Abstract
Experimental animal studies have demonstrated that oxidative stress plays an essential role during ischemic stroke. In addition to oxidizing macromolecules leading to cell injury, oxidants are also involved in cell death/survival signal pathways and cause mitochondrial dysfunction. Nuclear factor erythroid 2-related factor 2 (Nrf2) represents one of the major regulators implicated in the endogenous defense system against oxidative stress. We have studied the expression and activation status of Nrf2 under stroke-like conditions using the temporary middle cerebral artery occlusion rat model. Inactive Nrf2 is proteasomal degraded within minutes but stabilized during activation. We analyzed Nrf2 activation and the resulting accumulation in post-ischemic rat brain cells using double immunofluorescence staining with antibodies directed against Nrf2 and cell type-specific markers. The core infarct region showed no obvious positive staining signal for Nrf2 24 h after the initiation of artery occlusion. However, Nrf2 immunoreactivity was detectable in the ipsilateral penumbra where microglia, astrocytes, and neurons contained Nrf2. Interestingly, Nrf2 was also significantly upregulated in neurons but not in other cell types of the unaffected contralateral site. These results provide strong evidence that Nrf2 is involved in acute stroke-dependent neurodegeneration in the penumbra but not core region and indicate the presence of a systemic Nrf2 activator independent from oxidative stress.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
There is general agreement that oxidative stress is a major critical challenge in the pathogenesis of stroke. Oxidative stress can cause cell death by damaging cardinal cellular components such as lipids, proteins, or DNA/RNA. Besides, it also interferes with different cell death-/survival-signalling pathways and destabilizes mitochondrial structure and function. In addition to direct cytotoxic effects occurring immediately after ischemia/reperfusion, the burst of free radicals provokes additionally the formation of inflammatory mediators such as TNF-alpha and distinct interleukins through redox-mediated signalling pathways, leading to post-ischemic/reperfusion inflammatory injury (Chen et al. 2011).
Over the course of evolution, cells have developed complex cellular defense mechanisms and strategies to cope with and defend against oxidative stress. A battery of genes encoding detoxifying and anti-oxidative enzymes is orchestrated upon exposure to reactive oxygen species. Among them, the activation of nuclear factor erythroid 2-related factor 2 (Nrf2) by reactive oxygen species (ROS) or mitogen activated protein kinase (MAPK) kinases initiates or enhances the transcription of genes coding for anti-oxidative enzymes but also for the neuroprotective cytokine interleukin-6 (Kensler et al. 2007; Wruck et al. 2011). Many of these genes commonly regulated by Nrf2 have been shown to be active during damaging conditions (Wruck et al. 2009) and to be neuroprotective (Brandenburg et al. 2010; Calkins et al. 2009; Kipp and Beyer 2009; Wruck et al. 2007; Wruck et al. 2008). Previous studies have shown that the increase of Nrf2 activity by small molecules provides sufficient protection against cerebral ischemia in vivo (Kraft et al. 2004; Satoh et al. 2006; Shah et al. 2010; Shih et al. 2005; Yang et al. 2009). Despite this evidence, no reliable data are at present available demonstrating a direct local activation of Nrf2 in the acute ischemic phase within the penumbra and/or core of the acute ischemic brain. Therefore, we aimed in the present study to determine the expression and activation level of Nrf2 during the course of stroke using the well-established middle cerebral artery (MCAO) rat model (Kramer et al. 2010). Furthermore, we evaluated the cell type-specific expression of Nrf2 in these tissues by double immunofluorescence stainings for astroglial, microglial, and neuronal markers.
Material and Methods
Animals
Male Wistar rats (12–14 weeks old, 380–410 g, Charles River, Germany) were maintained in a pathogen-free and climate-controlled environment with access to water and food ad libitum and were handled according to the rules of “Care of Animal Subjects” (North Rhine-Westphalia, Germany). Research and animal care procedures were approved by the Review Board for the Care of Animal Subjects of the district government (North Rhine-Westphalia, Germany). A total of six animals were tested in this study.
