Abstract
The increase of antibiotic resistance has become a problem. Probiotic bacteria play an important role in preventive/supportive medicine. Therefore, we examined the inhibitory effects of four different Lactobacillus species’ (L. acidophilus-La, L. plantarum-Lp, L. fermentum-Lf and L. rhamnosus-Lr) cell-free supernatants (CFSs) on growth, adhesion, invasion, and biofilm formation of Staphylococcus aureus and effects of S. aureus, CFSs, and S. aureus-CFSs co-existence on human osteoblast (HOB) cell viability. Growth alterations were measured spectrophotometrically. Adhesive/invasive bacterial counts were detected by colony counting. Biofilm was evaluated using microtiter plate assay. The MTT assay was used for detection of HOB cell viability. The growth of MSSA significantly (P < 0.01) decreased in the presence of two CFSs (Lf and Lr) (P < 0.01); the growth of MRSA significantly (P < 0.05) reduced in the presence of La CFSs. All tested CFSs were found to reduce adhesion and invasion of MSSA (P < 0.0001). The adhesion of MRSA was enhanced (P < 0.0001) in the presence of all CFSs except La and the invasion of MRSA was decreased (P < 0.01) in the presence of Lr and Lf CFSs. All tested CFSs were shown to inhibit biofilm formation significantly (P < 0.0001). The reduction of S. aureus infected HOB cell viability and exposed to all CFSs except Lr that was found to be significant (P < 0.0001). The viability of HOB cell during co-incubation with MSSA and CFSs was shown to be decreased significantly. However co-existence of MRSA and CFSs did not alter HOB cell viability. These results suggested that lactobacilli as probiotics have low protective effects on MRSA-infected host cells.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Probiotics are defined as living microorganisms which promote the host health. There are some studies showing that probiotics can be used not only for prevention of infections, but also as alternative therapeutics for the treatment of infections especially caused by multi-drug resistant pathogens [1,2,3,4]. Lactobacilli are one of the most effective probiotics, for preventing and control of oral, gastrointestinal, and urogenital infections [5,6,7,8,9,10,11,12]. There are several mechanisms for the beneficial effects of probiotics such as immunomodulation, inhibition of pathogen’s adhesion/invasion/growth due to the ability of probiotic microorganisms’ formation of many compounds with fermentative and/or antimicrobial activities, secretions of proteins which degrade carbohydrate receptors, and production of receptor analogs and bio-surfactants to compete against pathogens for nutrient and adhesion sites [2, 13,14,15,16].
In the present study, we aimed to evaluate the possible inhibitory effects of cell-free supernatants (CFSs) obtained from various lactobacilli on growth, adhesion, and invasion ability of S. aureus in human osteoblast cell (HOB) culture and in vitro biofilm formation. In the meantime, we aimed to detect the effects of CFSs and S. aureus and co-existence of S. aureus + CFSs on HOB cell viability.
Materials and Methods
Bacteria, Media, and Cell-Free Supernatants
In the present study, two different Staphylococcus aureus strains (MSSA ATCC 25923 and MRSA ATTC 43300) and four Lactobacillus species (Lactobacillus rhamnosus ATCC 53103-Lr, Lactobacillus fermentum ATCC 9338-Lf, Lactobacillus acidophilus ATCC 314-La, and Lactobacillus plantarum ATCC 14917-Lp) were used. Lactobacilli were chosen according to their wide usage in dairy products, fruit drinks, chewing gums, and tablets available on market [17, 18].
Lactobacillus strains were grown in de Man-Rogosa-Sharpe (MRS) broth (Conda, Spain) under anaerobic and S. aureus strains were grown in Tryptic Soy Agar (TSA) under aerobic conditions at 37 °C for 24 h. All strains were stored in − 80 °C.
The supernatants (CFSs) from lactobacilli were obtained by filtration (0.2 µm pore size) followed by the centrifugation of the overnight cultures of lactobacilli at 4000 rpm for 30 min at 4 °C [19].
Human Osteoblast (HOB) Cell Culture
Human Osteoblast (HOB) cells (406-05F, Sigma-Aldrich) were cultured in high-glucose Dulbecco's Modified Eagle Medium (DMEM) (Sigma, 5546) containing 50 U/mL penicillin and 50 μg/mL streptomycin (Biological Industries, 03-031-1B), 1% 2 mM l-glutamin (Biological Industries, BI03-020-1B), and 10% fetal bovine serum (FBS) (Biowest, S1810-500). Cells were seeded in 96-well plates (1 × 104 seeding density per each well) for growth and methylthiazolyldiphenyltetrazolium bromide (MTT) assays or in 24-well plates (5 × 104 seeding density per each well) for invasion and adhesion assays and incubated overnight at 37 °C under 5% CO2 to obtain a confluent monolayer (4 × 104 cells in 96-well plates and 2.4 × 105 cells in 24-well plates at confluency) cell culture.
