Abstract
We reported previously that both a cannabinoid receptor 2 (CB2R) agonist and a cannabinoid receptor 1 (CB1R) antagonist were protective in the treatment of transient middle cerebral artery occlusion/reperfusion injury (MCAO/R) and that they acted in a synergistic manner when administered in combination. The goal of the current study was to determine which of the potential cannabinoid receptors participate in the protective effects of this drug combination in a mouse model of MCAO/R. The effects of administration of the CB2R agonist/CB1R antagonist combination on infarct size and cerebral blood flow during a 1-h occlusion were tested in CB1R-deficient animals, CB2R-deficient animals, and animals treated with capsazepine, the antagonist for the vanilloid receptor type I (TRPV1) and WAY100135, the antagonist for the hydroxytryptamine1A receptor (5-HT1A). The protective effect of the CB2R agonist/CB1R antagonist combination on infarct size was not influenced by the absence of the CB1R nor by blocking the TRPV1 receptor, but was attenuated by the absence of CB2R and by blocking the 5-HT1A receptor. Increases in cerebral blood flow and arteriolar diameter were also found to be independent of the CB1R and TRPV1 receptor. In conclusion, administration of the CB2R agonist/CB1R antagonist combination causes a significant reduction in infarct size in the MCAO/R model. The protective effect involves both the CB2R and the 5-HT1A receptor. Neither the CB1R nor the TRPV1 receptors appear to participate in this response.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The endocannabinoid system is comprised of cannabinoid receptors, the endogenous ligands N-arachidonoylethanolamide (anandamide) and 2-arachidonoylglycerol (2-AG), and the enzymes responsible for the inactivation and degradation of the ligands. The two best known and most widely studied cannabinoid receptors are the cannabinoid receptor 1 (CB1R) and the cannabinoid receptor 2 (CB2R). Although sharing significant homology, the two receptors have different and sometimes opposite actions [1].
Both the CB1R and CB2R receptors belong to the G(i/o) protein-coupled receptors. Activation of these receptors inhibits adenylate cyclase, stimulates phospholipase A and C, and regulates ion channels [2]. Their stimulation also leads to phosphorylation and activation of mitogen-activated protein kinases, including p42/p44 MAPK, p38 MAPK, and c-Jun N-terminal kinase [3]. The CB1R was first thought to affect almost exclusively nerve synaptic terminals and to mediate the feedback inhibition of synaptic transmission. Later studies provided evidence that the CB1R may also function on endothelial and immune cells [4]. Although found on neurons in very restricted areas, CB2R is thought to function primarily in immune cells including neutrophils, monocytes, lymphocytes, and microglia [5].
The therapeutic potential of the endocannabinoid system for treatment of stroke has been recognized by a number of investigators [6, 7]. Initially, based upon the finding that activating the CB1R was protective in pure excitotoxic injury models, it was speculated that CB1R agonists had the potential to protect neurons following stroke [8–12]. This hypothesis appeared to be confirmed by the finding that mice deficient in CB1R were more susceptible to stroke [13]. However, the role of CB1R activation following stroke has become an area of controversy since it was reported that CB1R antagonists also appear to protect the brain from damage following stroke [14–18].
The effects of CB2R activation in ischemia/reperfusion are much more consistent [7, 14]. Administration of CB2R agonists prior to or within a few hours of ischemia/reperfusion injury reduced infarct size and improved motor function [7, 14]. This effect appears to be due to the inhibition of postischemic inflammatory processes mediated primarily through the reduction in leukocyte migration into the central nervous system (CNS) [19]. We were the first to report that administration of the selective CB2R agonist O-1966 attenuated leukocyte rolling and adhesion to pial microvessels following transient middle cerebral artery occlusion and reperfusion [20].
In addition to CB1R and CB2R, it has been speculated that cannabinoids may have activity at other receptors, including the vanilloid receptor type I (TRPV1) [21, 22]. Cannabidiol, a component of cannabis with very low affinity for CB1R and CB2R, was shown to activate the hydroxytryptamine1A receptor (5-HT1A) [23, 24]. The activation of receptors other than CB1R or CB2R by cannabinoid agonists, or by compounds previously considered to act as selective CB1 or CB2 receptor antagonists, contributes to the confusion regarding the biological role of CB1R or CB2R.
