Abstract
Low levels of IgM auto-antibodies have been reported in health and disease. IgM anti-neutrophil cytoplasmic antibodies (ANCA) have been reported in patients with ANCA-associated vasculitis (AAV). We sought to investigate if healthy individuals may have IgM ANCA in their sera. The first aim of the study was to determine whether IgM ANCA was present in healthy individuals and in patients with ANCA-associated vasculitis. The second aim was to determine what happens to IgM ANCA levels over time. The third aim was to determine whether bacterial infections affected IgM ANCA levels in non-AAV patients. Sera from healthy individuals and patients with AAV were tested for IgM ANCA by immunofluorescence on fixed neutrophils, immunoprecipitation, Western blot and ELISA. Peripheral blood mononuclear cells were isolated and tested by ELISpot for circulating IgM ANCA B cells. To determine whether infection affected IgM ANCA levels, we studied non-AAV patients with bacterial endocarditis or Staphylococcus aureus bacteraemia and measured IgM ANCA levels over time. IgM ANCA is detectable in both healthy individuals and patients with AAV and the titres decreased with increasing age. Circulating IgM ANCA B cells were identified by ELISpot. In the presence of infection, we could not find a significant change in IgM ANCA levels. We report the presence of low-level specific IgM ANCA in the sera of healthy individuals and in patients with ANCA-associated vasculitis. Bacterial infection did not affect the level of IgM ANCA in this small study.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Anti-neutrophil cytoplasmic antibodies (ANCA)-associated vasculitis (AAV) is a necrotising vasculitis predominantly affecting small vessels. This disease is typically associated with autoreactive IgG ANCA to either myeloperoxidase (MPO-ANCA) associated with microscopic Polyangiitis (MPA) or proteinase-3 (PR3-ANCA) most often in association with Granulomatosis with Polyangiitis (GPA) [1]. In AAV, these antibodies are most commonly IgG ANCA, but occasionally IgA ANCA and IgM ANCA [2,3,4,5,6,7,8].
IgM ANCA has previously been described in association with disease, particularly in patients with AAV and alveolar haemorrhage [3, 5, 9]. The initial studies were descriptive collections of case studies in patients with systemic vasculitis and pulmonary haemorrhage [3, 5]. Investigators in the past had speculated that IgM ANCA may be related to delayed isotype switching to IgG ANCA [3, 5]. Most recently, Clain et al. tested for IgM PR3-ANCA in patients from two major AAV clinical trials [9]. They found that alveolar haemorrhage was nearly three times more frequent among those who tested positive for IgM PR3-ANCA. They speculated that the association of pulmonary haemorrhage and IgM PR3-ANCA may be linked by infection [9].
One of the most investigated associations between infection and AAV is with Staphylococcus aureus (S. aureus) [10]. There are reports of S. aureus infections including endocarditis and the subsequent development of either IgG ANCA or AAV [11, 12]. In patients with known AAV, different investigators have shown higher rates of relapse in AAV patients with chronic nasal carriage of S. aureus [13, 14, 28]. Furthermore, patients in remission were less likely to relapse if they received sulfamethoxazole and trimethoprim [15].
Chronic infections are also associated with the transient development of IgG ANCA including bacterial endocarditis [16,17,18,19,20,21,22]. The vast majority of these cases did not develop AAV disease [17, 19]. IgG ANCA has also been detected following bacterial, viral, protozoal and fungal infections [23,24,25,26]. The clinical significance of IgG ANCA in the presence of chronic or transient infection is uncertain in the absence of AAV. Indeed, low level and low affinity IgG ANCA has been reported in healthy individuals [27,28,29]. From the finding that IgG ANCA was present in healthy individuals, Cui et al speculated that IgM and IgA ANCA were also likely to be present as part of the normal repertoire [27].
Self-reactive antibodies (natural autoantibodies) are present in healthy individuals and perform an important role in the innate immune system [30]. Furthermore, not all autoantibodies are associated with disease [31, 32]. Natural autoantibodies (NAA) are present in healthy individuals [33, 34]; they are generally IgM immunoglobulins encoded by germline genes and display poly-reactivity but low affinity towards a wide range of self-antigens [33].
Given this context, the first aim of this study was to determine whether IgM ANCA to PR3 and MPO was present in the sera of healthy individuals and in patients with AAV in remission. The second aim was to determine what happens to IgM ANCA levels over time. The third aim was to determine whether bacterial infections affected IgM ANCA levels in non-AAV patients.
Materials and methods
AAV patients and healthy individuals recruited to study IgM ANCA
Adult healthy control individuals and AAV patients over 35 years of age were recruited to study IgM ANCA in human sera. Control individuals were excluded from recruitment if they had an autoimmune disease or were taking immunosuppressive medications. All AAV patients were required to be in complete remission as defined by the absence of clinical disease activity for at least 6 months prior to recruitment. Patients were eligible for recruitment if they were receiving maintenance immunosuppressive therapy. The AAV patients were divided by their IgG ANCA serotype into PR3-ANCA or MPO-ANCA. All participants had blood taken at baseline and the sera was stored at − 80 °C. Some healthy individuals had donated blood 12 years apart, and we made use of these stored sera for a longitudinal study of IgM ANCA.
Non-AAV patients with endocarditis and/or S. aureus bacteraemia
For the third part of our study, we recruited adult non-AAV patients admitted to hospital with S. aureus bacteraemia to study the effect of infection on IgM ANCA levels. Patients were eligible to enter the study if they fulfilled the modified Duke’s criteria for endocarditis [35]. We also recruited adult control individuals. Control individuals were excluded from recruitment if they had an autoimmune disease, were taking immunosuppressive medications or had evidence of an active infection. After consent was obtained, serum samples were collected at baseline and day 28 and stored at − 80 °C.
This study complies with the Declaration of Helsinki. Both the University of Adelaide and University of Tasmania ethics committees provided approval. All patients gave informed consent before enrolment and blood collection.
