Abstract
Tension-free repairs are performed commonly in inguinal hernia operations. The objective of the present study is to compare the outcomes of three different tension-free repair methods known as Lichtenstein, Rutkow–Robbins, and Gilbert double layer. One-hundred and fifty patients diagnosed with inguinal hernia were randomly split into three groups. The comparisons across groups were carried out in terms of operation length, postoperative pain, femoral vein flow velocity, early and late complications, recurrence rates, length of hospital stay, time required to return to work, and cost analysis. No difference was found between the groups regarding age, gender, type and classification of hernia, postoperative pain, and late complications (p > 0.05). Operation length was 53.70 ± 12.32 min in the Lichtenstein group, 44.29 ± 12.37 min in the Rutkow–Robbins group, and 45.21 ± 14.36 min in the Gilbert group (p < 0.05). Mean preoperative and postoperative femoral vein flow velocity values were 13.88 ± 2.237 and 13.42 ± 2.239 cm/s for Lichtenstein group, 12.64 ± 2.98 and 12.16 ± 2.736 cm/s for Rutkow–Robbins group, and 16.02 ± 3.19 and 15.52 ± 3.358 cm/s for the Gilbert group, respectively. Statistical difference was found between all the groups (p < 0.001). However, no difference was determined between the groups regarding the decrease rates (p = 0.977). Among early complications, hematoma was observed in one (2 %) patient of Lichtenstein group, five (10 %) patients of Rutkow–Robbins group, and three (6 %) patients of Gilbert group (p = 0.033). Cost analysis produced the following results for Lichtenstein, Rutkow–Robbins, and Gilbert groups: US $157.94 ± 50.05, $481.57 ± 11.32, and $501.51 ± 73.59, respectively (p < 0.001). Lichtenstein operation was found to be more advantageous compared with the other techniques in terms of cost analysis as well as having unaffected femoral blood flow. Therefore, we believe that Lichtenstein repair is still the most appropriate surgical option in patients diagnosed with inguinal hernia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Approximately 12,000 hernia operations are performed in Finland, whereas 80,000 and 800,000 are conducted in England and USA, respectively. Although the exact prevalence is still unknown, its prevalence among men is around 4–7 % [1]. As people get older, hernia incidence, strangulation frequency, and length of hospital stay exhibit rises [2]. While the underlying etiology has not been understood yet, processus vaginalis patency, genetic inheritance, and erect posture are held responsible for its development [3].
Currently, hernia is treated with surgery. Hernia surgeries comprise 10–15 % of all general surgery procedures [4]. In terms of recurrence and complication rates, tension-free repairs are the most commonly preferred operative techniques. Lichtenstein method and it’s modifications such as Gilbert and Rutkow–Robbins are known to be tension-free anterior approaches which have been found to produce considerably low recurrence and complication rates [5, 6]. Moreover, the fact that those operations can also be performed under local anesthesia instead of general or spinal anesthesia provides yet another advantage. In the present study, we aimed to compare the Lichtenstein technique with Rutkow–Robbins and Gilbert double layer techniques in inguinal hernia repair with regard to operation length, postoperative pain, femoral vein flow velocity, early and late complications, recurrence rates, length of hospital stay, time required to return to work, and cost analysis.