We reported previously that both a CB2R agonist and a CB1R antagonist were protective in the transient middle cerebral artery occlusion/reperfusion (MCAO/R) model and that they acted in a synergistic manner when administered in combination [14]. The mechanism involved in this synergistic effect remains to be determined. The goal of the current investigation is to determine which receptors participate in the protective effects of this drug combination in the MCAO/R model.
Materials and Methods
Animals
The cerebral ischemia/reperfusion studies were carried out on 8-week-old male C57BL/6 mice from Taconic Farms (Hudson, NY). CB1 receptor knockout mice (C57BL/6), CB2 receptor knockout mice (B6.129P2-Cnr2tm1Dgen/J), and wild-type mice (C57BL/6) were obtained from the Jackson Laboratories (Bar Harbor, ME). All experiments were conducted in accordance with the guidelines approved by the Institutional Animal Care and Use Committee at Temple University.
Middle Cerebral Artery Occlusion and Reperfusion
The animals were anesthetized with an intraperitoneal injection of a ketamine (100 mg/mL)–xylazine (20 mg/mL) mixture (1:1) at a dose of 1 mL/kg. Body temperature was maintained at 37 ± 5 °C by using a heating lamp and heating pad. Middle cerebral artery occlusion was achieved by the intraluminal filament methods [25]. Briefly, a midline neck incision was made using an operation microscope; the right common carotid artery (CCA), external carotid artery (ECA), and internal carotid artery (ICA) were isolated. The ECA was ligated with a 6-0 silk suture distal from the ICA–ECA branch and then cut distal from the ligated point. Another 6-0 silk suture was tied loosely around the ECA close to the origin at the CCA. A blunted 5-0 monofilament nylon suture coated with poly-l-lysine (0.1 % in deionized water, Sigma Inc., St. Louis, MO) was introduced from a small incision on the ECA and then advanced into the circle of Willis, and finally to the origin of the middle cerebral artery. The silk suture around the ECA stump was tied tightly to prevent bleeding and secure the nylon suture. The nylon suture was removed after 60 min of occlusion, and ECA was permanently tied. Reperfusion was confirmed when pulsations were again observed in the ICA. The same surgical procedures were performed on sham animals without occlusions of the middle cerebral artery.
Regional Cerebral Blood Flow
A laserPro Blood Perfusion Monitor (TSI, Inc., Shoreview, MN, USA) was used to monitor and record regional cerebral blood flow (rCBF) prior to ischemia during MCAO and reperfusion. A 1-mm diameter microfiber laser Doppler probe was attached to the skull 4 mm lateral and 2 mm posterior of the bregma. The MCAO was considered adequate if rCBF showed a sharp drop to 25 % of the baseline (pre-ischemia) level, otherwise animals were excluded [26].
Cranial Windows
On the day of cranial window implantation, the animals were anesthetized with an intraperitoneal injection of ketamine (100 mg/mL)–xylazine (20 mg/mL) mixture (1:1) at a dose of 1 mL/kg. The head was shaved and positioned in a stereotactic head holder. A 1-cm area of skin on the dorsal surface of the skull over the right cortical hemisphere was excised, and the periosteum was removed. A 4-mm diameter circular craniotomy was performed using a high-speed drill (Champ-Air Dental Drill, Benco Dental) over the right parietal cortex extending from the attachment of the temporal muscle to the midpoint of the sagittal suture in the coronal direction and aligned to the middle of the sagittal suture, so that the window contained terminal branches of the middle cerebral artery. Normal saline was dripped over the cranium to avoid thermal injury to the cortex. A 5-mm diameter coverglass was then placed over the exposed brain, and an airtight seal was produced using Nexaband Quick Gel. The coverglass provided adequate mechanical protection from infection or contamination. A recovery period of 4 days was allowed between implantation of the cranial window and the induction of transient focal ischemia.
Injection of the CB1R Antagonist, CB2R Agonist, TRPV1 Antagonist, and 5-HT1A antagonist
The CB1R antagonist (SR141716A), the CB2R antagonist (SR144528) (Tocris, MO), and CB2R agonist (O-1966) (BTG, Inc., MA) were dissolved in a DMSO/cremophor/saline mixed solution (1:1:18). The CB1R antagonist (SR141716), the CB2R antagonist (SR144528), and the CB2R agonist (O-1966) were administered at 5 mg/kg. The TRPV1 antagonist capsazepine (Tocris) was dissolved in an ethanol/saline mixed solution (1:9). The 5-HT1A antagonist WAY100135 (Tocris) was dissolved in saline. Both capsazepine and WAY100135 were administered at 10 mg/kg. All compounds were given by inraperitoneal (i.p.) injection.