Enzyme-linked immunosorbent assay (ELISA)
The total serum IgM concentration of each sample was measured in duplicate by ELISA (Bethyl Laboratory). To reduce inter-individual variability, all serum samples were diluted to 20 μg/ml of total IgM using the Organtec ANCA kit sample diluent prior to testing for IgM ANCA. IgM and IgG to PR3 and MPO were measured using anti-MPO and anti-PR3 ELISA kits, respectively (Orgentec Diagnostika). To measure IgM ANCA (IgM PR3 and IgM MPO), the method was modified by using anti-human IgM antibodies specific for the Fc portion of the human IgM heavy chain labelled with horseradish peroxidase (Organtec Diagnostika). To exclude interference from endogenous myeloperoxidase, we compared secondary antibodies conjugated to either horseradish peroxidase or alkaline phosphatase. All ELISA plates were read at 640 nm for Quanti Blue (Invivogen) or 450 nm for TMB (Sigma). To avoid any false positive IgM ANCA results due to the presence of IgM rheumatoid factor, all serum samples were tested for the presence of IgM rheumatoid factor by nephelometry, and any positive sample was excluded from further testing. In order to compare OD values across the plates, the samples were run simultaneously with a positive and negative control on each ELISA plate.
For IgM PR3-ANCA and IgM MPO-ANCA, we defined the cut-off level as mean IgM ANCA OD value ± 1 standard deviation of the normal distribution found in healthy individuals. For the purposes of this report, levels above this cut-off were considered high and those below this cut-off were considered low.
Immunofluorescence and confocal microscopy of stained human neutrophils
Sera from five patients with PR3-AAV, five patients with MPO-AAV and ten healthy participants with known high levels of IgM PR3-ANCA or IgM MPO-ANCA as determined by ELISA were used to stain for neutrophil immunofluorescence (INOVA Diagnostics). Ethanol-fixed neutrophil slides (Immuno Concept) were incubated with serum diluted 1:50 for 1 h at room temperature in a humid chamber. The slides were washed 3 times in Tris-HCL buffer for 10 min each time. Secondary antibody anti-human IgM or IgG conjugated to Alexa 488 (Molecular Probes) was added for further 30 min and washed as above and prepared with mounting media (10% glycerol in PBS). Fluorescent cell staining was analysed using a Nikon fluorescent microscope.
Pre-absorption IgM MPO-ANCA
The pre-absorption studies were performed on the combined sera of healthy individuals (n = 10) that had previously tested high to either IgM MPO-ANCA or IgM PR3-ANCA by ELISA. One hundred microlitres of diluted (1:50) pooled serum was pre-incubated with 5 μg of either purified MPO, PR3 (both from Athens Research) or human serum albumin (CSL) for 30 min at room temperature, then centrifuged 20 × 103g for 10 min. These pre-treated sera were then tested by ELISA for IgM ANCA in four replicates.
Immunoprecipitation and Western blot
IgM ANCA immunoprecipitation was performed using anti-human IgM agarose beads (Sigma) to capture human IgM followed by incubation with ANCA antigens and immunoblotting. Fifty microlitres of the bead suspension was mixed with 300 μl of sera. Beads were incubated for 60 min at 4 °C. Beads were washed three times with 50 mM Tris-buffered saline (TBS) pH 7.4 prior to incubation with either 2 μg of MPO protein (Merck), 2 μg of PR3 protein (Wieslab), lysate of 10 × 106 neutrophils or lysate of 10 × 106 Jurkat cells. The mixture was incubated at 4 °C for 60 min. Beads were washed again in TBS. Twenty microlitres of SDS sample buffer with 0.25% 2-mercaptoethanol was added to the beads. Samples were heated at 70 °C for 10 min and proteins were separated by 12% SDS-PAGE. Proteins were transferred onto a PVDF membrane and blocked with PBS containing 2% skim milk and 0.02% Tween20 for 30 min. Membranes were probed with either anti-MPO rabbit polyclonal antibody diluted 1:1000 (Agilent) for 1 h, or anti-PR3 rabbit polyclonal antibody diluted 1:100 (kindly provided by Dr. Wieslander) overnight at 4 °C. Membranes were probed with mouse anti-rabbit antibody conjugated to alkaline phosphatase diluted 1:1000 (Rockland Immunochemicals). The membrane was developed with ECF luminescence substrate (Amersham Biosciences) and read in a fluorescence scanner (Typhoon™ 9410). To exclude non-specific interactions with cationic ANCA antigens, agarose anti-IgM beads were pre-treated with highly cationic poly-L-lysine prior to immunoprecipitation.
Peripheral blood mononuclear cell (PBMC) separation, culture and IgM enzyme-linked ImmunoSpot (ELISpot)
Buffy coats were obtained from ten healthy blood donors. PBMC separation from the buffy coat was performed by density gradient over Lymphoprep™ (Axis-Shield). After washing, cells were resuspended in culture media (RPMI 1640 supplemented with 10% foetal calf serum, 2 mM L-glutamine, 100 U/ml penicillin, 100 μg/ml gentamicin to a final concentration of 1 × 106 cells/ml). Once the PBMCs were suspended in media, B cells were then isolated by positive selection using anti-CD19 paramagnetic beads (Miltenyi Biotec). Isolated B cells were mixed with an equivalent number of cells from the B cell-depleted fraction of PBMCs. Cells were washed in complete media, adjusted to 2 × 106 cells/ml and cultured in the presence of CpGB 3.2 μg/ml (Geneworks) and IL-2 for 96 h at 37 °C in 5% CO2. In our previous work, we had shown that CpGB stimulated IgG ANCA production in patients with AAV [36]. A day before harvesting the cells, MultiScreen HTS 96-well plates (Merck) were activated with 15 μl of 70% methanol for 2 min and washed three times with endotoxin-free PBS. The wells were coated overnight with 100 μl of either polymorphonuclear or Jurkat cell lysates normalised to 20 μg/ml of protein or goat anti human IgM (Jackson ImmunoResearch) diluted 1:100 in carbonate/bicarbonate buffer, 0.15 M, pH 9.6.
