Abstract
Posterior fossa tumors (PFT) are the most common pediatric brain tumors, and the study of the somatic and cognitive status of PFT survivors still remains a critical problem. Since cerebellar damage can affect eye movement centers located in the vermis and hemispheres, such patients suffer from disturbances in visual perception, visual-spatial functions, reading, etc. Our investigation aimed at describing oculomotor impairments in PFT survivors linked to core oculomotor functions assessed through eye tracking method: gaze holding, reflexive saccades, and organization of voluntary saccades and their dependency on age at tumor diagnosis. Also, we investigated the relationship between oculomotor functions and ataxia measured with International Cooperative Ataxia Rating Scale (ICARS). A total of 110 children (patients and age-matched healthy controls, aged 9–17 years old) participated in the study. We found that the earlier the child had a tumor, the more impaired gaze holding (p = 0.0031) and fewer isometric saccades (p = 0.035) were observed at the time of examination. The above-mentioned functions in healthy controls improved with age. Visual scanning was also impaired compared to controls but was not related to age at diagnosis. A positive correlation between ICARS scores and number of hypermetric saccades (r = 0.309, p = 0.039), but no correlation with the number of hypometric saccades (r = − 0.008, p = 0.956). Furthermore, number of hypometric saccades did not differ between patients and controls (p = 0.238). Thus, primarily hypermetric saccades can be considered a prominent oculomotor symptom of cerebellar tumors. Our study provides basis for new methods of PFT diagnosis and rehabilitation procedure evaluation, both playing essential roles in modern pediatric neurooncology.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
It is widely known that cerebellar patients have various types of sensory, motor, and cognitive disturbances resulting from lesions of the cerebellum of different etiologies. Oculomotor impairments such as gaze-evoked and downbeat nystagmus, square wave jerks, intrusive saccades, and saccadic dysmetria are frequently observed symptoms indicating lesions flocculus/paraflocculus, uvula/nodulus, oculomotor vermis, fastigial nuclei, or their projections to other eye movement structures [1, 2]. We consider oculomotor impairments to be important to a great extent for both motor and cognitive domains because motor areas and structures involved in the saccadic system also serve various cognitive activities such as perception, attention, memory, reading, etc. [3, 4]. Plenty of investigations have described particular motor, oculomotor, and neuropsychological abnormalities, but separately, in cerebellar patients [5,6,7,8,9,10], while only a few studies have shown the association between them [11, 12]. Moreover, the impact of the cerebellar tumor on oculomotor dysfunction was revealed only in several studies, despite the earliest evidence appearing in the 1950s [13,14,15,16]. Further studies included patients with SCA, cerebellar stroke, etc., apart from the patients with cerebellar tumors [17,18,19]. We believe the investigation of cerebellar dysfunction due to tumors and its treatment, especially in still-developing brains in pediatric patients, to be of utmost importance.
Posterior fossa tumors (PFT) are the most common pediatric brain tumors, comprising a wide range of low- and high-grade tumors such as medulloblastoma (30–40%), astrocytoma (30–35%), and ependymoma (10%), which differ in their histology and etiology [20]. Treatment of PFT consists of surgery, chemo- and radiotherapy, depending on its malignancy, metastasis stage, and treatment response. New advanced treatment approaches have resulted in increased survival rates, making long-term negative effect mitigation and quality of life improvement in PFT survivors the key issue of pediatric neurooncology [21].
Neuropsychological investigations in PFT survivors who underwent treatment show disturbances in the visuospatial organization, rotation, attention, planning, memory tasks, audio-verbal processing, timing, and affective reactions [10, 22, 23]. This combination is called Schmahmann/cerebellar cognitive affective syndrome. These disturbances result from damage to neural circuits serving interconnections between the cerebellum and cerebral association areas [24]. As to the motor characteristics of PFT survivors, some studies show muscle weakness, gait and posture disturbances, and fine motor skill degradation arising from impaired cerebellar-cerebral sensorimotor representations [25, 26]. Only a few studies on cancer patients (not PFT) have emphasized the role of treatment on oculomotor functions such as poor smooth pursuit accuracy and saccades with a disproportionally shorter amplitude [27].
Our investigation aimed to describe impairments in core oculomotor functions in PFT survivors: gaze fixation, reflexive saccades (measured as execution accuracy to appeared stimuli), and organization of voluntary saccades (their parameters during visual search). We also performed a correlation analysis of saccadic accuracy indicators and International ICARS scores in patients to determine relationships between motor and oculomotor performance deficits due to cerebellar dysfunction.
Materials and Methods
Participants
Sixty-six patients (41 boys and 25 girls; 12.75 ± 2.63 years of age, mean ± SD) receiving rehabilitation courses at the Clinical Rehabilitation Research Center “Russkoe Pole” (Checkov, Russia) participated in the study. The patients were diagnosed with different types of posterior fossa tumors: medulloblastoma (n = 40), pilocytic astrocytoma (n = 21), and anaplastic ependymoma (n = 5) and were in remission for at least 4 months at the time of the study. The data on their clinical history are shown in Table 1. Fifty-four age-matched (26 boys and 28 girls; 12.98 ± 2.39 y.o.) healthy children without a history of neurological diseases served as a control group. The participants that had severe (or any—in case of healthy controls) neurological, ophthalmologic (such as strabismus, ophthalmoplegia, amblyopia, and low visual acuity (± 2 diopters and more)), or cognitive impairments (reduced intelligence on the Raven test) had been excluded from the study. The research protocol was approved by the Ethics Committee of the Dmitry Rogachev National Research Center of Pediatric Hematology, Oncology, and Immunology (protocol number 8e/13-17 of 27.10.2017) and is in accordance with Helsinki Declaration. Written informed consent was obtained from all participants over the age of 15 or from their legal representatives in the case of younger participants.
