Abstract
Avian pathogenic E. coli (APEC), an extra-intestinal pathogenic E. coli (ExPEC), causes colibacillosis in poultry and is also a potential foodborne zoonotic pathogen. Currently, APEC infections in poultry are controlled by antibiotic medication; however, the emergence of multi-drug-resistant APEC strains and increased restrictions on the use of antibiotics in food-producing animals necessitate the development of new antibiotic alternative therapies. Here, we tested the anti-APEC activity of multiple commensal and probiotic bacteria in an agar-well diffusion assay and identified Lacticaseibacillus rhamnosus GG and Bifidobacterium lactis Bb12 producing strong zone of inhibition against APEC. In co-culture assay, L. rhamnosus GG and B. lactis Bb12 completely inhibited the APEC growth by 24 h. Further investigation revealed that antibacterial product(s) in the culture supernatants of L. rhamnosus GG and B. lactis Bb12 were responsible for the anti-APEC activity. The analysis of culture supernatants using LC–MS/MS identified multiple novel bioactive peptides (VQAAQAGDTKPIEV, AFDNTDTSLDSTFKSA, VTDTSGKAGTTKISNV, and AESSDTNLVNAKAA) in addition to the production of lactic acid. The oral administration (108 CFU/chicken) of L. rhamnosus GG significantly (P < 0.001) reduced the colonization (~ 1.6 logs) of APEC in the cecum of chickens. Cecal microbiota analysis revealed that L. rhamnosus GG moderated the APEC-induced alterations of the microbial community in the cecum of chickens. Further, L. rhamnosus GG decreased (P < 0.05) the abundance of phylum Proteobacteria, particularly those belonging to Enterobacteriaceae (Escherichia-Shigella) family. These studies indicate that L. rhamnosus GG is a promising probiotic to control APEC infections in chickens. Further studies are needed to optimize the delivery of L. rhamnosus GG in feed or water and in conditions simulating the field to facilitate its development for commercial applications.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Avian pathogenic E. coli (APEC), an extra-intestinal pathogenic E. coli (ExPEC), is one of the most common bacterial pathogens of poultry [1, 2]. APEC continues to pose a formidable challenge to the poultry industry worldwide despite improvements in the poultry production systems over the years [1, 2]. APEC infects all species of poultry, including broilers, layers, breeders, and turkeys of all ages (9.52 to 36.73% prevalence), and in all types of production systems [1, 2]. In the United States (US), it is estimated that at least 30% of commercial flocks are affected by APEC at any point of time [2, 3]. APEC causes a wide range of localized and systemic infections in poultry, including yolk sac infection, omphalitis, respiratory tract infection, swollen head syndrome, septicemia, polyserositis, coligranuloma, enteritis, cellulitis, and salphingitis, collectively referred as colibacillosis [1, 2, 4]. Colibacillosis results in high morbidity and mortality (up to 20%) and decreased meat (2% decline in body weight) and egg production (loss up to 15%) [1, 2, 4]. More severely, in young chickens, APEC is associated with up to 53.5% mortality [1, 2, 4]. Further, APEC is also responsible for 36–43% of carcass condemnations at slaughter [1, 2, 4]. Altogether, APEC infections result in multi-million dollars annual losses to all facets of the poultry industry and remain as a serious impediment to the sustainable poultry production worldwide.
APEC has been also reported as a potential foodborne zoonotic pathogen, which can be transmitted to humans through consumption of contaminated poultry products [2, 5]. In particular, APEC has genetic similarities with human ExPECs (uropathogenic E. coli (UPEC) and neonatal meningitis E. coli (NMEC)), possesses virulence genes characteristics of UPEC/NMEC, and causes urinary tract infection and meningitis in rodent models as similar to UPEC and NMEC [2]. Colicin-V (ColV) plasmids specific to APEC have been also detected in human clinical E. coli isolates suggesting evidence of potential foodborne transmission of APEC from poultry to humans even though concrete evidence is still lacking [2, 5]. In addition, APEC is also considered a source of antibiotic resistance genes (ARGs) to human pathogens, which can make the human infections difficult to treat [6]. Thus, APEC is a threat to both poultry and human health.
Antibiotics are commonly used to control APEC infections in poultry [2, 7, 8]. However, APEC resistance to multiple antibiotics, including tetracyclines, sulfonamides, aminoglycosides, quinolones, and β-lactams, has been reported worldwide [2, 9]. Up to 92% of APEC isolated in the US, Europe, and Australia were resistant to three or more antibiotics, particularly against tetracyclines, aminoglycosides, and sulfonamides [2, 10]. Further, many countries (particularly US and European Union) have recommended the limited use of antibiotics in food-producing animals, including poultry, with a goal of reducing the selection pressure and subsequent emergence and transmission of antibiotic-resistant bacteria to humans [2, 11]. However, limiting on-farm use of antibiotics could significantly increase morbidity and mortality, thereby compromising production efficiency, food safety, and security [12]. Therefore, there is a critical need for developing new effective alternatives to antibiotics which can enhance the poultry health and production, mitigate antibiotic resistance problem, promote antibiotic stewardship, and safeguard the human health.
Probiotics are defined as live microorganisms which when administered in adequate amounts confer health benefits to the host [13]. Probiotics exhibit antibacterial activities, promote the growth, maintain the healthy gut, and strengthen the immune system; therefore, these can serve as alternatives to antibiotics to control the bacterial infections as well as to enhance the production [14]. Probiotics exert their antibacterial effects through different mechanisms of action, such as (i) enhancement of epithelial barrier functions, (ii) competitive exclusion of pathogenic microorganisms, (iii) production of antimicrobial substances, and (iv) modulation of the host immune system [14,15,16]. Lacticaseibacillus rhamnosus, Lactobacillus acidophilus, Lactobacillus johnsonii, Limosilactobacillus reuteri, Lactiplantibacillus plantarum subsp. plantarum, Limosilactobacillus fermentum, Lactobacillus helveticus, Lactobacillus gasseri, Bifidobacterium bifidum, B. lactis, B. infantis, and B. breve are the most commonly used probiotics in humans and food animals [17,18,19]. These probiotics have shown antimicrobial activities against various bacterial and viral pathogens, including Helicobacter, Salmonella, Listeria, Shigella, E. coli, Vibrio, Campylobacter, and Rotavirus [16, 18]. Other probiotics have also shown proven benefits to the poultry health, particularly against Salmonella and Campylobacter [20,21,22,23,24,25,26,27,28]. L. plantarum subsp. plantarum, L. reuteri, Ligilactobacillus salivarius, Lacticaseibacillus casei, and E. coli Nissle 1917 reduced the Salmonella colonization [20, 24, 26, 28, 29]. L. salivarius, L. johnsonii, and L. casei reduced the colonization of Campylobacter [22, 27, 29]. L. plantarum subsp. plantarum reduced the APEC colonization [23,24,25]. However, there is overall lack of studies specifically demonstrating the activity of probiotic species against APEC. Further, information is also lacking on the bioactive substances secreted/released by these probiotics as well as their interactions with commensal microbes and/or pathogens in the gut which limits the understanding of the probiotic’s mechanism(s) of action and reproducible use in industrial settings.
The objective of this study is to identify the probiotic species effective against APEC infection in poultry. Here, we identified probiotic bacteria, L. rhamnosus GG, effective in reducing APEC colonization in chickens. We also identified novel peptides derived from L. rhamnosus GG which are inhibitory to APEC growth. Further, we investigated the interactions of L. rhamnosus GG with commensal microbes and APEC in the gut microbiome of chickens. Our results show that L. rhamnosus GG can be developed as a preventative measure against APEC infections in chickens.
Materials and Methods
Bacterial Strains and Culture Conditions
The commensal and probiotic bacteria used in this study along with their culture conditions and media requirements for growth are listed in Table 1. BD GasPak™ EZ container system (Becton, Dickinson and Company, NJ, USA) or MiniMacs anaerobic workstation (Microbiology International, MD, USA) was used to grow commensal and probiotic bacteria requiring the anaerobic conditions. APEC serotype O78, primarily used in this study, was kindly provided by Dr. Johnson (University of Minnesota, Saint Paul, MN, USA) and was isolated from the lung of a turkey clinically diagnosed with colibacillosis [30]. Other APEC serotypes O1, O2, O8, O15, O18, O35, O109, and O115 were kindly provided by Drs. Nolan and Logue (University of Georgia, Athens, GA, USA). Luria–Bertani (LB) broth (BD Difco™) was used for the routine propagation of APEC serotypes. APEC serotypes stored at − 80 °C in glycerol were grown overnight in LB broth at 37 °C with shaking at 200 rpm.
Agar-well Diffusion Assay
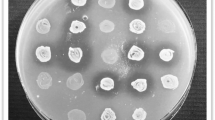
To determine the inhibitory activity of commensal and probiotic bacteria against APEC, agar-well diffusion assay was conducted as described previously [31]. Briefly, LB agar plate was spread with 100 µL of APEC O78 (107 CFU/mL), and 100 µL of fully grown stationary phase whole cultures (adjusted to OD600: 1) of commensal and probiotic bacteria was aliquoted into the wells bored in the agar plate. The plate was incubated at 37 °C, and zone of inhibition was measured at 12 h and 24 h post-incubation. The inhibitory activity of L. rhamnosus GG and B. lactis Bb12 was also tested with different culture volumes (200 µL, 150 µL, and 50 µL) and against other APEC serotypes as described above. Assay was also conducted with cell-free supernatants (CFSs) of L. rhamnosus GG and B. lactis Bb12 and supernatant-free L. rhamnosus GG and B. lactis Bb12 itself. CFSs were prepared by centrifugation of whole cultures at 10,000 × g for 10 min at 4 °C followed by filtration through 0.22 µm filter. The supernatant-free cultures were washed once and resuspended in PBS to check the activity of L. rhamnosus GG and B. lactis Bb12 itself. Two independent experiments were conducted.
