Abstract
In obesity, cardiometabolic risk markers show worsening trends with increasing blood pressure (BP). We assumed that risk markers show similar trends across BP categories (normotension, high normal BP, hypertension) in metabolic abnormalities-free subjects (without obesity, insulin resistance, atherogenic dyslipidemia, hyperuricemia, microinflammation) and those presenting them. Data from 2547 (48.1% males) subjects aged 16–23 years were analyzed. The prevalence of males increased across BP categories. Forty-seven percent of individuals with elevated BP were metabolic abnormalities-free. Among 1461 metabolic abnormalities-free subjects, 9% had high normal BP, and 4% hypertension; among 1086 individuals presenting metabolic abnormalities, the prevalence reached 13% and 6%, respectively, (p < 0.001). Both groups displayed similar BP values in corresponding BP categories and significant trends in markers of adiposity, insulin resistance, HDL-cholesterol, atherogenic index of plasma, uric acid, adiponectinemia, and antioxidant capacity of plasma across BP categories. In metabolic abnormalities-free individuals, also significant trends in soluble receptors for advanced glycation end products were revealed. Continuous metabolic syndrome score, a measure of cardiometabolic risk, increased across BP categories regardless of presence or absence of metabolic abnormalities. Multivariate regression models selected male gender, fat-free mass, and uric acid as significant independent predictors for determining BP. Our data emphasize that having a BP outside the normal range significantly worsens risk for cardiometabolic disease in young individuals even if the thresholds for any of the risk factors are not exceeded. Longitudinal studies are needed to assess whether in patients with elevated BP the prognosis of adverse outcomes differs between those presenting and not presenting metabolic abnormalities.
Similar content being viewed by others
Introduction
In adults, high blood pressure (BP) strongly associates with an increased risk for cardiovascular events, renal disease, and mortality [1]. Increased BP in adulthood has its origins in early youth: adult BP correlates with BP and body mass index (BMI) in adolescence [2]. The upward trend in adolescent high normal BP (HNBP, formerly termed prehypertension) and hypertension (HT) have risen in parallel with increasing trends in the prevalence of overweight and obesity [3]. Juveniles with overweight- or obesity-related HNBP and HT present biochemical profile (e.g., elevated total cholesterol, low-density lipoprotein cholesterol (LDL-C), triacylglycerols (TAG), fasting plasma insulin, high-sensitive C-reactive protein (hsCRP), uric acid, reduced high-density lipoprotein cholesterol (HDL-C), adiponectin, insulin sensitivity markers) [4,5,6] indicative of increased cardiometabolic risk.
In a representative cohort of 18–29 years old Slovaks, elevated BP was the second most prevalent component of metabolic syndrome, with about fourfold higher prevalence than that of metabolic syndrome [7]. Thus, we anticipated that a proportion of Slovaks with elevated BP presents metabolic abnormalities-free phenotype. It remains unclear whether cardiometabolic risk factors and biomarkers display similar trends across BP categories (NT, HNBP, HT) in individuals presenting and not presenting metabolic abnormalities. We presumed that metabolic abnormalities-free subjects will display lower BP values and more favorable values of risk factors and biomarkers compared with individuals presenting metabolic abnormalities, while the trends across BP categories will be significant regardless of the presence or absence of abnormalities. To this point, we analyzed data obtained in a secondary-school-based survey carried out in Bratislava region. Trends for cardiometabolic risk factors (i.e., proxy measures of obesity, glucose homeostasis, lipid profile) and biomarkers (inflammatory and oxidative status markers, uric acid, markers of renal function, concentrations of adiponectin and circulating soluble receptors of advanced glycation end products (sRAGE)) across BP categories were investigated.
Subjects and methods
Study design
This study was conducted within the cross-sectional survey “Respect for Health”, which aimed to assess the cardiometabolic status of secondary school students in Bratislava region. Participation was voluntary. The study was approved by the Ethics Board of the Health Department of the Bratislava Self-governing Region. All the procedures were in accordance with the Declaration of Helsinki. The study protocol has been explained in detail previously [8]. A written informed consent was obtained from the parents of children under 18 years of age, and from the full-aged participants. Exclusion criteria were acute or chronic illness; non-Caucasian, foreign nationality; pregnancy and lactation in females.