In a separate experiment, plates were coated with of tetanus toxoid (TT) or 10 μg/ml of either PR3, MPO purified protein (Athens Research). The plates were washed and blocked with 100 μl of complete media and incubated for 90 min at 37 °C. Meanwhile, purified B cells from buffy coats were collected, washed four times in complete media and adjusted to a final cell density of 4 × 106 cells/ml and cultured with CpGB (Geneworks) for 7 days. One hundred microlitres per well of cells was placed in 96-well filter plates in triplicate and cultured for 18 h. Plates were washed with PBS, followed by PBS containing 0.05% Tween-20. Wells were incubated with 100 μl/well of goat anti-human IgM or IgG biotin conjugate (Jackson ImmunoResearch), diluted 1:5000 at room temperature for 2 h. Wells were washed, and 100 μl/well of alkaline phosphatase-conjugated streptavidin (Jackson ImmunoResearch) diluted 1:5000 was added and incubated for 2 h. Plates were washed and developed by adding 100 μl/well of BCIP/NBT Plus (Mabtech). The reaction was stopped at 8 min by rinsing the plate with running water. The wells were passed through an AID plate reader to determine the numbers of peripheral IgM and IgG ANCA positive B cells present (Autoimmun Diagnostika).
Inhibition of MPO peroxidase activity by serum
High through-put 384 wells (Sigma) were coated with 10 μg of purified human myeloperoxidase MPO protein (Athens Research) in carbonate/bicarbonate buffer, 0.15 M, pH 9.6, 25 μl per well and incubated over night at 4 °C. Plates were then washed twice with PBS containing 0.02% Tween 20, 100 μl per well, and blocked with PBS containing 1% human albumin (CSL), 30 μl per well for 30 min. Wells were washed 3× as above before adding 25 μl per well of the test serum, diluted 1:10 in PBS. Plates were incubated for 2 h at room temperature, washed 3× as above. Peroxidase activity was measured by adding 20 μl of TMB substrate and incubated for 1 h at 37 °C followed by adding 20 μl of 1 M phosphoric acid and read at 450 nm.
Statistical analysis
Statistical data analysis was carried out using Stata Software version 15.0. Student’s t tests and Chi-squared tests were used for all demographic comparisons. Scatterplots were used to compare each type of ANCA in the patient groups and healthy controls. Linear regression was used to estimate the difference in mean ANCA levels between each group, adjusted for age. Pearson’s correlation coefficient was used to determine whether there was a relationship between IgM MPO-ANCA, IgM PR3-ANCA and the corresponding IgG ANCA antigens. To compare IgM B cell numbers to different antigens in the ELISpot, we used a Wilcoxon matched-pairs signed-rank test.
To compare results in the infection groups, t tests were used to compare the mean ANCA levels. Multi-level-mixed-effects linear regression models with random intercepts and random slopes for individuals were used to estimate the mean changes in ANCA levels over time in each group, with time modelled as a continuous covariate (days since baseline) in the infection cohort. The mean changes over time for each group were calculated as the average daily change over time. For all statistical analyses, a p value of < 0.05 was considered significant.
Results
Demographics of the AAV patients and control individuals recruited to study IgM ANCA
The study recruited 45 healthy control individuals and 41 patients with AAV. There was no significant difference between the mean age of the AAV patients and the healthy individuals (p = 0.25) in this cohort. There were no significant differences in any of the other demographic variables (Table 1).
IgM ANCA is detectable in both healthy control individuals and in AAV patients
We were able to detect IgM ANCA to both MPO and PR3 in control individuals and in AAV patients who were in remission by ELISA (Fig. 1a and b). Healthy control individuals, PR3-AAV and MPO-AAV patients all showed detectable levels of IgM PR3-ANCA and IgM MPO-ANCA. There was no significant difference in the IgM PR3-ANCA titres between control individuals and PR3-AAV patients (p = 0.38) and MPO-AAV patients (p = 0.57). Similarly, there was no significant difference in the IgM MPO-ANCA titres between control individuals and MPO-AAV patients (p = 0.11) and PR3-AAV patients (p = 0.25). We found a significant relationship between increasing age and declining IgM ANCA level for both IgM PR3-ANCA (p = 0.001) and IgM MPO-ANCA (p = 0.001) among the populations studied (Fig. 1c).
IgM ANCA levels in healthy individuals, PR3-AAV patients and MPO-AAV patients. The values for IgM to PR3-ANCA and MPO-ANCA are given in OD units. a, b. There was no significant difference in IgM ANCA levels in any of the groups compared. c IgM-MPO ANCA declined by 0.002 OD 450 nm per year (p = 0.001) and IgM PR3-ANCA decreased by 0.004 OD 450 nm per year (p = 0.001). d, e Longitudinal data shown for each individual (n = 5). Neg Control = negative control OD value of secondary conjugate only.
There was no statistically significant correlation between IgM MPO-ANCA and IgG MPO-ANCA in MPO-AAV patients (p = 0.72). There was no statistically significant correlation between IgM PR3-ANCA and IgG PR3-ANCA in PR3-AAV patients (p = 0.70).
Longitudinal cohort of healthy individuals over 12 years
There were five healthy individuals whose sera had been collected and stored in our laboratory on two different occasions separated by 12 years apart. The group was too small to perform any statistical analysis. Descriptively, all participants’ IgM PR3-ANCA and IgM MPO-ANCA decreased over time (Fig. 1d and e). There was a single individual in whom the IgM PR3-ANCA increased slightly over time. The mean IgM PR3-ANCA decreased at an average rate of 0.008 OD/year and the IgM MPO-ANCA decreased at an average of 0.007 OD/year.