Co-culture Assay
To determine the anti-APEC activity of L. rhamnosus GG and B. lactis Bb12 in liquid media, co-culture assay was conducted as previously described [32]. Briefly, 107 CFU/mL of L. rhamnosus GG or B. lactis Bb12 and APEC O78 were incubated together in 5 mL of co-culture media (contains 100% MRS and 100% LB; pH 6.75 at 0 h) at 37 °C under anaerobic conditions with shaking at 50 rpm followed by the quantification of viable APEC O78 every 12 h until 24 h. Lactobacillus acidophilus and Levilactobacillus brevis were used for the comparison of anti-APEC activity as these two Lactobacillus species are commonly used probiotics in animal and human studies, and several commercial probiotics currently being used in poultry industry contain these Lactobacillus species in their formulations. Two independent experiments were conducted.
Trans-well Migration Assay
To determine if the anti-APEC activity of L. rhamnosus GG and B. lactis Bb12 is due to bacterial cells itself or due to bacteria secreted/released products, trans-well migration assay was conducted. Assay was conducted using 0.22 µm Ultrafree-MC microcentrifuge tubes with removable filters (Millipore Sigma, MA, USA). Briefly, 16–18 h grown L. rhamnosus GG and B. lactis Bb12 cultures were aliquoted into the tube containing filter, whereas APEC O78 culture (107 CFU/mL) was aliquoted into the microcentrifuge tube below the filter. The filter tube was removed before aliquoting 700 μL of APEC culture into the microcentrifuge tube, then filter tube was inserted back, and 700 μL of L. rhamnosus GG/B. lactis Bb12 culture was added above the filter in the filter tube. Sufficient volume (700 μL) was added to the microcentrifuge tube to allow contact with the tube containing the filter. The tubes were incubated at 37 °C under anaerobic conditions with shaking at 50 rpm. The viability of APEC O78 was quantified at 12 h and 24 h post-incubation. Two independent experiments were conducted.
Effect of pH on Anti-APEC Activity
It is reported in studies that Lactobacillus and Bifidobacterium strains exhibit antimicrobial activity by lowering the pH of the media [32, 33]. To observe the pH change, pH of the L. rhamnosus GG and B. lactis Bb12 cultures grown in co-culture media (MRS + LB) were measured every 12 h until 48 h in a separate experiment. To determine the effect of pH on L. rhamnosus GG and B. lactis Bb12 inhibitory activity against APEC O78, co-culture media (MRS + LB) was adjusted to different pH (4.0, 4.5, 5.0, 5.5, and 6.0) using 3 M HCL and tested for anti-APEC activity as described above. Additionally, pH tolerance of APEC O78 was determined by growing APEC in LB media adjusted to different pH (4.0, 4.5, 5.0, 5.5, and 6.0) for 24 h [34]. Two independent experiments were conducted.
Characterization of Nature of Antibacterial Product(s)
To understand the nature of secreted/released product(s), CFSs of 24 h grown L. rhamnosus GG and B. lactis Bb12 cultures were subjected to heat and proteolytic enzyme treatments as described previously [35, 36]. The CFSs were subjected for heat (121 °C; autoclave) or proteinase K (1 mg/mL, 37 °C for 3 h) treatment and tested for inhibitory activity against APEC O78 in an agar-well gel diffusion assay as described above. Further, L. rhamnosus GG and B. lactis Bb12 CFSs were fractionated using a Amicon® Ultra centrifugal filter (Millipore Sigma) with mol. wt. cut-off (MWCO) of 3 kDa. The filtrates containing products less than 3 kDa were tested for inhibitory activity and compared with the inhibitory activity of unfractionated CFSs of L. rhamnosus GG and B. lactis Bb12 cultures. Two independent experiments were conducted.
Profiling of Organic Acid Production
To quantify the organic acids in the CFSs of L. rhamnosus GG and B. lactis Bb12 cultures, LC–MS/MS coupled with isotope-labeled chemical derivatization method was used as described previously [37]. For the preparation of CFSs, L. rhamnosus GG and B. lactis Bb12 were grown overnight, adjusted to OD600 1.0 (~ 109 CFU/mL), and sub-cultured (500 μL) in fresh media (14.5 mL) for 24 h at 37 °C under anaerobic conditions. The quantity of organic acids in the CFSs of L. rhamnosus GG/B. lactis Bb12 and APEC 078 co-cultures was also determined as above. Lactobacillus acidophilus and Levilactobacillus brevis were used to compare the organic acid profiles. The LC–MS/MS Poroshell 120 SB C18 column containing solvent A, H2O + 0.1% formic acid, and solvent B, acetonitrile (MeCN) + 0.1% formic acid, was used for the LC–MS/MS analysis. Standard solutions of acetic, propionic, butyric, and lactic acids (Sigma-Aldrich, MO, USA) were used to generate the calibration curves and quantify the concentration of organic acids in the CFSs. Sodium 13C-lactic acid was used as an internal standard.
Identification of Bioactive Peptides
To identify the bioactive peptides present in L. rhamnosus GG and B. lactis Bb12 CFSs, LC–MS/MS was used as described previously [38]. To prepare the CFSs, L. rhamnosus GG and B. lactis Bb12 were grown anaerobically for 24 h, centrifuged (1000 rpm, 10 min, 25 °C), and washed with sterile water. The L. rhamnosus GG and B. lactis Bb12 pellets were resuspended in sterile water containing 2% glucose and incubated for 24 h under anaerobic conditions [38]. The L. rhamnosus GG and B. lactis Bb12 cultures were then centrifuged (1000 rpm, 10 min, 4 °C), and CFSs were separated by filtering through 0.22 µm filter. Lactobacillus acidophilus and Levilactobacillus brevis were used to compare the peptide profiles. To prepare the samples for LC–MS/MS run, CFSs (1.8 mL) were passed three times through HyperSep™ Hypercarb™ SPE cartridge (50 mg; ThermoFisher Scientific, MA, USA). The cartridge was washed twice with water (150 µL) to remove salts, and peptides were eluted (20 µL) using 50% MeCN and 0.1% trifluoroacetic acid (TFA). The elutes (0.5 µL) were injected into LC–MS/MS EasySpray C18-Fusion column set at HCD (higher energy collision dissociation) and CID (ion-trap-based collision-induced dissociation) collision energy settings. The solvent A, H2O + 0.1% formic acid, and solvent B, MeCN + 0.1% formic acid, were used. The data generated were analyzed using Proteome Discoverer 2.2 software (ThermoFisher Scientific) using UniProt Lactobacillus or Bifidobacterium database with settings of no modifications and non-specific cleavage.
The five common highly abundant peptides in CFSs of both L. rhamnosus GG and B. lactis Bb12 (FSAVALSAVALSKPGHVNA, AESSDTNLVNAKAA, VQAAQAGDTKPIEV, AFDNTDTSLDSTFKSA, and VTDTSGKAGTTKISNV) were synthesized (GenScript, NJ, USA) and tested for anti-APEC activity by conducting kinetic time-inhibition assay as described previously [7]. Briefly, peptides dissolved in dimethyl sulfoxide (DMSO) at 200 mM concentrations were added (12 mM; final concentration of 6% DMSO) to APEC suspension (105 CFU/mL; LB media) in a 96-well plate. The plate was then incubated in TECAN Sunrise™ absorbance microplate reader (NC, USA) at 37 °C with OD600 measurement set at every 30 min for 12 h [7]. Untreated APEC (0% DMSO) and APEC treated with 6% DMSO were included as controls. DMSO at 6% in our earlier study showed no significant effect on APEC growth, only when used at 8% concentration significant effect on APEC growth was observed [7]. Three independent experiments were conducted.
Cell Culture Studies
The anti-APEC activity of L. rhamnosus GG and B. lactis Bb12 CFSs was studied in cell culture model using polarized HT-29 (Human Colorectal Adenocarcinoma Cell Line; ATCC HTB-38) cells, maintained in complete Dulbecco’s modified Eagle’s medium (DMEM, Gibco, MA, USA) supplemented with 10% fetal bovine serum (FBS, Gibco), 2 mM L-glutamine, 5 mM galactose, 1% penicillin–streptomycin (PS) solution, and 0.1 mM non-essential amino acids (NEAA) [39]. To evaluate the effect of CFSs of L. rhamnosus GG and B. lactis Bb12 on APEC O78 adhesion to HT-29 cells, 10% CFSs from the 24 h grown L. rhamnosus GG and B. lactis Bb12 cultures were added to the wells containing HT-29 monolayers, which was incubated for 3 h as described previously [40]. The CFSs diluted to 10% were used as they were non-toxic to HT-29 cells as well as non-inhibitory to APEC growth at this concentration (data not shown). Prior to treatment with CFSs, the polarized HT-29 cells were washed and incubated for 2 h in DMEM containing no antibiotics and FBS. After treatment, the HT-29 cells were washed with DPBS, infected with APEC O78 (MOI 100) and incubated for 3 h. For infection, the logarithmic phase grown APEC O78 was pelleted, washed, and resuspended in DMEM at OD600 0.05 (5 × 107 CFU/mL). The infected HT-29 cells were washed three times, and the adherent APEC O78 was enumerated after lysis with 0.5% Triton X-100 followed by serial dilution (ten-fold) and plating on LB agar plate.
To determine the effect of CFSs on APEC O78 invasion, the HT-29 cells were pre-treated with CFSs and infected with APEC O78 as described above. Following 3-h incubation with APEC O78, the HT-29 cells were washed three times and treated with DMEM containing 150 µg/mL gentamicin for 1 h. The HT-29 cells were washed twice with DPBS, lysed and invaded APEC O78 was quantified as described above. Two independent experiments were conducted with three replicates in each experiment. The effect of pre-treatment (3 h) of L. rhamnosus GG and B. lactis Bb12 cells itself after separation of culture supernatant by centrifugation and washing as above was also determined. The washed L. rhamnosus GG and B. lactis Bb12 pellets were resuspended in DMEM at OD600 1.0 (~ 109 CFU/mL) prior to adding into the wells containing HT-29 monolayers, and procedure as above was followed.