Study population
Two thousand seven hundred forty nine White Caucasians of Central European descent (47.9% males) aged 11–32 years participated in the study. After exclusion of 161 subjects (5 displaying FPG > 6.9 mmol/l; 41 with hsCRP > 10 mg/l, and 156 probands aged < 16 or >23 years), 2547 (48.1% males) aged 16–23 years were included into present analysis. Representative sample for 16–23-year-old enrolled students, with 95% confidence interval and 80% power, was calculated as 1220 boys and 1230 girls.
Anthropometric and BP measurements
Anthropometric and BP measurements were performed at secondary schools, as described previously [8]. To ensure uniform operating procedures, personnel was trained and provided by written instructions on performance of measurements. Anthropometric measurements were performed in subjects wearing light clothes standing barefoot. Height was measured with portable stadiometer, waist circumference using a flexible tape, body weight using digital scales (Omron BF510, Kyoto, Japan) equipped for determination of total body fat percentage employing bioimpedance method. BMI, waist-to-height ratio (WHtR), and fat-free mass [9] were calculated. Three BP and heart rate measurements using automated device (Omron M-6 COMFORT, Kyoto, Japan) were taken on the right arm, in subjects seated for 10 min. The mean of the last two readings was recorded.
Biochemical analyses
Blood was sampled from participants after overnight fasting. At the central laboratory, blood counts (Sysmex XE-2100 analyser, Sysmex Corporation, Kobe, Japan) and standard blood chemistry analyses (plasma fasting glucose, insulin, total cholesterol, HDL-C, TAG, creatinine, hsCRP, and uric acid) were performed (ADVIA analysers, Siemens, Erlangen, Germany). Plasma total L-homocysteine was measured using a fluorescence polarization immunoassay (Abbott AxSym analyzer, Abbott Park, IL, USA). In spot urine, microalbuminuria was assessed as albumin (immunoturbidimetrically) to creatinine ratio. LDL-C concentration (Friedewald equation), non-HDL-C, atherogenic index of plasma [10], the quantitative insulin sensitivity check index (QUICKI), and estimated glomerular filtration rate (eGFR, using Schwartz or MDRD formula, as appropriate) were calculated. Enzyme-linked immunoassays were employed to determine plasma concentrations of adiponectin, and soluble RAGE (sRAGE, i.e., the total pool of soluble forms of RAGE, including an endogenous secretory RAGE (esRAGE), R&D, Minneapolis, MN, USA), and esRAGE (B-Bridge International, Inc., Mountain View, CA, USA) according to the manufacturers’ instructions. Total antioxidant capacity of plasma (spectrophotometrically) and concentrations of thiobarbituric acid reactive substances (TBARS, fluorometrically) [11] were measured (Sapphire II instrument, Tecan, Vienna, Austria).
Classification of BP, cardiometabolic risk factors, and abnormalities
Normotension was classified as SBP < 130 and DBP < 85 mm Hg; HNBP as SBP 130–139 mm Hg and/or DBP 85–90 mm Hg, and HT as SBP ≥ 140 mm Hg and/or DBP ≥ 90 mm Hg [12]. Since the age- and sex-specific waist circumference percentiles for Slovak adolescents are not published, WHtR was used as a proxy measure of central obesity. Subjects not presenting either of cardiometabolic risk factors, e.g., central obesity (WHtR ≥ 0.5); elevated fasting glycemia (≥5.6 mmol/l), elevated TAG (≥1.7 mmol/l), low HDL-C (<1.03 mmol/l (males) and <1.29 mmol/l (females)); and biomarkers, e.g., elevated atherogenic index (≥0.11), elevated uric acid (≥420 mmol/l (males), ≥340 mmol/l (females)), elevated fasting insulinemia (≥20 μIU/ml), elevated hsCRP (>3 mg/l) were considered as metabolic abnormalities-free; those manifesting ≥1 risk factors or biomarkers were classified as presenting abnormalities. Metabolic syndrome was classified as presence of ≥3 components out of 5 (e.g., SBP ≥ 130 mm Hg and/or DBP ≥ 85 mm Hg, WHtR ≥ 0.5, plasma glucose ≥ 5.6 mmol/l, TAG ≥ 1.7 mmol/l, HDL-C < 1.03 mmol/l (males) and <1.29 mmol/l (females)). Continuous metabolic syndrome score was calculated as WHtR/0.5 + FPG/5.6 + TAG/1.7 + SBP/130 − HDL-C/1.02 (males) or 1.28 (females) [13]. To ascertain that an increasing trend of the score across BP categories is not driven solely by increasing BP, continuous metabolic syndrome score was alternatively calculated by omitting the BP component from the equation.
