) resulted in peak concentrations of <36 mg/L by 10–14 days of PNA while maintaining trough concentrations above 15 mg/L throughout the 49 days PNA.
Conclusion
Higher-than-standard caffeine dosing may be needed for extremely premature neonates, especially for those with lower birth weights.
Impact
-
Extremely premature neonates with a lower birth weight may require a higher weight-based caffeine dosing due to their higher weight-adjusted clearance and shorter half-lives.
-
Not only do these extremely premature neonates have a higher risk of developing bronchopulmonary dysplasia due to their structurally underdeveloped lungs, but the low birth weight-related underdosing may further contribute to the reduced caffeine effectiveness.
-
Higher-than-standard caffeine citrate dosing (e.g., 10 mg/kg/day maintenance dose) may be needed to further prevent bronchopulmonary dysplasia.
Similar content being viewed by others
Introduction
Apnea of prematurity (AOP) occurs in almost all extremely premature neonates (<28 weeks gestational age [GA]).1 AOP is associated with bronchopulmonary dysplasia (BPD) due to the lung injuries resulting from long-term oxygen use and mechanical ventilation.1,2 Caffeine is a respiratory stimulant that effectively treats AOP and reduces the rate of BPD.1,3 Despite the prevalent use of caffeine, BPD occurs in one-third of neonates <28 weeks GA.4 Not only do these extremely premature neonates have a higher risk of developing BPD due to their structurally underdeveloped lungs, but the optimal caffeine dosing in this population remains unknown.5,6 Caffeine has a US Food and Drug Administration (FDA)-labeled indication for AOP in neonates between 28 and 33 weeks GA, and the caffeine citrate standard dose regimen is a 20 mg/kg loading dose (LD) followed by a 5 mg/kg daily maintenance dose.7 In neonates with <28 weeks GA, doses larger than 5 mg/kg/day are commonly used off-label, aiming to improve the caffeine effectiveness.4,8 Identifying the optimal caffeine dosing in neonates <28 weeks GA may further reduce AOP and prevent BPD and the related complications.
In premature neonates, because rapid growth and maturation significantly affect drug distribution and elimination, the upward titration of caffeine doses during the first few weeks of life is needed to maintain a similar steady-state plasma concentration.9,10 Furthermore, neonates with different birth weights have different rates of weight gain; the birth weight could further complicate the relationship between the weight-based dose and caffeine plasma concentrations.11 For example, premature neonates with a lower birth weight gain weight slower; however, their postnatal caffeine clearance improves at a rate comparable to those with a higher birth weight.11,12,13 As a result, the caffeine clearance of neonates with lower birth weights improves relatively faster. Therefore, higher weight-based caffeine dosing may be needed for neonates with lower birth weight. To demonstrate the impact of birth weight on caffeine dosing, this study aimed to (1) compare the caffeine pharmacokinetics among premature neonates <28 weeks GA with different birth weight, and (2) evaluate the plasma concentrations obtained from off-label (>5 mg/kg/day) versus standard (5 mg/kg/day) caffeine dose regimens.
Methods
Study design
This was a pharmacokinetic simulation study of premature neonates. The simulation was performed using a similar approach described in a previous study by Koch et al.10 Briefly, the simulation involved three steps: (1) create virtual patients with body weight that changes from 0 to 49 days of postnatal age (PNA) based on the age-weight relationship published in the literature;11 (2) determine the pharmacokinetic parameters (i.e., clearance, volume of distribution [Vd], and half-life) based on published pharmacokinetic models that account for significant covariates (i.e., body weight, PNA, and GA); and (3) simulate caffeine base (one-half of the dose when expressed as caffeine citrate) concentration-time profiles of various caffeine citrate dosing regimens based on the pharmacokinetic parameters determined in the previous step. Institutional review board approval was waived, as this study did not meet the criteria for human subject research.