Materials and Methods
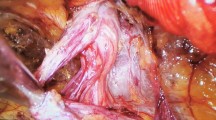
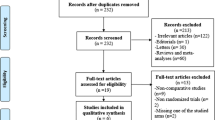
Following the approval of the institutional ethics committee, the study was conducted on 150 patients admitted to the General Surgery Department of Ankara University and General Surgery Department of Bartin State Hospital. One hundred and fifty cases were operated with a minimum of 4 years maximum duration of 9 years follow-up period between January 2000 and July 2005. The patients were randomly allocated to three groups as to include 50 individuals in each (simple randomization was used in this study as a method of randomization, throwing heads or tails). While Lichtenstein operation was performed in the first group, Rutkow–Robbins was performed on patients of the second group, and Gilbert double layer was applied in the third group. The cases with coexisting systemic diseases, such as immune system deficiency, diabetes mellitus, cirrhosis, as well as Gilbert type 7 and 8 hernia, were excluded from the study [7]. All the patients’ hemogram count, liver function tests, renal function tests, EKG, chest radiography, and pre-operative coagulation were performed. In Lichtenstein method, polypropylene mesh of 6 × 11 cm size was fixed inferiorly to the ligamentum inguinale and superiorly to the fascia transversalis with a 2/0 polypropylene suture. While applying Rutkow–Robbins onlay method, premade Rutkow plug hernia sac was prepared and placed into the abdomen before being sutured to the internal ring on which the onlay graft was fixed inferiorly to the ligamentum inguinale and superiorly to the fascia transversalis with a 2/0 polypropylene suture. In double layer Gilbert repair, for direct and indirect hernias, hernial sac was prepared and the lower layer of the graft was placed into the Bougras area by descending down to the Cooper ligament. Upper layer was fixed inferiorly to the ligamentum inguinale and superiorly to the fascia transversalis with a 2/0 polypropylene suture. We have applied drain with suspected cases of bleeding. Postoperatively, the patients were evaluated in terms of drain placement, early and late complications, and recurrence rates within 1 year. Preoperative pains of the cases were assessed at 1, 7, and 30 days with visual analog scale. In order to evaluate the changes in the femoral vein flow, patients were subjected to bilateral femoral vein Doppler US preoperatively, and a repeat Doppler US was performed postoperatively at 1 month. Cost analysis included bed charges, preoperative and postoperative drugs, and consumable materials used during the anesthesia and operation.
Statistical Analysis
Kolmogorov–Smirnov test was used to evaluate whether the distribution of variables were normal. Therefore, one-way ANOVA was used to compare the age, BMI, time, and work-off periods among Lichtenstein, Rutkow–Robbins, and Gilbert groups, besides used to compare the Doppler results among same groups separately for preop and postop terms. Kruskal–Wallis analysis of variance was used to compare the hospitalization time and cost effectivity among Lichtenstein, Rutkow–Robbins, and Gilbert groups, besides used to compare the VAS results among same groups separately for first, seventh, and 30th days. Friedman analysis of variance was comparing the VAS values among first, seventh, and 30th days separately for Lichtenstein, Rutkow–Robbins, and Gilbert groups. Two related sample t test was used to compare the Doppler results between preop and postop terms separately for Lichtenstein, Rutkow–Robbins, and Gilbert groups. Repeated measures two-way ANOVA test was used to analyze the difference of Doppler results (preop–postop) among Lichtenstein, Rutkow–Robbins, and Gilbert groups. Pearson’s chi-square test was used to compare the categorical variables among three groups. The continuous variables were presented as the mean and standard deviation. The categorical variables were presented as the count and percentage. A p value <0.05 was considered significant. Analyses were performed using commercial software (SPSS 16.0 demo).
Results
None of the three methods showed a statistically significant difference regarding age, gender, hernia type, and hernia distribution based on the modified Gilbert classification (p > 0.05) (Table 1). Body mass index assessment was 26.448 ± 4.94 in the Lichtenstein group, 25.078 ± 3.71 in the Rutkow–Robbins group, and 24.22 ± 2.71 in the Gilbert group. There was a statistically significant difference between the groups (p = 0.012) (Table 1).
While 75 (50 %) of 150 patients were operated on under local anesthesia, 49 (32.7 %) and 26 (17.3 %) of them were operated on under spinal anesthesia and general anesthesia, respectively. In Lichtenstein group, 25 (50 %) patients were operated on under local anesthesia, whereas 15 (30 %) and ten (20 %) were operated on under spinal and general anesthesia, respectively. Among the individuals in Rutkow–Robbins group, 28 (56 %) were operated on under local anesthesia, while 12 (24 %) and ten (20 %) were subjected to spinal and general anesthesia, respectively. In Gilbert group, 22 (44 %) patients were operated on under local anesthesia, whereas 20 (40 %) and eight (16 %) were subjected to spinal and general anesthesia, respectively. No statistical difference was found relative to the applied anesthesia method (p = 0.791) (Table 1).
Operation length was 51.70 ± 12.32 min in the Lichtenstein group, 50.29 ± 12.37 min in the Rutkow–Robbins group, and 60.21 ± 14.36 min in the Gilbert group. There was a statistically significant difference between the groups regarding operation lengths (p < 0.05) (Table 1).
Drain was used in 15 (10 %) patients in total. Drain was applied to eight (16 %) patients in Lichtenstein group, whereas three (6 %) and four (8 %) patients in the Rutkow–Robbins and Gilbert groups. There was no statistically significant difference between the groups (p = 0.22) (Table 1).