Both patients and healthy controls were asked to perform three tasks to assess parameters of saccadic movements. To evaluate the impact of age on performance of the oculomotor system, we divided children into three groups depending on their age: 9–11, 12–14, and 15–17 years old. Table 2 shows the number of participants in each group in every oculomotor test utilized in this analysis. We have also taken into account the age at tumor diagnosis (according to the neurooncologist’s recommendation), dividing participants into four groups: 0–3, 4–6, 7–12, and over 13 years old.
In order to assess the severity of motor dysfunction, the patients were individually evaluated by the same certified neurologist, and each was assigned an ICARS score [28]. The general ICARS score ranks the posture and gait disturbances, limb functions, speech, and oculomotor disorders. ICARS scores are applicable to children treated for cerebellar tumors [29].
Oculomotor Study
Setup
Participants were seated in an armchair placed in a quiet, dark room with their heads fixed positioned with a chinrest and forehead support. Eye movements were recorded with the Arrington eye tracker (Arrington Research, Inc., USA) at a sampling rate of 60 samples/s. Each trial of eye movement recordings started with a standard 9-point calibration sequence for the entire testing area of the computer monitor used to present the visual stimuli. This calibration procedure preceded presentation of each oculomotor task to warrant better data collection accuracy. Gaze data were acquired from the right eye. The oculomotor tasks were presented and controlled by the ViewPoint EyeTracker® 2.9.2.5 software (Arrington Research, Inc., USA). Saccade onset and offset were detected using a built-in velocity threshold criterion and were continuously monitored by an experimenter. Visual stimuli were presented on a 23″ Samsung monitor (at a 1920 × 1080 pixel resolution); the active area of the monitor was located at 60 cm, in front of a participant’s eyes, thus forming a field with a 45° × 26° visual angle.
The oculomotor study consisted of three oculomotor tests exploring core eye movement functions. The tasks separated by short breaks were consecutively presented from the easiest to the hardest to accommodate children in the experimental environment. The experimenter provided the participants with the instructions for each task at the beginning of each recording session. The execution of an entire battery of tasks required approximately 15 min and was not too taxing for the children.
Tasks
Gaze Holding (GH, Fig. 1a)
The goal of the task was to determine the stability of gaze fixation. The black central fixation point (FP) was initially shown at the center of the screen for 4–5 s. The test sequence consisted of presentation of the green dot (~ 1° in diameter; 15° left/right and 8° up/down from the center of the screen), 20 s each, at four eccentric locations on the screen. The participant was instructed: “Look at the green dot and follow it when it reappears at another place. The dot will stay at the same location for a while.” The areas of the ellipses that fitted the gaze positions were obtained.
Visually Guided Saccade (VGS, Fig. 1b)
This task enabled an evaluation of the accuracy of reflexive saccades to the stimulus that appeared horizontally or vertically. The FP was shown as in GH. A square with a 10° side was then presented. In its corners, a red circle (~ 1° in diameter) appeared consequently in the clockwise direction for 500 ms, evoking visually guided saccades. The participant was instructed: “Follow the red circle and jump when the circle moves to the next position.” In total, the participant had to perform 24 saccades with an amplitude of 10°. The ratios of isometric, hypometric, hypermetric, and corrective saccades were determined.
Visual Search (VS, Fig. 1c)
This task was designed to assess the organization of voluntary saccades during image scanning when performing a simple cognitive task (object counting requiring visual search). The FP was shown as in GH. Then ten black dots (~ 1° in diameter) were shown on the monitor, arranged in pseudo-random order. The participant instruction was as follows: “Count the number of dots and state it aloud.” We analyzed task execution time, number of fixations, their average duration, scanpath, and average saccade amplitude.
Oculomotor Data Analysis
We used the ViewPoint EyeTracker ® 2.9.2.5 software (Arrington Research, Inc., USA) ViewPoint EyeTracker ® 2.9.2.5 software (Arrington Research, Inc., USA) to extract gaze coordinates. To extract events (fixations and saccades) from these coordinates, Data Analysis software (Arrington Research, Inc., USA) was used.
In the GH, the obtained raw gaze coordinates during gaze holding on the stimulus were filtered in the MATLAB 2013 software (Mathworks, Inc., Natick, MA) using ± 2σ distribution filter. Then the resulting coordinates were fitted with an ellipse using the fit_ellipse function (https://www.mathworks.com/matlabcentral/fileexchange/3215-fit_ellipse) [30]. The calculated area of the ellipses was converted into square degrees of visual angle (deg2). The ellipse areas were calculated for each of the four stimulus positions for each participant, with the exception of artifact values caused by incorrect pupil detection (approximately 10% of the data).