Intravital Microscopy and Measurement of Cerebral Arteriolar Diameter Changes
The animals were anesthetized and immobilized on a plexiglass stage during MCAO. Intravital microscopy was performed with an epi-illuminiscence microscope (BX10, Olympus, Japan) which was equipped with a digital camera (Cooke 1600, Cooke Corporation, Romulus, MI). FITC-dextran (MW, 150,000) (Sigma, Inc., St. Louis, MO) was injected at 25 mg/kg i.v. before MCAO and was used to visualize the cerebral microvasculature. Cerebral arteriolar changes during MCAO were recorded at different time spots during MCAO and were analyzed offline.
Infarct Volume and Edema Assessment
The animals were euthanized with an overdose of pentobarbital (200 mg/kg, i.p) 24 h after MCAO, and the brains were removed and chilled on ice for 10 min to slightly harden the tissue. Five 2-mm coronal sections were cut using a mouse brain matrix (Zivic Lab, Pittsburgh, PA, USA). The brain sections were placed in 2 % triphenyltetrazolium chloride (TTC) (Sigma, Inc., St. Louis, MO, USA) dissolved in saline and stained for 20 min at 37 °C in the dark. The brain sections were then fixed in 4 % paraformaldehyde at 4 °C for 24 h, and the anterior and caudal face of each section was scanned by a flatbed color scanner (Microtek, Inc., Carson, CA, USA). The resulting images were captured as JPEG files and analyzed with the NIH image software. The infarct volumes were corrected for brain edema/swelling; the hemispheric infarct volume in each section was calculated by subtracting the area of normal TTC-stained tissue in the hemisphere ipsilateral to the ligation from the contralateral nonischemic area to generate the infarct fraction (percent) as described by Swanson et al. and Lin et al. [27, 28]. Cerebral edema was determined by the percent increase of the ipsilateral/contralateral area [29].
Statistical Analysis
Statistical comparisons of infarct size data were performed using a one-way ANOVA followed by the Tukey–Kramer test for post hoc analysis for all groups. The rCBF and arteriolar diameter changes were analyzed by two-way ANOVA (times, treatment) followed by Bonferroni’s test. Data were presented as means ± SEM. A statistically significant difference was assumed at P < 0.05.
Results
Effect on Infarct Volume
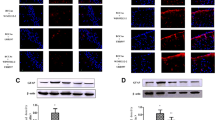
Administration of the CB2R agonist O-1966 1 h prior to the occlusion of the middle cerebral artery in wild-type mice reduced infarct volume at 24 h post-reperfusion by approximately 50 %, and as expected, the CB2R antagonist SR144528 reversed the protective effect of O-1966. By itself, the CB2R antagonist did not significantly affect the infarct volume. In contrast, the CB1R antagonist SR141716A had a protective effect by itself and synergized with O-1966 in terms of protective activity (Fig. 1a). Next we investigated the role of CB1R and CB2R in the protective effect of O-1966/SR141716A in the transient MCAO/R model by using CB1R- or CB2R-deficient mice. The combined O-1966/SR141716A was as effective in CB1R-deficient mice as in littermate controls. In contrast, the protective effect was lost in CB2R-deficient mice (Fig. 1b), indicating that CB2R, but not CB1R, plays a role in the beneficial effect of the O-1966/SR141716A treatment.