Prior to infection with S. aureus, cells were washed twice with phosphate-buffered saline (PBS), fresh antimicrobial solution-free DMEM, and 20 μL (per each well/96-well plates)/50 μL (per each well/24-well plates) CFS were added. After the well plates were incubated for 1 h [20, 21], the cells were infected with overnight culture of S. aureus in TSB (106 CFU/mL bacteria in each well) for 3 h [22].
The cells were incubated for 3 h for growth [22],1 h for adhesion [22,23,24],3 h for invasion assays [23, 24], and 4 h for viability assay [25] at 37 °C in CO2.
Bacterial Growth
Cells seeded in 96-well plates with/without CFS of each lactobacillus and infected with each S. aureus were incubated at 37 °C with 5% CO2 for three hours. Bacterial growth was measured at 600 nm via spectrophotometric method. The effects of each CFS were determined by comparing absorbance results of growth in infected HOB cell culture with/without CFSs.
All analyses were tested in duplicate and each experiment was performed twice.
Bacterial Adhesion
Cells seeded in 24-well plates with/without CFS of each lactobacillus and infected with each S. aureus were incubated at 37 °C under 5% CO2 for one hour. The wells were washed three times with PBS to remove non-adherent bacteria. To detect adhered bacteria, cell cultures were treated with 500 µl 0.025% Triton X-100 for 5 min at 37 °C in 5% CO2 to detach and lyse the cell monolayer. Bacterial colonies were counted after the cell lysates were inoculated on TSA and incubated at 37 °C for 24 h. The effects of each CFSs were determined by comparing colony counts obtained from cell lysates of cell cultures with and without CFS [23, 24].
All samples were tested in duplicate and each experiment was performed twice.
Bacterial Invasion
Cells seeded in 24-well plates with/without CFS of each lactobacillus and infected with each S. aureus were incubated at 37 °C under 5% CO2 for 3 h. Cells were washed with PBS and fresh medium containing 200 μg/mL gentamycin was added to kill extracellular bacteria. The plates were re-incubated at 37 °C for one hour in 5% CO2. To remove extracellular bacteria, cells were washed three times with PBS and 500 µl 0.025% Triton X-100 was used to lyse the cells. Cell lysates were homogenized and inoculated on TSA and incubated at 37 °C for 24 h to detect invasive bacteria. The effects of each CFS were determined by comparing colony counts obtained from cell lysates of cell cultures with and without CFS [23, 24].
All samples were tested in duplicate and each experiment was performed twice.
Bacterial Biofilm Formation
For the detection of biofilm formations, microtiter plate assay was used.
Bacteria were cultured in TSB-glucose (1%v/v) at 37 °C for 24 h and diluted 1/50 in fresh TSB-glucose, yielding a final concentration of approximately 107 CFU/mL. Each well containing 20 µL from cultivated bacteria, 80 µL TSB, and 100 µL of each cell-free supernatant were incubated at 37 °C for 24 h. After incubation, supernatants were aspirated from wells gently and the wells were washed three times with 250 μL PBS to remove any unattached bacteria and air-dried. 200 μL of 99% methanol was added to each well to fixate for 15 min and aspiration was performed in each well. To detect biofilm mass, wells were stained with 200 μL 0.1% crystal violet (in water) for 5 min. Excess stain was gently rinsed off with tap water, and the plates were air-dried. The stain was solubilized by adding 200 μL of 95% ethanol. Biofilm formations were determined by optical density measurement in a spectrophotometer at 450 nm. We interpreted our results, according to four categories as described previously by Christensen et al. (1985) [26].
We used E. coli ATCC 25,922 as positive control (a biofilm forming strain was used as an internal control) and TSB-glucose (without CFSs) as negative control.
The assay was repeated three times.
Cell Viability
Cells seeded in 96-well plates with/without CFS of each Lactobacillus are infected/non-infected with each S. aureus strains and incubated at 37 °C under 5% CO2 for three hours. After the wells were washed three times with PBS to remove all residues including medium, bacteria, and CFSs, fresh culture media was added to each well. Cell viability was examined by methylthiazolyldiphenyltetrazolium bromide (MTT) assay. Stock solution of MTT (12 mM) (Neofrox 3580 MTT) was prepared as described by Mosmann (1983) and added to each well [25]. After incubation at 37 °C for 4 h, the media was removed from the wells and the remained formosan crystals in wells were dissolved in 70 µL of dimethyl sulfoxide (DMSO) for 10 min. Absorbance was measured at 540 nm. The effects of each S. aureus and CFSs seperatly on HOB cells and the effects of each S. aureus on HOB cells in the presence of S. aureus strains and CFSs together were determined by comparing absorbance results.
All samples were tested in duplicate and each experiment was performed twice.