In VGS task, saccades were considered isometric if their amplitude (A) fell in the range of 8.5–11.5°, as dysmetria consists of a 10% deviation from correct amplitude (in our case, 10°) (Thuttell et al. 2007), and the device detection error is 0.5°. Therefore, hypometric saccades (undershoot, A < 8.5°), hypermetric (overshoot, A > 11.5°), and corrective saccades (following dysmetric saccades, 1.5° < A < 5°) were analyzed. Ratios of iso-, hypo-, hyper-metric, and corrective saccades to the total number of saccades were calculated for each participant.
In the VS task, the patient had to count the total number of dots and to report the result to the examiner. The time period between the task onset and the vocal report was considered an execution time. The scanning trajectory was estimated as the sum of the amplitudes of all performed saccades. We excluded from the analysis the fixations that lasted for less than 80 ms. We obtained these measures from each participant.
Statistical Analysis
We run the Mann–Whitney test (U) to compare the oculomotor parameters between all patients and all healthy controls, while the Kruskal–Wallis test (H) was used to compare oculomotor parameters between the three age groups of patients and the healthy controls. The H-test was also used to compare the parameters in patients subdivided into four groups based on age at diagnosis. We applied post hoc parametric tests with correction for multiple comparisons when the nonparametric ones showed significant differences between the groups.
To determine whether the level of ataxic symptoms was related to the extent of oculomotor deficits, we run the Spearman’s rank correlation tests to compare the ICARS scores and oculomotor parameters obtained during VGS tasks. P-values of less than 0.05 were considered significant. Trends (p < 0.1) are marked in the figures and tables. All the analyses were performed with the software package STATISTICA v. 13.3 (TIBCO Software Inc., USA).
Results
Gaze Holding
The comparison between patient and healthy control groups showed that ellipse areas had significantly increased in patients, with a median of 2.32 (range 0.21–30.73) vs 1.22 (0.19–10.53) deg2 (U = 9026.0, p = 0.00001). The visualization of task performance demonstrates different oculomotor impairments that disrupt stable fixation in patients: horizontal or vertical gaze-evoked nystagmus, intrusive saccades, and involuntary saccades of high amplitude caused by attention disturbances (Fig. 2a, b).
Left: visualization of GH test via Matlab fit_ellipse function (a healthy control; b patient). Gaze coordinates were approximated by ellipses using the least squares method. Axes show pixels of the screen. Middle: VGS (c healthy control; d patient). Right: VS (e healthy control; f patient). c–f 2D plots of oculomotor performance. Saccades are indicated in red and fixations in green. Vertical scale bars are 5°
Analysis of age impact on gaze holding was performed within each group. In patients, the ellipse areas did not significantly differ between the three age groups, while in healthy controls they did (Table 3). Further analysis showed that ellipse areas were significantly different between the youngest and oldest groups (p = 0.002), thus indicating the decline in fixation instability with age in healthy controls.
When comparing ellipse areas in four age groups depending on the age of diagnosis in patients, a significant progressive decrease in fixation instability was observed (H3.205 = 13.89, p = 0.0031; Fig. 3a). The earlier the child was diagnosed with a PFT, the more unstable was the gaze holding at the time of the study. The differences between groups 0–3 and 7–12 years old and 0–3 and over 13 y.o. reached the level of statistical significance.
Dependence of ellipse areas (a) and proportion of isometric saccades (b) on the time of diagnosis. The bars show medians, minimax values, and interquartile range. P-levels of statistical significance (post hoc analysis with corrections for multiple comparisons); n = number of observations in each group
Visually Guided Saccade
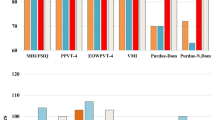
Analysis of distinct oculomotor patterns revealed a significantly greater number of isometric (U = 159.5, p = 0.00001), hypermetric (U = 141.0, p = 0.00001), and corrective (U = 160.5, p = 0.00001) saccades in patients vs. controls, while the number of hypometric saccades did not differ significantly (U = 755.0, p = 0.238) (Fig. 4). The visualization of task performance demonstrates hypermetric saccades occurred in patient (Fig. 2c, d).
Within each group, we analyzed dependence of performance in different visual tests on the age of subjects. In healthy controls (Fig. 5), the number of isometric saccades increases (H2.37 = 8.24, p = 0.016), while the number of hypometric saccades statistically significantly declines (H2.37 = 9.45, p = 0.009) with age. Further analysis showed that proportions of iso- and hypometric saccades significantly differed between the youngest (9–11 y.o.) and both older (12–14 and 15–17 y.o.) groups (all at p < 0.05), indicating the increase of saccadic accuracy with age in healthy controls. In contrast, no significant changes in the abovementioned measures of visual performance with age were observed in patients.
Patients diagnosed with a tumor at an older age had significantly higher numbers of isometric saccades (H2.44 = 6.69, p = 0.035; Fig. 3b), as well as hypometric and corrective saccades (H2.44 = 6.48, p = 0.039, and H2.44 = 6.00, p = 0.049, respectively). Patients diagnosed with tumor at youngest age (0–3 y.o.) were excluded only from this analysis because of the small size of the sample (3 observations).
