Abstract
In response to hypoxia, tissues have to implement numerous mechanisms to enhance oxygen delivery, including the activation of angiogenesis. This work investigates the angiogenic response of the hypoxic caudate putamen after several recovery times.
Adult Wistar rats were submitted to acute hypoxia and analysed after 0 h, 24 h and 5 days of reoxygenation. Expression of hypoxia-inducible factor-1 alfa (HIF-1α) and angiogenesis-related genes including vascular endothelial growth factor (VEGF), adrenomedullin (ADM) and transforming growth factor-beta 1 (TGF-β1) was determined by both RT-PCR and ELISA. For vessel labelling, lectin location and expression were analysed using histochemical and image processing techniques (fractal dimension).
Expression of Hif-1α, Vegf, Adm and Tgf-β1 mRNA rose immediately after hypoxia and this increase persisted in some cases after 5 days post-hypoxia. While VEGF and TGF-β1 protein levels increased parallel to mRNA expression, ADM remained unaltered. The quantification of the striatal vessel network showed a significant augmentation at 24 h of reoxygenation.
These results reveal that not only short-term hypoxia, but also the subsequent reoxygenation period, up-regulate the angiogenic pathway in the rat caudate putamen as a neuroprotective mechanism to hypoxia that seeks to maintain a proper blood supply to the hypoxic tissue, thereby minimizing the adverse effects of oxygen deprivation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Diminished oxygen delivery and tissue oxygen deprivation are the consequence as well as the cause of many neurological, cardiovascular, and respiratory disorders (Mathur et al. 1999; Janssens et al. 2000). To overcome such situations of hypoxia, cells express a variety of genes which allow adaptation to decreased oxygen availability. Hypoxia-inducible factor-1 (HIF-1) is a transcription factor that regulates the adaptive response to hypoxia. HIF-1 is a basic helix-loop-helix/PAS protein consisting of the constitutively expressed β-subunit (HIF-1β) and one of two oxygen-regulated α-subunits (HIF-1α or HIF-2α) (Wenger 2002). In hypoxia, the α/β heterodimeric HIF complex regulates a great number of target genes involved in angiogenesis, vasodilation, erythropoiesis, and glycolysis by binding to hypoxia response elements (HREs) in the promoter regions of such genes (Singh et al. 2012). The HIF-1-dependent target genes include vascular endothelial growth factor (VEGF), adrenomedullin (ADM), transforming growth factor-beta 1 (TGF-β1), inducible nitric oxide synthase (iNOS) and erythropoietin (EPO) (Bani Hashemi et al. 2008).
One potential mechanism to counterbalance tissue hypoxia is the induction of angiogenesis. Hypoxia stimulates vessel growth through the up-regulation of numerous proangiogenic pathways. In this sense, hypoxia has been shown to affect vessel patterning, maturation, and function (Cassavaugh and Lounsbury 2011; Krock et al. 2011). The most potent proangiogenic factor is VEGF, a selective endothelial mitogen and vascular permeability factor, which is generally inducible by hypoxia (Ferrara and Davis-Srnyth 1997). There are at least five different VEGF homodimeric isoforms of 206, 189, 165, 145 and 121 amino acids, termed VEGF-A206, 189, 165, 145 and 121, which are produced by alternative splicing (Jussila and Alitalo 2002). VEGF is a direct target of HIF-1 as well as other factors related to cell division and migration, such as TGF-β. The TGF-β family of growth factors mediates vascular development and regulates endothelial responses to mechanical, inflammatory and hypoxic stress. The important role of TGF-β in vascular physiology is indicated by defective vasculogenesis and striking vascular inflammation, leading to death in mice null for TGF-β receptors (Dickson et al. 1995; Sanford et al. 1997). Particularly, TGF-β1 has been reported to modulate the activity of VEGF (Berse et al. 1999; Chávez et al. 2000; Renner et al. 2002). ADM is another HIF-1-dependent vasoactive target gene with an angiogenic effect, in part mediated by promoting VEGF expression. As a regulatory peptide, ADM has the capacity to dilate cerebral vessels and increase vascular permeability (Withers et al. 1996). ADM is up-regulated under hypoxic conditions and influences the recovery of blood flow in ischemic tissues (Iimuro et al. 2004; Knowles et al. 2004).
The caudate putamen is a basal ganglion of the brain that is particularly vulnerable to the hypoxic damage (Erecinska and Silver 1996). It contains a high density of dopaminergic nerve terminals and neuronal connections from the glutamatergic corticostriatal pathway. However, little is known about the angiogenic response of this brain ganglion under hypoxic conditions. In this light, the present study seeks to elucidate the effect of hypoxic challenge on the angiogenic pathway in the rat caudate putamen. It bears mentioning that this is the first time-course study which examines the behaviour of angiogenesis-related genes, as well as the vessel network in the adult rat striatum submitted to hypoxia and analysed after several reoxygenation times.