Statistical analyses
Nonnormally distributed data were logarithmically transformed. Two sets of data were compared using two-sided Student’s t test. One-way analysis of variance (ANOVA) was used to compare the variables between BP categories. Post-hoc Bonferroni test was run to correct for multiple comparisons. Frequencies were compared employing the chi-square test. Pearson correlation coefficients were calculated. Data are given as mean ± SD, or as counts and percentages. p values < 0.05 were considered statistically significant. Analyses were performed using the SPSS v.16 for Windows software (SPSS Inc., Chicago, IL, USA). Multivariate analysis using the Orthogonal Projections to Latent Structures (OPLS, Simca v.15 software, Sartorius Stedim Data Analytics AB, Umea, Sweden) was employed to identify the set of explanatory variables predicting the dependent ones, e.g., SBP and DBP. WHtR, fat-free mass, QUICKI, non-HDL-C, atherogenic index, uric acid, urinary albumin-to-creatinine ratio, homocysteine, adiponectin, antioxidant capacity of plasma, and esRAGE were entered as independent variables. Prior to modeling, variables with high skewness and low min/max ratio were logarithmically transformed and all data were mean-centered. Variables with variable of importance for the projection values ≥1.00 were considered as important contributors.
Results
Whole cohort
In the first step, we aimed to affirm the differences between metabolic abnormalities-presenting and abnormalities-free subjects (Table 1). 42.6% of participants presented metabolic abnormalities. The prevalence of males was similar among subjects presenting and not presenting metabolic abnormalities. Individuals presenting metabolic abnormalities displayed mildly but significantly higher BP values, while the prevalence of elevated SBP or DBP did not differ significantly between the groups. Two groups differed significantly by all variables except for age; height; total cholesterol, TBARS, and homocysteine concentrations; and markers of renal function.
Next, we focused on differences cross BP categories. 84.3% of participants presented NT, 10.8% had HNBP, and 4.9% were hypertensive (Table 2). Normotensive subjects were slightly older compared with HNBP and HT groups. The prevalence of males rose significantly across BP categories. As expected, mean BP values increased across BP categories and the prevalence of elevated SBP as well as DBP was higher among hypertensive subjects compared with those presenting HNBP. Except for total cholesterol, hsCRP, and TBARS concentrations, eGFR and leukocyte counts, all variables showed significant trends across BP categories. The prevalence of metabolic syndrome and all risk markers except for low HDL-C and elevated hsCRP concentrations differed significantly between BP categories (Table 2).
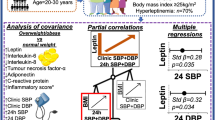
Continuous metabolic syndrome score, even if calculated without the BP component, and uricemia correlated directly with SBP and DBP (Table 3). Among anthropometric variables, fat-free mass displayed the highest correlations with BP, those with WHtR or BMI were much lower (Table 3). Similarly, uricemia correlated more tightly with fat-free mass compared with WHtR, or BMI (r = 0.668, 0.258, 0.317, respectively; p < 0.001, all).
The OPLS model indicated that (male) sex, fat-free mass, and uric acid levels are significant predictors of both SBP and DBP. Moreover, WHtR, QUICKI, and atherogenic index of plasma appeared as additional independent predictors of DBP. Models explained 43 and 10% of variability in SBP and DBP, respectively (Table 4).
Individuals presenting metabolic abnormalities
Among subjects manifesting at least one metabolic abnormality, 80.7% were normotensive, 13% presented HNBP, and 6.3% HT (Table 5). The prevalence of males in HNBP and HT groups was about twofold higher compared with their prevalence among NT subjects. Normotensive individuals were slightly younger compared with those presenting HT. SBP and DBP increased across BP categories. While the prevalence of elevated SBP was similar in HNBP and HT groups, that of elevated DBP was higher among hypertensive subjects. As in the whole group, concentrations of total cholesterol, hsCRP, and TBARS; eGFR and leukocyte counts did not differ significantly between BP categories. Moreover, three groups displayed similar TAG, sRAGE, and esRAGE levels. All other variables showed significant trends across BP categories, however, the post-hoc test failed to indicate significance for HDL-C and urinary albumin-to-creatinine ratio. The increasing trend in metabolic syndrome score (Table 5) remained significant even after the exclusion of BP component (NT: 3.46 ± 0.43, HNBP: 3.61 ± 0.44, HT: 3.72 ± 0.47; p < 0.001). The prevalence of central obesity, elevated uric acid levels, and that of metabolic syndrome rose across BP categories, while that of low HDL-C was the highest among normotensive subjects (Table 5).