Correlations with ICARS Scores
In order to reveal the relationships between patients’ saccadic accuracy measured in VGS task and ataxic symptoms, we performed the correlation analysis. Patients were found to have a positive correlation between ICARS scores and numbers of hypermetric (r = 0.309, p = 0.039), corrective saccades (r = 0.329, p = 0.027), and negative correlation between ICARS scores and number of isometric saccades (r = − 0.423, p = 0.004). Conversely, ICARS scores were not correlated with the number of hypometric saccades (r = − 0.008, p = 0.956).
Visual Search
Comparison of patient and healthy control groups’ performance showed a significant decline in parameters that we have called “cognitive” in patients: increased task execution time, number of fixations, and prolonged scanpath (Table 4). However, “physiological” parameters such as fixation duration and saccadic amplitudes did not differ significantly. The visualization of task performance demonstrates a large number of returning saccades to the same point, presumably for re-counting. At the same time, a healthy child counts a point with almost one fixation (Fig. 2e, f).
The analysis of oculomotor performance dynamics revealed no significant dependence on current age (Table 3) or age at diagnosis either in the patient group or in healthy controls.
Discussion
In the present study, we analyzed core oculomotor functions in pediatric PFT survivors, their dependence on the age and age of the diagnosis, and their relationships with the severity of ataxic symptoms. We observed typical cerebellar oculomotor abnormalities: unstable fixation, dysmetric saccades, and impaired visual scanning described in existing research on other cohorts. However, the most remarkable finding consists in the demonstration of significant differences in the number of hypermetric, but not hypometric, saccades between patients and healthy control groups, and the association of hypermetric, but not hypometric, saccades with ataxic symptoms.
In patients with PFT, the tumor development and its treatment by surgery, radiotherapy, and chemotherapy lead to damage to the cerebellar structures, including those involved in the saccadic system control and their connections with other brain areas. During the surgical removal of the tumor, required for medulloblastoma, astrocytoma, and ependymoma treatment, neurosurgeons often remove damaged cerebellar tissues in a large volume, which results in the inevitable damage to the structure of the oculomotor and vestibular cerebellum, cerebellar hemispheres, and their afferent and efferent projections. Moreover, chemotherapy, especially when combined with radiotherapy, causes general CNS damage and neurotoxic side effects [31].
Our analysis revealed significant impairment in gaze stability during gaze holding in patients when compared to healthy controls (Fig. 2a, b). Areas of the vestibular cerebellum, flocculus and paraflocculus, play an essential role in gaze fixation mechanisms [1, 32]. These regions are known to be closely associated with positive feedback to the saccade brainstem generator via NPH (nucleus prepositus hypoglossi) and MVN (medial vestibular nucleus), and damage to the vestibular cerebellum or its efferent projections is known to provoke a disruption of the brainstem generator during gaze holding [2, 33]. As a result of damage, cerebellar patients have oculomotor disorders such as spontaneous nystagmus, postassacadic drift, and intrusive saccades that disrupt the stable fixation on the visual object [13, 17, 34]. In our study, we analyzed the nature of the instability in oculomotor functions in patients qualitatively, based on the video-monitoring the oculomotor behavior during recording. In patients, oculomotor disruptions manifested as spontaneous nystagmus (horizontal, vertical, sometimes diagonal) and low-amplitude intrusive saccades. Visual attention disruption manifested in the form of irrelevant high-amplitude saccades that shift gaze away from the presented stimulus, indicating that the subject is incapable of focusing on it. Visual attention disorders in patients with cerebellar lesions are often associated with dysfunction of the cerebellar hemispheres [24]. Occasionally, patients experience mixed disturbances of both oculomotor and attention disruptions in the form of horizontal nystagmus and high-amplitude saccades.
In healthy controls, we also found high-amplitude saccades, shifting fovea from the presented stimulus; however, they were more often manifested in the younger age group, expressed in larger areas of ellipses. The analysis of age-related dynamics showed a systematic increase in the stability of gaze holding with age, demonstrating the most mature fixation process in the older age group (Table 3). Our data is consistent with previous studies [35, 36]. We did not find significant age-related dynamics in gaze holding parameters in patients with PFT, although in the middle and youngest age groups ellipse was smaller, than in the eldest one (Table 3). This indicates that the impairments of the oculomotor mechanisms in this sample of patients cannot be associated with their age since the patients were in different periods of remission, that is, the manifestation of the tumor and its treatment occurred at different ages for each patient.
However, our further analysis revealed a strong dependence of oculomotor impairments on age at diagnosis (Fig. 3). The later the child begins to develop a tumor, the more stable the process of gaze fixation is, and more isometric saccades are observed at the time of the study. This finding is in line with studies that have shown that CNS tumor development age is a negative prognostic factor since most of the structures and afferent-efferent systems are less formed at an earlier age and may not form properly as a result of the ongoing pathological process [37, 38]. Thus, in children who develop a tumor at an older age (older than 13 years), the development of the tumor and its subsequent treatment are less damaging to the almost fully formed gaze fixation and precise saccade generation. This assumption is supported by the observed dynamics of oculomotor functions’ maturation in healthy children, as described above and below in the text.