Statistical Analysis
Statistical analysis was determined by using one-way ANOVA followed by Tukey's multiple comparisons test. All measurements were compared to control conditions. All results are presented as mean ± SD.
Multiple comparisons were made at a level of P < 0.05 and the significance values were indicated as *: P < 0.05, **: P < 0.01, and ***: P < 0.001 in the manuscript.
Results
Bacterial Growth
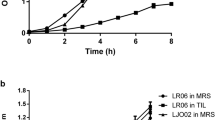
The growth of MSSA was statistically significantly (P < 0.01) decreased in the presence of Lf and Lr CFSs (P < 0.01), while the growth of MRSA was statistically significantly (P < 0.05) reduced in the presence of only La’ CFSs (Fig. 1a, b).
Effects of different lactobacilli CFSs on growth of S. aureus strains. The alterations were determined by comparing with control (S. aureus-infected HOB cells). a Growth alterations of MSSA; b Growth alterations of MRSA. The growth of bacteria in the presence of HOB cells were examined using one-way ANOVA followed by Tukey's multiple comparisons test *,**: Significant at P < 0.05 level and P < 0.01 level values, respectively
Bacterial Adhesion
All tested CFSs were found to reduce the adhesion of MSSA, and these results were statistically significant (P < 0.0001) when compared with the result of the experiment without CFSs.
The adhesion of MRSA was enhanced in the presence all of CFSs except La, and these results were statistically significant (P < 0.0001) (Fig. 2a, b).
Effects of different lactobacilli CFSs on adhesion of S. aureus strain. The alterations were determined by comparing with control (S. aureus-infected HOB cells). a Counts of adhered MSSA; b Counts of adhered MRSA. The adhesion of bacteria in the presence of HOB cells were examined using one-way ANOVA followed by Tukey's multiple comparisons test ***: Significant at P < 0.0001 level
Bacterial Invasion
All tested CFSs were found to reduce the invasion of MSSA, the differences were found to be statistically significant (P < 0.0001) when compared with the result of the experiment without CFSs. However, the invasion of MRSA was decreased in the presence of Lr and Lf CFSs, and these results were statistically significant (P < 0.01) (Fig. 3a, b).
Effects of different lactobacilli CFSs on invasion of S. aureus strains. The alterations were determined by comparing with control (HOB cells infected with S. aureus strains). a Counts of invasive MSSA; b Counts of invasive MRSA. The invasion of bacteria in the presence of HOB cells were examined using one-way ANOVA followed by Tukey's multiple comparisons test. **,***: Significant at P < 0.01 level and P < 0.0001 level values, respectively
Bacterial Biofilm Formation
All tested cell-free supernatants of lactobacilli were shown to inhibit biofilm formation of both S. aureus strains in 24 and 48 h significantly (P < 0.0001) (Fig. 4a, b).
Effects of different lactobacilli CFSs on biofilm of S. aureus strains. The alterations were determined by comparing with control (S. aureus strains). a Biofilm alterations of MSSA; b Biofilm alterations of MRSA. The biofilm formation of bacteria in the presence of CFSs was examined using one-way ANOVA followed by Tukey's multiple comparisons test ***: Significant at P < 0.0001 level
The figure shows the average absorbance results of both 24 and 48 h assays.
HOB Cell Viability
We examined the effects of MRSA, MSSA, and all CFSs on the viability of HOB cells on their own. According to these analyses, the viability of HOB cells were shown to be reduced statistically significant in the presence of S. aureus strains and CFSs except Lr CFS (P < 0.0001). These viability percentages are as follows: MSSA by 40.8 ± 9%, MRSA by 64.3 ± 8%, La by 47.6 ± 9%, Lp by 34.3 ± 9%, and Lf by 36.6 ± 8%) (Fig. 5).
Effects of different lactobacilli CFSs and S. aureus strains on HOB cell viability. The alterations were determined by comparing with control (HOB cells). The cell viability in the presence of CFSs and/or bacteria were examined using one-way ANOVA followed by Tukey's multiple comparisons test ***: Significant at P < 0.0001 level
We also examined the effects of S. aureus in the presence of all CFSs on the viability of HOB cells co-existence conditions. According to these analyses the viability of HOB cell during co-incubation with MSSA and CFSs was shown to be decreased significantly. The viability percentages are as follows: La by 83.7 ± 4%, Lp by 96 ± 4%, Lf by 65.3 ± 12%, and Lr by 53.7 ± 14%. However, during co-incubation with MRSA, the pre-treatment of HOB cells with CFSs did not alter viability significantly (Fig. 6a, b).