2 Methods
2.1 Animals
The study was performed on mature adult (4–5 months old) male albino Wistar rats kept under standard conditions of light and temperature and allowed ad libitum access to food and water. All the experiments were conducted according to E.U. guidelines on the use of animals for biochemical research (86/609/EU), as well as to the Guiding Principles in the Care and Use of Laboratory Animals, endorsed by the American Physiological Society.
2.2 Experimental procedure
The acute hypobaric hypoxia was carried out as previously published by our group (Lopez-Ramos et al. 2005; Rus et al. 2010a). Briefly, animals were placed in a chamber connected to a vacumm pump with a controlled air inflow and outflow. The acute hypobaric hypoxia was induced by reducing the barometric pressure to 225 mm Hg, resulting in a 48 mm Hg oxygen partial pressure. These conditions were maintained for 20 min. The ascent and descent speeds were kept at less than 1.000 feet/min. After the hypoxia period, animals were kept under normobaric normoxic conditions for different reoxygenation times (0 h, 24 h and 5 days), and then were sacrificed. Control animals were sacrificed after being maintained for 20 min in the chamber under normobaric normoxic conditions.
A total of 20 albino Wistar rats were used for the biochemical experiments (5 animals per experimental group). After the corresponding reoxygenation times, the rats were killed by cervical dislocation and the striatum was immediately removed, rinsed in saline solution, and stored at −80°C until used. For histochemistry, 20 rats (5 animals per experimental group) were anaesthetized with Ketolar (15 mg/100 g BW; Parke Davis, Madrid, Spain) and Rompun (1:5 v/v diluted in Ketolar; Bayer, Leverkusen, Germany), and then perfused in each reoxygenation time. The caudate putamen was removed, rinsed in saline solution, and fixated.
2.3 Quantitative Real-Time Polymerase Chain Reaction (RT-PCR) for Hif-1α (hypoxia-inducible factor-1 alfa), Vegf (vascular endothelial growth factor), Adm (adrenomedullin) and Tgf-β1 (transforming growth factor-beta 1)
The caudate putamen was homogenized in sterile PBS buffer (1:3 w/v) with a homogenator (Pellet Pestle Motor Cordless, Kontes, USA), and total RNA was directly isolated using PeqGold Microspin Total RNA kit (PeqLab, Erlangen, Germany) according to the manufacturer’s protocol. cDNA was synthesized from 1.5 μg total RNA using iScript cDNA Synthesis Kit (Bio-Rad), also following the manufacturer’s instructions.
FAM-labelled rat Hif-1α (Assay ID: Rn00577560_m1), Vegf-a (Assay ID: Rn00582935_m1), Adm (Assay ID: Rn00562327_m1), and Tgf-β1 (Assay ID: Rn99999016_m1) TaqMan gene expression assays were purchased from Applied Biosystems. VIC labelled endogenous reference gene 18S ribosomal RNA (Assay ID: Hs99999901_s1) TaqMan gene expression assay was also purchased from Applied Biosystems. 18S ribosomal RNA has been reported to be the most appropriate housekeeping gene for hypoxia experiments (Nagelkerke et al. 2010).
RT-PCR reactions were carried out in the CFX-96™ thermal cycler (Bio-Rad) according to Applied Biosystems amplification conditions, and following the manufacturer’s protocol for absolute quantification. For each sample, expression levels for the transcripts of interest were normalized to that of the endogenous 18S ribosomal RNA, and data were calculated as fold expression relative to the average of the control group. The relative expression of Hif-1α, Vegf-a, Adm, and Tgf-β1 was calculated by the 2[–ΔΔC(T)] method (Li et al. 2006).
2.4 Enzyme-linked immunosorbent assay (ELISA) for VEGF (vascular endothelial growth factor), ADM (adrenomedullin) and TGF-β1 (transforming growth factor-beta 1)
The caudate putamen was homogenized in PBS buffer (1:3 w/v) with a homogenator (Pellet Pestle Motor Cordless, Kontes, USA). Homogenates were centrifuged at 40.000 rpm during 30 min and the supernatant was collected. VEGF, TGF-β1, and ADM protein concentration was determined using Rat VEGF-A ELISA kit (Ab Frontier, Cat. No. LF-EK50417), Rat TGF-β1 ELISA kit (Ab Frontier, Cat. No. LF-EK50357) and ELISA kit for rat Adrenomedullin (Uscn Life, Cat. No. E90220Ra) respectively, according to the manufacturer’s protocol. Total protein concentrations were determined by the Bradford method (Bradford 1976), using bovine serum albumin as the standard. Final VEGF, ADM and TGF-β1 values were referred to the total protein concentration in the initial extracts.