Specificity of binding of IgM ANCA antibodies
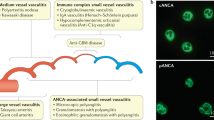
To further investigate the specificity of IgM ANCA in healthy individuals, a series of experiments was performed to probe the binding of IgM ANCA antibodies. We found that healthy individual’s and AAV patient’s sera contained IgM antibodies that were capable of staining neutrophils by immunofluorescence by varying intensities (Fig. 2). Staining of ethanol-fixed neutrophils showed the expected perinuclear staining for IgG MPO-ANCA (Fig. 2a) and the cytoplasmic pattern for IgG PR3-ANCA (Fig. 2c). In healthy controls, there is staining by IgM ANCA (Fig. 2f and h) although the pattern is not as well defined as that for IgG ANCA towards MPO and PR3.
Immunofluoresence and confocal microscopy of stained human neutrophils. Representative examples of ethanol-fixed neutrophils stained by serum from a MPO-AAV patient (a, b), a PR3-AAV patient (c, d) and healthy individuals (e–h). The presence of IgG-ANCA in a, c or IgM-ANCA in b, d, f and h was tested for by using either anti-human IgG or IgM conjugated with Alexa 488 (green)
Pre-absorption of serum with purified MPO reduced the ELISA reactivity towards MPO by IgM MPO-ANCA but did not affect the reactivity towards PR3 by IgM PR3-ANCA (Fig. 3a). Conversely, pre-absorption with PR3 reduced the reactivity towards PR3 by IgM PR3-ANCA but did not affect the reactivity towards MPO by IgM MPO-ANCA (Fig. 3a).
ELISA, immunoprecipitation and ELISpot to determine whether serum IgM-ANCA from healthy individuals is capable of binding neutrophil antigens specifically. a Prior to undergoing IgM ANCA ELISA, pooled serum from healthy individuals (n = 10) with either high IgM MPO-ANCA or high IgM PR3-ANCA was pre-absorbed with 5 μg of either albumin (Alb), MPO or PR3. The results showed antigen-specific absorption indicating antigen-specific binding of IgM ANCA. b Serum from a healthy individual with high IgM MPO-ANCA by ELISA is capable of immunoprecitipating MPO from PMN lysate and native MPO protein (lanes 2 and 5) but not Jurkat cell lysate which lacks MPO (lane 3). b Anti-IgM agarose beads were loaded with IgM from 2 healthy individuals (one with high level IgM MPO-ANCA in lane 1 and one with low level IgM MPO-ANCA in lane 2), IgM from 2 MPO-AAV patients (lanes 3 and 4) and IgM from two IgM-myeloma patients (lanes 5 and 6). A weak band was evident in lane 1 from the individual with high IgM MPO-ANCA. MPO-AAV patients in lanes 3 and 4, both of whom had much higher IgM MPO-ANCA by ELISA compared to healthy individuals, immunoprecipitated much more MPO, IgM from IgM-myeloma patients failed to immunoprecipitate MPO. d Similarly, beads loaded with IgM from three different healthy individuals with high levels of anti-PR3 IgM by ELISA were able to immunoprecipitate purified PR3 protein. e Pre-treatment with poly-L-lysine (PLL) failed to completely abrogate the capacity of serum to immunoprecipitate MPO or PR3 antigens. f IgM ELISpot of PBMC from normal individuals demonstrate the presence of higher number of circulating IgM-producing cells recognizing antigens in neutrophil lysate compared to Jurkat lysate (p = 0.05)
We performed sequential immunoprecipitation followed by immunoblotting to determine if serum IgM antibodies were capable of binding their target antigens. Serum from a healthy individual with high IgM MPO-ANCA was able to immunoprecipitate MPO when mixed with either myeloperoxidase alone or polymorphonuclear cell lysate containing MPO, but not Jurkat cell lysate which did not contain MPO (Fig. 3b).
To exclude non-specific binding of IgM towards MPO, we coated anti-IgM beads with serum containing paraprotein from two IgM myeloma patients. These sera failed to immunoprecipitate MPO despite high levels of total IgM (Fig. 3c lanes 5 and 6). A weak band was evident in the healthy individual with high IgM MPO-ANCA (Fig. 3c lane 1). Two MPO-AAV patients, who had much higher IgM MPO-ANCA by ELISA compared to healthy individuals, immunoprecipitated much more MPO (Fig. 3c lanes 3 and 4). Beads coated with sera from three healthy individuals who had tested high for IgM PR3-ANCA on ELISA also immunoprecipitated purified PR3 (Fig. 3d). Pre-treatment with poly-L-lysine failed to completely abrogate serum IgM binding to MPO and PR3, indicating that the binding of IgM to MPO and PR3 could not have occurred entirely via non-specific charge interaction (Fig. 3e).
Results from the ELISpot data showed that there were significantly more B cells that were detectable by the plate reader in association with polymorphonuclear lysate than compared to Jurkat lysate (p = 0.05) (Fig. 3f). In order to detect low level of ANCA reactive B cells, we stimulated PBMCs with CpGB (TLR9 ligand) prior to the ELISpot assay. We could easily detect circulating IgM-producing B cells with reactivity towards MPO, PR3 and TT in healthy individuals. Of interest, we also detected very low levels of IgG-producing B cells with reactivity towards the same antigens (Suppl Fig. 1).
Serum inhibits the peroxidase activity of MPO
We wanted to explore the potential physiological function of IgM ANCA. In this regard, we tested the peroxidase activity of plate-bound MPO in the presence of serum containing varying amount of IgM ANCA. We found that serum with high level of IgM-ANCA had a greater inhibitory effect on MPO peroxidase activity compared to serum with a low level of IgM-ANCA (Suppl Fig. 2).
IgM ANCA infection cohort
Demographics of the non-AAV patients with endocarditis and/or S. aureus bacteraemia
There were 27 non-AAV patients with bacterial infection eligible to participate in this study. Of these 27 individuals, 19 gave informed consent, of whom ten had bacterial endocarditis and nine had S. aureus bacteraemia. We obtained 11-paired samples from these non-AAV patients at baseline and at follow-up ranging between days 20 and 42. A total of six of the non-AAV patients died and one patient with bacteraemia withdrew consent. We also studied ten healthy individuals as a comparison group. The causative organisms, type of infection and demographic details of the non-AAV patients are listed in Table 2.