Continuous metabolic syndrome score (regardless whether calculated with or without the BP component), and uric acid level correlated directly with SBP, as well as DBP (Table 3). As in the entire cohort, fat-free mass showed the highest association with SBP. BMI displayed the highest correlation with DBP (Table 3). Uric acid concentration correlated significantly with fat-free mass, WHtR, and BMI (r = 0.648, 0.225, 0.287, respectively; p < 0.001, all).
In multivariate analysis, (male) sex, fat-free mass, WHtR, and uric acid were significant independent predictors of both SBP and DBP. The model described 46% of variability in SBP, and 13% in DBP (Table 4).
Individuals not presenting metabolic abnormalities
In abnormalities-free subjects, the prevalence of NT, HNBP, and HT reached 87%, 9.2%, and 3.8%, respectively (Table 6). As in the group presenting metabolic abnormalities, the prevalence of males among subjects with HNBP and HT was about twofold higher compared with their prevalence among normotensive subjects. SBP and DBP increased across three BP categories but mean BP values in corresponding BP categories (NT, HNBP, HT) did not differ significantly between subjects presenting and not presenting metabolic abnormalities. The prevalence of elevated SBP as well as that of DBP was higher among hypertensive subjects compared with those presenting HNBP. However, in corresponding BP categories, the prevalence did not differ significantly between subjects with or without metabolic abnormalities (elevated SBP: p = 0.262 and 0.732, respectively; elevated DBP: p = 0.231 and 0.733, respectively; Tables 5 and 6). As in metabolic abnormalities-presenting subjects, we did not reveal significant trends across BP categories for total cholesterol, TAG, eGFR, hsCRP, TBARS, and leukocyte counts. However, abnormalities-free subjects generally presented lower mean values of TAG, hsCRP, and leukocyte counts. We neither revealed significant trends across BP categories for age; heart rate; fasting insulin, LDL-C, non-HDL-C, and homocysteine concentrations; or urinary albumin-to-creatinine ratio. Nevertheless, metabolic abnormalities-free subjects displayed lower insulin and non-HDL-C levels compared with their peers presenting abnormalities. Anthropometric measures showed significant trends and differences across BP categories. Except for height, they differed significantly from those in corresponding BP category of individuals presenting abnormalities. In contrast to findings in metabolic abnormalities-presenting individuals, trends across BP categories for glycemia, sRAGE, and esRAGE concentrations were significant in abnormalities-free subjects. These variables also differed significantly between two groups of normotensive individuals. All other variables showed significant trends across BP categories and in most BP categories differed significantly from the values observed in subjects presenting abnormalities (Table 6). Metabolic syndrome score showed an increasing trend across BP categories even if calculated by omitting the BP component (NT: 3.42 ± 0.26, HNBP: 3.47 ± 0.27, HT: 3.52 ± 0.26; p = 0.003).
Continuous metabolic syndrome score and uricemia correlated directly with SBP and DBP (Table 3). Among anthropometric variables, fat-free mass showed the highest correlation with SBP or DBP (Table 3), as well as with uricemia (fat-free mass: r = 0.679; WHtR: r = 0.147; BMI: r = 0.229; p < 0.001, all).
Multivariate model indicated that (male) sex, fat-free mass, and uric acid are significant determinants of SBP or DBP. QUICKI and atherogenic index were selected as additional significant predictors of DBP. Variability in SBP or DBP explained by the models was 41% and 6%, respectively (Table 4).
Discussion
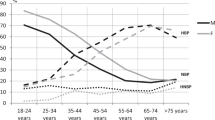
Different methodologies and age differences of studied cohorts complicate the comparison of published data on the prevalence of HNBP, HT, or elevated BP (i.e., HNBP + HT) in juveniles. The prevalence of elevated BP in our study (16%) is in line with 18% prevalence reported for a presentative cohort of 18–29-year-old Slovaks [7]. In White Caucasian adolescents, the prevalence of HNBP varies between 8 and 55%, and that of HT reaches 2–22%, with higher prevalence in males compared with females and overweight/obese individuals compared with normal weight subjects [9, 14,15,16]. The prevalence in our study (HNBP:11%, HT:5%) fits into the above-mentioned ranges. It is difficult to determine whether it realistically reflects the prevalence among secondary school students in Bratislava region or is biased by voluntary participation since we have no data on individuals who did not take part in the survey.