Visual analog scale values at day 1 were 1.52 ± 1.26 for Lichtenstein group, 1.92 ± 1.08 for Rutkow–Robbins group, and 2.32 ± 1.84 for Gilbert group, whereas visual analog scale values at day 7 were 0.68 ± 1.03 for Lichtenstein group, 0.80 ± 0.95 for Rutkow–Robbins group, and 1.0 ± 1.52 for Gilbert group. Visual analog scale results at 30 days were 0.16 ± 0.55 in the Lichtenstein group, 0.08 ± 0.27 in the Rutkow–Robbins group, and 0.28 ± 0.73 in the Gilbert group. No statistically significant difference was determined for any of the groups at 1, 7, and 30 days (p = 0.135, p = 0.740, p = 0.562, respectively) (Table 2).
None of the patients demonstrated a urinary retention in the postoperative early period follow-up. Postoperative hematoma was observed in nine (6 %) patients in total. While there was only one (2 %) hematoma case in the Lichtenstein group, five (10 %) and three (6 %) patients exhibited hematoma in the Rutkow–Robbins and Gilbert groups, respectively (p = 0.033). None of the patients showed early period superficial incisional surgical site infection, deep incisional surgical site infection, organ-space infection. Moreover, none of the patients displayed an early period recurrence.
Late period follow-ups of the patients revealed 16 (10.66 %) cases with numbness in the incision sites and medial aspect of thighs. This complication was determined in five (10 %) patients in the Lichtenstein group, four (8 %) patients in the Rutkow–Robbins group, and seven (14 %) patients in the Gilbert group. However, no statistically significant difference was found between the groups (p = 0.896). None of the patients exhibited a recurrence within the follow-up period.
In the Lichtenstein group, mean preoperative femoral vein flow velocity and postoperative femoral vein flow velocity were 13.88 ± 2.237 and 13.42 ± 2.239 cm/s, respectively (p > 0.001). In the Rutkow–Robbins group, mean preoperative femoral vein flow velocity and postoperative femoral vein flow velocity were 12.64 ± 2.98 and 12.16 ± 2.736 cm/s, respectively (p < 0.001). In the Rutkow–Robbins group, mean preoperative femoral vein flow velocity and postoperative femoral vein flow velocity were 16.02 ± 3.19 and 15.52 ± 3.358 cm/s, respectively (p < 0.001) (Table 3).
Length of hospital stay was 2.08 ± 0.70 days in the Lichtenstein group, whereas 2.12 ± 0.78 and 2.13 ± 0.78 days in the Rutkow–Robbins and Gilbert groups, respectively. However, there was no statistically significant difference between the groups (p = 0.939) (Table 1).
Time required to return to work was 23.60 ± 2.53 days in the Lichtenstein group, while it was 25.12 ± 2.08 and 24.61 ± 2.80 days in the Rutkow–Robbins and Gilbert groups, respectively. However, no statistically significant difference was determined across the groups (p = 0.084) (Table 1).
According to the cost analysis, Lichtenstein repair was found to cost US $157.94 ± 50.05, whereas Rutkow–Robbins and Gilbert operations were determined to cost US $481.57 ± 11.32 and 501.51 ± 73.59 in total, respectively. There was a statistically significant difference between the groups (p < 0.001) (table for costs).
Discussion
Inguinal hernia operations are still one of the most commonly encountered procedures in the lifetime of a general surgeon. While it is seen frequently, it is generally considered as a simple operation, but its anatomical planes are complicated [8]. Although surgical treatment dates back to considerably old times, modern surgical treatment is recognized to begin with Bassini [9]. In hernia surgery, the best indicator of the success of the operation is the recurrence which is totally based on objective criteria. While recurrence rates in tension operations of inguinal hernia vary depending on the applied method, it is reported to be about 5–10 % among primary cases and 5–30 % in cases of recurrence[10–12]. Currently, the success of Shouldice operation, which has been studied on large series and has become a gold standard with low recurrence rates, cannot be repeated universally [13]. The common target in tension-free inguinal hernia repairs is to apply a totally tension-free support with a reliable prosthetic material implantation and to achieve long-term reinforcement of posterior wall of inguinal hernia or possible hernia sites. Currently, particularly the recurrences at early period (first 2 years) are recognized to arise from the tension of the suture line [10, 12]. First, physicians tried to use relaxing incision, but then it was found to have no effect over the problem. The idea to totally and permanently reinforce the posterior wall of the inguinal canal has become popular with Lichtenstein[14, 15]. Lichtenstein reported a 0 % recurrence rate in his study (1989) in which 1,000 cases were treated with onlay method, and the study received both negative and positive criticism worldwide [14–16]. The results obtained by other clinics that apply the Lichtenstein onlay method show consistency with the results of Lichtenstein [17].