To evaluate the impact of birth weight on caffeine weight-based dosing, caffeine pharmacokinetics and plasma concentration were compared at various PNAs among neonates <28 weeks GA with different birth weight, who were given higher versus standard caffeine dose regimens. Caffeine base plasma concentrations of 15–20 mg/L have been suggested to be more efficacious than lower concentrations.10,14 For this study, 15 mg/L was used as a reference therapeutic threshold for caffeine therapy. Caffeine citrate dose regimens used in the simulation included (1) a 20 mg/kg LD followed by 5 mg/kg every 24 h (i.e., standard dose); (2) a 20 mg/kg LD followed by 5 mg/kg every 12 h (5BID); and (3) a 20 mg/kg LD followed by 10 mg/kg every 24 h (10Daily). The weight-based dosing was calculated for each day and accounted for the daily body weight.
Pharmacokinetic simulation
Caffeine pharmacokinetic parameters are influenced by body weight, GA, and PNA as described in the published pharmacokinetic models.15,16,17,18 Three virtual neonates categorized as extremely premature (<28 weeks GA) and with very low birth weight to extremely low birth weights (1050, 750, and 550 g) were selected in this study to compare the impact of birth weight on the pharmacokinetics of caffeine.19 Subsequently, the mathematical growth models reported by Ehrenkranz et al.11 were utilized to determine the daily body weight from 0 to 49 days of PNA. A neonate typically has an initial decrease in body weight, but will regain birth weight within 2 weeks, followed by a weight gain of approximately 15 g/kg/day.11 The weight-age relationships for neonates of different birth weight reported in Ehrenkranz et al.11 were expressed in a piecewise quadratic function; however, the estimated parameter values were not reported (see Supplementary material for details on the growth models). Growth curves were digitized using WebPlotDigitizer (http://automeris.io/WebPlotDigitizer/) and estimated the parameters using Phoenix® WinNonlin® version 8.3 (Certara, Inc., Princeton, NJ). The parameters that describe the weight change were then used to determine the daily body weight and the daily caffeine dose used in our simulations.
Using the body weight and PNA that were determined for each virtual patient from 0 to 49 days of PNA, their daily pharmacokinetic parameters were calculated. Similar to the approach described by Koch et al.,10 the pharmacokinetic parameters (i.e., clearance and Vd) in this study were determined using the average value of the pharmacokinetic parameters from the models by Charles et al.15 and Falcao et al.16 (see Supplementary material for details on the pharmacokinetic models). The pharmacokinetic models from other authors17,18 were not used as they either reported an abnormally high Vd or assumed a constant Vd. The weight-adjusted clearance was calculated using the daily clearance value divided by the daily body weight. Half-life (T1/2) was derived using the following equation:
Then, the caffeine base concentration-time profiles were estimated using the predicted pharmacokinetic parameters. A one-compartment model well described the caffeine pharmacokinetic profiles and was used for the simulation:
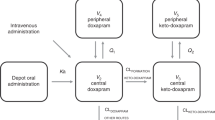
where C is the caffeine concentration, C0 is the concentration immediately after dosing, and t is time after dosing. Caffeine concentrations were calculated based on the amount of caffeine base administered, which is half that of caffeine citrate. As caffeine was given repeatedly, caffeine concentrations determined from the daily pharmacokinetic parameters of a virtual patient from nth dose superimposed the concentrations determined from the (n – 1)th dose, resulting in the accumulation of caffeine plasma concentration. The simulation used intravenous bolus administration as the route of administration, and caffeine therapy was initiated on the day of birth. Caffeine base concentration-time profile simulations were performed in RStudio version 1.4.1106 (PBC, Boston, MA).
Results
Body weights from 0 to 49 days of PNA of the three virtual neonates with 550, 750, and 1050 g birth weight that were extracted from the data reported by Enrenkranz et al.11 are shown in Fig. 1a. The simulated caffeine Vd, clearance, and half-life of the virtual neonates at each PNA are illustrated in Fig. 1b–d. The Vd of caffeine was directly proportional to their body weight; therefore, the changes in Vd over time resembled the changes in body weight (Fig. 1a, b). As such, both body weight and Vd slightly decreased during the first few days of life and increased thereafter, with neonates of lower birth weights having a slower rate of gaining body weight and Vd. As expected, neonates with greater birth weights had a higher clearance throughout the 49 days of PNA. While comparing half-lives (a function of clearance and Vd), the half-life of all virtual neonates shortened rapidly with increasing PNA. The half-life of the neonate with the lowest birth weight (550 g) decreased most significantly and became the shortest after a few days of life (Fig. 1d).
a Growth curves neonates with birth weights of 1050 g (solid line), 750 g (dashed line), and 550 g (dotted line) based on the data reported by Enrenkranz et al.10 b Changes in volume of distribution, c clearance, and d half-life from 0 to 49 days postnatal age.