In our study, almost half (e.g., 47%) of young individuals with elevated BP were metabolic abnormalities-free, i.e., insulin sensitive, not presenting central obesity, atherogenic dyslipidemia, hsCRP > 3 mg/l, or hyperuricemia. In contrast to our hypothesis, these subjects displayed similar mean BP values across BP categories as their peers presenting metabolic abnormalities. Thus, the presence of metabolic abnormalities neither seemed to be a prerequisite for manifestation of HNBP or HT nor it indicated a more severe elevation of BP. As expected, individuals manifesting abnormalities displayed less favorable values of all risk factors and of almost all biomarkers compared with their abnormalities-free counterparts. However, continuous metabolic syndrome score increased across BP categories both in metabolic abnormalities-presenting (by about 12%) and abnormalities-free individuals (by about 9%). Continuous metabolic syndrome score allows for exact estimation of the individual cardiometabolic burden even in individuals not presenting with metabolic syndrome [17]. In juveniles, it associates with atherosclerotic risk assessed as carotid arterial stiffness [18]. Childhood continuous metabolic syndrome score is a reliable predictor of cardiometabolic risk in adulthood and in adults it predicts long-term risk of development of cardiometabolic disease, cardiovascular and overall mortality [19,20,21]. Thus, even the presence of “asymptomatic” HNBP or HT indicates an increased cardiometabolic risk. In all patients with elevated BP, attention should be paid even to changes in risk factors and markers occurring within the “normal range.”
BP increases with increasing measures of general and central obesity and the prevalence of HNBP and HT is higher in overweight and obese adolescents compared with those displaying normal weight [14, 15]. However, a recent large study in young adults [9], as well as our data, show that association between BP and fat-free mass is much stronger than that with BMI or WHtR. Fat-free mass was a strong independent predictor of both SBP and DBP regardless of presence or absence of metabolic abnormalities. High impact of fat-free mass on BP is probably secondary, reflecting the high correlation between fat-free mass and uric acid levels [9], documented also in our study. Accordingly, the multivariate analysis confirmed a significant impact of uricemia on BP in all settings. This finding supports the hypothesis that uric acid plays a role in the early pathogenesis of primary HT in juveniles [22]. Moreover, uric acid may induce insulin resistance and higher uric acid levels increase the risk of later development of atherogenic dyslipidemia [23, 24]. Albeit insulin sensitivity decreased and markers of atherogenic dyslipidemia worsened across BP categories, in multivariate analysis they showed a significant impact only on DBP, in the entire cohort and subjects not presenting metabolic abnormalities. Thus, male gender, fat-free mass, and uric acid give a large contribution in determining BP in young population with rather low prevalence of central obesity. However, substantially higher prevalence of elevated BP in our males as well as known sex differences in the pathophysiology of metabolic syndrome and presentation of metabolic abnormalities [7, 25] raise the question whether our findings on trends across BP categories apply equally to males and females.
Adolescents with obesity-associated HT present low adiponectin levels [6]. Recent data suggest that a negative association between adiponectin and BP is independent of fatness and insulin resistance [26]. Despite that adiponectinemia showed a decreasing trend across BP categories, in multivariate regression it did not associate with BP in either group. Thus, decline in adiponectinemia across BP categories probably rather reflected increasing adiposity and a rising prevalence of males who display lower adiponectin concentrations compared with females. Elevation of BP per se probably does not elicit decline in adiponectinemia.
Oxidative stress my act as a trigger of both inflammation and HT, while it remains unclear whether inflammation is a cause or effect of HT, with evidence to support either scenario in a likely vicious cycle [27]. Data on inflammatory and oxidative status markers in juveniles with elevated BP are scares. Elevated BP associated with elevated inflammatory markers (mostly analyzed by the hsCRP assay) [28]. We did not reveal significant trends in leukocyte counts or in hsCRP concentrations across BP categories. Juveniles with essential HT presented higher levels of lipid peroxidation products and oxidized-to-reduced glutathione ratio compared with BMI-matched normotensive controls [29]. In our cohort, antioxidant capacity of plasma increased while lipid peroxidation products (TBARS) remained unchanged across BP categories. Via induction of oxidative and inflammatory damage to vasculature, homocysteine may cause changes that finally manifest in rise in BP [30]. In contrast with a different study in young subjects [28], we revealed a rise of homocysteine levels across BP categories in subjects presenting metabolic abnormalities. However, the multivariate analysis results do not support an association between homocysteine levels and BP. The role of imbalance in oxidative status and associated chronic low-grade inflammation in the pathogenesis of HT in juveniles requires further studies.