a Percent infarcted ischemic hemisphere 24 h following reperfusion in mice treated with vehicle, O-1966, a CB1R antagonist (SR141716A), a CB2R antagonist (SR144528), O-1966 + CBR1 antagonist or O-1966 + CB2R antagonist 1 h prior to MCAO. Groups under the vertical lines differ significantly (p < .05) from the connecting group under the circle (n = 7–8 in each group). The results are shown as infarct fraction (percent) after correction for cerebral edema (adapted from [14]). b Effects of combined treatment in WT, CB2R-deficient, and CB1R-deficient mice, as well as in WT pretreated with O-1966/SR141716A in the presence of capsazepine (a TRPV1 antagonist) or WAY100135 (a 5-HT1A antagonist). The blockers were administered just prior to administration of the cannabinoids. Results are shown as infarct fraction (percent) corrected for cerebral edema. Groups under the vertical lines differ significantly (p < .05) from the connecting group under the circle (n = 7–8 in each group). c Effects of the CB1R antagonist SR141716A, in the presence or absence of the 5-HT1A antagonist WAY100135 on infarct size (*p < .05, n = 5–6 in each group)
Since SR141716A has been characterized as a selective CB1R blocker with no activity on the CB2R [30], its protective effect in the MCAO/R model cannot be mediated through CB2R. Therefore, we tested the effects of selective blockers for the TRPV1 and the 5-HT1A receptor which have been reported to bind cannabinoids. In wild-type mice, capsazepine, a TRPV1 blocker did not affect the protective effect of O-1966/SR141716A, whereas WAY100135, a 5-HT1A blocker reversed the protective effect (Fig. 1b). These results suggest that the 5-HT1A, receptor but not the vanilloid receptor type I, is the best candidate for the effect of SR141716A. This conclusion is supported by the fact that the 5-HT1A blocker also reversed the protective effect of SR141716A alone (Fig. 1c).
Effect on Blood Flow During Occlusion
Since the protective effect of synthetic cannabinoids in ischemia/reperfusion injury could be due at least partially to an increase in blood flow during occlusion of the middle cerebral artery, we recorded regional cerebral blood flow (rCBF) prior to ischemia during MCAO and during reperfusion using a laser Doppler flow monitor. Although administration of either the CB2R agonist O-1966 or of the CB1R antagonist SR141716A did not significantly increase blood flow during occlusion, when administered in combination the two compounds caused a significant increase in blood flow [14]. The increase in blood flow during occlusion was present in wild-type controls, CB1R-deficient mice, and in the presence of the TRPVI blocker. Consistent with the effect on infarct size, CB2R-deficient mice and animals treated with the 5-HT1A blocker exhibited a diminished increase in blood flow (Fig. 2). These results indicate that the combined O-1966/SR141716A treatment results in an increase in blood flow during reperfusion, and that similar to the effect on infarct volume, the effect on blood flow is mediated through CB2R and 5-HT1A receptors.
Effects of the combined O-1966/SR141716A treatment on regional cerebral blood flow (rCBF) during MCAO, as measured by a laser Doppler. Flow was measured in wild-type animals receiving only vehicle or SR141716A and O-1966 in combination. Flow was also measured in wild-type animals treated with the drug combination along with capsazapine and animals treated with the drug combination along with WAY100135. Flow was also measured in CB1- and CB2-deficient animals treated with the drug combination (**p < 0.01, *p < 0.05 vs vehicle-treated control group, n = 5–6 in each group)
Effect on Arteriolar Diameter
The increase in blood flow caused by O-1966/SR141716A might be related to an increase in arteriolar diameter. Arteriolar diameters were measured at different time points by intravital microscopy in mice injected with FITC-dextran prior to MCAO (Fig. 3). The O-1966/SR141716A treatment did not cause any changes in arteriolar diameter in the absence of MCAO. However, following MCAO, O-1966/SR141716A caused a significant increase in arteriolar diameter starting with 10 min after MCAO and persisting for the entire observation period (60 min). The effect was blocked by administration of the 5-HT1A blocker WAY100135 (Fig. 4).
Administration During Reperfusion
Since the increased blood flow induced by O-1966/SR141716A during the occlusion of the middle cerebral artery could be the reason for the protective effect observed with the combined pretreatment, we determined whether the posttreatment was also effective in terms of infarct fraction. Wild-type mice were either pretreated (1 h before MCAO) or posttreated (1 h post-MCAO) with vehicle (control) or O-1966/SR141716A. Posttreatment had a significant effect on reducing infarct fraction (Fig. 5). There was also trend for a reduction cerebral edema, but the edema effects did not reach statistical significance.