Recurrences after inguinal hernia repairs are categorized in two groups as early (mechanic, within first postoperative 2 years) and late (metabolic, many years after the operation) period recurrences. While the tension in the reinforced line is held responsible for the early recurrences, disruptions in the collagen metabolism of transverse fascia and similar structures are held accountable for late recurrences [18, 19]. Several complications have been reported in the literature (although not frequently) for Rutkow–Robbins procedures due to less dissection such as orchitis and nerve damage. It is possible disadvantages are pubic recurrence because of applying a graft that does not run over the pubis and problems about reinforcement of the posterior wall due to shrinkage of the unsutured onlay graft. In the present study, hematoma was observed in the patients as an early complication. No other early period complications were found. Hematoma showed the highest incidence in the Rutkow–Robbins group and the lowest in the Lichtenstein group. We believe that the reason behind that significant difference was the higher amount of drain usage among patients of Lichtenstein group. The most common complication in the late period follow-up of the patients was numbness in the surgical incision site and medial portion of the thigh. Isemer et al. determined the incidence of numbness in the thigh area as 2.4 % after Rutkow–Robbins operation [20]. Forte et al. conducted a study and following Lichtenstein operation, the incidence of numbness in the thigh area was found to be 4.3 % [21]. In our series, 14 (9.33 %) patients showed this complication in total. Five (10 %) patients in the Lichtenstein group displayed this complication, whereas four (8 %) and five (10) patients showed it in the Rutkow–Robbins and Gilbert groups, respectively. However, no significant difference was found between the groups.
As known, the length of operation depends on many factors such as surgeon’s experience, obesity, and use of premade mesh. Therefore, various studies report different operation lengths. While Zeybek et al. report the mean length of operation as 48 min, Karatepe et al. report that length as 50 min [22, 23]. However, Janu P.G. et al. performed a study by applying Lichtenstein method and found the mean operation length as 111 ± 2 min. Isemer et al. conducted Rutkow–Robbins operations in which the mean operation length was 37.8 ± 15.85 min [19, 20]. Turculet et al. carried out Gilbert double layer operations among which the mean operation length was 65 min [24]. In the present study, our results were consistent with the literature. The operation length of Gilbert group was found to be longer than those of Rutkow–Robbins and Lichtenstein groups. However, the mean length in Rutkow–Robbins group was lower than that of Lichtenstein group. We believe that higher BMI index of Lichtenstein group may be the reason behind this difference.
Gilbert double layer repair differs from the other two techniques with longer operation length and higher intraoperative pain in operations under local anesthesia [25]. In light of the results of our study that includes a limited number of cases, we believe that spinal anesthesia may be a better choice instead of local anesthesia in Gilbert double layer operations. However, patients subjected to Lichtenstein repair under local anesthesia are reported to suffer less postoperative pain and earlier mobilization [26].
Femoral venous blood flows were measured with Doppler USG both preoperatively and postoperatively in all the groups, and statistically significant decrease was determined across the groups. However, regarding the reduction rates of venous blood flows, none of the groups displayed a statistically significant difference. In a previous study performed by Rutkow–Robbins, femoral compression was found in four patients [5]. In the current study, we found no compression or occlusion among our patients.
Regarding length of hospital stay, C. S. Huang et al. conducted a study and compared the patients treated with Prolene and plug in which the hospital stay was found to be 1.31 + 1.00 days for Prolene patients and 1.45 ± 1.43 for plug patients [27]. Isemer et al. determined the length of hospital stay as 2.09 ± 1.35 [20]. In the present study, our results showed consistency with the literature.
The length of time required to return to work depends on the applied mesh and operation technique as well as the motivation for recovery alongside socioeconomic and cultural level of the patient. Therefore, while determining the time required to return to work, evaluating patient’s ability to walk and work out along with the assessment of driving time may be more appropriate. In a previous study, the time required to return to work has been associated with annual income and the level of social security premiums. Duration of postoperative pain and the time required to return to work have been found to be longer in the worker’s compensation group than in the commercial insurance group [28]. Isemer et al. found the time required to return to work as 15.3 ± 12.42 days in their study [23]. In a study conducted by Sven Bringman et al., it was 16.5 days in the group treated with Prolene, whereas 16 days in the Vypro group [29]. Return to work takes longer in our country due to sociocultural reasons.