Surgery and tMCAO
Anesthesia was induced by inhalation of 5% isoflurane (Abbott, Ludwigshafen, Germany) for 2 min and maintained at 2–2.5% (depending on each animal and operation step) using a face mask. Body temperature was kept throughout surgery at 37°C ± 0.5°C using a heating blanket and lamp. Laser–Doppler flowmetry (Moor instruments VMS-LDF2, Axminster, UK) was used to monitor cerebral blood flow on the ipsi- and contralateral side for 1 h during surgery. The 2-mm Laser–Doppler measuring sensors were placed 1–2 mm posterior and 4–5 mm lateral to the bregma on the left and right skull hemisphere depending on highest blood perfusion units (BPU) after a small skin incision at the ipsilateral side. To ensure that the BPU digitized the cortical vascular territory of the middle cerebra artery (MCA), the common carotid artery was clipped temporary resulting in a decrease of BPU. Prior to fixation of the sensors, the skull was carefully thinned out to assure that the reduction of BPU is not due to reduction in external carotid artery (ECA) blood flow. Focal cerebral ischemia was induced by occlusion of the left MCA as previously described (Kramer et al. 2010) with some minor modifications. Following a small midline neck skin incision, the left common carotid artery (CCA), internal carotid artery (ICA), and ECA were exposed. Subsequently, the ECA was transiently clipped and the CCA was ligated proximally. The vagus nerve was carefully preserved. To avoid protrusion into the A. pterygopalatina, the head was bended aside and a commercially available catheter (Asahi PTCA Guide Wire Soft, Abbott Vascular) was subsequently introduced from the lumen of the distal CCA at the bifurcation as far as a resistance was manually observed. Directly before insertion of the catheter into the ICA, baseline values of cerebral blood flow (CBF) were measured (for illustrations of the technique please see Fig. 1). In the study, only those animals which showed a reduction of regional CBF by >50% compared to baseline before temporary middle cerebral artery occlusion (tMCAO) were included.
TTC Tissue Staining
At 24 h after tMCAO, the animals were deeply anesthetized again (5% isoflurane) and received an intraperitoneal injection of an overdose of pentobarbital (328 mg/kg). Afterwards, animals were intracardially perfused with physiological NaCl. Brains were dissected and placed in a rat brain matrix (Alto Brain Matrix stainless steel 1 mm rat coronal 300-600GM; Havard Apparatus Holliston, MA, USA). Two-millimeter coronal slices were cut and incubated for 20 min at 37°C in 2,3,5-triphenyl-tetrazoliumchloride (TTC, Fluka, Steinheim, Germany) for determination of the infarct size. TTC is a marker for metabolic function and represents a reliable indicator of ischemic areas for up to 3 days after ischemia (Kramer et al. 2010). Metabolic active tissue is typically stained red after TTC exposure, whereas necrotic tissue remains pale.
Double Immunofluorescence
At 24 h after tMCAO, all animals were deeply anesthetized again (5% isoflurane) and received an intraperitoneal injection of an overdose of pentobarbital (328 mg/kg). For immunohistochemistry, rats were intracardially perfused with 2% (w/v) paraformaldehyde (Roth, Karlsruhe, Germany) containing 15% (v/v) saturated picric acid at pH 7.4 (AppliedChem GmbH, Darmstadt, Germany). Brains were post-fixed overnight in the same perfusion solution. Then, the brains were paraffin-embedded (Merck KGaA, Darmstadt, Germany). Thereafter, coronal sections, each 5 μm thick, were made and rehydrated using standard protocols. After incubation with 0.1% Triton X in PBS for 10 min at room temperature and antigen retrieval using microwave, sections were blocked in 0.1 M Tris–HCl pH 7.5 containing 1.5% bovine serum albumin (BSA; Sigma Chemical Company, Germany) for 10 min. Slides were incubated at 4°C overnight with a pair of primary antibodies diluted in TRIS containing 1.5% BSA. The following primary antibodies were used for this study: rabbit polyclonal anti-Nrf2 antibody, 1:50; mouse monoclonal anti-SMI32 antibody, 1:1,000; mouse monoclonal anti-glial fibrillary acidic protein (GFAP) antibody, 1:250; and goat polyclonal anti-Iba1 antibody, 1:100 (all Abcam, Cambridge, UK). Finally, the slices were incubated with donkey anti-rabbit AlexaFluor 488 (Molecular Probes, USA), goat anti-mouse Cy3 (Sigma, Germany), or Donkey anti-goat AlexaFluor 555 (all 1:250; Molecular Probes, USA) for 1 h at room temperature. Nuclear staining was performed with bisbenzimide (Sigma, Germany). Cells were digitally photographed using a Zeiss Axio Z1 Imager microscope (Zeiss, Göttingen, Germany).