Scanning Electron Microscopy (SEM)
To determine the modes of action of L. rhamnosus GG and B. lactis Bb12, APEC O78 was treated with CFSs of L. rhamnosus GG and B. lactis Bb12 and imaged using Hitachi S-4700 scanning electron microscope as described previously [7]. Briefly, APEC O78 culture adjusted at OD600 1.0 (1 × 109 CFU/mL) was treated with CFSs prepared from 24 h grown L. rhamnosus GG and B. lactis Bb12 for 2 h at 37 °C with shaking at 200 rpm. Following treatment, culture was processed for SEM as described previously [7].
Efficacy of L. rhamnosus GG and B. lactis Bb12 in Chickens
Animal study was approved by The Ohio State University Institutional Animal Care and Use Committee (IACUC, protocol # 2010A00000149). Chickens were euthanized using CO2 following American Veterinary Medical Association (AVMA) guidelines. Standard animal husbandry practices were followed throughout the experiment. Feed and water were provided ad libitum.
The efficacy of L. rhamnosus GG and B. lactis Bb12 and their combination (1:1) was tested in 1-day-old specific pathogen free (SPF) Leghorn chickens (n = 10/group). From day 1, L. rhamnosus GG and B. lactis Bb12 were administered orally (200 µL in PBS; 108 CFU/chicken), once a day, until day 14. On day 7, chickens were infected orally with rifampicin-resistant (Rifr) APEC O78 (7.5 × 107 CFU/chicken) as described previously [23, 24, 41]. Before the infection, random cloacal swabs were collected from each group (n = 2/group) to confirm the absence of APEC. Chickens infected with APEC but not treated with probiotic (positive control, PC) and not infected with APEC and not treated with probiotic (negative control, NC) were included as controls. On day 15, chickens were euthanized, and tissues (cecum, liver, and heart) were aseptically collected for APEC quantification. The tissues were homogenized in PBS, and the suspensions were ten-fold serially diluted and plated on MacConkey agar plates containing 50 µg/mL rifampicin. Body weight of chickens was measured at days 1 and 15.
The L. rhamnosus GG-specific quantitative polymerase chain reaction (qPCR) was performed to assess the presence of L. rhamnosus GG in the cecum of L. rhamnosus GG-treated chickens as previously described [42]. The primers (Table S1) were obtained from Integrated DNA Technologies (IDT). The qPCR (two-step) was performed using Maxima SYBR Green/ROX qPCR master mix (ThermoFisher Scientific) following the manufacturer’s instructions in a RealPlex2 Mastercycler® (Eppendorf, CT, USA) with single cycle of 95 °C for 10 min and 40 cycles of amplification with 95 °C for 15 s denaturing and 60 °C for 1 min annealing temperatures. PureLink™ Microbiome DNA Purification Kit (ThermoFisher Scientific) was used to extract the microbial DNA from the cecal contents (approximately 0.2 g) of the chickens. RNase A treatment (2–3 µL of 100 mg/mL solution per sample; Qiagen, MD, USA) was performed to remove the RNA. DNA quantity and quality were measured using NanoDrop 2000c Spectrophotometer (ThermoFisher Scientific). The standard L. rhamnosus GG qPCR curve was used to enumerate the L. rhamnosus GG which was generated by making ten-fold serial dilutions of L. rhamnosus GG DNA extracted (MasterPure™ DNA Purification Kit; Epicentre, WI, USA) from OD600 1.0 L. rhamnosus GG (~ 109 CFU/mL) culture. The qPCR was also performed for microbial DNA extracted from cecal contents of NC chickens to confirm the specificity of L. rhamnosus GG primers.
Cecal Microbiome Analysis
To investigate the impact of L. rhamnosus GG treatment on the cecal microbiome of chickens, 16S rRNA-based microbiome study was conducted as previously described [43, 44]. DNA was extracted from 0.2 g of cecal contents using PureLink™ Microbiome DNA Purification Kit (ThermoFisher Scientific) and treated with RNase A (2–3 µL of 100 mg/mL solution per sample; Qiagen). DNA quantity and quality were measured using NanoDrop 2000c Spectrophotometer (ThermoFisher Scientific). The extracted DNA samples were subjected to 16S rRNA V4-V5 sequencing at the molecular and cellular imaging center (MCIC) (https://mcic.osu.edu/genomics/illumina-sequencing). Amplicon libraries were prepared using IFU KAPA HiFi HotStart ReadyMixPCR Kit (Roche, NJ, USA), and PCR clean-up was performed using Agencourt AMPure XP beads (BECKMAN COULTER Life Sciences, CA, USA). Nextera XT DNA Library Preparation Kit (Illumina, CA, USA) was used to generate Illumina library, and sequencing was performed using Illumina MiSeq platform generating paired end 300-bp reads.
For the microbiota analysis, QIIME (Quantitative Insights Into Microbial Ecology) 2 bioinformatics platform [45] (https://qiime2.org/) was used. Quality control of the raw reads was performed using FastQC 0.11.8 (Babraham Bioinformatics). Trimmomatic-0.33 was used to trim the adaptor and other Illumina-specific sequences (http://www.usadellab.org/cms/?page=trimmomatic). The trimmed sequences (fastq.gz) were imported into the QIIME 2 as a manifest file format (PairedEndManifestPhred33V2). The feature table construction and additional filtering of the sequences was performed using DADA2 [46]. The taxonomic analysis was performed using Naive Bayes classifiers trained on Silva 132 99% OTUs (silva-132–99-nb-classifier.qza) database. The phylogenetic diversity was analyzed using align-to-tree-mafft-fasttree pipeline, and alpha (Shannon’s diversity index) and beta diversity (Bray–Curtis distance) were analyzed using core-metrics-phylogenetic pipeline (https://docs.qiime2.org/2019.7/tutorials/moving-pictures/). The statistical difference (P < 0.05) in the taxonomic composition between the L. rhamnosus GG treated, PC (APEC infected but not treated with L. rhamnosus GG), and NC (non-APEC infected and non-L. rhamnosus GG treated) groups was determined using the Man-Whitney U test. The alpha and beta diversity were analyzed using the Kruskal–Wallis and PERMANOVA tests (P < 0.05), respectively.
Statistical Analysis
The statistical significance (P < 0.05) of bacterial viability reduction and inhibition of adhesion and invasion was calculated using two-way ANOVA followed by the Bonferroni post-test. The statistical significance (P < 0.05) of treatment on reduction of APEC load and increment in body weight was calculated using the Man-Whitney U test.
Results
L. rhamnosus GG and B. lactis Bb12 Induced Strong Zone of Inhibition Against APEC Serotypes
Of the several whole cultures of commensal and probiotic bacteria tested (Table 1), L. rhamnosus GG and B. lactis Bb12 induced large zone of inhibition against APEC 078 at 12 h (14.5 ± 0.5 and 13.5 ± 0.5) and 24 h (12.5 ± 0.5 and 11.5 ± 0.5) post-incubation in agar-well diffusion assay (Table 2). Enterococcus faecalis, Levilactobacillus brevis, Bifidobacterium adolescentis, and Bacteroides thetaiotaomicron also induced zone of inhibition at 12 h (9.5 ± 0.5, 9.5 ± 0.5, 12.5 ± 0.5, and 9.5 ± 0.5, respectively); however, no zone of inhibition was observed at 24 h. The decrease in inhibition at 24 h might be due to lack of continuous production of inhibitory substances in solid media by commensal and probiotic bacteria as stationary phase grown cultures were used in the assay. Slight but not measurable zone of inhibition was also observed with Lactobacillus acidophilus, Streptococcus bovis, and Bifidobacterium longum (data not shown). No zone of inhibition was observed with E. coli Nissle 1917 and E. coli G58-1.
The zone of inhibition induced by L. rhamnosus GG and B. lactis Bb12 against APEC 078 was volume dependent. Large zone of inhibition was observed when incubated with 200 µL (18.5 ± 0.5 and 17.5 ± 0.5) of culture volume followed by 150 (16.5 ± 0.5 and 15.5 ± 0.5), 100 µL (14.5 ± 0.5 and 13.5 ± 0.5), and 50 µL (10.5 ± 0.5 and 10.0 ± 1.0). Further, L. rhamnosus GG and B. lactis Bb12 also induced similar zone of inhibition against other multiple pre-dominant APEC (O1, O2, O8, O15, O18, O35, O109, and O115) serotypes (Table S2).
No Viable APEC Was Detected When APEC Was Incubated with L. rhamnosus GG and B. lactis Bb12
The growth of APEC was not compromised in co-culture (100% MRS + 100% LB) media as compared to LB media (Fig. S1A). The significant reduction (P < 0.001) in viable APEC was observed at 12 h when incubated with L. rhamnosus GG and B. lactis Bb12 in co-culture media, whereas no reduction was observed when incubated with L. acidophilus and L. brevis. At 24 h, no viable APEC was recovered when incubated with L. rhamnosus GG and B. lactis Bb12, whereas slight reduction (< 2 logs) was also observed when incubated with L. acidophilus and L. brevis (Fig. 1A).