2.5 Histological procedures for vessel labelling
Biotinylated lectin from Lycopersicon esculentum specific for N-acetyl-glucosamine and N-acetyl-polylactosamine oligomers is used as the best marker for brain endothelium (Mazzetti et al. 2004). Deeply anaesthetized animals were perfused through the left ventricle with 50 mL of 0.01 M phosphate-buffered saline (PBS; pH 7.4), and then with 250 mL of 4% paraformaldehyde in 0.1 M phosphate buffer (PB). The caudate putamen was removed and then post-fixed for a further 4 h in the same fixative at room temperature. Each sample was then cryoprotected by immersion overnight at 4°C in 0.1 M PB containing 30% sucrose. After that, the caudate putamen was embedded in O.C.T medium and frozen in 2-methylbutane pre-chilled in liquid nitrogen. Serial rostro-caudal sections (15 μm) were cut using a cryostat (Leica CM1950, Germany).
Free-floating sections were washed in Tris-HCl (1 M) and incubated in 1:100 Lycopersicon esculentum Lectin (10 μg/mL, Sigma-Aldrich, Ref. L0651) diluted in Tris-HCl buffer (1 M) overnight at 4°C. After the incubation, sections were washed in PBS buffer (0.01 M, pH 7.4), and then incubated in Cy3-Streptavidin (Sigma-Aldrich, Ref. S6402) solution diluted in PBS buffer (1:50) for 30 min.
2.6 Quantification of fractal dimension of vascular surface area
Vascular surface area was quantified by computerized-assisted image analysis using ImageJ (an NIH image analysis and processing software downloaded free from http://rsbweb.nih.gov/ij/ ). One random 1.56 mm2 field (image 10×) on each section, and five random sections (from rostral to caudal striatum) for each rat, were digitally captured from a fluorescence microscope (Olympus BX51). The fractal dimension was estimated using the box-counting method as previously described (Di Ieva et al. 2007), since it makes it possible to estimate the global complexity of a set of irregularly shaped objects, like two-dimensional vascularity (Abu-Eid and Landini 2003).
2.7 Statistical analysis
Data were expressed as mean ± SD (standard deviation). The statistical treatment to evaluate significant differences between groups was performed with SPSS 17.0 software. The data followed neither a normal distribution (tested with Kolmogorov-Smirnov test; α-value = 0.05), nor the principle of homoscedasticity (tested with Levene test; α-value = 0.05); therefore they were tested using the Kruskal Wallis test. The degree of statistical significance was established by applying the U Mann Whitney test to compare differences between means. The statistically significant differences vs. the control group were expressed as *p < 0.05; **p < 0.001.
3 Results
3.1 mRNA expression of hypoxia-inducible genes
The expression of Hif-1α, Vegf, Adm and Tgf-β1 was determined by RT-PCR using TaqMan technology. The mRNA expression of these hypoxia-inducible genes was significantly increased immediately after the hypoxic stimuli. Particularly, Hif-1α mRNA expression (figure 1) augmented at 0 h (p < 0.05) and 5 days post-hypoxia (p < 0.05) in comparison to the control group. The quantitative analysis of Vegf mRNA expression (figure 2) showed a statistically significant increase throughout the reoxygenation period (0 h, 24 h and 5 days: p < 0.05). Finally, while Adm mRNA levels (figure 3) followed the same pattern as Hif-1α mRNA (0 h, 5 days: p < 0.05), Tgf-β1 (figure 4) only rose immediately after hypoxia (0 h: p < 0.05).
Hypoxia-inducible factor-1 alfa (Hif-1α) mRNA expression in the rat caudate putamen. Experimental groups: Control and 0 h, 24 h and 5 days post-hypoxia. Results were expressed as arbitrary units. Results are mean values of three independent experiments and five animals per group. All experiments were performed in triplicates, and the values were used to calculate the ratio of Hif-1α to 18S ribosomal RNA, with a value of 1 used as the control. The statistically significant differences vs. the control group were expressed as *p < 0.05.
Vascular endothelial growth factor (Vegf) mRNA expression in the rat caudate putamen. Experimental groups: Control and 0 h, 24 h and 5 days post-hypoxia. Results were expressed as arbitrary units. Results are mean values of three independent experiments and five animals per group. All experiments were performed in triplicates, and the values were used to calculate the ratio of Vegf to 18S ribosomal RNA, with a value of 1 used as the control. The statistically significant differences vs. the control group were expressed as *p < 0.05.
Adrenomedullin (Adm) mRNA expression in the rat caudate putamen. Experimental groups: Control and 0 h, 24 h and 5 days post-hypoxia. Results were expressed as arbitrary units. Results are mean values of three independent experiments and five animals per group. All experiments were performed in triplicates, and the values were used to calculate the ratio of Adm to 18S ribosomal RNA, with a value of 1 used as the control. The statistically significant differences vs. the control group were expressed as *p < 0.05.