The comparison of visually guided saccades revealed a significantly decreased number of isometric saccades and increased hypermetric saccades in patients with PFT (Fig. 3c, d; 4). Saccadic hypermetria due to impairments to oculomotor cerebellum, including the dorsal vermis (lobules V–VII) and caudal fastigial nuclei [1, 2, 39]. Bilateral lesions of the fastigial nuclei result in saccade hypermetria in all directions, whereas unilateral lesions of fastigial nuclei or dorsal vermis lead to hypermetria only in ipsi- or contraversive direction to the side of the lesion [2, 40]. Our data are consistent with several studies of saccade hypermetria in cerebellar patients [14, 17, 41,42,43]. However, in contrast with the previous studies, we did not find a significant difference in the number of hypometric saccades. Hypometric saccades were found in healthy patients in several studies [44,45,46], but authors do not explain the presence of such saccades, pointing only to the fact that with age, children have fewer hypometric saccades [44, 46, 47]. According to our data, hypometria in healthy children also decreases with age (mirrorlike isometric saccades, Fig. 5), especially after 11 years, consistent with the literature data (after 8–10 years). Therefore, hypometria occasional hypometria is within normal range, as some authors have pointed out [44, 46].
This finding is supported by an analysis of relationships between the severity of ataxic symptoms and saccadic accuracy indicators. We found positive correlations between the number of hypermetric, corrective saccades, and ICARS scores, meaning that worse motor performance is associated with greater saccadic amplitude and its correction. In contrast, we observed neither significant nor borderline correlation between ICARS scores and the number of hypometric saccades (r = − 0.008; p = 0.956).
Moreover, we observed corrective saccades in both patients and healthy controls; however, in healthy controls, they occurred in significantly smaller numbers despite a comparable number of hypometric saccades (Fig. 4). Hence, we speculate that hypometric saccades are corrected much less often, which confirms the earlier assumption about hypometria being physiologically normal. It also appears that hypermetria rather than hypometria is considered to be a more serious deviation by the cerebellum, resulting in a greater percentage of corrections.
Thus, summarizing our results, we would like to emphasize that it is the hypermetric saccades that can be considered a prominent sign (and diagnostic parameter) of cerebellar dysfunction acquired after tumor’s treatment.
The comparison of visual search revealed a significant decline in “cognitive parameters”—task execution time, number of fixations, and scan path—whereas no significant differences in “physiological” parameters, such as fixation durations and saccadic amplitudes, were observed in patients with PFT (Fig. 2e, f; Table 4). The revealed results and visualization of oculomotor activity during the task indicate the presence of repeated saccadic patterns that return the fovea and, with it, the focus of the patient's attention to the already counted objects for re-fixation. Such gaze returns are associated with disturbances in detecting and memorizing object locations within visual field, reflecting difficulties in spatial orientation and impaired integration of visual-spatial processes [48]. Our results are consistent with studies that have shown impaired cognitive processes, in particular visual spatial attention and perception, in patients with cerebellar dysfunction, including those who were treated for cerebellar tumors [10, 22, 23]. Such disorders, which are part of the cerebellar cognitive-affective syndrome, are caused by a failure in the cerebellar-cortical interaction carried out by the cortical-pontocerebellar afferent pathways and the cerebellar-thalamic-cortical efferent pathways [24]. The main areas of the cerebellum involved in the processes of visual attention and spatial perception are the areas of the posterior lobe of the left hemisphere of the cerebellum [24, 49]. Through the thalamus, they project to the posterior parietal cortical regions involved in visual-spatial processing and attention [24, 50].
In this regard, the absence of differences in “physiological” indicators looks ambiguous (Table 4). Despite our results on visually guided saccades, we found no hypermetria or differences in amplitude in voluntary saccades between patients and healthy controls, suggesting different mechanism for voluntary saccade execution compared to reflexive (visually guided) saccades. Frontal oculomotor cortical fields play more important role in voluntary saccades execution, while parietal oculomotor fields, which have direct projections onto superior colliculus and brainstem saccadic generator, participate in spatial tasks [51]. In voluntary saccades, in contrast to the reflexive oculomotor reactions in the visually guided paradigm, the participation of the cerebellum is reduced. A similar effect is observed in Parkinson’s disease, when dopamine deficiency in the nigrostriatal system has a smaller effect on saccades’ parameters when free viewing the image compared to the hypometric visually guided saccades [52].
The absence of age influence on the parameters of visual-spatial task performance agrees with some studies [53, 54] and does not agree with others [23]. Starowicz-Filip et al. [23] reported an improvement in visual-spatial skills with age; however, patients’ remission period was the key component. It should be noted that healthy controls also lack age dynamics of task performance parameters (Table 3). In this regard, we can conclude that children of all ages can successfully cope with such a simple cognitive task of searching and counting only ten objects.
Conclusion
In the present study, we demonstrate the involvement of the cerebellum in saccadic system core functioning and visual perception in pediatric PFT survivors. Tumor and its treatment lead to cerebellar dysfunction, causing disorders of the visual-oculomotor system found in children of different age groups. Specifically, hypermetric saccades could be considered a prominent oculomotor symptom of cerebellar tumors. At the same time, later age of disease progression appears to correspond with lesser oculomotor deficits. The obtained data and the application of the eye tracking method provide theoretical and methodical basis for the diagnosis of cerebellar oncological diseases and evaluation of the effectiveness of rehabilitation measures that play an essential role in modern pediatric neurooncology.
Data Availability
Data are available on request.