A Viability of APEC in co-culture assay when incubated together with different probiotics. APEC O78 culture grown alone in co-culture media was used as a control. B Viability of APEC in trans-well migration assay. L. rhamnosus GG and B. lactis Bb12 cultures were aliquoted into the tube containing filter, whereas APEC O78 culture was aliquoted in to the microcentrifuge tube below the filter. APEC O78 culture grown with APEC O78 culture above the filter was used as a control. LGG, Lacticaseibacillus rhamnosus GG; Bb12, Bifidobacterium lactis Bb12; LA, Lactobacillus acidophilus; Lbrev, Levilactobacillus brevis; *P < 0.05, ***P < 0.001, two-way ANOVA Bonferroni post-test
L. rhamnosus GG and B. lactis Bb12 Secreted/Released Products Are Responsible for Anti-APEC Activity
As observed in co-culture assay, both L. rhamnosus GG and B. lactis Bb12 CFSs significantly (P < 0.001) reduced the viable APEC population at 12 h, and no viable APEC was detected at 24 h (Fig. 1B) in trans-well migration assay. Further, L. rhamnosus GG and B. lactis Bb12 CFSs also induced the zone of inhibition similar to L. rhamnosus GG and B. lactis Bb12 whole culture in agar-well diffusion assay (Table 3). However, no zone of inhibition was induced by L. rhamnosus GG and B. lactis Bb12 cells itself after CFSs were separated and cells resuspended in PBS. Further, the heat- and proteolysis-treated CFSs of L. rhamnosus GG and B. lactis Bb12 retained the anti-APEC activity similar to untreated CFSs (Table 3). Similarly, fractionated (< 3 kDa) CFSs of L. rhamnosus GG and B. lactis Bb12 also exhibited the anti-APEC activity similar to unfractionated CFSs (Table 3), suggesting that secreted/released products are heat stable, proteolysis resistant, and of low mol. wt. in size.
The shortened bacterial cells measuring ~ 0.5–1 µM with bulbous swelling were observed after treatment with L. rhamnosus GG and B. lactis Bb12 CFSs as compared to untreated bacterial cells which measured ~ 1.5–2 µM in length (Fig. 2).
Scanning electron microscopy (SEM) images showing morphology of untreated APEC or APEC treated with CFSs (cell-free supernatants) of L. rhamnosus GG and B. lactis Bb12. APEC was treated with CFSs prepared from 24 h grown culture of L. rhamnosus GG and B. lactis Bb12 for 2 h at 37 °C with shaking at 200 rpm. Bars: 1 μM
Activity of L. rhamnosus GG and B. lactis Bb12 Is pH-Independent
It has been previously shown that probiotic lactic acid bacteria exert inhibitory effect against pathogenic bacteria by lowering the pH [32, 33]. Therefore, we monitored the changes in pH when APEC was co-cultured with L. rhamnosus GG, B. lactis Bb12, L. acidophilus, and L. brevis. At 24 h, the lowest pH was observed when APEC was co-cultured with B. lactis Bb12 (4.12), followed by L. rhamnosus GG (4.37), L. acidophilus (4.66), and L. brevis (4.96) (Table 4). We further quantified the viability of APEC in co-culture media adjusted to different pH (ranging 4.0 to 6.0) in order to determine the effect of pH on L. rhamnosus GG and B. lactis Bb12 anti-APEC activity. No significant effect on the viability of APEC was observed, except at pH 4.0 (Fig. S1B); however, significant number (~ 5.4 logs) of APEC was still viable even at pH 4 after 24 h compared to no viable APEC recovered when incubated with L. rhamnosus GG and B. lactis Bb12 (Fig S1B). APEC was also pH-tolerant up to pH 4.0 when incubated for 24 h in LB media alone adjusted to different pH (ranging 4.0 to 6.0; data not shown). These studies suggest that pH alone is not responsible for anti-APEC activity of L. rhamnosus GG and B. lactis Bb12.
L. rhamnosus GG and B. lactis Bb12 Contain Lactic Acid and Multiple Small Peptides in Their Cell-Free Supernatants
LC–MS/MS coupled with isotope-labeled chemical derivatization method was used to quantify the organic acids produced by L. rhamnosus GG, B. lactis Bb12, L. acidophilus, and L. brevis [37]. The standard curves of lactic (y = 0.0006x-0.2761, R2 = 0.9865), acetic (y = 0.0006x-0.3419, R2 = 0.9807), propionic (y = 0.00012x-0.577, R2 = 0.9839), and butyric acids (y = 0.0017x-0.6008, R2 = 0.9855) were generated to quantitate the concentration of organic acids in CFSs (Fig. S2A–D). Lactic acid was predominantly present in all CFSs (Fig. 3A). The highest concentration of lactic acid was observed in CFS of B. lactis Bb12 (0.090 M) followed by L. rhamnosus GG (0.067 M), L. brevis (0.059 M), and L. acidophilus (0.044 M). Interestingly, higher concentrations of lactic acid were produced by L. rhamnosus GG (0.26 M), B. lactis Bb12 (0.24 M), and L. acidophilus (0.19 M) when co-cultured with APEC compared to monoculture (Fig. 3B).
Concentration of organic acids in cell-free supernatants (CFSs) of different probiotics when cultured alone (A) or co-cultured with APEC (B). MRS media were used as a control in monoculture study, and APEC O78 culture grown alone in co-culture media was used as a control in co-culture study. LGG, Lacticaseibacillus rhamnosus GG; Bb12, Bifidobacterium lactis Bb12; LA, Lactobacillus acidophilus; Lbrev, Levilactobacillus brevis
LC–MS/MS analysis of CFSs eluted through HyperSep™ Hypercarb™ SPE cartridge was also performed to identify the bioactive molecules secreted/released by L. rhamnosus GG, B. lactis Bb12, L. acidophilus, and L. brevis [38]. At HCD (higher energy collision dissociation) setting, 57 peptides (Dataset 1) were identified, whereas 152 peptides were identified at CID (ion-trap-based collision-induced dissociation) setting (Dataset 2). A total of 33 peptides (Table 5) of mol. wt. less than 3 kDa were identified in common in both HCD and CID settings. Consistent with strong anti-APEC activity of L. rhamnosus GG and B. lactis Bb12 compared to L. acidophilus and L. brevis, these peptides were mostly present in CFSs of L. rhamnosus GG and B. lactis Bb12.
L. rhamnosus GG and B. lactis Bb12 Cell-Free Supernatants Reduced the Adhesion and Invasion of APEC in HT-29 Cells
The HT-29 cells were pre-treated with 10% CFSs (concentration non-toxic to HT-29 cells and non-inhibitory to APEC growth) for 3 h to determine the effect of CFSs on adhesion and invasion of APEC. Both the CFSs significantly reduced (P < 0.05) the percent of original inocula of APEC adhered and invaded in HT-29 cells (Fig. 4). However, no effect on the adhesion and invasion was observed when HT-29 cells were pre-treated with L. rhamnosus GG and B. lactis Bb12 cells itself after CFSs were separated and cells resuspended in DMEM (data not shown).
Percent of original inocula of APEC O78 adhered and invaded in HT-29 cells when pretreated with cell-free supernatants (CFSs) of L. rhamnosus GG and B. lactis Bb12. LGG, Lacticaseibacillus rhamnosus GG; Bb12, Bifidobacterium lactis Bb12; DMEM, Dulbecco’s modified Eagle medium; **P < 0.01, ***P < 0.001, two-way ANOVA Bonferroni post-test
L. rhamnosus GG Reduced the Colonization of APEC in Cecum of Chickens
The efficacy of L. rhamnosus GG and B. lactis Bb12 and their combination (1:1) was tested in chickens by administering orally (108 CFU/chicken) for 14 days. The L. rhamnosus GG treatment significantly reduced (P < 0.001; 1.6 logs) the APEC load in cecum 7 days post-infection as compared to APEC infected but not probiotic treated (PC; positive control) chickens (Fig. 5A). On the other hand, only 0.6 log APEC reduction was observed in B. lactis Bb12-treated chickens. No L. rhamnosus GG-treated chickens were positive for APEC in internal organs (liver and heart), whereas 10% and 20% of chickens were APEC positive in B. lactis Bb12-treated and untreated groups, respectively (data not shown). Surprisingly, the combination treatment with L. rhamnosus GG and B. lactis Bb12 only resulted in 0.4 log reduction in APEC load.
A APEC load in cecum of chickens treated with L. rhamnosus GG, B. lactis Bb12 or L. rhamnosus GG and B. lactis Bb12 combination compared to PC (APEC infected but not probiotic treated; positive control) group. B Body weight gain of chickens treated with L. rhamnosus GG, B. lactis Bb12 or L. rhamnosus GG and B. lactis Bb12 combination compared to PC and NC (non- APEC infected and non-probiotic treated; negative control) groups. LGG, Lacticaseibacillus rhamnosus GG; Bb12, Bifidobacterium lactis Bb12; *P < 0.05, **P < 0.01, Man-Whitney U test
L. rhamnosus GG treatment also significantly (P < 0.05; 12 g in 2 weeks) increased the body weight gain of chickens as compared to not APEC-infected and not probiotic-treated (NC; negative control) chickens (Fig. 5B), whereas no significant increase in body weight was observed in chickens treated with B. lactis Bb12 (6.6 g) or L. rhamnosus GG and B. lactis Bb12 combination (2.6 g).
We performed L. rhamnosus GG-specific qPCR to quantitate L. rhamnosus GG in the cecum of L. rhamnosus GG-treated chickens [42]. The standard L. rhamnosus GG qPCR curve was generated (Fig. S3A) and used to quantitate L. rhamnosus GG in cecum. At day 15, ~ 6.3 logs of L. rhamnosus GG (on average) were enumerated in cecum (Fig. S3B). No amplification of L. rhamnosus GG was observed in cecal contents of NC chickens. These results suggest that L. rhamnosus GG can resist the low gastric pH and high intestinal bile salt concentrations of the chicken’s gut.
L. rhamnosus GG Reduced the Enterobacteriaceae (Escherichia-Shigella) Abundance in Cecum of Chickens
The analysis of alpha diversity (or Shannon index) revealed no significant difference in the microbial richness between the treatment groups (Fig. 6A). However, the microbial community of APEC infected but not treated (PC) chickens was dissimilar to L. rhamnosus GG treated and non-infected and non-treated (NC) chickens when beta diversity was analyzed using Bray–Curtis dissimilarity index (Fig. 6B). The microbial communities of L. rhamnosus GG-treated and NC chickens were similar, suggesting that L. rhamnosus GG moderated the APEC-induced alterations of microbial community in the cecum of chickens.