Transforming growth factor-beta 1 (Tgf-β1) mRNA expression in the rat caudate putamen. Experimental groups: Control and 0 h, 24 h and 5 days post-hypoxia. Results were expressed as arbitrary units. Results are mean values of three independent experiments and five animals per group. All experiments were performed in triplicates, and the values were used to calculate the ratio of Tgf-β1 to 18S ribosomal RNA, with a value of 1 used as the control. The statistically significant differences vs. the control group were expressed as *p < 0.05.
3.2 Protein expression of proangiogenic genes
The VEGF protein level (figure 5) significantly rose from 0 h to 5 days of reoxygenation (p < 0.001), showing a trend similar to that of Vegf mRNA expression. However, ADM protein expression remained unaltered in the hypoxic groups vs. control (figure 6). In parallel with the greater Tgf-β1 mRNA expression, the TGF-β1 protein level (figure 7) increased just after the hypoxic insult (0 h: p < 0.05).
Vascular endothelial growth factor (VEGF) protein expression (ELISA) in the rat caudate putamen. Experimental groups: Control and 0 h, 24 h and 5 days post-hypoxia. Results are mean values of three independent experiments with five animals per group. The statistically significant differences vs. the control group were expressed as **p < 0.001.
Adrenomedullin (ADM) protein expression (ELISA) in the rat caudate putamen. Experimental groups: Control and 0 h, 24 h and 5 days post-hypoxia. Results are mean values of three independent experiments with five animals per group. There were no statistically significant differences vs. the control group.
Transforming growth factor-beta 1 (TGF-β1) protein expression (ELISA) in the rat caudate putamen. Experimental groups: Control and 0 h, 24 h and 5 days post-hypoxia. Results are mean values of three independent experiments with five animals per group. The statistically significant differences vs. the control group were expressed as *p < 0.05.
3.3 Location and quantification of vascular surface area
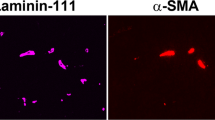
For vessel labelling, lectin location and expression were analysed using both histochemical and image processing techniques, including the box-counting method for estimating the fractal dimension. No labelling was detected in the negative controls when lectin was omitted. The microphotographs showed that the blood vessels were homogeneously distributed throughout the rat caudate putamen (figure 8). The cylindrical shape of the vessels is visible, as is the circular or elliptical lumen. The quantification of the vessel network in this brain ganglion (figure 9) showed a significant increase at 24 h post-hypoxia (p < 0.05).
Representative microphotographs of histological sections of rat caudate putamen stained for lectin histochemistry. Experimental groups: Control and 0 h, 24 h and 5 days post-hypoxia. The blood vessels are homogeneously distributed throughout the rat caudate putamen in all the experimental groups. The cylindrical shape of the vessels is visible, as is the circular or elliptical lumen.
Quantitative data from image analysis (fractal dimension of vascular surface area) of histological sections of rat caudate putamen stained for lectin histochemistry. Experimental groups: Control and 0 h, 24 h and 5 days post-hypoxia. Results are mean values of 25 microphotographs (five microphotographs per animal and five animals per group). The statistically significant differences vs. the control group were expressed as *p < 0.05.
4 Discussion
Hypoxia is a common cause of cell death and is involved in many disease processes. The activation of angiogenesis is a potential mechanism to counterbalance tissue hypoxia. Striatal neurons are highly vulnerable to hypoxia (Erecinska and Silver 1996), but few works have investigated the response of this brain ganglion to situations of oxygen deficiency. Therefore, the angiogenic response of the hypoxic caudate putamen remains unknown, despite the importance of these situations, which we have formerly investigated in several vital organs (central nervous system, CNS: Martínez-Romero et al. 2006; Cañuelo et al. 2007; lung: Rus et al. 2010b; heart: Rus et al. 2011).
Hypoxia-inducible factor-1 (HIF-1) is a transcriptional regulator of oxygen homeostasis and a key factor to generate adaptive responses through the up-regulation of various target genes involved in angiogenesis, including vascular endothelial growth factor (VEGF), adrenomedullin (ADM) and transforming growth factor-beta 1 (TGF-β1). Our results show an increase in Hif-1α expression in the caudate putamen of rats submitted to acute hypoxia/reoxygenation, suggesting that such situations may induce the implementation of a number of cellular mechanisms to boost oxygen delivery to the hypoxic striatum. Similar results have previously been described in the hypoxic brain (Wiener et al. 1996) and cerebellum (Kaur et al. 2006).