Abbreviations
- PFT:
-
posterior fossa tumor
- ICARS:
-
International Cooperative Ataxia Rating Scale
- GH:
-
gaze holding task
- VGS:
-
visually guided saccade task
- VS:
-
visual search
- FP:
-
fixation point
- HC:
-
healthy controls
References
Leigh RJ, Zee DS. The neurology of eye movements. 5th ed. New York: Oxford University Press; 2015.
Beh SC, Frohman TC, Frohman EM, Biousse V, Galetta S. Cerebellar control of eye movements. J Neuroophthalmol. 2017;37:87–98. https://doi.org/10.1097/WNO.0000000000000456.
Rayner K, Castelhano MS. Eye movements during reading, scene perception, visual search, and while looking at print advertisements. In: Wedel M, Pieters R, editors. Visual marketing: From attention to action. Taylor & Francis Group/Lawrence Erlbaum Associates; 2008. p. 9–42.
Rolfs M, Schweitzer R. Coupling perception to action through incidental sensory consequences of motor behaviour. Nat Rev Psychol. 2022;1:112–23. https://doi.org/10.1038/s44159-021-00015-x.
Termsarasab P, Thammongkolchai T, Rucker JC, Frucht SJ. The diagnostic value of saccades in movement disorder patients: a practical guide and review. J Clin Mov Disord. 2015;2:14.
Christova P, Anderson JH, Gomez CM. Impaired eye movements in presymptomatic spinocerebellar ataxia type 6. Arch Neurol. 2008;65:530–6.
Stolze H, Klebe S, Petersen G, Raethjen J, Wenzelburger R, Witt K, et al. Typical features of cerebellar ataxic gait. J Neurol Neurosurg Psychiatry. 2002;73:310–2.
Buckley E, Mazzà C, McNeill A. A systematic review of the gait characteristics associated with cerebellar ataxia. Gait Posture. 2018;60:154–63.
Palliyath S, Hallett M, Thomas SL, Lebiedowska MK. Gait in patients with cerebellar ataxia. Mov Disord. 1998;13:958–64.
Cámara S, Fournier MC, Cordero P, et al. Neuropsychological profile in children with posterior fossa tumors with or without postoperative cerebellar mutism syndrome (CMS). Cerebellum. 2020;19:78–88. https://doi.org/10.1007/s12311-019-01088-4.
Crowdy KA, Kaur-Mann D, Cooper HL, Mansfield AG, Offord JL, Marple-Horvat DE. Rehearsal by eye movement improves visuomotor performance in cerebellar patients. Exp Brain Res. 2002;146:244–7.
Aizenshtein A, Shurupova M, Shipilov A, Latanov A, Skvortsov D. Kasatkin V. Diagnostics of ataxia in children who survived cerebellar tumor: the relationship between parameters of tandem gait, saccadic system and postural stability. In: Velichkovsky BM, Balaban PM, Ushakov VL, editors. Advances in cognitive research, artificial intelligence and neuroinformatics, Intercognsci 2020. Advances in intelligent systems and computing, vol. 1358. Cham: Springer. https://doi.org/10.1007/978-3-030-71637-0_70.
Cogan DG. Ocular dysmetria; flutter-like oscillations of the eyes, and opsoclonus. AMA Arch Ophthalmol. 1954;51(3):318–35. https://doi.org/10.1001/archopht.1954.00920040324006.
Selhorst JB, Stark L, Ochs AL, Hoyt WF. Disorders in cerebellar ocular motor control. I. Saccadic overshoot dysmetria. An oculographic, control system and clinico-anatomical analysis. Brain. 1976;99(3):497–508. https://doi.org/10.1093/brain/99.3.497.
Selhorst JB, Stark L, Ochs AL, Hoyt WF. Disorders in cerebellar ocular motor control. II. Macrosaccadic oscillation. An oculographic, control system and clinico-anatomical analysis. Brain. 1976;99(3):509–22. https://doi.org/10.1093/brain/99.3.509.
Isotalo E, Niemelä M, Pyykkö I, Summanen P. Hemangioblastoma and oculomotor pathology. Acta Otolaryngol Suppl. 1997;529:119–22. https://doi.org/10.3109/00016489709124100.
Wennmo C, Hindfelt B, Pyykkö I. Eye movements in cerebellar and combined cerebellobrainstem diseases. Ann Otol Rhinol Laryngol. 1983;92(2 Pt 1):165–71. https://doi.org/10.1177/000348948309200214.
Golla H, Tziridis K, Haarmeier T, Catz N, Barash S, Thier P. Reduced saccadic resilience and impaired saccadic adaptation due to cerebellar disease. Eur J Neurosci. 2008;27(1):132–44. https://doi.org/10.1111/j.1460-9568.2007.05996.x.
Oh AJ, Chen T, Shariati MA, Jehangir N, Hwang TN, Liao YJ. A simple saccadic reading test to assess ocular motor function in cerebellar ataxia. PloS One. 2018;13(11):e0203924. https://doi.org/10.1371/journal.pone.0203924.
Ostrom QT, Gittleman H, Liao P, Rouse C, Chen Y, Dowling J, Wolinsky Y, Kruchko C, Barnholtz-Sloan J. CBTRUS statistical report: primary brain and central nervous system tumors diagnosed in the United States in 2007-2011. Neuro Oncol. 2014;16(Suppl 4):iv1–63. https://doi.org/10.1093/neuonc/nou223.