Alpha diversity (Shannon index) (A) and beta diversity (Bray–Curtis dissimilarity index) (B) of cecal microbial community of chickens treated with L. rhamnosus GG compared to PC (APEC infected but not probiotic treated; positive control) and NC (non-APEC infected and non-probiotic treated; negative control) groups. Relative abundance of cecal microbiota at the phylum (C) and family (D) level in chickens treated with L. rhamnosus GG compared to PC and NC groups. LGG, Lacticaseibacillus rhamnosus GG; *P < 0.05, Man-Whitney U test
The L. rhamnosus GG treatment significantly (P < 0.05) increased (80.22 to 92.98%) the Firmicutes abundance, whereas decreased (19.72 to 6.11%) the Proteobacteria abundance as compared to PC chickens (Fig. 6C). Specifically, in Firmicutes, the abundance of bacteria belonging to Erysipelotrichia (3.64 to 14.23%) class or Erysipelotrichales (3.64 to 12.99%) order was increased. On the other hand, in Proteobacteria, the abundance of bacteria belonging to Gammaproteobacteria (19.72 to 6.72%) class or Enterobacteriales (19.57 to 6.11%) order was decreased. At the family level, the abundance of Enterobacteriaceae (19.57 to 6.11%) and Enterococcaceae (1.03 to 0.09%) was significantly decreased (P < 0.05), whereas the abundance of Erysipelotrichaceae was significantly (P < 0.05) increased (3.64 to 12.99%) (Fig. 6D). At the genus level, the abundance of Escherichia-Shigella (16.45 to 4.20%), Enterococcus (1.03 to 0.09%), Flavonifractor (6.73 to 2.24%), and Lachnospiraceae (uncultured) (4.51 to 0%) was significantly decreased (P < 0.05), whereas abundance of Erysipelatoclostridium (3.60 to 12.93%), Negativibacillus (0 to 1.54%), DTU089 (0 to 1.02%), Butyricicoccus (1.08 to 2.45%), Blautia (0 to 2.10%), and Lactobacillus (0.03 to 0.56%) was increased (Table 6).
Compared to NC chickens, the abundance of Bacillales (0 to 3.61%) order was significantly increased in L. rhamnosus GG-treated chickens. At the family level, the abundance of Bacillaceae (0 to 3.61%), Clostridiaceae 1 (0 to 0.64%), and Ruminococcaceae (18.73 to 32.35%) was increased, whereas abundance of Lachnospiraceae (62.85 to 42.58%) was significantly decreased (Fig. 6D). At the genus level, the abundance of Bacillus (0 to 3.61%), DTU089 (0 to 1.02%), and Negativibacillus (0 to 1.54%) was significantly (P < 0.05) increased.
The abundance of bacteria belonging to Clostridia (82.51 to 70.77%) class or Clostridiales (82.51 to 70.77%) order was significantly (P < 0.05) decreased in PC chickens as compared to NC chickens. At the family level, the abundance of Lachnospiraceae (62.85 to 46.38%) was decreased (Fig. 6D). At the genus level, the abundance of Candidatus Soleaferrea (1.31 to 0.34%) and Caproiciproducens (0.77 to 0.05%) was significantly decreased, whereas abundance of Flavonifractor (2.68 to 6.73%) and Lachnospiraceae (uncultured) (0 to 4.51%) was significantly increased (Table 6).
Peptides Identified in the Cell-Free Supernatants of L. rhamnosus GG and B. lactis Bb12 Are Inhibitory to APEC
Out of 33 peptides identified by LC–MS/MS both at HCD and CID settings, five highly abundant common peptides present in both L. rhamnosus GG and B. lactis Bb12 were tested for anti-APEC activity. Three peptides (VQAAQAGDTKPIEV, AFDNTDTSLDSTFKSA, and VTDTSGKAGTTKISNV) were completely inhibitory to APEC (Fig. 7) at 12 mM concentration. The mass spectrometry (MS) peaks for these peptides are shown in Figs. S4 and S5. Peptide AESSDTNLVNAKAA was slightly inhibitory to APEC, whereas FSAVALSAVALSKPGHVNA did not affect the APEC growth.
Discussion
The efficacy of L. rhamnosus GG has been demonstrated to reduce infections caused by different bacterial pathogens in different animal hosts [40, 47,48,49,50,51,52,53,54,55]. L. rhamnosus GG administration reduced the S. infantis colonization in jejunum and its translocation to internal organs of piglets [47, 53], S. Typhimurium colonization in jejunum of piglets [48], and S. Typhimurium-induced deaths in mouse model [49]. Similarly, L. rhamnosus GG reduced the jejunal and ileal lesions caused by S. enterica serovar 4,[5],12:i: in piglets [50]. Further, the culture supernatant of L. rhamnosus GG increased the resistance to systemic E. coli K1 infection in neonatal rats by reducing intestinal bacterial colonization, translocation, and dissemination to extra-intestinal sites [40, 55]. The mortality of mice was reduced when L. rhamnosus GG was administered in experimental model of septic peritonitis by preventing systemic bacteremia [51, 54]. L. rhamnosus GG supplementation also reduced the mortality in fish (red tilapia) challenged with Aeromonas veronii [52]. Our results demonstrate that L. rhamnosus GG is also a promising preventative against APEC infection in chickens.
Previously, several antimicrobial peptides have been isolated and characterized from L. rhamnosus GG and other Lactobacillus sps. A 37.3 kDa postbiotic, HM0539, was identified in L. rhamnosus GG (ATCC 53,103) supernatant through LC–MS/MS analysis [56]. HM0539 showed beneficial effects against E. coli K1 infection in neonatal rats by promoting maturation of intestinal defense; however, effect on growth of E. coli K1 was not evaluated. Similar to our finding, multiple small peptides (NPSRQERR, PDENK, VHTAPK, MLNERVK, YTRGLPM, GKLSNK, and LSQKSVK) of < 1 kDa mol. wt. were identified in L. rhamnosus GG conditional media; they also showed growth inhibitory activity against Enteroaggregative E. coli (EAEC) O42 [57] and APEC serotypes [58]. Two major secreted proteins, p75 (major secreted protein 1; Msp1) and p40 (major secreted protein 2; Msp2), resembling cell wall hydrolases were identified in L. rhamnosus GG supernatant with reported functions in promoting the survival and growth of intestinal epithelial cells [59]. In another study, a 1.3 kDa peptide was isolated from supernatant of L. gasseri SF1109 with anti-bacterial, anti-biofilm, and immunomodulatory activities against Pseudomonas aeruginosa and E. coli [60]. A 1.1 kDa peptide (NVGVLXPPXLV; acidocin LCHV) was purified from supernatant of L. acidophilus n.v. Er 317/402 strain Narine that has broad spectrum of activity against Gram-positive and Gram-negative pathogens [61]. Peptides (SGADTTFLTK, LVGKKVQTE, and GTLIGQDYK) isolated from supernatant of L. plantarum CECT 749 have also displayed antifungal activity against Aspergillus parasiticus and Penicillium expansum [62]. These findings suggest that small peptides have potential to be developed as new therapeutics against APEC infections. From this study, we identified three novel peptides (VQAAQAGDTKPIEV, AFDNTDTSLDSTFKSA, and VTDTSGKAGTTKISNV) in the cell-free supernatant of L. rhamnosus GG that have anti-APEC activity (Fig. 7, Table 5). Further characterization of these three bioactive peptides is necessary to develop them as potential new anti-APEC therapeutics. In the current study, we only tested five highly abundant peptides for their bioactivity. Testing of additional peptides identified from this study can identify additional new anti-APEC therapeutic candidates.
The abundance of bacteria belonging to phylum Proteobacteria, particularly Enterobacteriaceae family (Escherichia-Shigella), was decreased in gut microbiota of chickens treated with L. rhamnosus GG (Fig. 6, Table 6). The increase in phylum Proteobacteria which includes many opportunistic bacteria is associated with low productivity and pro-inflammatory cytokine profile in chickens [63]. The Proteobacteria abundance was also decreased when L. rhamnosus GG was supplemented in mice having dysbiosis of colon microbiota induced by experimental sepsis [64]. Similar to our finding, the abundance of Akkermansia, a genus belonging to phylum Firmicutes, was increased in those mice treated with L. rhamnosus GG [64]. The L. rhamnosus GG treatment in those mice reduced the sepsis-induced mortality by modulating the microbiota dysbiosis, likely by decreasing the Enterobacteriaceae and Enterococcaceae abundance, similar to what we observed in our study [64]. Firmicutes abundance was also increased in pre-weaning piglets treated with L. rhamnosus GG [65]. L. rhamnosus GG treatment in those piglets was proven beneficial for intestinal health as it enhanced the biological, physical, and immunological barriers of intestinal mucosa [65]. On contrary to Proteobacteria, the increase in phylum Firmicutes is associated with high productivity and anti-inflammatory cytokine profile in chickens [63]. The abundance of bacteria belonging to genus Escherichia was also decreased in gut microbiota of children who consumed L. rhamnosus GG indicating the ability of L. rhamnosus GG to prevent bacterial infections [66]. The increased abundance of bacteria belonging to Erysipelotrichaceae family was observed in L. rhamnosus GG treated chickens in our study, which is reported to be associated with improved growth and feed conversion in chickens [67]. These results indicate that L. rhamnosus GG can modulate the gut microbiota composition in different hosts to resist bacterial infections. Interestingly, Flavonifractor abundance was also increased in S. Typhimurium-infected chickens [68], similar to what we observed in APEC-infected chickens in our study. This suggests that Flavonifractor could be a potential gut microbial marker to monitor enteric infections in chickens; however, further investigations are needed to establish this cause-and-effect relationship.