Regarding the proangiogenic genes, the expression of Vegf, Adm and Tgf-β1 followed the same pattern of Hif-1α and increased after short-term hypoxia. In this sense, the up-regulation of these vasoactive target genes may indicate the functional activation of HIF-1. Particularly, Vegf mRNA expression significantly rose throughout the reoxygenation period until 5 days post-hypoxia, suggesting that this HIF-1-target gene may play an important role in the response of the striatum to acute hypoxia. The upregulation of Vegf under hypoxic conditions agrees with other works performed in rat brain (Bani Hashemi et al. 2008), rat cerebellum (Kaur et al. 2006), and mouse brain (Kuo, et al. 1999). Furthermore, VEGF protein expression increased parallel to Vegf gene expression, implying an effective coordination between transcription and translation in order to develop a successful angiogenic response in the hypoxic caudate putamen. In this context, increased VEGF protein expression has previously been reported after hypoxia in the striatum (Mammen et al. 2011), brain (Kuo et al. 1999), and cerebellum (Kaur et al. 2006).
Similarly, Adm gene expression was significantly activated in the rat caudate putamen at 0 h and 5 days post-hypoxia. Previous studies confirm the induction of Adm in the CNS after hypoxia (Serrano et al. 2008; Bani Hashemi et al. 2008). However, this greater mRNA expression did not correspond to a higher ADM protein level. In agreement, Peebles et al. did not detect enhanced ADM protein expression in the CNS after hypoxia (Peebles et al. 2008). Nevertheless, increases in both ADM gene and protein expression have been reported in the hypoxic CNS (Nakanishi et al. 2004; Serrano et al. 2008). This discrepancy may be due to the different hypoxia models used, as well as to the organs or tissues studied. Based on these results, we propose that the stress induced by our hypoxia/reoxygenation model is not sufficiently strong or prolonged to cause the translation of the Adm mRNA. This hypothesis may be confirmed by previous results, which corroborated that the activation of ADM gene and protein depends on the time of exposure to hypoxia, so that the greatest increases occur after long exposure to hypoxia (Kitamuro et al. 2000). Furthermore, it has been suggested that hypoxia may decrease the percentage of translatable Adm mRNA (Hwang et al. 2007). In this context, the lack of a change in ADM level despite an increase in Adm mRNA has been shown after blockade of glycolysis with 2-deoxyglucose (Autelitano et al. 1999). This metabolic alteration has been proposed to mimic several features of hypoxia (Yuan et al. 1994; Bright et al. 1995). The 2-deoxyglucose mediated inhibition of ADM secretion most likely results in reduced ADM receptor activation, which might lead to stimulation of Adm gene expression (Autelitano et al. 1999). Both hypoxia and 2-deoxyglucose have been reported to increase intracellular Ca2+ levels, which may ultimately lead to vasoconstriction (Yuan et al. 1994; Bright et al. 1995). However, whether the hypoxia or 2-deoxyglucose mediated activation of Adm gene expression without greater ADM level is directly dependent on intracellular Ca2+ concentrations is yet to be established.
TGF-β1 is another hypoxia-inducible gene, which is involved in stabilizing HIF-1α (McMahon et al. 2006). Parallel to Hif-1α, Vegf and Adm expression, Tgf-β1 mRNA was induced immediately after the hypoxic insult in the rat caudate putamen. Similar results were found in the brain after hypoxia (Klempt et al. 1992; Huang et al. 2010). In addition, TGF-β1 protein expression also increased at 0 h of reoxygenation, suggesting a role for this transcription factor in the angiogenic response of the caudate putamen to hypoxia.
Finally, to test whether the upregulation of the angiogenesis-related genes led to an effective physiological change in the vasculature of the hypoxic caudate putamen, we analysed the vessel network in this brain ganglion using the glycoprotein lectin, an effective endothelial marker (Mazzetti et al. 2004). Our data reflected a significantly denser striatal vessel network at 24 h of reoxygenation, implying vascular adaptation after short-term hypoxia in the rat caudate putamen. In this context, brain vessel density has been reported to increase in the striatum after chronic hypoxia, leading to greater regional blood flow (LaManna et al. 1992; Patt et al. 1997). On the other hand, all the angiogenic factors analysed augmented immediately after the hypoxic episode, while the increase in the vessel network was noted at 24 h post-hypoxia. This lack of correlation may have occurred because the process of creation of blood vessels is long and complex and can last from hours to days, depending on the tissue and physiological state (Krupinski et al. 1994; Pettersson et al. 2000). On the other hand, our results also show that the blood vessel density returned to basal values 5 days after the hypoxic stimulus, although VEGF protein levels remained increased. In this sense, once the vessel network has expanded enough to re-establish the blood flow to the hypoxic tissues (24 h post-hypoxia), it may return to the baseline level. Similar data were reported by Pichiule and LaManna (2002), showing that the capillary density in the rat cerebral cortex was increased by chronic hypoxia and fell to basal levels after 7 days of normoxic recovery. Moreover, other pro-angiogenic factor, TGF-β1, was not increased from 24 h post-hypoxia in the hypoxic striatum, which may contribute partly to the regression of the vessel network thereafter.