In the past, postoperative pain following tension repairs was an important and a frequently encountered problem. Particularly after tension-free operations performed with mesh, postoperative pain, return to normal activity, and chronic pain incidence have been found to display decreases [30]. While E. Prieto-Díaz-Chávez et al. reported more frequent and prolonged analgesic usage in the conventional hernioplasty than in tension-free operations, on the contrary, another study underscored the absence of difference between the aforementioned two groups[31, 32]. The factors leading to postoperative pain after inguinal hernia repair have been investigated in the previous studies, and while applied surgical technique, gender, direct or indirect nature of hernia have been found be important, the occupation of patients has been found to have no influence. However, postoperative pain incidence has been found to be higher among young people [33, 34]. It is commonly encountered as a result of the nerve entrapment caused by the mesh. It is seen in 12 % of patients. Ilioinguinal nerve entrapment causes pain in the hernia region and scrotum. Injuries across the genital branches of genitofemoral nerve generate hypersensitivity over the inguinal area [35]. In the current study, according to the results based on visual analog scale, there was no statistically significant difference between the three groups at days 1, 7, and 30 with regard to postoperative pain.
In terms of cost analysis, there was no statistically significant difference regarding the length of hospital stay and the applied anesthesia. Therefore, the most influential factor in cost analysis is the cost of the graft. That is why Lichtenstein group was found to have a significantly low cost.
In conclusion, our study presented a randomized comparison of three homogenous series published by different hernia centers. We believe that Lichtenstein operation is more advantageous than others due to cost as well as having no influence over the femoral blood flow. Therefore, Lichtenstein technique is recognized as the most advantageous method in inguinal hernia repairs. We believe that this conclusion will be solidified by future studies including larger series.
References
Paajanen H (2007) A single-surgeon randomized trial comparing three composite meshes on chronic pain after Lichtenstein hernia repair in local anesthesia. Hernia 11:335–339
Rutkow IM (1998) Epidemiologic, economic and sociologic aspects of hernia surgery in the United States in the 1990’s. Surg Clin North Am 78:941–951
Abrahamson J (1998) Etiology and pathophysiology of primary and recurrent groin hernia formation. Surg Clin North Am 78:953–972
Schumpelick V, Treutner KH, Arlt G (1994) Inguinal hernia repair in adults. Lancet 344:375–379
Rutkow IM, Robbins AW (1993) “Tension-free” inguinal herniorraphy: a preliminary report on the “mesh-plug” technique. Surgery 114:3–8
Gilbert AI, Graham MF, Voigt WJ (1999) A bilayer patch device for inguinal hernia repair. Hernia 3:161–166
Gilbert AI (1989) An anatomic and functional classification for the diagnosis and treatment of inguinal hernia. Am J Surg 157:331–333
Read RC (1996) Hernia. In: Zuidema GD (ed) Shackelford’s surgery of the alimentary tract, vol: 5. WB Saunders, Philadelphia, pp 93–226, Stedman’s medical dictionary 1982
Bendavid R (1989) New techniques in hernia repair. World J Surg 13:522–531
Stoppa RE, Diarra B, Mertl P (1997) The retroperitoneal spermatic sheath: an anatomic structure of surgical interest. Hernia 1:55–59
Than VK, Putz T, Rohde H (1992) A randomized controlled trial for inguinal hernia repair to compare the Shouldice and the Bassini–Kirshner operation. Int Surg 77:235–237
Panos RG, Beck DE, Maresh JE, Harford FJ (1992) Preliminary results of a prospective randomized study of Cooper’s ligament versus Shouldice herniography technique. Surg Gynecol Obstet 175:315–319
Shulman AG, Amid PK, Lichtenstein IL (1995) A survey of non-expert surgeons using the open tension-free mesh patch repair for primary inguinal hernias. Int Surg 80:35–36