Circulating variants of RAGE may competitively inhibit binding of ligands to cell-membrane-bound RAGE, thus ameliorate responses toward tissue dysfunction resulting from oxidative stress generation, inflammatory, atherogenic, and diabetogenic responses [31, 32]. In adults, virtually all components of metabolic syndrome show significant relationship with sRAGE [33]. Hypertensive adults present lower sRAGE levels compared with their normotensive counterparts and an inverse association between BP and sRAGE levels [33, 34]. Despite that we observed a decreasing trend in sRAGE and esRAGE levels across BP categories in the whole cohort and in metabolic abnormalities-free individuals, in multivariate analysis esRAGE did not appear as a significant predictor of BP. However, a declining trend observed in the group not presenting metabolic abnormalities warrants attention since low sRAGE levels indicate in nondiabetic subjects an increased risk of development of diabetes, cardiovascular disease, or death [35].
The strength of our study comprises a large cohort of young subjects, suitable to explore metabolic changes occurring “early” given to onset of BP elevation; simultaneous determination of cardiometabolic risk factors and numerous biomarkers; and cardiometabolic characteristics of subjects with HNBP and HT not presenting additional metabolic abnormalities. Limitations follow from voluntary participation and potential participation of close relatives. Our data based on a single-occasion assessment of BP neither can be viewed as clinical diagnosis of HNBP or HT nor as a reliable estimate of the prevalence of metabolic abnormalities-free elevated BP phenotype. Assessed risk factors and biomarkers poorly explained variability in DBP, suggesting that other variables not investigated herein, such as genetic background, family history, socio-economic status, behavioral patterns, or other biochemical markers, are more robust determinants of BP. The cross-sectional study design only allows for the establishment of associations and not causal relationships. There is a limitation of generalizing our findings to populations with different epidemiological, anthropometric, or clinical characteristics.
Cardiometabolic risk is a continual progressive function and it cannot simply be assumed as present or absent, depending on whether thresholds of risk factors are exceeded or not. We show that elevated BP associates with concomitant rise in severity of cardiometabolic risk determined as continuous metabolic syndrome score even in “asymptomatic” subjects, e.g., those not presenting a single risk factor or marker exceeding the increased risk-indicating cut-off point. Since the calculation of continuous metabolic syndrome score is easy, it should be recommended as an estimate of the baseline risk at diagnosis of elevated BP, as well as for longitudinal assessment of individual’s cardiometabolic risk in clinical practice. As the prevalence of all metabolic abnormalities increases with ageing, question arises to what extent is the elevated BP-associated metabolic abnormalities-free phenotype a transient condition. Data on prognosis of adverse outcomes in metabolic abnormalities-free patients with HNBP and HT, compared with normotensive with or without abnormalities, or those with elevated BP presenting abnormalities, are lacking. Thus, further studies are needed to estimate the clinical impact of presentation of elevated BP metabolic abnormalities-free phenotype.
Summary
What is known about this topic
-
High BP, an important risk factor for mortality in adults, has its origin in early youth.
-
Juveniles with obesity-associated elevated BP present blood chemistry profile indicative of increased cardiometabolic risk.
What this study adds
-
About a half of 16–23 years old Slovak students with elevated BP present metabolic abnormalities-free phenotype (i.e., without central obesity, insulin resistance, atherogenic dyslipidemia, hyperuricemia, or elevated hsCRP).
-
Across BP categories (normotension, HNBP, HT), abnormalities-presenting, and abnormalities-free subjects display similar mean SBP and DBP. Cardiometabolic risk factors and markers, and continuous metabolic syndrome score (a proxy measure of cardiometabolic risk), show worsening trends across BP categories regardless of presence or absence of metabolic abnormalities.
-
Male gender, fat-free mass, and uric acid levels are independent predictors of BP in metabolic abnormalities-free and abnormalities-presenting young subjects.
References
Psaty BM, Furberg CD, Kuller LH, Cushman M, Savage PJ, Levine D, et al. Association between blood pressure level and the risk of myocardial infarction, stroke, and total mortality: the cardiovascular health study. Arch Intern Med. 2001;161:1183–92.