After adjusting for the body weight, the clearance was higher in neonates with lower birth weights compared to those with higher birth weights (Fig. 2a). Consistently, the caffeine base plasma concentrations were lower among neonates with lower birth weights after receiving a caffeine citrate LD of 20 mg/kg followed by 5 mg/kg daily (Fig. 2b). The three neonates with <28 weeks GA and different birth weights had an initial increase in caffeine concentrations that peaked around 7–14 days PNA (peak concentration range: 17.6–18.9 mg/L; trough: 14.8–16.1 mg/L). After the 7–14 days PNA, the caffeine concentration decreased and stabilized around day 28 PNA (Fig. 2b). The neonates with birth weight of 750 and 1050 g achieved the therapeutic through concentration threshold within 7 days of therapy. However, the caffeine trough concentration fell below 15 mg/L at 12 and 16 days of PNA for the neonate with the birth weight of 750 and 1050 g, respectively. For the neonate with 550 g birth weight, the standard dose did not produce a caffeine trough concentration that is above the 15 mg/L therapeutic threshold throughout the first 49 days of life.
a Weight-adjusted clearance (CL) of neonates with birth weights of 550, 750, and 1050 g, and b simulated caffeine base concentration-time profiles of neonates <28 weeks gestational age with different birth weights who received a caffeine citrate loading dose of 20 mg/kg followed by a maintenance dose of 5 mg/kg once daily.
While comparing the various dosing regimens, the higher doses (5BID and 10Daily) resulted in caffeine concentrations that are greater than the 15 mg/L threshold within 2 days of therapy and stay above threshold through day 49 of PNA (Fig. 3a, b). These higher doses approached peak concentrations of <36 mg/L by 10–14 days of PNA, compared with a peak of <20 mg/L from the standard dose. Only slight differences in the caffeine concentration-time profiles were observed between the 5BID and 10Daily doses. The 10Daily dose produced 1–2 mg/L higher peak and lower trough concentrations compared with the 5BID dose (Fig. 3b).
a Simulated caffeine base concentration-time profiles of neonates <28 weeks gestational age with different birth weights who received a caffeine citrate loading dose of 20 mg/kg followed by a maintenance dose of 5 mg/kg twice daily. b Simulated caffeine base concentration-time profiles of neonates with a birth weight of 750 g who received a caffeine citrate loading dose of 20 mg/kg followed by a maintenance dose of 5 mg/kg twice daily versus 10 mg/kg once daily.
Discussion
Our simulations showed that the neonates <28 weeks GA with lower birth weights had lower weight-adjusted clearances, shorter half-lives, and lower plasma concentrations after receiving the FDA-labeled caffeine citrate dose regimen compared with those with higher birth weights. The trough concentrations of the neonate with the lowest birth weight (550 g) did not achieve the therapeutic threshold; meanwhile, the trough concentrations of the higher-birth-weight neonates fell below the threshold after 2 weeks. These findings suggest that the FDA-labeled weight-based caffeine dose regimen is insufficient in neonates <28 weeks GA, especially in those with a lower birth weight. Consistently, our previous study showed that two-thirds of premature neonates required a caffeine dose >5 mg/kg/day, which the majority of these requiring 10 mg/kg daily or 5 mg/kg twice daily.20
As caffeine is primarily (85%) excreted unchanged in the urine during the first few weeks of life, the rapid increase in renal function in premature neonates results in the increase in clearance and decrease in half-life of caffeine.21 Although renal function improves slower in premature neonates compared with the term neonates, the velocity of renal function improvement appeared to be comparable among premature neonates with birth weight <2500 g.13,22 Likewise in our simulations, the caffeine clearance increased at a similar rate for all neonates, with a slightly faster rate for the neonate with the highest birth weight of 1050 g (Fig. 1c). Since those with lower birth weight had a significantly smaller weight gain (Fig. 1a; 80 and 250 g weight gain by 28 days PNA for birth weights of 550 and 1050 g, respectively), their weight-adjusted clearance increased to a greater degree compared with those with higher birth weights (Fig. 2a). On the other hand, Vd increased in proportion to the body weight in all neonates. As the weight-adjusted Vd stayed constant, and weight-adjusted clearance increased, the resulting half-life decreased with neonatal growth. Because neonates with lower birth weights had higher weight-adjusted clearance compared with those with higher birth weights, they had shorter half-lives. Collectively, the results suggest that neonates with a lower birth weight require a higher weight-based caffeine dosing due to their higher weight-adjusted clearance and shorter half-lives.