IgM PR3 and IgM MPO in non-AAV patients with bacterial infection
At baseline, there was no significant difference in either IgM PR3-ANCA or IgM MPO-ANCA levels between the healthy individuals, patients with bacteraemia or endocarditis (Fig. 4a and b). We used a multi-level mixed-effects linear regression model that showed that on average, there was a slight decrease in IgM PR3-ANCA and IgM MPO-ANCA levels over time in patients with either bacteraemia or endocarditis; however, this was not statistically significant. When the groups with endocarditis and bacteraemia were combined as a group, there also was no significant change in IgM PR3-ANCA or IgM MPO-ANCA over the study period. There was also no mean change in IgM ANCA levels in healthy individuals over time. None of the non-AAV patients with bacterial infection developed IgG ANCA or AAV disease.
Study of serum IgM ANCA in the course of bacterial infection IgM ANCA levels at day 1 and follow-up at days 20–42 in healthy individuals and those with bacteraemia and endocarditis. a, b The median values and range of ANCA levels in each of the three groups at baseline and days 20–42 are shown in the box and whiskers graph where the top of the box represents the 75th percentile, the middle line the median value and the lowest line the 25th percentile
Discussion
In this study, we have demonstrated the presence of IgM MPO-ANCA and IgM PR3-ANCA in control individuals and in AAV patients in remission. We have shown by different experimental methods that IgM MPO-ANCA and IgM PR3-ANCA are antigen-specific. The level of IgM ANCA did not change in association with bacterial infection.
The finding of IgM ANCA antibodies in control individuals, as well as patients with AAV, is in keeping with animal studies that have supported the possibility of IgM ANCA being part of the normal repertoire. Vittecoq et al studied IgM ANCA in two strains of lupus-prone mice [37]. They found IgM polyclonal anti-MPO antibodies to be antigen-specific in the sera of both mice strains. The authors speculated that this autoantibody population of IgM MPO-ANCA emerged from natural autoantibodies in these murine populations [37].
The level of IgM PR3-ANCA and IgM MPO-ANCA declined with age in all groups studied. Other studies in both humans and animals have also shown a decline in IgM natural autoantibodies with age as reported by Lacroix-Desmazes et al. [38]. This is in keeping with other studies that reported that natural autoantibody levels decrease with age [38,39,40].
We found evidence of peripherally circulating IgM B cells in healthy individuals that recognised MPO and PR3 antigens. This was consistent with our findings of specific IgM MPO-ANCA and IgM PR3-ANCA as demonstrated by ELISA. IgM ANCA may perform a regulatory function to neutralise free ANCA antigens such as MPO in the circulation released from apoptotic neutrophils. The ability of IgM MPO-ANCA in healthy individuals to stain neutrophils, to inhibit the peroxidase function of MPO and to immuno-precipitate MPO supports this possibility.
The removal of circulating MPO by IgM MPO-ANCA could also be of major importance to prevent MPO-derived oxidation and its deleterious consequences [41, 42]. van Leeuwen et al have shown in a mouse model that passive immunisation with a natural IgM antibody directed to HOCl-oxLDL could reduce atherosclerotic plaque development [43]. For PR3, PR3-SERPINA1 system is efficient at mopping up excess PR3, whereas free MPO may be reliant on IgM-MPO ANCA to inactivate the free enzyme [44, 45]. These possibilities regarding the role of IgM MPO-ANCA warrant further investigation.
Several groups have reported IgM ANCA in patients with active AAV [3, 9]. More recently, Clain et al hypothesised that infection could have triggered the production of IgM PR3-ANCA. Given the long-held suspicion of infection acting as a trigger for production of ANCA, and given our confirmation of IgM ANCA in healthy individuals, we specifically looked for changes in the level of IgM ANCA in patients without AAV and with serious bacterial infections. We were unable to demonstrate any significant change in IgM ANCA level in the presence of bacterial endocarditis or S. aureus bacteraemia. Larger studies are also needed to examine IgM ANCA and infection more comprehensively. Of interest, none of our non-AAV patients with S. aureus endocarditis went on to developed IgG ANCA or AAV during the period of follow-up. Future studies could compare the IgG ANCA in patients with endocarditis to those with AAV.
The physiological role of IgM ANCA is not known. We note that the fall in IgM ANCA titre with age among healthy individuals, as demonstrated by this study, coincides with the onset of AAV among older individuals. We wonder whether this fall in physiological levels of IgM ANCA may predispose to AAV disease onset.
Several authors have proposed that IgM natural autoantibodies may have a role in maintaining immunological homeostasis and prevent autoimmunity [32, 46,47,48]. However, the precise immunogenic relationship between germline-encoded protective natural IgM and pathogenic IgG in autoimmune pathogenesis is still poorly understood [32]. Potentially, IgM ANCA in health and remission may play a role in the regulation of the pathogenic IgG ANCA response. Jayne et al. proposed the importance of IgM in the regulation of IgG ANCA response when studying the role of intravenous immunoglobulin in the treatment of AAV [49]. Rossi et al. showed that the sera of patients in remission from vasculitis contained ANCA anti-idiotypic antibodies of IgG and IgM class which inhibited the binding of ANCA (from acute sera) to neutrophil antigens [50]. Potentially, IgM ANCA may also inhibit the binding of IgG ANCA to neutrophil surface antigens thereby preventing neutrophil activation and the enzyme release cascade that can cause tissue damage. Franssen et al. postulated that elevated IgG MPO-ANCA may play a pathophysiologic role in the process of glomerulosclerosis and progressive chronic kidney disease [51].