Lauer RM, Clarke WR. Childhood risk factors for high adult blood pressure: the Muscatine Study. Pediatrics. 1989;84:633–41.
Kelly RK, Magnussen CG, Sabin MA, Cheung M, Juonala M. Development of hypertension in overweight adolescents: a review. Adolesc Health Med Ther. 2015;6:171–87.
Noronha JA, Medeiros CC, Cardoso Ada S, Gonzaga NC, Ramos AT, Ramos AL. C-reactive protein and its relation to high blood pressure in overweight or obese children and adolescents. Rev Paul Pediatr. 2013;31:331–7.
Freedman DS, Dietz WH, Srinivasan SR, Berenson GS. The relation of overweight to cardiovascular risk factors among children and adolescents: the Bogalusa Heart Study. Pediatrics. 1999;103:1175–82.
De Las Heras J, Lee S, Bacha F, Tfayli H, Arslanian S. Cross-sectional association between blood pressure, in vivo insulin sensitivity and adiponectin in overweight adolescents. Horm Res Paediatr. 2011;76:379–85.
Mokan M, Galajda P, Pridavkova D, Tomaskova V, Sutarik L, Krucinska L, et al. Prevalence of diabetes mellitus and metabolic syndrome in Slovakia. Diabetes Res Clin Pr. 2008;81:238–42.
Gurecka R, Koborova I, Sebek J, Sebekova K. Presence of cardiometabolic risk factors is not associated with microalbuminuria in 14-to-20-years old Slovak adolescents: a cross-sectional, population study. PLoS ONE. 2015;10:e0129311.
Sidoti A, Nigrelli S, Rosati A, Bigazzi R, Caprioli R, Fanelli R, et al. Body mass index, fat free mass, uric acid, and renal function as blood pressure levels determinants in young adults. Nephrology. 2017;22:279–85.
Dobiasova M, Frohlich J. The plasma parameter log (TG/HDL-C) as an atherogenic index: correlation with lipoprotein particle size and esterification rate in apoB-lipoprotein-depleted plasma (FER(HDL)). Clin Biochem. 2001;34:583–8.
Karlik M, Valkovic P, Hancinova V, Krizova L, Tothova L, Celec P. Markers of oxidative stress in plasma and saliva in patients with multiple sclerosis. Clin Biochem. 2015;48:24–8.
Lurbe E, Agabiti-Rosei E, Cruickshank JK, Dominiczak A, Erdine S, Hirth A, et al. 2016 European Society of Hypertension guidelines for the management of high blood pressure in children and adolescents. J Hypertens. 2016;34:1887–920.
Soldatovic I, Vukovic R, Culafic D, Gajic M, Dimitrijevic-Sreckovic V. siMS score: simple method for quantifying metabolic syndrome. PLoS ONE. 2016;11:e0146143.
McNiece KL, Poffenbarger TS, Turner JL, Franco KD, Sorof JM, Portman RJ. Prevalence of hypertension and pre-hypertension among adolescents. J Pediatr. 2007;150:640–4. 644.e1.
Dulskiene V, Kuciene R, Medzioniene J, Benetis R. Association between obesity and high blood pressure among Lithuanian adolescents: a cross-sectional study. Ital J Pediatr. 2014;40:102.
Menghetti E, Strisciuglio P, Spagnolo A, Carletti M, Paciotti G, Muzzi G, et al. Hypertension and obesity in Italian school children: the role of diet, lifestyle and family history. Nutr Metab Cardiovasc Dis. 2015;25:602–7.
Sebekova K, Sebek J. Continuous metabolic syndrome score (siMS) enables quantification of severity of cardiometabolic affliction in individuals not presenting with metabolic syndrome. Bratisl Lek Listy. 2018;119:675–8.
DeBoer MD, Gurka MJ, Woo JG, Morrison JA. Severity of metabolic syndrome as a predictor of cardiovascular disease between childhood and adulthood: the Princeton Lipid Research Cohort Study. J Am Coll Cardiol. 2015;66:755–7.
Pandit D, Chiplonkar S, Khadilkar A, Kinare A, Khadilkar V. Efficacy of a continuous metabolic syndrome score in Indian children for detecting subclinical atherosclerotic risk. Int J Obes. 2011;35:1318–24.
Jung KJ, Jee YH, Jee SH. Metabolic risk score and vascular mortality among Korean adults. Asia Pac J Public Health. 2017;29:122–31.