Alterations of HOB cell viability during co-incubation with different lactobacilli CFSs and S. aureus strains. The modulations were determined by comparing with control (S. aureus-infected HOB cells). a HOB cell viability in the presence of MSSA; b HOB cell viability in the presence of MRSA. The cell viabilities were examined using one-way ANOVA followed by Tukey's multiple comparisons test ***: Significant at P < 0.0001 level
Discussion
In our study, CFSs obtained from different Lactobacillus species were examined for the potential role of bioactive compounds in the supernatants on growth, adhesion, and invasion of S. aureus in HOB cell culture and on the cell viability of the HOB cell line. L. plantarum, L. fermentum, L. acidophilus, and L. rhamnosus which we used in our experiments are the mostly investigated strains for their possible inhibitory effects on growth and virulence factors of bacteria [19, 27,28,29,30,31,32,33,34,35].
It is well known that lactobacilli are able to increase phagocytic activity of human macrophages, to inhibit growth, adhesion, and invasion of pathogens by either competing with them or by changing environmental conditions by producing some bioactive compounds such as bacteriocins, lactic and other organic acids, hydrogen peroxide, and bio-surfactants. These compounds have effects on cell membrane integrity, membrane structure and enzyme activities, and cause DNA damage [16, 17, 36,37,38,39,40,41,42].
In the previous studies, it has been shown that different lactobacilli’s CFSs inhibited the growth of pathogens such as E. coli, S. aureus, S. epidermidis, K. pneumoniae, P. fluorescens, P. aeruginosa, S. mutans, L. monocytogenes, V. cholerae, and Salmonella [30, 43,44,45,46,47,48,49,50,51,52]. In our study, we found that CFSs of L. fermentum and L. plantarum inhibit the growth of MSSA; the growth of MRSA was shown to be reduced in the presence of only L. acidophilus’s CFS.
One of the most important virulence factors of bacteria is the ability of adhesion on host cells or medical devices. The inhibitory effects of various lactobacilli’s CFSs on adhesion were investigated in different studies performed in different cell lines [41, 53,54,55]. Whereas adhesions of L. monocytogenes, Salmonella, S. dysenteriae and E. coli were found to be decreased/inhibited [21, 50, 56], adhesion of E. coli O157:H7 and Enteroaggregative E. coli were found to be not affected [10, 35, 57]. In our study, we found that the adhesion of MSSA was inhibited in the presence of all lactobacilli’s CFSs, but the adhesion of MRSA was enhanced in the presence of CFSs of Lp, Lr, and Lf.
Different lactobacilli’s CFSs were shown to prevent different bacterial invasion/internalization process in various cell lines [30, 47, 56, 58,59,60,61,62]. As an example, different CFSs have protective roles against invasion of L. monocytenes and Enteroinvasive E. coli [20, 50]. Consistent with these studies, we have shown that all the tested lactobacilli’s CFSs inhibited the invasion of MSSA, but only CFSs of L. fermentum and L. rhamnosus were found to inhibit the invasion of MRSA.
Another important virulence factor of S. aureus is biofilm formation which is known to increase virulence of microorganism. Many authors reported that biofilm formation of S. aureus, Candida albicans, P. aeruginosa, E. coli, S. mutans, B. cereus, and Vibrio [33, 34, 52, 63,64,65,66] was inhibited in the presence of CFSs of different Lactobacillus species. Consistent with these studies, we have also shown that all four CFSs have effectively found to inhibit the biofilm formation of both S. aureus strains. All these results indicate that lactobacilli CFSs have anti-biofilm effects on pathogens.
When bacteria infect host cells, viabilities of both host cells and bacterium alter. In our study, the individual effects of MSSA, MRSA, and all CFSs on HOB cell viability were examined. In addition, we also investigated the viability of MSSA and MRSA-infected HOB cell line in the presence of CFSs. Various studies have showed that CFSs obtained from different lactobacilli have toxic activity on different cell lines such as HT-29, Caco-2, HeLa, MCF-7, and AGS [67,68,69]. Consistent with these studies, in our study, all lactobacilli’s CFSs except L. rhamnosus inhibited the viability of HOB cell line. As some authors suggest that this inhibitory effect is related with decreased pH levels and increased lactic acid levels provided by lactobacilli CFSs [67, 68, 70].
We also found that infection of HOB cells with both two S. aureus strains has also significant inhibitory effect on the viability of HOB cells. In consistent with previous studies, the viability of MRSA-infected HOB cells were shown to be not altered significantly in the presence of all tested CFSs [41, 58, 61, 71]. In contrast with these results, MSSA-infected HOB cells viabilities were shown to be inhibited in the presence of CFSs when compared to MRSA-infected HOB cells.
In consistent with previous studies, we found an antagonist relationship between lactobacilli and S. aureus. In our study, the growth alterations of S. aureus were investigated in HOB cell culture; as far as we know, this is the first study examining the effects of lactobacilli’s CFSs on growth of S. aureus in cell culture. The most important result is that all CFSs were found to be less effective for inhibiting the antibiotic resistant S. aureus strain representing as the problematical bacteria. These results indicate that antibiotic resistance become a major concern during the selection of the pathogenic strains for using in the experiments investigating the inhibitory potentials of probiotics.