These results may imply that striatal cells can detect situations of oxygen deficiency and respond to acute hypoxia by activating Hif-1α, which might initiate the angiogenic pathway by activating Vegf, Adm and Tgf-β1. As mentioned above, mRNA expression of these hypoxia-inducible genes immediately rose after hypoxia and returned to basal levels at 24 h of reoxygenation. In consequence, VEGF and TGF-β1 protein expression augmented in the rat striatum, leading to greater vessel density at 24 h post-hypoxia. Nevertheless, a VEGF-induced increase in the vessel network can generate the haemodynamic steal phenomena (Wang et al. 2005). That is, an increase in the vessel density without an augmentation in the blood supply can lead to reduced blood flow. Accordingly, the significant proangiogenic response detected immediately after acute hypoxia in the rat striatum may have led to a profuse vessel network capable of inducing the haemodynamic steal phenomena during the post-hypoxia period. This phenomena may thereby provoke transient hypoxia with the subsequent re-activation of the hypoxia-inducible genes (Hif-1α, Vegf and Adm), as revealed by our data at 5 days of reoxygenation.
In short, endogenous acute hypoxia-inducible mechanisms in the rat caudate putamen include the activation of the angiogenic pathway. Our results reveal that the proangiogenic factors, especially VEGF, were induced by both short-term hypoxia and the following reoxygenation period. As a result of this induction, a significant increase in the striatal vessel network was detected in this brain ganglion, in order to reduce the negative consequences of oxygen deprivation.
References
Abu-Eid E and Landini G 2003 Quantification of the global and local complexity of the epithelial-connective ti ssue interface of normal, dysplastic, and neoplastic oral mucosae using digital imaging. Pathol. Res. Pract. 199 475–482
Autelitano DJ, Tang F and Little PJ 1999 Rapid regulation of adrenomedullin in metabolically compromised vascular smooth muscle cells. J. Hypertens. 17 373–379
Bani Hashemi S, Braun J, Bernhardt WM, Rascher W, Dötsch J and Trollmann R 2008 HIF-1alpha subunit and vasoactive HIF-1-dependent genes are involved in carbon monoxide-induced cerebral hypoxic stress response. Eur. J. Appl. Physiol. 104 95–102
Berse B, Hunt JA, Diegel RJ, Morganelli P, Yeo K, Brown F and Fava RA 1999 Hypoxia augments cytokine (transforming growth factor-beta (TGF-β) and IL-1)-induced vascular endothelial growth factor secretion by human synovial fibroblasts. Clin. Exp. Immunol. 115 176–182
Bradford MM 1976 A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal. Biochem. 72 248–254
Bright RT, Salvaterra CG, Rubin LJ and Yuan X-J 1995 Inhibition of glycolysis by 2- DG increases [Ca2+]i in pulmonary arterial smooth muscle cells. Am. J. Physiol. 269 L203–L208
Cañuelo A, Siles E, Martínez-Romero R, Peinado MA and Martínez-Lara E 2007 The nitric oxide system response to hypoxia/reoxygenation in the aged cerebral cortex. Exp. Gerontol. 42 1137–1145
Cassavaugh J and Lounsbury KM 2011Hypoxia-mediated biological control. J. Cell Biochem. 112 735–744
Chávez JC, Agani F, Pichiule P and LaManna JC 2000 Expression of hypoxia-inducible factor-1alpha in the brain of rats during chronic hypoxia. J. Appl. Physiol. 89 1937–1942
Di Ieva A, Grizzi F, Ceva-Grimaldi G, Russo C, Gaetani P, Aimar E, Levi D, Pisano P, et al. 2007 Fractal dimension as a quantitator of the microvasculature of normal and adenomatous pituitary tissue. J. Anat. 211 673–680
Dickson MC, Martin JS, Cousins FM, Kulkarni AB, Karlsson S and Akhurst RJ 1995 Defective haematopoiesis and vasculogenesis in transforming growth factor- β 1 knock out mice. Development 121 1845–1854
Erecinska M and Silver IA 1996 Calcium handling by hippocampal neurons under physiologic and pathologic conditions. Adv. Neurol. 71 119–136
Ferrara N and Davis-Srnyth T 1997 The biology of vascular endothelial growth factor. Endocr. Rev. 18 4–25
Huang RQ, Cheng HL, Zhao XD, Dai W, Zhuang Z, Wu Y, Liu Y and Shi JX 2010 Preliminary study on the effect of trauma-induced secondary cellular hypoxia in brain injury. Neurosci. Lett. 473 22–27