Because of the increasingly higher weight-adjusted clearance among the lower-birth-weights, the constant weight-based dosing is expected to produce lower steady-state plasma concentrations over time compared with neonates with higher birth weights. Our simulations demonstrated that the virtual premature neonate with the lowest birth weight (i.e., 550 g) who received the standard dose had the lowest caffeine concentration and a higher risk of being subtherapeutic. A target caffeine base concentration of >15 mg/L was selected as it was associated with an increased efficacy of caffeine for AOP and a reduction in BPD occurance.14,23,24,25 Interestingly, the neonate with the lowest birth weight did not achieve the 15 mg/L trough target throughout the 49 days PNA. For neonates with birth weight ≥750 g, the caffeine trough concentration fell below the 15 mg/L threshold around 12–16 days of PNA. Therefore, all neonates <28 weeks GA are likely requiring doses higher than the standard caffeine citrate dose in order to achieve the therapeutic goal.
Doses higher than the standard dose have been shown to be beneficial in decreasing apnea frequency, improving neurodevelopmental outcomes, and preventing BPD among premature neonates with very low birth weight.6,26,27 In an observational study, Salemi et al.20 reported that neonates who received a standard caffeine dose regimen required a dose increase to >5 mg/kg/day around 2–3 weeks PNA, at a postmenstrual age of approximately 30 weeks in an effort to decrease the number of apnea events. The timing of such dosing increases coincides with the timing of our simulated caffeine trough concentration falling below the therapeutic threshold among neonates with birth weight ≥750 g. Using the 15 mg/L as the therapeutic threshold, Koch et al.10 suggested that for a neonate with 28 weeks of GA and birth weight of 1150 g, caffeine dosing should be increased by 1 mg/kg every 1–2 weeks to achieve stable caffeine concentrations that are above the threshold.10 However, this dosing strategy may not apply to neonates with different birth weights because of their various weight-adjusted clearance trajectories as shown in our simulations (Fig. 2a). On the contrary, Puia-Dumitrescu et al.4 reported that higher caffeine doses were not associated with the occurrence of BPD. This may be because their study included neonates <28 weeks GA who were initiated on caffeine at various PNAs. Early administration of caffeine has been associated with a lower rate of BPD.28,29
Higher caffeine doses and plasma concentrations >50 mg/L may increase the risk for adverse events such as tachycardia and ventricular hemorrhage.7,23,28 We found that higher caffeine doses (10Daily or 5BID) resulted in peak concentrations of <36 mg/L by 10–14 days of PNA, compared with a peak of <20 mg/L from the standard dose. Meanwhile, the trough concentrations remained above the 15 mg/L threshold throughout the 49 days of PNA. An additional adverse effect noted with caffeine is necrotizing enterocolitis, but Puia-Dumitrescu et al.4 noted that increased cumulative and daily caffeine dose were not associated with necrotizing enterocolitis. These findings suggest that the 10 mg/kg per day provides higher peak concentrations but no greater risk of adverse events than standard dosing.
A dose of 5 mg/kg/dose twice daily compared to 10 mg/kg/dose daily may provide a narrower range of plasma concentrations. However, our results have shown that the 10Daily and 5BID regimens produced concentration-time profiles with minimal difference (1–2 mg/L difference in peak and trough concentrations). A retrospective study by Rebentisch et al.30 compared the caffeine regimens (10Daily versus 5BID) and found no significant difference in the frequency of apneic and bradycardic events. However, Salemi et al.20 reported a higher rate of tachycardia that resulted in a dose decrease among neonates receiving 10Daily compared with those who received 5BID dose (22.0 versus 13.2%). However, it was a retrospective study; the authors only documented tachycardia that resulted in a dose decrease or discontinuation of caffeine and tachycardia may have been confounded by other factors such as the severity of illness.