There are several limitations to our study. The study sample size is small; however, it is an age-matched population and it is representative of the AAV population. In relation to non-AAV patients with infection, the sample size was small and our study may have been underpowered to detect a real change in IgM ANCA levels with infection. For the infection study, not all samples were adequately paired because several patients had succumbed to their illness. In relation to the characteristics of IgM ANCA, a shortcoming of our study is that we did not examine the affinity and epitope specificity of these antibodies in healthy individuals compared to AAV patients and non-AAV patients with infections. Lastly, all the AAV patients studied here had been in remission. It would be relevant to also measure IgM-ANCA in patients with active AAV disease.
IgM ANCA has been associated with pulmonary haemorrhage in patients with AAV. Cambridge and colleagues reported that the variable region of the gene encoding monoclonal IgM ANCA derived from a patient with AAV had undergone antigen-driven response away from the germ line sequence [52]. These reports suggest that in some instance, IgM ANCA may be qualitatively different to the IgM ANCA found in health. Therefore, it is important to understand the regulation of IgM ANCA production in health, and the factors that may be responsible for IgM affinity maturation and possible class switching in disease. Further investigations are needed to determine the origin, avidity, binding affinity and epitope specificity of IgM ANCA in both health and in disease.
Conclusions
We have confirmed that normal healthy individuals and patients with AAV in remission have antigen-specific IgM ANCA. The IgM ANCA levels did not change following bacterial infection, but does decline with age in all groups studied. Further investigation is required to determine the role of IgM ANCA in health and AAV.
References
Jennette JC, Falk RJ, Bacon PA, Basu N, Cid MC, Ferrario F, et al. 2012 revised international Chapel Hill consensus conference nomenclature of Vasculitides. Arthritis Rheum. 2013;65(1):1–11. https://doi.org/10.1002/art.37715.
Kelley JM, Monach PA, Ji C, Zhou Y, Wu J, Tanaka S, et al. IgA and IgG antineutrophil cytoplasmic antibody engagement of fc receptor genetic variants influences granulomatosis with polyangiitis. Proc Natl Acad Sci U S A. 2011;108(51):20736–41. https://doi.org/10.1073/pnas.1109227109.
Esnault VL, Soleimani B, Keogan MT, Brownlee AA, Jayne DR, Lockwood CM. Association of IgM with IgG ANCA in patients presenting with pulmonary hemorrhage. Kidney Int. 1992;41(5):1304–10.
Esnault VL, Ronda N, Jayne DR, Lockwood CM. Association of ANCA isotype and affinity with disease expression. J Autoimmun. 1993;6(2):197–205. https://doi.org/10.1006/jaut.1993.1017.
Jayne DR, Jones SJ, Severn A, Shaunak S, Murphy J, Lockwood CM. Severe pulmonary hemorrhage and systemic vasculitis in association with circulating anti-neutrophil cytoplasm antibodies of IgM class only. Clin Nephrol. 1989;32(3):101–6.
Sandin C, Eriksson P, Segelmark M, Skogh T, Kastbom A. IgA- and SIgA anti-PR3 antibodies in serum versus organ involvement and disease activity in PR3-ANCA-associated vasculitis. Clin Exp Immunol. 2016;184(2):208–15. https://doi.org/10.1111/cei.12769.
Nassberger L, Sjoholm AG, Bygren P, Thysell H, Hojer-Madsen M, Rasmussen N. Circulating anti-neutrophil cytoplasm antibodies in patients with rapidly progressive glomerulonephritis and extracapillary proliferation. J Intern Med. 1989;225(3):191–6.
Shida H, Nakazawa D, Tateyama Y, Miyoshi A, Kusunoki Y, Hattanda F, et al. The presence of anti-Lactoferrin antibodies in a subgroup of eosinophilic granulomatosis with Polyangiitis patients and their possible contribution to enhancement of neutrophil extracellular trap formation. Front Immunol. 2016;7:636. https://doi.org/10.3389/fimmu.2016.00636.
Clain JM, Hummel AM, Stone JH, Fervenza FC, Hoffman GS, Kallenberg CG, et al. Immunoglobulin (Ig) M antibodies to proteinase 3 in granulomatosis with polyangiitis and microscopic polyangiitis. Clin Exp Immunol. 2017;188(1):174–81. https://doi.org/10.1111/cei.12925.
Stegeman CA, Tervaert JW, Sluiter WJ, Manson WL, de Jong PE, Kallenberg CG. Association of chronic nasal carriage of Staphylococcus aureus and higher relapse rates in Wegener granulomatosis. Ann Intern Med. 1994;120(1):12–7.
Miranda-Filloy JA, Veiga JA, Juarez Y, Gonzalez-Juanatey C, Gonzalez-Gay MA, Garcia-Porrua C. Microscopic polyangiitis following recurrent Staphylococcus aureus bacteremia and infectious endocarditis. Clin Exp Rheumatol. 2006;24(6):705–6.
Kasmani R, Okoli K, Naraharisetty K, Gunning W, Shapiro JI, Ratnam S. Microscopic polyangiitis triggered by recurrent methicillin-resistant Staphylococcus aureus bacteremia. Int Urol Nephrol. 2010;42(3):821–4. https://doi.org/10.1007/s11255-009-9652-8.
Zycinska K, Wardyn KA, Zielonka TM, Demkow U, Traburzynski MS. Chronic crusting, nasal carriage of Staphylococcus aureus and relapse rate in pulmonary Wegener's granulomatosis. J Physiol Pharmacol. 2008;59(Suppl 6):825–31.
Salmela A, Rasmussen N, Tervaert JWC, Jayne DRW, Ekstrand A, European Vasculitis Study G. Chronic nasal Staphylococcus aureus carriage identifies a subset of newly diagnosed granulomatosis with polyangiitis patients with high relapse rate. Rheumatology (Oxford). 2017;56(6):965–72. https://doi.org/10.1093/rheumatology/kex001.
Stegeman CA, Tervaert JW, de Jong PE, Kallenberg CG. Trimethoprim-sulfamethoxazole (co-trimoxazole) for the prevention of relapses of Wegener's granulomatosis. Dutch co-Trimoxazole Wegener Study group. N Engl J Med. 1996;335(1):16–20.