Effects of post-MCAO treatment with O-1966/SR141716A. The mice were subjected to MCAO and treated 1 h later with O-1966/SR141716A or vehicle (control) (**p < 0.01, *p < 0.05 vs vehicle-treated control group, n = 6 in each group). Results are shown as infarct fraction (percent) corrected for cerebral edema
Discussion
The interest in the potential for cannabinoids and cannabinoid analogs to provide CNS protection in a number of pathological conditions increased significantly during the last decade. Cannabinoid receptors can be activated by endogenous ligands, including N-arachidonoylethanolamide (anandamide) and 2-arachidonoylglycerol (2-AG) [1]. There is evidence that the production of endogenous cannabinoids increases following stroke [6, 31–34]. CNS ischemia/reperfusion injury also modulates the density of both CB1R and CB2R, although their upregulation occurs at different times, presumably due to the presence of various cell types expressing CB1R and CB2R [14]. Whether the effect of the increased production of endogenous cannabinoids has a positive or negative effect following stroke remains to be determined.
The role of CB1R activation following stroke is controversial. Initially, based on studies of excitotoxicity models, activation of the CB1R was presumed to protect the brain from secondary excitotoxic injury [8–12]. In addition, CB1R-deficient mice were reported to have a poor outcome compared to wild-type controls following ischemia/reperfusion injury [13]. However, later studies raised questions about the protective role of CB1R signaling in stroke. The protective effect was greatly diminished if the CB1R-mediated hypothermic effect was blocked [35]. We and others reported that administration of CB1R antagonists was protective following transient occlusion of the middle cerebral artery [14–18]. This finding does not support a protective effect for CB1R activation following ischemia.
The results related to CB2R activation are much more consistent. There is significant evidence that administration of CB2R agonists attenuates damage resulting from ischemia/reperfusion injury [7, 14]. In addition to their neuroprotective effect, CB2R agonists have the advantage of not eliciting any of the psychoactive effects resulting from CB1R activation. Administration of a CB2R agonist prior to or within a few hours of ischemia/reperfusion injury reduced infarct size and improved motor function. This effect appears to be primarily mediated through an inhibition of harmful inflammatory responses following ischemia [20]. Our laboratory was the first to demonstrate that administration of a selective CB2R agonist (O-1966) attenuated leukocyte rolling and adhesion to pial microvessels following transient middle cerebral artery occlusion. Immunohistochemical staining 24 h later confirmed a decrease in adhesion molecule expression and leukocyte invasion in the brain [20]. CB2R agonists have been shown to decrease leukocyte invasion in a number of other disease models and in in vitro studies [36]. There are numerous potential cellular targets such as leukocytes, endothelial cells, and microglia [37–44]. There is also evidence for an inhibition of inflammatory cytokines/chemokines by CB2R activation [40]. In addition to demonstrating a protective effect following ischemia/reperfusion injury, Murikinati and colleagues found similar protection in a mouse model of permanent ischemia, associated with a reduction in CNS neutrophil invasion [45].
Activation of CB2R triggers a series of signal transduction pathways leading to inhibition of neurotoxic agents such as TNF-α, IL-6, and nitric oxide [46]. Activated microglia plays an active role in cerebral ischemia/reperfusion injury through the release of inflammatory cytokines, proteolytic enzymes, and neurotoxins. In this context, the fact that microglia CB2R receptors are upregulated by inflammatory stimuli [38, 47, 48] is particularly relevant. There is also evidence that the CB1R and CB2R differentially regulate the production of reactive oxygen species. Han and colleagues reported that blocking the CB1R in conjunction with activation of the CB2R suppressed the proinflammatory responses of macrophages [49].
A number of synthetic compounds have been developed to serve as selective ligands for the cannabinoid receptors. Included among those are O-1966 (200 times greater affinity for CB2R than for CB1R) and SR141716A, a selective inhibitor for CB1R [50]. Similar to a previous report from our laboratory [14], we show here that both the CB2R agonist O-1966 and the CB1R antagonist SR141716A reduces infarct size in a transient cerebral ischemia model. In contrast to the CB1R antagonist, the CB2R antagonist SR144528 was not protective by itself and reversed the protective effect of O-1966. This indicates that CB2R signaling plays a role in the protective effect of O-1966 in ischemia/reperfusion injury. Interestingly, the protective effect of the combined O-1966/SR141716 treatment was significantly higher than the effects of separate O-1966 or SR141716 administrations, suggesting the involvement of different receptors. The goal of the current investigation was to evaluate the nature of the receptors involved in the synergistic protective effect of O-1966 plus SR144716A.