Hwang IS, Fung ML, Liong EC, Tipoe GL and Tang F 2007 Age-related changes in adrenomedullin expression and hypoxia-inducible factor-1 activity in the rat lung and their responses to hypoxia. J. Gerontol. A Biol. Sci. Med. Sci. 62 41–49
Iimuro S, Shindo T, Moriyama N, Amaki T, Niu P, Takeda N, Iwata H, Zhang Y, et al. 2004 Angiogenic effects of adrenomedullin in ischemia and tumor growth. Circ. Res. 95 415–423
Janssens, J P, Pautex, S, Hilleret, H and Michel, J P 2000 Sleep disordered breathing in the elderly. Aging (Milano) 12 417–429
Jussila L and Alitalo K 2002 Vascular growth factors and lymphangiogenesis. Physiol. Rev. 82 673–700
Kaur C, Sivakumar V, Zhang Y and Ling EA 2006 Hypoxia-Induced Astrocytic Reaction and Increased Vascular Permeability in the Rat Cerebellum. Glia 54 826–839
Kitamuro T, Takahashi K, Nakayama M, Murakami O, Hida W, Shirato K and Shibahara S 2000 Induction of adrenomedullin during hypoxia in cultured human glioblastoma cells. J. Neurochem. 75 1826–1833
Klempt ND, Sirimanne E, Gunn AJ, Klempt M, Singh K, Williams C and Gluckman PD 1992 Hypoxia-ischemia induces transforming growth factor beta 1 mRNA in the infant rat brain. Brain Res. Mol. Brain Res. 13 93–101
Knowles HJ, Tian YM, Mole DR and Harris AL 2004 Novel mechanism of action for hydralazine: induction of hypoxia-inducible factor-1a, vascular endothelial growth factor, and angiogenesis by inhibition of prolyl hydroxylases. Circ. Res. 95 162–169
Krock B, Skuli N and Simon MC 2011 Hypoxia-induced angiogenesis: good and evil. Genes Cancer 2 1117–1133
Krupinski J, Kaluza J, Kumar P, Kumar S and Wang JM 1994 Role of angiogenesis in patients with cerebral ischemic stroke. Stroke 25 1794–1798
Kuo NT, Benhayon D, Przybylski RJ, Martin RJ and LaManna JC 1999 Prolonged hypoxia increases vascular endothelial growth factor mRNA and protein in adult mouse brain J. Appl. Physiol. 86 260–264
LaManna JC, Vendel LM and Farrell RM 1992 Brain adaptation to chronic hypobaric hypoxia in rats. J. Appl. Physiol. 72 2238–2243
Li H, Witte K, August M, Brausch I, Godtel-Armbrust U, Habermeier A, Closs EI, et al. 2006 Reversal of endothelial nitric oxide synthase uncoupling and up-regulation of endothelial nitric oxide synthase expression lowers blood pressure in hypertensive rats. J. Am. Coll. Cardiol. 47 2536–2544
Lopez-Ramos JC, Martinez-Romero R, Molina F, Cañuelo A, Martinez-Lara E, Siles E and Peinado MA 2005 Evidence of a decrease in nitric oxide-storage molecules following acute hypoxia and/or hypobaria, by means of chemiluminescence analysis. Nitric Oxide 13 62–67
Mammen A, Kubin J, Greeley WJ, Schears GJ, Pastuszko P, F Wilson D and Pastuszko A 2011 Effect of hypoxia on expression of selected proteins involved in regulation of apoptotic activity in striatum of newborn piglets. Neurochem. Res. 36 746–753
Martínez-Romero R, Cañuelo A, Martínez- Lara E, Hernández R, Del Moral ML, Pedrosa JA, Peinado MA and Siles E 2006 Aging affects but does not eliminate the enzymatic antioxidative response to hypoxia/reoxygenation in cerebral cortex. Exp. Gerontol. 41 25–31
Mathur R, Cox IJ, Oatridge A, Shephard DT, Shaw RJ and Taylor-Robinson SD 1999 Cerebral bioenergetics in stable chronic obstructive pulmonary disease. Am. J. Respir. Crit. Care Med. 160 1994–1999
Mazzetti S, Frigerio S, Gelati M, Salmaggi A, Vitellaro-Zuccarello L 2004 Lycopersicon esculentum lectin: an effective and versatile endothelial marker of normal and tumoral blood vessels in the central nervous system. Eur. J. Histochem. 48 423–428
McMahon S, Charbonneau M, Grandmont S, Richard DE and Dubois CM 2006 Transforming growth factor beta1 induces hypoxia-inducible factor-1 stabilization through selective inhibition of PHD2 expression. J. Biol. Chem. 281 24171–24181
Nagelkerke A, Mujcic H, Wouters B and Span PN 2010 18S is an appropriate housekeeping gene for in vitro hypoxia experiments. Br. J. Cancer 103 590
Nakanishi K, Osada H, Uenoyama M, Kanazawa F, Ohrui N, Masaki Y, Hayashi T, Kanatani Y, et al. 2004 Expressions of adrenomedullin mRNA and protein in rats with hypobaric hypoxia-induced pulmonary hypertension. Am. J. Physiol Heart Circ. Physiol. 286 H2159– H2168