Phillips CA, Barakat LP, Pollock BH, Bailey LC, Beidas RS. Implementation science in pediatric oncology: a narrative review and future directions. Pediatr Blood Cancer. 2022;69(4):e29579. https://doi.org/10.1002/pbc.29579.
Schmahmann JD, Sherman JC. The cerebellar cognitive affective syndrome. Brain. 1998;121:561–79.
Starowicz-Filip A, Chrobak AA, Milczarek O, Kwiatkowski S. The visuospatial functions in children after cerebellar low-grade astrocytoma surgery: a contribution to the pediatric neuropsychology of the cerebellum. J Neuropsychol. 2017;11(2):201–21. https://doi.org/10.1111/jnp.12093.
Schmahmann JD, Guell X, Stoodley CJ, Halko MA. The theory and neuroscience of cerebellar cognition. Annu Rev Neurosci. 2019;8(42):337–64. https://doi.org/10.1146/annurev-neuro-070918-050258.
Einarsson EJ, Patel M, Petersen H, Wiebe T, Magnusson M, Moëll C, Fransson PA. Oculomotor deficits after chemotherapy in childhood. PloS One. 2016;11(1):e0147703. https://doi.org/10.1371/journal.pone.0147703.
Davis EE, Pitchford NJ, Jaspan T, McArthur D, Walker D. Development of cognitive and motor function following cerebellar tumor injury sustained in early childhood. Cortex. 2010;46(7):919–32. https://doi.org/10.1016/j.cortex.2009.10.001.
Kasatkin V, Deviaterikova A, Shurupova M, Karelin A. The feasibility and efficacy of short-term visual-motor training in pediatric posterior fossa tumor survivors. Eur J Phys Rehabil Med. 2022;58(1):51–9. https://doi.org/10.23736/S1973-9087.21.06854-4.
Trouillas P, Takayanagi T, Hallett M, Currier RD, Subramony SH, Wessel K, Bryer A, Diener HC, Massaquoi S, Gomez CM, Coutinho P, Ben Hamida M, Campanella G, Filla A, Schut L, Timann D, Honnorat J, Nighoghossian N, Manyam B. International cooperative ataxia rating scale for pharmacological assessment of the cerebellar syndrome. The Ataxia Neuropharmacology Committee of the World Federation of Neurology. J Neurol Sci. 1997;145(2):205–11. https://doi.org/10.1016/s0022-510x(96)00231-6.
Kieffer V, Longaud A, Callu D, Laroussinie F, Viguier D, Grill J, Dellatolas G. Teachers’ report of learning and behavioural difficulties in children treated for cerebellar tumours. Brain Inj. 2012;26(7-8):1014–20. https://doi.org/10.3109/02699052.2012.661116.
Ohad, G. Fit_Ellipse. MATLAB central file exchange. Available online: https://www.mathworks.com/matlabcentral/fileexchange/3215-fit_ellipse (Accessed on 5 May 2022).
Nguyen NP, Sallah S, Karlsson U, Antoine JE. Combined chemotherapy and radiation therapy for head and neck malignancies: quality of life issues. Cancer. 2002;94(4):1131–41. https://doi.org/10.1002/cncr.10257.
Manto M, Bower JM, Conforto AB, Delgado-García JM, da Guarda SN, Gerwig M, Habas C, Hagura N, Ivry RB, Mariën P, Molinari M, Naito E, Nowak DA, Oulad Ben Taib N, Pelisson D, Tesche CD, Tilikete C, Timmann D. Consensus paper: roles of the cerebellum in motor control--the diversity of ideas on cerebellar involvement in movement. Cerebellum. 2012;11(2):457–87. https://doi.org/10.1007/s12311-011-0331-9.
Arnold DB, Robinson DA. The oculomotor integrator: testing of a neural network model. Exp Brain Res. 1997;113(1):57–74. https://doi.org/10.1007/BF02454142.
Büttner U, Grundei T. Gaze-evoked nystagmus and smooth pursuit deficits: their relationship studied in 52 patients. J Neurol. 1995;242:384–9.
Ygge J, Aring E, Han Y, Bolzani R, Hellström A. Fixation stability in normal children. Ann N Y Acad Sci. 2005;1039:480–3. https://doi.org/10.1196/annals.1325.049.
Aring E, Grönlund MA, Hellström A, Ygge J. Visual fixation development in children. Graefes Arch Clin Exp Ophthalmol. 2007;245(11):1659–65. https://doi.org/10.1007/s00417-007-0585-6.
Armstrong GT. Long-term survivors of childhood central nervous system malignancies: the experience of the Childhood Cancer Survivor Study. Eur J Paediatr Neurol. 2010;14(4):298–303. https://doi.org/10.1016/j.ejpn.2009.12.006.
Mulhern RK, Merchant TE, Gajjar A, Reddick WE, Kun LE. Late neurocognitive sequelae in survivors of brain tumours in childhood. Lancet Oncol. 2004;5(7):399–408. https://doi.org/10.1016/S1470-2045(04)01507-4.
Robinson FR, Fuchs AF. The role of the cerebellum in voluntary eye movements. Annu Rev Neurosci. 2001;24:981–1004. https://doi.org/10.1146/annurev.neuro.24.1.981.
Goffart L, Chen LL, Sparks DL. Saccade dysmetria during functional perturbation of the caudal fastigial nucleus in the monkey. Ann N Y Acad Sci. 2003;1004:220–8. https://doi.org/10.1196/annals.1303.019.