The fact that the protective effect of the combined O-1966/SR144716A treatment was maintained in CB1R-deficient mice at the same level as in wild-type controls eliminates the involvement of CB1R. In contrast, the protective effect was lost in CB2R-deficient mice. These results indicate that CB2R, but not CB1R, mediates the protective effect of O-1966/SR144716A. Although this explains the effect of the CB2R agonist O-1966, the receptor mediating the effect of SR141716A remains to be identified, since its affinity for the CB2R is quite low [30]. Although effective as a CB1R antagonist, with little activity at the CB2R, the possibility remains that SR 141716A could act on receptors other than CB1R/CB2R. Cannabinoids have been reported to signal through the TRPV1 and the 5-HT1A receptors [35]. The protective effect of cannabidiol, a cannabinoid with very low affinity for the CB1R and CB2R, in global and focal ischemic injury was shown to be reversed by WAY 100135, a 5-HT1A antagonist [23].
We investigated the possible involvement of TRPV1 and 5-HT1A by evaluating the effect of the combined O-1966/SR144716A treatment in the presence of the TRPV1 antagonist capsazepine and of the 5-HT1A receptor antagonist WAY100135. Blocking the TRPV1 receptor had no influence on the ability to reduce infarct size, indicating that, similar to CB1R, the TRPV1 receptor did not mediate the protective effect of O-1966/SR144716A. In contrast, WAY100135 reversed the protective effect of O-1966/SR144716A indicating that the 5-HT1A receptor participates in the protective response. The involvement of 5-HT1A was also confirmed by the fact WAY100135 reversed the protective effect of SR141716 alone.
In addition to reducing infarct size, the administration of O-1966/SR144716A improved blood flow during the occlusion period, indicating enhanced collateral flow. Neither the CB1R antagonist nor the CB2R agonist, given alone, had a significant effect on blood flow during occlusion. Similar to the results regarding infarct size, CB1R or vanilloid receptor signaling did not affect the improvement in blood flow by O-1966/SR144716A, whereas the lack of CB2R or inhibition of 5-HT1A reduced the effect. This supports the involvement of CB2R and 5-HT1A receptor, but not of CB1R or TRPV1 receptors. Although O-1966/SR144716A did not affect arteriolar diameter under normal conditions, there was a significant increase in arteriolar diameter during occlusion in animals treated with the CB1R antagonist/CB2R agonist combination. The increase in arteriolar diameter was completely inhibited when the 5-HT1A receptor was blocked, again highlighting the involvement of the 5-HT1A receptor.
Finally, since the CB1R antagonist/CB2R agonist treatment prior to occlusion was effective, we examined whether a protective effect can be observed upon administration following reperfusion. The post-MCAO O-1966/SR144716A treatment still provided a protective effect in terms of infarct size and a trend to reduce cerebral edema. In future studies, we plan to examine the effect of the combined treatment on blood flow when administered at various time periods after reperfusion to determine whether the drug combination might attenuate the prolonged delayed hypoperfusion associated with stroke.
In summary, combined administration of the CB1R antagonist SR141716A and of the CB2R agonist O-1966 causes a significant reduction in infarct size in the MCAO/R model. The protective effect involves both the CB2R and the 5-hydroxytryptamine1A receptor. The CB1R or the vanilloid receptor type I do not appear to participate in this response.
References
Pacher P, Batkai S, Kunos G. The endocannabinoid system as an emerging target of pharmacotherapy. Pharmacol Rev. 2006;58(3):389–462.
Howlett AC. Cannabinoid receptor signaling. Handb Exp Pharmacol. 2005;168:53–79.
Turu G, Hunyady L. Signal transduction of the CB1 cannabinoid receptor. J Mol Endocrinol. 2010;44(2):75–85.
Pacher P, Steffens S. The emerging role of the endocannabinoid system in cardiovascular disease. Semin Immunopathol. 2009;31(1):63–77.
Di Marzo V. The endocannabinoid system: its general strategy of action, tools for its pharmacological manipulation and potential therapeutic exploitation. Pharmacol Res. 2009;60(2):77–84.
Hillard CJ. Role of cannabinoids and endocannabinoids in cerebral ischemia. Curr Pharm Des. 2008;14(23):2347–61.