Lichtenstein IL, Schulman AG, Amid PK, Montllor MM (1989) The tension-free hernioplasty. Am J Surg 157:188–193
Bailey IS, Karran SE, Toyn K, Brough P, Ranaboldo C, Karrn SJ (1992) Community surveillance of complications after hernia surgery. BMJ 304:469–471
Lichtenstein IL, Shulman AG, Amid PK (1993) The cause, prevention, and treatment of recurrent groin hernia. Surg Clin North Am 73:529–544
Nyhus LM (1993) Individualization of hernia repair: a new era. Surgery 114:1–2
Rutkow IM, Robbins AW (1998) The mesh plug technique for recurrent groin herniorraphy: an nine-year experience of 407 repairs. Surgery 124:844–847
Janu PG, Sellers KD, Mangiante EC (1997) Mesh inguinal herniorraphy: a ten year review. Am Surg 63:1065–1071
Isemer FE, Dathe V, Peschka B, Heinze R, Radke A (2004) Rutkow PerFix-plug repair for primary and recurrent inguinal hernias—a prospective study. Surg Technol Int 12:129–136
Forte A, D’Urso A, Gallinaro LS, Lo Storto G, Bosco MR, Vietri F, Beltrami V (2002) Complications of inguinal hernia repair. G Chir 23:88–92
Zeybek N, Tas H, Peker Y, Yildiz F, Akdeniz A, Tufan T (2008) Comparison of modified darn repair and Lichtenstein repair of primary inguinal hernias. J Surg Res 146:225–229
Karatepe O, Adas G, Battal M, Gulcicek OB, Polat Y, Altiok M, Karahan S (2008) The comparison of preperitoneal and Lichtenstein repair for incarcerated groin hernias: a randomised controlled trial. Int J Surg 6:189–192
Turculet C, Feodor T, Dinescu G, Petrică R, Rădulescu S, Beuran M (2007) Bi-layer hernioplasty in day surgery. Chirurgia (Bucur) 102:433–438
van Veen RN, Mahabier C, Dawson I, Hop WC, Kok NF, Lange JF, Jeekel J (2008) Spinal or local anesthesia in Lichtenstein hernia repair: a randomized controlled trial. Ann Surg 247:428–433
Gultekin FA, Kuruahvecioglu O, Karamercan A, Ege B, Ersoy E, Tatlicioglu E (2007) A prospective comparison of local and spinal anesthesia for inguinal hernia repair. Hernia 11:153–156
Huang CS, Huang CC, Lien HH (2005) Prolene hernia system compared with mesh plug technique: a prospective study of short- to mid-term outcomes in primary groin hernia repair. Hernia 9:167–171
Salcedo-Wasicek MC, Thirlby RC (1995) Postoperative course after inguinal herniorrhaphy. A case-controlled comparison of patients receiving workers’ compensation vs patients with commercial insurance. Arch Surg 130:29–32
Bringman S, Heikkinen TJ, Wollert S, Osterberg J, Smedberg S, Granlund H, Ramel S, Fellander G, Anderberg B (2004) Early results of a single-blinded, randomized, controlled, Internet-based multicenter trial comparing Prolene and Vypro II mesh in Lichtenstein hernioplasty. Hernia 8:127–134
Stephenson BM (2003) Complications of open groin hernia repair. Surg Clin North Am 83:1255–1278
Prieto-Díaz-Chávez E, Medina-Chávez JL, González-Ojeda A, Coll-Cárdenas R, Uribarren-Berrueta O, Trujillo-Hernández B, Vásquez C (2005) Tension-free hernioplasty versus conventional hernioplasty for inguinal hernia repair. Surg Today 35:1047–1053
Vrijland WW, van den Tol MP, Luijendijk RW, Hop WC, Busschbach JJ, de Lange DC et al (2002) Randomized clinical trial of non-mesh versus mesh repair of primary inguinal hernia. Br J Surg 89:293–297
Page B, Paterson C, Young D, O’Dwyer PJ (2002) Pain from primary inguinal hernia and the effect of repair on pain. Br J Surg 89:1315–1318
Lau H, Lee F (2001) Determinant factors of pain after ambulatory inguinal herniorrhaphy: a multiple-variate analysis. Hernia 5:17–20
Ziprin P, Williams P, Foster ME (1999) External oblique aponeurosis nerve entrapment as a cause of groin pain in the athlete. Br J Surg 80:566–568
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Karaca, A.S., Ersoy, O.F., Ozkan, N. et al. Comparison of Inguinal Hernia Repairs Performed with Lichtenstein, Rutkow–Robbins, and Gilbert Double Layer Graft Methods. Indian J Surg 77, 28–33 (2015). https://doi.org/10.1007/s12262-013-0809-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12262-013-0809-4