Our study had limitations. First, this is a pharmacokinetic simulation study. Although both pharmacokinetic models used in our simulation were appropriately developed and were based on patients with demographics of typical premature neonates that require caffeine therapy, longitudinal evaluation of the pharmacokinetics of neonates with different birth weights may be needed to confirm our findings. Second, the variability of the pharmacokinetic parameters was not introduced in our simulation. However, we aimed to compare the mean pharmacokinetic parameter values and caffeine concentrations in order to illustrate the average impact of patient birth weight on the caffeine dosing regimens. Third, the pharmacodynamics (concentration-effect relationship) in neonates of different GA and PNA were not known. We assumed that maintaining a caffeine concentration within the 15–35 mg/L therapeutic range is beneficial for all age groups. Last, other patient factors such as organ functions and disease states that may confound the clinical outcomes (i.e., apnea and bradycardia) were not considered in our simulation. Polymorphisms related to caffeine outcomes in AOP have been reported.25
In summary, this simulation study showed that neonates with lower birth weight may be at a higher risk of having subtherapeutic caffeine concentrations. Although premature neonates with lower birth weight may have a higher risk of AOP and BPD due to less than ideal intrauterine growth and maturation, low birth weight-related underdosing as illustrated in our study may further reduce the effectiveness of caffeine.1,31 We propose that dosing higher than the standard caffeine citrate dose regimen (e.g., 10 mg/kg/day dosing) is needed to optimize the caffeine treatment of AOP and prevent long-term consequences such as BPD. Future large randomized, controlled trials are needed to determine the optimal caffeine dosing regimens and the effect of birth weight and postnatal weight gain should be considered.
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Eichenwald, E. C. AAP Committee on Fetus and Newborn Apnea of prematurity. Pediatrics 137, e20153757 (2016).
Zhao, J., Gonzalez, F. & Mu, D. Apnea of prematurity: from cause to treatment. Eur. J. Pediatr. 170, 1097–1105 (2011).
Schmidt, B. et al. Caffeine therapy for apnea of prematurity. N. Engl. J. Med. 354, 2112–2121 (2006).
Puia-Dumitrescu, M. et al. Dosing and safety of off-label use of caffeine citrate in premature infants. J. Pediatr. 211, 27–32.e21 (2019).
Thébaud, B. et al. Bronchopulmonary dysplasia. Nat. Rev. Dis. Prim. 5, 78–78 (2019).
Vliegenthart, R., Miedema, M., Hutten, G. J., van Kaam, A. H. & Onland, W. High versus standard dose caffeine for apnoea: a systematic review. Arch. Dis. Child Fetal Neonatal Ed. 103, F523–f529 (2018).
Cafcit [Package Insert on the Internet] (Eatontown (NJ): Hikma Pharmaceuticals Inc.; 1999, Revised Dec 2019, accessed Aug 2021). https://www.Accessdata.Fda.Gov/Drugsatfda_Docs/Label/2020/020793s019lbl.Pdf.
Greenberg, J. M. et al. Respiratory medication use in extremely premature (<29 weeks) infants during initial nicu hospitalization: results from the prematurity and respiratory outcomes program. Pediatr. Pulmonol. 55, 360–368 (2020).
O’Hara, K., Wright, I. M. R., Schneider, J. J., Jones, A. L. & Martin, J. H. Pharmacokinetics in neonatal prescribing: evidence base, paradigms and the future. Br. J. Clin. Pharm. 80, 1281–1288 (2015).
Koch, G. et al. Caffeine citrate dosing adjustments to assure stable caffeine concentrations in preterm neonates. J. Pediatr. 191, 50–56.e51 (2017).
Ehrenkranz, R. A. et al. Longitudinal growth of hospitalized very low birth weight infants. Pediatrics 104, 280–289 (1999).
al-Alaiyan, S. et al. Caffeine metabolism in premature infants. J. Clin. Pharm. 41, 620–627 (2001).