Satoskar AA, Suleiman S, Ayoub I, Hemminger J, Parikh S, Brodsky SV, et al. Staphylococcus infection-associated GN - Spectrum of IgA staining and prevalence of ANCA in a single-center cohort. Clin J Am Soc Nephrol. 2017;12(1):39–49. https://doi.org/10.2215/CJN.05070516.
Ying CM, Yao DT, Ding HH, Yang CD. Infective endocarditis with antineutrophil cytoplasmic antibody: report of 13 cases and literature review. PLoS One. 2014;9(2):e89777. https://doi.org/10.1371/journal.pone.0089777.
Mahr A, Batteux F, Tubiana S, Goulvestre C, Wolff M, Papo T, et al. Brief report: prevalence of antineutrophil cytoplasmic antibodies in infective endocarditis. Arthritis Rheumatol. 2014;66(6):1672–7. https://doi.org/10.1002/art.38389.
Bonaci-Nikolic B, Andrejevic S, Pavlovic M, Dimcic Z, Ivanovic B, Nikolic M. Prolonged infections associated with antineutrophil cytoplasmic antibodies specific to proteinase 3 and myeloperoxidase: diagnostic and therapeutic challenge. Clin Rheumatol. 2010;29(8):893–904. https://doi.org/10.1007/s10067-010-1424-4.
Medina F, Camargo A, Moreno J, Zonana-Nacach A, Aceves-Avila J, Fraga A. Anti-neutrophil cytoplasmic autoantibodies in leprosy. Br J Rheumatol. 1998;37(3):270–3.
Efthimiou J, Spickett G, Lane D, Thompson A. Antineutrophil cytoplasmic antibodies, cystic fibrosis, and infection. Lancet. 1991;337(8748):1037–8.
Boils CL, Nasr SH, Walker PD, Couser WG, Larsen CP. Update on endocarditis-associated glomerulonephritis. Kidney Int. 2015;87(6):1241–9. https://doi.org/10.1038/ki.2014.424.
Hermann J, Demel U, Stunzner D, Daghofer E, Tilz G, Graninger W. Clinical interpretation of antineutrophil cytoplasmic antibodies: parvovirus B19 infection as a pitfall. Ann Rheum Dis. 2005;64(4):641–3.
Yahya TM, Benedict S, Shalabi A, Bayoumi R. Anti-neutrophil cytoplasmic antibody (ANCA) in malaria is directed against cathepsin G. Clin Exp Immunol. 1997;110(1):41–4.
Esquivel-Valerio JA, Flores-Suarez LF, Rodriguez-Amado J, Garza-Elizondo MA, Rendon A, Salinas-Carmona MC. Antineutrophil cytoplasm autoantibodies in patients with tuberculosis are directed against bactericidal/permeability increasing protein and are detected after treatment initiation. Clin Exp Rheumatol. 2010;28(1 Suppl 57):35–9.
Asano S, Mizuno S, Okachi S, Aso H, Wakahara K, Hashimoto N, et al. Antineutrophil cytoplasmic antibody-associated Vasculitis superimposed on infection-related glomerulonephritis secondary to pulmonary Mycobacterium avium complex infection. Intern Med. 2016;55(17):2439–45. https://doi.org/10.2169/internalmedicine.55.6588.
Cui Z, Zhao MH, Segelmark M, Hellmark T. Natural autoantibodies to myeloperoxidase, proteinase 3, and the glomerular basement membrane are present in normal individuals. Kidney Int. 2010;78(6):590–7. https://doi.org/10.1038/ki.2010.198.
Xu PC, Cui Z, Chen M, Hellmark T, Zhao MH. Comparison of characteristics of natural autoantibodies against myeloperoxidase and anti-myeloperoxidase autoantibodies from patients with microscopic polyangiitis. Rheumatology (Oxford). 50(7):1236–43. https://doi.org/10.1093/rheumatology/ker085.
Mathieson PW, Lockwood CM, Oliveira DB. T and B cell responses to neutrophil cytoplasmic antigens in systemic vasculitis. Clin Immunol Immunopathol. 1992;63(2):135–41.
Avrameas S, Guilbert B, Mahana W, Matsiota P, Ternynck T. Recognition of self and non-self constituents by polyspecific autoreceptors. Int Rev Immunol. 1988;3(1–2):1–15.
Avrameas S. Natural autoantibodies: from 'horror autotoxicus' to 'gnothi seauton'. Immunol Today. 1991;12(5):154–9. https://doi.org/10.1016/S0167-5699(05)80045-3.
Gronwall C, Silverman GJ. Natural IgM: beneficial autoantibodies for the control of inflammatory and autoimmune disease. J Clin Immunol. 2014;34(Suppl 1):S12–21. https://doi.org/10.1007/s10875-014-0025-4.
Coutinho A, Kazatchkine MD, Avrameas S. Natural autoantibodies. Curr Opin Immunol. 1995;7(6):812–8.
Lacroix-Desmazes S, Kaveri SV, Mouthon L, Ayouba A, Malanchere E, Coutinho A, et al. Self-reactive antibodies (natural autoantibodies) in healthy individuals. J Immunol Methods. 1998;216(1–2):117–37.
Li JS, Sexton DJ, Mick N, Nettles R, Fowler VG Jr, Ryan T, et al. Proposed modifications to the Duke criteria for the diagnosis of infective endocarditis. Clin Infect Dis. 2000;30(4):633–8. https://doi.org/10.1086/313753.
Hurtado PR, Jeffs L, Nitschke J, Patel M, Sarvestani G, Cassidy J, et al. CpG oligodeoxynucleotide stimulates production of anti-neutrophil cytoplasmic antibodies in ANCA associated vasculitis. BMC Immunol. 2008;9:34.
Vittecoq O, Brard F, Jovelin F, Le Loet X, Tron F, Gilbert D. IgM anti-myeloperoxidase antibody-secreting lymphocytes are present in the peripheral repertoire of lupus mice but rarely differentiate into IgG-producing cells. Clin Exp Immunol. 1999;118(1):122–30.