There are some limitations in the present study such as the growth alterations of pathogenic bacteria are tested in live cell condition (HOB cell line). As the incubation of MRSA and MSSA were not prolonged for 24 h, growth curve was not able to be detected in order to avoid deleterious effect on the HOB cells.
HOB cell and S. aureus interactions are not yet clearly known. The knowledge of invasion ability of S. aureus in cell culture assays is limited in the literature and to clarify the difference between adhesion and invasion capacity of MRSA, future investigations with different cell lines are needed. In the present study, we found that MRSA and MSSA strain had different cytotoxic effects on HOB cells. We chose these strains according to their different antibiotic resistance properties, but the other biological characteristics of them (different virulence mechanisms, etc.) may be major determinatives.
References
FAO/WHO (2001) Joint FAO/WHO Expert consultation on evaluation of health and nutritional properties of probiotics in food including powder milk with live lactic acid bacteria. https://www.who.int/foodsafety/publications/fs_management/en/probiotics.pdf. Accessed 13 Dec 2019
Lash BW, Mysliwiec TH, Gourama H, Mysliwiec TH (2005) Detection and partial characterization of a broad-range bacteriocin produced by Lactobacillus plantarum (ATCC 8014). Food Microbiol 22:199–204
Oelschlaeger TA (2010) Mechanisms of probiotic actions—a review. Int J Med Microbiol 300:57–62
Todorov SD, Meincken M, Dicks LM (2006) Factors affecting the adsorption of bacteriocins ST194BZ and ST23LD to Lactobacillus sakei and Enterococcus sp. J Gen Appl Microbiol 52:159–167
Morelli L, Zonenenschain D, Piano M, Cognein P (2004) Utilization of the intestinal tract as a delivery system for urogenital probiotics. J Clin Gastroenterol 38:107–110
Servin AL (2004) Antagonistic activities of lactobacilli and bifidobacteria against microbial pathogens. FEMS Microbiol Rev 28:405–440
Wu CC, Lin CT, Wu CY, Peng WS, Lee MJ, Tsai YC (2015) Inhibitory effect of Lactobacillus salivarius on Streptococcus mutans biofilm formation. Mol Oral Microbiol 30:16–26
Wagner RD, Johnson SJ (2012) Probiotic lactobacillus and estrogen effects on vaginal epithelial gene expression responses to Candida albicans. J Biomed Sci 19:58
Juárez Tomás MS, Wiese B, Nader-Macías ME (2005) Effects of culture conditions on the growth and auto-aggregation ability of vaginal Lactobacillus johnsonii CRL 1294. J Appl Microbiol 99:1383–1391
Miyazaki Y, Kamiya S, Hanawa T, Fukuda M, Kawakami H, Takahashi H, Yokota H (2010) Effect of probiotic bacterial strains of Lactobacillus, Bifidobacterium, and Enterococcus on enteroaggregative Escherichia coli. J Infect Chem 16:10–18
Behnsen J, Deriu E, Sassone-Corsi M, Raffatellu M (2013) Probiotics: properties, examples, and specific applications. Cold Spring Harb Perspect Med 3:a010074
Turroni F, Ventura M, Buttó LF, Duranti S, O’Toole PW, Motherway MOC, van Sinderen D (2014) Molecular dialogue between the human gut microbiota and the host: a Lactobacillus and Bifidobacterium perspective. Cell Mol Life Sci 71:183–203
Jung S, Park OJ, Kim AR, Ahn KB, Lee D, Kum KY, Yun CH, Han SH (2019) Lipoteichoic acids of lactobacilli inhibit Enterococcus faecalis biofilm formation and disrupt the preformed biofilm. J Microbiol 57:310–315
Makino S, Ikegami S, Kano H, Sashihara T, Sugano H, Horiuchi H, Saito T, Oda M (2006) Immunomodulatory effects of polysaccharides produced by Lactobacillus delbrueckii ssp. bulgaricus OLL1073R-1. J Dairy Sci 89:2873–2881
Stoyancheva G, Marzotto M, Dellaglio F, Torriani S (2014) Bacteriocin production and gene sequencing analysis from vaginal Lactobacillus strains. Arch Microbiol 196:645–653
Tomaro-Duchesneau C, Saha S, Malhotra M, Coussa-Charley M, Al-Salami H, Jones M, Prakash S (2012) Lactobacillus fermentum NCIMB 5221 has a greater ferulic acid production compared to other ferulic acid esterase producing Lactobacilli. Int J Probiotics Prebiotics 7(1):23–32