Patt S, Sampaolo S, Théallier-Jankó A, Tschairkin I and Cervós-Navarro J 1997 Cerebral angiogenesis triggered by severe chronic hypoxia displays regional differences. J. Cereb. Blood Flow Metab. 17 801–806
Peebles KC, Richards AM, Celi L, McGrattan K, Murrell CJ and Ainslie PN 2008 Human cerebral arteriovenous vasoactive exchange during alterations in arterial blood gases. J. Appl. Physiol. 105 1060–1068
Pettersson A, Nagy JA, Brown LF, Sundberg C, Morgan E, Jungles S, Carter R, Krieger JE, et al. 2000 Heterogeneity of the angiogenic response induced in different normal adult tissues by vascular permeability factor/vascular endothelial growth factor. Lab. Invest. 80 99–115
Pichiule P and LaManna JC 2002 Angiopoietin-2 and rat brain capillary remodeling during adaptation and deadaptation to prolonged mild hypoxia. J. Appl. Physiol. 93 1131–1139
Renner U, Lohrer P, Schaaf L, Feirer M, Schmitt K, Onofri C, Arzt E and Stalla GK 2002 Transforming growth factor-beta stimulates vascular endothelial growth factor production by folliculostellate pituitary cells. Endocrinology 143 3759–3765
Rus A, Del Moral ML, Molina F and Peinado MA 2011 Upregulation of cardiac NO/NOS system during short-term hypoxia and the subsequent reoxygenation period. Eur. J. Histochem. 55 e17
Rus A, Peinado MA, Castro L and Del Moral ML 2010a Lung eNOS and iNOS are reoxygenation time-dependent upregulated after acute hypoxia. Anat. Rec. (Hoboken) 293 1089–1098
Rus A, Molina F, Peinado MA, del Moral ML 2010b Endothelial NOS-derived nitric oxide prevents injury resulting from reoxygenation in the hypoxic lung. Free Radic. Res. 44 1027–1035
Sanford LP, Ormsby I, Gittenberger-de Groot AC, Sariola H, Friedman R, Boivin GP, Cardell EL and Doetschman T 1997 TGF β2 knockout mice have multiple developmental defects that are non-overlapping with other TGF β knockout phenotypes. Development 124 2659–2670
Serrano J, Fernández AP, Sánchez J, Rodrigo J and Martínez A 2008 Adrenomedullin expression is up-regulated by acute hypobaric hypoxia in the cerebral cortex of the adult rat. Brain Pathol. 18 434–442
Singh N, Sharma G, Mishra V and Raghubir R 2012 Hypoxia inducible factor-1: Its potential role in cerebral ischemia. Cell Mol. Neurobiol. 32 491–507
Wang Y, Kilic E, Kilic U, Weber B, Bassetti CL, Marti HH and Hermann DM 2005 VEGF overexpression induces post-ischaemic neuroprotection, but facilitates haemodynamic steal phenomena. Brain 128 52–63
Wenger RH 2002 Cellular adaptation to hypoxia: O2-sensing protein hydroxylases, hypoxia-inducible transcription factors, and O2-regulated gene expression. FASEB J. 16 1151–1162
Wiener CM, Booth G and Semenza GL 1996 In vivo expression of mRNAs encoding hypoxia-inducible factor 1. Biochem. Biophys. Res. Commun. 225 485–488
Withers DJ, Coppock HA, Seufferlein T, Smith DM, Bloom SR and Rozengurt E 1996 Adrenomedullin stimulates DNA synthesis and cell proliferation via elevation of cAMP in Swiss 3T3 cells. FEBS Lett. 378 83–87
Yuan X-J, Tod ML, Rubin LJ and Blaustein MP 1994 Deoxyglucose and reduced glutathione mimic effects of hypoxia on K+ and Ca2+ conductances in pulmonary arterial cells. Am. J. Physiol. 267 L52–L63
Acknowledgements
We wish to thank to Dr Rafael Lomas for his statistic assistance. This work was supported by Instituto de Salud Carlos III (PI081222), University of Jaén (RFC/PP2008/UJA_08_16_20), Junta de Andalucía (BIO-0184), and Fondo Europeo de Desarrollo Regional (FEDER).
Author information
Authors and Affiliations
Corresponding author
Additional information
Corresponding editor: NEERAJ JAIN
MS received 26 June 2012; accepted 02 April 2013
Corresponding editor: Neeraj Jain
[Molina F, Rus A, Peinado MA and del Moral ML 2013 Short-term hypoxia/reoxygenation activates the angiogenic pathway in rat caudate putamen. J. Biosci. 38 1–9] DOI 10.1007/s12038-013-9327-6
Rights and permissions
About this article
Cite this article
Molina, F., Rus, A., Peinado, M. et al. Short-term hypoxia/reoxygenation activates the angiogenic pathway in rat caudate putamen. J Biosci 38, 363–371 (2013). https://doi.org/10.1007/s12038-013-9327-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12038-013-9327-6