The adhesion and invasion of APEC to HT-29 cells was reduced when pre-treated with sub-inhibitory concentration of L. rhamnosus GG supernatant (Fig. 4). It is possible that pre-treatment of L. rhamnosus GG supernatant enhanced the integrity of HT-29 colorectal epithelial cells [40], thus improving the epithelial barrier function and decreasing the adhesion and invasion of APEC. Similar to what we observed in our study, pre-treatment of L. rhamnosus GG supernatant reduced the adhesion, invasion, and translocation of E. coli K1 to human colorectal epithelial (Caco-2) monolayer cells [40]. The pre-treatment of L. rhamnosus GG supernatant also inhibited the adherence of S. aureus to primary human keratinocytes [69] and adhesion and invasion to human osteoblast (HOB) cells [70]. However, in contrast to our finding, pre-treatment of L. rhamnosus GG cells itself decreased the intracellular invasion of S. infantis in porcine jejunal epithelial (IPEC-J2) cells [53] and adhesion, invasion, and transcytosis of E. coli K1 in Caco-2 cells [55]. Interestingly, the simultaneous addition (no-pre-treatment) of L. rhamnosus GG also reduced the adhesion, invasion, and translocation of C. jejuni to chicken (B10X1) and pig (CLAB) small intestinal epithelial cell lines [71]. These findings indicate that L. rhamnosus GG itself or its cell-free supernatant can exhibit anti-bacterial effects to competitively exclude different pathogens at infection sites, thereby preventing the diseases.
As reported in other studies [32, 33], L. rhamnosus GG effect against APEC can be multi-factorial that includes production of lactic acid, secretion/release of small peptides, and others. The shortened cells with bulbous swelling were observed in SEM after APEC was treated with L. rhamnosus GG supernatant (Fig. 2). Similar morphology was observed when E. coli was treated antimicrobial peptides, gramicidin S, and α-helical peptidyl-glycylleucine-carboxyamide (PGLa) [72], indicating the likely damage of the bacterial cell envelope upon treatment with L. rhamnosus GG CFS.
In summary, our study evaluated different probiotic and commensal bacteria and identified L. rhamnosus GG as a potential preventative measure against APEC infection in chickens. We identified multiple small novel bioactive peptides that can be developed as non-antibiotic therapeutics against APEC in the future. We also uncovered L. rhamnosus GG interactions with APEC and commensal microbes in the gut microbiota of chickens which can facilitate the understanding of mechanism behind L. rhamnosus GG anti-bacterial effects. Our future studies will optimize the delivery of L. rhamnosus GG in feed or water, test the efficacy of L. rhamnosus GG under conditions mimicking the field, and evaluate the identified peptides in chickens.
Availability of Data and Material
All data generated or analyzed during this study are included in this published article (and its supplementary information files).
References
Lutful Kabir SM (2010) Avian colibacillosis and salmonellosis: a closer look at epidemiology, pathogenesis, diagnosis, control and public health concerns. Int J Environ Res Public Health 7(1):89–114. https://doi.org/10.3390/ijerph7010089
Kathayat D, Lokesh D, Ranjit S, Rajashekara G (2021) Avian pathogenic Escherichia coli (APEC): an overview of virulence and pathogenesis factors, zoonotic potential, and control strategies. Pathogens 10(4):467. https://doi.org/10.3390/pathogens10040467
Johnson TJ, Wannemuehler Y, Doetkott C, Johnson SJ, Rosenberger SC, Nolan LK (2008) Identification of minimal predictors of avian pathogenic Escherichia coli virulence for use as a rapid diagnostic tool. J Clin Microbiol 46(12):3987–3996. https://doi.org/10.1128/jcm.00816-08
Mellata M (2013) Human and avian extraintestinal pathogenic Escherichia coli: infections, zoonotic risks, and antibiotic resistance trends. Foodborne Pathog Dis 10(11):916–932. https://doi.org/10.1089/fpd.2013.1533
Liu CM, Stegger M, Aziz M, Johnson TJ, Waits K, Nordstrom L, Gauld L, Weaver B, Rolland D, Statham S, Horwinski J, Sariya S, Davis GS, Sokurenko E, Keim P, Johnson JR, Price LB (2018) Escherichia coli ST131-H22 as a foodborne uropathogen. MBio 9(4):e00470-e518. https://doi.org/10.1128/mBio.00470-18
Osman KM, Kappell AD, Elhadidy M, ElMougy F, El-Ghany WAA, Orabi A, Mubarak AS, Dawoud TM, Hemeg HA, Moussa IMI, Hessain AM, Yousef HMY (2018) Poultry hatcheries as potential reservoirs for antimicrobial-resistant Escherichia coli: a risk to public health and food safety. Sci Rep 8(1):5859. https://doi.org/10.1038/s41598-018-23962-7
Kathayat D, Helmy YA, Deblais L, Rajashekara G (2018) Novel small molecules affecting cell membrane as potential therapeutics for avian pathogenic Escherichia coli. Sci Rep 8(1):15329. https://doi.org/10.1038/s41598-018-33587-5
Dho-Moulin M, Fairbrother JM (1999) Avian pathogenic Escherichia coli (APEC). Vet Res 30(2–3):299–316
Nhung NT, Chansiripornchai N, Carrique-Mas JJ (2017) Antimicrobial resistance in bacterial poultry pathogens: a review. Fron Vet Sci 4:126. https://doi.org/10.3389/fvets.2017.00126
Gyles CL (2008) Antimicrobial resistance in selected bacteria from poultry. Anim Health Res Rev 9(2):149–158. https://doi.org/10.1017/S1466252308001552
Van Boeckel TP, Brower C, Gilbert M, Grenfell BT, Levin SA, Robinson TP, Teillant A, Laxminarayan R (2015) Global trends in antimicrobial use in food animals. Proc Natl Acad Sci USA 112(18):5649–5654. https://doi.org/10.1073/pnas.1503141112
Hao H, Cheng G, Iqbal Z, Ai X, Hussain HI, Huang L, Dai M, Wang Y, Liu Z, Yuan Z (2014) Benefits and risks of antimicrobial use in food-producing animals. Front Microbiol 5:288. https://doi.org/10.3389/fmicb.2014.00288
Fijan S (2014) Microorganisms with claimed probiotic properties: an overview of recent literature. Int J Environ Res Public Health 11(5):4745–4767. https://doi.org/10.3390/ijerph110504745
Bermudez-Brito M, Plaza-Díaz J, Muñoz-Quezada S, Gómez-Llorente C, Gil A (2012) Probiotic mechanisms of action. Ann Nutr Metab 61(2):160–174. https://doi.org/10.1159/000342079
Sánchez B, Delgado S, Blanco-Míguez A, Lourenço A, Gueimonde M, Margolles A (2017) Probiotics, gut microbiota, and their influence on host health and disease. Mol Nutr Food Res 61(1). https://doi.org/10.1002/mnfr.201600240
Servin AL (2004) Antagonistic activities of lactobacilli and bifidobacteria against microbial pathogens. FEMS Microbiol Rev 28(4):405–440. https://doi.org/10.1016/j.femsre.2004.01.003
Ciorba MA (2012) A gastroenterologist’s guide to probiotics. Clin Gastroentero Hepatol 10(9):960–968. https://doi.org/10.1016/j.cgh.2012.03.024
Lievin-Le Moal V, Servin AL (2014) Anti-infective activities of Lactobacillus strains in the human intestinal microbiota: from probiotics to gastrointestinal anti-infectious biotherapeutic agents. Clin Microbiol Rev 27(2):167–199. https://doi.org/10.1128/cmr.00080-13
Vlasova AN, Kandasamy S, Chattha KS, Rajashekara G, Saif LJ (2016) Comparison of probiotic lactobacilli and bifidobacteria effects, immune responses and rotavirus vaccines and infection in different host species. Vet Immunol Immunopathol 172:72–84. https://doi.org/10.1016/j.vetimm.2016.01.003
Carter A, Adams M, La Ragione RM, Woodward MJ (2017) Colonisation of poultry by Salmonella Enteritidis S1400 is reduced by combined administration of Lactobacillus salivarius 59 and Enterococcus faecium PXN-33. Vet Microbiol 199:100–107. https://doi.org/10.1016/j.vetmic.2016.12.029
Van Coillie E, Goris J, Cleenwerck I, Grijspeerdt K, Botteldoorn N, Van Immerseel F, De Buck J, Vancanneyt M, Swings J, Herman L, Heyndrickx M (2007) Identification of lactobacilli isolated from the cloaca and vagina of laying hens and characterization for potential use as probiotics to control Salmonella Enteritidis. J Appl Microbiol 102(4):1095–1106. https://doi.org/10.1111/j.1365-2672.2006.03164.x
Saint-Cyr MJ, Haddad N, Taminiau B, Poezevara T, Quesne S, Amelot M, Daube G, Chemaly M, Dousset X, Guyard-Nicodeme M (2017) Use of the potential probiotic strain Lactobacillus salivarius SMXD51 to control Campylobacter jejuni in broilers. Int J Food Microbiol 247:9–17. https://doi.org/10.1016/j.ijfoodmicro.2016.07.003
Wang S, Peng Q, Jia HM, Zeng XF, Zhu JL, Hou CL, Liu XT, Yang FJ, Qiao SY (2017) Prevention of Escherichia coli infection in broiler chickens with Lactobacillus plantarum B1. Poult Sci 96(8):2576–2586. https://doi.org/10.3382/ps/pex061