Semiquantitative Histomorphometric Analysis
The stained slides from three tMCAO rats, three sham-operated control rats, and three control rats were independently scored in a double-blind fashion. The Nrf2 immunostaining was evaluated by means of a four-point scale: −/−, no expression; +, low expression; ++, moderate expression; and +++, high expression. The semiquantitative basis for the scoring was based on the apparent intensity of the labeling of specific cells and not the percentage of the section surface, which was positively labeled. Two observers independently reviewed and compared the arrays. Using this approach, an interobserver variation in histomorphometric scoring was minimal and the majority of scores were identical. In cases where variation was found, the difference was never more than 1 unit.
Results
Laser–Doppler monitoring revealed that in all rats included in the study, relative regional blood flow values were reduced by >50% compared to pre-ischemic values within several minutes after induction of tMCAO and remained stable during tMCAO (data not shown). TTC staining allowed a perfect outline of the infarcted ipsilateral cerebral cortex including the border between core and penumbra (Fig. 2a) and via anti-SMI32 immunohistostaining (Figs. 1 and 2b). Further analysis and allocation of immunoreactive cells to the infract subregions were performed according to the penumbra delineation. To identify Nrf2-positive cell types, we performed double immunofluorescence studies for Nrf2 in combination with a neuronal cell marker (SMI32), an astroglial cell marker, GFAP, or a microglial cell marker, ionized calcium-binding adaptor molecule 1 (Iba1) which also labels peripheral macrophages.
a TTC-stained 2-mm coronal brain slice of a male rat shows the white infarct area 24 h after tMCAO. Red color indicates intact tissue; pale white tissue reflects the core region. b Immunohistostaining of a comparable brain region with anti-SMI32 antibodies. 1 and 2 are higher magnifications of the core/penumbra border region of b. Asterisks mark the penumbra region
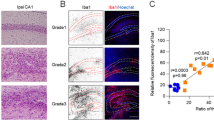
Brain slices from untreated control (data not shown) and sham-operated control rats showed only sparse immunoreactivity for Nrf2. Also, the core infarct region revealed no significant positive staining signals for Nrf2 (Fig. 3, 4, and 5). In contrast, microglia (Fig. 3), astrocytes (Fig. 4), as well as neurons (Fig. 5) stained distinctly positive for Nrf2 in the penumbra region surrounding the core infarct area. In addition, we observed immunopositive-Nrf2 cells in the ipsilateral cerebral cortex representing microglia (Fig. 3), astrocytes (Fig. 4), and neurons (Fig. 5). In the contralateral cortex, Nrf2 was significantly upregulated only in neurons but not in microglia or astrocytes compared to sham-operated controls (Fig. 5). The results of the semiquantitative histomorphometric analysis have been summarized in Table 1.
Fluorescence microscopy for Nrf2 in microglia in rat brains after tMCAO. Coronal plane of brain sections from rats with tMCAO was subsequently fixed and labeled using anti-Nrf2 (green) and anti-Iba-1 (red) antibodies to identify microglia. Nuclei were stained with DAPI (blue). Left panel ipsilateral, right panel contralateral, controls were sham-operated rats. The figures show representative results from three independent experiments performed in duplicate. Scale bars in overview = 200 μm. Scale bars in detail image = 20 μm. Left panel showed ipsilateral core, penumbra, and cortex region; right panel showed the analogous contralateral regions
Fluorescence microscopy for Nrf2 in astroglia in rat brains after tMCAO. Coronal plane of brain sections from rats with tMCAO was subsequently fixed and labeled using anti-Nrf2 (green) and anti-GFAP (red) antibodies to identify astroglia. Nuclei were stained with DAPI (blue). Left panel ipsilateral, right panel contralateral, controls were sham-operated rats. The figures show representative results from three independent experiments performed in duplicate. Scale bars in overview = 200 μm. Scale bars in detail image = 20 μm. Left panel showed ipsilateral core, penumbra, and cortex region; right panel showed the analogous contralateral regions
Fluorescence microscopy for Nrf2 in neurons in rat brains after tMCAO. Coronal plane of brain sections from rats with tMCAO was subsequently fixed and labeled using anti-Nrf2 (green) and anti-SMI32 (red) antibodies to identify neurons. Nuclei were stained with DAPI (blue). Left panel ipsilateral, right panel contralateral, controls were sham-operated rats. The figures show representative results from three independent experiments performed in duplicate. Scale bars in overview = 200 μm. Scale bars in detail image = 20 μm. Left panel showed ipsilateral core, penumbra, and cortex region; right panel showed the analogous contralateral regions
Discussion
In the present report, we investigated the expression of the transcription factor Nrf2 in brain specimens of male rats with tMCAO or sham-operated animals using double immunofluorescence. Inactive Nrf2 is typically proteosomal degraded within minutes but stabilized during activation under damaging conditions. The study was undertaken to determine whether Nrf2 is locally activated under acute ischemic stroke-like conditions in the infarct areal and, thus, plays a role in the oxidative stress-related pathogenesis of this disease. Furthermore, we aimed to attribute Nrf2 expression to different cell types known to be primarily targeted and secondarily implicated in the acute inflammatory and oxidative stress scenario. We have measured Nrf2 activation and resulting accumulation in post-ischemic rat brains (1 h ischemia and 23 h recovery of stroke) using double immunofluorescence staining with antibodies directed against Nrf2 and cell type-specific markers for neurons, astroglia, and microglia.