DeBoer MD, Gurka MJ. Clinical utility of metabolic syndrome severity scores: considerations for practitioners. Diabetes Metab Syndr Obes. 2017;10:65–72.
Feig DI, Johnson RJ. The role of uric acid in pediatric hypertension. J Ren Nutr. 2007;17:79–83.
King C, Lanaspa MA, Jensen T, Tolan DR, Sanchez-Lozada LG, Johnson RJ. Uric acid as a cause of the metabolic syndrome. Contrib Nephrol. 2018;192:88–102.
Kuwabara M, Borghi C, Cicero AFG, Hisatome I, Niwa K, Ohno M, et al. Elevated serum uric acid increases risks for developing high LDL cholesterol and hypertriglyceridemia: a five-year cohort study in Japan. Int J Cardiol. 2018;261:183–8.
Rochlani Y, Pothineni NV, Mehta JL. Metabolic syndrome: does it differ between women and men? Cardiovasc Drugs Ther. 2015;29:329–38.
Brambilla P, Antolini L, Street ME, Giussani M, Galbiati S, Valsecchi MG, et al. Adiponectin and hypertension in normal-weight and obese children. Am J Hypertens. 2013;26:257–64.
Dinh QN, Drummond GR, Sobey CG, Chrissobolis S. Roles of inflammation, oxidative stress, and vascular dysfunction in hypertension. Biomed Res Int. 2014;2014:406960.
Litwin M, Michalkiewicz J, Niemirska A, Gackowska L, Kubiszewska I, Wierzbicka A, et al. Inflammatory activation in children with primary hypertension. Pediatr Nephrol. 2010;25:1711–8.
Turi S, Friedman A, Bereczki C, Papp F, Kovacs J, Karg E, et al. Oxidative stress in juvenile essential hypertension. J Hypertens. 2003;21:145–52.
Papatheodorou L, Weiss N. Vascular oxidant stress and inflammation in hyperhomocysteinemia. Antioxid Redox Signal. 2007;9:1941–58.
Hudson BI, Carter AM, Harja E, Kalea AZ, Arriero M, Yang H, et al. Identification, classification, and expression of RAGE gene splice variants. FASEB J. 2008;22:1572–80.
Stern D, Yan SD, Yan SF, Schmidt AM. Receptor for advanced glycation endproducts: a multiligand receptor magnifying cell stress in diverse pathologic settings. Adv Drug Deliv Rev. 2002;54:1615–25.
Sebekova K, Krivosikova Z, Gajdos M. Total plasma Nepsilon-(carboxymethyl)lysine and sRAGE levels are inversely associated with a number of metabolic syndrome risk factors in non-diabetic young-to-middle-aged medication-free subjects. Clin Chem Lab Med. 2014;52:139–49.
Geroldi D, Falcone C, Emanuele E, D’Angelo A, Calcagnino M, Buzzi MP, et al. Decreased plasma levels of soluble receptor for advanced glycation end-products in patients with essential hypertension. J Hypertens. 2005;23:1725–9.
Selvin E, Halushka MK, Rawlings AM, Hoogeveen RC, Ballantyne CM, Coresh J, et al. sRAGE and risk of diabetes, cardiovascular disease, and death. Diabetes. 2013;62:2116–21.
Acknowledgements
The authors wish to thank all those who put their effort toward the accomplishment of the Respect for Health study.
Funding
This study was funded by the Scientific Grant Agency of the Ministry of Education, Science, Research and Sport of the Slovak Republic and the Slovak Academy of Sciences (VEGA), grant no. 1/0637/13; the Slovak Research and Development Agency (APVV), grant no. 0447–12; and Bratislava Self-Governing Region. The sponsors had no role in study design; in the collection, analysis and interpretation of data; in the writing of the report; and in the decision to submit the article for publication.
Author information
Authors and Affiliations
Contributions
All authors were involved in developing the study concept, interpretation of results, editing, revising the article critically, and have approved the final version of this submission. RG, MCs and IK contributed to acquisition of data and helped to establish the database. JS undertook all the statistical analysis of the data. KS contributed to study design and wrote the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Šebeková, K., Gurecká, R., Csongová, M. et al. Elevated blood pressure-associated cardiometabolic risk factors and biomarkers in 16–23 years old students with or without metabolic abnormalities. J Hum Hypertens 35, 37–48 (2021). https://doi.org/10.1038/s41371-020-0309-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41371-020-0309-5
- Springer Nature Limited