Foltz KL, Ritzi MM, Barrett NW, Evans NP, Collins D, Sriranganathan N, Mahsoub H, Dalloul RA, Sewell J, Persia ME (2017) Efficacy of Lactobacillus plantarum supplementation in broilers challenged with avian pathogenic Escherichia coli and Salmonella Typhimurium. J Appl Poult Res 26(3):316–324. https://doi.org/10.3382/japr/pfw074
Ding S, Wang Y, Yan W, Li A, Jiang H, Fang J (2019) Effects of Lactobacillus plantarum 15–1 and fructooligosaccharides on the response of broilers to pathogenic Escherichia coli O78 challenge. PLoS One 14(6):e0212079. https://doi.org/10.1371/journal.pone.0212079
Forkus B, Ritter S, Vlysidis M, Geldart K, Kaznessis YN (2017) Antimicrobial probiotics reduce Salmonella enterica in turkey gastrointestinal tracts. Sci Rep 7:40695. https://doi.org/10.1038/srep40695
Mañes-Lázaro R, Van Diemen PM, Pin C, Mayer MJ, Stevens MP, Narbad A (2017) Administration of Lactobacillus johnsonii FI9785 to chickens affects colonisation by Campylobacter jejuni and the intestinal microbiota. Br Poult Sci 58(4):373–381. https://doi.org/10.1080/00071668.2017.1307322
Nakphaichit M, Sobanbua S, Siemuang S, Vongsangnak W, Nakayama J, Nitisinprasert S (2019) Protective effect of Lactobacillus reuteri KUB-AC5 against Salmonella Enteritidis challenge in chickens. Benef Microbes 10(1):43–54. https://doi.org/10.3920/bm2018.0034
Tabashsum Z, Peng M, Alvarado-Martinez Z, Aditya A, Bhatti J, Romo PB, Young A, Biswas D (2020) Competitive reduction of poultry-borne enteric bacterial pathogens in chicken gut with bioactive Lactobacillus casei. Sci Rep 10(1):16259. https://doi.org/10.1038/s41598-020-73316-5
Mangiamele P, Nicholson B, Wannemuehler Y, Seemann T, Logue CM, Li G, Tivendale KA, Nolan LK (2013) Complete genome sequence of the avian pathogenic Escherichia coli strain APEC O78. Genome Announc 1(2):e0002613. https://doi.org/10.1128/genomeA.00026-13
Fijan S (2016) Antimicrobial effect of probiotics against common pathogens. In: Rao V, Rao LG (eds) Probiotics and prebiotics in human nutrition and health. InTech, Rijeka, p Ch. 10. https://doi.org/10.5772/63141
De Keersmaecker SC, Verhoeven TL, Desair J, Marchal K, Vanderleyden J, Nagy I (2006) Strong antimicrobial activity of Lactobacillus rhamnosus GG against Salmonella Typhimurium is due to accumulation of lactic acid. FEMS Microbiol Lett 259(1):89–96. https://doi.org/10.1111/j.1574-6968.2006.00250.x
Fayol-Messaoudi D, Berger CN, Coconnier-Polter M-H, Liévin-Le Moal V, Servin AL (2005) pH-, lactic acid-, and non-lactic acid-dependent activities of probiotic lactobacilli against Salmonella enterica serovar Typhimurium. Appl Environ Microbiol 71(10):6008–6013. https://doi.org/10.1128/AEM.71.10.6008-6013
Xu Y, Zhao Z, Tong W, Ding Y, Liu B, Shi Y, Wang J, Sun S, Liu M, Wang Y, Qi Q, Xian M, Zhao G (2020) An acid-tolerance response system protecting exponentially growing Escherichia coli. Nat Commun 11(1):1496. https://doi.org/10.1038/s41467-020-15350-5
Shokryazdan P, Sieo CC, Kalavathy R, Liang JB, Alitheen NB, Faseleh Jahromi M, Ho YW (2014) Probiotic potential of Lactobacillus strains with antimicrobial activity against some human pathogenic strains. BioMed Res Int 2014:927268. https://doi.org/10.1155/2014/927268
Zhang Y, Zhang L, Du M, Yi H, Guo C, Tuo Y, Han X, Li J, Zhang L, Yang L (2011) Antimicrobial activity against Shigella sonnei and probiotic properties of wild lactobacilli from fermented food. Microbiol Res 167(1):27–31. https://doi.org/10.1016/j.micres.2011.02.006
Han J, Lin K, Sequeira C, Borchers CH (2015) An isotope-labeled chemical derivatization method for the quantitation of short-chain fatty acids in human feces by liquid chromatography-tandem mass spectrometry. Anal Chim Acta 854:86–94. https://doi.org/10.1016/j.aca.2014.11.015
Connor RI (2016) Bioactive molecules produced by probiotic bacteria and methods for isolating and using the same. United States trustees of Dartmouth College US20160024149A1
Helmy YA, Kassem II, Kumar A, Rajashekara G (2017) In vitro evaluation of the impact of the probiotic E. coli Nissle (1917) on Campylobacter jejuni’s invasion and intracellular survival in human colonic cells. Front Microbiol 8:1588. https://doi.org/10.3389/fmicb.2017.01588
He X, Zeng Q, Puthiyakunnon S, Zeng Z, Yang W, Qiu J, Du L, Boddu S, Wu T, Cai D, Huang S-H, Cao H (2017) Lactobacillus rhamnosus GG supernatant enhance neonatal resistance to systemic Escherichia coli K1 infection by accelerating development of intestinal defense. Sci Rep 7:43305. https://doi.org/10.1038/srep43305
Zhang L, Zhang L, Xa Z, Zeng X, Zhou L, Cao G, Ag C, Yang C (2016) Effects of dietary supplementation of probiotic, Clostridium butyricum, on growth performance, immune response, intestinal barrier function, and digestive enzyme activity in broiler chickens challenged with Escherichia coli K88. J Anim Sci Biotechnol 7:3. https://doi.org/10.1186/s40104-016-0061-4
Dommels YEM, Kemperman RA, Zebregs YEMP, Draaisma RB, Jol A, Wolvers DAW, Vaughan EE, Albers R (2009) Survival of Lactobacillus reuteri DSM 17938 and Lactobacillus rhamnosus GG in the human gastrointestinal tract with daily consumption of a low-fat probiotic spread. Appl Environ Microbiol 75(19):6198–6204. https://doi.org/10.1128/AEM.01054-09
Deblais L, Helmy YA, Kathayat D, Huang H-c, Miller SA, Rajashekara G (2018) Novel imidazole and methoxybenzylamine growth inhibitors affecting Salmonella cell envelope integrity and its persistence in chickens. Sci Rep 8(1):13381. https://doi.org/10.1038/s41598-018-31249-0
Helmy YA, Kathayat D, Ghanem M, Jung K, Closs G Jr, Deblais L, Srivastava V, El-Gazzar M, Rajashekara G (2020) Identification and characterization of novel small molecule inhibitors to control Mycoplasma gallisepticum infection in chickens. Vet Microbiol 247:108799. https://doi.org/10.1016/j.vetmic.2020.108799
Bolyen E, Rideout JR, Dillon MR, Bokulich NA, Abnet CC, Al-Ghalith GA, Alexander H, Alm EJ, Arumugam M, Asnicar F, Bai Y, Bisanz JE, Bittinger K, Brejnrod A, Brislawn CJ, Brown CT, Callahan BJ, Caraballo-Rodríguez AM, Chase J, Cope EK, Da Silva R, Diener C, Dorrestein PC, Douglas GM, Durall DM, Duvallet C, Edwardson CF, Ernst M, Estaki M, Fouquier J, Gauglitz JM, Gibbons SM, Gibson DL, Gonzalez A, Gorlick K, Guo J, Hillmann B, Holmes S, Holste H, Huttenhower C, Huttley GA, Janssen S, Jarmusch AK, Jiang L, Kaehler BD, Kang KB, Keefe CR, Keim P, Kelley ST, Knights D, Koester I, Kosciolek T, Kreps J, Langille MGI, Lee J, Ley R, Liu Y-X, Loftfield E, Lozupone C, Maher M, Marotz C, Martin BD, McDonald D, McIver LJ, Melnik AV, Metcalf JL, Morgan SC, Morton JT, Naimey AT, Navas-Molina JA, Nothias LF, Orchanian SB, Pearson T, Peoples SL, Petras D, Preuss ML, Pruesse E, Rasmussen LB, Rivers A, Robeson MS, Rosenthal P, Segata N, Shaffer M, Shiffer A, Sinha R, Song SJ, Spear JR, Swafford AD, Thompson LR, Torres PJ, Trinh P, Tripathi A, Turnbaugh PJ, Ul-Hasan S, van der Hooft JJJ, Vargas F, Vázquez-Baeza Y, Vogtmann E, von Hippel M, Walters W, Wan Y, Wang M, Warren J, Weber KC, Williamson CHD, Willis AD, Xu ZZ, Zaneveld JR, Zhang Y, Zhu Q, Knight R, Caporaso JG (2019) Reproducible, interactive, scalable and extensible microbiome data science using QIIME 2. Nat Biotechnol 37(8):852–857. https://doi.org/10.1038/s41587-019-0209-9
Callahan BJ, McMurdie PJ, Rosen MJ, Han AW, Johnson AJ, Holmes SP (2016) DADA2: high-resolution sample inference from Illumina amplicon data. Nat Methods 13(7):581–583. https://doi.org/10.1038/nmeth.3869
Yang G-Y, Yu J, Su J-H, Jiao L-G, Liu X, Zhu Y-H (2017) Oral administration of Lactobacillus rhamnosus GG ameliorates Salmonella infantis-induced inflammation in a pig model via activation of the IL-22BP/IL-22/STAT3 pathway. Front Cell Infect Microbiol 7:323. https://doi.org/10.3389/fcimb.2017.00323
Splichalova A, Jenistova V, Splichalova Z, Splichal I (2019) Colonization of preterm gnotobiotic piglets with probiotic Lactobacillus rhamnosus GG and its interference with Salmonella Typhimurium. Clin Exp Immunol 195(3):381–394. https://doi.org/10.1111/cei.13236
Liu J, Hu D, Chen Y, Huang H, Zhang H, Zhao J, Gu Z, Chen W (2018) Strain-specific properties of Lactobacillus plantarum for prevention of Salmonella infection. Food Funct 9(7):3673–3682. https://doi.org/10.1039/c8fo00365c