Zhang M, et al. Modulation of cannabinoid receptor activation as a neuroprotective strategy for EAE and stroke. J Neuroimmune Pharmacol. 2009;4(2):249–59.
Shen M, Thayer SA. Cannabinoid receptor agonists protect cultured rat hippocampal neurons from excitotoxicity. Mol Pharmacol. 1998;54(3):459–62.
Shen M, et al. Cannabinoid receptor agonists inhibit glutamatergic synaptic transmission in rat hippocampal cultures. J Neurosci. 1996;16(14):4322–34.
Abood ME, et al. Activation of the CB1 cannabinoid receptor protects cultured mouse spinal neurons against excitotoxicity. Neurosci Lett. 2001;309(3):197–201.
van der Stelt M, et al. Acute neuronal injury, excitotoxicity, and the endocannabinoid system. Mol Neurobiol. 2002;26(2–3):317–46.
Schlicker EK, Kathmann M. Modulation of transmitter release via presynaptic cannabinoid receptors. Trends Pharmacol Sciences. 2001;22(11):565–72.
Parmentier-Batteur S, et al. Increased severity of stroke in CB1 cannabinoid receptor knock-out mice. J Neurosci. 2002;22(22):9771–5.
Zhang M, et al. Modulation of the balance between cannabinoid CB(1) and CB(2) receptor activation during cerebral ischemic/reperfusion injury. Neuroscience. 2008;152(3):753–60.
Berger C, et al. Massive accumulation of N-acylethanolamines after stroke. Cell signalling in acute cerebral ischemia? J Neurochem. 2004;88(5):1159–67.
Muthian S, et al. Anandamide content is increased and CB1 cannabinoid receptor blockade is protective during transient, focal cerebral ischemia. Neuroscience. 2004;129(3):743–50.
Felder CC, et al. LY320135, a novel cannabinoid CB1 receptor antagonist, unmasks coupling of the CB1 receptor to stimulation of cAMP accumulation. J Pharmacol Exp Ther. 1998;284(1):291–7.
Pegorini S, et al. Vanilloid VR1 receptor is involved in rimonabant-induced neuroprotection. Br J Pharmacol. 2006;147(5):552–9.
Zhang M, et al. CB(2) receptor activation attenuates microcirculatory dysfunction during cerebral ischemic/reperfusion injury. Microvasc Res. 2009;78(1):86–94.
Zhang M, et al. Cannabinoid CB(2) receptor activation decreases cerebral infarction in a mouse focal ischemia/reperfusion model. J Cereb Blood Flow Metab. 2007;27(7):1387–96.
Zygmunt PM, et al. Vanilloid receptors on sensory nerves mediate the vasodilator action of anandamide. Nature. 1999;400(6743):452–7.
Smart D, et al. The endogenous lipid anandamide is a full agonist at the human vanilloid receptor (hVR1). Br J Pharmacol. 2000;129(2):227–30.
Mishima K, et al. Cannabidiol prevents cerebral infarction via a serotonergic 5-hydroxytryptamine1A receptor-dependent mechanism. Stroke. 2005;36(5):1077–82.
Russo EB, et al. Agonistic properties of cannabidiol at 5-HT1a receptors. Neurochem Res. 2005;30(8):1037–43.
Hata R, et al. A reproducible model of middle cerebral artery occlusion in mice: hemodynamic, biochemical, and magnetic resonance imaging. J Cereb Blood Flow Metab. 1998;18(4):367–75.
Tsuchiya D, et al. Effect of suture size and carotid clip application upon blood flow and infarct volume after permanent and temporary middle cerebral artery occlusion in mice. Brain Res. 2003;970(1–2):131–9.
Swanson RA, et al. A semiautomated method for measuring brain infarct volume. J Cereb Blood Flow Metab. 1990;10(2):290–3.
Lin TN, et al. Effect of brain edema on infarct volume in a focal cerebral ischemia model in rats. Stroke. 1993;24(1):117–21.
Vannucci SJ, et al. Experimental stroke in the female diabetic, db/db, mouse. J Cereb Blood Flow Metab. 2001;21(1):52–60.
Rinaldi-Carmona M, et al. SR141716A, a potent and selective antagonist of the brain cannabinoid receptor. FEBS Lett. 1994;350(2–3):240–4.