Lacroix-Desmazes S, Mouthon L, Kaveri SV, Kazatchkine MD, Weksler ME. Stability of natural self-reactive antibody repertoires during aging. J Clin Immunol. 1999;19(1):26–34.
Simell B, Lahdenkari M, Reunanen A, Kayhty H, Vakevainen M. Effects of ageing and gender on naturally acquired antibodies to pneumococcal capsular polysaccharides and virulence-associated proteins. Clin Vaccine Immunol. 2008;15(9):1391–7. https://doi.org/10.1128/CVI.00110-08.
Griffin DO, Holodick NE, Rothstein TL. Human B1 cells in umbilical cord and adult peripheral blood express the novel phenotype CD20+ CD27+ CD43+ CD70. J Exp Med. 2011;208(1):67–80. https://doi.org/10.1084/jem.20101499.
Karakas M, Koenig W, Zierer A, Herder C, Rottbauer W, Baumert J, et al. Myeloperoxidase is associated with incident coronary heart disease independently of traditional risk factors: results from the MONICA/KORA Augsburg study. J Intern Med. 2012;271(1):43–50. https://doi.org/10.1111/j.1365-2796.2011.02397.x.
Zhang R, Brennan ML, Fu X, Aviles RJ, Pearce GL, Penn MS, et al. Association between myeloperoxidase levels and risk of coronary artery disease. JAMA. 2001;286(17):2136–42.
van Leeuwen M, Kemna MJ, de Winther MP, Boon L, Duijvestijn AM, Henatsch D, et al. Passive immunization with hypochlorite-oxLDL specific antibodies reduces plaque volume in LDL receptor-deficient mice. PLoS One. 2013;8(7):e68039. https://doi.org/10.1371/journal.pone.0068039.
Duranton J, Bieth JG. Inhibition of proteinase 3 by [alpha]1-antitrypsin in vitro predicts very fast inhibition in vivo. Am J Respir Cell Mol Biol. 2003;29(1):57–61. https://doi.org/10.1165/rcmb.2002-0258OC.
Baslund B, Petersen J, Permin H, Wiik A, Wieslander J. Measurements of proteinase 3 and its complexes with alpha 1-proteinase inhibitor and anti-neutrophil cytoplasm antibodies (ANCA) in plasma. J Immunol Methods. 1994;175(2):215–25.
Lobo PI. Role of natural autoantibodies and natural IgM anti-leucocyte autoantibodies in health and disease. Front Immunol. 2016;7:198. https://doi.org/10.3389/fimmu.2016.00198.
Silosi I, Silosi CA, Boldeanu MV, Cojocaru M, Biciusca V, Avramescu CS, et al. The role of autoantibodies in health and disease. Romanian J Morphol Embryol. 2016;57(2 Suppl):633–8.
Boes M, Schmidt T, Linkemann K, Beaudette BC, Marshak-Rothstein A, Chen J. Accelerated development of IgG autoantibodies and autoimmune disease in the absence of secreted IgM. Proc Natl Acad Sci U S A. 2000;97(3):1184–9.
Jayne DR, Esnault VL, Lockwood CM. ANCA anti-idiotype antibodies and the treatment of systemic vasculitis with intravenous immunoglobulin. J Autoimmun. 1993;6(2):207–19. https://doi.org/10.1006/jaut.1993.1018.
Rossi F, Jayne DR, Lockwood CM, Kazatchkine MD. Anti-idiotypes against anti-neutrophil cytoplasmic antigen autoantibodies in normal human polyspecific IgG for therapeutic use and in the remission sera of patients with systemic vasculitis. Clin Exp Immunol. 1991;83(2):298–303.
Franssen CF, Stegeman CA, Oost-Kort WW, Kallenberg CG, Limburg PC, Tiebosch A, et al. Determinants of renal outcome in anti-myeloperoxidase-associated necrotizing crescentic glomerulonephritis. J Am Soc Nephrol. 1998;9(10):1915–23.
Longhurst C, Ehrenstein MR, Leaker B, Stevenson FK, Spellerberg M, Chapman C, et al. Analysis of immunoglobulin variable region genes of a human IgM anti-myeloperoxidase antibody derived from a patient with vasculitis. Immunology. 1996;87(2):334–8.
Exley AR, Bacon PA, Luqmani RA, Kitas GD, Gordon C, Savage CO, et al. Development and initial validation of the Vasculitis damage index for the standardized clinical assessment of damage in the systemic vasculitides. Arthritis Rheum. 1997;40(2):371–80.
Acknowledgements
We acknowledge the support from the Royal Adelaide Hospital Research Committee. We also thank the generosity of patients and healthy individuals who participated in this study. Thank you to Dr J Weislander of Department of Autoimmunology, Statens Seruminstitut, Copenhagen, Denmark for the gift of anti-PR3 rabbit polyclonal antibody.
Funding
This work was supported by the Royal Adelaide Hospital Renal research fund and the Royal Hobart Hospital Renal research fund.
Author information
Authors and Affiliations
Contributions
PRH, LJ and CAP conceived the study, performed the experiments and wrote the ethics applications.
PRH, AN, PT, ED, GBP, LJ and CAP assisted in patient sample collection and processing.
AN, PT, ED assisted with patient identification and sample collection.
PRH and KC created all figures.
KC performed all statistical analysis.
LJ wrote the manuscript draft.
All authors edited and contributed to the final draft.
Corresponding author
Ethics declarations
This study complies with the Declaration of Helsinki. Both the University of Adelaide and University of Tasmania ethics committees provided approval. All patients gave informed consent before enrolment and blood collection.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jeffs, L., Peh, C., Nelson, A. et al. IgM ANCA in healthy individuals and in patients with ANCA-associated vasculitis. Immunol Res 67, 325–336 (2019). https://doi.org/10.1007/s12026-019-09091-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12026-019-09091-x