Bueva, A. & Guignard, J. P. Renal function in preterm neonates. Pediatr. Res. 36, 572–577 (1994).
Kahn, D. J. & Godin, R. Is it time to embrace the caffeine level? Pediatrics 137, e20160403A (2016).
Charles, B. G. et al. Caffeine citrate treatment for extremely premature infants with apnea: population pharmacokinetics, absolute bioavailability, and implications for therapeutic drug monitoring. Ther. Drug Monit. 30, 709–716 (2008).
Falcão, A. C. et al. Population pharmacokinetics of caffeine in premature neonates. Eur. J. Clin. Pharm. 52, 211–217 (1997).
Lee, T. C., Charles, B., Steer, P., Flenady, V. & Shearman, A. Population pharmacokinetics of intravenous caffeine in neonates with apnea of prematurity. Clin. Pharm. Ther. 61, 628–640 (1997).
Thomson, A. H., Kerr, S. & Wright, S. Population pharmacokinetics of caffeine in neonates and young infants. Ther. Drug Monit. 18, 245–253 (1996).
Olsen, I. E., Groveman, S. A., Lawson, M. L., Clark, R. H. & Zemel, B. S. New intrauterine growth curves based on United States data. Pediatrics 125, e214–e224 (2010).
Salemi, L. A. et al. Evaluation of the use of caffeine citrate maintenance doses >5 mg/kg/day in preterm neonates for apnea of prematurity. J. Pediatr. Pharm. Ther. 26, 608–614 (2021).
Aldridge, A., Aranda, J. V. & Neims, A. H. Caffeine metabolism in the newborn. Clin. Pharm. Ther. 25, 447–453 (1979).
Wu, Y. et al. Prediction of glomerular filtration rate maturation across preterm and term neonates and young infants using inulin as marker. AAPS J. 24, 38 (2022).
Gal, P. Caffeine therapeutic drug monitoring is necessary and cost-effective. J. Pediatr. Pharm. Ther. 12, 212–215 (2007).
Alur, P., Bollampalli, V., Bell, T., Hussain, N. & Liss, J. Serum caffeine concentrations and short-term outcomes in premature infants of ⩽29 weeks of gestation. J. Perinatol. 35, 434–438 (2015).
Long, J. Y. et al. Caffeine for the pharmacological treatment of apnea of prematurity in the NICU: dose selection conundrum, therapeutic drug monitoring and genetic factors. Front Pharm. 12, 681842 (2021).
Ravichandran, S. et al. Higher daily doses of caffeine lowered the incidence of moderate to severe neurodevelopmental disabilities in very low birth weight infants. Acta Paediatr. 108, 430–435 (2019).
Chen, J., Jin, L. & Chen, X. Efficacy and safety of different maintenance doses of caffeine citrate for treatment of apnea in premature infants: a systematic review and meta-analysis. Biomed. Res. Int. 2018, 9061234 (2018).
Moschino, L. et al. Caffeine in preterm infants: where are we in 2020? ERJ Open Res. 6, 00330–02019 (2020).
Davis, P. G. et al. Caffeine for apnea of prematurity trial: benefits may vary in subgroups. J. Pediatr. 156, 382–387 (2010).
Rebentisch, A., Kovey, K. & Denslow, S. An evaluation of twice-daily dosing of caffeine for apnea of prematurity. J. Pediatr. Pharm. Ther. 26, 253–257 (2021).
Cosmi, E., Fanelli, T., Visentin, S., Trevisanuto, D. & Zanardo, V. Consequences in infants that were intrauterine growth restricted. J. Pregnancy 2011, 364381 (2011).
Author information
Authors and Affiliations
Contributions
S.Y.L., P.N.J., and J.L.M. all contributed substantially to conception and design, acquisition of data, or analysis and interpretation of data, as well as drafting the article and revising it critically; C.B.M. contributed substantially to the interpretation of data and drafting the article and revising it critically.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Lim, S.Y., May, C.B., Johnson, P.N. et al. Caffeine dosing in premature neonates: impact of birth weight on a pharmacokinetic simulation study. Pediatr Res 93, 696–700 (2023). https://doi.org/10.1038/s41390-022-02172-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-022-02172-y
- Springer Nature America, Inc.