Karska-Wysocki B, Bazo M, Smoragiewicz W (2010) Antibacterial activity of Lactobacillus acidophilus and Lactobacillus casei against methicillin-resistant Staphylococcus aureus (MRSA). Microbiol Res 165:674–686
Nigam A, Kumar A, Madhusuda HV, Bhola N (2012) In-vitro Screening of antibacterial activity of lactic acid bacteria against common enteric pathogens. J Biomed Sci 1:4
Saha S, Tomaro-Duchesneau C, Malhotra M, Tabrizian M, Prakash S (2012) Suppression of Streptococcus mutans and Candida albicans by probiotics: an in vitro study. Dentistry 2(6):141–148
Khodaii Z, Ghaderian SMH, Natanzi MM (2017) Probiotic bacteria and their supernatants protect enterocyte cell lines from enteroinvasive Escherichia coli (EIEC) invasion. Int J Mol Cell Med 6:183
Nantavisai K, Puttikamonkul S, Chotelersak K, Taweechotipatr M (2018) In vitro adhesion property and competition against enteropathogens of Lactobacillus strains isolated from Thai infants. Songklanakarin J Sci Tec 40:69–74
Hugo AA, Kakisu E, De Antoni GL, Pérez PF (2008) Lactobacilli antagonize biological effects of enterohaemorrhagic Escherichia coli in vitro. Lett Appl Microbiol 46:613–619
Castilho IG, Dantas STA, Langoni H, Araújo JP Jr, Fernandes A Jr, Alvarenga FC, Maia L, Cagnini DQ, Rall VL (2017) Host-pathogen interactions in bovine mammary epithelial cells and HeLa cells by Staphylococcus aureus isolated from subclinical bovine mastitis. J Dairy Sci 100:6414–6421
Artini M, Scoarughi GL, Papa R, Cellini A, Carpentieri A, Pucci P, Amoresano A, Gazzola S, Cocconcelli PS, Selan L (2011) A new anti-infective strategy to reduce adhesion-mediated virulence in Staphylococcus aureus affecting surface proteins. Int J Immunopathol Pharmacol 24:661–672
Mosmann T (1983) Rapid colorimetric assay for cellular growth and survival: application to proliferation and cytotoxicity assays. J Immunol Methol 65:55–63
Christensen GD, Simpson WA, Younger JJ, Baddour LM, Barrett FF, Melton DM, Beachey EH (1985) Adherence of coagulase-negative staphylococci to plastic tissue culture plates: a quantitative model for the adherence of staphylococci to medical devices. J Clin Microbiol 22:996–1006
Bohora AA, Kokate SR (2017) Good bugs vs bad bugs: evaluation of inhibitory effect of selected probiotics against Enterococcus faecalis. J Contemp Dent Pract 18:312–316
Bulgasem BY, Lani MN, Hassan Z, Yusoff WMW, Fnaish SG (2016) Antifungal activity of lactic acid bacteria strains isolated from natural honey against pathogenic Candida species. Mycobiology 44:302–309
Delley M, Bruttin A, Richard M, Affolter M, Rezzonico E, Brück WM (2015) In vitro activity of commercial probiotic Lactobacillus strains against uropathogenic Escherichia coli. FEMS Microbiol Lett 362:13
Liu J, Hu D, Chen Y, Huang H, Zhang H, Zhao J, Gu Z, Chen W (2018) Strain-specific properties of Lactobacillus plantarum for prevention of Salmonella infection. Food Funct 9:3673–3682
Montecinos FEM, Jofre FM, Amendola I, Goncalves CR, Leao MVP, Dos Santos SSF (2016) Relationship between the probiotic Lactobacillus rhamnosus and Enterococcus faecalis during the biofilm formation. Afr J Microbiol Res 10:1182–1186
Mohammedsaeed W, McBain AJ, Cruickshank SM, O’Neill CA (2014) Lactobacillus rhamnosus GG inhibits the toxic effects of Staphylococcus aureus on epidermal keratinocytes. Appl Environ Microbiol 80:5773–5781
Raj A, Bhati P, Bhadekar R (2017) Effect of lactic acid bacteria on biofilm formation by Streptococcus mutans: an ın vitro study. Int J Pharm Sci Res 8:2533–2538
Vacheva A, Georgieva R, Danova S, Mihova R, Marhova M, Kostadinova S, Vasileva K, Bivolarska M, Stoitsova S (2012) Modulation of Escherichia coli biofilm growth by cell-free spent cultures from lactobacilli. Open Life Sci 7:219–229
Kim Y, Kim SH, Whang KY, Kim YJ, Oh S (2018) Inhibition of Escherichia coli O157: H7 attachment by interactions between lactic acid bacteria and intestinal epithelial cells. J Microbiol Biotech 18:1278–1285
Merghni A, Dallel I, Noumi E, Kadmi Y, Hentati H, Tobji S, Amor AB, Mastouri M (2017) Antioxidant and antiproliferative potential of biosurfactants isolated from Lactobacillus casei and their anti-biofilm effect in oral Staphylococcus aureus strains. Microb Pathog 104:84–89