Felder CC, et al. Isolation and measurement of the endogenous cannabinoid receptor agonist, anandamide, in brain and peripheral tissues of human and rat. FEBS Lett. 1996;393(2–3):231–5.
Degn M, et al. Changes in brain levels of N-acylethanolamines and 2-arachidonoylglycerol in focal cerebral ischemia in mice. J Neurochem. 2007;103(5):1907–16.
Schabitz WR, et al. Release of fatty acid amides in a patient with hemispheric stroke: a microdialysis study. Stroke. 2002;33(8):2112–4.
Naccarato M, et al. Possible Anandamide and Palmitoylethanolamide involvement in human stroke. Lipids Health Dis. 2010;9:47.
Hayakawa K, et al. Cannabidiol prevents infarction via the non-CB1 cannabinoid receptor mechanism. Neuroreport. 2004;15(15):2381–5.
Rajesh M, et al. CB2-receptor stimulation attenuates TNF-alpha-induced human endothelial cell activation, transendothelial migration of monocytes, and monocyte-endothelial adhesion. Am J Physiol Heart Circ Physiol. 2007;293(4):H2210–8.
Chen Y, et al. Endothelin-1 and nitric oxide affect human cerebromicrovascular endothelial responses and signal transduction. Acta Neurochir Suppl. 2000;76:131–5.
Maresz K, et al. Modulation of the cannabinoid CB2 receptor in microglial cells in response to inflammatory stimuli. J Neurochem. 2005;95(2):437–45.
Golech SA, et al. Human brain endothelium: coexpression and function of vanilloid and endocannabinoid receptors. Brain Res Mol Brain Res. 2004;132(1):87–92.
Ghosh S, et al. Cannabinoid receptor CB2 modulates the CXCL12/CXCR4-mediated chemotaxis of T lymphocytes. Mol Immunol. 2006;43(14):2169–79.
Carrier EJ, Patel S, Hillard CJ. Endocannabinoids in neuroimmunology and stress. Curr Drug Targets CNS Neurol Disord. 2005;4(6):657–65.
Hillard CJ, et al. Inhibition of 2-arachidonoylglycerol catabolism modulates vasoconstriction of rat middle cerebral artery by the thromboxane mimetic, U-46619. Br J Pharmacol. 2007;152(5):691–8.
Montecucco F, et al. CB2 cannabinoid receptor agonist JWH-015 modulates human monocyte migration through defined intracellular signaling pathways. Am J Physiol Heart Circ Physiol. 2008;294(3):H1145–55.
Montecucco F, et al. CB(2) cannabinoid receptor activation is cardioprotective in a mouse model of ischemia/reperfusion. J Mol Cell Cardiol. 2009;46(5):612–20.
Murikinati S, et al. Activation of cannabinoid 2 receptors protects against cerebral ischemia by inhibiting neutrophil recruitment. FASEB J. 2009;24(3):788–98.
Klein TW, Newton CA, Friedman H. Cannabinoids and the immune system. Pain Res Manag. 2001;6(2):95–101.
Nunez E, et al. Cannabinoid CB2 receptors are expressed by perivascular microglial cells in the human brain: an immunohistochemical study. Synapse. 2004;53(4):208–13.
Stella N. Cannabinoid and cannabinoid-like receptors in microglia, astrocytes, and astrocytomas. Glia. 2010;58(9):1017–30.
Han KH, et al. CB1 and CB2 cannabinoid receptors differentially regulate the production of reactive oxygen species by macrophages. Cardiovasc Res. 2009;84(3):378–86.
Wiley JL, et al. Resorcinol derivatives: a novel template for the development of cannabinoid CB(1)/CB(2) and CB(2)-selective agonists. J Pharmacol Exp Ther. 2002;301(2):679–89.
Acknowledgments
This project was supported, in part, by grants 1RO1AI084065 (DG and RFT), DA P30 13429 (DG, RFT, and MZ), DA005488 (AM and MA), and DA009789 (AM and MA) from the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhang, M., Mahadevan, A., Amere, M. et al. Unique Effects of Compounds Active at Both Cannabinoid and Serotonin Receptors During Stroke. Transl. Stroke Res. 3, 348–356 (2012). https://doi.org/10.1007/s12975-012-0197-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12975-012-0197-2