Within the ischemic cerebrovascular region, there are two major zones of injury, the core ischemic zone and penumbra. The latter represents a rim of ischemic but still viable cerebral cells which are functionally stable and can be protected from cell death depending on the delay of reperfusion and presence of anti-inflammatory/anti-apoptotic molecules. The core ischemic zone showed no Nrf2 staining. The most likely explanation for this observation might be that the local blood flow reduction in the core region and the associated cell death are reduced and provoked very rapidly respectively to such a level that transcription and translation is no longer detectable. Since cell degeneration in the core appears immediately after the onset of ischemia within the first minutes to an hour, RNA and protein degradation is complete. The time of assessment, e.g., 24 h after initiation of stroke in this study, does therefore not allow drawing conclusions. Nevertheless, delayed oxidative stress phenomena which occur in response to these early degenerating signs might not have a chance to activate Nrf2 in the core. In contrast to the core, a significant increase in Nrf2 expression was found in the ischemic penumbra in both glial and neuronal cells. It is known that in this region, reoxygenation results in a high level of oxidative stress which appears damaging but at a sublethal level (Carbonell and Rama 2007). Hence, the penumbra is this stroke-associated tissue where Nrf2 activation is believed to be beneficial and might subsequently contribute to cell protection and survival.
The activation state of Nrf2 in healthy glial and neuronal cells is below the detection level. Therefore, it was an unexpected finding that Nrf2 activation was significantly induced in neurons of the unaffected cortex region in tMCAO rats. Because this activation occurs ipsilateral as well as contralateral, we are tempted to speculate about the existence of an unknown factor(s) that might act as intrinsic Nrf2 activator.
We hypothesize that growth factors or cyto- and chemokines which are typically active during ischemia may be involved in Nrf2 regulation via MAP kinase signalling without the occurrence of ROS. In addition to neurochemical mediators, also cross-hemispheral neural connections might also be a possible way to activate Nrf2 in the contralateral side. This possibility is suggested by MRI evidence in humans undergoing stroke rehabilitation, as well as by experimental studies in rat (Kim et al. 2005). Although speculative, this effect might play a role to prone primarily not affected brain tissue to forthcoming oxidative stress caused by nearby cell degeneration. In support for such an assumption is that Nrf2 was only seen in neurons. Thus, Nrf2 activation in the penumbra region is obviously a reaction on the massive ROS production as a result of reoxygenation, whereas Nrf2 activation in the unimpaired cortex regions can be seen as a pre-adaptation to oxidative stress.
In conclusion, our study highlights Nrf2 as a neuroprotective factor under ischemic stroke conditions. It is becoming evident that Nrf2 activation is able to protect the brain after initiation of injury, making Nrf2 a rewarding therapeutic target.