Poppi LB, Rivaldi JD, Coutinho TS, Astolfi-Ferreira CS, Ferreira AJP, Mancilha IM (2015) Effect of Lactobacillus sp. isolates supernatant on Escherichia coli O157: H7 enhances the role of organic acids production as a factor for pathogen control. Pesq Vet Bras 35:353–359
Aminnezhad S, Kermanshahi RK, Ranjbar R (2015) Evaluation of synergistic interactions between cell-free supernatant of Lactobacillus strains and amikacin and gentamicin against Pseudomonas aeruginosa. Jundishapur J Microbiol 8:4
Kim JU, Kim Y, Han KS, Oh S, Whang KY, Kim JN, Kim SH (2006) Function of cell-bound and released exopolysaccharides produced by Lactobacillus rhamnosus ATCC 9595. J Microbiol Biotechnol 16:939–945
Stecher B, Hardt WD (2011) Mechanisms controlling pathogen colonization of the gut. Curr Opin Microbiol 14:82–91
Jayashree S, Karthikeyan R, Nithyalakshmi S, Ranjani J, Gunasekaran P, Rajendhran J (2018) Anti-adhesion property of the potential probiotic strain Lactobacillus fermentum 8711 against methicillin-resistant Staphylococcus aureus (MRSA). Front Microbiol 9:411
Alvarez-Olmos MI, Oberhelman RA (2001) Probiotic agents and infectious diseases: a modern perspective on a traditional therapy. Clin Infect Dis 32(11):1567–1576
Gutiérrez S, Martínez-Blanco H, Rodríguez-Aparicio LB, Ferrero MA (2016) Effect of fermented broth from lactic acid bacteria on pathogenic bacteria proliferation. J Dairy Sci 99(4):2654–2665
Hor YY, Liong MT (2014) Use of extracellular extracts of lactic acid bacteria and bifidobacteria for the inhibition of dermatological pathogen Staphylococcus aureus. Dermatol Sin 32(3):141–147
Cadieux PA, Burton J, Devillard E et al (2009) Lactobacillus by-products inhibit the growth and virulence ofuropathogenic Escherichia coli. J Physiol Pharmacol 60(6):13–18
Chen CC, Lai CC, Huang HL, Huang WY, Toh HS, Weng TC et al (2019) Antimicrobial activity of Lactobacillus species against carbapenem-resistant Enterobacteriaceae. Front Microbiol 10:789
Terraf MCL, Tomás MSJ, Rault L, Le Loir Y, Even S, Nader-Macías MEF (2017) In vitro effect of vaginal lactobacilli on the growth and adhesion abilities of uropathogenic Escherichia coli. Arch Microbiol 199(5):767–774
Singh N, Sharma C, Gulhane RD, Rokana N, Singh BP, Puniya AK, Panwar H (2018) Inhibitory effects of lactobacilli of goat’s milk origin against growth and biofilm formation by pathogens: an in vitro study. Food Biosci 22:129–138
Wasfi R, Abd El-Rahman OA, Zafer MM, Ashour HM (2018) Probiotic Lactobacillus sp. inhibit growth, biofilm formation and gene expression of caries-inducing Streptococcus mutans. J Cell Mol Med 22(3):1972–1983
Castellano P, Ibarreche MP, Borges LL, Arias FN, Ross GR, De Martinis EP (2018) Lactobacillus spp. impair the ability of Listeria monocytogenes FBUNT to adhere to and invade Caco-2 cells. Biotechnol Lett 40(8):1237–1244
Bilkova A, Sepova HK, Bukovsky M, Bezakova L (2011) Antibacterial potential of lactobacilli isolated from a lamb. Vet Med 56(56):319–324
Kaur S, Sharma P, Kalia N, Singh J, Kaur S (2018) Anti-biofilm properties of the fecal probiotic Lactobacilli against Vibrio spp. Front Cell Infect Microbiol 8:120
Yan X, Gu S, Cui X, Shi Y, Wen S, Chen H, Ge J (2019) Antimicrobial, anti-adhesive and anti-biofilm potential of biosurfactants isolated from Pediococcus acidilactici and Lactobacillus plantarum against Staphylococcus aureus CMCC26003. Microb Pathog 127:12–20
Mukherjee S, Ramesh A (2015) Bacteriocin-producing strains of Lactobacillus plantarum inhibit adhesion of Staphylococcus aureus to extracellular matrix: quantitative insight and implications in antibacterial therapy. J Med Microbiol 64(12):1514–1526
Ren D, Li C, Qin Y, Yin R, Li X, Tian M et al (2012) Inhibition of Staphylococcus aureus adherence to Caco-2 cells by lactobacilli and cell surface properties that influence attachment. Anaerobe 18(5):508–515
He X, Zeng Q, Puthiyakunnon S, Zeng Z, Yang W, Qiu J et al (2017) Lactobacillus rhamnosus GG supernatant enhance neonatal resistance to systemic Escherichia coli K1 infection by accelerating development of intestinal defense. Sci Rep 7:1–14