Yu J, Zhu Y-H, Yang G-Y, Zhang W, Zhou D, Su J-H, Wang J-F (2017) Anti-inflammatory capacity of Lactobacillus rhamnosus GG in monophasic variant Salmonella infected piglets is correlated with impeding NLRP6-mediated host inflammatory responses. Vet Microbiol 210:91–100. https://doi.org/10.1016/j.vetmic.2017.08.008
Khailova L, Frank DN, Dominguez JA, Wischmeyer PE (2013) Probiotic administration reduces mortality and improves intestinal epithelial homeostasis in experimental sepsis. Anesthesiology 119(1):166–177. https://doi.org/10.1097/ALN.0b013e318291c2fc
Sewaka M, Trullas C, Chotiko A, Rodkhum C, Chansue N, Boonanuntanasarn S, Pirarat N (2019) Efficacy of synbiotic Jerusalem artichoke and Lactobacillus rhamnosus GG-supplemented diets on growth performance, serum biochemical parameters, intestinal morphology, immune parameters and protection against Aeromonas veronii in juvenile red tilapia (Oreochromis spp.). Fish Shellfish Immunol 86:260–268. https://doi.org/10.1016/j.fsi.2018.11.026
Zhang W, Zhu Y-H, Yang G-Y, Liu X, Xia B, Hu X, Su J-H, Wang J-F (2018) Lactobacillus rhamnosus GG affects microbiota and suppresses autophagy in the intestines of pigs ahallenged with Salmonella infantis. Front Microbiol 8:2705. https://doi.org/10.3389/fmicb.2017.02705
Chen L, Li H, Li J, Chen Y, Yang Y (2019) Lactobacillus rhamnosus GG treatment improves intestinal permeability and modulates microbiota dysbiosis in an experimental model of sepsis. Int J Mol Med 43(3):1139–1148. https://doi.org/10.3892/ijmm.2019.4050
Huang S-H, He L, Zhou Y, Wu C-H, Jong A (2009) Lactobacillus rhamnosus GG suppresses meningitic E. coli K1 penetration across human intestinal epithelial cells in vitro and protects neonatal rats against experimental hematogenous meningitis. Int J Microbiol 647862. https://doi.org/10.1155/2009/647862
Gao J, Li Y, Wan Y, Hu T, Liu L, Yang S, Gong Z, Zeng Q, Wei Y, Yang W, Zeng Z, He X, Huang S-H, Cao H (2019) A novel postbiotic from Lactobacillus rhamnosus GG with a beneficial effect on intestinal barrier function. Front Microbiol 10:477. https://doi.org/10.3389/fmicb.2019.00477
Lu R, Fasano S, Madayiputhiya N, Morin NP, Nataro J, Fasano A (2009) Isolation, identification, and characterization of small bioactive peptides from Lactobacillus GG conditional media that exert both anti-Gram-negative and Gram-positive bactericidal activity. J Pediatr Gastroenterol Nutr 49(1):23–30. https://doi.org/10.1097/MPG.0b013e3181924d1e
Kathayat D, Closs G Jr, Helmy YA, Lokesh D, Ranjit S, Rajashekara G (2021) Peptides affecting outer membrane lipid asymmetry (MlaA-OmpC/F) system reduce avian pathogenic Escherichia coli (APEC) colonization in chickens. Appl Environ Microbiol 87(17):e0056721. https://doi.org/10.1128/aem.00567-21
Claes IJ, Schoofs G, Regulski K, Courtin P, Chapot-Chartier MP, Rolain T, Hols P, von Ossowski I, Reunanen J, de Vos WM, Palva A, Vanderleyden J, De Keersmaecker SC, Lebeer S (2012) Genetic and biochemical characterization of the cell wall hydrolase activity of the major secreted protein of Lactobacillus rhamnosus GG. PLoS One 7(2):e31588. https://doi.org/10.1371/journal.pone.0031588
Zanfardino A, Criscuolo G, Di Luccia B, Pizzo E, Ciavatta ML, Notomista E, Carpentieri A, Pezzella A, Varcamonti M (2017) Identification of a new small bioactive peptide from Lactobacillus gasseri supernatant. Benef Microbes 8(1):133–141. https://doi.org/10.3920/bm2016.0098
Mkrtchyan H, Gibbons S, Heidelberger S, Zloh M, Limaki HK (2010) Purification, characterisation and identification of acidocin LCHV, an antimicrobial peptide produced by Lactobacillus acidophilus n.v. Er 317/402 strain Narine. Int J Antimicrob Agents 35(3):255–260. https://doi.org/10.1016/j.ijantimicag.2009.11.017
Luz C, Saladino F, Luciano FB, Mañes J, Meca G (2017) In vitro antifungal activity of bioactive peptides produced by Lactobacillus plantarum against Aspergillus parasiticus and Penicillium expansum. LWT 81:128–135. https://doi.org/10.1016/j.lwt.2017.03.053
Diaz Carrasco JM, Casanova NA, Fernández Miyakawa ME (2019) Microbiota, gut health and chicken productivity: what is the connection? Microorganisms 7(10):374. https://doi.org/10.3390/microorganisms7100374
Chen L, Li H, Chen Y, Yang Y (2020) Probiotic Lactobacillus rhamnosus GG reduces mortality of septic mice by modulating gut microbiota composition and metabolic profiles. Nutr 78:110863. https://doi.org/10.1016/j.nut.2020.110863
Wang Y, Gong L, Wu Y-P, Cui Z-W, Wang Y-Q, Huang Y, Zhang X-P, Li W-F (2019) Oral administration of Lactobacillus rhamnosus GG to newborn piglets augments gut barrier function in pre-weaning piglets. J Zhejiang Univ Sci B 20(2):180–192. https://doi.org/10.1631/jzus.B1800022
Korpela K, Salonen A, Virta LJ, Kumpu M, Kekkonen RA, de Vos WM (2016) Lactobacillus rhamnosus GG intake modifies preschool children’s intestinal microbiota, alleviates penicillin-associated changes, and reduces antibiotic use. PLoS One 11(4):e0154012. https://doi.org/10.1371/journal.pone.0154012
Stanley D, Hughes RJ, Geier MS, Moore RJ (2016) Bacteria within the gastrointestinal tract microbiota correlated with improved growth and feed conversion: challenges presented for the identification of performance enhancing probiotic bacteria. Front Microbiol 7:187. https://doi.org/10.3389/fmicb.2016.00187
Khan S, Chousalkar KK (2020) Salmonella Typhimurium infection disrupts but continuous feeding of Bacillus based probiotic restores gut microbiota in infected hens. J Anim Sci Biotechnol 11:29. https://doi.org/10.1186/s40104-020-0433-7
Mohammedsaeed W, McBain AJ, Cruickshank SM, O’Neill CA (2014) Lactobacillus rhamnosus GG inhibits the toxic effects of Staphylococcus aureus on epidermal keratinocytes. Appl Environ Microbiol 80(18):5773–5781. https://doi.org/10.1128/AEM.00861-14
Kalaycı Yüksek F, Gümüş D, Gündoğan Gİ, Anğ Küçüker M (2020) Cell-free Lactobacillus sp supernatants modulate Staphylococcus aureus growth, adhesion and invasion to human osteoblast (HOB) cells. Curr Microbiol 78(1):125–132. https://doi.org/10.1007/s00284-020-02247-1
Šikić Pogačar M, Langerholc T, Mičetić-Turk D, Možina SS, Klančnik A (2020) Effect of Lactobacillus spp. on adhesion, invasion, and translocation of Campylobacter jejuni in chicken and pig small-intestinal epithelial cell lines. BMC Vet Res 16(1):34. https://doi.org/10.1186/s12917-020-2238-5
Hartmann M, Berditsch M, Hawecker J, Ardakani MF, Gerthsen D, Ulrich AS (2010) Damage of the bacterial cell envelope by antimicrobial peptides gramicidin S and PGLa as revealed by transmission and scanning electron microscopy. Antimicrob Agents Chemother 54(8):3132–3142. https://doi.org/10.1128/AAC.00124-10
Acknowledgements
We thank Sochina Ranjit and Dhwani Parsana for technical assistance. We thank Wilbur Ouma for bioinformatics assistance. We thank MCIC and MS&P facilities, The Ohio State University, for analysis of samples for microbiome and LC-MS/MS studies. We thank Dr. Hanson, Megan Strother, Sara Tallmadge, and Ronna Wood for animal care and assistance with animal studies.
Funding
The research in Dr. Rajashekara laboratory was supported by the US Department of Agriculture National Institute for Food and Agriculture (USDA-NIFA) (Grant # 2015–68004-23131, 2020–6701-31401), The Ohio State University internal grants, and North Central Region Sustainable Research and Education (NCR-SARE) (Grant # GNC18-259).
Author information
Authors and Affiliations
Contributions
Conceptualization: GR, DK, and GC. Methodology: GR, DK, GC, YH, LD, and VS. Formal analysis and investigation: GR, DK, GC, YH, LD, and VS. Writing-original draft preparation: DK. Writing-review and editing: GR and DK. Funding acquisition: GR. Resources: GR. Supervision: GR.
Corresponding author
Ethics declarations
Ethics Approval
Animal study was approved by The Ohio State University Institutional Animal Care and Use Committee (IACUC, protocol # 2010A00000149).
Consent to Participate
Not applicable.
Consent for Publication
All authors read and approved the final manuscript.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kathayat, D., Closs, G., Helmy, Y.A. et al. In Vitro and In Vivo Evaluation of Lacticaseibacillus rhamnosus GG and Bifidobacterium lactis Bb12 Against Avian Pathogenic Escherichia coli and Identification of Novel Probiotic-Derived Bioactive Peptides. Probiotics & Antimicro. Prot. 14, 1012–1028 (2022). https://doi.org/10.1007/s12602-021-09840-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12602-021-09840-1