Swartz BE, Li S, Bespalova I, Burmeister M, Dulaney E, Robinson FR, Leigh RJ. Pathogenesis of clinical signs in recessive ataxia with saccadic intrusions. Ann Neurol. 2003;54(6):824–8. https://doi.org/10.1002/ana.10758.
Alexandre MF, Rivaud-Péchoux S, Challe G, Durr A, Gaymard B. Functional consequences of oculomotor disorders in hereditary cerebellar ataxias. Cerebellum. 2013;12(3):396–405. https://doi.org/10.1007/s12311-012-0433-z.
Eggert T, Straube A. Saccade variability in healthy subjects and cerebellar patients. Prog Brain Res. 2019;249:141–52. https://doi.org/10.1016/bs.pbr.2019.03.021.
Irving EL, Steinbach MJ, Lillakas L, Babu RJ, Hutchings N. Horizontal saccade dynamics across the human life span. Invest Ophthalmol Vis Sci. 2006;47(6):2478–84. https://doi.org/10.1167/iovs.05-1311.
Gaertner C, Wiener-Vacher S, Kapoula Z. Up/down anisotropies of vertical saccades in healthy children depending on the mode and the depth of execution. Int J Dev Neurosci. 2016;52:82–92. https://doi.org/10.1016/j.ijdevneu.2016.04.003.
Hopf S, Liesenfeld M, Schmidtmann I, Ashayer S, Pitz S. Age dependent normative data of vertical and horizontal reflexive saccades. PloS One. 2018;13(9):e0204008. https://doi.org/10.1371/journal.pone.0204008.
Munoz DP, Broughton JR, Goldring JE, Armstrong IT. Age-related performance of human subjects on saccadic eye movement tasks. Exp Brain Res. 1998;121:391–400. https://doi.org/10.1007/s002210050473.
Zihl J. Visual scanning behavior in patients with homonymous. Neuropsychologia. 1995;33(3):287–303. https://doi.org/10.1016/0028-3932(94)00119-a.
O'Halloran CJ, Kinsella GJ, Storey E. The cerebellum and neuropsychological functioning: a critical review. J Clin Exp Neuropsychol. 2012;34(1):35–56. https://doi.org/10.1080/13803395.2011.614599.
Baillieux H, De Smet HJ, Dobbeleir A, Paquier PF, De Deyn PP, Mariën P. Cognitive and affective disturbances following focal cerebellar damage in adults: a neuropsychological and SPECT study. Cortex. 2010;46(7):869–79. https://doi.org/10.1016/j.cortex.2009.09.002.
Andersen RA, Snyder LH, Bradley DC, Xing J. Multimodal representation of space in the posterior parietal cortex and its use in planning movements. Annu Rev Neurosci. 1997;20:303–30. https://doi.org/10.1146/annurev.neuro.20.1.303.
Litvinova AS, Ratmanova PO, Evina EI, Bogdanov RR, Kunitsyna AN, Napalkov DA. Age-related changes in saccadic eye movements in healthy subjects and patients with Parkinson’s disease. Fiziol Cheloveka. 2011;37(2):40–7. Russian
Levisohn L, Cronin-Golomb A, Schmahmann JD. Neuropsychological consequences of cerebellar tumour resection in children: cerebellar cognitive affective syndrome in a paediatric population. Brain. 2000;123(Pt 5):1041–50. https://doi.org/10.1093/brain/123.5.1041.
Steinlin M, Imfeld S, Zulauf P, Boltshauser E, Lövblad KO, Ridolfi Lüthy A, Perrig W, Kaufmann F. Neuropsychological long-term sequelae after posterior fossa tumour resection during childhood. Brain. 2003;126(Pt 9):1998–2008. https://doi.org/10.1093/brain/awg195.
Acknowledgements
The authors would like to thank the head of the Clinical Rehabilitation Research Center “Russkoe Pole,” Alexander Karelin, and the head of the Neurocognitive Department, Vladimir Kasatkin, for supporting this study, as well as Alexander Myasnikov for careful reading of the manuscript.
Author information
Authors and Affiliations
Contributions
Conceptualization: M.S. and A.L.; methodology: M.S. and A.L.; software: M.S.; validation: A.L.; formal analysis: M.S. and A.L.; investigation: M.S.; resources: M.S.; data curation: M.S. and A.L.; writing—original draft preparation: M.S.; writing—review and editing: A.L.; visualization: M.S.; supervision: A.L.; project administration: M.S and A.L. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Ethics Approval
All procedures were approved by the ethics committee of Dmitry Rogachev National Research Center of Pediatric Hematology, Oncology, and Immunology (protocol number 8e/13-17 of 27.10.2017) and were run according to the Declaration of Helsinki. The parents of our patients provided written informed consent.
Consent to Participate
Informed consent was obtained from legal guardians. Written informed consent was obtained from all participants over the age of 15 or from their legal representatives in the case of younger participants. A copy of the consent form is available for review by the editor of this journal.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shurupova, M.A., Latanov, A.V. Oculomotor Impairments in Children After Posterior Fossa Tumors Treatment. Cerebellum 23, 444–454 (2024). https://doi.org/10.1007/s12311-023-01553-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12311-023-01553-1