Jankowska A, Laubitz D, Antushevich H, Zabielski R, Grzesiuk E (2008) Competition of Lactobacillus paracasei with Salmonella enterica for adhesion to Caco-2 cells. BioMed Res Int. https://doi.org/10.1155/2008/357964
Bouchard DS, Rault L, Berkova N, Le Loir Y, Even S (2013) Inhibition of Staphylococcus aureus invasion into bovine mammary epithelial cells by contact with live Lactobacillus casei. Appl Environ Microbiol 79(3):877–885
Hirano J, Yoshida T, Sugiyama T, Koide N, Mori I, Yokochi T (2003) The effect of Lactobacillus rhamnosus on enterohemorrhagic Escherichia coli infection of human intestinal cells in vitro. Microbiol Immunol 47(6):405–409
Alamdary SZ, Bakhshi B, Soudi S (2018) The anti-apoptotic and anti-inflammatory effect of Lactobacillus acidophilus on Shigella sonnei and Vibrio cholerae interaction with intestinal epithelial cells: a comparison between invasive and non-invasive bacteria. PLoS ONE 13(6):1–16
Moorthy G, Murali MR, Devaraj SN (2010) Lactobacilli inhibit Shigella dysenteriae 1 induced pro-inflammatory response and cytotoxicity in host cells via impediment of Shigella–host interactions. Digest Liv Dis 42(1):33–39
Campana R, Federici S, Ciandrini E, Baffone W (2012) Antagonistic activity of Lactobacillus acidophilus ATCC 4356 on the growth and adhesion/invasion characteristics of human Campylobacter jejuni. Curr Microbiol 64(4):371–378
Zamani H, Rahbar S, Garakoui SR, Sahebi AA, Jafari H (2017) Antibiofilm potential of Lactobacillus plantarum spp. cell free supernatant (CFS) against multidrug resistant bacterial pathogens. Pharm Biomed Res 3(2):39–44
Frickmann H, Klenk C, Warnke P, Redanz S, Podbielski A (2018) Influence of probiotic culture supernatants on in vitro biofilm formation of staphylococci. Eur J Microbiol Immunol 8(4):119–127
Koohestani M, Moradi M, Tajik H, Badali A (2018) Effects of cell-free supernatant of Lactobacillus acidophilus LA5 and Lactobacillus casei 431 against planktonic form and biofilm of Staphylococcus aureus. Vet Res For 9(4):301
Khiralla GM, Mohamed EA, Farag AG, Elhariry H (2015) Antibiofilm effect of Lactobacillus pentosus and Lactobacillus plantarum cell-free supernatants against some bacterial pathogens. J Biotech Res 6:86
Chen ZY, Hsieh YM, Huang CC, Tsai CC (2017) Inhibitory effects of probiotic Lactobacillus on the growth of human colonic carcinoma cell line HT-29. Molecules 22(1):107
Sadeghi-Aliabadi H, Mohammadi F, Fazeli H, Mirlohi M (2014) Effects of Lactobacillus plantarum A7 with probiotic potential on colon cancer and normal cells proliferation in comparison with a commercial strain. Iran J Bas Med Sci 17(10):815
Nami Y, Abdullah N, Haghshenas B, Radiah D, Rosli R, Khosroushahi AY (2014) Probiotic potential and biotherapeutic effects of newly isolated vaginal Lactobacillus acidophilus 36YL strain on cancer cells. Anaerobe 28:29–36
Motevaseli E, Shirzad M, Akrami SM, Mousavi AS, Mirsalehian A, Modarressi MH (2013) Normal and tumour cervical cells respond differently to vaginal lactobacilli, independent of pH and lactate. J Med Microbiol 62(7):1065–1072
Burkholder KM, Bhunia AK (2009) Salmonella enterica serovar Typhimurium adhesion and cytotoxicity during epithelial cell stress is reduced by Lactobacillus rhamnosus GG. Gut Pathog 1(1):14
Author information
Authors and Affiliations
Contributions
Concept: FKY, DG, and MAK. Data collection & Processing: FKY, DG, and GİG. Analysis & Interpretation: FKY, DG, and GİG. Literature Research: FKY, DG, and MAK. Writing: FKY, DG, and MAK. Critical Reviews: FKY, DG, GİG, and MAK.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there are no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kalaycı Yüksek, F., Gümüş, D., Gündoğan, G.İ. et al. Cell-Free Lactobacillus sp Supernatants Modulate Staphylococcus aureus Growth, Adhesion and Invasion to Human Osteoblast (HOB) Cells. Curr Microbiol 78, 125–132 (2021). https://doi.org/10.1007/s00284-020-02247-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00284-020-02247-1