References
Brandenburg LO, Kipp M, Lucius R, Pufe T, Wruck CJ (2010) Sulforaphane suppresses LPS-induced inflammation in primary rat microglia. Inflamm Res 59(6):443–450
Calkins MJ, Johnson DA, Townsend JA, Vargas MR, Dowell JA, Williamson TP, Kraft AD, Lee JM, Li J, Johnson JA (2009) The Nrf2/ARE pathway as a potential therapeutic target in neurodegenerative disease. Antioxid Redox Signal 11(3):497–508
Carbonell T, Rama R (2007) Iron, oxidative stress and early neurological deterioration in ischemic stroke. Curr Med Chem 14(8):857–874
Chen H, Yoshioka H, Kim GS, Jung JE, Okami N, Sakata H, Maier CM, Narasimhan P, Goeders CE, Chan P (2011) Oxidative stress in ischemic brain damage: mechanisms of cell death and potential molecular targets for neuroprotection. Antioxid Redox Signal 14(8):1505–1517, 15
Kensler TW, Wakabayashi N, Biswal S (2007) Cell survival responses to environmental stresses via the Keap1-Nrf2-ARE pathway. Annu Rev Pharmacol Toxicol 47:89–116
Kim YR, Huang IJ, Lee SR, Tejima E, Mandeville JB, van Meer MP, Dai G, Choi YW, Dijkhuizen RM, Lo EH, Rosen BR (2005) Measurements of BOLD/CBV ratio show altered fMRI hemodynamics during stroke recovery in rats. J Cereb Blood Flow Metab 25(7):820–829
Kipp M, Beyer C (2009) Impact of sex steroids on neuroinflammatory processes and experimental multiple sclerosis. Front Neuroendocrinol 30(2):188–200
Kraft AD, Johnson DA, Johnson JA (2004) Nuclear factor E2-related factor 2-dependent antioxidant response element activation by tert-butylhydroquinone and sulforaphane occurring preferentially in astrocytes conditions neurons against oxidative insult. J Neurosci 24(5):1101–1112
Kramer M, Dang J, Baertling F, Denecke B, Clarner T, Kirsch C, Beyer C, Kipp M (2010) TTC staining of damaged brain areas after MCA occlusion in the rat does not constrict quantitative gene and protein analyses. J Neurosci Methods 187(1):84–89
Satoh T, Okamoto SI, Cui J, Watanabe Y, Furuta K, Suzuki M, Tohyama K, Lipton SA (2006) Activation of the Keap1/Nrf2 pathway for neuroprotection by electrophilic [correction of electrophillic] phase II inducers. Proc Natl Acad Sci USA 103(3):768–773
Shah ZA, Li RC, Ahmad AS, Kensler TW, Yamamoto M, Biswal S, Dore S (2010) The flavanol (−)-epicatechin prevents stroke damage through the Nrf2/HO1 pathway. J Cereb Blood Flow Metab 30(12):1951–1961
Shih AY, Li P, Murphy TH (2005) A small-molecule-inducible Nrf2-mediated antioxidant response provides effective prophylaxis against cerebral ischemia in vivo. J Neurosci 25(44):10321–10335
Wruck CJ, Claussen M, Fuhrmann G, Romer L, Schulz A, Pufe T, Waetzig V, Peipp M, Herdegen T, Gotz ME (2007) Luteolin protects rat PC12 and C6 cells against MPP+ induced toxicity via an ERK dependent Keap1-Nrf2-ARE pathway. J Neural Transm Suppl 72:57–67
Wruck CJ, Gotz ME, Herdegen T, Varoga D, Brandenburg LO, Pufe T (2008) Kavalactones protect neural cells against amyloid beta peptide-induced neurotoxicity via extracellular signal-regulated kinase 1/2-dependent nuclear factor erythroid 2-related factor 2 activation. Mol Pharmacol 73(6):1785–1795
Wruck CJ, Huppertz B, Bose P, Brandenburg LO, Pufe T, Kadyrov M (2009) Role of a fetal defence mechanism against oxidative stress in the aetiology of preeclampsia. Histopathology 55(1):102–106
Wruck CJ, Streetz K, Pavic G, Goetz ME, Tohidnezhad M, Brandenburg LO, Varoga D, Eickelberg O, Herdegen T, Trautwein C, Chan K, Kan YW, Pufe T (2011) Nrf2 induces interleukin-6 (IL-6) expression via an antioxidant response element within the IL-6 promoter. J Biol Chem 286(6):4493–4499
Yang C, Zhang X, Fan H, Liu Y (2009) Curcumin upregulates transcription factor Nrf2, HO-1 expression and protects rat brains against focal ischemia. Brain Res 1282:133–141
Acknowledgments
The technical support by Helga Helten and Michaela Nicolau is acknowledged. We thank Wolfgang Graulich for the production of the illustration (Fig. 1). The work was supported by IZKF BIOMAT (CB) and START (CW and MK) of the Faculty of Medicine, RWTH Aachen University as well as sponsored by B. Braun Melsungen AG (Germany).
Author information
Authors and Affiliations
Corresponding author
Additional information
Jon Dang and Lars-Ove Brandenburg contributed equally in this study.
Rights and permissions
About this article
Cite this article
Dang, J., Brandenburg, LO., Rosen, C. et al. Nrf2 Expression by Neurons, Astroglia, and Microglia in the Cerebral Cortical Penumbra of Ischemic Rats. J Mol Neurosci 46, 578–584 (2012). https://doi.org/10.1007/s12031-011-9645-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12031-011-9645-9